Soft tissue reconstruction with the superior gluteal artery perforator f lap
|
|
|
- Naomi Robbins
- 6 years ago
- Views:
Transcription
1 Clin Plastic Surg 30 (2003) Soft tissue reconstruction with the superior gluteal artery perforator f lap Phillip N. Blondeel, MD, PhD*, Koenraad Van Landuyt, MD, Moustapha Hamdi, MD, Stan J. Monstrey, MD, PhD Department of Plastic and Reconstructive Surgery, University Hospital Gent, De Pintelaan 185, 2K12C, B-9000 Gent, Belgium Perforator flaps are one of the most recent developments in reconstructive microsurgery. In the last few years they have revolutionalized our opinions on flap harvesting. Perforator flaps are harvested from the same donor sites as the conventional myocutaneous flaps, but the goal is to harvest only a (sensory) skin and fat paddle. The underlying muscle that usually was harvested, completely or partially, with the skin and subcutaneous fat, with the thought that the muscle would protect the vascular pedicle, is split longitudinally in the direction of the muscle fibers. One or several transmuscular perforating vessels that provide blood flow to the subdermal plexus of the skin island are dissected from between the muscle fibers until larger axial vessels are reached. The perforator itself can be cut before entering the axial vessels if an anastomosis to small recipient vessels is preferred; generally, the main vessels are followed and cut further on to increase vessel diameter, pedicle length, and flexibility during shaping. By meticulous dissection, the motor nerves and the collateral blood circulation of the remaining muscle are carefully preserved so that the muscle s function is not affected. The superior gluteal artery perforator (SGAP) flap is the descendant of the traditional gluteus maximus myocutaneous flap [1]. The latter flap, based either on the superior or inferior gluteal artery, did not gain much popularity because of its drawbacks. Surgical * Corresponding author. address: phillip.blondeel@rug.ac.be (P.N. Blondeel). exposure of the donor vessels is difficult, the vascular pedicle is short, and the flap dissection is difficult and may result in injury to the adjacent sciatic nerve. Pain and paresthesias following exposure of the sciatic nerve after flap harvesting are disturbing complications. Partial resection of the gluteus maximus muscle can eventually result in weakness of muscle function in abduction and extension of the thigh, depending on the level of activities of the patient. Koshima et al [2] first described the pedicled SGAP flap for the use in pressure sore treatment. The flap was based on multiple perforators, including the parasacral perforators, which allowed only a limited transposition maneuver. Allen and Tucker [3] reported the use of the free SGAP flap in breast reconstruction. Shortly thereafter, our group reported on the use of the pedicled SGAP for sacral pressure sores [4]. This time, the flap was isolated on one single perforator which allowed a combination of transposition and rotation, and provided a much longer range of flap movement. In 1999, the sensory innervation of the flap was described and the advantages of the use of the flap as an alternative in breast reconstruction was reconfirmed [5,6]. Based on a single perforator, it is possible to raise skin flaps of up to 30 cm by 13 cm with a pedicle length of 6 cm to 10.5 cm, and leave behind an anatomically and functionally intact muscle [4,6]. Flap dimensions are limited by the possibility of primary closure of the donor site, rather than by vascularization of the flap. This article describes the indications for which we have been using the SGAP flap, the surgical technique to harvest the flap, the advantages, and disadvantages /03/$ see front matter D 2003 Elsevier Inc. All rights reserved. doi: /s (03)
2 372 P.N. Blondeel et al / Clin Plastic Surg 30 (2003) Flap harvesting: surgical technique The relatively constant anatomy of the superior gluteal artery and the small number of perforators that cross the fascia perpendicularly, make it easy to preoperatively identify the location of the perforators by unidirectional Doppler flowmetry. Preoperatively, the location where the superior gluteal artery exits the suprapiriform foramen is marked on the skin at the proximal one third of a line that connects the posterior superior iliac spine and the apex of the greater trochanter. The position of the piriform muscle is located by connecting the middle of a line between the posterior superior iliac spine and the coccyx with the superior edge of the greater trochanter of the femur (Fig.1A). The main perforators are localized by unidirectional Doppler flowmetry in an area above the piriform muscle, laterodistally to the exit point of the superior gluteal artery and parallel to the first line. A fusiform skin island is drawn over the perforators (Fig. 1B). In the treatment of pressure sores, triangular-shaped flaps can sometimes be used combined with V-Y advancement and closure. The axis of the skin island can be positioned in any direction over the identified perforators but will be strongly influenced by skin tension during donor site closure. This means that for larger flaps, a horizontal or slightly oblique (from mediocaudal to laterocranial) position is preferred (see Fig.1B). This allows easy closure, even with a certain amount of lifting of the buttock and without too much residual contour deformity. Specifically, in breast reconstruction, the slightly more horizontal-oblique positioning of the flap will provide a scar that can be completely hidden by normal underwear. Harvesting is performed with the patient in either the lateral decubitus or prone position, depending on the indication. Harvesting of the flap starts laterocranially. After incising the skin and the analog of Scarpa s fascia at this part of the body, the nervi clunii superiores can be identified at the superior edge of the flap, above the muscle fascia. If these nerves are large enough to be identified and dissected, they can be included in the flap. The number, course, and branching of these nerves are variable, and, in general, the more distally the flap is harvested, the greater the chance that the nerves have split into undetectable small side branches. Nevertheless, in cases where the nerve can be isolated, it can be dissected more cranially on top of the deep fascia, often accompanied by a small blood vessel. Above the crista iliaca, the sensory nerve pierces the deep fascia. The origin of these nerves is the posterior rami of the intercostal nerves from T12 to L2 [6]. Undermining of the flap and the search for the perforator starts at the most laterocranial part of the flap. At this point, the gluteus medius muscle should not be mistaken for the gluteus maximus muscle. The gluteus medius muscle can be discerned by the more vertical orientation of its fibers. After the superior border of the gluteus maximus muscle is reached, dissection proceeds above the muscle fascia parallel to the direction of the gluteus maximus muscle fibers. When the dissection approaches the area where the perforator pierces through the fascia, previously marked by the preoperative Doppler, the muscle fascia is incised and the dissection continues on top of the muscle. The individual perimysia that run parallel with the muscle fibers and connect with the overlying fascia are transected one by one. After a suitable perforator is encountered (the more lateral the perforator, the longer the pedicle), muscle fibers around it are split longitudinally to expose the perforator (Fig. 2A). Wide exposure and a bloodless dissection are two extremely important points in the dissection of any type of perforator flap; this is also true for the dissection of the SGAP flap. The muscle fibers of the gluteus maximus need to be split longitudinally, along the epimysium that embraces the perforating vessels, from the sacrum down to the distal tendinous part of the muscle just above the trochanter. This wide exposure permits easy dissection of the perforator and avoids working in a small hole with poor visibility. The muscle is split all the way down to its anterior surface. In the more anterior part, small motor branches are often observed that easily can be preserved because they are some distance from the perforator itself. After opening the muscle, the perforator can be seen running within the epimysium. The epimysium is cut at both sides parallel to the perforator, and all of the side branches are ligated carefully (Fig. 2B). Attention must also be paid to the small side branches on the backside of the perforator. Lifting the perforator with a vessel loop is helpful. Alternatively, the entire flap can be flipped laterally to obtain good exposure of the perforator from a medial point of view. The dissection continues down to the anterior fascia of the gluteus maximus muscle. This is a strong, and often thick, distinctive structure through which the vessels perforate. If the size and length of the perforators are acceptable at this point, the vessels can be cut if a free flap is harvested. More often, larger or longer vessels are preferred and dissection has to be continued below the anterior fascia. This fascia is opened, once again paying attention to wide exposure of this area (Fig. 2C). Soon, many large side branches will be encountered that come from all directions. After clearing off the loose fat tissue around these
3 P.N. Blondeel et al / Clin Plastic Surg 30 (2003) Fig. 1. (A) Markings of the anatomical landmarks and localization of the perforators. The dotted lines delineate the area where main perforators of the superior gluteal artery (SGA) can be expected. PIS, posterior iliac spine; TROCH, trochanter; X, location of a major perforator. (B) Positioning of the skin paddle in case of a free SGAP breast reconstruction.
