Lipoprotein-Associated Phospholipase A2 Is an Independent Predictor of Incident Coronary Heart Disease in an Apparently Healthy Older Population
|
|
|
- Tracey Davidson
- 5 years ago
- Views:
Transcription
1 Journal of the American College of Cardiology Vol. 51, No. 9, by the American College of Cardiology Foundation ISSN /08/$34.00 Published by Elsevier Inc. doi: /j.jacc Coronary Heart Disease Lipoprotein-Associated Phospholipase A2 Is an Independent Predictor of Incident Coronary Heart Disease in an Apparently Healthy Older Population The Rancho Bernardo Study Lori B. Daniels, MD,* Gail A. Laughlin, PHD, Mark J. Sarno, BA, Ricki Bettencourt, MS, Robert L. Wolfert, PHD, Elizabeth Barrett-Connor, MD San Diego, La Jolla, and South San Francisco, California Objectives Background Methods Results Conclusions Lipoprotein-associated phospholipase A2 (Lp-PLA2) levels predict incident coronary heart disease (CHD) in adults without known CHD, independent of heart disease risk factors. We examined whether the independent association was apparent in older adults. Serum levels of Lp-PLA2, an enzyme that hydrolyzes oxidized phospholipids to yield potentially proatherogenic particles, have been associated with CHD and may help predict cardiovascular risk. Participants were 1,077 community-dwelling men and women, median age 72 years, who had no known CHD at baseline (1984 to 1987) when blood samples and risk factor data were collected. Participants were followed for CHD events for a mean of 16 years, through Cox proportional hazards regression models were used to examine the association of serum Lp-PLA2 with incident CHD (myocardial infarction, angina, or coronary revascularization). The Lp-PLA2 levels positively correlated with age (r 0.09), body mass index (r 0.11), low-density lipoprotein (r 0.37), triglycerides (r 0.25), and C-reactive protein (r 0.10), and negatively correlated with high-density lipoprotein (r 0.27) (all p 0.05). During follow-up, 228 participants had incident CHD events. Lipoproteinassociated phospholipase A2 levels in the second, third, and fourth quartiles predicted an increased risk of CHD compared with the lowest quartile (hazard ratios 1.66, 1.80, and 1.89, respectively; p 0.05 for each). This association persisted after adjusting for C-reactive protein and other CHD risk factors. Elevated Lp-PLA2 levels predict CHD events in apparently healthy older adults, independent of CHD risk factors. (J Am Coll Cardiol 2008;51:913 9) 2008 by the American College of Cardiology Foundation Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor acetylhydrolase, is a 50-kd calcium-independent enzyme synthesized by macrophages and platelets (1). It is a member of the phospholipase A2 superfamily, and is colocated with and highly expressed by macrophages within the necrotic core and the fibrotic cap of From the *Division of Cardiology, Department of Medicine, University of California at San Diego, San Diego, California; Department of Family and Preventive Medicine, University of California at San Diego, La Jolla, California; and diadexus, Inc., South San Francisco, California. The Rancho Bernardo study was funded by research grant AG07181 from the National Institute on Aging and grant DK31801 from the National Institute of Diabetes and Digestive and Kidney Diseases. The present analysis was supported, in part, by a grant from the American Heart Association (to Dr. Daniels). The Lp-PLA2 levels were measured by diadexus, Inc. Mr. Sarno and Ms. Bettencourt have received consulting fees from diadexus, Inc. Dr. Wolfert is employed by and owns stock options in diadexus, Inc. Steven E. Nissen, MD, MACC, served as Guest Editor for this paper. Manuscript received June 27, 2007; revised manuscript received October 10, 2007, accepted October 11, advanced rupture-prone plaques (2,3). The primary enzymatic role of Lp-PLA2 is to hydrolyze oxidized phospholipids, yielding the proinflammatory and proatherogenic products, lysophosphatidylcholine and oxidized nonesterified fatty acids. These bioactive products play critical roles in the induction of chemotactic response, endothelial cell dysfunction, and smooth muscle cell apoptosis (4). As such, Lp-PLA2 appears to be a key mediator of the proatherogenic process. Several epidemiologic studies support the proatherogenic effects of Lp-PLA2, most of which have included only middle-aged men. Higher Lp-PLA2 levels were strongly associated with an increased risk of incident coronary heart disease (CHD) in a nested case-control analysis of 1,740 men with a mean age of 57 years from WOSCOPS (West of Scotland Coronary Prevention Study) (5) and in a prospective cohort analysis of 934 men ages 45 to 64 years from the MONICA (Monitoring Trends and Determinants
2 914 Daniels et al. JACC Vol. 51, No. 9, 2008 Lp-PLA2 Predicts Incident CHD in Older Adults March 4, 2008:913 9 Abbreviations and Acronyms BMI body mass index CHD coronary heart disease CI confidence interval CRP C-reactive protein HDL high-density lipoprotein HR hazard ratio LDL low-density lipoprotein Lp-PLA2 lipoproteinassociated phospholipase A2 in Cardiovascular Diseases) study (6). The significant elevation in risk persisted in these studies after adjustment for traditional risk factors and C-reactive protein (CRP), a marker of systemic inflammation. A case-cohort analysis from the ARIC (Atherosclerosis Risk In Communities) study, which included both men and women (n 1,652) ages 45 to 64 years, reported a strong positive relationship between Lp-PLA2 levels and CHD outcomes. The association was independent of traditional risk factors and CRP only in those with low-density lipoprotein (LDL) cholesterol 130 mg/dl (7). A nested case-control analysis of 246 low-risk women from the Women s Health study (mean age 60 years) also reported higher Lp-PLA2 levels in women with increased CHD risk, but adjustment for other cardiovascular risk factors eliminated the association (8), suggesting that Lp-PLA2 may not be as strong a predictor of CHD in women. Because age is the single most powerful predictor of heart disease, it is possible that Lp-PLA2 levels do not contribute anything further to CHD risk prediction in the elderly. Currently, limited data are available on Lp-PLA2 mass levels and incident CHD in the elderly. In the Rotterdam study, where the mean age of subjects was 70 years and median follow-up was 7 years, those with higher baseline levels of Lp-PLA2 activity were at increased risk for CHD and ischemic stroke, but data on LDL cholesterol levels or Lp-PLA2 mass levels were not reported (9). We investigated the ability of Lp-PLA2 to predict fatal and nonfatal CHD events independent of traditional risk factors and CRP in community-dwelling older men and women who were in apparently good health and were followed for an average of 16 years. Methods Study population. The Rancho Bernardo study is an ongoing population-based study of healthy aging in Caucasian residents of a Southern California community, which was established in Between 1984 and 1987, 82% of surviving community-dwelling older participants attended a research clinic visit, which served as the baseline visit for the present report. The subjects of this report are the 1,077 participants age 40 years who at baseline had no history of cardiovascular disease (myocardial infarction, coronary revascularization, angina, stroke, or transient ischemic attack), who were not current users of hormone therapy, and who had sufficient archived serum for measurement of Lp-PLA2. The study protocol was approved by the Institutional Review Board at the University of California, San Diego; all participants provided written, informed consent. Medical history and incident CHD information were obtained using standardized questionnaires at baseline, at clinic visits approximately every 4 years thereafter, and from periodic mailings. Follow-up continued through 2002, an 18-year follow-up (mean follow-up 16 years). Study participants were classified as incident CHD cases if at any time during the follow-up period they had a fatal or nonfatal myocardial infarction, coronary revascularization, or angina (grades 1 or 2 by Rose criteria) (10). Myocardial infarction was diagnosed based on a history of physician-diagnosed myocardial infarction or evidence of myocardial infarction on resting 12-lead electrocardiogram using the Whitehall criteria as applied in the World Health Organization s Multinational Study of Diabetes and Vascular Disease (Minnesota codes 1.1 to 1.2 [major Q-wave] or [left bundle branch block]) (11,12). At another study visit, diagnosis of a heart attack had been validated in 85% of the cases by a panel of cardiologists who reviewed the medical records of a 30% sample of this cohort. Vital status was known for 96% of participants. Death certificates were obtained for 95% of all decedents and coded by a certified nosologist using the International Classification of Disease-9th Revision criteria; decedents whose death certificates were unavailable were excluded from this analysis. Fatal CHD included deaths assigned codes 410 through 414. Participants who were alive and event-free were censored at the end of follow-up (December 31, 2002), or at the date of their last follow-up for the 4% whose status was unknown. Subjects who died of non- CHD causes were censored at time of death. Measurements. Baseline data for these analyses were obtained in 1984 to Information on medical history, medication use, physical activity (exercise 3 times per week, yes/no), alcohol consumption (1 drinks per day vs. less or none), and current smoking (yes/no) was obtained using standard questionnaires. Current medication use was validated by examination of pills and prescriptions brought to the clinic for that purpose. Blood pressure was measured by standard protocol as the mean of 2 readings after the participant had been sitting for 5 min. Body mass index (BMI) (kg/m 2 ) was derived from height and weight measured in the clinic with participants wearing light clothing and no shoes. Blood samples were obtained by venipuncture between 7:30 AM and 11:00 AM after a requested 12-h fast. Serum and plasma were separated and stored at 70 C. Lipids and lipoproteins were measured on fresh samples in a Lipid Research Clinic laboratory at the University of California at San Diego (San Diego, Calfornia). Total cholesterol and triglyceride levels were measured by enzymatic techniques using an ABA-200 biochromatic analyzer (Abbott Laboratories, Irving, Texas). High-density lipoprotein (HDL) cholesterol was measured by precipitating other circulating lipoproteins with heparin and manganese chloride accord-
