L ast year new cases of colorectal
|
|
|
- Lucy Lucas
- 5 years ago
- Views:
Transcription
1 223 REVIEW Non-steroidal anti-inflammatory drugs and colorectal cancer prevention S Sangha, M Yao, M M Wolfe... Colorectal cancer is the second leading cause of cancer deaths in the United States. Currently, the most effective strategy available for colon cancer prevention is endoscopic screening, with polypectomy or surgical resection for advanced lesions. This intervention carries with it many concerns regarding cost, patient acceptance, and the growing burden of surveillance colonoscopies for patients with polyps. Further improvements in the understanding of the multistep model of colorectal carcinogenesis will probably lead to the development of other primary and secondary prevention strategies. Data obtained from animal and epidemiological studies and most recently from randomised, placebo controlled trials, suggest that non-steroidal anti-inflammatory drugs may prove effective chemopreventive agents in different groups of people, from patients with familial tous polyposis to those with sporadic s.... See end of article for authors affiliations... Correspondence to: Dr M M Wolfe, Boston Medical Center, Section of Gastroenterology, 650 Albany Street, Boston, MA 02118, USA; michael. wolfe@bmc.org Submitted 3 April 2004 Accepted 5 August L ast year new cases of colorectal cancer (CRC) were diagnosed in the United States, and people died from complications of their disease. 1 Overall, about one half of patients diagnosed with CRC ultimately die from the disease. This poor outcome is related to inadequate screening of the population, resulting in detection of the disease at an advanced stage when curative resection is no longer possible. Our understanding of the development of colon cancer has progressed rapidly over the past decades, and it is now well established that most colorectal cancer develops from neoplastic precursor lesions. The multistep progression of an tous polyp to invasive cancer is now well explicated and offers opportunities for targeted chemoprevention. In a prospective necropsy study involving the colon, s were found in 36.9% of male cases and 28.7% of female cases, with the prevalence and multiplicity of polyps increasing with advancing age. 2 The subgroup of people with s offers an excellent opportunity for specific chemoprevention with various agents, such as non-steroidal anti-inflammatory drugs (NSAIDs), which are known to inhibit tumorigenesis based upon animal and epidemiological studies and, more recently, upon prospective trials. In this review, we will discuss the molecular basis for the chemopreventive effect of NSAIDs, as well as the numerous epidemiological and prospective studies that have assessed the effect of NSAIDs Postgrad Med J 2005;81: doi: /pgmj both in patients with hereditary colon cancer syndromes, as well as those with sporadic colorectal cancer. Although not the focus of this review, other agents that have been considered in CRC chemoprevention include folate, calcium, hormone replacement therapy, vitamins, antioxidants, and fibre. Of these, folate has been studied most extensively and shows significant benefit. In a prospective cohort study, following up patients, Giovannucci et al showed a relative risk reduction of 0.71 (95% confidence intervals, 0.56 to 0.89), with the greatest benefit in those taking folate supplementation. 3 MECHANISMS OF NSAID INHIBITION IN COLON CARCINOGENESIS NSAIDs are known potent inhibitors of cyclooxygenase (COX) enzymes, resulting in decreased prostaglandin synthesis, which, in turn, induces tumour cell apoptosis. Other studies have shown that NSAIDs also promote apoptosis through COX independent pathways. A combination of these effects is the probable source of the antineoplastic effect of NSAIDs, which continues to be an area of intense research. The mechanism of inhibition of COX activity by aspirin and NSAIDs was first described by Vane in In the early 1990s, several groups reported the discovery of two COX isoforms. 5 6 COX-1, the constitutively expressed form, seems to function as a physiological regulatory enzyme in most tissues. COX-2, however, is strongly inducible and plays an integral part in several physiological and pathological processes, including cell proliferation and inflammatory responses. COX-2 mrna expression and protein were found to be increased in human colorectal s and adenocarcinomas. 7 8 Conversely, specific COX-2 inhibition, either by targeted knockout of the COX-2 gene or by pharmacological intervention, has been shown to effectively decrease the growth of murine intestinal s In a rat model of chemically induced colorectal cancer, the COX-2 selective inhibitor celecoxib suppressed the formation of aberrant crypt foci, precursors of s. 12 Celecoxib also inhibited the incidence and multiplicity of colon tumours by 93% and 97%, respectively. 13 As noted above COX-2 overexpression is important during colorectal carcinogenesis, however it is unclear exactly where in the multistep process COX-2 deregulation occurs (fig 1). Abbreviations: NSAID, non-steroidal anti-inflammatory drug; CRC, colorectal cancer; COX, cyclooxygenase; FAP, familial tous polyposis; HNPCC, hereditary non-polyposis colorectal cancer
2 224 Sangha, Yao, Wolfe Because COX-2 overexpression occurs even in small s, it is thought to represent an early event, promoting tumour proliferation and suppression of apoptosis. In vitro, many NSAIDs including sulindac, indomethacin, naproxen, peroxicam, aspirin, and COX-2 specific inhibitors are known to cause apoptosis in colon cancer cells. Thus, a growing body of experimental data supports the hypothesis that NSAIDs exert their chemopreventive effect by restoring to normal the frequency of apoptosis in colonic mucosa. 15 CHEMOPREVENTION IN HEREDITARY COLON CANCER Hereditary colorectal cancer, best defined in the familial tous polyposis (FAP) and hereditary non-polyposis colorectal cancer (HNPCC) syndromes, has been estimated to account for 15% of all colon cancers occurring in the general population. 16 Chemoprevention is of special interest in patients with germline mutations resulting in FAP or HNPCC as these patients are at risk for the development of tumours in multiple organs. Most of the studies to date have concentrated on the role on NSAIDs in FAP. In brief, FAP results from mutations in the APC gene (chromosome 5q), and pedigree analysis shows an autosomal dominant pattern with nearly complete penetrance. Typically, patients with FAP develop diffuse colorectal polyposis by their adolescent years, and, if untreated, will be diagnosed with colorectal cancer by 40 years of age. Currently, the most effective management is initial intensive endoscopic surveillance starting at age Once the number of polyps increases to a level that eliminates the possibility of safe endoscopic treatment, prophylactic total colectomy or subtotal colectomy followed by annual endoscopy of the remaining rectum is recommended. Patients with FAP are also at an increased risk for other malignancies, particularly small bowel, stomach, and extraintestinal neoplasia such as desmoid tumours, papillary thyroid carcinoma, sarcomas, hepatoblastoma, pancreatic carcinoma, and medulloblastoma. Although it is recommended that FAP patients be screened for duodenal s with upper endoscopy, APC mutation COX-2 overexpression Figure 1 action. k-ras mutation 18q genes P53 mutation Normal epithelium Dysplastic aberrant cryptic foci Early Intermediate Late Carcinoma Multistep progression of colon cancer and sites of NSAID screening for other extracolonic tumours is not routinely performed. Chemoprevention in FAP has been studied intensively both in animals and humans, using agents such as ascorbic acid, calcium, and, most promisingly, NSAIDs. FAP research has benefited from a mutant mouse model with multiple intestinal neoplasias (Min), which harbours mutations of the APC gene Multiple studies using the Min mouse model have provided encouraging results with both nonselective and selective NSAIDs, reducing tumour burden, size, and multiplicity. 20 In humans, numerous uncontrolled and controlled studies have evaluated the effects of NSAIDS, particularly sulindac, and now the more selective COX-2 inhibitor celecoxib, on polyp size and number (table 1). The data are encouraging, and celecoxib was shown in one study to cause regression of polyps in patients with FAP. 21 However, studies have additionally shown that withdrawal of treatment results in the recurrence of polyps, and patients receiving sulindac therapy have been reported to develop CRC. 20 Therefore, because of concerns regarding the length of treatment required, the development of CRC in patients receiving treatment, chemoprevention with NSAIDS has not replaced conventional endoscopic surveillance and colectomy recommendations in FAP patients. Of particular interest in FAP are common extracolonic malignancies such as desmoid tumours and duodenal adenocarcinomas, which represent important targets for chemoprevention agents. Studies have shown that sulindac may be effective in the treatment of early duodenal s in FAP. 22 Celecoxib at a dose of 400 mg twice daily has been shown to decrease duodenal polyposis in patients with clinically significant disease at baseline (greater than 5% covered by polyps), a 31% reduction in involved areas compared with 8% taking placebo (p = 0.049). 