4 374 P.N. Blondeel et al / Clin Plastic Surg 30 (2003) vessels, the main gluteal vessels are exposed. A decision has to be made about where to cut the vessels (in case of a free flap). Two points influence this. First, depending on the size of the recipient vessels, comparable vessel diameters will try to be obtained. Second, a segment of artery and vein without any side branches over a distance of 4 mm to 5 mm is identified to facilitate later microanastomoses. In the case of a pedicled flap, it must be decided if dissecting the area in front of the anterior fascia will add significantly more mobility to the flap. The plexus of side branches is often close to the apertura piriformis; ligating these branches only will devascularize the area even more, which precludes the use of a gluteus maximus muscle flap in a later phase. Donor site closure is started by undermining of the skin edges. Primarily, the distal skin flap is undermined to achieve a limited buttock lift. Undermining over the crista iliaca and trochanter is avoided, if possible, because this will interrupt important periostium-to-skin attachments and increase the risk of postoperative seroma formation. Deep sutures are placed on the superficial Scarpa-like fascia and skin closure is performed by a layer of resorbable subdermal stitches and 2-octyl cyanoacrylate (Dermabond, Ethicon Inc, New Brunswick, NJ) skin adhesive. Indications Breast reconstruction Earlier, we described the free SGAP flap as a valuable second choice for autologous breast recon- Fig. 2. Intraoperative view after (A) splitting the muscle along the epimysium, (B) incising the epimysium parallel to the perforator (arrow), and (C) opening the fascia anterior to the gluteus maximus muscle (arrow).
5 P.N. Blondeel et al / Clin Plastic Surg 30 (2003) Fig. 2 (continued).
6 376 P.N. Blondeel et al / Clin Plastic Surg 30 (2003)
7 P.N. Blondeel et al / Clin Plastic Surg 30 (2003) Fig. 3. (A) Pre- and (B,C) postoperative images of a 51-year-old woman who underwent a secondary autologous breast reconstruction with a free SGAP flap following right subtotal mastectomy for invasive breast cancer. struction after the deep inferior epigastric perforator (DIEP) flap [6]. The SGAP flap can be used for total or partial breast reconstruction (Fig. 3) and is indicated in patients who have an asthenic body habitus or excessive abdominal scarring. An increasing number of patients present for breast reconstruction or autologous breast augmentation following liposuction of the abdomen or abdominoplasty. Patients who have a family history of breast cancer should carefully consider having these procedures at the abdominal wall, because this will eliminate an important option for breast reconstruction. Although a single subcostal or midline scar is not a contraindication for DIEP flap harvesting, multiple abdominal scars following intra-abdominal surgery might pose such a risk for postoperative wound complications that one needs to resort to the SGAP flap. If a DIEP flap has already been harvested for previous breast cancer or after DIEP flap failure, the SGAP flap is a valuable alternative. Currently, we will design the flap in a more horizontal position. Additionally, we will add a small fish tail at the medial tip of the flap to avoid dog-ear formation in the median gluteal crease (see Fig. 1B). Flaps are also designed to be longer, so that the breast can be shaped in the form of a hammock, with care taken to reconstruct the anterior axillary fold and the full width of the inframammary crease and breast. During flap harvesting, the patient is positioned in lateral decubitus with the arm of the affected side free
8 378 P.N. Blondeel et al / Clin Plastic Surg 30 (2003) Fig. 4. (A) Pre-, (B,C) intra-, and (D) postoperative images of 32-year-old man with a large sacral pressure sore that was treated with debridement and single stage closure with a pedicled SGAP flap.
