Comparison of ultrasound-guided supraclavicular block according to the various volumes of local anesthetic
|
|
|
- Eustacia Blake
- 5 years ago
- Views:
Transcription
1 Clinical Research Article Korean J Anesthesiol 2013 June 64(6): Comparison of ultrasound-guided supraclavicular block according to the various volumes of local anesthetic Dae Geun Jeon, Seok Kon Kim, Bong Jin Kang, in A Kwon, Jae Gyok Song, and Soo i Jeon Department of Anesthesiology and Pain edicine, College of edicine, Dankook University, Cheonan, Korea Background: The ultrasound guidance in regional nerve blocks has recently been introduced and gaining popularity. Ultrasound-guided supraclavicular block has many advantages including the higher success rate, faster onset time, and fewer complications. The aim of this study was to examine the clinical data according to the varied volume of local anesthetics in the ultrasound-guided supraclavicular block. ethods: One hundred twenty patients were randomized into four groups, according to the local anesthetic volume used:,,, and. Supraclavicular blocks were performed with 1% mepivacaine 35 ml, 30 ml, 25 ml, and 20 ml, respectively. The success rate, onset time, and complications were checked and evaluated. Results: The success rate (66.7%) was lower in than that of (96.7%) (P < 0.05). The average onset times of,,, and were 14.3 ± 6.9 min, 13.6 ± 4.5 min, 16.7 ± 4.6 min, and 16.5 ± 3.7 min, respectively. There were no significant differences. Horner's syndrome was higher in (P < 0.05). Conclusions: In conclusion, we achieved 90% success rate with 30 ml of 1% mepivacaine. Therefore, we suggest 30 ml of local anesthetic volume for ultrasound-guided supraclavicular block. (Korean J Anesthesiol 2013; 64: ) Key Words: Regional nerve blocks, Supraclavicular block, Ultrasound guidance. Introduction Supraclavicular block provides excellent anesthesia for upper limb surgery [1,2]. oreover, ultrasound guidance in supra clavicular block has been introduced and gaining popularity [3]. Ultrasound-guided supraclavicular block has many advantages including the higher success rate, faster onset time, and fewer complications [4-6]. In the previous studies on the ultrasoundguided axillary blocks and interscalene blocks, the possibility of the reduced volume of local anesthetics was demonstrated [7-10]. However, there is some controversy in such reduced anesthetics volume in the ultrasound-guided supraclavicular block [11,12]. In the previous studies on the minimum effective volume for the ultrasound-guided supraclavicular block, the Dixon and assey up and down method (DUD) and biased coin Received: August 30, Revised: 1st, October 9, 2012; 2nd, October 25, 2012; 3rd, November 7, Accepted: November 11, Corresponding author: Dae Geun Jeon,.D., Department of Anesthesiology and Pain edicine, College of edicine, Dankook University, 16-6, Anseo-dong, Dongnam-gu, Cheonan , Korea. Tel: , ax: , timepain@hanmail.net CC This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( creativecommons.org/licenses/by-nc/3.0/), which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Copyright c the Korean Society of Anesthesiologists, 2013
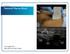
2 Korean J Anesthesiol Jeon et al. design up and down method (BUD) were used to calculate the minimum effective volume (EV) 50, EV90, and EV95, respectively [11,12]. These effective volumes were speculated by statistical calculation. However, Orebaugh et al. [13] indicated that the results from the DUD may be different from those of the clinical practice, and the comparison of the varied anesthetic volumes in the clinical practice has not been studied in the ultrasound-guided supraclavicular block. The aim of this study was to examine the clinical data according to the varied volumes of local anesthetics in the ultrasound-guided supraclavicular block. aterials and ethods After the approval of Institutional Review Board and obtaining patients' written informed consent, one hundred twenty patients undergoing forearm and hand surgery were randomly assigned to one of four groups to receive ultrasoundguided supraclavicular block with 1% mepivacaine 35 ml (Group 35), 30 ml (), 25 ml (), or 20 ml (). Exclusion criteria included patients with diseases affecting sensory or motor functions of the upper extremity, pregnant patients, allergy to local anesthetics, and contraindication to regional anesthesia. or ultrasound-guided supraclavicular block, an ultrasound machine (Vivid I R, GE Yokogawa edical Systems Ltd., Tokyo, Japan) and a 12 Hz linear type probe were used. The supraclavicular fossa was scanned to locate the subclavian artery and brachial plexus cluster after skin preparation. After local infiltration of skin, a 22 gauge, 5 cm, short beveled insulated needle (Stimuplex R A, B. Braun, elsungen AG, Germany) was advanced from the lateral to medial in the long axis of the ultrasound beam. Once the needle tip was located around the ig. 1. Ultrasound image in the supraclavicular block. SA: subclavian artery, BP: brachial plexus, N: needle. brachial plexus cluster (ig. 1), a nerve stimulator (Stimulpex R, B. Braun, elsungen AG, Germany) was turned on with 2 Hz, starting from 1.0 ma down to 0.5 ma. Local anesthetic was injected in real time with the presence of muscle twitch with the nerve stimulation. If no motor response was obtained, the injection was performed under ultrasound imaging alone without nerve stimulation. In order to avoid intraneural injection, we confirmed that the location of the needle tip was not in the nerves before each injection. However, the needle tip was not always visualized. Therefore, 0.5 ml of 1.5% mepivacaine was injected as a test dose. If patients did not complain of paresthesia or pain, or the injection pressure was not high, the remaining dose of 1.5% mepivacaine was injected incrementally with withdrawing the needle. If local anesthetic did not reach some parts of the brachial plexus, the needle was repositioned until the appropriate image was obtained. We checked the sensory anesthesia with 26 gauge needle every 5 minutes up to 30 minutes after injection of local anesthetic in all 5 cutaneous nerve distributions (musculo cutaneous nerve: lateral side of the forearm, radial nerve: dorsum of the hand over the 2nd metacarpophalangeal joint, ulnar nerve: little finger, median nerve: medial thenar eminence, and medial cutaneous nerve: medial side of the forearm) by a research assistant who was blinded for over 30 minutes after the injection of local anesthetic. The onset of anesthesia was defined as a complete sensory anesthesia in each of the nerve distributions. We analyzed the success rate in two aspects: the success rate of each nerve and all five nerves. The success rate of each nerve was named individual nerve s success rate, and the success rate of all five nerves was termed complete success rate. The successful block of individual nerve was defined as the onset of sensory anesthesia in each nerve s distributions, and a complete successful block was defined as a complete sensory anesthesia in all 5 cutaneous nerve distributions of the forearm at 30 minutes after the local anesthetic injection and operability. Then, all patients were checked for complications such as Horner's syndrome, voice changes, and chest discomfort. The patients who had failed blockades had general anesthesia or sedation with midazolam and pethidine. Statistical analysis was performed with SPSS version 12. The sample size (n = 120) was determined based on the following criteria: a significance level of 5% and a power of 80% from the pilot study. The age, height, weight, and onset time of block were compared among the four groups by one-way analysis of variance (ANOVA) and Tukey post hoc tests. The age, height, weight, and body mass index were also compared between the successful and failed cases. or intergroup comparisons, the distribution of data was first evaluated for normality using the Shapiro-Wilk test. The normally distributed data and non- 495
