PO Box 2345, Beijing , China World J Gastroenterol 2005;11(44): World Journal of Gastroenterology ISSN
|
|
|
- Merilyn Cannon
- 6 years ago
- Views:
Transcription
1 PO Box 2345, Beijing 00023, China World J Gastroenterol 2005;(44): World Journal of Gastroenterology ISSN wjg@wjgnet.com ELSEVIER 2005 The WJG Press and Elsevier Inc. All rights reserved. CLINICAL RESEARCH Appropriateness of indication and diagnostic yield of colonoscopy: First report based on the 2000 guidelines of the American Society for Gastrointestinal Endoscopy Iqbal Siddique, Krishna Mohan, Fuad Hasan, Anjum Memon, Istvan Patty, Basil Al-Nakib Iqbal Siddique, Fuad Hasan, Basil Al-Nakib, Department of Medicine, Faculty of Medicine, Kuwait University, Kuwait Iqbal Siddique, Krishna Mohan, Fuad Hasan, Istvan Patty, Basil Al-Nakib, Thunayan Al-Ghanim Gastroenterology Center, Al-Amiri Hospital, Kuwait Anjum Memon, Department of Public Health and Primary Care, Institute of Public Health, University of Cambridge, Cambridge, United Kingdom Correspondence to: Dr Iqbal Siddique, Department of Medicine, Faculty of Medicine, Kuwait University, PO Box 24923, Safat 30, Kuwait. isiddique@hsc.edu.kw Telephone: Fax: Received: Accepted: Abstract AIM: To assess the appropriateness of referrals and to determine the diagnostic yield of colonoscopy according to the 2000 guidelines of the American Society for Gastrointestinal Endoscopy (ASGE). METHODS: A total of 736 consecutive patients (45 males, 32 females; mean age 43.6±6.6 years) undergoing colonoscopy during October 200-March 2002 were prospectively enrolled in the study. The 2000 ASGE guidelines were used to assess the appropriateness of the indications for the procedure. Diagnostic yield was defined as the ratio between significant findings detected on colonoscopy and the total number of procedures performed for that indication. RESULTS: The large majority (64%) of patients had colonoscopy for an indication that was considered generally indicated, it was generally not indicated for 20%, and it was not listed for 6% in the guidelines. The diagnostic yield of colonoscopy was highest for the generally indicated (38%) followed by not listed (3%) and generally not indicated (5%) categories. In the multivariable analysis, the diagnostic yield was independently associated with the appropriateness of indication that was generally indicated (odds ratio=2.3) and referrals by gastroenterologist (odds ratio =.9). CONCLUSION: There is a high likelihood of inappropriate referrals for colonoscopy in an open-access endoscopy system. The diagnostic yield of the procedure is dependent on the appropriateness of indication and referring physician s specialty. Certain indications not listed in the guidelines have an intermediate diagnostic yield and further studies are required to evaluate whether they should be included in future revisions of the ASGE guidelines The WJG Press and Elsevier Inc. All rights reserved. Key words: Colonoscopy; Indications; Diagnostic yield; Guidelines; Appropriateness Siddique I, Mohan K, Hasan F, Memon A, Patty I, Al-Nakib B. Appropriateness of indication and diagnostic yield of colonoscopy: First report based on the 2000 guidelines of the American Society for Gastrointestinal Endoscopy. World J Gastroenterol 2005; (44): INTRODUCTION Over the last two decades, there has been a remarkable advancement in gastrointestinal endoscopy, and colonoscopy has become the most commonly performed procedure for the diagnosis and treatment of diseases of the large intestine as well as screening for colon cancer [,2]. The increasing availability of colonoscopy, however, has also led to an inappropriate referral and overuse of this procedure, which is reported to range between 5% and 35% in different studies [3-6]. Consensus-based guidelines for appropriate referral of both upper and lower gastrointestinal endoscopic procedures have been developed by several expert panels [7,8]. The American Society for Gastrointestinal Endoscopy (ASGE) has also developed and periodically reviews the guidelines on the appropriate use of these procedures with the latest update made in the year 2000 [9]. The diagnostic yield of an endoscopic procedure is defined as its capacity for identifying a lesion that is potentially important to patient care and has been reported for both upper and lower endoscopy in relation to the appropriateness of the indication [8]. For colonoscopy, it is reported to range 40-45% for procedures that are referred for appropriate indications, and 5-20% for those with inappropriate indications [3,6,8,0]. The objectives of this study were to evaluate the appropriateness of referrals for colonoscopy based on
2 7008 ISSN CN 4-29/ R World J Gastroenterol November 28, 2005 Volume Number 44 the 2000 ASGE guidelines on the appropriate use of gastrointestinal endoscopy, and to assess the diagnostic yield of the procedure according to these guidelines. MATERIALS AND METHODS For administrative purposes, Kuwait with its population of about 2.2 million is divided into six districts, each with a well-defined area and population. Medical services in each district comprise a network of primary care clinics and a general public hospital. In addition, there are a number of centralized specialty hospitals. Our study was conducted at the Thunayan Al-Ghanim Gastroenterology Center, which offers modern facilities in gastrointestinal endoscopy, and treatment and follow-up of gastroenterology and hepatology patients. The center provides open access endoscopy services for five out of six general public hospitals in Kuwait. Primary care physicians and specialists working in hospitals can directly refer patients for endoscopy. The majority of endoscopies are performed without prior consultation with a gastroenterologist. This study was carried out prospectively between October 200 and March Demographic data, in/outpatient status, specialty of the referring physician, indications for the procedure, and results of colonoscopy (including histologic reports, if any) were recorded in a standardized form specifically developed for this study. The year 2000 ASGE guidelines were used to determine the appropriateness of indication(s) for the procedure. These guidelines were printed on the form used for data collection, but the headings generally indicated and generally not indicated were omitted to avoid bias. Before starting the colonoscopy, the endoscopist obtained a brief history from the patient to confirm the indications for the procedure and to exclude any contraindications. If the indications were not listed in the ASGE guidelines, the endoscopist was asked to record it separately on the form. If the patient had more than one indication for colonoscopy and at least one of these was generally indicated by the guidelines, then the procedure was considered appropriate. Diagnostic yield in relation to each indication was defined as the ratio between significant findings detected on colonoscopy and the total number of procedures performed for that indication. Based on the criteria followed in previous studies [3,6,], the presence of any of the following lesions was considered as a significant finding on colonoscopy: a pre-malignant or malignant lesion, inflammatory bowel disease (IBD) (either newly diagnosed or a more precise diagnosis or determination of the extent of the disease that influenced immediate management of the disease), angiodysplasia, stricture (benign or malignant), other colitides (infectious, ischemic, eosinophilic, microscopic), and diverticulosis (as a definite or presumptive cause of acute hematochezia) [2]. The following were not considered as significant findings: normal colonoscopy, hemorrhoids, anal fissures, previously established IBD, uncomplicated diverticulosis, and nonadenomatous polyps. The study was carried out in accordance with the ethical standards of our institution and the Helsinki Declaration as revised in 989. We used Student s t-test to compare the difference between two means and the normal Z test to assess the significant difference between two proportions. Multiple logistic regression analysis was performed to study the clinical parameters independently associated with diagnostic yield of colonoscopy. P<0.05 was considered statistically significant. All P values presented are two sided. The data were analyzed using SPSS 3.0 for Windows software (SPSS Inc., Chicago, IL, USA). RESULTS A total of 759 patients were referred for colonoscopy during the study period. Colonoscopy could not be performed in 23 of these patients because of inadequate bowel preparation. None of the patients had any contraindications for the procedure. Table shows the demographic and clinical characteristics of the 736 patients (45 males, 32 females) who were prospectively enrolled in the study. The mean age of the patients was 43.6±6.6 years (range -90 years), and the large majority (82.3%) were outpatients. The majority of the patients were referred by general physicians (34.6%) and surgeons (33.4%). Table Demographic and clinical characteristic of 736 patients undergoing colonoscopy in Kuwait Characteristic n (%) Gender Male 45 (56.4) Female 32 (43.6) Age (yr) Mean age (SD) 43.6 (6.6) <5 3 (4.2) (59.9) (35.9) Referring clinician General physician 255 (34.6) Surgeon 246 (33.4) Gastroenterologist 205 (27.9) Pediatric gastroenterologist 22 (3.0) Other 8 (.) Clinical status Inpatient 30 (7.7) Outpatient 606 (82.3) Oncologist (6), gynecologist (2). Indications for colonoscopy Of the 736 patients, 468 (63.6%) had colonoscopy for an indication that was considered appropriate according to the ASGE guidelines (Table 2). The two most common indications were hematochezia and diarrhea of
