thereby acutely disrupting the permeability barrier (2). Such
|
|
|
- Tyler Rich
- 5 years ago
- Views:
Transcription
1 Fatty Acids Are Required for Epidermal Permeability Barrier Function Man Mao-Qiang, Peter M. Elias, and Kenneth R. Feingold Departments ofdermatology and Medicine, University of California, San Francisco, California 94143; and Dermatology Service and Metabolism Section, Medical Service, Department of Veterans Affairs Medical Center, San Francisco, California Abstract The permeability barrier is mediated by a mixture of ceramides, sterols, and free fatty acids arranged as extracellular lamellar bilayers in the stratum corneum. Whereas prior studies have shown that cholesterol and ceramides are required for normal barrier function, definitive evidence for the importance of nonessential fatty acids is not available. To determine whether epidermal fatty acid synthesis also is required for barrier homeostasis, we applied 5-(tetradecyloxy)-2-furancarboxylic acid (TOFA), an inhibitor of acetyl CoA carboxylase, after disruption of the barrier by acetone or tape stripping. TOFA inhibits epidermal fatty acid by 50% and significantly - delays barrier recovery. Moreover, coadministration of palmitate with TOFA normalizes barrier recovery, indicating that the delay is due to a deficiency in bulk fatty acids. Furthermore, TOFA treatment also delays the return of lipids to the stratum corneum and results in abnormalities in the structure of lamellar bodies, the organelle which delivers lipid to the stratum corneum. In addition, the organization of secreted lamellar body material into lamellar bilayers within the stratum corneum interstices is disrupted by TOFA treatment. Finally, these abnormalities in lamellar body and stratum corneum membrane structure are corrected by coapplication of palmitate with TOFA. These results demonstrate a requirement for bulk fatty acids in barrier homeostasis. Thus, inhibiting the epidermal synthesis of any of the three key lipids that form the extracellular, lipid-enriched membranes of the stratum corneum results in an impairment in barrier homeostasis. (J. Clin. Invest : ) Key words: transepidermal water loss. fatty acid synthesis. 5-(tetradecyloxy)-2-furancarboxylic acid * stratum corneum lipids * permeability barrier Introduction The cutaneous permeability barrier is essential for terrestrial life. This permeability barrier is located in the stratum corneum and is mediated by lipid-enriched membrane multilayers with a characteristic lamellar repeat structure within the intercellular spaces ( 1 ). The lipids in the intercellular domains consist primarily ofceramides, cholesterol, and free fatty acids ( 1 ). Topical application of organic solvents, such as acetone, or tape stripping remove these lipids from the stratum corneum, Address correspondence to Kenneth R. Feingold, M. D., Metabolism Section ( 11IF), Department ofveterans Affairs Medical Center, 4150 Clement Street, San Francisco, CA Receivedfor publication 4 August 1992 and in revisedform 28 January The Journal of Clinical Investigation, Inc. Volume 92, August 1993, thereby acutely disrupting the permeability barrier (2). Such acute perturbations initiate a sequence of events that rapidly results in the return of lipids to the stratum corneum and the restoration of barrier function (2). These events include: (a) the rapid secretion ofpreformed lamellar bodies by the stratum granulosum cells (3); (b) an increase in cholesterol, sphingolipid, and fatty acid synthesis in the epidermis (2, 4-6); and (c) the increased formation and accelerated secretion ofnewly synthesized lamellar bodies by the stratum granulosum cells (3). The increase in both cholesterol and fatty acid synthesis in the epidermis occurs within an hour or two after disruption of the barrier, whereas the increase in sphingolipid synthesis is delayed (6 h or later) (2, 4-6). To assess the role of specific lipids in the barrier further, we have used inhibitors oflipid synthesis. Blocking the synthesis of cholesterol with competitive inhibitors of HMG CoA reductase, such as lovastatin or fluvastatin, delays barrier recovery after acetone treatment, which is associated with a decrease in the return of cholesterol to the stratum corneum (7, 8). Moreover, either mevalonate, the immediate product ofthe enzyme, or cholesterol, the final product of the biosynthetic pathway overcomes the inhibition and restores barrier recovery to normal indicating that the delay in barrier recovery is due to the inhibition of HMG CoA reductase (7). Likewise, inhibition of sphingolipid synthesis, with,b-choloroalanine, an inhibitor of serine palmitoyl transferase, delays barrier repair (9). The decrease in barrier repair in the,b-chloroalanine-treated animals is associated with a decrease in the return of sphingolipids to the stratum corneum (9). Barrier repair rates are normalized by providing exogenous sphingolipids demonstrating that the effect of 3-chloroalanine on barrier repair is due to sphingolipid synthesis inhibition rather than a nonspecific toxic effect (9). Although these studies indicate that cholesterol and sphingolipids are required for barrier homeostasis, little is known regarding the requirement for nonessential fatty acids, the third remaining major class of lipids in the stratum corneum lipid mixture. Whereas the essential fatty acid, linoleate, is required for barrier function, it largely occupies the w-esterified position on acyl ceramides ( 10, 1 1). Yet, as noted above, previous studies demonstrated that disruption of the barrier stimulates bulk epidermal fatty acid synthesis (2, 5). The purpose of the present study was to determine if inhibiting epidermal fatty acid synthesis after acute perturbations of barrier function would delay barrier repair, demonstrating a requirement not only for essential fatty acids, but also bulk free fatty acids in barrier homeostasis. Methods Materials. Male hairless mice (hr/hr), 8-12 wk old, were purchased from Simonsen Laboratories (Gilroy, CA) and fed mouse diet (Ralston-PurinaCo., St. Louis, MO) and water ad lib. Acetone and propyl- Fatty Acids Are Requiredfor Epidermal Permeability Barrier Function 791
2 ene glycol were purchased from Fisher Scientific (Fairlane, NJ). Palmitic acid methyl ester was purchased from Sigma Chemical Co. (St. Louis, MO). Ruthenium tetroxide was purchased from Polysciences Inc. (Warrington, PA). Tritiated water (5 Ci/ml) and [ '4C]acetate (60 mci/mmol) were purchased from New England Nuclear (Boston, MA). Thin layer chromatography polygram Sil G plates were purchased from Brinkmann Instruments (Westbury, NY). Cytosint scintillation liquid was purchased from ICN Pharmaceuticals, Inc. (Irvine, CA). Fluvastatin (XU62-320, fluindostatin) was a gift from Dr. A. Stutz, Sandoz Research Institute, Vienna, Austria. 5-tetradecyloxy-2- furancarboxylic acid (TOFA)' (MDL 14514) was a gift from Dr. E. Bohme, Marion Merrill Dow Research Institute, Marion Merrill Dow Inc., Cincinnati, OH. Epicholesterol was purchased from Research Plus Steroid Laboratories (Denville, NJ). Animal procedures. Male hairless mice were treated with absolute acetone to disrupt the barrier while under anesthesia as previously described (3-6). Alternatively, barrier disruption was achieved by repeated application of cellophane tape (four to six times). Both procedures were terminated when transepidermal water loss (TEWL) rates reached 2-6 mg/cm2 per h, as measured with an electrolytic water analyzer (Meeco Inc., Warrington, PA). Immediately after acetone treatment or tape stripping the entire flank of cohorts of animals were treated with: (a) vehicle consisting of propylene glycol:ethanol 70:30 vol/vol; (b) fluvastatin, 400 Mg in vehicle; (c) TOFA, 130,g in vehicle; (d) palmitic acid, 200 ug in vehicle; (e) cholesterol, 400 jig in vehicle; (f) epicholesterol, 400 Mg in vehicle; or (g) combinations ofthe above. TEWL was measured at 2, 4, and 6 h after disrupting the barrier and drug application. Because the extent of barrier disruption varied from animal to animal, barrier recovery is expressed as percent of maximal TEWL (value immediately after disrupting barrier) rather than in absolute values. Lipid synthesis. The effect of TOFA and fluvastatin on fatty acid and cholesterol synthesis in vitro and in vivo was assessed in mice after disrupting the barrier with either acetone treatment or tape stripping. In the in vivo studies, tritiated water (20 mci/0.2 ml) was administered 1 h after barrier disruption. 2 h later, blood samples were taken and the animals killed. Whole skin was excised and the epidermis separated from the dermis by heat separation, as described previously (4, 5). The incorporation oftritiated water into cholesterol and fatty acids was determined after saponification, extraction with petroleum ether, and thin layer chromatography as described in detail in previous publications (4, 5). The specific activity of tritiated water in serum samples was used to calculate the incorporation rates. Results are presented as nanomoles product formed per 2 hours per milligram ofepidermal wet weight. In the in vitro studies, the animals were killed 1 h after barrier disruption and skin samples were incubated for 2 h at 37 C in a 2-ml solution of 10 mm EDTA in Dulbecco's PBS, calcium and magnesium free, containing 40 MCi [ '4C]acetate, as described previously ( 12, 13). After stopping the reaction by immersion in iced PBS, the epidermis was separated from the dermis and the quantity of labeled fatty acids and cholesterol determined in the epidermis after saponification, extraction, and thin layer chromatography, as described previously (4, 5, 13). Results are expressed as nanomoles incorporated per hour per gram epidermis. Because of variations in the rates of lipid synthesis from month to month, only the results from animals that were studied simultaneously under identical conditions are compared. Histochemistry. Skin biopsies were taken from mice at the indicated times after barrier disruption with acetone plus various topical treatments. Samples were snap frozen in liquid nitrogen, sectioned at 4,Mm, and stained with Nile red for the depiction of lipid distribution in skin ( 14). Sections were visualized in a microscope equipped for epifluorescence (Ortholux II; E. Leitz, Inc., Rockleigh, NJ). 1. Abbreviations used in this paper: TEWL, transepidermal water loss; TOFA, 5-(tetradecyloxy)-2-furancarboxylic acid. Electron microscopy. Samples were taken from control and treated areas 2 h after various treatments, minced to 0.5 cm2, fixed in modified Karnovsky's fixative overnight, washed in 0.1 M cacodylate buffer and postfixed in 0.2% ruthenium tetroxide (RuO4) containing 0.5 potassium ferrocyanide in 0.1 M cacodylate buffer for 30 min as recently described ( 15 ) nm ultrathin sections were examined in an electron microscope ( loa; Carl Zeiss Inc., Thornwood, NY) operating at 60 KV. Statistical significance was determined using the Student's t test. A two-tailed t test was used when the direction of change was unknown. When the direction of change was known from previous experiments a one-tailed t test was used. Results Effects of TOFA and fluvastatin on lipid synthesis. To determine whether topical TOFA treatment inhibits epidermal fatty acid synthesis, we measured ['4C ] acetate incorporation into epidermal lipids in vitro (Table I). As reported previously (2, 4, 5), disruption of the barrier by acetone treatment stimulates both fatty acid and cholesterol synthesis in the epidermis (Table I, line 1 vs. line 2). Similarly, disruption of the barrier by tape stripping also increases epidermal fatty acid and cholesterol synthesis (Table I, line 4 vs. line 5). With TOFA treatment, after acetone disruption of the barrier, the incorporation of [14C]acetate into fatty acids is decreased 44%, while ['4C]- Table I. Lipid Synthesis In Vitro Experiment 1 1) Untreated + vehicle (n = 6) 2) Acetone + vehicle (n = 6) 3) Acetone + TOFA (n = 6) 1 vs. 2 2 vs. 3 Experiment 2 4) Untreated + vehicle (n = 3) 5) Tape stripping + vehicle (n = 3) 6) Tape stripping + TOFA (n = 3) 4 vs. 5 5 vs. 6 Experiment 3 7) Acetone + vehicle (n = 3) 8) Acetone + fluvastatin (n = 3) 7 vs. 8 Experiment 4 9) Tape stripping + vehicle (n = 3) 10) Tape stripping + fluvastatin (n = 3) 9vs. 10 Fatty acids Cholesterol nmol incorporated/h per g epidermis 19.1± ± ±1.58 P < ± ± ±0.52 P < 0.01 P < ± ± ± ± ± ± ± ± ± ±1.17 P< ± ± ± ±0.14 The cutaneous permeability barrier was disrupted by either acetone treatment or tape stripping followed by the indicated treatment. 1 h after barrier disruption, the animals were killed and skin samples incubated in ['4C]acetate for 2 h at 370C. The epidermis was separated from the dermis and the incorporation of acetate into fatty acids and cholesterol in the epidermis determined after saponification, extraction, and thin layer chromatography. n = number of animals. 792 M. Mao-Qiang, P. M. Elias, and K R. Feingold