3 Ultrasound-guided supraclavicular block Vol. 64, No. 6, June 2013 normally distributed data were compared using Student s and ann-whitney test, respectively. The sex, success rate, and the incidence of complications were compared using Chi-square test or isher s exact test. A P value < 0.05 was considered significant. Results One hundred twenty patients were included in this study. There were no differences in the characteristics between the four groups (Table 1). The complete success rates of,, Group 25, and were 96.7%, %, 80.0%, and 66.7%, respectively. The success rate of was lower than that of (P < 0.05) (Table 2). The individual success rate of the ulnar nerve and medial cutaneous nerve were lower than those of other nerves (P < 0.05) (Table 2). The average height and weight in failed cases were larger than those in the successful cases (P < 0.05) (Table 3). In Group 35, one failure was operated under sedation only. In Group 30, one failure was operated under sedation, and another two Table 1. Demographic Data Sex (/) 19/ ± ± ± / ± ± ± / ± ± ± / ± ± ± 11.2 Data are mean ± standard deviation. : supraclavicular block with 35 ml of 1% mepivacaine, : supraclavicular block with 30 ml of 1% mepivacaine, : supraclavicular block with 25 ml of 1% mepivacaine, : supraclavicular block with 20 ml of 1% mepivacaine. failures received general anesthesia. In, four failures were given sedation only, and 2 failures received general anesthesia. In, six failures were operated under sedation only, and four failures received general anesthesia (Table 4). Table 3. Demographic Data of Successful Cases and ailed Cases Total Sex (/) BI (kg m -2 ) Sex (/) BI (kg m -2 ) Sex (/) BI (kg m -2 ) Sex (/) BI (kg m -2 ) Sex (/) BI (kg m -2 ) Successful cases 18/ ± ( ) 63.6 ± ± / ± ± ( ) ( ) 12/ ± ± ± ± / ± ± ± ± /38 46 ( ) 166 ( ) 63.8 ± ± 2.9 ailed cases 1/ / ± 3.8* ± (65-76) ( ) 6/ ± ± 5.2* 76.3 ± 9.3* 24.7 ± 1.9 7/ ± 12.6* ± 10.7* 70.0 ± ± / ( ) ( ) 72.0 ± 9.7* 23.8 ± 1.9 Data are mean ± standard deviation and medians (interquartile range). : supraclavicular block with 35 ml of 1% mepivacaine, : supraclavicular block with 30 ml of 1% mepivacaine, : supraclavicular block with 25 ml of 1% mepivacaine, : supraclavicular block with 20 ml of 1% mepivacaine. *P < 0.05 compared with successful cases, using Student s t-test. P < 0.05 compared with successful cases,using ann-whitney test. Table 2. The Success Rate of Individual Nerve and the Complete Success Rate of All ive Nerves edian nerve Radial nerve usculocutaneous nerve Ulnar nerve edial cutaneous nerve All 5 nerves (Complete successful block) 96.7 (29/30) 96.7 (29/30) 96.7 (29/30) 83.3 (25/30) 80.0 (24/30) 80.0* (24/30) 73.3* (22/30) 70.0* (21/30) 66.7* (20/30) Data are expressed in percents. ( ) = the number of blocked patients/the number of total patients. : supraclavicular block with 35 ml of 1% mepivacaine, : supraclavicular block with 30 ml of 1% mepivacaine, : supraclavicular block with 25 ml of 1% mepivacaine, : supraclavicular block with 20 ml of 1% mepivacaine. *P < 0.05 compared with, using isher s exact test. 496
4 Korean J Anesthesiol Jeon et al. Table 4. Demographic Characteristics of the Patients with an Unsuccessful Block Patients with failed block Sex Age (yr) Height (cm) Weight (kg) Spared nerve Supplementation G35-1 G30-1 G30-2 G30-3 G25-1 G25-2 G25-3 G25-4 G25-5 G25-6 G20-1 G20-2 G20-3 G20-4 G20-5 G20-6 G20-7 G20-8 G20-9 G Ulnar, d.c Ulnar, d.c ed, ulnar, c, d.c Ulnar Ulnar, d.c edian, d.c Ulnar edian, ulnar, radial, c edian, ulnar, d.c Ulnar, d.c edian, ulnar, d.c Ulnar edian, d.c Ulnar, d.c Ulnar, d.c Ulnar, c, d.c G35: supraclavicular block with 35 ml of 1% mepivacaine, G30: supraclavicular block with 30 ml of 1% mepivacaine, G25: supraclavicular block with 25 ml of 1% mepivacaine, G20: supraclavicular block with 20 ml of 1% mepivacaine. : male, : female, ed: median nerve, d.c: medial cutaneous nerve, c: musculocutaneous nerve. Table 5. Onset Time of Each of the ive Terminal Nerves and All ive Nerves Time to onset (min) Sensory distribution edian nerve Radial nerve usculocutaneous nerve Ulnar nerve edial cutaneous nerve All 5 nerves 10.1 ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± 3.7 Data are mean ± standard deviation. : supraclavicular block with 35 ml of 1% mepivacaine, : supraclavicular block with 30 ml of 1% mepivacaine, : supraclavicular block with 25 ml of 1% mepivacaine, : supraclavicular block with 20 ml of 1% mepivacaine. The average onset times of the five nerves were 14.3 ± 6.9 min (), 13.6 ± 4.5 min (), 16.7 ± 4.6 min (Group 25), and 16.5 ± 3.7 min (), respectively. There were no significant differences (Table 5). Horner's syndrome in was higher than other groups (P < 0.05). There was no significant difference in the incidences of chest discomfort and voice change (Table 6). Discussion Systemic local anesthetic toxicity is still frequent and dose dependent. Therefore, reducing the dose of local anesthetic in regional anesthesia can contribute to the safety of regional anesthesia [1]. Some authors demonstrated the possibility Table 6. Incidence of Side Effects in the Block Horner's syndrome Chest discomfort Voice change 76.7 (23/30) 13.3 (4/30) 3.3 (1/30) 43.3* (13/30) 16.7 (5/30) 3.3 (1/30) Group * (13/30) 16.7 (5/30) 0 (0/30) 46.7* (14/30) 6.7 (2/30) 3.3 (1/30) Data are expressed in percents. ( ) = the number of symptomatic patients/the number of total patients. : supraclavicular block with 35 ml of 1% mepivacaine, : supraclavicular block with 30 ml of 1% mepivacaine, : supraclavicular block with 25 ml of 1% mepivacaine, : supraclavicular block with 20 ml of 1% mepivacaine. *P < 0.05 compared with, using Chi-square test. 497
5 Ultrasound-guided supraclavicular block Vol. 64, No. 6, June 2013 of dose reduction in ultrasound-guided axillary blocks and interscalene blocks [7-10]. However, such possibility in ultrasound-guided supraclavicular block is controversial [11,12]. Duggan et al. [11] estimated EV95 and EV50 to be 42 ml and 23 ml, respectively, using DUD. According to the study results, it was concluded that they could not reduce the volume of local anesthetic in ultrasound-guided supraclavicular block. Tran et al. [12] calculated EV90 to be 32 ml, using BUD for ultrasound-guided supraclavicular block in their study. This volume (32 ml) for 90% success rate was lower compared with the conventional technique using 40 ml of local anesthetics. However their results were derived from the estimated values using BUD. The limitations of Duggan et al. s study were the wide confidence interval and no comparison with the conventional supraclavicular block [11]. The limitations of Tran et al. [11] were that the operators were trainees and 16-point scale including motor block was used for definition of successful block [12]. Therefore, we think that their estimated EV90 (32 ml) may be larger than the local anesthetic volume for surgical anesthesia. Orebaugh et al. [13] indicated that the results from DUD do not seem to be easily translated to the clinical practice of peripheral nerve blockade. Therefore, we decided to perform a clinical comparison of the success rates with varied volumes of local anesthetics in ultrasound-guided supraclavicular block. Before the commencement of the study, we planned the study with 40 ml, 35 ml, 30 ml, 25 ml and 20 ml of local anesthetic based on the results (EV 95 = 42 ml, EV90 = 32 ml, and EV 50 = 23 ml) from the previous studies [11,12]. However, the success rate of ultrasound-guided supraclavicular block with local anesthetic 35 ml in the preliminary study was 