Emmanouil S. Brilakis 1{, Joseph P. McConnell 2, Ryan J. Lennon 3, Ahmad A. Elesber 1, Jeffrey G. Meyer 2, and Peter B. Berger 4 * Introduction
|
|
|
- Alfred Kelly
- 5 years ago
- Views:
Transcription
1 European Heart Journal (2005) 26, doi: /eurheartj/ehi010 Clinical research Association of lipoprotein-associated phospholipase A2 levels with coronary artery disease risk factors, angiographic coronary artery disease, and major adverse events at follow-up Emmanouil S. Brilakis 1{, Joseph P. McConnell 2, Ryan J. Lennon 3, Ahmad A. Elesber 1, Jeffrey G. Meyer 2, and Peter B. Berger 4 * 1 Division of Cardiovascular Diseases, Department of Internal Medicine, Mayo Clinic, 200 First Street SW, Rochester, MN 55905, USA 2 Department of Laboratory Medicine and Pathology, Mayo Clinic, Rochester, MN, USA 3 Division of Biostatistics, Mayo Clinic, Rochester, MN, USA 4 Division of Cardiovascular Diseases, Duke Clinical Research Institute, Durham, NC 27715, USA Received 20 April 2004; revised 1 August 2004; accepted 3 September 2004; online publish-ahead-of-print 29 November 2004 See page 107 for the editorial comment on this article (doi: /eurheartj/ehi042) KEYWORDS Lipoprotein-associated phospholipase A2; C-reactive protein; Acute myocardial infarction; Coronary disease Aims We aimed to evaluate the association of lipoprotein-associated phospholipase A2 (Lp-PLA2) with coronary artery disease (CAD) risk factors, with the severity of angiographic CAD, and with the incidence of major adverse events. Methods and results We measured Lp-PLA2 levels in 504 consecutive patients undergoing clinically indicated coronary angiography. Mean age was years and 38% were women. The mean (+SD) Lp-PLA2 level (ng/ml) was Lp-PLA2 levels correlated with male gender, LDL, HDL, and total cholesterol, fibrinogen, and creatinine. Lp-PLA2 levels correlated with the extent of angiographic CAD on univariate but not on multivariable analysis. During a median follow-up of 4.0 years, 72 major adverse events occurred in 61 of 466 (13%) contacted patients (20 deaths, 14 myocardial infarctions, 28 coronary revascularizations, and 10 strokes). Higher Lp-PLA2 levels were associated with a greater risk of events: the hazard ratio per SD was 1.28 (95% CI , P ¼ 0.009), and remained significant after adjusting for clinical and lipid variables and C-reactive protein. Conclusion Higher Lp-PLA2 levels were associated with a higher incidence of major adverse events at follow-up, independently of traditional CAD risk factors and C-reactive protein. Introduction Lipoprotein-associated phospholipase A2 (Lp-PLA2) is a 50-kDalton enzyme that belongs to the A2 phospholipase * Corresponding author. Tel: þ ; fax: þ address: berger.peter@duke.edu { Present address: University of Texas Southwestern Medical School, 5323 Harry Hines Blvd, Dallas, TX 75216, USA superfamily. 1 Lp-PLA2 is produced by macrophages and lymphocytes and 80% of it circulates bound, mainly to LDL. 2 Whether Lp-PLA2 is predominantly proatherogenic or anti-atherogenic is controversial. Most evidence from animal 3 and human 2 5 studies suggests it is pro-atherogenic. The first aim of our study was to examine the association between Lp-PLA2 and: (i) traditional and emerging coronary artery disease (CAD) risk factors: age, gender, European Heart Journal vol. 26 no. 2 & The European Society of Cardiology 2004; all rights reserved.
2 138 E.S. Brilakis et al. smoking, hypertension, obesity, total, high-density lipoprotein (HDL), and low-density lipoprotein (LDL) cholesterol, triglycerides, and homocysteine; (ii) the presence of an acute coronary syndrome; (iii) the presence and extent of angiographic CAD; and (iv) the incidence of major adverse events at follow-up. The second aim was to examine the impact on those associations when other risk factors, such as clinical and lipid parameters and C-reactive protein (CRP) were included in multivariable analyses. Methods Patient population The population included 504 patients (97% Caucasian), aged years, undergoing clinically-indicated coronary angiography at our institution between June 1998 and January Patients were excluded if they had diabetes mellitus, smoking history.50 pack-years, history of organ transplantation, pregnancy, prior coronary revascularization, bleeding disorders, blood transfusion within 30 days, HIV infection, renal failure, or prior chest radiation therapy. The most frequent indications for angiography were acute coronary syndrome (34%), an abnormal nuclear imaging study (25%), and dyspnoea upon exertion (27%). The 504 patients represent.90% of patients eligible for this study during the enrolment period (the remaining patients refused to participate). The study was approved by our Institutional Review Board, and all subjects provided written informed consent. Four hundred and sixty-six patients (92.5%) were contacted by a follow-up questionnaire or by telephone in September The remaining 38 patients either refused to participate in the follow-up (18, 47%) or could not be contacted (20, 53%). The medical records of the patients who had an event were obtained and reviewed in order to ascertain the type of the event or the cause of death. Acute coronary syndromes and stroke Patients were classified as having unstable angina (UA) if they had new-onset chest pain or if they had a significant unexplained change in the pattern of stable angina (such as increased frequency, intensity, or duration, or decreased response to nitrates) in the previous 2 months. Patients were defined as having an acute myocardial infarction (AMI) if they had cardiac marker elevation [total creatinine kinase (CK) more than 3 the upper limit of normal, or cardiac troponin (T) more than the upper limit of normal] in association with chest pain or ischaemic electrocardiographic changes. Stroke was defined as a new neurological defect persisting for.24 h (CT or MRI documentation was available in 9 of 10 patients). Angiographic analysis Coronary angiograms were analysed according to the segmental classification proposed by the Coronary Artery Surgery Study (CASS) investigators. 6 The maximum-diameter stenosis in each of 27 coronary artery segments was assessed with hand-held callipers or visual analysis. Angiograms were analysed blinded to risk factors and biochemical analyses. The extent of CAD was quantified as follows: normal coronaries (smooth arteries with no stenosis or stenosis,10%), mild disease (reduction in luminal diameter between 10% and 50%), single-vessel disease (.50% luminal diameter stenosis in one coronary artery or its major branches), two-vessel coronary artery disease (.50% stenoses in two coronary arteries), and three-vessel disease (.50% stenoses in three coronary arteries). Parameter definitions The body mass index (BMI) was calculated by dividing the patient s weight in kilograms by the square of the patient s height in metres. Patients were classified as normal weight (BMI ), overweight (BMI ), and obese (BMI 30). Patients were considered to be hypertensive if their blood pressure was.140/90 mmhg, or if they were being treated with antihypertensive medications. Major adverse events consisted of any of the following: death, AMI, coronary revascularization, or stroke. Blood collection and biochemical analyses Blood was collected in EDTA-treated tubes and divided into aliquots for measurement of plasma risk factors. Fibrinogen was measured using immunoturbidimetric methods on a Roche COBAS MIRA system. Lipids (total cholesterol, triglycerides, and HDL cholesterol) were measured using standard automated enzymatic methods on a Roche COBAS MIRA system. LDL cholesterol was calculated as total cholesterol minus HDL cholesterol and 20% of the triglyceride level (all expressed in mg/dl). Total plasma homocysteine was measured by high performance liquid chromatography following reduction of the disulfide bonds with Tris (2-carboxyethyl) phosphine hydrochloride and derivatization with SBD-F (7-fluoro-2-oxa-1, 3-diazole-4-sulfonate). Cysteamine was used as an internal standard. CRP was measured using a sensitive latex particle-enhanced immunoturbidimetric assay on a Hitachi 912 automated analyser, using reagents from Kamiya Biomedical Company. The CRP assay was sensitive to 0.15 mg/l and was standardized against the IFCC/BCR/CAP CRM 470 CRP references. Lp-PLA2 measurement Lp-PLA2 mass was measured in plasma aliquots that were collected at the time of enrolment and stored at 2708C using an enzyme-linked immunoassay (PLAC TM test, diadexus, Inc., CA, USA). 2,4 Samples were incubated in microtitre plate wells with immobilized monoclonal antibody (2C10) against Lp-PLA2. The enzyme was identified by a second monoclonal anti-lp-pla2 antibody (4B4) labelled with horseradish peroxidase. The standard was recombinant Lp-PLA2. The range of detection was ng/ml and the interassay coefficients of variation were 7.8% at 276 ng/ml, 6.1% at 257 ng/ml, and 13.5% at 105 ng/ml. There was no cross-reactivity with other A2 phospholipases. 2 All analyses were performed blinded to risk factors, biochemical, and clinical characteristics. The mean Lp-PLA2 value in our study was ng/ml, which was lower than the values reported from previous studies [mean Lp-PLA2 level was ng/ml in the West of Scotland Coronary Prevention Study (WOSCOPS) patients 4 ]. Although the antibodies used in our method were the same antibodies as used in previous studies, the recombinant Lp-PLA2 that we used as calibrator in the Lp-PLA2 assay had greater than five-fold more immunological action than the standard used previously. This accounts for the differences in recovered values in the patient samples (Robert Wolfert, diadexus Inc., personal communication).
