Nephrotic Syndrome. Abstract. MK Mani Chief Nephrologist, Apollo Hospital, 21, Greams Lane, Chennai
|
|
|
- Paulina Carr
- 6 years ago
- Views:
Transcription
1 Nephrotic Syndrome MK Mani Chief Nephrologist, Apollo Hospital, 21, Greams Lane, Chennai Abstract Much information has become available in recent times about the structure of the glomerular basement membrane (GBM), the pathway of filtration of proteins, and the barriers to passage of proteins through the GBM. There is both a size barrier and a charge barrier. The main location of both of these is the slit diaphragm between the foot processes of the glomerular epithelial cells. Apart from the effects of the disease causing the nephrotic syndrome, proteinuria is itself harmful to the kidney. It leads to focal glomerular sclerosis, tubular damage, apoptosis of tubular cells, and release of cytokines causing chronic interstitial changes and progressive renal failure. Hypoproteinaemia can be associated with oedema, hyperlipidaemia, and a hypercoagulable state. Changing concepts of management include the understanding that a high protein diet can itself increase proteinuria and is therefore counterproductive. It is also very difficult to correct proteinuria by giving more protein since most of the extra protein is excreted in the urine. It is therefore essential to reduce proteinuria, preferably by curing the condition leading to the nephrotic state, but failing that with the use of ACE inhibitors. Lipid abnormalities are usually reversed if proteinuria can be controlled, but if proteinuria persists it is essential to correct the lipids with appropriate diet and therapy. Measurement of the urinary protein creatinine ratio in a spot sample of urine is a simple and effective way to monitor the progression of the disease and the success of treatment. Definition The traditional definition of the nephrotic syndrome is the association of massive proteinuria with hypoalbuminaemia and oedema. Since there are some patients with massive proteinuria who do not become oedematous, the definition was altered to the passage of 3.5 g protein per 1.73 sq m body surface area in 24 hours. Neither definition should be slavishly adhered to. Proteinuria arises when there is an increase in the permeability of the glomerular capillary to protein. In other words the glomerular clearance of protein increases. A certain amount of blood is cleared of its protein content each minute. If serum albumin is 4.2 g/dl, and if the protein clearance is 0.1 ml/min, the patient will lose 4.2 mg of protein per minute, or g of protein per day. When serum albumin falls to 2.1 g/dl, with the same leak of protein, urinary protein will fall to g/day, and will fall below the mathematical definition of the nephrotic syndrome. However, the disease and its severity are the same, only it has lasted longer and the patient is more ill. It would be absurd to withdraw the diagnosis of the nephrotic syndrome. One should therefore combine both definitions with a touch of commonsense. In any case, the nephrotic syndrome is not a disease entity. It is only a symptom complex that can be produced by many diseases, each with its own treatment and its own course and prognosis. One should recognise that and proceed to make a full diagnosis in every patient so that appropriate treatment may be administered. The pathogenesis of severe proteinuria The filtration pathway through the glomerulus begins with the capillary endothelium, which has large pores called fenestrae that can easily be traversed by proteins. They can thus reach the glomerular basement membrane (GBM). The GBM behaves as if it has pores, though these pores have not been demonstrated even with the electron microscope. The size of the pores follows 632
2 a bimodal distribution, the majority, through which filtration of small molecules takes place (normal glomerular filtration) being small. A very few have a substantially larger diameter, and permit the filtration of proteins. In disease states it is possible for the number of these pores to vary independently of each other, so one can get many more large pores with significant proteinuria, and at the same time there may be far fewer small pores, leading to reduced GFR. The major barrier to protein filtration, however, lies in the slit diaphragm which bridges the slits between the foot processes of the glomerular epithelial cells, at their junction with the GBM. 1,2 It has been found that molecules of a protein, nephrin, stretch from opposing foot processes and bridge the gap. They are stabilised in that position by another compound called podocin. Yet another substance, CD2AP, binds nephrin to the podocyte. Any disruption, caused by defective structure due to genetic defects, or to antibodies to one or more components, leads to proteinuria. This knowledge has not yet led to any remedy for the nephrotic syndrome. Another cause of proteinuria at this level is damage to the epithelial cells. Foot processes fuse and get lifted off the GBM, leaving a wide gap through which protein can leak. Apart from the structure that provides a size barrier, the GBM has a coating of glycosaminoglycans that provide a charge barrier. These are negatively charged molecules that inhibit the passage of the negatively charged proteins. The earliest damage to the GBM is associated with loss of this negative charge, as a result of which the smaller molecule, albumin, is allowed to filter through though the size barrier restrains larger globulins. The ill effects of proteinuria Progressive renal failure Irrespective of the disease causing the nephrotic syndrome, proteinuria itself has harmful effects on the kidney. By mechanisms described below, it leads to focal glomerular sclerosis, tubular cell apoptosis and interstitial fibrosis. 