3 acetate incorporation into cholesterol is not significantly altered (Table I, line 2 vs. line 3). Moreover, after acutely disrupting the barrier by an alternative physical method, cellophane tape stripping, topical TOFA treatment also inhibits fatty acid synthesis (70% decrease) while not significantly altering the incorporation of [ '4C] acetate into cholesterol (Table I, line 5 vs. line 6). Thus, TOFA treatment abolishes the increase in epidermal fatty acid synthesis induced by disrupting the barrier by either acetone treatment or tape stripping. After barrier disruption by either acetone treatment or tape stripping, fluvastatin inhibits cholesterol synthesis without significantly altering fatty acid synthesis (Table I, line 7 vs. line 8, line 9 vs. line 10). This result is similar to that previously observed after topical lovastatin administration (7). Previous studies have demonstrated that after acetone disruption ofthe barrier, the in vivo incorporation of3h20 into cholesterol and fatty acids is increased approximately two- to threefold in the epidermis (4, 5). Similarly, disruption of the barrier by tape stripping also stimulates the incorporation of 3H20 into cholesterol and fatty acids in the epidermis (cholesterol: control 0.107±0.041 vs. tape stripped 1.24±0.381 P < 0.01; fatty acids: control 8.00±1.27 vs. tape stripped 12.24±2.12 nmol incorporated/2 h per mg epidermis P <.05, n = 9 for each group). To further confirm that topical TOFA inhibits fatty acid synthesis in the epidermis after barrier disruption, we also determined the effect of this compound on 3H20 incorporation Table II. Lipid Synthesis In Vivo Fatty acids Cholesterol nmol incorporated/2 h per mg epidermis Acetone treatment Experiment 1 1) Vehicle (n = 3) 10.32± ±0.22 2) TOFA (n = 3) 4.74± ±0.09 Experiment 2 3) Vehicle (n = 6) 11.2± ± ) Fluvastatin (n = 6) 10.9± ±0.058 Tape stripping Experiment 1 5) Vehicle (n =3) 19.03± ±0.21 6) TOFA (n = 3) 8.33± ±0.03 P<0.001 Experiment 2 7) Vehicle (n = 3) 19.2± ± ) Fluvastatin (n = 3) 15.8± ±0.012 The cutaneous permeability barrier was disrupted by either acetone treatment or tape stripping followed by the indicated treatment. 1 h after barrier disruption, the animals were injected with 20 mci 3H20. 2 h later, the animals were killed, the skin excised, and the epidermis separated from the dermis by heat separation. The incorporation of 3H20 in cholesterol and fatty acids was determined after saponification, extraction, and thin layer chromatography. n = number of animals. into lipids in vivo (Table II). With TOFA treatment, after acetone disruption of the barrier, the incorporation of tritiated water into fatty acids in the epidermis of intact mice is decreased 55% in comparison to animals treated with vehicle (line 1 vs. line 2). Epidermal cholesterol synthesis also appears to be decreased in the TOFA-treated animals compared to controls, but this difference does not achieve statistical significance. After disruption of the barrier by tape stripping, TOFA also significantly inhibits the incorporation of tritiated water into fatty acids in the epidermis (56% decrease) while not significantly affecting cholesterol synthesis (Table II, line 5 vs. line 6). Furthermore, topical fluvastatin inhibits cholesterol synthesis in the epidermis without altering fatty acid synthesis after disruption of the barrier by acetone treatment or tape stripping (Table II, line 3 vs. line 4, line 7 vs. line 8). Finally, topical TOFA treatment of animals with normal barrier function does not alter tritiated water incorporation into fatty acids in the epidermis (Vehicle (n = 3):12.9±3.5 vs. TOFA (n = 3): 15.6±1.9 nmol 3H20 incorporated/ 2 h per mg epidermis; ). Thus, in animals with a perturbed barrier, TOFA causes a marked inhibition of epidermal fatty acid synthesis, but exhibits only modest effects on cholesterol synthesis. In contrast, TOFA has no effect on epidermal lipid synthesis in animals with normal barrier function. Effects of TOFA on permeability barrier recovery. Having shown that TOFA treatment inhibits fatty acid synthesis after barrier perturbation, we next determined whether such inhibition would lead to alterations in barrier recovery. After barrier disruption with acetone treatment, transepidermal water loss rapidly recovers towards normal, such that by 6 h TEWL levels normalize by 40-50% (Table III). This rapid recovery of barrier function is similar to results previously reported by this laboratory (7-9, 14). In contrast, a single application oftopical TOFA significantly impairs barrier recovery at 2, 4, and 6 h (Table III). To determine whether the effect of TOFA is due to inhibition of fatty acid synthesis or instead attributable to toxicity or unrelated effects of the drug, we next applied palmitic acid simultaneously with TOFA. As seen in Table III, barrier recov- Table III. Effect of TOFA on Barrier Recovery 2h 4h 6h percent maximal TEWL Acetone Vehicle (n = 30) 80.5± ± ±3.0 TOFA (n = 22) ±3.6* 85.2±3.5* 74.6±5.5* TOFA + palmitic acid (n = 23) 80.4±3.5* ±4.5' TOFA + cholesterol (n = 15) 93.8± ± ±3.6* Tape stripped Vehicle (n = 14) 116± ± ±4.4 TOFA (n = 13) 245±21 * 155±13.4* 97.0±6.5* TOFA + palmitic acid (n = 24) 159±8.2** 99.9±6.9*t 78.4±5.0*1 * P < vs. vehicle. t P < vs. TOFA. vs. vehicle. 11 vs. TOFA. 1 P < 0.01 vs. vehicle. Fatty Acids Are Requiredfor Epidermal Permeability Barrier Function 793
4 ery improves when palmitic acid is coapplied with TOFA to acetone-treated animals. In contrast, simultaneous applications of cholesterol with TOFA does not significantly improve barrier recovery. These results indicate first that the defect in barrier recovery induced by TOFA is not due to unrelated drug effects or toxicity, and second, that the delay is primarily due to inhibition of fatty acid synthesis, since TOFA effects can be overcome by providing exogenous fatty acids alone. To determine whether the inhibition in barrier recovery produced by TOFA treatment is related to barrier recovery in general or other responses to acetone treatment, we next determined the effect of topical TOFA treatment in an unrelated acute model ofbarrier disruption, cellophane tape stripping. As shown in Table III, TOFA treatment delays barrier recovery after tape stripping when compared with animals treated with vehicle alone. Moreover, coadministration of palmitic acid with TOFA also partially restores barrier recovery in this model, as in the acetone-treated animals. These results provide further evidence for the requirement for local epidermal fatty acid synthesis in barrier homeostasis. In animals with a normal barrier, TOFA treatment, even when applied for several days, does not affect barrier function. As described above, TOFA does not affect lipid synthesis in animals with a normal barrier, and therefore it is not surprising that this drug does not alter barrier function when applied to normal epidermis. Prior studies and the experiments shown in Table IV (line 1 vs. line 3) demonstrate that inhibition of cholesterol synthesis causes a delay in the early stages of barrier recovery (7, 8). We next assessed the effects ofsimultaneous inhibition offatty acid and cholesterol synthesis. As shown in Table IV, coapplications of TOFA and the HMG CoA reductase inhibitor, fluvastatin, result in an even more striking impairment in barrier Table IV. Effect ofinibiting Cholesterol and Fatty Acid Synthesis on Barrier Recovery 2h 4h 6h percent maximal TEWL 1) Vehicle (n = 30) 80.5± ± ±3.0 2) TOFA (n = 22) 101.4± ± ±5.5 3) Fluvastatin (n = 13) 122.2± ± ±3.8 4) T+F(n= 23) 130± ± ±6.1 5) T + F + PA + cholesterol (n = 12) 62.6± ± ±3.3 6) T+F+PA + epicholesterol (n = 12) 137± ± ±8.0 1 vs. 2 P < P < P < I vs. 3 P< P< 0.01 P< I vs. 4 P < P < P < vs.4 P<0.001 P<0.001 P< vs.4 P<0.001 P< vs. 5 P<0.001 P<0.001 P< vs.6 P<0.01 P<0.05 5vs.6 P<0.001 P<0.001 P<0.001 recovery than is achieved with either inhibitor alone (line 4 vs. lines 2 or 3). Moreover, exogenous fatty acids and cholesterol applied with the two inhibitors result in normalization of barrier recovery (line 4 vs. line 5). In contrast, simultaneous applications of TOFA plus palmitate and fluvastatin plus epicholesterol (3-a-cholesterol), an inert free sterol that does not substitute for cholesterol in forming lamellar membranes ( 16), results in barrier recovery rates comparable to fluvastatin alone (line 3 vs. line 6). Together, these results demonstrate that the inhibition of barrier recovery induced by TOFA and fluvastatin can be attributed to the inhibition offatty acid and cholesterol synthesis, and again is not simply due to nonspecific toxicity. Moreover, the observation that epicholesterol cannot substitute for cholesterol shows that the corrective effects of coapplied lipids is not due to bulk hydrophobic properties of the lipid, but instead to specific requirements for each lipid species. Lipid histochemistry of TOFA-treated animals. We next determined whether TOFA treatment delays the reaccumulation of stainable neutral lipids in the stratum corneum (Fig. 1, A-D). As seen in Fig. 1 A, before acetone treatment the stratum corneum displays intense green-gold fluorescence. Immediately after acetone treatment this band is lost, and the stratum corneum is barely visible (Fig. 1 B). Pilosebaceous structures in the dermis, however, continue to stain intensely, serving as a positive control (shown in Fig. 1 D; see below). By 4 h after acetone treatment plus vehicle applications, greengold fluorescence is beginning to return to the stratum corneum (Fig. 1 C). In contrast, TOFA treatment of acetone-perturbed skin resulted in a delay in the return ofstainable neutral lipid to the stratum corneum (Fig. 1 D); i.e., TOFA-treated samples appeared indistinguishable from samples obtained immediately after acetone treatment (Fig. 1 D; compare Fig. 1 B). These results demonstrate that the TOFA-induced inhibition of fatty acid synthesis results in a delay in the reappearance of stainable neutral lipid in the stratum corneum in parallel to the delay in barrier recovery. Ultrastructural observations of TOFA-treated epidermis. To gain further insights into the mechanism by which TOFA inhibits barrier repair, we next examined the ultrastructure of TOFA-treated epidermis (Fig. 2, A-E). 