3 Lipoprotein-associated phospholipase A2 levels 139 Statistical analysis Most continuous variables are summarized as mean + standard deviation. Variables with heavily skewed distributions (CRP, homocysteine, triglycerides, and creatinine) are reported as medians, with first and third quartiles in parentheses. Discrete variables are presented as frequencies and group percentages. The association of continuous variables with the extent of CAD (none, mild, one-, two-, or three-vessel disease) was tested using a linear contrast in association with one-way analysis-of-variance. The Armitage trend test was used to assess the association between categorical variables and the extent of CAD. Differences in distribution between other groups were tested using one-way analysis of variance or the Kruskal Wallis test. Spearman s correlation coefficient was used to assess linear relationships between continuous variables. Multiple regression models were used to estimate conditional relationships. The covariates used in the logistic models for CAD and Cox proportional hazards models for incidence of major adverse events were age, gender, smoking history, hypertension, total and HDL cholesterol, triglycerides, and CRP. Heavily skewed variables were logarithmically transformed for use in these models. The proportional hazards assumption was satisfied for both Lp-PLA2 and log(crp). Linearity was assessed for the continuous variables in logistic and Cox regression models by the use of generalized additive models. Splines were fitted and the fitted results, plus point-wise 95% confidence intervals, were plotted. In this way the linearity was assessed visually, by evaluating whether a straight line would fit through the confidence limits. All hypothesis tests were two-tailed with a 0.05 Type I error rate. Results Patient characteristics Table 1 summarizes the study population characteristics. Mean age was years and 38% were women. Coronary angiography revealed normal coronaries in 122 patients (24%), mild disease in 111 patients (22%), and one-, two-, and three-vessel disease in 85 (17%), 80 (16%), and 106 (21%) patients, respectively. As expected, patients with significant CAD were more likely to be male, older, and to have a history of hyperlipidaemia, hypertension, or myocardial infarction (Table 1). Patients with significant CAD also had a higher mean creatinine, LDL cholesterol, fibrinogen, and Lp-PLA2, and lower HDL cholesterol. Mean Lp-PLA2 level was ng/ml, and its distribution is shown in Figure 1. Lp-PLA2 in acute coronary syndromes Of the 504 patients, 169 had an acute coronary syndrome: 41 had an AMI and 128 had UA. Lp-PLA2 levels were similar in patients with or without an acute coronary syndrome (Table 2). In contrast, median CRP was significantly higher in AMI patients (Table 2). Therefore, analyses of the correlation between CRP and the extent of angiographic CAD were performed in only the 463 patients who did not have an AMI at the time of study enrolment (Tables 1, 3, and 4). Associations of Lp-PLA2 Lp-PLA2 was significantly higher in men and was positively associated with creatinine, total and LDL cholesterol, and fibrinogen, and was negatively associated with HDL (Tables 3 and 4). It was not significantly associated with age, BMI, current smoking, hypertension, systolic or diastolic blood pressure, triglycerides, homocysteine, or CRP. CRP correlated with age, gender (higher in women), history of hypertension, BMI, systolic blood pressure, total cholesterol, LDL cholesterol, triglycerides, and fibrinogen, but not with homocysteine or HDL cholesterol (Tables 3 and 4). Lp-PLA2 and angiographic CAD Lp-PLA2 levels were higher in patients with more extensive angiographic CAD, even when AMI patients were excluded (Table 1). However, after adjusting for clinical and lipid variables (age, gender, smoking, hypertension, total and HDL cholesterol, triglycerides, and CRP), Lp-PLA2 was not independently predictive of angiographic CAD. CRP levels did not have a statistically significant association with angiographic CAD on either univariate (Table 1) or multivariable analysis (OR ¼ 1.13 per standard deviation, P ¼ 0.16). Lp-PLA2 and major adverse events During a median follow-up of 4.0 years (interquartile range years), 72 major adverse events occurred in 61 of 466 patients (the Kaplan Meier estimated event rate was 3.2% at 1 year and 10% at 4 years): 20 patients died (6 cardiac deaths), 14 had a myocardial infarction, 26 underwent coronary revascularization (15 percutaneous intervention only, 9 coronary artery bypass surgery only, and 2 with both), and 10 had a stroke. Seven patients had two events and two had three (one patient had a myocardial infarction, percutaneous coronary intervention and coronary artery bypass grafting surgery, and one had a myocardial infarction, a stroke, and eventually died). On univariate analysis, higher levels of both Lp-PLA2 and CRP (log-transformed) were associated with the higher incidence of events: the hazard ratio (HR) per standard deviation was 1.28 and 1.40, respectively (Table 5). Figure 2 depicts the incidence of major adverse events in the study population over time, classified according to Lp-PLA2 levels (tertiles), suggesting that individuals in the lowest tertile had fewer events during the follow-up period than those in the upper two tertiles. Cox proportional hazard models were developed to examine the association of Lp-PLA2 with events. Those models included Lp-PLA2, age, gender, smoking history, hypertension, total and HDL cholesterol, triglycerides, and log-crp. Both Lp-PLA2 and log-crp were independent predictors of major adverse events (HR per standard deviation 1.30 and 1.34, respectively) (Table 5).
4 Table 1 Clinical characteristics of the study population, classified according to the extent of CAD at angiography All patients (n ¼ 504) No CAD (n ¼ 122) Mild CAD (n ¼ 111) One-vessel CAD (n ¼ 85) Two-vessel CAD (n ¼ 80) Three-vessel CAD (n ¼ 106) Age, years ,0.001 Female (%) 192 (38) 76 (62) 55 (50) 22 (26) 18 (23) 21 (20),0.001 Hypertension (%) 232 (46) 39 (32) 50 (45) 42 (49) 46 (58) 55 (52),0.001 Current smoking (%) 40 (8) 8 (7) 9 (8) 12 (14) 7 (9) 4 (4) 0.58 History of AMI (%) 77 (15) 3 (2) 6 (5) 16 (19) 20 (25) 32 (30),0.001 History of CHF (%) 59 (12) 25 (20) 19 (17) 6 (7) 3 (4) 6 (6),0.001 Family history of CAD (%) 128 (25) 27 (22) 24 (22) 20 (24) 28 (35) 29 (27) 0.10 History of hyperlipidaemia (%) 286 (57) 44 (36) 52 (47) 45 (53) 66 (83) 79 (75),0.001 BMI, kg/m Creatinine, mmol/l a 97 (88 115) 97 (88 106) 97 (80 106) 106 (88 115) 106 (88 115) 106 (97 115),0.001 Total cholesterol, mmol/l Triglycerides, mmol/l a 1.7 ( ) 1.5 ( ) 1.8 ( ) 1.8 ( ) 1.7 ( ) 1.8 ( ) HDL cholesterol, mmol/l ,0.001 LDL cholesterol, mmol/l Homocysteine, mmol/l a 8.8 ( ) 8.6 ( ) 8.6 ( ) 8.7 ( ) 8.8 ( ) 9.6 ( ) Fibrinogen, mg/dl ,0.001 CRP, mg/l a 2.9 ( ) 3.2 ( ) 2.5 ( ) 2.9 ( ) 2.9 ( ) 3.0 ( ) 0.27 Lp-PLA2, ng/ml Plus minus values are mean + standard deviation. a Median (interquartile range). CHF, congestive heart failure. P-value 140 E.S. Brilakis et al.