23 No studies have shown the utility of NSAIDs in treating desmoid tumours. Currently, no definitive recommendations have been formulated regarding the use of NSAIDs in patients with FAP. Based upon the studies mentioned above, some centres are increasingly using NSAIDs to delay the necessity for colectomy, and thereafter to decrease polyp formation in the retained rectum after subtotal colectomy. Celecoxib was approved recently by the US Food and Drug Administration for use in this setting. Additionally, the use of NSAIDs, particularly celecoxib, seems to be a useful adjunct in patients with duodenal polyposis. Chemoprevention with NSAIDs in HNPCC has not been as vigorously evaluated either in animal models or in human trials. Interestingly, COX-2 is overexpressed less commonly in HNPCC than in sporadic CRC. 24 Conversely, aspirin and sulindac have been shown to reduce the microsatellite instability (MSI) phenotype of CRC cell lines caused by mutations in the hmlh1, hmsh2, and hmsh6 genes. 24 Further studies are required, and an ongoing trial, concerted action polyp prevention (CAPP II), will shed further light on the role of NSAIDs in HNPCC. CHEMOPREVENTION IN SPORADIC COLON CANCER Studies showing the efficacy of NSAIDs in hereditary CRC have provided a basis for investigating the role of NSAIDs in primary and secondary prevention of sporadic CRC. Several large prospective cohort and randomised, placebo controlled trials have examined aspirin as a chemopreventive agent, both in preventing CRC and the development of polyps. Table 2 provides an overview of the trials. Three major prospective cohort studies addressed the effect of primary prophylaxis with aspirin on CRC. In the cancer prevention study II, people answered questionnaires regarding their aspirin use, with death from CRC the primary
3 Non-steroidals and colorectal cancer prevention 225 Table 1 Randomised, placebo controlled trials of colorectal cancer chemoprevention in familial tous polyposis Study Patients (n) Agent Dose Outcome Labayle et al 33 9 Sulindac 100 mg thrice daily Decrease in polyp number compared with placebo (p,0.01) Nugent et al Sulindac 200 mg twice daily Decrease in polyp number compared with placebo (p = 0.01) Giardiello et al Celecoxib 100 mg twice daily 44% decrease in polyp number (p = 0.014) Steinbach et al Celecoxib 100 mg twice daily 12% decrease in polyp number Celecoxib 400 mg twice daily 28% decrease in polyp number (p = 0.33 and p = respectively) end point of the study. 25 More frequent use of aspirin, at least 16 times a month, was associated with a noticeable decrease in the relative risk, 0.60 for men and 0.58 for women (95% confidence intervals, 0.40 to 0.89 and 0.37 to 0.90, respectively). Similarly, two other cohort studies, the health professionals follow-up study and the nurses health study, found a decrease in the relative risk for developing CRC with regular aspirin use. Interestingly, in the second study, minimal risk reduction with aspirin use was detected during the initial nine years, but the relative risk declined to 0.56 after 20 years of use. 27 Although these studies found a protective benefit among aspirin users, the duration and frequency of dosing has yet to be established. Only one randomised, placebo controlled trial has addressed the effect of aspirin on the development of CRC. The physicians health study followed up male physicians, primarily to assess the effect of aspirin on the risk of developing coronary artery disease. 28 Analysis of the data with respect to CRC showed no significant difference between the treatment and control groups. Notably, the treatment was 325 mg every other day, continuously for five years, and the patients were followed up for 12 years thereafter. It is possible that the treatment and follow up periods were of insufficient duration to show significant differences, as the development of CRC from the precursor lesion averages 10 or more years. Perhaps a more viable end point in evaluating the efficacy of aspirin treatment would be the development of tous polyps. Two recent, well designed trials have been published addressing this very issue. Sandler et al randomised 635 patients with previous CRC, definitively cured, to receive either 325 mg of aspirin daily or a placebo. 29 The study was Table 2 Chemoprevention trials in non-hereditary colon cancer terminated after a median treatment period of 31 months, at which time one or more s were found in 17% of patients taking aspirin and 27% of patients taking placebo (p = 0.004). Another study, published at the same time, randomised 1121 patients with history of recent s to receive placebo, 81 mg of aspirin, or 325 mg of aspirin daily. 30 A follow up colonoscopy was performed about one year after randomisation in 1084 of the patients. The incidence of one or more s was 47% in the placebo group, 38% in the 81 mg aspirin group, and 45% in the 325 mg aspirin group (global p = 0.04). More importantly, for the larger s, measuring at least 1 cm or with tubulovillous or villous features, the relative risks were as follows: 0.59 (95% confidence intervals, 0.38 to 0.92) for the 81 mg treatment arm, and 0.83 (95% confidence intervals, 0.55 to 1.23) for the 325 mg treatment arm. The authors did not provide a clear explanation for the greater risk reduction with the lower aspirin dose. They speculated that the most probable reason for the difference was chance, as both the 81 mg and the 325 mg dose seem to suppress prostaglandin values to similar extents. There was no significant difference in the incidence of adverse events among the various patient groups, including gastrointestinal haemorrhage and haemorrhagic stroke, which might be attributable to the short duration of aspirin treatment. Once again, these trials provide encouraging data regarding aspirin use, especially in secondary prophylaxis for patients with a history of s or CRC. The duration and dose are, however, not well established (one trial curiously found the 81 mg dose to be more effective than the 325 mg dose 30 ), and the cumulative safety profile must be weighed against the benefit of the treatment. Furthermore, additional studies need Study Design Number Agent Outcome Thun et al 25 (cancer prevention study II) Prospective cohort Aspirin Relative risk reduction of death from colorectal cancer 0.60 for men and 0.58 for women Giovannucci et al 26 (health professionals study) Prospective cohort Aspirin Relative risk of colon cancer decreased to 0.35 with continuous, regular use Giovannucci et al 27 (curses health study) Prospective cohort Aspirin Relative risk of colon cancer decreased to 0.56 with 20 years of regular use Gann et al 28, Sturmer et al 36 (physicians health study) Randomised, placebo controlled, then prospective cohort Aspirin No significant difference in colon cancer even after 12 years of follow up Baron et al 30 (polyp prevention study) Randomised, placebo controlled 1121 Aspirin Relative risk of large (at least 1 cm) decreased to 0.59 in patients receiving 81 mg aspirin daily Sandler et al 29 (colorectal prevention study) Randomised, placebo 635 Aspirin Relative risk of recurrent in patients with prior colorectal cancer was decreased to 0.65
4 226 Sangha, Yao, Wolfe to be done to assess if secondary prophylaxis can actually be helpful in reducing the frequency of surveillance colonoscopy. Cost effectiveness and safety of aspirin for primary prophylaxis are even less clear, because such an approach would require long term use, greater than 10 years, in a large segment of the population only at average risk for CRC. Chemoprevention would also require a comparison with successful screening strategies already in place. DISCUSSION In summary, several recent experimental, epidemiological, and controlled trials have investigated the usefulness of NSAIDs in CRC chemoprevention. The major cohort studies and placebo controlled trials in FAP and sporadic CRC prevention are summarised in tables 1 and 2. At this stage, no definitive recommendations have been established regarding the use of any NSAIDs or aspirin in primary or secondary prophylaxis, or as a substitute for screening or surveillance protocols. The most promising arena for NSAID use is secondary prophylaxis in patients who have had CRC or s in the past. These patients are at an increased risk for developing further lesions, and the benefit of prophylaxis may thus outweigh the risks of major gastrointestinal bleeding or haemorrhagic stroke associated with the use of these agents. Further studies need to investigate whether NSAID prophylaxis can reduce current endoscopic surveillance recommendations. In addition, long term studies evaluating the use of selective COX-2 inhibitors, which seem to carry a lower risk for the development of gastrointestinal haemorrhage, 31 will be necessary before recommending their use for not only secondary, but also primary, CRC prophylaxis. The use of NSAIDs or aspirin in primary prevention of CRC has not been validated. Chemoprophylaxis in average risk patients would require regular aspirin use for at least 10 to 20 years, and the cumulative risk of major adverse events may outweigh any reduction in CRC risk. Interestingly, although the benefit of aspirin in coronary artery disease has been established, the US Preventive Services Task Force does not recommend aspirin unless the five year risk for coronary Key points N NSAIDs are potent inhibitors of cyclooxygenase (COX) enzymes. Studies have shown NSAIDs produce their antineoplastic effect through COX dependent and independent pathways. N NSAIDs were first studied intensively in hereditary CRC, particularly FAP. Currently, certain centres use NSAIDs to delay the time to colectomy, as prophylaxis in patients with retained rectum after subtotal colectomy, and also as chemoprevention for duodenal polyposis. This approach does not presently affect recommendations for surveillance. N In sporadic CRC, the most promising arena for NSAID use is secondary prophylaxis in patients who have had either CRC or s in the past. N Use of NSAIDs or aspirin in primary prevention of CRC has not been validated. Chemoprophylaxis in average risk patients would require regular medication use for at least years, and the cumulative risk of major adverse events may outweigh any reduction in CRC risk. N Chemoprophylaxis with NSAIDs/aspirin does not replace or change current recommendations for CRC screening or surveillance. artery disease is at least three 3%. 