A Non-calorie-restricted Low-carbohydrate Diet is Effective as an Alternative Therapy for Patients with Type 2 Diabetes
|
|
|
- Kimberly McDonald
- 6 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE A Non-calorie-restricted Low-carbohydrate Diet is Effective as an Alternative Therapy for Patients with Type 2 Diabetes Yoshifumi Yamada, Junichi Uchida, Hisa Izumi, Yoko Tsukamoto, Gaku Inoue, Yuichi Watanabe, Junichiro Irie and Satoru Yamada Abstract Objective Although caloric restriction is a widely used intervention to reduce body weight and insulin resistance, many patients are unable to comply with such dietary therapy for long periods. The clinical effectiveness of low-carbohydrate diets was recently described in a position statement of Diabetes UK and a scientific review conducted by the American Diabetes Association. However, randomised trials of dietary interventions in Japanese patients with type 2 diabetes are scarce. Therefore, the aim of this study was to examine the effects of a non-calorie-restricted, low-carbohydrate diet in Japanese patients unable to adhere to a calorie-restricted diet. Methods The enrolled patients were randomly allocated to receive a conventional calorie-restricted diet or low-carbohydrate diet. The patients received consultations every two months from a registered dietician for six months. We compared the effects of the two dietary interventions on glycaemic control and metabolic profiles. Results The HbA1c levels decreased significantly from baseline to six months in the low-carbohydrate diet group (baseline 7.6±0.4%, six months 7.0±0.7%, p=0.03) but not in the calorie-restricted group (baseline 7.7±0.6%, six months 7.5±1.0%, ), (between-group comparison, p=0.03). The patients in the former group also experienced improvements in their triglyceride levels, without experiencing any major adverse effects or a decline in the quality of life. Conclusion Our findings suggest that a low-carbohydrate diet is effective in lowering the HbA1c and triglyceride levels in patients with type 2 diabetes who are unable to adhere to a calorie-restricted diet. Key words: calorie restriction, low-carbohydrate diet, type 2 diabetes (Intern Med 53: 13-19, 2014) () Introduction Type 2 diabetes is a worldwide pandemic that is accompanied by an obesity pandemic (1, 2). Visceral fat accumulation is a significant risk factor for the onset of metabolic syndrome and diabetes (3), and weight reduction is a recommended target for the first-line treatment and prevention of diabetes (4). The American Diabetes Association (ADA) recommends that monitoring carbohydrate intake should be a component of diabetes therapy (4). Moreover, since 2008, the ADA has also recognised that low-carbohydrate diets, as well as calorie-restricted diets, are effective interventions for weight reduction (5). Notably, this recommendation differs from that reported in 2007, when the ADA did not recommend a carbohydrate intake of <130 g/day (6). Furthermore, Diabetes UK recently proposed that low-carbohydrate diets may also provide an effective treatment option (7), and the ADA reported the effectiveness of such diets for blood glucose and lipid management in a systematic review (8). In contrast, the Japan Diabetes Society (JDS) currently recommends calorie restriction (25-35 kcal/kg of ideal body weight) for blood glucose management (9). Although calorie restriction has been confirmed to be effective for treating metabolic disorders, aging, carcinogenesis and dementia in Diabetes Center, Kitasato Institute Hospital, Japan Received for publication April 25, 2013; Accepted for publication July 25, 2013 Correspondence to Dr. Satoru Yamada, yamada-s@insti.kitasato-u.ac.jp 13
2 Rhesus monkeys (10), it may be difficult to adhere to such a diet for long periods. Therefore, we examined the effectiveness of a noncalorie-restricted, low-carbohydrate diet for blood glucose and body weight management in Japanese patients with type 2 diabetes who were unable to adhere to a calorie-restricted diet. Materials and Methods Study design and subjects This study was a single centre, 6-month, comparative, two-arm, randomised, open-label trial performed between April 1, 2011 and January 31, We recruited patients with type 2 diabetes who were being treated in our outpatient clinic who had received guidance regarding calorie restriction at least once and whose HbA1c level at enrolment was %, suggesting that their blood glucose level was not adequately controlled. Patients with proteinuria of >1.0 g/day, a serum creatinine level of >132 μmol/l (men) or 106 μmol/l (women), an aspartate aminotransferase (AST) or alanine aminotransferase (ALT) level of >3 times the upper limit of normal, a history of myocardial infarction or stroke within six months before study entry or an absolute change in the HbA1c of >1.0% within six months before study entry were excluded from this study. We avoided recruiting any patients with ketosis because ketoacidosis, which is a life-threatening complication, are reported during ketogenic low-carbohydrate diet (11, 12). The enrolled patients were randomly allocated to receive either a non-calorie-restricted, low-carbohydrate diet (hereafter low-carbohydrate diet) or calorie-restricted diet using a permuted randomised block of four patients per block. The patients and investigators were not masked to group assignment. This study was undertaken in accordance with the Declaration of Helsinki and the Guidelines for Good Clinical Practice and was approved by our institutional review board (study ID ). Written informed consent was obtained from all enrolled patients. Procedures The enrolled patients were followed up at our outpatient clinic every two months. They received diet instructions at every medical consultation. During the study period, we did not change the medications, unless hypoglycaemia occurred. The HbA1c level, laboratory blood tests, body weight and incidence of hypoglycaemic episodes since the previous visit were recorded every two months. Dietary intake over the three days prior to each visit was also recorded. The primary objective was to compare the reductions in the HbA1c level and body weight from baseline to the end of the 6-month treatment period between the two groups. The secondary efficacy variables included the lipid levels (total cholesterol (TC), triglycerides (TGs), high-density lipoprotein cholesterol (HDL-C) and low-density lipoprotein cholesterol (LDL-C) calculated using the Friedewald equation), blood pressure, markers of atherosclerosis (pulse-wave velocity (PWV), ankle-brachial pressure index (ABI) and toe-brachial pressure index (TBI)), the renal function (urinary nitrogen (UN), creatinine (Cr) and estimated glomerular filtration rate (egfr), albumin-to-creatinine ratio (ACR)), the urinary albumin (UA) level and the levels of liver enzymes (AST, ALT and γ-glutamyl transpeptidase (γgtp)). To evaluate the effects of the diets on the quality of life, the patients completed the Diabetes Treatment Satisfaction Questionnaire (DTSQ) (13) and the Problem Areas In Diabetes (PAID) scale (14) at enrolment and at the end of the study. The safety variables included adverse events reported by the patients or noted by the investigators, standard hematologic and blood chemistry tests, body weight and hypoglycaemia. Hypoglycaemia was defined as an event with typical symptoms (e.g., sweating, palpitations and feelings of hunger) with or without confirmation by a plasma glucose level of <70 mg/dl. Meal instruction Patients who were assigned to the calorie-restricted diet received face-to-face guidance on how to calculate their calorie intake by classifying macronutrients. The target calorie intake was defined based on the Japan Diabetes Society recommendations, as follows: total calorie intake (kcal) = ideal body weight (kg; =height (m) height (m) 22) 25. The target intake of specific macronutrients was as follows: carbohydrates=50-60%, protein= g/kg (<20%) and fat=<25% (9). For the low-carbohydrate diet, we set the total carbohydrate intake to be <130 g/day, as proposed by Accurso et al. (15). To prevent ketosis (11, 12, 16), we set the lower limit of carbohydrate intake to 70 g/day. To prevent postprandial hyperglycaemia, the target carbohydrate content in each meal was g, and the subjects were allowedtoconsumesweetscontaining5gofcarbohydrates twice daily, thus resulting in a total carbohydrate intake of g/day. To avoid any possible influence of the experience and consulting skills of the dieticians in this study, four registered dieticians instructed the patients in both groups. Sample size calculation We estimated that the change in the HbA1c level over six months would be 0.0±0.5% in the calorie-restricted group and 0.7±0.5% in the low-carbohydrate group. We needed 22 patients, with α=0.05 and power=0.90. Therefore, we decided to enrol 24 patients in this study. Statistical analysis The results are presented as the mean±standard deviation. The Mann-Whitney U test was used for within-group and between-group comparisons. The Spearman s rank correlation test was used to assess the correlations between the carbohydrate or calorie intake and outcomes. Values of p<0.05 were considered to indicate a statistically significant differ- 14