94.7%, which was similar to EV95 in Duggan et al. [11]. or this reason, we excluded the 40 ml of local anesthetic volume in the study. In general, the volume of local anesthetic for conventional supraclavicular block is known to be 40 ml [14]. A 90.3% success rate was achieved with the traditional technique using 40 ml local anesthetics [15]. Ultrasound-guided techniques allowed for the reduction of the volume to 30 ml of mepivacaine 1% with an equivalent success rate. Therefore, we could state that the volume of local anesthetics could be reduced. In addition, this volume was similar to EV90 (32 ml) from Tran et al. [12]. However, this result was disappointing. We expected to reduce the local anesthetic volume to be 20 ml in ultrasound-guided supraclavicular block before commencing the study, because the minimum effective volume could be reduced to 8-20 ml in the ultrasound-guided axillary blocks [7,8]. We suggest a possible explanation as to why we could not reduce the volume of local anesthetic to be 20 ml as we expected in spite of using ultrasound. Cornish et al. [16,17] injected contrast dye into the tunnel that surrounded brachial plexus and observed various patterns of flow within the tunnel. The dye did not spread homogeneously. With this observation, they asserted that the brachial plexus was surrounded within the rigid-walled tunnel as differently from the simple tubular structure, such as a sheath. In simple tubular structure, the local anesthetic injected at one point can spread throughout the tunnel. However, compartmentalization is present in the rigid tunnel, because the layers of connective tissue are not homogeneous. Therefore, the injection at one point in this rigid-walled tunnel may not spread to other nerves in the tunnel. With this theory, we presumed that the lower volume of local anesthetic was not able to spread to all nerves in this study. At this point, we wondered why the reduction of local anesthetic in ultrasound-guided axillary block could be possible [7,8]. We assumed that four nerves (radial, median, ulnar, musculocutaneous nerve) could be distinguished by ultrasound, and injected 3-5 ml of local anesthetic to each nerve in the axillary region. However, in the supraclavicular region, each nerve could not be distinguished, it is located in the form of a cluster. Therefore, the local anesthetics should be filled in the tunnel, thus permitting no marked reduction in the volume from that used traditionally. We also found that the height and weight were larger in the failed cases (P < 0.05) (Table 3). With this finding, we compared the differences under the condition with same local anesthetic volume (,,, and ). As a result, the height and weight of failed cases were larger in Group 25, and the height of failed cases was larger in. The age in,, and the total patients were lower in the failed cases (P < 0.05). Therefore, the rigid-walled tunnels containing the brachial plexus in the supraclavicular region may be larger in the failed cases, but it is difficult to conclude such with the limited data of this study. Thus, we suggest that further studies should be performed to elucidate the factors influencing the success rate. In our study, the success rates of ulnar and medial cutaneous nerve were lower than those of other nerves. This can be explained by the brachial plexus anatomy and the approach technique used in this study. The ulnar and medial cutaneous nerves are derived from the inferior trunk of brachial plexus. The approach to inferior trunk is difficult by lateral to medial approach in plane used in this study. As the needle advances through the brachial plexus bundle to reach the inferior trunk, there may be a nerve damage. We suggest that different approach techniques (e.g. multiple approach including the out of plane technique) should be applied to increase the success rate with the lower volume of local anesthetics. There were some patients who complained of chest discomfort in this study. However, the chest X-ray was not taken since 498
6 Korean J Anesthesiol Jeon et al. pneumothorax was not a concern, and no patients complained of chest discomfort after the surgery. We presume that transient hemi-diaphragmatic paresis may have occurred in some of the patients with the chest discomfort. In conclusion, we achieved 90% success rate with 30 ml of 1% mepivacaine. This result corresponds to EV90 in the previous study using BUD. Therefore, we suggest 30 ml of local anesthetic volume for the ultrasound-guided supraclavicular block. References 1. Wedel DJ, Horlokcer TT. iller's Anesthesia. 7th ed. Philadelphia, Churchill Living Stone. 2010, p organ GE, ikhail S, urray J. Clinical Anesthesiology. 4th ed. New York, Lange edical Books/cGraw-Hill edical Publishing Division. 2006, p Stone B, Wang R, Price DD. Ultrasound-guided supraclavicular brachial plexus nerve block vs procedural sedation for the treatment of upper extremity emergencies. Am J Emerg ed 2008; 26: Sites BD, Beach L, Spence BC, Wiley CW, Shiffrin J, Hartman GS, et al. Ultrasound guidance improves the success rate of a perivascular axillary plexus block. Acta Anaesthesiol Scand 2006; 50: Kapral S, Krafft P, Eibenberger K, itzgerald R, Gosch, Weinstabl C. Ultrasound-guided supraclavicular approach for regional anesthesia of the brachial plexus. Anesth Analg 1994; 78: Perlas A, Lobo G, Lo N, Brull R, Chan VW, Karkhanis R. Ultrasoundguided supraclavicular block: outcome of 510 consecutive cases. Reg Anesth Pain ed 2009; 34: O'Donnell BD, Ryan H, O'Sullivan O, Iohom G. Ultrasound-guided axillary brachial plexus block with 20 milliliters local anesthetic mixture versus general anesthesia for upper limb trauma surgery: an observer-blinded, prospective, randomized, controlled trial. Anesth Analg 2009; 109: Harper GK, Stafford A, Hill DA. inimum volume of local anaesthetic required to surround each of the constituent nerves of the axillary brachial plexus, using ultrasound guidance: a pilot study. Br J Anaesth 2010; 104: cnaught A, Shastri U, Carmichael N, Awad IT, Columb, Cheung J, et al. Ultrasound reduces the minimum effective local anesthetic volume compared with peripheral nerve stimulation for interscalene block. Br J Anaesth 2011; 106: Kuruba S, Singh SK. Ultrasound reduces the minimum effective local anaesthetic volume. Br J Anaesth 2011; 106: Duggan E, Beheiry HE, Perlas A, Lupu, Nuica A, Chan VW, et al. inimum effective volume of local anesthetic for ultrasoundguided supraclvicular brachial plexus block. Reg Anesth Pain ed 2009; 34: Tran de QH, Dugani S, Correa JA, Dyachenko A, Alsenosy N, inlayson RJ. inimum effective volume of lidocaine for ultrasoundguided supraclavicular block. Reg Anesth Pain ed 2011; 36: Orebaugh SL, Williams BA, Bigeleisen PE. The up-down methodology and practical peripheral nerve blockade. Reg Anesth Pain ed 2010; 35: Jankovic D, Wells C. Regional Nerve Blocks. 2th ed. Vienna, Blackwell Science. 2001, pp Jeon DG, Kim WI. Comparison of a supraclavicular block showing upper arm twitching response with a supraclavicular block showing wrist or finger twitching response. Korean J Anesthesiol 2010; 58: Cornish PB, Leaper CJ, Hahn JL. The "axillary tunnel": an anatomic reappraisal of the limits and dynamics of spread during brachial plexus blockade. Anesth Analg 2007; 104: Cornish PB, Leaper C. The sheath of the brachial plexus: fact or fiction? Anesthesiology 2006; 105:
An evaluation of brachial plexus block using a nerve stimulator versus ultrasound guidance: A randomized controlled trial
 Original Article An evaluation of brachial plexus block using a nerve versus ultrasound guidance: A randomized controlled trial Shivinder Singh, Rakhee Goyal, Kishan Kumar Upadhyay, Navdeep Sethi, Ram
