The management of gastric polyps
|
|
|
- Sharon Wilkins
- 6 years ago
- Views:
Transcription
1 The management of gastric polyps Andrew F Goddard, 1 Rawya Badreldin, 2 D Mark Pritchard, 3 Marjorie M Walker, 4 Bryan Warren, 5 on behalf of the British Society of Gastroenterology 1 Digestive Diseases Centre, Royal Derby Hospital, Derby, UK 2 Department of Gastroenterology, James Paget Hospital, Great Yarmouth, Norfolk, UK 3 Division of Gastroenterology, School of Clinical Sciences, University of Liverpool, UK 4 Department of Histopathology, Faculty of Medicine, Imperial College, London, UK 5 Department of Pathology, John Radcliffe Hospital, Oxford, UK Correspondence to Dr Andrew F Goddard, Digestive Diseases Centre, Royal Derby Hospital, Uttoxeter Road, Derby DE22 3NE, UK; andrew. goddard@derbyhospitals.nhs.uk Revised 19 February 2010 Accepted 24 February 2010 ABSTRACT Background Gastric polyps are important as some have malignant potential. If such polyps are left untreated, gastric cancer may result. The malignant potential depends on the histological type of the polyp. The literature base is relatively weak and any recommendations made must be viewed in light of this. Definition Gastric polyps are sessile or pedunculated lesions that originate in the gastric epithelium or submucosa and protrude into the stomach lumen. Malignant potential Depending on histological type, some gastric polyps (adenomas and hyperplastic polyps) have malignant potential and are precursors of early gastric cancer. They may also indicate an increased risk of intestinal or extra-intestinal malignancy. SUMMARY OF RECOMMENDATIONS (QUALITY OF EVIDENCE, BENEFIT/HARM RATIO, STRENGTH OF RECOMMENDATION) < All types of gastric polyp detected at endoscopy need to be sampled for which forceps biopsy usually suffices (moderate, net benefit, qualified) < Biopsy of intervening non-polypoid gastric mucosa is recommended for all hyperplastic and adenomatous polyps (moderate, uncertain trade-offs, qualified) < If Helicobacter pylori is detected in patients with hyperplastic and adenomatous polyps, it should be eradicated (moderate, net benefit, qualified) < All gastric polyps with dysplastic foci and symptomatic polyps should be completely removed (moderate, net benefit, qualified) < All gastric adenomatous polyps should be removed when safe to do so (high, net benefit, definitive) < If adenomatous polyps are detected, an examination of the whole stomach should be made for mucosal abnormalities and any such abnormalities should be biopsied (moderate, net benefit, definitive) < Familial adenomatous polyposis should be considered as a diagnosis in young patients with numerous fundic gland polyps (low, uncertain trade offs, qualified) < Endoscopists performing polypectomies must be proficient in performing endoscopic haemostasis techniques (low, net benefits, definitive) < Repeat gastroscopy should be performed at 1 year for all polyps with dysplasia that have not been removed (moderate, net benefits, qualified) < Repeat gastroscopy should be performed at 1 year following complete polypectomy for high risk polyps (moderate, net benefits, qualified) ORIGIN AND PURPOSE OF THESE GUIDELINES The widespread use of endoscopy has resulted in increased detection of gastric mucosal lesions, many of which are found incidentally. Gastric polyps do not represent a uniform entity and encompass a wide variety of pathology that has differing malignant potential and there are currently no guidelines for the management of these lesions. This guideline aims to characterise gastric polyps and provide a framework for management. However, recommendations for diagnosis and treatment of these polyps remain controversial, as there is no consensus. Specifically, these guidelines do not cover the management of early gastric cancer. Scope These guidelines are primarily intended for all endoscopists performing gastroscopy. Literature search A search of Medline was made using key words: gastric polyps, adenomas, hyperplastic polyps, fundic gland polyps, inflammatory fibroid polyps, familial adenomatous polyposis, juvenile polyps, juvenile polyposis, PeutzeJeghers syndrome and Cowden s disease. Grading of recommendations The quality of evidence for recommendations made in these guidelines based on the GRADE system. 1 Each recommendation is graded according to the quality of evidence, the relative benefit/harm of following the recommendation and the strength of recommendation. Quality of evidence is graded as: highdfurther research very unlikely to change our confidence in the estimate of effect; moderatedfurther research likely to have an important effect on our confidence on the estimate effect and may change the estimate; lowdfurther research very likely to have an important impact on our confidence of the estimate of effect and is likely to change the estimate; or very lowdestimate of effect is very uncertain. Benefiteharm is graded as: net benefitdthe intervention clearly does more good than harm; trade offsdthere are important trade offs between the benefits and harm; uncertain trade offsdit is not clear whether the intervention does more good than harm; or no net benefitsdthe intervention clearly does not do more good than harm. Strength of recommendation is recommended as: definitiveda judgement that most informed people would make; or qualifiedda judgement that the majority of well informed clinicians would make but a substantial minority would not Gut 2010;59:1270e1276. doi: /gut
2 Methodology of guideline preparation The literature review was performed by the five authors of the guideline and draft guidelines were prepared. The draft guideline was then reviewed by all members of the British Society of Gastroenterology (BSG) Gastroduodenal Section and Pathology Section Committees. Two meetings were held involving all members of the Gastroduodenal Section Committee to redraft the guideline. This redraft, once approved by the committee, was then reviewed by the BSG Clinical Services and Standards Committee. Further changes were made following recommendations from this committee and a consensus guideline prepared. The consensus guideline was sent to all 279 members of the BSG gastroduodenal section. Members were asked to assess each recommendation made and rate them as agree, neutral or disagree. This feedback was collated and a consensus meeting held of ten representatives from the BSG gastroduodenal and pathology sections. The members of this consensus panel are listed in appendix 1. A final version of the guideline was then prepared. INTRODUCTION Polyps are usually asymptomatic and >90% are found incidentally. Larger polyps can present with bleeding, anaemia, abdominal pain or gastric outlet obstruction. Although some types of polyps may have typical appearances at endoscopy the presence of dysplasia cannot be determined without histological assessment. Therefore all types of gastric polyp must be sampled to determine the pre-malignant risk. Some polyps are an expression of a genetic disease and may also indicate an increased risk of intestinal or extra-intestinal malignancy. Other precancerous conditions of the stomach include chronic atrophic gastritis and intestinal metaplasia. TYPES AND CLASSIFICATION OF POLYPS The most common types of benign epithelial gastric polyps (BEGPs) are fundic gland polyps, hyperplastic polyps and adenomas. If there are multiple gastric polyps present, these are usually of the same histological type. 2 The WHO has classified gastric polyps 3 4 but this classification is controversial. An updated classification is suggested in box 1. Fundic gland polyps Fundic gland polyps (also called Elster s glandular cysts) occur in two distinct clinicopathological settings: as sporadic polyps and polyps associated with the syndrome, familial adenomatous polyposis coli. Sporadic fundic gland polyps Fundic gland polyps (FGPs) constitute 16e51% of BEGPs 5e7 and may be observed in 0.8e23% of endoscopies. 8e10 They are usually multiple transparent sessile polyps, 1e5 mm in diameter, located in the body and fundus. Microscopy shows cystically dilated glands lined by gastric body type mucosa. 8 A single study 8 of 56 consecutive patients with FGPs suggested they can be diagnosed with a high degree of accuracy based on endoscopic appearance alone. Sporadic FGPs are usually caused by activating mutations of the beta-catenin gene and usually number less than ten. 13 Dysplasia occurs in <1% of sporadic FGPs. 14e16 FGPs are not associated with atrophic gastritis and the prevalence of Helicobacter pylori infection is very low in these patients. 17e20 Case reports have shown that H pylori infection may have an inhibitory effect on the development of FGPs but the cause of fundic Box 1 Classification of gastric polyps Epithelial polyps < Fundic gland polyp < Hyperplastic polyp < Adenomatous polyp < Hamartomatous polyps Juvenile polyp PeutzeJeghers syndrome Cowden s syndrome < Polyposis syndromes (non-hamartomatous) Juvenile polyposis Familial adenomatous polyposis Non-mucosal intramural polyps < Gastrointestinal stromal tumour < Leiomyoma < Inflammatory fibroid polyp < Fibroma and fibromyoma < Lipoma < Ectopic pancreas < Neurogenic and vascular tumours < Neuroendocrine tumours (carcinoids) gland polyps remains uncertain, and these polyps may regress or even disappear in time. 21 Proton pump inhibitor-associated gastric polyps Since 1993 there have been reports of the role of long-term proton pump inhibitors (PPIs) in the genesis of fundic gland polyps In one study FGPs were present in 23% of patients on PPIs compared with 12% of patients not taking a PPI. 10 The polyps are usually small (<1 cm) and occur in the proximal/midgastric body. 23 These reports have been retrospective studies and show that the mean interval for polyp development was 32.5 months and that they regress within 3 months of PPI cessation. However, other studies have not demonstrated adefinitive link between long-term PPIs and FGPs. 24e26 Similarly, a prospective long (median of 11 years) follow-up study of 230 patients could not show any de novo FGPs. 27 Histologically, in body mucosa, long-term PPI use induces enterochromaffin cell-like (ECL) hyperplasia and typical parietal cell protrusion and glands are lined by cells with a serrated rather than a smooth border. 23 Fundic gland polyps in familial adenomatous polyposis FGPs are common in patients with familial adenomatous polyposis (FAP) and arise from mutation of the APC gene. 22 In this context, they are usually multiple and can carpet the body of the stomach. Epithelial dysplasia occurs in 25e41% of FAP associated polyps. 13 The management of FAP is discussed later in this guideline. There is no evidence as to how to differentiate between sporadic FGP and FAP-associated FGP at endoscopy. The presence of dysplastic foci should arouse suspicion of FAP Two studies have shown the presence of colonic adenomas (7e45%) and adenocarcinomas (0e4.7%) in patients with sporadic FGPs However, this high rate of colonic neoplasia has not been confirmed in other studies. Therefore, while the presence of numerous FGPs may be a manifestation of FAP, there is no clear evidence about the number of polyps needed to indicate further investigation is Gut 2010;59:1270e1276. doi: /gut
