The most common presentation of autoimmune pancreatitis. A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer
|
|
|
- Jasmine Jennings
- 5 years ago
- Views:
Transcription
1 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7: A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS C. SMYRK, JONATHAN E. CLAIN,* RANDALL K. PEARSON,* BRET T. PETERSEN,* MARK A. TOPAZIAN,* and SANTHI S. VEGE* *Miles and Shirley Fiterman Center for Digestive Diseases, Department of Diagnostic Radiology, and Department of Anatomic Pathology, Mayo Clinic College of Medicine, Rochester, Minnesota See Editorial on page 1026; see related article, Sandanayake NS et al, on page 1089 in this issue of CGH. BACKGROUND & AIMS: Autoimmune pancreatitis (AIP) and pancreatic cancer (PaC) have similar presentations; a diagnostic strategy is needed to distinguish the 2 diseases. METHODS: We compared computed tomography images (for pancreas and other organ involvement), serum IgG4 levels, histology data, and the response to steroids between patients with AIP (n 48) and those with PaC (n 100). RESULTS: Pancreatic imaging findings stratified patients into 3 groups. Group 1 was highly suggestive of AIP, with diffuse pancreatic enlargement without group 3 features (n 25, 100% AIP). Group 2 was indeterminate, with normal-sized pancreas or focal pancreatic enlargement without group 3 features (n 20, 75% AIP). Group 3 was highly suggestive of PaC, with presence of 1 low-density mass, pancreatic duct cutoff, or upstream pancreatic atrophy (n 103, 92% PaC). Although all patients in group 1 had AIP, only 20 of the 25 patients had increased serum IgG4 levels and/or other organ involvement. Of the patients in groups 2 and 3 who did not have cancer, all those with serum IgG4 levels 2-fold the upper limit of normal or a combination of increased serum IgG4 levels and other organ involvement (n 15) had AIP. In AIP subjects without supportive serologic evidence or other organ involvement (n 14), diagnosis required pancreatic core biopsy (n 7), steroid trial (n 5), or resection (n 2). CONCLUSIONS: PaC can be distinguished from AIP by pancreatic imaging, measurement of serum IgG4 levels, and determination of other organ involvement. However, a pancreatic core biopsy, steroid trial, or surgery is required for diagnosis in approximately 30% of patients with AIP. View this article s video abstract at The most common presentation of autoimmune pancreatitis (AIP) reported worldwide is with obstructive jaundice and pancreatic enlargement that mimics the presentation of pancreatic cancer (PaC). 1 4 AIP is rare compared with PaC; less than 5% of patients undergoing resection for suspicion of PaC have AIP. 5 Because of lack of a simple diagnostic test for AIP, its recognition poses a significant clinical challenge. Recent studies have, therefore, studied the usefulness of a variety of techniques including pancreatic histology, 6 imaging (computed tomography [CT] 7 or positron emission tomography 8 ), serology (serum IgG4, 9 11 serum carbonic anhydrase II), other organ involvement (eg, ampullary biopsy), 12,13 or response to steroids 14 to diagnose AIP and distinguish it from PaC. A strategy to distinguish AIP from PaC by using a combination of clinical, serologic, and radiologic findings has recently been proposed by Kamisawa et al. 15 In this study we compared the clinical presenting symptoms of AIP and PaC to identify diagnostic clues that distinguish the 2 diseases. The presenting symptoms of AIP and PaC often lead to performance of an abdominal CT scan. We compared CT imaging features of the 2 diseases to identify features that are highly suggestive of AIP, features that have high predictive value for PaC, and those that are indeterminate. Elevated serum IgG4 level is a useful marker of AIP, 9,10 and elevated Ca 19-9 is the best known serum marker for PaC. However, in 2 recent Western studies, 10,16 7% 10% of PaC patients had elevated IgG4 levels. In the present study we compared the sensitivity and specificity of serum IgG4 and Ca 19-9 as markers for AIP and PaC, respectively. Pancreatic fine-needle aspiration cytology is usually obtained to diagnose PaC. AIP cannot be definitively diagnosed on fineneedle aspiration; to make a tissue diagnosis of AIP, a pancreatic core biopsy is required to look for unique histologic and immunohistologic characteristics. 1 However, core biopsy of the pancreas is often not feasible as a result of lack of expertise or of location of mass/enlargement in the pancreas or is inconclusive when obtained. In such patients, one is faced with the choice of pancreatic resection versus a short course of steroids to diagnose AIP. 14 The use of a therapeutic trial of steroids to diagnose AIP has justifiably raised concerns regarding its overuse in patients with likely PaC and consequent delay in pancreatic surgery for cancer patients wrongly treated with steroids. 17,18 The goals of our study were to develop a strategy that can help physicians identify AIP among subjects presenting with obstructive jaundice and/or a pancreatic mass/enlargement. We also define the indications for pancreatic core biopsy and for steroid trial to diagnose AIP. On the basis of the results of our comparative study of the features of AIP and PaC, we have revised our previously published HISORt criteria. 1 Abbreviations used in this paper: AIP, autoimmune pancreatitis; CT, computed tomography; PaC, pancreatic cancer by the AGA Institute /09/$36.00 doi: /j.cgh