Original Article An evaluation of brachial plexus block using a nerve versus ultrasound guidance: A randomized controlled trial Shivinder Singh, Rakhee Goyal, Kishan Kumar Upadhyay, Navdeep Sethi, Ram
Ultrasound Guided Regional Nerve Blocks
 Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound-guided nerve blocks in the emergency department
 Full Text Online @ www.onlinejets.org Case Series DOI: 10.4103/0974-2700.58655 Ultrasound-guided nerve blocks in the emergency department Sanjeev Bhoi, Amit Chandra 1, Sagar Galwankar 2 Department of Emergency
Full Text Online @ www.onlinejets.org Case Series DOI: 10.4103/0974-2700.58655 Ultrasound-guided nerve blocks in the emergency department Sanjeev Bhoi, Amit Chandra 1, Sagar Galwankar 2 Department of Emergency
Ultrasound guidance showing real-time local anesthetic extravasation during injection of two lateral popliteal sciatic nerve blocks
 CASE REPORT Ultrasound guidance showing real-time local anesthetic extravasation during injection of two lateral popliteal sciatic nerve blocks Brian Osman, Andres Missair, Robyn S. Weisman, Catalina Castillo-Pedraza,
CASE REPORT Ultrasound guidance showing real-time local anesthetic extravasation during injection of two lateral popliteal sciatic nerve blocks Brian Osman, Andres Missair, Robyn S. Weisman, Catalina Castillo-Pedraza,
Estimation of Stellate Ganglion Block Injection Point Using the Cricoid Cartilage as Landmark Through X-ray Review
 Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
ASSESSMENT OF THE ROLE OF DEXAMETHASONE AS AN ADJUVANT IN SUPRACLAVICULAR BLOCK FOR UPPER LIMB SURGERIES
 ORIGINAL ARTICLE ASSESSMENT OF THE ROLE OF DEXAMETHASONE AS AN ADJUVANT IN SUPRACLAVICULAR BLOCK FOR UPPER LIMB SURGERIES Priyesh Bhaskar, Mamta Harjai (e) ISSN Online: 2321-9599 (p) ISSN Print: 2348-6805
ORIGINAL ARTICLE ASSESSMENT OF THE ROLE OF DEXAMETHASONE AS AN ADJUVANT IN SUPRACLAVICULAR BLOCK FOR UPPER LIMB SURGERIES Priyesh Bhaskar, Mamta Harjai (e) ISSN Online: 2321-9599 (p) ISSN Print: 2348-6805
The relationship of the musculocutaneous nerve to the brachial plexus evaluated by MRI
 DOI 10.1007/s10877-015-9807-3 ORIGINAL RESEARCH The relationship of the musculocutaneous nerve to the brachial plexus evaluated by MRI Trygve Kjelstrup 1,2 Axel R. Sauter 3 Per K. Hol 2,4 Received: 23
DOI 10.1007/s10877-015-9807-3 ORIGINAL RESEARCH The relationship of the musculocutaneous nerve to the brachial plexus evaluated by MRI Trygve Kjelstrup 1,2 Axel R. Sauter 3 Per K. Hol 2,4 Received: 23
SUPRACLAVICULAR REGIONAL ANAESTHESIA REANALYSED: THE CORNISH TECHNIQUE
 THE JOURNAL OF NEW YORK SCHOOL OF REGIONAL ANESTHESIA SUPRACLAVICULAR REGIONAL ANAESTHESIA REANALYSED: THE BY CORHISH PB Author Affiliation: Nelson, New Zealand This essay is based on a project which has
THE JOURNAL OF NEW YORK SCHOOL OF REGIONAL ANESTHESIA SUPRACLAVICULAR REGIONAL ANAESTHESIA REANALYSED: THE BY CORHISH PB Author Affiliation: Nelson, New Zealand This essay is based on a project which has
S Kannan, Prem Kumar. Assistant Professor, Saveetha Medical College and Hospital, Chennai.
 Original Article CLINICAL COMPARISON OF TWO DIFFERENT VOLUMES OF 0.5% BUPIVACAINE FOR CLAVICULAR SURGERIES USING COMBINED INTERSCALENE AND SUPERFICIAL CERVICAL PLEXUS BLOCK 2 S Kannan, Prem Kumar,2 Assistant
Original Article CLINICAL COMPARISON OF TWO DIFFERENT VOLUMES OF 0.5% BUPIVACAINE FOR CLAVICULAR SURGERIES USING COMBINED INTERSCALENE AND SUPERFICIAL CERVICAL PLEXUS BLOCK 2 S Kannan, Prem Kumar,2 Assistant
Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block
 Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
Ultrasound-guided supraclavicular block
 THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Assessment of topographic brachial plexus nerves variations at the axilla using ultrasonography
 BJA Advance Access published August, 00 British Journal of Anaesthesia Page of doi:./bja/aep0 Assessment of topographic brachial plexus nerves variations at the axilla using ultrasonography J.-L. Christophe,
BJA Advance Access published August, 00 British Journal of Anaesthesia Page of doi:./bja/aep0 Assessment of topographic brachial plexus nerves variations at the axilla using ultrasonography J.-L. Christophe,
Minimum Effective Volume of Lidocaine for Ultrasound-Guided Infraclavicular Block
 ULTRASOUND ARTICLE Minimum Effective Volume of Lidocaine for Ultrasound-Guided Infraclavicular Block De Q.H. Tran, MD, FRCPC,* Shubada Dugani, MBBS, FRCA,* Alina Dyachenko, MSc,Þ José A. Correa, PhD,þ
ULTRASOUND ARTICLE Minimum Effective Volume of Lidocaine for Ultrasound-Guided Infraclavicular Block De Q.H. Tran, MD, FRCPC,* Shubada Dugani, MBBS, FRCA,* Alina Dyachenko, MSc,Þ José A. Correa, PhD,þ
Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical Trial
 J Arch Mil Med. 1 August; (3): e1977. Published online 1 August 3. DOI: 1.81/jamm.1977 Research Article Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical
J Arch Mil Med. 1 August; (3): e1977. Published online 1 August 3. DOI: 1.81/jamm.1977 Research Article Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical
Intraneural injection during nerve stimulator-guided sciatic nerve block at the popliteal fossa
 British Journal of Anaesthesia 102 (6): 855 61 (2009) doi:10.1093/bja/aep097 Advance Access publication May 6, 2009 Intraneural injection during nerve stimulator-guided sciatic nerve block at the popliteal
British Journal of Anaesthesia 102 (6): 855 61 (2009) doi:10.1093/bja/aep097 Advance Access publication May 6, 2009 Intraneural injection during nerve stimulator-guided sciatic nerve block at the popliteal
Original article: Supraclavicular block with 0.5% levobupivacaine and 0.5% ropivacainecomparative
 Original article: Supraclavicular block with 0.5% levobupivacaine and 0.5% ropivacainecomparative study Dr.V.Sai Dilip 1, Dr.G.Chandra Sekhar 1, Dr.Gopala Krishna Murthy 1, Dr.A.S.Kameswara Rao 1, Dr.K.Sivaji
Original article: Supraclavicular block with 0.5% levobupivacaine and 0.5% ropivacainecomparative study Dr.V.Sai Dilip 1, Dr.G.Chandra Sekhar 1, Dr.Gopala Krishna Murthy 1, Dr.A.S.Kameswara Rao 1, Dr.K.Sivaji
Dr. Georgi Valchev Fellow in regional anaesthesia UZ Leuven
 Dr. Georgi Valchev Fellow in regional anaesthesia UZ Leuven 55 years old woman Latarjetprocedure ASA-1, 49 kg. NKDA Informed consent for RA ISB with catheter uneventful throughout, rate 4/4/60 according
Dr. Georgi Valchev Fellow in regional anaesthesia UZ Leuven 55 years old woman Latarjetprocedure ASA-1, 49 kg. NKDA Informed consent for RA ISB with catheter uneventful throughout, rate 4/4/60 according
Diana Mathioudakis DEAA EDIC AFRCA. consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d)
 & Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
& Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
USRA OF THE UPPER EXTREMITY
 USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
Ultrasound-guided supraclavicular brachial plexus nerve block vs procedural sedation for the treatment of upper extremity emergencies
 American Journal of Emergency Medicine (2008) 26, 706 710 www.elsevier.com/locate/ajem Brief Report Ultrasound-guided supraclavicular brachial plexus nerve vs procedural for the treatment of upper extremity
American Journal of Emergency Medicine (2008) 26, 706 710 www.elsevier.com/locate/ajem Brief Report Ultrasound-guided supraclavicular brachial plexus nerve vs procedural for the treatment of upper extremity
Comparison Of 0.5%Bupivacaine And 0.5% Bupivacaine Plus Buprenorphine in Brachial Plexus Block
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 1 Ver. VIII (Jan. 2016), PP 01-08 www.iosrjournals.org Comparison Of 0.5%Bupivacaine And 0.5%
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 1 Ver. VIII (Jan. 2016), PP 01-08 www.iosrjournals.org Comparison Of 0.5%Bupivacaine And 0.5%
International Journal of Clinical And Diagnostic Research ISSN Volume 3, Issue 2, Mar-Apr 2015.
