SAQs for Dentistry. Third Edition
|
|
|
- Amanda McKenzie
- 5 years ago
- Views:
Transcription
1 SAQs for Dentistry Third Edition Kathleen F M Fan PhD, MBBS, BDS, FDSRCS (Eng), FRCS (Ed), FRCS (OMFS) Consultant Oral and Maxillofacial Surgeon, Honorary Senior Lecturer King s College Hospital, London Judith Jones BDS, MSc, FDSRCS (Eng), PhD, FDS (OS), FHEA Reader / Honorary Consultant, Department of Oral and Maxillofacial Surgery, Queen Mary University of London, Barts and the London School of Medicine and Dentistry, Institute of Dentistry
2 Contents List of Contributors Introduction vi vii 1 Child Dental Health and Orthodontics 1 2 Restorative Dentistry 49 3 Oral Surgery Oral Medicine Oral Pathology Oral Radiography/Radiology Human Disease and Therapeutics General Dentistry 383 Index 439
3 3 Oral Surgery
4 ORAL SURGERY Local anaesthetics (a) You plan to extract a lower left first permanent molar tooth on a fit and healthy 34-year-old patient using 25% lidocaine with adrenaline 1: You plan to carry out an inferior dental/alveolar block, but what other nerves will you need to anaesthetise for the extraction to be carried out, and which injections will you give to achieve this? (b) Once you have given your injections how will you test each nerve to see whether it is anaesthetised? (c) What are the techniques for giving an inferior dental/alveolar block? Please give an advantage and disadvantage for each of the techniques. (d) The patient is still feeling discomfort when you try to elevate the tooth. What alternative techniques or anaesthetic agents could you try?
5 162 ORAL SURGERY Answer 3.1 (a) An inferior dental (alveolar) block (IDB) of the nerves will anaesthetise the pulp of the tooth to be extracted. Which technique is used (see section c) for an IDB will determine whether you need to use other injection techniques, eg with certain high IDBs the long buccal nerve is blocked at the same time as the inferior dental/alveolar nerve. Hence, if not already anaesthetised, the long buccal nerve will need to be anaesthetised, because this supplies the buccal tissues adjacent to the tooth. You will also need to anaesthetise the lingual nerve because this supplies the lingual tissues adjacent to the tooth, and can be given at the same time as the IDB. (b) To test that the various injection techniques have been successful, you will need to probe in different areas. Probing in the buccal gingival sulcus of the lower first permanent molar to be extracted will test whether the long buccal nerve has been anaesthetised. Probing in the lingual gingival sulcus of the lower first permanent molar to be extracted will test whether the lingual nerve has been anaesthetised. Hence it is necessary to probe at another site to determine whether your IDB has been successful. As the buccal mucosa anterior to the mental foramen will be anaesthetised in a successful IDB, this area can be probed to determine whether the inferior dental/alveolar nerve has been successfully anaesthetised. However, care must be taken not to do this too close to the midine, because there is crossover supply from fibres on the contralateral side and a false-negative result may occur. (c) IDB techniques are shown below.
6 ORAL SURGERY 163 Technique of IDB Advantages Disadvantages Direct technique, also known as Halstead s technique Simple If needle inserted in wrong position, may encounter internal oblique ridge and prevent advancement to lingula Indirect technique Gets round the problem of hitting the internal oblique ridge on insertion of the needle More movement of needle within tissues Anterior ramus technique Can be done in patients with limited mouth opening Needle movement in the tissues Gow Gates technique Blocks the long buccal nerve at same time, as well as accessory nerve supplies such as the mylohyoid and auricular temporal nerves Takes longer to work because the nerve trunk is larger at this point Possibility of intravascular injection into maxillary or middle meningeal arteries or veins Akinosi technique Can be done in patients with limited mouth opening Blocks long buccal nerve at same time, as well as accessory nerve supplies such as the mylohyoid and auricular temporal nerves Takes longer to work because the nerve trunk is larger at this point Possibility of intravascular injection into maxillary or middle meningeal arteries or veins (d) Other techniques that could be used: Intraligamentous injection Intraosseous injection Other agents: lidocaine is the gold standard dental local anaesthetic, but in refractory cases it is possible to use articaine as an alternative/ adjunctive anaesthetic agent. As a 4% solution, it is stronger than lidocaine and often helps anaesthesia to be achieved in difficult cases.
7 164 ORAL SURGERY 3.2 (a) You are seeing a patient who needs to have a tooth surgically removed in your practice. One of the principles of flap design is that vital structures should be avoided. Name two vital structures that you should avoid when carrying out surgical tooth removal in the maxilla and the mandible. (b) What are the other principles to which you should adhere when designing a mucoperiosteal flap for surgical tooth extraction? (c) You wish to remove a lower left, second premolar tooth; a diagram of the tooth to be removed is shown. Please draw on it where you would place your incisions and explain your reasons for siting them there.
8 ORAL SURGERY 165 (d) After the procedure you wish to suture the wound. What functions do sutures perform? (e) Name two different sutures that could be used to suture an intraoral wound and an advantage of each.
9 166 ORAL SURGERY Answer 3.2 (a) Maxilla: greater palatine artery; nasopalatine nerves and arteries Mandible: lingual nerve and mental nerve (b) Mucoperisoteal flaps that are raised when surgically removing a tooth need to: Provide adequate access to the surgical site Retain a good blood supply to the mucoperiosteal flap, so the base must be broader than the apex, unless the flap includes a decentsized artery within the flap Avoid vital structures such as local nerves and blood vessels Have their margins placed on sound bone and not over the area where you are removing bone Be able to be extended if necessary Be able to be closed appropriately at the end of the operation (c) There is no single universally accepted flap design. However, so long as the principles of flap design are adhered to, then the design will be appropriate. When designing a flap in this area two- or three-sided flaps are appropriate and, depending on preference, some operators will place the relieving incision in a two-sided flap mesially, whereas others will place it distally. It is important to include the whole interdental papilla in the flap to make suturing at the end easier. The relieving incisions must be flared to ensure a larger base than apex for a good blood supply. In the figure are two designs: one a three-sided flap and the other a two-sided flap with a mesial relieving incision.
10 ORAL SURGERY 167 (d) Sutures primarily approximate and hold the wound margins in the appropriate place to enable them to heal. The smaller the space between the two wound margins, the quicker the wound will heal. Sutures will help in holding the mucoperiosteal flap over bone, which will reduce the risk of it becoming non-vital. Sutures also help haemostasis. (e) Non-resorbable: braided: black silk soft and easy to knot monofilament: Prolene hygienic Resorbable: braided: polyglactin (Vicryl) or Polysorb, which is a glycolide/ lactide co-polymer soft, easy to knot, resorbs so patient does not need to have sutures removed monofilament: poliglecaprone 25 (Monocryl) hygienic, resorbable but slow resorption
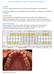
11 168 ORAL SURGERY 3.3 (a) A fit and healthy patient presents to your surgery complaining of recurrent episodes of pain and swelling of the gum in the region of an impacted, lower right wisdom tooth. What is the most likely diagnosis? (b) A radiograph of the tooth involved is shown here. How would you describe the position of the tooth?
12 ORAL SURGERY 169 (c) What is the relationship of the inferior dental canal to the tooth, as judged by this radiographic view? What are the likely implications of this appearance and how would you proceed? (d) Coronectomy: what is the rationale behind a coronectomy and what are the complications of carrying it out?