2 h after vehicle treatment ofacetone-disrupted skin, the appearance oflamellar bodies and their secreted contents at the stratum granulosum-stratum corneum interface appears comparable to normal (Fig. 2, D and E). Moreover, normal lamellar bilayers are already present within the intercellular spaces in the lower to mid-stratum corneum (Fig. 2, D, double arrows). In contrast, TOFA treatment drastically alters the internal lamellar structure and organization of epidermal lamellar bodies (Fig. 2 C). At the stratum granulosum-stratum corneum interface, the secreted contents of lamellar bodies appear disorganized and they only partially fill the intercellular spaces (Fig. 2 B). Furthermore, the intercellular domains of the outer layers of TOFA-treated stratum corneum reveal a complete absence of normal bilayer structures; instead, fragments and whorls of lamellae partially fill the intercellular spaces, leaving a vacuolated appearance (Fig. 2 A). However, when palmitate is coapplied with TOFA (Fig. 2 A, +P), the internal structure of lamellar bodies is normalized (Fig. 2 A, inserts below), and normal bilayers reappear within the stratum corneum interstices (Fig. 2A, insert above). T, TOFA; F, fluvastatin; PA, palmitic acid. These results show that inhibition of fatty acid synthesis by 794 M. Mao-Qiang, P. M. Elias, and K R. Feingold
5 I Figure 1. Frozen sections of hairless mice epidermis stained with the neutral lipid fluorophore, Nile red. (A) Control, untreated skin: note intense green-gold fluorescence of stratum corneum (SC) (arrows). (B) Immediately after acetone treatment: note absence of SC staining (brackets). (C) 4 h after acetone treatment: note partial return of green-gold fluorescense in SC (arrows). (D) 4 h after acetone treatment plus one TOFA application: note lack of stainable lipid in SC (brackets), comparable to appearance immediately after acetone treatment. Also note positive staining of pilosebaceous structures in dermis (asterisks). Dashed line indicates dermal-epidermal junction. Magnification, 200. TOFA leads to disruption ofthe lamellar body secretory system and the resultant intercellular bilayers in the stratum corneum. Discussion Previous studies have demonstrated that both cholesterol and sphingolipid synthesis in the epidermis are crucial for normal restoration of barrier function after acute disruption of the barrier (7-9). Inhibition of either epidermal cholesterol or sphingolipid synthesis results in the formation of abnormal lamellar bodies and a delay in the return ofthe respective lipid to the stratum corneum resulting in impaired barrier recovery (7-9). Most importantly, the inhibition ofbarrier repair can be overcome by topically providing the missing lipid, either cholesterol or sphingolipid, demonstrating that the inhibition of barrier recovery is not due to nonspecific toxicity, but rather the presence ofboth ofthese two lipid species is required for the formation of the water impermeable extracellular membranes of the stratum corneum (7-9). The present study demonstrates that after acute disruption of the barrier, epidermal fatty acid synthesis is also crucial for normal restoration ofbarrier function. Topical treatment with TOFA inhibits epidermal fatty acid synthesis by 50% in - both acetone-treated and tape-stripped animals; i.e., to rates less than or equal to levels in untreated epidermis. In contrast, topical TOFA treatment did not effect epidermal fatty acid synthesis in animals with an intact barrier. We suspect that the failure of TOFA treatment to inhibit epidermal fatty acid synthesis in animals with a normal barrier is due to the inability of TOFA to penetrate intact stratum corneum. Thus, disrupting the stratum corneum permeability barrier by either acetone treatment or tape stripping allows for the transcutaneous absorption oftofa resulting in inhibition of fatty acid synthesis. In addition to inhibiting epidermal fatty acid synthesis, topical TOFA treatment also causes a modest decrease in epidermal cholesterol synthesis, which did not achieve statistical significance in any of the experiments. This marked decrease in fatty acid synthesis with a modest decrease in cholesterol synthesis has also been noted in the liver after TOFA treatment (17-19). A single topical application of TOFA significantly impairs barrier recovery after disruption by acetone treatment or tape stripping. That this delay can be attributed to deficiency of newly synthesized fatty acids is shown by the override experiments. Providing exogenous fatty acids by the topical coapplication of palmitate, simultaneously with TOFA, improves barrier recovery. In contrast, topical treatment with cholesterol has no significant beneficial effect on barrier recovery. Moreover, in other studies, we have shown that the application of palmitic acid alone after barrier disruption impairs rather than enhances barrier recovery (20). These observations strongly suggest that the delay in barrier recovery caused by TOFA is Fatty Acids Are Requiredfor Epidermal Permeability Barrier Function 795
6 i7-mi. Figure 2. Ultrastructure of epidermis 2 h after TOFA (±palmitate) treatment. A-C show epidermis after TOFA treatment, while D and E show vehicle-treated controls. Note abnormal lamellar bodies with TOFA treatment (C, single arrows; compare normal lamellar bodies in E). Secreted lamellar body contents at the stratum granulosum (SG)-strateum corneum (SC) interface only partially fill the intercellular domains (B, double arrows), leaving extensive clefts. At higher levels within the SC, the intercellular lamellar bilayers do not form normally; instead lamellar form short arrays or whorls (A, double arrows) leaving extensive clefts (compare normal SG-SC interface (open arrows) and lamellar bilayers (double arrows) in D. Finally, coapplications of palmitate (+P) with TOFA normalize the appearance of lamellar bodies (A, +P, lower insets), as well as lamellar bilayer structure (A, +P, upper inset). A and insets, X 145,000; B, X 102,500; C, X155,000; D, x86,000; E, X 108, M. Mao-Qiang, P. M. Elias, and K. R. Feingold
7 specifically due to the inhibition of fatty acid synthesis and not due to nonspecific drug toxicity. This and prior studies have demonstrated that, as with inhibition of fatty acid synthesis, the inhibition of cholesterol synthesis also impairs the early phases of barrier recovery (7, 8). These studies further show that when TOFA and fluvastatin, an inhibitor of cholesterol synthesis, are coapplied there is a marked inhibition of barrier recovery. In fact, with the two inhibitors together there is no recovery ofbarrier function during the 6 h of study. Notably, providing palmitate and cholesterol simultaneously with the two inhibitors restores barrier recovery to normal. In contrast, providing palmitate and epicholesterol, an inert free sterol that can not substitute for cholesterol in forming membrane structures ( 16), results in barrier recovery rates comparable to fluvastatin treatment alone. These observations provide still further evidence that the delay in barrier recovery is specifically linked to inhibition of epidermal lipid synthesis. Fatty acids are substrates for the formation of sphingolipids, and as stated above, sphingolipids are important constituents of the stratum corneum permeability barrier. However, it is unlikely that the effect oftofa on barrier recovery observed here can be attributed to inhibition of sphingolipid formation because prior studies have suggested that preformed stores of sphingolipids appear to suffice for the early stages of barrier recovery (5, 9). Sphingolipid synthesis is only stimulated at later time points after barrier disruption (5), and a specific inhibitor of sphingolipid synthesis, f3-chloroalanine, produced a defect in barrier recovery only during the later phases of barrier repair ( h) (9). In contrast, inhibiting epidermal fatty acid synthesis with TOFA inhibits the early phases of barrier recovery. As reported in previous publications, topical acetone treatment extracts lipids from the stratum corneum resulting in the disappearance of stainable neutral lipids (Fig. 1, B vs. A) (7, 14). Within a few hours after acetone treatment, stainable neutral lipids begin to return to the stratum corneum (Fig. 1 C) ( 14), in parallel to the restoration of barrier function. In contrast, in TOFA-treated animals, there is a delay in the return of neutral lipids to the stratum corneum (Fig. 1, D vs. C). Thus, inhibiting fatty acid synthesis delays the return of lipids to the stratum corneum which may account for the impaired barrier recovery. The basis for this delay in the return of lipids to the stratum corneum in TOFA-treated animals was revealed by the ultrastructural studies. As discussed in detail in prior publications, the exocytosis of lamellar bodies is an important route by which lipids are delivered to the extracellular domains of the stratum corneum (reviewed in 3, 21-23). The lamellar body secretory system appears to be activated by barrier disruption because lamellar material appears in greater than normal quantities at the stratum granulosum-stratum corneum interface (3). In TOFA-treated animals, both the internal structure and organization of lamellar bodies are disrupted (Fig. 2 C). Furthermore, the quantities of secreted lamellar body material at the stratum granulosum-stratum corneum interface are diminished, and the organization of this material is also abnormal within the intercellular spaces at all levels of the stratum corneum (Fig. 2, A and B). However, when palmitate is coapplied with TOFA, the internal structure of lamellar bodies is normalized (Fig. 2 A, inset), and normal bilayers appear at all levels within the stratum corneum interstices by 4 h. These observations suggest that the TOFA-induced deficiency in nascent fatty acids leads to alterations in lamellar body content. These abnormalities in the lamellar body secretory system may account for the delay in both the return ofstainable lipids to the stratum corneum and the delayed restoration of barrier function with TOFA treatment. Remarkably, all ofthese changes in lamellar body internal structure and stratum corneum intercellular lamellar organization occur and are reversed within 4 h, once again emphasizing both the rapidity ofthe repair response and the fluidity of the intercellular domains. In recent studies, we have shown that substantial percutaneous transport, delivery to keratinocytes, and processing through the lamellar body secretory system occurs by 2 h after topical lipid application to acetone-treated murine skin (20). In summary, these results demonstrate first a requirement for bulk fatty acids for permeability barrier homeostasis, and second, the central role ofthe lamellar body secretory system in mediating changes in barrier function. Third and finally, these results demonstrate that diminution of any of the three key lipids that form the extracellular, lipid-enriched membranes of the stratum corneum results in a delay in the return of lipids to the stratum corneum and an impairment in the recovery of barrier function. Acknowledgments We thank P. Herranz for excellent secretarial assistance. This work was supported by grants from the Research Service ofthe Department of Veterans Affairs and the National Institutes of Health (AR and AR-39639). References 1. Elias, P. M Epidermal lipids, barrier function and desquamation. J. Invest. Dermatol. 