3 JACC Vol. 51, No. 9, 2008 March 4, 2008:913 9 Daniels et al. Lp-PLA2 Predicts Incident CHD in Older Adults 915 ing to the standard Lipid Research Clinics protocol (13). Low-density lipoprotein cholesterol was estimated using the Friedewald formula (14). Plasma glucose levels were measured by the glucose oxidase method. In 2000, plasma levels of high-sensitivity CRP were measured in a university hospital laboratory using an automated high-sensitivity assay (N Latex CRP mono, Dade Behring, Marburg, Germany; sensitivity 0.2 mg/l) on previously unthawed plasma that had been stored at 70 C. Lipoprotein-associated phospholipase A2 mass levels were measured in 2005 using the PLAC test (diadexus, Inc., South San Francisco, California) on frozen sera from the same visit, which had been thawed 2 times previously. The manufacturer reports that samples can be frozen and thawed up to 6 times without affecting Lp-PLA2 quantification. The assay is a microplate-based enzyme-linked immunoadsorbent assay, employing 2 monoclonal antibodies specific for Lp-PLA2, and calibrated to a recombinant enzyme standard. The assay sensitivity was 1.3 ng/ml and intra- and interassay coefficients of variation were 6% and 9%, respectively. Subjects were classified as persons with diabetes according to 1999 World Health Organization criteria if the fasting plasma glucose was 126 mg/dl, the 2-h glucose after oral glucose tolerance test was 200 mg/dl, if they were taking insulin or oral diabetes medication, or if they were diagnosed as a patient with diabetes by a physician (15). Statistical methods. Means are expressed standard deviation. High-density lipoprotein, triglycerides, CRP, and Lp-PLA2 were not normally distributed and were log transformed for analyses; geometric means are reported. Baseline characteristics were compared between cases and noncases using general linear models adjusted for age for continuous variables and chi-square analysis for categorical variables; categorical variables were adjusted using the adjusted proportions module in STATA, which calculates adjusted probabilities from logistic regression estimates (16). Associations between Lp-PLA2 and other risk factors were examined using Spearman rank-order correlation. Multivariate Cox proportional hazards regression models were developed to determine the association of Lp-PLA2 with incident CHD. The primary null hypothesis was that Lp-PLA2 was not predictive of CHD events over and above various demographic variables and traditional risk factors. Results were expressed as hazard ratios (HRs) with 95% confidence intervals (CIs). Study participants were categorized into quartiles of Lp-PLA2, and 4 sequential Cox regression models were generated. Model 1 adjusted for age and gender. For Model 2, life-style, risk factor, and laboratory covariates from Table 1 were analyzed, and univariate predictors of CHD events were identified if significant at p This process yielded age, gender, HDL, triglycerides, LDL, fasting plasma glucose, systolic blood pressure, diabetes, hypertension, and Lp-PLA2 as potential predictors. Cox regression analysis was performed using these 10 Age-Adjusted Risk (1984Factors 1987) and Mean Medications SD or Prevalence at Baseline of Table 1 Age-Adjusted Mean SD or Prevalence of Risk Factors and Medications at Baseline (1984 to 1987) Variable Cases (n 228) Noncases (n 849) p Value (Cases Vs. Noncases) Age, yrs* Women, %* Lifestyle factors, % Current smoker Exercise 3 /week Alcohol daily Medication use, % Aspirin Lipid-lowering drugs Beta-blockers Risk factors Diabetes, % Hypertension, % BMI Systolic BP, mm Hg Diastolic BP, mm Hg Laboratory values Total cholesterol, mg/dl HDL, mg/dl LDL, mg/dl Triglycerides, mg/dl Fasting plasma glucose, g/dl CRP, mg/l Lp-PLA2, ng/ml *Unadjusted mean; all others are age-adjusted; geometric mean. BMI body mass index; BP blood pressure; CRP C-reactive protein; HDL high-density lipoprotein; LDL low-density lipoprotein; Lp-PLA2 lipoprotein-associated phospholipase A2; SD standard deviation. covariates (Model 2), and those that were significant at p 0.05 (age, gender, fasting plasma glucose, systolic blood pressure, and Lp-PLA2) were retained in the final Model 3. No 2-way interactions were identified. Model 4 incorporated the same covariates as Model 3 but included only the subset of participants who had CRP measurements available (n 815) so that the effect of adding CRP to the model could be distinguished from any effect due to loss of power. Model 5 was the same as Model 4, but with CRP added as a covariate. All variables were treated as continuous variables except gender, diabetes, history of hypertension, smoking status, physical activity, and alcohol consumption, which were treated as dichotomous variables. The lowest quartile was the reference group for all regressions. Age-adjusted survival curves were generated by the average covariate method, computing a survival curve for each group with age set to the average value for the study sample (17). Receiver-operating characteristic curves were constructed after adjustment for covariates, and the area under the curve with its 95% CI was calculated. Significance of differences between receiver-operating characteristic curves were tested using a nonparametric approach to the analysis of areas under correlated curves (18). A 2-tailed p 0.05 was considered statistically significant. Data were analyzed using SAS, version 9.1
4 916 Daniels et al. JACC Vol. 51, No. 9, 2008 Lp-PLA2 Predicts Incident CHD in Older Adults March 4, 2008:913 9 (SAS Institute, Cary, North Carolina) and STATA version 9 (Stata Corp., College Station, Texas). Results Baseline characteristics. Of the 1,077 participants in the study population, 228 (131 men, 97 women) experienced a CHD event during follow-up (mean 16 years) and were categorized as cases. The events included 86 (37.7%) fatal myocardial infarction, 70 (30.7%) nonfatal myocardial infarction, 43 (18.9%) angina, and 29 (12.7%) revascularization procedures, with mean time to event of 7.6 years. Noncases included 446 men and 403 women. Baseline characteristics of the study population by CHD status are shown in Table 1. In an analysis of baseline risk factors and medication use, the study population was similar to the overall cohort from which it was derived except that those without Lp-PLA2 measurements (n 494) were slightly younger (69 vs. 70 years, p 0.01), more likely to be women (59% vs. 46%, p 0.01), slightly more likely to have diabetes (17% vs. 13%, p 0.02), and had lower diastolic blood pressure (76 mm Hg vs. 78 mm Hg, p 0.001). As shown in Table 1, at baseline individuals who later experienced CHD events were significantly older (mean age years vs years) and had significantly higher BMI, systolic blood pressure, LDL, and Lp-PLA2 (538 ng/ml vs. 494 ng/ml, p 0.001) and significantly lower HDL levels than noncases. No significant differences by CHD status were observed for CRP, diastolic blood pressure, total cholesterol, triglycerides, or interleukin 6, nor were there differences in gender distribution or in the prevalence of smoking, diabetes, or hypertension in cases versus noncases. Lp-PLA2 values and associations with other risk factors. Median Lp-PLA2 levels were similar in participants who were older than 70 compared with those who were younger and did not differ by gender, diabetes, or smoking status (Table 2). Lipoprotein-associated phospholipase A2 levels were significantly lower in participants who drank alcohol daily compared with less frequent drinkers. Lipoproteinassociated phospholipase A2 levels positively correlated (all p 0.05) with total cholesterol (r 0.29), LDL cholesterol (r 0.37), and triglycerides (r 0.25) and negatively correlated with HDL cholesterol (r 0.27) (Table 3). Weak, but significant, positive associations were also observed between Lp-PLA2 and systolic blood pressure (r 0.08), CRP (r 0.10), and BMI (r 0.11) (Table 3). Lipoprotein-associated phospholipase A2 levels did not differ by use of aspirin or beta-blockers (data not shown). Prediction of incident CHD. In an age- and genderadjusted Cox proportional hazards regression model, participants with Lp-PLA2 levels in the second, third, and fourth quartiles had 66%, 80%, and 89% increased risk of incident CHD compared with those in the lowest quartile (all p 0.05) (Table 4, Model 1). Results remained Median Lp-PLA2 Levels by Baseline Characteristics Table 2 Median Lp-PLA2 Levels by Baseline Characteristics Variable n Lp-PLA2 (ng/ml) IQR p Value Gender Male Female Age, yrs Diabetes Diabetic patients Nondiabetic patients Smoking Current smokers Nonsmokers Exercise Exercise 3 per week Exercise 3 per week Alcohol Daily alcohol drinkers Less than daily drinkers IQR interquartile range; Lp-PLA2 lipoprotein-associated phospholipase A2. significant after further adjustment for cardiovascular risk factors (Model 2); only fasting plasma glucose levels and systolic blood pressure remained in the final model (Model 3). When analysis was limited to those who had CRP measurements, results were significant for the third and fourth quartiles of Lp-PLA2 (Model 4), with risk estimates similar to those for the entire study group. Additional adjustment for CRP levels had minimal effect on the Lp-PLA2-incident CHD association (Model 5). Results were also similar when those with LDL levels above the median were compared with those with LDL levels below the median (data not shown). There was no interaction of gender and Lp-PLA2 in any of these models. Figure 1 shows graded age-adjusted CHD event-free survival by Lp-PLA2 tertile (p 0.01). Receiver-operating characteristic curves were constructed to evaluate the incremental benefit of Lp-PLA2 in predicting incident CHD. Although the addition of CRP to a model including age, gender, hypertension, diabetes, smoking, and exercise did not change the area under the curve (0.595 [95% CI to 0.640] vs [95% CI to 0.641], p 0.93), the further addition of Lp-PLA2 significantly increased the area under the curve to (95% CI to 0.662) (p 0.04) (Table 5). The overall findings remained the same when the definition of incident CHD excluded angina or was limited to myocardial infarction or revascularization or myocardial infarction alone. Discussion In the present study of older community-dwelling individuals, Lp-PLA2 levels were significantly higher in those who