32 In fact, cost effectiveness analyses of aspirin for primary prophylaxis have shown an increase in cost per life saved when compared with any of the current screening recommendations. 32 In conclusion, to better appreciate the cost and side effects of aspirin in primary and secondary CRC chemoprophylaxis, it is useful to compare the number of people needed to be treated to achieve particular end points. For primary prevention of CRC or death from CRC, the numbers needed to treat are and 1250, respectively. Because primary prophylaxis requires treatment for at least 10 years or more, toxicity related to aspirin becomes an additional concern. This point is further highlighted upon reviewing the numbers needed to treat for adverse effects: 100 for gastrointestinal haemorrhage, for major gastrointestinal haemorrhage, and 800 for haemorrhagic stroke. In contrast, for secondary prevention of of any size or prevention of advanced neoplasm, the number of people needed to achieve significance are 10 and 19, respectively. 32 These data seem to support the usefulness of aspirin for secondary CRC prophylaxis, but not necessarily primary prevention.... Authors affiliations S Sangha, M Yao, M M Wolfe, Section of Gastroenterology, Boston University School of Medicine, Boston, Massachusetts, USA Funding: none Conflicts of interest: none declared. REFERENCES 1 Jemal A, Murray T, Samuels A, et al. Cancer statistics, CA Cancer J Clin 2003;53: Williams AR, Balasooriya BA, Day DW. Polyps and cancer of the large bowel: a necropsy study in Liverpool. Gut 1982;23: Giovannucci E, Stampfer MJ, Colditz GA, et al. Folate, methionine, and alcohol intake and risk of colorectal. J Natl Cancer Inst 1993;85: Vane JR. Inhibition of prostaglandin synthesis as a mechanism of action for aspirin-like drugs. Nat New Biol 1971;231: Masferrer JL, Seibert K, Zweifel B, et al. Endogenous glucocorticoids regulate an inducible cyclooxygenase enzyme. Proc Natl Acad Sci U S A 1992;89: Kujubu DA, Fletcher BS, Varnum BC, et al. TIS10, a phorbol ester tumor promoter-inducible mrna from Swiss 3T3 cells, encodes a novel prostaglandin synthase/cyclooxygenase homologue. J Biol Chem 1991;266: Tsujii M, Kawano S, DuBois RN. Cyclooxygenase-2 expression in human colon cancer cells increases metastatic potential. Proc Natl Acad Sci U S A 1997;94: Kargman SL, O Neill GP, Vickers PJ, et al. Expression of prostaglandin G/H synthase-1 and -2 protein in human colon cancer. Cancer Res 1995;55: Oshima M, Dinchuk JE, Kargman SL, et al. Suppression of intestinal polyposis in Apc delta716 knockout mice by inhibition of cyclooxygenase 2 (COX-2). Cell 1996;87: Reddy BS, Rao CV, Seibert K. Evaluation of cyclooxygenase-2 inhibitor for potential chemopreventive properties in colon carcinogenesis. Cancer Res 1996;56: Oshima M, Murai N, Kargman S, et al. Chemoprevention of intestinal polyposis in the Apcdelta716 mouse by rofecoxib, a specific cyclooxygenase- 2 inhibitor. Cancer Res 2001;61: Yoshimi N, Kawabata K, Hara A, et al. Inhibitory effect of NS-398, a selective cyclooxygenase-2 inhibitor, on azoxymethane-induced aberrant crypt foci in colon carcinogenesis of F344 rats. Jpn J Cancer Res 1997;88: Kawamori T, Rao CV, Seibert K, et al. Chemopreventive activity of celecoxib, a specific cyclooxygenase-2 inhibitor, against colon carcinogenesis. Cancer Res 1998;58: Janne PA, Mayer RJ. Chemoprevention of colorectal cancer. N Engl J Med 2000;342: Chan TA. Nonsteroidal anti-inflammatory drugs, apoptosis, and colon-cancer chemoprevention. Lancet Oncol 2002;3: Lynch HT, de la Chapelle A. Hereditary colorectal cancer. N Engl J Med 2003;348: Moser AR, Pitot HC, Dove WF. A dominant mutation that predisposes to multiple intestinal neoplasia in the mouse. Science 1990;247: Su LK, Kinzler KW, Vogelstein B, et al. Multiple intestinal neoplasia caused by a mutation in the murine homolog of the APC gene. Science 1992;256: Levy DB, Smith KJ, Beazer-Barclay Y, et al. Inactivation of both APC alleles in human and mouse tumors. Cancer Res 1994;54:
5 Non-steroidals and colorectal cancer prevention Hawk E, Lubet R, Limburg P. Chemoprevention in hereditary colorectal cancer syndromes. Cancer 1999;86(suppl 11): Steinbach G, Lynch PM, Phillips RK, et al. The effect of celecoxib, a cyclooxygenase-2 inhibitor, in familial tous polyposis. N Engl J Med 2000;342: Debinski HS, Trojan J, Nugent KP, et al. Effect of sulindac on small polyps in familial tous polyposis. Lancet 1995;345: Phillips RK, Wallace MH, Lynch PM, et al. A randomised, double blind, placebo controlled study of celecoxib, a selective cyclooxygenase 2 inhibitor, on duodenal polyposis in familial tous polyposis. Gut 2002;50: Sinicrope FA, Lemoine M, Xi L, et al. Reduced expression of cyclooxygenase 2 proteins in hereditary nonpolyposis colorectal cancers relative to sporadic cancers. Gastroenterology 1999;117: Thun MJ, Namboodiri MM, Heath CW Jr. Aspirin use and reduced risk of fatal colon cancer. N Engl J Med 1991;325: Giovannucci E, Rimm EB, Stampfer MJ, et al. Aspirin use and the risk for colorectal cancer and in male health professionals. Ann Intern Med 1994;121: Giovannucci E, Egan KM, Hunter DJ, et al. Aspirin and the risk of colorectal cancer in women. N Engl J Med 1995;333: Gann PH, Manson JE, Glynn RJ, et al. Low-dose aspirin and incidence of colorectal tumors in a randomized trial. J Natl Cancer Inst 1993;85: Sandler RS, Halabi S, Baron JA, et al. A randomized trial of aspirin to prevent colorectal s in patients with previous colorectal cancer. N Engl J Med 2003;348: Baron JA, Cole BF, Sandler RS, et al. A randomized trial of aspirin to prevent colorectal s. N Engl J Med 2003;348: Bombardier C, Laine L, Reicin A, et al. Comparison of upper gastrointestinal toxicity of rofecoxib and naproxen in patients with rheumatoid arthritis. VIGOR Study Group. N Engl J Med 2000;343: Imperiale TF. Aspirin and the prevention of colorectal cancer. N Engl J Med 2003;348: Labayle D, Fischer D, Vielh P, et al. Sulindac causes regression of rectal polyps in familial tous polyposis. Gastroenterology 1991;101: Nugent KP, Farmer KC, Spigelman AD, et al. Randomized controlled trial of the effect of sulindac on duodenal and rectal polyposis and cell proliferation in patients with familial tous polyposis. Br J Surg 1993;80: Giardiello FM, Hamilton SR, Krush AJ, et al. Treatment of colonic and rectal s with sulindac in familial tous polyposis. N Engl J Med 1993;328: Sturmer T, Glynn RJ, Lee IM, et al. Aspirin use and colorectal cancer: post-trial follow-up data from the physicians health study. Ann Intern Med 1998;128: FILLER... SMON, clioquinol, and copper I n addition to being an antimicrobial, clioquinol is a copper-zinc (Cu-Zn) chelator. Recent understanding of the metallobiology of Alzheimer s disease (AD) has led to renewed interest in clioquinol. Knowledge regarding metal-ion metabolism in the brain has suggested that Ab precipitation and toxicity in AD is caused by abnormal interaction with metal ions like Cu and Zn. 1 Cu and Zn are found at high levels in neocortical regions prone to AD abnormality. Clioquinol has been shown to increase solubilisation of Ab in the AD plaque from postmortem human brain tissue and to reduce brain Ab deposition in a transgenic mouse model of AD. 2 These bench findings led to a pilot clinical trial of clioquinol in AD that showed the drug to be well tolerated. 