80: Feingold, K. R The regulation and role ofepidermal lipid synthesis. Adv. Lipid Res. 24: Menon, G. K., K. R. Feingold, and P. M. Elias The lamellar body secretory response to barrier disruption. J. Invest. Dermatol. 98: Menon, G. K., K. R. Feingold, A. H. Moser, B. E. Brown, and P. M. Elias De novo sterologenesis in the skin. II. Regulation by cutaneous barrier requirements. J. Lipid Res. 26: Grubauer, G., K. R. Feingold, and P. M. Elias The relationship of epidermal lipogenesis to cutaneous barrier function. J. Lipid Res. 28: Holleran, W. M., K. R. Feingold, M. Mao-Qiang, W. N. Gao, J. M. Lee, and P. M. Elias Regulation ofepidermal sphingolipid synthesis by permeability barrier function. J. Lipid Res. 32: Feingold, K. R., M. Mao-Qiang, W. N. Gao, G. K. Menon, and P. M. Elias Cholesterol synthesis is required for cutaneous barrier function in mice. J. Clin. Invest. 86: Menon, G. K., K. R. Feingold, M. Mao-Qiang, M. Schaude, and P. M. Elias Structural basis for the barrier abnormality following inhibition of HMG CoA reductase in murine epidermis. J. Invest. Dermatol. 98: Holleran, W. M., M. Mao-Qiang, W. N. Gao, G. K. Menon, P. M. Elias, and K. R. Feingold Sphingolipids are required for mammalian barrier function: inhibition of sphingolipid synthesis delays barrier recovery after acute perturbation. J. Clin. Invest. 88: Prottey, C Essential fatty acids and the skin. Br. J. Dermatol. 94: Wertz, P. W., and D. T. Downing Glycolipids in mammalian epidermis: structure and function in the water barrier. Science (Wash. DC). 217: Monger, D. J., M. L. Williams, K. R. Feingold, B. E. Brown, and P. M. Elias Localization ofsites oflipid biosynthesis in mammalian epidermis. J. Lipid Res. 29: Fatty Acids Are Requiredfor Epidermal Permeability Barrier Function 797
8 13. Proksch, E., P. M. Elias, and K. R. Feingold Regulation of 3-hydroxy-3-methylglutaryl-coenzyme A reductase activity in murine epidermis: modulation of enzyme content and activation state by barrier requirements. J. Clin. Invest. 85: Grubauer, G., P. M. Elias, and K. R. Feingold Transepidermal water loss: the signal for recovery ofbarrier structure and function. J. Lipid Res. 30: Hou, S. Y. E., A. K. Mitra, S. H. White, G. K. Menon, R. Ghadially, and P. M. Elias Membrane structures in normal and essential fatty acid deficient stratum corneum: characterization by ruthenium tetroxide staining and x-ray diffraction. J. Invest. Dermatol. 96: Elias, P. M., D. S. Friend, and J. Goerke Membrane sterol heterogeneity: freeze fracture detection with saponins and filipin. J. Histochem. Cytochem. 27: Panek, E., G. A. Cook, and N. W. Cornell Inhibition by 5-(tetradexyloxy)-2-furoic acid of fatty acid and cholesterol synthesis in isolated rat hepatocytes. Lipids. 12: McCune, S. A., and R. A. Harris Mechanism responsible for 5-(tetradexyloxy)-2-furoic acid inhibition of hepatic lipogenesis. J. Bio. Chem. 254: Fukuda, N., and J. A. Ontko Interactions between fatty acid synthesis, oxidation, and esterification in the production oftriglyceride rich lipoproteins by the liver. J. Lipid Res. 25: Mao-Qiang, M., K. R. Feingold, and P. M. Elias Effects of exogenous lipids on permeability barrier recovery in acetone treated murine skin. Arch. Dermatol. In press. 21. Odland, G. P., and K. Holbrook The lamellar granules of epidermis. Curr. ProbL. Dermatol. 9: Landmann, L The epidermal permeability barrier. Anat. Embryol. 178: Elias, P. M., and G. K. Menon Structural and lipid biochemical correlates of the epidermal permeability barrier. Adv. Lipid Res. 24: M. Mao-Qiang, P. M. Elias, and K R. Feingold
Skin Barrier Function as a Self-Organizing System
 Review Forma, 15, 227 232, 2000 Skin Barrier Function as a Self-Organizing System Mitsuhiro DENDA Shiseido Research Center, 2-12-1 Fukuura, Kanazawa-ku, Yokohama, Kanagawa 236-8643, Japan E-mail: mitsuhiro.denda@to.shiseido.co.jp
Review Forma, 15, 227 232, 2000 Skin Barrier Function as a Self-Organizing System Mitsuhiro DENDA Shiseido Research Center, 2-12-1 Fukuura, Kanazawa-ku, Yokohama, Kanagawa 236-8643, Japan E-mail: mitsuhiro.denda@to.shiseido.co.jp
Topical Mevalonic Acid Stimulates De Novo Cholesterol Synthesis and Epidermal Permeability Barrier Homeostasis in Aged Mice 1
 Topical Mevalonic Acid Stimulates De Novo Cholesterol Synthesis and Epidermal Permeability Barrier Homeostasis in Aged Mice 1 Akinori Haratake, Kenji Ikenaga,* Norito Katoh,* Hideyo Uchiwa, Shinya Hirano,*
Topical Mevalonic Acid Stimulates De Novo Cholesterol Synthesis and Epidermal Permeability Barrier Homeostasis in Aged Mice 1 Akinori Haratake, Kenji Ikenaga,* Norito Katoh,* Hideyo Uchiwa, Shinya Hirano,*
Relationship of epidermal lipogenesis to cutaneous barrier function
 Relationship of epidermal lipogenesis to cutaneous barrier function Gerhard Grubauer, Kenneth R. Feingold, and Peter M. Elias Dermatology and Medical Services, Veterans Administration Medical Center, and
Relationship of epidermal lipogenesis to cutaneous barrier function Gerhard Grubauer, Kenneth R. Feingold, and Peter M. Elias Dermatology and Medical Services, Veterans Administration Medical Center, and
Extracellular processing of phospholipids is required for permeability barrier homeostasis
 Extracellular processing of phospholipids is required for permeability barrier homeostasis Man Mao-Qiang, Kenneth R. Feingold, Mahendra Jain, and Peter M. Elias Dermatology and Medical (Metabolism) Services,
Extracellular processing of phospholipids is required for permeability barrier homeostasis Man Mao-Qiang, Kenneth R. Feingold, Mahendra Jain, and Peter M. Elias Dermatology and Medical (Metabolism) Services,
Transepidermal water loss: the signal for recovery of barrier structure and function
 Transepidermal water loss: the signal for recovery of barrier structure and function Gerhard Grubauer, Peter M. Elias, and Kenneth R. Feingold Dermatology and Medical Services, Veterans Administration
Transepidermal water loss: the signal for recovery of barrier structure and function Gerhard Grubauer, Peter M. Elias, and Kenneth R. Feingold Dermatology and Medical Services, Veterans Administration
Regulation. De novo sterologenesis in the skin. 11. by cutaneous barrier requirements
 De novo sterologenesis in the skin. 11. by cutaneous barrier requirements Regulation Gopinathan K. Menon, Kenneth R. Feingold, Arthur H. Moser, Barbara E. Brown, and Peter M. Elias Dermatology and Medical
De novo sterologenesis in the skin. 11. by cutaneous barrier requirements Regulation Gopinathan K. Menon, Kenneth R. Feingold, Arthur H. Moser, Barbara E. Brown, and Peter M. Elias Dermatology and Medical
The epidermis displays a characteristic calcium (Ca )
 Formation of the Epidermal Calcium Gradient Coincides with Key Milestones of Barrier Ontogenesis in the Rodent Peter M. Elias, Patricia Nau, Karen Hanley, Chris Cullander,* Debra Crumrine, Graham Bench,
Formation of the Epidermal Calcium Gradient Coincides with Key Milestones of Barrier Ontogenesis in the Rodent Peter M. Elias, Patricia Nau, Karen Hanley, Chris Cullander,* Debra Crumrine, Graham Bench,
Imiquimod-Induced Interleukin-1a Stimulation Improves Barrier Homeostasis in Aged Murine Epidermis
 Imiquimod-Induced Interleukin-1a Stimulation Improves Barrier Homeostasis in Aged Murine Epidermis Chantel O. Barland, Elizabeth Zettersten, Barbara S. Brown, Jianqin Ye, Peter M. Elias, and Ruby Ghadially
Imiquimod-Induced Interleukin-1a Stimulation Improves Barrier Homeostasis in Aged Murine Epidermis Chantel O. Barland, Elizabeth Zettersten, Barbara S. Brown, Jianqin Ye, Peter M. Elias, and Ruby Ghadially
The Aged Epidermal Permeability Barrier Structural, Functional, and Lipid Biochemical Abnormalities in Humans and a Senescent Murine Model
 The Aged Epidermal Permeability Barrier Structural, Functional, and Lipid Biochemical Abnormalities in Humans and a Senescent Murine Model Ruby Ghadially,** Barbara E. Brown,* Sandy M. Sequeira-Martin,*
The Aged Epidermal Permeability Barrier Structural, Functional, and Lipid Biochemical Abnormalities in Humans and a Senescent Murine Model Ruby Ghadially,** Barbara E. Brown,* Sandy M. Sequeira-Martin,*
Lipid content and lipid type as determinants of the epidermal permeability barrier
 Lipid content and lipid type as determinants of the epidermal permeability barrier Gerhard Grubauer, Kenneth R. Feingold, Ronald M. Harris, and Peter M. Elias Dermatology and Medical Services, Veterans
Lipid content and lipid type as determinants of the epidermal permeability barrier Gerhard Grubauer, Kenneth R. Feingold, Ronald M. Harris, and Peter M. Elias Dermatology and Medical Services, Veterans
Induction of Selected Lipid Metabolic Enzymes and Differentiation-Linked Structural Proteins by Air Exposure in Fetal Rat Skin Explants
 Induction of Selected Lipid Metabolic Enzymes and Differentiation-Linked Structural Proteins by Air Exposure in Fetal Rat Skin Explants László G. Kömüves,* Karen Hanley,*, Yan Jiang,* Chika Katagiri,*
Induction of Selected Lipid Metabolic Enzymes and Differentiation-Linked Structural Proteins by Air Exposure in Fetal Rat Skin Explants László G. Kömüves,* Karen Hanley,*, Yan Jiang,* Chika Katagiri,*
The Role of Epidermal Lipids in Cutaneous Permeability Barrier Homeostasis
 The Role of Epidermal Lipids in Cutaneous Permeability Barrier Homeostasis Kenneth R. Feingold Metabolism Section, Medical Service, Department of Veterans Affairs Medical Center, University of California
The Role of Epidermal Lipids in Cutaneous Permeability Barrier Homeostasis Kenneth R. Feingold Metabolism Section, Medical Service, Department of Veterans Affairs Medical Center, University of California
The Changes of Epidermal Calcium Gradient and Transitional Cells after Prolonged Occlusion Following Tape Stripping in the Murine Epidermis
 The Changes of Epidermal Calcium Gradient and Transitional Cells after Prolonged Occlusion Following Tape Stripping in the Murine Epidermis Sung Ku Ahn, Sang Min Hwang, Shao Jun Jiang, Eung Ho Choi, and
The Changes of Epidermal Calcium Gradient and Transitional Cells after Prolonged Occlusion Following Tape Stripping in the Murine Epidermis Sung Ku Ahn, Sang Min Hwang, Shao Jun Jiang, Eung Ho Choi, and
Glucosylceramide synthase activity in murine epidermis: localization, regulation, and requirement for barrier homeostasis.
 Glucosylceramide synthase activity in murine epidermis: quantitation, localization, regulation, and requirement for barrier homeostasis Chujor S. N. Chujor, Kenneth R. Feingold, Peter M. Elias, and Walter
Glucosylceramide synthase activity in murine epidermis: quantitation, localization, regulation, and requirement for barrier homeostasis Chujor S. N. Chujor, Kenneth R. Feingold, Peter M. Elias, and Walter
Topical Preparations
 Topical Preparations One of the functions of the skin is to protect the internal body components against the external environment and thus to control the passage of chemicals into and out of the body.
