Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review
|
|
|
- Elaine George
- 5 years ago
- Views:
Transcription
1 Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) ! The Author(s) 2018 Reprints and permissions: sagepub.co.uk/journalspermissions.nav DOI: / journals.sagepub.com/home/imr Wen-Ling Hsu 1,2, Shu-Min Chang 1, Pei-Yin Wu 3 and Chin-Chuan Chang 1,4 Abstract Autoimmune pancreatitis (AP) is a rare autoimmune pancreatic manifestation of systemic immunoglobulin G4 (IgG4)-related sclerosing disease. Distinguishing between AP and pancreatic cancer is crucial because the clinical courses, treatments, and prognoses of these two disease entities are quite different. We herein report a case involving a 52-year-old man with subacute epigastralgia who visited our hospital for evaluation of a suspicious pancreatic mass found during esophagogastroduodenoscopy. Enhanced computed tomography (CT) revealed an enlarged lesion in the pancreatic head with encasement of hepatic vessels. The lesion also exhibited increased 18 F- fluorodeoxyglucose accumulation on positron emission tomography/ct imaging, which was highly suggestive of pancreatic cancer. After open biopsy, morphologic examination showed an inflammatory infiltrate in the pancreas, which was compatible with chronic sclerotic pancreatitis. Further laboratory tests revealed an elevated serum IgG4 level, and the diagnosis of sclerotic pancreatitis was then confirmed. After corticosteroid treatment, the pancreatic lesion showed shrinkage on follow-up CT, and the serum IgG4 titer decreased to the normal range. This case suggests that clinicians should be familiar with the clinical presentations and diagnostic criteria of AP versus pancreatic cancer. An awareness of the differences between these diseases may avoid misdiagnosis and unnecessary surgical intervention. 1 Department of Nuclear Medicine, Kaohsiung Medical University Hospital, Kaohsiung, Taiwan 2 Department of Medical Imaging and Radiological Sciences, Kaohsiung Medical University, Kaohsiung, Taiwan 3 Concord Clinic, Linya District, Kaohsiung, Taiwan 4 Institute of Clinical Medicine, Kaohsiung Medical University, Kaohsiung, Taiwan Corresponding author: Chin-Chuan Chang, Department of Nuclear Medicine, Kaohsiung Medical University Hospital, No. 100 Tzyou 1st Road, Kaohsiung 80756, Taiwan. chinuan@gmail.com Creative Commons Non Commercial CC-BY-NC: This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 License ( which permits non-commercial use, reproduction and distribution of the work without further permission provided the original work is attributed as specified on the SAGE and Open Access pages (
2 1658 Journal of International Medical Research 46(4) Keywords Autoimmune pancreatitis, pancreatic cancer, IgG4-related sclerosing disease, FDG PET/CT, epigastralgia, inflammatory infiltration Date received: 24 August 2017; accepted: 24 October 2017 Introduction Autoimmune pancreatitis (AP) is a rare autoimmune pancreatic manifestation of systemic immunoglobulin G4 (IgG4)- related sclerosing disease. AP is clinically characterized by irregular narrowing of the main pancreatic duct, lymphoplasmacytic inflammation of the pancreas, and hypergammaglobulinemia. The presence of a hypermetabolic pancreatic mass allows AP to clinically mimic pancreatic cancer. Differentiation between AP and pancreatic cancer is crucial because the clinical courses, treatments, and prognoses of these two disease entities are quite different. AP responds well to glucocorticoid therapy, while pancreatic cancer may require surgical intervention with or without adjuvant chemotherapy. Although the diagnostic criteria for AP have been revised, 1 4 clinical or radiological differentiation between AP and pancreatic cancer remains difficult. We herein report a case involving a patient with AP who presented with a hypermetabolic pancreatic mass that mimicked pancreatic cancer. Case report A 52-year-old man with medically controlled hypertension visited a local medical clinic because of a 1-month history of intermittent epigastralgia. The symptom was not associated with food intake or daily exercise, and there were no aggravating factors. However, the epigastralgia improved to a certain degree when the patient assumed a bent body position. His laboratory tests revealed mildly elevated liver enzymes, including glutamate oxaloacetate transaminase of 64 IU/L (reference range, IU/L), glutamate pyruvate transaminase of 80 IU/L (reference range, IU/L), alkaline phosphate of 178 IU/L (reference range, IU/L), total bilirubin of 2.26 mg/dl (reference range, mg/dl), direct bilirubin of 1.46 mg/dl (reference range, mg/dl), and gamma glutamyl transpeptidase of 391 IU/L (reference range, 7 64 IU/L). The results of other laboratory tests, including a complete blood count/differential count, cholesterol profile, electrolytes, renal function parameters, and tumor markers (including a-fetoprotein, carbohydrate antigen 19-9, and carcinoembryonic antigen) were within the normal range. Esophagogastroduodenoscopy revealed gastritis and external compression of the duodenum, which raised suspicion for a pancreatic tumor. Abdominal ultrasonography showed a tumor in the uncinate process of the pancreas. The patient then presented to Kaohsiung Medical University Hospital, a tertiary medical center in southern Taiwan, for further medical evaluation. Abdominal computed tomography (CT) with contrast enhancement (Figure 1) revealed a lobulated mass lesion with a cystic component in the pancreatic head. Encasement of the common hepatic artery and main portal vein was also depicted. A malignant pancreatic tumor was suspected, and CT-guided biopsy of the lesion was performed. The tiny specimen showed fibrous tissue with focal sclerotic stroma and focal lymphoid cell aggregation. Cytokeratin and synaptophysin immunostaining revealed no