9 P.N. Blondeel et al / Clin Plastic Surg 30 (2003) Fig. 4 (continued). and the upper body twisted back 60 to allow a simultaneous two-team approach to the donor and recipient sites. The axillary vessels should not be used for SGAP breast reconstruction. Pedicle length is often insufficient and the establishment of the sentinel biopsy technique avoids exposure and dissection of axilla and thoracodorsal vessels. The preferred recipient vessels for the SGAP flap are either the perforators of the internal mammary vessels at the second or third intercostal space (perforator-to-perforator flap) or the internal mammary vessels themselves at the third or fourth costochondral junction. Perforators can be looked for either between skin and pectoralis muscle or between the rib cage and the pectoralis muscle. After vessel microanastomosis, the patient is placed in the dorsal decubitus position and sat up to perform adequate shaping and achieve acceptable symmetry. Operating time ranges between 4 and 6 hours. Dorsal pelvic area: sacrum As a pedicled flap, the SGAP flap is an excellent tool to cover large sacral and gluteal defects [2,4]. The ischium can also be reached because of the long pedicle and the wide range of the flap, but the inferior gluteal artery perforator is probably a better choice to cover defects in that region [7]. The SGAP flap is particularly suited to reconstruct large sacral midline defects in one stage, especially in the nonplegic patient. Although a pedicled fasciocutaneous flap is the first choice for smaller defects, the SGAP flap is a step between these flaps and the myocutaneous flaps of that region. Because the SGAP flap preserves the vascularization to the gluteus maximus muscle, it eliminates less options than a myocutaneous flap and preserves the opportunity for later reconstructions with muscle or other flaps, if a recurrence should occur (Fig. 4). The pedicled SGAP flap for sacral pressure sores is a good learning model for surgeons who have limited experience with perforator flaps. If this is the case, a conservative approach to the flap can be chosen. The upper border of the flap should be designed as a sector of an imaginary rotation flap, in which the flap could be reconverted if a dissection error is made during harvesting, or if no suitable perforator is encountered during the dissection. This provides the technique with an additional safety factor. The superior border of the flap is incised first, without beveling, through skin, subcutaneous tissue, and fascia to the muscle. From there, the flap is detached from the muscle, until the chosen perforator is encountered. Dissection of the perforator is similar
10 380 P.N. Blondeel et al / Clin Plastic Surg 30 (2003) to that described earlier. After one has obtained certainty of the patency of the nourishing vessels, the lower border can be incised and the flap can be transferred. By dissecting the nourishing vessel through the muscle, a considerable pedicle length is gained; this gives the flap its superior mobility. In most cases, the length of the pedicle allows the use of healthy skin from a distant, untraumatized zone. One single perforator is sufficient to vascularize the entire flap, because the angiosomes in this part of the body are relatively large. A single blood vessel pedicle also provides more liberty in shaping and a wider range of motion. The donor site is always closed primarily. Operating time ranges between 2 and 3 hours. Dorsal lower trunk Wounds at the dorsal lower trunk or lumbar area can be caused by acute trauma, have a congenital origin (ie, myelomeningocoele), or be a consequence of chronic internal (exposed ostheosynthesis material) or external pressure (pressure sores). Deep defects with exposure of vital structures over and around the lumbar spine have always been troublesome to cover. Most frequently, local fasciocutaneous flaps or the pedicled turn-over latissimus dorsi muscle flap were used. Because of the poor vascularization of those flaps, partial flap necrosis and wound healing problems were observed at the point where the flap was needed the most. Free flap surgery in this area is particularly difficult, because of the absence of decent-sized recipient vessels. Currently, the extended SGAP provides a more reliable solution. The conventional design of the skin island, as described earlier, can be extended more laterally or laterodistally to increase the length of the axis of the flap. The dissection is identical to the SGAP for sacral pressure sores, but the flap is now rotated counterclockwise. By maximally splitting the gluteus maximus muscle cranially, an important cranial displacement can be added, which provides coverage up to L1-T12 [8]. Proximal lower extremity reconstruction Because of the thickness of the subcutaneous layer of the SGAP flap, even in thin patients, this flap is not suited for reconstruction of the head and neck, upper extremity, or distal lower extremity. In exceptional cases in the area of the upper leg, the SGAP can be used to fill deep defects and to fill dead space. Indications are limited, however, and if the defect cannot be covered in a pedicled fashion, then the flap needs to be transferred as a free flap. Discussion The work of Taylor and Daniel [9] was a milestone in the development of new flaps that are used in reconstructive (micro-) surgery. Their main goal was to develop new donor sites for tissue transfer by thoroughly studying and documenting the vascular anatomy of the entire human body. Consequently, it was their intention to harvest skin flaps on the septoand musculocutaneous perforators that they had identified. It was concluded, nevertheless, that harvesting of these flaps would probably be safer if the septum, fascia, or muscle that surrounds the perforating vessels was harvested with the overlying subcutaneous fat and skin island. Because clinical microsurgery was still in its pioneer phase, the lack of sophisticated microsurgical instruments and optical devices probably influenced that decision. The microsurgical anastomosis of larger, well-known vessels was considered to be safer than performing anastomoses of small perforating vessels. Their work was crucial in the development of perforator flaps. Basically, there was no reason to sacrifice the muscle through which the perforating vessels traversed, other than the fear that the vessel would be damaged during dissection or that the muscle had a protective role to play on the perforating vessels. Over the last decades, several reconstructive surgeons believed that resecting a part or the entire muscle could not always be compensated for by the action of its neighboring agonists. This led to the development of more muscle-sparing techniques in an attempt to preserve as much of the muscle function as possible. Probably the most popular example is the evolution of the pedicled transverse rectus abdominis myocutaneous (TRAM) flap into the free TRAM flap, and, later, into the muscle-sparing TRAM flap. It was only logical to go one step further and reduce the amount of muscle resection so that the muscle would be split in the direction of its muscle fibers, the perforating vessels would be dissected from between these muscle fibers, and all muscle would be left in place. This important step was first taken in a clinical case by Koshima and Soeda [10] when they used the thin paraumbilical perforator flap to reconstruct a tongue and groin defect. A second article on the same subject was published by Koshima et al [11] in The first reports of the use of the DIEP flap for breast reconstruction were by Allen and Treece [12] and our group [13]. Despite the initial positive results, there was considerable skepticism concerning the technique. In 1994, Cormack and Lamberty [14] regarded the technique as more a demonstration of technical skill than a significant advance in flap construction.