Topical Preparations One of the functions of the skin is to protect the internal body components against the external environment and thus to control the passage of chemicals into and out of the body.
of the Epidermal Permeability Barrier in the Rat
 Glucocorticoids Accelerate Fetal Maturation of the Epidermal Permeability Barrier in the Rat Michelle Aszterbaum, * Kenneth R. Feingold, ** Gopinathan K. Menon, * and Mary L. Williams,*0 Departments of
Glucocorticoids Accelerate Fetal Maturation of the Epidermal Permeability Barrier in the Rat Michelle Aszterbaum, * Kenneth R. Feingold, ** Gopinathan K. Menon, * and Mary L. Williams,*0 Departments of
Investigations on the mechanism of hypercholesterolemia observed in copper deficiency in rats
 J. Biosci., Vol. 12, Number 2, June 1987, pp. 137 142. Printed in India. Investigations on the mechanism of hypercholesterolemia observed in copper deficiency in rats P. VALSALA and P. A. KURUP Department
J. Biosci., Vol. 12, Number 2, June 1987, pp. 137 142. Printed in India. Investigations on the mechanism of hypercholesterolemia observed in copper deficiency in rats P. VALSALA and P. A. KURUP Department
Permeability barrier requirements regulate epidermal P-glucocerebrosidase
 Permeability barrier requirements regulate epidermal P-glucocerebrosidase Walter M. Holleran, ** Yutaka Takagi, tt Gopinathan K. Menon,** Simon M. Jackson, Jane M. Lee:. Kenneth R. Feingold,*.t*** and
Permeability barrier requirements regulate epidermal P-glucocerebrosidase Walter M. Holleran, ** Yutaka Takagi, tt Gopinathan K. Menon,** Simon M. Jackson, Jane M. Lee:. Kenneth R. Feingold,*.t*** and
The lipid barrier of the Stratum Corneum
 The lipid barrier of the Stratum Corneum Stratum Corneum: the "Bricks and Mortar" model Ceramides (40-65% total lipids) HN O Glucoceramides HN O O HO O cerabrosidase Cholesteryl sulphate Free fatty acids
The lipid barrier of the Stratum Corneum Stratum Corneum: the "Bricks and Mortar" model Ceramides (40-65% total lipids) HN O Glucoceramides HN O O HO O cerabrosidase Cholesteryl sulphate Free fatty acids
8 Influence of permeation modulators on the behaviour of a SC lipid model mixture
 8 Influence of permeation modulators on the behaviour of a SC lipid model mixture 8.1 Introduction In the foregoing parts of this thesis, a model membrane system of SC lipids has been developed and characterized.
8 Influence of permeation modulators on the behaviour of a SC lipid model mixture 8.1 Introduction In the foregoing parts of this thesis, a model membrane system of SC lipids has been developed and characterized.
Association of Cyclic Adenosine Monophosphate with Permeability Barrier Homeostasis of Murine Skin
 Association of Cyclic Adenosine Monophosphate with Permeability Barrier Homeostasis of Murine Skin Mitsuhiro Denda, Shigeyoshi Fuziwara, and Kaori Inoue Shiseido Research Center, Yokohama, Japan see related
Association of Cyclic Adenosine Monophosphate with Permeability Barrier Homeostasis of Murine Skin Mitsuhiro Denda, Shigeyoshi Fuziwara, and Kaori Inoue Shiseido Research Center, Yokohama, Japan see related
A unique gel matrix moisturizer delivers better skin barrier through increase of long chain acyl ceramide species
 Poster 7487 A unique gel matrix moisturizer delivers better skin barrier through increase of long chain acyl ceramide species Apostolos Pappas 1, Allison Rush 1, Anna Nicolaou 2, Julie Bianchini 1, Luke
Poster 7487 A unique gel matrix moisturizer delivers better skin barrier through increase of long chain acyl ceramide species Apostolos Pappas 1, Allison Rush 1, Anna Nicolaou 2, Julie Bianchini 1, Luke
Application of Skin-Identical Ceramide 3 for Enhanced Skin Moisturization and Smoothness: Latest Results
 Application of Skin-Identical Ceramide 3 for Enhanced Skin Moisturization and Smoothness: Latest Results By Ute Wollenweber* and Dr. Mike Farwick* Keywords: Ceramides, Stratum corneum, skin moisturization,
Application of Skin-Identical Ceramide 3 for Enhanced Skin Moisturization and Smoothness: Latest Results By Ute Wollenweber* and Dr. Mike Farwick* Keywords: Ceramides, Stratum corneum, skin moisturization,
Comparative Anatomical Factors Affecting Topical Delivery
 Comparative Anatomical Factors Affecting Topical Delivery Nancy A. Monteiro-Riviere, Ph.D., Fellow ATS Professor of Investigative Dermatology and Toxicology Center for Chemical Toxicology Research and
Comparative Anatomical Factors Affecting Topical Delivery Nancy A. Monteiro-Riviere, Ph.D., Fellow ATS Professor of Investigative Dermatology and Toxicology Center for Chemical Toxicology Research and
Stimulation of fatty acid biosynthesis by dietary cholesterol and of cholesterol synthesis by dietary fatty acid
 Stimulation of fatty acid biosynthesis by dietary cholesterol and of cholesterol synthesis by dietary fatty acid Thomas V. Fungwe, James E. Fox, Lauren M. Cagen, Henry G. Wilcox, and Murray Heimberg' Departments
Stimulation of fatty acid biosynthesis by dietary cholesterol and of cholesterol synthesis by dietary fatty acid Thomas V. Fungwe, James E. Fox, Lauren M. Cagen, Henry G. Wilcox, and Murray Heimberg' Departments
This week s topic will be: Evidence for the Fluid Mosaic Model. Developing theories, testing hypotheses and techniques for visualizing cells
 Tutorials, while not mandatory, will allow you to improve your final grade in this course. Thank you for your attendance to date. These notes are not a substitute for the discussions that we will have
Tutorials, while not mandatory, will allow you to improve your final grade in this course. Thank you for your attendance to date. These notes are not a substitute for the discussions that we will have
Chapter 26 Biochemistry 5th edition. phospholipids. Sphingolipids. Cholesterol. db=books&itool=toolbar
 http://www.ncbi.nlm.nih.gov/sites/entrez? db=books&itool=toolbar 1 The surface of a soap bubble is a bilayer formed by detergent molecules 2 Chapter 26 Biochemistry 5th edition phospholipids Sphingolipids
http://www.ncbi.nlm.nih.gov/sites/entrez? db=books&itool=toolbar 1 The surface of a soap bubble is a bilayer formed by detergent molecules 2 Chapter 26 Biochemistry 5th edition phospholipids Sphingolipids
Glycerol replacement corrects defective skin hydration, elasticity, and barrier function in aquaporin-3-deficient mice
 Glycerol replacement corrects defective skin hydration, elasticity, and barrier function in aquaporin-3-deficient mice Mariko Hara* and A. S. Verkman* *Departments of Medicine and Physiology, Cardiovascular
Glycerol replacement corrects defective skin hydration, elasticity, and barrier function in aquaporin-3-deficient mice Mariko Hara* and A. S. Verkman* *Departments of Medicine and Physiology, Cardiovascular
Oxidation of Long Chain Fatty Acids
 Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Cutaneous Barrier Perturbation Stimulates Cytokine
 Cutaneous Barrier Perturbation Stimulates Cytokine Production in the Epidermis of Mice Ladonna C. Wood, Simon M. Jackson, Peter M. Elias, Carl Grunfeld, and Kenneth R. Feingold Dermatology and Medical
Cutaneous Barrier Perturbation Stimulates Cytokine Production in the Epidermis of Mice Ladonna C. Wood, Simon M. Jackson, Peter M. Elias, Carl Grunfeld, and Kenneth R. Feingold Dermatology and Medical
Expression and Regulation of 1-Acyl-sn-glycerol-3-phosphate. Acyltransferases in the Epidermis
 Expression and Regulation of 1-Acyl-sn-glycerol-3-phosphate Acyltransferases in the Epidermis Biao Lu, Yan J. Jiang, Mao Q. Man, Barbara Brown, Peter M. Elias, and Kenneth R. Feingold* Dermatology and
Expression and Regulation of 1-Acyl-sn-glycerol-3-phosphate Acyltransferases in the Epidermis Biao Lu, Yan J. Jiang, Mao Q. Man, Barbara Brown, Peter M. Elias, and Kenneth R. Feingold* Dermatology and
1.4 Page 1 Cell Membranes S. Preston 1
 AS Unit 1: Basic Biochemistry and Cell Organisation Name: Date: Topic 1.3 Cell Membranes and Transport Page 1 1.3 Cell Membranes and Transport from your syllabus l. Cell Membrane Structure 1. Read and
AS Unit 1: Basic Biochemistry and Cell Organisation Name: Date: Topic 1.3 Cell Membranes and Transport Page 1 1.3 Cell Membranes and Transport from your syllabus l. Cell Membrane Structure 1. Read and
Biological role of lipids
 Lipids Lipids Organic compounds present in living organisms, insoluble in water but able to be extracted by organic solvents such as: chloroform, acetone, benzene. Extraction = the action of taking out
Lipids Lipids Organic compounds present in living organisms, insoluble in water but able to be extracted by organic solvents such as: chloroform, acetone, benzene. Extraction = the action of taking out
THE SITE OF STEROL AND SQUALENE SYNTHESIS IN THE HUMAN SKIN123
 THE SITE OF STEROL AND SQUALENE SYNTHESIS IN THE HUMAN SKIN123 N. NICOLAIDES, PH.D. AND STEPHEN ROTHMAN, M.D. In earlier work (1) it was demonstrated that human scalp skin is an efficient organ for synthesizing
THE SITE OF STEROL AND SQUALENE SYNTHESIS IN THE HUMAN SKIN123 N. NICOLAIDES, PH.D. AND STEPHEN ROTHMAN, M.D. In earlier work (1) it was demonstrated that human scalp skin is an efficient organ for synthesizing
Update on emollients
 Update on emollients Amal Mhanna, MD Pediatric Dermatologist Clemenceau Medical Center Disclosure: I was a member of an advisory board y for J&J and received honoraria. Emollients and moisturizers are
Update on emollients Amal Mhanna, MD Pediatric Dermatologist Clemenceau Medical Center Disclosure: I was a member of an advisory board y for J&J and received honoraria. Emollients and moisturizers are
Roles of Lipids. principal form of stored energy major constituents of cell membranes vitamins messengers intra and extracellular
 Roles of Lipids principal form of stored energy major constituents of cell membranes vitamins messengers intra and extracellular = Oxidation of fatty acids Central energy-yielding pathway in animals. O
Roles of Lipids principal form of stored energy major constituents of cell membranes vitamins messengers intra and extracellular = Oxidation of fatty acids Central energy-yielding pathway in animals. O
Evaluation of the Percutaneous Absorption of Tramadol, In Lipoderm, Into Inner Ear Feline Skin, In Vitro, Using the Franz Skin Finite Dose Model
 Evaluation of the Percutaneous Absorption of Tramadol, In Lipoderm, Into Inner Ear Feline Skin, In Vitro, Using the Franz Skin Finite Dose Model Lipoderm Performs Well in Feline Inner Ear Test Study Summary
Evaluation of the Percutaneous Absorption of Tramadol, In Lipoderm, Into Inner Ear Feline Skin, In Vitro, Using the Franz Skin Finite Dose Model Lipoderm Performs Well in Feline Inner Ear Test Study Summary
VARIABILITY IN THE CHEMICAL COMPOSITION OF HUMAN SKIN SURFACE LIPIDS* DONALD T. DOWNING, Ph.D., JOHN S. STRAUSS, M.D. AND PETER E. POCHI, M.D.