3,4 The more severe the proteinuria, the more rapid the development of chronic interstitial fibrosis and therefore chronic renal failure. It is important to reduce proteinuria. Focal and segmental glomerulosclerosis The first part to suffer is the glomerulus. It is clear that proteinuria leads to secondary glomerular sclerosis. Various mechanisms have been postulated. Foot processes fuse and lose their attachment to the GBM, exposing it to the cells of the parietal epithelium, which proliferate, adhere to the GBM, and release cytokines that lead to sclerosis. Some of the protein is absorbed through megalin molecules on the epithelial cells. When the cell is overloaded with protein, cytokines are released that cause proliferation of cells and sclerosis. Proteins also accumulate in the mesangium and induce cytokines that induce cellular proliferation and increased production of matrix, thereby leading to focal sclerosis. Tubular apoptosis and interstitial fibrosis Filtered protein is endocytosed by megalin at the luminal border of the cells, and taken up by lysosomes. If the capacity of the lysosomes to digest these proteins is exceeded, they rupture and release their digestive contents into the cytoplasm. Ammonia is released and activates complement at the basolateral membrane. Complement mediated fibrosis leads to chronic interstitial damage. The lysosomal enzymes digest the cell contents. Damaged cells also release osteopontin and macrophage chemoattractant polypeptide which draw inflammatory cells to the interstitium. Cytokines released by these cells add to interstitial fibrosis. Proteinuria also leads to apoptosis of tubular cells. Extra-renal effects Oedema The traditional view of the nephrotic syndrome is that it leads to hypoproteinaemia, low plasma osmolality with leakage of fluid into the interstitium and underfilling of the circulation. This in turn leads to reduced renal perfusion, release of renin and hence of aldosterone, which retains salt and secondarily water. While this may be true in minimal lesion nephropathy, in most other conditions there is overfilling of the circulation, and other explanations must be found. It has been demonstrated that albumin in the proximal tubular lumen directly stimulates the sodium hydrogen exchanger leading to retention of sodium. In the principal cells of the cortical collecting duct, over activity of Na +,K + -ATPase and the epithelial Na channel have been demonstrated. There is resistance to the action of atrial natriuretic peptide in the collecting duct, and this adds to sodium retention. The mechanisms of these changes have not yet been determined, but our understanding is surely and steadily improving. The distinction between under and over fill is important because a patient with overfill should benefit with diuretics, whereas if there is underfill diuretics may lower the circulating blood volume further and make the patient feel weak, or precipitate syncope from low blood pressure. Coagulation abnormalities 5 It is not only the plasma proteins that are lost in the urine. Various factors which play a part in the coagulation cascade also leak through. Zymogens (factors IX, XI and XII) normally regulate coagulation activity and are lost in the urine in the nephrotic syndrome. Hypoalbuminaemia stimulates the liver to produce more proteins, and the manufacture of factors V and VIII is increased along with molecules like albumin, as well as factors II, VII and X. Fibrinogen levels are also increased due to greater hepatic synthesis. Antithrombin III is also lost in the urine. In balance, there is loss of anticlotting factors and increased levels of pro coagulation factors, and this renders the patient more prone to intravascular coagulation. Renal vein thrombosis is especially common in membranous nephropathy and in some children with minimal lesion nephropathy. The dangers are of sudden loss of renal function, and of spread to the inferior vena cava followed by pulmonary embolism. Lipid abnormalities 6 Cholesterol and phospholipid levels rise early, triglyceride late in the course of the disease. HDL cholesterol may be normal or sometimes low. I do not have the space to discuss the mechanisms. Hyperlipidaemia contributes to early atherosclerosis, and leads to coronary artery disease. It may also contribute to focal glomerular sclerosis and progression of chronic renal failure. nephrotic syndrome 633