5 JACC Vol. 51, No. 9, 2008 March 4, 2008:913 9 Correlation Lp-PLA2 andbetween Other Risk Factors Table 3 Correlation Between Lp-PLA2 and Other Risk Factors Risk Factor Spearman Rho p Value Age BMI Systolic BP Diastolic BP Total cholesterol HDL LDL Triglycerides Fasting plasma glucose CRP Daniels et al. Lp-PLA2 Predicts Incident CHD in Older Adults 917 Abbreviations as in Table 1. developed CHD compared with those who did not. Associations between Lp-PLA2 and LDL, HDL, total cholesterol, and triglycerides were especially strong, and the magnitude of the correlations was in good agreement with previous studies (7,19). Despite these associations, Lp- PLA2 remained a strong and independent predictor of fatal and nonfatal CHD events, over and above these and other traditional risk factors. Thus, Lp-PLA2 added information to lipid and lipoprotein prediction of future CHD and may identify subpopulations at risk for CHD who would not be identified otherwise. A similar independent association of Lp-PLA2 with CHD risk was reported in the younger participants from the WOSCOPS (5) and ARIC (7,19) studies and in a nested case-control study from the Rotterdam study (9). We now confirm these results for the first time in a cohort of apparently HRs by Lp-PLA2 (95% CIs) Quartile* for Incident CHD Table 4 HRs (95% CIs) for Incident CHD by Lp-PLA2 Quartile* Lp-PLA2 Quartiles 2nd Quartile 3rd Quartile 4th Quartile ( ng/ml) ( ng/ml) (>625.2 ng/ml) Model ( ) 1.80 ( ) 1.89 ( ) [269] [270] [269] Model ( ) 1.71 ( ) 1.61 ( ) [269] [270] [269] Model ( ) 1.83 ( ) 1.81 ( ) [269] [270] [269] Model ( ) 1.93 ( ) 1.75 ( ) [211] [198] [199] Model ( ) 1.96 ( ) 1.75 ( ) [211] [198] [199] *Lowest quartile ( ng/ml) is reference. The number in brackets is the n for each quartile. Quartile cutpoints were calculated based on the sample of 1,077. The n for Q1 is [269] for Models 1, 2, and 3 and [209] for Models 4 and 5. Model 1 (n 1,077): adjusted for age and gender; Model 2 (n 1,077): adjusted for age, gender, fasting plasma glucose, systolic blood pressure, hypertension, diabetes, low-density lipoprotein, lnhigh-density lipoprotein, and lntriglycerides; Model 3 (n 1,077): adjusted for age, gender, fasting plasma glucose, systolic blood pressure; Model 4 (n 815): Model 3, but includes only those subjects who had C-reactive protein measured (C-reactive protein not in the model); Model 5 (n 815): Model 4 C-reactive protein. CHD coronary heart disease; CI confidence interval; HR hazard ratio; ln natural logarithm; Lp-PLA2 lipoprotein-associated phospholipase A2. Figure 1 Age-Adjusted Event-Free Survival by Lp-PLA2 Tertile Age-adjusted survival free of fatal or nonfatal myocardial infarction, coronary revascularization, or angina, by lipoprotein-associated phospholipase A2 (Lp- PLA2) tertile (low to ng/ml; medium to ng/ml; high to 3,126.8 ng/ml). CHD coronary heart disease. healthy older men and women followed for a longer period of time. In agreement with the ARIC and Rotterdam studies (7,9,19), the adjusted risk of incident CHD was significantly elevated beginning in the second quartile of Lp-PLA2, suggesting that, as in middle-aged adults, even minimally elevated Lp-PLA2 values are associated with an increased risk of developing CHD in older adults. The addition of CRP to the fully adjusted model did not diminish the predictive capability of Lp-PLA2, evidence that the 2 markers are not codependent. This is in agreement with previous studies in which Lp-PLA2 maintained significance in models adjusted for CRP and all traditional factors in WOSCOPS (relative risk per 1 standard deviation 1.18, 95% CI 1.05 to 1.33) (5) and ARIC (HR of highest tertile in the LDL 130 mg/dl population 2.08, 95% CI 1.20 to 3.62) (7). Similar results were also seen for the 2 highest quartiles of Lp-PLA2 in the Rotterdam study CHD analysis (9). Predictive to Increase inincident Accuracy the AUCCHD of Various as Measured Multivariate by an Models Table 5 Predictive Accuracy of Various Multivariate Models to Predict Incident CHD as Measured by an Increase in the AUC Model Adjusted for AUC (95% CI) p Value* 1. Age, gender, hypertension, diabetes, ( ) smoking, exercise 2. Above covariates plus CRP ( ) Above covariates plus CRP and ( ) Lp-PLA2 *p values are for comparisons between 2 consecutive models. AUC area under the receiver-operating characteristic curve; CRP C-reactive protein; other abbreviations as in Table 4.
6 918 Daniels et al. JACC Vol. 51, No. 9, 2008 Lp-PLA2 Predicts Incident CHD in Older Adults March 4, 2008:913 9 One difference of note is the higher distribution of Lp- PLA2 values in the present study compared with that seen in previous studies. Mean values of Lp-PLA2 in young adults in the CARDIA (Coronary Artery Risk Development in Young Adults) study were 296 ng/ml and 267 ng/ml in cases and control subjects, respectively (20). The middle-aged population evaluated in the ARIC study reported Lp-PLA2 mean values of 404 ng/ml and 373 ng/ml in cases and control subjects. The higher values observed in the present study (538 ng/ml for cases, 494 ng/ml for noncases) may reflect the higher risk in an older population, an effect of the decade-long storage of samples, or may result from other as yet undetermined factors. Although we found no difference in Lp-PLA2 values in participants older or younger than the median age of 70 years, Lp-PLA2 values were significantly higher in subjects 55 years of age compared with those seen in subjects age 55 years, lending credence to an age-associated increment in Lp-PLA2 at midlife. Although the absolute Lp-PLA2 values in this study are higher than in previous studies, the correlations between Lp-PLA2 levels and other measures such as LDL and HDL are almost identical to those seen in prior studies (6,7,9), supporting the utility if not the optimal cutpoint for our values. As a corollary to the observed higher Lp-PLA2 levels in this older population, it is likely that nearly all subjects had some degree of cardiovascular disease pathology since atherosclerotic burden increases with age. Thus, HRs for cases versus noncases might be somewhat lower than in a population where the noncases have a lower atherosclerotic burden. However, our observed HR for incident CHD of 1.6 for the highest versus lowest quartile in the present study is only slightly lower than the reported HR of approximately 1.8 from WOSCOPS (though quintiles were used there). One advantage of our study is that the cohort was recruited in the 1970s. At the time samples were drawn, available pharmacotherapies were limited, and only 5 participants were taking lipid-lowering medications. Also during this time period, few were taking aspirin regularly for cardiovascular prevention. If our subjects use of statins, angiotensinconverting enzyme inhibitors, and anti-inflammatory medications was more in line with the present higher levels of use, the perceived utility of Lp-PLA2 might have been altered. It is unknown whether the modern pharmacotherapies would attenuate, accentuate, or have no effect on the predictive capability of Lp-PLA2. Additional studies are required to identify and characterize the magnitude of any such alterations. Conclusions In summary, in a cohort of community-dwelling older adults followed for an average of 16 years, measurement of Lp-PLA2 mass demonstrated strong predictive capability for subsequent CHD events. This predictive capability was independent of traditional risk factors of CHD and in accord with previous findings. The present study extends the previous findings into the older population and represents a potential clinical application of Lp-PLA2 measurements in identification of individuals at risk for CHD who would not otherwise be identified by traditional measures. Reprint requests and correspondence: Dr. Lori B. Daniels, Mail Code 0986, 9350 Campus Point Drive, Suite 1D, La Jolla, California lbdaniels@ucsd.edu. REFERENCES 1. Tjoelker LW, Eberhardt C, Unger J, et al. Plasma platelet-activating factor acetylhydrolase is a secreted phospholipase A2 with a catalytic triad. J Biol Chem 1995;270: Hakkinen T, Luoma JS, Hiltunen MO, et al. Lipoprotein-associated phospholipase A(2), platelet-activating factor acetylhydrolase, is expressed by macrophages in human and rabbit atherosclerotic lesions. Arterioscler Thromb Vasc Biol 1999;19: Kolodgie FD, Burke AP, Skorija KS, et al. Lipoprotein-associated phospholipase A2 protein