 THE JOURNAL OF INYESTIOATJVE DERMATOLOGY Copyright 16 by The Williams & Wilkins Co. Vol. 53, No. 6 Printed in U.S.A. VARIABILITY IN THE CHEMICAL COMPOSITION OF HUMAN SKIN SURFACE LIPIDS* DONALD T. DOWNING,
THE JOURNAL OF INYESTIOATJVE DERMATOLOGY Copyright 16 by The Williams & Wilkins Co. Vol. 53, No. 6 Printed in U.S.A. VARIABILITY IN THE CHEMICAL COMPOSITION OF HUMAN SKIN SURFACE LIPIDS* DONALD T. DOWNING,
Absolute rates of cholesterol synthesis in extrahepatic tissues measured with 3H-labeled water and 14C-labeled substrates
 Absolute rates of cholesterol synthesis in extrahepatic tissues measured with 3H-labeled water and 14C-labeled substrates John M. Andersen and John M. Dietschy' Departments of Pediatrics and Internal Medicine,
Absolute rates of cholesterol synthesis in extrahepatic tissues measured with 3H-labeled water and 14C-labeled substrates John M. Andersen and John M. Dietschy' Departments of Pediatrics and Internal Medicine,
DESCRIPTION. Dosage: % Recommended ph:
 EVOIL JJB SENSATION DESCRIPTION Consists of a multifunctional emollient obtained from natural vegetable oils. High content (ca. 25 %) of long chain length fatty acid. Contains up to 75 % of unsaturated
EVOIL JJB SENSATION DESCRIPTION Consists of a multifunctional emollient obtained from natural vegetable oils. High content (ca. 25 %) of long chain length fatty acid. Contains up to 75 % of unsaturated
Commentary. New mechanisms by which statins lower plasma cholesterol. Henri Brunengraber
 Commentary New mechanisms by which statins lower plasma cholesterol Henri Brunengraber Department of Nutrition Case Western Reserve University Cleveland, OH 44109 Phone: 216 368 6429 Fax: 216 368 6560
Commentary New mechanisms by which statins lower plasma cholesterol Henri Brunengraber Department of Nutrition Case Western Reserve University Cleveland, OH 44109 Phone: 216 368 6429 Fax: 216 368 6560
Effects of Skin Surface Temperature on Epidermal Permeability Barrier Homeostasis
 ORIGINAL ARTICLE Effects of Skin Surface Temperature on Epidermal Permeability Barrier Homeostasis Mitsuhiro Denda 1, Takaaki Sokabe 2, Tomoko Fukumi-Tominaga 2 and Makoto Tominaga 2 Members of the transient
ORIGINAL ARTICLE Effects of Skin Surface Temperature on Epidermal Permeability Barrier Homeostasis Mitsuhiro Denda 1, Takaaki Sokabe 2, Tomoko Fukumi-Tominaga 2 and Makoto Tominaga 2 Members of the transient
DAILY CARE FOR DRY, IRRITATED AND REACTIVE SKIN. Physiogel A.I. Help your patients restore skin balance and well-being
 DAILY CARE FOR DRY, IRRITATED AND REACTIVE SKIN Help your patients restore skin balance and well-being Dry, irritated and reactive skin a question of balance Changes in the lipid barrier (1) Neurological
DAILY CARE FOR DRY, IRRITATED AND REACTIVE SKIN Help your patients restore skin balance and well-being Dry, irritated and reactive skin a question of balance Changes in the lipid barrier (1) Neurological
Stratum Corneum Acidification Is Impaired in Moderately Aged Human and Murine Skin
 ORIGINAL ARTICLE Stratum Corneum Acidification Is Impaired in Moderately Aged Human and Murine Skin Eung-Ho Choi 1,2, Mao-Qiang Man 1,PuXu 1, Shujun Xin 3, Zhili Liu 3, Debra A. Crumrine 1, Yan J. Jiang
ORIGINAL ARTICLE Stratum Corneum Acidification Is Impaired in Moderately Aged Human and Murine Skin Eung-Ho Choi 1,2, Mao-Qiang Man 1,PuXu 1, Shujun Xin 3, Zhili Liu 3, Debra A. Crumrine 1, Yan J. Jiang
In Vivo Histological Evaluation of a Novel YSGG Ablative Fractional Device for Cutaneous Remodeling
 In Vivo Histological Evaluation of a Novel YSGG Ablative Fractional Device for Cutaneous Remodeling Walfre Franco, PhD a1, Brian D. Zelickson, MD b, Victor E. Ross, MD c a Cutera Inc., Brisbane, CA b Abbott
In Vivo Histological Evaluation of a Novel YSGG Ablative Fractional Device for Cutaneous Remodeling Walfre Franco, PhD a1, Brian D. Zelickson, MD b, Victor E. Ross, MD c a Cutera Inc., Brisbane, CA b Abbott
Patterned acquisition of skin barrier function during development
 Development 125, 1541-1552 (1998) Printed in Great Britain The Company of Biologists Limited 1998 DEV1249 1541 Patterned acquisition of skin barrier function during development Matthew J. Hardman*, Paraskevi
Development 125, 1541-1552 (1998) Printed in Great Britain The Company of Biologists Limited 1998 DEV1249 1541 Patterned acquisition of skin barrier function during development Matthew J. Hardman*, Paraskevi
(From Arnold Biological Laboratory, Brown University, ProVence) P~s 3 To 5. Materials and Methods
 Published Online: 25 January, 1955 Supp Info: http://doi.org/10.1083/jcb.1.1.13 Downloaded from jcb.rupress.org on June 21, 2018 HISTOLOGY AND CYTOCHEMISTRY OF HUMAN SKIN IX. THE Dm~mUT~ON Ot NoN-SP~.c~Ic
Published Online: 25 January, 1955 Supp Info: http://doi.org/10.1083/jcb.1.1.13 Downloaded from jcb.rupress.org on June 21, 2018 HISTOLOGY AND CYTOCHEMISTRY OF HUMAN SKIN IX. THE Dm~mUT~ON Ot NoN-SP~.c~Ic
PRODUCT DATA SHEET. Updated: 07/2012 Approved: Dr. Victoria Donat
 PRODUCT DATA SHEET is a Refined Vegetable Oil composition enriched with other ingredients and specifically developed to enhance anti stretch activity. The composition helps to prevent and eliminate stretch
PRODUCT DATA SHEET is a Refined Vegetable Oil composition enriched with other ingredients and specifically developed to enhance anti stretch activity. The composition helps to prevent and eliminate stretch
Roles for tumor necrosis factor receptor p55 and sphingomyelinase in repairing the cutaneous permeability barrier
 Roles for tumor necrosis factor receptor p55 and sphingomyelinase in repairing the cutaneous permeability barrier Jens-Michael Jensen, 1 Stefan Schütze, 2 Michael Förl, 1 Martin Krönke, 2 and Ehrhardt
Roles for tumor necrosis factor receptor p55 and sphingomyelinase in repairing the cutaneous permeability barrier Jens-Michael Jensen, 1 Stefan Schütze, 2 Michael Förl, 1 Martin Krönke, 2 and Ehrhardt
ab SREBP-2 Translocation Assay Kit (Cell-Based)
 ab133114 SREBP-2 Translocation Assay Kit (Cell-Based) Instructions for Use For analysis of translocation of SREBP-2 into nuclei. This product is for research use only and is not intended for diagnostic
ab133114 SREBP-2 Translocation Assay Kit (Cell-Based) Instructions for Use For analysis of translocation of SREBP-2 into nuclei. This product is for research use only and is not intended for diagnostic
Needle free Mesotherapy
 Needle free Mesotherapy Transdermal Electroporation Skin One of the main functions of the skin is toactasabarrier protecting our body from the environment The skin is a natural barrier preventing the passage
Needle free Mesotherapy Transdermal Electroporation Skin One of the main functions of the skin is toactasabarrier protecting our body from the environment The skin is a natural barrier preventing the passage
Biomolecules: lipids
 Biomolecules: lipids Organic biomolecules: lipids Organic amphiphilic compounds insoluble in water Easily extracted from animal and vegetal cells using apolar solvents Fundamental to build cell's shape
Biomolecules: lipids Organic biomolecules: lipids Organic amphiphilic compounds insoluble in water Easily extracted from animal and vegetal cells using apolar solvents Fundamental to build cell's shape
An Aquaporin-inspired Lipid Concentrate for Mature Skin
 An Aquaporin-inspired Lipid Concentrate for Mature Skin Mike Farwick, Betty Santonnat and Peter Lersch EVONIK Goldschmidt GmbH, Essen, Germany Kees Korevaar EVONIK Cosmoferm B.V., Delft, Netherlands Anthony
An Aquaporin-inspired Lipid Concentrate for Mature Skin Mike Farwick, Betty Santonnat and Peter Lersch EVONIK Goldschmidt GmbH, Essen, Germany Kees Korevaar EVONIK Cosmoferm B.V., Delft, Netherlands Anthony
Lipids and barrier function of the skin
 Acta Derm Venereol 2000; Supp 208: 7±11 Lipids and barrier function of the skin PHILIP W. WERTZ Dows Institute, University of Iowa, Iowa City, USA The purpose of the present manuscript is to review the
Acta Derm Venereol 2000; Supp 208: 7±11 Lipids and barrier function of the skin PHILIP W. WERTZ Dows Institute, University of Iowa, Iowa City, USA The purpose of the present manuscript is to review the
Membrane Lipids & Cholesterol Metabolism
 Membrane Lipids & Cholesterol Metabolism Learning Objectives 1. How Are Acylglycerols and Compound Lipids Produced? 2. The synthesis of Sphingolipids from Ceramide 3. Diseases due to Disruption of Lipid
Membrane Lipids & Cholesterol Metabolism Learning Objectives 1. How Are Acylglycerols and Compound Lipids Produced? 2. The synthesis of Sphingolipids from Ceramide 3. Diseases due to Disruption of Lipid
Cells & Tissues. Chapter 3
 Cells & Tissues Chapter 3 Cell Theory Cell is structural and functional unit of life Activity of an organism is dependent upon its cells Principle of Complementarity functions of cells are dependent upon
Cells & Tissues Chapter 3 Cell Theory Cell is structural and functional unit of life Activity of an organism is dependent upon its cells Principle of Complementarity functions of cells are dependent upon
Dermal Technology Laboratory Ltd
 Dermal Technology Laboratory Ltd EFSA Guidance on Dermal Absorption (2017) : Industry View j Prof. Jon Heylings Chairman, DTL Ltd Professor of Toxicology Keele University, UK History DTL is an independent
Dermal Technology Laboratory Ltd EFSA Guidance on Dermal Absorption (2017) : Industry View j Prof. Jon Heylings Chairman, DTL Ltd Professor of Toxicology Keele University, UK History DTL is an independent
Active Beauty Rubixyl Anti stress-ageing peptide. Crafted by synthesis
 Active Beauty Rubixyl Anti stress-ageing peptide Crafted by synthesis Focus on the product The skin barrier function The most crucial part of the skin barrier functions is the stratum corneum. The stratum
