Clinical and Pathological Features of Cutaneous Malignant Melanoma: A Retrospective Analysis of 124 Japanese Patients
|
|
|
- Clyde Harmon
- 6 years ago
- Views:
Transcription
1 Clinical and Pathological Features of Cutaneous Malignant Melanoma: A Retrospective Analysis of 24 Japanese Patients Yoshie Kuno, Kazuyuki Ishihara, Naoya Yamazaki and Kiyoshi Mukai 2 'Dermatology Division and 2 Clinical Laboratory Division, National Cancer Center Hospital, Tokyo A review of mainly histopathologic factors associated with the survival of patients with malignant melanoma was carried out in a retrospective study of 24 Japanese patients treated at the National Cancer Center Hospital between July 962 and December 992. There were 6 females and 64 males, and the median follow-up period was 52.7 months (range,. to 25. months). The histologic features included tumor thickness, level of invasion, histologic subtype, ulceration, pigmentation, and cell type. Melanomas thicker than.5 mm (P<.) and with ulceration (P<.) had a significantly worse prognosis. With regard to histologic type, ten-year survival was 65.% for acral lentiginous melanoma, 5.7% for nodular melanoma, and 47.% for superficial spreading melanoma (SSM), there being no significant differences among them. We suggest that the prognosis was affected not by histologic type but by the large radial or vertical growth component. With regard to clinical features, the clinicopathological stage, patient age, and year when the disease was diagnosed were reflected in the prognosis (P<.). Multifactorial analysis showed that the most significant prognostic variables were histopathologic type (SSM or other), stage (I and II or III and IV), and patient age (<7 or 2 7yr). (Jpn J Clin Oncol 26: 44-5, 996) Key words: Cutaneous malignant melanoma Histopathology Prognosis Introduction Since 787, when John Hunter wrote the first description of a patient with malignant melanoma, a 5-year-old man with a recurrent mass behind the angle of the lower jaw, knowledge of the epidemiology, pathology, and treatment of malignant melanoma has advanced considerately. A major step forward was Clark's recognition in 969 that the anatomic level of invasion of malignant melanoma could separate groups of patients with low, intermediate, and high risks of dying due to the disease. Subsequently, Breslow 2 ' recognized that the thickness of the primary tumor could be used to obtain similar information. Because the incidence of cutaneous melanoma in Japan is much lower than that in Western countries with predominantly white population, it has not been possible to amass large series like those which have been used to assess prognostic factors of Received: August, 995 Accepted: November 6, 995 For reprints and all correspondence: Naoya Yamazaki, Dermatology Division, National Cancer Center Hospital, -, Tsukiji 5-chome, Chuo-ku, Tokyo 4 melanoma in white populations. We present here a review of the prognostic factors of primary cutaneous melanoma based on a Japanese patient population. Patients and Methods Between July 962 and December 992, 5 patients with cutaneous melanoma were referred to the National Cancer Center Hospital, Tokyo. Among them, we reanalyzed 2 patients with histopathologically proven primary cutaneous malignant melanoma. We concentrated mainly on histologic features, such as maximum tumor thickness, level of invasion, histologic subtype, ulceration, pigmentation, and cell type, and correlated them with clinical features including patient sex and age, primary site distribution, staging, and changes in survival rate. The age and sex distribution of the patients is shown in Table I, and the primary site and histologic subtype distribution is shown in Table II. Melanomas were divided into the following groups based on total vertical height: Group I melanoma in situ Group II melanomas 5=.75 mm thick 44 Jpn J Clin Oncol 26() 996 on 29 November 27
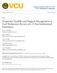
2 CLINICOPATHOLOGICAL ANALYSIS OF MELANOMA Table I. Patient Sex and Age Table II. Primary Location and Histologic Subtype Age 8 < Total Number of patients Male Female Head and neck Upper limbs Lower limbs Trunk Hand Foot Number of patients SSM LMM ALM NM Undiff Total SSM, superficial spreading melanoma; LMM, lentigo maligna melanoma; ALM, acral lentiginous melanoma; NM, nodular melanoma; Undiff., undifferentiated. Total 4(.%) 8 (6.5%) (.5%) 8 (4.5%) 2 (8.5%) 48 (8.7%) Fig.. Survival of 24 melanoma patients. Five-year overall survival rate was 6.6% and tenyear survival 56.9%. Group III melanomas >.75 mm and ^.5 mm thick Group IV melanomas >.5 mm and ^. mm thick Group V melanomas >. mm and ^4. mm thick Group VI melanomas >4. mm thick Tumor thickness was measured according to Breslow's method using on ocular micrometer. Level of invasion was determined according to Clark." Histologic subtypes were classified into four: (I) superficial spreading melanoma (SSM), (II) lentigo maligna melanoma (LMM), (III) acral lentiginous melanoma (ALM), and (IV) nodular melanoma (NM). All patients were retrospectively staged clinicopathologically as follows: Stage I localized primary melanoma, sl.5 mm thick Stage II localized primary melanoma, >.5 mm and <4. mm thick Stage HI metastasis to regional lymph nodes or melanomas thicker than 4. mm Stage IV disseminated melanoma Survival curves were calculated based on the method of Kaplan and Meier. ' The generalized Wilcoxon method 4 and long-rank method 5 ' were used to determine whether differences between curves were significant. Results The median follow-up period was 52.7 months (range,.-25. mo) for 24 patients and 87.9 months (range, mo) for 77 patients still alive at the time of the study. The overall survival rate for the 24 patients was 6.6% at 5 years and 56.9% at years (Fig. ). 45 on 29 November 27
3 KUNO ET AL Fig. 2. Overall survival curve according to age., <4 years (2);, 4-49 years (25);, 5-59 years ();, 6-69 years (26);, 7 years and over (24). The survival rate at 5 years was.6 for patients aged <4 years,.66 for those aged 4-49 years,.67 for those aged 5-59 years,.77 for those aged 6-69 years, and.6 for those aged 7 years and over. There was a significant difference between patients aged 7 years and over and those younger than 7 years (P<.). Clinical Factors (A) Patient Age and Sex: The median age of the 24 patients was 54 years. Those aged 7 years and over had a worse survival rate than those younger than 7 (P<.) (Fig. 2). Among stage III cases, the probability of survival was similar, the survival rates at 5 years being 6.% for patients < 4 years old, 62.5<Vo for those aged 4-49 years, 66.4% for those aged 5-59 years, 58.7% for those aged 6-69 years, and 2.% for those aged 7 years or over. All but one patient older than 7 died of melanoma. Overall, melanomas affected females and males almost equally (5.6% versus 48.4%). In our analysis, there was no significant difference in survival between the sex (Fig. ). (B) Anatomic Location of the Primary Lesion: Melanomas were divided evenly between two major anatomic locations: 49.2% were on the lower extremities, and 5.2% occurred at other sites (Table II). The five-year survival rate of patients with melanomas on the lower extremities (including the foot) was 64.8%, whereas that of patients with tumor at other sites was 49.7%. Patients with melanomas of the trunk had the worst 5-year survival rate of 7.9%. However, there was no significant difference in survival among any of the primary sites of melanoma. In our analysis, patients with melanomas on the sole showed better survival than those with lesions at other sites (Table III). (C) Staging: The overall survival of the 24 patients according to melanoma stage is shown in Fig. 4. Nine lesions of melanoma in situ or Clark's level I Fig.. Overall survival curve according to sex. male (64);, female (6). The survival rate at 5 years and years was.69 and.69 for females and.62 and.48 for males, respectively. There was no significant difference. Table III. Anatomic Location of Primary Melanoma Lower extremity (except foot and sole) Foot (except sole) Sole Upper extremity (except hand) Hand Trunk Head and neck No., number of patients. No Overall survival (%) 5-year -year L.L IC..:J..L JLL I Fig. 4. Overall survival curve according to staging. -, stage I (27);, stage II (25);, stage III (54);, stage IV (9). There was a significant difference between stages I+ and stages HI + IV (P<.). 46 Jpn J Clin Oncol 26() 996 on 29 November 27