expression in the natural progression of human coronary atherosclerosis. Arterioscler Thromb Vasc Biol 2006; 26: Yang EH, McConnell JP, Lennon RJ, et al. Lipoprotein-associated phospholipase A2 is an independent marker for coronary endothelial dysfunction in humans. Arterioscler Thromb Vasc Biol 2006; 26: Packard CJ, O Reilly DS, Caslake MJ, et al. Lipoprotein-associated phospholipase A2 as an independent predictor of coronary heart disease. West of Scotland Coronary Prevention study group. N Engl J Med 2000;343: Koenig W, Khuseyinova N, Lowel H, Trischler G, Meisinger C. Lipoprotein-associated phospholipase A2 adds to risk prediction of incident coronary events by C-reactive protein in apparently healthy middle-aged men from the general population: results from the 14-year follow-up of a large cohort from southern Germany. Circulation 2004;110: Ballantyne CM, Hoogeveen RC, Bang H, et al. Lipoproteinassociated phospholipase A2, high-sensitivity C-reactive protein, and risk for incident coronary heart disease in middle-aged men and women in the Atherosclerosis Risk in Communities (ARIC) study. Circulation 2004;109: Blake GJ, Dada N, Fox JC, Manson JE, Ridker PM. A prospective evaluation of lipoprotein-associated phospholipase A(2) levels and the risk of future cardiovascular events in women. J Am Coll Cardiol 2001;38: Oei HH, van der Meer IM, Hofman A, et al. Lipoprotein-associated phospholipase A2 activity is associated with risk of coronary heart disease and ischemic stroke: the Rotterdam study. Circulation 2005;111: Rose GA. The diagnosis of ischaemic heart pain and intermittent claudication in field surveys. Bull World Health Organ 1962;27: Diabetes Drafting Group. Prevalence of small vessel and large vessel disease in diabetic patients from 14 centres. The World Health Organisation Multinational Study of Vascular Disease in Diabetics. Diabetes drafting group. Diabetologia 1985;28 Suppl: Reid DD, Hamilton PJ, McCartney P, Rose G, Jarrett RJ, Keen H. Smoking and other risk factors for coronary heart-disease in British civil servants. Lancet 1976;2: National Heart and Lung Institute Lipid Research Clinics Program Laboratory Methods Committee. Manual of Laboratory Operations: Lipid and Lipoprotein Analysis. 2nd edition. Washington, DC: US Government Printing Office, DHEW publication no , Friedewald WT, Levy RI, Fredrickson DS. Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without use of the preparative ultracentrifuge. Clin Chem 1972;18: World Health Organization. Definition, Diagnosis and Classification of Diabetes Mellitus and its Complications: Report of a WHO
7 JACC Vol. 51, No. 9, 2008 March 4, 2008:913 9 Daniels et al. Lp-PLA2 Predicts Incident CHD in Older Adults 919 Consultation. Part 1: Diagnosis and Classification of Diabetes Mellitus. Geneva: World Health Org., Garrett J. Calculation of Adjusted Means and Proportions, Available at: Accessed January 28, Chang IM, Gelman R, Pagano M. Corrected group prognostic curves and summary statistics. J Chronic Dis 1982;35: DeLong ER, DeLong DM, Clarke-Pearson DL. Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 1988;44: Ballantyne CM, Hoogeveen RC, Bang H, et al. Lipoproteinassociated phospholipase A2, high-sensitivity C-reactive protein, and risk for incident ischemic stroke in middle-aged men and women in the Atherosclerosis Risk in Communities (ARIC) study. Arch Intern Med 2005;165: Iribarren C, Gross MD, Darbinian JA, Jacobs DR Jr., Sidney S, Loria CM. Association of lipoprotein-associated phospholipase A2 mass and activity with calcified coronary plaque in young adults: the CARDIA study. Arterioscler Thromb Vasc Biol 2005;25:
Emmanouil S. Brilakis 1{, Joseph P. McConnell 2, Ryan J. Lennon 3, Ahmad A. Elesber 1, Jeffrey G. Meyer 2, and Peter B. Berger 4 * Introduction
 European Heart Journal (2005) 26, 137 144 doi:10.1093/eurheartj/ehi010 Clinical research Association of lipoprotein-associated phospholipase A2 levels with coronary artery disease risk factors, angiographic
European Heart Journal (2005) 26, 137 144 doi:10.1093/eurheartj/ehi010 Clinical research Association of lipoprotein-associated phospholipase A2 levels with coronary artery disease risk factors, angiographic
ORIGINAL INVESTIGATION. C-Reactive Protein Concentration and Incident Hypertension in Young Adults
 ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
The Framingham Risk Score (FRS) is widely recommended
 C-Reactive Protein Modulates Risk Prediction Based on the Framingham Score Implications for Future Risk Assessment: Results From a Large Cohort Study in Southern Germany Wolfgang Koenig, MD; Hannelore
C-Reactive Protein Modulates Risk Prediction Based on the Framingham Score Implications for Future Risk Assessment: Results From a Large Cohort Study in Southern Germany Wolfgang Koenig, MD; Hannelore
Central pressures and prediction of cardiovascular events in erectile dysfunction patients
 Central pressures and prediction of cardiovascular events in erectile dysfunction patients N. Ioakeimidis, K. Rokkas, A. Angelis, Z. Kratiras, M. Abdelrasoul, C. Georgakopoulos, D. Terentes-Printzios,
Central pressures and prediction of cardiovascular events in erectile dysfunction patients N. Ioakeimidis, K. Rokkas, A. Angelis, Z. Kratiras, M. Abdelrasoul, C. Georgakopoulos, D. Terentes-Printzios,
The Framingham Coronary Heart Disease Risk Score
 Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
USING NON -TRADITIONAL RISK MARKERS IN ASSESSING CV RISK
 USING NON -TRADITIONAL RISK MARKERS IN ASSESSING CV RISK JAMES M FALKO MD PROFESSOR OF MEDICINE UNIVERSITY OF COLORADO Adapted from: Rader D. N Engl J Med. 2000 hs-crp (mg/l) 6 5 4 3 2 1 *p
USING NON -TRADITIONAL RISK MARKERS IN ASSESSING CV RISK JAMES M FALKO MD PROFESSOR OF MEDICINE UNIVERSITY OF COLORADO Adapted from: Rader D. N Engl J Med. 2000 hs-crp (mg/l) 6 5 4 3 2 1 *p
Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting glucose: The Rancho Bernardo Study
 Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
Journal of the American College of Cardiology Vol. 48, No. 2, by the American College of Cardiology Foundation ISSN /06/$32.
 Journal of the American College of Cardiology Vol. 48, No. 2, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.03.043
Journal of the American College of Cardiology Vol. 48, No. 2, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.03.043
(n=6279). Continuous variables are reported as mean with 95% confidence interval and T1 T2 T3. Number of subjects
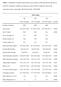 Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
A: Epidemiology update. Evidence that LDL-C and CRP identify different high-risk groups
 A: Epidemiology update Evidence that LDL-C and CRP identify different high-risk groups Women (n = 27,939; mean age 54.7 years) who were free of symptomatic cardiovascular (CV) disease at baseline were
A: Epidemiology update Evidence that LDL-C and CRP identify different high-risk groups Women (n = 27,939; mean age 54.7 years) who were free of symptomatic cardiovascular (CV) disease at baseline were
Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk. Original Policy Date
 MP 2.04.23 Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 2.04.23 Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review
This one thing can tell your heart s fortune and it s not what your doc has been testing you for!
 This one thing can tell your heart s fortune and it s not what your doc has been testing you for! By now, you are probably aware that there has been a lot of deception and misinformation out there about
This one thing can tell your heart s fortune and it s not what your doc has been testing you for! By now, you are probably aware that there has been a lot of deception and misinformation out there about
Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk
 Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk Policy Number: Original Effective Date: MM.02.018 10/01/2012 Line(s) of Business: Current Effective
Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk Policy Number: Original Effective Date: MM.02.018 10/01/2012 Line(s) of Business: Current Effective
Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association
 Measurement of Lipoprotein-Associated Phospholipase Page 1 of 11 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Measurement of Lipoprotein-Associated Phospholipase
Measurement of Lipoprotein-Associated Phospholipase Page 1 of 11 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Measurement of Lipoprotein-Associated Phospholipase
Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor
 Last Review Status/Date: September 2014 Page: 1 of 14 Description Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor acetylhydrolase, is an enzyme that hydrolyzes
Last Review Status/Date: September 2014 Page: 1 of 14 Description Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor acetylhydrolase, is an enzyme that hydrolyzes
John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam
 Latest Insights from the JUPITER Study John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam Inflammation, hscrp, and Vascular Prevention
Latest Insights from the JUPITER Study John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam Inflammation, hscrp, and Vascular Prevention
High-sensitivity Troponin T Predicts Recurrent Cardiovascular Events in Patients with Stable Coronary Heart Disease: KAROLA Study 8 Year FU
 ESC Congress 2011 Paris, France, August 27-31 KAROLA Session: Prevention: Are biomarkers worth their money? Abstract # 84698 High-sensitivity Troponin T Predicts Recurrent Cardiovascular Events in Patients
ESC Congress 2011 Paris, France, August 27-31 KAROLA Session: Prevention: Are biomarkers worth their money? Abstract # 84698 High-sensitivity Troponin T Predicts Recurrent Cardiovascular Events in Patients
GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS
 GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS Table of Contents List of authors pag 2 Supplemental figure I pag 3 Supplemental figure II pag 4 Supplemental
GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS Table of Contents List of authors pag 2 Supplemental figure I pag 3 Supplemental figure II pag 4 Supplemental
sad EFFECTIVE DATE: POLICY LAST UPDATED:
 Medical Coverage Policy Measurement of Small Low Density Lipoprotein Particles sad EFFECTIVE DATE: 02 16 2010 POLICY LAST UPDATED: 10 15 2013 OVERVIEW Lipoprotein-associated phospholipase A2 (Lp-PLA2),
Medical Coverage Policy Measurement of Small Low Density Lipoprotein Particles sad EFFECTIVE DATE: 02 16 2010 POLICY LAST UPDATED: 10 15 2013 OVERVIEW Lipoprotein-associated phospholipase A2 (Lp-PLA2),
Correlation of novel cardiac marker
 Correlation of novel cardiac marker and mortality in EGAT population. Soluble ST2 hscrp Poh Chanyavanich, MD SukitYamwong, MD Piyamitr Sritara, MD Ramathibodi hospital Background hscrp - the most widely
Correlation of novel cardiac marker and mortality in EGAT population. Soluble ST2 hscrp Poh Chanyavanich, MD SukitYamwong, MD Piyamitr Sritara, MD Ramathibodi hospital Background hscrp - the most widely
Lipid Management 2013 Statin Benefit Groups
 Clinical Integration Steering Committee Clinical Integration Chronic Disease Management Work Group Lipid Management 2013 Statin Benefit Groups Approved by Board Chair Signature Name (Please Print) Date
Clinical Integration Steering Committee Clinical Integration Chronic Disease Management Work Group Lipid Management 2013 Statin Benefit Groups Approved by Board Chair Signature Name (Please Print) Date
Spotty Calcification as a Marker of Accelerated Progression of Coronary Atherosclerosis : Insights from Serial Intravascular Ultrasound
 Spotty Calcification as a Marker of Accelerated Progression of Coronary Atherosclerosis : Insights from Serial Intravascular Ultrasound Department of Cardiovascular Medicine Heart and Vascular Institute
Spotty Calcification as a Marker of Accelerated Progression of Coronary Atherosclerosis : Insights from Serial Intravascular Ultrasound Department of Cardiovascular Medicine Heart and Vascular Institute
Autonomic nervous system, inflammation and preclinical carotid atherosclerosis in depressed subjects with coronary risk factors
 Autonomic nervous system, inflammation and preclinical carotid atherosclerosis in depressed subjects with coronary risk factors Carmine Pizzi 1 ; Lamberto Manzoli 2, Stefano Mancini 3 ; Gigliola Bedetti
Autonomic nervous system, inflammation and preclinical carotid atherosclerosis in depressed subjects with coronary risk factors Carmine Pizzi 1 ; Lamberto Manzoli 2, Stefano Mancini 3 ; Gigliola Bedetti
LIPOPROTEIN-ASSOCIATED PHOSPHOLIPASE A 2 : EFFECTS OF LOW DENSITY LIPOPROTEIN APHERESIS
 LIPOPROTEIN-ASSOCIATED PHOSPHOLIPASE A 2 : EFFECTS OF LOW DENSITY LIPOPROTEIN APHERESIS Patrick M. Moriarty, M.D., FACP, Director, Atherosclerosis and LDL-Apheresis Center, University of Kansas Medical
LIPOPROTEIN-ASSOCIATED PHOSPHOLIPASE A 2 : EFFECTS OF LOW DENSITY LIPOPROTEIN APHERESIS Patrick M. Moriarty, M.D., FACP, Director, Atherosclerosis and LDL-Apheresis Center, University of Kansas Medical
Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor
 Last Review Status/Date: September 2015 Page: 1 of 14 Description Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor acetylhydrolase, is an enzyme that hydrolyzes
Last Review Status/Date: September 2015 Page: 1 of 14 Description Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor acetylhydrolase, is an enzyme that hydrolyzes
Supplementary Table 1. Baseline Characteristics by Quintiles of Systolic and Diastolic Blood Pressures
 Supplementary Data Supplementary Table 1. Baseline Characteristics by Quintiles of Systolic and Diastolic Blood Pressures Quintiles of Systolic Blood Pressure Quintiles of Diastolic Blood Pressure Q1 Q2
Supplementary Data Supplementary Table 1. Baseline Characteristics by Quintiles of Systolic and Diastolic Blood Pressures Quintiles of Systolic Blood Pressure Quintiles of Diastolic Blood Pressure Q1 Q2
Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk
 Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk Policy Number: Original Effective Date: MM.02.018 10/01/2012 Line(s) of Business: Current Effective
Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk Policy Number: Original Effective Date: MM.02.018 10/01/2012 Line(s) of Business: Current Effective
Supplementary Online Content
 Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
JUPITER NEJM Poll. Panel Discussion: Literature that Should Have an Impact on our Practice: The JUPITER Study
 Panel Discussion: Literature that Should Have an Impact on our Practice: The Study Kaiser COAST 11 th Annual Conference Maui, August 2009 Robert Blumberg, MD, FACC Ralph Brindis, MD, MPH, FACC Primary
Panel Discussion: Literature that Should Have an Impact on our Practice: The Study Kaiser COAST 11 th Annual Conference Maui, August 2009 Robert Blumberg, MD, FACC Ralph Brindis, MD, MPH, FACC Primary
Small dense low-density lipoprotein is a risk for coronary artery disease in an urban Japanese cohort: The Suita study
 Small dense low-density lipoprotein is a risk for coronary artery disease in an urban Japanese cohort: The Suita study Hidenori Arai 1, Yoshihiro Kokubo 2, Makoto Watanabe 2, Tatsuya Sawamura 3, Tomonori
Small dense low-density lipoprotein is a risk for coronary artery disease in an urban Japanese cohort: The Suita study Hidenori Arai 1, Yoshihiro Kokubo 2, Makoto Watanabe 2, Tatsuya Sawamura 3, Tomonori
The JUPITER trial: What does it tell us? Alice Y.Y. Cheng, MD, FRCPC January 24, 2009
 The JUPITER trial: What does it tell us? Alice Y.Y. Cheng, MD, FRCPC January 24, 2009 Learning Objectives 1. Understand the role of statin therapy in the primary and secondary prevention of stroke 2. Explain
The JUPITER trial: What does it tell us? Alice Y.Y. Cheng, MD, FRCPC January 24, 2009 Learning Objectives 1. Understand the role of statin therapy in the primary and secondary prevention of stroke 2. Explain
Review of guidelines for management of dyslipidemia in diabetic patients
 2012 international Conference on Diabetes and metabolism (ICDM) Review of guidelines for management of dyslipidemia in diabetic patients Nan Hee Kim, MD, PhD Department of Internal Medicine, Korea University
2012 international Conference on Diabetes and metabolism (ICDM) Review of guidelines for management of dyslipidemia in diabetic patients Nan Hee Kim, MD, PhD Department of Internal Medicine, Korea University
300 Biomed Environ Sci, 2018; 31(4):
 300 Biomed Environ Sci, 2018; 31(4): 300-305 Letter to the Editor Combined Influence of Insulin Resistance and Inflammatory Biomarkers on Type 2 Diabetes: A Population-based Prospective Cohort Study of
300 Biomed Environ Sci, 2018; 31(4): 300-305 Letter to the Editor Combined Influence of Insulin Resistance and Inflammatory Biomarkers on Type 2 Diabetes: A Population-based Prospective Cohort Study of
STABILITY Stabilization of Atherosclerotic plaque By Initiation of darapladib TherapY. Harvey D White on behalf of The STABILITY Investigators
 STABILITY Stabilization of Atherosclerotic plaque By Initiation of darapladib TherapY Harvey D White on behalf of The STABILITY Investigators Lipoprotein- associated Phospholipase A 2 (Lp-PLA 2 ) activity:
STABILITY Stabilization of Atherosclerotic plaque By Initiation of darapladib TherapY Harvey D White on behalf of The STABILITY Investigators Lipoprotein- associated Phospholipase A 2 (Lp-PLA 2 ) activity:
Moderate alcohol consumption is associated with decreased
 Alcohol Consumption and Plasma Concentration of C-Reactive Protein Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Moderate alcohol intake has been associated with
Alcohol Consumption and Plasma Concentration of C-Reactive Protein Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Moderate alcohol intake has been associated with
Journal of the American College of Cardiology Vol. 36, No. 1, by the American College of Cardiology ISSN /00/$20.
 Journal of the American College of Cardiology Vol. 36, No. 1, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00680-X Lack
Journal of the American College of Cardiology Vol. 36, No. 1, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00680-X Lack
Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic
 Supplementary Information The title of the manuscript Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic stroke Xin-Wei He 1, Wei-Ling Li 1, Cai Li
Supplementary Information The title of the manuscript Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic stroke Xin-Wei He 1, Wei-Ling Li 1, Cai Li
Misperceptions still exist that cardiovascular disease is not a real problem for women.
 Management of Cardiovascular Risk Factors in the Cynthia A., MD University of California, San Diego ARHP 9/19/08 Disclosures Research support Wyeth, Lilly, Organon, Novo Nordisk, Pfizer Consultant fees
Management of Cardiovascular Risk Factors in the Cynthia A., MD University of California, San Diego ARHP 9/19/08 Disclosures Research support Wyeth, Lilly, Organon, Novo Nordisk, Pfizer Consultant fees
Environmental. Vascular / Tissue. Metabolics
 Global Risk Reduction--WINS Picking Mom and Dad-2016 Environmental Vascular / Tissue Metabolics Stop smoking-1b Physical activity-1b Weight control-1b Chelation therapy-3c Influenza vaccination-1b Blood
Global Risk Reduction--WINS Picking Mom and Dad-2016 Environmental Vascular / Tissue Metabolics Stop smoking-1b Physical activity-1b Weight control-1b Chelation therapy-3c Influenza vaccination-1b Blood
Enzyme Immunoassay for the Quantitative Determination of Lp-PLA 2 in Human Plasma and Serum.