3 warranted. When considering lower gastrointestinal investigation, it should be noted that almost all cases of classical FAP can be diagnosed on flexible sigmoidoscopy which is safer than colonoscopy. Recommendations for the management of FGPs < Polypectomy is not required for sporadic FGPs (moderate, net benefits, definitive). < Although FGPs have reliable endoscopic features, biopsy of probable FGPs is recommended to exclude dysplasia or adenocarcinoma (and possible FAP) and to exclude the need for polypectomy as required for other types of polyp (moderate, net benefit, qualified). < In patients with numerous FGP who are under 40 years of age, or where biopsies demonstrate dysplasia, colonic investigation should be performed to exclude FAP (low, uncertain trade offs, qualified). Hyperplastic polyps 5e7 17 Hyperplastic polyps (HYPPs) constitute 30e93% of all BEGPs and are sessile or pedunculated polyps less than 2 cm in diameter. They can occur as single polyps usually in the antrum or as multiple polyps throughout the stomach. Multiple hyperplastic polyps are also found in Menetrier s disease. Histologically, there is a proliferation of surface foveolar cells lining elongated, distorted pits that extend deep into the lamina propria. They may contain pyloric glands, chief cells, and parietal cells. Their histological appearance overlaps with hamartomas and inflammatory conditions. Polyp formation is strongly associated with chronic gastritis; Helicobacter-associated gastritis, pernicious anaemia, reactive or chemical gastritis when adjacent to ulcer erosions and around gastroenterostomy stomas Up to 80% of HYPPs have been found to regress after eradication of H pylori before endoscopic removal. 34e36 HYPPs rarely undergo neoplastic progression directly through neoplastic change in the polyp but are associated with an increased risk of synchronous cancer occurring elsewhere in the gastric mucosa. The prevalence of true dysplasia arising in hyperplastic polyps is debated 37e46 and reported rates have varied from 1.9% to 19% and cases of adenocarcinoma have been reported ranging from 0.6% to 2.1%. HYPPs also denote an increased risk of neoplasia in the surrounding abnormal gastric mucosa and are associated with the occurrence of synchronous cancer elsewhere in the gastric mucosa. 40 Multiple biopsies of the intervening mucosa are therefore needed in patients with HYPPs. The risk of adenocarcinoma in the surrounding mucosa is probably higher than in the polyp itself. There is controversy regarding whether gastric HYPPs can be simply biopsied or whether they should be entirely removed by polypectomy because of the risk of neoplasia and because forceps biopsy sampling may miss the dysplastic foci within a hyperplastic polyp. Some authors recommend performing polypectomy for all small polyps and periodic biopsy of larger hyperplastic polyps that are too big for polypectomy. Others recommend that, as cancer usually occurs in bigger hyperplastic polyps, only large hyperplastic polyps should be removed, due to the risk of gastric polypectomy. Surveillance of hyperplastic polyps that are not removed (either because of number or size) is probably safer than multiple polypectomies but there is no randomised evidence as to which approach should be taken. A single repeat endoscopy at 1 year is reasonable, but repeated surveillance after 1 year is not recommended due to lack of evidence. One study 47 has suggested that HYPP may cause gastrointestinal blood loss and should be removed in such patients. This has not been confirmed by other studies. Recommendations for the management of hyperplastic polyps < Hyperplastic polyps should be biopsied and an examination of the whole stomach should be made for mucosal abnormalities and any abnormalities biopsied (moderate, trade offs, definite) < Test for H pylori and eradicate when present (high, net benefit, definitive). Adenomatous polyps Gastric adenomas are true neoplasms and are precursors of gastric cancer. They are histological classified into tubular, villous and tubulovillous types. They constitute 3e26% of BEGPs, are frequently solitary and can be found anywhere in the stomach but are commonly found in the antrum. They frequently arise on a background of atrophic gastritis 48 and intestinal metaplasia, but there is no proven association with H pylori infection. Neoplastic progression is greater with polyps larger than 2 cm in diameter 49 and occurs in 28.5e40% of villous adenomas and 5% of tubular adenomas e53 There is also a strong association between gastric adenoma and synchronous or metachronous gastric adenocarcinoma The risk of association between adenomatous polyps and cancer increases with age. 45 Recommendations for management of adenomatous polyps < Complete removal of the adenoma should be performed when safe to do so (high, net benefit, definitive). < An examination of the whole stomach should be made for mucosal abnormalities and any abnormalities biopsied (high, net benefit, definitive). < Endoscopic follow-up is required following resection of gastric adenomas. Endoscopy should be repeated at 6 months for incompletely resected polyps or those with high grade dysplasia. Endoscopy can be repeated after 1 year for all other polyps (moderate, trade offs, qualified). Hamartomatous polyps Hamartomatous polyps are rare in the stomach and include juvenile polyps, polyps of PeutzeJeghers syndrome (PJS), and Cowden s disease. The follow-up recommendations of patients with these conditions are summarised in table 1. Juvenile polyps Juvenile polyps are found in the antrum. Solitary polyps have hamartomatous or inflammatory components and do not have a neoplastic potential. Histologically, these show irregular cysts lined by normal gastric epithelium; with possible stromal haemorrhage, surface ulceration and chronic inflammation due Table 1 Management of gastric polyps associated with polyposis syndromes Syndrome Familial adenomatous polyposis Lifetime risk of malignancy Surveillance recommendation 100% (colon) OGD every 2 years after age 18 Biopsy >5 polyps Remove polyps >1 cm Surveillance also required for duodenal polyps PeutzeJeghers >50% (extra-gi) OGD every 2 years after age 18 Biopsy >5 polyps Remove polyps >1cm Juvenile polyposis >50% OGD every 3 years after age 18 Cowden s Rare Eradicate H pylori No further OGD needed There is very little evidence for the following recommendations, but given the high risk of malignancy in these conditions careful surveillance is necessary. GI, gastro-intestinal; OGD, gastroscopy Gut 2010;59:1270e1276. doi: /gut
4 to torsion. Multiple polyps are associated with juvenile polyposis. PeutzeJeghers syndrome PJS is a rare autosomal dominant inherited condition, characterised by the presence of hamartomatous gastrointestinal polyps and mucocutaneous pigmentation of the lips, buccal mucosa and digits. Microscopically, hyperplastic glands lined by foveolar epithelium and broad bands of smooth muscle fibres that branch out are found. PJS increases the risk of both gastrointestinal cancer through the hamartomaeadenomaecarcinoma sequence and de novo malignant change. There is a 15-fold increase in extra-intestinal malignancies such as breast, endometrial, pancreatic and lung cancers. 54 Recommendation for PJS gastric polyps < Gastric polyps greater than 1 cm should be removed. As there is a high rate of recurrence, regular endoscopic follow-up and annual screening of other susceptible organs is recommended (moderate, trade offs, qualified). Cowden s syndrome Cowden s syndrome (CS) or multiple hamartoma syndrome is a rare autosomal dominant syndrome characterised by orocutaneous hamartomatous tumours, gastrointestinal polyps, abnormalities of the breast, thyroid gland and genitourinary system. The gastrointestinal polyps are generally benign and malignant transformation is seen very rarely. Common benign visceral tumours and hyperplastic conditions include gastrointestinal polyps, thyroid adenoma and goitre and, fibrocystic disease of the breast in female patients, and gynaecomastia in male patients. Malignancies of the thyroid, colon, small bowel, and genitourinary tract have been reported, as well as acute myelogenous (myeloid) leukaemia, non-hodgkin s lymphoma and breast carcinoma. Histologically, CS polyps have elongated cystically dilated glands with papillary infoldings with a connective tissue (neural or muscular) component. Familial polyposis syndromes A summary of the cancer risk and screening recommendations for the familial polyposis syndromes is shown in table 1. Familial adenomatous polyposis Familial adenomatous polyposis (FAP) is caused by a germline mutation in the adenomatous polyposis coli APC gene on chromosome 5q21 and has an autosomal dominant inheritance and a high incidence of gastric cancer. Affected family members develop numerous colorectal adenomas with virtually a 100% chance of malignant progression unless the colon is removed prophylactically. Gastric polyps occur in 30e100% of cases of FAP and these patients are said to have familial gastric polyposis (FGP). Most polyps are benign fundic gland polyps and gastric adenomatous polyps occur in only 5%, usually in the antrum. Duodenal adenomas and periampullary adenomas occur in 50e90% of patients, are usually malignant and are the main cause of mortality after prophylactic colectomy. There is a negative association with H pylori-associated chronic gastritis. 57 Sampling of polyps is required to determine whether they are adenomas or FGPs. Endoscopic surveillance of small gastric and duodenal polyps is required every 1e2 years until the patient reaches the age of 50 years but large polyps/adenomas may require more frequent surveillance. Surveillance frequency can be reduced to five yearly after the age of 50 years. Partial gastrectomy and local duodenal resection or pancreaticoduodenectomy may be required in selected patients. Juvenile polyposis This condition is associated with numerous mutations (BMPR1A, 10q22.3, SMAD4, 18q21.1) and is associated with gastric malignancy in over 50% of cases Juvenile polyposis is also associated with gastrointestinal bleeding 60 and proteinlosing enteropathy. Histologically, the glands are tortuous, elongated and cystically dilated and the background mucosa is oedematous and inflamed. Inflammatory fibroid polyps Inflammatory fibroid polyps (IFPs) constitute 3% of all BEGP 5 and are well-circumscribed lesions located in the antrum or prepyloric region, covered with a smooth surface of normal mucosa. They originate from the submucosa and should not be confused with inflammatory polyps, which are a commonly used misnomer for hyperplastic polyps. They occur in patients of all ages, but more commonly in the fifth to sixth decades of life, and more frequently in females. They do not have a malignant potential but are associated with chronic atrophic gastritis. Their aetiology remains obscure but there is a weak association with H pylori. 