R ecommendations for diagnosis and treatment of epithelial
|
|
|
- Florence Mosley
- 5 years ago
- Views:
Transcription
1 465 ORIGINAL ARTICLE Diagnostic accuracy of forceps biopsy versus polypectomy for gastric polyps: a prospective multicentre study S M Muehldorfer, M Stolte, P Martus, E G Hahn, C Ell, for the Multicenter Study Group Gastric Polyps... See end of article for authors affiliations... Correspondence to: Professor C Ell, Department of Medicine II, Dr-Horst-Schmidt-Kliniken, Ludwig-Erhard-Str 100, Wiesbaden, Germany Accepted for publication 18 June Gut 2002;50: Aims: To determine whether an adequate histological diagnosis of gastric polyps can be attained on the basis of forceps biopsy. Patients and methods: In a prospective multicentre study, 194 patients with 222 endoscopically removable gastric polyps (>5 mm) underwent forceps biopsy and complete polypectomy. Patients with fundic gland polyps and polyposis syndrome were not included. Specimens were evaluated by primary and reference pathologists, and the complication rate of gastric polypectomy was also determined. Results: Of the 222 polyps, histological examination of the polypectomy specimens revealed tumourlike lesions in 77% (10% focal foveolar hyperplasia, 59% hyperplastic polyps, 4% inflammatory fibroid polyps, 4% other polyps) and neoplasia in 19% (10% tubular adenoma, 2% tubulovillous adenoma, 1% high grade intraepithelial neoplasia, 6% ). When biopsy results were compared, complete agreement was found in 124 cases (55.8%) and, in an additional 77 cases (34.7%), the clinically important differentiation between tumour-like lesions and neoplasia was possible. However, relevant differences were found by the reference pathologist in six cases (2.7%), the most common reason being failure of biopsy to reveal foci of carcinoma in hyperplastic polyps. Bleeding was observed after polypectomy in 16 patients (7.2%), in 15 of whom it was managed conservatively. Conclusions: We recommend complete removal by an experienced endoscopist of all epithelial gastric polyps larger than 5 mm after thorough individualised risk-benefit analysis. R ecommendations for diagnosis and treatment of epithelial gastric polyps remain controversial as there is no consensus regarding their malignant potential or the reliability of endoscopic forceps biopsy. 1 4 According to the classification of gastric tumours and polyps established by the WHO, 5 the frequency of malignant transformation depends on histological type. The risk has been reported to be 0 8.6% (mean 2.1%) for hyperplastic polyps, approximately 5% for tubular adenomas, and % for villous adenomas and pyloric gland adenomas A precise histological classification therefore is essential for therapeutic action. Especially important is the reliability of the histological rating of forceps biopsy sampling with regard to the total polyp. The present study represents the first multicentre investigation to examine prospectively the accuracy of the histological evaluation of forceps biopsy sampling from gastric polyps in comparison with endoscopic polypectomy. To estimate the risk-benefit ratio of the latter procedure, complications were also documented. METHODS We studied 194 patients with a total of 222 gastric polyps. Altogether 28 study centres (13 hospitals and 15 gastroenterologists in private practice) were involved, each yielding a median of six polyps (1 37). Histological assessment of the polyps was performed by pathologists in nine departments of pathology. Every gastric polyp considered amenable to polypectomy (>5 mm) by the study participants was included. According to endoscopic criteria, those located submucosally were not included. Patients with polyposis syndrome and carcinoid tumours of the stomach were excluded. In addition, fundic gland polyps were also excluded as they are usually smaller than 5 mm and can readily be removed completely with biopsy forceps. 18 The histopathological assessment of the biopsy material and polyps was performed by the pathologist chosen by each study centre (the primary pathologist). As both specimens were to be evaluated independently of each other, the total polyp was sent to the pathologist only after the biopsy result was received. In preparation for the histopathological examination, the biopsy samples and polyps were fixed in neutral 10% buffered formalin and embedded in paraffin. The 4 µm sections were stained with haematoxylin and eosin. Sections were assessed according to the WHO classification of gastrointestinal tumours published in After completion of the study, the WHO classification was revised 19 and the term dysplasia was replaced with intraepithelial neoplasia. Accordingly, we updated the terminology in this paper. When the results of the primary pathologists showed relevant diagnostic differences between biopsy and polypectomy or focal carcinomas in hyperplastic polyps, these sections were blinded and reviewed by the reference pathologist (MS). Before the endoscopic procedure, written informed consent for polypectomy and participation in the study was obtained. If the patient so requested, sedation with midazolam or pharyngeal anaesthesia with xylocaine, or both, were administered. The estimated size and location of the polyps were documented by the endoscopist. At least two forceps biopsy samples were taken from every polyp. Endoscopic snare polypectomy was performed with monopolar diathermy current. Submucosal injection of diluted adrenaline in saline was allowed facultatively to elevate sessile polyps. Complications arising during polypectomy or in the subsequent observation period were also documented. Bleeding was rated as a
2 466 Muehldorfer, Stolte, Martus, et al No of polyps (%) No polyp tissue Tumour like lesion Neoplastic polyp Total Sessile Broad based Pedunculated Figure 1 Polyp growth pattern (sessile, broad based, or pedunculated) according to histological subgroup. complication when the endoscopist believed that therapeutic intervention was required to halt it. Diagnostic validity was assessed by classifying the polyps into three different subgroups: no epithelial polyp, tumourlike lesion, and neoplastic polyp. Owing to the very small number of specimens designated as no polyp tissue, adequate statistical comparison could not be made between these and the other subgroups. To determine sensitivity and predictive values of the histological results of biopsy and polypectomy specimens, these were compared with the ectomy result from the reference pathologist (MS) which was considered the gold standard. For the main results concerning diagnostic validity, confidence intervals are given. The dependency of the data from different polyps in the same patient was taken into account. For significance testing, only the first polyp from every patient was used. For determination of confidence intervals, all 222 polyps were used and included the correction of Rao and Scott 20 for related standard errors. The size of the polyps within the different subgroups was compared by analysis of variance. To obtain equality of variances and normal data distribution, a logarithmic transformation of raw values was performed. Categorical data were compared using the χ 2 test. For subgroup comparisons, Bonferroni s correction was applied. For comparison of complication rates, the sample was divided into two groups with non-experienced and experienced endoscopists. To achieve equality of variances for different complication rates, the arcsin transformation was applied. The level of significance was 0.05 (two sided) in all statistical tests. Statistical evaluation was performed with SPSSWIN. The study protocol was approved by the ethics committee of the University of Erlangen-Nuremberg. Table 1 Polypectomy specimens: histological results RESULTS Of the 194 patients (114 women, 80 men; age years (mean 70)), 24 had two polyps each and two patients had three (total 222 polyps). Mean polyp size was 10.5 mm (3 50), and tumour size did not differ among the subtypes of polyps (p>0.14). As noted, only polyps >5 mm were studied. The 3 mm polyps cited as the lower end of the range represent polypectomy specimens after reduction consequent to biopsy. In 160 patients (82.5%), the polyp was found incidentally as there were no suggestive clinical symptoms. In 10 patients (5.2%) gastroscopy was performed for gastrointestinal bleeding; in 19 (9.8%) anaemia was present; and in five (2.6%) a delay in gastric emptying was suspected. The polyps were most frequently located in the antrum (61.0%) and corpus (31.2%), and less frequently in the cardia (5.0%) and fundic region (2.8%). Of seven polyps in patients with a partially resected stomach, two were located in the anastomotic region. Location did not differ among the polyp subtypes (p>0.29). In 135 polyps (60.8%) the epithelial surface was macroscopically intact, 77 (34.7%) showed erosions, and 10 (4.5%) appeared bloody. Surface appearance was significantly different between tumour-like lesions and neoplastic polyps (p<0.01) with the latter more often showing an intact epithelium. The growth pattern was sessile in 85 (38.3%) of the polyps, broad based in 78 (35.1%), and pedunculated in 59 (26.6%). Neoplastic polyps were significantly more frequently sessile (p<0.01 after Bonferroni s correction); no difference was found between the other two shapes (p>0.5 without Bonferroni s correction) (fig 1). The histological results of the polypectomy specimens after re-evaluation of discrepant results by the reference pathologist were as follows: 171 polyps (77.0%) were tumour-like lesions, 44 (19.8%) were neoplastic, and seven (3.2%) showed no polyp tissue (table 1). In 56 polyps, focal foveolar hyperplasia was diagnosed by the primary pathologist on examination of the biopsy specimens only. This result was confirmed in only 18 cases (32.1%) after inspection of the polypectomy specimens. Of the remaining polyps, 31 (55.4%) were hyperplastic, five were inflammatory fibroid polyps, one was a tubular adenoma, and one was a Peutz-Jeghers polyp. When the histological results of all biopsy and polypectomy specimens of the primary pathologist only were compared, complete agreement was seen in 124 polyps (55.8%). In an additional 77 polyps (34.7%), the clinically crucial distinction between tumour-like lesion and neoplastic polyp was made. Frequency Per cent No polyp tissue Tubular adenoma Tubulovillous adenoma Villous adenoma High grade intraepithelial neoplasia in tubulovillous adenoma Tubular Papillary Signet ring cell carcinoma Tubular adenoma+tubular tubular Carcinoid tumour Focal foveolar hyperplasia Peutz-Jeghers polyp Brunner s gland heterotopia Inflammatory fibroid polyp Other non-neoplastic polyps Total 222