3 Table 1 : Causes of the nephrotic syndrome. Apollo Hospital patients in 20 years. Cause Percentage Minimal lesion nephropathy 35.4 Diabetic nephropathy 19.3 Focal and segmental glomerular sclerosis 10.4 Membranous nephropathy 9.9 Mesangial proliferative glomerulonephritis 7.4 Systemic lupus erythematosus 5.8 Membranoproliferative GN 5.4 Others 6.4 The diagnosis of the nephrotic syndrome As I wrote in my introduction, I do not believe it is necessary to quantitate urinary protein excretion to make a diagnosis of the nephrotic syndrome. The clinical picture should suffice, together with a demonstration of massive proteinuria. However, some indices are essential to assess the response of a patient to treatment, and to monitor the progress of the disease. These include serum urea, creatinine and albumin, and urinary protein excretion. While a 24 hour urine collection is the gold standard, it is inconvenient and therefore repeated estimation will face some resistance from the patient. It has been demonstrated in numerous studies that the protein creatinine ratio done on a spot sample of urine correlates well with the 24 hour urine protein, provided serum creatinine is 1.5 mg/dl or less. This alone is inadequate to follow up a patient, since, as discussed earlier, protein excretion could fall because the patient has gone into renal failure or because serum albumin levels have fallen. The combination of serum urea, creatinine and albumin with the urine protein creatinine ratio is therefore the most convenient and accurate way to follow up a patient. Is it necessary to establish the diagnosis in a patient with the nephrotic syndrome? In 1983, a very influential nephrologist of the USA suggested 7 that there was no necessity to bother with renal biopsy to make a diagnosis, at least initially, since every patient could be given a trial of steroids, and only those who failed to respond would need investigation. I am convinced that this opinion does not hold good for India, and did a study that bears out my conviction. 8 The risks of infection and other side effects are too great, and it is better to have a firm diagnosis before one embarks on treatment. The most common causes of the nephrotic syndrome in my unit are listed in Table 1. Minimal lesion nephropathy could be diagnosed in a child with the nephrotic syndrome, who does not have hypertension, microscopic haematuria or azotaemia. Diabetic nephropathy may be accepted in a patient with long standing, poorly controlled diabetes and diabetic retinopathy. Systemic lupus erythematosus requires a typical symptomatology of fever, skin rash and joint pains, and positive serology for lupus. In all other instances, renal biopsy is called for. It is especially important as only minimal lesion nephropathy and focal sclerosis respond to steroids alone. All the others require alkylating agents in addition, and even focal sclerosis requires a prolonged course of steroids. I will not go into the other causes of the nephrotic syndrome since all of them together account for only 6.4% of the patients. The management of the nephrotic syndrome Diet When one sees a patient with hypoalbuminaemia, the temptation is to give him a very high protein diet to compensate for the losses. It took the medical profession many years to realise that this is counterproductive. It does not work and it may be positively harmful. We have already seen that proteinuria itself damages the glomerulus as well as the tubule, and a high protein diet increases glomerular filtration and proteinuria. 9 There have been many explanations advanced, but the one that appeals to me most is the following: the macula densa has the capacity to sense the sodium and chloride content of urine flowing through the distal tubule. When the content is high, glomerular filtration is reduced by a process known as tubulo-glomerular feedback, and when it is low glomerular filtration increases. The bulk of filtered sodium is reabsorbed in the proximal convoluted tubule. There are many sodium transporters, through most of which sodium passes in linkage with some other substance. One of the transporters conveys sodium with amino acids. A person on a high protein diet will excrete a lot of amino acids in the urine, and the reabsorption in the proximal tubule will lead to increased reabsorption of sodium. Reabsorption of chloride runs in parallel with sodium, though the mechanisms are not as well understood. Excessive reabsorption of sodium in association with amino acids leads to less sodium and chloride passing the macula densa, and therefore to greater glomerular filtration. In other words, a high protein diet increases glomerular filtration and with it the excretion of protein, and greater risk of progressive glomerular and tubulointerstitial damage. Besides this, greater proteinuria makes it more difficult to correct the serum protein level, so a high protein diet does not work and is positively harmful. One should give the patient normal quantities of protein, and if there is renal failure protein intake should in fact be restricted as in any patient with renal failure. For the same reasons, it is harmful to give a patient intravenous infusion of albumin. The effect is to pour the albumin from the bottle into the toilet bowl using the patient as a conduit. Albumin is indicated only in the short term when hypoalbuminaemia is so severe that the patient is unable to stand because of orthostatic hypotension. Salt intake should be restricted in keeping with the oedema and the blood pressure, and saturated fats should also be restricted. Diuretics may be used if oedema is massive and troublesome, but I prefer to tackle the cause of the nephrotic syndrome as far as possible. Treat the cause of the nephrotic syndrome I do not have the space to deal with this in detail. For minimal lesion nephropathy, most Indian nephrologists use the protocol recommended in the Western literature. 10 I believe this delivers too massive a dose for Indian conditions and have evolved a lower dose and shorter courses that I have found effective with far fewer side effects (Table 2). 634