61 Polyps grow to 1e5 cm in diameter and the larger lesions often have a central depression, ulceration or a white cap. IFPs remain unchanged and asymptomatic for a long time but have the propensity to enlarge and cause gastric obstruction. Histology shows blood vessels surrounded by spindle cells (CD 34 and fascin positive) and chronic inflammatory cells, predominantly eosinophils. Multinucleated giant cells may be present, but they are not associated with a systemic allergic reaction or eosinophilia. IFPs may be amenable to complete endoscopic excision but extension into the deeper layers of the gastric wall sometimes preclude this, and for very deep polyps, forceps biopsy may be negative. Gastric neuroendocrine tumours (carcinoids) Management of gastric neuroendocrine tumours is discussed in detail in Guidelines for the management of gastroenteropancreatic neuroendocrine (including carcinoid) tumours 62 and will therefore only be summarised here. Most gastric NETs are composed of enterochromaffin-like (ECL) cells, which be identified histopathologically by immunostaining for markers such as chromogranin A or synaptophysin. There are three main subtypes. Type 1 tumours (approximately 80% of total) are usually sessile polyps and associated with (usually autoimmune) atrophic gastritis, pernicious anaemia, achlorhydria and hypergastrinaemia, with the elevated gastrin being produced by gastric antral G cells. Type 2 gastric NETs (approximately 5% of total) occur in patients with ZollingereEllison syndrome, usually in the setting of multiple endocrine neoplasia type 1 (MEN1). They are therefore associated with gastrinomas, hypergastrinaemia and gastric hyperacidity. Type 3 gastric NETs (approximately 15%) occur sporadically and are not associated with hypergastrinaemia. Treatment and prognosis is determined by tumour type, size of polyp(s) and by the presence or absence of metastases 62 Type 1 tumours carry a very good prognosis and may need no treatment if the tumours are small (<1 cm). Larger type 1 NETs should be treated by endoscopic polypectomy or surgical antrectomy should be considered. Type 2 gastric NETs usually regress if the gastrinoma can be completely removed surgically. Type 3 gastric NETs are associated with the worst prognosis and Gut 2010;59:1270e1276. doi: /gut
5 should be treated by surgical resection. Metastatic tumours of all types are amenable to a range of palliative treatments, as discussed in more detail elsewhere. 62 Recommendations for management of gastric NET < The type of gastric NETshould be determined in each case by biopsy of the lesion and surrounding normal mucosa, and measuring fasting serum gastrin concentration (moderate, trade offs, qualified). < Tumours should be staged appropriately and treatment options should be discussed with a neuroendocrine tumour multidisciplinary team (moderate, benefit, definitive). Stromal tumours Management of gastrointestinal stromal tumours (GISTs) is discussed in detail in the document Consensus meeting for the management of gastrointestinal stromal tumors. 65 Therefore only a brief summary will be included here. GISTs are rare connective tissue tumours that show similar differentiation patterns to the interstitial cells of Cajal and approximately 60e70% arise in the stomach. Activating mutations of the KIT or PDGFRA protooncogenes are thought to be the causal molecular events. Approximately 95% of tumours are therefore positive for CD117 (c-kit) by immunohistochemistry. The degree of local and metastatic spread of gastric GISTs should be evaluated by CT scan and endoscopic ultrasound. If the tumour is localised to the stomach it should be surgically resected. If the tumour is unresectable or if metastases are present at diagnosis or during follow-up, treatment with the tyrosine kinase inhibitor, imatinib, should be considered and treatment should usually be continued until progression, intolerance or patient refusal occurs. NICE guidelines on the use of imatinib therapy in this tumour type are available. 66 ENDOSCOPIC RECOMMENDATIONS Biopsying the gastric mucosa Given that most polyps found at endoscopy will be FGPs and therefore biopsies of the gastric mucosa are not indicated, it is not cost effective to recommend biopsying the surrounding mucosa in everyone. If biopsies are taken at the index endoscopy they do not need to be repeated at subsequent procedures. However, if they have not been taken, they are needed in patients with hyperplastic and adenomatous polyps. Polyp sampling; forceps biopsy or polypectomy Sampling of polyps greater than 5 mm by forceps biopsy raises concern about whether it is representative of the whole polyp or whether dysplasia or cancer may be missed. A prospective multicentre study of 222 endoscopically removable polyps (excluding fundic gastric polyps and polyposis syndrome) showed complete histological agreement between initial biopsies and polypectomy in 55.8% of cases and in 34.7% differentiation between tumourlike lesions and neoplasia was possible. 67 However, in 2.7% relevant differences were found, the most common being failure of biopsy to reveal foci of carcinoma in hyperplastic polyps. Thus the correct histological diagnosis can be obtained without a complete polypectomy in 97.3% of cases. Other series which looked at whether forceps biopsy is representative of the whole polyp showed discrepancy with rates ranging from 0% to 29%. 68e71 Occasionally, biopsies reveal normal mucosa in a gastric polypoid lesion, which may indicate either missed sampling or a submucosal, intramural or less commonly an extra-gastric lesion. There is a higher rate of disagreement for sessile gastric polyps and flat lesions, and in one series assessing flat early gastric cancers only 55% of biopsies agreed with histology of endoscopic mucosal resections (EMR). 72 There is limited data on complications following gastric polypectomy for benign polyps. Most studies in this area have evaluated the role of endoscopic therapy for treating early gastric cancers. Snare polypectomy and EMR in the stomach carry a high risk of complications. In the largest study, 7.2% patients had post-polypectomy bleeding, 80% of whom needed endoscopic therapeutic intervention. 67 Endoscopic mucosal resection (EMR) and endoscopic mucosal dissection (EMD) of 479 flat and raised early gastric cancers in Japan had a bleeding and perforation rate of 5%. 73 Therefore, given the risks of gastric polypectomy, it may be safer to only biopsy polyps in patients with co-morbidity or at risk of haemorrhage. Polyps <1 cm probably only require two biopsies, whereas larger polyps require three to four biopsies. The risks of polypectomy also require the clinician to be confident that polypectomy is indicated. Thus, given the difficulty in confirming definite dysplasia in some polyps, an agreement by two histopathologists that dysplasia is present is ideal before embarking on polypectomy. Recommendations for gastric polypectomy < Any polyp with a dysplastic focus should be completely removed when safe to do so (moderate, trade offs, qualified) < Endoscopists performing gastric polypectomy should be competent to manage the complications of bleeding (high, benefit, definitive). < The decision to perform a polypectomy must be weighed against the risk of complications especially in elderly patients with concomitant illness (high, benefit, definitive). An algorithm for the management of single and multiple gastric polyps is given in figure 1. Endoscopic follow-up All gastric polyps except FGPs and inflammatory fibroid polyps are associated with significantly increased gastric cancer risk. Table 2 summarises the characteristics of gastric polyps and their cancer risk. Adenoma With dysplasia or symptoms Gastric Polyp(s) Forceps biopsy of polyp(s) and surrounding mucosa if suspicion of non-fgp Polypectomy if safe to do so Follow up endoscopy in one year Hyperplastic polyp Eradicate H. pylori if present Repeat endoscopy at 1year Polyp persists No polyp Fundic gland polyp or Inflammatory fibroid polyp Consider FAP. Consider polypectomy if symptomatic No follow-up Figure 1 Algorithm for the management of gastric polyps. FAP, familial adenomatous polyposis Gut 2010;59:1270e1276. doi: /gut
6 Table 2 Gastric polyp characteristics and malignant potential Polyp type Usual number and size Usual site Malignant potential of polyp Malignant potential of background mucosa Management Sporadic fundic gland polyp Multiple 1e5 mm Upper and lower body Very low Very low Biopsy to confirm nature of polyp No follow-up needed Familial adenomatous polyposisassociated fundic gland polyp Multiple carpet <1 cm Upper and lower body Low Low Biopsy to confirm nature of polyp Repeat OGD every 2 years Hyperplastic Single 1e2 cm Antrum Low but significant Low Remove polyp if dysplastic Eradicate H pylori Repeat OGD 1 year Multiple <1 cm Lower body Low but significant Low Eradicate H pylori Repeat OGD 1 year Adenoma Single 1e2 cm Antrum High Significant Remove polyp Sample rest of gastric mucosa Repeat OGD at 1 year Inflammatory fibroid polyp Single 1e5 cm Antrum Very low Very low Biopsy to confirm nature of polyp Remove if causing obstruction No follow-up OGD, gastroscopy. There is no evidence as to whether gastric polyps need longterm surveillance, and given the cost implications of such a programme, only a single gastroscopy 1 year after the removal of polyps with dysplasia is recommended (in the absence of polyp syndromes). FUTURE RESEARCH AND AUDIT Future research topics The following are areas that preparation of these guidelines revealed as needing further research: < The necessity of biopsying typical appearing FGPs < The prevalence of FAP in young patients with >20 FGPs < The natural history of gastric polyps with and without dysplasia < The efficacy of H pylori eradication in patients with hyperplastic polyps < The risks/benefits of different surveillance intervals for gastroscopy following polypectomy < The risks/benefits of polypectomy versus biopsy for nonadenomatous gastric polyps Audit targets We recommend the following targets for audit: < >95% of single gastric polyps should be sampled together with the surrounding mucosa where necessary < >80% of adenomatous polyps should be removed and retrieved < >90% of patients with gastric polyps in whom H pylori is detected should have it eradicated successfully CONCLUSIONS The management of a patient in whom a gastric polyp has been detected endoscopically must include typing the lesion by histology and assessment of dysplasia. Most gastric polyps are benign and need minimal intervention or follow-up. However, some types of gastric polyp have significant malignant potential and it is the responsibility of the endoscopist to ensure that such polyps are identified and managed appropriately. Competing interests None declared. Provenance and peer review Not commissioned; externally peer reviewed. REFERENCES 1. Atkins D, Best D, Briss PA, et al. Grading quality of evidence and strength of recommendations. Br Med J 2004;328: Deppisch L, Rona VT. Gastric epithelial polyps. A 10 year study. J Clin Gastroenterol 1989;11:110e Jass JR, Sobin LH, Watanabe H. The World Health Organization s histologic classification of gastrointestinal tumours. A commentary on the second edition. Cancer 1990;66:2162e7. 