Totally Endoscopic (Thoracoscopic and Laparoscopic) Radical Esophagectomy with
|
|
|
- Anissa Berry
- 5 years ago
- Views:
Transcription
1 Surgical Science, 2014, 5, Published Online May 2014 in SciRes. Totally Endoscopic (Thoracoscopic and Laparoscopic) Radical Esophagectomy with Gastric Tube Reconstruction through a Small Neck Incision: An Early Experience with Thirty Egyptian Patients Adel Denewer *, Adel Fathi, Ahmed Setit, Mohamed Hegazy, Ashraf Khater, Osama Hussein, Sameh Roshdy, Fayez Shahatto, Fathy Denewer Department of Surgical Oncology, Oncology Center (OCMU), Faculty of Medicine, Mansoura University, Mansoura, Egypt * adeldenewer@mans.edu.eg Received 11 March 2014; revised 10 April 2014; accepted 17 April 2014 Copyright 2014 by authors and Scientific Research Publishing Inc. This work is licensed under the Creative Commons Attribution International License (CC BY). Abstract Background: Minimally invasive esophagectomy nowadays is replacing the classic open technique. Additional studies are needed to confirm its safety and efficacy. Methods: thirty patients with esophageal carcinoma were enrolled in this study. Patients were evaluated preoperatively and they underwent thoracoscopic and laparoscopic procedures for assessment of resectability. Resectablepatients underwent radical esophagectomy with gastric tube reconstruction through a four-cm neck incision. Results: 17 patients were operable and 13 patients were inoperable. The mean operative time for the whole procedure was 5.97 ± 1.66 hours. The mean blood loss was 250 ± cc. The mean overall hospital stay was ± 5.49 daysdays. Common postoperative complications included pneumonia (13.3%) pleural effusion (6.7%), cervical anastomotic leakage (10%), and wound infection (13.3%). One patient died in the early postoperative period. Conclusions: we conclude that totallyendoscopic (thoracoscopic and laparoscopic) esophagectomy is feasible and relatively safe technique. Beside its efficacy as an assessment tool, total esophagectomy and lymphadenectomy could be performed in the same time. Keywords Thoracoscopic, Laparoscopic, Radical Esophagectomy, Gastric Reconstruction, Esophagus Cancer * Corresponding author. How to cite this paper: Denewer, A., et al. (2014) Totally Endoscopic (Thoracoscopic and Laparoscopic) Radical Esophagectomy with Gastric Tube Reconstruction through a Small Neck Incision: An Early Experience with Thirty Egyptian Patients. Surgical Science, 5,
2 1. Background Esophageal cancer is the 8th most common cancer and the 4th most common gastrointestinal malignancy. It is 6th leading cause of cancer deaths worldwide [1]. The incidence of the esophageal cancer has been increased over the past 3 decades [2]. In the United States and the western world, this profound increase has been due to the increase in the incidence of adenocarcinoma of the esophagus. This major epidemiologic shift is thought to be related to gastroesophageal reflux disease, obesity, and Barrett s esophagus, the dominant risk factors for esophageal adenocarcinoma [2] [3]. The highest incidence rates are found in Asia and Sub-Saharan Africa and the lowest rates are found in Europe and North America. Generally, rates are much higher in men than in women [1]. Radical surgery currently offers the most realistic chance of cure from cancer of the esophagus when spread beyond the most superficial epithelial layers but not extending beyond the locoregional lymph nodes [4]. Although the efficacy of esophagectomy with extended lymphadenectomy remains to be proven by a prospective randomized study, some reports have shown that better survival could be obtained after extended rather than conventional lymphadenectomy [5]. The use of thoracoscopy and/or laparoscopy for esophageal resection was introduced in 1992 by Cushieri et al., aiming to further reduce pulmonary morbidity while potentially improving the oncological quality of the resection by enhancing visual control during the mediastinal dissection [6]. Over the last two decades, minimally invasive approaches have been described in several studies as a procedure for the treatment of both benign and malignant diseases that seems equivalent to the standard open esophagectomy [7] [8]. However, it is still considered one of the most complex surgical procedures, and many questions still remain unanswered regarding the oncologic results [9]. As the data about endoscopic esophagectomy are lacking among Egyptian in cancer patients, the aim of the current study is to assess the feasibility and oncological efficacy of thoracoscopically assisted esophagectomy in the management of esophageal cancer patients in a specialized oncology Center in North of Egypt. 2. Methods 2.1. Setting This study was conducted at the Surgical Oncology Unit, Oncology Centre, Mansoura University (OCMU) during the period between August 2010 and October Population Thirty patients with esophageal carcinoma were enrolled in this study. All patients were investigated preoperatively by clinical history and physical examination; Computed Tomography (CT) of the chest, abdomen and pelvis (Brilliance CT 64 slice Philips Netherlands 2005); barium swallow; endoscopy with biopsy and pulmonary function tests. Patients were excluded from this study when they have 1) locally advanced (invading the trachea or the great vessels) or metastatic disease; 2) poor performance Status (3 & 4 according to WHO Criteria); or 3) a previous pulmonary or pleural surgery Patient Preparation All patients were admitted three days prior to surgery. Pulmonary exercises in the form of spirometry, steam inhalation, and nebulization were performed. Central venous accesses were inserted. Patients were hydrated and received total parenteral nutrition (TPN) three days prior to the surgery to improve the general condition Surgical Procedures The choice of laparoscopic approach (abdominal or thoracic) was according to prior CT localization of the esophageal mass. Accordingly, thoracoscopy was the initial step for radiological evidence of thoracic esophageal tumors. After assessment, operable patients underwent thoracoscopic mobilization of the esophagus and nodal dissection and laparoscopic gastric mobilization and gastric tube creation. All procedures were done with epidural and general anesthesia with single lung ventilation which was achieved by using a left-sided double lumen endotracheal tube. The double lumen tube was replaced by the reg- 215