 PLAC Test ELISA Kit Enzyme Immunoassay for the Quantitative Determination of Lp-PLA 2 in Human Plasma and Serum 90123 www.plactest.com Diadexus, Inc. 349 Oyster Point Blvd. South San Francisco, CA 94080
PLAC Test ELISA Kit Enzyme Immunoassay for the Quantitative Determination of Lp-PLA 2 in Human Plasma and Serum 90123 www.plactest.com Diadexus, Inc. 349 Oyster Point Blvd. South San Francisco, CA 94080
HIGH LDL CHOLESTEROL IS NOT AN INDEPENDENT RISK FACTOR FOR HEART ATTACKS AND STROKES
 HIGH LDL CHOLESTEROL IS NOT AN INDEPENDENT RISK FACTOR FOR HEART ATTACKS AND STROKES A study published in the British Medical Journal shows that not only is high LDL cholesterol not a risk factor for all-caused
HIGH LDL CHOLESTEROL IS NOT AN INDEPENDENT RISK FACTOR FOR HEART ATTACKS AND STROKES A study published in the British Medical Journal shows that not only is high LDL cholesterol not a risk factor for all-caused
Inflammation and and Heart Heart Disease in Women Inflammation and Heart Disease
 Inflammation and Heart Disease in Women Inflammation and Heart Disease What is the link between een inflammation and atherosclerotic disease? What is the role of biomarkers in predicting cardiovascular
Inflammation and Heart Disease in Women Inflammation and Heart Disease What is the link between een inflammation and atherosclerotic disease? What is the role of biomarkers in predicting cardiovascular
CVD risk assessment using risk scores in primary and secondary prevention
 CVD risk assessment using risk scores in primary and secondary prevention Raul D. Santos MD, PhD Heart Institute-InCor University of Sao Paulo Brazil Disclosure Honoraria for consulting and speaker activities
CVD risk assessment using risk scores in primary and secondary prevention Raul D. Santos MD, PhD Heart Institute-InCor University of Sao Paulo Brazil Disclosure Honoraria for consulting and speaker activities
Comparison of Probability of Stroke Between the Copenhagen City Heart Study and the Framingham Study
 80 Comparison of Probability of Stroke Between the Copenhagen City Heart Study and the Framingham Study Thomas Truelsen, MB; Ewa Lindenstrtfm, MD; Gudrun Boysen, DMSc Background and Purpose We wished to
80 Comparison of Probability of Stroke Between the Copenhagen City Heart Study and the Framingham Study Thomas Truelsen, MB; Ewa Lindenstrtfm, MD; Gudrun Boysen, DMSc Background and Purpose We wished to
Total risk management of Cardiovascular diseases Nobuhiro Yamada
 Nobuhiro Yamada The worldwide burden of cardiovascular diseases (WHO) To prevent cardiovascular diseases Beyond LDL Multiple risk factors With common molecular basis The Current Burden of CVD CVD is responsible
Nobuhiro Yamada The worldwide burden of cardiovascular diseases (WHO) To prevent cardiovascular diseases Beyond LDL Multiple risk factors With common molecular basis The Current Burden of CVD CVD is responsible
Preventing Myocardial Infarction in the Young Adult in the First Place: How Do the National Cholesterol Education Panel III Guidelines Perform?
 Journal of the American College of Cardiology Vol. 41, No. 9, 2003 2003 by the American College of Cardiology Foundation ISSN 0735-1097/03/$30.00 Published by Elsevier Inc. doi:10.1016/s0735-1097(03)00187-6
Journal of the American College of Cardiology Vol. 41, No. 9, 2003 2003 by the American College of Cardiology Foundation ISSN 0735-1097/03/$30.00 Published by Elsevier Inc. doi:10.1016/s0735-1097(03)00187-6
Diabetologia 9 Springer-Verlag 1991
 Diabetologia (1991) 34:590-594 0012186X91001685 Diabetologia 9 Springer-Verlag 1991 Risk factors for macrovascular disease in mellitus: the London follow-up to the WHO Multinational Study of Vascular Disease
Diabetologia (1991) 34:590-594 0012186X91001685 Diabetologia 9 Springer-Verlag 1991 Risk factors for macrovascular disease in mellitus: the London follow-up to the WHO Multinational Study of Vascular Disease
Cardiovascular Complications of Diabetes
 VBWG Cardiovascular Complications of Diabetes Nicola Abate, M.D., F.N.L.A. Professor and Chief Division of Endocrinology and Metabolism The University of Texas Medical Branch Galveston, Texas Coronary
VBWG Cardiovascular Complications of Diabetes Nicola Abate, M.D., F.N.L.A. Professor and Chief Division of Endocrinology and Metabolism The University of Texas Medical Branch Galveston, Texas Coronary
Behind LDL: The Metabolism of ApoB, the Essential Apolipoprotein in LDL and VLDL
 Behind LDL: The Metabolism of ApoB, the Essential Apolipoprotein in LDL and VLDL Sung-Joon Lee, PhD Division of Food Science Institute of Biomedical Science and Safety Korea University Composition of Lipoproteins:
Behind LDL: The Metabolism of ApoB, the Essential Apolipoprotein in LDL and VLDL Sung-Joon Lee, PhD Division of Food Science Institute of Biomedical Science and Safety Korea University Composition of Lipoproteins:
The Whitehall II study originally comprised 10,308 (3413 women) individuals who, at
 Supplementary notes on Methods The study originally comprised 10,308 (3413 women) individuals who, at recruitment in 1985/8, were London-based government employees (civil servants) aged 35 to 55 years.
Supplementary notes on Methods The study originally comprised 10,308 (3413 women) individuals who, at recruitment in 1985/8, were London-based government employees (civil servants) aged 35 to 55 years.
There are many ways to lower triglycerides in humans: Which are the most relevant for pancreatitis and for CV risk?
 There are many ways to lower triglycerides in humans: Which are the most relevant for pancreatitis and for CV risk? Michael Davidson M.D. FACC, Diplomate of the American Board of Lipidology Professor,
There are many ways to lower triglycerides in humans: Which are the most relevant for pancreatitis and for CV risk? Michael Davidson M.D. FACC, Diplomate of the American Board of Lipidology Professor,
Clinical Investigation and Reports
 Clinical Investigation and Reports Lipoprotein-Associated Phospholipase A 2, High-Sensitivity C-Reactive Protein, and Risk for Incident Coronary Heart Disease in Middle-Aged Men and Women in the Atherosclerosis
Clinical Investigation and Reports Lipoprotein-Associated Phospholipase A 2, High-Sensitivity C-Reactive Protein, and Risk for Incident Coronary Heart Disease in Middle-Aged Men and Women in the Atherosclerosis
journal of medicine The new england Rosuvastatin to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein Abstract
 The new england journal of medicine established in 1812 november 20, 2008 vol. 359 no. 21 to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein Paul M Ridker, M.D., Eleanor Danielson,
The new england journal of medicine established in 1812 november 20, 2008 vol. 359 no. 21 to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein Paul M Ridker, M.D., Eleanor Danielson,
Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk
 Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk Policy Number: Original Effective Date: MM.02.018 10/01/2012 Line(s) of Business: Current Effective
Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk Policy Number: Original Effective Date: MM.02.018 10/01/2012 Line(s) of Business: Current Effective
Complications of Diabetes mellitus. Dr Bill Young 16 March 2015
 Complications of Diabetes mellitus Dr Bill Young 16 March 2015 Complications of diabetes Multi-organ involvement 2 The extent of diabetes complications At diagnosis as many as 50% of patients may have
Complications of Diabetes mellitus Dr Bill Young 16 March 2015 Complications of diabetes Multi-organ involvement 2 The extent of diabetes complications At diagnosis as many as 50% of patients may have
Journal of the American College of Cardiology Vol. 48, No. 7, by the American College of Cardiology Foundation ISSN /06/$32.
 Journal of the American College of Cardiology Vol. 48, No. 7, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.06.053
Journal of the American College of Cardiology Vol. 48, No. 7, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.06.053
egfr > 50 (n = 13,916)
 Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Inflammatory markers and long-term risk of ischemic heart disease in men A 13-year follow-up of the Quebec Cardiovascular Study
 Atherosclerosis 182 (2005) 315 321 Inflammatory markers and long-term risk of ischemic heart disease in men A 13-year follow-up of the Quebec Cardiovascular Study Annie C. St-Pierre a,b, Bernard Cantin
Atherosclerosis 182 (2005) 315 321 Inflammatory markers and long-term risk of ischemic heart disease in men A 13-year follow-up of the Quebec Cardiovascular Study Annie C. St-Pierre a,b, Bernard Cantin
Subclinical atherosclerosis in CVD: Risk stratification & management Raul Santos, MD
 Subclinical atherosclerosis in CVD: Risk stratification & management Raul Santos, MD Sao Paulo Medical School Sao Paolo, Brazil Subclinical atherosclerosis in CVD risk: Stratification & management Prof.
Subclinical atherosclerosis in CVD: Risk stratification & management Raul Santos, MD Sao Paulo Medical School Sao Paolo, Brazil Subclinical atherosclerosis in CVD risk: Stratification & management Prof.
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: 2.04.65 Novel Lipid Risk Factors in Risk Assessment and Management of Cardiovascular Disease 2.04.70 Genetic Testing for Lipoprotein(a)
FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: 2.04.65 Novel Lipid Risk Factors in Risk Assessment and Management of Cardiovascular Disease 2.04.70 Genetic Testing for Lipoprotein(a)
Adherence to a healthy diet in relation to cardiovascular incidence and risk markers: evidence from the Caerphilly Prospective Study
 DOI 10.1007/s00394-017-1408-0 ORIGINAL CONTRIBUTION Adherence to a healthy diet in relation to cardiovascular incidence and risk markers: evidence from the Caerphilly Prospective Study Elly Mertens 1,2
DOI 10.1007/s00394-017-1408-0 ORIGINAL CONTRIBUTION Adherence to a healthy diet in relation to cardiovascular incidence and risk markers: evidence from the Caerphilly Prospective Study Elly Mertens 1,2
Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis
 CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
10/17/16. Assessing cardiovascular risk through use of inflammation testing
 Assessing cardiovascular risk through use of inflammation testing Anthony L. Lyssy, DO Medical Director and Managing Partner Diamond Physicians Dallas, TX Response to Injury Hypothesis Injury Response
Assessing cardiovascular risk through use of inflammation testing Anthony L. Lyssy, DO Medical Director and Managing Partner Diamond Physicians Dallas, TX Response to Injury Hypothesis Injury Response
9/29/2015. Primary Prevention of Heart Disease: Objectives. Objectives. What works? What doesn t?