3 Siddique I et al. Indication and diagnostic yield of colonoscopy 7009 Table 2 Indications for colonoscopy among 468 patients referred for reasons generally indicated according to the 2000 ASGE guidelines Indication n (%) Hematochezia 5 (20.5) 2 Clinically significant diarrhea of unexplained origin 65(8.8) 3 Irritable bowel syndrome or chronic abdominal pain: colonoscopy done once to rule out organic disease 48(6.5) 4 Chronic inflammatory bowel disease of the colon, if more precise diagnosis or determination of the extent of 34 (4.6) activity of disease will influence immediate management 5 Unexplained iron deficiency anemia 27 (3.7) 6 Following adequate clearance of neoplastic polyp(s) survey at 3-5 year intervals 24 (3.3) 7 Colonoscopy to remove synchronous neoplastic lesions at or around time of curative resection of cancer 23 (3.) followed by colonoscopy at 3 years and 3-5 years thereafter to detect metachronous cancer 8 Evaluation of an abnormality on barium enema or other imaging study, which is likely to be clinically significant, 9 (2.6) such as a filling defect or stricture 9 Presence of fecal occult blood 2 (.6) 0 Examination to evaluate the entire colon for synchronous cancer or neoplastic polyps in a patient (.5) with treatable cancer or neoplastic polyp Excision of colonic polyp 9 (.2) 2 Balloon dilation of stenotic lesions (e.g., anastomotic strictures) 9 (.2) 3 Melena after an upper GI source has been excluded 8 (.) 4 In patients with ulcerative or Crohn's pancolitis eight or more years' duration or left sided colitis 5 8 (.) or more years' duration every -2 years with systematic biopsies to detect dysplasia 5 Treatment of bleeding from such lesions as vascular malformation, ulceration, neoplasia, and polypectomy 7 (.0) site (e.g., electrocoagulation, heater probe, laser or injection therapy) 6 Family history of sporadic colorectal cancer before the age of 60: colonoscopy every 5 years beginning 6 (0.8) at the age of 0 years earlier than the affected relative or every three years if adenoma is found 7 Intraoperative identification of a lesion not apparent at surgery (e.g., polypectomy site, location of a bleeding site) 3 (0.4) 8 Family history of hereditary non-polyposis colorectal cancer: colonoscopy every two years beginning at the age of 25, 2 (0.3) or five years younger than the earliest age of diagnosis of colorectal cancer. Annual colonoscopy beginning at the age of 40 9 Palliative treatment of stenosing or bleeding neoplasms (e.g., laser, electrocoagulation, stenting) 2 (0.3) unexplained etiology. Whereas, 49 (20.2%) patients underwent colonoscopy for an indication, which was generally not indicated (Table 3), and for 9 (6.2%) patients the indication for colonoscopy was not listed in the guidelines (Table 4). The most common indications for patients in these two categories were chronic, stable, irritable bowel syndrome or chronic abdominal pain, and constipation, respectively. Table 5 shows the appropriateness of indications for colonoscopy in relation to patients gender, age, admission status, and specialty of the referring physician. There was no material difference in the appropriateness of indications between males and females or in- and outpatients. The mean age of patients who had colonoscopy for an indication that was generally not indicated was significantly lower than those who had the procedure for an indication that was generally indicated or not listed in the guidelines (38.2 vs 44.7 years, P<0.000). Patients aged <5 years and those >50 years had a higher proportion of procedures for an indication that was considered generally indicated by the guidelines (77.4% and 74.6%, respectively). On the other hand, 29.5% of the patients aged 5-49 years had a significantly higher proportion of colonoscopies for an indication that was considered generally not indicated (P<0.000). There was no real difference in the age groups when the procedure was performed for an indication that was not listed in the guidelines. Pediatric gastroenterologists referred the highest proportion of patients (8.8%) for colonoscopy for an indication that was considered generally indicated, followed by adult gastroenterologists (66.8%), surgeons (62.2%) and general physicians (60.4%). Among other specialists, general physicians referred the highest proportion of patients for colonoscopy for a reason that was considered generally not indicated, while surgeons referred the highest proportion of patients for a not listed indication. Diagnostic yield of colonoscopy A total of 200 patients had one or more significant findings on colonoscopy giving an overall diagnostic yield of 27.2%. The most common significant findings were adenomatous polyps (29.5%), new diagnosis or more precise determination of the extent of IBD (23.5%) and colorectal cancer (2.0%). The yield of the procedures performed for generally indicated category was 37.8%, which was significantly higher than generally not indicated (4.7%, P<0.000) and not listed (3.4%, P<0.000) categories in the ASGE guidelines (Table 5). The yield of the procedures performed for not listed indications was also significantly higher than that for generally not indicated procedures (3.4% vs 4.7%, P<0.05). Inpatients had a higher diagnostic yield of
4 700 ISSN CN 4-29/ R World J Gastroenterol November 28, 2005 Volume Number 44 Table 3 Indications for colonoscopy among 49 patients referred for reasons generally not indicated according to the 2000 ASGE guidelines Indication n (%) Chronic, stable, irritable bowel syndrome or chronic abdominal pain 7 (5.9) 2 Routine follow-up of inflammatory bowel disease 5 (2.0) 3 Acute diarrhea 7 (.0) 4 Metastatic adenocarcinoma of unknown primary site in the absence of colonic signs or symptoms when it will not influence management 6 (0.8) 5 Upper GI bleeding or melena with a demonstrated upper gastrointestinal source 4 (0.5) Table 4 Indications for colonoscopy among 9 patients referred for reasons not listed in the 2000 ASGE guidelines Indication n (%) Constipation 7 (9.6) 2 Unexplained weight loss 4 (.9) 3 Normochromic anemia 7 (.0) 4 Perianal abscess or fistula 6 (0.8) 5 Abdominal mass of unknown origin 4 (0.5) 6 Periodic follow up of healed benign lesions 4 (0.5) 7 Surveillance after resection of colonic polyps or cancer, at different intervals from those recommended 3(0.4) 8 Intestinal obstruction 2 (0.3) 9 Routine examination of the colon in patients with no colon-related signs or symptoms about to have elective abdominal surgery for non-colonic disease 2 (0.3) 0 Others 6 (0.8) Table 5 Appropriateness of indication and diagnostic yield of colonoscopy according to patients characteristics Characteristic (no. of patients) Appropriateness of referral n (%) Diagnostic yield (%) Generally indicated Generally not indicated Not listed All patients (736) 468 (63.6) 49 (20.2) 9 (6.2) 27.2 Diagnostic yield 37.8% 4.7% 3.4% - Gender Male (45) 263(63.4) 87 (2.0) 65 (5.7) 28.0 Female (32) 205 (63.9) 62 (9.3) 54 (6.8) 26.2 Age (yr) Mean age (SD) 44.7 (7.3) 38.2 (2.) 46.3 (7.3) <5 (3) 24 (77.4) 2 (6.5) 5 (6.) (44) 247 (56.0) 30 (29.5) 64 (4.5) (264) 97 (74.6) 7 (6.4) 50 (8.9) 33.0 Referring clinician General physician (255) 54 (60.4) 63 (24.7) 38 (4.9) 8.0 Surgeon (246) 53 (62.2) 34 (3.8) 59 (24.0) 27.6 Gastroenterologist (205) 37 (66.8) 49 (23.9) 9 (9.3) 36.6 Pediatric gastroenterologist (22) 8 (8.8) (4.5) 3 (3.6) 50.0 Other 2 (8) 6 (75.0) 2 (25.0) 0 0 Clinical status Inpatient (30) 89 (68.5) 9 (4.6) 22 (6.9) 35.4 Outpatient (606) 379 (62.5) 30 (2.5) 97 (6.0) Oncologist (6), gynecologist (2).