3 ular endotracheal tube once the thoracic part of dissection was over, and the patient was placed in supine position. After intubation, the patient was placed in the prone position over a sand bag under the chest and pelvis leaving the abdomen free to allow respiratory movements with the right arm raised cranially to expose the right axillary fossa The Thoracoscopic Part Three ports were used: two 10 mm and one 5 mm. Thirty degree camera was used throughout the whole procedure. The ports, positions were as follows; 10 mm port at the seventh intercostal space (ICS) below the inferior angle of the scapula for camera 1); 5 mm port at fifth ICS 7 cm right lateral to the spinous process for right working hand 2); 10 mm port at ninth ICS 7 cm right lateral to the spinous process for left working hand 3) (Figure 1(a)). CO 2 pneumothorax was created by closed Veress technique in the seventh ICS. This site was used later as a camera port, maintaining insufflations pressure around 6 to 8 mmhg. After entering pleural space, adhesiolysis was performed, by the ACE harmonic shear. The first step was to assess resectability (by exclusion of lung or pleural metastases, invasion of vital structures or presence of fixed nodal disease). The inferior pulmonary ligament was divided to allow proper mobilization of the esophagus. The visceral pleura below the azygos vein that covers the esophagus was grasped and divided longitudinally with electrocautery hook dissector starting posteriorly at the posterior edge of the esophagus, anterior to the azygos vein, to the anterior edge of the esophagus and from the costo-phrenic angle inferiorly to the arch of the azygos vein superiorly. This part of the pleura over the esophagus was excised en bloc with the tumor. By retracting the esophagus ventrally, dissection continued separating the esophagus from the chest wall and descending thoracic aorta. In this step, the thoracic duct was visualized as a white glistening structure over the descending aorta and was protected. The vagal trunks were identified and divided. The left pleura was seen as a shining membrane and it was prone to injury in that situation. The infra-azygos dissection achieved a complete removal of the paraesophageal, subcarinal, hilar, and hiatal nodes. The esophagus was also separated all around from the pericardium, left pleura, arch of the aorta, and the descending aorta, and the azygos vein. The azygos vein was freed completely and was compressed by a non-toothed grasper for obliteration of the blood stream then it was sealed by a 10 mm Ligasure device (atlas) through a 10mm port (Figure 1(b)). Then, dissection was commenced above the level of the azygos with separation of the esophagus from the membranous portion of the trachea. By the end of this part of the operation, the entire esophagus from the thoracic inlet to the esophageal hiatus was mobilized (Figure 1(c)). Finally, insertion of one intercostal chest tube at the base of the lung through the 10mm port was done. Then the patient was turned and positioned for the next steps The Laparoscopic Abdominal Part In the case with the lower third esophageal carcinoma, laparoscopy was the initial step of the procedure. The stomach was mobilized completely with preservation of the gastro-epiploic vessels and lymphadenectomy of the celiac trunk was performed. The left gastric artery was sealed a 10 mm Ligasure device (atlas). After complete mobilization of the stomach and the lower esophagus up to the crus of the diaphragm, the stomach was divided by an endo GIA stapler (Ethicon ) in order to create a gastric tube (5 to 7 cm width) along the greater curvature (Figure 2(a)). The gastric tube was left attached to the gastric fundus (Figure 2(b)) The Cervical Part The neck was approached via a 4 cm incision at the anterior border of left sternocleidomastoid muscle. The esophagus was identified and dissection was continued posteriorly up to the prevertebral fascia. The left recurrent laryngeal nerve was identified and spared. A tape was passed around the esophagus to maintain traction (Figure 2(c)). Traction over the distal end of the esophagus was done to retrieve the specimen with the gastric tube attached to the specimen (Figure 2(d)). The nasogastric tube was removed and the esophagus was transected in the neck. Esophago-gastric tube anastomosis was performed using a3/0 Vicryl suture (Figure 3(a)) Patients Follow up All patients were referred to postoperative adjuvant chemotherapy and radiotherapy as indicated and they were 216
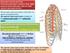
4 C A B (a) (b) A C B (c) Figure 1. (a) Patient and Port position; (b) Division of the azygos vein by Ligasure device 10 mm; (c) Mobilization of the esophagus (A) to the thoracic inlet (B), thoracic duct is visualized (C). 217
5 (a) (b) (c) Figure 2. (a) Creation of gastric tube with endo GIA stapler; (b) Gastric tube still attached to the gastric fundus; (c) Mobilization of the esophagus through small neck incision; (d) Extraction of the esophagus from the neck incision which is still attached to the gastric tube. followed up closely for detection of recurrence or metastasis. All patients were followed up regularly; biweekly in the first month, bimonthly in the following three months, monthly for six months, and every six months thereafter. Patients were censored if they developed the outcome (death, recurrence or metastasis) or at the study closure (October 2013). Follow up was carried out thought a full history, laboratory investigation and radiologic investigation including CT scanning of the chest and barium swallow (Figure 3(b)) Statistical Analyses Data were presented as mean and standard deviation (SD) for continuous data and proportion for categorical data. All statistical analyses were performed using SPSS version 20 (SPSS Inc., Chicago, IL, USA). 3. Results The mean age of the patients was ± years (30-80 years). They were 16 males (53.3%) and 14 females (46.7%). After pulmonary function tests, 14 patients (46.7%) were normal and 16 patients (53.3%) showed either obstructive, restrictive pulmonary disorders or both. Those patients received chest measures before the operation (Table 1) Histopathological Examination Reports confirmed SCC pathology in 16 patients (53.3%) and adenocarcinoma in 14 patients (46.7%). Fourteen (d) 218
6 patients (46.7%) were grade II and 16 patients (53.3%) were grade III. The most common site was lower third, being affected in 18 patients (60%). The mean tumor size was 5.65 ± 2.29 cm (range 2-12 cm). The most common clinical stage was stage II in 17patients (56.7%). Only 5patients (16.7%) received neoadjuvant chemoradiotherapy (Table 2) Thoracoscopic and Laparoscopic Assessment 17 patients (56.7%) were operable and 13 (43.3%) patients were found to be inoperable due to either small pleural nodules (n = 2), peritoneal nodules (n = 2), encasement of thoracic aorta (n = 1), encasement of celiac trunk (n = 1), presence of fixed lymph nodes (n = 6) or infiltration to the trachea (n = 1). The mean time of the thoracoscopic part was 3.38 h ± 0.88 h (range 2 h - 5 h) while in the abdominal part it was 2.59 h ± 0.78 h (range 1.5 h - 4 h). The mean operative blood loss was 250 cc ± cc (range100 cc cc) and there were no patients who received intraoperative blood transfusion. In onepatient (3.3%), left pleural injury occurred due to sever adhesions between the tumor and pleura. This injury did not affect the patient general condition intra operatively (Table 3). (a) (b) Figure 3. (a) Starting anastomosis between gastric tube and upper esophagus. Starting anastomosis between gastric tube and upper esophagus; (b) One year postoperative barium swallow showing the gastric tube. 219
7 Table 1. Demographic data of thirty cases of esophageal carcinoma. Age Mean ± SD Range Sex Male Female Comorbidity HTN Respiratory DM Hepatic Pulmonary function test Normal Obstructive Restrictive Combined obstructive and restrictive Chest measures Number ± Percentage Table 2. Tumor characteristics. Tumor type SCC Adenocarcinoma Tumor Site Upper 1/3 Middle 1/3 Lower 1/3 Tumor grade Grade I Grade II Grade III Stage grouping Stage I Stage II Stage III Tumor size Mean + SD Range Less than 3 cm (<3 cm) More than 3 cm (>3 cm) Neoadjuvant Number ± Percentage Postoperative Stay and Complications Overall hospital stay was ± 5.49 days (range days). Four patients developed pneumonia (13.3%) that was treated by antibiotics, good oxygen ventilation and nebulizer (Table 4). Two patients developed pleural effusion (6.7%); one of them was at the right side and was developed after removal of the chest tube. The effusion was then aspirated. The other one developed left pleural effusion in the same patient who had intraoperative 220
