Short-Term Restaging of Patients with Non-small Cell Lung Cancer Receiving Chemotherapy
|
|
|
- Ethelbert Cross
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Short-Term Restaging of Patients with Non-small Cell Lung Cancer Receiving Chemotherapy John F. Bruzzi, FFRRCSI,* Mylene Truong, MD,* Ralph Zinner, MD Jeremy J. Erasmus, MD,* Bradley Sabloff, MD,* and Reginald Munden, MD* Objective: To determine whether computed tomography (CT) performed within a month of receiving chemotherapy is useful in assessing response among patients with non-small cell lung cancer (NSCLC). Patients and Methods: Consecutive patients receiving chemotherapy for NSCLC who underwent short-term CT restaging between April 2001 and June 2005 were included in the study. Serial CT scans were performed within 31 days (mean, 24 days; range, 9-31 days) after receiving chemotherapy for all patients. Tumors were measured in consensus by two diagnostic radiologists. Tumor response was assessed using uni-dimensional tumor measurements according to Response Evaluation Criteria in Solid Tumors criteria. Results: There were 57 patients in the study (30 men, 27 women; mean age, 63 years; age range, years). Tumor histology included adenocarcinoma (n 30), squamous cell carcinoma (n 17), and NSCLC otherwise unspecified (n 10). Clinical tumor, node, metastasis stage was stage II (n 2), stage III (n 11), and stage IV (n 44). A significant change in tumor size was observed in eight patients (14%), with tumor regression in two (3%) and progression in six (11%). For these patients, CT scans were performed within 31 days (mean, 25 days; range, days). Among the six patients with tumor progression, early detection of therapeutic failure resulted in a change or a discontinuation of chemotherapy for five. Conclusion: Early restaging CT is useful in evaluating therapeutic response among patients with NSCLC and may allow the institution of more appropriate therapy. Key Words: Lung cancer, Staging, Restaging, CT, Chemotherapy. (J Thorac Oncol. 2006;1: ) Lung cancer is the leading cause of cancer-related deaths in both men and women in the United States and commonly presents with advanced disease. 1 Chemotherapy has been shown to increase the 5-year survival rate among patients with non-small cell lung cancer when added to surgery or 1 Departments of *Diagnostic Imaging and Head and Neck Thoracic Oncology, M.D. Anderson Cancer Center, Houston, Texas Address for correspondence: John Bruzzi, Department of Diagnostic Imaging, M.D. Anderson Cancer Center, Unit 57, 1515 Holcombe Blvd., Houston, TX jbruzzi@mdanderson.org Copyright 2006 by the International Association for the Study of Lung Cancer ISSN: /06/ radiation for patients who have local or regional disease. 2 9 In advanced disease, as a single modality, chemotherapy prolongs survival and improves quality of life as first- and second-line therapy. 7 9 However, after the initiation of chemotherapy, tumor progression can occur in up to one third of patients. 10 Early determination of this therapeutic failure is important in patient management and assists clinical decisions concerning discontinuation of ineffective treatment and institution of alternative therapy. However, the prevailing standard assessment of therapeutic response often precludes an early prediction of tumor response. In this regard, tumor response is usually determined using World Health Organization (WHO) 11 or Response Evaluation Criteria in Solid Tumors (RECIST) 12 criteria and is typically based on computed tomographic (CT) imaging with serial measurements of tumor size performed at 6- to 8-week intervals. The objective of this study was to assess whether changes in tumor size measured on serial CT scans performed earlier than the standard convention would allow an assessment of therapeutic response among patients with non-small cell lung cancer (NSCLC). PATIENTS AND METHODS We performed a retrospective review of CT scans from consecutive patients with NSCLC receiving chemotherapy at our institution between April 2001 and June Patients were eligible for inclusion into the study if they were receiving chemotherapy for histologically proven primary NSCLC and if they had undergone early restaging CT imaging of the chest at an interval of no longer than 31 days at least once while on treatment. We recorded demographic characteristics, tumor histology, tumor stage and grade, chemotherapy, and subsequent follow-up. The study was approved by our Institutional Review Board. All CT scans were performed on a helical (GE Hi- Speed, GE Healthcare, Milwaukee, WI) or multi-slice CT scanner (GE Lightspeed, GE Healthcare), with a collimation of 7-mm (single-slice helical scans) or between 1.25 and 2.5-mm (multi-slice scans). Axial images were reconstructed with a slice thickness of 1.25 to 7 mm. All scans were performed with IV contrast (300 mg/dl non-ionic iodinated contrast, injected at 3 4 ml/s). For each patient, the initial CT scan (scan 1) and the follow-up scan performed less than 31 days later (scan 2) were reviewed on a dedicated workstation (isite; Stentor Inc, Brisbane, CA) by two chest radi- Journal of Thoracic Oncology Volume 1, Number 5, June
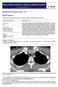
2 Bruzzi et al. Journal of Thoracic Oncology Volume 1, Number 5, June 2006 ologists who interpreted the scans together. All images were reviewed in both mediastinal soft tissue windows (center, 55; width, 500) and parenchymal lung windows (center, 600; width, 1500). Tumor measurements were made on two serial CT scans performed at an interval of less than or equal to 31 days (scan 1 and scan 2) that had been requested for restaging purposes while the patient was receiving chemotherapy for the treatment of NSCLC. On each scan, tumor measurements were performed in consensus by two radiologists at a joint interpretation session using electronic calipers and according to RECIST criteria. 12 Up to 10 tumor targets were identified on each scan (with a maximum of five in each organ) and measured along their longest axial diameter, and the sum of these measurements was recorded for each patient. Tumor measurements were performed using either soft tissue or lung window settings, according to the anatomical location of the tumor target and the visibility of the lesion: nodules or masses abutting the mediastinum or chest wall were measured on mediastinal soft tissue windows to accurately delineate them from normal adjacent soft tissue, whereas lesions surrounded entirely by lung parenchyma were measured on lung windows. The same window setting was used for both scans (scans 1 and 2) for each patient. Patients were excluded from the study if the tumor targets were not measurable, if the largest tumor target was smaller than 10 mm in diameter, or if the tumor was obscured by surrounding atelectasis or consolidation. Total tumor size was determined by calculating the sum of the measurements of the longest axial diameters of each of the tumor targets, according to RECIST criteria. Significant tumor progression and regression were defined by an overall increase of at least 20% or decrease of at least 30% in the total tumor size, respectively. A change in total tumor size of less than this was defined as stable disease. Statistical Analysis Results were documented using descriptive analyses of frequencies, means, and medians. Differences between patients who showed a significant change in tumor size (progression or partial response) and patients with stable disease were analyzed using Fisher s exact test. TABLE 1. Patient and tumor characteristics Patient characteristics Age (yr) 63 (37 85) Sex 30 men, 27 women Scan interval (days) 24 (9 31) Tumor pathology Adenocarcinoma 30 (52.5) Squamous cell carcinoma 17 (30) NSLC (NOS*) 10 (17.5) Tumor stage Stage I 0 Stage II 2 (4) Stage III 11 (19) Stage IV 44 (77) Current chemotherapy First-line 23 (40) Second-line 10 (18) More than second-line 24 (42) Chemotherapy type Platinum-based 18 (31) Single-agent tyrosine kinase inhibitor 16 (28) Combination tyrosine kinase inhibitor 6 (11) Other 17 (30) Total tumor size on first CT scan (cm) Mean 7.3 Median 6.2 Range Values are n (%) or mean (range). NOS, not otherwise specified; NSCLC, non-small cell lung cancer; CT, computed tomography. RESULTS A total of 57 