4. WHO classification of Tumours. Pathology and genetics: tumours of the digestive system. Lyon, France: IARC Press, Stolte M, Stich T, Eidt S, et al. Frequency, location and age and sex distribution of various types of gastric polyps. Endoscopy 1994;26:659e Morais DJ, Yamanaka A, Zeitun JM, et al. Gastric polyps: a retrospective analysis of 26,000 digestive endoscopies. Arq Gastroenterol 2007;44:14e Borch K, Skarsgard J, Franzen L, et al. Benign gastric polyps: morphological and functional origin. Dig Dis Sci 2003;48: Weston BR, Helper DJ, Rex DK. Positive predictive value of endoscopic features deemed typical of gastric fundic gland polyps. J Clin Gastroenterol 2003;36:399e Abraham SC, Nobukawa B, Giardiello FM, et al. Fundic gland polyps in familial adenomatous polyposis coli gene alteration. Am J Pathol 2000;157:747e Jalving M, Koornstra JJ, Wesseling J, et al. Increased risk of fundic gland polyps during long-term proton pump inhibitor therapy. Aliment Pharmacol Ther 2006;24:1341e braham SC, Nobukawa B, Giardiello FM, et al. Sporadic fundal gland polyps: common gastric polyps arising through activating mutations in the beta-catenin gene. Am J Pathol 2001;158:1005e Sekine S, Shibata T, Yamauchi Y, et al. Beat-catenin mutations in sporadic fundal gland polyps. Virchows Arch 2002;440:381e Burt R. Clinical management; gastric fundal gland polyps. Gastroenterology 2003;125:1462e Wu TT, Kornacki S, Rashid A, et al. Dysplasia and dysregulation of proliferation in foveolar and surface epithelia of fundic gland polyps from patients with familial adenomatous polyposis. Am J Surg Pathol 1998;22:293e Jalving M, Koornstra JJ, Gotz JM, et al. High-grade dysplasia in sporadic fundic gland polyps: a case report and review of the literature. Eur J Gastroenterol Hepatol 2003;15:1153e Stolte M, Vieth M, Ebert MP. High-grade dysplasia in sporadic fundic gland polyps: clinically relevant or not. Eur J Gastroenterol Hepatol 2003;15:1229e Stolte M. Clinical consequences of the endoscopic diagnosis of gastric polyps. Endoscopy 1995;27:32e Dickey W, Kenny BD, McConnell JB. Prevalence of fundic gland polyps in a western European population. J Clin Gastroenterol 1996;23:73e Sakai N, Tatsula M, Hirasawa R, et al. Low prevalence of Helicobacter pylori infection in patients with hamartomatous fundic polyps. Dig Dis Sci 1998;43:766e Shand AG, Taylor AC, Banerjee M, et al. Gastric fundic gland polyps in south-east Scotland: absence of adenomatous polyposis coli gene mutations and a strikingly low prevalence of Helicobacter pylori infection. J Gastroenterol Hepatol 2002;17:1161e Watanabe N, Seno H, Nakajima T, et al. Regression of fundic gland polyps following acquisition of Helicobacter pylori. Gut 2004;53: El-Zimaity HMT, Jackson FW, Graham DY. Fundic gland polyps developing during omeprazole therapy. Am J Gastroenterol 1997;92:1858e60. Gut 2010;59:1270e1276. doi: /gut
7 23. Choudhry U, Boyce HW Jr, Coppola D. Proton pump inhibitor-associated gastric polyps: A retrospective analysis of their frequency, and endoscopic, histologic, and ultrastructural characteristics. Am J Clin Pathol 1998;110:615e Declich P, Ferrara A, Galati F, et al. Do fundic gland polyps develop under long term omeprazole therapy? Am J Gastroenterol 1998;93: Declich P, Ambrosiani A, Bellone S, et al. Fundic gland polyps under omeprazole treatment. Am J Clin Pathol 1999;112:576e Vieth M, Stolte M. Fundic gland polyps are not induced by proton pump inhibitor therapy. Am J Clin Pathol 2001;116:716e Klinkenberg-Knol E, Nelis F, Dent J, et al. Long term omeprazole treatment in resistant gastroesophageal reflux disease: Efficacy, safety and influence on gastric mucosa. Gastroenterology 2000;118:661e Bianchi LK, Burke CA, Bennett AE, et al. Fundic gland dysplasia is common in familial adenomatous polyposis. Clin Gastroenterol Hepatol 2008;6:180e Abraham SC, Nobukawa B, Giardiello FM, et al. Fundic gland polyps in familial adenomatous polyposis: neoplasms with frequent somatic adenomatous polyposis coli gene alterations. Am J Pathol 2000;157:747e Declich P, Tavani E, Ferrara A, et al. Sporadic fundic gland polyps:clinicopathological features and associated diseases. Pol J Pathol 2005;56:131e Jung A, Vieth M, Maier O, et al. Fundic gland polyps (Elster s cysts) of the gastric mucosa. A marker for colorectal epithelial neoplasia? Pathol Res Pract 2002;198:731e Abraham SC, Singh VK, Yardley JH, et al. Hyperplastic polyps of the stomach: association with histological patterns of gastritis and gastric atrophy. Am J Surg Pathol 2001;25: Ohkusa T, Miwa H, Kumagai J, et al. Endoscopic, histological and serologic findings of gastric hyperplastic polyps after eradication of Helicobacter pylori: comparison between responder and non-responder cases. Digestion 2003;68:57e Ohkusa T, Takashimizu I, Fujiki K, et al. Disappearance of hyperplastic polyps in the stomach after eradication of Helicobacter pylori. A randomised, clinical trial. Ann Intern Med 1998;129:712e Ji F, Wang ZW, Ning JW, et al. Effect of drug treatment on hyperplastic polyps infected with Helicobacter pylori: a randomized, controlled trial. World J Gastroenterol 2006;12:1770e Ljubicic N,Banic M, Kujundzic M,et al. The effect of eradicating Helicobacter pylori infection on the course of adenomatous and hyperplastic gastric polyps. Eur J Gastroenterol Hepatol 1999;11:727e Ginsberg GG, Al-Kawas FH, Fleischer DE, et al. Gastric polyps; relationship of size and histology to cancer risk. Am J Gastroenterol 1996;91:714e Daibo M, Itabashi M, Hirota T. Malignant transformation of gastric hyperplastic polyps. Am J Gastroenterol 1987;82:1016e Rattan J, Arber N, Tiomny E, et al. Gastric polypoid lesions: an eight year study. Hepatogastroenterol 1993;40:107e Dirschmid K, Platz-Baudin C, Stolte M. Why is the hyperplastic polyp a marker for precancerous condition of the gastric mucosa. Virchows Arch 2006;448:80e Orlowska J, Pietrow D. Multifocal gastric carcinoma arising hyperplastic and adenomatous polyps. Am J Gastroenterol 1990;85:1629e Hizawa K, Fuchigami T, Iida M, et al. Possible neoplastic transformation within gastric hyperplastic polyp. Application of endoscopic polypectomy. Surg Endosc 1995;9:714e Zea Iriarte WL, Sekine I, Itsuno M, et al. Carcinomas in gastric hyperplastic polyps. A phenotypic study. Dig Dis Sci 1996;41:377e Orlawska J, Jarosz D, Pachlewski J, et al. Malignant transformation of benign epithelial polyps. Am J Gastroenterol 1995;90:2152e Cristallini E, Ascani S, Bolis G. Association between histologic type of polyp and carcinoma in the stomach. Gastrointesti Endosc 1992;38:481e Harju E. Gastric polyposis and malignancy. Br J Surg 1986;73:532e Al-Haddad M, Ward EM, Bouras EP, et al. Hyperplastic polyps of the gastric antrum in patients with gastrointestinal blood loss. Dig Dis Sci 2007;52:105e Yoshihara M, Sumii K, Haruma K, et al. Correlation of ratio of serum pepsinogen I and II with prevalence of gastric cancer and adenoma in Japanese subjects. Am J Gastroenterol 1998;93:1090e Saito K, Arai K, Mori M, et al. Effect of Helicobacter pylori eradication on malignant transformation of gastric adenoma. Gastrointest Endosc 2000;52:27e Tomasulo J. Gastric polyps. Histologic types and their relationship to gastric carcinoma. Cancer 1971;27:1346e Nakamura T, Nakano G. Histological classification and malignant change in gastric polyps. J Clin Pathol 1985;38:754e Schmitz JM, Stolte M. Gastric polyps as precancerous lesions. Gastrointest Endosc Clin N Am 1997;7:29e Lanza FL, Graham DY, Nelson, et al. Endoscopic upper gastrointestinal polypectomy. Report of 73 polypectomies in 63 patients. Am J Gastroenterol 1981;75:345e Giardiello FM, Welsh SB, Hamilton SR. Increased risk of cancer in the Peutz- Jeghers syndrome. N Engl J Med 1987;316:1511e Debrinsky HS, Spigelman AD, Hatfield A, et al. Upper intestinal surveillance in familial adenomatous polyposis. Eur J Cancer 1995;31: Burt RW. Hereditary polyposis syndromes and inheritance of adenomatous polyps. Semin Gastrointest Dis 1992;3: Nakamura S, Matsumoto T, Kobori Y, et al. Impact of Helicobacter pylori infection and mucosal atrophy on gastric lesions in patients with familial adenomatous polyposis. Gut 2002;51:485e Howe JR, Mitros FA, Summers RW. The risk of gastrointestinal carcinoma in familial juvenile polyposis. Ann Surg Oncol 1998;5:751e Hizawa K, Iida M, Yao T, et al. Juvenile polyposis of the stomach: clinicopathological features and its malignant potential. J Clin Pathol 1997;50:771e Winkler A, Hinterleitner TA, Hogenauer C, et al. Juvenile polyposis of the stomach causing recurrent upper gastrointestinal bleeding. Eur J Gastroenterol Hepatol 2007;19:87e Hirasaki S, Matsubara M, Ikeda F, et al. Gastric inflammatory fibroid polyp treated with Helicobacter pylori eradication therapy. Intern Med 2007;46:855e Ramage JK, Davies AHG, Ardill J, et al; on behalf of UKNETwork for neuroendocrine tumours. Guidelines for the management of gastroenteropancreatic neuroen-docrine (including carcinoid) tumours. Gut 2005;54(Suppl 4):iv1e Burkitt MD, Pritchard DM. Review article: pathogenesis and management of gastric carcinoid tumours. Aliment Pharmacol Ther 2006;24:1305e Modlin IM, Lye KD, Kidd M. Carcinoid tumors of the stomach. Surg Oncol 2003;12:153e Anon. Consensus meeting for the management of gastrointestinal stromal tumors: report of the GIST Consensus Conference of 20e21 March Ann Oncol 2005;16:566e National Institute for Clinical Excellence. NICE Technology Appraisal Guidance 86. Imatinib for the treatment of unresectable and/or metastatic gastro-intestinal stromal tumours. London: National Institute for Clinical Excellence, Mueldorfer SM, Stolte M, Martus P, et al. Diagnostic accuracy of forceps biopsy versus polypectomy for gastric polyps: a prospective multicentre study. Gut 2002;50:465e American Society of Gastrointestinal Endoscopy. The role of endoscopy in the surveillance of premalignant condition of the upper gastrointestinal tract. Gastrointest Endosc 1998;48:663e Seifert E, Elster K. Gastric polypectomy. Am J Gastroenterol 1975;63:451e Ottenjann R, Kunert H, Seib HJ. Is gastroscopic polypectomy a diagnostic necessity? Results of a prospective study. Dtsch Med Wochenschr 1984;109:443e Chua CL. Gastric polyps: the case for polypectomy and endoscopic surveillance. J R Coll Surg Edinb 1990;35:163e Szaloki T, Toth V, Tiszlavicz L, et al. Flat gastric polyps: results of forceps biopsy, endoscopic mucosal resection, and long-term follow-up. Scand J Gastroenterol 2006;41:1105e Ono H, Kondo H, Gotoda T, et al. Endoscopic mucosal resection for treatment of early gastric cancer. Gut 2001;48:225e9. APPENDIX 1 Members of the Gastric Polyp Guideline Consensus Panel Meeting, held 22 November 2009, St Mary s Hospital, London Dr Yeng Ang Professor Emad El-Omar Dr Andrew F Goddard (co-chair) Dr Robert Goldin Dr Philip Hardo Dr Robert PH Logan Professor Kenneth McColl Professor D Mark Pritchard Dr Tony Tham Dr Marjorie M Walker (co-chair) 1276 Gut 2010;59:1270e1276. doi: /gut
Gastric Polyps. Bible class
 Gastric Polyps Bible class 29.08.2018 Starting my training in gastroenterology, some decades ago, my first chief always told me that colonoscopy may seem technically more challenging but gastroscopy has
Gastric Polyps Bible class 29.08.2018 Starting my training in gastroenterology, some decades ago, my first chief always told me that colonoscopy may seem technically more challenging but gastroscopy has
Colonic Polyp. Najmeh Aletaha. MD
 Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Effect of Helicobacter pylori eradication on the regression of gastric polyps in National Cancer Screening Program
 ORIGINAL ARTICLE Korean J Intern Med 2018;33:506-511 Effect of Helicobacter pylori eradication on the regression of gastric polyps in National Cancer Screening Program Su Youn Nam 1,2, Bum Joon Park 2,
ORIGINAL ARTICLE Korean J Intern Med 2018;33:506-511 Effect of Helicobacter pylori eradication on the regression of gastric polyps in National Cancer Screening Program Su Youn Nam 1,2, Bum Joon Park 2,
Hyperplastische Polyps Innocent bystanders?