13 170 ORAL SURGERY Answer 3.3 (a) Recurrent pericoronitis (b) Mesioangularly impacted and partially erupted (c) The inferior dental canal crosses the root of the tooth and there is a radiolucent band across the root in this area. There is also loss of the superior cortical outline of the inferior dental canal as it crosses the tooth. This is likely to represent an intimate relationship between the inferior dental nerve and the roots of the tooth, which means that, if the tooth were to be removed, the patient would be at higher risk of damage to the inferior dental canal. In an ideal world a cone-beam CT (CBCT) scan would be the next step because this would provide a three-dimensional view of the area and provide a definitive answer as to the true relationship between the root and the nerve. If there is an intimate association or if no CBCT scan is available, then to minimise damage to the nerve the treatment options are: To leave the tooth in situ and treat each episode of pericoronitis as and when it occurs To remove the tooth in its entirety but accept that it has a higher than average risk of causing damage to the inferior dental nerve To carry out a coronectomy (d) A coronectomy is a procedure in which the crown of the tooth is removed and the vital roots are retained. The rationale is that not touching the roots will limit damage to the inferior dental nerve, and removing the crown will allow the mucosa to be sutured across to the lingual side, closing the wound primarily and thereby preventing any further episodes of pericoronitis. The possible complications are infection from or migration of the retained root. In some instances the root becomes mobile when the crown is sectioned and removed, and a mobile root cannot be left in situ so it is necessary to surgically remove the whole tooth.
14 ORAL SURGERY (a) Which patients should be referred to a specialist for urgent assessment according to the 2005 National Institute for Health and Care Excellence (NICE) guidelines on urgent referrals for suspected oral cancer? (b) As a general dental practitioner, to whom would you refer a patient for management if you suspected that they had a squamous cell carcinoma of the oral cavity? (c) What treatment modalities are commonly used for treating squamous cell carcinoma of the oral cavity? (d) What do you understand by the term palliative care?
15 172 ORAL SURGERY Answer 3.4 (a) Any patient with: Unexplained red and white patches (including suspected lichen planus) of the oral mucosa that are painful or bleeding or swollen. Note: a non-urgent referral should be made in the absence of these, ie not painful, bleeding or swollen. Unexplained ulceration of the oral mucosa persisting for more than 3 weeks Any adult patient with Unexplained tooth mobility persisting for more than 3 weeks An unexplained lump in the neck which has recently appeared or a lump which has not been diagnosed before that has changed over a period of 3 6 weeks (b) An oral and maxillofacial surgery consultant who manages oncology patients within a cancer centre would be the best person to manage the patient as the surgeon is part of a multidisciplinary team that can offer the patient holistic care. Oral medicine and oral surgery consultants will see patients referred for suspected squamous cell carcinomas (SCCs), and may arrange for biopsies to be performed but as they are not able to offer the patient definitive surgical treatment. Therefore, it would be ideal for the patient to be referred to the person who would be able to diagnose and manage that lesion from the start. (c) Surgery Radiotherapy Chemotherapy Combination of any of the above (d) According to the World Health Organization (2003), palliative care is an approach that improves the quality of life of patients and their families facing the problems associated with life-threatening illness, through the prevention and the relief of suffering by means of early identification and impeccable assessment and treatment of pain and other symptoms, physical, psychosocial and spiritual.
16 ORAL SURGERY (a) What are bisphosphonates? (b) You are a general dental practitioner who has a patient who is about to commence treatment with bisphosphonates. How would you manage them? (c) You have a patient who has been on oral bisphosphonates for 5 years and requires a dental extraction. Describe how you would manage this patient.
17 174 ORAL SURGERY Answer 3.5 (a) Bisphosphonate are pyrophosphate analogues that inhibit resorption of bone. Their proposed mechanism of action includes: Reduction of bone turnover Inhibition of osteoclast activity (b) Patients about to commence treatment with bisphosphonates should have been informed of the risk and benefits of the chosen drug by the prescribing physician including the risk of medication-related osteonecrosis of the jaw (MRONJ), which was previously known as bisphosphonate-related osteonecrosis of the jaw (BRONJ). The patient ideally should have a dental assessment prior to commencement of the drugs. This is especially important if the patient is to be given high-dose iv bisphosphonates. Patients should be informed of the importance of maintaining a high standard of dental health following treatment with bisphosphonate drugs, and the consequences of not doing so. Dental hard and soft tissues must be examined for any disease. Any active infection must be treated before commencement of the treatment. Any prosthesis must be carefully examined, as mucosal injury and breakdown is the second most commonly identified risk factor for MRONJ. Teeth which are in an acceptable condition but unlikely to be retained in the long term need careful consideration as future exodontia is a risk factor for MRONJ. Any teeth of dubious prognosis must also be removed. Patients should be advised on oral hygiene and preventive measures to minimise risk of dental disease. Patients must be educated about the signs and symptoms of MRONJ and to seek advice if they have concerns. Patients must be made dentally fit before commencement of the drug treatment.
18 ORAL SURGERY 175 (c) Current evidence would suggest that those at serious risk of MRONJ are likely to have been on iv bisphosphonates for more than 12 months or at least 36 months of oral bisphosphonates. Prevention is the best option and it is generally recommended that high-risk procedures, eg extractions, should be avoided and instead root canal treatment should be considered, even when it is not possible to restore the crown of the tooth to a functional form. There are some variations in the guidelines for exodontia from different countries, eg oral as oppose to parental (iv) bisphosphonates, and thus it is worthwhile checking your up-to-date local guidelines, in particular, Scottish Dental Clinical Effectiveness Programme ( The common steps usually followed are: 1 Preoperatively: Rinse with chlorhexidine mouthwash Prophylactic antibiotics (although this is not universally adopted by all clinicians, hence the need to consult with local guidelines) 2 Conservative surgical technique (atraumatic) 3 Primary closure of soft tissue where possible, without stripping periosteum 4 Postoperatively: Chlorhexidine mouthwash for 2 weeks or until mucosa has healed Antibiotics for 5 days (again this is not universally adopted see above) 5 Keep the patient under review until the socket has healed Do not attempt further extractions in other sextants of the mouth until the first socket has healed.
19 176 ORAL SURGERY 3.6 (a) In order to diagnose MRONJ, certain criteria must be met. What are they? (b) Apart from bisphosphonate drugs, what other types of drugs are associated with MRONJ? Give an example of each type, and list the conditions for which they are prescribed. (c) In which conditions might a patient be prescribed bisphosphonate medication? (d) What are the common routes of administration of bisphosphonate medication? (e) Which patients are most at risk of getting MRONJ? (f) Name some local risk factors.
20 ORAL SURGERY 177 Answer 3.6 (a) The patient must be taking or have taken anti-resorptive or antiangiogenic medication. The patient must have exposed bone or bone that can be probed through an intraoral or extraoral fistula in the maxillofacial region that has persisted for more than 8 weeks. There must be a history of radiotherapy to the jaws There must be no obvious metastatic disease to the jaws (see Ruggiero SL, Dodson TB, Fantasia J, et al. American Association of Oral and Maxillofacial Surgeons. Journal of Oral & Maxillofacial Surgery 2014; 72: ) (b) Bisphosphonates, along with other anti-resorptive medications such as denosumab are associated with MRONJ. The other group of drugs that are implicated is the anti-angiogenesis drugs such as bevacizumab and sunitinib. (c) Anti-resorptive drugs are taken for: Osteoporosis: both prevention and treatment Prevention of skeletal fractures in susceptible individuals Paget s disease Osteogenesis imperfecta Metastatic bone disease (usually in connection with breast or prostate carcinoma) Bisphosphonates are also used in the management of patients with multiple myeloma, although other anti-resorptives such as denosumab are not Anti-angiogenesis drugs are taken for renal cell carcinoma and gastric tumours (d) Oral and iv. (e) Patients who have been on high-dose potent medication by an iv route, usually for the management of malignancies.
21 178 ORAL SURGERY (f) Mandibular extractions All dentoalveolar surgery Periodontitis, presence of oral abscesses or infection Poor oral hygiene Denture-related trauma Thin mucosal coverage, eg lingual tori
22 ORAL SURGERY A fit and healthy 25-year-old patient attends your dental practice with a 2-day history of a painful, loose left mandibular first permanent molar after he was hit in the face with the cricket ball. (a) What key questions you would ask the patient? (b) What radiological investigations if any would you carry out after examination? (c) Following your examination and investigations, you are concerned that the mobile tooth is a result of a fractured mandible. How would you proceed? (d) If there was a mandibular fracture which radiological view(s) would demonstrate it? (e) What treatment is likely to be required in this case?