4 CLINICOPATHOLOGICAL ANALYSIS OF MELANOMA Table IV. Staging Analysis Sex male female Pigmentation present absent Margin Ulcer positive negative present absent Age at diagnosis <7 7 and over Year of treatment < Stages I and II No. P value P<.5 No., number of patients;, not significant Stages III and IV No. P value P<. Fig. 5. Overall survival curve of 54 patients with stage III. -, T4aN(2);, T4aNl ();, any T (without T4a)Nl (2). The survival rate at 5 years was.79 with T4aN and.6 with any TNI and T4aNl. There was a significant difference between patients with localized disease and those with regional disease (P<.). were excluded. The five-year survivals for patients with stage I, II, III and IV lesions were 86.7%, 74.%, 5.% and 22.5%, respectively. There was a significant difference in survival between stages II and HI (P<.5) and between stages HI and IV (P<.5), and there was a more significant difference between stages (I+ ) and (III + IV) (P<.). Univariate analysis showed a very significant difference between stages, indicating that patients with favorable disease features belonged to stages I and II. Therefore, we compared six factors between stages I and II combined and stages III and IV combined. There was no significant difference in the distribution of patients in terms of stage (Table IV). Because stage III was defined as melanoma with metastasis to regional lymph nodes or melanoma thicker than 4. mm, tumors at this stage were divided into the following three groups; (I) melanomas 4. mm or thicker without lymph node metastasis (2 tumors), (II) melanomas 4. mm or thicker with lymph node metastasis (2), and (III) melanomas thinner than 4. mm with lymph node metastasis (). There was a significant difference between groups I and II (P<.) and groups I and III (P<.), but not between groups II and III (Fig. 5). (D) Metastasis: Eighty-four patients with localized melanomas had a -year survival rate of 77.8%. Among patients with regional lymph node Fig. 6. Overall survival curve according to metastasis. -, NM (84);, NM ();, Ml (9). The survival rate at 5 years was.8 for patients with localized melanoma,.6 for those with regional metastasis, and.2 for those with disseminated metastasis. There was a significant difference between patients with localized melanomas and those with metastasis at first diagnosis (P<.). metastasis but no disseminated metastasis, 26 who underwent lymph node dissection (4 patients received radiotherapy and one immunotherapy postoperatively) had a -year survival rate of 2.8%. Nine patients with disseminated melanomas had a 5-year survival rate of 22.2% (Fig. 6). The first sites of distant metastasis were distant lymph nodes (4 cases), skin (), lung (), and brain (). There was a significant difference in survival between patients with localized melanoma and those with melanoma with metastasis (P<.). However, there was no significant difference in survival between melanoma patients with only regional lymph node metastasis and those with disseminated metastasis. 47 on 29 November 27
5 KUNO ET AL Years Years 8 Fig. 7. Overall survival curve according to Breslow level. -, <.75 mm ();, mm (8);,.5-. mm (26);,.-4. mm ();, >4. mm (48). The survival rate at 5 years was.8 for patients with <.75 mm melanoma,.92 for those with mm,.55 for those with.5-. mm tumors,.55 for those with.-4. mm tumors, and.5 for those with >4. mm tumors. Tumor thickness of.5 mm was an important cut off value for prognosis (P<.). Three melanomas thicker than the size of the specimen were excluded. Fig. 8. Overall survival curve according to Clark's level., level I ();, level II ();, level III (6);, level IV ();, level V (4). The survival rate at 5 years was.9 for patients with level,.8 for those with level II,.65 for those with level III,.5 for those with level IV, and.42 for those with level V. There was a significant difference between levels I + II + III and levels IV + V (P<.). Twenty melanomas occurring in the nail or genital regions were not classified. Table V. Five-year Survival Rate (%) in Relation to Histologic Subtype and Tumor Thickness Thickness <.75 mm mm.5-. mm.-4. mm 4. mm< SSM LMM... _ 5. ALM NM _ SSM, superficial spreading melanoma; LMM, lentigo maligna melanoma; ALM, acral lentiginous melanoma; NM, nodular melanoma. Fig. 9. Overall survival curve according to histologic subtype., superficial spreading melanoma (SSM) (4);, lentigo maligna melanoma (LMM) (6);, acral lentiginous melanoma (ALM) (44);, nodular melanoma (NM) (2). The survival rate at 5 years was.5 for SSM,.79 for LMM,.7 for ALM, and.52 for NM. On univariate analysis there was no significant difference. One melanoma had unclassified histology. Histopathological Factors (A) Tumor Thickness and Level of Invasion: Nine patients were classsified as group I, in group II, 8 in group III, 26 in group IV, 4 in group V, and 48 in group VI. Ten patients were classified as having level I melanoma, level II, 6 level III, level IV, and 4 level V. Twenty cases could not be classified; they included melanomas of the nail, a genital lesion and cases in which incomplete excision was performed. Figure 7 shows the actuarial survival curve according to tumor thickness. As demonstrated by this curve, a significant difference in survival was found between patients with melanomas thinner than.5 mm and those with melanomas.5 mm or thicker {P<.). Figure 8 shows the actuarial survival curve according to Clark's level. Survival time tended to be shortened for more advanced levels of invasion, but there was no significant difference between the levels. When level I, II and HI patients were collected into one group and level IV and V patients in another, there was a significant difference between the groups (P<.). (B) Histologic Subtype: Figure 9 shows the actuarial survival curve according to histologic subtype. LMM and ALM carried a better prognosis than NM or SSM. In each thickness group, analysis of the histologic subtype also revealed that SSM had a worse prognosis than the other subtypes (Table V), but there were no significant differences between the types. 48 Jpn J Clin Oncol 26() 996 on 29 November 27
6 CLINICOPATHOLOGICAL ANALYSIS OF MELANOMA too 9 Fig.. Overall survival curve according to ulceration. -, present (27);, absent (97). The survival rate at 5 and years was.4 and.27 for melanomas with ulceration and.7 and.66 for those with no ulceration, respectively. On univariable analysis there was a significant difference between presence and absence of ulceration (P<.). Fig.. Overall survival curve according to surgical margin., positive ();, negative (). There was no significant difference. (C) Ulceration (Histopathologic): Twenty-seven (2.8%) melanomas, including about one quarter of all melanomas of the foot, hand, trunk and upper extremities, were ulcerated. More than half of the patients with ulcerated lesions had melanomas thicker than 4. mm. The median thickness of the ulcerated lesions was.8 mm, compared with.8 mm for non-ulcerated lesions. The presence of melanoma ulceration was a significant risk factor for survival (P<.) (Fig. ). (D) Pigmentation: Six melanomas (4.8%) lacked cytoplasmic melanin [stage I (2 melanomas), stage II (), stage III (2), stage IV ()]. The presence of melanin in two melanomas could not be ascertained because of decalcification. The ten-year survival rate of patients with amelanotic lesions was 6.%, compared with 5.9% for patients with pigmented lesions. (E) Cell Type: The cell types constituting the bulk of the primary melanomas were divided into four groups: epitheloid, spindle, polymorphic and mixed. Ninety-six melanomas (77.4%) were of the epitheloid cell type. There was no significant difference in patient survival between the cell types. (F) Surgical Margin (Histopathologic): Histologic examination demonstrated the presence of malignant cells at the margin in cases which did not include incisional biopsy cases. Excluding four cases of disseminated melanoma, wide excision was performed for seven tumors. None of these showed documented local recurrence. The ten-year survival rate of patients with positive surgical margins was 2.%, whereas that of patients with negative margins was 6.%. There was no significant difference in survival in terms of surgical margin (Fig. ). 9 SO S 7 S 6 < I 5 "a I 2 6 Years Fig. 2. Overall survival curve according to period of initial presentation., < 977 (29);, (29)., (6);, (). There was a significant difference in survival between the period before 977 and each period after 977 (P<.). Other Factors We divided the patients into four chronological groups so that certain comparisons could be made concerning the behavior of melanoma over a -year period. In these groups, the proportion of stage I and II patients increased gradually with time from 24.% to 7.9%, 44.4% and 6.%, respectively, suggesting that the number of patients treated while the melanoma was still at an early stage had increased in recent years. For the last 5 years, we partitioned off three groups, one for every 5-year period; between 978 and 982 for the first period, between 98 and 987 for the second, and between 988 and 992 for the most recent. There was a significant difference in survival between the first group and the other groups (P<.) (Fig. 2). However, for 84 melanoma patients.49 on 29 November 27
7 KUNO ET AL. 9 8 S* 7 I 6 2 Fig.. Overall survival curve according to period of initial presentation and metastasis., <977 with no metastasis ();, < 977 with metastasis (8);, > 978 with no metastasis (7);, > 978 with metastasis (22). There was no significant difference among the groups. Table VI. Multivariate Analysis P value Hazard Lower Upper rate ratio Type (SSM or other) Stage (I and II or III and IV) Age(<7or and over) Breslow (<.5 or and over) Ulcer (+ or-) SSM, superficial spreading melanoma. without metastasis, and for 4 with metastasis, there was no significant difference in survival before and after 977 (Fig. ). Multivariate analysis showed that only histologic type (SSM or other), stage (I and II or III and IV), and patient age (<7 or 7 and over) were significant factors (Table VI). Discussion Tumor thickness has consistently been reported to be the most important independent prognostic variable in melanoma, 6 " 8 ' and in fact has been used as a quantitative parameter for defining subsets of patients with different survival rates. Patients with melanoma thicker than.5 mm had high mortality rates in the present study, similar to previous reports from Japan and Western countries. Although pathologic ulceration was shown to be highly significant by univariate analysis (P<.), it was not significant by multivariate analysis. Ulceration has been shown to be dependent on tumor thickness. Controversy exists as to whether the levels proposed by Clark" have any prognostic significance. In our examination of the -year survival rate, an increase in Clark's level was correlated with a shortened survival time. Although Clark's level was shown to be highly significant by univariate analysis (P<.), no significance was demonstrable by multivariate analysis. Its prognostic importance was replaced by the Breslow thickness. Among the four major histologic types, several studies have shown that SSM and LMM have a better patient survival rate than NM and ALM. 8 " " In the present study, there was no significant difference in survival between these types, although tumor thickness and stage for four types did not differ significantly. The prognosis of patients with ALM, which represents about 46% of all melanomas in Japanese, I2) has been reported to be very poor. ' However in our analysis, the survival rate of patients with ALM,-which accounts for 5.5% of all melanomas, was not poor. It has been suggested that the prognosis of ALM is worse because many cases are at an advanced stage at detection. In our series, however, the prognosis of ALM was rather better than that of SSM at the advanced stage. The year survival of patients with acral SSM and NM was 4.