2 1098 CHARI ET AL CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 7, No. 10 Methods The study was approved by Mayo Foundation Institutional Review Board. Pancreatic Cancer Case Ascertainment PaC cases were identified from a prospective database maintained by Mayo Clinic s Pancreas Cancer SPORE. One hundred PaC patients who had contrast-enhanced abdominal CT scans available for review, the majority of whom also had serum IgG4 and CA 19-9 measurement, were the subject of a detailed comparative study of PaC and AIP described below. All but 4 of the cases had histologic confirmation of the diagnosis of ductal adenocarcinoma of the pancreas. Autoimmune Pancreatitis Case Ascertainment One of the authors (S.T.C.) has maintained a database of all patients seen at Mayo Clinic Rochester who meet HISORt criteria for AIP (n 98). From this database, we included in this study all cases whose contrast-enhanced abdominal CT scan done at onset of illness was available for review (n 48). Comparative Study of Pancreatic Cancer and Autoimmune Pancreatitis: Clinical Symptoms The medical records of PaC (n 100) and AIP (n 48) patients were reviewed to abstract data on presence of the following features at initial presentation: obstructive jaundice, any abdominal pain, severe abdominal pain requiring therapy, back pain, anorexia, amount of weight loss, and new-onset diabetes. Pancreatic Imaging A single radiologist (N.T.), blinded to clinical diagnosis, reviewed CT scans of the 148 PaC and AIP patients and recorded the presence or absence of the following pancreatic abnormalities: presence of a low-density mass with or without pancreatic ductal dilatation, pancreatic duct cutoff, or upstream pancreatic parenchymal atrophy; diffuse enlargement of the gland without ductal dilatation ( 4 mm in diameter) or cutoff; focal enlargement of the gland without ductal dilatation or cutoff; diffuse pancreatic atrophy or calcification. Reflecting our clinical practice in which we do not routinely perform pancreatograms in the setting of obstructive jaundice, there were not enough patients in the cohort who had endoscopic retrograde cholangiopancreatogram or magnetic resonance cholangiopancreatogram to include these imaging modalities in the study. Serology The sensitivity and specificity of serum IgG4 and Ca 19-9 for diagnosis of AIP and PaC, respectively, were calculated by using data from all patients who had the values measured. Extrapancreatic Findings Extrapancreatic findings on CT scan suggestive of cancer including low-density liver lesions suspicious for metastases were noted. Scans were also carefully reviewed to identify typical other organ involvement seen in AIP, viz, kidney lesions suspicious for AIP-associated tubulointerstitial nephritis, 19 retroperitoneal fibrosis, and proximal bile duct enhancement on contrast CT. In addition, evidence of proximal extrahepatic bile duct strictures and intrahepatic bile duct strictures seen on cholangiograms (endoscopic, magnetic resonance, or percutaneous) was noted. Presence or history of salivary gland swelling or history of diagnosis of Sjogren s syndrome or ulcerative colitis was also noted. Histology The histology of the pancreas and extrapancreatic tissue biopsied (fine-needle aspiration or core biopsy) or resected was reviewed and categorized as (1) diagnostic of cancer, (2) diagnostic of AIP, and (3) inconclusive. Histology of AIP was further classified as lymphoplasmacytic sclerosing pancreatitis or idiopathic duct centric pancreatitis Response to Steroids In patients who received steroid therapy, the response to it was noted as reported earlier. 1 The most common regimen involved an induction dose of 40 mg for 4 weeks followed by a taper (5 mg/week) during a period of 8 weeks. Response to steroid therapy was defined as resolution/ marked improvement of pancreatic/extrapancreatic manifestation with steroid therapy. 1 Resolution was achieved when follow-up imaging showed normal biliary tree and pancreatic duct, and post-therapy cross-sectional imaging showed normal-appearing pancreas or pancreatic atrophy. Marked improvement was defined as measurable reduction in size but not resolution of pancreatic mass or improvement in biliary and pancreatic ductal irregularity, often permitting removal of biliary stents. Development of Strategy to Identify Autoimmune Pancreatitis in Subjects With Clinical Suspicion of Pancreatic Cancer Diagnostic characteristics (sensitivity and specificity) of individual features noted above were calculated. Positive and negative predictive values were not calculated because the prevalence of AIP in this cohort was much higher (32%) compared with the expected prevalence of 3% 5%. Instead, combinations of features with high specificity for AIP or PaC were identified. The strategy was based on the tools that we normally use to differentiate AIP from PaC, viz, abdominal CT scan, serology (Ca 19-9, IgG4), pancreatic fine-needle aspiration biopsy, and, if necessary and possible, pancreatic core biopsy. On the basis of these data and our own overall clinical experience and practice, we then defined revised HISORt criteria and a strategy that accurately distinguished AIP from PaC. We then determined what proportion of patients could not be diagnosed simply on the basis of review of clinical, radiologic, and serologic evidence. On the basis of this, we propose indications for core biopsy of the pancreas and steroid therapy. Validation of Results An independent patient cohort was assembled to validate the results, of whom 31 had biopsy-confirmed PaC, 3 had AIP, 6 had no pancreatic pathology, and 10 had a variety of low-density pancreatic masses and/or obstructive jaundice (5 had islet cell tumors, 2 each had serous cystadenoma and intraductal papillary mucinous neoplasm, and 1 had cholangiocarcinoma). The proportion of AIP in this validation set was deliberately kept low (6%), approximately that seen in subjects having surgery for suspicion of PaC, to determine whether the strategy can identify a disease that is normally of very low prevalence.
3 October 2009 DIAGNOSTIC STRATEGY TO DISTINGUISH AIP FROM PANCREATIC CANCER 1099 Results Comparison of Demographics and Clinical Presentation AIP patients were younger (mean age, vs years, P.006) and more likely to be male (85% vs 57%, P.001) compared with PaC patients. AIP patients presented with obstructive jaundice more often than PaC patients (87.5% vs 49%, P.001). However, a similar proportion of AIP and PaC patients had abdominal pain (58% vs 50%), severe abdominal pain (15% vs 10%), back pain (10% vs 6.4%), weight loss of 10 pounds (51% vs 42%), and anorexia (30% vs 21%). Pancreatic Findings on Computed Tomography Scan A number of pancreatic findings on CT distinguished PaC from AIP (Table 1). On the basis of these features, 3 groups could be identified: Imaging group 1: highly suggestive of AIP (n 25): diffuse pancreatic enlargement without features of group 3 (Figure 1A: sensitivity for AIP 52%, specificity for AIP 100%); Imaging group 2: suggestive of AIP (n 20): focal pancreatic enlargement without features of group 