3 Plasma Ab 42 concentrations decreased in the clioquinol group, plasma Zn concentrations increased, and there was no effect on plasma Cu. The authors felt that metal protein attenuating compound drugs like clioquinol are not gross tissue chelators, but facilitate dissociation of Cu and Zn from the lowest affinity metal binding sites on Ab. Alternatively, the clioquinol dose might have been too low to have an impact on serum Cu concentrations. Subacute myelo-optico-neuropathy (SMON) is characterised by paraparesis, sensory deficits, and visual impairment. The pathological findings include symmetrical demyelination of the lateral and posterior columns of the spinal cord with optic nerve and peripheral nerve involvement. Extensive epidemiological studies in Japan confirmed that SMON was attributable to ingestion of the antibacterial clioquinol. There were nearly cases of SMON in Japan by the end of This led to banning of clioquinol in Subsequently new cases of SMON disappeared. Before clioquinol can be studied on a large scale basis as a treatment for AD, its relation to SMON must be resolved. The mechanism of clioquinol induced SMON was never definitively established. Hypotheses include mitochondrial toxicity of the clioquinol-zn chelate and vitamin B12 deficiency. We propose a mechanism in which Cu is the mediator. Cu deficiency myelopathy bears striking similarities to the subacute combined degeneration seen in vitamin B12 deficiency 4 and to SMON. Optic neuritis has been reported in association with Cu deficiency. 5 Cu deficiency in ruminants is known to cause an ataxic myelopathy characterised by demyelination of the spinal cord white matter. We believe that a plausible mechanism of SMON is clioquinol induced Cu deficiency. The re-emergence of interest in clioquinol makes testing this hypothesis in available animal models an important issue. N Kumar, D S Knopman, Department of Neurology, Mayo Clinic, Rochester, USA Correspondence to: Dr N Kumar, 200 First Street, SW, Rochester, MN 55905, USA; kumar.neeraj@mayo.edu REFERENCES 1 Bush AI. The metallobiology of Alzheimer s disease. Trends Neurosci 2003;26: Cherny RA, Atwood CS, Xilinas ME, et al. Treatment with a copper-zinc chelator markedly and rapidly inhibits betaamyloid accumulation in Alzheimer s disease transgenic mice. Neuron 2001;30: Ritchie CW, Bush AI, Mackinnon A, et al. Metal-protein attenuation with iodochlorhydroxyquin (clioquinol) targeting Abeta amyloid deposition and toxicity in Alzheimer disease: a pilot phase 2 clinical trial. Arch Neurol 2003;60: Kumar N, Gross JB, Ahlskog EA. Copper deficiency myelopathy produces a clinical picture like subacute combined degeneration. Neurology 2004;63: Gregg XT, Reddy V, Prchal JT. Copper deficiency masquerading as myelodysplastic syndrome. Blood 2002;100:
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions. South Island Cancer Nurses Network September 2013
 For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
colorectal cancer Colorectal cancer hereditary sporadic Familial 1/12/2018
 colorectal cancer Adenocarcinoma of the colon and rectum is the third most common site of new cancer cases and deaths in men (following prostate and lung or bronchus cancer) and women (following breast
colorectal cancer Adenocarcinoma of the colon and rectum is the third most common site of new cancer cases and deaths in men (following prostate and lung or bronchus cancer) and women (following breast
Familial and Hereditary Colon Cancer
 Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial Adenomatous Polyposis
 Familial Adenomatous Polyposis 1 in 10,000 incidence 100 s to 1000 s of colonic adenomas by teens Cancer risk: colon, gastric, duodenum (periampulla), small bowel, pancreas, papillary thyroid, childhood
Familial Adenomatous Polyposis 1 in 10,000 incidence 100 s to 1000 s of colonic adenomas by teens Cancer risk: colon, gastric, duodenum (periampulla), small bowel, pancreas, papillary thyroid, childhood
Familial and Hereditary Colon Cancer
 Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Risk of Colorectal Cancer (CRC) Hereditary Syndromes in GI Cancer GENETIC MALPRACTICE
 Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Colorectal Neoplasia. Dr. Smita Devani MBChB, MRCP. Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi
 Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Personalized Aspirin Therapy
 Personalized Aspirin Therapy Nadir Arber, MD, MSc, MHA Head - Integrated Cancer Prevention Center Tel Aviv Medical Centre and Tel Aviv University Heidelberg 2014 CRC is Preventable Early detection Chemoprevention
Personalized Aspirin Therapy Nadir Arber, MD, MSc, MHA Head - Integrated Cancer Prevention Center Tel Aviv Medical Centre and Tel Aviv University Heidelberg 2014 CRC is Preventable Early detection Chemoprevention
The New England Journal of Medicine THE EFFECT OF CELECOXIB, A CYCLOOXYGENASE-2 INHIBITOR, IN FAMILIAL ADENOMATOUS POLYPOSIS
 THE EFFECT OF, A CYCLOOXYGENASE-2 INHIBITOR, IN FAMILIAL ADENOMATOUS POLYPOSIS GIDEON STEINBACH, M.D., PH.D., PATRICK M. LYNCH, M.D., J.D., ROBIN K.S. PHILLIPS, M.B., B.S., MARINA H. WALLACE, M.B., B.S.,
THE EFFECT OF, A CYCLOOXYGENASE-2 INHIBITOR, IN FAMILIAL ADENOMATOUS POLYPOSIS GIDEON STEINBACH, M.D., PH.D., PATRICK M. LYNCH, M.D., J.D., ROBIN K.S. PHILLIPS, M.B., B.S., MARINA H. WALLACE, M.B., B.S.,
Mr Chris Wakeman. General Surgeon University of Otago, Christchurch. 12:15-12:40 Management of Colorectal Cancer
 Mr Chris Wakeman General Surgeon University of Otago, Christchurch 12:15-12:40 Management of Colorectal Cancer Bowel cancer Chris Wakeman Colorectal Surgeon Christchurch Sam Simon (Simpsons) Elizabeth
Mr Chris Wakeman General Surgeon University of Otago, Christchurch 12:15-12:40 Management of Colorectal Cancer Bowel cancer Chris Wakeman Colorectal Surgeon Christchurch Sam Simon (Simpsons) Elizabeth
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS. Family Health Clinical Genetics. Clinical Genetics department
 GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
PENETRANCE ACTIONABILITY SIGNIFICANCE/BURDEN OF DISEASE NEXT STEPS. YES ( 1 of above) YES (Proceed to Stage II)
 Stage I: Binning Dashboard GENE/GENE PANEL: APC ACTIONABILITY 1. Is there a qualifying resource, such as a practice guideline or systematic review, for the genetic condition? 2. Does the practice guideline
Stage I: Binning Dashboard GENE/GENE PANEL: APC ACTIONABILITY 1. Is there a qualifying resource, such as a practice guideline or systematic review, for the genetic condition? 2. Does the practice guideline
B Base excision repair, in MUTYH-associated polyposis and colorectal cancer, BRAF testing, for hereditary colorectal cancer, 696
 Index Note: Page numbers of article titles are in boldface type. A Adenomatous polyposis, familial. See Familial adenomatous polyposis. Anal anastomosis, ileal-pouch, proctocolectomy with, in FAP, 591
Index Note: Page numbers of article titles are in boldface type. A Adenomatous polyposis, familial. See Familial adenomatous polyposis. Anal anastomosis, ileal-pouch, proctocolectomy with, in FAP, 591
Prevention and Early Detection of Colorectal Cancer
 Prevention and Early Detection of Colorectal Cancer JMAJ 44(6): 255 259, 2001 Toshio SAWADA Vice Director, Gunma Prefectural Cancer Center Abstract: Chemoprevention and early detection are key to reducing
Prevention and Early Detection of Colorectal Cancer JMAJ 44(6): 255 259, 2001 Toshio SAWADA Vice Director, Gunma Prefectural Cancer Center Abstract: Chemoprevention and early detection are key to reducing
Hereditary Colorectal Cancer Syndromes Miguel A. Rodriguez-Bigas, MD
 Hereditary Colorectal Cancer Syndromes Miguel A. Rodriguez-Bigas, MD Living Beyond Cancer A-Z January 12,2019 Hereditary CRC Syndromes Objectives are to discuss the : Most common Hereditary CRC syndromes
Hereditary Colorectal Cancer Syndromes Miguel A. Rodriguez-Bigas, MD Living Beyond Cancer A-Z January 12,2019 Hereditary CRC Syndromes Objectives are to discuss the : Most common Hereditary CRC syndromes
YES NO UNKNOWN. Stage I: Rule-Out Dashboard ACTIONABILITY PENETRANCE SIGNIFICANCE/BURDEN OF DISEASE NEXT STEPS. YES ( 1 of above)
 Stage I: Rule-Out Dashboard GENE/GENE PANEL: SMAD4, BMPR1A DISORDER: Juvenile Polyposis Syndrome HGNC ID: 6670, 1076 OMIM ID: 174900, 175050 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource,
Stage I: Rule-Out Dashboard GENE/GENE PANEL: SMAD4, BMPR1A DISORDER: Juvenile Polyposis Syndrome HGNC ID: 6670, 1076 OMIM ID: 174900, 175050 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource,
Precision Cancer Prevention: Hereditary Polyposis Syndromes
 Precision Cancer Prevention: Hereditary Polyposis Syndromes N. Jewel Samadder, MD, MSC, FRCPC HUNTSMAN CANCER INSTITUTE UNIVERSITY OF UTAH Familial Adenomatous Polyposis Familial Adenomatous Polyposis
Precision Cancer Prevention: Hereditary Polyposis Syndromes N. Jewel Samadder, MD, MSC, FRCPC HUNTSMAN CANCER INSTITUTE UNIVERSITY OF UTAH Familial Adenomatous Polyposis Familial Adenomatous Polyposis
Multistep nature of cancer development. Cancer genes
 Multistep nature of cancer development Phenotypic progression loss of control over cell growth/death (neoplasm) invasiveness (carcinoma) distal spread (metastatic tumor) Genetic progression multiple genetic
Multistep nature of cancer development Phenotypic progression loss of control over cell growth/death (neoplasm) invasiveness (carcinoma) distal spread (metastatic tumor) Genetic progression multiple genetic
Colonic polyps and colon cancer. Andrew Macpherson Director of Gastroentology University of Bern
 Colonic polyps and colon cancer Andrew Macpherson Director of Gastroentology University of Bern Improtance of the problem of colon cancers - Epidemiology Lifetime risk 5% Incidence/10 5 /annum (US Detroit
Colonic polyps and colon cancer Andrew Macpherson Director of Gastroentology University of Bern Improtance of the problem of colon cancers - Epidemiology Lifetime risk 5% Incidence/10 5 /annum (US Detroit
Colorectal adenocarcinoma leading cancer in developed countries In US, annual deaths due to colorectal adenocarcinoma 57,000.