11 P.N. Blondeel et al / Clin Plastic Surg 30 (2003) The question if the muscle that was spared would be functional was well founded. Although in 1995 Allen and Tucker [3] reported the use of the SGAP flap in breast reconstruction and Angrigiani et al [15] reported the first thoracodorsal artery perforator (TAP) flap, no scientific study had demonstrated the advantage of sparing the muscle on muscle function. The prospective study by our group in 1997 [16] clearly demonstrated that saving the rectus abdominis muscle reduced the donor site morbidity to an absolute minimum. Although no prospective donor morbidity studies have been performed on other donor sites, it is logical that more muscle function will be preserved if the muscle is left intact. Preserving the muscle function relies on respecting the vascularization by collateral blood vessels, and more importantly, preserving the continuity of the motor nerve branches that pass through the plane of dissection. If the motor nerves of the donor site muscle are cut during splitting or lifting of the muscle, the donor morbidity will be comparable to that of a muscle-sparing myocutaneous flap. The advantages of using an SGAP flap for the indications mentioned earlier are: (1) the abundance of adipose tissue in the gluteal area, even in thin patients; (2) a better intraoperative exposure and a longer vascular pedicle compared with its myocutaneous predecessor; (3) a well-hidden scar; (4) excellent projection of the reconstructed breast compared with the DIEP and TRAM flap; and (5) the preservation of the integrity of the gluteus maximus muscle. The donor morbidity is the lowest that can be offered to the patient today. Including a sensate branch of the nervi clunii superiores can provide better quality and quantity of sensation to the flap [5,6]. Leaving the muscle intact avoids exposure of any nerves or bony eminences. Absence of a muscle cuff around the vascular pedicle also avoids postoperative atrophy and aids in modeling the flap, especially in breast reconstruction. Not resecting any muscle also results decreased postoperative pain and thus, a swifter rehabilitation. This leads to a shorter hospital stay, and, therefore, reduced costs. By harvesting skin and fat from the superior part of the buttock, it is possible to minimize any contour deformities and position the final scar within the bikini line. Finally, the preservation of the viability and function of the muscle at the donor site makes the rare case of total flap loss less dramatic, because only skin and subcutaneous fat are lost. In the case of a pedicled flap, the tissues used in the SGAP flap come from a distance from the ulcus or wound, and, as such, they are less inflamed, less edematous, and less prone to dehiscence. The length of the pedicle gives the flap an impressive mobility and allows for easy tissue transposition without tension. The inset of the flap is always tension-free and the donor defect can always be closed primarily. The firmer consistency of gluteal fat makes it more difficult to mold the flap, especially for breast reconstruction. Additional minor secondary corrections might be necessary to obtain the desired shape. The skin paddle that is included is often smaller than a TRAM or DIEP flap and should be considered in the preoperative planning. Although the contour deformity is considerably less than with the myocutaneous flaps, unilateral harvesting may necessitate a secondary correction of the contralateral side. In our early experience with treating sacral pressure sores, there was a tendency for seroma formation underneath the flaps. This was reduced by harvesting the flap in a suprafascial plane instead of below the gluteus maximus muscle fascia. In general, the steep learning curve is the main disadvantage of perforator flaps. Nevertheless, the technique of dissecting perforating vessels is not more difficult or tedious than other microsurgical procedures. To the contrary, if specific surgical acts and retraction are applied and adapted microsurgical instruments and optical devices are used, the dissection can be safe because the vessels are always under direct visual control. Perforator flap dissection is often more about patience than about skills. Wide exposure of the surgical field and bloodless dissection are key to complication-free surgery. Perfecting this new style of dissecting can be time consuming, especially during the early cases, and will add a considerable amount of operating time. After the surgeon is familiar with the technique, the operative time for a perforator flap procedure may be comparable or even less than for a myocutaneous flap. International courses on perforator flaps are organized yearly to teach the concepts to interested surgeons. The clinical experience and the favorable results with perforator flaps in several centers in Europe, Asia, and the United States have shown that this technique is new, but sufficiently reliable, to be used in daily clinical practice and is reproducible by other colleagues. The combination of the advantages that were discussed earlier, and the fact that all intrinsic advantages of each myocutaneous flap is preserved, make perforator flaps even more attractive. Although no scientific data are available on the physiology of blood flow in perforator flaps, the clinical experience [5,6,17 19] has proven that the blood flow through one perforator is almost always sufficient to vascularize a large overlying skin island. The design of that skin island may nevertheless be a little different than
12 382 P.N. Blondeel et al / Clin Plastic Surg 30 (2003) that of its myocutaneous predecessor. Skin islands must be centered on top of the perforator or following the direction of the main branches of the perforator within the flap, as if it would be an axial pattern flap. A larger amount of partial- or fat necrosis may be encountered if the conventional design is applied [20]. Summary The development of the perforator flap technique revolutionized the practice of soft tissue transfer. The main goal of this technique is muscle sparing at the donor site for function and strength. Meanwhile, this concept is being widely applied for reconstruction of tissues throughout the entire body. Perforator flaps are the ultimate upgrade of the well-known myocutaneous flaps. Theoretically, any myocutaneous flap can be harvested as a perforator flap if skin resurfacing is needed. Although the DIEP flap, the anterolateral thigh flap, and the TAP flap are probably more frequently used for breast, trunk, and upper and lower limb reconstruction, as well as head and neck reconstruction, the SGAP flap takes its own position in the large group of perforator flaps and has its own specific indications. References [1] Fujino T, Harashina T, Aoyagi F. Reconstruction for aplasia of the breast and pectoral region by microvascular transfer of a free flap from the buttock. Plast Reconstr Surg 1975;56: [2] Koshima I, Moriguchi T, Soeda S, et al. Gluteal perforator-based flap for repair of sacral pressure sores. Plast Reconstr Surg 1993;91: [3] Allen RJ, Tucker Jr C. Superior gluteal artery perforator free flap for breast reconstruction. Plast Reconstr Surg 1995;95: [4] Verpaele AM, Blondeel PN, Van Landuyt K, et al. The superior gluteal artery perforator flap: an additional tool in the treatment of pressure sores. Br J Plast Surg 1999;52: [5] Blondeel PN, De Muynck M, Mete D, et al. Sensate nerve repair in perforator flaps for autologous breast reconstruction: sensational or senseless? Br J Plast Surg 1999;52: [6] Blondeel PhN. The sensate free superior gluteal artery perforator (S-GAP) flap: a valuable alternative in autologous breast reconstruction. Br J Plast Surg 1999; 52: [7] Higgins JP, Orlando GS, Blondeel PN. Ischial pressure sore reconstruction using an inferior gluteal artery perforator (IGAP) flap. Br J Plast Surg 2002;55: [8] Roche NA, Van Landuyt K, Blondeel PN, et al. The use of pedicled perforator flaps for reconstruction of lumbosacral defects. Ann Plast Surg 2000;45(1): [9] Taylor GI, Daniel RK. The anatomy of several free flap donor sites. Plast Reconstr Surg 1975;56: [10] Koshima I, Soeda S. Inferior epigastric artery skin flap without rectus abdominis muscle. Br J Plast Surg 1989; 42: [11] Koshima I, Moriguchi T, Soeda S, et al. Free thin paraumbilical perforator-based flaps. Ann Plast Surg 1992; 29:12 7. [12] Allen RJ, Treece P. Deep inferior epigastric perforator flap for breast reconstruction. Ann Plast Surg 1994;32: [13] Blondeel PN, Boeckx WD. Refinements in free flap breast reconstruction: the free bilateral deep inferior epigastric perforator flap anastomosed to the internal mammary artery. Br J Plast Surg 1994;47: [14] Cormack GC, Lamberty BG. The arterial anatomy of skin flaps. 