Active Beauty Rubixyl Anti stress-ageing peptide Crafted by synthesis Focus on the product The skin barrier function The most crucial part of the skin barrier functions is the stratum corneum. The stratum
Nanostructure of the Epidermal Extracellular Space as Observed by Cryo-Electron Microscopy of Vitreous Sections of Human Skin
 Nanostructure of the Epidermal Extracellular Space as Observed by Cryo-Electron Microscopy of Vitreous Sections of Human Skin Ashraf Al-Amoudi, Jacques Dubochet,w and Lars Norlénwz Laboratory of Ultrastructural
Nanostructure of the Epidermal Extracellular Space as Observed by Cryo-Electron Microscopy of Vitreous Sections of Human Skin Ashraf Al-Amoudi, Jacques Dubochet,w and Lars Norlénwz Laboratory of Ultrastructural
ichthyosis represents the only form in which the enzymatic
 Rapid Publications Elevated n-alkanes in Congenital lchthyosiform Erythroderma Phenotypic Differentiation of Two Types of Autosomal Recessive Ichthyosis Mary L. Williams and Peter M. Elias Dermatology
Rapid Publications Elevated n-alkanes in Congenital lchthyosiform Erythroderma Phenotypic Differentiation of Two Types of Autosomal Recessive Ichthyosis Mary L. Williams and Peter M. Elias Dermatology
The Cell Membrane. Usman Sumo Friend Tambunan Arli Aditya Parikesit. Bioinformatics Group Faculty of Mathematics and Science University of Indonesia
 The Cell Membrane Usman Sumo Friend Tambunan Arli Aditya Parikesit Bioinformatics Group Faculty of Mathematics and Science University of Indonesia Overview Cell membrane separates living cell from nonliving
The Cell Membrane Usman Sumo Friend Tambunan Arli Aditya Parikesit Bioinformatics Group Faculty of Mathematics and Science University of Indonesia Overview Cell membrane separates living cell from nonliving
CHY2026: General Biochemistry. Lipid Metabolism
 CHY2026: General Biochemistry Lipid Metabolism Lipid Digestion Lipid Metabolism Fats (triglycerides) are high metabolic energy molecules Fats yield 9.3 kcal of energy (carbohydrates and proteins 4.1 kcal)
CHY2026: General Biochemistry Lipid Metabolism Lipid Digestion Lipid Metabolism Fats (triglycerides) are high metabolic energy molecules Fats yield 9.3 kcal of energy (carbohydrates and proteins 4.1 kcal)
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/20911 holds various files of this Leiden University dissertation. Author: Janssens, Michelle Title: Atopic eczema : the role of stratum corneum lipids in
Cover Page The handle http://hdl.handle.net/1887/20911 holds various files of this Leiden University dissertation. Author: Janssens, Michelle Title: Atopic eczema : the role of stratum corneum lipids in
Boundary Lipid bilayer Selectively Permeable Fluid mosaic of lipids and proteins Contains embedded proteins
 1 Boundary Lipid bilayer Selectively Permeable Fluid mosaic of lipids and proteins Contains embedded proteins 2 Phosphate head hydrophilic Fatty acid tails hydrophobic Amphipathic Phosphate attracted to
1 Boundary Lipid bilayer Selectively Permeable Fluid mosaic of lipids and proteins Contains embedded proteins 2 Phosphate head hydrophilic Fatty acid tails hydrophobic Amphipathic Phosphate attracted to
Diffusion, Osmosis and Active Transport
 Diffusion, Osmosis and Active Transport Particles like atoms, molecules and ions are always moving Movement increases with temperature (affects phases of matter - solid, liquid, gas) Solids - atoms, molecules
Diffusion, Osmosis and Active Transport Particles like atoms, molecules and ions are always moving Movement increases with temperature (affects phases of matter - solid, liquid, gas) Solids - atoms, molecules
Localization of De Novo Sterologenesis in Mammalian Skin
 0022-202X/ 8/81 04-065$02.00/ 0 THE JOURNAL OF INV ESTIGATIVE DERMATOLOGY, 8 1:65-69, 198 Copyright 198 by The Will iams & Wilkins Co. Localization of De Novo Sterologenesis in Mammalian Skin val. 81,
0022-202X/ 8/81 04-065$02.00/ 0 THE JOURNAL OF INV ESTIGATIVE DERMATOLOGY, 8 1:65-69, 198 Copyright 198 by The Will iams & Wilkins Co. Localization of De Novo Sterologenesis in Mammalian Skin val. 81,
IN a previous publication (Hewitt, 1954) a description was given of the
 i 9 9 Further Observations on the Histochemistry of Fat Absorption in the Small Intestine of the Rat By W. HEWITT, M.B., B.S. (From the Department of Anatomy, St. Thomas' Hospital Medical School, London,
i 9 9 Further Observations on the Histochemistry of Fat Absorption in the Small Intestine of the Rat By W. HEWITT, M.B., B.S. (From the Department of Anatomy, St. Thomas' Hospital Medical School, London,
cholesterol structure Cholesterol FAQs Cholesterol promotes the liquid-ordered phase of membranes Friday, October 15, 2010
 cholesterol structure most plasma cholesterol is in the esterified form (not found in cells or membranes) cholesterol functions in all membranes (drives formation of lipid microdomains) cholesterol is
cholesterol structure most plasma cholesterol is in the esterified form (not found in cells or membranes) cholesterol functions in all membranes (drives formation of lipid microdomains) cholesterol is
Role of ceramide 1 in the molecular organization of the stratum corneum lipids
 Role of ceramide 1 in the molecular organization of the stratum corneum lipids J. A. Bouwstra, 1, * G. S. Gooris,* F. E. R. Dubbelaar,* A. M. Weerheim, A. P. IJzerman* and M. Ponec Leiden/Amsterdam Center
Role of ceramide 1 in the molecular organization of the stratum corneum lipids J. A. Bouwstra, 1, * G. S. Gooris,* F. E. R. Dubbelaar,* A. M. Weerheim, A. P. IJzerman* and M. Ponec Leiden/Amsterdam Center
Classification, functions and structure
 Classification, functions and structure Elena Rivneac PhD, Associate Professor Department of Biochemistry and Clinical Biochemistry State University of Medicine and Pharmacy "Nicolae Testemitanu" Lipids
Classification, functions and structure Elena Rivneac PhD, Associate Professor Department of Biochemistry and Clinical Biochemistry State University of Medicine and Pharmacy "Nicolae Testemitanu" Lipids
Classification of Lipids
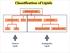 Classification of Lipids Neutral Lipids Amphipathic Lipids Amphipathic Lipids Most cell-membrane lipids are one of two main classes of amphipathic hydrolyzable lipids. Glycerophospholipids (phosphoglycerides):
Classification of Lipids Neutral Lipids Amphipathic Lipids Amphipathic Lipids Most cell-membrane lipids are one of two main classes of amphipathic hydrolyzable lipids. Glycerophospholipids (phosphoglycerides):
Stratum corneum lipids: the effect of ageing and the seasons
 Arch Dermatol Res (1996) 288 : 765 770 Springer-Verlag 1996 ORIGINAL PAPER J. Rogers C. Harding A. Mayo J. Banks A. Rawlings Stratum corneum lipids: the effect of ageing and the seasons Received: 17 October
Arch Dermatol Res (1996) 288 : 765 770 Springer-Verlag 1996 ORIGINAL PAPER J. Rogers C. Harding A. Mayo J. Banks A. Rawlings Stratum corneum lipids: the effect of ageing and the seasons Received: 17 October
The Function of Emollients in Skin Care
 The Function of Emollients in Skin Care Benjamin Schwartz Ontario SCC Education Day September 18, 2018 Lipid knowledge for the personal care industry Emollient - definition Wikipedia: complex mixtures
The Function of Emollients in Skin Care Benjamin Schwartz Ontario SCC Education Day September 18, 2018 Lipid knowledge for the personal care industry Emollient - definition Wikipedia: complex mixtures
The outer frontier: the importance of lipid metabolism in the skin
 The outer frontier: the importance of lipid metabolism in the skin Kenneth R. Feingold 1 Metabolism Section, Department of Veterans Affairs Medical Center, University of California, San Francisco, CA 94121
The outer frontier: the importance of lipid metabolism in the skin Kenneth R. Feingold 1 Metabolism Section, Department of Veterans Affairs Medical Center, University of California, San Francisco, CA 94121
LIPID METABOLISM. Sri Widia A Jusman Department of Biochemistry & Molecular Biology FMUI
 LIPID METABOLISM Sri Widia A Jusman Department of Biochemistry & Molecular Biology FMUI Lipid metabolism is concerned mainly with fatty acids cholesterol Source of fatty acids from dietary fat de novo
LIPID METABOLISM Sri Widia A Jusman Department of Biochemistry & Molecular Biology FMUI Lipid metabolism is concerned mainly with fatty acids cholesterol Source of fatty acids from dietary fat de novo
Cell Membranes. Dr. Diala Abu-Hassan School of Medicine Cell and Molecular Biology
 Cell Membranes Dr. Diala Abu-Hassan School of Medicine Dr.abuhassand@gmail.com Cell and Molecular Biology Organelles 2Dr. Diala Abu-Hassan Membrane proteins Major components of cells Nucleic acids DNA
Cell Membranes Dr. Diala Abu-Hassan School of Medicine Dr.abuhassand@gmail.com Cell and Molecular Biology Organelles 2Dr. Diala Abu-Hassan Membrane proteins Major components of cells Nucleic acids DNA
Lipids and Membranes
 Lipids and Membranes Presented by Dr. Mohammad Saadeh The requirements for the Pharmaceutical Biochemistry I Philadelphia University Faculty of pharmacy Biological membranes are composed of lipid bilayers
Lipids and Membranes Presented by Dr. Mohammad Saadeh The requirements for the Pharmaceutical Biochemistry I Philadelphia University Faculty of pharmacy Biological membranes are composed of lipid bilayers
Cholesterol Synthesis in BYP.3ssed Segments of the Small Intestine in Hyperphagic Rats
 GASTROENTEROLOGY 1 9 8 9 ; 9 6 : 3 0 7-1 ~ Cholesterol Synthesis in BYP.3ssed Segments of the Small Intestine in Hyperphagic Rats KENNETH R. FEINGOLD, QI-HUA ZENG, MOUNZER SOUED, and ARTHUR H. MOSER Department
GASTROENTEROLOGY 1 9 8 9 ; 9 6 : 3 0 7-1 ~ Cholesterol Synthesis in BYP.3ssed Segments of the Small Intestine in Hyperphagic Rats KENNETH R. FEINGOLD, QI-HUA ZENG, MOUNZER SOUED, and ARTHUR H. MOSER Department
WHAT IS ActiLipid? WHAT IS IT FOR? HOW IS IT DIFFERENT? WHAT DOES IT DO?