3 Assessed for eligibility (n=24) Table 1. Baseline Characteristics of the Patients Allocated to Each Diet Allocated to : low-carbohydrate diet (n=12) Received intervention (n=12) Randomised (n=24) Figure 1. Flow diagram of the patients. ence. Allocated to : calorie-restricted diet (n=12) Received intervention (n=12) Completed (n=12, 100%) Completed (n=12, 100%) Study population Results The methodology of recruitment and screening is summarized in Fig. 1. A total of 24 patients with type 2 diabetes (mean age, 63.3±11.7 years; 50% women) who were being followed up at our outpatient clinic were enrolled and randomly allocated to receive either a low-carbohydrate diet or calorie-restricted diet. The general characteristics of the enrolled patients in each group are shown in Table 1. There were no statistically significant differences in any of the parameters between the two groups. The low-carbohydrate diet improved the blood glucose levels and lipid levels (Table 2) Six months after starting the diet, the HbA1c levels were significantly lower than those observed at baseline in the low-carbohydrate group (baseline 7.6±0.4%, six months 7.0±0.7%, p=0.03), whereas there were no changes in the HbA1c levels in the calorie-restricted group (baseline 7.7± 0.6%, six months 7.5±1.0%, not significant ()) (Fig. 2a). The low-carbohydrate diet significantly improved the HbA1c levels in comparison with the calorie-restricted diet (p= 0.03). The fasting plasma glucose levels were similar between baseline and at six months in both groups. Body weight, BMI and blood pressure did not change significantly in either group. In terms of the lipid levels, the TG levels significantly decreased in the low-carbohydrate group (baseline 141.7±76.2 mg/dl, six months 83.5±40.6 mg/dl, p=0.02), whereas no Low-carbohydrate diet Calorie-restricted diet Age (years) 63.3 ± ± 10.2 Sex (male/female) 7/5 5/7 Duration of diabetes (years) 8.9 ± ± 4.8 BMI (kg/m 2 ) 24.5 ± ± 3.0 BW (kg) 67.0 ± ± 7.7 HbA1c (NGSP) (%) 7.6 ± ± 0.6 LDL-C (mg/dl) 99.8 ± ± 20.5 TG (mg/dl) ± ± 86.4 HDL-C (mg/dl) 62.8 ± ± 19.1 SBP (mmhg) ± ± 10.7 DBP (mmhg) 72.6 ± ± 10.6 DTSQ total score (except items 2 and 3) 24.0 ± ± 3.3 PAID score 42.1 ± ± 12.6 Glucose-lowering drug no. (%) Insulin 3 (25.0) 4 (33.3) Metformin 5 (41.7) 1 (8.3) Sulfonylurea 5 (41.7) 8 (66.7) Glinide 1 (8.3) 0 (0.0) Thiazolidinedione 4 (33.3) 6 (50.0) -Glucosidase inhibitor 2 (16.7) 0 (0.0) DPP-4 inhibitor 2 (16.7) 3 (25.0) GLP-1 0 (0.0) 0 (0.0) None 0 (0.0) 0 (0.0) History of major microvascular disease Retinopathy None SDR 0 2 PPDR 1 0 PDR 1 0 Nephropathy Stage Stage Stage 3A 1 1 Stage 3B, 4, Values are means ± standard deviation. There were no statistically significant differences between the two groups for any parameter. BMI: body mass index, BW: body weight, HbA1c: haemoglobin A1c, NGSP: National Glycohemoglobin Standardization Program, LDL-C: low-density lipoprotein cholesterol, TG: triglyceride, HDL-C: high-density lipoprotein cholesterol, SBP: systolic blood pressure, DBP: diastolic blood pressure, DTSQ: Diabetes Treatment Satisfaction Questionnaire, PAID: Problem Areas In Diabetes scale, DPP: dipeptidyl peptidase, GLP: glucagon-like peptide, SDR: simple diabetic retinopathy, PPDR: pre proliferative diabetic retinopathy, PDR: proliferative diabetic retinopathy changes in the TG levels occurred in the calorie-restricted group (baseline 155.2±86.4 mg/dl, six months 148.4±90.7 mg/dl, ) (Fig. 2b). However, the difference between the two groups was not statistically significant (p=0.08). The other markers of lipid profiles, the LDL-C levels and the HDL-C levels, were not altered in either group. Neither diet significantly affected markers of atherosclerosis, such as ABI, TBI and PWV. Although we were concerned that excess protein intake may cause deterioration of the renal function in the lowcarbohydrate group, we found no changes in the markers of the renal function (i.e., UN, Cr, egfr and ACR) during the 6-month study in either group. A marker of the liver function, the ALT level, tended to improve in the lowcarbohydrate group, likely due to the decrease in liver fat 15
4 Table 2. Efficacy Outcomes Variable Low-carbohydrate diet Calorie-restricted diet p value* Baseline 6 months p value Baseline 6 months p value HbA1c NGSP 7.6 ± ± ± ± 1.0 (%) (0.45) 0.03 FPG (mg/dl) 138 ± ± ± ± 26 (0.40) (0.42) (0.33) BW (kg) 67.0 ± ± ± 68.1 ± 7.7 (0.62) 7.0 (0.56) (0.80) BMI (kg/m 2 ) 24.5 ± ± ± 27.0 ± 3.0 (0.39) 2.2 (0.42) (0.86) LDL-C (mg/dl) 99.8 ± ± ± ± TG (mg/dl) ± ± ± ± HDL-C (mg/dl) 62.8 ± ± ± 59.8 ± 19.1 (0.44) 13.9 SBP (mmhg) ± ± ± ± DBP (mmhg) 72.6 ± ± ± 74.8 ± 10.1 (0.11) 10.1 PWV (cm/sec) 1,723.0 ± 1,788.8 ± 1,616.0 ± 1,626.3 ± (0.60) ABI ± ± ± ± (0.24) TBI ± ± ± ± (0.54) UN (mg/dl) 15.3 ± ± ± 13.1 ± 3.4 (0.47) 5.8 egfr 65.0 ± (ml/min/1.73m ± ± ± 13.2 ) (0.71) 12.6 ACR (mg/gcr) ± 96.8 ± ± 53.0 ± UA (mg/dl) 5.6 ± ± ± ± 1.4 AST (U/L) 26.9 ± ± ± 31.7 ± 17.1 (0.36) 27.0 ALT (U/L) 28.6 ± ± ± ± 17.5 GTP (U/L) 38.5 ± ± ± 35.8 ± 25.4 (0.53) 33.7 DTSQ total score 24.0 ± ± ± 21.6 ± 3.3 (0.23) 4.5 DTSQ item 2: 3.67 ± 3.50 ± ± ± 0.94 High BS (0.13) 1.37 DTSQ item 3: 1.75 ± 1.17 ± ± ± 1.53 Low BS 1.14 PAID score 42.1 ± ± ± 57.8 ± 12.6 (0.37) 11.9 (0.58) (0.82) (0.42) (0.91) (0.44) (0.80) (0.33) (0.89) 0.07 (0.98) (0.98) (0.49) 0.08 (0.13) (0.54) (0.30) (0.36) (0.91) (0.39) (0.21) (0.29) (0.11) (0.18) (0.21) (0.31) (0.64) *For between-group comparisons; for within-group comparisons. Values are means ± standard deviation. HbA1c: haemoglobin A1c, : not significant, FBG: fasting blood glucose, BW: body weight, BMI: body mass index, NGSP: National Glycohemoglobin Standardization Program, LDL-C: low-density lipoprotein cholesterol, TG: triglyceride, HDL-C: high-density lipoprotein cholesterol, SBP: systolic blood pressure, DBP: diastolic blood pressure, PWV: pulse-wave velocity, ABI: ankle brachial pressure index, TBI: toe brachial pressure index, UN: urinary nitrogen, egfr: estimated glomerular filtration index, ACR: albumin-to-creatinine ratio, UA: urinary albumin, AST: aspartate aminotransferase, ALT: alanine aminotransferase, GTP: -glutamyl transpeptidase, DTSQ: Diabetes Treatment Satisfaction Questionnaire, BS: blood sugar, PAID: Problem Areas In Diabetes scale content associated with the reduction in body weight. However, we did not assess the liver fat content using ultrasound or magnetic resonance spectrometry in this study. Concerning the quality of life, the DTSQ score and the PAID score did not change in either group. Taken together, these results indicate that the lowcarbohydrate diet achieved greater improvements in the blood glucose and TG levels than the calorie-restricted diet. Particularly, the low-carbohydrate diet significantly improved the HbA1c levels in comparison with the calorierestricted diet. Three patients treated with a sulfonylurea or insulin in the low-carbohydrate group experienced symptomatic hypoglycaemia, although the events did not recur after adjusting the medications. None of the patients developed ketonuria during the study. 16
5 Figure 2. Changes in the HbA1c (a) and triglyceride (b) levels during the 6-month intervention. Solid line: caloric restriction diet, dotted line: low-carbohydrate diet Table 3. Nutrition Intake at 6 Months Low-carbohydrate diet Calorie-restricted diet p value* Intake Energy Energy Intake ratio (%) ratio (%) All patients Calorie intake (kcal) 1,634 ± ,610 ± (0.84) Males Calorie intake (kcal) 1,891 ± 400 1,684 ± 526 (0.42) Calorie intake/ibw 29.9 ± ± 8.5 (0.68) Females Calorie intake (kcal) 1,274± 507 1,557 ± 286 (0.22) Calorie intake/ibw 24.1± ± 5.2 (0.17) Intake of specific nutrients Protein (g) ± ± ± ± Protein/BW ± ± Fat (g) 82.1 ± ± ± ± Carbohydrate (g) ± ± ± ± Salt (g) 10.2 ± ± 2.4 (0.30) *For between-group comparisons. Values are means ± standard deviation. : not significant, IBW: ideal body weight, BW: body weight Nutrient intake at six months Although we did not prescribe calorie restriction to the patients assigned to the low-carbohydrate group, the calorie intake at six months was actually similar in both groups (Table 3). Stratified by sex, the calorie intake in the lowcarbohydrate group tended to be higher in men and lower in women compared with that observed in the calorie-restricted group. The relative nutrient intake of carbohydrates, protein and fat was 29.8±12.5%, 25.3±7.3% and 45.4±8.9% in the low-carbohydrate group, compared with 51.0±4.6%, 16.6± 2.8% and 32.3±5.2%, respectively, in the calorie-restricted group. The carbohydrate intake was significantly lower in the low-carbohydrate group than in the calorie-restricted group. The mean carbohydrate intake in the lowcarbohydrate group was <130 g/day, suggesting that most patients were able to adhere to the meal instructions. Correlations between carbohydrate or calorie intake and outcomes We next performed correlation analyses in 10 patients with nutrient intake data both at baseline and at the end of the study (five patients in each group). In these patients, we found that the change in body weight was significantly correlated with the change in carbohydrate intake (r=0.764, p= ) and the change in calorie intake (r=0.769, p= ). The change in the HbA1c level was significantly correlated with the change in carbohydrate intake (r=0.670, p=0.0321) but not with the change in calorie intake (r= 0.439, ). Discussion In this randomised study, we examined whether a noncalorie-restricted, low-carbohydrate diet is effective and safe in Japanese patients with type 2 diabetes and inadequate glycaemic control while on a calorie-restricted diet. Significant improvements in the HbA1c level were observed in the low-carbohydrate group but not in the calorie-restricted group. Overall, these findings are compatible with the recommendations of the ADA (4, 5, 8) and Diabetes UK (7). We also found improvements in the TG levels in the low- 17
6 carbohydrate group. Two previous meta-analyses, which included five trials (17) and 13 trials (18), respectively, showed worsening of the TC and LDL-C levels and improvements in the TG and HDL-C levels with a lowcarbohydrate diet. However, another meta-analysis of 22 trialsshowednodeteriorationinthetcorldl-clevelsand significant improvements in the TG and HDL-C levels with a low-carbohydrate diet (19). Consistent with that report, we found improvements in the TG levels without deterioration in the TC or LDL-C levels. Therefore, a low-carbohydrate diet appears to have beneficial effects on lipid profiles as well as glycaemic control. The ADA recommends monitoring the renal function and protein intake, particularly in patients with nephropathy, during low-carbohydrate dietary interventions in addition to monitoring lipid profiles (4, 5). Although the subjects in the low-carbohydrate group consumed less carbohydrates, more protein and more fat than those in the calorie-restricted group, the renal function did not deteriorate in the former group. The protein intake in the low-carbohydrate group in this study was 1.6±0.6 g/kg. Although the Japanese Reference Diet Intake report 2010 recommended an upper limit of protein intake of 2.0 g/kg (20) based on data from critically ill patients, critically ill patients should be allowed to receive undernutrition (21) and the Dietary Reference Intake in the US has no upper limit for protein intake (22). Although a previous report claimed that atherosclerosis may be caused by a low-carbohydrate diet (23), we did not observe cerebrovascular end points due to the short observation period. There was no deterioration in the levels of markers of atherosclerosis (i.e., ABI, TBI and PWV) in the low-carbohydrate group. It is necessary to evaluate the longterm safety of low-carbohydrate diets for atherosclerosis carefully in the future. Although we did not limit calorie intake in the lowcarbohydrate diet group, the calorie intake at six months after the intervention was almost equal in both groups. In the low-carbohydrate diet group, the patients ate protein and fat, such as meat or fish, in substitution of carbohydrates. As a result, the quantity of the meal increased and the patients may therefore more easily feel full. In addition, lightly seasoned staple foods (such as rice, bread, noodles and so on), which are rich in carbohydrates, may promote overeating of strongly seasoned side dishes (such as meat, fish and so on), and it may be difficult to frequently eat only side dishes. On the other hand, because all enrolled patients had previously received guidance on calorie restriction at least once, we cannot deny the possibility that the patients allocated to the low-carbohydrate diet group limited not only the carbohydrate volume, but also the calorie intake under the influence of former meal instruction. There are several limitations to this study that should be discussed. First, the number of subjects enrolled was too small to detect significant differences in the between-group and within-group comparisons. Santos et al. reviewed 23 reports, consisting of 1,141 patients in total, concerning the effects of low-carbohydrate diets and reported that lowcarbohydrate diets are clearly associated with significant decreases in body weight, BMI, abdominal circumference, systolic blood pressure, diastolic blood pressure, plasma TG, fasting plasma glucose, glycated haemoglobin, plasma insulin and plasma CRP as well as increases in HDL-C (24). We did not observe any significant improvements in body weight, BMI, blood pressure or HDL-C in this study; however, increasing the number of subjects may prove the significant effectiveness of low-carbohydrate diets in improving these parameters. Second, this was a 6-month study. Several clinical trials of low-carbohydrate diets have shown small or moderate rebounds in clinical parameters between six months and 12 months after starting the intervention (25, 26). Therefore, the improvements in the HbA1c levels and body weight observed at six months in our study may be attenuated over a longer observation period. In conclusion, we found that a non-calorie-restricted, lowcarbohydrate diet is effective in lowering the HbA1c and TG levels and is safe as an alternative therapy for patients with type 2 diabetes. Because the number of subjects enrolled was small and the study duration was short, longer multicentre studies with a larger sample size are needed to confirm our findings. The authors state that they have no Conflict of Interest (COI). References 1. The diabetes pandemic. Lancet 378: 99, Ramachandran A, Ma RC, Sneharatha C. Diabetes in Asia. Lancet 375: , Alberti KG, Zimmet P, Shaw J; IDF Epidemiology Task Force Consensus Group. The metabolic syndrome: a new worldwide definition. Lancet 366: , American Diabetes Association. Standards of medical care in diabetes Diabetes Care 35: S11-S63, American Diabetes Association. Nutrition recommendations and interventions for diabetes. Diabetes Care 31: S61-S78, American Diabetes Association. Nutrition recommendations and interventions for diabetes. Diabetes Care 30: S48-S65, Dyson PA, Kelly T, Deakin A, et al. Diabetes UK evidence-based nutrition guidelines for the prevention and management of diabetes. Diabet Med 28: , Wheeler ML, Dunbar SA, Jaacks LM, et al. Macronutrients, food groups, and eating patterns in the management of diabetes: a systematic review of the literature, Diabetes Care 35: , Japan Diabetes Society. Diet therapy. In: Treatment Guide for Diabetes Bunkodo, Tokyo, 2012: (in Japanese). 10. Colman RJ, Anderson RM, Johnson SC, et al. Caloric restriction delays disease onset and mortality in rhesus monkeys. Science 325: , Chen TY, Smith W, Rosenstock JL, Lessnau KD. A lifethreatening complication of Atkins diet. Lancet 367: 958, Shah P, Isley WL. Ketoacidosis during a low-carbohydrate diet. N Engl J Med 354: 97-98, Bradley C. Diabetes Treatment Satisfaction Questionnaire. Change version for use alongside status version provides appropriate solution where ceiling effects occur. Diabetes Care 22: , Welch GW, Jacobson AM, Polonsky WH. The Problem Areas in 18
7 Diabetes Scale. An evaluation of its clinical utility. Diabetes Care 20: , Accurso A, Bernstein RK, Dahlgvist A, et al. Dietary carbohydrate restriction in type 2 diabetes mellitus and metabolic syndrome: time for a critical appraisal. Nutr Metab (Lond) 5: 9, Westman EC, Feinman RD, Mavropoulos JC, et al. Lowcarbohydrate nutrition and metabolism. Am J Clin Nutr 86: , Nordmann AJ, Nordmann A, Briel M, et al. Effects of lowcarbohydrate vs low-fat diets on weight loss and cardiovascular risk factors. Arch Intern Med 166: , Hession M, Rolland C, Kulkarni U, Wise A, Broom J. Systematic review of randomized controlled trials of low-carbohydrate vs. low-fat/low-calorie diets in the management of obesity and its comorbidities. Obes Rev 10: 36-50, Kodama S, Saito K, Tanaka S, et al. Influence of fat and carbohydrate proportions on the metabolic profile in patients with type 2 diabetes: a meta-analysis. Diabetes Care 32: , Ministry of Health, Labour, and Welfare, Japan. Protein, in Dietary Reference Intakes for Japanese Daiichi Shuppan Publishing Co., Tokyo, 2010: (in Japanese). 21. Casaer MP, Mesotten D, Hermans G, et al. Early versus late parenteral nutrition in critically ill adults. N Engl J Med 365: , Institute of Medicine of the National Academies. Protein and Amino Acids, in Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids. The National Academies Press, Washington DC, 2005: Smith SR. A look at the low-carbohydrate diet. N Engl J Med 361: , Santos FL, Esteves SS, da Costa Pereira A, Yancy WS Jr, Nunes JP. Systematic review and meta-analysis of clinical trials of the effects of low carbohydrate diets on cardiovascular risk factors. Obes Rev 13: , Shai I, Schwarzfuchs D, Henkin Y, et al. Weight loss with a lowcarbohydrate, Mediterranean, or low-fat diet. N Engl J Med 359: , Gardner CD, Kiazand A, Alhassan S, et al. Comparison of the Atkins, Zone, Ornish, and LEARN diets for change in weight and related risk factors among overweight premenopausal women: the A TO Z Weight Loss Study: a randomized trial. JAMA 297: , The Japanese Society of Internal Medicine 19
SCIENTIFIC STUDY REPORT
 PAGE 1 18-NOV-2016 SCIENTIFIC STUDY REPORT Study Title: Real-Life Effectiveness and Care Patterns of Diabetes Management The RECAP-DM Study 1 EXECUTIVE SUMMARY Introduction: Despite the well-established
PAGE 1 18-NOV-2016 SCIENTIFIC STUDY REPORT Study Title: Real-Life Effectiveness and Care Patterns of Diabetes Management The RECAP-DM Study 1 EXECUTIVE SUMMARY Introduction: Despite the well-established
Non-insulin treatment in Type 1 DM Sang Yong Kim
 Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Nutritional Recommendations for the Diabetes Managements
 In the name of God Nutritional for the Diabetes Managements Zohreh Mazloom. PhD Shiraz University of Medical Sciences School of Nutrition and Food Sciences Department of Clinical Nutrition OVERVIEW Healthful
In the name of God Nutritional for the Diabetes Managements Zohreh Mazloom. PhD Shiraz University of Medical Sciences School of Nutrition and Food Sciences Department of Clinical Nutrition OVERVIEW Healthful
American Diabetes Association: Standards of Medical Care in Diabetes 2015
 American Diabetes Association: Standards of Medical Care in Diabetes 2015 Synopsis of ADA standards relevant to the 11 th Scope of Work under Task B.2 ASSESSMENT OF GLYCEMIC CONTROL Recommendations: Perform
American Diabetes Association: Standards of Medical Care in Diabetes 2015 Synopsis of ADA standards relevant to the 11 th Scope of Work under Task B.2 ASSESSMENT OF GLYCEMIC CONTROL Recommendations: Perform
A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes
 A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Hypotheses: Among individuals with type 2 diabetes, the risks of major microvascular
A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Hypotheses: Among individuals with type 2 diabetes, the risks of major microvascular
Case study: Lean adult with no complications, newly diagnosed with type 2 diabetes
 Case study: Lean adult with no complications, newly diagnosed with type 2 diabetes Authored by Clifford Bailey and James LaSalle on behalf of the Global Partnership for Effective Diabetes Management. The
Case study: Lean adult with no complications, newly diagnosed with type 2 diabetes Authored by Clifford Bailey and James LaSalle on behalf of the Global Partnership for Effective Diabetes Management. The
Obesity may attenuate the HbA1c-lowering effect of sitagliptin in Japanese type 2 diabetic patients
 ORIGINAL ARTICLE Obesity may attenuate the HbA1c-lowering effect of sitagliptin in Japanese type 2 diabetic patients Yukihiro Bando, Hideo Kanehara, Keiko Aoki, Azusa Hisada, Daisyu Toya, Nobuyoshi Tanaka
ORIGINAL ARTICLE Obesity may attenuate the HbA1c-lowering effect of sitagliptin in Japanese type 2 diabetic patients Yukihiro Bando, Hideo Kanehara, Keiko Aoki, Azusa Hisada, Daisyu Toya, Nobuyoshi Tanaka
Establishment of Efficacy of Intervention in those with Metabolic Syndrome. Dr Wendy Russell - ILSI Europe Expert Group
 Establishment of Efficacy of Intervention in those with Metabolic Syndrome Dr Wendy Russell - ILSI Europe Expert Group Conflict of interest regarding this presentation: I have no conflict of interest to
Establishment of Efficacy of Intervention in those with Metabolic Syndrome Dr Wendy Russell - ILSI Europe Expert Group Conflict of interest regarding this presentation: I have no conflict of interest to
A Randomized Controlled Trial of a Mini Low-Carbohydrate Diet and an Energy-Controlled Diet Among Japanese Patients With Type 2 Diabetes
 Original Article J Clin Med Res. 2018;10(3):182-188 A Randomized Controlled Trial of a Mini Low-Carbohydrate Diet and an Energy-Controlled Diet Among Japanese Patients With Type 2 Diabetes Masayo Kimura
Original Article J Clin Med Res. 2018;10(3):182-188 A Randomized Controlled Trial of a Mini Low-Carbohydrate Diet and an Energy-Controlled Diet Among Japanese Patients With Type 2 Diabetes Masayo Kimura
Macronutrients and Dietary Patterns for Glucose Control
 제 20 회대한당뇨병학회춘계학술대회 Macronutrients and Dietary Patterns for Glucose Control 2017.5.13 서울대학교병원임정현 Conflict of interest disclosure None Committee of Scientific Affairs Contents Review of Nutrition Recommendation
제 20 회대한당뇨병학회춘계학술대회 Macronutrients and Dietary Patterns for Glucose Control 2017.5.13 서울대학교병원임정현 Conflict of interest disclosure None Committee of Scientific Affairs Contents Review of Nutrition Recommendation
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone
 Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
6.1. Feeding specifications for people with diabetes mellitus type 1
 6 Feeding 61 Feeding specifications for people with diabetes mellitus type 1 It is important that the food intake of people with DM1 is balanced, varied and that it meets the caloric needs, and takes into
6 Feeding 61 Feeding specifications for people with diabetes mellitus type 1 It is important that the food intake of people with DM1 is balanced, varied and that it meets the caloric needs, and takes into
egfr > 50 (n = 13,916)
 Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Application of the Diabetes Algorithm to a Patient
 Application of the Diabetes Algorithm to a Patient Apply knowledge gained from this activity to improve disease management and outcomes for patients with T2DM and obesity Note: The cases in this deck represent
Application of the Diabetes Algorithm to a Patient Apply knowledge gained from this activity to improve disease management and outcomes for patients with T2DM and obesity Note: The cases in this deck represent
Screening Results. Juniata College. Juniata College. Screening Results. October 11, October 12, 2016
 Juniata College Screening Results Juniata College Screening Results October 11, 2016 & October 12, 2016 JUNIATA COLLEGE The J.C. Blair Hospital CARES team screened 55 Juniata College employees on October
Juniata College Screening Results Juniata College Screening Results October 11, 2016 & October 12, 2016 JUNIATA COLLEGE The J.C. Blair Hospital CARES team screened 55 Juniata College employees on October
Hypertension with Comorbidities Treatment of Metabolic Risk Factors in Children and Adolescents
 Hypertension with Comorbidities Treatment of Metabolic Risk Factors in Children and Adolescents Stella Stabouli Ass. Professor Pediatrics 1 st Department of Pediatrics Hippocratio Hospital Evaluation of
Hypertension with Comorbidities Treatment of Metabolic Risk Factors in Children and Adolescents Stella Stabouli Ass. Professor Pediatrics 1 st Department of Pediatrics Hippocratio Hospital Evaluation of
ORIGINAL ARTICLE. Abstract
 ORIGINAL ARTICLE Association between Hemoglobin and Diabetes in Relation to the Triglycerides-to-High-Density Lipoprotein Cholesterol (TG-HDL) Ratio in Japanese Individuals: The Nagasaki Islands Study
ORIGINAL ARTICLE Association between Hemoglobin and Diabetes in Relation to the Triglycerides-to-High-Density Lipoprotein Cholesterol (TG-HDL) Ratio in Japanese Individuals: The Nagasaki Islands Study
Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic
 Supplementary Information The title of the manuscript Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic stroke Xin-Wei He 1, Wei-Ling Li 1, Cai Li
Supplementary Information The title of the manuscript Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic stroke Xin-Wei He 1, Wei-Ling Li 1, Cai Li
DIABETES AND LABORATORY TESTS. Author: Josephine Davis
 DIABETES AND LABORATORY TESTS Author: Josephine Davis LAB TESTS Think twice before you test. What is the reason for testing? Laboratory tests are generally requested in primary care for one of the following
DIABETES AND LABORATORY TESTS Author: Josephine Davis LAB TESTS Think twice before you test. What is the reason for testing? Laboratory tests are generally requested in primary care for one of the following
Personal Diabetes Passport
 Personal Diabetes Passport Contact information: Name: Physician: Diabetes Education Centre: Dietitian: Ophthalmologist: Chiropodist: Type of Diabetes: Type 1 (T1DM) Increased risk for diabetes Type 2(T2DM)
Personal Diabetes Passport Contact information: Name: Physician: Diabetes Education Centre: Dietitian: Ophthalmologist: Chiropodist: Type of Diabetes: Type 1 (T1DM) Increased risk for diabetes Type 2(T2DM)
year resident, Department of Medicine, B. J. Medical college, Ahmedabad.
 Clinical Study of Type 2 Diabetes Mellitus Patients with or without Cerebrovascular Feature and Its Correlation with Other Comorbidity / Diabetic Complication Vivek Sidhapura 1*, Bipin Amin 2, Amit Potulwar
Clinical Study of Type 2 Diabetes Mellitus Patients with or without Cerebrovascular Feature and Its Correlation with Other Comorbidity / Diabetic Complication Vivek Sidhapura 1*, Bipin Amin 2, Amit Potulwar
Supplementary Table 1. Criteria for selection of normal control individuals among healthy volunteers
 Supplementary Table 1. Criteria for selection of normal control individuals among healthy volunteers Medical parameters Cut-off values BMI (kg/m 2 ) 25.0 Waist (cm) (Men and Women) (Men) 85, (Women) 90
Supplementary Table 1. Criteria for selection of normal control individuals among healthy volunteers Medical parameters Cut-off values BMI (kg/m 2 ) 25.0 Waist (cm) (Men and Women) (Men) 85, (Women) 90
Obesity, Insulin Resistance, Metabolic Syndrome, and the Natural History of Type 2 Diabetes
 Obesity, Insulin Resistance, Metabolic Syndrome, and the Natural History of Type 2 Diabetes Genetics, environment, and lifestyle (obesity, inactivity, poor diet) Impaired fasting glucose Decreased β-cell
Obesity, Insulin Resistance, Metabolic Syndrome, and the Natural History of Type 2 Diabetes Genetics, environment, and lifestyle (obesity, inactivity, poor diet) Impaired fasting glucose Decreased β-cell
J-DOIT3 The Japan Diabetes Optimal Integrated Treatment Study for 3 Major Risk Factors of Cardiovascular Diseases
 J-DOIT3 The Japan Diabetes Optimal Integrated Treatment Study for 3 Major Risk Factors of Cardiovascular Diseases A randomized controlled study comparing intensive therapy and conventional therapy in the
J-DOIT3 The Japan Diabetes Optimal Integrated Treatment Study for 3 Major Risk Factors of Cardiovascular Diseases A randomized controlled study comparing intensive therapy and conventional therapy in the
Multiple Factors Should Be Considered When Setting a Glycemic Goal
 Multiple Facts Should Be Considered When Setting a Glycemic Goal Patient attitude and expected treatment effts Risks potentially associated with hypoglycemia, other adverse events Disease duration Me stringent
Multiple Facts Should Be Considered When Setting a Glycemic Goal Patient attitude and expected treatment effts Risks potentially associated with hypoglycemia, other adverse events Disease duration Me stringent
Metformin should be considered in all patients with type 2 diabetes unless contra-indicated
 November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
Policy Statement Low carbohydrate diets for the management of Type 2 Diabetes in adults
 Policy Statement Low carbohydrate diets for the management of Type 2 Diabetes in adults Summary The role and the amounts of carbohydrate in foods as part of the diet of people with type 2 diabetes is often
Policy Statement Low carbohydrate diets for the management of Type 2 Diabetes in adults Summary The role and the amounts of carbohydrate in foods as part of the diet of people with type 2 diabetes is often
The Many Faces of T2DM in Long-term Care Facilities
 The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
DOI: /jemds/2014/2044 ORIGINAL ARTICLE
 AN OBSERVATIONAL STUDY COMPARING SITAGLIPTIN TO METFORMIN AS A INITIAL MONOTHERAPY IN TYPE 2 DIABETES MELLITUS PATIENTS Mohd. Riyaz 1, Imran 2, Rinu Manuel 3, Nidhisha K. Joseph 4 HOW TO CITE THIS ARTICLE:
AN OBSERVATIONAL STUDY COMPARING SITAGLIPTIN TO METFORMIN AS A INITIAL MONOTHERAPY IN TYPE 2 DIABETES MELLITUS PATIENTS Mohd. Riyaz 1, Imran 2, Rinu Manuel 3, Nidhisha K. Joseph 4 HOW TO CITE THIS ARTICLE:
Objectives. Objectives. Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015
 Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015 Presentation downloaded from http://ce.unthsc.edu Objectives Understand that the obesity epidemic is also affecting children and adolescents
Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015 Presentation downloaded from http://ce.unthsc.edu Objectives Understand that the obesity epidemic is also affecting children and adolescents
Diabetes and Hypertension
 Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Investigators, study sites Multicenter, 35 US sites. Coordinating Investigator: Richard Bergenstal, MD
 STUDY SYNOPSIS Study number Title HMR1964A/3502 Apidra (insulin glulisine) administered in a fixed-bolus regimen vs. variable-bolus regimen based on carbohydrate counting in adult subjects with type 2
STUDY SYNOPSIS Study number Title HMR1964A/3502 Apidra (insulin glulisine) administered in a fixed-bolus regimen vs. variable-bolus regimen based on carbohydrate counting in adult subjects with type 2
TUE Physician Guidelines Medical Information to Support the Decisions of TUE Committees Diabetes Mellitus DIABETES MELLITUS
 DIABETES MELLITUS 1. Introduction Diabetes is a global epidemic with 415 million people affected worldwide equivalent to the total population of the USA, Canada and Mexico. In recognition of this, the
DIABETES MELLITUS 1. Introduction Diabetes is a global epidemic with 415 million people affected worldwide equivalent to the total population of the USA, Canada and Mexico. In recognition of this, the
ATHLETES & PRESCRIBING PHYSICIANS PLEASE READ
 ATHLETES & PRESCRIBING PHYSICIANS PLEASE READ USADA can grant a Therapeutic Use Exemption (TUE) in compliance with the World Anti- Doping Agency International Standard for TUEs. The TUE application process
ATHLETES & PRESCRIBING PHYSICIANS PLEASE READ USADA can grant a Therapeutic Use Exemption (TUE) in compliance with the World Anti- Doping Agency International Standard for TUEs. The TUE application process
Data Analysis Plan for assessing clinical efficacy and safety of ER niacin/laropiprant in the HPS2-THRIVE trial
 Data Analysis Plan for assessing clinical efficacy and safety of ER niacin/laropiprant in the HPS2-THRIVE trial 1 Background This Data Analysis Plan describes the strategy, rationale and statistical methods
Data Analysis Plan for assessing clinical efficacy and safety of ER niacin/laropiprant in the HPS2-THRIVE trial 1 Background This Data Analysis Plan describes the strategy, rationale and statistical methods
Objectives. Medical Nutrition Therapy (MNT) for Diabetes Evidence-based Recommendations. No financial disclosures
 Medical Nutrition Therapy (MNT) for Diabetes Evidence-based Recommendations Advances in Internal Medicine 2013 Sarah Kim, MD Assistant Clinical Professor, UCSF-SFGH No financial disclosures Objectives
Medical Nutrition Therapy (MNT) for Diabetes Evidence-based Recommendations Advances in Internal Medicine 2013 Sarah Kim, MD Assistant Clinical Professor, UCSF-SFGH No financial disclosures Objectives
Clinical Approach to Achieving Treatment Targets: Case Vignette Discussion
 Clinical Approach to Achieving Treatment Targets: Case Vignette Discussion Om P. Ganda, MD; Kirit Tolia, MD, FACE Postcardiac Follow-up in a 66-Year-Old Man Slide 1. Dr. Ganda: Now we will present a case
Clinical Approach to Achieving Treatment Targets: Case Vignette Discussion Om P. Ganda, MD; Kirit Tolia, MD, FACE Postcardiac Follow-up in a 66-Year-Old Man Slide 1. Dr. Ganda: Now we will present a case
Sponsor / Company: Sanofi Drug substance(s): Insulin Glargine (HOE901) Insulin Glulisine (HMR1964)
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Effects of Sodium-Glucose Cotransporter 2 Inhibitors on Metabolic Parameters in Patients With Type 2 Diabetes: A Chart-Based Analysis
 Elmer ress Original Article J Clin Med Res. 2016;8(3):237-243 Effects of Sodium-Glucose Cotransporter 2 Inhibitors on Metabolic Parameters in Patients With Type 2 Diabetes: A Chart-Based Analysis Hisayuki
Elmer ress Original Article J Clin Med Res. 2016;8(3):237-243 Effects of Sodium-Glucose Cotransporter 2 Inhibitors on Metabolic Parameters in Patients With Type 2 Diabetes: A Chart-Based Analysis Hisayuki
Clinical Study Factors Associated with the Decline of Kidney Function Differ among egfr Strata in Subjects with Type 2 Diabetes Mellitus
 International Endocrinology Volume 2012, Article ID 687867, 6 pages doi:10.1155/2012/687867 Clinical Study Factors Associated with the Decline of Kidney Function Differ among egfr Strata in Subjects with
International Endocrinology Volume 2012, Article ID 687867, 6 pages doi:10.1155/2012/687867 Clinical Study Factors Associated with the Decline of Kidney Function Differ among egfr Strata in Subjects with
Ketogenic Diets-good, bad, indifferent? Peter Clifton CSIRO Human Nutrition
 Ketogenic Diets-good, bad, indifferent? Peter Clifton CSIRO Human Nutrition Presenter Disclosure Information
Ketogenic Diets-good, bad, indifferent? Peter Clifton CSIRO Human Nutrition Presenter Disclosure Information
Changes and clinical significance of serum vaspin levels in patients with type 2 diabetes
 Changes and clinical significance of serum vaspin levels in patients with type 2 diabetes L. Yang*, S.J. Chen*, G.Y. Yuan, D. Wang and J.J. Chen Department of Endocrinology, Affiliated Hospital of Jiangsu
Changes and clinical significance of serum vaspin levels in patients with type 2 diabetes L. Yang*, S.J. Chen*, G.Y. Yuan, D. Wang and J.J. Chen Department of Endocrinology, Affiliated Hospital of Jiangsu
SMJ Singapore Medical Journal
 SMJ Singapore Medical Journal ONLINE FIRST PUBLICATION Online first papers have undergone full scientific review and copyediting, but have not been typeset or proofread. To cite this article, use the DOIs
SMJ Singapore Medical Journal ONLINE FIRST PUBLICATION Online first papers have undergone full scientific review and copyediting, but have not been typeset or proofread. To cite this article, use the DOIs
MTE 4 and 9 Macronutrient Mix: Ideal Intake vs. Real-World Eating? References:
 MTE 4 and 9 Macronutrient Mix: Ideal Intake vs. Real-World Eating? Bayview Room, Bay Level Marion J. Franz, MS, RDN, CDE Saturday, March 5, 2016 2:00 p.m. 3:30 p.m. and 3:45 p.m. 5:15 p.m. Research trials
MTE 4 and 9 Macronutrient Mix: Ideal Intake vs. Real-World Eating? Bayview Room, Bay Level Marion J. Franz, MS, RDN, CDE Saturday, March 5, 2016 2:00 p.m. 3:30 p.m. and 3:45 p.m. 5:15 p.m. Research trials
Efficacy/pharmacodynamics: 85 Safety: 89
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor/Company: Sanofi Drug substance:
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor/Company: Sanofi Drug substance:
Felix Vallotton Ball (1899) LDL-C management in Asian diabetes: moderate vs. high intensity statin --- a lesson from EMPATHY study
 Felix Vallotton Ball (1899) LDL-C management in Asian diabetes: moderate vs. high intensity statin --- a lesson from EMPATHY study Conflict of interest disclosure None Committee of Scientific Affairs Committee
Felix Vallotton Ball (1899) LDL-C management in Asian diabetes: moderate vs. high intensity statin --- a lesson from EMPATHY study Conflict of interest disclosure None Committee of Scientific Affairs Committee
Case study: Adult with uncontrolled type 2 diabetes of long duration and cardiovascular disease
 Case study: Adult with uncontrolled type 2 diabetes of long duration and cardiovascular disease Authored by Paul Zimmet and Richard Nesto on behalf of the Global Partnership for Effective Diabetes Management.
Case study: Adult with uncontrolled type 2 diabetes of long duration and cardiovascular disease Authored by Paul Zimmet and Richard Nesto on behalf of the Global Partnership for Effective Diabetes Management.
RCHC Clinical Guidelines Type 2 Diabetes; Adults
 RCHC Clinical Guidelines Type 2 Diabetes; Adults Screening for diabetes in asymptomatic adults 1 Population: Aged > 45 years; Aged < 45 years who are overweight (BMI> 25kg/m 2 ) and have an additional
RCHC Clinical Guidelines Type 2 Diabetes; Adults Screening for diabetes in asymptomatic adults 1 Population: Aged > 45 years; Aged < 45 years who are overweight (BMI> 25kg/m 2 ) and have an additional
Project Summary: Draft Proposal Continued RESULTS. on the DASH Diet and 30 of the 40 original subjects on the Pro-DASH Diet.
 Project Summary: Draft Proposal Continued RESULTS Subjects The HNFE 3034 Spring 2013 semester s research study included 34 of the 38 original subjects on the DASH Diet and 30 of the 40 original subjects
Project Summary: Draft Proposal Continued RESULTS Subjects The HNFE 3034 Spring 2013 semester s research study included 34 of the 38 original subjects on the DASH Diet and 30 of the 40 original subjects
Cardiovascular Risk Factors among Diabetic Patients Attending a Nigerian Teaching Hospital. O Alao, S Adebisi, G Jombo, D Joseph, O Damulak, F Puepet
 ISPUB.COM The Internet Journal of Endocrinology Volume 6 Number 1 Cardiovascular Risk Factors among Diabetic Patients Attending a Nigerian Teaching Hospital. O Alao, S Adebisi, G Jombo, D Joseph, O Damulak,
ISPUB.COM The Internet Journal of Endocrinology Volume 6 Number 1 Cardiovascular Risk Factors among Diabetic Patients Attending a Nigerian Teaching Hospital. O Alao, S Adebisi, G Jombo, D Joseph, O Damulak,
Andrejs Kalvelis 1, MD, PhD, Inga Stukena 2, MD, Guntis Bahs 3 MD, PhD & Aivars Lejnieks 4, MD, PhD ABSTRACT INTRODUCTION. Riga Stradins University
 CARDIOVASCULAR RISK FACTORS ORIGINAL ARTICLE Do We Correctly Assess the Risk of Cardiovascular Disease? Characteristics of Risk Factors for Cardiovascular Disease Depending on the Sex and Age of Patients
CARDIOVASCULAR RISK FACTORS ORIGINAL ARTICLE Do We Correctly Assess the Risk of Cardiovascular Disease? Characteristics of Risk Factors for Cardiovascular Disease Depending on the Sex and Age of Patients
Patients characteristics associated with better glycemic response to teneligliptin and metformin therapy in type 2 diabetes: a retrospective study
 International Journal of Advances in Medicine Gadge PV et al. Int J Adv Med. 2018 Apr;5(2):424-428 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20181082
International Journal of Advances in Medicine Gadge PV et al. Int J Adv Med. 2018 Apr;5(2):424-428 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20181082
Ministry of Health, Labour and Welfare Prevention of Kidney Disease Progression Action Plan
 9 th IKEAJ-CKD International Symposium Ministry of Health, Labour and Welfare Prevention of Kidney Disease Progression Action Plan Division of Nephrology, Hypertension and Endocrinology, Department of
9 th IKEAJ-CKD International Symposium Ministry of Health, Labour and Welfare Prevention of Kidney Disease Progression Action Plan Division of Nephrology, Hypertension and Endocrinology, Department of
Obesity Prevention and Control: Provider Education with Patient Intervention
 Obesity Prevention and : Provider Education with Patient Summary Evidence Table and Population Cohen et al. (1991) 1987-1988 : RCT Location: Pittsburgh, PA Physician training session by a behavioral psychologist
Obesity Prevention and : Provider Education with Patient Summary Evidence Table and Population Cohen et al. (1991) 1987-1988 : RCT Location: Pittsburgh, PA Physician training session by a behavioral psychologist
Metabolic Syndrome among Type-2 Diabetic Patients in Benghazi- Libya: A pilot study. Arab Medical University. Benghazi, Libya
 Original Article Metabolic Syndrome among Type-2 Diabetic Patients in Benghazi- Libya: A pilot study Alshkri MM 1, Elmehdawi RR 2 1 Benghazi Diabetes Center. 2 Medical Department, Faculty of Medicine,
Original Article Metabolic Syndrome among Type-2 Diabetic Patients in Benghazi- Libya: A pilot study Alshkri MM 1, Elmehdawi RR 2 1 Benghazi Diabetes Center. 2 Medical Department, Faculty of Medicine,
Prediction of Homeostasis Model Assessment of Insulin Resistance in Japanese Subjects
 Tokai J Exp Clin Med., Vol. 37, No. 4, pp. 12-16, 212 Prediction of Homeostasis Model Assessment of Insulin Resistance in Japanese Subjects Masako NEGAMI, Eiko TAKAHASHI, Hiroki OTSUKA and Kengo MORIYAMA
Tokai J Exp Clin Med., Vol. 37, No. 4, pp. 12-16, 212 Prediction of Homeostasis Model Assessment of Insulin Resistance in Japanese Subjects Masako NEGAMI, Eiko TAKAHASHI, Hiroki OTSUKA and Kengo MORIYAMA
Association between arterial stiffness and cardiovascular risk factors in a pediatric population
 + Association between arterial stiffness and cardiovascular risk factors in a pediatric population Maria Perticone Department of Experimental and Clinical Medicine University Magna Graecia of Catanzaro
+ Association between arterial stiffness and cardiovascular risk factors in a pediatric population Maria Perticone Department of Experimental and Clinical Medicine University Magna Graecia of Catanzaro
Impact of Physical Activity on Metabolic Change in Type 2 Diabetes Mellitus Patients
 2012 International Conference on Life Science and Engineering IPCBEE vol.45 (2012) (2012) IACSIT Press, Singapore DOI: 10.7763/IPCBEE. 2012. V45. 14 Impact of Physical Activity on Metabolic Change in Type
2012 International Conference on Life Science and Engineering IPCBEE vol.45 (2012) (2012) IACSIT Press, Singapore DOI: 10.7763/IPCBEE. 2012. V45. 14 Impact of Physical Activity on Metabolic Change in Type
Diabetes Mellitus: A Cardiovascular Disease
 Diabetes Mellitus: A Cardiovascular Disease Nestoras Mathioudakis, M.D. Assistant Professor of Medicine Division of Endocrinology, Diabetes, & Metabolism September 30, 2013 1 The ABCs of cardiovascular
Diabetes Mellitus: A Cardiovascular Disease Nestoras Mathioudakis, M.D. Assistant Professor of Medicine Division of Endocrinology, Diabetes, & Metabolism September 30, 2013 1 The ABCs of cardiovascular
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
Targeted Nutrition Therapy Nutrition Masters Course
 Targeted Nutrition Therapy Nutrition Masters Course Nilima Desai, MPH, RD Learning Objectives Review clinical studies on innovative, targeted nutrition therapies for: o Blood glucose management o Dyslipidemia
Targeted Nutrition Therapy Nutrition Masters Course Nilima Desai, MPH, RD Learning Objectives Review clinical studies on innovative, targeted nutrition therapies for: o Blood glucose management o Dyslipidemia
Table S2: Anthropometric, clinical, cardiovascular and appetite outcome changes over 8 weeks (baseline-week 8) by snack group
 Table S1: Nutrient composition of cracker and almond snacks Cracker* Almond** Weight, g 77.5 g (5 sheets) 56.7 g (2 oz.) Energy, kcal 338 364 Carbohydrate, g (kcal) 62.5 12.6 Dietary fiber, g 2.5 8.1 Protein,
Table S1: Nutrient composition of cracker and almond snacks Cracker* Almond** Weight, g 77.5 g (5 sheets) 56.7 g (2 oz.) Energy, kcal 338 364 Carbohydrate, g (kcal) 62.5 12.6 Dietary fiber, g 2.5 8.1 Protein,
ABSTRACT ORIGINAL RESEARCH. Ichiro Nakamura. Hiroshi Maegawa. Kazuyuki Tobe. Satoshi Uno
 Adv Ther (2019) 36:923 949 https://doi.org/10.1007/s12325-019-0895-1 ORIGINAL RESEARCH Safety and Effectiveness of Ipragliflozin for Type 2 Diabetes in Japan: 12-Month Interim Results of the STELLA-LONG
Adv Ther (2019) 36:923 949 https://doi.org/10.1007/s12325-019-0895-1 ORIGINAL RESEARCH Safety and Effectiveness of Ipragliflozin for Type 2 Diabetes in Japan: 12-Month Interim Results of the STELLA-LONG
Common Diabetes-related Terms
 Common Diabetes-related Terms A1C An A1C test measures a person's average blood glucose level over two to three months. Hemoglobin is the part of a red blood cell that carries oxygen to the cells and sometimes
Common Diabetes-related Terms A1C An A1C test measures a person's average blood glucose level over two to three months. Hemoglobin is the part of a red blood cell that carries oxygen to the cells and sometimes
Abstract. KEY WORDS: obesity, type 2 diabetes, metabolic surgery, laparoscopic sleeve gastrectomy and bariatric surgery. Introduction.
 Original Article Early metabolic response after laparoscopic sleeve gastrectomy in obese diabetes. Glycative Stress Research Online edition : ISSN 2188-3610 Print edition : ISSN 2188-3602 Received : August
Original Article Early metabolic response after laparoscopic sleeve gastrectomy in obese diabetes. Glycative Stress Research Online edition : ISSN 2188-3610 Print edition : ISSN 2188-3602 Received : August
Nomogram of the Relation of Brachial-Ankle Pulse Wave Velocity with Blood Pressure
 801 Original Article Nomogram of the Relation of Brachial-Ankle Pulse Wave Velocity with Blood Pressure Akira YAMASHINA, Hirofumi TOMIYAMA, Tomio ARAI, Yutaka KOJI, Minoru YAMBE, Hiroaki MOTOBE, Zydem
801 Original Article Nomogram of the Relation of Brachial-Ankle Pulse Wave Velocity with Blood Pressure Akira YAMASHINA, Hirofumi TOMIYAMA, Tomio ARAI, Yutaka KOJI, Minoru YAMBE, Hiroaki MOTOBE, Zydem
Supplementary Online Content
 Supplementary Online Content Larsen JR, Vedtofte L, Jakobsen MSL, et al. Effect of liraglutide treatment on prediabetes and overweight or obesity in clozapine- or olanzapine-treated patients with schizophrenia
Supplementary Online Content Larsen JR, Vedtofte L, Jakobsen MSL, et al. Effect of liraglutide treatment on prediabetes and overweight or obesity in clozapine- or olanzapine-treated patients with schizophrenia
SYNOPSIS. Abbreviated Clinical Study Report. Study Code: RIMON_L_01031 Document Status: Synopsis V 2.1 Date: 16-Oct Title of the study:
 SYNOPSIS Title of the study: Investigator(s): A 12-month multicentre, randomised, double-blind, placebo-controlled study with two parallel groups to assess the effects of rimonabant 20 mg in patients with
SYNOPSIS Title of the study: Investigator(s): A 12-month multicentre, randomised, double-blind, placebo-controlled study with two parallel groups to assess the effects of rimonabant 20 mg in patients with
VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005
 VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005 1 Any adult in the health care system 2 Obtain blood pressure (BP) (Reliable,
VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005 1 Any adult in the health care system 2 Obtain blood pressure (BP) (Reliable,
A pilot Study of 25-Hydroxy Vitamin D in Egyptian Diabetic Patients with Diabetic Retinopathy
 A pilot Study of 25-Hydroxy Vitamin D in Egyptian Diabetic Patients with Diabetic Retinopathy El-Orabi HA 1, Halawa MR 1, Abd El-Salam MM 1, Eliewa TF 2 and Sherif NSE 1 Internal Medicine and Endocrinology
A pilot Study of 25-Hydroxy Vitamin D in Egyptian Diabetic Patients with Diabetic Retinopathy El-Orabi HA 1, Halawa MR 1, Abd El-Salam MM 1, Eliewa TF 2 and Sherif NSE 1 Internal Medicine and Endocrinology
Differences in Emotional Distress among Inpatients with Type 1, Obese Type 2, and Non-Obese Type 2 Diabetes Mellitus
 ORIGINAL ARTICLE Differences in Emotional Distress among Inpatients with Type 1, Obese Type 2, and Non-Obese Type 2 Diabetes Mellitus Yoshiko Miyawaki 1, Hiromi Iwahashi 2, Yukiyoshi Okauchi 3, Yoshiko
ORIGINAL ARTICLE Differences in Emotional Distress among Inpatients with Type 1, Obese Type 2, and Non-Obese Type 2 Diabetes Mellitus Yoshiko Miyawaki 1, Hiromi Iwahashi 2, Yukiyoshi Okauchi 3, Yoshiko
Some important concepts. 1. glucose requirement is < 130 g/d
 A Protein-rich rich Diet as a Cornerstone of a Healthy Lifestyle Donald K. Layman, Ph.D. Professor of Nutrition Dept. Food Science & Human Nutrition University of Illinois at Urbana-Champaign Outline:
A Protein-rich rich Diet as a Cornerstone of a Healthy Lifestyle Donald K. Layman, Ph.D. Professor of Nutrition Dept. Food Science & Human Nutrition University of Illinois at Urbana-Champaign Outline:
Diabetes Mellitus Case Study
 COLORADO STATE UNIVERSITY Diabetes Mellitus Case Study Medical Nutrition Therapy By: Emily Lancaster 9/28/2012 [Type the abstract of the document here. The abstract is typically a short summary of the
COLORADO STATE UNIVERSITY Diabetes Mellitus Case Study Medical Nutrition Therapy By: Emily Lancaster 9/28/2012 [Type the abstract of the document here. The abstract is typically a short summary of the
Hiroyuki Daikuhara 1, Fumi Kikuchi 2 and Toshihiko Ishida 2. Introduction. Original Article
 447310DVR9410.1177/1479164112447310Daikuhara et al.diabetes and Vascular Disease Research 2012 Original Article The combination of OLmesartan and a CAlcium channel blocker (azelnidipine) or candesartan
447310DVR9410.1177/1479164112447310Daikuhara et al.diabetes and Vascular Disease Research 2012 Original Article The combination of OLmesartan and a CAlcium channel blocker (azelnidipine) or candesartan
Adult Diabetes Clinician Guide NOVEMBER 2017
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
ADVANCE post trial ObservatioNal Study
 Hot Topics in Diabetes 50 th EASD, Vienna 2014 ADVANCE post trial ObservatioNal Study Sophia Zoungas The George Institute The University of Sydney Rationale and Study Design Sophia Zoungas The George Institute
Hot Topics in Diabetes 50 th EASD, Vienna 2014 ADVANCE post trial ObservatioNal Study Sophia Zoungas The George Institute The University of Sydney Rationale and Study Design Sophia Zoungas The George Institute
Why Do We Treat Obesity? Epidemiology
 Why Do We Treat Obesity? Epidemiology Epidemiology of Obesity U.S. Epidemic 2 More than Two Thirds of US Adults Are Overweight or Obese 87.5 NHANES Data US Adults Age 2 Years (Crude Estimate) Population
Why Do We Treat Obesity? Epidemiology Epidemiology of Obesity U.S. Epidemic 2 More than Two Thirds of US Adults Are Overweight or Obese 87.5 NHANES Data US Adults Age 2 Years (Crude Estimate) Population
Patient enrolment details CKDOD registry
 Patient enrolment details CKDOD registry Personal Information Date of enrolment D D Date of birth D D Gender Descent Height cm m History of smoking Y N U Date of first diagnosis of CKD D D Primary Cause
Patient enrolment details CKDOD registry Personal Information Date of enrolment D D Date of birth D D Gender Descent Height cm m History of smoking Y N U Date of first diagnosis of CKD D D Primary Cause
Waist Circumference Measurements in Special Metabolic Syndrome Medical Checkups for Employees of a Japanese University: A Follow-up Study
 ORIGINAL ARTICLES Waist Circumference Measurements in Special Metabolic Syndrome Medical Checkups for Employees of a Japanese University: A Follow-up Study Naohito Kawasaki 1, 2) Hisato Tominaga 1), Fumihiko
ORIGINAL ARTICLES Waist Circumference Measurements in Special Metabolic Syndrome Medical Checkups for Employees of a Japanese University: A Follow-up Study Naohito Kawasaki 1, 2) Hisato Tominaga 1), Fumihiko
OBESITY IN PRIMARY CARE
 OBESITY IN PRIMARY CARE Obesity- definition Is a chronic disease In ICD 10 E66 Overweight and obesity are defined as abnormal or excessive fat accumulation that may impair health. Obesity is a leading
OBESITY IN PRIMARY CARE Obesity- definition Is a chronic disease In ICD 10 E66 Overweight and obesity are defined as abnormal or excessive fat accumulation that may impair health. Obesity is a leading
Disclosures. Diabetes and Cardiovascular Risk Management. Learning Objectives. Atherosclerotic Cardiovascular Disease
 Disclosures Diabetes and Cardiovascular Risk Management Tony Hampton, MD, MBA Medical Director Advocate Aurora Operating System Advocate Aurora Healthcare Downers Grove, IL No conflicts or disclosures
Disclosures Diabetes and Cardiovascular Risk Management Tony Hampton, MD, MBA Medical Director Advocate Aurora Operating System Advocate Aurora Healthcare Downers Grove, IL No conflicts or disclosures
RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES
 RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES Risk Factors or Complications Glycemic Control Fasting & Capillary Plasma Glucose Anti-platelet
RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES Risk Factors or Complications Glycemic Control Fasting & Capillary Plasma Glucose Anti-platelet
Type 2 Diabetes Mellitus 2011
 2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
NOTES. Developed by Fabio Comana, MA., MS., All rights Reserved Page 1
 Session 455: Core Essentials in Science Fabio Comana, MA, MS, NASM CPT, CES & PES; ACE CPT & LWMC; ACSM HFS, NSCA CSCS; CISSN National Academy of Sports Medicine fabio.comana@nasm.org NOTES Developed by
Session 455: Core Essentials in Science Fabio Comana, MA, MS, NASM CPT, CES & PES; ACE CPT & LWMC; ACSM HFS, NSCA CSCS; CISSN National Academy of Sports Medicine fabio.comana@nasm.org NOTES Developed by
Original Article J Clin Med Res 2012;4(4): ress. Elmer
 Elmer Original Article ress Effects of 6-Month Sitagliptin Treatment on Glucose and Lipid Metabolism, Blood Pressure, Body Weight and Renal Function in Type 2 Diabetic Patients: A Chart-Based Analysis
Elmer Original Article ress Effects of 6-Month Sitagliptin Treatment on Glucose and Lipid Metabolism, Blood Pressure, Body Weight and Renal Function in Type 2 Diabetic Patients: A Chart-Based Analysis
sitagliptin, 25mg, 50mg and 100mg film-coated tablets (Januvia ) SMC No. (1083/15) Merck Sharp and Dohme UK Ltd
 sitagliptin, 25mg, 50mg and 100mg film-coated tablets (Januvia ) SMC No. (1083/15) Merck Sharp and Dohme UK Ltd 07 August 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the
sitagliptin, 25mg, 50mg and 100mg film-coated tablets (Januvia ) SMC No. (1083/15) Merck Sharp and Dohme UK Ltd 07 August 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Implications of The LookAHEAD Trial: Is Weight Loss Beneficial for Patients with Diabetes?
 Implications of The LookAHEAD Trial: Is Weight Loss Beneficial for Patients with Diabetes? Boston, MA November 7, 213 Edward S. Horton, MD Professor of Medicine Harvard Medical School Senior Investigator
Implications of The LookAHEAD Trial: Is Weight Loss Beneficial for Patients with Diabetes? Boston, MA November 7, 213 Edward S. Horton, MD Professor of Medicine Harvard Medical School Senior Investigator
Diabetes Mellitus Type 2
 Diabetes Mellitus Type 2 What is it? Diabetes is a common health problem in the U.S. and the world. In diabetes, the body does not use the food it digests well. It is hard for the body to use carbohydrates
Diabetes Mellitus Type 2 What is it? Diabetes is a common health problem in the U.S. and the world. In diabetes, the body does not use the food it digests well. It is hard for the body to use carbohydrates
Serum Retinol-binding Protein 4 Levels in Patients with Diabetic Retinopathy
 The Journal of International Medical Research 2010; 38: 95 99 Serum Retinol-binding Protein 4 Levels in Patients with Diabetic Retinopathy Z-Z LI 1, X-Z LU 2, J-B LIU 1 AND L CHEN 1 1 Department of Endocrinology,
The Journal of International Medical Research 2010; 38: 95 99 Serum Retinol-binding Protein 4 Levels in Patients with Diabetic Retinopathy Z-Z LI 1, X-Z LU 2, J-B LIU 1 AND L CHEN 1 1 Department of Endocrinology,
(Carbohydrate, protein, and fat contain calories. Only carbohydrates directly affect blood glucose levels) [14] 2013 ADA % 30% (systematic
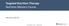
![(Carbohydrate, protein, and fat contain calories. Only carbohydrates directly affect blood glucose levels) [14] 2013 ADA % 30% (systematic (Carbohydrate, protein, and fat contain calories. Only carbohydrates directly affect blood glucose levels) [14] 2013 ADA % 30% (systematic](/thumbs/93/113040546.jpg) 116 [ ] diabetes mellitus, low carbohydrate diet 2014; 24: 116-123 DOI: 10.3966/168232812014092403002 [1-9] 50-60% 30% (systematic review) (meta-analysis) [10] ADA(American Diabetes Association) ADA 2007
116 [ ] diabetes mellitus, low carbohydrate diet 2014; 24: 116-123 DOI: 10.3966/168232812014092403002 [1-9] 50-60% 30% (systematic review) (meta-analysis) [10] ADA(American Diabetes Association) ADA 2007
Supplementary Online Content
 Supplementary Online Content Afkarian M, Zelnick L, Hall YN, et al. Clinical manifestations of kidney disease among US adults with diabetes, 1988-2014. JAMA. doi:10.1001/jama.2016.10924 emethods efigure
Supplementary Online Content Afkarian M, Zelnick L, Hall YN, et al. Clinical manifestations of kidney disease among US adults with diabetes, 1988-2014. JAMA. doi:10.1001/jama.2016.10924 emethods efigure
OBESITY 2008: DIET, EXERCISE, DRUGS, AND SURGERY
 OBESITY 2008: DIET, EXERCISE, DRUGS, AND SURGERY Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Declaration of full disclosure: No conflict of interest CLASSIFICATION OF OVERWEIGHT
OBESITY 2008: DIET, EXERCISE, DRUGS, AND SURGERY Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Declaration of full disclosure: No conflict of interest CLASSIFICATION OF OVERWEIGHT
CLINICAL TRIAL. Nobuya Inagaki 1 *,HirokiSano 2,YoshifumiSeki 2, Shingo Kuroda 2, Kohei Kaku 3
 Efficacy and safety of once-weekly oral trelagliptin switched from once-daily dipeptidyl peptidase-4 inhibitor in patients with type 2 diabetes mellitus: An open-label, phase 3 exploratory study Nobuya
Efficacy and safety of once-weekly oral trelagliptin switched from once-daily dipeptidyl peptidase-4 inhibitor in patients with type 2 diabetes mellitus: An open-label, phase 3 exploratory study Nobuya
L III: DIETARY APPROACH
 L III: DIETARY APPROACH FOR CARDIOVASCULAR DISEASE PREVENTION General Guidelines For Dietary Interventions 1. Obtain a healthy body weight 2. Obtain a desirable blood cholesterol and lipoprotein profile
L III: DIETARY APPROACH FOR CARDIOVASCULAR DISEASE PREVENTION General Guidelines For Dietary Interventions 1. Obtain a healthy body weight 2. Obtain a desirable blood cholesterol and lipoprotein profile
Sponsor / Company: Sanofi Drug substance(s): Insulin Glargine. Study Identifiers: NCT
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
TRANSPARENCY COMMITTEE
 The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 17 December 2014 JARDIANCE 10 mg, film-coated tablet B/30 tablets (CIP: 34009 278 928 5 1) JARDIANCE 25 mg, film-coated
The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 17 December 2014 JARDIANCE 10 mg, film-coated tablet B/30 tablets (CIP: 34009 278 928 5 1) JARDIANCE 25 mg, film-coated
Supplementary Table 1. Patient demographics and baseline characteristics (treated patients).
 Supplementary Table 1. Patient demographics and baseline characteristics (treated patients). Placebo (n=188) 10 mg (n=186) 25 mg (n=189) Total (n=563) Gender, n (%) Male 75 (40) 97 (52) 84 (44) 256 (45)
Supplementary Table 1. Patient demographics and baseline characteristics (treated patients). Placebo (n=188) 10 mg (n=186) 25 mg (n=189) Total (n=563) Gender, n (%) Male 75 (40) 97 (52) 84 (44) 256 (45)
Metabolic Syndrome. Shon Meek MD, PhD Mayo Clinic Florida Endocrinology
 Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