5 Lipoprotein-associated phospholipase A2 levels 141 and oxidatively modified non-esterified fatty acid, which may promote atherogenesis by functioning as monocyte chemoattractants and by inducing endothelial leukocyte adhesion molecules. 7,8 Lp-PLA2 and angiographic CAD Figure 1 When LDL cholesterol was substituted for total cholesterol and fibrinogen was added to the model, the effect of Lp-PLA2 remained statistically significant (HR per standard deviation 1.25, 95% CI , P ¼ 0.03), whereas the effect of log-crp became non-statistically significant (HR per standard deviation 1.10, 95% CI , P ¼ 0.58). Discussion Distribution of Lp-PLA2 levels in the study population. Our study demonstrates that Lp-PLA2: (i) is associated with gender, total LDL, and HDL cholesterol, fibrinogen, and creatinine but not with other traditional or emerging CAD risk factors such as age, hypertension, obesity, and CRP; (ii) is not increased in AMI patients, in contrast to acute-phase reactants such as CRP and fibrinogen; (iii) is associated with angiographic CAD on univariate but not multivariable analysis; and (iv) is associated with the incidence of major adverse events at follow-up independently of clinical and lipid risk factors and CRP. Associations of Lp-PLA2 Lp-PLA2 levels were measured in both men and women in this study; two previous such studies included either men (WOSCOPS sub-study), 4 or women, 5 but not both. In our study, Lp-PLA2 levels were higher in men, but the difference was no longer significant after adjusting for HDL, which was higher in women. The correlation between Lp-PLA2 and LDL observed in both the current and the WOSCOPS study was expected, since 80% of Lp-PLA2 is associated with LDL. 2 Similar to the WOSCOPS study, Lp-PLA2 was not associated with age or BMI. Both Lp-PLA2 and CRP were associated with lipid parameters (total cholesterol and LDL cholesterol; Tables 3 and 4). In contrast to what was reported in the WOSCOPS study where there was a very weak correlation, Lp-PLA2 had a significant negative association with HDL cholesterol in our study (Table 4). CRP was associated with obesity and AMI, whereas Lp-PLA2 was not. The difference in those associations suggests that Lp-PLA2 may act on the atherosclerotic process through different pathophysiological mechanisms than CRP. Lp-PLA2 cleaves oxidized phosphatidylcholine on LDL in the vessel wall to produce the bioactive lipids lysophosphatidylcholine Caslake et al. 2 demonstrated that Lp-PLA2 levels were higher in 94 patients with CAD than in 54 controls. The association persisted after adjusting for LDL and HDL cholesterol, smoking, and systolic blood pressure. However, this study had several important limitations: it was relatively small, only men were included, and coronary angiography was performed in only one-third of the patients, so that a possible association between Lp-PLA2 levels and the severity of CAD could not be explored. In our population, Lp-PLA2 was higher in patients with CAD than those without CAD, as also found by Caslake et al. However, in our study the association between Lp-PLA2 and CAD was not independent of other CAD risk factors. Compared with the study by Caslake et al., 2 our study differed in the following three ways: (i) a larger number of patients (504 vs. 148); (ii) data on the severity and the extent of CAD, rather than just the presence of CAD; and (iii) inclusion of a significant proportion of women (192 of 504, 38%). In the current study CRP did not correlate with the angiographic extent of atherosclerosis. In the largest published study correlating CRP with the extent of angiographic CAD, the correlation was weak (Pearson s correlation coefficients ), but reached statistical significance because of the large sample size (n ¼ 2554). 9 Lp-PLA2 and major adverse events In our study, higher Lp-PLA2 levels were associated with a higher incidence of major adverse events independently of traditional CAD risk factors and CRP, a finding that is consistent with the recently reported results from three other studies. 4,10 In the WOSCOPS population (exclusively men), Lp-PLA2 was a predictor of coronary events independent of CRP, fibrinogen level, white cell count, age, systolic blood pressure, plasma triglycerides, HDL cholesterol, and LDL cholesterol levels (relative risk 1.18 per 1 standard deviation increase in Lp-PLA2, P ¼ 0.005). 4 In the Atherosclerosis Risk in Communities (ARIC) study apparently healthy middle-aged men and women were followed for 6 years: 609 individuals developed CAD and were compared with 741 randomly selected controls. In subjects with LDL cholesterol below the median (130 mg/dl), Lp-PLA2 and CRP were both significantly and independently associated with CHD in fully adjusted models. Similarly, in a post hoc analysis of the MONICA (MONItoring trends and determinants of CArdiovascular disease) Augsburg cohort, Lp-PLA2 levels were significantly higher in the 97 of the 934 apparently healthy men aged who had suffered a coronary event during 14 years of follow-up (data presented at the
6 142 E.S. Brilakis et al. Table 2 Lp-PLA2, CRP, and fibrinogen levels in patients with and without an acute coronary syndrome AMI (n ¼ 41) UA (n ¼ 128) Non-ACS (n ¼ 335) P-value Lp-PLA2, ng/ml CRP, mg/l a 13.4 ( ) 3.2 ( ) 2.2 ( ),0.001 Fibrinogen, mg/dl ,0.001 Total cholesterol, mmol/l Triglycerides, mmol/l a 1.7 ( ) 1.7 ( ) 1.7 ( ) 0.74 HDL cholesterol, mmol/l ,0.001 LDL cholesterol, mmol/l Plus minus values are mean + standard deviation. a Median (interquartile range). ACS, acute coronary syndrome. Other abbreviations as in text and Table 1. Table 3 Relationship between Lp-PLA2 and CRP levels with gender, current smoking, hypertension, and BMI Lp-PLA2 a (n ¼ 504) Lp-PLA2 a (n ¼ 463 without AMI) CRP b (n ¼ 463 without AMI) Men ( ) Women ( ) P ,0.001 Current smoker ( ) Current non-smoker ( ) P Hypertension ( ) No hypertension ( ) P BMI, ( ) BMI ( ) BMI ( ) P ,0.001 a ng/ml. b mg/l, median, IQR. Abbreviations as in text and Table 1. Table 4 Relationship between Lp-PLA2, CRP, and other CAD risk factors Lp-PLA2 (n ¼ 504) Lp-PLA2 (n ¼ 463 without AMI) CRP (n ¼ 463 without AMI) Spearman s rho P Spearman s rho P Spearman s rho P Age BMI ,0.001 Systolic blood pressure Diastolic blood pressure Creatinine Total cholesterol 0.25, , Triglycerides HDL cholesterol 20.26, , LDL cholesterol 0.32, , Homocysteine Fibrinogen ,0.001 CRP Lp-PLA Abbreviations as in text.
7 Lipoprotein-associated phospholipase A2 levels 143 Table 5 Univariate and multivariable association between different baseline parameters and the incidence of major adverse events at follow-up Parameter (SD) Univariate HR (95% CI) P Multivariable HR (95% CI) a P Age (10.8 years) 1.59 ( ) ( ) Male gender 1.18 ( ) ( ) 0.38 Smoking history 1.22 ( ) ( ) 0.49 Hypertension 1.49 ( ) ( ) 0.20 Total cholesterol (1.17 mmol/l) 0.92 ( ) ( ) 0.08 HDL cholesterol (0.37 mmol/l) 0.82 ( ) ( ) 0.78 log triglycerides (0.01 mmol/l) 1.17 ( ) ( ) 0.11 log-crp (1.32 mg/l) 1.40 ( ) ( ) 0.02 Lp-PLA2 (92.8 ng/ml) 1.28 ( ) ( ) 0.01 a HRs were adjusted for Lp-PLA2, age, gender, smoking history, hypertension, total and HDL cholesterol, triglycerides, and log-crp. CI, confidence intervals. Other abbreviations as in text. Figure 2 Incidence of major adverse events in the study population (n ¼ 466) classified according to Lp-PLA2 levels (tertiles) American Heart Association Scientific Session in November 2003). In contrast, Blake et al. 5 did not find an independent association between Lp-PLA2 and cardiac events in a nested case control study of apparently healthy women from the Women s Health study, with 123 cases, 40% of which were stroke. Similar to the WOSCOPS, ARIC, and MONICA studies, in our study higher Lp-PLA2 levels were associated with a higher incidence of major adverse events independently of other CAD risk factors and CRP, suggesting that Lp-PLA2 may help in risk stratification of those patients. In contrast to the ARIC study, the predictive role of Lp-PLA2 appeared to be similar in patients with high or low LDL. The discordance between the weak association of Lp-PLA2 with angiographic CAD and the stronger association of Lp-PLA2 with major adverse events has also been observed with CRP, which was only weakly associated with coronary artery calcification but was strongly associated with clinical events in one study. 11 As specific inhibitors of Lp-PLA2 have been developed and shown to be orally active in animal models, 12 Lp-PLA2 has the potential to be a therapeutic target in patients with cardiovascular disease. 11 Limitations Measurements of Lp-PLA2 were performed on frozen rather than fresh plasma. We demonstrated that Lp-PLA2 is stable in samples stored at 48C or 2708C for at least 7 days and that repeated freeze thaw cycles (three cycles) did not reduce Lp-PLA2 concentration. The effect of long-term storage is yet to be addressed. Patients in this study were all referred for cardiac catheterization; therefore, our control patients may not be representative of the population-based controls believed to be free of atherosclerosis. However, the use of patients with normal coronary arteries on angiography also has strengths over using population-based controls, because the presence of subclinical coronary disease
8 144 E.S. Brilakis et al. can be excluded. Follow-up was obtained in 92.5% of patients and it is possible that some events were not detected. The incidence of major adverse events was low (13%), limiting the power of our study, but we were still able to detect a significant association between Lp-PLA2 and events. Conclusions Lp-PLA2 was associated with different risk factors for CAD than CRP. Higher Lp-PLA2 levels were associated with more severe angiographic CAD on univariate but not on multivariable analysis. Higher Lp-PLA2 levels were associated with a higher incidence of major adverse events during follow-up, independently of traditional CAD risk factors and CRP. Acknowledgements Supported in part by research grants from diadexus Inc., South San Francisco, CA, USA and Interleukin Genetics, Waltham, MA, USA. References 1. Tew DG, Southan C, Rice SQ et al. Purification, properties, sequencing, and cloning of a lipoprotein-associated, serine-dependent phospholipase involved in the oxidative modification of low-density lipoproteins. Arterioscler Thromb Vasc Biol 1996;16: Caslake MJ, Packard CJ, Suckling KE et al. Lipoprotein-associated phospholipase A(2), platelet-activating factor acetylhydrolase: a potential new risk factor for coronary artery disease. Atherosclerosis 2000;150: Hakkinen T, Luoma JS, Hiltunen MO et al. Lipoprotein-associated phospholipase A(2), platelet-activating factor acetylhydrolase, is expressed by macrophages in human and rabbit atherosclerotic lesions. Arterioscler Thromb Vasc Biol 1999;19: Packard CJ, O Reilly DS, Caslake MJ et al. Lipoprotein-associated phospholipase A2 as an independent predictor of coronary heart disease. West of Scotland Coronary Prevention Study Group. NEngl JMed2000;343: Blake GJ, Dada N, Fox JC et al. A prospective evaluation of lipoprotein-associated phospholipase A(2) levels and the risk of future cardiovascular events in women. J Am Coll Cardiol 2001;38: Killip T. The National Heart, Lung, and Blood Institute Coronary Artery Surgery Study (CASS). Circulation 1981;63(Suppl. 1): Tselepis AD, Chapman JM. Inflammation, bioactive lipids and atherosclerosis: potential roles of a lipoprotein-associated phospholipase A2, platelet activating factor-acetylhydrolase. Atheroscler Suppl 2002;3: MacPhee CH, Moores KE, Boyd HF et al. Lipoprotein-associated phospholipase A2, platelet-activating factor acetylhydrolase, generates two bioactive products during the oxidation of low-density lipoprotein: use of a novel inhibitor. Biochem J 1999; 338: Zebrack JS, Muhlestein JB, Horne BD, Anderson JL. C-reactive protein and angiographic coronary artery disease: independent and additive predictors of risk in subjects with angina. J Am Coll Cardiol 2002; 39: Ballantyne CM, Hoogeveen RC, Bang H et al. Lipoprotein-associated phospholipase A2, high-sensitivity C-reactive protein, and risk for incident coronary heart disease in middle-aged men and women in the Atherosclerosis Risk in Communities (ARIC) study. Circulation 2004;109: MacPhee CH. Lipoprotein-associated phospholipase A2: a potential new risk factor for coronary artery disease and a therapeutic target. Curr Opin Pharmacol 2001;1: Boyd HF, Fell SC, Hickey DM et al. Potent, orally active inhibitors of lipoprotein-associated phospholipase A(2): 1-(biphenylmethylamidoalkyl)-pyrimidones. Bioorg Med Chem Lett 2002;12:51 55.