3 Gastric polyps 467 Table 2 Biopsy and polypectomy specimens: histological results of the primary and reference pathologists No Primary pathologist (biopsy) Primary pathologist (ectomy) Reference pathologist (biopsy) Reference pathologist (ectomy) Relevant overestimation by the primary pathologist: 5 1 Tubular adenoma Foc. fov. hyperplasia Foc. fov. hyperplasia 2 Tubular adenoma 3 Tubular adenoma No polyp tissue No polyp tissue 4 No polyp tissue Tubular adenoma 5 Tubular adenoma and tubular adenoma Relevant underestimation by the primary pathologist: 4 6 Foc. fov. hyperplasia Tubular adenoma Tubular adenoma Tubular adenoma 7* and microcarcinoid and tubular 8 Foc. fov. hyperplasia and tubular Tubular adenoma Tubular Tubular adenoma 9 Foc. fov. hyperplasia Possible Peutz-Jeghers polyp Peutz-Jeghers polyp No relevant differences between primary and reference pathologist: Possible hyperplastic polyp Hamartoma No polyp tissue Inflamm. fibroid polyp 11 Tubular adenoma Foc. fov. hyperplasia Tubular adenoma No polyp tissue 12 Tubular Tubulovillous adenoma Tubular Tubular 13 Foc. fov. hyperplasia and carcinoid Carcinoid tumor tumour 14 Tubular adenoma Foc. fov. hyperplasia Tubular adenoma 15 Pyloric gland adenoma Tubular Tubular Tubular 16 Tubulovillous adenoma High grade intraepithelial neoplasia Tubular Tubular adenoma 17 Tubular adenoma and tubular adenoma Tubular adenoma Tubular adenoma and possible tubular 18 Possible hyperplastic polyp Hamartoma No polyp tissue Brunner s gland heterotopia 19* Tubular and tubular Tubular and tubular 20* No polyp tissue Tubular Possible hyperplastic polyp and tubular 21* and tubular *Concomitant presence of tumour-like lesions and neoplastic foci. Foc. fov., focal foveolar; Inflamm., inflammatory. However, in 21 cases (9.5%) there were important discrepancies: five polyps (2.3%) classified as neoplastic on biopsy were non-neoplastic or benign on polypectomy; seven (3.2%) polyps non-neoplastic or benign on biopsy were neoplastic or malignant on polypectomy; three (1.4%) hyperplastic polyps on biopsy were diagnosed as hamartoma; and six (2.7%) other hyperplastic polyps were found to have additional carcinoma or carcinoid tumour portions. These 21 preparations were sent to the reference pathologist who concurred with the primary pathologist s findings in 12 cases (57.1%). In nine cases (42.9%) however relevant disagreement occurred. Five specimens had been overestimated by the primary pathologist (that is, a tumour-like lesion had been diagnosed as neoplastic) and four specimens had been underestimated (see table 2). At the re-evaluation of these 21 cases by the reference pathologist, the clinically relevant differentiation between tumour-like lesion and neoplastic polyp was possible in 15 cases by inspection of the biopsy sections alone whereas in the remaining six cases comparison with the polypectomy sections uncovered relevant differences (table 3). Of these, biopsy failed to reveal foci of carcinoma in three hyperplastic and tubular polyps. In two specimens it is suspected that no polyp tissue was removed during biopsy in one and polypectomy in the other. In a further polyp, biopsy did not contain the relevant carcinoid tumour portion. In table 4, sensitivities and predictive values and their respective confidence intervals are given for the histological biopsy and polypectomy results of the primary pathologist as well as for the biopsy results of the reference pathologist. Values for tumour-like lesions and neoplastic polyps are tabulated separately. For both examiners, the validity of the histological biopsy results was lower than that of the polypectomy results of the primary pathologist. No lethal complications of polypectomy arose. Bleeding occurred in 16 patients (7.2%). It ceased spontaneously in three but required therapeutic intervention in 13 (injection in six, additional coagulation in one, additional clipping in three, clipping solely in two, laparotomy in one). Two of the patients required transfusion. In one patient an inflammatory reaction of the peritoneum owing to a closed perforation without free gas on x ray or signs of generalised peritonitis was suspected. The patient was managed conservatively. Table 3 Biopsy and polypectomy specimens: clinically relevant differences on histological examination by the reference pathologist Biopsy Tubular adenoma Focal foveolar hyperplasia Possible hyperplastic polyp Ectomy No polyp tissue Tubular adenoma Carcinoid tumour and tubular and tubular and tubular
4 468 Muehldorfer, Stolte, Martus, et al Table 4 Biopsy and polypectomy specimens: sensitivity, predictive value, and confidence limits* Examination Subgroup Sensitivity (CI) Predictive value (CI) Relative % Biopsy primary pathologist Neoplastic 0.89 ( ) 0.89 ( ) Biopsy reference pathologist 0.91 ( ) 0.98 ( ) Ectomy primary pathologist 0.98 ( ) 0.96 ( ) Prevalence 0.20 Biopsy primary pathologist Tumour-like 0.93 ( ) 0.97 ( ) Biopsy reference pathologist 0.96 ( ) 0.97 ( ) Ectomy primary pathologist 0.99 ( ) 0.97 ( ) Prevalence 0.77 *Biopsy results are those of both the primary and reference pathologists; polypectomy results are those of the primary pathologist. p<0.05 Minor complication Major complication Polyp size (mm) Figure 2 Complication frequency of polypectomy according to polyp size. Although the complication rate was not consistently proportionate to increasing tumour size (p>0.4), it was significantly higher in mid size (16 20 mm) than in small (<10 mm) tumours (p<0.05 after Bonferroni s correction with factor 6 according to the six possible paired comparisons). There was also a tendency for major complications to occur in larger polyps although this impression was not statistically significant owing to the small number of polyps in this group (fig 2). The complication rate for endoscopists with less experience with polypectomy (<7 polyps) was higher than for more experienced endoscopists (11.4% v 6.8%) although this difference was not statistically significant. DISCUSSION With the introduction of endoscopic polypectomy in the stomach in the early 1970s, an alternative to surgical ablation became available. 21 As forceps biopsies had been considered unreliable, the procedure enjoyed widespread use However, complications soon led to reconsideration of clearing the stomach of all polyps and to the use of forceps biopsy for decision making. To evaluate whether forceps biopsy is representative of the entire polyp, only three series, smaller than the present, have as yet been reported. 1 3 With a faulty differentiation between tumour-like lesions and neoplastic polyps rated as a clinically relevant difference, the discrepancy rate between biopsy and polypectomy results ranged from 0 to 29%. In our prospective multicentre study the clinically relevant discrimination between tumour-like lesions and neoplastic polyps with forceps biopsy after the initial examination by the primary pathologist was possible in 201 of 222 polyps (90.5%). After review of the specimens by the reference pathologist, only six cases (2.7%) with relevant differences from polypectomy results remained. The most important reason for the differing appraisal by the reference pathologist between these specimens was the presence of foci of carcinoma in hyperplastic polyps that were not gathered by forceps biopsy. In nine cases (4.1%) the reference pathologist found clinically relevant biopsy or polypectomy results that were different from those of the primary pathologist. On the one hand these results show that with a meticulous examination of the forceps biopsy samples by an experienced pathologist, a correct histological diagnosis can be obtained without a complete polypectomy in nearly all cases (97.3%). On the other hand, foci of carcinoma are present in a small percentage of hyperplastic polyps and may be missed with biopsy sampling. In our survey we found four such polyps (3.1%) in a total of 131 hyperplastic polyps, ranging from 10 to 50 mm (median 15 mm). In only one of these was the malignant focus detected by forceps biopsy. Since the first description in 1978 by Remmele and Kolb of a hyperplastic polyp containing a carcinoma, 24 several case reports have been published. Although at first it was thought that only hyperplastic polyps larger than 20 mm could contain malignant foci, this finding has more recently been observed in polyps of 5 mm The reported frequency differs considerably. One reason may be that in the older literature adenomas were misinterpreted as hyperplastic polyps containing intraepithelial neoplasia. On the other hand, regenerative alterations, which always occur in the erosive area in hyperplastic polyps, were in part overestimated as intraepithelial neoplasia. Stolte demonstrated malignant foci in only 0.3% of 2036 hyperplastic polyps. 6 In contrast, a meta-analysis of three other studies found malignant foci in 2.2% of 1072 polyps which compares well with our result of four carcinomas (3.1%) in a total of 131 hyperplastic polyps. Focal foveolar hyperplasia is considered a potential precursor of hyperplastic polyps by the WHO. However, Stolte et al showed that focal foveolar hyperplasia and hyperplastic polyps can readily be differentiated on the basis of architectural and cytological criteria, even in forceps biopsy material. 29 This estimation cannot be supported by the results of our study as more than 55% of the biopsy specimens initially judged to be focal foveolar hyperplasia were diagnosed as hyperplastic polyps after evaluation of the corresponding polypectomy specimens. In two cases, clinically crucial differentiations (a neoplastic polyp in one and a Peutz-Jeghers polyp in another) were not possible by the primary pathologist. A recommendation based on these data to remove all polyps classified as focal foveolar or hyperplastic on biopsy completely with the snare must be weighed against the possible risks of polypectomy. In our study, bleeding occurred in 16 patients (7.2%). With the exception of one case, managed by laparotomy, all others ceased spontaneously or could be controlled endoscopically. Transfusion was necessary in only two patients. This underscores the importance of proficiency in endoscopic haemostatic techniques by the endoscopic team as a prerequisite for performing polypectomy in the stomach.