5 Siddique I et al. Indication and diagnostic yield of colonoscopy 70 Table 6 Clinical findings on colonoscopy by appropriateness of referral Appropriateness of referral n (%) Generally indicated Generally not indicated Not listed Cancer 2 (4.5) 0 a 3 (2.5) Adenoma 54 (.5) (0.7) c 4 (3.4) a IBD 2 62 (3.2) 6 (4.0) c 8 (6.7) Other colitides 3 36 (.3) 0 (0.8) Angiodysplasia 5 (.) IBD, inflammatory bowel disease. 3 Non-specific colitis (3), infectious colitis (3), eosinophilic colitis (). a P<0.05 compared to Generally indicated. c P<0.005 compared to Generally indicated. Table 7 Odds ratios (OR) and 95% confidence intervals (95% CI) for association between selected clinical parameters and diagnostic yield of colonoscopy Parameter (n) Diagnostic yield (%) OR (95% CI 2 ) P Gender Female (32) Male (45) (0.8-.5) >0.50 Age (years) <50 (472) (264) (.-2.2) <0.05 Clinical status Outpatient (606) Inpatient (30) (.-2.4) <0.05 Referring clinician Other (53) Gastroenterologist (205) (.3-2.7) <0.00 Appropriateness of indication 3 Generally not indicated (49) Not listed (9) (.3-7.9) <0.05 Generally indicated (468) ( ) <0.00 OR, odds ratio. 2 CI, confidence interval. 3 colonoscopy compared to outpatients (35.4% vs 25.4%, P<0.05). The highest diagnostic yield was obtained in those aged <5 years, and in those who were referred by a gastroenterologist. Table 6 lists some of the significant findings on colonoscopy by appropriateness of referrals. Colorectal cancer, adenomatous polyps, and IBD were more likely to be detected, if the colonoscopy was performed for a generally indicated reason. The colon was reported as completely normal in 82.6% of the patients in the generally not indicated and 73.9% in not listed groups, compared to 5.7% in the generally indicated group. Determinants of diagnostic yield Table 7 shows the association between selected clinical parameters and diagnostic yield of colonoscopy. The probability of finding a clinically significant lesion was significantly higher in patients aged 50 years (odds ratio =.6), inpatients (odds ratio =.6), those referred by gastroenterologists (odds ratio =.9), and those who had the colonoscopy for generally indicated (odds ratio = 2.3) or not listed (odds ratio = 3.2) categories. After adjustment for the other variables, appropriateness of indications for colonoscopy according to the ASGE guidelines and referrals by gastroenterologist were the two independent parameters associated with the diagnostic yield. DISCUSSION To our knowledge, this is the first study to assess the appropriateness of referrals for colonoscopy and to determine the diagnostic yield according to the year 2000 ASGE guidelines. About 64% of our patients had an indication for colonoscopy that was appropriate or
6 702 ISSN CN 4-29/ R World J Gastroenterol November 28, 2005 Volume Number 44 generally indicated, according to the ASGE guidelines. This finding is similar to the 6-66% rate reported from open-access colonoscopy settings in the United States, Italy and Switzerland [3,5,6,8]. A higher rate (8%) has been reported in a study from the United States, where the referring physicians were instructed on the accepted indications for gastrointestinal endoscopy [4]. All these studies were based on the 992 version of the ASGE guidelines. The year 2000 guidelines include several new conditions for which colonoscopy is now considered generally indicated such as all patients presenting with hematochezia, while the older guidelines only considered colonoscopy to be appropriate, if the hematochezia was not thought to be from the rectum or a perianal source. In addition, screening of asymptomatic, average risk patients for colonic neoplasia and seven new therapeutic indications have been included in the new guidelines. Inclusion of these additional indications means that a higher proportion of the patients referred for open-access colonoscopy should have an appropriate indication for the procedure. In our study, the overall rate of generally indicated colonoscopies was comparable to the studies based on the 992 guidelines. It is noteworthy that our patients were relatively younger than those in other studies. Compared to an average age of years in other studies, the average age of our patients was about 44 years and 60% were aged between 5 and 49 years. This may be the reason why we did not have a higher proportion of patients referred for appropriate indications even though we used more liberal ASGE guidelines. We did, however, observe a higher rate of generally indicated colonoscopy for patients aged <5 years (77%), which is not unexpected as colonoscopy is usually not performed in children unless an appropriate indication is present, and for those aged >50 years (75%). We found no real difference between various specialties when patients were referred for a generally indicated colonoscopy. As for generally not indicated procedure, the rate was lowest for surgeons, while that for gastroenterologists was similar to general physicians. This finding is consistent with a study of open-access colonoscopy from Italy which reported similar rates of generally not indicated colonoscopy between gastroenterologists and family physicians [5], but is in contrast with studies of open access upper gastrointestinal endoscopy [3]. The majority (80%) of generally not indicated colonoscopies requested by gastroenterologists in our study were for chronic stable abdominal pain or irritable bowel syndrome (IBS), while the other 20% were for routine follow-up of IBD. This high referral rate of colonoscopy for chronic stable abdominal pain or IBS by gastroenterologists may be because in Kuwait many such patients after failing to respond to therapy are referred to the gastroenterology clinics by primary care physicians. When these patients were excluded from the analysis, the rate of generally indicated colonoscopy for gastroenterologists increased to about 83%, which was higher than that for all other specialties. In our study, the definition of significant findings was based on certain positive results on colonoscopy. A normal colonoscopy was not considered significant, although this may be relevant to patient care as it may rule out a serious disease in the colon. Our results show that the diagnostic yield of colonoscopy was independently associated with appropriateness of indications and referrals by gastroenterologists. Our findings are consistent with studies conducted in Europe and the United States [3,6,], but the difference between the yield of generally indicated and generally not indicated procedures (37.8% vs 4.7%) is much higher than reported in these studies. Charles et al. [3] reported that 40% of patients who have colonoscopy for an ASGE (992 version) approved indication have a significant pathological finding compared to 22% of those who do not meet the guidelines. Similarly, Morini et al. [6] have reported a diagnostic yield of 43% for generally indicated and 6% for generally not indicated categories. De Bosset et al. [], using the Swiss criteria developed by the Rand Corporation/University of California at Los Angeles (RAND/UCLA) panel, have reported a diagnostic yield of 26% for patients who have colonoscopy for an appropriate or uncertain indication and 7% for those with an inappropriate indication. The higher difference in the diagnostic yield of colonoscopy for a generally indicated and generally not indicated category seen in our study suggests that the 2000 ASGE guidelines for appropriate use of gastrointestinal endoscopy are more efficient in discriminating indications for colonoscopy than the earlier versions or the Swiss (RAND/UCLA) criteria. The year 2000 ASGE guidelines clearly differentiate between the generally indicated and generally not indicated colonoscopies in terms of the diagnostic yield of the procedure. Clinicians can therefore predict the expected yield of colonoscopy as long as the indications for the procedure can clearly be classified as generally indicated or generally not indicated. However, in clinical practice there are always some patients who undergo colonoscopy for indications that cannot be clearly classified into either of these two categories. It has been reported that about 2-28% of the patients undergoing colonoscopy have indications that are not listed in the ASGE guidelines [5,6,8]. In our study, the proportion of patients in not listed category was about 6% with a diagnostic yield of 3.4%, being about three times higher than the diagnostic yield of colonoscopy which is generally not indicated. Among the patients in the not listed category, three were diagnosed with colorectal cancer compared to none in the generally not indicated group and the proportion of patients diagnosed with adenomatous polyps and IBD was also higher. The ASGE guidelines appear to be deficient with regard to these not listed indications, but it is acknowledged that clinical considerations may occasionally justify a course of action at variance with the recommendations of the ASGE. The two most frequent unlisted indications in our study were constipation and unexplained weight loss, and all three cases of colorectal cancer were found in patients who underwent colonoscopy for constipation. Clear recommendations are needed for such common unlisted