3 or normalsized pancreas (Figure 1B: seen in 3% of PaC and 31% of AIP); Imaging group 3: highly suggestive of PaC (n 103): presence of 1 low-density mass, pancreatic duct cutoff, or distal atrophy (Figure 1C: sensitivity for PaC 95%, specificity for PaC 83%). Serology The data on serum IgG4 and Ca 19-9 levels in the subset of 100 PaC patients and 48 AIP patients in the CT study are provided in Table 1. Extrapancreatic Findings on Computed Tomography Scan: Extrapancreatic Findings CT scans showed liver lesions suspicious for metastases in 18% of cancer but not in AIP; other organ involvement Figure 1. Illustrative examples of imaging subgroups. (A) Group 1: diffusely enlarged pancreas without ductal dilatation (solid arrows) and with capsule-like rim (dashed arrows); (B) group 2: focally enlarged pancreas (arrow) without ductal dilatation or pancreatic atrophy (not shown); (C) group 3: low-density mass (solid black arrow) with ductal dilation (dashed arrow) and parenchymal atrophy (solid white arrow). suggestive of AIP was seen in 58% of AIP and 2% of PaC (Table 1). Renal lesions suggestive of AIP as described by Takahashi et al 19 were seen more often in AIP than cancer (23% vs 2%, P.001), and retroperitoneal fibrosis was seen only in association with AIP (12.5%). Bile duct enhancement was seen in both AIP and PaC. However, in PaC this was associated with the presence of a previously placed biliary stent. Cholangiograms revealed proximal extrahepatic and intrahepatic strictures in AIP (31%) but not in PaC. Ulcerative colitis was associated with AIP (6.25%) but not PaC. Table 1. Comparison of PaC and AIP Sensitivity Specificity PaC (n 100) AIP (n 48) P value For PaC For AIP CT findings (a) Low-density mass 89 (89) 7 (14.6) (b) Pancreatic duct cutoff 67 (67) 4 (8.3) (c) Distal pancreatic atrophy 53 (53) 3 (6.3) (d) Presence of a or b or c 92 (92) 8 (16.7) (d) Focal enlargement without a, b, or c Or normal-sized pancreas 5 (5) 15 (31.3) (e) Suggestive of liver metastases 18 (18) 0 (0) (g) Diffuse pancreatic enlargement without a, b, or c 0 (0) 25 (52.1) (h) Capsule-like rim around pancreas 0 (0) 18 (37.5) Other organ involvement a 2 (2) 28 (58.3) Serology Serum IgG4 140 mg/dl 10 (10) 39 (81.3) Serum IgG4 280 mg/dl ( 2 ULN) 0 (0) 24 (50) Ca U/L 70/91 (76.9) 9/39 (23.1) Ca U/L 56/91 (61.5) 3/39 (7.7) a Evidence of retroperitoneal fibrosis, renal involvement, proximal/intrahepatic bile duct stricture, on imaging studies or salivary gland enlargement on physical examination.
4 1100 CHARI ET AL CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 7, No. 10 Table 2. Revised HISORt Criteria: Definitions Category 1: Highly suggestive/diagnostic of AIP 2: Indeterminate/supportive of AIP 3: Highly suggestive/diagnostic of PaC H, Histology (pancreatic Any one of these: core biopsy or 1 (A) Lymphoplasmacytic sclerosing resection specimen) pancreatitis or (B) Abundant ( 10 cells/hpf) IgG4-positive cells with 2 of the following: Periductal lymphoplasmacytic infiltrate Obliterative phlebitis Storiform fibrosis 2 (A) Idiopathic duct centric pancreatitis or (B) Granulocyte epithelial lesion in pancreatic duct with minimal IgG4- positive cells in pancreatic parenchyma I, Imaging of pancreas Diffusely enlarged gland with featureless borders and delayed enhancement with or without capsule-like rim (Figure 1A) No features highly suggestive of cancer (I3, S3, or O3) Storiform fibrosis with lymphoplasmacytic infiltrate Focally enlarged gland without features highly suggestive of cancer (I3 or O3) (Figure 1B) S, Serology Serum IgG4 twice the upper limit of normal Elevated serum IgG4 ( twice the upper limit of normal) O, Other organ Radiologic evidence of involvement Rt, Response to steroid treatment Typical histology (eg, bile duct resection specimen, salivary gland) or Typical radiologic features positive IgG4 immunostaining in affected organ Resolution/marked improvement in pancreatic/extrapancreatic manifestation Hilar/Intrahepatic biliary strictures Renal involvement Retroperitoneal fibrosis Parotid/lacrimal gland enlargement Positive IgG4 immunostaining in organs not noted above (eg, gallbladder, ampulla) Inflammatory bowel disease a Positive for cancer on cytology/ resection specimen of pancreas or other organ Any of these (Figure 1C): Low-density mass Pancreatic ductal dilatation Pancreatic duct cutoff Upstream parenchymal atrophy Elevated Ca IU/mL after biliary decompression Liver lesions suggestive of or biopsy-proven metastases No response or increase in size of pancreatic mass No improvement in biliary stricture Rising CA 19-9 a Seen especially in association with idiopathic duct centric pancreatitis (up to 30%); only 6% of lymphoplasmacytic sclerosing pancreatitis have inflammatory bowel disease in which it is generally not included as other organ involvement. Histology In 96 of 100 PaC patients, there was histologic confirmation of adenocarcinoma; 4 declined biopsy or had severe comorbidities. Of those who had histologic confirmation, 30 had undergone pancreatic resection, and the rest (n 66) had biopsy of a primary tumor that was locally unresectable (n 45) or of metastatic lesions in the liver (n 15), lymph nodes (n 4), or mesentery (n 2). Of the 48 patients with AIP, histologic confirmation of diagnosis was obtained in 28 (58%), including 8 after pancreatic resection (3 before coming to Mayo) and 20 by pancreatic core biopsy and immunostaining; all had lymphoplasmacytic sclerosing pancreatitis. Response to Steroids Thirty-six of 48 AIP patients received steroids, and all responded. None of the 100 PaC patients in the study received steroids. Development of Revised HISORt Criteria On the basis of the comparative study of the features of PaC and AIP and a review of our entire experience with the 2 diseases, we propose revised HISORt criteria (Table 2) and the diagnosis of AIP on the basis of the revised criteria (Table 3). The revised criteria emphasize not only features highly suggestive or supportive of diagnosis of AIP but also highlight features highly suggestive of PaC. Development of Strategy for Work-Up of Patients Presenting With Pancreatic Mass/ Enlargement With or Without Obstructive Jaundice Clinical symptoms were not helpful in distinguishing PaC from AIP. Because a CT scan is often the first important clue to the diagnosis of both PaC and AIP, we stratified patients into 3 groups on the basis of CT features (Table 2); the proportion of patients with AIP progressively decreased from Imaging groups 1 through