2nd edition. Edinburgh: Churchill Livingstone; p. 87. [15] Angrigiani C, Grilli D, Siebert J. Latissimus dorsi musculocutaneous flap without muscle. Plast Reconstr Surg 1995;96: [16] Blondeel PN, Vanderstraeten GG, Monstrey SJ, et al. The donor site morbidity of free DIEP flaps and free TRAM flaps for breast reconstruction. Br J Plast Surg 1997;50: [17] Blondeel PN, Arnstein M, Verstraete K, et al. Venous congestion and blood flow in TRAM and DIEP flaps. Plast Reconstr Surg 2000;106: [18] Blondeel PN. One hundred free DIEP flap breast reconstructions: a personal experience. Br J Plast Surg 1999;52: [19] Blondeel PN, Van Landuyt KH, Monstrey SJ. Surgicaltechnical aspects of the free DIEP flap for breast reconstruction. Oper Tech Plast Reconstruct Surg 1999; 6(1): [20] Lantieri L, Serra M, Dallaserra M, et al. Conservation du muscle dans l utilisation du lambeau libre de grand droit en reconstruction mammaire: du TRAM au DIEP flap [in French]. Ann Chir Plast Esth 1997;42(2):
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
The most common type of breast reconstruction
 BREAST Breast Reconstruction with Perforator Flaps Jay W. Granzow, M.D., M.P.H. Joshua L. Levine, M.D. Ernest S. Chiu, M.D. Maria M. LoTempio, M.D. Robert J. Allen, M.D. New Orleans, La.; Charleston, S.C.;
BREAST Breast Reconstruction with Perforator Flaps Jay W. Granzow, M.D., M.P.H. Joshua L. Levine, M.D. Ernest S. Chiu, M.D. Maria M. LoTempio, M.D. Robert J. Allen, M.D. New Orleans, La.; Charleston, S.C.;
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
The lumbar artery perforator based island flap: anatomical study and case reports
 British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
The free thoracodorsal artery perforator flap in head and neck reconstruction
 European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
The progress in microsurgical procedures has led
 Original Article Breast reconstruction with free anterolateral thigh flap Ranjit Raje, Ramesh Chepauk, Kanti Shetty, Rajendra Prasad J. S. Plastic & Reconstructive Services, Department of Surgical Oncology,
Original Article Breast reconstruction with free anterolateral thigh flap Ranjit Raje, Ramesh Chepauk, Kanti Shetty, Rajendra Prasad J. S. Plastic & Reconstructive Services, Department of Surgical Oncology,
The superior gluteal artery perforator flap: an additional tool in the treatment of sacral pressure sores
 ritish Journal of Plastic Surgery (1999), 52, 385 391 1999 The ritish ssociation of Plastic Surgeons The superior gluteal artery perforator flap: an additional tool in the treatment of sacral pressure
ritish Journal of Plastic Surgery (1999), 52, 385 391 1999 The ritish ssociation of Plastic Surgeons The superior gluteal artery perforator flap: an additional tool in the treatment of sacral pressure
Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes
 DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
The gluteal perforator-based flap in repair of pressure sores
 The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects
 Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps
 BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
Breast Reconstruction Options
 Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study
 Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
Essential Anatomy for oncoplastic surgery. Omar Z. Youssef M.D Professor of surgical oncology NCI- Cairo University
 Essential Anatomy for oncoplastic surgery Omar Z. Youssef M.D Professor of surgical oncology NCI- Cairo University Introduction Rationale for anatomical basis for OPS Anatomical considerations: 1. Surface
Essential Anatomy for oncoplastic surgery Omar Z. Youssef M.D Professor of surgical oncology NCI- Cairo University Introduction Rationale for anatomical basis for OPS Anatomical considerations: 1. Surface
Tor Chiu. Deep Inferior Epigastric Artery Perforator Flap 161
 18 Deep Inferior Epigastric Artery Perforator Flap Tor Chiu Deep Inferior Epigastric Artery Perforator Flap 161 Deep Inferior Epigastric Artery Perforator Flap FLAP TERRITORY The deep inferior epigastric
18 Deep Inferior Epigastric Artery Perforator Flap Tor Chiu Deep Inferior Epigastric Artery Perforator Flap 161 Deep Inferior Epigastric Artery Perforator Flap FLAP TERRITORY The deep inferior epigastric
Citation for published version (APA): Benditte-Klepetko, H. C. (2014). Breast surgery: A problem of beauty or health?
 UvA-DARE (Digital Academic Repository) Breast surgery: A problem of beauty or health? Benditte-Klepetko, H.C. Link to publication Citation for published version (APA): Benditte-Klepetko, H. C. (2014).
UvA-DARE (Digital Academic Repository) Breast surgery: A problem of beauty or health? Benditte-Klepetko, H.C. Link to publication Citation for published version (APA): Benditte-Klepetko, H. C. (2014).
Anatomical study. Clinical study. R. Ogawa, H. Hyakusoku, M. Murakami, R. Aoki, K. Tanuma* and D. G. Pennington?
 British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
INTRODUCTION. Toshihiko Satake 1, Jun Sugawara 2, Kazunori Yasumura 1, Taro Mikami 2, Shinji Kobayashi 3, Jiro Maegawa 2. Idea and Innovation
 Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
Pedicled Gluteal Artery Perforator Flap for Sacral and Ischial Pressure Ulcer Reconstruction: Promising Prospects for Mauritius
 UNIVERSITY OF MAURITIUS RESEARCH JOURNAL Volume 17 2011 University of Mauritius, Réduit, Mauritius Pedicled Gluteal Artery Perforator Flap for Sacral and Ischial Pressure Ulcer Reconstruction: Promising
UNIVERSITY OF MAURITIUS RESEARCH JOURNAL Volume 17 2011 University of Mauritius, Réduit, Mauritius Pedicled Gluteal Artery Perforator Flap for Sacral and Ischial Pressure Ulcer Reconstruction: Promising
Medical Journal of the Volume 20 Islamic Republic of Iran Number 3 Fall 1385 November Original Articles
 Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography
 BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
Michael A. Howard a, Babak Mehrara b, * REVIEW. Introduction
 International Journal of Surgery (2005) 3, 53e60 www.int-journal-surgery.com REVIEW Emerging trends in microsurgical breast reconstruction: Deep inferior epigastric artery perforator (DIEP) and the superior
International Journal of Surgery (2005) 3, 53e60 www.int-journal-surgery.com REVIEW Emerging trends in microsurgical breast reconstruction: Deep inferior epigastric artery perforator (DIEP) and the superior
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage
 Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Breast reconstruction following mastectomy has
 Free full text on www.ijps.org Post-mastectomy breast reconstruction: Microsurgical methods Venkat Ramakrishnan, Makarand Tare St. Andrew s Centre for Burns and Plastic Surgery, BroomÞ eld Hospital, Chelmsford,
Free full text on www.ijps.org Post-mastectomy breast reconstruction: Microsurgical methods Venkat Ramakrishnan, Makarand Tare St. Andrew s Centre for Burns and Plastic Surgery, BroomÞ eld Hospital, Chelmsford,
Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps
 Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps Pierre M. Chevray, M.D., Ph.D. 1 ABSTRACT Breast reconstruction using autologous tissue is commonly accomplished using the transverse
Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps Pierre M. Chevray, M.D., Ph.D. 1 ABSTRACT Breast reconstruction using autologous tissue is commonly accomplished using the transverse
Few would deny that lower abdominal tissue BREAST. An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction.
 BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
The earlier clinic experience of the reverse-flow anterolateral thigh island flap
 British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
Anatomical relationship between arteries and veins in the paraumbilical region q
 The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction
 A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q
 The British Association of Plastic Surgeons (2003) 56, 395 400 The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q D. Erni*, Y.D. Harder
The British Association of Plastic Surgeons (2003) 56, 395 400 The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q D. Erni*, Y.D. Harder
Reconstruction of axillary scar contractures retrospective study of 124 cases over 25 years
 British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps
 Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
4/30/2010. Options for abdominal wall reconstruction. Scott L. Hansen, MD
 Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap
 Free full text on www.ijps.org Case Report DOI: 10.4103/0970-0358.63966 Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap Pearlie W. W. Tan, Chin-Ho Wong,
Free full text on www.ijps.org Case Report DOI: 10.4103/0970-0358.63966 Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap Pearlie W. W. Tan, Chin-Ho Wong,
The gastrocnemius with soleus bi-muscle flap
 The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
Samer Saour, Guido Libondi, Venkat Ramakrishnan. Introduction
 Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY RECTUS ABDOMINIS FLAP FOR HEAD & NECK RECONSTRUCTION Patrik Pipkorn, Brian Nussenbaum The rectus abdominis flap is based on the deep inferior
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY RECTUS ABDOMINIS FLAP FOR HEAD & NECK RECONSTRUCTION Patrik Pipkorn, Brian Nussenbaum The rectus abdominis flap is based on the deep inferior
THE pedicled flap, commonly used by the plastic surgeon in the reconstruction
 THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
Septic Bone and Joint Surgery
 Septic Bone and Joint Surgery Bearbeitet von Reinhard Schnettler 1. Auflage 2010. Buch. 328 S. Hardcover ISBN 978 3 13 149031 5 Format (B x L): 19,5 x 27 cm Weitere Fachgebiete > Medizin > Chirurgie >
Septic Bone and Joint Surgery Bearbeitet von Reinhard Schnettler 1. Auflage 2010. Buch. 328 S. Hardcover ISBN 978 3 13 149031 5 Format (B x L): 19,5 x 27 cm Weitere Fachgebiete > Medizin > Chirurgie >
Modified Radical Mastectomy
 Modified Radical Mastectomy Valerie L. Staradub, MD, and Monica Morrow, MD S urgical management options for breast cancer include modified radical mastectomy (MRM), MRM with immediate reconstruction, and
Modified Radical Mastectomy Valerie L. Staradub, MD, and Monica Morrow, MD S urgical management options for breast cancer include modified radical mastectomy (MRM), MRM with immediate reconstruction, and
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
A new operative technique for dissecting perforator vessel in perforator flap: a better way to minimize donor-site morbidity
 Original Article Page 1 of 7 A new operative technique for dissecting perforator vessel in perforator flap: a better way to minimize donor-site morbidity Limin Qing, Panfeng Wu, Zhouzheng Bing, Fang Yu,
Original Article Page 1 of 7 A new operative technique for dissecting perforator vessel in perforator flap: a better way to minimize donor-site morbidity Limin Qing, Panfeng Wu, Zhouzheng Bing, Fang Yu,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION
 CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
Kuwabara, Kaoru; Nonaka, Takashi; H. Citation Journal of Clinical Urology, 7(5),
 NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
Strattice Reconstructive Tissue Matrix used in the repair of rippling
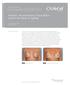 Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
No Drain Abdominoplasty: No More Excuses. Karol A Gutowski, MD, FACS
 No Drain Abdominoplasty: No More Excuses Karol A Gutowski, MD, FACS Disclosures NO financial interests in any suture company Will use brand names due to lack of distinguishing generic names Objectives
No Drain Abdominoplasty: No More Excuses Karol A Gutowski, MD, FACS Disclosures NO financial interests in any suture company Will use brand names due to lack of distinguishing generic names Objectives
RECONSTRUCTION OF SUBTOTAL DEFECTS OF THE NOSE BY ABDOMINAL TUBE FLAP. By MICHAL KRAUSS. Plastic Surgery Hospital, Polanica-Zdroj, Poland
 RECONSTRUCTION OF SUBTOTAL DEFECTS OF THE NOSE BY ABDOMINAL TUBE FLAP By MICHAL KRAUSS Plastic Surgery Hospital, Polanica-Zdroj, Poland RECONSTRUCTION of the nose is one of the composite procedures in
RECONSTRUCTION OF SUBTOTAL DEFECTS OF THE NOSE BY ABDOMINAL TUBE FLAP By MICHAL KRAUSS Plastic Surgery Hospital, Polanica-Zdroj, Poland RECONSTRUCTION of the nose is one of the composite procedures in
The Thoracodorsal Artery Perforator Flap: Clinical Experience and Anatomic Study with Emphasis on Harvest Techniques
 The Thoracodorsal Artery Perforator Flap: Clinical Experience and Anatomic Study with Emphasis on Harvest Techniques Aldo Benjamin Guerra, M.D., Stephen Eric Metzinger, M.D., Kiersten Maria Lund, M.D.,
The Thoracodorsal Artery Perforator Flap: Clinical Experience and Anatomic Study with Emphasis on Harvest Techniques Aldo Benjamin Guerra, M.D., Stephen Eric Metzinger, M.D., Kiersten Maria Lund, M.D.,
JMSCR Vol 07 Issue 01 Page January 2019
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i1.36 Original Article A Study on the
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i1.36 Original Article A Study on the
Breast Reconstruction
 Steven E. Copit, M.D. Chief- Division of Plastic Surgery Thomas Jefferson University Hospital Philadelphia, PA analysis of The Defect Skin Breast Volume Nipple Areola Complex analysis of The Defect the
Steven E. Copit, M.D. Chief- Division of Plastic Surgery Thomas Jefferson University Hospital Philadelphia, PA analysis of The Defect Skin Breast Volume Nipple Areola Complex analysis of The Defect the
The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction
 The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction Zachary Menn and Aldona Spiegel Weill Cornell Medical College, The Methodist Hospital, Houston, Texas,
The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction Zachary Menn and Aldona Spiegel Weill Cornell Medical College, The Methodist Hospital, Houston, Texas,
Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps
 e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Breast Restoration Surgery After a mastectomy
 UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
Gluteal region DR. GITANJALI KHORWAL
 Gluteal region DR. GITANJALI KHORWAL Gluteal region The transitional area between the trunk and the lower extremity. The gluteal region includes the rounded, posterior buttocks and the laterally placed
Gluteal region DR. GITANJALI KHORWAL Gluteal region The transitional area between the trunk and the lower extremity. The gluteal region includes the rounded, posterior buttocks and the laterally placed
Flaps vs Grafts. Ronen Avram, MD MSc FRCSC
 Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Anterolateral Thigh Flap for Postmastectomy Breast Reconstruction
 Anterolateral Thigh Flap for Postmastectomy Breast Reconstruction Fu-chan Wei, M.D., Sinikka Suominen, M.D., Ph.D., Ming-huei Cheng, M.D., Naci Celik, M.D., and Yung-lung Lai, M.D. Taipei, Taiwan Most
Anterolateral Thigh Flap for Postmastectomy Breast Reconstruction Fu-chan Wei, M.D., Sinikka Suominen, M.D., Ph.D., Ming-huei Cheng, M.D., Naci Celik, M.D., and Yung-lung Lai, M.D. Taipei, Taiwan Most
Primary closure of the deltopectoral flap-donor site without skin grafting
 Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Deep Inferior Epigastric Perforator Flap for Successful Simultaneous Breast and Chest Wall Reconstruction in a Poland Anomaly Patient
 CASE REPORT Deep Inferior Epigastric Perforator Flap for Successful Simultaneous Breast and Chest Wall Reconstruction in a Poland Anomaly Patient Han-Tsung Liao, MD, Ming-Huei Cheng, MD, Betul Gozel Ulusal,
CASE REPORT Deep Inferior Epigastric Perforator Flap for Successful Simultaneous Breast and Chest Wall Reconstruction in a Poland Anomaly Patient Han-Tsung Liao, MD, Ming-Huei Cheng, MD, Betul Gozel Ulusal,
A multiple logistic regression analysis of complications following microsurgical breast reconstruction
 Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Scapular & Parascapular flap FLAP TERRITORY ANATOMY. is normally accompanied by two venae comitantes.