% and 6.4%, respectively, reflecting the lack of a significant difference between ALM and SSM or NM,(the -year survival of ALM patients was 65.%). It was suggested that acral melanoma with a large radical or vertical growth component has a worse prognosis. In surgical therapy for acral lesions, decisions about removal are made on the basis of tumor thickness. Fundamentally, patients with subungual melanoma underwent amputation and those with tumors at other subsites received wide excision with a margin of to 5 cm. If melanomas were thicker than level IV and 4. mm, elective lymph node dissection was performed. Patient age was correlated with melanoma thickness, and older patients presented with thicker lesions. 5 ' In our study, patients aged 7 years and over had a less favorable prognosis, and all except one died of malignant melanoma. The median tumor thickness for melanoma patients in their 7th, 4th and 6th decades was 2. mm, compared with.5 mm for those in their 5th decade or in their rd decade or youngers. Thus, the distribution of melanoma depth was similar in each age group, as were the histologic subtype and stage. It was sug- 5 Jpn J Clin Oncol 26() 996 on 29 November 27
8 CLINICOPATHOLOGICAL ANALYSIS OF MELANOMA gested that age at initial diagnosis is an independent prognostic factor. Patients with stage III melanoma had a 5-year survival rate of 5.%. If regional metastasis was excluded, the rate was 78.5%. Patients with regional lymph node metastases at stage III had a 5-year survival rate of 6.%. Our analysis indicated that patients with stage III disease are better divided into two groups according to regional metastasis, as recommended by Worth et al. 5) or the American Joint Committee on Cancer. 6 * Over a -year period, the 5-year survival rate gradually improved, possibly because of the increased proportion of cases detected at an early stage. Various single- and multiple-agent chemotherapy regimens, including Dacarbazine (DTIC) [5-(,-dimethyl- -trazeno)-imidazole-4-carboxamide], have been used since 977. In fact, 7.7% of melanomas detected after 977 were treated by DTIC chemotherapy. From our data, it is unclear whether chemotherapy is a significant factor in survival. The role of combination chemotherapy in the treatment of melanoma is still controversial, 7 ' 8) and it is necessary to analyze further the correlation between treatment and survival. A review of the literature shows that certain histologic features are significant prognostic factors for survival. From our histopathologic analysis, melanomas thicker than.5 mm, with ulceration, and those showing a large radial or vertical growth component, had a worse prognosis, and clinically, melanoma patients aged 7 years and over and those with lesion on the trunk had a poor prognosis. Multifactorial analysis showed that the dominant factors affecting survival were (I) histologic type, (II) stage, and (III) age. References ) Clark WH Jr: The histogenesis and biologic behavior of primary human malignant melanomas of the skin. Cancer Res 29: , 969 2) Breslow A: Thickness, cross-sectional areas and depth of invasion in the prognosis of cutaneous melanoma. Ann Surg 72: 92-98, 97 ) Kaplan EL, Meier P: Nonparametric estimation from incomplete observation. I. Am Stat Assoc 5: , 958 4) Gehan E: A generalized Wilcoxon test for comparing arbitrarily single-censored samples! Biometrika 52: 2-224, 965 5) Peto R, Pike MC: Conservation of the approximation a (O-E)2/E in the log-rank test for survival data or tumor incidence data. Biometrics 29: , 97 6) Balch CM, Murad TM, Soong SJ, Ingalls AL, Halpern NB, Maddox WA: A multifactorial analysis of melanoma: prognostic histopathological features comparing Clark's and Breslow's staging methods. Ann Surg 88: , 978 7) Prade M, Bognel C, Charpentier P, Gadenne C, Duvillard P, Sancho-Garnier H, Petit JY: Malignant melanoma of the skin: prognostic factors derived from a multifactorial analysis of 29 cases. Am J Dermatopathol 4: 4-42, 982 8) Balch CM, Soong S-J, Shaw HM, Urist MM, McCarthy WH: An analysis of prognostic factors in 85 patients with cutaneous melanoma. In Cutaneous Melanoma, 2nd ed, Balch CM, JB Lippencott, Philadelphia. pl65-87, 992 9) Harrist TJ, Rigel DS, Day CL Jr, Sober AJ, Lew RA, Phodes AR, Harris MN, Kopf AW, Friedman RJ, Golomb FM Cosimi B, Gorstein F, Malt RA, Wood WC, Postel Hennesy P, Gumport SL, Roses DF, Minitzis MM, Raker JW, Fitzpatrick TB, Mihm MC: "Microscopic satellites" are more highly associated with regional lymph node metastases than is primary melanoma thickness. Cancer 5: , 984 ) Van der Esch EP, Cascinelli N, Preda F, Morabito A, Bufalino R: Stage I melanoma of the skin: evaluation of prognosis according to histologic characteristics. Cancer 48: , 98 ) Hacene K, Le Doussal V, Brunet M, Lemoine F, Guerin P, Hebert H: Prognostic index for clinical stage I cutaneous malignant melanoma. Cancer Res 4: , 98 2) Seiji M, Takematsu H, Hosokawa M, Obata M, Tomita Y, Kato T, Takahashi M, Mihm MC Jr: Acral melanoma in Japan. / Invest Dermatol 8: 56-6, 98 ) KcGovern VJ, Murad TM: Pathology of melanoma: clinical management and treatment results worldwide. In Cutaneous Melanoma, Balch CM, JB Lippencott, Philadelpha. p29, 985 4) Patterson RH, Helwig EB: Subungual malignant melanoma: a clinical-pathologic study. Cancer 46: , 98 5) Worth AJ, Gallagher RP, Elwood JM, Yang PC, Lamb C, Spinelli JJ, Wood WS, Threlfall WJ, Hill GB: Pathologic prognostic factors for cutaneous malignant melanoma: the Western Canada Melanoma Study. Int J Cancer 4: 7-75, 989 6) Beahrs OH, Myers MH: Manual for Staging of Cancer: American Joint Committee on Cancer. JB Lippencott, Philadelphia, p.7, 98 7) Houghton AN, Legha S, Bajorin DF: Chemotherapy for Metastatic Melanoma. In Cutaneous Melanoma. 2nd ed, Balch CM, JB Lippencott, Philadelphia. P498-58, 992 8) David R. Umberto V. John M: Malignant melanoma. Proceedings of ASCO 2: 8-94, 99 5 on 29 November 27
Malignant Melanoma in Turkey: A Single Institution s Experience on 475 Cases
 Malignant Melanoma in Turkey: A Single Institution s Experience on 475 Cases Faruk Tas, Sidika Kurul, Hakan Camlica and Erkan Topuz Institute of Oncology, Istanbul University, Istanbul, Turkey Received
Malignant Melanoma in Turkey: A Single Institution s Experience on 475 Cases Faruk Tas, Sidika Kurul, Hakan Camlica and Erkan Topuz Institute of Oncology, Istanbul University, Istanbul, Turkey Received
Katsuhiro Yamada, Natsuko Noguti, Masaaki Tsuda, Hazime Nagato, Naoko Hasunuma, Yoshihiro Umebayashi and Motomu Manabe
 Akita J Med 36 : 45-52, 2009 45 Katsuhiro Yamada, Natsuko Noguti, Masaaki Tsuda, Hazime Nagato, Naoko Hasunuma, Yoshihiro Umebayashi and Motomu Manabe (Received 22 December 2008, Accepted 15 January 2009)
Akita J Med 36 : 45-52, 2009 45 Katsuhiro Yamada, Natsuko Noguti, Masaaki Tsuda, Hazime Nagato, Naoko Hasunuma, Yoshihiro Umebayashi and Motomu Manabe (Received 22 December 2008, Accepted 15 January 2009)
Acral Melanoma in Japan
 Acral Melanoma in Japan MAKOTO SEUI, M.D., HIDEAKI TAKEMATSU, M.D., MICHIKO HOSOKAWA, M.D., MASAAKI OBATA, M.D., YASUSHI TOMITA, M.D., TAIZO KATO, M.D., MASAAKI TAKAHASHI, M.D., AND MARTIN C. MIHM, JR.,
Acral Melanoma in Japan MAKOTO SEUI, M.D., HIDEAKI TAKEMATSU, M.D., MICHIKO HOSOKAWA, M.D., MASAAKI OBATA, M.D., YASUSHI TOMITA, M.D., TAIZO KATO, M.D., MASAAKI TAKAHASHI, M.D., AND MARTIN C. MIHM, JR.,
Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival
 MOLECULAR AND CLINICAL ONCOLOGY 7: 1083-1088, 2017 Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival FARUK TAS
MOLECULAR AND CLINICAL ONCOLOGY 7: 1083-1088, 2017 Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival FARUK TAS
Polypoid Melanoma, A Virulent Variant of the Nodular Growth Pattern
 Polypoid Melanoma, A Virulent Variant of the Nodular Growth Pattern ELIZABETH A. MANCI, M.D., CHARLES M. BALCH, M.D..TARIQ M. MURAD, M.D., PH.D., AND SENG/JAW SOONG, PH.D. Manci, Elizabeth A., Balch, Charles
Polypoid Melanoma, A Virulent Variant of the Nodular Growth Pattern ELIZABETH A. MANCI, M.D., CHARLES M. BALCH, M.D..TARIQ M. MURAD, M.D., PH.D., AND SENG/JAW SOONG, PH.D. Manci, Elizabeth A., Balch, Charles
ORIGINAL ARTICLE. Clinical Node-Negative Thick Melanoma
 ORIGINAL ARTICLE Clinical Node-Negative Thick Melanoma George I. Salti, MD; Ashwin Kansagra, MD; Michael A. Warso, MD; Salve G. Ronan, MD ; Tapas K. Das Gupta, MD, PhD, DSc Background: Patients with T4
ORIGINAL ARTICLE Clinical Node-Negative Thick Melanoma George I. Salti, MD; Ashwin Kansagra, MD; Michael A. Warso, MD; Salve G. Ronan, MD ; Tapas K. Das Gupta, MD, PhD, DSc Background: Patients with T4
Surgical Margins in Cutaneous Melanoma (2 cm Versus 5 cm for Lesions Measuring Less Than 2.1-mm Thick)
 1941 Surgical Margins in Cutaneous Melanoma (2 cm Versus 5 cm for Lesions Measuring Less Than 2.1-mm Thick) Long-Term Results of a Large European Multicentric Phase III Study David Khayat, M.D., Ph.D.