4 Table 2 : My protocol for the management of minimal lesion nephropathy 1. Put the patient on prednisolone, the dose being 2 mg/kg body weight per day in a single dose each morning if the body weight is below 15 kg, 1 mg/kg if the weight is above 30 kg, and 30 mg if the weight is between 15 and 30 kg. 2. Check urine protein once a week. When proteinuria comes to nil, taper off prednisolone by 5 mg every three days and thus stop it. If the dose of prednisolone is above 50 mg, taper off by 10 mg every three days. 3. Approximately 30% of patients will not relapse, 30% will have a few relapses, and 30% are frequent relapsers. 4. If the patient develops oedema again, confirm the presence of proteinuria and wait for one week. Spontaneous remission occurs in 4% of patients in my experience. 5. If oedema and proteinuria persist for one week, start on prednisolone again as indicated above. 6. Up to three attacks may be treated in this fashion in any 12 month period. If the patient has a fourth attack within a year, he may receive prednisolone again as before, but in addition may receive cyclophosphamide in a dose of 2.5 mg/kg body weight, rounded off to the nearest 25 mg, given each morning. The leucocyte count may be checked once a week, and cyclophosphamide may be withheld if the count falls below 4000/cmm. Once that happens, the count may be checked every day and cyclophosphamide may be restarted when the count rises above 4000 again. If this happens within one week, the same dose may be given, but if it takes more than a week to recover the dose may be reduced to approximately 75% of the original dose. 7. Prednisolone may be tapered off when proteinuria disappears but cyclophosphamide may be continued for eight weeks, and then abruptly stopped. 8. Cyclophosphamide usually induces permanent or at least a longer remission. If relapse occurs after a course of this drug, treatment may be with prednisolone as indicated above. 9. If an alkylating agent is indicated again, it is unwise to repeat cyclophosphamide. The patient may be given chlorambucil in a dose of 0.2 mg/kg, continued for eight weeks with the same precautions as with cyclophosphamide. 10. If, at any time, the patient should receive prednisolone in appropriate dosage for eight weeks without response of proteinuria, he or she should undergo a renal biopsy to establish the accurate diagnosis and treat accordingly. 11. A very small number of patients will have minimal lesion nephropathy proved on biopsy, respond to steroids and will relapse whenever steroids are withdrawn. They are classed as steroid dependent, and will require long continued steroids. The minimal effective dose should be used. There is no specific treatment for diabetic nephropathy, and the non-specific measures of ACE inhibitors must be used. My protocol is detailed below. I would give a trial of prednisolone for all patients with focal glomerular sclerosis. Treatment is as for minimal lesion nephropathy, but since proteinuria will not disappear in a short time, it has to be maintained longer. I would assess protein excretion every month, and continue steroids as long as there is progressive decline in the leakage of protein. Once it stabilises, steroids may be tapered off and ACE inhibitors introduced. Membranous nephropathy responds to the Ponticelli regimen 11 in 69% of my patients, and to ACE inhibitors in 53%. The difference is not statistically significant, and either treatment may be used. If one fails, the other may be instituted. The therapy of mesangial proliferative glomerulonephritis (the most common cause of which is IgA nephropathy) and membranoproliferative glomerulonephritis is still disputed. I have found some patients with IgA nephropathy to respond to cyclophosphamide and prednisolone, but side effects are common and serious. If there is no response, it might be more effective and safe to use ACE inhibitors. Nephritis due to systemic lupus erythematosus almost always responds to prednisolone and cyclophosphamide. The readers are referred to the reference cited for details of therapy. 12 ACE inhibitors (ACEI) for the nephrotic syndrome ACEI have many actions in the nephrotic syndrome. The major effect may be haemodynamic. Reduced renal perfusion due to chronic renal disease and to reduced circulating blood volume stimulate the renin angiotensin system. Angiotensin II (A II) is released in the glomerulus. The first arteriole it comes in contact with is the efferent arteriole, which is also more richly endowed with A II receptors than the afferent arteriole. Preferential contraction of the efferent arteriole raises intraglomerular pressure and therefore both GFR and the leak of protein, both of which accelerate the decline in renal function. AII is also a growth factor and leads to proliferation of glomerular cells, and secondary release of cytokines leading to sclerosis and to interstitial fibrosis. ACEI counteract these effects, reduce proteinuria, and slow progression of renal disease, besides having an antihypertensive effect. On the other hand, reduced GFR can worsen renal failure, and the suppression of aldosterone could cause hyperkalaemia. I would start by estimating renal function (serum urea and creatinine), proteinuria (urine protein creatinine ratio if creatinine is below 1.5 mg/dl, 24 hour urine protein if it is above) and its effects (serum protein and