8 Table 3. Intraoperative details. Operative time (hrs) Thoracoscopic part Abdominal part Mean ± SD Range Operative blood loss (CC) Intra-operative Left pleural injury 1 case (3.3%) Convert to thoracotomy 0 Table 4. Overall hospital stay and postoperative complications. Overall hospital stay Mean + SD Range Number Percentage Pneumonia Pleural effusion RLN injury Cervical anastomosis leakage 3 10 Re-intervention Gastric conduit leakage 0 0 Thoracic duct leakage 0 0 DVT or Pulmonary embolism Postoperative bleeding 0 0 Wound infection day postoperative Mortality Median overall survival (months) 15 ± 5.81 (range 6 m - 24 m) Median disease free survival (range 6 m - 24 m) pleural injury. They were also managed conservatively by aspiration. Three patients (10%) developed cervical anastomotic leakage that was managed by conservative measures (TPN, liberal drainage, and proper antibiotic). The management was enough in one patient (in whom the fistula sealed spontaneously). On the other hand, one patientrequired surgical intervention and secondary repair with feeding jejunostomy and the third patient died after 18 days of operation due to sever mediastinitis. One patient (3.3%) developed deep venous thrombosis (DVT) postoperatively and he was treated by the standard regimen of anticoagulants. Four patients (13.3%) developed wound infection that was managed by antibiotics according the results of culture and sensitivity. Postoperative pathological examination revealed only two patients (6.7%) who had infiltrated lower safety margin while the majority of patients (93.3%) had negative safety margin. Lymph nodes were pathologically positive in 10 out of the 17 operable cases (58.8%) and were negative in the remaining 7 cases (41.2%). The mean total number of L.N. harvest (thoracoscopic and abdominal part) was ± 2.32 and the mean number of the mediastinal L.N. which was resected by thoracoscopy was Overall survival (OS) and disease free survival were assessed in the remaining 16 cases. The median overall survival was 15 ± 5.81 month (range 6-24 month). Overall survival was significantly affected by the clinical stage (P = 0.016). The median disease free survival was month (6-24). Disease free survival was significantly affected by the tumor size (P = 0.040), neoadjuvant therapy (P = 0.029), lymph node status (P = 0.020) and the clinical staging of cases (P = 0.007). 4. Discussion We are reporting a feasible and a relatively safe thoracoscopic and laparoscopic esophagectomy among a series of Egyptian patients with esophageal carcinoma. Comparing our population to previous studies showed a rela- 221
9 tively lower age. The mean age in the current study was around 59 years while in most series the mean age was ranging from years [8]. The finding may indicate a younger age of detection in our population compared with western populations which could be attributed to higher level of pollution in Nile Delta region in Egypt [10]. In the current study, the mean operative time of the total procedure was around 360 minutes, which is comparable to the time reported by several investigators. For example, Gao et al. conducted minimally invasive esophagectomy (MIE) in 96 patients and the mean operative time was 330 minutes [11]. Close enough, Kinjo et al. conducted hybrid MIE in 34 patients with an operative time of 264 minutes [12] and Schoppmann et al. conducted MIE in 31 patients with a mean operative time of 411 minutes [13]. The mean blood loss in this study was 250 ± cc. This was relatively lower than reported by Kinjo et al. who reported a mean blood loss of 536 cc [12] and Gao et al. who reported an average amount of 346 cc [11]. On the other hand, the current blood loss was slightly higher than that of Berger et al. who reported an average amount of 182 cc [14]. In our study, we used the ligasure only for cutting of the azygos vein. But in other studies, either clipping or double ligation with sutures was used as reported by Palanivelu et al. [15] or by using endo GIA stapler as reported by Berger et al. [14]. We found this new modification is less time consuming and less costly with no risk of bleeding found intraoperative or postoperative which may need further evaluation. The mean overall hospital stay in the current study was approximately 17.5 days. This was comparable to that observed by Mamidanna et al. who reported a hospital stay of 15 days [16] and Gao et al. reported a hospital stay of 12.6 days [11]. However, it was relatively shorter than reported by Kinjo et al. who reported a mean overall hospital stay of 23 days [12]. In our study, the postoperative hospital stay was longer in the patients that developed postoperative pneumonia rather than the other patients and it was also longer in patients of cervical anastomotic leakage. Postoperative pneumonia was reported as the most frequent morbidity after esophagectomy [7]. Similarly, the incidence of postoperative pneumonia in our study was the most frequent complication at 13.3%. The percentage was comparable to that observed by Gao et al. who reported 13.5% [11]. On the other hand, it was lower than the rates reported by Mamidanna et al. and Kinjo et al. who reported approximately 30% [12] [16]. The higher rate of pneumonia emphasized our efforts to request smoking cessation six weeks before the surgical resection, good preoperative chest measures, and using of intraoperative positive pressure once the thoracic esophagus has been completely mobilized. The early postoperative mortality in the current study was low at 3.3%. This was comparable to what was observed in previous studies. For example, early postoperative mortality was 2.1% in Gao et al. study [11], 4% in Mamidanna et al. study [16], and 7.7% in By Berger et al. study [14]. The median OS in the current study was 15 months (6-24). This was considerably lower than seen in some reports. Smithers et al. reported a median OS of 25 months in total MIE and 31 months in hybrid MIE [17]. Additionally, the median OS after MIE was estimated at 35 months by by Zingg et al. [18] and 51 months by Sundaram et al. [19] [20]. The average number of lymph nodes harvest in our study was 17. It ranged between 14 and 24 in different studies [12] [14] [20]. In a systematic review of 17 studies in 2012, the number of lymph nodes resected via MIE was 16 ( ) [8]. In our study, 93.3% of patients had a negative safety margin. This was similar to that reported by previous studies which ranged between 91% and 97% [12] [14]. In conclusion, totally endoscopic (thoracoscopic and laparoscopic) oesophagectomy is feasible and safe. Beside its efficacy as an assessment tool, total esophagectomy and lymphadenectomy could be performed at the same time. Acknowledgements We thank Dr. Aiman El-Saed; professor of community medicine, Mansoura University, for his support throughout this study. References [1] Ferlay, J., Shin, H.R., Bray, F., Forman, D., Mathers, C. and Parkin, D.M. (2010) Estimates of Worldwide Burden of Cancer in 2008: GLOBOCAN International Journal of Cancer, 127, [2] Holmes, R.S. and Vaughan, T.L. (2007) Epidemiology and Pathogenesis of Esophageal Cancer. Seminars in Radiation 222