Lipoprotein-Associated Phospholipase A2 Is an Independent Predictor of Incident Coronary Heart Disease in an Apparently Healthy Older Population
 Journal of the American College of Cardiology Vol. 51, No. 9, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.10.048
Journal of the American College of Cardiology Vol. 51, No. 9, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.10.048
High-sensitivity Troponin T Predicts Recurrent Cardiovascular Events in Patients with Stable Coronary Heart Disease: KAROLA Study 8 Year FU
 ESC Congress 2011 Paris, France, August 27-31 KAROLA Session: Prevention: Are biomarkers worth their money? Abstract # 84698 High-sensitivity Troponin T Predicts Recurrent Cardiovascular Events in Patients
ESC Congress 2011 Paris, France, August 27-31 KAROLA Session: Prevention: Are biomarkers worth their money? Abstract # 84698 High-sensitivity Troponin T Predicts Recurrent Cardiovascular Events in Patients
LIPOPROTEIN-ASSOCIATED PHOSPHOLIPASE A 2 : EFFECTS OF LOW DENSITY LIPOPROTEIN APHERESIS
 LIPOPROTEIN-ASSOCIATED PHOSPHOLIPASE A 2 : EFFECTS OF LOW DENSITY LIPOPROTEIN APHERESIS Patrick M. Moriarty, M.D., FACP, Director, Atherosclerosis and LDL-Apheresis Center, University of Kansas Medical
LIPOPROTEIN-ASSOCIATED PHOSPHOLIPASE A 2 : EFFECTS OF LOW DENSITY LIPOPROTEIN APHERESIS Patrick M. Moriarty, M.D., FACP, Director, Atherosclerosis and LDL-Apheresis Center, University of Kansas Medical
ORIGINAL INVESTIGATION. C-Reactive Protein Concentration and Incident Hypertension in Young Adults
 ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS
 GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS Table of Contents List of authors pag 2 Supplemental figure I pag 3 Supplemental figure II pag 4 Supplemental
GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS Table of Contents List of authors pag 2 Supplemental figure I pag 3 Supplemental figure II pag 4 Supplemental
Relationship between body mass index, coronary disease extension and clinical outcomes in patients with acute coronary syndrome
 Relationship between body mass index, coronary disease extension and clinical outcomes in patients with acute coronary syndrome Helder Dores, Luís Bronze Carvalho, Ingrid Rosário, Sílvio Leal, Maria João
Relationship between body mass index, coronary disease extension and clinical outcomes in patients with acute coronary syndrome Helder Dores, Luís Bronze Carvalho, Ingrid Rosário, Sílvio Leal, Maria João
Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic
 Supplementary Information The title of the manuscript Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic stroke Xin-Wei He 1, Wei-Ling Li 1, Cai Li
Supplementary Information The title of the manuscript Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic stroke Xin-Wei He 1, Wei-Ling Li 1, Cai Li
A: Epidemiology update. Evidence that LDL-C and CRP identify different high-risk groups
 A: Epidemiology update Evidence that LDL-C and CRP identify different high-risk groups Women (n = 27,939; mean age 54.7 years) who were free of symptomatic cardiovascular (CV) disease at baseline were
A: Epidemiology update Evidence that LDL-C and CRP identify different high-risk groups Women (n = 27,939; mean age 54.7 years) who were free of symptomatic cardiovascular (CV) disease at baseline were
Enzyme Immunoassay for the Quantitative Determination of Lp-PLA 2 in Human Plasma and Serum.
 PLAC Test ELISA Kit Enzyme Immunoassay for the Quantitative Determination of Lp-PLA 2 in Human Plasma and Serum 90123 www.plactest.com Diadexus, Inc. 349 Oyster Point Blvd. South San Francisco, CA 94080
PLAC Test ELISA Kit Enzyme Immunoassay for the Quantitative Determination of Lp-PLA 2 in Human Plasma and Serum 90123 www.plactest.com Diadexus, Inc. 349 Oyster Point Blvd. South San Francisco, CA 94080
Division of Cardiovascular Medicine, Jichi Medical University Saitama Medical Center, Japan
 Association between continuously elevated C-reactive protein and restenosis after percutaneous coronary intervention using drug-eluting stent in angina patients Division of Cardiovascular Medicine, Jichi
Association between continuously elevated C-reactive protein and restenosis after percutaneous coronary intervention using drug-eluting stent in angina patients Division of Cardiovascular Medicine, Jichi
Central pressures and prediction of cardiovascular events in erectile dysfunction patients
 Central pressures and prediction of cardiovascular events in erectile dysfunction patients N. Ioakeimidis, K. Rokkas, A. Angelis, Z. Kratiras, M. Abdelrasoul, C. Georgakopoulos, D. Terentes-Printzios,
Central pressures and prediction of cardiovascular events in erectile dysfunction patients N. Ioakeimidis, K. Rokkas, A. Angelis, Z. Kratiras, M. Abdelrasoul, C. Georgakopoulos, D. Terentes-Printzios,
(n=6279). Continuous variables are reported as mean with 95% confidence interval and T1 T2 T3. Number of subjects
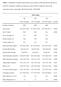 Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Table S1. Characteristics associated with frequency of nut consumption (full entire sample; Nn=4,416).
 Table S1. Characteristics associated with frequency of nut (full entire sample; Nn=4,416). Daily nut Nn= 212 Weekly nut Nn= 487 Monthly nut Nn= 1,276 Infrequent or never nut Nn= 2,441 Sex; n (%) men 52
Table S1. Characteristics associated with frequency of nut (full entire sample; Nn=4,416). Daily nut Nn= 212 Weekly nut Nn= 487 Monthly nut Nn= 1,276 Infrequent or never nut Nn= 2,441 Sex; n (%) men 52
LDL cholesterol (p = 0.40). However, higher levels of HDL cholesterol (> or =1.5 mmol/l [60 mg/dl]) were associated with less progression of CAC
![LDL cholesterol (p = 0.40). However, higher levels of HDL cholesterol (> or =1.5 mmol/l [60 mg/dl]) were associated with less progression of CAC LDL cholesterol (p = 0.40). However, higher levels of HDL cholesterol (> or =1.5 mmol/l [60 mg/dl]) were associated with less progression of CAC](/thumbs/88/116891773.jpg) Am J Cardiol (2004);94:729-32 Relation of degree of physical activity to coronary artery calcium score in asymptomatic individuals with multiple metabolic risk factors M. Y. Desai, et al. Ciccarone Preventive
Am J Cardiol (2004);94:729-32 Relation of degree of physical activity to coronary artery calcium score in asymptomatic individuals with multiple metabolic risk factors M. Y. Desai, et al. Ciccarone Preventive
Autonomic nervous system, inflammation and preclinical carotid atherosclerosis in depressed subjects with coronary risk factors
 Autonomic nervous system, inflammation and preclinical carotid atherosclerosis in depressed subjects with coronary risk factors Carmine Pizzi 1 ; Lamberto Manzoli 2, Stefano Mancini 3 ; Gigliola Bedetti
Autonomic nervous system, inflammation and preclinical carotid atherosclerosis in depressed subjects with coronary risk factors Carmine Pizzi 1 ; Lamberto Manzoli 2, Stefano Mancini 3 ; Gigliola Bedetti
Low fractional diastolic pressure in the ascending aorta increased the risk of coronary heart disease
 (2002) 16, 837 841 & 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Low fractional diastolic pressure in the ascending aorta increased the risk
(2002) 16, 837 841 & 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Low fractional diastolic pressure in the ascending aorta increased the risk
Correlation of novel cardiac marker
 Correlation of novel cardiac marker and mortality in EGAT population. Soluble ST2 hscrp Poh Chanyavanich, MD SukitYamwong, MD Piyamitr Sritara, MD Ramathibodi hospital Background hscrp - the most widely
Correlation of novel cardiac marker and mortality in EGAT population. Soluble ST2 hscrp Poh Chanyavanich, MD SukitYamwong, MD Piyamitr Sritara, MD Ramathibodi hospital Background hscrp - the most widely
Small dense low-density lipoprotein is a risk for coronary artery disease in an urban Japanese cohort: The Suita study
 Small dense low-density lipoprotein is a risk for coronary artery disease in an urban Japanese cohort: The Suita study Hidenori Arai 1, Yoshihiro Kokubo 2, Makoto Watanabe 2, Tatsuya Sawamura 3, Tomonori
Small dense low-density lipoprotein is a risk for coronary artery disease in an urban Japanese cohort: The Suita study Hidenori Arai 1, Yoshihiro Kokubo 2, Makoto Watanabe 2, Tatsuya Sawamura 3, Tomonori
The Framingham Coronary Heart Disease Risk Score
 Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
USING NON -TRADITIONAL RISK MARKERS IN ASSESSING CV RISK
 USING NON -TRADITIONAL RISK MARKERS IN ASSESSING CV RISK JAMES M FALKO MD PROFESSOR OF MEDICINE UNIVERSITY OF COLORADO Adapted from: Rader D. N Engl J Med. 2000 hs-crp (mg/l) 6 5 4 3 2 1 *p
USING NON -TRADITIONAL RISK MARKERS IN ASSESSING CV RISK JAMES M FALKO MD PROFESSOR OF MEDICINE UNIVERSITY OF COLORADO Adapted from: Rader D. N Engl J Med. 2000 hs-crp (mg/l) 6 5 4 3 2 1 *p