 Colonic Neoplasia Remotti Colorectal adenocarcinoma leading cancer in developed countries In US, annual incidence of colorectal adenocarcinoma 150,000. In US, annual deaths due to colorectal adenocarcinoma
Colonic Neoplasia Remotti Colorectal adenocarcinoma leading cancer in developed countries In US, annual incidence of colorectal adenocarcinoma 150,000. In US, annual deaths due to colorectal adenocarcinoma
Colonic Polyp. Najmeh Aletaha. MD
 Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Chemoprevention of Colorectal Cancer: Where We Stand
 Chemoprevention of Colorectal Cancer: Where We Stand Andrew T. Chan, MD, MPH Division of Gastroenterology Massachusetts General Hospital 2 nd World Congress on Controversies in Gastroenterology Xi an,
Chemoprevention of Colorectal Cancer: Where We Stand Andrew T. Chan, MD, MPH Division of Gastroenterology Massachusetts General Hospital 2 nd World Congress on Controversies in Gastroenterology Xi an,
1. Colorectal cancer epidemiology. Assessing and managing risk. Prevention
 Research Signpost 37/661 (2), Fort P.O. Trivandrum-695 023 Kerala, India The Challenge of Colorectal Cancer: A Review Book, 2011: 1-33 ISBN: 978-81-308-0460-6 Editor: Esther Uña Cidón 1. Colorectal cancer
Research Signpost 37/661 (2), Fort P.O. Trivandrum-695 023 Kerala, India The Challenge of Colorectal Cancer: A Review Book, 2011: 1-33 ISBN: 978-81-308-0460-6 Editor: Esther Uña Cidón 1. Colorectal cancer
Gastrointestinal Safety of Coxibs and Outcomes Studies: What s the Verdict?
 Vol. 23 No. 4S April 2002 Journal of Pain and Symptom Management S5 Proceedings from the Symposium The Evolution of Anti-Inflammatory Treatments in Arthritis: Current and Future Perspectives Gastrointestinal
Vol. 23 No. 4S April 2002 Journal of Pain and Symptom Management S5 Proceedings from the Symposium The Evolution of Anti-Inflammatory Treatments in Arthritis: Current and Future Perspectives Gastrointestinal
Latest Endoscopic Guidelines for FAP, HNPCC, IBD, and the General Population
 Latest Endoscopic Guidelines for FAP, HNPCC, IBD, and the General Population David T. Rubin, M.D. Assistant Professor of Medicine Inflammatory Bowel Disease Center MacLean Center for Clinical Medical Ethics
Latest Endoscopic Guidelines for FAP, HNPCC, IBD, and the General Population David T. Rubin, M.D. Assistant Professor of Medicine Inflammatory Bowel Disease Center MacLean Center for Clinical Medical Ethics
Issues in Emerging Health Technologies
 Issues in Emerging Health Technologies Issue 9 Dec 1999 COX-2 Inhibitors: A Role in Colorectal Cancer? The Technology Celecoxib is the first of a new class of nonsteroidal anti-inflammatory drugs (NSAIDS)
Issues in Emerging Health Technologies Issue 9 Dec 1999 COX-2 Inhibitors: A Role in Colorectal Cancer? The Technology Celecoxib is the first of a new class of nonsteroidal anti-inflammatory drugs (NSAIDS)
Primary Care Approach to Genetic Cancer Syndromes
 Primary Care Approach to Genetic Cancer Syndromes Jason M. Goldman, MD, FACP FAU School of Medicine Syndromes Hereditary Breast and Ovarian Cancer (HBOC) Hereditary Nonpolyposis Colorectal Cancer (HNPCC)
Primary Care Approach to Genetic Cancer Syndromes Jason M. Goldman, MD, FACP FAU School of Medicine Syndromes Hereditary Breast and Ovarian Cancer (HBOC) Hereditary Nonpolyposis Colorectal Cancer (HNPCC)
Cancer Genomics 101. BCCCP 2015 Annual Meeting
 Cancer Genomics 101 BCCCP 2015 Annual Meeting Objectives Identify red flags in a person s personal and family medical history that indicate a potential inherited susceptibility to cancer Develop a systematic
Cancer Genomics 101 BCCCP 2015 Annual Meeting Objectives Identify red flags in a person s personal and family medical history that indicate a potential inherited susceptibility to cancer Develop a systematic
Colon Cancer Screening & Surveillance. Amit Patel, MD PGY-4 GI Fellow
 Colon Cancer Screening & Surveillance Amit Patel, MD PGY-4 GI Fellow Epidemiology CRC incidence and mortality rates vary markedly around the world. Globally, CRC is the third most commonly diagnosed cancer
Colon Cancer Screening & Surveillance Amit Patel, MD PGY-4 GI Fellow Epidemiology CRC incidence and mortality rates vary markedly around the world. Globally, CRC is the third most commonly diagnosed cancer
EARLY DETECTION OF COLORECTAL CANCER. Epidemiology of CRC
 Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER Epidemiology of CRC Colorectal cancer (CRC) is a common and lethal disease Environmental
Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER Epidemiology of CRC Colorectal cancer (CRC) is a common and lethal disease Environmental
Chemoprevention of Colorectal Cancer: Ready for Routine Use?
 RRCR (2005) 166:213--230 Springer-Verlag 2005 Chemoprevention of Colorectal Cancer: Ready for Routine Use? Nadir Arber 1 ()) Bernard Levin 2 1 Department of Cancer Prevention, Tel-Aviv Medical Center,
RRCR (2005) 166:213--230 Springer-Verlag 2005 Chemoprevention of Colorectal Cancer: Ready for Routine Use? Nadir Arber 1 ()) Bernard Levin 2 1 Department of Cancer Prevention, Tel-Aviv Medical Center,
Hereditary Gastric Cancer
 Hereditary Gastric Cancer Dr Bastiaan de Boer Consultant Pathologist Department of Anatomical Pathology PathWest Laboratory Medicine, QE II Medical Centre Clinical Associate Professor School of Pathology
Hereditary Gastric Cancer Dr Bastiaan de Boer Consultant Pathologist Department of Anatomical Pathology PathWest Laboratory Medicine, QE II Medical Centre Clinical Associate Professor School of Pathology
GI Polyp syndromes in children. Screening and surveillance, surgery.
 Dr Warren Hyer Consultant Paediatric Gastroenterologist St Mark s Hospital, UK GI Polyp syndromes in children Screening and surveillance, surgery. No conflict of interests to declare Objectives Understand
Dr Warren Hyer Consultant Paediatric Gastroenterologist St Mark s Hospital, UK GI Polyp syndromes in children Screening and surveillance, surgery. No conflict of interests to declare Objectives Understand
Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER
 Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER Epidemiology of CRC Colorectal cancer (CRC) is a common and lethal disease Environmental
Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER Epidemiology of CRC Colorectal cancer (CRC) is a common and lethal disease Environmental
Endoscopic techniques for surveillance and treatment of FAP
 Endoscopic techniques for surveillance and treatment of FAP Evelien Dekker MD PhD Department of Gastroenterology & Hepatology Academic Medical Center Amsterdam The Netherlands FAP: endoscopic surveillance
Endoscopic techniques for surveillance and treatment of FAP Evelien Dekker MD PhD Department of Gastroenterology & Hepatology Academic Medical Center Amsterdam The Netherlands FAP: endoscopic surveillance
Characteristics of selective and non-selective NSAID use in Scotland
 Characteristics of selective and non-selective NSAID use in Scotland Alford KMG 1, Simpson C 1, Williams D 2 1 Department of General Practice & Primary Care, The University of Aberdeen. 2 Department of
Characteristics of selective and non-selective NSAID use in Scotland Alford KMG 1, Simpson C 1, Williams D 2 1 Department of General Practice & Primary Care, The University of Aberdeen. 2 Department of
Assessment of Correlation between Cyclo oxygen ase-2 Expression and Clinicopathological Features of Colorectal Carcinoma
 Med. J. Cairo Univ., Vol. 84, No. 1, September: 1029-1035, 2016 www.medicaljournalofcairouniversity.net Assessment of Correlation between Cyclo oxygen ase-2 Expression and Clinicopathological Features
Med. J. Cairo Univ., Vol. 84, No. 1, September: 1029-1035, 2016 www.medicaljournalofcairouniversity.net Assessment of Correlation between Cyclo oxygen ase-2 Expression and Clinicopathological Features
T he lifetime risk of developing colorectal cancer is 5%, with. Adenoma prevalence and cancer risk in familial non-polyposis colorectal cancer CANCER
 228 CANCER Adenoma prevalence and cancer risk in familial non-polyposis colorectal cancer G Lindgren, A Liljegren, E Jaramillo, C Rubio, A Lindblom... See end of article for authors affiliations... Correspondence
228 CANCER Adenoma prevalence and cancer risk in familial non-polyposis colorectal cancer G Lindgren, A Liljegren, E Jaramillo, C Rubio, A Lindblom... See end of article for authors affiliations... Correspondence
Objectives. Briefly summarize the current state of colorectal cancer
 Disclaimer I do not have any financial conflicts to disclose. I will not be promoting any service or product. This presentation is not meant to offer medical advice and is not intended to establish a standard
Disclaimer I do not have any financial conflicts to disclose. I will not be promoting any service or product. This presentation is not meant to offer medical advice and is not intended to establish a standard
Summary. Cezary ŁozińskiABDF, Witold KyclerABCDEF. Rep Pract Oncol Radiother, 2007; 12(4):
 Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Aspirin use and potential mechanisms for colorectal cancer prevention.
 Aspirin use and potential mechanisms for colorectal cancer prevention. C S Williams,, W Smalley, R N DuBois J Clin Invest. 1997;100(6):1325-1329. https://doi.org/10.1172/jci119651. Perspective Find the
Aspirin use and potential mechanisms for colorectal cancer prevention. C S Williams,, W Smalley, R N DuBois J Clin Invest. 1997;100(6):1325-1329. https://doi.org/10.1172/jci119651. Perspective Find the
COLON CANCER GENETICS (FOR SURGEONS) Mark W. Arnold MD Chief, Division of Colon and Rectal Surgery Professor of Surgery The Ohio State University
 COLON CANCER GENETICS (FOR SURGEONS) Mark W. Arnold MD Chief, Division of Colon and Rectal Surgery Professor of Surgery The Ohio State University 1. I am a surgeon; of course I have nothing to disclose.