7 Siddique I et al. Indication and diagnostic yield of colonoscopy 703 indications such as constipation as provided in the Swiss and American panel-based guidelines [8]. Further studies are needed to identify other common but unlisted indications that may be included in future versions of the ASGE guidelines. In summary, the results of this prospective study demonstrate that a large proportion of colonoscopies performed in an open-access system in Kuwait is for the indications considered inappropriate by, or not listed in the 2000 guidelines of the ASGE on appropriate use of gastrointestinal endoscopy. The probability of identifying a significant finding on colonoscopy is particularly higher when the indications for the procedure are judged to be appropriate by the ASGE guidelines, but a proportion of patients who undergo colonoscopy for an unlisted indication also have significant findings. Further studies are required to evaluate these unlisted indications to determine whether they should be included in future revisions of the guidelines. General physicians need further edification for appropriate referrals of patients for colonoscopy. REFERENCES Karasick S, Ehrlich SM, Levin DC, Harford RJ, Rosetti EF, Ricci JA, Beam LM, Gigliotti JV. Trends in use of barium enema examination, colonoscopy, and sigmoidoscopy: is use commensurate with risk of disease? Radiology 995; 95: Scott B. Endoscopic demands in the 90 s. Gut 990; 3: Charles RJ, Chak A, Cooper GS, Wong RC, Sivak MV Jr. Use of open access in GI endoscopy at an academic medical center. Gastrointest Endosc 999; 50: Mahajan RJ, Barthel JS, Marshall JB. Appropriateness of referrals for open-access endoscopy. How do physicians in different medical specialties do? Arch Intern Med 996; 56: Minoli G, Meucci G, Bortoli A, Garripoli A, Gullotta R, Leo P, Pera A, Prada A, Rocca F, Zambelli A. The ASGE guidelines for the appropriate use of colonoscopy in an open access system. Gastrointest Endosc 2000; 52: Morini S, Hassan C, Meucci G, Toldi A, Zullo A, Minoli G. Diagnostic yield of open access colonoscopy according to appropriateness. Gastrointest Endosc 200; 54: Burnand B, Vader JP, Froehlich F, Dupriez K, Larequi-Lauber T, Pache I, Dubois RW, Brook RH, Gonvers JJ. Reliability of panel-based guidelines for colonoscopy: an international comparison. Gastrointest Endosc 998; 47: Froehlich F, Pache I, Burnand B, Vader JP, Fried M, Beglinger C, Stalder G, Gyr K, Thorens J, Schneider C, Kosecoff J, Kolodny M, DuBois RW, Gonvers JJ, Brook RH. Performance of panel-based criteria to evaluate the appropriateness of colonoscopy: a prospective study. Gastrointest Endosc 998; 48: Appropriate use of gastrointestinal endoscopy. American Society for Gastrointestinal Endoscopy. Gastrointest Endosc 2000; 52: Berkowitz I, Kaplan M. Indications for colonoscopy. An analysis based on indications and diagnostic yield. S Afr Med J 993; 83: De Bosset V, Froehlich F, Rey JP, Thorens J, Schneider C, Wietlisbach V, Vader JP, Burnand B, Muhlhaupt B, Fried M, Gonvers JJ. Do explicit appropriateness criteria enhance the diagnostic yield of colonoscopy? Endoscopy 2002; 34: Jensen DM, Machicado GA, Jutabha R, Kovacs TO. Urgent colonoscopy for the diagnosis and treatment of severe diverticular hemorrhage. N Engl J Med 2000; 342: Minoli G, Prada A, Gambetta G, Formenti A, Schalling R, Lai L, Pera A. The ASGE guidelines for the appropriate use of upper gastrointestinal endoscopy in an open access system. Gastrointest Endosc 995; 42: Science Editor Wang XL and Guo SY Language Editor Elsevier HK
REFERRAL GUIDELINES: ENDOSCOPY
 Outpatient Referral Guidelines Page 1 REFERRAL GUIDELINES: Referrals for endoscopy must be made using the Essential Referral Content Gastrointestinal Endoscopy Referral Form Please fax the completed referral
Outpatient Referral Guidelines Page 1 REFERRAL GUIDELINES: Referrals for endoscopy must be made using the Essential Referral Content Gastrointestinal Endoscopy Referral Form Please fax the completed referral
Colonoscopy at the National Center for Early Detection of Cancer: Evaluating Indications and Diagnostic Yield
 COLONOSCOPY THE IRAQI POSTGRADUATE FOR EARLY MEDICAL DETECTION JOURNAL OF CANCER Colonoscopy at the National Center for Early Detection of Cancer: Evaluating Indications and Diagnostic Yield Maral F.Thabit*,
COLONOSCOPY THE IRAQI POSTGRADUATE FOR EARLY MEDICAL DETECTION JOURNAL OF CANCER Colonoscopy at the National Center for Early Detection of Cancer: Evaluating Indications and Diagnostic Yield Maral F.Thabit*,
General and Colonoscopy Data Collection Form
 Identifier: Sociodemographic Information Type: Zip Code: Inpatient Outpatient Birth Date: m m d d y y y y Gender: Height: (inches) Male Female Ethnicity: Weight: (pounds) African American White, Non-Hispanic
Identifier: Sociodemographic Information Type: Zip Code: Inpatient Outpatient Birth Date: m m d d y y y y Gender: Height: (inches) Male Female Ethnicity: Weight: (pounds) African American White, Non-Hispanic
Historical. Note: The parenthetical numbers in the Clinical Indications section refer to the source documents cited in the References Section below.
 Clinical UM Guideline Subject: Colonoscopy Guideline #: CG-SURG-01 Current Effective Date: 01/21/2015 Status: Revised Last Review Date: 05/15/2014 Description Colonoscopy describes the direct visual inspection
Clinical UM Guideline Subject: Colonoscopy Guideline #: CG-SURG-01 Current Effective Date: 01/21/2015 Status: Revised Last Review Date: 05/15/2014 Description Colonoscopy describes the direct visual inspection
Colonoscopy MM /01/2010. PPO; HMO; QUEST Integration 10/01/2017 Section: Surgery Place(s) of Service: Outpatient
 Colonoscopy Policy Number: Original Effective Date: MM.12.003 12/01/2010 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST Integration 10/01/2017 Section: Surgery Place(s) of Service: Outpatient
Colonoscopy Policy Number: Original Effective Date: MM.12.003 12/01/2010 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST Integration 10/01/2017 Section: Surgery Place(s) of Service: Outpatient
Quality Measures In Colonoscopy: Why Should I Care?
 Quality Measures In Colonoscopy: Why Should I Care? David Greenwald, MD, FASGE Professor of Clinical Medicine Albert Einstein College of Medicine Montefiore Medical Center Bronx, New York ACG/ASGE Best
Quality Measures In Colonoscopy: Why Should I Care? David Greenwald, MD, FASGE Professor of Clinical Medicine Albert Einstein College of Medicine Montefiore Medical Center Bronx, New York ACG/ASGE Best
Clinical UM Guideline
 Subject: Guideline #: Current Effective Date: 06/28/2016 Status: Revised Last Review Date: 05/05/2016 Description This document addresses colonoscopy, an endoscopic procedure which allows direct visual
Subject: Guideline #: Current Effective Date: 06/28/2016 Status: Revised Last Review Date: 05/05/2016 Description This document addresses colonoscopy, an endoscopic procedure which allows direct visual
Screening & Surveillance Guidelines
 Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Merit-based Incentive Payment system (MIPS) 2018 Qualified Clinical Data Registry (QCDR) Measure Specifications
 Merit-based Incentive Payment system (MIPS) 2018 Qualified Clinical Data Registry (QCDR) Measure Specifications This document contains a listing of the clinical quality measures which the New Hampshire
Merit-based Incentive Payment system (MIPS) 2018 Qualified Clinical Data Registry (QCDR) Measure Specifications This document contains a listing of the clinical quality measures which the New Hampshire
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn
Title Description Type / Priority
 Merit-based Incentive Payment system (MIPS) 2019 Qualified Clinical Data Registry (QCDR) Measure Specifications Summary Listing of QCDR measures supported by the NHCR Measure # NHCR4 NHCR5 GIQIC12 GIQIC15
Merit-based Incentive Payment system (MIPS) 2019 Qualified Clinical Data Registry (QCDR) Measure Specifications Summary Listing of QCDR measures supported by the NHCR Measure # NHCR4 NHCR5 GIQIC12 GIQIC15
GIQIC18 Appropriate follow-up interval of not less than 5 years for colonoscopies with findings of 1-2 tubular adenomas < 10 mm
 GI Quality Improvement Consortium, Ltd. (GIQuIC) 1 Following is an overview of the clinical quality measures in GIQuIC that can be reported to CMS for the Quality performance category of the Merit-Based
GI Quality Improvement Consortium, Ltd. (GIQuIC) 1 Following is an overview of the clinical quality measures in GIQuIC that can be reported to CMS for the Quality performance category of the Merit-Based
Frequency of Diagnosis of Colorectal Cancer with Double Contrast Barium Enema
 Bahrain Medical Bulletin, Vol.24, No.3, September 2002 Frequency of Diagnosis of Colorectal Cancer with Double Contrast Barium Enema Najeeb S Jamsheer, MD, FRCR* Neelam. Malik, MD, MNAMS** Objective: To
Bahrain Medical Bulletin, Vol.24, No.3, September 2002 Frequency of Diagnosis of Colorectal Cancer with Double Contrast Barium Enema Najeeb S Jamsheer, MD, FRCR* Neelam. Malik, MD, MNAMS** Objective: To
EGD Data Collection Form
 Sociodemographic Information Type Zip Code Gender Height (in inches) Race Ethnicity Inpatient Outpatient Male Female Birth Date Weight (in pounds) American Indian (Native American) or Alaska Native Asian