 Hyperplastische Polyps Innocent bystanders?? K. Geboes P th l i h O tl dk d Pathologische Ontleedkunde, KULeuven Content Historical Classification Relation Hyperplastic polyps carcinoma The concept cept
Hyperplastische Polyps Innocent bystanders?? K. Geboes P th l i h O tl dk d Pathologische Ontleedkunde, KULeuven Content Historical Classification Relation Hyperplastic polyps carcinoma The concept cept
Surveying the Colon; Polyps and Advances in Polypectomy
 Surveying the Colon; Polyps and Advances in Polypectomy Educational Objectives Identify classifications of polyps Describe several types of polyps Verbalize rationale for polypectomy Identify risk factors
Surveying the Colon; Polyps and Advances in Polypectomy Educational Objectives Identify classifications of polyps Describe several types of polyps Verbalize rationale for polypectomy Identify risk factors
General Comments. Hyperplastic polyps
 Gastric Lumps and Bumps: A tale of two polyps Henry D. Appelman, M.D. Department of Pathology University of Michigan appelman@umich.edu General Comments The stomach is far less rich in polyps than is the
Gastric Lumps and Bumps: A tale of two polyps Henry D. Appelman, M.D. Department of Pathology University of Michigan appelman@umich.edu General Comments The stomach is far less rich in polyps than is the
Hereditary Gastric Cancer
 Hereditary Gastric Cancer Dr Bastiaan de Boer Consultant Pathologist Department of Anatomical Pathology PathWest Laboratory Medicine, QE II Medical Centre Clinical Associate Professor School of Pathology
Hereditary Gastric Cancer Dr Bastiaan de Boer Consultant Pathologist Department of Anatomical Pathology PathWest Laboratory Medicine, QE II Medical Centre Clinical Associate Professor School of Pathology
Increased risk of fundic gland polyps during long-term proton pump inhibitor therapy
 Alimentary Pharmacology & Therapeutics Increased risk of fundic gland polyps during long-term proton pump inhibitor therapy M. JALVING*,,J.J.KOORNSTRA*,J.WESSELINGà, H.M.BOEZEN,S.DEJONG & J. H. KLEIBEUKER*
Alimentary Pharmacology & Therapeutics Increased risk of fundic gland polyps during long-term proton pump inhibitor therapy M. JALVING*,,J.J.KOORNSTRA*,J.WESSELINGà, H.M.BOEZEN,S.DEJONG & J. H. KLEIBEUKER*
The Clinicopathological Features of Gastric Hyperplastic Polyps with Neoplastic Transformations: A Suggestion of Indication for
 Gut and Liver, Vol. 3, No. 4, December 2009, pp. 271-275 original article The Clinicopathological Features of Gastric Hyperplastic Polyps with Neoplastic Transformations: A Suggestion of Indication for
Gut and Liver, Vol. 3, No. 4, December 2009, pp. 271-275 original article The Clinicopathological Features of Gastric Hyperplastic Polyps with Neoplastic Transformations: A Suggestion of Indication for
Gastrointestinal pathology 2018 lecture 4. Dr Heyam Awad FRCPath
 Gastrointestinal pathology 2018 lecture 4 Dr Heyam Awad FRCPath Topics to be covered Peptic ulcer disease Hiatal hernia Gastric neoplasms Peptic ulcer disease (PUD)= chronic gastric ulcer Causes H pylori
Gastrointestinal pathology 2018 lecture 4 Dr Heyam Awad FRCPath Topics to be covered Peptic ulcer disease Hiatal hernia Gastric neoplasms Peptic ulcer disease (PUD)= chronic gastric ulcer Causes H pylori
Familial Adenomatous Polyposis
 Familial Adenomatous Polyposis 1 in 10,000 incidence 100 s to 1000 s of colonic adenomas by teens Cancer risk: colon, gastric, duodenum (periampulla), small bowel, pancreas, papillary thyroid, childhood
Familial Adenomatous Polyposis 1 in 10,000 incidence 100 s to 1000 s of colonic adenomas by teens Cancer risk: colon, gastric, duodenum (periampulla), small bowel, pancreas, papillary thyroid, childhood
colorectal cancer Colorectal cancer hereditary sporadic Familial 1/12/2018
 colorectal cancer Adenocarcinoma of the colon and rectum is the third most common site of new cancer cases and deaths in men (following prostate and lung or bronchus cancer) and women (following breast
colorectal cancer Adenocarcinoma of the colon and rectum is the third most common site of new cancer cases and deaths in men (following prostate and lung or bronchus cancer) and women (following breast
Original Article Plugs clog the glandular outlets in fundic gland polyps
 Int J Clin Exp Pathol 2010;3(1):69-74 www.ijcep.com/ijcep904010 Original Article Plugs clog the glandular outlets in fundic gland polyps Carlos A Rubio Gastrointestinal and Liver Pathology Research Laboratory,
Int J Clin Exp Pathol 2010;3(1):69-74 www.ijcep.com/ijcep904010 Original Article Plugs clog the glandular outlets in fundic gland polyps Carlos A Rubio Gastrointestinal and Liver Pathology Research Laboratory,
Principles of diagnosis, work-up and therapy The Gastroenterologist s role
 Principles of diagnosis, work-up and therapy The Gastroenterologist s role Dr. Christos G. Toumpanakis MD PhD FRCP Consultant in Gastroenterology/Neuroendocrine Tumours Hon. Senior Lecturer University
Principles of diagnosis, work-up and therapy The Gastroenterologist s role Dr. Christos G. Toumpanakis MD PhD FRCP Consultant in Gastroenterology/Neuroendocrine Tumours Hon. Senior Lecturer University
Endoscopic Corner CASE 1. Sirimontaporn N Klaikaew N Imraporn B Rerknimitr R
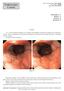 Endoscopic Corner Sirimontaporn N, et al. THAI J GASTROENTEROL 2010 Vol. 11 No. 3 Sept. - Dec. 2010 171 Sirimontaporn N Klaikaew N Imraporn B Rerknimitr R CASE 1 A 47- year-old female presented to the
Endoscopic Corner Sirimontaporn N, et al. THAI J GASTROENTEROL 2010 Vol. 11 No. 3 Sept. - Dec. 2010 171 Sirimontaporn N Klaikaew N Imraporn B Rerknimitr R CASE 1 A 47- year-old female presented to the
Fundic gland polyps, initially described in association with
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:849 854 No Association Between Gastric Fundic Gland Polyps and Gastrointestinal Neoplasia in a Study of Over 100,000 Patients ROBERT M. GENTA,*, CHRISTOPHER
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:849 854 No Association Between Gastric Fundic Gland Polyps and Gastrointestinal Neoplasia in a Study of Over 100,000 Patients ROBERT M. GENTA,*, CHRISTOPHER
LIST OF ABBREVIATIONS
 Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Fundic Gland Polyposis in Patients Without Familial Adenomatosis Coli: Its Incidence and Clinical Features
 GASTROENTEROLOGY 1984;86;1437-42 ALIMENTARY TRACT Fundic Gland Polyposis in Patients Without Familial Adenomatosis Coli: Its Incidence and Clinical Features MITSUO IIDA, TSUNEYOSHI YAO, HIDENOBU WATANABE,
GASTROENTEROLOGY 1984;86;1437-42 ALIMENTARY TRACT Fundic Gland Polyposis in Patients Without Familial Adenomatosis Coli: Its Incidence and Clinical Features MITSUO IIDA, TSUNEYOSHI YAO, HIDENOBU WATANABE,
Pathology reports, related operative reports and consult letters must be provided with a request for assessment.
 Page 1 of 6 Polyposis Syndromes Inherited risk for colorectal cancer is associated with a number of polyposis syndromes (genes), some of which are well-defined and others are less common. Identification
Page 1 of 6 Polyposis Syndromes Inherited risk for colorectal cancer is associated with a number of polyposis syndromes (genes), some of which are well-defined and others are less common. Identification
Familial and Hereditary Colon Cancer
 Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY
 OPEN ACCESS TEXTBOOK OF GENERAL SURGERY COLORECTAL POLYPS P Goldberg POLYP A polyp is a localised elevated lesion arising from a epithelial surface. If it has a stalk it is called a pedunculated polyp
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY COLORECTAL POLYPS P Goldberg POLYP A polyp is a localised elevated lesion arising from a epithelial surface. If it has a stalk it is called a pedunculated polyp
Classification of polyposis syndromes two major groups. Adenomatous polyposis syndromes. Hamartomatous polyposis syndromes
 Hereditary polyposis syndromes Classification of polyposis syndromes two major groups adenomatous and non-adenomatous polyposis syndromes Adenomatous polyposis syndromes Familial adenomatous polyposis(fap)
Hereditary polyposis syndromes Classification of polyposis syndromes two major groups adenomatous and non-adenomatous polyposis syndromes Adenomatous polyposis syndromes Familial adenomatous polyposis(fap)
Summary. Cezary ŁozińskiABDF, Witold KyclerABCDEF. Rep Pract Oncol Radiother, 2007; 12(4):
 Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
FINAL HISTOLOGICAL DIAGNOSIS: Villo-adenomatous polyp with in-situ-carcinomatous foci (involving both adenomatous and villous component).