5 October 2009 DIAGNOSTIC STRATEGY TO DISTINGUISH AIP FROM PANCREATIC CANCER 1101 Table 3. Diagnosis of AIP Based on Revised HISORt Criteria On the basis of revised HISORt criteria (Table 2), AIP can be diagnosed by one of the following: A. Diagnostic histology: (H1) (1) On resection specimen Or (2) On pancreatic core biopsy (indicated when a patient with pancreatic mass and/or obstructive jaundice due to distal bile duct obstruction has a negative work-up for cancer and lacks the necessary collateral evidence of AIP on serology or other organ involvement (see Figure 2) B. Typical imaging (I1) any one of the following: Elevated IgG4 (S1/S2) Other organ involvement (O1/O2) Compatible histology (H2) C. Response to steroids (Rt1): Resolution/marked improvement in pancreatic/extrapancreatic manifestations in patients meeting criteria for steroid use: (1) Patients in groups A and B (2) Patients without typical imaging findings (I2/3) with negative work-up for cancer and who have 1 highly suggestive feature of AIP (serum IgG4 2 times upper limit of normal [S1] or definitive other organ involvement [O1] or 2 supportive features of AIP [ 2-fold elevation of serum IgG4 (S2), clinical/radiologic evidence of other organ involvement [O2], compatible histology [H2]) (3) A steroid trial in the absence of adequate or no collateral evidence of AIP must be used with caution 3 (25/25, 100%; 15/20, 75%; 8/103, 8%, respectively) (Table 4). Patients with radiologic findings highly suggestive of AIP (Imaging group 1) require less collateral evidence for diagnosis of AIP (any elevation in serum IgG4 level and/or suggestive or diagnostic other organ involvement) than patients with indeterminate radiologic findings or those with features highly suggestive of PaC (Imaging groups 2 and 3) (1 highly suggestive feature [eg, serum IgG4 2 upper limit of normal] or 2 suggestive features [eg, any elevation in serum IgG4 level and radiologic evidence of retroperitoneal fibrosis]). The difference between Imaging groups 2 and 3 is that in group 3, AIP should only be suspected if there is collateral evidence for the disease; those without such evidence should be managed as PaC. However, because of the relative rarity of AIP, all patients in Imaging groups 2 and 3 should undergo work-up of cancer before work-up for AIP. Overall in our study, 13 of 48 (27%) patients did not have appropriate serologic or other organ involvement evidence of AIP in the 3 radiologic groups. Such patients needed core biopsy, resection, or steroid trial to diagnose AIP. Validation Set In this set the proportion of AIP was more realistic, with only 3 of 50 patients having AIP. The majority of patients fit into Imaging group 3 (n 40), of whom none had AIP; 8 were in Imaging group 2, of whom 1 had AIP requiring core biopsy of pancreas to diagnose AIP. Only 2 patients were in Imaging group 1; both had collateral serologic evidence (one also had other organ involvement) of AIP, and both had AIP. Discussion In this comparative study of a large number of AIP and PaC patients, we found that CT features can stratify patients into groups that are highly likely to have AIP, those highly likely to have PaC, and those in whom the diagnosis is uncertain. Collateral evidence of AIP in the form of serum IgG4 elevation and other organ involvement can then help diagnose AIP in 70% of patients. However, 30% of AIP patients will require pancreatic core biopsy, steroid trial, or surgery to make the diagnosis. On the basis of this comparative study and a review of literature, we revised the HISORt criteria to include features highly suggestive of both AIP and PaC (Table 2) to avoid investigation of patients with a high likelihood of having PaC. To help physicians distinguish PaC from AIP, we propose a strategy for work-up of patients presenting with pancreatic mass and/or obstructive jaundice. A CT scan is often the first clue to the diagnosis of PaC or AIP in this setting. Therefore, we used CT as the first step in risk-stratifying patients presenting with obstructive jaundice with or without pancreatic mass. Three imaging groups could be identified, examples of which are illustrated in Figure 1: group 1, highly suggestive of AIP; group 2, which is indeterminate, and group 3, highly suggestive of PaC. It must be pointed out here that this exercise requires a radiologist thoroughly familiar with the 2 diseases. A common error in CT interpretation that we have encountered in practice is mistaking a normally enhancing generous pancreas of a young patient as a sausage-shaped diffuse enlargement of AIP. Patients with PaC are highly likely to have certain CT features (presence of 1 low-density mass, pancreatic duct cutoff, or distal atrophy); in our study, 95% of PaC patients had this finding (Imaging group 3). Two recent studies also reported that parenchymal atrophy and pancreatic ductal dilatation (noted on endoscopic retrograde cholangiopancreatography in one study) distinguished AIP from PaC. 15,24 Other features favoring cancer include a serum Ca 19-9 level of 150 U/mL, which was seen only in 7.7% of AIP. However, Ca 19-9 levels can be markedly elevated in AIP with untreated biliary obstruction. The presence of imaging features of metastases should also strongly suggest cancer. However, vascular involvement is seen in both AIP and PaC and is not a distinguishing feature. 7,15 Mild elevations of serum IgG4 level ( 2-fold upper limit of normal) are more likely to be false-positive than true AIP in this setting. 10 We recommend that patients with high-risk features Table 4. Proportion of PaC and AIP With Elevated Serum IgG4 and Other Organ Involvement in Imaging Subgroups 1 Through 3 Group 1 Group 2 Group 3 Criteria PaC 0 AIP 25 PaC 5 AIP 15 PaC 95 AIP 8 Serum IgG4 elevation 140 mg/dl 0 20 (80) 0 13 (87) 10 (10.5) 6 (75) Serum IgG4 280 mg/dl 0 15 (75) 0 7 (47) 0 3 (37.5) Other organ involvement suggestive/diagnostic of AIP 0 15 (75) 0 8 (53) 2 (2) 4 (50) Serum IgG4 2 ULN or serum IgG4 elevated OOI 0 15 (75) 0 9 (36) 0 5 (62.5) ULN, upper limit of normal; OOI, other organ involvement.