COLON CANCER GENETICS (FOR SURGEONS) Mark W. Arnold MD Chief, Division of Colon and Rectal Surgery Professor of Surgery The Ohio State University 1. I am a surgeon; of course I have nothing to disclose.
CANCER. Inherited Cancer Syndromes. Affects 25% of US population. Kills 19% of US population (2nd largest killer after heart disease)
 CANCER Affects 25% of US population Kills 19% of US population (2nd largest killer after heart disease) NOT one disease but 200-300 different defects Etiologic Factors In Cancer: Relative contributions
CANCER Affects 25% of US population Kills 19% of US population (2nd largest killer after heart disease) NOT one disease but 200-300 different defects Etiologic Factors In Cancer: Relative contributions
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines
 Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
COX-2 inhibitors: A cautionary tale. October 2, 2006
 COX-2 inhibitors: A cautionary tale October 2, 2006 Molecular interventions in human disease... An approach as old as human civilization. With whom the herbs have come together Like kingly chiefs unto
COX-2 inhibitors: A cautionary tale October 2, 2006 Molecular interventions in human disease... An approach as old as human civilization. With whom the herbs have come together Like kingly chiefs unto
27
 26 27 28 29 30 31 32 33 34 35 Diagnosis:? Diagnosis: Juvenile Polyposis with BMPR1A Mutation 36 Juvenile Polyposis Syndrome Rare Autosomal Dominant Disorder with Multiple Juvenile Polyps in GI Tract Juvenile
26 27 28 29 30 31 32 33 34 35 Diagnosis:? Diagnosis: Juvenile Polyposis with BMPR1A Mutation 36 Juvenile Polyposis Syndrome Rare Autosomal Dominant Disorder with Multiple Juvenile Polyps in GI Tract Juvenile
Pathology reports, related operative reports and consult letters must be provided with a request for assessment.
 Page 1 of 6 Polyposis Syndromes Inherited risk for colorectal cancer is associated with a number of polyposis syndromes (genes), some of which are well-defined and others are less common. Identification
Page 1 of 6 Polyposis Syndromes Inherited risk for colorectal cancer is associated with a number of polyposis syndromes (genes), some of which are well-defined and others are less common. Identification
The New England Journal of Medicine PRIMARY CHEMOPREVENTION OF FAMILIAL ADENOMATOUS POLYPOSIS WITH SULINDAC. Study Population
 PRIMARY CHEMOPREVENTION OF FAMILIAL ADENOMATOUS POLYPOSIS WITH SULINDAC FRANCIS M. GIARDIELLO, M.D., VINCENT W. YANG, M.D., PH.D., LINDA M. HYLIND, B.S., R.N., ANNE J. KRUSH, M.S., GLORIA M. PETERSEN,
PRIMARY CHEMOPREVENTION OF FAMILIAL ADENOMATOUS POLYPOSIS WITH SULINDAC FRANCIS M. GIARDIELLO, M.D., VINCENT W. YANG, M.D., PH.D., LINDA M. HYLIND, B.S., R.N., ANNE J. KRUSH, M.S., GLORIA M. PETERSEN,
Colorectal Cancer. Mark Chapman. MA MS FRCS EBSQ(coloproct) 21 st March 2018 Consultant Coloproctologist
 Colorectal Cancer Mark Chapman MA MS FRCS EBSQ(coloproct) 21 st March 2018 Consultant Coloproctologist Overview Epidemiology of colorectal cancer Adenoma carcinoma sequence Tumour diagnosis & staging Treatment
Colorectal Cancer Mark Chapman MA MS FRCS EBSQ(coloproct) 21 st March 2018 Consultant Coloproctologist Overview Epidemiology of colorectal cancer Adenoma carcinoma sequence Tumour diagnosis & staging Treatment
Colon, or Colorectal, Cancer Information
 Colon, or Colorectal, Cancer Information Definition Colon, or colorectal, cancer is cancer that starts in the large intestine (colon) or the rectum (end of the colon). Other types of cancer can affect
Colon, or Colorectal, Cancer Information Definition Colon, or colorectal, cancer is cancer that starts in the large intestine (colon) or the rectum (end of the colon). Other types of cancer can affect
General Surgery Grand Grounds
 General Surgery Grand Grounds University of Colorado Health Sciences Center Case Presentation December 24, 2009 Adam Lackey, PGY-5 J.L. - 2111609 27 YO female with chief complaint of abdominal pain. PMHx:
General Surgery Grand Grounds University of Colorado Health Sciences Center Case Presentation December 24, 2009 Adam Lackey, PGY-5 J.L. - 2111609 27 YO female with chief complaint of abdominal pain. PMHx:
removal of adenomatous polyps detects important effectively as follow-up colonoscopy after both constitute a low-risk Patients with 1 or 2
 Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Development of Carcinoma Pathways
 The Construction of Genetic Pathway to Colorectal Cancer Moriah Wright, MD Clinical Fellow in Colorectal Surgery Creighton University School of Medicine Management of Colon and Diseases February 23, 2019
The Construction of Genetic Pathway to Colorectal Cancer Moriah Wright, MD Clinical Fellow in Colorectal Surgery Creighton University School of Medicine Management of Colon and Diseases February 23, 2019
PMS2 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table
 PMS2 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
PMS2 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal surgery prior as factor in laparoscopic colorectal surgery, 554 555 Abscess(es) CRC presenting as, 539 540 Adenocarcinoma of
Index Note: Page numbers of article titles are in boldface type. A Abdominal surgery prior as factor in laparoscopic colorectal surgery, 554 555 Abscess(es) CRC presenting as, 539 540 Adenocarcinoma of
RECENT RANDOMIZED INTERVENtion
 ORIGINAL CONTRIBUTION Long-term Use of Aspirin and Nonsteroidal Anti-inflammatory Drugs and Risk of Colorectal Cancer Andrew T. Chan, MD, MPH Edward L. Giovannucci, MD, ScD Jeffrey A. Meyerhardt, MD, MPH
ORIGINAL CONTRIBUTION Long-term Use of Aspirin and Nonsteroidal Anti-inflammatory Drugs and Risk of Colorectal Cancer Andrew T. Chan, MD, MPH Edward L. Giovannucci, MD, ScD Jeffrey A. Meyerhardt, MD, MPH
ACG Clinical Guideline: Colorectal Cancer Screening
 ACG Clinical Guideline: Colorectal Cancer Screening Douglas K. Rex, MD, FACG 1, David A. Johnson, MD, FACG 2, Joseph C. Anderson, MD 3, Phillip S. Schoenfeld, MD, MSEd, MSc (Epi), FACG 4, Carol A. Burke,
ACG Clinical Guideline: Colorectal Cancer Screening Douglas K. Rex, MD, FACG 1, David A. Johnson, MD, FACG 2, Joseph C. Anderson, MD 3, Phillip S. Schoenfeld, MD, MSEd, MSc (Epi), FACG 4, Carol A. Burke,
GENETICS OF COLORECTAL CANCER: HEREDITARY ASPECTS By. Magnitude of the Problem. Magnitude of the Problem. Cardinal Features of Lynch Syndrome
 GENETICS OF COLORECTAL CANCER: HEREDITARY ASPECTS By HENRY T. LYNCH, M.D. 1 Could this be hereditary Colon Cancer 4 Creighton University School of Medicine Omaha, Nebraska Magnitude of the Problem Annual
GENETICS OF COLORECTAL CANCER: HEREDITARY ASPECTS By HENRY T. LYNCH, M.D. 1 Could this be hereditary Colon Cancer 4 Creighton University School of Medicine Omaha, Nebraska Magnitude of the Problem Annual
HST.161 Molecular Biology and Genetics in Modern Medicine Fall 2007
 MIT OpenCourseWare http://ocw.mit.edu HST.161 Molecular Biology and Genetics in Modern Medicine Fall 2007 For information about citing these materials or our Terms of Use, visit: http://ocw.mit.edu/terms.
MIT OpenCourseWare http://ocw.mit.edu HST.161 Molecular Biology and Genetics in Modern Medicine Fall 2007 For information about citing these materials or our Terms of Use, visit: http://ocw.mit.edu/terms.
Resident Seminar Aug 19 th, 2015 Colon: Neoplastic. Scott Rieder Dr. Colquhoun
 Resident Seminar Aug 19 th, 2015 Colon: Neoplastic Scott Rieder Dr. Colquhoun Objectives Medical Expert: 1. The biologic basis of colon neoplasia 2. Colon cancer screening (guidelines and evidence) 3.
Resident Seminar Aug 19 th, 2015 Colon: Neoplastic Scott Rieder Dr. Colquhoun Objectives Medical Expert: 1. The biologic basis of colon neoplasia 2. Colon cancer screening (guidelines and evidence) 3.