The inhibition of CETP: From simply raising HDL-c to promoting cholesterol efflux and lowering of atherogenic lipoproteins Prof Dr J Wouter Jukema
 The inhibition of CETP: From simply raising HDL-c to promoting cholesterol efflux and lowering of atherogenic lipoproteins Prof Dr J Wouter Jukema Dept Cardiology, Leiden University Medical Center, Leiden,
The inhibition of CETP: From simply raising HDL-c to promoting cholesterol efflux and lowering of atherogenic lipoproteins Prof Dr J Wouter Jukema Dept Cardiology, Leiden University Medical Center, Leiden,
Impact of coronary atherosclerotic burden on clinical presentation and prognosis of patients with coronary artery disease
 Impact of coronary atherosclerotic burden on clinical presentation and prognosis of patients with coronary artery disease Gjin Ndrepepa, Tomohisa Tada, Massimiliano Fusaro, Lamin King, Martin Hadamitzky,
Impact of coronary atherosclerotic burden on clinical presentation and prognosis of patients with coronary artery disease Gjin Ndrepepa, Tomohisa Tada, Massimiliano Fusaro, Lamin King, Martin Hadamitzky,
Supplementary Online Content
 Supplementary Online Content Leibowitz M, Karpati T, Cohen-Stavi CJ, et al. Association between achieved low-density lipoprotein levels and major adverse cardiac events in patients with stable ischemic
Supplementary Online Content Leibowitz M, Karpati T, Cohen-Stavi CJ, et al. Association between achieved low-density lipoprotein levels and major adverse cardiac events in patients with stable ischemic
Tracking a Killer Molecule
 Tracking a Killer Molecule Mercodia Oxidized LDL ELISA www.mercodia.com Mercodia Oxidized LDL ELISA products Product Catalog No Kit size Oxidized LDL ELISA 10-1143-01 96 wells Oxidized LDL competitive
Tracking a Killer Molecule Mercodia Oxidized LDL ELISA www.mercodia.com Mercodia Oxidized LDL ELISA products Product Catalog No Kit size Oxidized LDL ELISA 10-1143-01 96 wells Oxidized LDL competitive
Clinical Trial Synopsis TL-OPI-518, NCT#
 Clinical Trial Synopsis, NCT# 00225264 Title of Study: A Double-Blind, Randomized, Comparator-Controlled Study in Subjects With Type 2 Diabetes Mellitus Comparing the Effects of Pioglitazone HCl vs Glimepiride
Clinical Trial Synopsis, NCT# 00225264 Title of Study: A Double-Blind, Randomized, Comparator-Controlled Study in Subjects With Type 2 Diabetes Mellitus Comparing the Effects of Pioglitazone HCl vs Glimepiride
Low ALT Levels Independently Associated with 22-Year All-Cause Mortality Among Coronary Heart Disease Patients
 Low ALT Levels Independently Associated with 22-Year All-Cause Mortality Among Coronary Heart Disease Patients N. Peltz-Sinvani, MD 1,4,R.Klempfner,MD 2,4, E. Ramaty, MD 1,4,B.A.Sela,PhD 3,4,I.Goldenberg,MD
Low ALT Levels Independently Associated with 22-Year All-Cause Mortality Among Coronary Heart Disease Patients N. Peltz-Sinvani, MD 1,4,R.Klempfner,MD 2,4, E. Ramaty, MD 1,4,B.A.Sela,PhD 3,4,I.Goldenberg,MD
Trial to Reduce. Aranesp* Therapy. Cardiovascular Events with
 Trial to Reduce Cardiovascular Events with Aranesp* Therapy John J.V. McMurray, Hajime Uno, Petr Jarolim, Akshay S. Desai, Dick de Zeeuw, Kai-Uwe Eckardt, Peter Ivanovich, Andrew S. Levey, Eldrin F. Lewis,
Trial to Reduce Cardiovascular Events with Aranesp* Therapy John J.V. McMurray, Hajime Uno, Petr Jarolim, Akshay S. Desai, Dick de Zeeuw, Kai-Uwe Eckardt, Peter Ivanovich, Andrew S. Levey, Eldrin F. Lewis,
JUPITER NEJM Poll. Panel Discussion: Literature that Should Have an Impact on our Practice: The JUPITER Study
 Panel Discussion: Literature that Should Have an Impact on our Practice: The Study Kaiser COAST 11 th Annual Conference Maui, August 2009 Robert Blumberg, MD, FACC Ralph Brindis, MD, MPH, FACC Primary
Panel Discussion: Literature that Should Have an Impact on our Practice: The Study Kaiser COAST 11 th Annual Conference Maui, August 2009 Robert Blumberg, MD, FACC Ralph Brindis, MD, MPH, FACC Primary
Cho et al., 2009 Journal of Cardiology (2009), 54:
 Endothelial Dysfunction, Increased Carotid Artery Intima-media Thickness and Pulse Wave Velocity, and Increased Level of Inflammatory Markers are Associated with Variant Angina Cho et al., 2009 Journal
Endothelial Dysfunction, Increased Carotid Artery Intima-media Thickness and Pulse Wave Velocity, and Increased Level of Inflammatory Markers are Associated with Variant Angina Cho et al., 2009 Journal
ARIC Manuscript Proposal # PC Reviewed: 2/10/09 Status: A Priority: 2 SC Reviewed: Status: Priority:
 ARIC Manuscript Proposal # 1475 PC Reviewed: 2/10/09 Status: A Priority: 2 SC Reviewed: Status: Priority: 1.a. Full Title: Hypertension, left ventricular hypertrophy, and risk of incident hospitalized
ARIC Manuscript Proposal # 1475 PC Reviewed: 2/10/09 Status: A Priority: 2 SC Reviewed: Status: Priority: 1.a. Full Title: Hypertension, left ventricular hypertrophy, and risk of incident hospitalized
Biomarkers in Vascular Inflammation (hscrp, Lp-PLA 2 )
 Biomarkers in Vascular Inflammation (hscrp, Lp-PLA 2 ) Inflammation; Current evidence supports a central role in all phases of the atherosclerosis from lesion initiation through to progression and, ultimately,
Biomarkers in Vascular Inflammation (hscrp, Lp-PLA 2 ) Inflammation; Current evidence supports a central role in all phases of the atherosclerosis from lesion initiation through to progression and, ultimately,
Lipoprotein (a) Disclosures 2/20/2013. Lipoprotein (a): Should We Measure? Should We Treat? Health Diagnostic Laboratory, Inc. No other disclosures
 Lipoprotein (a): Should We Measure? Should We Treat? Joseph P. McConnell, Ph.D. DABCC Health Diagnostic Laboratory Inc. Baptist Health South Florida Eleventh Annual Cardiovascular Disease Prevention International
Lipoprotein (a): Should We Measure? Should We Treat? Joseph P. McConnell, Ph.D. DABCC Health Diagnostic Laboratory Inc. Baptist Health South Florida Eleventh Annual Cardiovascular Disease Prevention International
Behind LDL: The Metabolism of ApoB, the Essential Apolipoprotein in LDL and VLDL
 Behind LDL: The Metabolism of ApoB, the Essential Apolipoprotein in LDL and VLDL Sung-Joon Lee, PhD Division of Food Science Institute of Biomedical Science and Safety Korea University Composition of Lipoproteins:
Behind LDL: The Metabolism of ApoB, the Essential Apolipoprotein in LDL and VLDL Sung-Joon Lee, PhD Division of Food Science Institute of Biomedical Science and Safety Korea University Composition of Lipoproteins:
Supplement materials:
 Supplement materials: Table S1: ICD-9 codes used to define prevalent comorbid conditions and incident conditions Comorbid condition ICD-9 code Hypertension 401-405 Diabetes mellitus 250.x Myocardial infarction
Supplement materials: Table S1: ICD-9 codes used to define prevalent comorbid conditions and incident conditions Comorbid condition ICD-9 code Hypertension 401-405 Diabetes mellitus 250.x Myocardial infarction
egfr > 50 (n = 13,916)
 Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
MEDICAL POLICY SUBJECT: INFLAMMATORY MARKERS OF CORONARY ARTERY DISEASE RISK. POLICY NUMBER: CATEGORY: Laboratory Tests
 MEDICAL POLICY PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
Diabetes and Occult Coronary Artery Disease
 Diabetes and Occult Coronary Artery Disease Mun K. Hong, MD, FACC, FSCAI Director, Cardiac Catheterization Laboratory & Interventional Cardiology St. Luke s-roosevelt Hospital Center New York, New York
Diabetes and Occult Coronary Artery Disease Mun K. Hong, MD, FACC, FSCAI Director, Cardiac Catheterization Laboratory & Interventional Cardiology St. Luke s-roosevelt Hospital Center New York, New York
Marshall Tulloch-Reid, MD, MPhil, DSc, FACE Epidemiology Research Unit Tropical Medicine Research Institute The University of the West Indies, Mona,
 Marshall Tulloch-Reid, MD, MPhil, DSc, FACE Epidemiology Research Unit Tropical Medicine Research Institute The University of the West Indies, Mona, Jamaica At the end of this presentation the participant
Marshall Tulloch-Reid, MD, MPhil, DSc, FACE Epidemiology Research Unit Tropical Medicine Research Institute The University of the West Indies, Mona, Jamaica At the end of this presentation the participant
The JUPITER trial: What does it tell us? Alice Y.Y. Cheng, MD, FRCPC January 24, 2009
 The JUPITER trial: What does it tell us? Alice Y.Y. Cheng, MD, FRCPC January 24, 2009 Learning Objectives 1. Understand the role of statin therapy in the primary and secondary prevention of stroke 2. Explain
The JUPITER trial: What does it tell us? Alice Y.Y. Cheng, MD, FRCPC January 24, 2009 Learning Objectives 1. Understand the role of statin therapy in the primary and secondary prevention of stroke 2. Explain
10/17/16. Assessing cardiovascular risk through use of inflammation testing
 Assessing cardiovascular risk through use of inflammation testing Anthony L. Lyssy, DO Medical Director and Managing Partner Diamond Physicians Dallas, TX Response to Injury Hypothesis Injury Response