 Anesthesiology Original Research International Journal of Clinical And Diagnostic Research ISSN 2395-3403 Volume 3, Issue 2, Mar-Apr 2015. Glorigin Lifesciences Private Limited. COMPARISON OF DEXMEDETOMIDINE
Anesthesiology Original Research International Journal of Clinical And Diagnostic Research ISSN 2395-3403 Volume 3, Issue 2, Mar-Apr 2015. Glorigin Lifesciences Private Limited. COMPARISON OF DEXMEDETOMIDINE
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
Comparison of Success Rate of Classical Supraclavicular Brachial Plexus Block with and without Nerve Stimulator
 MVP Journal of Medical Sciences, Vol 4(2), 135 140, July-December 2017 ISSN (Print) : 2348 263X ISSN (Online) : 2348-2648 DOI: 10.18311/mvpjms/2017/v4i2/11033 Comparison of Success Rate of Classical Supraclavicular
MVP Journal of Medical Sciences, Vol 4(2), 135 140, July-December 2017 ISSN (Print) : 2348 263X ISSN (Online) : 2348-2648 DOI: 10.18311/mvpjms/2017/v4i2/11033 Comparison of Success Rate of Classical Supraclavicular
Regional Anaesthesia: Minimizing risk and complications. Mafeitzeral Mamat Anaesthesiology & Critical Care Faculty of Medicine UiTM Sg Buloh
 Regional Anaesthesia: Minimizing risk and complications Mafeitzeral Mamat Anaesthesiology & Critical Care Faculty of Medicine UiTM Sg Buloh Regional anesthesia is an art. Remembering that even experts
Regional Anaesthesia: Minimizing risk and complications Mafeitzeral Mamat Anaesthesiology & Critical Care Faculty of Medicine UiTM Sg Buloh Regional anesthesia is an art. Remembering that even experts
Comparison of clonidine adjuvants to ropivacaine in subclavian perivascular approach of supra clavicular brachial plexus block
 Original Research Article Comparison of clonidine adjuvants to ropivacaine in subclavian perivascular approach of supra clavicular brachial plexus block S. Arul Rajan 1, N. Sathyan 2*, T. Murugan 3 1 Assistant
Original Research Article Comparison of clonidine adjuvants to ropivacaine in subclavian perivascular approach of supra clavicular brachial plexus block S. Arul Rajan 1, N. Sathyan 2*, T. Murugan 3 1 Assistant
DOI: / Page. 1 Dr. Seetharamaiah.S., 2 Dr. G.R.Santhilatha, 3 Dr. T.Venugopala rao, 4 Dr. Venugopalan.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. VII (Sep. 2015), PP 44-48 www.iosrjournals.org To evaluate the efficacy of Inj. Dexmedetomidine
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. VII (Sep. 2015), PP 44-48 www.iosrjournals.org To evaluate the efficacy of Inj. Dexmedetomidine
Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear Transducer
 ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
Current concepts and future trends in ultrasound-guided regional anesthesia Peter Marhofer, Harald Willschke and Stephan Kettner
 Current concepts and future trends in ultrasound-guided regional anesthesia Peter Marhofer, Harald Willschke and Stephan Kettner Department of Anaesthesia and Intensive Care Medicine, Medical University
Current concepts and future trends in ultrasound-guided regional anesthesia Peter Marhofer, Harald Willschke and Stephan Kettner Department of Anaesthesia and Intensive Care Medicine, Medical University
Maaike G. E. Fenten 3, Karin P. W. Schoenmakers 3, Petra J. C. Heesterbeek 2, Gert Jan Scheffer 3 and Rudolf Stienstra 1*
 Fenten et al. BMC Anesthesiology (2015) 15:130 DOI 10.1186/s12871-015-0110-0 RESEARCH ARTICLE Open Access Effect of local anesthetic concentration, dose and volume on the duration of single-injection ultrasound-guided
Fenten et al. BMC Anesthesiology (2015) 15:130 DOI 10.1186/s12871-015-0110-0 RESEARCH ARTICLE Open Access Effect of local anesthetic concentration, dose and volume on the duration of single-injection ultrasound-guided
Plantar Flexion Seems More Reliable than Dorsiflexion with Labat s Sciatic Nerve Block: A Prospective, Randomized Comparison
 Plantar Flexion Seems More Reliable than Dorsiflexion with Labat s Sciatic Nerve Block: A Prospective, Randomized Comparison Manuel Taboada, MD*, Peter G. Atanassoff, MD, Jaime Rodríguez, MD, PhD*, Joaquín
Plantar Flexion Seems More Reliable than Dorsiflexion with Labat s Sciatic Nerve Block: A Prospective, Randomized Comparison Manuel Taboada, MD*, Peter G. Atanassoff, MD, Jaime Rodríguez, MD, PhD*, Joaquín
A Comparative Evaluation of Techniques in Interscalene Brachial Plexus Block: Conventional blind, Nerve Stimulator Guided and Ultrasound Guided.
 DOI: 10.21276/aimdr.2016.2.3.16 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 A Comparative Evaluation of Techniques in Interscalene Brachial Plexus Block: Conventional blind, Nerve Stimulator
DOI: 10.21276/aimdr.2016.2.3.16 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 A Comparative Evaluation of Techniques in Interscalene Brachial Plexus Block: Conventional blind, Nerve Stimulator
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
A New Anterior Approach for Fluoroscopy-guided Suprascapular Nerve Block
 Original Article Korean J Pain 2012 July; Vol. 25, No. 3: 168-172 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.3.168 A New Anterior Approach for Fluoroscopy-guided Suprascapular
Original Article Korean J Pain 2012 July; Vol. 25, No. 3: 168-172 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.3.168 A New Anterior Approach for Fluoroscopy-guided Suprascapular
ISPUB.COM. Sonoanatomy Of The Ulnar Nerve In The Distal Forearm. A Thallaj, A El-Dawlatly, A Turkistani, O Zoraigi, M Shraf al-deen INTRODUCTION
 ISPUB.COM The Internet Journal of Anesthesiology Volume 15 Number 1 Sonoanatomy Of The Ulnar Nerve In The Distal Forearm A Thallaj, A El-Dawlatly, A Turkistani, O Zoraigi, M Shraf al-deen Citation A Thallaj,
ISPUB.COM The Internet Journal of Anesthesiology Volume 15 Number 1 Sonoanatomy Of The Ulnar Nerve In The Distal Forearm A Thallaj, A El-Dawlatly, A Turkistani, O Zoraigi, M Shraf al-deen Citation A Thallaj,
Ultrasound Guided Regional Anesthesia UGRA. Aric C Bunch, CRNA, MSN, CEN, EMT-P
 Ultrasound Guided Regional Anesthesia UGRA Aric C Bunch, CRNA, MSN, CEN, EMT-P Aric C Bunch Staff CRNA at Crozer Chester Medical Center and affiliated sites Adjunct Instructor Villanova University Staff
Ultrasound Guided Regional Anesthesia UGRA Aric C Bunch, CRNA, MSN, CEN, EMT-P Aric C Bunch Staff CRNA at Crozer Chester Medical Center and affiliated sites Adjunct Instructor Villanova University Staff
Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain
 International Journal of Anesthesiology Research, 2015, 3, 37-43 37 Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain Michael Meng 1, Reid
International Journal of Anesthesiology Research, 2015, 3, 37-43 37 Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain Michael Meng 1, Reid
Review Article Axillary Brachial Plexus Block
 Anesthesiology Research and Practice Volume 2011, Article ID 173796, 5 pages doi:10.1155/2011/173796 Review Article Axillary Brachial Plexus Block Ashish R. Satapathy and David M. Coventry Department of
Anesthesiology Research and Practice Volume 2011, Article ID 173796, 5 pages doi:10.1155/2011/173796 Review Article Axillary Brachial Plexus Block Ashish R. Satapathy and David M. Coventry Department of
Induction position for spinal anaesthesia: Sitting versus lateral position
 11 ORIGINAL ARTICLE Induction position for spinal anaesthesia: Sitting versus lateral position Khurrum Shahzad, Gauhar Afshan Abstract Objective: To compare the effect of induction position on block characteristics
11 ORIGINAL ARTICLE Induction position for spinal anaesthesia: Sitting versus lateral position Khurrum Shahzad, Gauhar Afshan Abstract Objective: To compare the effect of induction position on block characteristics
WITH ISOBARIC BUPIVACAINE (5 MG/ML)
 , 49, 2013, 3 63 (5 MG/ML) (5 MG/ML).,.,.,..,..,, SPINAL ANESTHESIA: COMPARISON OF ISOBARIC ROPIVACAINE (5 MG/ML) WITH ISOBARIC BUPIVACAINE (5 MG/ML) D. Tzoneva, Vl. Miladinov, Al. Todorov, M. P. Atanasova,