23 180 ORAL SURGERY Answer 3.7 (a) You would take the history and examination as usual to ascertain the current complaint, the history of the complaint, the patient s medical, dental and social history. However, in this type of injury, in particular, you would also want to know: The circumstances surrounding the incident Any loss of consciousness or any other injuries If his occlusion is deranged If there is any altered sensation in the distribution of the inferior alveolar/dental nerve The state of the tooth before the incident, eg pain and mobility (b) A panoramic radiograph to obtain an overview of the dentition and mandible. If there is insufficient detail of the region of the lower left mandibular first molar tooth then a periapical radiograph may be warranted to determine whether there is a fracture in the tooth or to determine the periodontal status of the tooth. (c) Immediately refer the patient to the nearest oral and maxillofacial surgery department for further assessment and management. (d) A dental panoramic radiograph and another view at another angle, usually a posterior-anterior view of the mandible (PA mandible). An alternative would be oblique lateral views of the mandible and PA mandible, but the oblique lateral views are often inferior to a panoramic radiograph. Cone-beam computed tomography (CT) or standard CT would also provide good information regarding the fracture but is not indicated in simple fractures due to the higher radiation dose relative to a dental panoramic radiograph and PA mandible. (e) It is likely that the fracture is displaced as the patient feels movement in the lower left first molar. Hence he requires surgical treatment in the form of open reduction and internal fixation of the fractured mandible. For a body of mandible fracture this is often accessed via an intraoral approach.
24 ORAL SURGERY (a) A fit and healthy 10-year-old child fell while playing on his microscooter and is brought into your surgery with evidence of injury to his maxillary anterior teeth. Your worry is that the child may have sustained an alveolar or dento-alveolar fracture. What are the differences between these two terms? (b) What features would lead you to suspect that the child had sustained a dento-alveolar fracture? (c) What investigations would you carry out and what findings would you expect? (d) Assuming the child is co-operative and there are no other injuries, how would you manage the dento-alveolar fracture? (e) What post-treatment instructions would you give the patient and his parents?
25 182 ORAL SURGERY Answer 3.8 (a) A fracture of the alveolar process may or may not involve the alveolar socket. A dento-alveolar fracture would involve fracture of the alveolar process and the socket. (b) (c) Teeth related to the fractured dento-alveolar segment are typically all mobile and move as a unit. An occlusal change will often be present due to the displacement of the entire segment. The teeth of the affected segment are often tender to percussion. Vitality testing of all the involved teeth this is usually negative. Radiographs usually two views are recommended for identification of fractures. Ideally, these should be at right angles to one another for better identification of fracture lines but in practice the views are usually taken with the X-ray tube head in two different positions. In the anterior region the options would be periapical views and an upper standard occlusal. A panoramic or a cone-beam CT may also be useful. Radiographic findings suggestive of a dento-alveolar fracture may present as: A radiolucent line between the fragments. However, the vertical line of the fracture may be difficult to see as it may run along the periodontal ligament space. The horizontal line may be located apical at the apex or coronal to the apex. An alteration in the outline shape of the root and discontinuity of the periodontal ligament An associated fracture(s) of the roots of the teeth. (d) After gaining consent you would: 1 Administer local analgesia 2 Reposition the displaced segment with digital pressure applied both labially and palatally or with forceps if necessary 3 Stabilise the fractured segment for 4 weeks with flexible splinting, such as: An acid etch splint with composite with or without a wire
26 ORAL SURGERY 183 Orthodontic brackets on the teeth and splinting with a flexible sectional archwire Preformed trauma arch bars (e) Soft diet for 1 week Explain that good oral hygiene is essential for healing of the tissue and that chlorhexidine mouthwash may be beneficial Explain the need for longer-term follow-up, as there is the risk of: Pulp necrosis Ankylosis Resorption associated with infection Bone loss Loss of tooth Current suggested guidelines for follow-up Splint removal and clinical and radiographic control after 4 weeks Clinical and radiographic control after 6 8 weeks, 4 months, 6 months, 1 year and yearly for 5 years For further information, please see (a) What does the term pericoronitis mean? Which teeth are most commonly affected by it? (b) What are the signs and symptoms of pericoronitis? (c) How do you treat acute pericoronitis?
27 184 ORAL SURGERY Answer 3.9 (a) Pericoronitis means infection of the tissue surrounding the crown of a tooth. The lower third molars are most commonly affected. (b) Depends on the severity of the infection: Mild swelling of soft tissue around the crown of the tooth, bad taste, pain Moderate lymphadenopathy, trismus, extraoral swelling Severe fever, malaise, spreading infection and abscess formation (c) Treatment depends on the severity of the infection. Management of mild infection includes: Oral hygiene instructions such as cleaning around the tooth and operculum with chlorhexidine or hot salty water Debridement of the area around the tooth and under the operculum Relief of trauma from opposing tooth grind cusps or extraction of the tooth Analgesics Antibiotics (metronidazole) Severe infection may need hospitalisation, intravenous antibiotics, removal of the lower third molar and/or incision and drainage.
28 ORAL SURGERY (a) What does the acronym NICE stand for? (b) NICE guidelines gives specific indications for removal of wisdom teeth. List five such indications. (c) What features on a radiograph would suggest that a wisdom tooth is associated with the inferior dental nerve? (d) What specific information must be given to a patient prior to removal of an impacted lower wisdom tooth, which you would not give if you were removing an upper wisdom tooth?
29 186 ORAL SURGERY Answer 3.10 (a) National Institute for Health and Care Excellence (b) Surgical removal of impacted third molars should be limited to patients with evidence of pathology such as (any five of the following): Caries Non-treatable pulpal and/or periapical pathology Cellulitis Abscess and osteomyelitis Internal and external resorption of the tooth or adjacent tooth Fracture of tooth Tooth/teeth impeding surgery or reconstructive jaw surgery Tooth is within the field of tumour resection (c) Loss, deviation or narrowing of the tramlines of the inferior dental canal, and a radiolucent band across the root of the tooth. (d) Information specific to lower wisdom teeth: numbness/tingling or altered sensation of the lower lip, chin and tongue which may be temporary or permanent. This information needs to be given to the patient because of the possibility of damage to the inferior dental nerve or the lingual nerve during the procedure.
FRACTURES AND LUXATIONS OF PERMANENT TEETH
 FRACTURES AND LUXATIONS OF PERMANENT TEETH 1. Treatment guidelines and alveolar bone Followup Procedures INFRACTION Clinical findings Radiographic findings Treatment Follow-Up Favorable Outcome Unfavorable
FRACTURES AND LUXATIONS OF PERMANENT TEETH 1. Treatment guidelines and alveolar bone Followup Procedures INFRACTION Clinical findings Radiographic findings Treatment Follow-Up Favorable Outcome Unfavorable
The Treatment of Traumatic Dental Injuries
 The Recommended Guidelines of the American Association of Endodontists for The Treatment of Traumatic Dental Injuries 2013 American Association of Endodontists Revised 9/13 The Recommended Guidelines of
The Recommended Guidelines of the American Association of Endodontists for The Treatment of Traumatic Dental Injuries 2013 American Association of Endodontists Revised 9/13 The Recommended Guidelines of
INDIANA HEALTH COVERAGE PROGRAMS
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
There are three referral categories used in the dental referral system:
 Restorative Dentistry Referral Criteria Restorative Dentistry referral criteria are outlined to provide General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists, Primary Care Specialists,
Restorative Dentistry Referral Criteria Restorative Dentistry referral criteria are outlined to provide General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists, Primary Care Specialists,