 Primary Prevention of Heart Disease: What works? What doesn t? Samia Mora, MD, MHS Associate Professor, Harvard Medical School Associate Physician, Brigham and Women s Hospital October 2, 2015 Financial
Primary Prevention of Heart Disease: What works? What doesn t? Samia Mora, MD, MHS Associate Professor, Harvard Medical School Associate Physician, Brigham and Women s Hospital October 2, 2015 Financial
Marshall Tulloch-Reid, MD, MPhil, DSc, FACE Epidemiology Research Unit Tropical Medicine Research Institute The University of the West Indies, Mona,
 Marshall Tulloch-Reid, MD, MPhil, DSc, FACE Epidemiology Research Unit Tropical Medicine Research Institute The University of the West Indies, Mona, Jamaica At the end of this presentation the participant
Marshall Tulloch-Reid, MD, MPhil, DSc, FACE Epidemiology Research Unit Tropical Medicine Research Institute The University of the West Indies, Mona, Jamaica At the end of this presentation the participant
Case Presentation. Rafael Bitzur The Bert W Strassburger Lipid Center Sheba Medical Center Tel Hashomer
 Case Presentation Rafael Bitzur The Bert W Strassburger Lipid Center Sheba Medical Center Tel Hashomer Case Presentation 50 YO man NSTEMI treated with PCI 1 month ago Medical History: Obesity: BMI 32,
Case Presentation Rafael Bitzur The Bert W Strassburger Lipid Center Sheba Medical Center Tel Hashomer Case Presentation 50 YO man NSTEMI treated with PCI 1 month ago Medical History: Obesity: BMI 32,
Since 1980, obesity has more than doubled worldwide, and in 2008 over 1.5 billion adults aged 20 years were overweight.
 Impact of metabolic comorbidity on the association between body mass index and health-related quality of life: a Scotland-wide cross-sectional study of 5,608 participants Dr. Zia Ul Haq Doctoral Research
Impact of metabolic comorbidity on the association between body mass index and health-related quality of life: a Scotland-wide cross-sectional study of 5,608 participants Dr. Zia Ul Haq Doctoral Research
Diabetes and Cardiovascular Risk Management Denise M. Kolanczyk, PharmD, BCPS-AQ Cardiology
 Diabetes and Cardiovascular Risk Management Denise M. Kolanczyk, PharmD, BCPS-AQ Cardiology Disclosures In compliance with the accrediting board policies, the American Diabetes Association requires the
Diabetes and Cardiovascular Risk Management Denise M. Kolanczyk, PharmD, BCPS-AQ Cardiology Disclosures In compliance with the accrediting board policies, the American Diabetes Association requires the
The Adult Treatment Panel (ATP) III of the National
 Metabolic Syndrome With and Without C-Reactive Protein as a Predictor of Coronary Heart Disease and Diabetes in the West of Scotland Coronary Prevention Study Naveed Sattar, MD; Allan Gaw, MD; Olga Scherbakova,
Metabolic Syndrome With and Without C-Reactive Protein as a Predictor of Coronary Heart Disease and Diabetes in the West of Scotland Coronary Prevention Study Naveed Sattar, MD; Allan Gaw, MD; Olga Scherbakova,
Know Your Number Aggregate Report Single Analysis Compared to National Averages
 Know Your Number Aggregate Report Single Analysis Compared to National s Client: Study Population: 2242 Population: 3,000 Date Range: 04/20/07-08/08/07 Version of Report: V6.2 Page 2 Study Population Demographics
Know Your Number Aggregate Report Single Analysis Compared to National s Client: Study Population: 2242 Population: 3,000 Date Range: 04/20/07-08/08/07 Version of Report: V6.2 Page 2 Study Population Demographics
Measurement of Lipoprotein- Associated Phospholipase A2 (Lp- PLA2) in the Assessment of Cardiovascular Risk
 Measurement of Lipoprotein- Associated Phospholipase A2 (Lp- PLA2) in the Assessment of Cardiovascular Risk Policy Number: 2.04.32 Last Review: 5/2018 Origination: 5/2007 Next Review: 11/2018 Policy Blue
Measurement of Lipoprotein- Associated Phospholipase A2 (Lp- PLA2) in the Assessment of Cardiovascular Risk Policy Number: 2.04.32 Last Review: 5/2018 Origination: 5/2007 Next Review: 11/2018 Policy Blue
Research Article Comparison of Different Anthropometric Measurements and Inflammatory Biomarkers
 International Inflammation Volume 2012, Article ID 124693, 5 pages doi:10.1155/2012/124693 Research Article Comparison of Different Anthropometric Measurements and Inflammatory Biomarkers Yaron Arbel,
International Inflammation Volume 2012, Article ID 124693, 5 pages doi:10.1155/2012/124693 Research Article Comparison of Different Anthropometric Measurements and Inflammatory Biomarkers Yaron Arbel,
Coronary Calcium Predicts Events Better With Absolute Calcium Scores Than Age-Sex-Race/Ethnicity Percentiles
 Journal of the American College of Cardiology Vol. 53, No. 4, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.07.072
Journal of the American College of Cardiology Vol. 53, No. 4, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.07.072
The TNT Trial Is It Time to Shift Our Goals in Clinical
 The TNT Trial Is It Time to Shift Our Goals in Clinical Angioplasty Summit Luncheon Symposium Korea Assoc Prof David Colquhoun 29 April 2005 University of Queensland, Wesley Hospital, Brisbane, Australia
The TNT Trial Is It Time to Shift Our Goals in Clinical Angioplasty Summit Luncheon Symposium Korea Assoc Prof David Colquhoun 29 April 2005 University of Queensland, Wesley Hospital, Brisbane, Australia
Weintraub, W et al NEJM March Khot, UN et al, JAMA 2003
 Global risk hscrp Should not be included in a Global Cardiovascular Risk Assessment. Jodi Tinkel, MD Assistant Professor Director of Cardiac Rehabilitation Associate Program Director, Cardiovascular Medicine
Global risk hscrp Should not be included in a Global Cardiovascular Risk Assessment. Jodi Tinkel, MD Assistant Professor Director of Cardiac Rehabilitation Associate Program Director, Cardiovascular Medicine
LDL cholesterol (p = 0.40). However, higher levels of HDL cholesterol (> or =1.5 mmol/l [60 mg/dl]) were associated with less progression of CAC
![LDL cholesterol (p = 0.40). However, higher levels of HDL cholesterol (> or =1.5 mmol/l [60 mg/dl]) were associated with less progression of CAC LDL cholesterol (p = 0.40). However, higher levels of HDL cholesterol (> or =1.5 mmol/l [60 mg/dl]) were associated with less progression of CAC](/thumbs/88/116891773.jpg) Am J Cardiol (2004);94:729-32 Relation of degree of physical activity to coronary artery calcium score in asymptomatic individuals with multiple metabolic risk factors M. Y. Desai, et al. Ciccarone Preventive
Am J Cardiol (2004);94:729-32 Relation of degree of physical activity to coronary artery calcium score in asymptomatic individuals with multiple metabolic risk factors M. Y. Desai, et al. Ciccarone Preventive
ORIGINAL INVESTIGATION. Relation of Triglyceride Levels, Fasting and Nonfasting, to Fatal and Nonfatal Coronary Heart Disease
 ORIGINAL INVESTIGATION Relation of Triglyceride Levels, Fasting and Nonfasting, to Fatal and Nonfatal Coronary Heart Disease Lynn E. Eberly, PhD; Jeremiah Stamler, MD; James D. Neaton, PhD; for the Multiple
ORIGINAL INVESTIGATION Relation of Triglyceride Levels, Fasting and Nonfasting, to Fatal and Nonfatal Coronary Heart Disease Lynn E. Eberly, PhD; Jeremiah Stamler, MD; James D. Neaton, PhD; for the Multiple
Diabetes and Heart Disease. Sarah Alexander, MD, FACC Assistant Professor of Medicine Rush University Medical Center
 Diabetes and Heart Disease Sarah Alexander, MD, FACC Assistant Professor of Medicine Rush University Medical Center No conflicts of interest or financial relationships to disclose. 2 What s the problem??
Diabetes and Heart Disease Sarah Alexander, MD, FACC Assistant Professor of Medicine Rush University Medical Center No conflicts of interest or financial relationships to disclose. 2 What s the problem??
Appendix This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors.