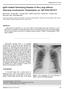
3 Hsu et al Figure 1. A sequential axial abdominal computed tomography scan shows a lobulated mass lesion with a cystic component and peripheral enhancement in the head and proximal body of the pancreas with exophytic growth (white arrows in a c). Encasement of the common hepatic artery and main portal vein is also depicted (white arrowheads in d ƒ). epithelial cancerous cells, and CD20 and CD3 immunostaining revealed no monoclonal lymphocyte proliferation. However, the diagnosis remained uncertain because the possibility of lymphoma could not be totally excluded. After the CT-guided biopsy, the patient developed more severe abdominal pain and an intermittent fever. Fluid accumulation was noted on abdominal ultrasonography. Empiric antibiotics (piperacillin/ tazobactam) were prescribed. A subsequent blood culture showed no growth of aerobic or anaerobic bacteria. After the fever subsided, 18 F-fluorodeoxyglucose (FDG) positron emission tomography (PET)/CT was performed and showed an FDG-avid, hypermetabolic, swollen soft tissue mass in the pancreatic head with a maximum standardized uptake value of 8.2 (Figure 2). Adjacent low-grade FDGavid lymph nodes with a maximum standardized uptake value of 3.1 were also noted. These findings were highly suggestive of a malignant pancreatic tumor with metastatic lymphadenopathy. No FDGavid lesions were present in the bilateral salivary glands, retroperitoneal spaces, or biliary tracts. An open biopsy was performed to obtain a larger specimen of the pancreatic lesion and confirm the diagnosis. Pathological examination showed chronic inflammatory infiltration of lymphocytes and plasma cells around the ductules and acini with sclerotic stroma (Figure 3). Cytokeratin immunostaining failed to disclose any epithelial malignancy. CD3 and CD20 immunostaining
4 1660 Journal of International Medical Research 46(4) Figure 2. Positron emission tomography/computed tomography (PET/CT) using 18 F-fluorodeoxyglucose shows a hypermetabolic tumor in the head of the pancreas with a maximum standardized uptake value of 8.2 (arrowheads). (a) Maximal intensity projection. (b) PET image. (c, d) Non-enhanced CT and fused PET and CT images at corresponding levels, respectively. Figure 3. Representative histological pictures (hematoxylin and eosin stain). (a) 100, (b) 400. These images show chronic inflammatory infiltration of lymphocytes and plasma cells around ductules and acini with sclerotic stroma in the pancreas.
5 Hsu et al Figure 4. (a f) Axial abdominal computed tomography scan 3 months after corticosteroid treatment shows marked shrinkage of the previous lobulated mass lesion (arrowheads). revealed a mixed population of B and T cells. Further immunohistochemical studies were negative for CD5, cyclin D1, Bcl-2, and CD10. Taken together, the morphology and immunohistochemical studies suggested a diagnosis of chronic sclerotic pancreatitis. We further checked the patient s serum immunoglobulin titers. Laboratory examination showed elevation of IgG (2390 mg/dl; reference range, mg/dl) and IgG4 (1170 mg/dl; reference range, mg/l), which was consistent with the clinical presentation of chronic sclerosing pancreatitis. IgA and IgM were within the reference ranges (310 mg/l and 142 mg/dl, respectively). The patient thereafter began corticosteroid treatment. One month after the corticosteroid treatment, his IgG and IgG4 levels decreased to 1920 mg/dl and 1110 mg/l, respectively. Three months after the corticosteroid treatment, follow-up abdominal CT showed shrinkage of the lesion (Figure 4), and the IgG and IgG4 levels decreased to 1090 mg/dl and 532 mg/l, respectively. After 48 months of follow-up, the patient was in good condition without symptoms or signs of relapse. The patient provided informed consent for all medical procedures performed. The institutional review board of our hospital waived the need for ethics approval for publication of this report because of the study design (retrospective chart review). Discussion AP is a type of rare chronic pancreatitis characterized by an autoimmune inflammatory mechanism. It occurs in both sexes; however, it is predominant in men (male: female ratio of 3:1). 5 With respect to age distribution, AP occurs mostly in elderly patients. 6 Clinically, patients with AP may present with obstructive jaundice and abdominal pain, and imaging examination may reveal a swelling mass. Impairment of