, 49, 2013, 3 63 (5 MG/ML) (5 MG/ML).,.,.,..,..,, SPINAL ANESTHESIA: COMPARISON OF ISOBARIC ROPIVACAINE (5 MG/ML) WITH ISOBARIC BUPIVACAINE (5 MG/ML) D. Tzoneva, Vl. Miladinov, Al. Todorov, M. P. Atanasova,
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology University of Washington, Seattle, WA
 ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
ULTRASOUND-GUIDED peripheral
 392 392 CANADIAN JOURNAL OF ANESTHESIA Images in Anesthesia Cadaveric ultrasound imaging for training in ultrasound-guided peripheral nerve blocks: upper extremity ULTRASOUND-GUIDED peripheral nerve blocks
392 392 CANADIAN JOURNAL OF ANESTHESIA Images in Anesthesia Cadaveric ultrasound imaging for training in ultrasound-guided peripheral nerve blocks: upper extremity ULTRASOUND-GUIDED peripheral nerve blocks
Addition of dexmedetomidine to bupivacaine in supraclavicular brachial plexus block
 ORIGINAL RESEARCH Recep Aksu, MD, Associate Professor Cihangir Bicer, MD, Associate Professor Department of Anesthesiology, Erciyes University, Medical Faculty, Kayseri, Turkey Addition of dexmedetomidine
ORIGINAL RESEARCH Recep Aksu, MD, Associate Professor Cihangir Bicer, MD, Associate Professor Department of Anesthesiology, Erciyes University, Medical Faculty, Kayseri, Turkey Addition of dexmedetomidine
Nerves of Upper limb. Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh
 Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
REVIEW ARTICLE Fifteen years of ultrasound guidance in regional anaesthesia: Part 1
 British Journal of Anaesthesia 104 (5): 538 46 (2010) doi:10.1093/bja/aeq069 Advance Access publication April 2, 2010 REVIEW ARTICLE Fifteen years of ultrasound guidance in regional anaesthesia: Part 1
British Journal of Anaesthesia 104 (5): 538 46 (2010) doi:10.1093/bja/aeq069 Advance Access publication April 2, 2010 REVIEW ARTICLE Fifteen years of ultrasound guidance in regional anaesthesia: Part 1
Comparison of single and triple injection methods for ultrasound guided interscalene brachial plexus blockade
 3006 EXPERIMENTAL AND THERAPEUTIC MEDICINE 15: 3006-3011, 2018 Comparison of single and triple injection methods for ultrasound guided interscalene brachial plexus blockade CUN JIN WANG *, YA LI GE *,
3006 EXPERIMENTAL AND THERAPEUTIC MEDICINE 15: 3006-3011, 2018 Comparison of single and triple injection methods for ultrasound guided interscalene brachial plexus blockade CUN JIN WANG *, YA LI GE *,
Sign up to receive ATOTW weekly
 PERIPHERAL NERVE BLOCKS GETTING STARTED ANAESTHESIA TUTORIAL OF THE WEEK 134 PUBLICATION DATE 18/05/09 Dr Kim Russon, Consultant Anaesthetist Dr Helen Findley, ST3 Anaesthetics Dr Zoe Harclerode, ST3 Anaesthetics
PERIPHERAL NERVE BLOCKS GETTING STARTED ANAESTHESIA TUTORIAL OF THE WEEK 134 PUBLICATION DATE 18/05/09 Dr Kim Russon, Consultant Anaesthetist Dr Helen Findley, ST3 Anaesthetics Dr Zoe Harclerode, ST3 Anaesthetics
The Comparison of the Result of Epiduroscopic Laser Neural Decompression between FBSS or Not
 Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Research Article A Comparative Study of Interscalene and Supraclavicular Approach of Brachial Plexus Block on Upper Limb Surgeries
 Cronicon OPEN ACCESS ANAESTHESIA Research Article A Comparative Study of Interscalene and Supraclavicular Approach of Brachial Plexus Block on Upper Limb Surgeries Susmita Bhattacharyya, KalyanBrata Mandal,
Cronicon OPEN ACCESS ANAESTHESIA Research Article A Comparative Study of Interscalene and Supraclavicular Approach of Brachial Plexus Block on Upper Limb Surgeries Susmita Bhattacharyya, KalyanBrata Mandal,
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Patient consent for peripheral nerve blocks
 Patient consent for peripheral nerve blocks 1 Membership of Working Party Dr Anand Sardesai Dr James French Dr Amit Pawa Consultant Anaesthetist, Cambridge, UK Consultant Anaesthetist, Nottingham, UK Consultant
Patient consent for peripheral nerve blocks 1 Membership of Working Party Dr Anand Sardesai Dr James French Dr Amit Pawa Consultant Anaesthetist, Cambridge, UK Consultant Anaesthetist, Nottingham, UK Consultant
Nerves of the upper limb Prof. Abdulameer Al-Nuaimi. E. mail:
 Nerves of the upper limb Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Brachial plexus Median nerve After originating from the brachial plexus in the axilla,
Nerves of the upper limb Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Brachial plexus Median nerve After originating from the brachial plexus in the axilla,
British Journal of Anaesthesia 98 (6): (2007) doi: /bja/aem100 Advance Access publication May 3, 2007 REGIONAL ANAESTHESIA Effects of ultr
 British Journal of Anaesthesia 98 (6): 823 7 (2007) doi:10.1093/bja/aem100 Advance Access publication May 3, 2007 REGIONAL ANAESTHESIA Effects of ultrasound guidance on the minimum effective anaesthetic
British Journal of Anaesthesia 98 (6): 823 7 (2007) doi:10.1093/bja/aem100 Advance Access publication May 3, 2007 REGIONAL ANAESTHESIA Effects of ultrasound guidance on the minimum effective anaesthetic
Guidance for Multiple Injection Axillary Brachial Plexus Block
 A Prospective, Randomized Comparison between Ultrasound versus Ultrasound with Nerve Stimulation Guidance for Multiple Injection Axillary Brachial Plexus Block Mostafa Muhammed Sabra, Ali Fotoh Ali El
A Prospective, Randomized Comparison between Ultrasound versus Ultrasound with Nerve Stimulation Guidance for Multiple Injection Axillary Brachial Plexus Block Mostafa Muhammed Sabra, Ali Fotoh Ali El
Ultrasound in Peripheral Nerve Interventions
 Ultrasound in Peripheral Nerve Interventions John L. Lin, M.D. Shepherd Center Assistant Clinical Professor Emory University, School of Medicine Outline Ultrasound basics Nerve blocks in physiatric setting
Ultrasound in Peripheral Nerve Interventions John L. Lin, M.D. Shepherd Center Assistant Clinical Professor Emory University, School of Medicine Outline Ultrasound basics Nerve blocks in physiatric setting
NerveGuard Automatic system for injection pressure limitation
 Automatic system for injection pressure limitation Peripheral nerve blocks 1 MADE IN GERMANY Causes and approaches Avoiding nerve damage during peripheral nerve blocks Ultrasound-guided localisation of
Automatic system for injection pressure limitation Peripheral nerve blocks 1 MADE IN GERMANY Causes and approaches Avoiding nerve damage during peripheral nerve blocks Ultrasound-guided localisation of
Anesthetic Efficacy of Different Ropivacaine Concentrations for Inferior Alveolar Nerve Block
 SCIENTIFIC REPORT Anesthetic Efficacy of Different Ropivacaine Concentrations for Inferior Alveolar Nerve Block Eman El-Sharrawy, MBBCh, MSc, MD,* and John A. Yagiela, DDS, PhD *Faculty of Dentistry, Tanta
SCIENTIFIC REPORT Anesthetic Efficacy of Different Ropivacaine Concentrations for Inferior Alveolar Nerve Block Eman El-Sharrawy, MBBCh, MSc, MD,* and John A. Yagiela, DDS, PhD *Faculty of Dentistry, Tanta
Ultrasound identification of nerve cords in the infraclavicular fossa: a clinical study
 O R I G I N A L A R T I C L E Ultrasound identification of nerve cords in the infraclavicular fossa: a clinical study A. DI FILIPPO 1, S. ORANDO 1, A. LUNA 1, L. GIANESELLO 2, A. BOCCACCINI 2, M. C. CAMPOLO
O R I G I N A L A R T I C L E Ultrasound identification of nerve cords in the infraclavicular fossa: a clinical study A. DI FILIPPO 1, S. ORANDO 1, A. LUNA 1, L. GIANESELLO 2, A. BOCCACCINI 2, M. C. CAMPOLO
ORIGINAL ARTICLE. S. S. Liu, 1 J. T. YaDeau, 2 P. M. Shaw, 3 S. Wilfred, 4 T. Shetty 5 and M. Gordon 6
 doi:10.1111/j.1365-2044.2011.06619.x ORIGINAL ARTICLE Incidence of unintentional intraneural injection and postoperative neurological complications with ultrasoundguided interscalene and supraclavicular
doi:10.1111/j.1365-2044.2011.06619.x ORIGINAL ARTICLE Incidence of unintentional intraneural injection and postoperative neurological complications with ultrasoundguided interscalene and supraclavicular
Lidocaine use in ultrasound-guided femoral nerve block: what is the minimum effective anaesthetic concentration (MEAC 90 )?