Assessing cardiovascular risk through use of inflammation testing Anthony L. Lyssy, DO Medical Director and Managing Partner Diamond Physicians Dallas, TX Response to Injury Hypothesis Injury Response
Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor
 Last Review Status/Date: September 2014 Page: 1 of 14 Description Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor acetylhydrolase, is an enzyme that hydrolyzes
Last Review Status/Date: September 2014 Page: 1 of 14 Description Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor acetylhydrolase, is an enzyme that hydrolyzes
Supplemental table 1. Dietary sources of protein among 2441 men from the Kuopio Ischaemic Heart Disease Risk Factor Study MEAT DAIRY OTHER ANIMAL
 ONLINE DATA SUPPLEMENT 1 SUPPLEMENTAL MATERIAL Pork Bacon Turkey Kidney Cream Cottage cheese Mutton and lamb Game (elk, reindeer) Supplemental table 1. Dietary sources of protein among 2441 men from the
ONLINE DATA SUPPLEMENT 1 SUPPLEMENTAL MATERIAL Pork Bacon Turkey Kidney Cream Cottage cheese Mutton and lamb Game (elk, reindeer) Supplemental table 1. Dietary sources of protein among 2441 men from the
CRP and fibrinogen imply clinical outcome of patients with type-2 diabetes. and coronary artery disease
 CRP and fibrinogen imply clinical outcome of patients with type-2 diabetes and coronary artery disease Marijan Bosevski 1, *, Golubinka Bosevska 1, Lily Stojanovska 2, Vasso Apostolopoulos 2, * 1 University
CRP and fibrinogen imply clinical outcome of patients with type-2 diabetes and coronary artery disease Marijan Bosevski 1, *, Golubinka Bosevska 1, Lily Stojanovska 2, Vasso Apostolopoulos 2, * 1 University
CLINICAL OUTCOME Vs SURROGATE MARKER
 CLINICAL OUTCOME Vs SURROGATE MARKER Statin Real Experience Dr. Mostafa Sherif Senior Medical Manager Pfizer Egypt & Sudan Objective Difference between Clinical outcome and surrogate marker Proper Clinical
CLINICAL OUTCOME Vs SURROGATE MARKER Statin Real Experience Dr. Mostafa Sherif Senior Medical Manager Pfizer Egypt & Sudan Objective Difference between Clinical outcome and surrogate marker Proper Clinical
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Clinical perspective It was recently discovered that small RNAs, called micrornas, circulate freely and stably in human plasma. This finding has sparked interest in the potential
SUPPLEMENTAL MATERIAL Clinical perspective It was recently discovered that small RNAs, called micrornas, circulate freely and stably in human plasma. This finding has sparked interest in the potential
Correlation between plasma lipoprotein-associated phospholipase A 2 and peripheral arterial disease
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 1451-1455, 2013 Correlation between plasma lipoprotein-associated phospholipase A 2 and peripheral arterial disease SHUAI-BING LI, FAN YANG, LI JING, JUAN MA, YA-DAN
EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 1451-1455, 2013 Correlation between plasma lipoprotein-associated phospholipase A 2 and peripheral arterial disease SHUAI-BING LI, FAN YANG, LI JING, JUAN MA, YA-DAN
sphingotest vr-hgh Risk Prediction of Incident Cardiovascular Disease
 sphingotest vr-hgh Risk Prediction of Incident Cardiovascular Disease Human Growth Hormone as Vascular Risk Biomarker sphingotec offers the vascular risk human Growth Hormone biomarker (vr-hgh) for the
sphingotest vr-hgh Risk Prediction of Incident Cardiovascular Disease Human Growth Hormone as Vascular Risk Biomarker sphingotec offers the vascular risk human Growth Hormone biomarker (vr-hgh) for the
Inflammation plays a major role in atherosclerosis, 1 and
 Soluble P-Selectin and the Risk of Future Cardiovascular Events Paul M. Ridker, MD; Julie E. Buring, ScD; Nader Rifai, PhD Background P-selectin, a cell-surface adhesion molecule involved in leukocyte
Soluble P-Selectin and the Risk of Future Cardiovascular Events Paul M. Ridker, MD; Julie E. Buring, ScD; Nader Rifai, PhD Background P-selectin, a cell-surface adhesion molecule involved in leukocyte
Fasting or non fasting?
 Vascular harmony Robert Chilton Professor of Medicine University of Texas Health Science Center Director of Cardiac Catheterization labs Director of clinical proteomics Which is best to measure Lower continues
Vascular harmony Robert Chilton Professor of Medicine University of Texas Health Science Center Director of Cardiac Catheterization labs Director of clinical proteomics Which is best to measure Lower continues
Supplemental Table 1. Standardized Serum Creatinine Measurements. Supplemental Table 3. Sensitivity Analyses with Additional Mortality Outcomes.
 SUPPLEMENTAL MATERIAL Supplemental Table 1. Standardized Serum Creatinine Measurements Supplemental Table 2. List of ICD 9 and ICD 10 Billing Codes Supplemental Table 3. Sensitivity Analyses with Additional
SUPPLEMENTAL MATERIAL Supplemental Table 1. Standardized Serum Creatinine Measurements Supplemental Table 2. List of ICD 9 and ICD 10 Billing Codes Supplemental Table 3. Sensitivity Analyses with Additional
CVD risk assessment using risk scores in primary and secondary prevention
 CVD risk assessment using risk scores in primary and secondary prevention Raul D. Santos MD, PhD Heart Institute-InCor University of Sao Paulo Brazil Disclosure Honoraria for consulting and speaker activities
CVD risk assessment using risk scores in primary and secondary prevention Raul D. Santos MD, PhD Heart Institute-InCor University of Sao Paulo Brazil Disclosure Honoraria for consulting and speaker activities
Know Your Number Aggregate Report Single Analysis Compared to National Averages
 Know Your Number Aggregate Report Single Analysis Compared to National s Client: Study Population: 2242 Population: 3,000 Date Range: 04/20/07-08/08/07 Version of Report: V6.2 Page 2 Study Population Demographics
Know Your Number Aggregate Report Single Analysis Compared to National s Client: Study Population: 2242 Population: 3,000 Date Range: 04/20/07-08/08/07 Version of Report: V6.2 Page 2 Study Population Demographics
Serum Creatinine and Blood Urea Nitrogen Levels in Patients with Coronary Artery Disease
 Serum Creatinine and Blood Urea Nitrogen Levels in Patients with Coronary Artery Disease MAK Akanda 1, KN Choudhury 2, MZ Ali 1, MK Kabir 3, LN Begum 4, LA Sayami 1 1 National Institute of Cardiovascular
Serum Creatinine and Blood Urea Nitrogen Levels in Patients with Coronary Artery Disease MAK Akanda 1, KN Choudhury 2, MZ Ali 1, MK Kabir 3, LN Begum 4, LA Sayami 1 1 National Institute of Cardiovascular
300 Biomed Environ Sci, 2018; 31(4):
 300 Biomed Environ Sci, 2018; 31(4): 300-305 Letter to the Editor Combined Influence of Insulin Resistance and Inflammatory Biomarkers on Type 2 Diabetes: A Population-based Prospective Cohort Study of
300 Biomed Environ Sci, 2018; 31(4): 300-305 Letter to the Editor Combined Influence of Insulin Resistance and Inflammatory Biomarkers on Type 2 Diabetes: A Population-based Prospective Cohort Study of
Review of guidelines for management of dyslipidemia in diabetic patients
 2012 international Conference on Diabetes and metabolism (ICDM) Review of guidelines for management of dyslipidemia in diabetic patients Nan Hee Kim, MD, PhD Department of Internal Medicine, Korea University
2012 international Conference on Diabetes and metabolism (ICDM) Review of guidelines for management of dyslipidemia in diabetic patients Nan Hee Kim, MD, PhD Department of Internal Medicine, Korea University
Risk Stratification of ACS Patients. Frans Van de Werf, MD, PhD University of Leuven, Belgium
 Risk Stratification of ACS Patients Frans Van de Werf, MD, PhD University of Leuven, Belgium Which type of ACS patients are we talking about to day? 4/14/2011 STEMI and NSTEMI in the NRMI registry from
Risk Stratification of ACS Patients Frans Van de Werf, MD, PhD University of Leuven, Belgium Which type of ACS patients are we talking about to day? 4/14/2011 STEMI and NSTEMI in the NRMI registry from
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Hospital and 1-year outcome after acute myocardial infarction in patients with diabetes mellitus and hypertension
 (2003) 17, 665 670 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Hospital and 1-year outcome after acute myocardial infarction in patients with
(2003) 17, 665 670 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Hospital and 1-year outcome after acute myocardial infarction in patients with
Andrejs Kalvelis 1, MD, PhD, Inga Stukena 2, MD, Guntis Bahs 3 MD, PhD & Aivars Lejnieks 4, MD, PhD ABSTRACT INTRODUCTION. Riga Stradins University
 CARDIOVASCULAR RISK FACTORS ORIGINAL ARTICLE Do We Correctly Assess the Risk of Cardiovascular Disease? Characteristics of Risk Factors for Cardiovascular Disease Depending on the Sex and Age of Patients