Copyright, 1995, by the Massachusetts Medical Society
 Copyright, 1995, by the Massachusetts Medical Society Volume 333 SEPTEMBER 7, 1995 Number 10 Mon Aug 21 0 12:41:54 ASPIRIN AND THE RISK OF COLORECTAL CANCER IN WOMEN EDWARD GIOVANNUCCI, M.D., KATHLEEN
Copyright, 1995, by the Massachusetts Medical Society Volume 333 SEPTEMBER 7, 1995 Number 10 Mon Aug 21 0 12:41:54 ASPIRIN AND THE RISK OF COLORECTAL CANCER IN WOMEN EDWARD GIOVANNUCCI, M.D., KATHLEEN
Classification of polyposis syndromes two major groups. Adenomatous polyposis syndromes. Hamartomatous polyposis syndromes
 Hereditary polyposis syndromes Classification of polyposis syndromes two major groups adenomatous and non-adenomatous polyposis syndromes Adenomatous polyposis syndromes Familial adenomatous polyposis(fap)
Hereditary polyposis syndromes Classification of polyposis syndromes two major groups adenomatous and non-adenomatous polyposis syndromes Adenomatous polyposis syndromes Familial adenomatous polyposis(fap)
A Patient s Guide to risk assessment. Hereditary Colorectal Cancer
 A Patient s Guide to risk assessment Hereditary Colorectal Cancer Hereditary Cancer Testing: Is it Right for You? Overview of Syndromes This workbook is designed to help you decide if hereditary cancer
A Patient s Guide to risk assessment Hereditary Colorectal Cancer Hereditary Cancer Testing: Is it Right for You? Overview of Syndromes This workbook is designed to help you decide if hereditary cancer
Is aspirin ready for colorectal cancer chemoprevention and adjuvant therapy?
 Is aspirin ready for colorectal cancer chemoprevention and adjuvant therapy? Robert Benamouzig Service de Gastroentérologie Hôpital Avicenne Bobigny, France Aspirin and Colorectal carcinogenesis Aspirin
Is aspirin ready for colorectal cancer chemoprevention and adjuvant therapy? Robert Benamouzig Service de Gastroentérologie Hôpital Avicenne Bobigny, France Aspirin and Colorectal carcinogenesis Aspirin
Hereditary Non Polyposis Colorectal Cancer(HNPCC) From clinic to genetics
 From clinic to genetics Question 1) Clinical pattern of inheritance of the HNPCC-Syndrome? Question 1) Clinical pattern of inheritance of the HNPCC-Syndrome? Autosomal dominant Question 2) Incidence of
From clinic to genetics Question 1) Clinical pattern of inheritance of the HNPCC-Syndrome? Question 1) Clinical pattern of inheritance of the HNPCC-Syndrome? Autosomal dominant Question 2) Incidence of
What All of Us Should Know About Cancer and Genetics
 What All of Us Should Know About Cancer and Genetics Beth A. Pletcher, MD, FAAP, FACMG Associate Professor of Pediatrics UMDNJ- New Jersey Medical School Disclosures I have no relevant financial relationships
What All of Us Should Know About Cancer and Genetics Beth A. Pletcher, MD, FAAP, FACMG Associate Professor of Pediatrics UMDNJ- New Jersey Medical School Disclosures I have no relevant financial relationships
Review article: the prevention of colorectal cancer
 Aliment Pharmacol Ther 2001; 15: 323±336. Review article: the prevention of colorectal cancer I. DOVE-EDWIN & H. J. W. THOMAS ICRF Family Cancer Clinic, St Mark's Hospital, Harrow, Middlesex, UK Accepted
Aliment Pharmacol Ther 2001; 15: 323±336. Review article: the prevention of colorectal cancer I. DOVE-EDWIN & H. J. W. THOMAS ICRF Family Cancer Clinic, St Mark's Hospital, Harrow, Middlesex, UK Accepted
Cyclooxygenase inhibitors in the chemoprevention of colorectal cancer
 Journal of BUON 9: 139-145, 2004 2004 Zerbinis Medical Publications. Printed in Greece REVIEW ARTICLE Cyclooxygenase inhibitors in the chemoprevention of colorectal cancer N. Stanojević-Bakić Department
Journal of BUON 9: 139-145, 2004 2004 Zerbinis Medical Publications. Printed in Greece REVIEW ARTICLE Cyclooxygenase inhibitors in the chemoprevention of colorectal cancer N. Stanojević-Bakić Department
ACG Clinical Guideline: Genetic Testing and Management of Hereditary Gastrointestinal Cancer Syndromes
 ACG Clinical Guideline: Genetic Testing and Management of Hereditary Gastrointestinal Cancer Syndromes Sapna Syngal, MD, MPH, FACG, 1,2,3 Randall E. Brand, MD, FACG, 4 James M. Church, MD, FACG, 5,6,7
ACG Clinical Guideline: Genetic Testing and Management of Hereditary Gastrointestinal Cancer Syndromes Sapna Syngal, MD, MPH, FACG, 1,2,3 Randall E. Brand, MD, FACG, 4 James M. Church, MD, FACG, 5,6,7
C olorectal adenomas are reputed to be precancerous
 568 COLORECTAL CANCER Incidence and recurrence rates of colorectal adenomas estimated by annually repeated colonoscopies on asymptomatic Japanese Y Yamaji, T Mitsushima, H Ikuma, H Watabe, M Okamoto, T
568 COLORECTAL CANCER Incidence and recurrence rates of colorectal adenomas estimated by annually repeated colonoscopies on asymptomatic Japanese Y Yamaji, T Mitsushima, H Ikuma, H Watabe, M Okamoto, T
Hereditary Cancer Registries: Service, Education and Research
 Hereditary Cancer Registries: Service, Education and Research Marcia Cruz-Correa, MD, PhD, FASGE, AGAF Associate Professor of Medicine, Biochemistry & Surgery Director, Gastrointestinal Oncology Program
Hereditary Cancer Registries: Service, Education and Research Marcia Cruz-Correa, MD, PhD, FASGE, AGAF Associate Professor of Medicine, Biochemistry & Surgery Director, Gastrointestinal Oncology Program
The New England Journal of Medicine. Review Articles. Mechanisms
 Review Articles Primary Care CHEMOPREVENTION OF COLORECTAL CANCER PASI A. JÄNNE, M.D., PH.D., AND ROBERT J. MAYER, M.D. COLORECTAL cancer is the second leading cause of cancer-related deaths in the United
Review Articles Primary Care CHEMOPREVENTION OF COLORECTAL CANCER PASI A. JÄNNE, M.D., PH.D., AND ROBERT J. MAYER, M.D. COLORECTAL cancer is the second leading cause of cancer-related deaths in the United
Content. Diagnostic approach and clinical management of Lynch Syndrome: guidelines. Terminology. Identification of Lynch Syndrome
 of Lynch Syndrome: guidelines 17/03/2009 Content Terminology Lynch Syndrome Presumed Lynch Syndrome Familial Colorectal Cancer Identification of Lynch Syndrome Amsterdam II criteria Revised Bethesda Guidelines
of Lynch Syndrome: guidelines 17/03/2009 Content Terminology Lynch Syndrome Presumed Lynch Syndrome Familial Colorectal Cancer Identification of Lynch Syndrome Amsterdam II criteria Revised Bethesda Guidelines
David P. Ryan, M.D. Clinical Director, MGH Cancer Center Chief, Hematology-Oncology, MGH
 Colon Cancer 2015 David P. Ryan, M.D. Clinical Director, MGH Cancer Center Chief, Hematology-Oncology, MGH Colon Cancer Case presentation 72yo woman presented 1/03 abd discomfort and nausea Found to have
Colon Cancer 2015 David P. Ryan, M.D. Clinical Director, MGH Cancer Center Chief, Hematology-Oncology, MGH Colon Cancer Case presentation 72yo woman presented 1/03 abd discomfort and nausea Found to have
Serrated Polyps and a Classification of Colorectal Cancer
 Serrated Polyps and a Classification of Colorectal Cancer Ian Chandler June 2011 Structure Serrated polyps and cancer Molecular biology The Jass classification The familiar but oversimplified Vogelsteingram
Serrated Polyps and a Classification of Colorectal Cancer Ian Chandler June 2011 Structure Serrated polyps and cancer Molecular biology The Jass classification The familiar but oversimplified Vogelsteingram
Hyperplastische Polyps Innocent bystanders?
 Hyperplastische Polyps Innocent bystanders?? K. Geboes P th l i h O tl dk d Pathologische Ontleedkunde, KULeuven Content Historical Classification Relation Hyperplastic polyps carcinoma The concept cept
Hyperplastische Polyps Innocent bystanders?? K. Geboes P th l i h O tl dk d Pathologische Ontleedkunde, KULeuven Content Historical Classification Relation Hyperplastic polyps carcinoma The concept cept
Cyclooxygenase-2 overexpression correlates with tumour recurrence, especially haematogenous metastasis, of colorectal cancer
 doi: 10.1054/ bjoc.2000.1270, available online at http://www.idealibrary.com on Cyclooxygenase-2 overexpression correlates with tumour recurrence, especially haematogenous metastasis, of colorectal cancer
doi: 10.1054/ bjoc.2000.1270, available online at http://www.idealibrary.com on Cyclooxygenase-2 overexpression correlates with tumour recurrence, especially haematogenous metastasis, of colorectal cancer
Colon Cancer and Hereditary Cancer Syndromes
 Colon Cancer and Hereditary Cancer Syndromes Gisela Keller Institute of Pathology Technische Universität München gisela.keller@lrz.tum.de Colon Cancer and Hereditary Cancer Syndromes epidemiology models
Colon Cancer and Hereditary Cancer Syndromes Gisela Keller Institute of Pathology Technische Universität München gisela.keller@lrz.tum.de Colon Cancer and Hereditary Cancer Syndromes epidemiology models
Neoplasia 18 lecture 6. Dr Heyam Awad MD, FRCPath
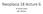 Neoplasia 18 lecture 6 Dr Heyam Awad MD, FRCPath ILOS 1. understand the role of TGF beta, contact inhibition and APC in tumorigenesis. 2. implement the above knowledge in understanding histopathology reports.