 SOLITARY VILLO ADENOMATOUS POLYP WITH CARCINOMATOUS CHANGES RECTUM: A Divvya B 1, M. Valluvan 2, Rehana Tippoo 3, P. Viswanathan 4, R. Baskaran 5 HOW TO CITE THIS ARTICLE: Divvya B, M. Valluvan, Rehana
SOLITARY VILLO ADENOMATOUS POLYP WITH CARCINOMATOUS CHANGES RECTUM: A Divvya B 1, M. Valluvan 2, Rehana Tippoo 3, P. Viswanathan 4, R. Baskaran 5 HOW TO CITE THIS ARTICLE: Divvya B, M. Valluvan, Rehana
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS. Family Health Clinical Genetics. Clinical Genetics department
 GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
Familial and Hereditary Colon Cancer
 Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci. Colon polyps. Colorectal cancer
 Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Colon polyps Colorectal cancer Harrison s Principles of Internal Medicine 18 Ed. 2012 Colorectal cancer 70% Colorectal cancer CRC and colon
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Colon polyps Colorectal cancer Harrison s Principles of Internal Medicine 18 Ed. 2012 Colorectal cancer 70% Colorectal cancer CRC and colon
ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID
 ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID Manoop S. Bhutani, MD, FASGE, FACG, FACP, AGAF, Doctor Honoris Causa Professor of Medicine Eminent Scientist of the Year 2008, World
ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID Manoop S. Bhutani, MD, FASGE, FACG, FACP, AGAF, Doctor Honoris Causa Professor of Medicine Eminent Scientist of the Year 2008, World
Colorectal Neoplasia. Dr. Smita Devani MBChB, MRCP. Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi
 Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions. South Island Cancer Nurses Network September 2013
 For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
General Session 7: Controversies in Screening and Surveillance in Colorectal Cancer
 General Session 7: Controversies in Screening and Surveillance in Colorectal Cancer Complexities of Pathological Assessment: Serrated Polyps/Adenomas Carolyn Compton, MD, PhD Professor of Life Sciences,
General Session 7: Controversies in Screening and Surveillance in Colorectal Cancer Complexities of Pathological Assessment: Serrated Polyps/Adenomas Carolyn Compton, MD, PhD Professor of Life Sciences,
Gastroenterology Tutorial
 Gastroenterology Tutorial Gastritis Poorly defined term that refers to inflammation of the stomach. Infection with H. pylori is the most common cause of gastritis. Most patients remain asymptomatic Some
Gastroenterology Tutorial Gastritis Poorly defined term that refers to inflammation of the stomach. Infection with H. pylori is the most common cause of gastritis. Most patients remain asymptomatic Some
YES NO UNKNOWN. Stage I: Rule-Out Dashboard ACTIONABILITY PENETRANCE SIGNIFICANCE/BURDEN OF DISEASE NEXT STEPS. YES ( 1 of above)
 Stage I: Rule-Out Dashboard GENE/GENE PANEL: SMAD4, BMPR1A DISORDER: Juvenile Polyposis Syndrome HGNC ID: 6670, 1076 OMIM ID: 174900, 175050 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource,
Stage I: Rule-Out Dashboard GENE/GENE PANEL: SMAD4, BMPR1A DISORDER: Juvenile Polyposis Syndrome HGNC ID: 6670, 1076 OMIM ID: 174900, 175050 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource,
Imaging Evaluation of Polyps. CT Colonography: Sessile Adenoma. Polyps, DALMs & Megacolon Objectives
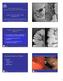 Polyps, DALMs & Megacolon: Pathology and Imaging of the Colon and Rectum Angela D. Levy and Leslie H. Sobin Washington, DC Drs. Levy and Sobin have indicated that they have no relationships which, in the
Polyps, DALMs & Megacolon: Pathology and Imaging of the Colon and Rectum Angela D. Levy and Leslie H. Sobin Washington, DC Drs. Levy and Sobin have indicated that they have no relationships which, in the
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines
 Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
27
 26 27 28 29 30 31 32 33 34 35 Diagnosis:? Diagnosis: Juvenile Polyposis with BMPR1A Mutation 36 Juvenile Polyposis Syndrome Rare Autosomal Dominant Disorder with Multiple Juvenile Polyps in GI Tract Juvenile
26 27 28 29 30 31 32 33 34 35 Diagnosis:? Diagnosis: Juvenile Polyposis with BMPR1A Mutation 36 Juvenile Polyposis Syndrome Rare Autosomal Dominant Disorder with Multiple Juvenile Polyps in GI Tract Juvenile
GI Polyp syndromes in children. Screening and surveillance, surgery.
 Dr Warren Hyer Consultant Paediatric Gastroenterologist St Mark s Hospital, UK GI Polyp syndromes in children Screening and surveillance, surgery. No conflict of interests to declare Objectives Understand
Dr Warren Hyer Consultant Paediatric Gastroenterologist St Mark s Hospital, UK GI Polyp syndromes in children Screening and surveillance, surgery. No conflict of interests to declare Objectives Understand
Polypoid lesions of the gastrointestinal tract
 Polypoid lesions of the gastrointestinal tract Professor Neil A Shepherd Gloucester & Cheltenham, UK 27 th IAP-AD Congress 2 nd Emirates Surgical Pathology Conference Dubai, 26 November 2015 Polypoid lesions
Polypoid lesions of the gastrointestinal tract Professor Neil A Shepherd Gloucester & Cheltenham, UK 27 th IAP-AD Congress 2 nd Emirates Surgical Pathology Conference Dubai, 26 November 2015 Polypoid lesions
Signet-ring cell carcinoma arising from a fundic gland polyp in the stomach
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i47.18044 World J Gastroenterol 2014 December 21; 20(47): 18044-18047 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i47.18044 World J Gastroenterol 2014 December 21; 20(47): 18044-18047 ISSN 1007-9327
Original Report. Carcinoid Tumors of the Stomach: A Clinical and Radiographic Study
 Aaron J. Binstock 1 C. Daniel Johnson 1 David H. Stephens 1 Ricardo V. Lloyd 2 Joel G. Fletcher 1 Received July 25, 2000; accepted after revision September 29, 2000. 1 Department of Radiology, Mayo Clinic,
Aaron J. Binstock 1 C. Daniel Johnson 1 David H. Stephens 1 Ricardo V. Lloyd 2 Joel G. Fletcher 1 Received July 25, 2000; accepted after revision September 29, 2000. 1 Department of Radiology, Mayo Clinic,
Carcinoid Tumors: The Beginning and End. Surgical Oncology Update 2011 Chris Baliski MD, FRCS BC Cancer Agency, CSI October 21, 2011
 Carcinoid Tumors: The Beginning and End Surgical Oncology Update 2011 Chris Baliski MD, FRCS BC Cancer Agency, CSI October 21, 2011 1 st described by Oberndofer(1907) Karzinoide = cancer like Arise from
Carcinoid Tumors: The Beginning and End Surgical Oncology Update 2011 Chris Baliski MD, FRCS BC Cancer Agency, CSI October 21, 2011 1 st described by Oberndofer(1907) Karzinoide = cancer like Arise from
Update on the pathological classification of gastritis. Hala El-Zimaity, M.D. M.S. Epidemiology McMaster University Hamilton, Ontario Canada
 Update on the pathological classification of gastritis Hala El-Zimaity, M.D. M.S. Epidemiology McMaster University Hamilton, Ontario Canada CLASSIFICATION GASTRITIS GASTROPATHY 1. Acute 2. Chronic 3. Uncommon
Update on the pathological classification of gastritis Hala El-Zimaity, M.D. M.S. Epidemiology McMaster University Hamilton, Ontario Canada CLASSIFICATION GASTRITIS GASTROPATHY 1. Acute 2. Chronic 3. Uncommon
Proton Pump Inhibitor Induction of Gastric Cobblestone-like Lesions in the Stomach
 doi: 10.2169/internalmedicine.7964-16 Intern Med Advance Publication http://internmed.jp ORIGINAL ARTICLE Proton Pump Inhibitor Induction of Gastric Cobblestone-like Lesions in the Stomach Kosuke Takahari
doi: 10.2169/internalmedicine.7964-16 Intern Med Advance Publication http://internmed.jp ORIGINAL ARTICLE Proton Pump Inhibitor Induction of Gastric Cobblestone-like Lesions in the Stomach Kosuke Takahari
Management of pt1 polyps. Maria Pellise
 Management of pt1 polyps Maria Pellise Early colorectal cancer Malignant polyp Screening programmes SM Invasive adenocar cinoma Advances in diagnostic & therapeutic endoscopy pt1 polyps 0.75 5.6% of large-bowel
Management of pt1 polyps Maria Pellise Early colorectal cancer Malignant polyp Screening programmes SM Invasive adenocar cinoma Advances in diagnostic & therapeutic endoscopy pt1 polyps 0.75 5.6% of large-bowel
Colonic polyps and colon cancer. Andrew Macpherson Director of Gastroentology University of Bern
 Colonic polyps and colon cancer Andrew Macpherson Director of Gastroentology University of Bern Improtance of the problem of colon cancers - Epidemiology Lifetime risk 5% Incidence/10 5 /annum (US Detroit
Colonic polyps and colon cancer Andrew Macpherson Director of Gastroentology University of Bern Improtance of the problem of colon cancers - Epidemiology Lifetime risk 5% Incidence/10 5 /annum (US Detroit
Subepithelial Lesions of the Gut: When Should I Worry?