 CTFA/INCI Name: Triticum Vulgare (Wheat) Germ Extract Olea Europaea (Olive) Fruit Extract Coleus Forskohlii Root Extract Polygonum Cuspidatum (Japanese Bamboo) Extract Helianthus Annuus (Sunflower) Seed
CTFA/INCI Name: Triticum Vulgare (Wheat) Germ Extract Olea Europaea (Olive) Fruit Extract Coleus Forskohlii Root Extract Polygonum Cuspidatum (Japanese Bamboo) Extract Helianthus Annuus (Sunflower) Seed
Lipo-amino acid cholesteryl derivatives promote recovery
 j. Soc. Cosmet. Chem., 47, 351-362 (November/December 1996) Lipo-amino acid cholesteryl derivatives promote recovery effect for damaged skin HIROJI ISHII, NAOKO MIKAMI, and KAZUTAMI SAKAMOTO, Ajinomoto
j. Soc. Cosmet. Chem., 47, 351-362 (November/December 1996) Lipo-amino acid cholesteryl derivatives promote recovery effect for damaged skin HIROJI ISHII, NAOKO MIKAMI, and KAZUTAMI SAKAMOTO, Ajinomoto
SKIN LIPIDS OF A NORMAL AND A MUTANT (ASEBIC) MOUSE STRAIN*
 TRE JOURNAL OF IN'VESTIGATIVE DERMATOLOGY Copyright 1986 by The Williams & Wilkins Co. Vol. 47, No. 5 Printed in U.S.A. SKIN LIPIDS OF A NORMAL AND A MUTANT (ASEBIC) MOUSE STRAIN* DAVID I. WILKINSON, PHD.
TRE JOURNAL OF IN'VESTIGATIVE DERMATOLOGY Copyright 1986 by The Williams & Wilkins Co. Vol. 47, No. 5 Printed in U.S.A. SKIN LIPIDS OF A NORMAL AND A MUTANT (ASEBIC) MOUSE STRAIN* DAVID I. WILKINSON, PHD.
Science that studies adverse skin effects and the substances that produce them
 Science that studies adverse skin effects and the substances that produce them Leena A. Nylander-French, Ph.D., CIH 159 Rosenau Tel: 966.3826 E-mail: leena_french@unc.edu Occupational skin diseases are
Science that studies adverse skin effects and the substances that produce them Leena A. Nylander-French, Ph.D., CIH 159 Rosenau Tel: 966.3826 E-mail: leena_french@unc.edu Occupational skin diseases are
Atopic dermatitis and the skin barrier
 Atopic dermatitis and the skin barrier Dani Hoolahan BVSc BVMS DACVD Veterinary Dermatology Clinic: Sydney, Canberra, Newcastle, Tasmania, Kiama, Coffs Harbour Newcastle Animal Referral and Emergency Centre
Atopic dermatitis and the skin barrier Dani Hoolahan BVSc BVMS DACVD Veterinary Dermatology Clinic: Sydney, Canberra, Newcastle, Tasmania, Kiama, Coffs Harbour Newcastle Animal Referral and Emergency Centre
Membrane Structure and Function
 Membrane Structure and Function Chapter 7 Objectives Define the following terms: amphipathic molecules, aquaporins, diffusion Distinguish between the following pairs or sets of terms: peripheral and integral
Membrane Structure and Function Chapter 7 Objectives Define the following terms: amphipathic molecules, aquaporins, diffusion Distinguish between the following pairs or sets of terms: peripheral and integral
You must answer FOUR of the SIX questions. Use a SEPARATE answer book for EACH question.
 UNIVERSITY OF EAST ANGLIA School of Pharmacy Main Series UG Examination 2016-17 DRUG DESIGN AND MECHANISMS OF DRUG ACTION PHA-5001Y Time allowed: 2 hours You must answer FOUR of the SIX questions. Use
UNIVERSITY OF EAST ANGLIA School of Pharmacy Main Series UG Examination 2016-17 DRUG DESIGN AND MECHANISMS OF DRUG ACTION PHA-5001Y Time allowed: 2 hours You must answer FOUR of the SIX questions. Use
ANSC/NUTR 618 Lipids & Lipid Metabolism
 I. Overall concepts A. Definitions ANC/NUTR 618 Lipids & Lipid Metabolism 1. De novo synthesis = synthesis from non-fatty acid precursors a. Carbohydrate precursors (glucose, lactate, and pyruvate) b.
I. Overall concepts A. Definitions ANC/NUTR 618 Lipids & Lipid Metabolism 1. De novo synthesis = synthesis from non-fatty acid precursors a. Carbohydrate precursors (glucose, lactate, and pyruvate) b.
ANSC/NUTR 618 LIPIDS & LIPID METABOLISM. Fatty Acid Elongation and Desaturation
 ANSC/NUTR 618 LIPIDS & LIPID METABOLISM I. Fatty acid elongation A. General 1. At least 60% of fatty acids in triacylglycerols are C18. 2. Free palmitic acid (16:0) synthesized in cytoplasm is elongated
ANSC/NUTR 618 LIPIDS & LIPID METABOLISM I. Fatty acid elongation A. General 1. At least 60% of fatty acids in triacylglycerols are C18. 2. Free palmitic acid (16:0) synthesized in cytoplasm is elongated
UNIREDUCE R-35 OIL SOLUBLE BIOACTIVE COMPLEX TO REDUCE SEBUM PRODUCTION IN OILY SKIN
 OIL SOLUBLE BIOACTIVE COMPLEX TO REDUCE SEBUM PRODUCTION IN OILY SKIN FM-097B TDS Unireduce R-35 en(04).doc Version: 04 / 19.05.2008 1/12 Contents 1. Introduction... 3 2. Concept of the Complex Unireduce
OIL SOLUBLE BIOACTIVE COMPLEX TO REDUCE SEBUM PRODUCTION IN OILY SKIN FM-097B TDS Unireduce R-35 en(04).doc Version: 04 / 19.05.2008 1/12 Contents 1. Introduction... 3 2. Concept of the Complex Unireduce
Test Bank for Lehninger Principles of Biochemistry 5th Edition by Nelson
 Test Bank for Lehninger Principles of Biochemistry 5th Edition by Nelson Link download full: http://testbankair.com/download/test-bank-forlehninger-principles-of-biochemistry-5th-edition-by-nelson/ Chapter
Test Bank for Lehninger Principles of Biochemistry 5th Edition by Nelson Link download full: http://testbankair.com/download/test-bank-forlehninger-principles-of-biochemistry-5th-edition-by-nelson/ Chapter
Biosynthesis of Fatty Acids. By Dr.QUTAIBA A. QASIM
 Biosynthesis of Fatty Acids By Dr.QUTAIBA A. QASIM Fatty Acids Definition Fatty acids are comprised of hydrocarbon chains terminating with carboxylic acid groups. Fatty acids and their associated derivatives
Biosynthesis of Fatty Acids By Dr.QUTAIBA A. QASIM Fatty Acids Definition Fatty acids are comprised of hydrocarbon chains terminating with carboxylic acid groups. Fatty acids and their associated derivatives
Pseudo-acylceramide with Linoleic Acid Produces Selective Recovery of
 Pseudo-acylceramide with Linoleic Acid Produces Selective Recovery of Diminished Cutaneous Barrier Function in Essential Fatty Acid-deficient Rats and Has an Inhibitory Effect on Epidermal Hyperplasia
Pseudo-acylceramide with Linoleic Acid Produces Selective Recovery of Diminished Cutaneous Barrier Function in Essential Fatty Acid-deficient Rats and Has an Inhibitory Effect on Epidermal Hyperplasia
Chapter 20 Lipids. Organic and Biochem
 Chapter 20 Lipids rganic and Biochem 20.1 Introduction Found in living organisms Insoluble in water but Soluble in non-polar substances Example of Lipid Solvent: diethyl ether Polar groups in lipids are
Chapter 20 Lipids rganic and Biochem 20.1 Introduction Found in living organisms Insoluble in water but Soluble in non-polar substances Example of Lipid Solvent: diethyl ether Polar groups in lipids are
Drugs, Bugs & Neutrons where are we and where do we go from here?
 Drugs, Bugs & Neutrons where are we and where do we go from here? Dave Barlow, Pharmacy Department, King s College London The Future and Next Generation Capabilities of Accelerator-driven Neutron and Muon
Drugs, Bugs & Neutrons where are we and where do we go from here? Dave Barlow, Pharmacy Department, King s College London The Future and Next Generation Capabilities of Accelerator-driven Neutron and Muon
Statin inhibition of HMG-CoA reductase: a 3-dimensional view
 Atherosclerosis Supplements 4 (2003) 3/8 www.elsevier.com/locate/atherosclerosis Statin inhibition of HMG-CoA reductase: a 3-dimensional view Eva Istvan * Department of Molecular Microbiology, Howard Hughes
Atherosclerosis Supplements 4 (2003) 3/8 www.elsevier.com/locate/atherosclerosis Statin inhibition of HMG-CoA reductase: a 3-dimensional view Eva Istvan * Department of Molecular Microbiology, Howard Hughes
Generation of Free Fatty Acids from Phospholipids Regulates Stratum Corneum Acidi cation and Integrity
 Generation of Free Fatty Acids from Phospholipids Regulates Stratum Corneum Acidi cation and Integrity Joachim W. Fluhr, Jack Kao, Mahendra Jain,* Sung K. Ahn, Kenneth R. Feingold, and Peter M. Elias Dermatology
Generation of Free Fatty Acids from Phospholipids Regulates Stratum Corneum Acidi cation and Integrity Joachim W. Fluhr, Jack Kao, Mahendra Jain,* Sung K. Ahn, Kenneth R. Feingold, and Peter M. Elias Dermatology
Skin and Liquid Crystal: A Brief Review on their Similarities
 ORIENTAL JOURNAL OF CHEMISTRY An International Open Free Access, Peer Reviewed Research Journal www.orientjchem.org ISSN: 0970-020 X CODEN: OJCHEG 2016, Vol. 32, No. (4): Pg. 2073-2078 Skin and Liquid
ORIENTAL JOURNAL OF CHEMISTRY An International Open Free Access, Peer Reviewed Research Journal www.orientjchem.org ISSN: 0970-020 X CODEN: OJCHEG 2016, Vol. 32, No. (4): Pg. 2073-2078 Skin and Liquid
Cellular control of cholesterol. Peter Takizawa Department of Cell Biology
 Cellular control of cholesterol Peter Takizawa Department of Cell Biology Brief overview of cholesterol s biological role Regulation of cholesterol synthesis Dietary and cellular uptake of cholesterol
Cellular control of cholesterol Peter Takizawa Department of Cell Biology Brief overview of cholesterol s biological role Regulation of cholesterol synthesis Dietary and cellular uptake of cholesterol
Lecture Series 4 Cellular Membranes. Reading Assignments. Selective and Semi-permeable Barriers
 Lecture Series 4 Cellular Membranes Reading Assignments Read Chapter 11 Membrane Structure Review Chapter 12 Membrane Transport Review Chapter 15 regarding Endocytosis and Exocytosis Read Chapter 20 (Cell
Lecture Series 4 Cellular Membranes Reading Assignments Read Chapter 11 Membrane Structure Review Chapter 12 Membrane Transport Review Chapter 15 regarding Endocytosis and Exocytosis Read Chapter 20 (Cell
Lecture Series 5 Cellular Membranes
 Lecture Series 5 Cellular Membranes Cellular Membranes A. Membrane Composition and Structure B. Animal Cell Adhesion C. Passive Processes of Membrane Transport D. Active Transport E. Endocytosis and Exocytosis
Lecture Series 5 Cellular Membranes Cellular Membranes A. Membrane Composition and Structure B. Animal Cell Adhesion C. Passive Processes of Membrane Transport D. Active Transport E. Endocytosis and Exocytosis