albumin). I would then start with 2.5 mg of enalapril twice daily. After one week, I would check serum urea and potassium. Urea may be allowed to rise by one third (e.g. 75 mg to 100 mg) and potassium to 5.5 meq/l. One should expect a rise in urea since GFR falls. This is the effect we are aiming for, and is not harmful if within limits. I prefer to use urea rather than creatinine to judge this effect since, if GFR is normal, the rise in creatinine would be small and may be within the limits of laboratory fluctuation. BP should also fall, and should be allowed to fall to between 100 and 110 mm systolic, provided the patient does not have troublesome orthostatic hypotension. There is no lower limit to the diastolic pressure. Enalapril may be increased by 5 mg every week (2.5 mg twice). When the dose of enalapril reaches 20 mg/day (10 mg twice daily), I would reassess renal function and urinary protein excretion. If there is some improvement in proteinuria without excessive decline in GFR, I would raise the dose in stages to 40 mg/day. There is no upper limit to the dose, and I have reached 200 mg in some patients, as long as there are no side effects. nephrotic syndrome 635
5 There is no point in increasing the dose if there is no progressive reduction in proteinuria. Once further increments cause no added benefit, the same dose of enalapril may be maintained and losartan may be added in a dose of 25 mg twice daily, increasing by 25 mg per week to 100 mg per day. Assessment of benefit may be done at every 100 mg level. I have some patients taking 300 mg of losartan per day. I should point out that the majority of patients would reach the maximum effective dose much below these levels, and it is futile to increase the dose once there is no progressive benefit. I use enalapril and losartan since these are the cheapest drugs in their class, and no added benefit has been found with more expensive congeners. If blood pressure falls too low, the dose of enalapril and losartan may be maintained and indomethacin added, starting with 25 mg twice daily, and increasing by 25 mg every week. NSAIDs reduce glomerular filtration by blocking the action of prostaglandins that are vasodilator. The vasoconstriction of the afferent arteriole that results leads to reduction of GFR and with it proteinuria, while raising the blood pressure. One must monitor blood urea and serum potassium once a week as for ACEI, and withdraw the drug or reduce the dose if there is progressive deterioration. The effect on proteinuria may be measured once a month and the dose should be increased only if there is a beneficial effect. Once BP rises to satisfactory levels, the dose of ACEI may be increased again. It is possible to reduce proteinuria substantially, often to normal levels, by these measures in the majority of patients. Treatment of hyperlipidaemia I would not rush to treat hyperlipidaemia in the average patient with the nephrotic syndrome, since lipid levels often normalise once proteinuria is controlled. If it proves impossible to induce a remission of the nephrotic syndrome, it is necessary to use a lipid lowering agent, and I would use a statin. I have found rosuvastatin to be especially effective. It should be remembered that the toxicity of all protein-bound drugs is increased when serum albumin levels are low, so one should start with the minimum dose, monitor the patient for side effects, and increase the dose gradually. Hyperlipidaemia may itself contribute to progressive worsening of renal function and to proteinuria, so control of lipids is desirable apart from the prevention of progressive atheromatous change. Coagulation abnormalities I would not ordinarily administer anticoagulants for the nephrotic syndrome. While the incidence of renal vein thrombosis has been variously reported to be between 7 and 70% of patients, it is rarely of clinical significance. However, once renal or other venous thrombosis is detected, the patient should be maintained on anticoagulant therapy to minimise the risk of pulmonary thromboembolism. Patients with membranous nephropathy are supposedly more prone to develop this complication, which should be suspected whenever a patient has a sudden decline in renal function with no obvious explanation. Follow up Even if you achieve a complete remission, please remember that there may be underlying disease activity and progressive subclinical deterioration is possible. Every patient should be cautioned to check BP, urinary protein excretion and renal function (blood urea and creatinine) once a year throughout his life. References 1. Johnson RJ. New insights into the pathogenesis of proteinuria. Am J Kidney Dis 2000;36: Tryggvason KI. Unraveling the mechanisms of glomerular ultrafiltration: Nephrin, a key component of the slit diaphragm. J Am Soc Nephrol 1999; 10: Burton C. The role of proteinuria in the progression of chronic renal failure. Am J Kidney Dis 1996;27: D Amico G, Bazzi C. Pathophysiology of proteinuria. Kidney Int 2003; 63: Llach F. Hypercoagulability, renal vein thrombosis, and other nephrotic complications of the nephrotic syndrome. Kidney Int 1985;28: Kaysen GA. Hyperlipidaemia in the nephrotic syndrome. Am J Kidney Dis 1988;12: Kassirer JP. Is renal biopsy necessary for optimal management of the idiopathic nephrotic syndrome? Kidney Int 1983;24: Mani MK. Is renal biopsy necessary in the management of the nephrotic syndrome? J Ass Physicians India 1989;37: Wiseman MJ, Hunt R, Goodwin A, Gross JL, Keen H, Viberti GC. Dietary composition and renal function in healthy subjects. Nephron 1987;46: Nephrotic syndrome in children: a randomized trial comparing two prednisone regimens in steroid-responsive patients who relapse early. Report of the International Study of Kidney Disease in Children. J Pediatr 1979;95: Ponticelli C, Passerini P. Treatment of membranous nephropathy. Nephrol Dial Transplant 2001;16 Suppl 5: Flanc RS, Roberts MA, Strippoli GF, Chadban SJ, Kerr PG, Atkins RC. Treatment of diffuse proliferative lupus nephritis: a meta-analysis of randomized controlled trials. Am J Kidney Dis 2004;43:
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Urinary bladder provides a temporary storage reservoir for urine
 Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Renal Physiology - Lectures
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM
 RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION
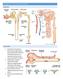 LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION
 3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Nephritic vs. Nephrotic Syndrome
 Page 1 of 18 Nephritic vs. Nephrotic Syndrome Terminology: Glomerulus: A network of blood capillaries contained within the cuplike end (Bowman s capsule) of a nephron. Glomerular filtration rate: The rate
Page 1 of 18 Nephritic vs. Nephrotic Syndrome Terminology: Glomerulus: A network of blood capillaries contained within the cuplike end (Bowman s capsule) of a nephron. Glomerular filtration rate: The rate
Paediatrics Dr. Bakr Lecture 3 Nephrotic Syndrome
 P a g e 1 DEFINITION Paediatrics Dr. Bakr Lecture 3 Nephrotic Syndrome Definition: nephrotic syndrome is a disorder characterized by heavy proteinuria with hypoprpteinimia,hyper lipidemia and edema. It
P a g e 1 DEFINITION Paediatrics Dr. Bakr Lecture 3 Nephrotic Syndrome Definition: nephrotic syndrome is a disorder characterized by heavy proteinuria with hypoprpteinimia,hyper lipidemia and edema. It
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Dr P Sigwadi Paediatric Nephrology
 Dr P Sigwadi Paediatric Nephrology Prevalence - 5-15 % on a single urine sample After a series of 4 tests only 0.1% of children had persistent positive proteinuria Persistent proteinuria indicates the
Dr P Sigwadi Paediatric Nephrology Prevalence - 5-15 % on a single urine sample After a series of 4 tests only 0.1% of children had persistent positive proteinuria Persistent proteinuria indicates the
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009
 www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers PROTEINURIA
www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers PROTEINURIA
Over- and underfill: not all nephrotic states are equal. Detlef Bockenhauer
 Over- and underfill: not all nephrotic states are equal Detlef Bockenhauer Objectives Review pathophysiology of oedema: undervs overfill Treatment options The clinical setting: case 1 A6-y old girl with
Over- and underfill: not all nephrotic states are equal Detlef Bockenhauer Objectives Review pathophysiology of oedema: undervs overfill Treatment options The clinical setting: case 1 A6-y old girl with
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Urinary system. Urinary system
 INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Ch 19: The Kidneys. Functional unit of kidneys:?? Developed by John Gallagher, MS, DVM
 Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Renal physiology II. Basic renal processes. Dr Alida Koorts BMS
 Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal Transporters- pathophysiology of drug - induced renal disorders. Lisa Harris, Pharmacist, John Hunter Hospital, Newcastle, 2015 November
 Renal Transporters- pathophysiology of drug - induced renal disorders Lisa Harris, Pharmacist, John Hunter Hospital, Newcastle, 2015 November Renal Failure Up to 25% of acute renal failure is drug induced
Renal Transporters- pathophysiology of drug - induced renal disorders Lisa Harris, Pharmacist, John Hunter Hospital, Newcastle, 2015 November Renal Failure Up to 25% of acute renal failure is drug induced
Glomerular filtration rate (GFR)
 LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note
![Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note](/thumbs/77/75431210.jpg) Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Renal System Physiology
 M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
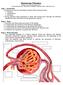 Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Formation of urine by the kidney involves
Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Formation of urine by the kidney involves
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
PHGY210 Renal Physiology
 PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
Introduction to the kidney: regulation of sodium & glucose. Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health
 Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
The kidneys are excretory and regulatory organs. By
 exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
Elevated Serum Creatinine, a simplified approach
 Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Overview of glomerular diseases
 Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
Kidney Structure. Renal Lobe = renal pyramid & overlying cortex. Renal Lobule = medullary ray & surrounding cortical labryinth.