 Subepithelial Lesions of the Gut: When Should I Worry? President, ASGE Chairman, GI & Hepatology Scottsdale, AZ Faigel.douglas@mayo.edu Case 55 yo male with reflux EGD for Barrett s Screening SET, mucosal
Subepithelial Lesions of the Gut: When Should I Worry? President, ASGE Chairman, GI & Hepatology Scottsdale, AZ Faigel.douglas@mayo.edu Case 55 yo male with reflux EGD for Barrett s Screening SET, mucosal
Changing Trends in Gastric Polyps
 Revista de InvestigaciÓn ClÍnica Contents available at PubMed www.clinicalandtranslationalinvestigation.com PERMANYER Rev Inves Clin. 2018;70:40-45 ORIGINAL ARTICLE Changing Trends in Gastric Polyps Magali
Revista de InvestigaciÓn ClÍnica Contents available at PubMed www.clinicalandtranslationalinvestigation.com PERMANYER Rev Inves Clin. 2018;70:40-45 ORIGINAL ARTICLE Changing Trends in Gastric Polyps Magali
ACG Clinical Guideline: Genetic Testing and Management of Hereditary Gastrointestinal Cancer Syndromes
 ACG Clinical Guideline: Genetic Testing and Management of Hereditary Gastrointestinal Cancer Syndromes Sapna Syngal, MD, MPH, FACG, 1,2,3 Randall E. Brand, MD, FACG, 4 James M. Church, MD, FACG, 5,6,7
ACG Clinical Guideline: Genetic Testing and Management of Hereditary Gastrointestinal Cancer Syndromes Sapna Syngal, MD, MPH, FACG, 1,2,3 Randall E. Brand, MD, FACG, 4 James M. Church, MD, FACG, 5,6,7
Endoscopic techniques for surveillance and treatment of FAP
 Endoscopic techniques for surveillance and treatment of FAP Evelien Dekker MD PhD Department of Gastroenterology & Hepatology Academic Medical Center Amsterdam The Netherlands FAP: endoscopic surveillance
Endoscopic techniques for surveillance and treatment of FAP Evelien Dekker MD PhD Department of Gastroenterology & Hepatology Academic Medical Center Amsterdam The Netherlands FAP: endoscopic surveillance
5/2/2018. Low Grade Dysplasia of GI Tract. High Grade Dysplasia of GI Tract. Dysplasia in Gastrointestinal Tract: Practical Pearls and Issues
 Dysplasia in Gastrointestinal Tract: Practical Pearls and Issues Arief Suriawinata, M.D. Professor of Pathology and Laboratory Medicine Geisel School of Medicine at Dartmouth Department of Pathology and
Dysplasia in Gastrointestinal Tract: Practical Pearls and Issues Arief Suriawinata, M.D. Professor of Pathology and Laboratory Medicine Geisel School of Medicine at Dartmouth Department of Pathology and
Dysplasia 4/19/2017. How do I practice Chromoendoscopy for Surveillance of Colitis? SCENIC: Polypoid Dysplasia in UC. Background
 SCENIC: Polypoid in UC Definition How do I practice for Surveillance of Colitis? Themos Dassopoulos, M.D. Director, BSW Center for IBD Themistocles.Dassopoulos@BSWHealth.org Tel: 469-800-7189 Cell: 314-686-2623
SCENIC: Polypoid in UC Definition How do I practice for Surveillance of Colitis? Themos Dassopoulos, M.D. Director, BSW Center for IBD Themistocles.Dassopoulos@BSWHealth.org Tel: 469-800-7189 Cell: 314-686-2623
Barrett s Esophagus. Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI
 Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Large Colorectal Adenomas An Approach to Pathologic Evaluation
 Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
Association of Helicobacter pylori infection with Atrophic gastritis in patients with Dyspepsia
 ADVANCES IN BIORESEARCH Adv. Biores., Vol 8 [3] May 2017: 137-141 2017 Society of Education, India Print ISSN 0976-4585; Online ISSN 2277-1573 Journal s URL:http://www.soeagra.com/abr.html CODEN: ABRDC3
ADVANCES IN BIORESEARCH Adv. Biores., Vol 8 [3] May 2017: 137-141 2017 Society of Education, India Print ISSN 0976-4585; Online ISSN 2277-1573 Journal s URL:http://www.soeagra.com/abr.html CODEN: ABRDC3
Bowel obstruction and tumors
 Bowel obstruction and tumors Intestinal Obstruction Obstruction of the GI tract may occur at any level, but the small intestine is most often involved because of its relatively narrow lumen. Causes: Hernias
Bowel obstruction and tumors Intestinal Obstruction Obstruction of the GI tract may occur at any level, but the small intestine is most often involved because of its relatively narrow lumen. Causes: Hernias
Unexpected Findings at Endoscopy
 The Endoscopic Incidentaloma: What to Tell Your Patient t with Unexpected Endoscopic Findings: Gastric Intestinal Metaplasia, Silent Ileitis, Carcinoid David Greenwald, MD Montefiore Medical Center Albert
The Endoscopic Incidentaloma: What to Tell Your Patient t with Unexpected Endoscopic Findings: Gastric Intestinal Metaplasia, Silent Ileitis, Carcinoid David Greenwald, MD Montefiore Medical Center Albert
1. Esophageal diverticulum located above the upper esophageal sphincter is called
 Test Bank for Robbins Basic Pathology 9th Edition by Kumar Link full download: http://testbankair.com/download/test-bank-for-robbins-basic-pathology-9thedition-by-kumar/ Chapter 14: Oral Cavity and Gastrointestinal
Test Bank for Robbins Basic Pathology 9th Edition by Kumar Link full download: http://testbankair.com/download/test-bank-for-robbins-basic-pathology-9thedition-by-kumar/ Chapter 14: Oral Cavity and Gastrointestinal
Endoscopic Corner CASE 1. Kimtrakool S Aniwan S Linlawan S Muangpaisarn P Sallapant S Rerknimitr R
 170 Endoscopic Corner Kimtrakool S Aniwan S Linlawan S Muangpaisarn P Sallapant S Rerknimitr R CASE 1 A 54-year-old woman underwent a colorectal cancer screening. Her fecal immunochemical test was positive.
170 Endoscopic Corner Kimtrakool S Aniwan S Linlawan S Muangpaisarn P Sallapant S Rerknimitr R CASE 1 A 54-year-old woman underwent a colorectal cancer screening. Her fecal immunochemical test was positive.
Rare GI Malignancies
 Rare GI Malignancies Jordan Karlitz, MD Associate Professor of Medicine, Division of Gastroenterology Director, Hereditary GI Cancer and Genetics Program Tulane University School of Medicine Outline Gastrointestinal
Rare GI Malignancies Jordan Karlitz, MD Associate Professor of Medicine, Division of Gastroenterology Director, Hereditary GI Cancer and Genetics Program Tulane University School of Medicine Outline Gastrointestinal
GI EMERGENCIES Acute Abdominal Pain
 GI EMERGENCIES Acute Abdominal Pain Marcia Cruz-Correa, MD, PhD, AGAF. FASGE Associate Professor of Medicine, Biochemistry, Surgery Director Translational Research University of Puerto Rico Comprehensive
GI EMERGENCIES Acute Abdominal Pain Marcia Cruz-Correa, MD, PhD, AGAF. FASGE Associate Professor of Medicine, Biochemistry, Surgery Director Translational Research University of Puerto Rico Comprehensive
COLON AND RECTUM SOLID TUMOR RULES ABSTRACTORS TRAINING
 COLON AND RECTUM SOLID TUMOR RULES ABSTRACTORS TRAINING COLON AND RECTUM SOLID TUMOR RULES Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent Terms Terms that are NOT Equivalent
COLON AND RECTUM SOLID TUMOR RULES ABSTRACTORS TRAINING COLON AND RECTUM SOLID TUMOR RULES Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent Terms Terms that are NOT Equivalent
R ecommendations for diagnosis and treatment of epithelial
 465 ORIGINAL ARTICLE Diagnostic accuracy of forceps biopsy versus polypectomy for gastric polyps: a prospective multicentre study S M Muehldorfer, M Stolte, P Martus, E G Hahn, C Ell, for the Multicenter
465 ORIGINAL ARTICLE Diagnostic accuracy of forceps biopsy versus polypectomy for gastric polyps: a prospective multicentre study S M Muehldorfer, M Stolte, P Martus, E G Hahn, C Ell, for the Multicenter
Pathology perspective of colonic polyposis syndromes
 Pathology perspective of colonic polyposis syndromes When are too many polyps too many? David Schaeffer Head and Consultant Pathologist, Department of Pathology and Laboratory Medicine, Vancouver General
Pathology perspective of colonic polyposis syndromes When are too many polyps too many? David Schaeffer Head and Consultant Pathologist, Department of Pathology and Laboratory Medicine, Vancouver General
Expert panel observations
 Expert panel observations Professor Neil A Shepherd Gloucester and Cheltenham, UK Gloucestershire Cellular Pathology Laboratory Three big issues in BCSP pathology serrated pathology & what do we do about
Expert panel observations Professor Neil A Shepherd Gloucester and Cheltenham, UK Gloucestershire Cellular Pathology Laboratory Three big issues in BCSP pathology serrated pathology & what do we do about
The Paris classification of colonic lesions
 The Paris classification of colonic lesions Training to improve the interobserver agreement among international experts Sascha van Doorn, MD, PhD-student in CRC-reserach group of Evelien Dekker Introduction
The Paris classification of colonic lesions Training to improve the interobserver agreement among international experts Sascha van Doorn, MD, PhD-student in CRC-reserach group of Evelien Dekker Introduction
Colon and Rectum: 2018 Solid Tumor Rules
 2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING Colon and Rectum: 2018 Solid Tumor Rules 1 Colon and Rectum Solid Tumor Rules Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent
2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING Colon and Rectum: 2018 Solid Tumor Rules 1 Colon and Rectum Solid Tumor Rules Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent
Polyps in general: is a descriptive term of forming a mass that is exophytic & polypoid.
 ميحرلا نمحرلا هللا مسب Gastric Tumors: Benign tumours & tumor-like conditions: -Mucosal: Gastric polyps (they are uncommon) -Mesenchymal tumours: Leiomyoma & Lipoma (can occur anywhere in the body) Malignant:
ميحرلا نمحرلا هللا مسب Gastric Tumors: Benign tumours & tumor-like conditions: -Mucosal: Gastric polyps (they are uncommon) -Mesenchymal tumours: Leiomyoma & Lipoma (can occur anywhere in the body) Malignant:
Risk of Colorectal Cancer (CRC) Hereditary Syndromes in GI Cancer GENETIC MALPRACTICE
 Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy
 Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy Authors: Dr Gordon Armstrong, Dr Sue Pritchard 1. General Comments 1.1 Cancer reporting: Biopsies
Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy Authors: Dr Gordon Armstrong, Dr Sue Pritchard 1. General Comments 1.1 Cancer reporting: Biopsies
Screening & Surveillance Guidelines
 Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Helicobacter pylori Improved Detection of Helicobacter pylori
 DOI:http://dx.doi.org/10.7314/APJCP.2016.17.4.2099 RESEARCH ARTICLE Improved Detection of Helicobacter pylori Infection and Premalignant Gastric Mucosa Using Conventional White Light Source Gastroscopy
DOI:http://dx.doi.org/10.7314/APJCP.2016.17.4.2099 RESEARCH ARTICLE Improved Detection of Helicobacter pylori Infection and Premalignant Gastric Mucosa Using Conventional White Light Source Gastroscopy
Duodenal adenomas Management. Dr Stratis Alexandridis Consultant Gastroenterologist BRI
 Duodenal adenomas Management Dr Stratis Alexandridis Consultant Gastroenterologist BRI Introduction Ampullary and non ampullary polyps of the duodenum are diagnosed within and outside genetic syndromes.
Duodenal adenomas Management Dr Stratis Alexandridis Consultant Gastroenterologist BRI Introduction Ampullary and non ampullary polyps of the duodenum are diagnosed within and outside genetic syndromes.