1941 Surgical Margins in Cutaneous Melanoma (2 cm Versus 5 cm for Lesions Measuring Less Than 2.1-mm Thick) Long-Term Results of a Large European Multicentric Phase III Study David Khayat, M.D., Ph.D.
Melanoma of the Skin INTRODUCTION SUMMARY OF CHANGES
 24 Melanoma of the Skin C44.0 Skin of lip, NOS C44.1 Eyelid C44.2 External ear C44.3 Skin of other and unspecified parts of face C44.4 Skin of scalp and neck C44.5 Skin of trunk C44.6 Skin of upper limb
24 Melanoma of the Skin C44.0 Skin of lip, NOS C44.1 Eyelid C44.2 External ear C44.3 Skin of other and unspecified parts of face C44.4 Skin of scalp and neck C44.5 Skin of trunk C44.6 Skin of upper limb
Melanoma of the Skin
 24 Melanoma of the Skin C44.0 Skin of lip, NOS C44.1 Eyelid C44.2 External ear C44.3 Skin of other and unspecified parts of face C44.4 Skin of scalp and neck C44.5 Skin of trunk C44. Skin of upper limb
24 Melanoma of the Skin C44.0 Skin of lip, NOS C44.1 Eyelid C44.2 External ear C44.3 Skin of other and unspecified parts of face C44.4 Skin of scalp and neck C44.5 Skin of trunk C44. Skin of upper limb
Melanoma Underwriting Presented at 2018 AHOU Conference. Hank George FALU
 Melanoma Underwriting Presented at 2018 AHOU Conference Hank George FALU MELANOMA EPIDEMIOLOGY 70-80,000 American cases annually Majority are in situ or thin > 20% are diagnosed age 45 8-9,000 melanoma
Melanoma Underwriting Presented at 2018 AHOU Conference Hank George FALU MELANOMA EPIDEMIOLOGY 70-80,000 American cases annually Majority are in situ or thin > 20% are diagnosed age 45 8-9,000 melanoma
ORIGINAL ARTICLE Cutaneous malignant melanoma: clinical and histopathological review of cases in a Malaysian tertiary referral centre
 Malaysian J Pathol 202; (2) : 97 0 ORIGINAL ARTICLE Cutaneous malignant melanoma: clinical and histopathological review of cases in a Malaysian tertiary referral centre Jayalakshmi PAILOOR, Kein-Seong
Malaysian J Pathol 202; (2) : 97 0 ORIGINAL ARTICLE Cutaneous malignant melanoma: clinical and histopathological review of cases in a Malaysian tertiary referral centre Jayalakshmi PAILOOR, Kein-Seong
Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy
 Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy Dale Han, MD Assistant Professor Department of Surgery Section of Surgical Oncology No disclosures Background Desmoplastic melanoma (DM)
Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy Dale Han, MD Assistant Professor Department of Surgery Section of Surgical Oncology No disclosures Background Desmoplastic melanoma (DM)
Melanoma. Kaushik Mukherjee MD A. Scott Pearson MD
 Melanoma Kaushik Mukherjee MD A. Scott Pearson MD Disclosures You still have to study Not all inclusive No Western blots Extensive use of Google Image Search and Sabiston Melanoma Basics 8 th most common
Melanoma Kaushik Mukherjee MD A. Scott Pearson MD Disclosures You still have to study Not all inclusive No Western blots Extensive use of Google Image Search and Sabiston Melanoma Basics 8 th most common
Racial differences in six major subtypes of melanoma: descriptive epidemiology
 Wang et al. BMC Cancer (2016) 16:691 DOI 10.1186/s12885-016-2747-6 RESEARCH ARTICLE Racial differences in six major subtypes of melanoma: descriptive epidemiology Yu Wang 1, Yinjun Zhao 2 and Shuangge
Wang et al. BMC Cancer (2016) 16:691 DOI 10.1186/s12885-016-2747-6 RESEARCH ARTICLE Racial differences in six major subtypes of melanoma: descriptive epidemiology Yu Wang 1, Yinjun Zhao 2 and Shuangge
Sentinel Lymph Node Status is the Most Important Prognostic Factor in Patients With Melanoma of the Scalp
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Sentinel Lymph Node Status is the Most Important Prognostic Factor in Patients With Melanoma of the Scalp
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Sentinel Lymph Node Status is the Most Important Prognostic Factor in Patients With Melanoma of the Scalp
Characteristics and Treatment of Cutaneous Melanoma of the Foot
 Characteristics and Treatment of Cutaneous Melanoma of the Foot Kyung Wook Nam, Yong Chan Bae,, Soo Bong Nam, Joo Hyung Kim, Hoon Soo Kim, Young Jin Choi Department of Plastic and Reconstructive Surgery,
Characteristics and Treatment of Cutaneous Melanoma of the Foot Kyung Wook Nam, Yong Chan Bae,, Soo Bong Nam, Joo Hyung Kim, Hoon Soo Kim, Young Jin Choi Department of Plastic and Reconstructive Surgery,
Intermediate-Thickness ( mm Thick)
 American Journal of Pathology, Vol. 133, No. 2, November 1988 Copyright American Association of Pathologists The Prognostic Significance of Tumor Vascularity in Intermediate-Thickness (0. 76-4.0 mm Thick)
American Journal of Pathology, Vol. 133, No. 2, November 1988 Copyright American Association of Pathologists The Prognostic Significance of Tumor Vascularity in Intermediate-Thickness (0. 76-4.0 mm Thick)
Johan Lyth, J Hansson, C Ingvar, E Mansson-Brahme, P Naredi, U Stierner, G Wagenius and C Lindholm. Linköping University Post Print
 Prognostic subclassifications of T1 cutaneous melanomas based on ulceration, tumour thickness and Clark s level of invasion: results of a population-based study from the Swedish Melanoma Register Johan
Prognostic subclassifications of T1 cutaneous melanomas based on ulceration, tumour thickness and Clark s level of invasion: results of a population-based study from the Swedish Melanoma Register Johan
Impact of Prognostic Factors
 Melanoma Prognostic Factors: where we started, where are we going? Impact of Prognostic Factors Staging Management Surgical intervention Adjuvant treatment Suraj Venna, MD Assistant Clinical Professor,
Melanoma Prognostic Factors: where we started, where are we going? Impact of Prognostic Factors Staging Management Surgical intervention Adjuvant treatment Suraj Venna, MD Assistant Clinical Professor,
Comparison of Melanoma Subtypes among Korean Patients by Morphologic Features and Ultraviolet Exposure
 Comparison of Melanoma Subtypes in Korean Patients Ann Dermatol Vol. 26, No. 4, 2014 http://dx.doi.org/10.5021/ad.2014.26.4.485 ORIGINAL ARTICLE Comparison of Melanoma Subtypes among Korean Patients by
Comparison of Melanoma Subtypes in Korean Patients Ann Dermatol Vol. 26, No. 4, 2014 http://dx.doi.org/10.5021/ad.2014.26.4.485 ORIGINAL ARTICLE Comparison of Melanoma Subtypes among Korean Patients by
An Overview of Melanoma. Harriet Kluger, M.D. Associate Professor Section of Medical Oncology Yale Cancer Center
 An Overview of Melanoma Harriet Kluger, M.D. Associate Professor Section of Medical Oncology Yale Cancer Center Melanoma Statistics Median age at presentation 45-55 55 years Incidence: 2003 54,200 cases
An Overview of Melanoma Harriet Kluger, M.D. Associate Professor Section of Medical Oncology Yale Cancer Center Melanoma Statistics Median age at presentation 45-55 55 years Incidence: 2003 54,200 cases
Amelanotic melanoma of the skin detailed review of the problem
 of the skin detailed review of the problem Strahil Strashilov 1, Veselin Kirov 2, Angel Yordanov 3, Yoana Simeonova 4 and Miroslava Mihailova 5 1. Department of Plastic Restorative, Reconstructive and
of the skin detailed review of the problem Strahil Strashilov 1, Veselin Kirov 2, Angel Yordanov 3, Yoana Simeonova 4 and Miroslava Mihailova 5 1. Department of Plastic Restorative, Reconstructive and
Breslow Thickness and Clark Level Evaluation in Albanian Cutaneous Melanoma
 Research DOI: 10.6003/jtad.16104a2 Breslow Thickness and Clark Level Evaluation in Albanian Cutaneous Melanoma Daniela Xhemalaj, MD, Mehdi Alimehmeti, MD, Susan Oupadia, MD, Majlinda Ikonomi, MD, Leart
Research DOI: 10.6003/jtad.16104a2 Breslow Thickness and Clark Level Evaluation in Albanian Cutaneous Melanoma Daniela Xhemalaj, MD, Mehdi Alimehmeti, MD, Susan Oupadia, MD, Majlinda Ikonomi, MD, Leart
Malignant tumors of melanocytes : Part 3. Deba P Sarma, MD., Omaha
 Malignant tumors of melanocytes : Part 3 Deba P Sarma, MD., Omaha Let s go over one case of melanoma using the following worksheet. Of the various essential information that needs to be included in the
Malignant tumors of melanocytes : Part 3 Deba P Sarma, MD., Omaha Let s go over one case of melanoma using the following worksheet. Of the various essential information that needs to be included in the
MALIGNANT MELANOMA OF THE HEEL
 MALIGNANT MELANOMA OF THE HEEL Pages with reference to book, From 50 To 53 Fazli M. Qazi ( Departments of Pathology, Khyber Medical College, Peshawar. ) Rahjm Gul ( Departments of Surgery, Khyber Medical
MALIGNANT MELANOMA OF THE HEEL Pages with reference to book, From 50 To 53 Fazli M. Qazi ( Departments of Pathology, Khyber Medical College, Peshawar. ) Rahjm Gul ( Departments of Surgery, Khyber Medical
Bone Metastases in Muscle-Invasive Bladder Cancer
 Journal of the Egyptian Nat. Cancer Inst., Vol. 18, No. 3, September: 03-08, 006 AZZA N. TAHER, M.D.* and MAGDY H. KOTB, M.D.** The Departments of Radiation Oncology* and Nuclear Medicine**, National Cancer
Journal of the Egyptian Nat. Cancer Inst., Vol. 18, No. 3, September: 03-08, 006 AZZA N. TAHER, M.D.* and MAGDY H. KOTB, M.D.** The Departments of Radiation Oncology* and Nuclear Medicine**, National Cancer
Prognostic Variables and Surgical Management of Foot Melanoma: Review of a 25-Year Institutional Experience
 Virginia Commonwealth University VCU Scholars Compass Surgery Publications Dept. of Surgery 11 Prognostic Variables and Surgical Management of Foot Melanoma: Review of a 5-Year Institutional Experience
Virginia Commonwealth University VCU Scholars Compass Surgery Publications Dept. of Surgery 11 Prognostic Variables and Surgical Management of Foot Melanoma: Review of a 5-Year Institutional Experience
Clinical Study Mucosal Melanoma in the Head and Neck Region: Different Clinical Features and Same Outcome to Cutaneous Melanoma
 ISRN Dermatology Volume 2013, Article ID 586915, 5 pages http://dx.doi.org/10.1155/2013/586915 Clinical Study Mucosal Melanoma in the Head and Neck Region: Different Clinical Features and Same Outcome
ISRN Dermatology Volume 2013, Article ID 586915, 5 pages http://dx.doi.org/10.1155/2013/586915 Clinical Study Mucosal Melanoma in the Head and Neck Region: Different Clinical Features and Same Outcome
1 Cancer Council Queensland, Brisbane, Queensland, Australia.
 Title: Diagnosis of an additional in situ does not influence survival for patients with a single invasive : A registry-based follow-up study Authors: Danny R Youlden1, Kiarash Khosrotehrani2, Adele C Green3,4,
Title: Diagnosis of an additional in situ does not influence survival for patients with a single invasive : A registry-based follow-up study Authors: Danny R Youlden1, Kiarash Khosrotehrani2, Adele C Green3,4,
Prognostic Significance of Grading and Staging Systems using MIB-1 Score in Adult Patients with Soft Tissue Sarcoma of the Extremities and Trunk
 843 Prognostic Significance of Grading and Staging Systems using MIB-1 Score in Adult Patients with Soft Tissue Sarcoma of the Extremities and Trunk Tadashi Hasegawa, M.D. 1 Seiichiro Yamamoto, Ph.D. 2
843 Prognostic Significance of Grading and Staging Systems using MIB-1 Score in Adult Patients with Soft Tissue Sarcoma of the Extremities and Trunk Tadashi Hasegawa, M.D. 1 Seiichiro Yamamoto, Ph.D. 2
The Clinical Significance of Tumor-Infiltrating Lymphocytes and Microscopic Satellites in Acral Melanoma in a Korean Population
 Clinical Significance of TIL and Ms in Korean Acral Melanoma Ann Dermatol Vol. 25, No. 1, 2013 http://dx.doi.org/10.5021/ad.2013.25.1.61 ORIGINAL ARTICLE The Clinical Significance of Tumor-Infiltrating
Clinical Significance of TIL and Ms in Korean Acral Melanoma Ann Dermatol Vol. 25, No. 1, 2013 http://dx.doi.org/10.5021/ad.2013.25.1.61 ORIGINAL ARTICLE The Clinical Significance of Tumor-Infiltrating
Protocol applies to melanoma of cutaneous surfaces only.
 Melanoma of the Skin Protocol applies to melanoma of cutaneous surfaces only. Procedures Biopsy (No Accompanying Checklist) Excision Re-excision Protocol revision date: January 2005 Based on AJCC/UICC
Melanoma of the Skin Protocol applies to melanoma of cutaneous surfaces only. Procedures Biopsy (No Accompanying Checklist) Excision Re-excision Protocol revision date: January 2005 Based on AJCC/UICC
Rebecca Vogel, PGY-4 March 5, 2012
 Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
SUBUNGUAL MALIGNANT MELANOMA ON THE RIGHT INDEX IN A DENTIST AFTER PROLONGED OCCUPATIONAL EXPOSURE TO X-RAYS
 SUBUNGUAL MALIGNANT MELANOMA ON THE RIGHT INDEX IN A DENTIST AFTER PROLONGED OCCUPATIONAL EXPOSURE TO X-RAYS J. HATZIS*, V. MAKROPOULOS**, N. AGNANTIS*** * Department of Skin and Venereal Diseases, University
SUBUNGUAL MALIGNANT MELANOMA ON THE RIGHT INDEX IN A DENTIST AFTER PROLONGED OCCUPATIONAL EXPOSURE TO X-RAYS J. HATZIS*, V. MAKROPOULOS**, N. AGNANTIS*** * Department of Skin and Venereal Diseases, University
Sentinel Lymph Node Biopsy in Patients With Thin Melanoma
 STUDY Sentinel Lymph Node Biopsy in Patients With Thin Melanoma Julie B. Lowe, MD; Eva Hurst, MD; Jeffrey F. Moley, MD; Lynn A. Cornelius, MD Objective: To define the percentage of positive sentinel lymph
STUDY Sentinel Lymph Node Biopsy in Patients With Thin Melanoma Julie B. Lowe, MD; Eva Hurst, MD; Jeffrey F. Moley, MD; Lynn A. Cornelius, MD Objective: To define the percentage of positive sentinel lymph
Research Article Melanoma in Buckinghamshire: Data from the Inception of the Skin Cancer Multidisciplinary Team
 Skin Cancer Volume 2013, Article ID 843282, 6 pages http://dx.doi.org/10.1155/2013/843282 Research Article Melanoma in Buckinghamshire: Data from the Inception of the Skin Cancer Multidisciplinary Team
Skin Cancer Volume 2013, Article ID 843282, 6 pages http://dx.doi.org/10.1155/2013/843282 Research Article Melanoma in Buckinghamshire: Data from the Inception of the Skin Cancer Multidisciplinary Team
Case Scenario 1 Worksheet. Primary Site C44.4 Morphology 8743/3 Laterality 0 Stage/ Prognostic Factors
 CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
Ethnic disparities in melanoma diagnosis and survival
 Ethnic disparities in melanoma diagnosis and survival The effects of socioeconomic status and health insurance coverage Amy M. Anderson-Mellies, MPH 1 Matthew J. Rioth, MD 1,2,3 Myles G. Cockburn, PhD
Ethnic disparities in melanoma diagnosis and survival The effects of socioeconomic status and health insurance coverage Amy M. Anderson-Mellies, MPH 1 Matthew J. Rioth, MD 1,2,3 Myles G. Cockburn, PhD
Updates on Melanoma: Are You Following the Latest Guidelines of Care? Jerry Brewer, MD
 Updates on Melanoma: Are You Following the Latest Guidelines of Care? Jerry Brewer, MD Disclosure Statement Update on Melanoma Are You Following the Latest Guidelines of Care? I, Jerry D. Brewer, MD, do
Updates on Melanoma: Are You Following the Latest Guidelines of Care? Jerry Brewer, MD Disclosure Statement Update on Melanoma Are You Following the Latest Guidelines of Care? I, Jerry D. Brewer, MD, do