patients with NSCLC who were receiving chemotherapy were eligible for inclusion in the study (30 men, 27 women; mean age, 63 years; age range, years). Table 1 summarizes the characteristics of the patients, tumor histology, grade, stage, and treatment. Most patients (n 42, 74%) had metastatic disease at the time of serial CT scanning and were undergoing definitive chemotherapy. The remaining patients (n 15, 26%) were receiving induction neoadjuvant therapy before anticipated surgical resection. Total tumor size at baseline (scan 1) as measured by RECIST criteria ranged between 1.1 and 30.9 cm (mean, 7.3 cm). The mean time interval between serial CT scans (scans 1 and 2) for each patient was 24 days (median, 24 days; range, 9 31 days). Indications for early follow-up CT scans included: routine restaging after chemotherapy (n 39), suspected pulmonary embolism (n 4), unexplained dyspnea (n 4), suspected pneumonia (n 3), investigation of abnormalities on chest radiographs (n 2), shoulder-tip pain (n 1), abdominal pain (n 1), lethargy (n 1), evaluation of a pleural effusion (n 1), and in the course of assessment of hematuria (n 1). Eight patients had suspected tumor progression either on clinical grounds (n 6) or because of chest radiograph abnormalities (n 2); there were no specific signs suggestive of disease progression among the remaining 49 patients. The frequency and magnitude of tumor response or progression during this time interval was assessed for each patient (Table 2). A total of eight patients (14%) demonstrated significant interval changes in total tumor size during the time period between the two CT scans. Among these patients, CT scans were performed between 17 and 31 days (mean, 25 days). In two patients with metastatic adenocarcinoma, tumor size decreased by more than 30% (mean, 36%; range, 32 40%) over a period of 20 to 24 days (mean, 22 days) (Fig. 1), allowing chemotherapy to be continued with greater confidence. In the six other patients, significant increases in tumor size were measured (mean, 26%; range, 21 33%), occurring over periods of 17 days to 31 days (mean, 26 days) (Figs. 2 and 3). The histology of these tumors was adenocarcinoma (n 3), squamous cell carcinoma (n 2), and NSCLC not otherwise specified (n 1). For four of these patients (two with adenocarcinoma, two with squamous cell carcinoma), histology demonstrated 426 Copyright 2006 by the International Association for the Study of Lung Cancer
3 Journal of Thoracic Oncology Volume 1, Number 5, June 2006 Short-Term Restaging of Non-small Cell Lung Cancer TABLE 2. interval Tumor response during short-term follow-up Change in total tumor size Patients (n 57) Magnitude of tumor response (%) Partial response 30% reduction in size 2 (3) 36 (32-40) Stable disease 20 30% reduction in size 1 (2) % reduction in size 6 (11) 13 (10-18) 10% change in size 34 (59) 2 (-9 6) 10 20% increase in size 8 (14) 13 (10-15) Tumor progression 20% increase in size 6 (11) 26 (21-33) Values are n(%) or n(range). FIGURE 3. The patient was a 60-year-old man with metastatic non-small cell lung cancer. A, CT image (mediastinal windows) shows an 11.2-cm left hilar mass causing marked compression of the left main pulmonary artery (arrow). B, CT image (mediastinal windows) 31 days after chemotherapy shows interval enlargement of primary mass measured at 12.2 cm and causing more marked compression of the left main pulmonary artery (arrow). difference was not statistically significant when compared with patients without metastases (p 0.3, Fisher s exact test). Similarly, tumor progression at short-term follow-up did not vary significantly with respect to first-line chemotherapy versus second-line or more chemotherapy (p 0.4). FIGURE 1. The patient was a 37-year-old man with poorly differentiated metastatic adenocarcinoma. A, CT image (mediastinal windows) before treatment shows necrotic primary tumor in left upper lobe (arrow). Mass measured 30.1 mm in longest axis. B, CT image (mediastinal windows) 20 days after chemotherapy shows significant interval reduction in size of primary mass (arrow) to 18 mm in longest axis. FIGURE 2. The patient was an 85-year-old woman with metastatic adenocarcinoma. A, CT image (mediastinal window) before treatment shows irregular 6.4-cm soft tissue mass in the left upper lobe abutting mediastinum. B, CTim- age 28 days after chemotherapy shows interval enlargement of mass to 7.5 cm, which now has a larger interface with the mediastinum. poorly differentiated tumors. For five of these patients, chemotherapy was discontinued (n 4) or changed to a different regimen (n 1) as a result of the CT findings. The sixth patient died shortly after scan 2 as a result of disease progression. Table 3 summarizes the changes in tumor size according to patient, tumor, and treatment characteristics. Tumor progression at short-term follow-up was observed only among patients with metastatic disease (n 6, 14%), but the DISCUSSION Therapeutic response to chemotherapy among patients with NSCLC can be determined clinically, biochemically, or by surgical pathologic restaging or image-based serial measurements of tumor size. 12,13 Because tumor measurements before and after chemotherapy are usually considered preferable in the determination of therapeutic effectiveness, patients are typically evaluated using serial CT scans. Based on growth rates/doubling times of NSCLC, it is generally accepted that CT is of limited use in the early assessment of therapeutic response among patients with NSCLC treated with chemotherapy. Consequently, CT is typically performed at intervals of 6 weeks to 2 months in most current protocols, a time period that corresponds to an assessment of therapeutic response after at least two cycles of conventional chemotherapy. However, earlier detection of tumor growth in patients with tumors that are resistant to chemotherapy is of potential benefit because it allows the timely discontinuation or change of chemotherapy regimens that are ineffective and can help to avoid a delay in the administration of potentially effective second- or third-line chemotherapy agents. Conventional restaging methods using CT scanning depend on anatomical changes in tumor size. However, accurate determination of response may require functional and molecular techniques that assess metabolism, growth kinetics, angiogenesis growth factors, tumor cell markers, and in vivo genetic alterations and gene expression. 14 Recently, positron emission tomography (PET) imaging using the glucose analogue [18F]-fluoro-2-deoxy-D-glucose (FDG), has been advocated as an alternative to anatomic imaging in the assessment of therapeutic response. It has been reported that FDG-PET imaging can be used to determine therapeutic response earlier and more accurately than CT However, a poor understanding of the underlying cellular mechanisms, absence of consensus concerning optimal time to image for Copyright 2006 by the International Association for the Study of Lung Cancer 427
4 Bruzzi et al. Journal of Thoracic Oncology Volume 1, Number 5, June 2006 TABLE 3. Characteristics of patients and tumors according to response Patients Characteristic Partial response Stable disease Tumor progression Patients (n 57) 2 (3) 49 (86) 6 (11) Age (yr) 58 (37 79) 63 (42 81) 64 (58 69) Men (n 30) 1 (2) 24 (42) 1 (2) Women (n 27) 1 (2) 25 (40) 5 (5) Follow-up interval (days) 22 (20 24) 23 (9 31) 26 (17 31) Histology Adenocarcinoma (n 30) 2 (3) 26 (46) 3 (5) Squamous cell (n 17) 0 15 (26) 2 (3) NSCLC NOS (n 10) 0 9 (15) 1 (2) Poorly differentiated (n 19) 1 (2) 15 (26) 4 (7) Stage I(n 1) II (n 2) 0 2 (3) 0 III (n 12) 0 11 (19) 0 IV (n 42) 2 (3) 36 (63) 6 (11) Chemotherapy First-line (n 23) 2 (3) 20 (35) 1 (2) Second-line (n 10) 0 8 (14) 2 (3) More than second-line (n 24) 0 21 (37) 3 (5) Chemotherapy type Platinum-based (n 18) 0 18 (31) 0 Single-agent tyrosine kinase inhibitor (n 16) 1 (2) 14 (25) 1 (2) Combination tyrosine kinase inhibitor (n 6) 1 (2) 4 (7) 1 (2) Other (n 17) 13 (23) 4 (7) Values are n(%) or median (range). NSCLC, non-small cell lung cancer; NOS, not otherwise specified therapeutic response, and numerous methodological issues regarding quantification and reproducibility of FDG uptake have limited its clinical application. 