CARDIOVASCULAR RISK FACTORS ORIGINAL ARTICLE Do We Correctly Assess the Risk of Cardiovascular Disease? Characteristics of Risk Factors for Cardiovascular Disease Depending on the Sex and Age of Patients
Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk. Original Policy Date
 MP 2.04.23 Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 2.04.23 Measurement of Lipoprotein-Associated Phospholipase A2 (Lp-PLA2) in the Assessment of Cardiovascular Risk Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review
Decreased Inflammatory Markers in Diabetic Patients with Angiographically Proved Coronary Artery Disease after 18 Months of Statins Therapy
 Decreased Inflammatory Markers in Diabetic Patients with Angiographically Proved Coronary Artery Disease after 18 Months of Statins Therapy DANIEL LIGHEZAN, ROXANA BUZAS, CORINA SERBAN, IOANA SUCEAVA University
Decreased Inflammatory Markers in Diabetic Patients with Angiographically Proved Coronary Artery Disease after 18 Months of Statins Therapy DANIEL LIGHEZAN, ROXANA BUZAS, CORINA SERBAN, IOANA SUCEAVA University
Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis
 CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
STABILITY Stabilization of Atherosclerotic plaque By Initiation of darapladib TherapY. Harvey D White on behalf of The STABILITY Investigators
 STABILITY Stabilization of Atherosclerotic plaque By Initiation of darapladib TherapY Harvey D White on behalf of The STABILITY Investigators Lipoprotein- associated Phospholipase A 2 (Lp-PLA 2 ) activity:
STABILITY Stabilization of Atherosclerotic plaque By Initiation of darapladib TherapY Harvey D White on behalf of The STABILITY Investigators Lipoprotein- associated Phospholipase A 2 (Lp-PLA 2 ) activity:
Supplementary Note Details of the patient populations studied Strengths and weakness of the study
 Supplementary Note Details of the patient populations studied TVD and NCA patients. Patients were recruited to the TVD (triple vessel disease) group who had significant coronary artery disease (defined
Supplementary Note Details of the patient populations studied TVD and NCA patients. Patients were recruited to the TVD (triple vessel disease) group who had significant coronary artery disease (defined
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases
 Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Long-term prognostic value of N-Terminal Pro-Brain Natriuretic Peptide (NT-proBNP) changes within one year in patients with coronary heart disease
 Long-term prognostic value of N-Terminal Pro-Brain Natriuretic Peptide (NT-proBNP) changes within one year in patients with coronary heart disease D. Dallmeier 1, D. Rothenbacher 2, W. Koenig 1, H. Brenner
Long-term prognostic value of N-Terminal Pro-Brain Natriuretic Peptide (NT-proBNP) changes within one year in patients with coronary heart disease D. Dallmeier 1, D. Rothenbacher 2, W. Koenig 1, H. Brenner
There are many ways to lower triglycerides in humans: Which are the most relevant for pancreatitis and for CV risk?
 There are many ways to lower triglycerides in humans: Which are the most relevant for pancreatitis and for CV risk? Michael Davidson M.D. FACC, Diplomate of the American Board of Lipidology Professor,
There are many ways to lower triglycerides in humans: Which are the most relevant for pancreatitis and for CV risk? Michael Davidson M.D. FACC, Diplomate of the American Board of Lipidology Professor,
Supplementary Online Content
 Supplementary Online Content Pedersen SB, Langsted A, Nordestgaard BG. Nonfasting mild-to-moderate hypertriglyceridemia and risk of acute pancreatitis. JAMA Intern Med. Published online November 7, 2016.
Supplementary Online Content Pedersen SB, Langsted A, Nordestgaard BG. Nonfasting mild-to-moderate hypertriglyceridemia and risk of acute pancreatitis. JAMA Intern Med. Published online November 7, 2016.
Journal of the American College of Cardiology Vol. 36, No. 1, by the American College of Cardiology ISSN /00/$20.
 Journal of the American College of Cardiology Vol. 36, No. 1, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00680-X Lack
Journal of the American College of Cardiology Vol. 36, No. 1, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00680-X Lack
Supplementary table 1 Demographic and clinical characteristics of participants by paraoxonase-1 (PON-1) gene polymorphisms
 Supplementary table 1 Demographic and clinical characteristics of participants by paraoxonase-1 (PON-1) gene polymorphisms QQ QR/RR n = 36 n = 80 Men (%) 20 (55) 54 (67) 0.216 Age (years) 57 ± 10 56 ±
Supplementary table 1 Demographic and clinical characteristics of participants by paraoxonase-1 (PON-1) gene polymorphisms QQ QR/RR n = 36 n = 80 Men (%) 20 (55) 54 (67) 0.216 Age (years) 57 ± 10 56 ±
 Biomarkers in Acute Cardiac Disease Samir Arnaout, M.D.FESC Associate Professor of Medicine Internal Medicine i & Cardiology American University of Beirut Time course of the appearance of various markers
Biomarkers in Acute Cardiac Disease Samir Arnaout, M.D.FESC Associate Professor of Medicine Internal Medicine i & Cardiology American University of Beirut Time course of the appearance of various markers
sad EFFECTIVE DATE: POLICY LAST UPDATED:
 Medical Coverage Policy Measurement of Small Low Density Lipoprotein Particles sad EFFECTIVE DATE: 02 16 2010 POLICY LAST UPDATED: 10 15 2013 OVERVIEW Lipoprotein-associated phospholipase A2 (Lp-PLA2),
Medical Coverage Policy Measurement of Small Low Density Lipoprotein Particles sad EFFECTIVE DATE: 02 16 2010 POLICY LAST UPDATED: 10 15 2013 OVERVIEW Lipoprotein-associated phospholipase A2 (Lp-PLA2),
Effects of a dietary intervention to reduce saturated fat on markers of inflammation and cardiovascular disease.
 Michael Garshick, MD PGY-1 Columbia University Medical Center Effects of a dietary intervention to reduce saturated fat on markers of inflammation and cardiovascular disease. Study Purpose and Rationale:
Michael Garshick, MD PGY-1 Columbia University Medical Center Effects of a dietary intervention to reduce saturated fat on markers of inflammation and cardiovascular disease. Study Purpose and Rationale:
The Diabetes Link to Heart Disease
 The Diabetes Link to Heart Disease Anthony Abe DeSantis, MD September 18, 2015 University of WA Division of Metabolism, Endocrinology and Nutrition Oswald Toosweet Case #1 68 yo M with T2DM Diagnosed DM
The Diabetes Link to Heart Disease Anthony Abe DeSantis, MD September 18, 2015 University of WA Division of Metabolism, Endocrinology and Nutrition Oswald Toosweet Case #1 68 yo M with T2DM Diagnosed DM
The TNT Trial Is It Time to Shift Our Goals in Clinical
 The TNT Trial Is It Time to Shift Our Goals in Clinical Angioplasty Summit Luncheon Symposium Korea Assoc Prof David Colquhoun 29 April 2005 University of Queensland, Wesley Hospital, Brisbane, Australia
The TNT Trial Is It Time to Shift Our Goals in Clinical Angioplasty Summit Luncheon Symposium Korea Assoc Prof David Colquhoun 29 April 2005 University of Queensland, Wesley Hospital, Brisbane, Australia
Supplementary Online Content
 Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
SUPPLEMENTAL MATERIAL. Supplemental Methods. Duke CAD Index
 SUPPLEMENTAL MATERIAL Supplemental Methods Duke CAD Index The Duke CAD index, originally developed by David F. Kong, is an angiographic score that hierarchically assigns prognostic weights (0-100) based
SUPPLEMENTAL MATERIAL Supplemental Methods Duke CAD Index The Duke CAD index, originally developed by David F. Kong, is an angiographic score that hierarchically assigns prognostic weights (0-100) based
Clinical Trial Synopsis TL-OPI-516, NCT#
 Clinical Trial Synopsis, NCT#00225277 Title of Study: A Double-Blind, Randomized, Comparator-Controlled Study in Subjects With Type 2 Diabetes Mellitus Comparing the Effects of Pioglitazone HCl Versus
Clinical Trial Synopsis, NCT#00225277 Title of Study: A Double-Blind, Randomized, Comparator-Controlled Study in Subjects With Type 2 Diabetes Mellitus Comparing the Effects of Pioglitazone HCl Versus
Heart Rate in Patients with Coronary Artery Disease - the Lower the Better? An Analysis from the Treating to New Targets (TNT) trial
 Heart Rate in Patients with Coronary Artery Disease - the Lower the Better? An Analysis from the Treating to New Targets (TNT) trial Sripal Bangalore, MD, MHA, Chuan-Chuan Wun, PhD, David A DeMicco, PharmD,
Heart Rate in Patients with Coronary Artery Disease - the Lower the Better? An Analysis from the Treating to New Targets (TNT) trial Sripal Bangalore, MD, MHA, Chuan-Chuan Wun, PhD, David A DeMicco, PharmD,
and Restenosis Yangsoo Jang, MD, PhD. Yonsei University College of Medicine
 PPAR- Agonist and In-Stent Restenosis Yangsoo Jang, MD, PhD. Yonsei University College of Medicine Peroxisome Proliferator- activated Receptors (PPAR) Lipid-activated transcription factors : => regulating