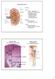 Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
EXCRETION IN HUMANS 31 JULY 2013
 EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
CONTROLLING THE INTERNAL ENVIRONMENT
 AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19
![QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19](/thumbs/77/74887026.jpg) QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion,
QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion,
Mr. I.K 58 years old
 Mr. I.K 58 years old Hospitalized because of marked pitting peripheral edema (bilateral crural and perimalleolar edema) and uncontrolled blood pressure (BP 150/100 mmhg under treatment). since age 54 years
Mr. I.K 58 years old Hospitalized because of marked pitting peripheral edema (bilateral crural and perimalleolar edema) and uncontrolled blood pressure (BP 150/100 mmhg under treatment). since age 54 years
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
Glomerular Pathology- 1 Nephrotic Syndrome. Dr. Nisreen Abu Shahin
 Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph
 The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
Lecture 16: The Nephron
 Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
A. Correct! Flushing acids from the system will assist in re-establishing the acid-base equilibrium in the blood.
 OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
Basic Functions of the Kidneys
 Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Glomerular pathology in systemic disease
 Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Nephrotic Syndrome. Department of pediatrics The first affiliated hospital Sun Yat Sen University. Yue Zhihui ( 岳智慧 )
 Nephrotic Syndrome Department of pediatrics The first affiliated hospital Sun Yat Sen University Yue Zhihui ( 岳智慧 ) yuezhihui810@yahoo.com.cn Contents Definition Pathophysiology Clinical manifestation
Nephrotic Syndrome Department of pediatrics The first affiliated hospital Sun Yat Sen University Yue Zhihui ( 岳智慧 ) yuezhihui810@yahoo.com.cn Contents Definition Pathophysiology Clinical manifestation
By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences. Body fluids and.
 By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences Body fluids and Renal physiology 25 Volume and Osmolality of Extracellular and Intracellular Fluids
By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences Body fluids and Renal physiology 25 Volume and Osmolality of Extracellular and Intracellular Fluids
Renal Functions: Renal Functions: Renal Function: Produce Urine
 Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Chapter 4: Steroid-resistant nephrotic syndrome in children Kidney International Supplements (2012) 2, ; doi: /kisup.2012.
 http://www.kidney-international.org & 2012 KDIGO Chapter 4: Steroid-resistant nephrotic syndrome in children Kidney International Supplements (2012) 2, 172 176; doi:10.1038/kisup.2012.17 INTRODUCTION This
http://www.kidney-international.org & 2012 KDIGO Chapter 4: Steroid-resistant nephrotic syndrome in children Kidney International Supplements (2012) 2, 172 176; doi:10.1038/kisup.2012.17 INTRODUCTION This
Urinary System (Anatomy & Physiology)
 Urinary System (Anatomy & Physiology) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran The Urinary System
Urinary System (Anatomy & Physiology) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran The Urinary System
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
URINARY SYSTEM. Urinary System
 URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Diabetic Nephropathy
 Diabetic Nephropathy Objectives: Know what Diabetic Nephropathy means. Know how common is Diabetic nephropathy in Saudi Arabia and to appreciate how bad are this complications. Know the risk factors of
Diabetic Nephropathy Objectives: Know what Diabetic Nephropathy means. Know how common is Diabetic nephropathy in Saudi Arabia and to appreciate how bad are this complications. Know the risk factors of
41B. Metabolism produces wastes that must be eliminated from the body. This. Renal System Physiology: Computer Simulation
 41B E X E R C I S E Renal System Physiology: Computer Simulation O B J E C T I V E S 1. To define the following terms: glomerulus, glomerular capsule, renal corpuscle, renal tubule, nephron, proximal convoluted
41B E X E R C I S E Renal System Physiology: Computer Simulation O B J E C T I V E S 1. To define the following terms: glomerulus, glomerular capsule, renal corpuscle, renal tubule, nephron, proximal convoluted
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Stages of Chronic Kidney Disease (CKD)
 Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Management of Nephrotic Syndrome
 Management of Nephrotic Syndrome 1. Introduction Incidence 2-4/100,000. Boys > girls 3:2; age of onset 2-6 years 80% of cases in children is due to minimal change (MCD) of which 80% will respond to steroid
Management of Nephrotic Syndrome 1. Introduction Incidence 2-4/100,000. Boys > girls 3:2; age of onset 2-6 years 80% of cases in children is due to minimal change (MCD) of which 80% will respond to steroid
Proteinuria. Louisiana State University
 Proteinuria W S A V A W C P, 2005 David F. Senior Louisiana State University The normal glomerulus is a highly selective barrier for filtration based on size (and on charge in the case of larger molecules).
Proteinuria W S A V A W C P, 2005 David F. Senior Louisiana State University The normal glomerulus is a highly selective barrier for filtration based on size (and on charge in the case of larger molecules).
COMPLETE INHIBITION OF RENAL RESERVE IN CHRONIC RENAL FAILURE BY A COMBINATION OF ACEI AND ARB
 COMPLETE INHIBITION OF RENAL RESERVE IN CHRONIC RENAL FAILURE BY A COMBINATION OF ACEI AND ARB CG Musso ¹, J Reynaldi¹, N Imperiali ¹, L Algranati ¹, DG Oreopoulos ² Nephrology Department Hospital Italiano
COMPLETE INHIBITION OF RENAL RESERVE IN CHRONIC RENAL FAILURE BY A COMBINATION OF ACEI AND ARB CG Musso ¹, J Reynaldi¹, N Imperiali ¹, L Algranati ¹, DG Oreopoulos ² Nephrology Department Hospital Italiano
General introduction of nephrology. Xiaoqiang Ding M.D., Ph.D. Department of nephrology Zhongshan Hospital, Fudan University
 General introduction of nephrology Xiaoqiang Ding M.D., Ph.D. Department of nephrology Zhongshan Hospital, Fudan University Terminology Kidney,renal Nephrology Scope of nephrology Kidney diseases and
General introduction of nephrology Xiaoqiang Ding M.D., Ph.D. Department of nephrology Zhongshan Hospital, Fudan University Terminology Kidney,renal Nephrology Scope of nephrology Kidney diseases and
A clinical syndrome, composed mainly of:
 Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome.
 Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY
 RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
MAJOR FUNCTIONS OF THE KIDNEY
 MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
1. remove: waste products: urea, creatinine, and uric acid foreign chemicals: drugs, water soluble vitamins, and food additives, etc.
 Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
Physiology of Excretory Systems
 Physiology of Excretory Systems Fig 12-2 (a) Urea is formed by the ornithine-urea cycle in most vertebrates. Because ATP is required for the first step, nitrogen excretion in ureotelic animals is more
Physiology of Excretory Systems Fig 12-2 (a) Urea is formed by the ornithine-urea cycle in most vertebrates. Because ATP is required for the first step, nitrogen excretion in ureotelic animals is more
HYPERTENSION IN CKD. LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL
 HYPERTENSION IN CKD LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL Stages in Progression of Chronic Kidney Disease and Therapeutic Strategies Complications Normal Increased risk Damage GFR
HYPERTENSION IN CKD LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL Stages in Progression of Chronic Kidney Disease and Therapeutic Strategies Complications Normal Increased risk Damage GFR
I. Metabolic Wastes Metabolic Waste:
 I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
Renal Blood flow; Renal Clearance. Dr Sitelbanat
 Renal Blood flow; Renal Clearance Dr Sitelbanat Objectives At the end of this lecture student should be able to describe: Renal blood flow Autoregulation of GFR and RBF Regulation of GFR The Calcuation
Renal Blood flow; Renal Clearance Dr Sitelbanat Objectives At the end of this lecture student should be able to describe: Renal blood flow Autoregulation of GFR and RBF Regulation of GFR The Calcuation
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