Neoplasia 18 lecture 6 Dr Heyam Awad MD, FRCPath ILOS 1. understand the role of TGF beta, contact inhibition and APC in tumorigenesis. 2. implement the above knowledge in understanding histopathology reports.
Bowel obstruction and tumors
 Bowel obstruction and tumors Intestinal Obstruction Obstruction of the GI tract may occur at any level, but the small intestine is most often involved because of its relatively narrow lumen. Causes: Hernias
Bowel obstruction and tumors Intestinal Obstruction Obstruction of the GI tract may occur at any level, but the small intestine is most often involved because of its relatively narrow lumen. Causes: Hernias
2018 National Academy of Medicine Annual Meeting
 2018 National Academy of Medicine Annual Meeting October 15, 2018 Targeting Cancer with Precision Prevention Ernest Hawk, M.D., M.P.H. What is Precision Prevention? The concept of precision medicine prevention
2018 National Academy of Medicine Annual Meeting October 15, 2018 Targeting Cancer with Precision Prevention Ernest Hawk, M.D., M.P.H. What is Precision Prevention? The concept of precision medicine prevention
Asingle inherited mutant gene may be enough to
 396 Cancer Inheritance STEVEN A. FRANK Asingle inherited mutant gene may be enough to cause a very high cancer risk. Single-mutation cases have provided much insight into the genetic basis of carcinogenesis,
396 Cancer Inheritance STEVEN A. FRANK Asingle inherited mutant gene may be enough to cause a very high cancer risk. Single-mutation cases have provided much insight into the genetic basis of carcinogenesis,
COX-2 inhibitors: A cautionary tale
 COX-2 inhibitors: A cautionary tale October 1, 2007 Molecular interventions in human disease... An approach as old as human civilization. With whom the herbs have come together Like kingly chiefs unto
COX-2 inhibitors: A cautionary tale October 1, 2007 Molecular interventions in human disease... An approach as old as human civilization. With whom the herbs have come together Like kingly chiefs unto
By: Tania Cortas, MD Arizona Oncology 03/10/2015
 By: Tania Cortas, MD Arizona Oncology 03/10/2015 Epidemiology In the United States, CRC incidence rates have declined about 2 to 3 percent per year over the last 15 years Death rates from CRC have declined
By: Tania Cortas, MD Arizona Oncology 03/10/2015 Epidemiology In the United States, CRC incidence rates have declined about 2 to 3 percent per year over the last 15 years Death rates from CRC have declined
Analysis of Human DNA in Stool Samples as a Technique for Colorectal Cancer Screening
 Analysis of Human DNA in Stool Samples as a Technique for Colorectal Cancer Screening Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
Analysis of Human DNA in Stool Samples as a Technique for Colorectal Cancer Screening Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY
 OPEN ACCESS TEXTBOOK OF GENERAL SURGERY COLORECTAL POLYPS P Goldberg POLYP A polyp is a localised elevated lesion arising from a epithelial surface. If it has a stalk it is called a pedunculated polyp
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY COLORECTAL POLYPS P Goldberg POLYP A polyp is a localised elevated lesion arising from a epithelial surface. If it has a stalk it is called a pedunculated polyp
Adenoma detection rate in 41,010 patients from Southwest China
 ONCOLOGY LETTERS 9: 2073-2077, 2015 Adenoma detection rate in 41,010 patients from Southwest China BIN CAI 1, ZHIXIAN LIU 1, YANSONG XU 2, WEIYUAN WEI 3 and SEN ZHANG 1 Departments of 1 Colorectal Surgery;
ONCOLOGY LETTERS 9: 2073-2077, 2015 Adenoma detection rate in 41,010 patients from Southwest China BIN CAI 1, ZHIXIAN LIU 1, YANSONG XU 2, WEIYUAN WEI 3 and SEN ZHANG 1 Departments of 1 Colorectal Surgery;
Chemoprevention of colon cancer: Current status and future prospects
 Cancer and Metastasis Reviews 21: 323 348, 2002. 2002 Kluwer Academic Publishers. Printed in the Netherlands. Chemoprevention of colon cancer: Current status and future prospects David M. Gustin 1 and
Cancer and Metastasis Reviews 21: 323 348, 2002. 2002 Kluwer Academic Publishers. Printed in the Netherlands. Chemoprevention of colon cancer: Current status and future prospects David M. Gustin 1 and
Surveillance of Individuals At High Risk For Developing Pancreatic Cancer
 Surveillance of Individuals At High Risk For Developing Pancreatic Cancer Marco Bruno Erasmus Medical Center, Rotterdam Pancreatic Cancer Facts & figures One of the most fatal malignancies Overall 5-year
Surveillance of Individuals At High Risk For Developing Pancreatic Cancer Marco Bruno Erasmus Medical Center, Rotterdam Pancreatic Cancer Facts & figures One of the most fatal malignancies Overall 5-year
Precision Chemoprevention with Aspirin
 Precision Chemoprevention with Aspirin Andrew T. Chan, MD, MPH Clinical and Translational Epidemiology Unit Division of Gastroenterology Massachusetts General Hospital February 3-5, 2016 Lansdowne Resort,
Precision Chemoprevention with Aspirin Andrew T. Chan, MD, MPH Clinical and Translational Epidemiology Unit Division of Gastroenterology Massachusetts General Hospital February 3-5, 2016 Lansdowne Resort,
Page 1. Is the Risk This High? Dysplasia in the IBD Patient. Dysplasia in the Non IBD Patient. Increased Risk of CRC in Ulcerative Colitis
 Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Review article: the incidence and prevalence of colorectal cancer in inflammatory bowel disease
 Aliment Pharmacol Ther 23; 18 (Suppl. 2): 1 5. Review article: the incidence and prevalence of colorectal cancer in inflammatory bowel disease P. MUNKHOLM Department of Medical Gastroenterology, Hvidovre
Aliment Pharmacol Ther 23; 18 (Suppl. 2): 1 5. Review article: the incidence and prevalence of colorectal cancer in inflammatory bowel disease P. MUNKHOLM Department of Medical Gastroenterology, Hvidovre
University of Groningen. Heredity nonpolyposis colorectal cancer Rijcken, Fleur Elise Marie
 University of Groningen Heredity nonpolyposis colorectal cancer Rijcken, Fleur Elise Marie IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Heredity nonpolyposis colorectal cancer Rijcken, Fleur Elise Marie IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
Is ALS a multistep process?
 Is ALS a multistep process? Neil Pearce, London School of Hygiene and Tropical Medicine Ammar Al-Chalabi, Institute of Psychiatry, King s College London Zoe Rutter-Locher, King s College London Is ALS
Is ALS a multistep process? Neil Pearce, London School of Hygiene and Tropical Medicine Ammar Al-Chalabi, Institute of Psychiatry, King s College London Zoe Rutter-Locher, King s College London Is ALS
Correlation between COX-2 and APC Expression in Left Versus Right-sided Human Colon Cancer
 Correlation between COX-2 and APC Expression in Left Versus Right-sided Human Colon Cancer A. NASIR 1,2, A. LOPEZ 5, D. BOULWARE 3, M. MALAFA 5 and D. COPPOLA 1,2,4,5 Departments of 1 Anatomic Pathology,
Correlation between COX-2 and APC Expression in Left Versus Right-sided Human Colon Cancer A. NASIR 1,2, A. LOPEZ 5, D. BOULWARE 3, M. MALAFA 5 and D. COPPOLA 1,2,4,5 Departments of 1 Anatomic Pathology,
Management of higher risk of colorectal cancer. Huw Thomas
 Management of higher risk of colorectal cancer Huw Thomas Colorectal Cancer 41,000 new cases pa in UK 16,000 deaths pa 60% 5 year survival Adenoma-carcinoma sequence (Morson) Survival vs stage (Dukes)
Management of higher risk of colorectal cancer Huw Thomas Colorectal Cancer 41,000 new cases pa in UK 16,000 deaths pa 60% 5 year survival Adenoma-carcinoma sequence (Morson) Survival vs stage (Dukes)
Sessile Serrated Polyps
 Årsmøtet i Den norske Patologforening 2014 Sessile Serrated Polyps Tor J. Eide Oslo Universitetssykehus The term serrated include a group of lesions with a sawtoothlike appearance of the crypts and the
Årsmøtet i Den norske Patologforening 2014 Sessile Serrated Polyps Tor J. Eide Oslo Universitetssykehus The term serrated include a group of lesions with a sawtoothlike appearance of the crypts and the
Adenomatous Polyposis Syndromes (FAP/AFAP and MAP)
 A Patient s Guide to risk assessment Adenomatous Polyposis Syndromes (FAP/AFAP and MAP) Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary cancer
A Patient s Guide to risk assessment Adenomatous Polyposis Syndromes (FAP/AFAP and MAP) Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary cancer
MSH6 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table
 MSH6 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
MSH6 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