PPAR- Agonist and In-Stent Restenosis Yangsoo Jang, MD, PhD. Yonsei University College of Medicine Peroxisome Proliferator- activated Receptors (PPAR) Lipid-activated transcription factors : => regulating
The Clinical Unmet need in the patient with Diabetes and ACS
 The Clinical Unmet need in the patient with Diabetes and ACS Professor Kausik Ray (UK) BSc(hons), MBChB, MD, MPhil, FRCP (lon), FRCP (ed), FACC, FESC, FAHA Diabetes is a global public health challenge
The Clinical Unmet need in the patient with Diabetes and ACS Professor Kausik Ray (UK) BSc(hons), MBChB, MD, MPhil, FRCP (lon), FRCP (ed), FACC, FESC, FAHA Diabetes is a global public health challenge
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Weintraub WS, Grau-Sepulveda MV, Weiss JM, et al. Comparative
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Weintraub WS, Grau-Sepulveda MV, Weiss JM, et al. Comparative
Assessment of vitamin D levels in patients with acute coronary syndrome
 ORIGINAL ARTICLE East J Med 21(4): 178-182, 2016 Assessment of vitamin D levels in patients with acute coronary syndrome Hakki Simsek and Naci Babat * Yuzuncu Yil University, Faculty of Medicine, Cardiology
ORIGINAL ARTICLE East J Med 21(4): 178-182, 2016 Assessment of vitamin D levels in patients with acute coronary syndrome Hakki Simsek and Naci Babat * Yuzuncu Yil University, Faculty of Medicine, Cardiology
Treatment of Cardiovascular Risk Factors. Kevin M Hayes D.O. F.A.C.C. First Coast Heart and Vascular Center
 Treatment of Cardiovascular Risk Factors Kevin M Hayes D.O. F.A.C.C. First Coast Heart and Vascular Center Disclosures: None Objectives What do risk factors tell us What to check and when Does treatment
Treatment of Cardiovascular Risk Factors Kevin M Hayes D.O. F.A.C.C. First Coast Heart and Vascular Center Disclosures: None Objectives What do risk factors tell us What to check and when Does treatment
C-Reactive Protein and Your Heart
 C-Reactive Protein and Your Heart By: James L. Holly, MD Inflammation is the process by which the body responds to injury. Laboratory evidence and findings at autopsy studies suggest that the inflammatory
C-Reactive Protein and Your Heart By: James L. Holly, MD Inflammation is the process by which the body responds to injury. Laboratory evidence and findings at autopsy studies suggest that the inflammatory
Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association
 Measurement of Lipoprotein-Associated Phospholipase Page 1 of 11 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Measurement of Lipoprotein-Associated Phospholipase
Measurement of Lipoprotein-Associated Phospholipase Page 1 of 11 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Measurement of Lipoprotein-Associated Phospholipase
ATEF ELBAHRY,FACA,FICA,MISCP,FVBWG.
 Hyperglycemia and Coronary Events: where is the link? ATEF ELBAHRY,FACA,FICA,MISCP,FVBWG. Cardiovascular (CV) disease is the primary complication of diabetes ~65% of deaths are due to CV disease Coronary
Hyperglycemia and Coronary Events: where is the link? ATEF ELBAHRY,FACA,FICA,MISCP,FVBWG. Cardiovascular (CV) disease is the primary complication of diabetes ~65% of deaths are due to CV disease Coronary
Long-Term Complications of Diabetes Mellitus Macrovascular Complication
 Long-Term Complications of Diabetes Mellitus Macrovascular Complication Sung Hee Choi MD, PhD Professor, Seoul National University College of Medicine, SNUBH, Bundang Hospital Diabetes = CVD equivalent
Long-Term Complications of Diabetes Mellitus Macrovascular Complication Sung Hee Choi MD, PhD Professor, Seoul National University College of Medicine, SNUBH, Bundang Hospital Diabetes = CVD equivalent
Ticagrelor compared with clopidogrel in patients with acute coronary syndromes the PLATO trial
 compared with clopidogrel in patients with acute coronary syndromes the PLATO trial August 30, 2009 at 08.00 CET PLATO background In NSTE-ACS and STEMI, current guidelines recommend 12 months aspirin and
compared with clopidogrel in patients with acute coronary syndromes the PLATO trial August 30, 2009 at 08.00 CET PLATO background In NSTE-ACS and STEMI, current guidelines recommend 12 months aspirin and
The New England Journal of Medicine AS AN INDEPENDENT PREDICTOR OF CORONARY HEART DISEASE. phospholipase A 2
 LIPOPROTEIN-ASSOCIATED PHOSPHOLIPASE AS AN INDEPENDENT PREDICTOR OF CORONARY HEART DISEASE CHRIS J. PACKARD, D.SC., DENIS S.J. O REILLY, M.D., MURIEL J. CASLAKE, PH.D., ALEX D. MCMAHON, PH.D., IAN FORD,
LIPOPROTEIN-ASSOCIATED PHOSPHOLIPASE AS AN INDEPENDENT PREDICTOR OF CORONARY HEART DISEASE CHRIS J. PACKARD, D.SC., DENIS S.J. O REILLY, M.D., MURIEL J. CASLAKE, PH.D., ALEX D. MCMAHON, PH.D., IAN FORD,
Lipid Risk Factors (Novel) in Risk Assessment and Management of Cardiovascular Disease
 Lipid Risk Factors (Novel) in Risk Assessment and Management of Cardiovascular Disease Policy Number: Original Effective Date: MM.02.013 02/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO;
Lipid Risk Factors (Novel) in Risk Assessment and Management of Cardiovascular Disease Policy Number: Original Effective Date: MM.02.013 02/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO;
Clinical Investigation and Reports
 Clinical Investigation and Reports Lipoprotein-Associated Phospholipase A 2, High-Sensitivity C-Reactive Protein, and Risk for Incident Coronary Heart Disease in Middle-Aged Men and Women in the Atherosclerosis
Clinical Investigation and Reports Lipoprotein-Associated Phospholipase A 2, High-Sensitivity C-Reactive Protein, and Risk for Incident Coronary Heart Disease in Middle-Aged Men and Women in the Atherosclerosis
John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam
 Latest Insights from the JUPITER Study John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam Inflammation, hscrp, and Vascular Prevention
Latest Insights from the JUPITER Study John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam Inflammation, hscrp, and Vascular Prevention
PATIENTS AND METHODS:
 BACKGROUND: Rheumatoid arthritis (RA) is a chronic systemic inflammatory disease characterized by erosive synovitis that involves peripheral joints and implicates an important influence in the quality
BACKGROUND: Rheumatoid arthritis (RA) is a chronic systemic inflammatory disease characterized by erosive synovitis that involves peripheral joints and implicates an important influence in the quality
Patient characteristics Intervention Comparison Length of followup
 ISCHAEMIA TESTING CHAPTER TESTING FOR MYCOCARDIAL ISCHAEMIA VERSUS NOT TESTING FOR MYOCARDIAL ISCHAEMIA Ref ID: 4154 Reference Wienbergen H, Kai GA, Schiele R et al. Actual clinical practice exercise ing
ISCHAEMIA TESTING CHAPTER TESTING FOR MYCOCARDIAL ISCHAEMIA VERSUS NOT TESTING FOR MYOCARDIAL ISCHAEMIA Ref ID: 4154 Reference Wienbergen H, Kai GA, Schiele R et al. Actual clinical practice exercise ing
Inflammation and and Heart Heart Disease in Women Inflammation and Heart Disease
 Inflammation and Heart Disease in Women Inflammation and Heart Disease What is the link between een inflammation and atherosclerotic disease? What is the role of biomarkers in predicting cardiovascular
Inflammation and Heart Disease in Women Inflammation and Heart Disease What is the link between een inflammation and atherosclerotic disease? What is the role of biomarkers in predicting cardiovascular
Clopidogrel Date: 15 July 2008
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription Sponsor/company: sanofi-aventis ClinicalTrials.gov
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription Sponsor/company: sanofi-aventis ClinicalTrials.gov
Inflammation as A Target for Therapy. Focus on Residual Inflammatory Risk
 ESC Rome Monday August 29, 2016 Inflammation as A Target for Therapy Focus on Residual Inflammatory Risk Paul M Ridker, MD Eugene Braunwald Professor of Medicine Harvard Medical School Director, Center
ESC Rome Monday August 29, 2016 Inflammation as A Target for Therapy Focus on Residual Inflammatory Risk Paul M Ridker, MD Eugene Braunwald Professor of Medicine Harvard Medical School Director, Center
The Impact of Smoking on Acute Ischemic Stroke
 Smoking The Impact of Smoking on Acute Ischemic Stroke Wei-Chieh Weng, M.D. Department of Neurology, Chang-Gung Memorial Hospital, Kee-Lung, Taiwan Smoking related mortality Atherosclerotic vascular disease
Smoking The Impact of Smoking on Acute Ischemic Stroke Wei-Chieh Weng, M.D. Department of Neurology, Chang-Gung Memorial Hospital, Kee-Lung, Taiwan Smoking related mortality Atherosclerotic vascular disease
Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor
 Last Review Status/Date: September 2015 Page: 1 of 14 Description Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor acetylhydrolase, is an enzyme that hydrolyzes
Last Review Status/Date: September 2015 Page: 1 of 14 Description Lipoprotein-associated phospholipase A2 (Lp-PLA2), also known as platelet-activating factor acetylhydrolase, is an enzyme that hydrolyzes