6 1662 Journal of International Medical Research 46(4) pancreatic endocrine or exocrine function may also be present. Up to half of patients may have glucose intolerance. Some patients are diagnosed with diabetes mellitus and AP simultaneously, while some exhibit progression of pre-existing diabetes mellitus at the onset of AP. The clinical symptoms of AP, especially localized AP, mimic those of pancreatic cancer. However, the clinical course, treatment, and prognosis are quite different between AP and pancreatic cancer; thus, correct differentiation between these two diseases is clinically very important. AP is classified into type 1 or type 2 depending on its histopathological findings. Type 1 AP, also termed lymphoplasmacytic sclerosing pancreatitis, is microscopically characterized by dense infiltration of T lymphocytes and IgG4-postive plasma cells, storiform fibrosis, and obliterative phlebitis. The main histological feature of type 2 AP (idiopathic duct-centric pancreatitis) is neutrophilic infiltration in the epithelium of the pancreatic ducts. No diagnostic serologic markers for AP are currently available. Therefore, the diagnosis is mainly based upon the presence of abnormal signs unique to AP. Diagnostic criteria were recently developed in Asia 1,2 and the United States. 3 In 2008, Korean and Japanese pancreatologists revised the diagnostic consensus on AP. 4 In June 2017, Chari 7 wrote an article on the evolution of the diagnostic criteria for AP while celebrating the 15th anniversary of clinical gastroenterology and hepatology. Five cardinal features are used to diagnose AP: imaging findings of the pancreatic ducts and parenchyma, serology, involvement of other organs, pancreatic histology, and clinical responsiveness to steroid therapy. The typical imaging finding of the pancreatic ducts and parenchyma is diffuse enlargement with delayed enhancement, sometimes associated with rim-like enhancement. This enhancement pattern is caused by fibroinflammatory change of the peripancreatic adipose tissue, which is rarely seen in pancreatic cancer. Corresponding patterns of perfusion abnormalities are seen on magnetic resonance imaging (MRI). Diffusionweighted MRI shows lower apparent diffusion coefficients, playing an important role in differentiating AP from pancreatic cancer. 8 Endoscopic retrograde cholangiopancreatography may show irregular narrowing of the main pancreatic duct. Other less characteristic findings include focal to multifocal enlargement of the pancreatic glandular tissues. The patient in the present case did not undergo MRI examination. Contrastenhanced CT showed a lobulated mass lesion with a cystic component, and heterogeneous enhancement was noted in the pancreatic head. The imaging features of enhanced CT were not typical for localized AP. Certain pancreatic neoplasms, such as mucinous cystadenocarcinoma of the pancreas, may present characteristic imaging findings. Furthermore, because of the localized entity and encasement of the common hepaticarteryandmainportalveininthepresent case, it was difficult to differentiate the lesion from pancreatic cancer. Elevated Hounsfield units during the delayed phase of the CT scan may help distinguish localized AP from pancreatic cancer 9 ; however, the clinician and radiologist in the present case suggested tissue biopsy because a malignant pancreatic tumor could not be completely excluded. AP appears to be a pancreatic manifestation of IgG4-related sclerosing disease based on histological and immunohistochemical examination of various organs in patients with AP. Such disease, which may clinically overlap or include AP, sclerosing cholecystitis/cholangitis, sclerosing sialadenitis/dacryoadenitis, inflammatory pseudotumors, and retroperitoneal fibrosis, is a systemic disorder affecting multiple organs with clinically apparent tissue fibrosis and obliterative phlebitis. 10 The disease extent and degree vary clinically depending on
7 Hsu et al the size and numbers of involved organs. 11 The affected organs, including the pancreas, may be synchronous or metachronous. 12 An FDG PET/CT scan can help differentiate AP from pancreatic malignancy, especially in patients with increased uptake in the salivary glands, lacrimal glands, kidneys, and sometimes in other extrapancreatic organs. 13 Although some reports have described clinical detection of AP by FDG PET/CT, 14,15 improvement is needed in the use of FDG PET/CT for differential diagnosis between AP and pancreatic cancer. 16 Differentiation is difficult because both AP and pancreatic cancer present a hypermetabolic status and increased FDG accumulation, as shown in the present case. AP is the pancreatic manifestation of IgG4-related sclerosing disease; approximately two-thirds of patients with AP have an elevated serum IgG4 level. 17 However, elevation of serum IgG4 is not specific to AP. Mild elevation (1 2 times the upper limit of the reference range) is seen in 10% to 15% of patients with cholangiocarcinoma, 18 primary sclerosing cholangitis, 19 and pancreatic malignancy. 20 In a study by Hamano et al., 21 a significant difference in the IgG4 concentration was observed between patients with and without AP (median, 663 vs. 51 mg/dl, respectively). The use of a cut-off value for a higher serum IgG4 concentration (>135 mg/dl) resulted in high accuracy (97%), sensitivity (95%), and specificity (97%) for the differentiation of AP from pancreatic cancer. In our patient, the serum IgG4 level was 1170 mg/dl at the time of the initial diagnosis. This was a clue to the diagnosis of AP. However, the IgG4 level was about 1.4 times the upper limit of the reference range. Because of different reference ranges, we could not apply the above-mentioned cutoff value to our patient. Confirmative diagnosis in our patient was based on pathological examination. The patient in this case underwent an open biopsy to obtain a confirmative pathological specimen. This procedure was relatively invasive. The use of endoscopic ultrasonography-guided fine needle aspiration (EUS-FNA) to evaluate solid pancreatic masses has been described in previous reports. 