 British Journal of Anaesthesia 110 (6): 1040 4 (2013) Advance Access publication 5 February 2013. doi:10.1093/bja/aes595 REGIONAL ANAESTHESIA Lidocaine use in ultrasound-guided femoral nerve block: what
British Journal of Anaesthesia 110 (6): 1040 4 (2013) Advance Access publication 5 February 2013. doi:10.1093/bja/aes595 REGIONAL ANAESTHESIA Lidocaine use in ultrasound-guided femoral nerve block: what
NerveGuard Automatic system for injection pressure limitation
 NerveGuard Automatic system for injection pressure limitation Peripheral nerve blocks MADE IN GERMANY Causes and approaches Avoiding nerve damage during peripheral nerve blocks Ultrasound-guided localisation
NerveGuard Automatic system for injection pressure limitation Peripheral nerve blocks MADE IN GERMANY Causes and approaches Avoiding nerve damage during peripheral nerve blocks Ultrasound-guided localisation
Dexamethasone or Dexmedetomidine as Local Anesthetic Adjuvants for Ultrasound-guided Axillary Brachial Plexus Blocks with Nerve Stimulation
 Original Article Korean J Pain 2016 January; Vol. 29, No. 1: 29-33 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2016.29.1.29 Dexamethasone or Dexmedetomidine as Local Anesthetic Adjuvants
Original Article Korean J Pain 2016 January; Vol. 29, No. 1: 29-33 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2016.29.1.29 Dexamethasone or Dexmedetomidine as Local Anesthetic Adjuvants
Citation for published version (APA): Wegener, J. T. (2013). Educational and clinical aspects of peripheral nerve blockade
 UvA-DARE (Digital Academic Repository) Educational and clinical aspects of peripheral nerve blockade Wegener, Jessica Link to publication Citation for published version (APA): Wegener, J. T. (2013). Educational
UvA-DARE (Digital Academic Repository) Educational and clinical aspects of peripheral nerve blockade Wegener, Jessica Link to publication Citation for published version (APA): Wegener, J. T. (2013). Educational
C HAPTER 6 Peripheral Nerve Blocks. Viveta Lobo, MD Arun Nagdev, MD Laleh Gharahbaghian, MD
 C HAPTER 6 Peripheral Nerve Blocks Viveta Lobo, MD Arun Nagdev, MD Laleh Gharahbaghian, MD SECTION 1 Introduction INDICATIONS Acute pain is a common emergency department (ED) complaint with emergency physicians
C HAPTER 6 Peripheral Nerve Blocks Viveta Lobo, MD Arun Nagdev, MD Laleh Gharahbaghian, MD SECTION 1 Introduction INDICATIONS Acute pain is a common emergency department (ED) complaint with emergency physicians
inerve Guide to Nerves 2009
 inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
Peripheral nerve blocks in children
 Peripheral nerve blocks in children Peter Marhofer, MD Department of Anaesthesia and Intensive Care Medicine, Medical University Vienna A-1090 Vienna, Austria, Europe peter.marhofer@meduniwien.ac.at www.sono-nerve.com
Peripheral nerve blocks in children Peter Marhofer, MD Department of Anaesthesia and Intensive Care Medicine, Medical University Vienna A-1090 Vienna, Austria, Europe peter.marhofer@meduniwien.ac.at www.sono-nerve.com
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
JOURNAL OF PHARMACEUTICAL AND BIOMEDICAL SCIENCES
 JOURNAL OF PHARMACEUTICAL AND BIOMEDICAL SCIENCES Singh R, Bisoi P, Mohanty SN, Debata PC. Study On Effect of Dexmedetomidine When Added To Bupivacaine On The Onset Time And Duration Of Block In Supraclavicular
JOURNAL OF PHARMACEUTICAL AND BIOMEDICAL SCIENCES Singh R, Bisoi P, Mohanty SN, Debata PC. Study On Effect of Dexmedetomidine When Added To Bupivacaine On The Onset Time And Duration Of Block In Supraclavicular
Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report
 SHORT REPORT Eur J Anat, 10 (3): 61-66 (2006) Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report K. Ramachandran, I. Kanakasabapathy and
SHORT REPORT Eur J Anat, 10 (3): 61-66 (2006) Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report K. Ramachandran, I. Kanakasabapathy and
Distribution of Local Anesthetic in Axillary Brachial Plexus Block
 Anesthesiology 2002; 96:1315 24 2002 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Distribution of Local Anesthetic in Axillary Brachial Plexus Block A Clinical and Magnetic
Anesthesiology 2002; 96:1315 24 2002 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Distribution of Local Anesthetic in Axillary Brachial Plexus Block A Clinical and Magnetic
Interscalene brachial plexus blockade - indications, anatomy, practical performance
 08RC2 Interscalene brachial plexus blockade - indications, anatomy, practical performance Urs Eichenberger Department of Anaesthesiology and Pain Therapy, University Hospital of Bern, Switzerland Saturday,
08RC2 Interscalene brachial plexus blockade - indications, anatomy, practical performance Urs Eichenberger Department of Anaesthesiology and Pain Therapy, University Hospital of Bern, Switzerland Saturday,
Pneumothorax Post Brachial Plexus Block Guided by Ultrasound: a Case Report
 Rev Bras Anestesiol 2012; 62: 5: 741-747 CLINICAL INFORMATION CLINICAL INFORMATION Pneumothorax Post Brachial Plexus Block Guided by Ultrasound: a Case Report Beatriz L. S. Mandim 1, Rodrigo R. Alves 2,
Rev Bras Anestesiol 2012; 62: 5: 741-747 CLINICAL INFORMATION CLINICAL INFORMATION Pneumothorax Post Brachial Plexus Block Guided by Ultrasound: a Case Report Beatriz L. S. Mandim 1, Rodrigo R. Alves 2,
This qualitative systematic review will summarize the existing
 REVIEW ARTICLE Ultrasound and Review of Evidence for Lower Extremity Peripheral Nerve Blocks Francis V. Salinas, MD Abstract: This qualitative systematic review summarizes existing evidence from randomized
REVIEW ARTICLE Ultrasound and Review of Evidence for Lower Extremity Peripheral Nerve Blocks Francis V. Salinas, MD Abstract: This qualitative systematic review summarizes existing evidence from randomized
Ultrasound-guided Supraclavicular Nerve Block In-plane Technique: Comparison of Conventional vs Skin Wheal Standoff Technique
 ORIGINAL ARTICLE Ultrasound-guided Supraclavicular 10.5005/jp-journals-10046-0061 Nerve Block In-plane Technique Ultrasound-guided Supraclavicular Nerve Block In-plane Technique: Comparison of Conventional
ORIGINAL ARTICLE Ultrasound-guided Supraclavicular 10.5005/jp-journals-10046-0061 Nerve Block In-plane Technique Ultrasound-guided Supraclavicular Nerve Block In-plane Technique: Comparison of Conventional
USRA OF THE LOWER EXTREMITY
 USRA OF THE LOWER EXTREMITY Christian R. Falyar, CRNA, DNAP Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE LOWER EXTREMITY Christian R. Falyar, CRNA, DNAP Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
Nerve Injury. 1) Upper Lesions of the Brachial Plexus called Erb- Duchene Palsy or syndrome.
 Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
(Senior Resident, Dept of Anaesthesia, Dr. D. Y. Patil Medical College, Dr. D. Y. Patil Vidyapeeth [DPU], Pune)
![(Senior Resident, Dept of Anaesthesia, Dr. D. Y. Patil Medical College, Dr. D. Y. Patil Vidyapeeth [DPU], Pune) (Senior Resident, Dept of Anaesthesia, Dr. D. Y. Patil Medical College, Dr. D. Y. Patil Vidyapeeth [DPU], Pune)](/thumbs/82/85649280.jpg) IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 25-29 www.iosrjournals.org To Compare the Efficacy of Dexamethasone
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 25-29 www.iosrjournals.org To Compare the Efficacy of Dexamethasone
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist
 Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
CHAPTER 5 Femoral Nerve Block. Arun Nagdev, MD Mike Mallin, MD, RDCS, RDMS
 CHAPTER 5 Femoral Nerve Block Arun Nagdev, MD Mike Mallin, MD, RDCS, RDMS SECTION 1 Introduction An ultrasound-guided femoral nerve block (USFNB) can be a rapid and definitive tool for pain control for
CHAPTER 5 Femoral Nerve Block Arun Nagdev, MD Mike Mallin, MD, RDCS, RDMS SECTION 1 Introduction An ultrasound-guided femoral nerve block (USFNB) can be a rapid and definitive tool for pain control for
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Vascular Access (venous (peripheral and central) and arterial)
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Basics of US Regional Anaesthesia. November 2008
 Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
INTRODUCTION. Getting the best scan. Choosing a probe. Choosing the frequency
 Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination
Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination
The infraclavicular brachial plexus block by the coracoid approach is clinically effective: an observational study of 150 patients
 253 Regional Anesthesia and Pain The infraclavicular brachial plexus block by the coracoid approach is clinically effective: an observational study of 150 patients [Le bloc infraclaviculaire du plexus
253 Regional Anesthesia and Pain The infraclavicular brachial plexus block by the coracoid approach is clinically effective: an observational study of 150 patients [Le bloc infraclaviculaire du plexus
Review Article Ultrasound-Guided Regional Anesthesia for Procedures of the Upper Extremity
 Anesthesiology Research and Practice Volume 2011, Article ID 579824, 6 pages doi:10.1155/2011/579824 Review Article Ultrasound-Guided Regional Anesthesia for Procedures of the Upper Extremity Farheen Mirza
Anesthesiology Research and Practice Volume 2011, Article ID 579824, 6 pages doi:10.1155/2011/579824 Review Article Ultrasound-Guided Regional Anesthesia for Procedures of the Upper Extremity Farheen Mirza
Brachial Plexus Block, a Comparison of Nerve Locator versus Paresthesia Technique
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. X. (Feb. 2014), PP 06-10 Brachial Plexus Block, a Comparison of Nerve Locator versus
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. X. (Feb. 2014), PP 06-10 Brachial Plexus Block, a Comparison of Nerve Locator versus
Gi-Soo Lee, Chan Kang*, You Gun Won, Byung-Hak Oh, June-Bum Jun
 Comparison of Postoperative Pain Control Methods After Bony Surgery In the Foot And Ankle Gi-Soo Lee, Chan Kang*, You Gun Won, Byung-Hak Oh, June-Bum Jun Department of Orthopedic Surgery, College of Medicine,
Comparison of Postoperative Pain Control Methods After Bony Surgery In the Foot And Ankle Gi-Soo Lee, Chan Kang*, You Gun Won, Byung-Hak Oh, June-Bum Jun Department of Orthopedic Surgery, College of Medicine,
Anesthesia & Pain Research
 Research Article Anesthesia & Pain Research ISSN 2639-846X Topical 2% Gel for Analgesia and Patient Comfort during Interscalene Brachial Plexus and Axillary Blocks: A Noninferiority Randomized Trial Bouts
Research Article Anesthesia & Pain Research ISSN 2639-846X Topical 2% Gel for Analgesia and Patient Comfort during Interscalene Brachial Plexus and Axillary Blocks: A Noninferiority Randomized Trial Bouts
Original Research Article. Kiran Kumar G. V. 1, Rammohan Gurram 1, Gajanan Fultambkar 1 *, Amit Omprakash Gupta 2, Onkar C.
 International Journal of Research in Medical Sciences Kumar KGV et al. Int J Res Med Sci. 2018 Jul;6(7):2503-2507 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20182844
International Journal of Research in Medical Sciences Kumar KGV et al. Int J Res Med Sci. 2018 Jul;6(7):2503-2507 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20182844
The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (7), Page
 The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (7), Page 1655-1662 Effect of Adding Ketamine as An Adjuvant to Lidocaine in Ultrasound Guided Supraclavicular Brachial Plexus Block Mohamed
The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (7), Page 1655-1662 Effect of Adding Ketamine as An Adjuvant to Lidocaine in Ultrasound Guided Supraclavicular Brachial Plexus Block Mohamed
Ultrasound Guided Lower Extremity Blocks
 Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
*the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone
 *the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone - muscles in the arm : *brachialis muscle *Biceps brachii
*the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone - muscles in the arm : *brachialis muscle *Biceps brachii
*Our main subject is the brachial plexus but it's important to understand the spinal cord first in order to understand the brachial plexus.
 *Our main subject is the brachial plexus but it's important to understand the spinal cord first in order to understand the brachial plexus. *Vertebral column is formed by the union of 33 sequential vertebrae
*Our main subject is the brachial plexus but it's important to understand the spinal cord first in order to understand the brachial plexus. *Vertebral column is formed by the union of 33 sequential vertebrae
Regional Anesthesia for Children in the Twenty-First Century
 Curr Anesthesiol Rep (2013) 3:49 56 DOI 10.1007/s40140-012-0003-4 PEDIATRIC ANESTHESIA (J LERMAN, SECTION EDITOR) Regional Anesthesia for Children in the Twenty-First Century Amod Sawardekar Santhanam
Curr Anesthesiol Rep (2013) 3:49 56 DOI 10.1007/s40140-012-0003-4 PEDIATRIC ANESTHESIA (J LERMAN, SECTION EDITOR) Regional Anesthesia for Children in the Twenty-First Century Amod Sawardekar Santhanam
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics
 Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
Ultrasound-Guided Regional Anesthesia for Peripheral Nerve Blocks: An Evidence- Based Outcome Review
 Ultrasound-Guided Regional Anesthesia for Peripheral Nerve Blocks: An Evidence- Based Outcome Review John G. Antonakakis, MD a, *, Paul H. Ting, MD b, Brian Sites, MD c KEYWORD Ultrasonography Regional
Ultrasound-Guided Regional Anesthesia for Peripheral Nerve Blocks: An Evidence- Based Outcome Review John G. Antonakakis, MD a, *, Paul H. Ting, MD b, Brian Sites, MD c KEYWORD Ultrasonography Regional
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5. September 30, 2011
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
The arm: *For images refer back to the slides
 The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