Sociodemographic Information Type Zip Code Gender Height (in inches) Race Ethnicity Inpatient Outpatient Male Female Birth Date Weight (in pounds) American Indian (Native American) or Alaska Native Asian
Appropriateness of the Indication for Colonoscopy: Systematic Review and Meta-analysis
 reviews Appropriateness of the Indication for Colonoscopy: Systematic Review and Meta-analysis Cesare Hassan 1, Emilio Di Giulio 2, Riccardo Marmo 2, Angelo Zullo 1, Bruno Annibale 3 1) Gastroenterology
reviews Appropriateness of the Indication for Colonoscopy: Systematic Review and Meta-analysis Cesare Hassan 1, Emilio Di Giulio 2, Riccardo Marmo 2, Angelo Zullo 1, Bruno Annibale 3 1) Gastroenterology
Epidemiology and Treatment of Colonic Angiodysplasia; a Population-Based Study. Naomi G. Diggs, MD Lisa L. Strate, MD MPH March 2, 2010
 Epidemiology and Treatment of Colonic Angiodysplasia; a Population-Based Study. Naomi G. Diggs, MD Lisa L. Strate, MD MPH March 2, 2010 Background Angiodysplasia is an important cause of occult and acute
Epidemiology and Treatment of Colonic Angiodysplasia; a Population-Based Study. Naomi G. Diggs, MD Lisa L. Strate, MD MPH March 2, 2010 Background Angiodysplasia is an important cause of occult and acute
Quality ID #439: Age Appropriate Screening Colonoscopy National Quality Strategy Domain: Efficiency and Cost Reduction
 Quality ID #439: Age Appropriate Screening Colonoscopy National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Efficiency DESCRIPTION:
Quality ID #439: Age Appropriate Screening Colonoscopy National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Efficiency DESCRIPTION:
APPROPRIATENESS OF COLONOSCOPY appropriateness of colonoscopy by indication based on accepted published guidelines, the overall yield of colonoscopy,
 9402R#3 25/11/03+pdf Original Article Appropriateness of Colonoscopy in a Tertiary Referral Centre Mohd Faisal Jabar, Muhd Ezman Abdul Halim and Yunus A. Gul, Department of Surgery, University Putra Malaysia,
9402R#3 25/11/03+pdf Original Article Appropriateness of Colonoscopy in a Tertiary Referral Centre Mohd Faisal Jabar, Muhd Ezman Abdul Halim and Yunus A. Gul, Department of Surgery, University Putra Malaysia,
DIGESTIVE SYSTEM SURGICAL PROCEDURES May 1, 2015 INTESTINES (EXCEPT RECTUM) Asst Surg Anae
 ENDOSCOPY Z50 Duodenoscopy (not to be claimed if Z399 and/or Z00 performed on same patient within 3 months)... 92.10 Z9 Subsequent procedure (within three months following previous endoscopic procedure)...
ENDOSCOPY Z50 Duodenoscopy (not to be claimed if Z399 and/or Z00 performed on same patient within 3 months)... 92.10 Z9 Subsequent procedure (within three months following previous endoscopic procedure)...
removal of adenomatous polyps detects important effectively as follow-up colonoscopy after both constitute a low-risk Patients with 1 or 2
 Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography
 Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography 2019 Released 2019 health.govt.nz Citation: Ministry of Health. 2019. Referral Criteria for Direct Access
Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography 2019 Released 2019 health.govt.nz Citation: Ministry of Health. 2019. Referral Criteria for Direct Access
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines
 Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Objectives. Definitions. Colorectal Cancer Screening 5/8/2018. Payam Afshar, MS, MD Kaiser Permanente, San Diego. Colorectal cancer background
 Colorectal Cancer Screening Payam Afshar, MS, MD Kaiser Permanente, San Diego Objectives Colorectal cancer background Colorectal cancer screening populations Colorectal cancer screening modalities Colonoscopy
Colorectal Cancer Screening Payam Afshar, MS, MD Kaiser Permanente, San Diego Objectives Colorectal cancer background Colorectal cancer screening populations Colorectal cancer screening modalities Colonoscopy
Structured Follow-Up after Colorectal Cancer Resection: Overrated. R. Taylor Ripley University of Colorado Grand Rounds April 23, 2007
 Structured Follow-Up after Colorectal Cancer Resection: Overrated R. Taylor Ripley University of Colorado Grand Rounds April 23, 2007 Guidelines for Colonoscopy Production: Surveillance US Multi-Society
Structured Follow-Up after Colorectal Cancer Resection: Overrated R. Taylor Ripley University of Colorado Grand Rounds April 23, 2007 Guidelines for Colonoscopy Production: Surveillance US Multi-Society
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci. Colon polyps. Colorectal cancer
 Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Colon polyps Colorectal cancer Harrison s Principles of Internal Medicine 18 Ed. 2012 Colorectal cancer 70% Colorectal cancer CRC and colon
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Colon polyps Colorectal cancer Harrison s Principles of Internal Medicine 18 Ed. 2012 Colorectal cancer 70% Colorectal cancer CRC and colon
Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care
 Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
Latest Endoscopic Guidelines for FAP, HNPCC, IBD, and the General Population
 Latest Endoscopic Guidelines for FAP, HNPCC, IBD, and the General Population David T. Rubin, M.D. Assistant Professor of Medicine Inflammatory Bowel Disease Center MacLean Center for Clinical Medical Ethics
Latest Endoscopic Guidelines for FAP, HNPCC, IBD, and the General Population David T. Rubin, M.D. Assistant Professor of Medicine Inflammatory Bowel Disease Center MacLean Center for Clinical Medical Ethics
Billing Guideline. Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/14 Last revision effective 4/16
 Billing Guideline Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/14 Last revision effective 4/16 Florida Hospital Care Advantage plans include full coverage of in-network
Billing Guideline Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/14 Last revision effective 4/16 Florida Hospital Care Advantage plans include full coverage of in-network
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Oakland K, Jairath V, Uberoi R, et al. Derivation
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Oakland K, Jairath V, Uberoi R, et al. Derivation
Screening for Colorectal Cancer in the Elderly. The Broad Perspective
 Screening for Colorectal Cancer in the Elderly Charles J. Kahi, MD, MSCR Indiana University School of Medicine Richard L. Roudebush VA Medical Center Indianapolis, Indiana ACG Regional Midwest Course Symposium
Screening for Colorectal Cancer in the Elderly Charles J. Kahi, MD, MSCR Indiana University School of Medicine Richard L. Roudebush VA Medical Center Indianapolis, Indiana ACG Regional Midwest Course Symposium
GI Quality Improvement Consortium, Ltd. (GIQuIC) QCDR Non-PQRS Measure Specifications
 GI Quality Improvement Consortium, Ltd. (GIQuIC) 1 Following is an overview of the clinical quality measures in GIQuIC that can be reported to CMS for the Physician Quality Report System (PQRS) via GIQuIC
GI Quality Improvement Consortium, Ltd. (GIQuIC) 1 Following is an overview of the clinical quality measures in GIQuIC that can be reported to CMS for the Physician Quality Report System (PQRS) via GIQuIC
GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY
 Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Guidelines for Colonoscopy Surveillance After Screening and Polypectomy: A Consensus Update by the US Multi-Society Task Force on Colorectal Cancer
 Guidelines for Colonoscopy Surveillance After Screening and Polypectomy: A Consensus Update by the US Multi-Society Task Force on Colorectal Cancer David A. Lieberman, 1 Douglas K. Rex, 2 Sidney J. Winawer,
Guidelines for Colonoscopy Surveillance After Screening and Polypectomy: A Consensus Update by the US Multi-Society Task Force on Colorectal Cancer David A. Lieberman, 1 Douglas K. Rex, 2 Sidney J. Winawer,
Page 1. Is the Risk This High? Dysplasia in the IBD Patient. Dysplasia in the Non IBD Patient. Increased Risk of CRC in Ulcerative Colitis
 Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
When to Scope in Lower GI Bleeding: It Must Be Done Now. Lisa L. Strate, MD, MPH Assistant Professor of Medicine University of Washington, Seattle, WA
 When to Scope in Lower GI Bleeding: It Must Be Done Now Lisa L. Strate, MD, MPH Assistant Professor of Medicine University of Washington, Seattle, WA Outline Epidemiology Overview of available tests Urgent
When to Scope in Lower GI Bleeding: It Must Be Done Now Lisa L. Strate, MD, MPH Assistant Professor of Medicine University of Washington, Seattle, WA Outline Epidemiology Overview of available tests Urgent
CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING
 CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING This guideline is designed to assist practitioners by providing the framework for colorectal cancer (CRC) screening, and is not intended to replace
CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING This guideline is designed to assist practitioners by providing the framework for colorectal cancer (CRC) screening, and is not intended to replace
The 2012 SAGE Wait Time Program: Survey of Access to GastroEnterology in Canada Can J Gastroenterol 2013;27:83-9.