10 Oncology, 17, [3] Wei, J.T. and Shaheen, N. (2003) The Changing Epidemiology of Esophageal Adenocarcinoma. Seminars in Gastrointestinal Disease, 14, [4] Lerut, T., Coosemans, W., De Leyn, P., Van Raemdonck, D., Nafteux, P. and Moons, J. (2001) Optimizing Treatment of Carcinoma of the Esophagus and Gastroesophageal Junction. Surgical Oncology Clinics of North America, 10, [5] Akiyama, H., Tsurumaru, M., Udagawa, H. and Kajiyama, Y. (1994) Radical Lymph Node Dissection for Cancer of the Thoracic Esophagus. Annals of Surgery, 220, ; Discussion [6] Cuschieri, A., Shimi, S. and Banting, S. (1992) Endoscopic Oesophagectomy through a Right Thoracoscopic Approach. Journal of the Royal College of Surgeons of Edinburgh, 37, [7] Ben-David, K., Sarosi, G.A., Cendan, J.C., Howard, D., Rossidis, G. and Hochwald, S.N. (2012) Decreasing Morbidity and Mortality in 100 Consecutive Minimally Invasive Esophagectomies. Surgical Endoscopy, 26, [8] Dantoc, M.M., Cox, M.R. and Eslick, G.D. (2012) Does Minimally Invasive Esophagectomy (Mie) Provide for Comparable Oncologic Outcomes to Open Techniques? A Systematic Review. Journal of Gastrointestinal Surgery: Official Journal of the Society for Surgery of the Alimentary Tract, 16, [9] Benzoni, E., Terrosu, G., Bresadola, V., Uzzau, A., Intini, S., Noce, L., Cedolini, C., Bresadola, F. and De Anna, D. (2004) A Comparative Study of the Transhiatal Laparoscopic Approach versus Laparoscopic Gastric Mobilisation and Right Open Transthoracic Esophagectomy for Esophageal Cancer Management. Journal of Gastrointestinal and Liver Diseases, 16, [10] Elewa, H.H. (2010) Potentialities of Water Resources Pollution of the Nile River Delta, Egypt. The Open Hydrology Journal, 4, [11] Gao, Y., Wang, Y., Chen, L. and Zhao, Y. (2011) Comparison of Open Three-Field and Minimally-Invasive Esophagectomy for Esophageal Cancer. Interactive Cardiovascular and Thoracic Surgery, 12, [12] Kinjo, Y., Kurita, N., Nakamura, F., Okabe, H., Tanaka, E., Kataoka, Y., Itami, A., Sakai, Y. and Fukuhara, S. (2012) Effectiveness of Combined Thoracoscopic-Laparoscopic Esophagectomy: Comparison of Postoperative Complications and Midterm Oncological Outcomes in Patients with Esophageal Cancer. Surgical Endoscopy, 26, [13] Schoppmann, S.F., Prager, G., Langer, F.B., Riegler, F.M., Kabon, B., Fleischmann, E. and Zacherl, J. (2010) Open versus Minimally Invasive Esophagectomy: A Single-Center Case Controlled Study. Surgical Endoscopy, 24, [14] Berger, A.C., Bloomenthal, A., Weksler, B., Evans, N., Chojnacki, K.A., Yeo, C.J. and Rosato, E.L. (2011) Oncologic Efficacy Is not Compromised, and May Be Improved with Minimally Invasive Esophagectomy. Journal of the American College of Surgeons, 212, [15] Palanivelu, C., Prakash, A., Senthilkumar, R., Senthilnathan, P., Parthasarathi, R., Rajan, P.S. and Venkatachlam, S. (2006) Minimally Invasive Esophagectomy: Thoracoscopic Mobilization of the Esophagus and Mediastinal Lymphadenectomy in Prone Position Experience of 130 Patients. Journal of the American College of Surgeons, 203, [16] Mamidanna, R., Bottle, A., Aylin, P., Faiz, O. and Hanna, G.B. (2012) Short-Term Outcomes Following Open versus Minimally Invasive Esophagectomy for Cancer in England: A Population-Based National Study. Annals of Surgery, 255, [17] Smithers, B.M., Gotley, D.C., Martin, I. and Thomas, J.M. (2007) Comparison of the Outcomes between Open and Minimally Invasive Esophagectomy. Annals of Surgery, 245, [18] Zingg, U., McQuinn, A., DiValentino, D., Esterman, A.J., Bessell, J.R., Thompson, S.K., Jamieson, G.G. and Watson, D.I. (2009) Minimally Invasive versus Open Esophagectomy for Patients with Esophageal Cancer. The Annals of Thoracic Surgery, 87, [19] Sundaram, A., Geronimo, J.C., Willer, B.L., Hoshino, M., Torgersen, Z., Juhasz, A., Lee, T.H. and Mittal, S.K. (2012) Survival and Quality of Life after Minimally Invasive Esophagectomy: A Single-Surgeon Experience. Surgical Endoscopy, 26, [20] Singh, R.K., Pham, T.H., Diggs, B.S., Perkins, S. and Hunter, J.G. (2011) Minimally Invasive Esophagectomy Provides Equivalent Oncologic Outcomes to Open Esophagectomy for Locally Advanced (Stage II or III) Esophageal Carcinoma. Archives of Surgery, 146,
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
Minimally Invasive Esophagectomy
 Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Determining the Optimal Surgical Approach to Esophageal Cancer
 Determining the Optimal Surgical Approach to Esophageal Cancer Amit Bhargava, MD Attending Thoracic Surgeon Department of Cardiovascular and Thoracic Surgery Open Esophagectomy versus Minimally Invasive
Determining the Optimal Surgical Approach to Esophageal Cancer Amit Bhargava, MD Attending Thoracic Surgeon Department of Cardiovascular and Thoracic Surgery Open Esophagectomy versus Minimally Invasive
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
Controversies in management of squamous esophageal cancer
 2015.06.12 12.47.48 Page 4(1) IS-1 Controversies in management of squamous esophageal cancer C S Pramesh Thoracic Surgery, Department of Surgical Oncology, Tata Memorial Centre, India In Asia, squamous
2015.06.12 12.47.48 Page 4(1) IS-1 Controversies in management of squamous esophageal cancer C S Pramesh Thoracic Surgery, Department of Surgical Oncology, Tata Memorial Centre, India In Asia, squamous
MINIMALLY INVASIVE ESOPHAGECTOMY FOR CANCER: where do we stand?
 MINIMALLY INVASIVE ESOPHAGECTOMY FOR CANCER: where do we stand? Ph Nafteux, MD Copenhagen, Nov 3rd 2011 Department of Thoracic Surgery, University Hospitals Leuven, Belgium W. Coosemans, H. Decaluwé, Ph.
MINIMALLY INVASIVE ESOPHAGECTOMY FOR CANCER: where do we stand? Ph Nafteux, MD Copenhagen, Nov 3rd 2011 Department of Thoracic Surgery, University Hospitals Leuven, Belgium W. Coosemans, H. Decaluwé, Ph.
1. Epidemiology of Esophageal Cancer 2. Operative Strategies 3. Minimally Invasive Esophagectomy 4. Video
 Minimally Invasive Esophagectomy Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ESOPHAGEAL
Minimally Invasive Esophagectomy Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ESOPHAGEAL
Part II. A randomized trial
 77 Part II A randomized trial 78 79 Chapter 5 Preliminary experience of minimally invasive esophagectomy for cancer. Maas KW Biere SSAY Gisbertz SS van der Peet DL M.A. Cuesta Submitted 80 Chapter 5 ABSTRACT
77 Part II A randomized trial 78 79 Chapter 5 Preliminary experience of minimally invasive esophagectomy for cancer. Maas KW Biere SSAY Gisbertz SS van der Peet DL M.A. Cuesta Submitted 80 Chapter 5 ABSTRACT
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012
 Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
Minimally Invasive Esophagectomy- Valuable. Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006
 Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
The Learning Curve for Minimally Invasive Esophagectomy
 The Learning Curve for Minimally Invasive Esophagectomy AATS Focus on Thoracic Surgery Mastering Surgical Innovation Las Vegas Nevada Oct. 27-28 2017 Scott J Swanson, M.D. Professor of Surgery Harvard
The Learning Curve for Minimally Invasive Esophagectomy AATS Focus on Thoracic Surgery Mastering Surgical Innovation Las Vegas Nevada Oct. 27-28 2017 Scott J Swanson, M.D. Professor of Surgery Harvard
General introduction and outline of thesis
 General introduction and outline of thesis General introduction and outline of thesis 11 GENERAL INTRODUCTION AND OUTLINE OF THESIS The incidence of esophageal cancer is increasing in the western world.
General introduction and outline of thesis General introduction and outline of thesis 11 GENERAL INTRODUCTION AND OUTLINE OF THESIS The incidence of esophageal cancer is increasing in the western world.
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
AATS Focus on Thoracic Surgery: Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017?
 AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
Robotic-assisted McKeown esophagectomy
 Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Robotic-assisted right inferior lobectomy
 Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Management of Esophageal Cancer: Evidence Based Review of Current Guidelines. Madhuri Rao, MD PGY-5 SUNY Downstate Medical Center
 Management of Esophageal Cancer: Evidence Based Review of Current Guidelines Madhuri Rao, MD PGY-5 SUNY Downstate Medical Center Case Presentation 68 y/o male PMH: NIDDM, HTN, hyperlipidemia, CAD s/p stents,
Management of Esophageal Cancer: Evidence Based Review of Current Guidelines Madhuri Rao, MD PGY-5 SUNY Downstate Medical Center Case Presentation 68 y/o male PMH: NIDDM, HTN, hyperlipidemia, CAD s/p stents,
Robotic-assisted right upper lobectomy
 Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Case Scenario 1. The patient has now completed his neoadjuvant chemoradiation and has been cleared for surgery.
 Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Uniportal video-assisted thoracic surgery for esophageal cancer
 Surgical Technique on Esophageal Surgery Uniportal video-assisted thoracic surgery for esophageal cancer Hasan F. Batirel Thoracic Surgery Department, Marmara University Hospital, Istanbul, Turkey Correspondence
Surgical Technique on Esophageal Surgery Uniportal video-assisted thoracic surgery for esophageal cancer Hasan F. Batirel Thoracic Surgery Department, Marmara University Hospital, Istanbul, Turkey Correspondence
Minimally invasive esophagectomy (MIE) has increasingly
 Minimally Invasive Ivor Lewis Esophagectomy David R. Jones, MD Minimally invasive esophagectomy (MIE) has increasingly been adopted by thoracic surgeons in both academic and community-based practices as
Minimally Invasive Ivor Lewis Esophagectomy David R. Jones, MD Minimally invasive esophagectomy (MIE) has increasingly been adopted by thoracic surgeons in both academic and community-based practices as
Uniportal thoracoscopy combined with laparoscopy as minimally invasive treatment of esophageal cancer
 Case Report Uniportal thoracoscopy combined with laparoscopy as minimally invasive treatment of esophageal cancer Francesco Paolo Caronia 1, Ettore Arrigo 1, Andrea Valentino Failla 2, Francesco Sgalambro
Case Report Uniportal thoracoscopy combined with laparoscopy as minimally invasive treatment of esophageal cancer Francesco Paolo Caronia 1, Ettore Arrigo 1, Andrea Valentino Failla 2, Francesco Sgalambro
Minimally Invasive Esophagectomy: OVERRATED!!! Sagar Damle UCHSC December 11, 2006
 Minimally Invasive Esophagectomy: OVERRATED!!! Sagar Damle UCHSC December 11, 2006 Esophageal Cancer - Est. 15,000 cases in 2006 - Est. 14,000 deaths - Overall 5-year survival: 15.6% - 33.6 % for local
Minimally Invasive Esophagectomy: OVERRATED!!! Sagar Damle UCHSC December 11, 2006 Esophageal Cancer - Est. 15,000 cases in 2006 - Est. 14,000 deaths - Overall 5-year survival: 15.6% - 33.6 % for local
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer
 Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Lymph node metastasis is one of the most important prognostic
 ORIGINAL ARTICLE Comparison of Survival and Recurrence Pattern Between Two-Field and Three-Field Lymph Node Dissections for Upper Thoracic Esophageal Squamous Cell Carcinoma Young Mog Shim, MD, Hong Kwan
ORIGINAL ARTICLE Comparison of Survival and Recurrence Pattern Between Two-Field and Three-Field Lymph Node Dissections for Upper Thoracic Esophageal Squamous Cell Carcinoma Young Mog Shim, MD, Hong Kwan
A video demonstration of the Li s anastomosis the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma
 Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Esophageal Cancer. What is esophageal cancer?
 Scan for mobile link. Esophageal Cancer Esophageal cancer occurs when cancer cells develop in the esophagus. The two main types are squamous cell carcinoma and adenocarcinoma. Esophageal cancer may not
Scan for mobile link. Esophageal Cancer Esophageal cancer occurs when cancer cells develop in the esophagus. The two main types are squamous cell carcinoma and adenocarcinoma. Esophageal cancer may not
Robotic Surgery for Esophageal Cancer
 Robotic Surgery for Esophageal Cancer Kemp H. Kernstine, MD PhD Division of Thoracic Surgery City of Hope Medical Center and Beckman Research Institute May 1, 2010 Esophageal Cancer on the Rise JNCI 2005,
Robotic Surgery for Esophageal Cancer Kemp H. Kernstine, MD PhD Division of Thoracic Surgery City of Hope Medical Center and Beckman Research Institute May 1, 2010 Esophageal Cancer on the Rise JNCI 2005,
A Proposed Strategy for Treatment of Superficial Carcinoma. in the Thoracic Esophagus Based on an Analysis. of Lymph Node Metastasis
 Kitakanto Med J 2002 ; 52 : 189-193 189 A Proposed Strategy for Treatment of Superficial Carcinoma in the Thoracic Esophagus Based on an Analysis of Lymph Node Metastasis Susumu Kawate,' Susumu Ohwada,'
Kitakanto Med J 2002 ; 52 : 189-193 189 A Proposed Strategy for Treatment of Superficial Carcinoma in the Thoracic Esophagus Based on an Analysis of Lymph Node Metastasis Susumu Kawate,' Susumu Ohwada,'
Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe
 Case Report Page 1 of 5 Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe Hailei Du, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Dingpei Han, Kai Chen, Jie Xiang, Hecheng
Case Report Page 1 of 5 Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe Hailei Du, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Dingpei Han, Kai Chen, Jie Xiang, Hecheng
DATA REPORT. August 2014
 AUDIT DATA REPORT August 2014 Prepared for the Australian and New Zealand Gastric and Oesophageal Surgical Association by the Royal Australasian College of Surgeons 199 Ward St, North Adelaide, SA 5006
AUDIT DATA REPORT August 2014 Prepared for the Australian and New Zealand Gastric and Oesophageal Surgical Association by the Royal Australasian College of Surgeons 199 Ward St, North Adelaide, SA 5006
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
T3 NSCLC: Chest Wall, Diaphragm, Mediastinum
 for T3 NSCLC: Chest Wall, Diaphragm, Mediastinum AATS Postgraduate Course April 29, 2012 Thomas A. D Amico MD Professor of Surgery, Chief of Thoracic Surgery Duke University Health System Disclosure No
for T3 NSCLC: Chest Wall, Diaphragm, Mediastinum AATS Postgraduate Course April 29, 2012 Thomas A. D Amico MD Professor of Surgery, Chief of Thoracic Surgery Duke University Health System Disclosure No
Guidelines for Laparoscopic Resection of Curable Colon and Rectal Cancer
 SAGES Society of American Gastrointestinal and Endoscopic Surgeons http://www.sages.org Guidelines for Laparoscopic Resection of Curable Colon and Rectal Cancer Author : SAGES Webmaster PREAMBLE The following
SAGES Society of American Gastrointestinal and Endoscopic Surgeons http://www.sages.org Guidelines for Laparoscopic Resection of Curable Colon and Rectal Cancer Author : SAGES Webmaster PREAMBLE The following
Review Article Review of Minimally Invasive Esophagectomy and Current Controversies
 Gastroenterology Research and Practice Volume 2012, Article ID 683213, 7 pages doi:10.1155/2012/683213 Review Article Review of Minimally Invasive Esophagectomy and Current Controversies T. Kim, S. N.