22,23 EUS-FNA is less invasive and has a high accuracy rate (>90%) for distinguishing benign from malignant pancreatic masses. 24 EUS-FNA may be suggested to confirm the diagnosis when esophagogastroduodenoscopy reveals external compression of the duodenum, which raises suspicion for a pancreatic tumor. AP is a fibroinflammatory disease in which severe inflammation may be present in the early phase. Effective treatment should involve anti-inflammatory therapy to achieve relief from symptoms and perhaps decrease or delay the progression to fibrosis. Furthermore, when it is difficult to obtain a definitive diagnosis clinically, preceding corticosteroid therapy may help the diagnosis. A poor response to therapy may raise the possibility of a malignant pancreatic tumor, and reevaluation of the diagnosis may be needed. According to established guidelines, 25,26 steroid treatment is the standard therapy for AP. Initially, oral prednisolone (30 40 mg/day or 0.6 mg/kg per day) is administered for 2 to 4 weeks; thereafter, the dose is tapered by 5 mg every 1 to 2 weeks. This treatment may be continued for 3 to 6 months while carefully monitoring the patient s symptoms and biochemical, serological, and imaging findings until a maintenance dose is reached. Morphological and serological evaluation should be performed to assess the disease responsiveness. Our patient s IgG and IgG4 levels decreased within 1 month and continued to decrease to the normal range at 3 months after the initial steroid therapy was begun. This response helped to confirm the disease entity. On the follow-up CT scan 3 months later,
8 1664 Journal of International Medical Research 46(4) the tumor in the pancreatic head had shrunk. To prevent relapse, maintenance therapy at 2.5 to 5.0 mg/day is recommended for almost all patients for at least 6 months. Maintenance therapy may be withdrawn for patients who have achieved complete remission 1 year after the initial steroid therapy. The patient remained in good condition without symptoms or signs of relapse during a follow-up period of 48 months. The results of a multicenter trial on the best approach to long-term management of AP are being eagerly awaited. In summary, AP is an IgG4-related sclerosing disease of the pancreas that may also involve other organs. The prevalence of AP is relatively low compared with pancreatic cancer. It is a benign disease with different therapy and prognosis compared with malignant pancreatic cancer; however, misdiagnosis between these two diseases readily occurs, especially in patients with localized AP. Clinicians should be aware of this disease and be familiar with the diagnostic criteria to avoid misdiagnosis and unnecessary surgical intervention. Acknowledgments We thank Dr. Chun-Chieh Wu at the Department of Pathology, Kaohsiung Medical University Hospital, Kaohsiung, Taiwan, for his review of the pathological slides and help with the diagnosis. Declaration of conflicting interests The authors declare that there is no conflict of interest. Funding This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors. References 1. Kim KP, Kim MH, Kim JC, et al. Diagnostic criteria for autoimmune chronic pancreatitis revisited. World J Gastroenterol 2006; 12: /05/ Okazaki K, Kawa S, Kamisawa T, et al. Clinical diagnostic criteria of autoimmune pancreatitis: revised proposal. J Gastroenterol 2006; 41: /08/26. DOI: / s Chari ST, Smyrk TC, Levy MJ, et al. Diagnosis of autoimmune pancreatitis: the Mayo Clinic experience. Clin Gastroenterol Hepatol 2006; 4: quiz /07/18. DOI: /j.cgh Otsuki M, Chung JB, Okazaki K, et al. Asian diagnostic criteria for autoimmune pancreatitis: consensus of the Japan-Korea Symposium on Autoimmune Pancreatitis. J Gastroenterol 2008; 43: /07/ 05. DOI: /s Hart PA, Kamisawa T, Brugge WR, et al. Long-term outcomes of autoimmune pancreatitis: a multicentre, international analysis. Gut 2013; 62: /12/13. DOI: /gutjnl Kamisawa T, Yoshiike M, Egawa N, et al. Chronic pancreatitis in the elderly in Japan. Pancreatology 2004; 4: ; discussion /05/19. DOI: / Chari ST. Diagnosis of autoimmune pancreatitis: the evolution of diagnostic criteria for a rare disease. Clin Gastroenterol Hepatol 2017; 15: /06/22. DOI: /j.cgh Kamisawa T, Takuma K, Anjiki H, et al. Differentiation of autoimmune pancreatitis from pancreatic cancer by diffusionweighted MRI. Am J Gastroenterol 2010; 105: /03/11. DOI: / ajg Sun GF, Zuo CJ, Shao CW, et al. Focal autoimmune pancreatitis: radiological characteristics help to distinguish from pancreatic cancer. World J Gastroenterol 2013; 19: /06/27. DOI: /wjg. v19.i Takuma K, Kamisawa T, Gopalakrishna R, et al. Strategy to differentiate autoimmune pancreatitis from pancreas cancer. World J Gastroenterol 2012; 18: /03/ 15. DOI: /wjg.v18.i