5 Gastric polyps 469 Additionally, in one patient a closed perforation was suspected. In summary, in a total of three patients (1.4%) major but not lethal complications occurred. As expected, we observed an increase in the frequency of complications with increasing polyp size. However, the largest polyps (21 50 mm) were associated with a lower complication rate than the mid sized polyps although the number in the former subgroup was small (12 polyps 5.4%). In view of the risk-benefit profile (2.3% undetected foci of carcinoma in hyperplastic polyps on biopsy; 1.4% major complications of polypectomy), complete endoscopic removal of even smaller polyps rated as hyperplastic on biopsy must be considered. Regarding focal foveolar hyperplasia, this recommendation should be adapted to the endoscopic appearance of the polyp. For polyps with characteristic macroscopic features (size <5 mm, multiple occurrence, location in the antrum 6 ), no further action seems to be justified. For all other polyps rated as focal foveolar hyperplasia on biopsy, endoscopic polypectomy should be considered also as in the clinical setting no unequivocal differentiation from other histological polyp types based on forceps biopsy specimens seems to be possible at present. Of course, the patient s general condition (especially age and concomitant illnesses that might be exacerbated by possible complications) should also be a factor. There is no controversy regarding indications for removal of adenomatous polyps as the adenoma-carcinoma sequence holds true in gastric as well as colorectal polyps. 630 In our series, the concomitant presence of adenomatous and carcinomatous portions in a single polyp was observed in two specimens. Here in contrast with carcinomatous foci in APPENDIX The participants in the study group are shown in Table A1. Table A1 Participants in the study group hyperplastic polyps underestimation on biopsy is not clinically relevant as all adenomas must be removed completely. Owing to the characteristically sessile growth pattern of adenomas and carcinomas, submucosal injection is recommended to facilitate complete endoscopic removal. In many cases, an endoscopic classification can be attempted as most adenomas reveal an intact mucosal surface whereas hyperplastic polyps and carcinomas frequently show erosions and bleeding. 31 As the sensitivity and specificity of endoscopic diagnosis are unknown, histological examination remains mandatory. In all other polyp types (22 (9.9%) in our study), polypectomy would only be necessary when the polyps are symptomatic or produce complications (bleeding, obstruction). As the remaining number of poly types is limited, a general recommendation to remove all epithelial gastric polyps larger than 5 mm primarily without prior histological clarification by forceps biopsy may be justified. In conclusion, the results of our study show that in a clinical setting focal foveolar hyperplasia larger than 5 mm cannot be unequivocally differentiated from other histological polyp types based on forceps biopsy specimens alone and hyperplastic gastric polyps can contain neoplastic foci that might not be diagnosed by forceps biopsy alone. Even if the bleeding rate after snare polypectomy appears to be higher in the stomach than in the colon, the majority of cases can be managed endoscopically. Therefore, we recommend removal by an experienced endoscopist of all epithelial gastric polyps larger than 5 mm after thorough individualised risk-benefit analysis. W Barina/W Simon, Würzburg W Bachmann/L Bolle, Frankenwaldklinik, Kronach J Giedl, Inst für Pathologie Weiden KJ Dümlein, Erlangen C Ell/SM Mühldorfer, Med Klinik I der FAU Erlangen-Nürnberg B Kaduk, Path Inst München C Ferentzi/I Wild, Nürnberg B Feinauer, Kreiskrankenhaus Mühlacker T Kirchner/Ch Wittekind/H Steininger, Path Anat Inst der FAU Erlangen-Nürnberg E v Fritsch, Erlangen H Frotz, Marien KH, Bergisch Gladbach H Kühn/D Dang, Path Inst Fürth P Janetschek, München B Krakamp, Städt. KH, Köln-Merheim K Müller, Path Inst Überlingen W Kerzel/R Thiemann, Forchheim P Lederer/K Kusch, Waldkrankenhaus, Erlangen G Röckelein/H Wiesinger/U Zimmermann, Path Anat Inst Regensburg E Meier, Amberg CE Manegold, Evangelisches KH, Holzminden G Seitz, Path Inst Bamberg R Muckelbauer/W Muckelbauer, Scheβlitz H Schönekäs/KT Steurer/R Meyer, VI Med Klinik, Nürnberg M Stolte, Inst für Pathologie Bayreuth E Ruess, Böblingen H Schweikert, Kreiskrankenhaus Münchberg P H Wünsch, Path. Inst Nürnberg J Schenk/J Zeus, Erlangen B Schmack/K Wagner, Bayreuth R Scholz, Bamberg H J Schreiber, Bamberg R Kellner/E Spangler/S Weidenhiller, Regensburg K Seitz, KH Kreis, Sigmaringen O Stadelmann/C Langmann, II Med Klinik, Fürth H J Weis/K Schmidt, II Med Klinik, Bamberg KH Wiedmann/F Ehrnsperger, II Med Klinik, Regensburg H Worlicek, Regensburg
6 470 Muehldorfer, Stolte, Martus, et al... Authors affiliations S M Muehldorfer, E G Hahn, Department of Medicine I, University of Erlangen-Nuremberg, Germany M Stolte, Institute of Pathology, Bayreuth, Germany P Martus, Institute of Medical Informatics, Statistics and Epidemiology, FU of Berlin, Germany C Ell, Department of Medicine II, HSK, Wiesbaden, Germany REFERENCES 1 Seifert E, Elster K. Gastric polypectomy. Am J Gastroenterol 1975;63: Ottenjann R, Kunert H, Seib HJ. Is gastroscopic polypectomy a diagnostic necessity? Results of a prospective study. Dtsch Med Wochenschr 1984;109: Chua CL. Gastric polyps: the case for polypectomy and endoscopic surveillance. J R Coll Surg Edinb 1990;35: Ginsberg GG, Al-Kawas FH, Fleischer DE, et al. Gastric polyps: relationship of size and histology to cancer risk. Am J Gastroenterol 1996;91: Jass JR, Sobin LH, Watanabe H. The World Health Organization s histologic classification of gastrointestinal tumors. A commentary on the second edition. Cancer 1990;66: Stolte M. Clinical consequences of the endoscopic diagnosis of gastric polyps. Endoscopy 1995;27: Kamiya T, Morishita T, Asakura H, et al. Histoclinical long-standing follow-up study of hyperplastic polyps of the stomach. Am J Gastroenterol 1981;75: Orlowska J, Jarosz D, Pachlewski J, et al. Malignant transformation of benign epithelial gastric polyps. Am J Gastroenterol 1995;90: Ming SC. The classification and significance of gastric polyps. In: Yardley JH, Morson BC, Abel MR, eds. The gastrointestinal tract. Baltimore: Williams and Wilkins, 1977: Daibo M, Itabashi M, Hirota T. Malignant transformation of gastric hyperplastic polyps. Am J Gastroenterol 1987;82: Zea-Iriarte WL, Sekine I, Itsuno M, et al. Carcinoma in gastric hyperplastic polyps. A phenotypic study. Dig Dis Sci 1996;41: Elster K. Histologic classification of gastric polyps. In: Morson BC, ed. Pathology of the gastrointestinal tract. Berlin: Springer-Verlag, 1976: Tomasulo J. Gastric polyps. Histologic types and their relationship to gastric carcinoma. Cancer 1971;27: Ming SC. Epithelial polyps of the stomach. In: Ming SC, Goldman H, eds. Pathology of the gastrointestinal tract. Philadelphia: WB Saunders, 1992: Orlowska J, Pietrow D. Multifocal gastric carcinoma arising from hyperplastic and adenomatous polyps. Am J Gastroenterol 1990;85: Lanza FL, Graham DY, Nelson RS, et al. Endoscopic upper gastrointestinal polypectomy. Report of 73 polypectomies in 63 patients. Am J Gastroenterol 1981;75: Nakamura T, Nakano G. Histopathological classification and malignant change in gastric polyps. J Clin Pathol 1985;38: Schmitz JM, Stolte M. Gastric polyps as precancerous lesions. Gastrointest Endosc Clin N Am 1997;7: Hamilton SR, Aaltonen LA, eds. Tumours of the digestive system. Lyon: IARC Press, Rao JN, Scott AJ. A simple method for the analysis of clustered binary data. Biometrics 1992;48: Classen M, Demling L. Surgical gastroscopy: removal of gastric polyps using a fiber-optic gastroscope. Dtsch Med Wochenschr 1971;96: Seifert E, Elster K. Endoscopic polypectomy in the stomach. Indication, technic, and results. Dtsch Med Wochenschr 1972;97: Singer M, Busse R, Elster K, et al. Endoscopic polypectomy in the upper gastrointestinal tract. Endoscopy 1975;7: Remmele W, Kolb EF. Malignant transformation of hyperplasiogenic polyps of the stomach case report. Endoscopy 1978;10: Rosen S, Hoak D. Intramucosal carcinoma developing in a hyperplastic gastric polyp. Gastrointest Endosc 1993;39: Yamaguchi K, Shiraishi G, Maeda S, et al. Adenocarcinoma in hyperplastic polyp of the stomach. Am J Gastroenterol 1990;85: Ghazi A, Ferstenberg H, Shinya H. Endoscopic gastroduodenal polypectomy. Ann Surg 1984;200: Gschwantler M, Pulgram T, Feichtenschlager T, et al. Gastric carcinoma arising from a hyperplasiogenic polyp with a diameter of less than 2 centimeters. Z Gastroenterol 1995;33: Stolte M, Bethke B, Sticht T, et al. Differentiation of focal foveolar hyperplasia from hyperplastic polyps in gastric biopsy material. Pathol Res Pract 1995;191: Kamiya T, Morishita T, Asakura H, et al. Long-term follow-up study on gastric adenoma and its relation to gastric protruded carcinoma. Cancer 1982;50: Stolte M, Sticht T, Eidt S, et al. Frequency, location, and age and sex distribution of various types of gastric polyp. Endoscopy 1994;26: Gut: first published as /gut on 1 April Downloaded from on 22 July 2018 by guest. Protected by copyright.
The Clinicopathological Features of Gastric Hyperplastic Polyps with Neoplastic Transformations: A Suggestion of Indication for
 Gut and Liver, Vol. 3, No. 4, December 2009, pp. 271-275 original article The Clinicopathological Features of Gastric Hyperplastic Polyps with Neoplastic Transformations: A Suggestion of Indication for
Gut and Liver, Vol. 3, No. 4, December 2009, pp. 271-275 original article The Clinicopathological Features of Gastric Hyperplastic Polyps with Neoplastic Transformations: A Suggestion of Indication for
Hyperplastische Polyps Innocent bystanders?
 Hyperplastische Polyps Innocent bystanders?? K. Geboes P th l i h O tl dk d Pathologische Ontleedkunde, KULeuven Content Historical Classification Relation Hyperplastic polyps carcinoma The concept cept
Hyperplastische Polyps Innocent bystanders?? K. Geboes P th l i h O tl dk d Pathologische Ontleedkunde, KULeuven Content Historical Classification Relation Hyperplastic polyps carcinoma The concept cept
Gastric Polyps. Bible class
 Gastric Polyps Bible class 29.08.2018 Starting my training in gastroenterology, some decades ago, my first chief always told me that colonoscopy may seem technically more challenging but gastroscopy has
Gastric Polyps Bible class 29.08.2018 Starting my training in gastroenterology, some decades ago, my first chief always told me that colonoscopy may seem technically more challenging but gastroscopy has
Large Colorectal Adenomas An Approach to Pathologic Evaluation
 Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
Fundic Gland Polyposis in Patients Without Familial Adenomatosis Coli: Its Incidence and Clinical Features
 GASTROENTEROLOGY 1984;86;1437-42 ALIMENTARY TRACT Fundic Gland Polyposis in Patients Without Familial Adenomatosis Coli: Its Incidence and Clinical Features MITSUO IIDA, TSUNEYOSHI YAO, HIDENOBU WATANABE,
GASTROENTEROLOGY 1984;86;1437-42 ALIMENTARY TRACT Fundic Gland Polyposis in Patients Without Familial Adenomatosis Coli: Its Incidence and Clinical Features MITSUO IIDA, TSUNEYOSHI YAO, HIDENOBU WATANABE,
The Incidence and Significance of Villous Change in Adenomatous Polyps
 The Incidence and Significance Villous Change in Adenomatous Polyps CHRISTOPHER H. K. FUNC, M.D., AND HARVEY GOLDMAN, M.D. Department Pathology, Harvard Medical School and Beth Israel Hospital, Boston,
The Incidence and Significance Villous Change in Adenomatous Polyps CHRISTOPHER H. K. FUNC, M.D., AND HARVEY GOLDMAN, M.D. Department Pathology, Harvard Medical School and Beth Israel Hospital, Boston,
Surveying the Colon; Polyps and Advances in Polypectomy
 Surveying the Colon; Polyps and Advances in Polypectomy Educational Objectives Identify classifications of polyps Describe several types of polyps Verbalize rationale for polypectomy Identify risk factors
Surveying the Colon; Polyps and Advances in Polypectomy Educational Objectives Identify classifications of polyps Describe several types of polyps Verbalize rationale for polypectomy Identify risk factors
Effect of Helicobacter pylori eradication on the regression of gastric polyps in National Cancer Screening Program
 ORIGINAL ARTICLE Korean J Intern Med 2018;33:506-511 Effect of Helicobacter pylori eradication on the regression of gastric polyps in National Cancer Screening Program Su Youn Nam 1,2, Bum Joon Park 2,
ORIGINAL ARTICLE Korean J Intern Med 2018;33:506-511 Effect of Helicobacter pylori eradication on the regression of gastric polyps in National Cancer Screening Program Su Youn Nam 1,2, Bum Joon Park 2,
Serrated neoplasia of the stomach: a new entity
 J Clin Pathol 2001;54:849 853 849 Serrated neoplasia of the stomach: a new entity C A Rubio Gastrointestinal and Liver Pathology Research Laboratory, Karolinska Institute and Hospital, 171 76 Stockholm,
J Clin Pathol 2001;54:849 853 849 Serrated neoplasia of the stomach: a new entity C A Rubio Gastrointestinal and Liver Pathology Research Laboratory, Karolinska Institute and Hospital, 171 76 Stockholm,
Colon and Rectum: 2018 Solid Tumor Rules
 2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING Colon and Rectum: 2018 Solid Tumor Rules 1 Colon and Rectum Solid Tumor Rules Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent
2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING Colon and Rectum: 2018 Solid Tumor Rules 1 Colon and Rectum Solid Tumor Rules Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent
Colonic Polyp. Najmeh Aletaha. MD
 Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Hereditary Gastric Cancer
 Hereditary Gastric Cancer Dr Bastiaan de Boer Consultant Pathologist Department of Anatomical Pathology PathWest Laboratory Medicine, QE II Medical Centre Clinical Associate Professor School of Pathology
Hereditary Gastric Cancer Dr Bastiaan de Boer Consultant Pathologist Department of Anatomical Pathology PathWest Laboratory Medicine, QE II Medical Centre Clinical Associate Professor School of Pathology
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia
 Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
COLON AND RECTUM SOLID TUMOR RULES ABSTRACTORS TRAINING
 COLON AND RECTUM SOLID TUMOR RULES ABSTRACTORS TRAINING COLON AND RECTUM SOLID TUMOR RULES Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent Terms Terms that are NOT Equivalent
COLON AND RECTUM SOLID TUMOR RULES ABSTRACTORS TRAINING COLON AND RECTUM SOLID TUMOR RULES Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent Terms Terms that are NOT Equivalent
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines
 Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Pathology in Slovenian CRC screening programme:
 Pathology in Slovenian CRC screening programme: Findings, organisation and quality assurance Snježana Frković Grazio University Medical Center Ljubljana, Slovenia Slovenia s population: 2 million Incidence
Pathology in Slovenian CRC screening programme: Findings, organisation and quality assurance Snježana Frković Grazio University Medical Center Ljubljana, Slovenia Slovenia s population: 2 million Incidence
Summary. Cezary ŁozińskiABDF, Witold KyclerABCDEF. Rep Pract Oncol Radiother, 2007; 12(4):
 Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Advanced techniques for resection of large polyps. John G. Lee, MD February 2, 2018
 Advanced techniques for resection of large polyps John G. Lee, MD February 2, 2018 Background 1cm - large polyp on screening 2cm - large for polypectomy 3cm giant polyp 10-15% of polyps can t be removed
Advanced techniques for resection of large polyps John G. Lee, MD February 2, 2018 Background 1cm - large polyp on screening 2cm - large for polypectomy 3cm giant polyp 10-15% of polyps can t be removed
what is the alternative mechanism of histogenesis? Aspects of the morphology of the adenomacarcinoma Morphology of the
 Refer to: Morson B: Polyps and cancer of the large bowel. West J Med 125:93-99, Aug 1976 THE WESTERN Journal of Miedicine Polyps and Cancer of the Large Bowel BASIL MORSON, MD, London MORTALITY STATISTICS
Refer to: Morson B: Polyps and cancer of the large bowel. West J Med 125:93-99, Aug 1976 THE WESTERN Journal of Miedicine Polyps and Cancer of the Large Bowel BASIL MORSON, MD, London MORTALITY STATISTICS
Histopathogenesis of intestinal metaplasia: minute
 J Clin Pathol 1987;40:13-18 Histopathogenesis of intestinal metaplasia: minute lesions of intestinal metaplasia in ulcerated stomachs K MUKAWA, T NAKAMURA, G NAKANO, Y NAGAMACHI From the First Department
J Clin Pathol 1987;40:13-18 Histopathogenesis of intestinal metaplasia: minute lesions of intestinal metaplasia in ulcerated stomachs K MUKAWA, T NAKAMURA, G NAKANO, Y NAGAMACHI From the First Department
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci. Colon polyps. Colorectal cancer
 Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Colon polyps Colorectal cancer Harrison s Principles of Internal Medicine 18 Ed. 2012 Colorectal cancer 70% Colorectal cancer CRC and colon
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Colon polyps Colorectal cancer Harrison s Principles of Internal Medicine 18 Ed. 2012 Colorectal cancer 70% Colorectal cancer CRC and colon
removal of adenomatous polyps detects important effectively as follow-up colonoscopy after both constitute a low-risk Patients with 1 or 2
 Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
General Comments. Hyperplastic polyps
 Gastric Lumps and Bumps: A tale of two polyps Henry D. Appelman, M.D. Department of Pathology University of Michigan appelman@umich.edu General Comments The stomach is far less rich in polyps than is the
Gastric Lumps and Bumps: A tale of two polyps Henry D. Appelman, M.D. Department of Pathology University of Michigan appelman@umich.edu General Comments The stomach is far less rich in polyps than is the
Combination of Paris and Vienna Classifications may Optimize Follow-Up of Gastric Epithelial Neoplasia Patients
 CLINICAL RESEARCH e-issn 1643-3750 DOI: 10.12659/MSM.892697 Received: 2014.10.09 Accepted: 2014.12.03 Published: 2015.04.05 Combination of Paris and Vienna Classifications may Optimize Follow-Up of Gastric
CLINICAL RESEARCH e-issn 1643-3750 DOI: 10.12659/MSM.892697 Received: 2014.10.09 Accepted: 2014.12.03 Published: 2015.04.05 Combination of Paris and Vienna Classifications may Optimize Follow-Up of Gastric
References. GI Biopsies. What Should Pathologists Assistants Know About Gastrointestinal Histopathology? James M Crawford, MD, PhD
 What Should Pathologists Assistants Know About Gastrointestinal Histopathology? James M Crawford, MD, PhD jcrawford1@nshs.edu Executive Director and Senior Vice President for Laboratory Services North
What Should Pathologists Assistants Know About Gastrointestinal Histopathology? James M Crawford, MD, PhD jcrawford1@nshs.edu Executive Director and Senior Vice President for Laboratory Services North
Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens
 ISPUB.COM The Internet Journal of Pathology Volume 12 Number 1 Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens C Rose, H Wu Citation C Rose, H Wu.. The Internet Journal of Pathology.
ISPUB.COM The Internet Journal of Pathology Volume 12 Number 1 Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens C Rose, H Wu Citation C Rose, H Wu.. The Internet Journal of Pathology.
Luminal Histological Outline and Colonic Adenoma Phenotypes
 Luminal Histological Outline and Colonic Adenoma Phenotypes CARLOS A. RUBIO Gastrointestinal and Liver Pathology Research Laboratory, Department of Pathology, Karolinska Institute and University Hospital,
Luminal Histological Outline and Colonic Adenoma Phenotypes CARLOS A. RUBIO Gastrointestinal and Liver Pathology Research Laboratory, Department of Pathology, Karolinska Institute and University Hospital,
The management of gastric polyps
 The management of gastric polyps Andrew F Goddard, 1 Rawya Badreldin, 2 D Mark Pritchard, 3 Marjorie M Walker, 4 Bryan Warren, 5 on behalf of the British Society of Gastroenterology 1 Digestive Diseases
The management of gastric polyps Andrew F Goddard, 1 Rawya Badreldin, 2 D Mark Pritchard, 3 Marjorie M Walker, 4 Bryan Warren, 5 on behalf of the British Society of Gastroenterology 1 Digestive Diseases
Helicobacter pylori Improved Detection of Helicobacter pylori
 DOI:http://dx.doi.org/10.7314/APJCP.2016.17.4.2099 RESEARCH ARTICLE Improved Detection of Helicobacter pylori Infection and Premalignant Gastric Mucosa Using Conventional White Light Source Gastroscopy
DOI:http://dx.doi.org/10.7314/APJCP.2016.17.4.2099 RESEARCH ARTICLE Improved Detection of Helicobacter pylori Infection and Premalignant Gastric Mucosa Using Conventional White Light Source Gastroscopy
Imaging Evaluation of Polyps. CT Colonography: Sessile Adenoma. Polyps, DALMs & Megacolon Objectives
 Polyps, DALMs & Megacolon: Pathology and Imaging of the Colon and Rectum Angela D. Levy and Leslie H. Sobin Washington, DC Drs. Levy and Sobin have indicated that they have no relationships which, in the
Polyps, DALMs & Megacolon: Pathology and Imaging of the Colon and Rectum Angela D. Levy and Leslie H. Sobin Washington, DC Drs. Levy and Sobin have indicated that they have no relationships which, in the
The Paris classification of colonic lesions
 The Paris classification of colonic lesions Training to improve the interobserver agreement among international experts Sascha van Doorn, MD, PhD-student in CRC-reserach group of Evelien Dekker Introduction
The Paris classification of colonic lesions Training to improve the interobserver agreement among international experts Sascha van Doorn, MD, PhD-student in CRC-reserach group of Evelien Dekker Introduction
Page 1. Is the Risk This High? Dysplasia in the IBD Patient. Dysplasia in the Non IBD Patient. Increased Risk of CRC in Ulcerative Colitis
 Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Expert panel observations
 Expert panel observations Professor Neil A Shepherd Gloucester and Cheltenham, UK Gloucestershire Cellular Pathology Laboratory Three big issues in BCSP pathology serrated pathology & what do we do about
Expert panel observations Professor Neil A Shepherd Gloucester and Cheltenham, UK Gloucestershire Cellular Pathology Laboratory Three big issues in BCSP pathology serrated pathology & what do we do about
Management of pt1 polyps. Maria Pellise
 Management of pt1 polyps Maria Pellise Early colorectal cancer Malignant polyp Screening programmes SM Invasive adenocar cinoma Advances in diagnostic & therapeutic endoscopy pt1 polyps 0.75 5.6% of large-bowel
Management of pt1 polyps Maria Pellise Early colorectal cancer Malignant polyp Screening programmes SM Invasive adenocar cinoma Advances in diagnostic & therapeutic endoscopy pt1 polyps 0.75 5.6% of large-bowel
A Significant Number of Sessile Serrated Adenomas Might Not Be Accurately Diagnosed in Daily Practice
 Gut and Liver, Vol. 4, No. 4, December 2010, pp. 498-502 original article A Significant Number of Sessile Serrated Adenomas Might Not Be Accurately Diagnosed in Daily Practice Soo Woong Kim*, Jae Myung
Gut and Liver, Vol. 4, No. 4, December 2010, pp. 498-502 original article A Significant Number of Sessile Serrated Adenomas Might Not Be Accurately Diagnosed in Daily Practice Soo Woong Kim*, Jae Myung
Malignant colorectal polyps: venous invasion and
 774 Gut, 1991,32, 774-778 Malignant colorectal polyps: venous invasion and successful treatment by endoscopic polypectomy Department of Pathology J M Geraghty Endoscopy Unit C B Williams and ICRF Colorectal
774 Gut, 1991,32, 774-778 Malignant colorectal polyps: venous invasion and successful treatment by endoscopic polypectomy Department of Pathology J M Geraghty Endoscopy Unit C B Williams and ICRF Colorectal
Clinicopathological Characteristics of Superficial Type
 Diagnostic and Therapeutic Endoscopy, 1995, Vol. 2, pp. 99-105 Reprints available directly from the publisher Photocopying permitted by license only (C) 1995 Harwood Academic Publishers GmbH Printed in
Diagnostic and Therapeutic Endoscopy, 1995, Vol. 2, pp. 99-105 Reprints available directly from the publisher Photocopying permitted by license only (C) 1995 Harwood Academic Publishers GmbH Printed in
General Session 7: Controversies in Screening and Surveillance in Colorectal Cancer
 General Session 7: Controversies in Screening and Surveillance in Colorectal Cancer Complexities of Pathological Assessment: Serrated Polyps/Adenomas Carolyn Compton, MD, PhD Professor of Life Sciences,
General Session 7: Controversies in Screening and Surveillance in Colorectal Cancer Complexities of Pathological Assessment: Serrated Polyps/Adenomas Carolyn Compton, MD, PhD Professor of Life Sciences,
Paris classification (2003) 삼성의료원내과이준행
 Paris classification (2003) 삼성의료원내과이준행 JGCA classification - Japanese Gastric Cancer Association - Type 0 superficial polypoid, flat/depressed, or excavated tumors Type 1 polypoid carcinomas, usually attached
Paris classification (2003) 삼성의료원내과이준행 JGCA classification - Japanese Gastric Cancer Association - Type 0 superficial polypoid, flat/depressed, or excavated tumors Type 1 polypoid carcinomas, usually attached
How to treat early gastric cancer? Endoscopy
 How to treat early gastric cancer? Endoscopy Presented by Pierre H. Deprez Institution Cliniques universitaires Saint-Luc, Brussels Université catholique de Louvain 2 3 4 5 6 Background Diagnostic or therapeutic
How to treat early gastric cancer? Endoscopy Presented by Pierre H. Deprez Institution Cliniques universitaires Saint-Luc, Brussels Université catholique de Louvain 2 3 4 5 6 Background Diagnostic or therapeutic
The Usefulness Of Narrow Band Imaging Endoscopy For The Real Time Characterization Of Colonic Lesions
 Acta Medica Marisiensis 2016;62(2):182-186 DOI: 10.1515/amma-2016-0004 RESEARCH ARTICLE The Usefulness Of Narrow Band Imaging Endoscopy For The Real Time Characterization Of Colonic Lesions Boeriu Alina
Acta Medica Marisiensis 2016;62(2):182-186 DOI: 10.1515/amma-2016-0004 RESEARCH ARTICLE The Usefulness Of Narrow Band Imaging Endoscopy For The Real Time Characterization Of Colonic Lesions Boeriu Alina
Clinico-Pathological Study of Endoscopic Gastric Biopsies
 Original Article Clinico-Pathological Study of Endoscopic Gastric Biopsies SumalathaKasturi, Raju Mulaka 2 Associate Professor Department of Pathology Chalmeda Anand Rao Institute of Medical Sciences Karimnagar,
Original Article Clinico-Pathological Study of Endoscopic Gastric Biopsies SumalathaKasturi, Raju Mulaka 2 Associate Professor Department of Pathology Chalmeda Anand Rao Institute of Medical Sciences Karimnagar,
Polypectomy and Local Resections of the Colorectum Structured Pathology Reporting Proforma
 Polypectomy and Local Resections of the Colorectum Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth
Polypectomy and Local Resections of the Colorectum Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth
Signet-ring cell carcinoma arising from a fundic gland polyp in the stomach
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i47.18044 World J Gastroenterol 2014 December 21; 20(47): 18044-18047 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i47.18044 World J Gastroenterol 2014 December 21; 20(47): 18044-18047 ISSN 1007-9327
Endoscopic Submucosal Dissection ESD
 Endoscopic Submucosal Dissection ESD Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated
Endoscopic Submucosal Dissection ESD Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated
HISTOPATHOLOGICAL STUDY OF ENDOSCOPIC BIOPSIES OF STOMACH
 HISTOPATHOLOGICAL STUDY OF ENDOSCOPIC BIOPSIES OF STOMACH Pages with reference to book, From 177 To 179 Javed Iqbal Kazi, Syed Mahmood Alam ( Departments of Pathology, Jinnah Postgraduate Medical Centre,
HISTOPATHOLOGICAL STUDY OF ENDOSCOPIC BIOPSIES OF STOMACH Pages with reference to book, From 177 To 179 Javed Iqbal Kazi, Syed Mahmood Alam ( Departments of Pathology, Jinnah Postgraduate Medical Centre,
Multifocal Adenocarcinomas Arising within a Gastric Inverted Hyperplastic Polyp
 The Korean Journal of Pathology 2012; 46: 387-391 CSE REPORT Multifocal denocarcinomas rising within a Gastric Inverted Hyperplastic Polyp Hyun-Soo Kim Eun-Jung Hwang 1 Jae-Young Jang 1 Juhie Lee 2 Youn
The Korean Journal of Pathology 2012; 46: 387-391 CSE REPORT Multifocal denocarcinomas rising within a Gastric Inverted Hyperplastic Polyp Hyun-Soo Kim Eun-Jung Hwang 1 Jae-Young Jang 1 Juhie Lee 2 Youn
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY
 OPEN ACCESS TEXTBOOK OF GENERAL SURGERY COLORECTAL POLYPS P Goldberg POLYP A polyp is a localised elevated lesion arising from a epithelial surface. If it has a stalk it is called a pedunculated polyp
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY COLORECTAL POLYPS P Goldberg POLYP A polyp is a localised elevated lesion arising from a epithelial surface. If it has a stalk it is called a pedunculated polyp
Romanian Journal of Morphology and Embryology 2006, 47(3):
 Romanian Journal of Morphology and Embryology 26, 7(3):239 23 ORIGINAL PAPER Predictive parameters for advanced neoplastic adenomas and colorectal cancer in patients with colonic polyps a study in a tertiary
Romanian Journal of Morphology and Embryology 26, 7(3):239 23 ORIGINAL PAPER Predictive parameters for advanced neoplastic adenomas and colorectal cancer in patients with colonic polyps a study in a tertiary
Incidence and Management of Hemorrhage after Endoscopic Removal of Colorectal Lesions
 Showa Univ J Med Sci 12(3), 253-258, September 2000 Original Incidence and Management of Hemorrhage after Endoscopic Removal of Colorectal Lesions Masaaki MATSUKAWA, Mototsugu FUJIMORI, Takahiko KOUDA,
Showa Univ J Med Sci 12(3), 253-258, September 2000 Original Incidence and Management of Hemorrhage after Endoscopic Removal of Colorectal Lesions Masaaki MATSUKAWA, Mototsugu FUJIMORI, Takahiko KOUDA,
High grade dysplasia of the gastric mucosa: a marker
 Gut, 1990,31,977-983 University Departments of Surgery M Lansdown D Johnston and Pathology P Quirke M F Dixon and Department of Medical Gastroenterology, General Infirmary, Leeds LS1 3EX A T R Axon Correspondence
Gut, 1990,31,977-983 University Departments of Surgery M Lansdown D Johnston and Pathology P Quirke M F Dixon and Department of Medical Gastroenterology, General Infirmary, Leeds LS1 3EX A T R Axon Correspondence
Spartan Medical Research Journal
 Spartan Medical Research Journal Research at Michigan State University College of Osteopathic Medicine Volume 2 Number 2 Winter, 2017 Pages 14-21 Title: Endoscopic Combined Snare-Forceps Technique for
Spartan Medical Research Journal Research at Michigan State University College of Osteopathic Medicine Volume 2 Number 2 Winter, 2017 Pages 14-21 Title: Endoscopic Combined Snare-Forceps Technique for
Predict, Resect and discard : Yes we can! (at least in some hands)
 Diminutive polyps : Real time endoscopic histology Predict, Resect and discard : Yes we can! (at least in some hands) Robert Benamouzig Hôpital Avicenne AP-HP & Paris 13 University France Why it is important?
Diminutive polyps : Real time endoscopic histology Predict, Resect and discard : Yes we can! (at least in some hands) Robert Benamouzig Hôpital Avicenne AP-HP & Paris 13 University France Why it is important?
Fundic gland polyps, initially described in association with
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:849 854 No Association Between Gastric Fundic Gland Polyps and Gastrointestinal Neoplasia in a Study of Over 100,000 Patients ROBERT M. GENTA,*, CHRISTOPHER
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:849 854 No Association Between Gastric Fundic Gland Polyps and Gastrointestinal Neoplasia in a Study of Over 100,000 Patients ROBERT M. GENTA,*, CHRISTOPHER
YES NO UNKNOWN. Stage I: Rule-Out Dashboard ACTIONABILITY PENETRANCE SIGNIFICANCE/BURDEN OF DISEASE NEXT STEPS. YES ( 1 of above)
 Stage I: Rule-Out Dashboard GENE/GENE PANEL: SMAD4, BMPR1A DISORDER: Juvenile Polyposis Syndrome HGNC ID: 6670, 1076 OMIM ID: 174900, 175050 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource,
Stage I: Rule-Out Dashboard GENE/GENE PANEL: SMAD4, BMPR1A DISORDER: Juvenile Polyposis Syndrome HGNC ID: 6670, 1076 OMIM ID: 174900, 175050 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource,
Endoscopic Corner CASE 1. Kimtrakool S Aniwan S Linlawan S Muangpaisarn P Sallapant S Rerknimitr R
 170 Endoscopic Corner Kimtrakool S Aniwan S Linlawan S Muangpaisarn P Sallapant S Rerknimitr R CASE 1 A 54-year-old woman underwent a colorectal cancer screening. Her fecal immunochemical test was positive.
170 Endoscopic Corner Kimtrakool S Aniwan S Linlawan S Muangpaisarn P Sallapant S Rerknimitr R CASE 1 A 54-year-old woman underwent a colorectal cancer screening. Her fecal immunochemical test was positive.
Expression of the GLUT1 and p53 Protein in Atypical Mucosal Lesions Obtained from Gastric Biopsy Specimens
 The Korean Journal of Pathology 2006; 40: 32-8 Expression of the GLUT1 and p53 Protein in Atypical Mucosal Lesions Obtained from Gastric Biopsy Specimens In Gu Do Youn Wha Kim Yong-Koo Park Department
The Korean Journal of Pathology 2006; 40: 32-8 Expression of the GLUT1 and p53 Protein in Atypical Mucosal Lesions Obtained from Gastric Biopsy Specimens In Gu Do Youn Wha Kim Yong-Koo Park Department
EMR, ESD and Beyond. Peter Draganov MD. Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida
 EMR, ESD and Beyond Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated by Endoscopy
EMR, ESD and Beyond Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated by Endoscopy
proposed Vienna classification of gastrointestinal
 Gut 2;47:251 255 251 For list of authors ayliations, please see appendix. Correspondence to: Dr R Schlemper, Department of Internal Medicine, Fukuoka University School of Medicine, 7-45-1 Nanakuma, Jonan-ku,
Gut 2;47:251 255 251 For list of authors ayliations, please see appendix. Correspondence to: Dr R Schlemper, Department of Internal Medicine, Fukuoka University School of Medicine, 7-45-1 Nanakuma, Jonan-ku,
Upper GIT IV Gastric cancer
 Upper GIT IV Gastric cancer Luigi Tornillo PathoBasic 23.10.2014 Pathology Introduction Classification Morphogenesis Problems Intraepithelial neoplasia Surveillance EGJ Predictive factors Gastric cancer
Upper GIT IV Gastric cancer Luigi Tornillo PathoBasic 23.10.2014 Pathology Introduction Classification Morphogenesis Problems Intraepithelial neoplasia Surveillance EGJ Predictive factors Gastric cancer
Pathology in Slovenian CRC screening programme: Organisation and quality assurance. Snježana Frković Grazio and Matej Bračko
 Pathology in Slovenian CRC screening programme: Organisation and quality assurance Snježana Frković Grazio and Matej Bračko June 2009 to December 2013 (first three rounds) 33 969 colonoscopies were performed
Pathology in Slovenian CRC screening programme: Organisation and quality assurance Snježana Frković Grazio and Matej Bračko June 2009 to December 2013 (first three rounds) 33 969 colonoscopies were performed
Dysplasia 4/19/2017. How do I practice Chromoendoscopy for Surveillance of Colitis? SCENIC: Polypoid Dysplasia in UC. Background
 SCENIC: Polypoid in UC Definition How do I practice for Surveillance of Colitis? Themos Dassopoulos, M.D. Director, BSW Center for IBD Themistocles.Dassopoulos@BSWHealth.org Tel: 469-800-7189 Cell: 314-686-2623
SCENIC: Polypoid in UC Definition How do I practice for Surveillance of Colitis? Themos Dassopoulos, M.D. Director, BSW Center for IBD Themistocles.Dassopoulos@BSWHealth.org Tel: 469-800-7189 Cell: 314-686-2623
Colonic adenomas-a colonoscopy survey
 Gut, 1979, 20, 240-245 Colonic adenomas-a colonoscopy survey P. E. GILLESPIE, T. J. CHAMBERS, K. W. CHAN, F. DORONZO, B. C. MORSON, AND C. B. WILLIAMS From St Mark's Hospital, City Road, London SUMMARY
Gut, 1979, 20, 240-245 Colonic adenomas-a colonoscopy survey P. E. GILLESPIE, T. J. CHAMBERS, K. W. CHAN, F. DORONZO, B. C. MORSON, AND C. B. WILLIAMS From St Mark's Hospital, City Road, London SUMMARY
Colon Cancer Screening. Layth Al-Jashaami, MD GI Fellow, PGY 4
 Colon Cancer Screening Layth Al-Jashaami, MD GI Fellow, PGY 4 -Colorectal cancer (CRC) is a common and lethal cancer. -It has the highest incidence among GI cancers in the US, estimated to be newly diagnosed
Colon Cancer Screening Layth Al-Jashaami, MD GI Fellow, PGY 4 -Colorectal cancer (CRC) is a common and lethal cancer. -It has the highest incidence among GI cancers in the US, estimated to be newly diagnosed
S rectal polyps that show atypia, adenocarcinoma,
 HOW RELIABLE IS BIOPSY OF RECTAL POLYPS? A Clinical and Morphological Study of 107 Cases C. ALEXANDER HELLWIG, M.D., AND EDGARD BARBOSA. nr.d. OME OVERLY cautious pathologists call all S rectal polyps
HOW RELIABLE IS BIOPSY OF RECTAL POLYPS? A Clinical and Morphological Study of 107 Cases C. ALEXANDER HELLWIG, M.D., AND EDGARD BARBOSA. nr.d. OME OVERLY cautious pathologists call all S rectal polyps
Primary mucinous adenocarcinoma developing in an ileostomy stoma
 Gut, 1988, 29, 1607-1612 Primary mucinous adenocarcinoma developing in an ileostomy stoma P J SMART, S SASTRY, AND S WELLS From the Departments of Histopathology and Surgery, Bolton General Hospital, Fan
Gut, 1988, 29, 1607-1612 Primary mucinous adenocarcinoma developing in an ileostomy stoma P J SMART, S SASTRY, AND S WELLS From the Departments of Histopathology and Surgery, Bolton General Hospital, Fan
White Rose Research Online URL for this paper: Version: Accepted Version
 This is a repository copy of Patients with Endoscopically Visible Polypoid Adenomatous Lesions Within the Extent of Ulcerative Colitis Have an Increased Risk of Colorectal Cancer Despite Endoscopic Resection.
This is a repository copy of Patients with Endoscopically Visible Polypoid Adenomatous Lesions Within the Extent of Ulcerative Colitis Have an Increased Risk of Colorectal Cancer Despite Endoscopic Resection.
Endoscopic techniques for surveillance and treatment of FAP
 Endoscopic techniques for surveillance and treatment of FAP Evelien Dekker MD PhD Department of Gastroenterology & Hepatology Academic Medical Center Amsterdam The Netherlands FAP: endoscopic surveillance
Endoscopic techniques for surveillance and treatment of FAP Evelien Dekker MD PhD Department of Gastroenterology & Hepatology Academic Medical Center Amsterdam The Netherlands FAP: endoscopic surveillance
Update on Colonic Serrated (and Conventional) Adenomatous Polyps
 Update on Colonic Serrated (and Conventional) Adenomatous Polyps Maui, HI 2018 Robert D. Odze, MD, FRCPC Chief, Division of GI Pathology Professor of Pathology Brigham and Women s Hospital Harvard Medical
Update on Colonic Serrated (and Conventional) Adenomatous Polyps Maui, HI 2018 Robert D. Odze, MD, FRCPC Chief, Division of GI Pathology Professor of Pathology Brigham and Women s Hospital Harvard Medical
Stage 4 gastric adenocarcinoma icd 10
 > Stage 4 gastric adenocarcinoma icd 10 stage iii; Carcinoma of colon, stage iv; Colon cancer metastatic to unspecified site; Hereditary nonpolyposis colon cancer; Malignant tumor of colon; Metastasis.
> Stage 4 gastric adenocarcinoma icd 10 stage iii; Carcinoma of colon, stage iv; Colon cancer metastatic to unspecified site; Hereditary nonpolyposis colon cancer; Malignant tumor of colon; Metastasis.
Gastric atrophy: use of OLGA staging system in practice
 Gastroenterology and Hepatology From Bed to Bench. 2016 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE Gastric atrophy: use of OLGA staging system in practice Mahsa
Gastroenterology and Hepatology From Bed to Bench. 2016 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE Gastric atrophy: use of OLGA staging system in practice Mahsa
Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy
 Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy Authors: Dr Gordon Armstrong, Dr Sue Pritchard 1. General Comments 1.1 Cancer reporting: Biopsies
Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy Authors: Dr Gordon Armstrong, Dr Sue Pritchard 1. General Comments 1.1 Cancer reporting: Biopsies
Appendix 4: WHO Classification of Tumours of the pancreas 17
 S3.01 The WHO histological tumour type must be recorded. CS3.01a The histological type of the tumour should be recorded based on the current WHO classification 17 (refer to Appendices 4-7). Appendix 4:
S3.01 The WHO histological tumour type must be recorded. CS3.01a The histological type of the tumour should be recorded based on the current WHO classification 17 (refer to Appendices 4-7). Appendix 4:
Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care
 Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
FINAL HISTOLOGICAL DIAGNOSIS: Villo-adenomatous polyp with in-situ-carcinomatous foci (involving both adenomatous and villous component).
 SOLITARY VILLO ADENOMATOUS POLYP WITH CARCINOMATOUS CHANGES RECTUM: A Divvya B 1, M. Valluvan 2, Rehana Tippoo 3, P. Viswanathan 4, R. Baskaran 5 HOW TO CITE THIS ARTICLE: Divvya B, M. Valluvan, Rehana
SOLITARY VILLO ADENOMATOUS POLYP WITH CARCINOMATOUS CHANGES RECTUM: A Divvya B 1, M. Valluvan 2, Rehana Tippoo 3, P. Viswanathan 4, R. Baskaran 5 HOW TO CITE THIS ARTICLE: Divvya B, M. Valluvan, Rehana
The surface mucous cells and the cardiac and pyloric glands secrete mucus which protects the stomach from self-digestion.
 PATHOLOGY OF THE STOMACH Stomach mucosa Gastric mucosa is covered by a layer of mucus. The mucosal glands comprise the cardiac glands, the fundic glands in the fundus and body of the stomach, and the pyloric
PATHOLOGY OF THE STOMACH Stomach mucosa Gastric mucosa is covered by a layer of mucus. The mucosal glands comprise the cardiac glands, the fundic glands in the fundus and body of the stomach, and the pyloric
Principles of diagnosis, work-up and therapy The Gastroenterologist s role
 Principles of diagnosis, work-up and therapy The Gastroenterologist s role Dr. Christos G. Toumpanakis MD PhD FRCP Consultant in Gastroenterology/Neuroendocrine Tumours Hon. Senior Lecturer University
Principles of diagnosis, work-up and therapy The Gastroenterologist s role Dr. Christos G. Toumpanakis MD PhD FRCP Consultant in Gastroenterology/Neuroendocrine Tumours Hon. Senior Lecturer University
WEO CRC SC Meeting. Barcelona, Spain October 23, 2015
 WEO CRC SC Meeting Barcelona, Spain October 23, 2015 Identification of serrated polyposis syndrome in the context of population-based CRC screening programs Evelien Dekker Academic Medical Center Amsterdam,
WEO CRC SC Meeting Barcelona, Spain October 23, 2015 Identification of serrated polyposis syndrome in the context of population-based CRC screening programs Evelien Dekker Academic Medical Center Amsterdam,
Magnifying Endoscopy and Chromoendoscopy of the Upper Gastrointestinal Tract
 Magnifying Endoscopy and Chromoendoscopy of the Upper Gastrointestinal Tract Alina M.Boeriu 1, Daniela E.Dobru 1, Simona Mocan 2 1) Department of Gastroenterology, University of Medicine and Pharmacy;
Magnifying Endoscopy and Chromoendoscopy of the Upper Gastrointestinal Tract Alina M.Boeriu 1, Daniela E.Dobru 1, Simona Mocan 2 1) Department of Gastroenterology, University of Medicine and Pharmacy;
Diagnostic accuracy of pit pattern and vascular pattern in colorectal lesions
 Diagnostic accuracy of pit pattern and vascular pattern in colorectal lesions Digestive Disease Center, Showa University Northern Yokohama Hospital Department of Pathology Yoshiki Wada, Shin-ei Kudo, Hiroshi
Diagnostic accuracy of pit pattern and vascular pattern in colorectal lesions Digestive Disease Center, Showa University Northern Yokohama Hospital Department of Pathology Yoshiki Wada, Shin-ei Kudo, Hiroshi
LIST OF ABBREVIATIONS
 Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Adenomatosis of small intestine: case report
 Adenomatosis of small intestine: case report T NAKAMURA, H KIMURA, G NAKANO From the Department of Surgery, Gunma University School of Medicine, Maebashi, Japan J Clin Pathol 1986;39:981-986 SUMMARY A
Adenomatosis of small intestine: case report T NAKAMURA, H KIMURA, G NAKANO From the Department of Surgery, Gunma University School of Medicine, Maebashi, Japan J Clin Pathol 1986;39:981-986 SUMMARY A
Quality Measures In Colonoscopy: Why Should I Care?
 Quality Measures In Colonoscopy: Why Should I Care? David Greenwald, MD, FASGE Professor of Clinical Medicine Albert Einstein College of Medicine Montefiore Medical Center Bronx, New York ACG/ASGE Best
Quality Measures In Colonoscopy: Why Should I Care? David Greenwald, MD, FASGE Professor of Clinical Medicine Albert Einstein College of Medicine Montefiore Medical Center Bronx, New York ACG/ASGE Best
Sedated gastroscopy improves detection of gastric polyps
 3116 Sedated gastroscopy improves detection of gastric polyps MENG JUN CHEN, WEI WU, SHUANG PAN, CHUN JING LIN, LE MEI DONG, ZHOU FENG CHEN, JIAN SHENG WU and ZHI MING HUANG Department of Gastroenterology,
3116 Sedated gastroscopy improves detection of gastric polyps MENG JUN CHEN, WEI WU, SHUANG PAN, CHUN JING LIN, LE MEI DONG, ZHOU FENG CHEN, JIAN SHENG WU and ZHI MING HUANG Department of Gastroenterology,
GI Polyp syndromes in children. Screening and surveillance, surgery.
 Dr Warren Hyer Consultant Paediatric Gastroenterologist St Mark s Hospital, UK GI Polyp syndromes in children Screening and surveillance, surgery. No conflict of interests to declare Objectives Understand
Dr Warren Hyer Consultant Paediatric Gastroenterologist St Mark s Hospital, UK GI Polyp syndromes in children Screening and surveillance, surgery. No conflict of interests to declare Objectives Understand
Latest Endoscopic Guidelines for FAP, HNPCC, IBD, and the General Population
 Latest Endoscopic Guidelines for FAP, HNPCC, IBD, and the General Population David T. Rubin, M.D. Assistant Professor of Medicine Inflammatory Bowel Disease Center MacLean Center for Clinical Medical Ethics
Latest Endoscopic Guidelines for FAP, HNPCC, IBD, and the General Population David T. Rubin, M.D. Assistant Professor of Medicine Inflammatory Bowel Disease Center MacLean Center for Clinical Medical Ethics
Peutz Jegher's Syndrome (Gastro-intestinal Polyposis) and Its Complications
 Peutz Jegher's Syndrome (Gastro-intestinal Polyposis) and Its Complications Pages with reference to book, From 154 To 155 Zakiuddin G. Oonwala, Sina Aziz ( Department of Surgery, Dow Medical College and
Peutz Jegher's Syndrome (Gastro-intestinal Polyposis) and Its Complications Pages with reference to book, From 154 To 155 Zakiuddin G. Oonwala, Sina Aziz ( Department of Surgery, Dow Medical College and
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus
 Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Diagnosis and management of gastric dysplasia
 REVIEW Korean J Intern Med 2016;31:201-209 Diagnosis and management of gastric dysplasia Jae Kyu Sung Department of Internal Medicine, Chungnam National University School of Medicine, Daejeon, Korea Received
REVIEW Korean J Intern Med 2016;31:201-209 Diagnosis and management of gastric dysplasia Jae Kyu Sung Department of Internal Medicine, Chungnam National University School of Medicine, Daejeon, Korea Received
Bowel obstruction and tumors
 Bowel obstruction and tumors Intestinal Obstruction Obstruction of the GI tract may occur at any level, but the small intestine is most often involved because of its relatively narrow lumen. Causes: Hernias
Bowel obstruction and tumors Intestinal Obstruction Obstruction of the GI tract may occur at any level, but the small intestine is most often involved because of its relatively narrow lumen. Causes: Hernias
colorectal cancer Colorectal cancer hereditary sporadic Familial 1/12/2018
 colorectal cancer Adenocarcinoma of the colon and rectum is the third most common site of new cancer cases and deaths in men (following prostate and lung or bronchus cancer) and women (following breast
colorectal cancer Adenocarcinoma of the colon and rectum is the third most common site of new cancer cases and deaths in men (following prostate and lung or bronchus cancer) and women (following breast
Giant Brunner s Gland Hamartoma of the Duodenal Bulb Presenting with Upper Gastrointestinal Bleeding and Obstruction
 CSE REPORT Clin Endosc 2016;49:570-574 https://doi.org/10.5946/ce.2016.022 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open ccess Giant runner s Gland Hamartoma of the Duodenal ulb Presenting with Upper
CSE REPORT Clin Endosc 2016;49:570-574 https://doi.org/10.5946/ce.2016.022 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open ccess Giant runner s Gland Hamartoma of the Duodenal ulb Presenting with Upper
What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you)
 What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you) Jonathan N. Glickman MD PhD Director, GI Pathology, Caris Diagnostics, Newton, MA Associate Professor of Pathology,
What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you) Jonathan N. Glickman MD PhD Director, GI Pathology, Caris Diagnostics, Newton, MA Associate Professor of Pathology,
Colon Polyp Morphology on Double-Contrast Barium Enema: Its Pathologic Predictive Value
 965 David J. Ott 1 David W. Gelfand 1 Wallace C. Wu 2 Deborah S. Ablin 1-3 Received March 21, 1983; accepted after revision July 8, 1983. 'Department of Radiology, Bowman Gray School of Medicine, Winston-Salem,
965 David J. Ott 1 David W. Gelfand 1 Wallace C. Wu 2 Deborah S. Ablin 1-3 Received March 21, 1983; accepted after revision July 8, 1983. 'Department of Radiology, Bowman Gray School of Medicine, Winston-Salem,
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus
 New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
malignant polyp Daily Challenges in Digestive Endoscopy for Endoscopists and Endoscopy Nurses BSGIE Annual Meeting 18/09/2014 Mechelen
 Plan Incidental finding of a malignant polyp 1. What is a polyp malignant? 2. Role of the pathologist and the endoscopist 3. Quantitative and qualitative risk assessment 4. How to decide what to do? Hubert
Plan Incidental finding of a malignant polyp 1. What is a polyp malignant? 2. Role of the pathologist and the endoscopist 3. Quantitative and qualitative risk assessment 4. How to decide what to do? Hubert
Endoscopic Corner CASE 1. Sirimontaporn N Klaikaew N Imraporn B Rerknimitr R
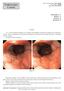 Endoscopic Corner Sirimontaporn N, et al. THAI J GASTROENTEROL 2010 Vol. 11 No. 3 Sept. - Dec. 2010 171 Sirimontaporn N Klaikaew N Imraporn B Rerknimitr R CASE 1 A 47- year-old female presented to the
Endoscopic Corner Sirimontaporn N, et al. THAI J GASTROENTEROL 2010 Vol. 11 No. 3 Sept. - Dec. 2010 171 Sirimontaporn N Klaikaew N Imraporn B Rerknimitr R CASE 1 A 47- year-old female presented to the
Gastric polyps - classification and diagnostic
 Gastric polyps - classification and diagnostic Poster No.: C-0684 Congress: ECR 2017 Type: Educational Exhibit Authors: A. I. Georgescu, A.-M. Bratu, C. Zaharia; Bucharest/RO Keywords: Gastrointestinal
Gastric polyps - classification and diagnostic Poster No.: C-0684 Congress: ECR 2017 Type: Educational Exhibit Authors: A. I. Georgescu, A.-M. Bratu, C. Zaharia; Bucharest/RO Keywords: Gastrointestinal
A Histomorphological Study of Polyps And Polypoid Lesions Of Gastrointestinal Tract From South India
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 12 Ver. 1 (December. 2018), PP 25-30 www.iosrjournals.org A Histomorphological Study of Polyps
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 12 Ver. 1 (December. 2018), PP 25-30 www.iosrjournals.org A Histomorphological Study of Polyps
University Mainz. Early Gastric Cancer. Ralf Kiesslich. Johannes Gutenberg University Mainz, Germany. Early Gastric Cancer 15.6.
 Ralf Kiesslich Johannes Gutenberg University Mainz, Germany DIAGNOSIS Unmask lesions - Chromoendoscopy -NBI Red flag technology - Autofluorescence Surface and detail analysis - Magnifying endoscopy - High
Ralf Kiesslich Johannes Gutenberg University Mainz, Germany DIAGNOSIS Unmask lesions - Chromoendoscopy -NBI Red flag technology - Autofluorescence Surface and detail analysis - Magnifying endoscopy - High