 The 2012 SAGE Wait Time Program: Survey of Access to GastroEnterology in Canada Can J Gastroenterol 2013;27:83-9. Desmond Leddin MB, David Armstrong MD, Mark Borgaonkar MD, Ronald J Bridges MD, Carlo A
The 2012 SAGE Wait Time Program: Survey of Access to GastroEnterology in Canada Can J Gastroenterol 2013;27:83-9. Desmond Leddin MB, David Armstrong MD, Mark Borgaonkar MD, Ronald J Bridges MD, Carlo A
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Virtual Colonoscopy / CT Colonography Page 1 of 19 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Virtual Colonoscopy / CT Colonography Professional Institutional
Virtual Colonoscopy / CT Colonography Page 1 of 19 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Virtual Colonoscopy / CT Colonography Professional Institutional
Wireless Capsule Endoscopy to Diagnose Disorders of the Small Bowel, Esophagus, and Colon
 Wireless Capsule Endoscopy to Diagnose Disorders of the Small Bowel, Esophagus, and Colon Policy Number: 6.01.33 Last Review: 4/2018 Origination: 4/2003 Next Review: 4/2019 Policy Blue Cross and Blue Shield
Wireless Capsule Endoscopy to Diagnose Disorders of the Small Bowel, Esophagus, and Colon Policy Number: 6.01.33 Last Review: 4/2018 Origination: 4/2003 Next Review: 4/2019 Policy Blue Cross and Blue Shield
LIST OF ABBREVIATIONS
 Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
2015 Gastroenterology Survival Guide
 2015 Gastroenterology Survival Guide Chapter 11: ICD-9 Coding Your first line of ICD-9 coding is to attach signs or symptoms to your claim, but even after your gastroenterologist performs a diagnostic
2015 Gastroenterology Survival Guide Chapter 11: ICD-9 Coding Your first line of ICD-9 coding is to attach signs or symptoms to your claim, but even after your gastroenterologist performs a diagnostic
Colon Cancer Detection by Rendezvous Colonoscopy : Successful Removal of Stuck Colon Capsule by Conventional Colonoscopy
 19 Colon Cancer Detection by Rendezvous Colonoscopy : Successful Removal of Stuck Colon Capsule by Conventional Colonoscopy István Rácz Márta Jánoki Hussam Saleh Department of Gastroenterology, Petz Aladár
19 Colon Cancer Detection by Rendezvous Colonoscopy : Successful Removal of Stuck Colon Capsule by Conventional Colonoscopy István Rácz Márta Jánoki Hussam Saleh Department of Gastroenterology, Petz Aladár
Quality Assurance and Colonoscopy
 522 Original Article Quality Assurance and Colonoscopy G. Minoli 1, G. Meucci 1, A. Prada 2, V Terruzzi 1, A. Bortoli 2, R. Gullotta 3, F. Rocca 4, E. Lesinigo 4, M. Curzio 3 'Division of Medicine, Valduce
522 Original Article Quality Assurance and Colonoscopy G. Minoli 1, G. Meucci 1, A. Prada 2, V Terruzzi 1, A. Bortoli 2, R. Gullotta 3, F. Rocca 4, E. Lesinigo 4, M. Curzio 3 'Division of Medicine, Valduce
Colorectal Cancer Screening: Cost-Effectiveness and Adverse events October, 2005
 Colorectal Cancer Screening: Cost-Effectiveness and Adverse events October, 2005 David Lieberman MD Chief, Division of Gastroenterology Oregon Health and Science University Portland VAMC Portland, Oregon
Colorectal Cancer Screening: Cost-Effectiveness and Adverse events October, 2005 David Lieberman MD Chief, Division of Gastroenterology Oregon Health and Science University Portland VAMC Portland, Oregon
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: capsule_endoscopy_wireless 5/2002 5/2016 5/2017 11/2016 Description of Procedure or Service Wireless capsule
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: capsule_endoscopy_wireless 5/2002 5/2016 5/2017 11/2016 Description of Procedure or Service Wireless capsule
Increasing the number of older persons in the United
 Current Capacity for Endoscopic Colorectal Cancer Screening in the United States: Data from the National Cancer Institute Survey of Colorectal Cancer Screening Practices Martin L. Brown, PhD, Carrie N.
Current Capacity for Endoscopic Colorectal Cancer Screening in the United States: Data from the National Cancer Institute Survey of Colorectal Cancer Screening Practices Martin L. Brown, PhD, Carrie N.
Role of radiology in colo-rectal bleedings. Alban DENYS MD FCIRSE EBIR CHUV LAUSANNE
 Role of radiology in colo-rectal bleedings Alban DENYS MD FCIRSE EBIR CHUV LAUSANNE Epidemiology Lower GI bleeding accounts for 20-25% of all GI bleeding Annual incidence in USA :21-27/100000 Longstreth
Role of radiology in colo-rectal bleedings Alban DENYS MD FCIRSE EBIR CHUV LAUSANNE Epidemiology Lower GI bleeding accounts for 20-25% of all GI bleeding Annual incidence in USA :21-27/100000 Longstreth
Colorectal Cancer Screening And Related Ancillary Services
 Manual: Policy Title: Reimbursement Policy Colorectal Cancer Screening And Related Ancillary Services Section: Preventive Services Subsection: None Date of Origin: 11/20/2015 Policy Number: RPM046 Last
Manual: Policy Title: Reimbursement Policy Colorectal Cancer Screening And Related Ancillary Services Section: Preventive Services Subsection: None Date of Origin: 11/20/2015 Policy Number: RPM046 Last
Colonoscopy Quality Data
 Colonoscopy Quality Data www.dhsgi.com Introduction Colorectal cancer is the second leading cause of cancer related deaths in the United States, in men and women combined. In 2016, there are expected to
Colonoscopy Quality Data www.dhsgi.com Introduction Colorectal cancer is the second leading cause of cancer related deaths in the United States, in men and women combined. In 2016, there are expected to
Spectrum of Diverticular Disease. Outline
 Spectrum of Disease ACG Postgraduate Course January 24, 2015 Lisa Strate, MD, MPH Associate Professor of Medicine University of Washington, Seattle, WA Outline Traditional theories and updated perspectives
Spectrum of Disease ACG Postgraduate Course January 24, 2015 Lisa Strate, MD, MPH Associate Professor of Medicine University of Washington, Seattle, WA Outline Traditional theories and updated perspectives
Management Of Rectal Bleeding In The Community: How A Shared Care Approach Can Benefit Dr. Daniel Lee
 Management Of Rectal Bleeding In The Community: How A Shared Care Approach Can Benefit Dr. Daniel Lee MD, MMed (S'pore), FRCS (Edin) Associate Consultant Department of Surgery 9 January 2016 Incidence
Management Of Rectal Bleeding In The Community: How A Shared Care Approach Can Benefit Dr. Daniel Lee MD, MMed (S'pore), FRCS (Edin) Associate Consultant Department of Surgery 9 January 2016 Incidence
LET S TALK ABOUT CANCER
 LET S TALK ABOUT CANCER COLORECTAL CANCER AND CROHN S DISEASE & ULCERATIVE COLITIS crohnsandcolitis.ca BACKGROUND Colorectal cancer is the second-leading cause of cancer death in this country. In 2013,
LET S TALK ABOUT CANCER COLORECTAL CANCER AND CROHN S DISEASE & ULCERATIVE COLITIS crohnsandcolitis.ca BACKGROUND Colorectal cancer is the second-leading cause of cancer death in this country. In 2013,
This is the portion of the intestine which lies between the small intestine and the outlet (Anus).
 THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Outcome High Priority
 Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Preventive Care 2019 COLLECTION TYPE: MIPS CLINICAL QUALITY
Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Preventive Care 2019 COLLECTION TYPE: MIPS CLINICAL QUALITY
FY 2016 MCRCEDP Approved ICD-10 Code List
 Approved List C18.0 Malignant neoplasm of cecum C18.1 Malignant neoplasm of appendix C18.2 Malignant neoplasm of ascending colon C18.3 Malignant neoplasm of hepatic flexure C18.4 Malignant neoplasm of
Approved List C18.0 Malignant neoplasm of cecum C18.1 Malignant neoplasm of appendix C18.2 Malignant neoplasm of ascending colon C18.3 Malignant neoplasm of hepatic flexure C18.4 Malignant neoplasm of
Clinical Management of Obscure- Overt Gastrointestinal Bleeding. Presented by Dr. 張瀚文
 Clinical Management of Obscure- Overt Gastrointestinal Bleeding Presented by Dr. 張瀚文 Definition Obscure: : hard to understand; not clear. Overt: : public; not secret. Occult: : hidden from the knowledge
Clinical Management of Obscure- Overt Gastrointestinal Bleeding Presented by Dr. 張瀚文 Definition Obscure: : hard to understand; not clear. Overt: : public; not secret. Occult: : hidden from the knowledge
Research Article Adenoma and Polyp Detection Rates in Colonoscopy according to Indication
 Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 7207595, 6 pages https://doi.org/10.1155/2017/7207595 Research Article Adenoma and Polyp Detection Rates in Colonoscopy according
Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 7207595, 6 pages https://doi.org/10.1155/2017/7207595 Research Article Adenoma and Polyp Detection Rates in Colonoscopy according
FECAL OCCULT BLOOD TEST
 MEDICAL POLICY For use with the UnitedHealthcare Laboratory Benefit Management Program, administered by BeaconLBS FECAL OCCULT BLOOD TEST Policy Number: CMP - 023 Effective Date: January 1, 2018 Table
MEDICAL POLICY For use with the UnitedHealthcare Laboratory Benefit Management Program, administered by BeaconLBS FECAL OCCULT BLOOD TEST Policy Number: CMP - 023 Effective Date: January 1, 2018 Table
C olorectal adenomas are reputed to be precancerous
 568 COLORECTAL CANCER Incidence and recurrence rates of colorectal adenomas estimated by annually repeated colonoscopies on asymptomatic Japanese Y Yamaji, T Mitsushima, H Ikuma, H Watabe, M Okamoto, T
568 COLORECTAL CANCER Incidence and recurrence rates of colorectal adenomas estimated by annually repeated colonoscopies on asymptomatic Japanese Y Yamaji, T Mitsushima, H Ikuma, H Watabe, M Okamoto, T
Guidelines for Breast, Cervical and Colorectal Cancer Screening
 Guidelines for Breast, Cervical and Colorectal Cancer Screening Your recommendation counts. Talk to your patients about screening for cancer. CancerCare Manitoba provides organized, population-based screening
Guidelines for Breast, Cervical and Colorectal Cancer Screening Your recommendation counts. Talk to your patients about screening for cancer. CancerCare Manitoba provides organized, population-based screening
Joint Session with ACOFP and Cancer Treatment Centers of America (CTCA): Cancer Screening: Consensus & Controversies. Ashish Sangal, M.D.
 Joint Session with ACOFP and Cancer Treatment Centers of America (CTCA): Cancer Screening: Consensus & Controversies Ashish Sangal, M.D. Cancer Screening: Consensus & Controversies Ashish Sangal, MD Director,
Joint Session with ACOFP and Cancer Treatment Centers of America (CTCA): Cancer Screening: Consensus & Controversies Ashish Sangal, M.D. Cancer Screening: Consensus & Controversies Ashish Sangal, MD Director,
Updates in Colorectal Cancer Screening & Prevention
 Updates in Colorectal Cancer Screening & Prevention Swati G. Patel, MD MS Assistant Professor of Medicine Division of Gastroenterology & Hepatology Gastrointestinal Cancer Risk and Prevention Clinic University
Updates in Colorectal Cancer Screening & Prevention Swati G. Patel, MD MS Assistant Professor of Medicine Division of Gastroenterology & Hepatology Gastrointestinal Cancer Risk and Prevention Clinic University
Colon, or Colorectal, Cancer Information
 Colon, or Colorectal, Cancer Information Definition Colon, or colorectal, cancer is cancer that starts in the large intestine (colon) or the rectum (end of the colon). Other types of cancer can affect
Colon, or Colorectal, Cancer Information Definition Colon, or colorectal, cancer is cancer that starts in the large intestine (colon) or the rectum (end of the colon). Other types of cancer can affect
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
GI Polyp syndromes in children. Screening and surveillance, surgery.
 Dr Warren Hyer Consultant Paediatric Gastroenterologist St Mark s Hospital, UK GI Polyp syndromes in children Screening and surveillance, surgery. No conflict of interests to declare Objectives Understand
Dr Warren Hyer Consultant Paediatric Gastroenterologist St Mark s Hospital, UK GI Polyp syndromes in children Screening and surveillance, surgery. No conflict of interests to declare Objectives Understand
Colorectal Cancer Screening: Recommendations for Physicians and Patients from the U.S. Multi-Society Task Force on Colorectal Cancer
 Colorectal Cancer Screening: Recommendations for Physicians and Patients from the U.S. Multi-Society Task Force on Colorectal Cancer Douglas K. Rex, MD, MACG 1, C. Richard Boland, MD 2, Jason A. Dominitz,
Colorectal Cancer Screening: Recommendations for Physicians and Patients from the U.S. Multi-Society Task Force on Colorectal Cancer Douglas K. Rex, MD, MACG 1, C. Richard Boland, MD 2, Jason A. Dominitz,
Filiform polyposis of ulcerative colitis
 Filiform polyposis of ulcerative colitis Authors: Keisuke Yamada, Hironori Samura, Tatsuya Kinjo, Tetsu Kinjo, Akira Hokama, Jiro Fujita Article type: Clinical image Received: December 7, 2018. Accepted:
Filiform polyposis of ulcerative colitis Authors: Keisuke Yamada, Hironori Samura, Tatsuya Kinjo, Tetsu Kinjo, Akira Hokama, Jiro Fujita Article type: Clinical image Received: December 7, 2018. Accepted:
The Role of Surgery in Inflammatory Bowel Disease. Cory D Barrat, MD Colon and Rectal Surgeon Mercy Health
 The Role of Surgery in Inflammatory Bowel Disease Cory D Barrat, MD Colon and Rectal Surgeon Mercy Health THANKS FOR INVITING ME! I have no financial disclosures Outline - Who am I and what do I do? -
The Role of Surgery in Inflammatory Bowel Disease Cory D Barrat, MD Colon and Rectal Surgeon Mercy Health THANKS FOR INVITING ME! I have no financial disclosures Outline - Who am I and what do I do? -
Gastroenterology Fellowship Program
 Gastroenterology Fellowship Program Outpatient Clinical Rotations I. Overview A. Three Year Continuity Clinic Experience All gastroenterology fellows will be required to have a ½ day continuity clinic
Gastroenterology Fellowship Program Outpatient Clinical Rotations I. Overview A. Three Year Continuity Clinic Experience All gastroenterology fellows will be required to have a ½ day continuity clinic
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
Bowel Cancer Information Leaflet THE DIGESTIVE SYSTEM
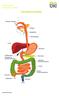 THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
Local Coverage Determination for Colorectal Cancer Screening (L29796)
 Page 1 of 15 Home Medicare Medicaid CHIP About CMS Regulations & Guidance Research, Statistics, Data & Systems Outreach & E People with Medicare & Medicaid Questions Careers Newsroom Contact CMS Acronyms
Page 1 of 15 Home Medicare Medicaid CHIP About CMS Regulations & Guidance Research, Statistics, Data & Systems Outreach & E People with Medicare & Medicaid Questions Careers Newsroom Contact CMS Acronyms
Estimates of complications and clinically significant findings in screening and surveillance colonoscopy
 Oregon Health & Science University OHSU Digital Commons Scholar Archive February 2011 Estimates of complications and clinically significant findings in screening and surveillance colonoscopy J. Lucas Williams
Oregon Health & Science University OHSU Digital Commons Scholar Archive February 2011 Estimates of complications and clinically significant findings in screening and surveillance colonoscopy J. Lucas Williams
2. Describe pros/cons of screening interventions (including colonoscopy, CT colography, fecal tests)
 Learning Objectives 1. Review principles of colon adenoma/cancer biology that permit successful prevention regimes 2. Describe pros/cons of screening interventions (including colonoscopy, CT colography,
Learning Objectives 1. Review principles of colon adenoma/cancer biology that permit successful prevention regimes 2. Describe pros/cons of screening interventions (including colonoscopy, CT colography,
Colorectal Cancer Prevention Quantity and Quality Count
 Colorectal Cancer Prevention Quantity and Quality Count Ernesto Drelichman, MD Gastrointestinal Surgery & Endoscopy Providence Hospital Key Messages Colorectal cancer can be prevented Screening reduces