Neoplastic Colon Polyps. Joyce Au SUNY Downstate Grand Rounds, October 18, 2012
 Neoplastic Colon Polyps Joyce Au SUNY Downstate Grand Rounds, October 18, 2012 CASE 55M with Hepatitis C, COPD (FEV1=45%), s/p vasectomy, knee surgery Meds: albuterol, flunisolide, mometasone, tiotropium
Neoplastic Colon Polyps Joyce Au SUNY Downstate Grand Rounds, October 18, 2012 CASE 55M with Hepatitis C, COPD (FEV1=45%), s/p vasectomy, knee surgery Meds: albuterol, flunisolide, mometasone, tiotropium
Page 1. Is the Risk This High? Dysplasia in the IBD Patient. Dysplasia in the Non IBD Patient. Increased Risk of CRC in Ulcerative Colitis
 Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
malignant polyp Daily Challenges in Digestive Endoscopy for Endoscopists and Endoscopy Nurses BSGIE Annual Meeting 18/09/2014 Mechelen
 Plan Incidental finding of a malignant polyp 1. What is a polyp malignant? 2. Role of the pathologist and the endoscopist 3. Quantitative and qualitative risk assessment 4. How to decide what to do? Hubert
Plan Incidental finding of a malignant polyp 1. What is a polyp malignant? 2. Role of the pathologist and the endoscopist 3. Quantitative and qualitative risk assessment 4. How to decide what to do? Hubert
CLINICAL CASE OF ACUTE BLEEDING FROM ADENOMATOUS GASTRIC POLYP AT THE TIME OF SINGLE INTAKE OF HIGH DOSE ASPIRIN
 Trakia Journal of Sciences, Vol. 8, No 4, pp 27-33, 2010 Copyright 2010 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) ISSN 1313-3551 (online) Original Contribution
Trakia Journal of Sciences, Vol. 8, No 4, pp 27-33, 2010 Copyright 2010 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) ISSN 1313-3551 (online) Original Contribution
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/48400
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/48400
The surface mucous cells and the cardiac and pyloric glands secrete mucus which protects the stomach from self-digestion.
 PATHOLOGY OF THE STOMACH Stomach mucosa Gastric mucosa is covered by a layer of mucus. The mucosal glands comprise the cardiac glands, the fundic glands in the fundus and body of the stomach, and the pyloric
PATHOLOGY OF THE STOMACH Stomach mucosa Gastric mucosa is covered by a layer of mucus. The mucosal glands comprise the cardiac glands, the fundic glands in the fundus and body of the stomach, and the pyloric
GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY
 Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Barrett s Esophagus: Old Dog, New Tricks
 Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Objectives. Definitions. Colorectal Cancer Screening 5/8/2018. Payam Afshar, MS, MD Kaiser Permanente, San Diego. Colorectal cancer background
 Colorectal Cancer Screening Payam Afshar, MS, MD Kaiser Permanente, San Diego Objectives Colorectal cancer background Colorectal cancer screening populations Colorectal cancer screening modalities Colonoscopy
Colorectal Cancer Screening Payam Afshar, MS, MD Kaiser Permanente, San Diego Objectives Colorectal cancer background Colorectal cancer screening populations Colorectal cancer screening modalities Colonoscopy
Colon Cancer Screening & Surveillance. Amit Patel, MD PGY-4 GI Fellow
 Colon Cancer Screening & Surveillance Amit Patel, MD PGY-4 GI Fellow Epidemiology CRC incidence and mortality rates vary markedly around the world. Globally, CRC is the third most commonly diagnosed cancer
Colon Cancer Screening & Surveillance Amit Patel, MD PGY-4 GI Fellow Epidemiology CRC incidence and mortality rates vary markedly around the world. Globally, CRC is the third most commonly diagnosed cancer
Appendix 4: WHO Classification of Tumours of the pancreas 17
 S3.01 The WHO histological tumour type must be recorded. CS3.01a The histological type of the tumour should be recorded based on the current WHO classification 17 (refer to Appendices 4-7). Appendix 4:
S3.01 The WHO histological tumour type must be recorded. CS3.01a The histological type of the tumour should be recorded based on the current WHO classification 17 (refer to Appendices 4-7). Appendix 4:
Advanced techniques for resection of large polyps. John G. Lee, MD February 2, 2018
 Advanced techniques for resection of large polyps John G. Lee, MD February 2, 2018 Background 1cm - large polyp on screening 2cm - large for polypectomy 3cm giant polyp 10-15% of polyps can t be removed
Advanced techniques for resection of large polyps John G. Lee, MD February 2, 2018 Background 1cm - large polyp on screening 2cm - large for polypectomy 3cm giant polyp 10-15% of polyps can t be removed
Magnifying Endoscopy and Chromoendoscopy of the Upper Gastrointestinal Tract
 Magnifying Endoscopy and Chromoendoscopy of the Upper Gastrointestinal Tract Alina M.Boeriu 1, Daniela E.Dobru 1, Simona Mocan 2 1) Department of Gastroenterology, University of Medicine and Pharmacy;
Magnifying Endoscopy and Chromoendoscopy of the Upper Gastrointestinal Tract Alina M.Boeriu 1, Daniela E.Dobru 1, Simona Mocan 2 1) Department of Gastroenterology, University of Medicine and Pharmacy;
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE
 SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
How to characterize dysplastic lesions in IBD?
 How to characterize dysplastic lesions in IBD? Name: Institution: Helmut Neumann, MD, PhD, FASGE University Medical Center Mainz What do we know? Patients with IBD carry an increased risk of developing
How to characterize dysplastic lesions in IBD? Name: Institution: Helmut Neumann, MD, PhD, FASGE University Medical Center Mainz What do we know? Patients with IBD carry an increased risk of developing
Gastrointestinal Malignancies. Dr Rodney ITAKI Pathology Division, SMHS, UPNG Anatomical Pathology Discipline
 Gastrointestinal Malignancies Dr Rodney ITAKI Pathology Division, SMHS, UPNG Anatomical Pathology Discipline Esophagus normal anatomy Hollow tube 23-25cm long in adults Extends from pharynx to level of
Gastrointestinal Malignancies Dr Rodney ITAKI Pathology Division, SMHS, UPNG Anatomical Pathology Discipline Esophagus normal anatomy Hollow tube 23-25cm long in adults Extends from pharynx to level of
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal surgery prior as factor in laparoscopic colorectal surgery, 554 555 Abscess(es) CRC presenting as, 539 540 Adenocarcinoma of
Index Note: Page numbers of article titles are in boldface type. A Abdominal surgery prior as factor in laparoscopic colorectal surgery, 554 555 Abscess(es) CRC presenting as, 539 540 Adenocarcinoma of
Paris classification (2003) 삼성의료원내과이준행
 Paris classification (2003) 삼성의료원내과이준행 JGCA classification - Japanese Gastric Cancer Association - Type 0 superficial polypoid, flat/depressed, or excavated tumors Type 1 polypoid carcinomas, usually attached
Paris classification (2003) 삼성의료원내과이준행 JGCA classification - Japanese Gastric Cancer Association - Type 0 superficial polypoid, flat/depressed, or excavated tumors Type 1 polypoid carcinomas, usually attached
UK National Screening Committee. Screening for Stomach Cancer. 12 February 2016
 14/397 UK National Screening Committee Screening for Stomach Cancer 12 February 2016 Aim 1. To ask the UK National Screening Committee to make a recommendation, based upon the evidence presented in this
14/397 UK National Screening Committee Screening for Stomach Cancer 12 February 2016 Aim 1. To ask the UK National Screening Committee to make a recommendation, based upon the evidence presented in this
PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT.
 PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT. OESOPHAGEAL LESIONS OESOPHAGITIS AND OTHER NON NEOPLASTIC DISORDERS Corrosive Gastroesophageal reflux (GERD), Pills, Acid intake,
PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT. OESOPHAGEAL LESIONS OESOPHAGITIS AND OTHER NON NEOPLASTIC DISORDERS Corrosive Gastroesophageal reflux (GERD), Pills, Acid intake,
Endoscopic approach to subepithelial lesions
 513538TAG7310.1177/1756283X13513538Therapeutic Advances in GastroenterologyL Menon and JM Buscaglia research-article2013 Therapeutic Advances in Gastroenterology Review Endoscopic approach to subepithelial
513538TAG7310.1177/1756283X13513538Therapeutic Advances in GastroenterologyL Menon and JM Buscaglia research-article2013 Therapeutic Advances in Gastroenterology Review Endoscopic approach to subepithelial
When is a programmed follow-up meaningful and how should it be done? Professor Alastair Watson University of Liverpool
 When is a programmed follow-up meaningful and how should it be done? Professor Alastair Watson University of Liverpool Adenomas/Carcinoma Sequence Providing Time for Screening Normal 5-20 yrs 5-15 yrs
When is a programmed follow-up meaningful and how should it be done? Professor Alastair Watson University of Liverpool Adenomas/Carcinoma Sequence Providing Time for Screening Normal 5-20 yrs 5-15 yrs
Figure 1. Polypectomy specimen. Inset: Colonoscopy.
 Case: A 69 year- old man with a history of gastrointestinal polyps presents with occult blood in the stool and iron deficiency anemia. He reports no weight loss, melena or hematochezia. Colonoscopy shows
Case: A 69 year- old man with a history of gastrointestinal polyps presents with occult blood in the stool and iron deficiency anemia. He reports no weight loss, melena or hematochezia. Colonoscopy shows
Small Bowel Cases. Introduction. Introduction, Continued 12/7/2011. Lesions Found on endoscopic biopsies Just Like Signing Out
 Small Bowel Cases Lesions Found on endoscopic biopsies Just Like Signing Out Introduction Small intestinal biopsies have a few special pitfalls, for example: Neuroendocrine tumors are readily mistaken
Small Bowel Cases Lesions Found on endoscopic biopsies Just Like Signing Out Introduction Small intestinal biopsies have a few special pitfalls, for example: Neuroendocrine tumors are readily mistaken
Introduction of GB polyp
 Management of Gallbladder Polyp as Physician's View Sang Hyub Lee, MD, PhD Seoul National University College of Medicine Seoul National University Bundang Hospital Department of Internal Medicine Division
Management of Gallbladder Polyp as Physician's View Sang Hyub Lee, MD, PhD Seoul National University College of Medicine Seoul National University Bundang Hospital Department of Internal Medicine Division
Surgical Management of Neuroendocrine Tumors of the Gut. Richard Hodin MD Professor of Surgery Massachusetts General Hospital Harvard Medical School
 Surgical Management of Neuroendocrine Tumors of the Gut Richard Hodin MD Professor of Surgery Massachusetts General Hospital Harvard Medical School Sites of GI Carcinoid Tumors Small intestine 44% Rectum
Surgical Management of Neuroendocrine Tumors of the Gut Richard Hodin MD Professor of Surgery Massachusetts General Hospital Harvard Medical School Sites of GI Carcinoid Tumors Small intestine 44% Rectum
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia
 Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Polypectomy and Local Resections of the Colorectum Structured Pathology Reporting Proforma
 Polypectomy and Local Resections of the Colorectum Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth
Polypectomy and Local Resections of the Colorectum Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth
