Autoimmune pancreatitis (AIP) was described more than a
|
|
|
- Jasmine Horton
- 5 years ago
- Views:
Transcription
1 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5: The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,* NICHOLAS I. CHURCH, MANUEL RODRIGUEZ JUSTO,* PHILIPPA MUNSON, NEOMAL SANDANAYAKE, EDWARD W. SEWARD, KEITH MILLER, MARCO NOVELLI,* ADRIAN R. W. HATFIELD, STEPHEN P. PEREIRA,, and GEORGE J. M. WEBSTER, *Department of Histopathology, and Department of Gastroenterology, University College Hospital, London, United Kingdom; the The Institute of Hepatology, and UCL Advanced Diagnostics, Department of Pathology, University College Hospital, London, United Kingdom Background & Aims: Autoimmune pancreatitis (AIP) is recognized increasingly as a multisystem disorder. We evaluated the use of immunoglobulin (Ig)G4 immunostaining of pancreatic and extrapancreatic biopsy specimens to make a definitive diagnosis of AIP. Methods: Seventeen biopsy specimens and 3 gallbladder resections were assessed from 11 patients with clinical and radiologic features of AIP. Biopsy specimens from pancreas, liver, colon, stomach, duodenum, bone marrow, salivary gland, and kidney were analyzed morphologically, immunostained for IgG4- positive plasma cells, and compared with controls. Results: Positive IgG4 immunostaining enabled a definitive diagnosis in 10 of 11 (91%) AIP patients. In both pancreatic and extrapancreatic tissues, high levels of IgG4 immunostaining (>10 IgG4-positive plasma cells/highpower field) were found in 17 of 20 (85%) specimens from AIP patients compared with 1 of 175 (0.6%) specimens from controls (P <.05). Positive extrapancreatic IgG4 immunostaining was found in 8 of 11 (73%) patients, including all those with diagnostic features in the pancreas. Increased tissue IgG4 was found irrespective of serum IgG4 level. Conclusions: The finding of IgG4 immunostaining within a range of clinically involved tissues supports the hypothesis that AIP is a multisystem disease. Positive IgG4 immunostaining in extrapancreatic tissues may allow a definitive diagnosis of AIP to be made in those with evidence of pancreatic disease, without the necessity of pancreatic biopsy or surgical exploration. Immunostaining of involved tissue for IgG4 may be particularly useful when AIP is suspected clinically but the serum IgG4 level is normal. Autoimmune pancreatitis (AIP) was described more than a decade ago. 1 It often presents with a pancreatic mass and stricturing of the bile and pancreatic ducts, which may mimic pancreatobiliary cancer. Making a diagnosis is vital because steroid therapy may be effective, 2 4 allowing unnecessary surgery to be avoided. The disease largely has been described in Japan, but small patient series from Europe and the United States suggest that this rare condition occurs globally. 4 6 Diagnostic criteria for AIP have centered on clinical, radiologic, and pathologic features within the pancreas, and have relied on the demonstration of a lymphoplasmacytic pancreatic infiltrate to make a definitive diagnosis. 1,7,8 However, a percutaneous pancreatic biopsy procedure may be difficult technically, with a complication rate of up to 4.6%, 9 and so alternative diagnostic options would be preferable. In addition, the concept of AIP now is changing to one of a multisystem disorder, in which there may be clinical involvement of a range of organs. Both extrapancreatic gastrointestinal sites (eg, intrahepatic and hilar bile ducts, gallbladder, colon, duodenum, stomach, and duodenal papilla 4,5,10 12 ) and extragastrointestinal tissues (eg, retroperitoneal structures, lymph nodes, bone marrow, salivary gland, lung, kidney, mediastinum, thyroid, and prostate ) may be involved. Cases also have been reported in which pancreatic disease was not a feature at the time of diagnosis. 14 Extrapancreatic disease can be treated effectively with steroid therapy, 10 making recognition of this component an important aspect of disease management. Chari et al 5 recently proposed a new diagnostic scheme based on the use of Histology, Imaging, Serology, Other organ involvement, and Response to steroid therapy the (HISORt) criteria. In contrast to previous criteria, this classification takes greater account of extrapancreatic involvement in making a diagnosis of AIP. However, their criteria still propose that a definitive diagnosis of AIP can be made only on morphologic and immunohistochemical appearances in pancreatic tissue. Finkelberg et al 19 also proposed diagnostic criteria that include histologic evaluation of a restricted range of extrapancreatic tissues. However, there are little published data on the reliability of extrapancreatic biopsies from a wide range of clinically involved organs in making a diagnosis of AIP. 20 Furthermore, most published studies on the involvement of extrapancreatic tissues in AIP have relied on the histologic assessment of surgical resections, not core biopsy specimens. The histologic diagnosis of AIP may be difficult, in part because of the small volume of tissue often available from core biopsy specimens, and patchy disease distribution. 21 Specific features of AIP have been documented for the pancreas, but in extrapancreatic organs there is a paucity of consistently reported features for AIP, beyond a lymphoplasmacytic infiltrate, fibrosis, and obliterative phlebitis, 10 which may be seen in chronic inflammation as a result of a range of causes. This limits the use of morphology alone in making a definitive histologic diagnosis in extrapancreatic organs. Increased serum immunoglobulin (Ig)G4 levels has been reported to be more than 95% specific and sensitive for AIP. 24 However, recent data from the United States 5 and the United Abbreviations used in this paper: AIP, autoimmune pancreatitis; HPF, high-power field; Ig, immunoglobulin by the AGA Institute /07/$32.00 doi: /j.cgh
2 1230 DEHERAGODA ET AL CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 5, No. 10 Table 1. Demographic, Clinical, and Initial Histologic Findings in 11 Patients Included in the Study Patient no. Patient age and race Serum IgG4 (N 1.64 g/l) Tissue from clinically involved organs Original diagnosis on H&E sections 1 53-year-old male Caucasian Increased Liver Large duct obstruction 2 51-year-old male Afro-Caribbean Increased Pancreas Liver Kidney Chronic pancreatitis Nonspecific features a Chronic tubulointerstitial nephritis a 3 64-year-old male South Asian Increased Bone marrow Duodenum Stomach Salivary gland 4 52-year-old male South Asian Normal Pancreas Gallbladder Liver Nonspecific features a Eosinophilic duodenitis a Chronic gastritis a Chronic sialadenitis a Chronic pancreatitis Chronic cholecystitis a Large duct obstruction 5 54-year-old male Caucasian Normal Pancreas Chronic pancreatitis 6 47-year-old male Caucasian Normal Liver Large duct obstruction 7 77-year-old male Caucasian Increased Gallbladder Chronic cholecystitis a 8 28-year-old male Caucasian Normal Liver AIP-associated biliary disease 9 49-year-old male Japanese Increased Liver AIP-associated biliary disease year-old male South Asian Normal Liver Pancreas Large duct obstruction a Chronic pancreatitis a year-old male Caucasian Normal Gallbladder Colon a Indicates diagnosis before referral. Chronic cholecystitis a Nonspecific features Kingdom 6 have shown lower sensitivities of 71% and 68%, respectively, for increased serum IgG4 levels on testing at a single time point. The aim of this study was to assess the diagnostic use of IgG4 immunostaining of pancreatic and extrapancreatic tissues in AIP and assess the sensitivity of tissue IgG4 immunostaining compared with measurement of serum IgG4 in making a diagnosis of AIP. Materials and Methods Patients Eleven consecutive patients (all male) seen in our center between 2004 and 2006 in whom a diagnosis of AIP was made and in whom archival tissue and biopsy specimens obtained at admission to our unit were available for assessment, were included in the study. The diagnosis of AIP was suspected on the basis of clinical and radiologic features 4 using published diagnostic criteria for the disease. 8 Patient details, the histologic material available for analysis, and the initial histologic diagnoses at referral are shown in Table 1. Serum IgG4 levels were measured in all patients at presentation and during follow-up evaluation. Patients diagnosed with AIP were commenced on steroid therapy and their response to treatment was monitored. Materials All tissue was formalin fixed and paraffin embedded. Twenty-two tissue specimens from AIP patients were available for analysis, of which 19 were biopsy specimens (4 pancreatic, 7 liver, 1 renal, 1 colonic, 1 duodenal, 2 gastric, 2 bone marrow, and 1 salivary gland) and 3 were gallbladder resections. For controls, both normal biopsy specimens and inflamed tissue samples were selected. The latter were chosen to include diseases with a similar degree of inflammatory cell infiltration (number of specimens): pancreas: chronic calcific pancreatitis (10), normal (10), pancreatic ductal adenocarcinoma (20); liver: chronic hepatitis C (10), normal (10); gallbladder: chronic cholecystitis (10), normal (10); salivary gland: chronic sialadenitis (10), normal (8); duodenum and colon: active chronic duodenitis/colitis (10/10), normal duodenum (10), normal colon (10); bone marrow: myeloma (10), normal (10); kidney: chronic tubulointerstitial nephritis (10), normal (7). Methods All pancreatic and extrapancreatic biopsy specimens were reviewed by 2 pathologists (M.G.D. and M.R.-J.) familiar with the morphologic appearances of AIP. The original diagnosis from the corresponding pathology report was recorded. H&E-stained tissue sections from AIP patients were assessed for the presence of morphologic features reported to be specific for AIP. These included fibrosis and a lymphoplasmacytic infiltrate (with periductal involvement, preservation of ductal epithelium, and loss of exocrine tissue in the pancreas) and obliterative phlebitis with preservation of arterial anatomy Successive serial sections were immunostained with CD138, 1/100 dilution (Dako, Ely, UK) to detect plasma cells. Mouse monoclonal CD38, 1/200 dilution (Novocastra Laboratories, Newcastle, UK), was used to detect plasma cells in the liver. Plasma cells identified in this way were assessed for their expression of IgG4 by immunostaining with mouse anti-human monoclonal IgG4 antibody, 1/200 dilution (The Binding Site, Birmingham, UK). All immunostained sections had dewaxing and antigen retrieval performed on Bond MaX machines (Vision Biosystems, Newcastle, UK). Slides for CD138 were retrieved in ER1 for 20 minutes and those for CD38 and IgG4 for 30 minutes. The primary antibody was developed using Bond Polymer Refine Detection (DS9800, Vision Biosystems) and visualized with DAB (3,3 diaminobenzidine). Numbers of IgG4-positive plasma cells per high-power field (HPF) (magnification, 400 ) were counted in 10 HPFs containing the densest lymphoplasmacytic
3 October 2007 IgG4 IMMUNOSTAINING IN AIP 1231 infiltrate. Where tissue volume was small, a minimum of 5 HPFs was assessed. The mean number of IgG4-positive plasma cells in a single HPF was calculated and the result was expressed as IgG4-positive plasma cells/hpf. Specimens were considered as positive for a diagnosis of AIP if there was a lymphoplasmacytic infiltrate and there were greater than 10 IgG4-positive plasma cells/hpf. 15 The Mann Whitney U test was chosen to assess for any statistically significant differences between the mean numbers of IgG4-positive plasma cells in patient tissue vs normal and inflamed controls for pancreatic, liver, and gallbladder specimens. Results Morphologic Appearances of Biopsy Tissue on H and E Sections Two tissue samples (1 bone marrow trephine from patient 2, and a gastric biopsy specimen from patient 4) were normal morphologically and therefore were not analyzed further. In 18 of 20 specimens (9 of 11 patients) the original diagnosis made on H&E sections alone was that of an organ-specific chronic inflammatory condition, or nonspecific features (Table 1). On review of the pancreatic biopsy specimens, characteristic morphologic features of AIP were seen in 3 of 4 (75%). In addition, the investigators observed nuclear streaming artifact, which refers to the elongated and distorted nuclei of fibroblasts and inflammatory cells, in all pancreatic biopsy specimens (Figure 1A). Review of extrapancreatic tissues showed all cases to contain a lymphoplasmacytic infiltrate with a mild to moderate increase in eosinophils. With the exception of 1 gallbladder and the bone marrow sample, all extrapancreatic tissues showed variable degrees of fibrosis with nuclear streaming artifact (Figure 1E, H, and K). Beyond this, no other specific features were noted. Nuclear streaming artifact was not seen in any of our control tissues. Liver biopsy specimens from 2 patients (patients 8 and 9) showed the histologic features of large duct obstruction. However, concurrent IgG4 immunostaining in these cases (in conjunction with suggestive clinical and radiologic features) led to an initial diagnosis of AIP-related biliary disease. Immunoglobulin G4 Immunostaining Increased numbers of IgG4-positive plasma cells ( 10/ HPF) were seen in 18 of 20 tissue specimens (Figures 1 and 2). In contrast, 174 of 175 control tissues showed less than 3 IgG4-positive plasma cells/hpf (Figure 2). The Mann Whitney U test showed a statistically significant difference in the mean numbers of IgG4-positive plasma cells between patient tissues and normal and inflamed controls (pancreas: range of IgG4- positive plasma cells/hpf in patient tissue, 8 22; median, 20; P.0021; liver: range of IgG4-positive plasma cells/hpf in patient tissue, 8 28; median, 17; P.0001; gallbladder: range of IgG4-positive plasma cells/hpf in patient tissue, 28 61; median, 28; P.007). The small number of specimens available from other extrapancreatic tissues precluded statistical analysis. Nevertheless, an increased level of IgG4-positive plasma cells was seen in samples of salivary gland, stomach, duodenum, colon, kidney, and bone marrow in AIP patients, which was not found in comparative controls (Figure 2). IgG4 immunostaining of extrapancreatic tissues was positive in 8 of 11 (73%) patients. Positive IgG4 immunostaining of extrapancreatic tissue was found in all 3 patients in whom pancreatic histology was diagnostic of AIP. In 6 of 11 patients (55%), serum IgG4 was normal at presentation to our center. Nevertheless, IgG4 immunostaining was positive in 5 of 6 (83%) of these patients. False Positives One of 20 (5%) pancreatic ductal adenocarcinoma biopsy specimens used as controls showed 10 IgG4-positive plasma cells/hpf. The morphologic appearances in this biopsy specimen were unequivocally those of adenocarcinoma and no features of AIP were present. The IgG4-positive plasma cells were associated closely with adenocarcinoma cells. False Negatives Biopsy specimens from 2 AIP patients showed fewer than 10 IgG4-positive plasma cells/hpf. The pancreatic biopsy specimen from patient 5 showed extensive fibrosis and fewer than 4 plasma cells/hpf were present for assessment. Patient 4 had a liver biopsy specimen in which there was very little portal tract tissue for the assessment of plasma cells (only 4 HPFs could be assessed). Patient Response to Steroid Therapy All patients with AIP were commenced on oral steroid therapy. All had a clinical, radiologic, and biochemical response, further supporting the diagnosis of AIP, as we have reported in 9 of these patients recently. 4 Discussion AIP is now accepted to be a global disease, 6,25 and not confined to Japan, from where most reports have arisen. As more cases and small series have been published, the involvement of extrapancreatic tissues has been appreciated, and it may be that the pancreas represents just one target of a multisystem disease. 5 Although new diagnostic criteria for AIP have placed greater importance on extrapancreatic disease 5,19 than did previous criteria, 1 all require pancreatic histology to make a definitive diagnosis. An alternative to a pancreatic biopsy examination would be attractive, particularly in those with extrapancreatic involvement. A diagnosis of AIP made solely on morphologic grounds requires the presence of a constellation of histologic features, and although the lymphoplasmacytic infiltrate, fibrosis, and obliterative phlebitis that is seen in the pancreas has been reported in extrapancreatic tissue, 10,15 consistent and specific morphologic features have, to date, only been described for the pancreas. In this study IgG4 immunostaining added to the diagnostic accuracy that was possible by morphologic examination alone. The value of nuclear streaming artifact as a specific diagnostic feature for AIP awaits further evaluation on larger numbers of tissue specimens. Beyond this feature, H&E analysis of extrapancreatic tissue showed characteristic features of AIP in less than 20% of patients, but the addition of IgG4 immunostaining increased this yield to 73%. With respect to pancreatic tissue analysis, it is of note that although a histologic diagnosis of AIP could be made on pancreatic biopsy specimens in 3 of 4 patients, all 3 of these
4 1232 DEHERAGODA ET AL CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 5, No. 10 Figure 1. (A) H&E-stained section (magnification, 100 ) of pancreatic biopsy specimen from patient 10 showing fibrosis, a lymphoplasmacytic infiltrate within pancreatic lobules, with nuclear streaming artifact surrounding a venule showing obliterative phlebitis (V). There is relative preservation of arterioles (A). (B) H&E-stained section of pancreatic biopsy from patient 10 (magnification, 200 ) with a lymphoplasmacytic infiltrate surrounding pancreatic ducts (D). There is atrophy of exocrine pancreatic tissue with preservation of islets (I). (C) IgG4 immunostaining of plasma cells within the pancreatic biopsy from patient 10 (magnification, 400 ). (D) H&E-stained section (magnification, 100 ) of liver biopsy from patient 6 showing the lymphoplasmacytic infiltrate within portal tracts. (E) H&E-stained section of a portal tract from the liver biopsy on patient 6 showing the features of large duct obstruction with a mild increase in eosinophils and nuclear streaming artifact (N) (magnification, 200 ). (F) IgG4 immunostaining of plasma cells within portal tracts from the liver biopsy on patient 6 (magnification, 400 ). (G) H&E-stained section (magnification, 100 ) of salivary gland from patient 3 showing a lymphoplasmacytic infiltrate with lymphoid follicle formation. (H) H&E-stained section (magnification, 200 ) of salivary gland from patient 3 showing a lymphoplasmacytic infiltrate and nuclear streaming artifact (N) within lobules (magnification, 200 ). (I) IgG4 immunostaining of plasma cells within salivary gland from patient 3 (magnification, 400 ). (J) H&E-stained section (magnification, 100 ) of duodenum from patient 3. (K) H&E-stained section of duodenal biopsy from patient 3 (magnification, 200 ) of duodenum showing fibrosis with nuclear streaming artifact (N) and a lymphoplasmacytic infiltrate with a prominence of eosinophils (E). (L) IgG4 immunostaining of duodenal biopsy from patient 3 (magnification, 400 ). Plasma cells expressing IgG4 were identified on the basis of CD138 staining of adjacent tissue sections and characteristic plasma cell morphology (an eccentrically placed nucleus that has a clock face appearance and abundant cytoplasm). patients had positive IgG4 immunostaining of extrapancreatic tissue. This suggests that pancreatic biopsy examination may not have been necessary diagnostically. Small studies have suggested that the diagnosis of AIP may be made on biopsy specimens from the stomach26 and duodenal papilla,11 both of which are easily and safely obtained endoscopically. In the case of AIP in which IgG4 immunostaining of a pancreatic biopsy specimen was negative (patient 5), histology showed severe fibrosis, and the numbers of plasma cells were too low for assessment. It is of note that the serum IgG4 was normal in this case. The appearances in this biopsy specimen may represent a late burned-out stage of disease and therefore high numbers of IgG4-expressing cells may not be a feature. A chronologic assessment of histologic features during the natural course of AIP has not been reported. It would be interesting to see if (as is our clinical impression) the intensity of the
5 October 2007 IgG4 IMMUNOSTAINING IN AIP 1233 Figure 2. Mean numbers of IgG4-positive plasma cells in AIP patients vs normal and inflamed controls. SG, salivary gland. lymphoplasmacytic infiltrate and the IgG4 positive staining is highest during the earlier phase of the disease, and whether the longer the disease persists the more that fibrosis predominates and the infiltrate reduces. Steroid treatment might be less effective in this late stage, emphasizing the need to make an early diagnosis. Inflammatory mass lesions in AIP are known to remit/improve spontaneously over time, 2 and increased IgG4 levels may normalize in response to treatment. 24 The finding of extrapancreatic involvement in many of our patients supports the argument that clinical features previously thought to represent other diseases occurring in association with AIP (eg, sclerosing cholangitis and renal involvement) may in fact all be manifestations of the same multisystem disease. 5 Our data also support the recent publication from the Mayo Clinic and their proposal of the HISORt criteria, which places greater emphasis on extrapancreatic disease than was the case for previous criteria for AIP. Restricting the nomenclature of this condition to the pancreas may be misleading and the suggested term IgG4-related systemic disease 27 may have merit over AIP, and is supported by our data on IgG4 immunostaining of extrapancreatic tissue. The majority of our patients had normal serum IgG4 levels on initial testing. Despite this we showed IgG4 immunostaining of pancreatic and extrapancreatic tissue in 10 of 11 (91%) patients, and in 5 of 6 patients (83%) with normal serum IgG4 levels at presentation. A caveat to these data is that serum IgG4 level often was not taken at the same time point as tissue samples, with some biopsy specimens taken when AIP was not clinically considered, and serum IgG4 levels therefore were not measured. With the knowledge that serum IgG4 levels may fluctuate over time, 4,24 levels may have settled by the time of serologic testing. We found that serum IgG4 became positive in 3 of 6 patients (50%) with normal levels on initial testing, and that through repeat testing increased levels were found in 8 of 11 patients (73%). Nevertheless, our findings are in accordance with data from Chari et al, 5 who showed normal serum IgG4 levels in 29% of their patients, but positive pancreatic IgG4 immunostaining in all of these cases. The presence of positive IgG4 immunostaining in 5% of our pancreatic adenocarcinoma controls illustrates the importance of combining the clinical, radiologic, and histologic appearances when interpreting the results of IgG4 immunostaining. The occasional presence of increased IgG4 in association with pancreatic cancer has been reported previously, 19,28 and is unexplained, but the morphologic appearances of adenocarcinoma and the lymphoplasmacytic infiltrates that characterize AIP are distinctly different. These observations emphasize the necessity not to interpret the results of IgG4 immunostaining in isolation. They perhaps further support the use of extrapancreatic biopsy specimens in making a diagnosis of AIP in patients presenting with pancreatic or hilar masses in whom the clinical and radiologic differential diagnosis between AIP and carcinoma is difficult. In summary, our study adds to the emerging data on the pathologic and clinical nature of AIP, providing further evidence of the multiorgan nature of this disease in many patients. Based on our experience we would argue that a definitive diagnosis of AIP should not have to rely on pancreatic biopsy specimens but also could be made on the basis of an IgG4-positive inflammatory infiltrate within clinically involved extrapancreatic tissue, if imaging also suggests pancreatic disease. In addition, our data have shown that IgG4 immunostaining of involved tissue may be particularly useful when AIP is suspected clinically, but the serum IgG4 level is normal. References 1. Yoshida K, Toki F, Takeuchi T, et al. Chronic pancreatitis caused by an autoimmune abnormality. Proposal of the concept of autoimmune pancreatitis. Dig Dis Sci 1995;40: Wakabayashi T, Kawaura Y, Satomura Y, et al. Long term prognosis of duct narrowing chronic pancreatitis: strategy for steroid treatment. Pancreas 2005;30: Kamisawa T, Yoshiike M, Egawa N, et al. Treating patients with autoimmune pancreatitis: results from a long term follow up study. Pancreatology 2005;5:
6 1234 DEHERAGODA ET AL CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 5, No Church NI, Periera SP, Deheragoda MG, et al. Autoimmune pancreatitis: response to therapy in a UK series. Gastroenterology 2006:1300:A Chari ST, Smyrk TC, Levy MJ, et al. Diagnosis of autoimmune pancreatitis: the Mayo Clinic Experience. Clin Gastroenterol Hepatol 2006;4: Kim KP, Kim MH, Lee SS, et al. Autoimmune pancreatitis: it may be a worldwide entity. Gastroenterology 2004;126: Japan PS. Diagnostic criteria for autoimmune pancreatitis by the Japan Pancreas Society. J Jpn Pancreas Soc 2002;17: Okazaki K, Chiba T. Autoimmune related pancreatitis. Gut 2002; 51: Amin Z, Theis B, Russell R, et al. Diagnosing pancreatic cancer: the role of percutaneous biopsy and CT. Clin Radiol 2006;61: Kamisawa T, Egawa N, Nakajima H, et al. Extrapancreatic lesions in autoimmune pancreatitis. J Clin Gastroenterol 2005;39: Kamisawa T, Egawa N, Nakajima H, et al. Usefulness of biopsying the major duodenal papilla to diagnose autoimmune pancreatitis: a prospective study using IgG4-immunostaining. World J Gastroenterol 2006;12: Kamisawa T, Tu Y, Nakajima H, et al. Sclerosing cholecystitis associated with autoimmune pancreatitis. World J Gastroenterol 2006;12: Kamisawa T, Nakajima H, Egawa N, et al. IgG4-related sclerosing disease incorporating sclerosing pancreatitis, cholangitis, sialadenitis and retroperitoneal fibrosis with lymphadenopathy. Pancreatology 2006;6: Zen Y, Sawazaki A, Miyayama S, et al. A case of retroperitoneal and mediastinal fibrosis exhibiting elevated levels of IgG4 in the absence of sclerosing pancreatitis (autoimmune pancreatitis). Hum Pathol 2006;37: Kamisawa T, Funata N, Hayashi Y, et al. A new clinicopathological entity of IgG4 related autoimmune disease. J Gastroenterol 2003;38: Hirano K, Kawabe T, Komatsu Y, et al. High rate pulmonary involvement in autoimmune pancreatitis. Intern Med J 2006;36: Irie H, Honda H, Baba S, et al. Autoimmune pancreatitis: CT and MR characteristics. AJR Am J Roentgenol 1998;170: Yoshimura Y, Tadeka S, Ieki Y, et al. IgG4-associated prostatitis complicating autoimmune pancreatitis. Intern Med 2006;45: Finkelberg DL, Sahani D, Deshpande V, et al. Autoimmune pancreatitis. N Engl J Med 2006;355: Chari ST, Echelmeyer S. Can histopathology be the gold standard for diagnosing autoimmune pancreatitis? Gastroenterology 2005;129: Kloppel G, Luttges J, Lohr M, et al. Autoimmune pancreatitis: pathological, clinical and immunological features. Pancreas 2003;27: Notohara K, Burgart LJ, Yadav D, et al. Idiopathic chronic pancreatitis with periductal lymphoplasmacytic infiltration: clinicopathologic features of 35 cases. Am J Surg Pathol 2003;27: Zamboni G, Luttges J, Capelli P, et al. Histopathological features of diagnostic and clinical relevance in autoimmune pancreatitis: a study on 53 resection specimens and 9 biopsy specimens. Virchows Arch 2004;445: Hamano H, Kawa S, Horiuchi A, et al. High serum IgG4 concentrations in patients with sclerosing pancreatitis. N Engl J Med 2001;344: Varadarajulu S, Cotton PB. Autoimmune pancreatitis: is it relevant in the west? Gastroenterology 2003;125: Kamisawa T, Egawa N, Nakajima H, et al. Gastrointestinal findings in patients with autoimmune pancreatitis. Endoscopy 2005; 37: Saeki T, Saito A, Hiura T, et al. Lymphoplasmacytic infiltration of multiple organs with immunoreactivity for IgG4: IgG4 related systemic disease. Intern Med 2006;45: Pearson RK, Longnecker DS, Chari ST, et al. Controversies in clinical pancreatology: autoimmune pancreatitis: does it exist? Pancreas 2003;27:1 13. Address requests for reprints to: Dr. George Webster, Department of Gastroenterology, University College Hospital, 235 Euston Road, London NW1 2BU, United Kingdom. george.webster@uclh.nhs.uk; fax: (44) This work was undertaken at UCLH/UCL who received a portion of funding from the Department of Health s NIHR Biomedical Research Centres Funding Scheme.
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
IgG4-related sclerosing disease
 IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
Autoimmune Pancreatitis: A Great Imitator
 Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Autoimmune pancreatitis (AIP) can be defined as a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic Pancreatitis of Other Etiology
 94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
Overview of Diagnostic Criteria for Autoimmune Pancreatitis
 2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis?
 CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
The most common presentation of autoimmune pancreatitis. A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy
 ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma
 Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Diagnostic Algorithm for Autoimmune Pancreatitis in Korea
 Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
Ulcerative Colitis and Immunoglobulin G4
 Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Immunoglobulin G4-Related Disease with Several Inflammatory Foci
 CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
IgG4 Disease. General Principles of IgG4-related disease. EL Cluvar, AC Bateman
 IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
Renal manifestations of IgG4-related systemic disease
 Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Autoimmune pancreatitis
 Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4
 238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis
 CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
Cerebral involvement in IgG4-related disease
 ORIGINAL RESEARCH Clinical Medicine 2015 Vol 15, No 2: 130 4 Cerebral involvement in IgG4-related disease Authors: Deepak Joshi, A Rolf Jager, B Steven Hurel, C Stephen P Pereira, D Gavin J Johnson, E
ORIGINAL RESEARCH Clinical Medicine 2015 Vol 15, No 2: 130 4 Cerebral involvement in IgG4-related disease Authors: Deepak Joshi, A Rolf Jager, B Steven Hurel, C Stephen P Pereira, D Gavin J Johnson, E
An Autopsy Case of Autoimmune Pancreatitis
 MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
Autoimmune pancreatitis (AIP), a clinical entity originally
 Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management
 Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Review Article The Utility of Serum IgG4 Concentrations as a Biomarker
 International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
Autoimmune Pancreatitis and Retroperitoneal Fibrosis
 Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Chronic Sclerosing Dacryoadenitis
 The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
Overview of the Immunoglobulin G4-related Disease Spectrum
 Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Hideaki Miura, Yasutaka Miyachi. Department of Internal Medicine, Social Insurance Central General Hospital. Tokyo, Japan
 CASE REPORT IgG4-Related Retroperitoneal Fibrosis and Sclerosing Cholangitis Independent of Autoimmune Pancreatitis. A Recurrent Case after a 5-Year History of Spontaneous Remission Hideaki Miura, Yasutaka
CASE REPORT IgG4-Related Retroperitoneal Fibrosis and Sclerosing Cholangitis Independent of Autoimmune Pancreatitis. A Recurrent Case after a 5-Year History of Spontaneous Remission Hideaki Miura, Yasutaka
CME/SAM. Increased Immunoglobulin (Ig) G4 Positive Plasma Cell Density and IgG4/IgG Ratio Are Not Specific for IgG4- Related Disease in the Skin
 Increased Immunoglobulin (Ig) G4 Positive Plasma Cell Density and IgG4/IgG Ratio Are Not Specific for IgG4- Related Disease in the Skin Julia S. Lehman, MD, 1,2 Thomas C. Smyrk, MD, 1 and Mark R. Pittelkow,
Increased Immunoglobulin (Ig) G4 Positive Plasma Cell Density and IgG4/IgG Ratio Are Not Specific for IgG4- Related Disease in the Skin Julia S. Lehman, MD, 1,2 Thomas C. Smyrk, MD, 1 and Mark R. Pittelkow,
Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease
 Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA. Dr. Tejaswi Sindhiya Ragni
 AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
IgG4-related hypophysitis presenting as a pituitary adenoma with systemic disease
 Asian Journal of Surgery (2013) 36, 93e97 Available online at www.sciencedirect.com journal homepage: www.e-asianjournalsurgery.com CASE REPORT IgG4-related hypophysitis presenting as a pituitary adenoma
Asian Journal of Surgery (2013) 36, 93e97 Available online at www.sciencedirect.com journal homepage: www.e-asianjournalsurgery.com CASE REPORT IgG4-related hypophysitis presenting as a pituitary adenoma
Renal Pathology Case Conference. Case 2
 Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT
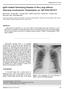 J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
Autoimmune pancreatitis (AIP) is a chronic fibroinflammatory
 Review Article Autoimmune Pancreatitis More Than Just a Pancreatic Disease? A Contemporary Review of Its Pathology Vikram Deshpande, MD; Mari Mino-Kenudson, MD; William Brugge, MD; Gregory Y. Lauwers,
Review Article Autoimmune Pancreatitis More Than Just a Pancreatic Disease? A Contemporary Review of Its Pathology Vikram Deshpande, MD; Mari Mino-Kenudson, MD; William Brugge, MD; Gregory Y. Lauwers,
IgG4-Related Sclerosing Cholangitis
 REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Autoimmune pancreatitis / IgG4-associated cholangitis and primary sclerosing cholangitis Overlapping or separate diseases? q
 Journal of Hepatology 51 (2009) 398 402 Review Autoimmune pancreatitis / IgG4-associated cholangitis and primary sclerosing cholangitis Overlapping or separate diseases? q George J.M. Webster 1,2, *, Stephen
Journal of Hepatology 51 (2009) 398 402 Review Autoimmune pancreatitis / IgG4-associated cholangitis and primary sclerosing cholangitis Overlapping or separate diseases? q George J.M. Webster 1,2, *, Stephen
IgG4 cholangitis Case Report: Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam.
 IgG4 cholangitis New Perspectives on Biliary Tract Disease Case Report: male, 64 yrs, truck driver and car industry worker Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam
IgG4 cholangitis New Perspectives on Biliary Tract Disease Case Report: male, 64 yrs, truck driver and car industry worker Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis
 Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings
 Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Where a licence is displayed above, please note the terms and conditions of the licence govern your use of this document.
 Frequency and significance of IgG4 immunohistochemical staining in liver explants from patients with primary sclerosing cholangitis Fischer, Sandra; Trivedi, Palak; Ward, Stephen; Greig, Paul D.; Therapondos,
Frequency and significance of IgG4 immunohistochemical staining in liver explants from patients with primary sclerosing cholangitis Fischer, Sandra; Trivedi, Palak; Ward, Stephen; Greig, Paul D.; Therapondos,
IgG4-related disease: features and treatment response in a multi-ethnic cohort in Singapore
 IgG4-related disease: features and treatment response in a multi-ethnic cohort in Singapore W. Fong 1,2,3, I. Liew 1, D. Tan 2,3,4, K.H. Lim 5, A. Low 6, Y.Y. Leung 1,2 1 Department of Rheumatology and
IgG4-related disease: features and treatment response in a multi-ethnic cohort in Singapore W. Fong 1,2,3, I. Liew 1, D. Tan 2,3,4, K.H. Lim 5, A. Low 6, Y.Y. Leung 1,2 1 Department of Rheumatology and
IgG4-related Sclerosing Disease: Autoimmune Pancreatitis and Extrapancreatic
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Pancreatic Cancer Masquerading as Pancreatitis
 Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
How 5 Diseases Became One. Moez Tajdin R3 McGill University
 How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
Autoimmune Pancreatitis: A Succinct Overview
 REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
 Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Strategy to differentiate autoimmune pancreatitis from pancreas cancer
 Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Histological diagnosis of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study with EUS-FNA
 J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
Key words: diagnosis, immunoglobulin G4, immunoglobulin G4-related diseases, immunohistochemistry, pseudolymphoma. CASE HISTORY
 doi: 10.1111/1346-8138.12301 Journal of Dermatology 2013; 40: 998 1003 ORIGINAL ARTICLE Case of immunoglobulin G4-related skin disease: Possible immunoglobulin G4-related skin disease cases in cutaneous
doi: 10.1111/1346-8138.12301 Journal of Dermatology 2013; 40: 998 1003 ORIGINAL ARTICLE Case of immunoglobulin G4-related skin disease: Possible immunoglobulin G4-related skin disease cases in cutaneous
Chronic Pancreatitis
 Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Tratamiento endoscópico de la CEP. En quien como y cuando?
 Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Objectives. Intraoperative Consultation of the Whipple Resection Specimen. Pancreas Anatomy. Pancreatic ductal carcinoma 11/10/2014
 Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Autoimmune pancreatitis: the classification puzzle
 Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Immunoglobulin G4 (IgG4)-related disease, a systemic,
 IgG4-Related Disease of the Gastrointestinal Tract A 21st Century Chameleon Vikram Deshpande, MD Context. Immunoglobulin G4 (IgG4) related disease is a systemic fibroinflammatory disease capable of affecting
IgG4-Related Disease of the Gastrointestinal Tract A 21st Century Chameleon Vikram Deshpande, MD Context. Immunoglobulin G4 (IgG4) related disease is a systemic fibroinflammatory disease capable of affecting
Autoimmune pancreatitis can transform into chronic features similar to advanced
 Autoimmune pancreatitis can transform into chronic features similar to advanced chronic pancreatitis with functional insufficiency following severe calcification Short Title: AIP can transform into chronic
Autoimmune pancreatitis can transform into chronic features similar to advanced chronic pancreatitis with functional insufficiency following severe calcification Short Title: AIP can transform into chronic
Immunoglobulin G4-Related Sclerosing Disease Involving the Urethra: Case Report
 Case Report http://dx.doi.org/10.3348/kjr.2012.13.6.803 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(6):803-807 Immunoglobulin G4-Related Sclerosing Disease Involving the Urethra: Case Report
Case Report http://dx.doi.org/10.3348/kjr.2012.13.6.803 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(6):803-807 Immunoglobulin G4-Related Sclerosing Disease Involving the Urethra: Case Report
Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related Disease
 Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Incidence of Malignancy in Type 1 Autoimmune Pancreatitis
 ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review
 Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
IgG4 ᛶ ᝈ䛸 ᶫᮏ ᕫච ᛶ ⅖ ḷᒣ Ꮫ య Ꮫ ぬ㐨
 IgG4 Autoimmune pancreatitis Histopathological features: Diffuse lymphoplasmacytic infiltration Stromal fibrosis Acinar atrophy Obliterative phlebitis 1. Hamano et al reported that serum IgG4 levels were
IgG4 Autoimmune pancreatitis Histopathological features: Diffuse lymphoplasmacytic infiltration Stromal fibrosis Acinar atrophy Obliterative phlebitis 1. Hamano et al reported that serum IgG4 levels were
Case Report IgG4-Related Nasal Pseudotumor
 Case Reports in Otolaryngology Volume 2015, Article ID 749890, 4 pages http://dx.doi.org/10.1155/2015/749890 Case Report IgG4-Related Nasal Pseudotumor L. K. Døsen, 1 P. Jebsen, 2 B. Dingsør, 3 and R.
Case Reports in Otolaryngology Volume 2015, Article ID 749890, 4 pages http://dx.doi.org/10.1155/2015/749890 Case Report IgG4-Related Nasal Pseudotumor L. K. Døsen, 1 P. Jebsen, 2 B. Dingsør, 3 and R.
A 53 year-old woman with a lung mass, right hilar mass and mediastinal adenopathy.
 November 2015 Case of the Month A 53 year-old woman with a lung mass, right hilar mass and mediastinal adenopathy. Contributed by: Rasha Salama, M.D., IU Department of Pathology and Laboratory Medicine
November 2015 Case of the Month A 53 year-old woman with a lung mass, right hilar mass and mediastinal adenopathy. Contributed by: Rasha Salama, M.D., IU Department of Pathology and Laboratory Medicine
IgG4-related sclerosing cholangitis: all we need to know
 J Gastroenterol (2016) 51:295 312 DOI 10.1007/s00535-016-1163-7 REVIEW IgG4-related sclerosing cholangitis: all we need to know Yoh Zen 1 Hiroshi Kawakami 2 Jung Hoon Kim 3 Received: 24 December 2015 /
J Gastroenterol (2016) 51:295 312 DOI 10.1007/s00535-016-1163-7 REVIEW IgG4-related sclerosing cholangitis: all we need to know Yoh Zen 1 Hiroshi Kawakami 2 Jung Hoon Kim 3 Received: 24 December 2015 /
University of Texas-MD Anderson Cancer Center, Houston, Texas, USA. University of Medicine and Pharmacy Craiova, Romania
 Case Report A Diagnostic Challenge: Pancreatic Cancer or Autoimmune Pancreatitis? IRINA MIHAELA CAZACU 1,2, ADRIANA ALEXANDRA LUZURIAGA CHAVEZ 1, ADRIAN SAFTOIU 2, TONYA G. WHITLOW 1, PRIYA BHOSALE 3,
Case Report A Diagnostic Challenge: Pancreatic Cancer or Autoimmune Pancreatitis? IRINA MIHAELA CAZACU 1,2, ADRIANA ALEXANDRA LUZURIAGA CHAVEZ 1, ADRIAN SAFTOIU 2, TONYA G. WHITLOW 1, PRIYA BHOSALE 3,
Hilar cholangiocarcinoma. Frank Wessels, Maarten van Leeuwen, UMCU utrecht
 Hilar cholangiocarcinoma Frank Wessels, Maarten van Leeuwen, UMCU utrecht Content Anatomy Biliary strictures (Hilar) Cholangiocarcinoom Staging Biliary tract 1 st order Ductus hepatica dextra Ductus hepaticus
Hilar cholangiocarcinoma Frank Wessels, Maarten van Leeuwen, UMCU utrecht Content Anatomy Biliary strictures (Hilar) Cholangiocarcinoom Staging Biliary tract 1 st order Ductus hepatica dextra Ductus hepaticus
The Pathology of IgG4-Related Disease in the Bile Duct and Pancreas
 242 The Pathology of IgG4-Related Disease in the Bile Duct and Pancreas Yoh Zen, MD, PhD, FRCPath 1 1 Department of Diagnostic Pathology, Kobe University Graduate School of Medicine, Kobe, Japan Semin
242 The Pathology of IgG4-Related Disease in the Bile Duct and Pancreas Yoh Zen, MD, PhD, FRCPath 1 1 Department of Diagnostic Pathology, Kobe University Graduate School of Medicine, Kobe, Japan Semin
PANCREAS, CLINICAL LIVER, BILIARY
 GASTROENTEROLOGY 2008;134:440 446 Substitution of Aspartic Acid at Position 57 of the DQ 1 Affects Relapse of Autoimmune Pancreatitis DO HYUN PARK,* MYUNG HWAN KIM, HEUNG BUM OH, OH JOONG KWON, YOUNG JIN
GASTROENTEROLOGY 2008;134:440 446 Substitution of Aspartic Acid at Position 57 of the DQ 1 Affects Relapse of Autoimmune Pancreatitis DO HYUN PARK,* MYUNG HWAN KIM, HEUNG BUM OH, OH JOONG KWON, YOUNG JIN
Title: An ulcerated gastric ulcer and pseudotumour with pancreatic affectation associated with immunoglobulin G4-
 Title: An ulcerated gastric ulcer and pseudotumour with pancreatic affectation associated with immunoglobulin G4- related disease: a case report and literature review Authors: María Isabel Ortuño Moreno,
Title: An ulcerated gastric ulcer and pseudotumour with pancreatic affectation associated with immunoglobulin G4- related disease: a case report and literature review Authors: María Isabel Ortuño Moreno,
IgG4-related sclerosing disease
 Online Submissions: wjg.wjgnet.com World J Gastroenterol 2008 July 7; 14(25): 3948-3955 wjg@wjgnet.com World Journal of Gastroenterology ISSN 1007-9327 doi:10.3748/wjg.14.3948 2008 The WJG Press. All rights
Online Submissions: wjg.wjgnet.com World J Gastroenterol 2008 July 7; 14(25): 3948-3955 wjg@wjgnet.com World Journal of Gastroenterology ISSN 1007-9327 doi:10.3748/wjg.14.3948 2008 The WJG Press. All rights
Among the benign intraepithelial melanocytic proliferations, Inflamed Conjunctival Nevi. Histopathological Criteria. Resident Short Reviews
 Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
IgG4-related systemic disease (ISD) is a multisystem
 Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
FOR PUBLIC CONSULTATION ONLY. Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD)
 Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD) NHS England FOR PUBLIC CONSULTATION ONLY Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4- RD) First published:
Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD) NHS England FOR PUBLIC CONSULTATION ONLY Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4- RD) First published:
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction
 Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
An Intraductal Papillary Neoplasm of the Bile Duct at the Duodenal Papilla
 Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Incidence of Malignancies in Patients with IgG4-related Disease
 ORIGINAL ARTICLE Incidence of Malignancies in Patients with IgG4-related Disease Kenji Hirano 1, Minoru Tada 1, Naoki Sasahira 1, Hiroyuki Isayama 1, Suguru Mizuno 1, Kaoru Takagi 1, Takeo Watanabe 1,
ORIGINAL ARTICLE Incidence of Malignancies in Patients with IgG4-related Disease Kenji Hirano 1, Minoru Tada 1, Naoki Sasahira 1, Hiroyuki Isayama 1, Suguru Mizuno 1, Kaoru Takagi 1, Takeo Watanabe 1,
Clinical Study IgG4-Related Disease Is Not Associated with Antibody to the Phospholipase A2 Receptor
 International Rheumatology Volume 2012, Article ID 139409, 6 pages doi:10.1155/2012/139409 Clinical Study IgG4-Related Disease Is Not Associated with Antibody to the Phospholipase A2 Receptor Arezou Khosroshahi,
International Rheumatology Volume 2012, Article ID 139409, 6 pages doi:10.1155/2012/139409 Clinical Study IgG4-Related Disease Is Not Associated with Antibody to the Phospholipase A2 Receptor Arezou Khosroshahi,
Clinical outcomes and pathological characteristics of immunoglobulin G4-related ophthalmic disease versus orbital inflammatory pseudotumor
 ORIGINAL ARTICLE Korean J Intern Med 2019;34:220-226 Clinical outcomes and pathological characteristics of immunoglobulin G4-related ophthalmic disease versus orbital inflammatory pseudotumor Hong Ki Min
ORIGINAL ARTICLE Korean J Intern Med 2019;34:220-226 Clinical outcomes and pathological characteristics of immunoglobulin G4-related ophthalmic disease versus orbital inflammatory pseudotumor Hong Ki Min
The newly recognized fibroinflammatory condition. An orphan disease: IgG4-related spinal pachymeningitis: report of 2 cases
 case report J Neurosurg Spine 25:790 794, 2016 An orphan disease: IgG4-related spinal pachymeningitis: report of 2 cases Bishan D. Radotra, MD, 1 Ashish Aggarwal, DNB, MCh, 2 Ankur Kapoor, MS, MCh, 2 Navneet
case report J Neurosurg Spine 25:790 794, 2016 An orphan disease: IgG4-related spinal pachymeningitis: report of 2 cases Bishan D. Radotra, MD, 1 Ashish Aggarwal, DNB, MCh, 2 Ankur Kapoor, MS, MCh, 2 Navneet
IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal
 CASE REPORT IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal Miho Otani 1, Masahiro Morinaga 1, Yoshihiko Nakajima 1, Hiromi Tomioka 2, Michiko Nishii
CASE REPORT IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal Miho Otani 1, Masahiro Morinaga 1, Yoshihiko Nakajima 1, Hiromi Tomioka 2, Michiko Nishii
Diseases of pancreas - Chronic pancreatitis
 Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Disclosure of Relevant Financial Relationships
 Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
Anatomy of the biliary tract
 Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14
 Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
A Case of IgG4-Related Disease Presenting as Massive Pleural Effusion and Thrombophlebitis
 CASE REPORT http://dx.doi.org/10.4046/trd.2014.76.4.179 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;76:179-183 A Case of IgG4-Related Disease Presenting as Massive Pleural Effusion
CASE REPORT http://dx.doi.org/10.4046/trd.2014.76.4.179 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;76:179-183 A Case of IgG4-Related Disease Presenting as Massive Pleural Effusion
Type 2 Autoimmune Pancreatitis with Crohn s Disease
 doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases
 MULTIMEDIA ARTICLE - Clinical Imaging Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases Vien X Nguyen 1, Giovanni De Petris 2, Ba D Nguyen 3 Departments
MULTIMEDIA ARTICLE - Clinical Imaging Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases Vien X Nguyen 1, Giovanni De Petris 2, Ba D Nguyen 3 Departments
p53 expression in invasive pancreatic adenocarcinoma and precursor lesions
 Malaysian J Pathol 2011; 33(2) : 89 94 ORIGINAL ARTICLE p53 expression in invasive pancreatic adenocarcinoma and precursor lesions NORFADZILAH MY MBBCH,* Jayalakshmi PAILOOR MPath, FRCPath,* RETNESWARI
Malaysian J Pathol 2011; 33(2) : 89 94 ORIGINAL ARTICLE p53 expression in invasive pancreatic adenocarcinoma and precursor lesions NORFADZILAH MY MBBCH,* Jayalakshmi PAILOOR MPath, FRCPath,* RETNESWARI
Autoimmune Liver Diseases
 2nd Pannonia Congress of pathology Hepato-biliary pathology Autoimmune Liver Diseases Vera Ferlan Marolt Institute of pathology, Medical faculty, University of Ljubljana Slovenia Siofok, Hungary, May 2012
2nd Pannonia Congress of pathology Hepato-biliary pathology Autoimmune Liver Diseases Vera Ferlan Marolt Institute of pathology, Medical faculty, University of Ljubljana Slovenia Siofok, Hungary, May 2012
Gastric Carcinoma with Lymphoid Stroma: Association with Epstein Virus Genome demonstrated by PCR
 Gastric Carcinoma with Lymphoid Stroma: Association with Epstein Virus Genome demonstrated by PCR Pages with reference to book, From 305 To 307 Irshad N. Soomro,Samina Noorali,Syed Abdul Aziz,Suhail Muzaffar,Shahid
Gastric Carcinoma with Lymphoid Stroma: Association with Epstein Virus Genome demonstrated by PCR Pages with reference to book, From 305 To 307 Irshad N. Soomro,Samina Noorali,Syed Abdul Aziz,Suhail Muzaffar,Shahid
Consensus Statement on the Pathology of IgG4-Related Disease
 Consensus Statement on the Pathology of IgG4-Related Disease The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation Deshpande,
Consensus Statement on the Pathology of IgG4-Related Disease The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation Deshpande,
Azathioprine Induced Pancreatitis in a Patient with Co-Existing Autoimmune Pancreatitis and Hepatitis
 CASE REPORT Azathioprine Induced Pancreatitis in a Patient with Co-Existing Autoimmune Pancreatitis and Hepatitis Preethi GK Venkatesh, Udayakumar Navaneethan Digestive Disease Institute, Cleveland Clinic
CASE REPORT Azathioprine Induced Pancreatitis in a Patient with Co-Existing Autoimmune Pancreatitis and Hepatitis Preethi GK Venkatesh, Udayakumar Navaneethan Digestive Disease Institute, Cleveland Clinic
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint
 GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
Autoimmune Pancreatitis: Case Series and Review of the Literature.
 Available online at www.annclinlabsci.org Annals of Clinical & Laboratory Science, vol. 39, no. 2, 2009 167 Autoimmune Pancreatitis: Case Series and Review of the Literature. Rada Shakov, 1 Joseph R. DePasquale,
Available online at www.annclinlabsci.org Annals of Clinical & Laboratory Science, vol. 39, no. 2, 2009 167 Autoimmune Pancreatitis: Case Series and Review of the Literature. Rada Shakov, 1 Joseph R. DePasquale,