> 6000 Mutations in Melanoma. Tests That Cay Be Employed. FISH for Additions/Deletions. Comparative Genomic Hybridization
 Winter Clinical 2017: The Assessment and Diagnosis of Melanoma Whitney A. High, MD, JD, MEng Associate Professor, Dermatology & Pathology Director of Dermatopathology (Dermatology) University of Colorado
Winter Clinical 2017: The Assessment and Diagnosis of Melanoma Whitney A. High, MD, JD, MEng Associate Professor, Dermatology & Pathology Director of Dermatopathology (Dermatology) University of Colorado
Springer Healthcare. Staging and Diagnosing Cutaneous Melanoma. Concise Reference. Dirk Schadendorf, Corinna Kochs, Elisabeth Livingstone
 Concise Reference Staging and Diagnosing Cutaneous Melanoma Dirk Schadendorf, Corinna Kochs, Elisabeth Livingstone Extracted from Handbook of Cutaneous Melanoma: A Guide to Diagnosis and Treatment Published
Concise Reference Staging and Diagnosing Cutaneous Melanoma Dirk Schadendorf, Corinna Kochs, Elisabeth Livingstone Extracted from Handbook of Cutaneous Melanoma: A Guide to Diagnosis and Treatment Published
Prognostic value of tumour thickness in cutaneous malignant melanoma
 J Clin Pathol 1983;36:51-56 Prognostic value of tumour thickness in cutaneous malignant melanoma IONA JEFFREY, PATRICK ROYSTON, CHRISTOPHER SOWTER, GERARD SLAVIN, ASHLEY PRICE, ARIELA POMERANCE,* SALEEM
J Clin Pathol 1983;36:51-56 Prognostic value of tumour thickness in cutaneous malignant melanoma IONA JEFFREY, PATRICK ROYSTON, CHRISTOPHER SOWTER, GERARD SLAVIN, ASHLEY PRICE, ARIELA POMERANCE,* SALEEM
Melanoma-Back to Basics I Thought I Knew Ya! Paul K. Shitabata, M.D. Dermatopathologist APMG
 Melanoma-Back to Basics I Thought I Knew Ya! Paul K. Shitabata, M.D. Dermatopathologist APMG At tumor board, a surgeon insists that all level II melanomas are invasive since they have broken through the
Melanoma-Back to Basics I Thought I Knew Ya! Paul K. Shitabata, M.D. Dermatopathologist APMG At tumor board, a surgeon insists that all level II melanomas are invasive since they have broken through the
CUTANEOUS MALIGNANT MELANOMA IN SWEDISH CHILDREN AND TEENAGERS : A CLINICO-PATHOLOGICAL STUDY OF 130 CASES
 Int. J. Cancer: 80, 646 65 (999) 999 Wiley-Liss, Inc. Publication of the International Union Against Cancer Publication de l Union Internationale Contre le Cancer CUTANEOUS MALIGNANT MELANOMA IN SWEDISH
Int. J. Cancer: 80, 646 65 (999) 999 Wiley-Liss, Inc. Publication of the International Union Against Cancer Publication de l Union Internationale Contre le Cancer CUTANEOUS MALIGNANT MELANOMA IN SWEDISH
Melanoma and Dermoscopy. Disclosure Statement: ABCDE's of melanoma. Co-President, Usatine Media
 Melanoma and Dermoscopy Richard P. Usatine, MD, FAAFP Professor, Family and Community Medicine Professor, Dermatology and Cutaneous Surgery Medical Director, University Skin Clinic University of Texas
Melanoma and Dermoscopy Richard P. Usatine, MD, FAAFP Professor, Family and Community Medicine Professor, Dermatology and Cutaneous Surgery Medical Director, University Skin Clinic University of Texas
WHAT DOES THE PATHOLOGY REPORT MEAN?
 Melanoma WHAT IS MELANOMA? Melanoma is a type of cancer that affects cells called melanocytes. These cells are found mainly in skin but also in the lining of other areas such as nose and rectum, and also
Melanoma WHAT IS MELANOMA? Melanoma is a type of cancer that affects cells called melanocytes. These cells are found mainly in skin but also in the lining of other areas such as nose and rectum, and also
Time Course and Pattern of Metastasis of Cutaneous Melanoma Differ between Men and Women
 Time Course and Pattern of Metastasis of Cutaneous Melanoma Differ between Men and Women Liljana Mervic 1,2 * 1 Department of Dermatology, Center of Dermatooncology, University of Tüebingen, Germany, 2
Time Course and Pattern of Metastasis of Cutaneous Melanoma Differ between Men and Women Liljana Mervic 1,2 * 1 Department of Dermatology, Center of Dermatooncology, University of Tüebingen, Germany, 2
Contrast with Australian Guidelines A/Pr Pascale Guitera,
 Contrast with Australian Guidelines A/Pr Pascale Guitera, Dermatologist, Sydney University NO CONFLICT OF INTEREST Sydney Melanoma Diagnostic Centre, RPAH 2011 2008 225 pages 16 pages http://www.cancer.org.au/file/healthprofessionals/clinica
Contrast with Australian Guidelines A/Pr Pascale Guitera, Dermatologist, Sydney University NO CONFLICT OF INTEREST Sydney Melanoma Diagnostic Centre, RPAH 2011 2008 225 pages 16 pages http://www.cancer.org.au/file/healthprofessionals/clinica
Measurement of c-myc oncogene expression provides an accurate prognostic marker for acral lentiginous melanoma
 British Journal of Plastic Surgery (1999), 52, 122 126 1999 The British Association of Plastic Surgeons Measurement of c-myc oncogene expression provides an accurate prognostic marker for acral lentiginous
British Journal of Plastic Surgery (1999), 52, 122 126 1999 The British Association of Plastic Surgeons Measurement of c-myc oncogene expression provides an accurate prognostic marker for acral lentiginous
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Cutaneous Melanoma: Epidemiology (USA) The Sentinel Node in Head and Neck Melanoma. Cutaneous Melanoma: Epidemiology (USA)
 The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
PAPER. Prognostic Information From Sentinel Lymph Node Biopsy in Patients With Thick Melanoma
 PAPER Prognostic Information From Sentinel Lymph Node Biopsy in Patients With Thick Melanoma Charles R. Scoggins, MD, MBA; Adrianne L. Bowen, MD; Robert C. Martin II, MD, PhD; Michael J. Edwards, MD; Douglas
PAPER Prognostic Information From Sentinel Lymph Node Biopsy in Patients With Thick Melanoma Charles R. Scoggins, MD, MBA; Adrianne L. Bowen, MD; Robert C. Martin II, MD, PhD; Michael J. Edwards, MD; Douglas
This is a repository copy of Easily missed? Amelanotic melanoma. White Rose Research Online URL for this paper:
 This is a repository copy of Easily missed? Amelanotic melanoma. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/127789/ Version: Accepted Version Article: Muinonen-Martin,
This is a repository copy of Easily missed? Amelanotic melanoma. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/127789/ Version: Accepted Version Article: Muinonen-Martin,
Is There a Benefit to Sentinel Lymph Node Biopsy in Patients With T4 Melanoma?
 Is There a Benefit to Sentinel Lymph Node Biopsy in atients With T4 Melanoma? Csaba Gajdos, MD 1 ; Kent A. Griffith, MH, MS 2 ; Sandra L. Wong, MD 1 ; Timothy M. Johnson, MD 1,3 ; Alfred E. Chang, MD 1
Is There a Benefit to Sentinel Lymph Node Biopsy in atients With T4 Melanoma? Csaba Gajdos, MD 1 ; Kent A. Griffith, MH, MS 2 ; Sandra L. Wong, MD 1 ; Timothy M. Johnson, MD 1,3 ; Alfred E. Chang, MD 1
Epithelial Cancer- NMSC & Melanoma
 Epithelial Cancer- NMSC & Melanoma David Chin MB, BCh, BAO, LRCP, LRCS (Ireland) MCh(MD), PhD (UQ), FRCS, FRACS (Plast) Plastic & Reconstructive Surgeon Visiting Scientist Melanoma Genomic Group & Drug
Epithelial Cancer- NMSC & Melanoma David Chin MB, BCh, BAO, LRCP, LRCS (Ireland) MCh(MD), PhD (UQ), FRCS, FRACS (Plast) Plastic & Reconstructive Surgeon Visiting Scientist Melanoma Genomic Group & Drug
After primary tumor treatment, 30% of patients with malignant
 ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter.
 Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
University of Groningen
 University of Groningen Nodular Histologic Subtype and Ulceration are Tumor Factors Associated with High Risk of Recurrence in Sentinel Node-Negative Melanoma Patients Faut, Marloes; Wevers, Kevin; van
University of Groningen Nodular Histologic Subtype and Ulceration are Tumor Factors Associated with High Risk of Recurrence in Sentinel Node-Negative Melanoma Patients Faut, Marloes; Wevers, Kevin; van
12. Malignant Melanoma of Skin
 KEY FACTS 12. Malignant Melanoma of Skin ICD-9 172 On average 160 melanomas of the skin were registered per year. Twice as common in females than in males. Higher than expected numbers in Southern Board
KEY FACTS 12. Malignant Melanoma of Skin ICD-9 172 On average 160 melanomas of the skin were registered per year. Twice as common in females than in males. Higher than expected numbers in Southern Board
Desmoplastic Melanoma R/O BCC. Clinical Information. 74 y.o. man with lesion on left side of neck r/o BCC
 R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
6/22/2015. Original Paradigm. Correlating Histology and Molecular Findings in Melanocytic Neoplasms
 6 Correlating Histology and Molecular Findings in Melanocytic Neoplasms Pedram Gerami MD, Associate Professor of Dermatology and Pediatrics at Northwestern University Disclosures: I have been a consultant
6 Correlating Histology and Molecular Findings in Melanocytic Neoplasms Pedram Gerami MD, Associate Professor of Dermatology and Pediatrics at Northwestern University Disclosures: I have been a consultant
AJCC 8 Implementation January 1, 2018 Melanoma of the Skin. Suraj Venna
 AJCC 8 Implementation January 1, 2018 Melanoma of the Skin Suraj Venna Personalized Medicine AJCC 8 th Edition This Time It s Personal Traditional AJCC (TNM) population-based analyses of large databases
AJCC 8 Implementation January 1, 2018 Melanoma of the Skin Suraj Venna Personalized Medicine AJCC 8 th Edition This Time It s Personal Traditional AJCC (TNM) population-based analyses of large databases
Clinical Pathological Conference. Malignant Melanoma of the Vulva
 Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Dermatopathology. Dr. Rafael Botella Estrada. Hospital La Fe de Valencia
 Dermatopathology Dr. Rafael Botella Estrada. Hospital La Fe de Valencia Melanoma and mimics Dr. Martin Mihm Malignant lesions result from the accumulation of mutations Class I lesions (benign) Class II
Dermatopathology Dr. Rafael Botella Estrada. Hospital La Fe de Valencia Melanoma and mimics Dr. Martin Mihm Malignant lesions result from the accumulation of mutations Class I lesions (benign) Class II
Malignant melanoma of the eyelid skin:
 British Journal of Ophthalmology, 1985, 69, 180-186 Malignant melanoma of the eyelid skin: histopathology and behaviour A GARNER,' L KOORNNEEF,2 A LEVENE,3 AND J R 0 COLLIN4 From the 'Department of Pathology,
British Journal of Ophthalmology, 1985, 69, 180-186 Malignant melanoma of the eyelid skin: histopathology and behaviour A GARNER,' L KOORNNEEF,2 A LEVENE,3 AND J R 0 COLLIN4 From the 'Department of Pathology,
Primary Cutaneous Melanoma Pathology Reporting Proforma DD MM YYYY. *Tumour site. *Specimen laterality. *Specimen type
 Primary Cutaneous Melanoma Pathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth DD MM YYYY Sex Male Female
Primary Cutaneous Melanoma Pathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth DD MM YYYY Sex Male Female
Sentinel Lymph Node Biopsy for the T1 (Thin) Melanoma: Is It Necessary?
 Sentinel Lymph Node Biopsy for the T1 (Thin) Melanoma: Is It Necessary? Maurice Y. Nahabedian, MD Anthony P. Tufaro, MD Paul N. Manson, MD The use of sentinel lymph node biopsy for the T1 melanoma is controversial.
Sentinel Lymph Node Biopsy for the T1 (Thin) Melanoma: Is It Necessary? Maurice Y. Nahabedian, MD Anthony P. Tufaro, MD Paul N. Manson, MD The use of sentinel lymph node biopsy for the T1 melanoma is controversial.
Therapeutic Lymph Node Dissection in Melanoma: Different Prognosis for Different Macrometastasis Sites?
 Ann Surg Oncol (01) 19:91 91 DOI.14/s44-01-401- ORIGINAL ARTICLE MELANOMAS Therapeutic Lymph Node Dissection in Melanoma: Different Prognosis for Different Macrometastasis Sites? K. P. Wevers, MD, E. Bastiaannet,
Ann Surg Oncol (01) 19:91 91 DOI.14/s44-01-401- ORIGINAL ARTICLE MELANOMAS Therapeutic Lymph Node Dissection in Melanoma: Different Prognosis for Different Macrometastasis Sites? K. P. Wevers, MD, E. Bastiaannet,
Malignant Melanoma Early Stage. A guide for patients
 This melanoma patient brochure is designed to help educate melanoma patients and their caregivers. It was developed under the guidance of Dr. Michael Smylie, Professor, Department of Oncology, University
This melanoma patient brochure is designed to help educate melanoma patients and their caregivers. It was developed under the guidance of Dr. Michael Smylie, Professor, Department of Oncology, University
Interesting Case Series. Desmoplastic Melanoma
 Interesting Case Series Desmoplastic Melanoma Anthony Maurice Kordahi, MD, Joshua B. Elston, MD, Ellen M. Robertson, MD, and C. Wayne Cruse, MD Division of Plastic Surgery, Department of Surgery, University
Interesting Case Series Desmoplastic Melanoma Anthony Maurice Kordahi, MD, Joshua B. Elston, MD, Ellen M. Robertson, MD, and C. Wayne Cruse, MD Division of Plastic Surgery, Department of Surgery, University
NAACCR Webinar Series 1
 Collecting Cancer Data: Melanoma 2013 2014 NAACCR Webinar Series April 3, 2014 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
Collecting Cancer Data: Melanoma 2013 2014 NAACCR Webinar Series April 3, 2014 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
Topics for Discussion. Malignant Melanoma. Surgical Treatment. Current Treatment of Cutaneous Melanoma 5/17/2013. Lymph Regional nodes:
 Topics for Discussion What is a sentinel lymph node (SLN)? Utility of sentinel lymph biopsies: therapeutic or staging? Current Treatment of Cutaneous Melanoma Carlos Corvera, M.D. Associate Professor of
Topics for Discussion What is a sentinel lymph node (SLN)? Utility of sentinel lymph biopsies: therapeutic or staging? Current Treatment of Cutaneous Melanoma Carlos Corvera, M.D. Associate Professor of
You Are Going to Cut How Much Skin? Locoregional Surgical Treatment. Justin Rivard MD, MSc, FRCSC September 21, 2018
 You Are Going to Cut How Much Skin? Locoregional Surgical Treatment Justin Rivard MD, MSc, FRCSC September 21, 2018 Presenter Disclosure Faculty/Speaker: Justin Rivard Relationships with financial sponsors:
You Are Going to Cut How Much Skin? Locoregional Surgical Treatment Justin Rivard MD, MSc, FRCSC September 21, 2018 Presenter Disclosure Faculty/Speaker: Justin Rivard Relationships with financial sponsors:
Lung cancer pleural invasion was recognized as a poor prognostic
 Visceral pleural invasion classification in non small cell lung cancer: A proposal on the basis of outcome assessment Kimihiro Shimizu, MD a Junji Yoshida, MD a Kanji Nagai, MD a Mitsuyo Nishimura, MD
Visceral pleural invasion classification in non small cell lung cancer: A proposal on the basis of outcome assessment Kimihiro Shimizu, MD a Junji Yoshida, MD a Kanji Nagai, MD a Mitsuyo Nishimura, MD
Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer. Cheol Min Kang 2018/04/05
 Abstract No.: ABS-0075 Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer 2018/04/05 Cheol Min Kang Department of surgery, University of Ulsan
Abstract No.: ABS-0075 Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer 2018/04/05 Cheol Min Kang Department of surgery, University of Ulsan
Clinical Practice Guidelines
 Clinical Practice Guidelines Clinical Practice Guidelines for Melanoma Douglas Reintgen, MD, et al H. Lee Moffitt Cancer Center & Research Institute These clinical practice guidelines for melanoma have
Clinical Practice Guidelines Clinical Practice Guidelines for Melanoma Douglas Reintgen, MD, et al H. Lee Moffitt Cancer Center & Research Institute These clinical practice guidelines for melanoma have
ORIGINAL ARTICLE. Patterns of Recurrence in Patients With Melanoma After Radical Lymph Node Dissection
 ORIGINAL ARTICLE Patterns of Recurrence in Patients With Melanoma After Radical Lymph Node Dissection Nir Nathansohn, MD, MHA; Jacob Schachter, MD; Haim Gutman, MD Hypothesis: Previous interventions (excisional
ORIGINAL ARTICLE Patterns of Recurrence in Patients With Melanoma After Radical Lymph Node Dissection Nir Nathansohn, MD, MHA; Jacob Schachter, MD; Haim Gutman, MD Hypothesis: Previous interventions (excisional
Talk to Your Doctor. Fact Sheet