Colorectal Cancer Prevention Quantity and Quality Count Ernesto Drelichman, MD Gastrointestinal Surgery & Endoscopy Providence Hospital Key Messages Colorectal cancer can be prevented Screening reduces
Diagnostic and Therapeutic Approaches to Dysplasia in Inflammatory Bowel Diseases
 Diagnostic and Therapeutic Approaches to Dysplasia in Inflammatory Bowel Diseases Parakkal Deepak, M.B.B.S., M.S. Assistant Professor of Medicine Division of Gastroenterology John T. Milliken Department
Diagnostic and Therapeutic Approaches to Dysplasia in Inflammatory Bowel Diseases Parakkal Deepak, M.B.B.S., M.S. Assistant Professor of Medicine Division of Gastroenterology John T. Milliken Department
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint
 GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
Bleeding in the Digestive Tract
 Bleeding in the Digestive Tract National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health
Bleeding in the Digestive Tract National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health
Barrett s Esophagus. Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI
 Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Capsule Endoscopy: Is it Really Helpful in the Diagnosis of Small Bowel Diseases? Kashif Malik, Muhammad Joher Amin, Syed Waqar Hassan Shah
 Original Article Capsule Endoscopy: Is it Really Helpful in the Diagnosis of Small Bowel Diseases? Kashif Malik, Muhammad Joher Amin, Syed Waqar Hassan Shah ABSTRACT Objective: To determine the diagnostic
Original Article Capsule Endoscopy: Is it Really Helpful in the Diagnosis of Small Bowel Diseases? Kashif Malik, Muhammad Joher Amin, Syed Waqar Hassan Shah ABSTRACT Objective: To determine the diagnostic
Colon Cancer Screening. Layth Al-Jashaami, MD GI Fellow, PGY 4
 Colon Cancer Screening Layth Al-Jashaami, MD GI Fellow, PGY 4 -Colorectal cancer (CRC) is a common and lethal cancer. -It has the highest incidence among GI cancers in the US, estimated to be newly diagnosed
Colon Cancer Screening Layth Al-Jashaami, MD GI Fellow, PGY 4 -Colorectal cancer (CRC) is a common and lethal cancer. -It has the highest incidence among GI cancers in the US, estimated to be newly diagnosed
Surveying the Colon; Polyps and Advances in Polypectomy
 Surveying the Colon; Polyps and Advances in Polypectomy Educational Objectives Identify classifications of polyps Describe several types of polyps Verbalize rationale for polypectomy Identify risk factors
Surveying the Colon; Polyps and Advances in Polypectomy Educational Objectives Identify classifications of polyps Describe several types of polyps Verbalize rationale for polypectomy Identify risk factors
SMALL BOWEL GASTROINTESTINAL BLEEDING
 SMALL BOWEL GASTROINTESTINAL BLEEDING Giovanni DI NARDO giovanni.dinardo@uniroma1.it UOC Gastroenterologia ed Epatologia Pediatrica Dipartimento di Pediatria, Sapienza - Università di Roma (Direttore:
SMALL BOWEL GASTROINTESTINAL BLEEDING Giovanni DI NARDO giovanni.dinardo@uniroma1.it UOC Gastroenterologia ed Epatologia Pediatrica Dipartimento di Pediatria, Sapienza - Università di Roma (Direttore:
Colorectal Cancer Screening
 Recommendations from the U.S. Multi-Society Task Force on Colorectal Cancer Colorectal Cancer Screening Rex DK, Boland CR, Dominitz JA, Giardiello FM, Johnson DA, Kaltenbach T, Levin TR, Lieberman D, Robertson
Recommendations from the U.S. Multi-Society Task Force on Colorectal Cancer Colorectal Cancer Screening Rex DK, Boland CR, Dominitz JA, Giardiello FM, Johnson DA, Kaltenbach T, Levin TR, Lieberman D, Robertson
Summary. Cezary ŁozińskiABDF, Witold KyclerABCDEF. Rep Pract Oncol Radiother, 2007; 12(4):
 Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Digestive Health Southwest Endoscopy 2016 Quality Report
 Digestive Health 2016 Quality Report Our 2016 our quality and value management program focused on one primary area of interest: Performing high quality colonoscopy High quality Colonoscopy We selected
Digestive Health 2016 Quality Report Our 2016 our quality and value management program focused on one primary area of interest: Performing high quality colonoscopy High quality Colonoscopy We selected
Guideline scope Diverticular disease: diagnosis and management
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Diverticular disease: diagnosis and management The Department of Health in England has asked NICE to develop a clinical guideline on diverticular
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Diverticular disease: diagnosis and management The Department of Health in England has asked NICE to develop a clinical guideline on diverticular
Colon Cancer Screening and Surveillance. Louis V. Antignano, M.D. Wilson Gastroenterology October 11, 2011
 Colon Cancer Screening and Surveillance Louis V. Antignano, M.D. Wilson Gastroenterology October 11, 2011 Colorectal Cancer Preventable cancer Number 2 cancer killer in the USA Often curable if detected
Colon Cancer Screening and Surveillance Louis V. Antignano, M.D. Wilson Gastroenterology October 11, 2011 Colorectal Cancer Preventable cancer Number 2 cancer killer in the USA Often curable if detected
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
What do we need for diagnosis of IBD
 What do we need for diagnosis of IBD Kaichun Wu Dept. of Gastroenterology, Xijing Hospital Fourth Military Medical University Xi an an,, China In China UC 11.6/10 5,CD 1.4/10 5 Major cause of chronic diarrhea
What do we need for diagnosis of IBD Kaichun Wu Dept. of Gastroenterology, Xijing Hospital Fourth Military Medical University Xi an an,, China In China UC 11.6/10 5,CD 1.4/10 5 Major cause of chronic diarrhea
When is a programmed follow-up meaningful and how should it be done? Professor Alastair Watson University of Liverpool
 When is a programmed follow-up meaningful and how should it be done? Professor Alastair Watson University of Liverpool Adenomas/Carcinoma Sequence Providing Time for Screening Normal 5-20 yrs 5-15 yrs
When is a programmed follow-up meaningful and how should it be done? Professor Alastair Watson University of Liverpool Adenomas/Carcinoma Sequence Providing Time for Screening Normal 5-20 yrs 5-15 yrs
Chromoendoscopy - Should It Be Standard of Care in IBD?
 Chromoendoscopy - Should It Be Standard of Care in IBD? John F. Valentine, MD, FACG Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Utah What is the point of
Chromoendoscopy - Should It Be Standard of Care in IBD? John F. Valentine, MD, FACG Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Utah What is the point of
Neoplastic Colon Polyps. Joyce Au SUNY Downstate Grand Rounds, October 18, 2012
 Neoplastic Colon Polyps Joyce Au SUNY Downstate Grand Rounds, October 18, 2012 CASE 55M with Hepatitis C, COPD (FEV1=45%), s/p vasectomy, knee surgery Meds: albuterol, flunisolide, mometasone, tiotropium
Neoplastic Colon Polyps Joyce Au SUNY Downstate Grand Rounds, October 18, 2012 CASE 55M with Hepatitis C, COPD (FEV1=45%), s/p vasectomy, knee surgery Meds: albuterol, flunisolide, mometasone, tiotropium
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal surgery prior as factor in laparoscopic colorectal surgery, 554 555 Abscess(es) CRC presenting as, 539 540 Adenocarcinoma of
Index Note: Page numbers of article titles are in boldface type. A Abdominal surgery prior as factor in laparoscopic colorectal surgery, 554 555 Abscess(es) CRC presenting as, 539 540 Adenocarcinoma of
Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology
 Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology Faculty representative: David L. Burns, MD, CNSP Resident representative: Tom Castiglione, MD Revision date: March 6, 2006
Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology Faculty representative: David L. Burns, MD, CNSP Resident representative: Tom Castiglione, MD Revision date: March 6, 2006
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE
 SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
Wireless Capsule Endoscopy as a Diagnostic Technique in Disorders of the Small Bowel, Esophagus and Colon. Original Policy Date
 MP 6.01.23 Wireless Capsule Endoscopy as a Diagnostic Technique in Disorders of the Small Bowel, Esophagus and Colon Medical Policy Section Radiology Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 6.01.23 Wireless Capsule Endoscopy as a Diagnostic Technique in Disorders of the Small Bowel, Esophagus and Colon Medical Policy Section Radiology Issue 12:2013 Original Policy Date 12:2013 Last Review
Improving Access to Endoscopy at Safety-Net Hospitals. Lukejohn W. Day MD Assistant Professor of Medicine
 Improving Access to Endoscopy at Safety-Net Hospitals Lukejohn W. Day MD Assistant Professor of Medicine Goals Background Improving Access to Endoscopic Care Electronic referral: ereferral Direct Access
Improving Access to Endoscopy at Safety-Net Hospitals Lukejohn W. Day MD Assistant Professor of Medicine Goals Background Improving Access to Endoscopic Care Electronic referral: ereferral Direct Access
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE
 COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