 Scapular & Parascapular flap FLAP TERRITORY This is a composite flap that is situated over the scapula with various incisional arrangements. It can be harvested as a skin and subcutaneous tissue flap,
Scapular & Parascapular flap FLAP TERRITORY This is a composite flap that is situated over the scapula with various incisional arrangements. It can be harvested as a skin and subcutaneous tissue flap,
Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate surgical options
 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
Barbed Sutures in Progressive Tension Suture Technique Abdominoplasty. Karol A Gutowski, MD
 Barbed Sutures in Progressive Tension Suture Technique Abdominoplasty Karol A Gutowski, MD 1 Disclosures Speakers Bureau for AngioTech since April 2011 (Makers of Quill bi-directional barbed sutures) Technique
Barbed Sutures in Progressive Tension Suture Technique Abdominoplasty Karol A Gutowski, MD 1 Disclosures Speakers Bureau for AngioTech since April 2011 (Makers of Quill bi-directional barbed sutures) Technique
ABDOMINAL WALL & RECTUS SHEATH
 ABDOMINAL WALL & RECTUS SHEATH Learning Objectives Describe the anatomy, innervation and functions of the muscles of the anterior, lateral and posterior abdominal walls. Discuss their functional relations
ABDOMINAL WALL & RECTUS SHEATH Learning Objectives Describe the anatomy, innervation and functions of the muscles of the anterior, lateral and posterior abdominal walls. Discuss their functional relations
No Drain Abdominoplasty: No More Excuses. Karol A Gutowski, MD, FACS Instructional Course
 No Drain Abdominoplasty: No More Excuses Karol A Gutowski, MD, FACS Instructional Course Disclosures Angiotech/Surgical Specialties - Advisory Board AxcelRx Pharmacuticals - Advisory Board Suneva Medical
No Drain Abdominoplasty: No More Excuses Karol A Gutowski, MD, FACS Instructional Course Disclosures Angiotech/Surgical Specialties - Advisory Board AxcelRx Pharmacuticals - Advisory Board Suneva Medical
No Drain Abdominoplasty with Progressive Tension Sutures. Karol A Gutowski, MD, FACS
 No Drain Abdominoplasty with Progressive Tension Sutures Karol A Gutowski, MD, FACS Disclosures Suneva Medical Instructor Merz Advisory Board NO financial interests in any suture company Will use brand
No Drain Abdominoplasty with Progressive Tension Sutures Karol A Gutowski, MD, FACS Disclosures Suneva Medical Instructor Merz Advisory Board NO financial interests in any suture company Will use brand
J. Bryce Olenczak, MD, Matthew G. Stanwix, MD, and Gedge D. Rosson, MD
 CASE REPORT Complex Wound Closure of Partial Sacrectomy Defect With Human Acellular Dermal Matrix and Bilateral V to Y Gluteal Advancement Flaps in a Pediatric Patient J. Bryce Olenczak, MD, Matthew G.
CASE REPORT Complex Wound Closure of Partial Sacrectomy Defect With Human Acellular Dermal Matrix and Bilateral V to Y Gluteal Advancement Flaps in a Pediatric Patient J. Bryce Olenczak, MD, Matthew G.
Vertical mammaplasty has been developed
 BREAST Y-Scar Vertical Mammaplasty David A. Hidalgo, M.D. New York, N.Y. Background: Vertical mammaplasty is an effective alternative to inverted-t methods. Among other benefits, it results in a significantly
BREAST Y-Scar Vertical Mammaplasty David A. Hidalgo, M.D. New York, N.Y. Background: Vertical mammaplasty is an effective alternative to inverted-t methods. Among other benefits, it results in a significantly
Methods of autologous tissue breast reconstruction BREAST
 BREAST Comparison of Donor-Site Morbidity of SIEA, DIEP, and Muscle-Sparing TRAM Flaps for Breast Reconstruction Liza C. Wu, M.D. Anureet Bajaj, M.D. David W. Chang, M.D. Pierre M. Chevray, M.D., Ph.D.
BREAST Comparison of Donor-Site Morbidity of SIEA, DIEP, and Muscle-Sparing TRAM Flaps for Breast Reconstruction Liza C. Wu, M.D. Anureet Bajaj, M.D. David W. Chang, M.D. Pierre M. Chevray, M.D., Ph.D.