19 Additionally, the role of FDG-PET imaging in the assessment of therapeutic response requires further extensive evaluation similar to that used to validate the RECIST criteria before its routine use in the assessment of therapeutic response could be considered. Consequently, CT imaging, which is widely available and validated in the assessment of therapeutic response, remains the primary modality used in most clinical trials. However, a limitation of CT imaging is that the assessment of response to chemotherapy is not timely and often only allows a reevaluation of therapeutic options after two cycles of chemotherapy. The results of our study show that performing serial CT scans at short intervals can detect changes in tumor size after only one cycle of chemotherapy (3 4 weeks) and can change clinical management. In addition to demonstrating significant tumor regression in two patients (3%), which allowed therapy to be continued with greater confidence in these patients, six patients (11%) had significant progression of malignancy, resulting in discontinuation or change of chemotherapy drugs earlier than might otherwise have occurred. Potential limitations of our study include factors inherent to a retrospective review, i.e., the variability in time that patients received CT imaging after the initiation of therapy and the diversity in tumor histology of the patients and chemotherapy regimens received. It is possible that certain tumor types or chemotherapy regimens are more likely to be associated with rapid changes in tumor size. Unfortunately, it was not possible to predict this association from our study because of the relatively small numbers of patients and the wide variety of different chemotherapy regimens. A second limitation is that a conclusion could not reliably be drawn regarding the relation between tumor response at short-term follow-up and subsequent tumor behavior in those patients who demonstrated a non-significant change in size. Eight patients (14%) demonstrated tumor enlargement that was considered stable disease according to RECIST criteria (less than 20%). It is unclear whether the current RECIST definition of progression is applicable to short-term restaging scans, and it is possible that this earlier detection of an increase in tumor size portends a lack of response to therapy. In fact, chemotherapy was discontinued or changed for five of these patients. Because it is not clear whether an increase in size of less than 20% observed on a short-interval restaging scan can be used to confidently predict subsequent tumor behavior, a prospective study of the predictive value of short-interval restaging with CT in a more homogenous group of patients would be useful. In conclusion, CT imaging performed earlier than conventional restaging protocols is potentially useful in evaluat- 428 Copyright 2006 by the International Association for the Study of Lung Cancer
5 Journal of Thoracic Oncology Volume 1, Number 5, June 2006 Short-Term Restaging of Non-small Cell Lung Cancer ing therapeutic response among patients with NSCLC receiving chemotherapy. In particular, early restaging CT can identify tumors refractory to treatment and allow the institution of more appropriate therapy. REFERENCES 1. Jemal A, Siegel R, Ward E, et al. Cancer statistics, CA Cancer J Clin 2006;56: Ellis PA, Smith IE, Hardy JR, et al. Symptom relief with MVP (mitomycin C, vinblastine and cisplatin) chemotherapy in advanced nonsmall-cell lung cancer. Br J Cancer 1995;71: Arriagada R, Berman B, Dunant A. Cisplatin-based adjuvant chemotherapy in patients with completely resected non-small-cell lung cancer. N Engl J Med 2004;350: Dancey J, Shepherd FA, Gralla RJ. Quality of life assessment of second-line docetaxel versus best supportive care in patients with nonsmall-cell lung cancer previously treated with platinum-based chemotherapy: results of a prospective, randomized phase III trial. Lung Cancer 2004;43: Dillman RO, Seagren SL, Propert KJ, et al. A randomized trial of induction chemotherapy plus high dose radiation versus radiation alone in stage III non-small cell lung cancer. N Engl J Med 1990;323: Winton T, Livingston R, Johnson D. Vinorelbine plus cisplatin vs. observation in resected non-small-cell lung cancer. N Engl J Med 2006;352: Furuse K, Fukuoka M, Kawahara M. Phase III study of concurrent versus sequential thoracic radiotherapy in combination with mitomycin, vindesine, and cisplatin in unresectable stage III non-small-cell lung cancer. J Clin Oncol 1999;17: Thongprasert S, Sanguanmitra P, Juthapan W. Relationship between quality of life and clinical outcomes in advanced non-small cell lung cancer: best supportive care (BSC) versus BSC plus chemotherapy. Lung Cancer 1999;24: Cullen MH, Billingham LJ, Woodroffe CM, et al. Mitomycin, ifosfamide, and cisplatin in unresectable non-small-cell lung cancer: effects on survival and quality of life. J Clin Oncol 1999;17: Sekine I, Tamura T, Kunitoh H, et al. Progressive disease rate as a surrogate endpoint of phase II trials for non-small-cell lung cancer. Ann Oncol 1999;10: Miller AB, Hoogstraten B, Staquet M, Winkler A. Reporting results of cancer treatment. Cancer 1981;47: Therasse P, Arbuck SG, Eisenhauer EA, et al. New guidelines to evaluate the response to treatment in solid tumors. J Natl Cancer Inst 2000;92: Shankar LK, Sullivan DC. Functional imaging in lung cancer. J Clin Oncol 2006;23: Weissleder R. Molecular imaging: exploring the next frontier. Radiology 1999;212: Weber WA, Petersen V, Schmidt B, et al. Positron emission tomography in non-small-cell lung cancer: prediction of response to chemotherapy by quantitative assessment of glucose use. J Clin Oncol 2003;14: Ichiya Y, Kuwabara Y, Sasaki M, et al. A clinical evaluation of FDG-PET to assess the response in radiation therapy for bronchogenic carcinoma. Ann Nucl Med 1996;10: Choi NC, Fischman AJ, Niemierko A, et al. Dose-response relationship between probability of pathologic tumor control and glucose metabolic rate measured with FDG PET after preoperative chemoradiotherapy in locally advanced non-small cell lung cancer. Int J Radiat Oncol Biol Phys 2002;54: MacManus MP, Hicks RJ, Matthews JP, et al. Positron emission tomography is superior to computed tomography scanning for responseassessment after radical radiotherapy or chemoradiotherapy in patients with non-small cell lung cancer. J Clin Oncol 2003;21: Vansteenkiste J, Fischer BM, Dooms C, Mortensen J. Positron-emission tomography in prognostic and therapeutic assessment of lung cancer: systematic review. Lancet Oncol 2004;5: Copyright 2006 by the International Association for the Study of Lung Cancer 429
Evaluation of Lung Cancer Response: Current Practice and Advances
 Evaluation of Lung Cancer Response: Current Practice and Advances Jeremy J. Erasmus I have no financial relationships, arrangements or affiliations and this presentation will not include discussion of
Evaluation of Lung Cancer Response: Current Practice and Advances Jeremy J. Erasmus I have no financial relationships, arrangements or affiliations and this presentation will not include discussion of
Comparison of RECIST version 1.0 and 1.1 in assessment of tumor response by computed tomography in advanced gastric cancer
 Original Article Comparison of RECIST version 1.0 and 1.1 in assessment of tumor response by computed tomography in advanced gastric cancer Gil-Su Jang 1 *, Min-Jeong Kim 2 *, Hong-Il Ha 2, Jung Han Kim
Original Article Comparison of RECIST version 1.0 and 1.1 in assessment of tumor response by computed tomography in advanced gastric cancer Gil-Su Jang 1 *, Min-Jeong Kim 2 *, Hong-Il Ha 2, Jung Han Kim
CT Evaluation of Non-small Cell Lung Cancer Treated with Adenoviral p53 Gene Therapy
 ISPUB.COM The Internet Journal of Radiology Volume 3 Number 1 CT Evaluation of Non-small Cell Lung Cancer Treated with Adenoviral p53 Gene Therapy R Munden, M Truong, S Swisher, S Gupta, M Hicks, J Merritt,
ISPUB.COM The Internet Journal of Radiology Volume 3 Number 1 CT Evaluation of Non-small Cell Lung Cancer Treated with Adenoviral p53 Gene Therapy R Munden, M Truong, S Swisher, S Gupta, M Hicks, J Merritt,
Radiological staging of lung cancer. Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh
 Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Dr Sneha Shah Tata Memorial Hospital, Mumbai.
 Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Case Scenario 1. The patient agreed to a CT guided biopsy of the left upper lobe mass. This was performed and confirmed non-small cell carcinoma.
 Case Scenario 1 An 89 year old male patient presented with a progressive cough for approximately six weeks for which he received approximately three rounds of antibiotic therapy without response. A chest
Case Scenario 1 An 89 year old male patient presented with a progressive cough for approximately six weeks for which he received approximately three rounds of antibiotic therapy without response. A chest
Utility of 18 F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer
 Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
肺癌放射治療新進展 Recent Advance in Radiation Oncology in Lung Cancer 許峰銘成佳憲國立台灣大學醫學院附設醫院腫瘤醫學部
 肺癌放射治療新進展 Recent Advance in Radiation Oncology in Lung Cancer 許峰銘成佳憲國立台灣大學醫學院附設醫院腫瘤醫學部 Outline Current status of radiation oncology in lung cancer Focused on stage III non-small cell lung cancer Radiation
肺癌放射治療新進展 Recent Advance in Radiation Oncology in Lung Cancer 許峰銘成佳憲國立台灣大學醫學院附設醫院腫瘤醫學部 Outline Current status of radiation oncology in lung cancer Focused on stage III non-small cell lung cancer Radiation
Radiographic Assessment of Response An Overview of RECIST v1.1
 Radiographic Assessment of Response An Overview of RECIST v1.1 Stephen Liu, MD Georgetown University May 15 th, 2015 Presentation Objectives To understand the purpose of RECIST guidelines To describe the
Radiographic Assessment of Response An Overview of RECIST v1.1 Stephen Liu, MD Georgetown University May 15 th, 2015 Presentation Objectives To understand the purpose of RECIST guidelines To describe the
Welcome to the RECIST 1.1 Quick Reference
 Welcome to the RECIST 1.1 Quick Reference *Eisenhauer, E. A., et al. New response evaluation criteria in solid tumours: Revised RECIST guideline (version 1.1). Eur J Cancer 2009;45:228-47. Subject Eligibility
Welcome to the RECIST 1.1 Quick Reference *Eisenhauer, E. A., et al. New response evaluation criteria in solid tumours: Revised RECIST guideline (version 1.1). Eur J Cancer 2009;45:228-47. Subject Eligibility
Measuring Response in Solid Tumors: Comparison of RECIST and WHO Response Criteria
 Jpn J Clin Oncol 2003;33(10)533 537 Measuring Response in Solid Tumors: Comparison of RECIST and WHO Response Criteria Joon Oh Park 1, Soon Il Lee 1, Seo Young Song 1, Kihyun Kim 1, Won Seog Kim 1, Chul
Jpn J Clin Oncol 2003;33(10)533 537 Measuring Response in Solid Tumors: Comparison of RECIST and WHO Response Criteria Joon Oh Park 1, Soon Il Lee 1, Seo Young Song 1, Kihyun Kim 1, Won Seog Kim 1, Chul
THE EFFECT OF USING PET-CT FUSION ON TARGET VOLUME DELINEATION AND DOSE TO ORGANS AT RISK IN 3D RADIOTHERAPY PLANNING OF PATIENTS WITH NSSLC
 THE EFFECT OF USING PET-CT FUSION ON TARGET VOLUME DELINEATION AND DOSE TO ORGANS AT RISK IN 3D RADIOTHERAPY PLANNING OF PATIENTS WITH NSSLC Hana Al-Mahasneh,M.D*., Mohammad Khalaf Al-Fraessan, M.R.N,
THE EFFECT OF USING PET-CT FUSION ON TARGET VOLUME DELINEATION AND DOSE TO ORGANS AT RISK IN 3D RADIOTHERAPY PLANNING OF PATIENTS WITH NSSLC Hana Al-Mahasneh,M.D*., Mohammad Khalaf Al-Fraessan, M.R.N,
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010
 Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES
 MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES Although response is not the primary endpoint of this trial, subjects with measurable disease will be assessed by standard criteria. For the purposes of this
MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES Although response is not the primary endpoint of this trial, subjects with measurable disease will be assessed by standard criteria. For the purposes of this
Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer
 Original Article Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer Fangfang Chen 1 *, Yanwen Yao 2 *, Chunyan
Original Article Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer Fangfang Chen 1 *, Yanwen Yao 2 *, Chunyan
Radiologic assessment of response of tumors to treatment. Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1
 Radiologic assessment of response of tumors to treatment Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1 Objective response assessment is important to describe the treatment effect of
Radiologic assessment of response of tumors to treatment Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1 Objective response assessment is important to describe the treatment effect of
Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms
 Original Research Article Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms Anand Vachhani 1, Shashvat Modia 1*, Varun Garasia 1, Deepak Bhimani 1, C. Raychaudhuri
Original Research Article Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms Anand Vachhani 1, Shashvat Modia 1*, Varun Garasia 1, Deepak Bhimani 1, C. Raychaudhuri
The right middle lobe is the smallest lobe in the lung, and
 ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
GUIDELINES FOR CANCER IMAGING Lung Cancer
 GUIDELINES FOR CANCER IMAGING Lung Cancer Greater Manchester and Cheshire Cancer Network Cancer Imaging Cross-Cutting Group April 2010 1 INTRODUCTION This document is intended as a ready reference for
GUIDELINES FOR CANCER IMAGING Lung Cancer Greater Manchester and Cheshire Cancer Network Cancer Imaging Cross-Cutting Group April 2010 1 INTRODUCTION This document is intended as a ready reference for
Mediastinal Staging. Samer Kanaan, M.D.
 Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010
 LSU HEALTH SCIENCES CENTER NSCLC Guidelines Feist-Weiller Cancer Center Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010 Initial Evaluation/Intervention: 1. Pathology Review 2. History and Physical
LSU HEALTH SCIENCES CENTER NSCLC Guidelines Feist-Weiller Cancer Center Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010 Initial Evaluation/Intervention: 1. Pathology Review 2. History and Physical
Tumor Board Discussions: Case 1
 Tumor Board Discussions: Case 1 David S. Ettinger, MD The Alex Grass Professor of Oncology Johns Hopkins University School of Medicine Baltimore, Maryland Case #1 50-year-old Asian female, never smoker
Tumor Board Discussions: Case 1 David S. Ettinger, MD The Alex Grass Professor of Oncology Johns Hopkins University School of Medicine Baltimore, Maryland Case #1 50-year-old Asian female, never smoker
Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times
 Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times Andrea Borghesi, MD Davide Farina, MD Roberto Maroldi, MD Department of Radiology University of Brescia Brescia,
Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times Andrea Borghesi, MD Davide Farina, MD Roberto Maroldi, MD Department of Radiology University of Brescia Brescia,
Heterogeneity of N2 disease
 Locally Advanced NSCLC Surgery? No. Ramaswamy Govindan M.D Co-Director, Section of Medical Oncology Alvin J Siteman Cancer Center at Washington University School of Medicine St. Louis, Missouri Heterogeneity
Locally Advanced NSCLC Surgery? No. Ramaswamy Govindan M.D Co-Director, Section of Medical Oncology Alvin J Siteman Cancer Center at Washington University School of Medicine St. Louis, Missouri Heterogeneity
North of Scotland Cancer Network Clinical Management Guideline for Non Small Cell Lung Cancer
 THIS DOCUMENT IS North of Scotland Cancer Network Clinical Management Guideline for Non Small Cell Lung Cancer [Based on WOSCAN NSCLC CMG with further extensive consultation within NOSCAN] UNCONTROLLED
THIS DOCUMENT IS North of Scotland Cancer Network Clinical Management Guideline for Non Small Cell Lung Cancer [Based on WOSCAN NSCLC CMG with further extensive consultation within NOSCAN] UNCONTROLLED
Lung Cancer Epidemiology. AJCC Staging 6 th edition
 Surgery for stage IIIA NSCLC? Sometimes! Anne S. Tsao, M.D. Associate Professor Director, Mesothelioma Program Director, Thoracic Chemo-Radiation Program May 7, 2011 The University of Texas MD ANDERSON
Surgery for stage IIIA NSCLC? Sometimes! Anne S. Tsao, M.D. Associate Professor Director, Mesothelioma Program Director, Thoracic Chemo-Radiation Program May 7, 2011 The University of Texas MD ANDERSON
Paradigm shift - from "curing cancer" to making cancer a "chronic disease"
 Current Clinical Practice of Tumor Response Assessment David M. Panicek, MD Department of Radiology Memorial Sloan-Kettering Cancer Center, New York, NY Learning Objectives Review various response assessment
Current Clinical Practice of Tumor Response Assessment David M. Panicek, MD Department of Radiology Memorial Sloan-Kettering Cancer Center, New York, NY Learning Objectives Review various response assessment
How to evaluate tumor response? Yonsei University College of Medicine Kim, Beom Kyung
 How to evaluate tumor response? Yonsei University College of Medicine Kim, Beom Kyung End points in research for solid cancers Overall survival (OS) The most ideal one, but requires long follow-up duration
How to evaluate tumor response? Yonsei University College of Medicine Kim, Beom Kyung End points in research for solid cancers Overall survival (OS) The most ideal one, but requires long follow-up duration
CHAPTER 5 TUMOR SIZE DOES NOT PREDICT PATHOLOGICAL COMPLETE RESPONSE RATES AFTER PRE-OPERATIVE CHEMORADIOTHERAPY FOR NON-SMALL CELL LUNG CANCER
 TUMOR SIZE DOES NOT PREDICT PATHOLOGICAL COMPLETE RESPONSE RATES AFTER PRE-OPERATIVE CHEMORADIOTHERAPY FOR NON-SMALL CELL LUNG CANCER Cornelis G. Vos Max R. Dahele Chris Dickhoff Suresh Senan Erik Thunnissen
TUMOR SIZE DOES NOT PREDICT PATHOLOGICAL COMPLETE RESPONSE RATES AFTER PRE-OPERATIVE CHEMORADIOTHERAPY FOR NON-SMALL CELL LUNG CANCER Cornelis G. Vos Max R. Dahele Chris Dickhoff Suresh Senan Erik Thunnissen
PET/CT in lung cancer
 PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
Lung Cancer in Women: A Different Disease? James J. Stark, MD, FACP
 Lung Cancer in Women: A Different Disease? James J. Stark, MD, FACP Medical Director, Cancer Program and Director of Palliative Care Maryview Medical Center Professor of Medicine Eastern Virginia Medical
Lung Cancer in Women: A Different Disease? James J. Stark, MD, FACP Medical Director, Cancer Program and Director of Palliative Care Maryview Medical Center Professor of Medicine Eastern Virginia Medical
Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2
 Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2 The Committee for Management of CT-screening-detected Pulmonary Nodules 2009-2011 The Japanese Society of CT Screening
Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2 The Committee for Management of CT-screening-detected Pulmonary Nodules 2009-2011 The Japanese Society of CT Screening
The Itracacies of Staging Patients with Suspected Lung Cancer
 The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
PET in Rectal Carcinoma
 Case Report PET in Rectal Carcinoma Josefina Jofré M 1, Paulina Sierralta C 1, José Canessa G 1,2, Pamela Humeres A 3, Gabriel Castro M 4, Teresa Massardo V 1,4 1 Centro PET de Imágenes Moleculares, Hospital
Case Report PET in Rectal Carcinoma Josefina Jofré M 1, Paulina Sierralta C 1, José Canessa G 1,2, Pamela Humeres A 3, Gabriel Castro M 4, Teresa Massardo V 1,4 1 Centro PET de Imágenes Moleculares, Hospital
LUNG CANCER. Agnieszka Słowik, MD. Department of Oncology, University Hospital in Cracow Jagiellonian University
 LUNG CANCER Agnieszka Słowik, MD Department of Oncology, University Hospital in Cracow Jagiellonian University Epidemiology Most common malignancy worldwide Place of lung cancer among other malignancies
LUNG CANCER Agnieszka Słowik, MD Department of Oncology, University Hospital in Cracow Jagiellonian University Epidemiology Most common malignancy worldwide Place of lung cancer among other malignancies
Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis
 ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
Improving prediction of radiotherapy response and optimizing target definition by using FDG-PET for lung cancer patients
 Investigations and research Improving prediction of radiotherapy response and optimizing target definition by using FDG-PET for lung cancer patients R.J.H.M. Steenbakkers G.R. Borst M. van Herk H. Bartelink
Investigations and research Improving prediction of radiotherapy response and optimizing target definition by using FDG-PET for lung cancer patients R.J.H.M. Steenbakkers G.R. Borst M. van Herk H. Bartelink
Lung Cancer Update. HARMESH R NAIK, MD. February 28, 2001
 Lung Cancer Update HARMESH R NAIK, MD. February 28, 2001 Progress update Prevention Screening Staging Treatment Epidemiology Estimated 169,500 new cases Estimated 157,400 deaths Second commonest cancer
Lung Cancer Update HARMESH R NAIK, MD. February 28, 2001 Progress update Prevention Screening Staging Treatment Epidemiology Estimated 169,500 new cases Estimated 157,400 deaths Second commonest cancer
Response Evaluation after Stereotactic Ablative Radiotherapy for Lung Cancer
 Original Article PROGRESS in MEDICAL PHYSICS Vol. 26, No. 4, December, 2015 http://dx.doi.org/10.14316/pmp.2015.26.4.229 Response Evaluation after Stereotactic Ablative Radiotherapy for Lung Cancer Ji
Original Article PROGRESS in MEDICAL PHYSICS Vol. 26, No. 4, December, 2015 http://dx.doi.org/10.14316/pmp.2015.26.4.229 Response Evaluation after Stereotactic Ablative Radiotherapy for Lung Cancer Ji
Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón
 Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón Santiago Ponce Aix Servicio Oncología Médica Hospital Universitario 12 de Octubre Madrid Stage III: heterogenous disease
Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón Santiago Ponce Aix Servicio Oncología Médica Hospital Universitario 12 de Octubre Madrid Stage III: heterogenous disease
Protocol of Radiotherapy for Small Cell Lung Cancer
 107 年 12 月修訂 Protocol of Radiotherapy for Small Cell Lung Cancer Indication of radiotherapy Limited stage: AJCC (8th edition) stage I-III (T any, N any, M0) that can be safely treated with definitive RT
107 年 12 月修訂 Protocol of Radiotherapy for Small Cell Lung Cancer Indication of radiotherapy Limited stage: AJCC (8th edition) stage I-III (T any, N any, M0) that can be safely treated with definitive RT
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease
 Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Utility of PET-CT for detection of N2 or N3 nodal mestastases in the mediastinum in patients with non-small cell lung cancer (NSCLC)
 Utility of PET-CT for detection of N2 or N3 nodal mestastases in the mediastinum in patients with non-small cell lung cancer (NSCLC) Poster No.: C-1360 Congress: ECR 2015 Type: Scientific Exhibit Authors:
Utility of PET-CT for detection of N2 or N3 nodal mestastases in the mediastinum in patients with non-small cell lung cancer (NSCLC) Poster No.: C-1360 Congress: ECR 2015 Type: Scientific Exhibit Authors:
FDG PET/CT STAGING OF LUNG CANCER. Dr Shakher Ramdave
 FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
American College of Radiology ACR Appropriateness Criteria
 American College of Radiology ACR Criteria Radiologic Management of Thoracic Nodules and Masses Variant 1: Middle-aged patient (35 60 years old) with an incidental 1.5-cm lung nodule. The lesion was smooth.
American College of Radiology ACR Criteria Radiologic Management of Thoracic Nodules and Masses Variant 1: Middle-aged patient (35 60 years old) with an incidental 1.5-cm lung nodule. The lesion was smooth.
Sleeve lobectomy for lung adenocarcinoma treated with neoadjuvant afatinib
 Case Report Sleeve lobectomy for lung adenocarcinoma treated with neoadjuvant afatinib Ichiro Sakanoue 1, Hiroshi Hamakawa 1, Reiko Kaji 2, Yukihiro Imai 3, Nobuyuki Katakami 2, Yutaka Takahashi 1 1 Department
Case Report Sleeve lobectomy for lung adenocarcinoma treated with neoadjuvant afatinib Ichiro Sakanoue 1, Hiroshi Hamakawa 1, Reiko Kaji 2, Yukihiro Imai 3, Nobuyuki Katakami 2, Yutaka Takahashi 1 1 Department
Approach to Pulmonary Nodules
 Approach to Pulmonary Nodules Edwin Jackson, Jr., DO Assistant Professor-Clinical Director, James Early Detection Clinic Department of Internal Medicine Division of Pulmonary, Allergy, Critical Care and
Approach to Pulmonary Nodules Edwin Jackson, Jr., DO Assistant Professor-Clinical Director, James Early Detection Clinic Department of Internal Medicine Division of Pulmonary, Allergy, Critical Care and
Spectrum of Radiological Findings in Bronchogenic Carcinoma A Retrospective Study
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 01 Ver. VIII January. (2018), PP 43-59 www.iosrjournals.org Spectrum of Radiological Findings
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 01 Ver. VIII January. (2018), PP 43-59 www.iosrjournals.org Spectrum of Radiological Findings
Radiotherapy for Locoregional Recurrent Non-Small Cell Lung Cancer
 J Lung Cancer 2011;10(1):37-43 Radiotherapy for Locoregional Recurrent Non-Small Cell Lung Cancer Purpose: To retrospectively evaluate the outcomes and complications of curative radiotherapy for locoregionally
J Lung Cancer 2011;10(1):37-43 Radiotherapy for Locoregional Recurrent Non-Small Cell Lung Cancer Purpose: To retrospectively evaluate the outcomes and complications of curative radiotherapy for locoregionally
Imaging Decisions Start Here SM
 Owing to its high resolution and wide anatomic coverage, dynamic first-pass perfusion 320-detector-row CT outperforms PET/CT for distinguishing benign from malignant lung nodules, researchers from Japan
Owing to its high resolution and wide anatomic coverage, dynamic first-pass perfusion 320-detector-row CT outperforms PET/CT for distinguishing benign from malignant lung nodules, researchers from Japan
Reflex Testing Guidelines for Immunotherapy in Non-Small Cell Lung Cancer
 Reflex Testing Guidelines for Immunotherapy in Non-Small Cell Lung Cancer Jimmy Ruiz, MD Assistant Professor Thoracic Oncology Program Wake Forest Comprehensive Cancer Center Disclosures I have no actual
Reflex Testing Guidelines for Immunotherapy in Non-Small Cell Lung Cancer Jimmy Ruiz, MD Assistant Professor Thoracic Oncology Program Wake Forest Comprehensive Cancer Center Disclosures I have no actual
Locally advanced unresectable non small cell lung cancer
 ORIGINAL ARTICLE Docetaxel Consolidation Therapy Following Cisplatin, Vinorelbine, and Concurrent Thoracic Radiotherapy in Patients with Unresectable Stage III Non-small Cell Lung Cancer Ikuo Sekine,*
ORIGINAL ARTICLE Docetaxel Consolidation Therapy Following Cisplatin, Vinorelbine, and Concurrent Thoracic Radiotherapy in Patients with Unresectable Stage III Non-small Cell Lung Cancer Ikuo Sekine,*
Update on Small Cell Lung Cancer
 Welcome to Master Class for Oncologists Session 4: 10:00 AM - 10:45 AM San Francisco, CA October 23, 2009 Speaker: Bruce E. Johnson, MD Professor of Medicine, Dana-Farber Cancer Institute and Harvard Medical
Welcome to Master Class for Oncologists Session 4: 10:00 AM - 10:45 AM San Francisco, CA October 23, 2009 Speaker: Bruce E. Johnson, MD Professor of Medicine, Dana-Farber Cancer Institute and Harvard Medical
1/25/13 Right partial nephrectomy followed by completion right radical nephrectomy.
 History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer
 Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
The Role of PET / CT in Lung Cancer Staging
 July 2004 The Role of PET / CT in Lung Cancer Staging Vlad Vinarsky, Harvard Medical School Year IV Patient AM HPI: 81 yo F p/w hemoptysis x 1 month LLL lesion on CXR, not responsive to Abx 35 pack-year
July 2004 The Role of PET / CT in Lung Cancer Staging Vlad Vinarsky, Harvard Medical School Year IV Patient AM HPI: 81 yo F p/w hemoptysis x 1 month LLL lesion on CXR, not responsive to Abx 35 pack-year
NIH Public Access Author Manuscript AJR Am J Roentgenol. Author manuscript; available in PMC 2011 July 6.