6 1102 CHARI ET AL CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 7, No. 10 Figure 2. Strategy for distinguishing AIP from PaC. for PaC should only be investigated for AIP if they have some additional highly suggestive features of AIP (for example, retroperitoneal fibrosis or intrahepatic biliary strictures). Because of the rarity of AIP in this setting, we recommend that even patients with collateral evidence of AIP undergo work-up to exclude cancer before being investigated for AIP (Figure 2). In our study, a focal enlargement of the pancreas without CT features of PaC noted above was more frequent in AIP than in PaC. However, in the validation set in which only 6% of patients studied had AIP, only 1 of 8 patients with this finding had AIP. Therefore, we recommend that work-up to exclude cancer be done before a search for AIP is made. Provided cancer work-up is negative, the presence of additional serologic and other organ involvement evidence of AIP greatly increases its likelihood. Patients with typical imaging features of AIP (diffuse enlargement without features of PaC) are highly likely to have AIP and require less collateral evidence, which might include markedly elevated titers of gamma-globulin, antinuclear antibody, and rheumatoid factor. In fact, in the 131 PaC patients studied in the test and validation sets, none had a diffuse enlargement without other features of PaC. We did not include typical acute pancreatitis patients in the study because acute pancreatitis without biliary obstruction is not a common presentation of AIP. In our experience with patients with AIP, presentation with pancreatitis (severe abdominal pain and markedly elevated pancreatic enzymes) is very often associated with concomitant obstructive jaundice or abnormal liver tests as a result of biliary stricture. The findings of the comparative study and the ability of the proposed strategy to distinguish AIP from PaC were confirmed in an independent cohort of patients (validation set). On the basis of this exercise it is clear that 30% of AIP patients cannot be diagnosed simply on the basis of CT features, serology, and other organ involvement and will require a pancreatic core biopsy, steroid trial, or surgery to confirm diagnosis. It is important to define the indications for core biopsy and steroid trial for diagnosis of AIP. Pancreatic core biopsy is indicated when a patient with pancreatic mass and/or obstructive jaundice caused by distal bile duct obstruction has a negative work-up for cancer and lacks the necessary collateral evidence of AIP on serology or other organ involvement (Figure 2). Steroids are indicated under the following circumstances: (1) patients with typical imaging findings who have appropriate collateral findings of AIP or (2) patients without typical imaging findings who have negative work-up for cancer and have appropriate collateral evidence of AIP. A steroid trial in the complete absence of collateral evidence of AIP is strongly discouraged. There is a tendency to treat with steroids with the assumption that if it works it must be AIP. This is appropriate when patients are properly selected. However, when the pretest probability of having AIP in the patient being given steroids is low (eg, in typical painful chronic pancreatitis or functional dyspepsia) and the parameter being monitored for determining response is subjective (eg, abdominal pain), the positive response is likely a placebo effect or salutary nonspecific effect of steroids.
7 October 2009 DIAGNOSTIC STRATEGY TO DISTINGUISH AIP FROM PANCREATIC CANCER 1103 One of the limitations of our study is that the cohort of AIP has been retrospectively assembled. This is by necessity because AIP is an uncommon disease. However, we have been following this strategy in our practice since its formulation and have found it to be both helpful and accurate in distinguishing AIP from PaC. Our strategy uses tools typically available in most centers, and we have deliberately excluded techniques (such as intraductal ultrasonography) available only at more advanced centers. Although we do use endoscopic ultrasonography to obtain core biopsies of pancreas, we recognize that this expertise is not widely available, and the strategy does not mandate its use. The strategy also reflects the practice at our Center. For example, it does not mandate a pancreatogram for the diagnosis of AIP, as do the Japanese (endoscopic retrograde pancreatogram) and Korean (magnetic resonance pancreatogram) criteria. 25 This reflects our clinical practice as well as that of other centers across the United States in which diagnostic endoscopic retrograde pancreatograms are not routinely performed in patients presenting with obstructive jaundice. Therefore, we did not have enough patients in our study who had endoscopic retrograde cholangiopancreatography or magnetic resonance cholangiopancreatography to validate their utility. We are currently undertaking an international multicenter study of the sensitivity and specificity of endoscopic retrograde pancreatogram findings for the diagnosis of AIP and the interobserver variability in interpretation of the pancreatograms. As other diagnostic modalities are validated, they could be included in the strategy. In summary, we have compared the features of PaC and AIP to identify characteristic features of both diseases. This has led to modification of the previously published HISORt criteria and development of a clinical strategy to differentiate AIP from PaC. The results have been validated in an independent cohort of patients. Our results show that PaC and AIP can often be distinguished by a combination of pancreatic imaging features, serum IgG4, and other organ involvement. However, 30% of AIP patients will require pancreatic core biopsy, steroid trial, or surgery to make the diagnosis. Supplementary data To access the supplementary material accompanying this article, visit the online version of Clinical Gastroenterology and Hepatology at and at doi: / j.cgh References 1. Chari ST, Smyrk TC, Levy MJ, et al. Diagnosis of autoimmune pancreatitis: the Mayo Clinic experience. Clin Gastroenterol Hepatol 2006;4: Kamisawa T, Egawa N, Nakajima H, et al. Clinical difficulties in the differentiation of autoimmune pancreatitis and pancreatic carcinoma. Am J Gastroenterol 2003;98: Church NI, Pereira SP, Deheragoda MG, et al. Autoimmune pancreatitis: clinical and radiological features and objective response to steroid therapy in a UK series. Am J Gastroenterol 2007;102: Kim KP, Kim MH, Song MH, et al. Autoimmune chronic pancreatitis. Am J Gastroenterol 2004;99: Wolfson D, Barkin JS, Chari ST, et al. Management of pancreatic masses. Pancreas 2005;31: Bang SJ, Kim MH, Kim do H, et al. Is pancreatic core biopsy sufficient to diagnose autoimmune chronic pancreatitis? Pancreas 2008;36: Takahashi N, Fletcher JG, Fidler JL, et al. Dual-phase CT of autoimmune pancreatitis: a multireader study. AJR Am J Roentgenol 2008;190: Ozaki Y, Oguchi K, Hamano H, et al. Differentiation of autoimmune pancreatitis from suspected pancreatic cancer by fluorine-18 fluorodeoxyglucose positron emission tomography. J Gastroenterol 2008;43: Hamano H, Kawa S, Horiuchi A, et al. High serum IgG4 concentrations in patients with sclerosing pancreatitis. N Engl J Med 2001;344: Ghazale A, Chari ST, Smyrk TC, et al. Value of serum IgG4 in the diagnosis of autoimmune pancreatitis and in distinguishing it from pancreatic cancer. Am J Gastroenterol 2007;102: Morselli-Labate AM, Pezzilli R. Usefulness of serum IgG4 in the diagnosis and follow up of autoimmune pancreatitis: a systematic literature review and meta-analysis. J Gastroenterol Hepatol 2009;24: Kamisawa T, Tu Y, Egawa N, et al. A new diagnostic endoscopic tool for autoimmune pancreatitis. Gastrointest Endosc 2008;68: Sepehr A, Mino-Kenudson M, Ogawa F, et al. IgG4 to IgG plasma cells ratio of ampulla can help differentiate autoimmune pancreatitis from other mass forming pancreatic lesions. Am J Surg Pathol 2008;32: Moon SH, Kim MH, Park DH, et al. Is a 2-week steroid trial after initial negative investigation for malignancy useful in differentiating autoimmune pancreatitis from pancreatic cancer? A prospective outcome study. Gut 2008;57: Kamisawa T, Imai M, Yui Chen P, et al. Strategy for differentiating autoimmune pancreatitis from pancreatic cancer. Pancreas 2008;37:e62 e Raina A, Krasinskas AM, Greer JB, et al. Serum immunoglobulin G fraction 4 levels in pancreatic cancer: elevations not associated with autoimmune pancreatitis. Arch Pathol Lab Med 2008; 132: Gardner TB, Levy MJ, Takahashi N, et al. Misdiagnosis of autoimmune pancreatitis: a caution to clinicians. Am J Gastroenterol 2009; 104: Levy P, Hammel P, Ruszniewski P. Diagnostic challenge in autoimmune pancreatitis: beware of shipwreck! Gut 2008;57: Takahashi N, Kawashima A, Fletcher JG, et al. Renal involvement in patients with autoimmune pancreatitis: CT and MR imaging findings. Radiology 2007;242: Notohara K, Burgart LJ, Yadav D, et al. Idiopathic chronic pancreatitis with periductal lymphoplasmacytic infiltration: clinicopathologic features of 35 cases. Am J Surg Pathol 2003;27: Zamboni G, Luttges J, Capelli P, et al. Histopathological features of diagnostic and clinical relevance in autoimmune pancreatitis: a study on 53 resection specimens and 9 biopsy specimens. Virchows Arch 2004;445: Park DH, Kim M-H, Chari ST. Recent advances in autoimmune pancreatitis. Gut 2009 [Epub ahead of print]. 