Achieving ideal donor site aesthetics with autologous breast reconstruction
 Review Article Achieving ideal donor site aesthetics with autologous breast reconstruction Maurice Y. Nahabedian Department of Plastic Surgery, Georgetown University, Washington, DC 20007, USA Correspondence
Review Article Achieving ideal donor site aesthetics with autologous breast reconstruction Maurice Y. Nahabedian Department of Plastic Surgery, Georgetown University, Washington, DC 20007, USA Correspondence
-primarily by apposition of the anterior rectus
 2 Component separation Cop HARVEY CHIM, KAREN KIM EVANS, AND SAMIR MARDINI Mater al Introduction 7 Preoperative markings 7 Intraoperative details 9 Technique modification: Component separation with preservation
2 Component separation Cop HARVEY CHIM, KAREN KIM EVANS, AND SAMIR MARDINI Mater al Introduction 7 Preoperative markings 7 Intraoperative details 9 Technique modification: Component separation with preservation
CHARACTERISTICS OF THE ANTEROLATERAL THIGH FLAP IN A WESTERN POPULATION AND ITS APPLICATION IN HEAD AND NECK RECONSTRUCTION
 CHARACTERISTICS OF THE ANTEROLATERAL THIGH FLAP IN A WESTERN POPULATION AND ITS APPLICATION IN HEAD AND NECK RECONSTRUCTION Peirong Yu, MD Department of Plastic Surgery, The University of Texas M. D. Anderson
CHARACTERISTICS OF THE ANTEROLATERAL THIGH FLAP IN A WESTERN POPULATION AND ITS APPLICATION IN HEAD AND NECK RECONSTRUCTION Peirong Yu, MD Department of Plastic Surgery, The University of Texas M. D. Anderson
MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION. Adequate speech and swallowing are dependent
 ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
COMBINED ABDOMINAL FLAP FOR MAJOR HAND RECONSTRUCTION
 Int. J. Pharm. Med. & Bio. Sc. 2013 2014 Srinivas Somashekar et al., 2014 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 3, No. 1, January 2014 2014 IJPMBS. All Rights Reserved COMBINED ABDOMINAL FLAP
Int. J. Pharm. Med. & Bio. Sc. 2013 2014 Srinivas Somashekar et al., 2014 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 3, No. 1, January 2014 2014 IJPMBS. All Rights Reserved COMBINED ABDOMINAL FLAP
Breast Reconstruction Surgery
 Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Figure 1. Anatomy of the breast
 CHAPTER 12 BREAST RECONSTRUCTION Mihaela Rapolti, MD and Michelle Roughton, MD I. BREAST ANATOMY A. Mastering breast anatomy is essential for understanding how the breast changes with aging and principles
CHAPTER 12 BREAST RECONSTRUCTION Mihaela Rapolti, MD and Michelle Roughton, MD I. BREAST ANATOMY A. Mastering breast anatomy is essential for understanding how the breast changes with aging and principles
The posterolateral thoracotomy is still probably the
 Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
The University Of Jordan Faculty Of Medicine THE LOWER LIMB. Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan
 The University Of Jordan Faculty Of Medicine THE LOWER LIMB Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan Gluteal Region Cutaneous nerve supply of (Gluteal region) 1. Lateral cutaneous
The University Of Jordan Faculty Of Medicine THE LOWER LIMB Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan Gluteal Region Cutaneous nerve supply of (Gluteal region) 1. Lateral cutaneous
Basics of Flap Design
 Basics of Flap Design Reconstructive Ladder (Mathes & Nahai 1982) Consider the defect, systematically Move from simple to complex Occam s Razor Sutton s Law Ladder is simple, emphasizes closure over form
Basics of Flap Design Reconstructive Ladder (Mathes & Nahai 1982) Consider the defect, systematically Move from simple to complex Occam s Razor Sutton s Law Ladder is simple, emphasizes closure over form
Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 6 Number 1 Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem S Tripathy,
ISPUB.COM The Internet Journal of Plastic Surgery Volume 6 Number 1 Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem S Tripathy,
Advances in Localized Breast Cancer
 Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Breast Reconstruction: Current Strategies and Future Opportunities
 Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
cally, a distinct superior crease of the forehead marks this spot. The hairline and
 4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
A Retrospective Comparison of Perforator and Rotation Flaps for the Closure of Extensive Stage IV Sacral Pressure Ulcers
 A Retrospective Comparison of Perforator and Rotation Flaps for the Closure of Extensive Stage IV Sacral Pressure Ulcers Masaki Fujioka, MD, PhD; Kenji Hayashida, MD; Sin Morooka, MD; and Hiroto Saijo,
A Retrospective Comparison of Perforator and Rotation Flaps for the Closure of Extensive Stage IV Sacral Pressure Ulcers Masaki Fujioka, MD, PhD; Kenji Hayashida, MD; Sin Morooka, MD; and Hiroto Saijo,
Anatomical Study of Pectoral Nerves and its Implications in Surgery
 DOI: 10.7860/JCDR/2014/8631.4545 Anatomy Section Original Article Anatomical Study of Pectoral Nerves and its Implications in Surgery Prakash KG 1, Saniya K 2 ABSTRACT Introduction: This anatomical study
DOI: 10.7860/JCDR/2014/8631.4545 Anatomy Section Original Article Anatomical Study of Pectoral Nerves and its Implications in Surgery Prakash KG 1, Saniya K 2 ABSTRACT Introduction: This anatomical study
Inferior Gluteus Maximus Island Flap for Reconstruction of Ischial Pressure Sores
 Original Article Inferior Gluteus Maximus Island Flap for Reconstruction of Ischial Pressure Sores Yawar Sajjad, 1 Beenish Rahat, 2 Salman Hameed 3 Abstract Surgical management of ischial pressure sores
Original Article Inferior Gluteus Maximus Island Flap for Reconstruction of Ischial Pressure Sores Yawar Sajjad, 1 Beenish Rahat, 2 Salman Hameed 3 Abstract Surgical management of ischial pressure sores
Current Strategies in Breast Reconstruction
 Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
The Use of Perforator-Plus Fasciocutaneous Flaps For Sacral Pressure Ulcer Reconstruction
 Open Journal of Clinical & Medical Case Reports Volume 1 (2015) Issue 2 The Use of Perforator-Plus Fasciocutaneous Flaps For Sacral Pressure Ulcer Reconstruction Jon P VerHalen, MD FACS Adjunct Clinical
Open Journal of Clinical & Medical Case Reports Volume 1 (2015) Issue 2 The Use of Perforator-Plus Fasciocutaneous Flaps For Sacral Pressure Ulcer Reconstruction Jon P VerHalen, MD FACS Adjunct Clinical
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION
 Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer. Oncoplastic and Reconstructive Surgery
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress RECONSTRUCTIVE SURGERY I: LOCAL FLAPS Bryden J. Stanley, BVMS, MACVSc, MVetSc, Diplomate ACVS College of Veterinary
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress RECONSTRUCTIVE SURGERY I: LOCAL FLAPS Bryden J. Stanley, BVMS, MACVSc, MVetSc, Diplomate ACVS College of Veterinary