J. 0. AKINOSI, B.D.s., F.D.S.R.C.S.
 British Journal of Oral Surgery 15 (1977-78) 83-87 A NEW APPROACH TO THE MANDIBULAR NERVE BLOCK J. 0. AKINOSI, B.D.s., F.D.S.R.C.S. Department of Oral Surgery and Pathology, College of Medicine, Lagos
British Journal of Oral Surgery 15 (1977-78) 83-87 A NEW APPROACH TO THE MANDIBULAR NERVE BLOCK J. 0. AKINOSI, B.D.s., F.D.S.R.C.S. Department of Oral Surgery and Pathology, College of Medicine, Lagos
Patient information leaflet about Lower Wisdom Teeth (3 rd Molars)
 Patient information leaflet about Lower Wisdom Teeth (3 rd Molars) This leaflet is designed to give you more information about what the issues are with wisdom teeth, what treatment options may be given,
Patient information leaflet about Lower Wisdom Teeth (3 rd Molars) This leaflet is designed to give you more information about what the issues are with wisdom teeth, what treatment options may be given,
London Intermediate Minor Oral Surgery Referral Form PATIENT DETAILS
 London Intermediate Minor Oral Surgery Referral Form 22.06.18 PATIENT DETAILS Patient s Title and Name: Gender: Date of Birth: Patient s Address: Postcode Patient s email address: Contact Number: (mobile
London Intermediate Minor Oral Surgery Referral Form 22.06.18 PATIENT DETAILS Patient s Title and Name: Gender: Date of Birth: Patient s Address: Postcode Patient s email address: Contact Number: (mobile
IMPACTED CANINES. Unfortunately, this important tooth is the second most common tooth to be impacted after third molars
 IMPACTED CANINES After we talked about impacted third molars, today we ll discuss about maxillary impacted canines in upper dental arch, how to manage these cases as a dental surgeon. You will study about
IMPACTED CANINES After we talked about impacted third molars, today we ll discuss about maxillary impacted canines in upper dental arch, how to manage these cases as a dental surgeon. You will study about
Surgical removal of wisdom teeth
 Oral surgery/dr.hazem Lecture #8 Rand Herzallah Surgical removal of wisdom teeth Wisdom teeth extraction is harder than the extraction of any other teeth; because of: 1) The anatomical location of the
Oral surgery/dr.hazem Lecture #8 Rand Herzallah Surgical removal of wisdom teeth Wisdom teeth extraction is harder than the extraction of any other teeth; because of: 1) The anatomical location of the
Large Dentigerous Cyst
 Volume 16.2.1 Feb 2016 This Lecture Series qualifies for 0.5 Informal CPD Learning Hours Large Dentigerous Cyst By Dr Hassem Geha A 55 year-old male presented with a painless swelling in the right mandible.
Volume 16.2.1 Feb 2016 This Lecture Series qualifies for 0.5 Informal CPD Learning Hours Large Dentigerous Cyst By Dr Hassem Geha A 55 year-old male presented with a painless swelling in the right mandible.
2014 Update Revisions for: AAOMS Strategies for patient management with or at risk for medication-related osteonecrosis of the jaw:
 AAOMS Strategies for patient management with or at risk for medication-related osteonecrosis of the jaw: 2007 2009 2014 2014 Update Revisions for: Diagnosis, Staging, Management strategies, (our main interest)
AAOMS Strategies for patient management with or at risk for medication-related osteonecrosis of the jaw: 2007 2009 2014 2014 Update Revisions for: Diagnosis, Staging, Management strategies, (our main interest)
Radiographic assessment of lower third molar prior to surgery: A report of four cases
 Radiographic assessment of lower third molar prior to surgery: A report of four cases V Sreenivas Prasad Department of Oral and Maxillofacial Surgery, College of Dentistry, Gulf Medical University, Ajman,
Radiographic assessment of lower third molar prior to surgery: A report of four cases V Sreenivas Prasad Department of Oral and Maxillofacial Surgery, College of Dentistry, Gulf Medical University, Ajman,
Principles of Exodontia
 Principles of Exodontia *This lecture will help you selecting properly patients to do extraction for.. First of all and before extraction you have to deal with: # Pain management and anxiety control, by
Principles of Exodontia *This lecture will help you selecting properly patients to do extraction for.. First of all and before extraction you have to deal with: # Pain management and anxiety control, by
Oral Surgery. Basic Techniques of Dental Local Anesthesia. A variety of techniques used in administration and deposition of local anesthesia:
 Oral Surgery Lecture: 9 Dr. Saif Saadedeen Basic Techniques of Dental Local Anesthesia A variety of techniques used in administration and deposition of local anesthesia: 1. Topical anesthesia 2. Infiltration
Oral Surgery Lecture: 9 Dr. Saif Saadedeen Basic Techniques of Dental Local Anesthesia A variety of techniques used in administration and deposition of local anesthesia: 1. Topical anesthesia 2. Infiltration
Diagnosis. overt Examination. Definitive Examination. History. atient interview. Personal History. Clinical Examination.
 Diagnosis overt Examination History Definitive Examination atient interview Personal History Mental Attitude Medical History Dental History Clinical Examination Extra Oral Oral Radiographic Evaluation
Diagnosis overt Examination History Definitive Examination atient interview Personal History Mental Attitude Medical History Dental History Clinical Examination Extra Oral Oral Radiographic Evaluation
Subject: Removal of Teeth Guideline #: Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018
 DDental Policy Dental Subject: Removal of Teeth Guideline #: 07-101 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018 Description This document addresses the removal of teeth, erupted
DDental Policy Dental Subject: Removal of Teeth Guideline #: 07-101 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018 Description This document addresses the removal of teeth, erupted
Third molar (wisdom) teeth
 Third molar (wisdom) teeth This information leaflet is for patients who may need to have their third molar (wisdom) teeth removed. It explains why they may need to be removed, what is involved and any
Third molar (wisdom) teeth This information leaflet is for patients who may need to have their third molar (wisdom) teeth removed. It explains why they may need to be removed, what is involved and any
2018 Dental Code Set For dates of service from 1/1/ /31/2018
 D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT D0140 LIMITED ORAL EVALUATION - PROBLEM FOCUSED D0150 COMPREHENSIVE ORAL EVALUATION - NEW OR ESTABLISHED PATIENT D0160 DETAILED AND EXTENSIVE ORAL EVALUATION
D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT D0140 LIMITED ORAL EVALUATION - PROBLEM FOCUSED D0150 COMPREHENSIVE ORAL EVALUATION - NEW OR ESTABLISHED PATIENT D0160 DETAILED AND EXTENSIVE ORAL EVALUATION
2018 Dental Code Set
 D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0251 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0393 D0470 D0502 PERIODIC ORAL EVALUATION ESTABLISHED PATIENT LIMITED ORAL
D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0251 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0393 D0470 D0502 PERIODIC ORAL EVALUATION ESTABLISHED PATIENT LIMITED ORAL
DF1 Case Studies Surgical Case Michael Hicks
 DF1 Case Studies Surgical Case Michael Hicks North Western Deanery Background Miss M attended as a new patient requiring treatment. She was a nervous patient and required basic periodontal therapy, an
DF1 Case Studies Surgical Case Michael Hicks North Western Deanery Background Miss M attended as a new patient requiring treatment. She was a nervous patient and required basic periodontal therapy, an
MAXILLARY INJECTION TECHNIQUE. Chinthamani Laser Dental Clinic
 MAXILLARY INJECTION TECHNIQUE Chinthamani Laser Dental Clinic Introduction A number of injection techniques are available to aid in providing clinically adequate anesthesia of the teeth and soft and hard
MAXILLARY INJECTION TECHNIQUE Chinthamani Laser Dental Clinic Introduction A number of injection techniques are available to aid in providing clinically adequate anesthesia of the teeth and soft and hard
Dental Trauma in the Pediatric Population
 Dental Trauma in the Pediatric Population Juan F. Yepes DDS, MD, MPH, MS, DrPH Associate Professor of Pediatric Dentistry Indiana University School of Dentistry James Whitcomb Hospital for Children jfyepes@iupui.edu
Dental Trauma in the Pediatric Population Juan F. Yepes DDS, MD, MPH, MS, DrPH Associate Professor of Pediatric Dentistry Indiana University School of Dentistry James Whitcomb Hospital for Children jfyepes@iupui.edu
Dental Morphology and Vocabulary
 Dental Morphology and Vocabulary Palate Palate Palate 1 2 Hard Palate Rugae Hard Palate Palate Palate Soft Palate Palate Palate Soft Palate 4 Palate Hard Palate Soft Palate Maxillary Arch (Maxilla) (Uppers)
Dental Morphology and Vocabulary Palate Palate Palate 1 2 Hard Palate Rugae Hard Palate Palate Palate Soft Palate Palate Palate Soft Palate 4 Palate Hard Palate Soft Palate Maxillary Arch (Maxilla) (Uppers)
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
GUIDELINES FOR THE MANAGEMENT OF TRAUMATISED INCISORS
 GUIDELINES FOR THE MANAGEMENT OF TRAUMATISED INCISORS Dentists need to understand that the decision to remove or not reimplant an avulsed incisor must be made very carefully. The loss of such a tooth in
GUIDELINES FOR THE MANAGEMENT OF TRAUMATISED INCISORS Dentists need to understand that the decision to remove or not reimplant an avulsed incisor must be made very carefully. The loss of such a tooth in
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Complex Exodontia. Jone Kim, DDS, MS
 Complex Exodontia Jone Kim, DDS, MS Diplomate, American Board of Oral & Maxillofacial Surgery Lecturer, UCLA School of Dentistry, Dept. of Oral & Maxillofacial Surgery Principle of Complex Exodontia Principle
Complex Exodontia Jone Kim, DDS, MS Diplomate, American Board of Oral & Maxillofacial Surgery Lecturer, UCLA School of Dentistry, Dept. of Oral & Maxillofacial Surgery Principle of Complex Exodontia Principle
TRICOLLEGIATE DIPLOMA OF MEMBERSHIP IN ORAL SURGERY (M. Oral Surgery) APPENDIX A LEARNING OUTCOMES & BLUEPRINT
 TRICOLLEGIATE DIPLOMA OF MEMBERSHIP IN ORAL SURGERY (M. Oral Surgery) APPENDIX A LEARNING OUTCOMES & BLUEPRINT A - LEARNING OUTCOMES In brackets below the headings are cross references to corresponding
TRICOLLEGIATE DIPLOMA OF MEMBERSHIP IN ORAL SURGERY (M. Oral Surgery) APPENDIX A LEARNING OUTCOMES & BLUEPRINT A - LEARNING OUTCOMES In brackets below the headings are cross references to corresponding
Everything You Wanted to Know About Extractions but Were Afraid to Ask
 Everything You Wanted to Know About Extractions but Were Afraid to Ask Tooth extraction is a surgical procedure with serious potential complications and should only be performed by a trained veterinarian.