23. Zhang L, Notohara K, Levy MJ, et al. IgG4-positive plasma cell infiltration in the diagnosis of autoimmune pancreatitis. Mod Pathol 2007;20: Chang WI, Kim BJ, Lee JK, et al. The clinical and radiological characteristics of focal mass-forming autoimmune pancreatitis: comparison with chronic pancreatitis and pancreatic cancer. Pancreas Ryu JK, Lee KT, Kim MW. Comparison of diagnostic criteria for autoimmune pancreatitis. Korean J Pancr Biliary Dis 2007;12: Reprint requests Address requests for reprints to: Suresh T. Chari, MD, 200 First Street Southwest, Rochester, Minnesota chari.suresh@ mayo.edu; fax: (507) Conflicts of interest The authors disclose no conflicts.
Autoimmune pancreatitis (AIP) can be defined as a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
Autoimmune Pancreatitis: A Great Imitator
 Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Diagnostic Algorithm for Autoimmune Pancreatitis in Korea
 Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic Pancreatitis of Other Etiology
 94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
Autoimmune pancreatitis (AIP) was described more than a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis?
 CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma
 Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Type 2 Autoimmune Pancreatitis with Crohn s Disease
 doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease
 Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Autoimmune pancreatitis
 Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Overview of Diagnostic Criteria for Autoimmune Pancreatitis
 2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
Autoimmune pancreatitis (AIP), a clinical entity originally
 Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma
 Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Review Article The Utility of Serum IgG4 Concentrations as a Biomarker
 International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy
 ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings
 Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
IgG4-related sclerosing disease
 IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
Renal manifestations of IgG4-related systemic disease
 Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4
 238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
Immunoglobulin G4-Related Disease with Several Inflammatory Foci
 CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA. Dr. Tejaswi Sindhiya Ragni
 AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction
 Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
IgG4-Related Sclerosing Cholangitis
 REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
Autoimmune Pancreatitis & Cholangiopathy. Goal and Objectives
 Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Autoimmune Pancreatitis: A Succinct Overview
 REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management
 Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
An Autopsy Case of Autoimmune Pancreatitis
 MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
Tratamiento endoscópico de la CEP. En quien como y cuando?
 Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
IgG4 Disease. General Principles of IgG4-related disease. EL Cluvar, AC Bateman
 IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
Ulcerative Colitis and Immunoglobulin G4
 Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review
 Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
IgG4-related systemic disease (ISD) is a multisystem
 Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Chronic Pancreatitis
 Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Histological diagnosis of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study with EUS-FNA
 J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
An Approach to Pancreatic Cysts. Introduction
 An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico
 Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Title: Painless jaundice as an initial presentation of lung adenocarcinoma
 Title: Painless jaundice as an initial presentation of lung adenocarcinoma Authors: Irene Andaluz García, Irene González Partida, Javier Lucas Ramos, Jorge Yebra Carmona DOI: 10.17235/reed.2018.5587/2018
Title: Painless jaundice as an initial presentation of lung adenocarcinoma Authors: Irene Andaluz García, Irene González Partida, Javier Lucas Ramos, Jorge Yebra Carmona DOI: 10.17235/reed.2018.5587/2018
An Intraductal Papillary Neoplasm of the Bile Duct at the Duodenal Papilla
 Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
Autoimmune Pancreatitis and Retroperitoneal Fibrosis
 Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Strategy to differentiate autoimmune pancreatitis from pancreas cancer
 Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
Chronic Cholestatic Liver Diseases
 Chronic Cholestatic Liver Diseases - EASL Clinical Practice Guidelines - Rome, 8 October 2010 Ulrich Beuers Department of Gastroenterology and Hepatology Tytgat Institute of Liver and Intestinal Research
Chronic Cholestatic Liver Diseases - EASL Clinical Practice Guidelines - Rome, 8 October 2010 Ulrich Beuers Department of Gastroenterology and Hepatology Tytgat Institute of Liver and Intestinal Research
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
 Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
IgG4-related Sclerosing Disease: Autoimmune Pancreatitis and Extrapancreatic
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis
 Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Calcifying Obstructive Pancreatitis: A Study of Intraductal Papillary Mucinous Neoplasm Associated With Pancreatic Calcification
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2004;2:57 63 Calcifying Obstructive Pancreatitis: A Study of Intraductal Papillary Mucinous Neoplasm Associated With Pancreatic Calcification MAURICIO ZAPIACH,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2004;2:57 63 Calcifying Obstructive Pancreatitis: A Study of Intraductal Papillary Mucinous Neoplasm Associated With Pancreatic Calcification MAURICIO ZAPIACH,*
ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE
 ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE Dr. Sohan kumar sah *, Dr. Liu Sibin, Dr. sumendra raj pandey, Dr. Prakashmaan shah, Dr. Gaurishankar pandit, Dr. Suraj kurmi and Dr. Sanjay kumar jaiswal
ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE Dr. Sohan kumar sah *, Dr. Liu Sibin, Dr. sumendra raj pandey, Dr. Prakashmaan shah, Dr. Gaurishankar pandit, Dr. Suraj kurmi and Dr. Sanjay kumar jaiswal
Intraductal papillary mucinous neoplasm (IPMN) is a distinct
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Endoscopic Ultrasound Guided Trucut Biopsy of the Cyst Wall for Diagnosing Cystic Pancreatic Tumors
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:974 979 Endoscopic Ultrasound Guided Trucut Biopsy of the Cyst Wall for Diagnosing Cystic Pancreatic Tumors MICHAEL J. LEVY,* THOMAS C. SMYRK, RAGHURAM P.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:974 979 Endoscopic Ultrasound Guided Trucut Biopsy of the Cyst Wall for Diagnosing Cystic Pancreatic Tumors MICHAEL J. LEVY,* THOMAS C. SMYRK, RAGHURAM P.