Gastroenterology Research and Practice Volume 2012, Article ID 683213, 7 pages doi:10.1155/2012/683213 Review Article Review of Minimally Invasive Esophagectomy and Current Controversies T. Kim, S. N.
SURGICAL TECHNIQUE. Radical treatment for left upper-lobe cancer via complete VATS. Jun Liu, Fei Cui, Shu-Ben Li. Introduction
 SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
Robotic-assisted left inferior lobectomy
 Robotic Thoracic Surgery Column Robotic-assisted left inferior lobectomy Shiguang Xu, Hao Meng, Tong Wang, Wei Xu, Xingchi Liu, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Robotic Thoracic Surgery Column Robotic-assisted left inferior lobectomy Shiguang Xu, Hao Meng, Tong Wang, Wei Xu, Xingchi Liu, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
THE DESCENDING THORACIC AORTA
 Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
7/20/2017. Esophageal Cancer: A Less Common But Deadly Cancer. Objectives. Disclosure Statement NYNPA Conference October Saratoga New York
 Esophageal Cancer: A Less Common But Deadly Cancer 2017 NYNPA Conference October 18-22 Saratoga New York Mary McGreal DNP, RN, ANP-C, CCRN, CMC, Adjunct Professor at Stony Brook University School of Nursing
Esophageal Cancer: A Less Common But Deadly Cancer 2017 NYNPA Conference October 18-22 Saratoga New York Mary McGreal DNP, RN, ANP-C, CCRN, CMC, Adjunct Professor at Stony Brook University School of Nursing
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
Ruijin robotic thoracic surgery: S segmentectomy of the left upper lobe
 Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
ESOPHAGEAL CANCER. Dr. Paul Gardiner December 17, 2002 Discipline of Surgery Rounds
 ESOPHAGEAL CANCER Dr. Paul Gardiner December 17, 2002 Discipline of Surgery Rounds ESOPHAGEAL CANCER I. EPIDEMIOLOGY INCIDENCE, DIAGNOSIS & STAGING II. TREATMENT OPTIONS Current role of induction therapies
ESOPHAGEAL CANCER Dr. Paul Gardiner December 17, 2002 Discipline of Surgery Rounds ESOPHAGEAL CANCER I. EPIDEMIOLOGY INCIDENCE, DIAGNOSIS & STAGING II. TREATMENT OPTIONS Current role of induction therapies
Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 Final Pathology:
 Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 A 74 year old male with a history of GERD presents complaining of dysphagia. An esophagogastroduodenoscopy
Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 A 74 year old male with a history of GERD presents complaining of dysphagia. An esophagogastroduodenoscopy
Is closed thoracic drainage tube necessary for minimally invasive thoracoscopic-esophagectomy?
 Original Article Is closed thoracic drainage tube necessary for minimally invasive thoracoscopic-esophagectomy? Lei Cai 1 *, Yan Li 2 *, Wen-Bin Wang 1 *, Man Guo 1, Xiao Lian 1, Shu-Ao Xiao 1, Guang-Hui
Original Article Is closed thoracic drainage tube necessary for minimally invasive thoracoscopic-esophagectomy? Lei Cai 1 *, Yan Li 2 *, Wen-Bin Wang 1 *, Man Guo 1, Xiao Lian 1, Shu-Ao Xiao 1, Guang-Hui
Comparison of short-term therapeutic efficacy between minimally invasive Ivor-Lewis esophagectomy and Mckeown esophagectomy for esophageal cancer.
 Biomedical Research 2017; 28 (12): 5321-5326 ISSN 0970-938X www.biomedres.info Comparison of short-term therapeutic efficacy between minimally invasive Ivor-Lewis esophagectomy and Mckeown esophagectomy
Biomedical Research 2017; 28 (12): 5321-5326 ISSN 0970-938X www.biomedres.info Comparison of short-term therapeutic efficacy between minimally invasive Ivor-Lewis esophagectomy and Mckeown esophagectomy
Minimally invasive esophagectomy for esophageal squamous cell carcinoma Shanghai Chest Hospital experience
 Surgical Technique Minimally invasive esophagectomy for esophageal squamous cell carcinoma Shanghai Chest Hospital experience Bin Li #, Yu Yang #, Yifeng Sun, Rong Hua, Xiaobin Zhang, Xufeng Guo, Haiyong
Surgical Technique Minimally invasive esophagectomy for esophageal squamous cell carcinoma Shanghai Chest Hospital experience Bin Li #, Yu Yang #, Yifeng Sun, Rong Hua, Xiaobin Zhang, Xufeng Guo, Haiyong
Case Scenario year-old white male presented to personal physician with dyspepsia with reflux.
 Case Scenario 1 57-year-old white male presented to personal physician with dyspepsia with reflux. 7/12 EGD: In the gastroesophageal junction we found an exophytic tumor. The tumor occupies approximately
Case Scenario 1 57-year-old white male presented to personal physician with dyspepsia with reflux. 7/12 EGD: In the gastroesophageal junction we found an exophytic tumor. The tumor occupies approximately
Transcervical uniportal pulmonary lobectomy
 Original Article on Thoracic Surgery Page 1 of 6 Transcervical uniportal pulmonary lobectomy Marcin Zieliński 1, Tomasz Nabialek 2, Juliusz 3 1 Department of Thoracic Surgery, 2 Department of Anaesthesiology
Original Article on Thoracic Surgery Page 1 of 6 Transcervical uniportal pulmonary lobectomy Marcin Zieliński 1, Tomasz Nabialek 2, Juliusz 3 1 Department of Thoracic Surgery, 2 Department of Anaesthesiology
Totally thoracoscopic left upper lobe tri-segmentectomy
 Masters of Cardiothoracic Surgery Totally thoracoscopic left upper lobe tri-segmentectomy Dominique Gossot Thoracic Department, Institut Mutualiste Montsouris, Paris, France Correspondence to: Dominique
Masters of Cardiothoracic Surgery Totally thoracoscopic left upper lobe tri-segmentectomy Dominique Gossot Thoracic Department, Institut Mutualiste Montsouris, Paris, France Correspondence to: Dominique
Video-assisted thoracic surgery right upper lobe bronchial sleeve resection
 Original Article on Thoracic Surgery Video-assisted thoracic surgery right upper lobe bronchial sleeve resection Qianli Ma, Deruo Liu Department of Thoracic Surgery, China-Japan Friendship Hospital, Beijing
Original Article on Thoracic Surgery Video-assisted thoracic surgery right upper lobe bronchial sleeve resection Qianli Ma, Deruo Liu Department of Thoracic Surgery, China-Japan Friendship Hospital, Beijing
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
Very long-term outcomes of minimally invasive esophagectomy for esophageal squamous cell carcinoma
 JBUON 2015; 20(6): 1585-1591 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Very long-term outcomes of minimally invasive esophagectomy for esophageal
JBUON 2015; 20(6): 1585-1591 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Very long-term outcomes of minimally invasive esophagectomy for esophageal
Uniportal video-assisted thoracoscopic right upper posterior segmentectomy with systematic mediastinal lymphadenectomy
 Surgical Technique Uniportal video-assisted thoracoscopic right upper posterior segmentectomy with systematic mediastinal lymphadenectomy Guofei Zhang 1, Zhijun Wu 2, Yimin Wu 1, Gang Shen 1, Ying Chai
Surgical Technique Uniportal video-assisted thoracoscopic right upper posterior segmentectomy with systematic mediastinal lymphadenectomy Guofei Zhang 1, Zhijun Wu 2, Yimin Wu 1, Gang Shen 1, Ying Chai
Original Article Effects of laparo-thoracoscopic surgery and open surgery on pulmonary infection in elderly patients with esophageal cancer
 Int J Clin Exp Med 2018;11(7):7104-7110 www.ijcem.com /ISSN:1940-5901/IJCEM0054901 Original Article Effects of laparo-thoracoscopic surgery and open surgery on pulmonary infection in elderly patients with
Int J Clin Exp Med 2018;11(7):7104-7110 www.ijcem.com /ISSN:1940-5901/IJCEM0054901 Original Article Effects of laparo-thoracoscopic surgery and open surgery on pulmonary infection in elderly patients with
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
UCLA General Surgery Residency Program Rotation Educational Policy Goals and Objectives
 UPDATED: July 2009 ROTATION: THORACIC SURGERY UCLA General Surgery Residency Program ROTATION DIRECTOR: Mary Maish, M.D. CHIEF OF CARDIAC SURGERY: Robert Cameron, M.D. SITES: UCLA Medical Center - Westwood
UPDATED: July 2009 ROTATION: THORACIC SURGERY UCLA General Surgery Residency Program ROTATION DIRECTOR: Mary Maish, M.D. CHIEF OF CARDIAC SURGERY: Robert Cameron, M.D. SITES: UCLA Medical Center - Westwood
Uniportal video-assisted thoracic surgery for complicated pulmonary resections
 Review Article on Thoracic Surgery Uniportal video-assisted thoracic surgery for complicated pulmonary resections Ding-Pei Han, Jie Xiang, Run-Sen Jin, Yan-Xia Hu, He-Cheng Li Jiaotong University School
Review Article on Thoracic Surgery Uniportal video-assisted thoracic surgery for complicated pulmonary resections Ding-Pei Han, Jie Xiang, Run-Sen Jin, Yan-Xia Hu, He-Cheng Li Jiaotong University School
Mediastinal Staging. Samer Kanaan, M.D.
 Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Review of different approaches of the left recurrent laryngeal nerve area for lymphadenectomy during minimally invasive esophagectomy
 Review Article Review of different approaches of the left recurrent laryngeal nerve area for lymphadenectomy during minimally invasive esophagectomy Miguel A. Cuesta Gastrointestinal and Minimally Invasive
Review Article Review of different approaches of the left recurrent laryngeal nerve area for lymphadenectomy during minimally invasive esophagectomy Miguel A. Cuesta Gastrointestinal and Minimally Invasive
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Uniportal complete video-assisted thoracoscopic surgery lobectomy with partial pulmonary arterioplasty for lung cancer with calcified lymph node
 Surgical Technique Uniportal complete video-assisted thoracoscopic surgery lobectomy with partial pulmonary arterioplasty for lung cancer with calcified lymph node Guang-Suo Wang, Jian Wang, Zhan-Peng
Surgical Technique Uniportal complete video-assisted thoracoscopic surgery lobectomy with partial pulmonary arterioplasty for lung cancer with calcified lymph node Guang-Suo Wang, Jian Wang, Zhan-Peng
Di Lu 1#, Xiguang Liu 1#, Mei Li 1#, Siyang Feng 1#, Xiaoying Dong 1, Xuezhou Yu 2, Hua Wu 1, Gang Xiong 1, Ruijun Cai 1, Guoxin Li 3, Kaican Cai 1
 Case Report Three-port mediastino-laparoscopic esophagectomy (TPMLE) for an 81-year-old female with early-staged esophageal cancer: a case report of combining single-port mediastinoscopic esophagectomy
Case Report Three-port mediastino-laparoscopic esophagectomy (TPMLE) for an 81-year-old female with early-staged esophageal cancer: a case report of combining single-port mediastinoscopic esophagectomy
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Successful Resection of Esophageal Carcinoma Associated with Double Aortic Arch: A Case Report
 Successful Resection of Esophageal Carcinoma Associated with Double Aortic Arch: A Case Report NAOSHI KUBO 1, MASAICHI OHIRA 1, YOSHITO YAMASHITA 2, KATSUNOBU SAKURAI 1, HIROAKI TANAKA 1, KAZUYA MUGURUMA
Successful Resection of Esophageal Carcinoma Associated with Double Aortic Arch: A Case Report NAOSHI KUBO 1, MASAICHI OHIRA 1, YOSHITO YAMASHITA 2, KATSUNOBU SAKURAI 1, HIROAKI TANAKA 1, KAZUYA MUGURUMA
Thoracoscopic Lobectomy: Technical Aspects in Years of Progress
 Thoracoscopic Lobectomy: Technical Aspects in 2015 16 Years of Progress 8 th Masters of Minimally Invasive Thoracic Surgery Orlando September 25, 2015 Thomas A. D Amico MD Gary Hock Professor of Surgery
Thoracoscopic Lobectomy: Technical Aspects in 2015 16 Years of Progress 8 th Masters of Minimally Invasive Thoracic Surgery Orlando September 25, 2015 Thomas A. D Amico MD Gary Hock Professor of Surgery
Esophageal Cancer. Source: National Cancer Institute
 Esophageal Cancer Esophageal cancer forms in the tissues that line the esophagus, or the long, hollow tube that connects the mouth and stomach. Food and drink pass through the esophagus to be digested.
Esophageal Cancer Esophageal cancer forms in the tissues that line the esophagus, or the long, hollow tube that connects the mouth and stomach. Food and drink pass through the esophagus to be digested.