 NIH Public Access Author Manuscript Published in final edited form as: AJR Am J Roentgenol. 2010 September ; 195(3): W221 W228. doi:10.2214/ajr.09.3928. New Response Evaluation Criteria in Solid Tumors
NIH Public Access Author Manuscript Published in final edited form as: AJR Am J Roentgenol. 2010 September ; 195(3): W221 W228. doi:10.2214/ajr.09.3928. New Response Evaluation Criteria in Solid Tumors
POSITRON EMISSION TOMOGRAPHY (PET)
 Status Active Medical and Behavioral Health Policy Section: Radiology Policy Number: V-27 Effective Date: 08/27/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Radiology Policy Number: V-27 Effective Date: 08/27/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Diagnosis and Staging of Non-Small Cell Lung Cancer Carlos Eduardo Oliveira Baleeiro, MD. November 18, 2017
 Diagnosis and Staging of Non-Small Cell Lung Cancer Carlos Eduardo Oliveira Baleeiro, MD November 18, 2017 Disclosures I do not have a financial interest/arrangement or affiliation with one or more organizations
Diagnosis and Staging of Non-Small Cell Lung Cancer Carlos Eduardo Oliveira Baleeiro, MD November 18, 2017 Disclosures I do not have a financial interest/arrangement or affiliation with one or more organizations
PET-CT for radiotherapy planning in lung cancer: current recommendations and future directions
 PET-CT for radiotherapy planning in lung cancer: current recommendations and future directions Gerry Hanna Centre for Cancer Research and Cell Biology Queen s University of Belfast @gerryhanna Talk Outline
PET-CT for radiotherapy planning in lung cancer: current recommendations and future directions Gerry Hanna Centre for Cancer Research and Cell Biology Queen s University of Belfast @gerryhanna Talk Outline
PET/CT for Therapy Assessment in Oncology
 PET/CT for Therapy Assessment in Oncology Rodolfo Núñez Miller, M.D. Nuclear Medicine Section Division of Human Health International Atomic Energy Agency Vienna, Austria Clinical Applications of PET/CT
PET/CT for Therapy Assessment in Oncology Rodolfo Núñez Miller, M.D. Nuclear Medicine Section Division of Human Health International Atomic Energy Agency Vienna, Austria Clinical Applications of PET/CT
An Introduction to PET Imaging in Oncology
 January 2002 An Introduction to PET Imaging in Oncology Janet McLaren, Harvard Medical School Year III Basics of PET Principle of Physiologic Imaging: Allows in vivo visualization of structures by their
January 2002 An Introduction to PET Imaging in Oncology Janet McLaren, Harvard Medical School Year III Basics of PET Principle of Physiologic Imaging: Allows in vivo visualization of structures by their
TRANSPARENCY COMMITTEE OPINION. 29 April 2009
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 29 April 2009 NAVELBINE 20 mg, soft capsules B/1 (CIP: 365 948-4) NAVELBINE 30 mg, soft capsules B/1 (CIP: 365 949-0)
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 29 April 2009 NAVELBINE 20 mg, soft capsules B/1 (CIP: 365 948-4) NAVELBINE 30 mg, soft capsules B/1 (CIP: 365 949-0)
THORACIC MALIGNANCIES
 THORACIC MALIGNANCIES Summary for Malignant Malignancies. Lung Ca 1 Lung Cancer Non-Small Cell Lung Cancer Diagnostic Evaluation for Non-Small Lung Cancer 1. History and Physical examination. 2. CBCDE,
THORACIC MALIGNANCIES Summary for Malignant Malignancies. Lung Ca 1 Lung Cancer Non-Small Cell Lung Cancer Diagnostic Evaluation for Non-Small Lung Cancer 1. History and Physical examination. 2. CBCDE,
Chemo-radiotherapy in non-small cell lung cancer. HARMESH R NAIK, MD. September 25, 2002
 Chemo-radiotherapy in non-small cell lung cancer HARMESH R NAIK, MD. September 25, 2002 Epidemiology Estimated 170000 new cases Estimated 157,000 deaths Second commonest cancer diagnosis in men and women
Chemo-radiotherapy in non-small cell lung cancer HARMESH R NAIK, MD. September 25, 2002 Epidemiology Estimated 170000 new cases Estimated 157,000 deaths Second commonest cancer diagnosis in men and women
Management of advanced non small cell lung cancer
 Management of advanced non small cell lung cancer Jean-Paul Sculier Intensive Care & Thoracic Oncology Institut Jules Bordet Université Libre de Bruxelles (ULB) www.pneumocancero.com Declaration No conflict
Management of advanced non small cell lung cancer Jean-Paul Sculier Intensive Care & Thoracic Oncology Institut Jules Bordet Université Libre de Bruxelles (ULB) www.pneumocancero.com Declaration No conflict
Slide 1. Slide 2. Slide 3. Investigation and management of lung cancer Robert Rintoul. Epidemiology. Risk factors/aetiology
 Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
PET IMAGING (POSITRON EMISSION TOMOGRAPY) FACT SHEET
 Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Chapter 6. Hester Gietema Cornelia Schaefer-Prokop Willem Mali Gerard Groenewegen Mathias Prokop. Accepted for publication in Radiology
 Chapter 6 Interscan variability of semiautomated volume measurements in intraparenchymal pulmonary nodules using multidetector-row computed tomography: Influence of inspirational level, nodule size and
Chapter 6 Interscan variability of semiautomated volume measurements in intraparenchymal pulmonary nodules using multidetector-row computed tomography: Influence of inspirational level, nodule size and
A Proposed Strategy for Treatment of Superficial Carcinoma. in the Thoracic Esophagus Based on an Analysis. of Lymph Node Metastasis
 Kitakanto Med J 2002 ; 52 : 189-193 189 A Proposed Strategy for Treatment of Superficial Carcinoma in the Thoracic Esophagus Based on an Analysis of Lymph Node Metastasis Susumu Kawate,' Susumu Ohwada,'
Kitakanto Med J 2002 ; 52 : 189-193 189 A Proposed Strategy for Treatment of Superficial Carcinoma in the Thoracic Esophagus Based on an Analysis of Lymph Node Metastasis Susumu Kawate,' Susumu Ohwada,'
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 4/30/2011 Radiology Quiz of the Week # 18 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 4/30/2011 Radiology Quiz of the Week # 18 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Lung Cancer Staging: The Revised TNM Classification
 Norwegian Society of Thoracic Imaging Oslo, October 2011 Lung Cancer Staging: The Revised TNM Classification Sujal R Desai King s College Hospital, London Lung Cancer The Scale of the Problem Leading cause
Norwegian Society of Thoracic Imaging Oslo, October 2011 Lung Cancer Staging: The Revised TNM Classification Sujal R Desai King s College Hospital, London Lung Cancer The Scale of the Problem Leading cause
After primary tumor treatment, 30% of patients with malignant
 ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
PET CT for Staging Lung Cancer
 PET CT for Staging Lung Cancer Rohit Kochhar Consultant Radiologist Disclosures Neither I nor my immediate family members have financial relationships with commercial organizations that may have a direct
PET CT for Staging Lung Cancer Rohit Kochhar Consultant Radiologist Disclosures Neither I nor my immediate family members have financial relationships with commercial organizations that may have a direct
Sectional Anatomy Quiz - III
 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Non-small Cell Lung Cancer: Multidisciplinary Role: Role of Medical Oncologist
 Non-small Cell Lung Cancer: Multidisciplinary Role: Role of Medical Oncologist Vichien Srimuninnimit, MD. Medical Oncology Division Faculty of Medicine, Siriraj Hospital Outline Resectable NSCLC stage
Non-small Cell Lung Cancer: Multidisciplinary Role: Role of Medical Oncologist Vichien Srimuninnimit, MD. Medical Oncology Division Faculty of Medicine, Siriraj Hospital Outline Resectable NSCLC stage
Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!!