9 Hsu et al Kamisawa T, Takuma K, Egawa N, et al. Autoimmune pancreatitis and IgG4-related sclerosing disease. Nat Rev Gastroenterol Hepatol 2010; 7: /06/16. DOI: /nrgastro Takuma K, Kamisawa T, Anjiki H, et al. Metachronous extrapancreatic lesions in autoimmune pancreatitis. Intern Med 2010; 49: /03/ Kamisawa T, Takum K, Anjiki H, et al. FDG-PET/CT findings of autoimmune pancreatitis. Hepatogastroenterology 2010; 57: /08/ Han L, Jiang L, Tan H, et al. An atypical case of IgG4-related sclerosing pancreatitis on PET/CT imaging. Clin Nucl Med 2014; 39: e236 e /04/13. DOI: / RLU.0b013e Cao Z, Tian R, Zhang T, et al. Localized autoimmune pancreatitis: report of a case clinically mimicking pancreatic cancer and a literature review. Medicine (Baltimore) 2015; 94: e /10/27. DOI: / MD Nanni C, Romagnoli R, Rambaldi I, et al. FDG PET/CT in autoimmune pancreatitis. Eur J Nucl Med Mol Imaging 2014; 41: /02/25. DOI: / s Kamisawa T, Chari ST, Giday SA, et al. Clinical profile of autoimmune pancreatitis and its histological subtypes: an international multicenter survey. Pancreas 2011; 40: /07/13. DOI: / MPA.0b013e a Oseini AM, Chaiteerakij R, Shire AM, et al. Utility of serum immunoglobulin G4 in distinguishing immunoglobulin G4-associated cholangitis from cholangiocarcinoma. Hepatology 2011; 54: /06/16. DOI: /hep Bjornsson E, Chari S, Silveira M, et al. Primary sclerosing cholangitis associated with elevated immunoglobulin G4: clinical characteristics and response to therapy. Am J Ther 2011; 18: /03/17. DOI: /MJT.0b013e3181c9dac Raina A, Krasinskas AM, Greer JB, et al. Serum immunoglobulin G fraction 4 levels in pancreatic cancer: elevations not associated with autoimmune pancreatitis. Arch Pathol Lab Med 2008; 132: /01/ 10. DOI: / (2008)132[48: SIGFLI]2.0.CO; Hamano H, Kawa S, Horiuchi A, et al. High serum IgG4 concentrations in patients with sclerosing pancreatitis. N Engl J Med 2001; 344: /03/10. DOI: / NEJM Kanno A, Masamune A, Fujishima F, et al. Diagnosis of autoimmune pancreatitis by EUS-guided FNA using a 22-gauge needle: a prospective multicenter study. Gastrointest Endosc 2016; 84: e /04/14. DOI: /j.gie Kamisawa T, Anjiki H, Takuma K, et al. Endoscopic approach for diagnosing autoimmune pancreatitis. World J Gastrointest Endosc 2010; 2: /12/17. DOI: /wjge.v2.i Imai K, Matsubayashi H, Fukutomi A, et al. Endoscopic ultrasonography-guided fine needle aspiration biopsy using 22-gauge needle in diagnosis of autoimmune pancreatitis. Dig Liver Dis 2011; 43: / 07/08. DOI: /j.dld Kamisawa T, Shimosegawa T, Okazaki K, et al. Standard steroid treatment for autoimmune pancreatitis. Gut 2009; 58: /04/29. DOI: /gut Kamisawa T, Okazaki K, Kawa S, et al. Japanese consensus guidelines for management of autoimmune pancreatitis: III. Treatment and prognosis of AIP. J Gastroenterol 2010; 45: /03/ 10. DOI: /s
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Diagnostic Algorithm for Autoimmune Pancreatitis in Korea
 Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic Pancreatitis of Other Etiology
 94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis?
 CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
Autoimmune Pancreatitis: A Great Imitator
 Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
How 5 Diseases Became One. Moez Tajdin R3 McGill University
 How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
The most common presentation of autoimmune pancreatitis. A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
Immunoglobulin G4-Related Disease with Several Inflammatory Foci
 CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
Type 2 Autoimmune Pancreatitis with Crohn s Disease
 doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
IgG4-related sclerosing disease
 IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease
 Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy
 ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma
 Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
 Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Autoimmune Pancreatitis: A Succinct Overview
 REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT
 J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management
 Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Autoimmune pancreatitis (AIP) can be defined as a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
Autoimmune pancreatitis (AIP), a clinical entity originally
 Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Review Article The Utility of Serum IgG4 Concentrations as a Biomarker
 International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
Intrahepatic Sarcomatoid Cholangiocarcinoma with Portal Vein Thrombosis: A Case Report 1
 Intrahepatic Sarcomatoid Cholangiocarcinoma with Portal Vein Thrombosis: A Case Report 1 Jae-Hoon Lim, M.D., Jin Woong Kim, M.D., Suk Hee Heo, M.D., Yong Yeon Jeong, M.D., Heoung Keun Kang, M.D. A 53-year-old
Intrahepatic Sarcomatoid Cholangiocarcinoma with Portal Vein Thrombosis: A Case Report 1 Jae-Hoon Lim, M.D., Jin Woong Kim, M.D., Suk Hee Heo, M.D., Yong Yeon Jeong, M.D., Heoung Keun Kang, M.D. A 53-year-old
Overview of Diagnostic Criteria for Autoimmune Pancreatitis
 2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
IgG4 Disease. General Principles of IgG4-related disease. EL Cluvar, AC Bateman
 IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
A case of retroperitoneal fibrosis responding to steroid therapy
 Challenging Clinical Cases Vol. 43 (6): 1185-1189, November - December, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0520 A case of retroperitoneal fibrosis responding to steroid therapy Ryuta Watanabe 1, Akira
Challenging Clinical Cases Vol. 43 (6): 1185-1189, November - December, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0520 A case of retroperitoneal fibrosis responding to steroid therapy Ryuta Watanabe 1, Akira
Autoimmune pancreatitis (AIP) was described more than a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4