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms
 The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
'I GO FOR' (IG4) Autoimmune pancreatitis (AIP) and extrapancreatic imaging features.
 'I GO FOR' (IG4) Autoimmune pancreatitis (AIP) and extrapancreatic imaging features. Poster No.: C-2649 Congress: ECR 2013 Type: Educational Exhibit Authors: R. P. Patel, T. M. Chandler, S. Barrett, J.
'I GO FOR' (IG4) Autoimmune pancreatitis (AIP) and extrapancreatic imaging features. Poster No.: C-2649 Congress: ECR 2013 Type: Educational Exhibit Authors: R. P. Patel, T. M. Chandler, S. Barrett, J.
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts
 Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
EDUCATION PRACTICE. Primary Sclerosing Cholangitis: Patients With a Rising Alkaline Phosphatase at Annual Follow-up.
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:32 36 EDUCATION PRACTICE Primary Sclerosing Cholangitis: Patients With a Rising Alkaline Phosphatase at Annual Follow-up PHUNCHAI CHARATCHAROENWITTHAYA and
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:32 36 EDUCATION PRACTICE Primary Sclerosing Cholangitis: Patients With a Rising Alkaline Phosphatase at Annual Follow-up PHUNCHAI CHARATCHAROENWITTHAYA and
Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes
 Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes Evan A. Alston, MD 1 ; Sejong Bae, PhD 2 ; and Isam A. Eltoum, MD, MBA 1 BACKGROUND:
Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes Evan A. Alston, MD 1 ; Sejong Bae, PhD 2 ; and Isam A. Eltoum, MD, MBA 1 BACKGROUND:
MR cholangiopancreatography; Predicting imaging findings for differentiation of malignant bile ductal obstruction versus benign lesion
 Acta Med Kindai Univ Vol.43, No.1 1-8, 2018 1 MR cholangiopancreatography; Predicting imaging findings for differentiation of malignant bile ductal obstruction versus benign lesion Shojiro Hidaka 1,2,
Acta Med Kindai Univ Vol.43, No.1 1-8, 2018 1 MR cholangiopancreatography; Predicting imaging findings for differentiation of malignant bile ductal obstruction versus benign lesion Shojiro Hidaka 1,2,
Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers
 Case Reports in Medicine Volume 2015, Article ID 832463, 4 pages http://dx.doi.org/10.1155/2015/832463 Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers Alessandro
Case Reports in Medicine Volume 2015, Article ID 832463, 4 pages http://dx.doi.org/10.1155/2015/832463 Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers Alessandro
Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT
 O r i g i n a l a r t i c l e Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT O.L.M. Meijer 1, R.K. Weersma 1, E.J. van der Jagt 2, H.M. van Dullemen 1 * Departments of
O r i g i n a l a r t i c l e Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT O.L.M. Meijer 1, R.K. Weersma 1, E.J. van der Jagt 2, H.M. van Dullemen 1 * Departments of
Personal Profile. Name: 劉 XX Gender: Female Age: 53-y/o Past history. Hepatitis B carrier
 Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
University of Texas-MD Anderson Cancer Center, Houston, Texas, USA. University of Medicine and Pharmacy Craiova, Romania
 Case Report A Diagnostic Challenge: Pancreatic Cancer or Autoimmune Pancreatitis? IRINA MIHAELA CAZACU 1,2, ADRIANA ALEXANDRA LUZURIAGA CHAVEZ 1, ADRIAN SAFTOIU 2, TONYA G. WHITLOW 1, PRIYA BHOSALE 3,
Case Report A Diagnostic Challenge: Pancreatic Cancer or Autoimmune Pancreatitis? IRINA MIHAELA CAZACU 1,2, ADRIANA ALEXANDRA LUZURIAGA CHAVEZ 1, ADRIAN SAFTOIU 2, TONYA G. WHITLOW 1, PRIYA BHOSALE 3,
X-ray Corner. Imaging of The Pancreas. Pantongrag-Brown L
 X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
CHRONIC PANCREATITIS OR DUCTAL ADENOCARCINOMA? N. Volkan Adsay, \ MD
 CHRONIC PANCREATITIS OR DUCTAL ADENOCARCINOMA? N. Volkan Adsay, \ MD Case for discussion 67 y/o male Back pain and weight loss CT: 4.5 cm ill-defined, solid lesion in the head FNA/Core bx: Inconclusive
CHRONIC PANCREATITIS OR DUCTAL ADENOCARCINOMA? N. Volkan Adsay, \ MD Case for discussion 67 y/o male Back pain and weight loss CT: 4.5 cm ill-defined, solid lesion in the head FNA/Core bx: Inconclusive
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Case Reports. Intraductal Papillary Cholangiocarcinoma: Case Report and Review of the Literature INTRODUCTION CASE REPORT
 Case Reports Kongkam K, Rerknimitr R 45 Case Report and Review of the Literature Pradermchai Kongkam, M.D. Rungsun Rerknimitr, M.D. ABSTRACT A case of papillary cholangiocarcinoma is presented. A 64-year-old
Case Reports Kongkam K, Rerknimitr R 45 Case Report and Review of the Literature Pradermchai Kongkam, M.D. Rungsun Rerknimitr, M.D. ABSTRACT A case of papillary cholangiocarcinoma is presented. A 64-year-old
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
PAPER. Experience With 208 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas
 PAPER Experience With 0 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas Thomas Schnelldorfer, MD; Michael G. Sarr, MD; David M. Nagorney, MD; Lizhi Zhang, MD; Thomas C. Smyrk, MD;