 The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
Lung cancer remains the leading cause of cancer death
 Time Course of Early Response to Chemotherapy in Non Small Cell Lung Cancer Patients with 18 F-FDG PET/CT Claude Nahmias 1, Wahid T. Hanna 1, Lindi M. Wahl 2, Misty J. Long 1, Karl F. Hubner 1, and David
Time Course of Early Response to Chemotherapy in Non Small Cell Lung Cancer Patients with 18 F-FDG PET/CT Claude Nahmias 1, Wahid T. Hanna 1, Lindi M. Wahl 2, Misty J. Long 1, Karl F. Hubner 1, and David
ANZUP SURVEILLANCE RECOMMENDATIONS FOR METASTATIC TESTICULAR CANCER POST-CHEMOTHERAPY
 ANZUP SURVEILLANCE RECOMMENDATIONS FOR METASTATIC TESTICULAR CANCER POST-CHEMOTHERAPY Note: These surveillance recommendations are provided as recommendations only. Clinicians should take into account
ANZUP SURVEILLANCE RECOMMENDATIONS FOR METASTATIC TESTICULAR CANCER POST-CHEMOTHERAPY Note: These surveillance recommendations are provided as recommendations only. Clinicians should take into account
The surgeon: new surgical aproaches
 The surgeon: new surgical aproaches Paul Van Schil, MD Department of Thoracic and Vascular Surgery Antwerp University, Belgium no disclosures, no conflict of interest Malignant pleural mesothelioma: clinical,
The surgeon: new surgical aproaches Paul Van Schil, MD Department of Thoracic and Vascular Surgery Antwerp University, Belgium no disclosures, no conflict of interest Malignant pleural mesothelioma: clinical,
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
PET/CT Frequently Asked Questions
 PET/CT Frequently Asked Questions General Q: Is FDG PET specific for cancer? A: No, it is a marker of metabolism. In general, any disease that causes increased metabolism can result in increased FDG uptake
PET/CT Frequently Asked Questions General Q: Is FDG PET specific for cancer? A: No, it is a marker of metabolism. In general, any disease that causes increased metabolism can result in increased FDG uptake
EVIDENCE BASED MANAGEMENT OF STAGE III NSCLC MILIND BALDI
 EVIDENCE BASED MANAGEMENT OF STAGE III NSCLC MILIND BALDI Overview Introduction Diagnostic work up Treatment Group 1 Group 2 Group 3 Stage III lung cancer Historically was defined as locoregionally advanced
EVIDENCE BASED MANAGEMENT OF STAGE III NSCLC MILIND BALDI Overview Introduction Diagnostic work up Treatment Group 1 Group 2 Group 3 Stage III lung cancer Historically was defined as locoregionally advanced
Tumor response assessment by the single-lesion measurement per organ in small cell lung cancer
 Original Article Tumor response assessment by the single-lesion measurement per organ in small cell lung cancer Soong Goo Jung 1, Jung Han Kim 1, Hyeong Su Kim 1, Kyoung Ju Kim 2, Ik Yang 3 1 Department
Original Article Tumor response assessment by the single-lesion measurement per organ in small cell lung cancer Soong Goo Jung 1, Jung Han Kim 1, Hyeong Su Kim 1, Kyoung Ju Kim 2, Ik Yang 3 1 Department
Controversies in management of squamous esophageal cancer
 2015.06.12 12.47.48 Page 4(1) IS-1 Controversies in management of squamous esophageal cancer C S Pramesh Thoracic Surgery, Department of Surgical Oncology, Tata Memorial Centre, India In Asia, squamous
2015.06.12 12.47.48 Page 4(1) IS-1 Controversies in management of squamous esophageal cancer C S Pramesh Thoracic Surgery, Department of Surgical Oncology, Tata Memorial Centre, India In Asia, squamous
The treatment of breast cancer patients who have metastatic
 Early Prediction of Response to Chemotherapy in Metastatic Breast Cancer Using Sequential F-FDG PET Joerg Dose Schwarz, MD 1 ; Michael Bader, MD 1 ; Lars Jenicke, MD 2 ; Gabriele Hemminger, MD 1 ; Fritz
Early Prediction of Response to Chemotherapy in Metastatic Breast Cancer Using Sequential F-FDG PET Joerg Dose Schwarz, MD 1 ; Michael Bader, MD 1 ; Lars Jenicke, MD 2 ; Gabriele Hemminger, MD 1 ; Fritz
OBJECTIVES. Solitary Solid Spiculated Nodule. What would you do next? Case Based Discussion: State of the Art Management of Lung Nodules.
 Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD
 Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Staging recurrent ovarian cancer with 18 FDG PET/CT
 ONCOLOGY LETTERS 5: 593-597, 2013 Staging recurrent ovarian cancer with FDG PET/CT SANJA DRAGOSAVAC 1, SOPHIE DERCHAIN 2, NELSON M.G. CASERTA 3 and GUSTAVO DE SOUZA 2 1 DIMEN Medicina Nuclear and PET/CT
ONCOLOGY LETTERS 5: 593-597, 2013 Staging recurrent ovarian cancer with FDG PET/CT SANJA DRAGOSAVAC 1, SOPHIE DERCHAIN 2, NELSON M.G. CASERTA 3 and GUSTAVO DE SOUZA 2 1 DIMEN Medicina Nuclear and PET/CT
CT Contrast Protocols for Different Organ Imaging
 CT Contrast Protocols for Different Organ Imaging g Paul Shreve, M.D. Advanced Radiology Services, P.C. & Spectrum Health Grand Rapids, MI, USA Correlative Imaging Council Society of Nuclear Medicine 56
CT Contrast Protocols for Different Organ Imaging g Paul Shreve, M.D. Advanced Radiology Services, P.C. & Spectrum Health Grand Rapids, MI, USA Correlative Imaging Council Society of Nuclear Medicine 56
RECIST 1.1 and SWOG Protocol Section 10
 RECIST 1.1 and SWOG Protocol Section 10 Louise Highleyman, Data Coordinator SWOG Statistics and Data Management Center Response Evaluation Criteria in Solid Tumors (RECIST) 1.1 2009: Revised RECIST guideline
RECIST 1.1 and SWOG Protocol Section 10 Louise Highleyman, Data Coordinator SWOG Statistics and Data Management Center Response Evaluation Criteria in Solid Tumors (RECIST) 1.1 2009: Revised RECIST guideline
Tumor Response in Patients With Advanced Non Small Cell Lung Cancer: Perfusion CT Evaluation of Chemotherapy and Radiation Therapy
 Cardiopulmonary Imaging Original Research Wang et al. CT of Non Small Cell Lung Cancer Cardiopulmonary Imaging Original Research Jianwei Wang 1 Ning Wu 1 Matthew D. Cham 2 Ying Song 1 Wang J, Wu N, Cham
Cardiopulmonary Imaging Original Research Wang et al. CT of Non Small Cell Lung Cancer Cardiopulmonary Imaging Original Research Jianwei Wang 1 Ning Wu 1 Matthew D. Cham 2 Ying Song 1 Wang J, Wu N, Cham
Noninvasive Differential Diagnosis of Pulmonary Nodules Using the Standardized Uptake Value Index
 doi: 10.5761/atcs.oa.14-00241 Original Article Noninvasive Differential Diagnosis of Pulmonary Nodules Using the Standardized Uptake Value Index Satoshi Shiono, MD, 1 Naoki Yanagawa, MD, 2 Masami Abiko,
doi: 10.5761/atcs.oa.14-00241 Original Article Noninvasive Differential Diagnosis of Pulmonary Nodules Using the Standardized Uptake Value Index Satoshi Shiono, MD, 1 Naoki Yanagawa, MD, 2 Masami Abiko,
Radiology Pathology Conference
 Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
PET/CT in breast cancer staging
 PET/CT in breast cancer staging Anni Morsing Consultant, PhD, DMSc Rigshospitalet 1 18F- FDG PET/CT for breastcancer staging Where is the clinical impact? To which women should 18F- FDG PET/CT be offered?
PET/CT in breast cancer staging Anni Morsing Consultant, PhD, DMSc Rigshospitalet 1 18F- FDG PET/CT for breastcancer staging Where is the clinical impact? To which women should 18F- FDG PET/CT be offered?
Treatment Strategy for Patients With Surgically Discovered N2 Stage IIIA Non-Small Cell Lung Cancer
 Treatment Strategy for Patients With Surgically Discovered N2 Stage IIIA Non-Small Cell Lung Cancer Ryoichi Nakanishi, MD, Toshihiro Osaki, MD, Kozo Nakanishi, MD, Ichiro Yoshino, MD, Takashi Yoshimatsu,
Treatment Strategy for Patients With Surgically Discovered N2 Stage IIIA Non-Small Cell Lung Cancer Ryoichi Nakanishi, MD, Toshihiro Osaki, MD, Kozo Nakanishi, MD, Ichiro Yoshino, MD, Takashi Yoshimatsu,
GROUP 1: Peripheral tumour with normal hilar and mediastinum on staging CT with no disant metastases. Including: Excluding:
 GROUP 1: Including: Excluding: Peripheral tumour with normal hilar and mediastinum on staging CT with no disant metastases Solid pulmonary nodules 8mm diameter / 300mm3 volume and BROCK risk of malignancy
GROUP 1: Including: Excluding: Peripheral tumour with normal hilar and mediastinum on staging CT with no disant metastases Solid pulmonary nodules 8mm diameter / 300mm3 volume and BROCK risk of malignancy
objectives Pitfalls and Pearls in PET/CT imaging Kevin Robinson, DO Assistant Professor Department of Radiology Michigan State University
 objectives Pitfalls and Pearls in PET/CT imaging Kevin Robinson, DO Assistant Professor Department of Radiology Michigan State University To determine the regions of physiologic activity To understand
objectives Pitfalls and Pearls in PET/CT imaging Kevin Robinson, DO Assistant Professor Department of Radiology Michigan State University To determine the regions of physiologic activity To understand