Everything You Wanted to Know About Extractions but Were Afraid to Ask Tooth extraction is a surgical procedure with serious potential complications and should only be performed by a trained veterinarian.
LIST OF COVERED DENTAL SERVICES
 LIST OF COVERED DENTAL SERVICES The following is a complete list of those dental Services which will be considered for payment by Constitution Life Insurance Company after the expiration of any applicable
LIST OF COVERED DENTAL SERVICES The following is a complete list of those dental Services which will be considered for payment by Constitution Life Insurance Company after the expiration of any applicable
CORONECTOMY OF MANDIBULAR WISDOM TEETH: A CASE SERIES AND BRIEF REVIEW OF LITERATURE
 26 DENTAL STUDENTS RESEARCH CORONECTOMY OF MANDIBULAR WISDOM TEETH: A CASE SERIES AND BRIEF REVIEW OF LITERATURE Rasha Alafaleg1 1 SAN DANETH 1 Bachelor of Dental Surgery, University of Health Sciences,
26 DENTAL STUDENTS RESEARCH CORONECTOMY OF MANDIBULAR WISDOM TEETH: A CASE SERIES AND BRIEF REVIEW OF LITERATURE Rasha Alafaleg1 1 SAN DANETH 1 Bachelor of Dental Surgery, University of Health Sciences,
For the Patient: Bisphosphonates and Oral Health in Multiple Myeloma
 For the Patient: Bisphosphonates and Oral Health in Multiple Myeloma Regular dental care is very important for all cancer patients. As soon as possible after your cancer diagnosis, your dentist should
For the Patient: Bisphosphonates and Oral Health in Multiple Myeloma Regular dental care is very important for all cancer patients. As soon as possible after your cancer diagnosis, your dentist should
DINA Dental. Prepaid Plan Highlights. Prepaid Plan Bi-weekly Premiums $ 7.00 $10.76 $ Employee Only Employee + One Employee + Family
 DINA Dental Prepaid Plan Highlights NO Claim Forms NO Maximums NO Deductibles NO Waiting Period - Some Preventive and Diagnostic Services Provided at NO CHARGE - Over 180 procedures covered by co-payments
DINA Dental Prepaid Plan Highlights NO Claim Forms NO Maximums NO Deductibles NO Waiting Period - Some Preventive and Diagnostic Services Provided at NO CHARGE - Over 180 procedures covered by co-payments
For Dentists and Other Dental Professionals: Dental Screening Program for Patients Who May Need Hematopoietic Stem Cell Transplantation (HSCT)
 For Dentists and Other Dental Professionals: Dental Screening Program for Patients Who May Need Hematopoietic Stem Cell Transplantation (HSCT) Dear Dental Care Provider, Thank you for your contribution
For Dentists and Other Dental Professionals: Dental Screening Program for Patients Who May Need Hematopoietic Stem Cell Transplantation (HSCT) Dear Dental Care Provider, Thank you for your contribution
HDS PROCEDURE CODE GUIDELINES
 D0100 - D0999 Clinical Oral Evaluations D0120 - D0180 The codes in this section have been revised to recognize the cognitive skills necessary for patient evaluation. The collection and recording of some
D0100 - D0999 Clinical Oral Evaluations D0120 - D0180 The codes in this section have been revised to recognize the cognitive skills necessary for patient evaluation. The collection and recording of some
Principles of endodontic surgery
 Principles of endodontic surgery Note: the doctor said that this lecture mainly contain notes, so we should study it from the book for further information (chapter 18) principles of endodontic surgery.
Principles of endodontic surgery Note: the doctor said that this lecture mainly contain notes, so we should study it from the book for further information (chapter 18) principles of endodontic surgery.
Senior Dental Insurance Scheduled Allowance
 Senior Dental Insurance Scheduled Allowance LIST OF COVERED DENTAL SERVICES The following is a complete list of those dental services which will be considered for payment by The American Progressive Life
Senior Dental Insurance Scheduled Allowance LIST OF COVERED DENTAL SERVICES The following is a complete list of those dental services which will be considered for payment by The American Progressive Life
Types of Wisdom Teeth Positions
 The Wise Guide to Wisdom Teeth Extraction H. Ryan Kazemi, DMD 11 Types of Wisdom Teeth Positions Erupted: The tooth has completely emerged through the gum tissue and is visible. This occurs when there
The Wise Guide to Wisdom Teeth Extraction H. Ryan Kazemi, DMD 11 Types of Wisdom Teeth Positions Erupted: The tooth has completely emerged through the gum tissue and is visible. This occurs when there
SURGICAL EXTRACTION OF IMPACTED TEETH
 UnitedHealthcare Dental Clinical Policy SURGICAL EXTRACTION OF IMPACTED TEETH Policy Number: DCP006.03 Effective Date: December 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1
UnitedHealthcare Dental Clinical Policy SURGICAL EXTRACTION OF IMPACTED TEETH Policy Number: DCP006.03 Effective Date: December 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1
Techniques of local anesthesia in the mandible
 Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
CHAPTER 6 Dental Services
 CHAPTER 6 Dental Services Propunere noua clasificare proceduri folosind codificarea ICD-10-AM versiunea 3, 30 martie 2004 BLOCK 450 Dental examination 97012-00 Periodic oral examination 97013-00 Limited
CHAPTER 6 Dental Services Propunere noua clasificare proceduri folosind codificarea ICD-10-AM versiunea 3, 30 martie 2004 BLOCK 450 Dental examination 97012-00 Periodic oral examination 97013-00 Limited
COMBINED PERIODONTAL-ENDODONTIC LESION. By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur
 COMBINED PERIODONTAL-ENDODONTIC LESION By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur Differential diagnosis For differential diagnostic purposed the endo-perio
COMBINED PERIODONTAL-ENDODONTIC LESION By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur Differential diagnosis For differential diagnostic purposed the endo-perio
Digital Imaging from a new perspective
 TREATMENT CENTRES HANDPIECES HYGIENE SYSTEMS X-RAY SYSTEMS CEREC TREATMENT CENTRES HANDPIECES HYGIENE SYSTEMS X-RAY SYSTEMS CEREC SIRONA CREATING AND MAINTAINING VALUE. You are right to expect a great
TREATMENT CENTRES HANDPIECES HYGIENE SYSTEMS X-RAY SYSTEMS CEREC TREATMENT CENTRES HANDPIECES HYGIENE SYSTEMS X-RAY SYSTEMS CEREC SIRONA CREATING AND MAINTAINING VALUE. You are right to expect a great
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Department of Oral & Maxillofacial Surgery. Referral Guidelines
 Department of Oral & Maxillofacial Surgery Referral Guidelines 2015 To all General Dental Practitioners and General Medical Practitioners The Department of Oral & Maxillofacial Surgery has outpatient clinics
Department of Oral & Maxillofacial Surgery Referral Guidelines 2015 To all General Dental Practitioners and General Medical Practitioners The Department of Oral & Maxillofacial Surgery has outpatient clinics
King's College Hospital Dental School, London, S.E. 5.
 OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
THE EVALUATION OF FOREIGN DENTAL DEGREES FOR EQUIVALENCE WITH SOUTH AFRICAN DENTAL DEGREES
 553 Madiba Street Arcadia, Pretoria PO Box 205 Pretoria, 0001 Tel: +27 (12) 338 9459 Email: nkululekon@hpcsa.co.za Website: www.hpcsa.co.za MEDICAL AND DENTAL PROFESSIONS BOARD FORM 176A- DP v4. THE EVALUATION
553 Madiba Street Arcadia, Pretoria PO Box 205 Pretoria, 0001 Tel: +27 (12) 338 9459 Email: nkululekon@hpcsa.co.za Website: www.hpcsa.co.za MEDICAL AND DENTAL PROFESSIONS BOARD FORM 176A- DP v4. THE EVALUATION
Examination of teeth and gingiva
 Examination of teeth and gingiva Siriporn Chattipakorn, DDS, PhD. SUBJECTIVE HISTORY Chief complaint In patient s own words My tooth hurts when I chew hard foods I can t drink cold drink I have bad breath
Examination of teeth and gingiva Siriporn Chattipakorn, DDS, PhD. SUBJECTIVE HISTORY Chief complaint In patient s own words My tooth hurts when I chew hard foods I can t drink cold drink I have bad breath
RETIREE DENTAL PLAN. RETIREE DENTAL PLAN FEE SCHEDULE Page 1 of 8
 D0120 periodic oral evaluation $ 30.50 D0140 limited oral evaluation problem focused $ 30.50 D0150 comprehensive oral evaluation - new or established patient $ 30.50 D0160 detailed and extensive oral evaluation
D0120 periodic oral evaluation $ 30.50 D0140 limited oral evaluation problem focused $ 30.50 D0150 comprehensive oral evaluation - new or established patient $ 30.50 D0160 detailed and extensive oral evaluation
Maxillary LA: Techniques. Ra ed Salma BDS, MSc, JBOMFS, MFDRCSI
 Maxillary LA: Techniques Ra ed Salma BDS, MSc, JBOMFS, MFDRCSI dr.raedsalma@riyadh.edu.sa https://sites.google.com/a/riyadh.edu.sa/raed/ LA Options for the Maxilla Infiltration Submucosal Supraperiosteal
Maxillary LA: Techniques Ra ed Salma BDS, MSc, JBOMFS, MFDRCSI dr.raedsalma@riyadh.edu.sa https://sites.google.com/a/riyadh.edu.sa/raed/ LA Options for the Maxilla Infiltration Submucosal Supraperiosteal
6610 NE 181st Street, Suite #1, Kenmore, WA
 660 NE 8st Street, Suite #, Kenmore, WA 9808 www.northshoredentalacademy.com.08.900 READ CHAPTER The Professional Dental Assistant (p.-9) No Key Terms Recall Questions:,,,, and 6 CLASS SYLLABUS DAY READ
660 NE 8st Street, Suite #, Kenmore, WA 9808 www.northshoredentalacademy.com.08.900 READ CHAPTER The Professional Dental Assistant (p.-9) No Key Terms Recall Questions:,,,, and 6 CLASS SYLLABUS DAY READ
Diagnostic No One of (D0210, D0330) per 36 Month(s) Per patient No No Ten of (D0230) per 1 Day(s) Per patient.
 Dental and Authorization Guide Diagnostic services include the oral examinations, and selected radiographs, needed to assess the oral health, diagnose oral pathology, and develop an adequate treatment
Dental and Authorization Guide Diagnostic services include the oral examinations, and selected radiographs, needed to assess the oral health, diagnose oral pathology, and develop an adequate treatment
PERIODONTAL CASE PRESENTATION - 1
 PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
Fee Schedule Detail Procedure Procedure Description Code Fee
 Fee Schedule Detail Procedure Procedure Description Code Fee D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT $ 32.29 D0140 LIMITED ORAL EVALUATION-PROBLEM FOCUSED $ 53.02 D0150 COMPREHENSIVE ORAL
Fee Schedule Detail Procedure Procedure Description Code Fee D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT $ 32.29 D0140 LIMITED ORAL EVALUATION-PROBLEM FOCUSED $ 53.02 D0150 COMPREHENSIVE ORAL
Appendix 1 - Restorative Dentistry Referral Guidelines for referring practitioners
 Appendix 1 - Restorative Dentistry Referral Guidelines for referring practitioners These guidelines are intended to assist General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists and
Appendix 1 - Restorative Dentistry Referral Guidelines for referring practitioners These guidelines are intended to assist General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists and
PRE-OP and POST-OP SURGICAL CONSIDERATIONS
 PRE-OP and POST-OP SURGICAL CONSIDERATIONS Darlene Sorrell, DMD, is not an oral surgeon. AIDC is an out-patient facility. 29 years of experience in IHS. Advanced General Practice Residency. No access
PRE-OP and POST-OP SURGICAL CONSIDERATIONS Darlene Sorrell, DMD, is not an oral surgeon. AIDC is an out-patient facility. 29 years of experience in IHS. Advanced General Practice Residency. No access
General Dentist Fee Schedule
 General Dentist Fee Schedule ADA Diagnostic D0120 Periodic oral evaluation $0 $72 $72 D0140 Limited oral evaluation problem focused $77 $107 $30 D0150 Comprehensive oral evaluation new or established patient
General Dentist Fee Schedule ADA Diagnostic D0120 Periodic oral evaluation $0 $72 $72 D0140 Limited oral evaluation problem focused $77 $107 $30 D0150 Comprehensive oral evaluation new or established patient
General Dentist Fee Schedule
 General Dentist Fee Schedule Diagnostic D0120 Periodic oral evaluation $0 $59 $59 D0140 Limited oral evaluation problem focused $71 $88 $17 D0150 Comprehensive oral evaluation new or established patient
General Dentist Fee Schedule Diagnostic D0120 Periodic oral evaluation $0 $59 $59 D0140 Limited oral evaluation problem focused $71 $88 $17 D0150 Comprehensive oral evaluation new or established patient
MDG Dental Plan Comparison
 D0999 Office visit during regular hours, general dentist only Evaluations D0120 Periodic oral examination - established patient D0140 Limited oral evaluation - problem focused D0145 Oral evaluation for
D0999 Office visit during regular hours, general dentist only Evaluations D0120 Periodic oral examination - established patient D0140 Limited oral evaluation - problem focused D0145 Oral evaluation for
Fundamental & Preventive Curvatures of Teeth and Tooth Development. Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L.
 Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Code Description Cap Freq D5660 ADD CLASP TO EXISTING PARTIAL DENTURE - PER TOOTH 4 1
 Code Description Cap Freq D5660 ADD CLASP TO EXISTING PARTIAL DENTURE - PER TOOTH D5650 ADD TOOTH TO EXISTING PARTIAL DENTURE D5411 ADJUST COMPLETE DENTURE - MANDIBULAR D5410 ADJUST COMPLETE DENTURE -
Code Description Cap Freq D5660 ADD CLASP TO EXISTING PARTIAL DENTURE - PER TOOTH D5650 ADD TOOTH TO EXISTING PARTIAL DENTURE D5411 ADJUST COMPLETE DENTURE - MANDIBULAR D5410 ADJUST COMPLETE DENTURE -
Emergency Management of Trauma
 Aims and Objectives Emergency Management of Trauma Susan Parekh/Paul Ashley Unit of Paediatric Dentistry Knowledge and understanding of the following: Epidemiology of traumatic injuries Classification
Aims and Objectives Emergency Management of Trauma Susan Parekh/Paul Ashley Unit of Paediatric Dentistry Knowledge and understanding of the following: Epidemiology of traumatic injuries Classification
CHAPTER 8 SECTION 1.4 ORAL SURGERY TRICARE/CHAMPUS POLICY MANUAL M DEC 1998 SPECIAL BENEFIT INFORMATION
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
NC Medicaid Dental Reimbursement Rates General Dentist, Oral Surgeon, Pediatric Dentist, Periodontist, & Orthodontist Effective Date: January 1, 2017
 NC Dental Reimbursement s Refer to the NC and Health Choice Clinical Coverage Policies on the DMA website. D0120 Periodic oral evaluation 24.51 D0140 Limited oral evaluation - problem focused 34.94 D0145
NC Dental Reimbursement s Refer to the NC and Health Choice Clinical Coverage Policies on the DMA website. D0120 Periodic oral evaluation 24.51 D0140 Limited oral evaluation - problem focused 34.94 D0145
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2016 Dental Code Set For dates of service from 1/1/16-12/31/16
 HCPCS DESCRIPTIONS D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0260 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0470 D0502 D1110 D1206 D1208 D1352 D2140 D2150 D2160 D2161
HCPCS DESCRIPTIONS D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0260 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0470 D0502 D1110 D1206 D1208 D1352 D2140 D2150 D2160 D2161
Contemporary Atraumatic Oral Surgery for General Dentists. Getting it Right, So Things Don t Go Wrong
 Contemporary Atraumatic Oral Surgery for General Dentists Getting it Right, So Things Don t Go Wrong Alan Jeroff DMD ajeroff@dentistry.ubc.ca Patient Evaluation Medical Clinical Record Keeping Dentoalveolar
Contemporary Atraumatic Oral Surgery for General Dentists Getting it Right, So Things Don t Go Wrong Alan Jeroff DMD ajeroff@dentistry.ubc.ca Patient Evaluation Medical Clinical Record Keeping Dentoalveolar
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Buccal approach in surgical removal of lingually embedded teeth: a report of 2 cases
 Dental Journal Mahidol Dental Journal Case report Buccal approach in surgical removal of lingually embedded teeth: a report of 2 cases Thatsanai Tangmankongworakoon 1, Nattamet Wongsirichat 2 1 Lad Yao
Dental Journal Mahidol Dental Journal Case report Buccal approach in surgical removal of lingually embedded teeth: a report of 2 cases Thatsanai Tangmankongworakoon 1, Nattamet Wongsirichat 2 1 Lad Yao
PROBITY SERVICES CLARIFICATION OF CODES IN SDR FOR PROBITY PURPOSES
 PROBITY SERVICES CLARIFICATION OF CODES IN SDR FOR PROBITY PURPOSES Purpose of the paper: The purpose of this paper is to provide clarification to all GDPs in terms of how patient records are assessed
PROBITY SERVICES CLARIFICATION OF CODES IN SDR FOR PROBITY PURPOSES Purpose of the paper: The purpose of this paper is to provide clarification to all GDPs in terms of how patient records are assessed
Staywell FL Child Medicaid Plan Benefits
 The following is a complete list of dental procedures for which benefits are payable under this Plan. For beneficiaries under age 21, additional coverage may be available with documentation of medical
The following is a complete list of dental procedures for which benefits are payable under this Plan. For beneficiaries under age 21, additional coverage may be available with documentation of medical
Mesial Step Class I or Class III Dependent upon extent of step seen clinically and patient s growth pattern Refer for early evaluation (by 8 years)
 Orthodontics and Dentofacial Development Overview Development of Dentition Treatment Retention and Relapse Growth of Naso-Maxillary Complex Develops postnatally entirely by intramenbranous ossification
Orthodontics and Dentofacial Development Overview Development of Dentition Treatment Retention and Relapse Growth of Naso-Maxillary Complex Develops postnatally entirely by intramenbranous ossification
SECURE CHOICE INDIVIDUAL COPAYMENT SCHEDULE
 DentiCare of Alabama, Inc. 3595 Grandview Parkway, Suite 650 Birmingham, AL 35243 SECURE CHOICE INDIVIDUAL COPAYMENT SCHEDULE SECTION I: PLAN DENTIST SERVICES (Subject to Exclusions and Limitations Listed
DentiCare of Alabama, Inc. 3595 Grandview Parkway, Suite 650 Birmingham, AL 35243 SECURE CHOICE INDIVIDUAL COPAYMENT SCHEDULE SECTION I: PLAN DENTIST SERVICES (Subject to Exclusions and Limitations Listed
GUARANTY ASSURANCE COMPANY Dina Dental of Louisiana Pre-Paid Group & Individual
 Effective: January 1, 2016 Eligibility: (866) 436-3093 GUARANTY ASSURANCE COMPANY Dina Dental of Louisiana Pre-Paid Group & Individual Diagnostic D0999 Office Visit Copay - Per Person, Per Visit $9.00
Effective: January 1, 2016 Eligibility: (866) 436-3093 GUARANTY ASSURANCE COMPANY Dina Dental of Louisiana Pre-Paid Group & Individual Diagnostic D0999 Office Visit Copay - Per Person, Per Visit $9.00
When is the Best Time to Have my Wisdom Teeth Removed?
 When a wisdom tooth is partially erupted, food and bacteria collect under the gum causing a local infection. This may result in bad breath, pain, swelling and trismus (inability to open the mouth fully).
When a wisdom tooth is partially erupted, food and bacteria collect under the gum causing a local infection. This may result in bad breath, pain, swelling and trismus (inability to open the mouth fully).