 238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
Autoimmune Pancreatitis & Cholangiopathy. Goal and Objectives
 Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Overview of the Immunoglobulin G4-related Disease Spectrum
 Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Radiology Pathology Conference
 Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers
 Case Reports in Medicine Volume 2015, Article ID 832463, 4 pages http://dx.doi.org/10.1155/2015/832463 Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers Alessandro
Case Reports in Medicine Volume 2015, Article ID 832463, 4 pages http://dx.doi.org/10.1155/2015/832463 Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers Alessandro
Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
Pancreatic Cancer Masquerading as Pancreatitis
 Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
Evaluation of Liver Mass Lesions. American College of Gastroenterology 2013 Regional Postgraduate Course
 Evaluation of Liver Mass Lesions American College of Gastroenterology 2013 Regional Postgraduate Course Lewis R. Roberts, MB ChB, PhD Division of Gastroenterology and Hepatology Mayo Clinic College of
Evaluation of Liver Mass Lesions American College of Gastroenterology 2013 Regional Postgraduate Course Lewis R. Roberts, MB ChB, PhD Division of Gastroenterology and Hepatology Mayo Clinic College of
Case Report Multiple Hypovascular Tumors in Kidney: A Rare Case Report and Differential Diagnosis
 Volume 2013, Article ID 595193, 4 pages http://dx.doi.org/10.1155/2013/595193 Case Report Multiple Hypovascular Tumors in Kidney: A Rare Case Report and Differential Diagnosis Pei-Yu Wu, 1 Sheng-Fung Lin,
Volume 2013, Article ID 595193, 4 pages http://dx.doi.org/10.1155/2013/595193 Case Report Multiple Hypovascular Tumors in Kidney: A Rare Case Report and Differential Diagnosis Pei-Yu Wu, 1 Sheng-Fung Lin,
Among the benign intraepithelial melanocytic proliferations, Inflamed Conjunctival Nevi. Histopathological Criteria. Resident Short Reviews
 Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Autoimmune Pancreatitis and Retroperitoneal Fibrosis
 Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Renal manifestations of IgG4-related systemic disease
 Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
IgG4-related Sclerosing Disease: Autoimmune Pancreatitis and Extrapancreatic
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus
 Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus Omar Abu Suliman, MBBS, SB-ORL Senior Registrar, otolaryngology Head & neck surgery King Abdullah Medical City, Makkah,
Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus Omar Abu Suliman, MBBS, SB-ORL Senior Registrar, otolaryngology Head & neck surgery King Abdullah Medical City, Makkah,
IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal
 CASE REPORT IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal Miho Otani 1, Masahiro Morinaga 1, Yoshihiko Nakajima 1, Hiromi Tomioka 2, Michiko Nishii
CASE REPORT IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal Miho Otani 1, Masahiro Morinaga 1, Yoshihiko Nakajima 1, Hiromi Tomioka 2, Michiko Nishii
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
LIVER SPECIALTY CONFERENCE USCAP Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA
 LIVER SPECIALTY CONFERENCE USCAP 2016 Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA Nothing to disclose Case History 47-year-old male, long standing ileal
LIVER SPECIALTY CONFERENCE USCAP 2016 Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA Nothing to disclose Case History 47-year-old male, long standing ileal
췌장의단일종괴형태로재발해원발성췌장암으로오인된재발성폐암
 Case Report The Korean Journal of Pancreas and Biliary Tract 2018;23:172-176 https://doi.org/10.15279/kpba.2018.23.4.172 pissn 1976-3573 eissn 2288-0941 췌장의단일종괴형태로재발해원발성췌장암으로오인된재발성폐암 대구가톨릭대학교의과대학내과학교실
Case Report The Korean Journal of Pancreas and Biliary Tract 2018;23:172-176 https://doi.org/10.15279/kpba.2018.23.4.172 pissn 1976-3573 eissn 2288-0941 췌장의단일종괴형태로재발해원발성췌장암으로오인된재발성폐암 대구가톨릭대학교의과대학내과학교실
CASE REPORT. Masakuni Fujii 1*, Masao Yoshioka 1, Takefumi Niguma 2, Hiroaki Saito 1,ToruKojima 2, Soichiro Nose 3 and Junji Shiode 1
 Fujii et al. Journal of Medical Case Reports 2014, 8:243 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A solid pseudopapillary neoplasm without cysts that occurred in a patient diagnosed by endoscopic
Fujii et al. Journal of Medical Case Reports 2014, 8:243 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A solid pseudopapillary neoplasm without cysts that occurred in a patient diagnosed by endoscopic
Autoimmune pancreatitis
 Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA. Dr. Tejaswi Sindhiya Ragni
 AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case report Solid pseudopapillary tumor: a rare neoplasm of the pancreas
 Gastroenterology Report 2 (2014) 145 149, doi:10.1093/gastro/gou006 Advance access publication 28 February 2014 Case report Solid pseudopapillary tumor: a rare neoplasm of the pancreas Asim Shuja 1, *
Gastroenterology Report 2 (2014) 145 149, doi:10.1093/gastro/gou006 Advance access publication 28 February 2014 Case report Solid pseudopapillary tumor: a rare neoplasm of the pancreas Asim Shuja 1, *
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings
 Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
Dual-time-point FDG-PET/CT Imaging of Temporal Bone Chondroblastoma: A Report of Two Cases