PAPER Experience With 0 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas Thomas Schnelldorfer, MD; Michael G. Sarr, MD; David M. Nagorney, MD; Lizhi Zhang, MD; Thomas C. Smyrk, MD;
Cerebral involvement in IgG4-related disease
 ORIGINAL RESEARCH Clinical Medicine 2015 Vol 15, No 2: 130 4 Cerebral involvement in IgG4-related disease Authors: Deepak Joshi, A Rolf Jager, B Steven Hurel, C Stephen P Pereira, D Gavin J Johnson, E
ORIGINAL RESEARCH Clinical Medicine 2015 Vol 15, No 2: 130 4 Cerebral involvement in IgG4-related disease Authors: Deepak Joshi, A Rolf Jager, B Steven Hurel, C Stephen P Pereira, D Gavin J Johnson, E
Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones
 MULTIMEDIA ARTICLE - Clinical Imaging Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones Stefania De Lisi 1, Elisabetta Buscarini
MULTIMEDIA ARTICLE - Clinical Imaging Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones Stefania De Lisi 1, Elisabetta Buscarini
IgG4 cholangitis Case Report: Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam.
 IgG4 cholangitis New Perspectives on Biliary Tract Disease Case Report: male, 64 yrs, truck driver and car industry worker Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam
IgG4 cholangitis New Perspectives on Biliary Tract Disease Case Report: male, 64 yrs, truck driver and car industry worker Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
ENDOSCOPY IN COMPETITION DIAGNOSTICS. Dr. med. Dirk Hartmann Klinikum Ludwigshafen
 Falk Symposium 166 GI Endoscopy Standards and Innovations Mainz, 18. 19. September 2008 ENDOSCOPY IN COMPETITION DIAGNOSTICS Dr. med. Dirk Hartmann Klinikum Ludwigshafen ENDOSCOPY IN COMPETITION Competing
Falk Symposium 166 GI Endoscopy Standards and Innovations Mainz, 18. 19. September 2008 ENDOSCOPY IN COMPETITION DIAGNOSTICS Dr. med. Dirk Hartmann Klinikum Ludwigshafen ENDOSCOPY IN COMPETITION Competing
A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis
 CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
How 5 Diseases Became One. Moez Tajdin R3 McGill University
 How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
X-Ray Corner. Imaging Approach to Cystic Liver Lesions. Pantongrag-Brown L. Solitary cystic liver lesions. Hepatic simple cyst (Figure 1)
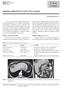 THAI J 136 Imaging Approach to Cystic Liver Lesions GASTROENTEROL 2013 X-Ray Corner Imaging Approach to Cystic Liver Lesions Pantongrag-Brown L Cystic liver lesions are common findings in daily practice
THAI J 136 Imaging Approach to Cystic Liver Lesions GASTROENTEROL 2013 X-Ray Corner Imaging Approach to Cystic Liver Lesions Pantongrag-Brown L Cystic liver lesions are common findings in daily practice
Mural nodules are predictors of malignancy in mucusproducing. Histologic and Imaging Features of Mural Nodules in Mucinous Pancreatic Cysts.
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:192 198 Histologic and Imaging Features of Mural Nodules in Mucinous Pancreatic Cysts NING ZHONG,*, LIZHI ZHANG, NAOKI TAKAHASHI, VLADISLAV SHALMIYEV,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:192 198 Histologic and Imaging Features of Mural Nodules in Mucinous Pancreatic Cysts NING ZHONG,*, LIZHI ZHANG, NAOKI TAKAHASHI, VLADISLAV SHALMIYEV,*
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas
 CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
Evidence based imaging of the pancreas
 Evidence based imaging of the pancreas D.Vanbeckevoort, D.Bielen, K.Op de beeck, R.Vanslembrouck Department of Radiology Chairman Prof. Dr. R.Oyen Non-invasive imaging tests available for the diagnosis
Evidence based imaging of the pancreas D.Vanbeckevoort, D.Bielen, K.Op de beeck, R.Vanslembrouck Department of Radiology Chairman Prof. Dr. R.Oyen Non-invasive imaging tests available for the diagnosis
Abstract. Introduction. Salah Abobaker Ali
 Sensitivity and specificity of combined fine needle aspiration cytology and cell block biopsy versus needle core biopsy in the diagnosis of sonographically detected abdominal masses Salah Abobaker Ali
Sensitivity and specificity of combined fine needle aspiration cytology and cell block biopsy versus needle core biopsy in the diagnosis of sonographically detected abdominal masses Salah Abobaker Ali
Objectives. Intraoperative Consultation of the Whipple Resection Specimen. Pancreas Anatomy. Pancreatic ductal carcinoma 11/10/2014
 Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Pancreatic Cancer Masquerading as Pancreatitis
 Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
ACG Clinical Guideline: Primary Sclerosing Cholangitis
 ACG Clinical Guideline: Primary Sclerosing Cholangitis Keith D. Lindor, MD, FACG 1, Kris V. Kowdley, MD, FACG 2, and M. Edwyn Harrison, MD 3 1 College of Health Solutions, Arizona State University, Phoenix,
ACG Clinical Guideline: Primary Sclerosing Cholangitis Keith D. Lindor, MD, FACG 1, Kris V. Kowdley, MD, FACG 2, and M. Edwyn Harrison, MD 3 1 College of Health Solutions, Arizona State University, Phoenix,