Dr.Sepideh Falah-kooshki
 Dr.Sepideh Falah-kooshki MAXILLA Premaxillary/median palatal suture (radiolucent). Incisive fossa and foramen (radiolucent). Nasal passages (radiolucent). Nasal septum (radiopaque). Anterior nasal spine
Dr.Sepideh Falah-kooshki MAXILLA Premaxillary/median palatal suture (radiolucent). Incisive fossa and foramen (radiolucent). Nasal passages (radiolucent). Nasal septum (radiopaque). Anterior nasal spine
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Relation between the complex diagnostics and the complications of the wisdom-tooth surgery
 Relation between the complex diagnostics and the complications of the wisdom-tooth surgery Changes of the "surgical profile" at the Dental Surgery Department of the Oral & Maxillofacial Surgery Clinic,
Relation between the complex diagnostics and the complications of the wisdom-tooth surgery Changes of the "surgical profile" at the Dental Surgery Department of the Oral & Maxillofacial Surgery Clinic,
Upper arch. 1Prosthodontics. Dr.Bassam Ali Al-Turaihi. Basic anatomy & & landmark of denture & mouth
 1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
YOUR COMPREHENSIVE GUIDE TO. Wisdom Teeth. (03) omfs.com.au
 YOUR COMPREHENSIVE GUIDE TO Wisdom Teeth (03) 9347 3788 omfs.com.au Wisdom teeth 3 Symptoms caused by impacted wisdom teeth 4 Treatment options 5 The removal procedure 6 Important facts to consider with
YOUR COMPREHENSIVE GUIDE TO Wisdom Teeth (03) 9347 3788 omfs.com.au Wisdom teeth 3 Symptoms caused by impacted wisdom teeth 4 Treatment options 5 The removal procedure 6 Important facts to consider with
Case report: Replacement of failing 2 stage implants by basal implants and conventional bridgework
 Case report: Replacement of failing 2 stage implants by basal implants and conventional bridgework Authors Dr. Aleksandar Lazarov Solunska Str. 3 BG-1000 Sofia Bulgaria Email: alex.lazarov@yahoo.co.uk
Case report: Replacement of failing 2 stage implants by basal implants and conventional bridgework Authors Dr. Aleksandar Lazarov Solunska Str. 3 BG-1000 Sofia Bulgaria Email: alex.lazarov@yahoo.co.uk
Delta Dental of Colorado EXCLUSIVE PANEL OPTION (EPO) Schedule EPO 1B List of Patient Co-Payments. * See Special Provisions on Last Page
 List of Co-Payments Code edure Code Definition Co-Pay DIAGNOSTIC CODES D0120 Periodic oral evaluation - established patient $10.00 D0140 Limited oral evaluation - problem focused $10.00 D0145 Oral evaluation
List of Co-Payments Code edure Code Definition Co-Pay DIAGNOSTIC CODES D0120 Periodic oral evaluation - established patient $10.00 D0140 Limited oral evaluation - problem focused $10.00 D0145 Oral evaluation
SECTION XVI. EssentialSmile Ped 111, ST, INN, Pediatric Dental SCHEDULE OF BENEFITS
 SECTION XVI. EssentialSmile Ped 111, ST, INN, Pediatric Dental SCHEDULE OF BENEFITS COST-SHARING PEDIATRIC DENTAL CARE ESSENTIAL HEALTH BENEFIT Deductible One (1) Member under age 19 Two (2) or more Members
SECTION XVI. EssentialSmile Ped 111, ST, INN, Pediatric Dental SCHEDULE OF BENEFITS COST-SHARING PEDIATRIC DENTAL CARE ESSENTIAL HEALTH BENEFIT Deductible One (1) Member under age 19 Two (2) or more Members
Appendix 4. Case Summary Template. Social history. Patient (Name and Date of birth): Presenting complaints. History Medical history
 Appendix 4 Case Summary Template Patient (Name and Date of birth): Presenting complaints Chief complaint Subsidiary complaints History of complaints Patient s expectations History Medical history Medical
Appendix 4 Case Summary Template Patient (Name and Date of birth): Presenting complaints Chief complaint Subsidiary complaints History of complaints Patient s expectations History Medical history Medical
This Presentation Is Trademarked by Lawrence H. Zager, D.D.S.
 This Presentation Is Trademarked by Lawrence H. Zager, D.D.S.! The next presentation is from the private collection of patient s treated in my practice with the use of implants and other prosthetic devices
This Presentation Is Trademarked by Lawrence H. Zager, D.D.S.! The next presentation is from the private collection of patient s treated in my practice with the use of implants and other prosthetic devices
HSCSN Table Top Reference Guide
 Age Limitation Covered One per 6 months per dentist or dental group. Only one exam (D0120) every 6 months per dentist or dental D0120 iodic oral evaluation 0-20 No group. D0140 Limited oral evaluation
Age Limitation Covered One per 6 months per dentist or dental group. Only one exam (D0120) every 6 months per dentist or dental D0120 iodic oral evaluation 0-20 No group. D0140 Limited oral evaluation
Attachment G. Orthodontic Criteria Index Form Comprehensive D8080. ABBREVIATIONS CRITERIA for Permanent Dentition YES NO
 First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
 This schedule applies to services provided by a participating General Dentist and is an extensive list of most common procedures. The purpose of this schedule is to establish the maximum fee that a General
This schedule applies to services provided by a participating General Dentist and is an extensive list of most common procedures. The purpose of this schedule is to establish the maximum fee that a General
 This schedule applies to services provided by a participating General Dentist and is an extensive list of most common procedures. The purpose of this schedule is to establish the maximum fee that a General
This schedule applies to services provided by a participating General Dentist and is an extensive list of most common procedures. The purpose of this schedule is to establish the maximum fee that a General
BOSTON TEACHERS UNION PARAPROFESSIONAL HEALTH AND WELFARE FUND Schedule of Covered Dental Procedures for the Dental Plan - Effective January 1, 2009
 TYPE 1 D0120 Periodic oral evaluation 27.81 D0140 Limited oral evaluation - problem focused 43.15 D0145 Oral evaluation for a patient under three years of age and 22.20 counseling with primary caregiver
TYPE 1 D0120 Periodic oral evaluation 27.81 D0140 Limited oral evaluation - problem focused 43.15 D0145 Oral evaluation for a patient under three years of age and 22.20 counseling with primary caregiver
Course Syllabus Wayne County Community College District DA 120 Dental Specialties
 Course Syllabus Wayne County Community College District DA 120 Dental Specialties CREDIT HOURS: 2.00 CONTACT HOURS:.00 COURSE DESCRIPTION: This is a lecture course designed to expose the dental assisting
Course Syllabus Wayne County Community College District DA 120 Dental Specialties CREDIT HOURS: 2.00 CONTACT HOURS:.00 COURSE DESCRIPTION: This is a lecture course designed to expose the dental assisting
DELTA DENTAL PPO EPO PLAN DESIGN CP070
 DELTA DENTAL PPO EPO PLAN DESIGN CP070 SCHEDULE OF BENEFITS AND The benefits shown below are performed as deemed appropriate by the attending Dentist subject to the limitations and exclusions of the program.
DELTA DENTAL PPO EPO PLAN DESIGN CP070 SCHEDULE OF BENEFITS AND The benefits shown below are performed as deemed appropriate by the attending Dentist subject to the limitations and exclusions of the program.
Improve your smile and overall well-being with. Dental Health Services. Dental Health Services. Difference today!
 Improve your smile and overall well-being with Dental Health Services Great oral health is essential for your overall well-being. With a Dental Health Services plan, you can achieve a healthy smile while
Improve your smile and overall well-being with Dental Health Services Great oral health is essential for your overall well-being. With a Dental Health Services plan, you can achieve a healthy smile while
Educational Training Document
 Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
NC Medicaid Dental Reimbursement Rates General Dentist, Oral Surgeon, Pediatric Dentist, Periodontist, & Orthodontist Effective Date: January 1, 2014
 NC Medicaid Dental Reimbursement Rates General Dentist, Oral Surgeon, Pediatric Dentist, Periodontist, & Orthodontist Effective Date: January 1, 2014 The inclusion of a rate on this table does not guarantee
NC Medicaid Dental Reimbursement Rates General Dentist, Oral Surgeon, Pediatric Dentist, Periodontist, & Orthodontist Effective Date: January 1, 2014 The inclusion of a rate on this table does not guarantee
IRON WORKERS BENEFIT TRUST SCHEDULE OF DENTAL SERVICES AND SUPPLIES D0100-D0999 I. Diagnostic Clinical Oral Evaluations periodic oral evaluation
 D0120 IRON WORKERS BENEFIT TRUST SCHEDULE OF DENTAL SERVICES AND SUPPLIES D0100-D0999 I. Diagnostic Clinical Oral Evaluations periodic oral evaluation established patient* $ 66.50 D0140 limited oral evaluation
D0120 IRON WORKERS BENEFIT TRUST SCHEDULE OF DENTAL SERVICES AND SUPPLIES D0100-D0999 I. Diagnostic Clinical Oral Evaluations periodic oral evaluation established patient* $ 66.50 D0140 limited oral evaluation
Exclusive Panel Option (EPO 1-B) a feature of the Delta Dental PPO Denver Public Schools- Group #
 Exclusive Panel Option (EPO 1-B) a feature of the Delta Dental PPO Denver Public Schools- Group #6694 7.2011 MAXIMUM BENEFIT Calendar Year Orthodontic Lifetime CALENDAR YEAR DEDUCTIBLE WHO CAN BE COVERED
Exclusive Panel Option (EPO 1-B) a feature of the Delta Dental PPO Denver Public Schools- Group #6694 7.2011 MAXIMUM BENEFIT Calendar Year Orthodontic Lifetime CALENDAR YEAR DEDUCTIBLE WHO CAN BE COVERED