 Appendix This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Appendix to: Banks E, Crouch SR, Korda RJ, et al. Absolute risk of cardiovascular
Appendix This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Appendix to: Banks E, Crouch SR, Korda RJ, et al. Absolute risk of cardiovascular
Heart Rate in Patients with Coronary Artery Disease - the Lower the Better? An Analysis from the Treating to New Targets (TNT) trial
 Heart Rate in Patients with Coronary Artery Disease - the Lower the Better? An Analysis from the Treating to New Targets (TNT) trial Sripal Bangalore, MD, MHA, Chuan-Chuan Wun, PhD, David A DeMicco, PharmD,
Heart Rate in Patients with Coronary Artery Disease - the Lower the Better? An Analysis from the Treating to New Targets (TNT) trial Sripal Bangalore, MD, MHA, Chuan-Chuan Wun, PhD, David A DeMicco, PharmD,
Plasma fibrinogen level, BMI and lipid profile in type 2 diabetes mellitus with hypertension
 World Journal of Pharmaceutical Sciences ISSN (Print): 2321-3310; ISSN (Online): 2321-3086 Published by Atom and Cell Publishers All Rights Reserved Available online at: http://www.wjpsonline.org/ Original
World Journal of Pharmaceutical Sciences ISSN (Print): 2321-3310; ISSN (Online): 2321-3086 Published by Atom and Cell Publishers All Rights Reserved Available online at: http://www.wjpsonline.org/ Original
Ischemic Heart and Cerebrovascular Disease. Harold E. Lebovitz, MD, FACE Kathmandu November 2010
 Ischemic Heart and Cerebrovascular Disease Harold E. Lebovitz, MD, FACE Kathmandu November 2010 Relationships Between Diabetes and Ischemic Heart Disease Risk of Cardiovascular Disease in Different Categories
Ischemic Heart and Cerebrovascular Disease Harold E. Lebovitz, MD, FACE Kathmandu November 2010 Relationships Between Diabetes and Ischemic Heart Disease Risk of Cardiovascular Disease in Different Categories
Tracking a Killer Molecule
 Tracking a Killer Molecule Mercodia Oxidized LDL ELISA www.mercodia.com Mercodia Oxidized LDL ELISA products Product Catalog No Kit size Oxidized LDL ELISA 10-1143-01 96 wells Oxidized LDL competitive
Tracking a Killer Molecule Mercodia Oxidized LDL ELISA www.mercodia.com Mercodia Oxidized LDL ELISA products Product Catalog No Kit size Oxidized LDL ELISA 10-1143-01 96 wells Oxidized LDL competitive
Table 1 Baseline characteristics of 60 hemodialysis patients with atrial fibrillation and warfarin use
 Table 1 Baseline characteristics of 60 hemodialysis patients with atrial fibrillation and warfarin use Baseline characteristics Users (n = 28) Non-users (n = 32) P value Age (years) 67.8 (9.4) 68.4 (8.5)
Table 1 Baseline characteristics of 60 hemodialysis patients with atrial fibrillation and warfarin use Baseline characteristics Users (n = 28) Non-users (n = 32) P value Age (years) 67.8 (9.4) 68.4 (8.5)
Supplementary Online Content
 Supplementary Online Content Larsen JR, Vedtofte L, Jakobsen MSL, et al. Effect of liraglutide treatment on prediabetes and overweight or obesity in clozapine- or olanzapine-treated patients with schizophrenia
Supplementary Online Content Larsen JR, Vedtofte L, Jakobsen MSL, et al. Effect of liraglutide treatment on prediabetes and overweight or obesity in clozapine- or olanzapine-treated patients with schizophrenia
The Role of Vitamin D in Heart Disease. Janet Long, MSN, ACNP, CLS, FAHA, FNLA Cardiovascular Institute Rhode Island Hospital and The Miriam Hospital
 The Role of Vitamin D in Heart Disease Janet Long, MSN, ACNP, CLS, FAHA, FNLA Cardiovascular Institute Rhode Island Hospital and The Miriam Hospital None Conflict of Interest What is Vitamin D Produced
The Role of Vitamin D in Heart Disease Janet Long, MSN, ACNP, CLS, FAHA, FNLA Cardiovascular Institute Rhode Island Hospital and The Miriam Hospital None Conflict of Interest What is Vitamin D Produced
Supplementary Online Content
 Supplementary Online Content Pedersen SB, Langsted A, Nordestgaard BG. Nonfasting mild-to-moderate hypertriglyceridemia and risk of acute pancreatitis. JAMA Intern Med. Published online November 7, 2016.
Supplementary Online Content Pedersen SB, Langsted A, Nordestgaard BG. Nonfasting mild-to-moderate hypertriglyceridemia and risk of acute pancreatitis. JAMA Intern Med. Published online November 7, 2016.
Fasting or non fasting?
 Vascular harmony Robert Chilton Professor of Medicine University of Texas Health Science Center Director of Cardiac Catheterization labs Director of clinical proteomics Which is best to measure Lower continues
Vascular harmony Robert Chilton Professor of Medicine University of Texas Health Science Center Director of Cardiac Catheterization labs Director of clinical proteomics Which is best to measure Lower continues
Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden
 Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden Cardiovascular Disease Prevention (CVD) Three Strategies for CVD
Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden Cardiovascular Disease Prevention (CVD) Three Strategies for CVD
The Clinical Unmet need in the patient with Diabetes and ACS
 The Clinical Unmet need in the patient with Diabetes and ACS Professor Kausik Ray (UK) BSc(hons), MBChB, MD, MPhil, FRCP (lon), FRCP (ed), FACC, FESC, FAHA Diabetes is a global public health challenge
The Clinical Unmet need in the patient with Diabetes and ACS Professor Kausik Ray (UK) BSc(hons), MBChB, MD, MPhil, FRCP (lon), FRCP (ed), FACC, FESC, FAHA Diabetes is a global public health challenge
How would you manage Ms. Gold
 How would you manage Ms. Gold 32 yo Asian woman with dyslipidemia Current medications: Simvastatin 20mg QD Most recent lipid profile: TC = 246, TG = 100, LDL = 176, HDL = 50 What about Mr. Williams? 56
How would you manage Ms. Gold 32 yo Asian woman with dyslipidemia Current medications: Simvastatin 20mg QD Most recent lipid profile: TC = 246, TG = 100, LDL = 176, HDL = 50 What about Mr. Williams? 56
The Impact of Diabetes Mellitus and Prior Myocardial Infarction on Mortality From All Causes and From Coronary Heart Disease in Men
 Journal of the American College of Cardiology Vol. 40, No. 5, 2002 2002 by the American College of Cardiology Foundation ISSN 0735-1097/02/$22.00 Published by Elsevier Science Inc. PII S0735-1097(02)02044-2
Journal of the American College of Cardiology Vol. 40, No. 5, 2002 2002 by the American College of Cardiology Foundation ISSN 0735-1097/02/$22.00 Published by Elsevier Science Inc. PII S0735-1097(02)02044-2
Cottrell Memorial Lecture. Has Reversing Atherosclerosis Become the New Gold Standard in the Treatment of Cardiovascular Disease?
 Cottrell Memorial Lecture Has Reversing Atherosclerosis Become the New Gold Standard in the Treatment of Cardiovascular Disease? Stephen Nicholls MBBS PhD @SAHMRI_Heart Disclosures Research support: AstraZeneca,
Cottrell Memorial Lecture Has Reversing Atherosclerosis Become the New Gold Standard in the Treatment of Cardiovascular Disease? Stephen Nicholls MBBS PhD @SAHMRI_Heart Disclosures Research support: AstraZeneca,
Kathryn M. Rexrode, MD, MPH. Assistant Professor. Division of Preventive Medicine Brigham and Women s s Hospital Harvard Medical School
 Update: Hormones and Cardiovascular Disease in Women Kathryn M. Rexrode, MD, MPH Assistant Professor Division of Preventive Medicine Brigham and Women s s Hospital Harvard Medical School Overview Review
Update: Hormones and Cardiovascular Disease in Women Kathryn M. Rexrode, MD, MPH Assistant Professor Division of Preventive Medicine Brigham and Women s s Hospital Harvard Medical School Overview Review
Risk Factors for Heart Disease
 Risk Factors for Heart Disease Risk Factors we cannot change (Age, Gender, Family History) Risk Factors we can change (modifiable) Smoking Blood pressure Cholesterol Diabetes Inactivity Overweight Stress
Risk Factors for Heart Disease Risk Factors we cannot change (Age, Gender, Family History) Risk Factors we can change (modifiable) Smoking Blood pressure Cholesterol Diabetes Inactivity Overweight Stress
Lifetime clinical and economic benefits of statin-based LDL lowering in the 20-year Followup of the West of Scotland Coronary Prevention Study
 Lifetime clinical and economic benefits of statin-based LDL lowering in the 20-year Followup of the West of Scotland Coronary Prevention Study Harvey White Green Lane Cardiovascular Service and Cardiovascular
Lifetime clinical and economic benefits of statin-based LDL lowering in the 20-year Followup of the West of Scotland Coronary Prevention Study Harvey White Green Lane Cardiovascular Service and Cardiovascular
Long-term prognostic value of N-Terminal Pro-Brain Natriuretic Peptide (NT-proBNP) changes within one year in patients with coronary heart disease
 Long-term prognostic value of N-Terminal Pro-Brain Natriuretic Peptide (NT-proBNP) changes within one year in patients with coronary heart disease D. Dallmeier 1, D. Rothenbacher 2, W. Koenig 1, H. Brenner
Long-term prognostic value of N-Terminal Pro-Brain Natriuretic Peptide (NT-proBNP) changes within one year in patients with coronary heart disease D. Dallmeier 1, D. Rothenbacher 2, W. Koenig 1, H. Brenner
Dyslipedemia New Guidelines
 Dyslipedemia New Guidelines New ACC/AHA Prevention Guidelines on Blood Cholesterol November 12, 2013 Mohammed M Abd El Ghany Professor of Cardiology Cairo Universlty 1 1 0 Cholesterol Management Pharmacotherapy
Dyslipedemia New Guidelines New ACC/AHA Prevention Guidelines on Blood Cholesterol November 12, 2013 Mohammed M Abd El Ghany Professor of Cardiology Cairo Universlty 1 1 0 Cholesterol Management Pharmacotherapy
Guidelines on cardiovascular risk assessment and management
 European Heart Journal Supplements (2005) 7 (Supplement L), L5 L10 doi:10.1093/eurheartj/sui079 Guidelines on cardiovascular risk assessment and management David A. Wood 1,2 * 1 Cardiovascular Medicine
European Heart Journal Supplements (2005) 7 (Supplement L), L5 L10 doi:10.1093/eurheartj/sui079 Guidelines on cardiovascular risk assessment and management David A. Wood 1,2 * 1 Cardiovascular Medicine
Elevated Risk of Cardiovascular Disease Prior to Clinical Diagnosis of Type 2 Diabetes
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Elevated Risk of Cardiovascular Disease Prior to Clinical Diagnosis of Type 2 Diabetes FRANK B. HU, MD 1,2,3 MEIR J. STAMPFER,
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Elevated Risk of Cardiovascular Disease Prior to Clinical Diagnosis of Type 2 Diabetes FRANK B. HU, MD 1,2,3 MEIR J. STAMPFER,