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
Transhiatal Esophagectomy: Lower Mortality, Diminished Morbidity, Equal Effectiveness
 Transhiatal Esophagectomy: Lower Mortality, Diminished Morbidity, Equal Effectiveness Sunil Malhotra, M.D. Department of Surgery University of Colorado Resident Debate April 30, 2007 Esophageal Cancer
Transhiatal Esophagectomy: Lower Mortality, Diminished Morbidity, Equal Effectiveness Sunil Malhotra, M.D. Department of Surgery University of Colorado Resident Debate April 30, 2007 Esophageal Cancer
Oesophageal Cancer: The Image after Surgery
 Oesophageal Cancer: The Image after Surgery Poster No.: C-2253 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Loureiro, N. V. V. B. Marques, M. Palmeiro, P. Pereira, 1 1 1 1 2 1 1 2 1 R. Gil,
Oesophageal Cancer: The Image after Surgery Poster No.: C-2253 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Loureiro, N. V. V. B. Marques, M. Palmeiro, P. Pereira, 1 1 1 1 2 1 1 2 1 R. Gil,
Oesophageal Cancer: The Image after Surgery
 Oesophageal Cancer: The Image after Surgery Poster No.: C-2253 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Loureiro, N. V. V. B. Marques, M. Palmeiro, P. Pereira, 1 1 1 1 2 1 1 2 1 R. Gil,
Oesophageal Cancer: The Image after Surgery Poster No.: C-2253 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Loureiro, N. V. V. B. Marques, M. Palmeiro, P. Pereira, 1 1 1 1 2 1 1 2 1 R. Gil,
Charles Mulligan, MD, FACS, FCCP 26 March 2015
 Charles Mulligan, MD, FACS, FCCP 26 March 2015 Review lung cancer statistics Review the risk factors Discuss presentation and staging Discuss treatment options and outcomes Discuss the status of screening
Charles Mulligan, MD, FACS, FCCP 26 March 2015 Review lung cancer statistics Review the risk factors Discuss presentation and staging Discuss treatment options and outcomes Discuss the status of screening
Thoracoscopic S 6 segmentectomy: tricks to know
 Surgical Technique Page 1 of 6 Thoracoscopic S 6 segmentectomy: tricks to know Agathe Seguin-Givelet 1,2, Jon Lutz 1, Dominique Gossot 1 1 Thoracic Department, Institut Mutualiste Montsouris, Paris, France;
Surgical Technique Page 1 of 6 Thoracoscopic S 6 segmentectomy: tricks to know Agathe Seguin-Givelet 1,2, Jon Lutz 1, Dominique Gossot 1 1 Thoracic Department, Institut Mutualiste Montsouris, Paris, France;
Mediastinum It is a thick movable partition between the two pleural sacs & lungs. It contains all the structures which lie
 Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
OCCULT CERVICAL NODAL METASTASIS IN ESOPHAGEAL CANCER: PRELIMINARY RESULTS OF THREE-FIELD LYMPHADENECTOMY
 OCCULT CERVICAL NODAL METASTASIS IN ESOPHAGEAL CANCER: PRELIMINARY RESULTS OF THREE-FIELD LYMPHADENECTOMY Nasser K. Altorki, MD David B. Skinner, MD The extent of lymphadenectomy for carcinoma of the thoracic
OCCULT CERVICAL NODAL METASTASIS IN ESOPHAGEAL CANCER: PRELIMINARY RESULTS OF THREE-FIELD LYMPHADENECTOMY Nasser K. Altorki, MD David B. Skinner, MD The extent of lymphadenectomy for carcinoma of the thoracic
Laparoscopic Bladder-Preserving Surgery for Enterovesical Fistula Complicated with Benign Gastrointestinal Disease
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Esophageal cancer: Biology, natural history, staging and therapeutic options
 EGEUS 2nd Meeting Esophageal cancer: Biology, natural history, staging and therapeutic options Michael Bau Mortensen MD, Ph.D. Associate Professor of Surgery Centre for Surgical Ultrasound, Upper GI Section,
EGEUS 2nd Meeting Esophageal cancer: Biology, natural history, staging and therapeutic options Michael Bau Mortensen MD, Ph.D. Associate Professor of Surgery Centre for Surgical Ultrasound, Upper GI Section,
Laparoscopic and Thoracoscopic Ivor Lewis Esophagectomy With Colonic Interposition
 HOW TO DO IT Laparoscopic and Thoracoscopic Ivor Lewis Esophagectomy With Colonic Interposition Ninh T. Nguyen, MD, FACS, Marcelo Hinojosa, MD, Christine Fayad, BS, James Gray, BS, Zuri Murrell, MD, and
HOW TO DO IT Laparoscopic and Thoracoscopic Ivor Lewis Esophagectomy With Colonic Interposition Ninh T. Nguyen, MD, FACS, Marcelo Hinojosa, MD, Christine Fayad, BS, James Gray, BS, Zuri Murrell, MD, and
Sectional Anatomy Quiz - III
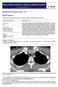 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Quiz Adenocarcinoma of the distal stomach has been increasing in the last 20 years. a. True b. False
 Quiz 1 1. Which of the following are risk factors for esophagus cancer. a. Obesity b. Gastroesophageal reflux c. Smoking and Alcohol d. All of the above 2. Adenocarcinoma of the distal stomach has been
Quiz 1 1. Which of the following are risk factors for esophagus cancer. a. Obesity b. Gastroesophageal reflux c. Smoking and Alcohol d. All of the above 2. Adenocarcinoma of the distal stomach has been
A comparison of short-term outcomes between Ivor-Lewis and McKeown minimally invasive esophagectomy
 Surgical Technique A comparison of short-term outcomes between Ivor-Lewis and McKeown minimally invasive esophagectomy Chunbo Zhai 1,2 *, Yongjing Liu 3 *, Wei Li 2, Tongzhen Xu 2, Guotao Yang 1, Hengxiao
Surgical Technique A comparison of short-term outcomes between Ivor-Lewis and McKeown minimally invasive esophagectomy Chunbo Zhai 1,2 *, Yongjing Liu 3 *, Wei Li 2, Tongzhen Xu 2, Guotao Yang 1, Hengxiao
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma
 Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given
Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
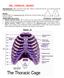 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
MEDIASTINAL STAGING surgical pro
 MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the
 My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
Esophageal Cancer Staging Essentials: The New TNM Staging System (7th edition) and Clinicoradiologic Implications
 Esophageal Cancer Staging Essentials: The New TNM Staging System (7th edition) and Clinicoradiologic Implications Poster No.: E-0060 Congress: ESTI 2012 Type: Scientific Exhibit Authors: K. Lee, T. J.
Esophageal Cancer Staging Essentials: The New TNM Staging System (7th edition) and Clinicoradiologic Implications Poster No.: E-0060 Congress: ESTI 2012 Type: Scientific Exhibit Authors: K. Lee, T. J.
Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012
 Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012 Esophageal Leiomyoma Introduction Case presentation Operative video Discussion Esophageal Leiomyoma Benign tumors of the
Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012 Esophageal Leiomyoma Introduction Case presentation Operative video Discussion Esophageal Leiomyoma Benign tumors of the
ANTICANCER RESEARCH 34: (2014)
 The Impact of Combined Thoracoscopic and Laparoscopic Surgery on Pulmonary Complications After Radical Esophagectomy in Patients With Resectable Esophageal Cancer NAOSHI KUBO 1, MASAICHI OHIRA 1, YOSHITO
The Impact of Combined Thoracoscopic and Laparoscopic Surgery on Pulmonary Complications After Radical Esophagectomy in Patients With Resectable Esophageal Cancer NAOSHI KUBO 1, MASAICHI OHIRA 1, YOSHITO
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER
 MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
Esophageal cancer. What is esophageal cancer? Esophageal cancer is a disease in which malignant (cancer) cells form in the tissues of the esophagus.
 Esophageal Cancer Esophageal cancer What is esophageal cancer? What are risk factors? Signs and symptoms Tests for esophageal cancer Stages of esophageal cancer Treatment options What is esophageal cancer?
Esophageal Cancer Esophageal cancer What is esophageal cancer? What are risk factors? Signs and symptoms Tests for esophageal cancer Stages of esophageal cancer Treatment options What is esophageal cancer?
The left thoracoabdominal and left neck approach to
 Esophagectomy: Left Thoracoabdominal and Left Neck Thomas W. Rice, MD *, The left thoracoabdominal and left neck approach to esophagectomy offers flexibility, versatility, and options. In the western world,
Esophagectomy: Left Thoracoabdominal and Left Neck Thomas W. Rice, MD *, The left thoracoabdominal and left neck approach to esophagectomy offers flexibility, versatility, and options. In the western world,
Thoracic Surgery; An Overview
 Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
 Lya Crichlow, MD Kings County Hospital Center September 3, 2009 Morbidity and Mortality Conference Case presentation 56 year old male who presented with 1 week history of dysphagia Unable to tolerate solids
Lya Crichlow, MD Kings County Hospital Center September 3, 2009 Morbidity and Mortality Conference Case presentation 56 year old male who presented with 1 week history of dysphagia Unable to tolerate solids
Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule
 Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Intraabdominal Roux-en-Y reconstruction with a novel stapling technique after laparoscopic distal gastrectomy
 Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