 Talk to Your Doctor Hearing the words you have skin cancer is overwhelming and would leave anyone with a lot of questions. If you have been diagnosed with Stage I or II cutaneous melanoma with no apparent
Talk to Your Doctor Hearing the words you have skin cancer is overwhelming and would leave anyone with a lot of questions. If you have been diagnosed with Stage I or II cutaneous melanoma with no apparent
Clinico-pathological Features of Patients with Melanoma and Positive Sentinel Lymph Node Biopsy: A Single Institution Experience
 2015;23(2):122-129 CLINICAL ARTICLE Clinico-pathological Features of Patients with Melanoma and Positive Sentinel Lymph Node Biopsy: A Single Institution Experience Damir Homolak 1, Mirna Šitum 2,3, Hrvoje
2015;23(2):122-129 CLINICAL ARTICLE Clinico-pathological Features of Patients with Melanoma and Positive Sentinel Lymph Node Biopsy: A Single Institution Experience Damir Homolak 1, Mirna Šitum 2,3, Hrvoje
Invasive Cutaneous Malignant Melanoma in Sweden, A Prospective, Population-Based Study of Survival and Prognostic Factors
 2067 Invasive Cutaneous Malignant Melanoma in Sweden, 1990 1999 A Prospective, Population-Based Study of Survival and Prognostic Factors Christer Lindholm, M.D., Ph.D. 1 Ronny Andersson, M.D. 2 * Monika
2067 Invasive Cutaneous Malignant Melanoma in Sweden, 1990 1999 A Prospective, Population-Based Study of Survival and Prognostic Factors Christer Lindholm, M.D., Ph.D. 1 Ronny Andersson, M.D. 2 * Monika
1
 www.clinicaloncology.com.ua 1 Prognostic factors of appearing micrometastases in sentinel lymph nodes in skin melanoma M.N.Kukushkina, S.I.Korovin, O.I.Solodyannikova, G.G.Sukach, A.Yu.Palivets, A.N.Potorocha,
www.clinicaloncology.com.ua 1 Prognostic factors of appearing micrometastases in sentinel lymph nodes in skin melanoma M.N.Kukushkina, S.I.Korovin, O.I.Solodyannikova, G.G.Sukach, A.Yu.Palivets, A.N.Potorocha,
World Articles of Ear, Nose and Throat Page 1
 World Articles of Ear, Nose and Throat ---------------------Page 1 Primary Malignant Melanoma of the Tongue: A Case Report Authors: Nanayakkara PR*, Arudchelvam JD** Ariyaratne JC*, Mendis K*, Jayasekera
World Articles of Ear, Nose and Throat ---------------------Page 1 Primary Malignant Melanoma of the Tongue: A Case Report Authors: Nanayakkara PR*, Arudchelvam JD** Ariyaratne JC*, Mendis K*, Jayasekera
Multiple Primary Melanoma in a Thai Male: A Case Report
 Case Report Multiple Primary Melanoma in a Thai Male: A Case Report J Med Assoc Thai 2014; 97 (Suppl. 2): S234-S238 Full text. e-journal: http://www.jmatonline.com Kittisak Payapvipapong MD*, Pinyapat
Case Report Multiple Primary Melanoma in a Thai Male: A Case Report J Med Assoc Thai 2014; 97 (Suppl. 2): S234-S238 Full text. e-journal: http://www.jmatonline.com Kittisak Payapvipapong MD*, Pinyapat
Long-Term Survival Analysis and Clinical Follow-Up in Acral Lentiginous Malignant Melanoma Undergoing Sentinel Lymph Node Biopsy in Korean Patients
 Ann Dermatol Vol. 26, No. 2, 2014 http://dx.doi.org/10.5021/ad.2014.26.2.177 ORIGINAL ARTICLE Long-Term Survival Analysis and Clinical Follow-Up in Acral Lentiginous Malignant Melanoma Undergoing Sentinel
Ann Dermatol Vol. 26, No. 2, 2014 http://dx.doi.org/10.5021/ad.2014.26.2.177 ORIGINAL ARTICLE Long-Term Survival Analysis and Clinical Follow-Up in Acral Lentiginous Malignant Melanoma Undergoing Sentinel
MOLECULAR ANALYSIS OF A SERIES OF ACRAL MELANOMAS IN SINGAPORE
 MOLECULAR ANALYSIS OF A SERIES OF ACRAL MELANOMAS IN SINGAPORE PoYin Tan Inny Busmanis Dept of Anatomical Pathology, Lynette Oon Head, Molecular Lab Singapore General Hospital ETHNIC GROUPS IN SINGAPORE
MOLECULAR ANALYSIS OF A SERIES OF ACRAL MELANOMAS IN SINGAPORE PoYin Tan Inny Busmanis Dept of Anatomical Pathology, Lynette Oon Head, Molecular Lab Singapore General Hospital ETHNIC GROUPS IN SINGAPORE
SKIN CANCER. Most common cancer diagnosis 40% of all cancers
 SKIN CANCER Most common cancer diagnosis 40% of all cancers OBJECTIVES Review common and uncommon cancers of the skin. Special emphasis on melanoma and dysplastic nevus Review pathology/tnm/staging, which
SKIN CANCER Most common cancer diagnosis 40% of all cancers OBJECTIVES Review common and uncommon cancers of the skin. Special emphasis on melanoma and dysplastic nevus Review pathology/tnm/staging, which
Poor prognosis for thin ulcerated melanomas and implications for a more aggressive approach to treatment
 Poor prognosis for thin ulcerated melanomas and implications for a more aggressive approach to treatment Makenzie L. Hawkins, MSPH 1 Matthew J. Rioth, MD 1,2 Megan M. Eguchi, MPH 1 Myles Cockburn, Phd
Poor prognosis for thin ulcerated melanomas and implications for a more aggressive approach to treatment Makenzie L. Hawkins, MSPH 1 Matthew J. Rioth, MD 1,2 Megan M. Eguchi, MPH 1 Myles Cockburn, Phd
STUDY. CME available online at
 STUDY Survival Differences Between Patients With Scalp or Neck Melanoma and Those With Melanoma of Other Sites in the Surveillance, Epidemiology, and End Results (SEER) Program Anne M. Lachiewicz, MPH;
STUDY Survival Differences Between Patients With Scalp or Neck Melanoma and Those With Melanoma of Other Sites in the Surveillance, Epidemiology, and End Results (SEER) Program Anne M. Lachiewicz, MPH;
Melanoma Update: 8th Edition of AJCC Staging System
 Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis
 Jpn J Clin Oncol 1997;27(5)305 309 Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis -, -, - - 1 Chest Department and 2 Section of Thoracic Surgery,
Jpn J Clin Oncol 1997;27(5)305 309 Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis -, -, - - 1 Chest Department and 2 Section of Thoracic Surgery,
Clinicopathologic Characteristics and Prognosis of Gastric Cancer in Young Patients
 Yonago Acta medica 2012;55:57 61 Clinicopathologic Characteristics and Prognosis of Gastric Cancer in Young Patients Hiroaki Saito, Seigo Takaya, Yoji Fukumoto, Tomohiro Osaki, Shigeru Tatebe and Masahide
Yonago Acta medica 2012;55:57 61 Clinicopathologic Characteristics and Prognosis of Gastric Cancer in Young Patients Hiroaki Saito, Seigo Takaya, Yoji Fukumoto, Tomohiro Osaki, Shigeru Tatebe and Masahide
Peritoneal Involvement in Stage II Colon Cancer
 Anatomic Pathology / PERITONEAL INVOLVEMENT IN STAGE II COLON CANCER Peritoneal Involvement in Stage II Colon Cancer A.M. Lennon, MB, MRCPI, H.E. Mulcahy, MD, MRCPI, J.M.P. Hyland, MCh, FRCS, FRCSI, C.
Anatomic Pathology / PERITONEAL INVOLVEMENT IN STAGE II COLON CANCER Peritoneal Involvement in Stage II Colon Cancer A.M. Lennon, MB, MRCPI, H.E. Mulcahy, MD, MRCPI, J.M.P. Hyland, MCh, FRCS, FRCSI, C.
Advances in Surgical Management of Primary Melanoma: Identifying Patients Who Need More than Conventional Wide Local Excision
 Advances in Surgical Management of Primary Melanoma: Identifying Patients Who Need More than Conventional Wide Local Excision Christopher J. Miller, MD Director of Penn Dermatology Oncology Center Associate
Advances in Surgical Management of Primary Melanoma: Identifying Patients Who Need More than Conventional Wide Local Excision Christopher J. Miller, MD Director of Penn Dermatology Oncology Center Associate
Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology
 Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology Outline Germline testing CDKN2A BRCA2 BAP1 Somatic testing Gene expression profiling (GEP) BRAF Germline vs Somatic testing
Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology Outline Germline testing CDKN2A BRCA2 BAP1 Somatic testing Gene expression profiling (GEP) BRAF Germline vs Somatic testing
Identifying Skin Cancer. Mary S. Stone MD Professor of Dermatology and Pathology University of Iowa Carver College of Medicine March, 2018
 Identifying Skin Cancer Mary S. Stone MD Professor of Dermatology and Pathology University of Iowa Carver College of Medicine March, 2018 American Cancer Society web site Skin Cancer Melanoma Non-Melanoma
Identifying Skin Cancer Mary S. Stone MD Professor of Dermatology and Pathology University of Iowa Carver College of Medicine March, 2018 American Cancer Society web site Skin Cancer Melanoma Non-Melanoma
Malignant Melanoma of the Head and Neck: A Brief Review of Pathophysiology, Current Staging, and Management
 The Ochsner Journal 8:181 185, 2008 f Academic Division of Ochsner Clinic Foundation Malignant Melanoma of the Head and Neck: A Brief Review of Pathophysiology, Current Staging, and Management Christian
The Ochsner Journal 8:181 185, 2008 f Academic Division of Ochsner Clinic Foundation Malignant Melanoma of the Head and Neck: A Brief Review of Pathophysiology, Current Staging, and Management Christian