 Dual-time-point FDG-PET/CT Imaging of Temporal Bone Chondroblastoma: A Report of Two Cases Akira Toriihara 1 *, Atsunobu Tsunoda 2, Akira Takemoto 3, Kazunori Kubota 1, Youichi Machida 1, Ukihide Tateishi
Dual-time-point FDG-PET/CT Imaging of Temporal Bone Chondroblastoma: A Report of Two Cases Akira Toriihara 1 *, Atsunobu Tsunoda 2, Akira Takemoto 3, Kazunori Kubota 1, Youichi Machida 1, Ukihide Tateishi
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Autoimmune pancreatitis associated to renal and aortic involvement: 3.0-TESLA magnetic resonance imaging in diagnosis and follow-up
 CASE REPORT Autoimmune pancreatitis associated to renal and aortic involvement: 3.0-TESLA magnetic resonance imaging in diagnosis and follow-up Rossella Graziani 1, Paoletta Preatoni 2, Silvia Carrara
CASE REPORT Autoimmune pancreatitis associated to renal and aortic involvement: 3.0-TESLA magnetic resonance imaging in diagnosis and follow-up Rossella Graziani 1, Paoletta Preatoni 2, Silvia Carrara
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
IgG4-Related Disease: Dataset of 235 Consecutive Patients
 IgG-Related Disease: Dataset of 235 Consecutive Patients Dai Inoue, MD, PhD, Kotaro Yoshida, MD, PhD, Norihide Yoneda, MD, PhD, Kumi Ozaki, MD, PhD, Takashi Matsubara, MD, PhD, Keiichi Nagai, MD, PhD,
IgG-Related Disease: Dataset of 235 Consecutive Patients Dai Inoue, MD, PhD, Kotaro Yoshida, MD, PhD, Norihide Yoneda, MD, PhD, Kumi Ozaki, MD, PhD, Takashi Matsubara, MD, PhD, Keiichi Nagai, MD, PhD,
Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related Disease
 Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Endoscopic Resection of Ampullary Neuroendocrine Tumor
 CASE REPORT Endoscopic Resection of Ampullary Neuroendocrine Tumor Hiroyuki Fukasawa, Shigetaka Tounou, Masashi Nabetani and Tomoki Michida Abstract We report the case of a 57-year-old man with a 1.0-cm
CASE REPORT Endoscopic Resection of Ampullary Neuroendocrine Tumor Hiroyuki Fukasawa, Shigetaka Tounou, Masashi Nabetani and Tomoki Michida Abstract We report the case of a 57-year-old man with a 1.0-cm
FDG-PET Findings of Intraductal Oncocytic Papillary Neoplasms of the Pancreas: Two Case Reports
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
IgG4-related disease: features and treatment response in a multi-ethnic cohort in Singapore
 IgG4-related disease: features and treatment response in a multi-ethnic cohort in Singapore W. Fong 1,2,3, I. Liew 1, D. Tan 2,3,4, K.H. Lim 5, A. Low 6, Y.Y. Leung 1,2 1 Department of Rheumatology and
IgG4-related disease: features and treatment response in a multi-ethnic cohort in Singapore W. Fong 1,2,3, I. Liew 1, D. Tan 2,3,4, K.H. Lim 5, A. Low 6, Y.Y. Leung 1,2 1 Department of Rheumatology and
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction
 Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
IgG4-related systemic disease (ISD) is a multisystem
 Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Key Points: Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective. Jenny Heathcote, MD. University of Toronto
 Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
Biliary cancers: imaging diagnosis. Study of 30 cases
 Biliary cancers: imaging diagnosis. Study of 30 cases N Hammoune, S Semlali, M Eddarai, T. Amil, M Zentar, S. El Kandri,, M Benameur,, S Chaouir. Radiology Department. Mohamed V Military Hospital. Rabat-
Biliary cancers: imaging diagnosis. Study of 30 cases N Hammoune, S Semlali, M Eddarai, T. Amil, M Zentar, S. El Kandri,, M Benameur,, S Chaouir. Radiology Department. Mohamed V Military Hospital. Rabat-
Hematologic Malignancies of the Liver : Spectrum of Disease. Zhou Jian
 Hematologic Malignancies of the Liver : Spectrum of Disease Zhou Jian 2015-7-8 Hematologic malignancies include a wide spectrum of lymphoproliferative and myeloproliferative disorders with nodal and extranodal
Hematologic Malignancies of the Liver : Spectrum of Disease Zhou Jian 2015-7-8 Hematologic malignancies include a wide spectrum of lymphoproliferative and myeloproliferative disorders with nodal and extranodal
Title: An ulcerated gastric ulcer and pseudotumour with pancreatic affectation associated with immunoglobulin G4-
 Title: An ulcerated gastric ulcer and pseudotumour with pancreatic affectation associated with immunoglobulin G4- related disease: a case report and literature review Authors: María Isabel Ortuño Moreno,
Title: An ulcerated gastric ulcer and pseudotumour with pancreatic affectation associated with immunoglobulin G4- related disease: a case report and literature review Authors: María Isabel Ortuño Moreno,
A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis
 CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
A Review of Liver Function Tests. James Gray Gastroenterology Vancouver
 A Review of Liver Function Tests James Gray Gastroenterology Vancouver Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
A Review of Liver Function Tests James Gray Gastroenterology Vancouver Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid
 The Korean Journal of Internal Medicine: 20:163-167, 2005 Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid Dae Keun Pyun, M.D., Won Beom Choi, M.D., Myung Hwan Kim, M.D.,
The Korean Journal of Internal Medicine: 20:163-167, 2005 Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid Dae Keun Pyun, M.D., Won Beom Choi, M.D., Myung Hwan Kim, M.D.,
Dr Sneha Shah Tata Memorial Hospital, Mumbai.
 Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Chronic Sclerosing Dacryoadenitis
 The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
IgG4-Related Sclerosing Cholangitis
 REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
Renal Pathology Case Conference. Case 2
 Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
Autoimmune pancreatitis: the classification puzzle
 Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Clinical outcomes and pathological characteristics of immunoglobulin G4-related ophthalmic disease versus orbital inflammatory pseudotumor
 ORIGINAL ARTICLE Korean J Intern Med 2019;34:220-226 Clinical outcomes and pathological characteristics of immunoglobulin G4-related ophthalmic disease versus orbital inflammatory pseudotumor Hong Ki Min
ORIGINAL ARTICLE Korean J Intern Med 2019;34:220-226 Clinical outcomes and pathological characteristics of immunoglobulin G4-related ophthalmic disease versus orbital inflammatory pseudotumor Hong Ki Min
Management of Rare Liver Tumours
 Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
Cystic Disease of the Liver Work Up and Management. Louis Ferrari MD, PGY 3 6/9/16 SUNY Downstate Medical Center
 Cystic Disease of the Liver Work Up and Management Louis Ferrari MD, PGY 3 6/9/16 SUNY Downstate Medical Center The Case 73F presents to clinic after diagnostic laparoscopy at OSH. Known liver mass for
Cystic Disease of the Liver Work Up and Management Louis Ferrari MD, PGY 3 6/9/16 SUNY Downstate Medical Center The Case 73F presents to clinic after diagnostic laparoscopy at OSH. Known liver mass for
Immunoglobulin G4-Related Sclerosing Disease Involving the Urethra: Case Report
 Case Report http://dx.doi.org/10.3348/kjr.2012.13.6.803 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(6):803-807 Immunoglobulin G4-Related Sclerosing Disease Involving the Urethra: Case Report
Case Report http://dx.doi.org/10.3348/kjr.2012.13.6.803 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(6):803-807 Immunoglobulin G4-Related Sclerosing Disease Involving the Urethra: Case Report
FINALIZED SEER SINQ S MAY 2012
 FINALIZED SEER SINQ S MAY 2012 : 20120039 Primary site/heme & Lymphoid Neoplasms: What site do I code this to and what rule applies? How did you arrive at this? Please advise. See discussion. Patient with
FINALIZED SEER SINQ S MAY 2012 : 20120039 Primary site/heme & Lymphoid Neoplasms: What site do I code this to and what rule applies? How did you arrive at this? Please advise. See discussion. Patient with
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts
 Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Ulcerative Colitis and Immunoglobulin G4
 Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Cancers of unknown primary : Knowing the unknown. Prof. Ahmed Hossain Professor of Medicine SSMC
 Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
CASE 1 Plasma Cell Infiltrates: Significance in post liver transplantation and in chronic liver disease
 CASE 1 Plasma Cell Infiltrates: Significance in post liver transplantation and in chronic liver disease Maria Isabel Fiel, M.D. The Mount Sinai Medical Center New York, New York Case A 57 yo man, 7 months
CASE 1 Plasma Cell Infiltrates: Significance in post liver transplantation and in chronic liver disease Maria Isabel Fiel, M.D. The Mount Sinai Medical Center New York, New York Case A 57 yo man, 7 months
Clinical Commissioning Policy Proposition:
 Clinical Commissioning Policy Proposition: Rituximab for immunoglobulin G4-related disease (IgG4-RD) Reference: NHS England A13X07/01 Information Reader Box (IRB) to be inserted on inside front cover for
Clinical Commissioning Policy Proposition: Rituximab for immunoglobulin G4-related disease (IgG4-RD) Reference: NHS England A13X07/01 Information Reader Box (IRB) to be inserted on inside front cover for
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Case of the Day Chest
 Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Testicular relapse of non-hodgkin Lymphoma noted on FDG-PET
 Testicular relapse of non-hodgkin Lymphoma noted on FDG-PET Stephen D. Scotti 1*, Jennifer Laudadio 2 1. Department of Radiology, North Carolina Baptist Hospital, Winston-Salem, NC, USA 2. Department of
Testicular relapse of non-hodgkin Lymphoma noted on FDG-PET Stephen D. Scotti 1*, Jennifer Laudadio 2 1. Department of Radiology, North Carolina Baptist Hospital, Winston-Salem, NC, USA 2. Department of
EUS FNA NEUROENDOCRINE TUMORS. A. Ginès Endocopy Unit Hospital Cínic. Barcelona (Spain)
 EUS FNA NEUROENDOCRINE TUMORS A. Ginès Endocopy Unit Hospital Cínic. Barcelona (Spain) GI NEUROENDOCRINE TUMORS GENERAL CONCEPTS Rare neoplasms arising from the neuroendocrine cells of the GI tract Include:
EUS FNA NEUROENDOCRINE TUMORS A. Ginès Endocopy Unit Hospital Cínic. Barcelona (Spain) GI NEUROENDOCRINE TUMORS GENERAL CONCEPTS Rare neoplasms arising from the neuroendocrine cells of the GI tract Include:
Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes
 Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes Evan A. Alston, MD 1 ; Sejong Bae, PhD 2 ; and Isam A. Eltoum, MD, MBA 1 BACKGROUND:
Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes Evan A. Alston, MD 1 ; Sejong Bae, PhD 2 ; and Isam A. Eltoum, MD, MBA 1 BACKGROUND:
