Chronic kidney disease (CKD) (Southampton pathway)
|
|
|
- Wendy Beasley
- 5 years ago
- Views:
Transcription
1 Background information Patient information Key messages for this pathway Definitions and abbreviations used in this pathway Classification of CKD Diagnosis of CKD Summary of referral criteria Screening for CKD in high risk groups Symptoms and signs suggestive of CKD Incidental finding Urinalysis and egfr Urinalysis result egfr result Assessment of isolated AMH Assessment of proteinuria with AMH Assessment of isolated proteinuria THRESHOLD for referral of patients with egfr <30ml/min Stage 4/5 CKD THRESHOLD for referral of patients with egfr 30-59ml/min Stage 3 CKD THRESHOLD for referral of patients with egfr 60ml/min Stage 1/2 CKD THRESHOLD for referral THRESHOLD for referral THRESHOLD for referral Are criteria for referral met? Consider Choose & Book Advice and Guidance Yes No Refer to Nephrology R Discharged to primary care Consider Choose & Book Advice and Guidance Go to CKD management in the community Go to CKD management in the community Refer to nephrology R Management by nephrology Discharged to primary care Go to CKD management in the community Page 1 of 13
2 1 Background information Since the introduction of egfr reporting in 2006 as part of the National Service Framework for Renal Services, an increasing number of patients with chronic kidney disease (CKD) have been identified. It is estimated that mild to moderate CKD (egfr >30ml/ min/1.73m²) has a prevalence of approximately 10% in the general population. Whilst the majority of patients with CKD have stable or slowly progressive disease, never reaching dialysis dependence, all have a significantly increased risk of cardiovascular (CV) disease, with a mortality rate approaching 40 times that of the general population. It is now well established that treatment of CKD from an early stage not only stabilises renal function but can also significantly reduce CV risk. In September 2008, NICE published guidelines for the management of CKD in primary care aimed at: earlier identification of CKD reducing the risk of progression to established renal failure reducing the risk of CV disease In light of these guidelines, this document provides local recommendations for the diagnosis, investigation and management of all stages of CKD in adults. The focus of these guidelines is to inform the assessment, investigation and management issues for all stages of CKD in adults, with particular emphasis on when and whom to refer for a specialist opinion. They are specific to CKD and do not cover acute kidney injury (AKI, previously known as acute renal failure), patients on dialysis or renal transplant patients. As with most guidelines, one size does not fit all and there may be circumstances where referral may seem inappropriate or unnecessary. For example, in patients with multiple co-morbidities, the primary care physician should make a judgement on how nephrological advice would impact upon the future of that individual. Similarly, while age should not be used to determine appropriateness of referral, any renal abnormality in a young adult warrants more concern than a similar abnormality in an elderly individual, bearing in mind that loss of renal function is expected with age. The renal service would be very happy to discuss any cases that are not clear-cut or that do not fall within the referral criteria. References: Department of Health (DH). National service framework for renal services. Part two: chronic kidney disease, acute renal failure and end of life care. London: DH; Renal Association (RA). Chronic kidney disease in adults: UK guidelines for identification, management and referral. London: RA; National Institute for Health and Clinical Evidence (NICE). Early identification and management of chronic kidney disease in adults in primary and secondary care. Clinical guideline 73. London: NICE; Kidney Disease Outcome Quality Initiative. K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, and stratification. Am J Kidney Dis 2002; 39 Suppl 1: S1-S Patient information Patient information on CKD can be found at 3 Key messages for this pathway This pathway has been locally developed for South West Hampshire, taking 2008 NICE guidelines and current Renal Association guidelines into account. Key messages for this pathway: PCR should be measured for CKD rather than ACR, which is more expensive and does not add extra information ACR remains essential for screening and assessment of microalbuminuria in diabetic renal disease Contributors to this pathway: Dr Kirsty Armstrong, SUHT Page 2 of 13
3 Dr Patrick Terry, NHSSC Dr Tim Thurston, NHSH 4 Classification of CKD CKD is classified into 5 stages of severity based on the egfr and the presence or absence of other markers of kidney damage. It is diagnosed when there is: egfr 60ml/min/1.73m 2 for > 3 months with structural and / or functional abnormalities of the kidneys egfr < 60ml/min/1.73m 2 for > 3 months with or without structural and / or functional abnormalities of the kidneys Stage 1 egfr 90ml/min/1.73m 2 normal or increased GFR with other evidence of kidney damage* prevalence 3.3% Stage 2 egfr 60-89ml/min/1.73m 2 slightly decreased GFR with other evidence of kidney damage* prevalence 3% Stage 3 egfr 45-59ml/min/1.73m 2 (Stage 3A) egfr 30-44ml/min/1.73m 2 (Stage 3B) moderately decreased GFR prevalence 4.3% Stage 4 egfr 15-29ml/min/1.73m 2 severe decrease in GFR prevalence 0.2% Stage 5 egfr <15ml/min/1.73m 2 established (end-stage) renal failure prevalence 0.2% *Other evidence of kidney damage may be one or more of the following: persistent microalbuminuria in diabetics persistent proteinuria; PCR 50mg/mmol (or ACR 30mg/mmol) persistent asymptomatic microscopic haematuria (AMH) and urological causes excluded (if > 50 years) see Asymptomatic microscopic haematuria pathway structural abnormalities of the renal tract eg polycystic kidneys, reflux nephropathy with scarring, single kidney biopsy-proven chronic glomerulonephritis Points to note: patients with egfr 60ml/min/1.73m 2 without other evidence of kidney damage do NOT have CKD and should not be subjected to further investigation patients with egfr 60ml/min/1.73m 2 and a normal urine dip do NOT need an ultrasound scan UNLESS there is a family history of renal disease (e.g. ADPKD), or a history of reflux nephropathy patients > 70 with Stage 3A CKD (egfr 45-59ml/min/1.73m²), stable renal function and no other evidence of kidney damage are unlikely to develop CKD-related complications Page 3 of 13
4 patients with Stage 3B CKD (egfr 30-44ml/min/1.73m²) are at far higher risk of CV disease and end-stage kidney disease than those with Stage 3A disease and should therefore be regarded as an important target group, particularly if there are risk factors for progression eg hypertension, diabetes, significant proteinuria or inherited kidney disease 5 Definitions and abbreviations used in this pathway Abbreviations ACEI: angiotensin-converting enzyme inhibitor ACR: albumin creatinine ratio ADPKD: autosomal dominant polycystic kidney disease AKI: acute kidney injury (previously acute renal failure) AMH: asymptomatic microscopic haematuria ARB: angiotensin-ii receptor blocker BP: blood pressure CKD: chronic kidney disease CV: cardiovascular egfr: estimated glomerular filtration rate NSAID: non-steroidal anti-inflammatory drug PCR: protein creatinine ratio PTH: parathyroid hormone RRT: renal replacement therapy (dialysis or transplant) SLE: systemic lupus erythematosis USS: ultrasound scan Definitions microalbuminuria: ACR > 2.5mg/mmol in men or > 3.5mg/mmol in women with diabetes nephrotic range proteinuria: PCR > 300mg/mmol (or ACR > 250mg/mmol) nephrotic syndrome: PCR>300mg/mmol, albumin<30g/l and oedema persistent AMH: 1+ blood on 2 out of 3 urine dip tests persistent proteinuria: 1+ protein on 2 out of 3 urine dip tests progressive CKD: sustained and progressive decline in egfr of > 10% from baseline over 6 months or less referral criteria for isolated proteinuria: PCR > 100mg/mmol (or ACR > 70mg/mmol) (unless known to be due to diabetes and already appropriately treated) refractory hypertension: Blood pressure > 150/90 despite the use of 4 anti-hypertensive agents at therapeutic doses significant proteinuria: PCR>50mg/mmol (or ACR>30mg/mmol) 6 Summary of referral criteria Summary of referral criteria and information required with referral can be found in this document CKD referral summary 7 Diagnosis of CKD Chronic kidney disease (CKD) is usually picked up in the following situations: during screening of patients deemed at high risk of developing CKD during screening of patients in whom there is a clinical suspicion of CKD as an incidental finding on a routine blood test, urine test or imaging test Page 4 of 13
5 The two common methods for detecting CKD are: 1. Estimated glomerular filtration rate (egfr) 2. Urinalysis 8 Screening for CKD in high risk groups Screen for occult CKD (egfr and urinalysis) at least annually in all adult patients with: conditions associated with a high risk of development of CKD, e.g. hypertension, diabetes mellitus, CV disease and heart failure conditions requiring long-term treatment with recognised nephrotoxins, e.g. ACE inhibitors (ACEIs) and angiotensin-ii receptor blockers (ARBs), non-steroidal anti-inflammatory drugs (NSAIDS), lithium, mesalazine and calcineurin inhibitors such as cyclosporin or tacrolimus multisystem diseases with potential kidney involvement, e.g. SLE, vasculitis, myeloma and rheumatoid arthritis family history of hereditary renal disease, e.g. autosomal dominant polycystic kidney disease (ADPKD) or Stage 5 CKD urological conditions including neurogenic bladder (e.g. spina bifida), surgical urinary diversion, renal stone disease, benign prostatic hypertrophy or lower urinary tract symptoms including recurrent UTIs history of nephritis in childhood 9 Symptoms and signs suggestive of CKD Patients presenting with any of the following symptoms and/or signs should have an egfr and urinalysis as part of their preliminary investigations: non-specific symptoms including anorexia, nausea, vomiting, lethargy, shortness of breath, weight loss, itching signs of fluid overload including unexplained weight gain, peripheral oedema, pleural effusions, hypertension 10 Incidental finding Occult CKD may be detected as an incidental finding on a routine blood test, urine dipstick or renal imaging such as an ultrasound. Abnormalities should prompt further investigation 11 Urinalysis and egfr The two common methods for detecting CKD are: 1. Urinalysis 2. egfr (estimated glomerular filtration rate) Urinalysis Urinalysis should be performed alongside measurement of creatinine and egfr in anyone being evaluated for CKD. A positive urinalysis, defined as: asymptomatic microscopic haematuria (AMH) ( 1+ on urine dipstick), proteinuria with AMH ( 1+ on urine dipstick) or isolated proteinuria which may be an indicator of CKD and should prompt further investigation egfr The egfr is now the routine test of renal function and is reported alongside creatinine. It is much better at identifying early renal disease compared to serum creatinine alone (up to 50% of renal function can be lost before the creatinine exceeds the reference range, particularly in the elderly). The egfr is estimated from the serum creatinine, gender and age. It should be multiplied by a correction factor of 1.2 for African- Caribbean patients. In broad terms, the egfr equates to the percentage of normal kidney function that someone has. Page 5 of 13
6 The egfr is not validated in the following patient groups, in whom results should be interpreted with caution. patients with AKI patients < 18 years of age during pregnancy patients with extremes of muscle mass e.g. malnutrition or muscle wasting disorders, amputees, body builders oedematous states e.g. congestive cardiac failure, chronic liver disease certain ethnic groups e.g. Asians and Chinese NB: allow for biological and analytical variability of serum creatinine (± 5%) when interpreting changes in the egfr over time. 12 Urinalysis result A negative urinalysis is defined as: absence or trace of blood absence of proteinuria Note: absence of proteinuria on a dipstick does NOT exclude microalbuminuria, and an ACR should be requested in all patients with diabetes, even when the urine dip is negative for protein A positive urinalysis may be any of the following and should prompt further investigations: 1. Isolated asymptomatic microscopic haematuria (AMH) ( 1+) 2. Proteinuria ( 1+) with AMH ( 1+) 3. Isolated proteinuria ( 1+) egfr should be measured in anyone being evaluated for Chronic Kidney Disease, regardless of the urinalysis result, to determine whether nephrology referral is indicated. See egfr result box. 13 egfr result egfr should be measured in anyone being evaluated for CKD even if the urinalysis is negative. CKD is classified into 5 stages of severity, based on the egfr and the presence or absence of other markers of kidney damage (refer to Classification of CKD box above). Points to note: patients with egfr 60mls/min/1.73m 2 without other evidence of kidney damage do NOT have CKD and should not be subjected to further investigation patients with egfr 60mls/min/1.73m 2 and a normal urine dip do NOT need an ultrasound scan UNLESS there is a family history of renal disease (e.g. ADPKD), or a history of reflux nephropathy patients > 70 years with Stage 3A CKD (egfr 45-59mls/min/1.73m²), stable renal function and no other evidence of kidney damage are unlikely to develop CKD-related complications patients with Stage 3B CKD (egfr 30-44mls/min/1.73m²) are at far higher risk of CV disease and end-stage kidney disease than those with Stage 3A disease and should therefore be regarded as an important target group, particularly if there are risk factors for progression eg hypertension, diabetes, significant proteinuria or inherited kidney disease 14 THRESHOLD for referral of patients with egfr 30-59ml/min Stage 3 CKD Refer to nephrology if: progressive CKD (see definition of progression below) refractory hypertension with Stage 3B CKD (egfr <45ml/min/1.73m 2) Page 6 of 13
7 suspected renal artery stenosis ie acute deterioration in kidney function after starting an ACEI or ARB (defined as a rise in serum creatinine 30% or a fall in egfr 25% within 2 weeks of ACEI or ARB introduction / dose increase (see Indications for ACEIs and ARBs in CKD management in the community) known or suspected genetic cause of renal disease eg ADPKD haemoglobin < 110g/L and non-renal causes excluded ( particularly if egfr <45ml/min/1.73m 2 ) (see Management of suspected renal anaemia in CKD management in the community) severe hyperkalaemia (K + > 6.0mmol/L) and unresponsive to changes in therapy(see Management of hyperkalaemia in CKD management in the community) NB: If K + > 7.0mmol/L, patient requires urgent referral to AMU for assessment Definition of progression The definition of progressive CKD is highly contentious. South West Hampshire Trusts have elected to follow the criteria for progression recommended by the Wessex Renal and Transplant Unit at Portsmouth, i.e. a sustained and progressive decline in egfr of > 10% from baseline over a 6 month period. To assess for progression in a patient with an abnormal egfr: 1. Review previous creatinine/egfr levels over as long a time as possible to assess trend 2. Obtain a minimum of 3 egfr readings over a period of 3-6 months Points to note: take into consideration risk factors for progression, e.g. significant proteinuria (PCR > 50mg/mmol), inherited kidney disease, diabetes or poorly controlled hypertension consider whether progression, if it should it continue at the same rate, would result in the patient reaching dialysis dependence in their lifetime in patients in whom you suspect an abnormal egfr may be due to AKI, rather than CKD, repeat egfr within 2 weeks or less depending on clinical scenario The following information should accompany the referral letter: full medical history including relevant renal history current (and recently changed) medications examination including blood pressures (previous and current), oedema etc urinalysis results including PCR (or ACR) (if relevant) a list of the dates and results of previous measurements of serum creatinine / egfr (particularly if not undertaken in Southampton lab) recent biochemical and haematological profile to include (if relevant) calcium, phosphate, bicarbonate, albumin, glucose, lipid profile, haemoglobin and haematinics results of a recent USS (within 6 months) if relevant. 15 Assessment of isolated AMH Isolated asymptomatic microscopic haematuria (AMH) ( 1+): exclude menstruation and UTI (by dipstick) repeat urinalysis if persistent AMH ( 2 out of 3 positive results) see THRESHOLD for referral 16 Assessment of proteinuria with AMH Proteinuria ( 1+) with asymptomatic microscopic haematuria (AMH) ( 1+): exclude menstruation and UTI (by dipstick) repeat urinalysis if persistent proteinuria ( 2 out of 3 positive results), send spot urine for PCR (or ACR) and see THRESHOLD for referral Page 7 of 13
8 Points to note: PCR (or ACR) should be measured preferably on an early morning mid-stream urine sample PCR is the better (and cheaper) test for monitoring patients with proteinuria as well as detecting proteinuria in non-diabetic patients multiplying the PCR by 10 approximates to the amount of protein per day e.g. PCR 100mg/mmol=proteinuria of 1g/24hr) ACR is the test of choice in patients with diabetes and should be requested even when the urine tests negative for protein (a negative dipstick for protein does not exclude microalbuminuria) for a diagnosis of microalbuminuria 2 abnormal results from 3 specimens are required 17 Assessment of isolated proteinuria Isolated proteinuria( 1+): exclude UTI by dipstick repeat urinalysis if persistent proteinuria ( 2 out of 3 positive results), send spot urine for PCR (or ACR) and see THRESHOLD for referral Points to note: PCR (or ACR) should be measured preferably on an early morning mid-stream urine sample PCR is the better (and cheaper) test for monitoring patients with proteinuria as well as detecting proteinuria in non-diabetic patients multiplying the PCR by 10 approximates to the amount of protein per day e.g. PCR 100mg/mmol=proteinuria of 1g/24hr) ACR is the test of choice in patients with diabetes and should be requested even when the urine tests negative for protein (a negative dip for protein does not exclude microalbuminuria) for a diagnosis of microalbuminuria 2 abnormal results from 3 specimens are required 18 THRESHOLD for referral of patients with egfr <30ml/min Stage 4/5 CKD As a general rule, all patients with newly diagnosed Stage 4 (egfr ml/min/1.73m 2 ) CKD or Stage 5 (egfr <15 ml/ min/1.73m 2 ) CKD should be referred or at least formally discussed with a nephrologist. This is to identify patients who may require renal replacement therapy (RRT) in the future and to ensure that an agreed and understood management plan is in place that can be activated as and when necessary. The only exceptions to this rule would be: patients in whom you deem further investigations / dialysis therapy to be inappropriate because of advanced age and / or significant comorbidities patients in whom severe renal impairment is part of another terminal illness patients who have specifically declined any further investigations or treatment In such individuals specialist assessment is unlikely to influence further management, and ongoing care in the community may be more appropriate (CKD management in the community pathway). In patients being referred the following information should accompany the referral letter: full medical history including relevant renal history current (and recently changed) medications examination including blood pressures (previous and current), oedema etc urinalysis results including PCR (or ACR) (if relevant) a list of the dates and results of previous measurements of serum creatinine / egfr (particularly if not undertaken in Southampton lab) recent biochemical and haematological profile to include calcium, phosphate, bicarbonate, albumin, glucose, lipid profile, haemoglobin and haematinics results of a recent USS (within 6 months) if available. Page 8 of 13
9 19 THRESHOLD for referral of patients with egfr 60ml/min Stage 1/2 CKD Refer to nephrology if: isolated persistant AMH and <50 years 50 years and urological causes excluded proteinuria (PCR 50mg/mmol (or ACR 30mg/mmol)) and persistent AMH significant proteinuria (PCR 100mg/mmol (or ACR 70mg/mmol)) suspected renal artery stenosis ie acute deterioration in kidney function after starting an ACEI or ARB (defined as a rise in serum creatinine 30% or a fall in egfr 25% within 2 weeks of ACEI or ARB introduction / dose increase (see Indications for ACEIs and ARBs in CKD management in the community) known or suspected genetic cause of renal disease eg ADPKD severe hyperkalaemia (K + > 6.0mmol/L) and unresponsive to changes in therapy(see Management of hyperkalaemia in CKD management in the community) Nb. If K + > 7.0mmol/L, patient requires urgent referral to AMU for assessment Points to note: in patients in whom you suspect an abnormal egfr may be due to AKI, rather than CKD, repeat egfr within 2 weeks or less depending on clinical scenario patients with egfr 60ml/min/1.73m 2 without other evidence of kidney damage do not have CKD and should not be subjected to further investigation The following information should accompany the referral letter: full medical history including relevant renal history current (and recently changed) medications examination including blood pressures (previous and current), oedema etc urinalysis results including ACR / PCR (if relevant) a list of the dates and results of previous measurements of serum creatinine / egfr (particularly if not undertaken in Southampton lab) recent biochemical and haematological profile (if relevant) results of a recent USS (within 6 months) only if there is a family history of renal disease, e.g. ADPKD or a history of reflux nephropathy NB: many patients with egfr 60ml/min/1.73m 2 can be managed via Choose and Book advice in the first instance 20 THRESHOLD for referral Refer to nephrology if isolated persistent AMH ( 2 out of 3 positive results) and < 50 years, or 50 years and urological causes have been excluded The following information should accompany the referral letter: full medical history including relevant renal history current (and recently changed) medications examination including blood pressures (previous and current), oedema etc urinalysis results a list of the dates and results of previous measurements of serum creatinine / egfr (particularly if not undertaken in Southampton lab) recent biochemical and haematological profile to include (if relevant) calcium, phosphate, bicarbonate, albumin, glucose, lipid profile, haemoglobin and haematinics results of a recent USS (within 6 months) if relevant. NB: patients with AMH may not need to be seen in clinic and will first be investigated via the "virtual" renal AMH pathway. Page 9 of 13
10 21 THRESHOLD for referral Refer to nephrology if: PCR 50mg/mmol (or ACR 30mg/mmol) and persistant AMH If PCR < 50mg/mmol (or ACR < 30mg/mmol), see Assessment of isolated AMH box. The following information should accompany the referral letter: full medical history including relevant renal history current (and recently changed) medications examination including blood pressures (previous and current), oedema etc urinalysis results including PCR (or ACR) a list of the dates and results of previous measurements of serum creatinine / egfr (particularly if not undertaken in Southampton lab) recent biochemical and haematological profile to include (if relevant) calcium, phosphate, bicarbonate, albumin, glucose, lipid profile, haemoglobin and haematinics results of a recent USS (within 6 months) if relevant. 22 THRESHOLD for referral Refer to nephrology if: PCR 100mg/mol (or ACR 70mg/mmol) The following information should accompany the referral letter: full medical history including relevant renal history current (and recently changed) medications examination including blood pressures (previous and current), oedema etc urinalysis results including PCR (or ACR) a list of the dates and results of previous measurements of serum creatinine / egfr (particularly if not undertaken in Southampton lab) recent biochemical and haematological profile to include (if relevant) calcium, phosphate, bicarbonate, albumin, glucose, lipid profile, haemoglobin and haematinics results of a recent USS (within 6 months) if relevant. 24 Consider Choose & Book Advice and Guidance Many patients with positive urinalysis and egfr >60ml/min/1.73m 2 can be managed via Choose and Book advice in the first instance. Local administrative info: Renal Medicine / Nephrology Inpatient and admin enquiries: Tel: Outpatient queries: Tel: Fax: Choose and Book services available: General nephrology Page 10 of 13
11 Difficult hypertension Systemic vasculitis CKD Consultants: Dr Kirsty Armstrong, MBBS PhD MRCP Specialty: Nephrology Contact: Dr Armstrong is fully trained in all areas of nephrology and has a special interest in cardiovascular risk factor modification in patients with chronic kidney disease or renal transplant Dr Mary Rogerson, FRCP Specialty: Renal and general medicine Contact: Dr Rogerson is the lead clinician for renal medicine at SUHT. Southampton Area 24-May Consider Choose & Book Advice and Guidance Many patients with positive urinalysis and egfr >60ml/min/1.73m 2 can be managed via Choose and Book advice in the first instance. Local administrative info: Renal Medicine / Nephrology Inpatient and admin enquiries: Tel: Outpatient queries: Tel: Fax: Choose and Book services available: General nephrology Difficult hypertension Systemic vasculitis CKD Consultants: Dr Kirsty Armstrong, MBBS PhD MRCP Specialty: Nephrology Contact: Dr Armstrong is fully trained in all areas of nephrology and has a special interest in cardiovascular risk factor modification in patients with chronic kidney disease or renal transplant Dr Mary Rogerson, FRCP Specialty: Renal and general medicine Contact: Dr Rogerson is the lead clinician for renal medicine at SUHT. Southampton Area 24-May Discharged to primary care Patients who are discharged back to primary care after a preliminary assessment should be managed according to the CKD management in the community pathway. Page 11 of 13
12 31 Management by nephrology Patients with progressive CKD and risk factors for progression, e.g. significant proteinuria, hypertension, diabetes or inherited kidney disease, are likely to remain under long term nephrological review. 32 Discharged to primary care Patients with stable CKD are likely to be discharged to primary care after a preliminary assessment or a period of monitoring. For advice on ongoing management, see CKD management in the community pathway. Page 12 of 13
13 Key Dates Published: 19-May-2011, by Southampton Area Valid until: 31-Jan-2013 Evidence summary for Chronic kidney disease (CKD) (Southampton pathway) This pathway has been developed according to the Map of Medicine editorial methodology ( The content of this pathway is based on high-quality guidelines [1,2,4-8,10] and critically appraised meta-analyses and systematic reviews [9]. Practice-based knowledge has been added by contributors with front-line clinical experience [3]. References This is a list of all the references that have passed critical appraisal for use in the care map Chronic kidney disease ID Reference 1 National Institute for Health and Clinical Evidence (NICE). Early identification and management of chronic kidney disease in adults in primary and secondary care. Clinical guideline 73. Clinical guideline 73. London: NICE; Department of Health (DH). National service framework for renal services. Part two: chronic kidney disease, acute renal failure and end of life care. London: DH; dh_ pdf 3 Contributors representing the Royal College of Physicians Renal Association (RA). Chronic kidney disease in adults: UK guidelines for identification, management and referral. London: RA; Joint Speciality Committee on Renal Medicine of the Royal College of Physicians of London (RCP) and the Renal Association (RA). Identification, management and referral of adults with chronic kidney disease. Guidelines for General Physicians and General Practitioners 5. London: RCP; Scottish Intercollegiate Guidelines Network (SIGN). Diagnosis and management of chronic kidney disease. A national clinical guideline. SIGN publication no Edinburgh: SIGN; American College of Radiology (ACR). ACR Appropriateness Criteria. Renal Failure. Reston, VA: ACR; logicimaging/renalfailuredoc15.aspx 8 National Collaborating Centre for Chronic Conditions (NCC-CC). Chronic kidney disease: national clinical guideline for early identification and management in adults in primary and secondary care. London: Royal College of Physicians; Schroth RJ, Hitchon CA, Uhanova J et al. Hepatitis B vaccination for patients with chronic renal failure. Cochrane Database Syst Rev 2004; CD Bolton WK. Renal physicians association clinical practice guideline: appropriate patient preparation for renal replacement therapy: guideline number 3. J Am Soc Nephrol 2003; 14: Page 13 of 13
QUICK REFERENCE FOR HEALTHCARE PROVIDERS
 KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma. Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree
 Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree Topics CKD background egfr background Patient with egfr Referral Guidelines
Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree Topics CKD background egfr background Patient with egfr Referral Guidelines
Professor Suetonia Palmer
 Professor Suetonia Palmer Department of Medicine Nephrologist Christchurch Hospital Christchurch 14:00-14:55 WS #108: The Kidney Test - When To Test and When to Refer ( and When Not To) 15:05-16:00 WS
Professor Suetonia Palmer Department of Medicine Nephrologist Christchurch Hospital Christchurch 14:00-14:55 WS #108: The Kidney Test - When To Test and When to Refer ( and When Not To) 15:05-16:00 WS
NORTHERN IRELAND GUIDELINES FOR MANAGEMENT OF CHRONIC KIDNEY DISEASE
 NORTHERN IRELAND GUIDELINES FOR MANAGEMENT OF CHRONIC KIDNEY DISEASE Practical points for use of estimated GFR + quality outcome framework indicators Developed by GAIN and the Northern Ireland Nephrology
NORTHERN IRELAND GUIDELINES FOR MANAGEMENT OF CHRONIC KIDNEY DISEASE Practical points for use of estimated GFR + quality outcome framework indicators Developed by GAIN and the Northern Ireland Nephrology
Identification, management and referral of adults with chronic kidney disease: concise guidelines
 Identification, management and referral of adults with chronic kidney disease: concise guidelines Abstract Chronic Kidney Disease (CKD) is often thought to be a relatively rare condition requiring specialist
Identification, management and referral of adults with chronic kidney disease: concise guidelines Abstract Chronic Kidney Disease (CKD) is often thought to be a relatively rare condition requiring specialist
The National Quality Standards for Chronic Kidney Disease
 The National Quality Standards for Chronic Kidney Disease Dr Robert Lewis Chief of Service, Wessex Kidney Centre, Portsmouth Specialist Committee Member Quality Standard for Chronic Kidney Disease, NICE
The National Quality Standards for Chronic Kidney Disease Dr Robert Lewis Chief of Service, Wessex Kidney Centre, Portsmouth Specialist Committee Member Quality Standard for Chronic Kidney Disease, NICE
Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus
 Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus 1 Contents Executive Summary... 3 How to Screen for Diabetic Nephropathy... 4 What to Measure... 4 Frequency
Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus 1 Contents Executive Summary... 3 How to Screen for Diabetic Nephropathy... 4 What to Measure... 4 Frequency
Nice CKD Clinical Guidelines 2014 The challenges and benefits they may bring toprimary care
 Nice CKD Clinical Guidelines 2014 The challenges and benefits they may bring toprimary care Paula D Souza Senior CKD Nurse Specialist Royal Devon and Exeter Healthcare Trust Introduction Background What
Nice CKD Clinical Guidelines 2014 The challenges and benefits they may bring toprimary care Paula D Souza Senior CKD Nurse Specialist Royal Devon and Exeter Healthcare Trust Introduction Background What
Chronic Kidney Disease
 Chronic Kidney Disease Presence of kidney damage or decreased kidney function for three or more months, - necessary to distinguish CKD from acute kidney disease. Ascertained either by kidney biopsy or
Chronic Kidney Disease Presence of kidney damage or decreased kidney function for three or more months, - necessary to distinguish CKD from acute kidney disease. Ascertained either by kidney biopsy or
VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERENCE CARDS Chronic Kidney Disease
 VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERECE CARDS Chronic Kidney Disease CKD VA/DoD Clinical Practice Guideline for the Management
VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERECE CARDS Chronic Kidney Disease CKD VA/DoD Clinical Practice Guideline for the Management
Chronic kidney disease screening and assessment
 Care map information Information resources for patients and carers Aboriginal and Torres Strait Islanders DEFINITION OF CKD egfr
Care map information Information resources for patients and carers Aboriginal and Torres Strait Islanders DEFINITION OF CKD egfr
Chronic Kidney Disease: Optimal and Coordinated Management
 Chronic Kidney Disease: Optimal and Coordinated Management Michael Copland, MD, FRCPC Presented at University of British Columbia s 42nd Annual Post Graduate Review in Family Medicine Conference, Vancouver,
Chronic Kidney Disease: Optimal and Coordinated Management Michael Copland, MD, FRCPC Presented at University of British Columbia s 42nd Annual Post Graduate Review in Family Medicine Conference, Vancouver,
Primary Care Approach to Management of CKD
 Primary Care Approach to Management of CKD This PowerPoint was developed through a collaboration between the National Kidney Foundation and ASCP. Copyright 2018 National Kidney Foundation and ASCP Low
Primary Care Approach to Management of CKD This PowerPoint was developed through a collaboration between the National Kidney Foundation and ASCP. Copyright 2018 National Kidney Foundation and ASCP Low
Office Management of Reduced GFR Practical advice for the management of CKD
 Office Management of Reduced GFR Practical advice for the management of CKD CKD Online Education CME for Primary Care April 27, 2016 Monica Beaulieu, MD FRCPC MHA CHAIR PROVINCIAL KIDNEY CARE COMMITTEE
Office Management of Reduced GFR Practical advice for the management of CKD CKD Online Education CME for Primary Care April 27, 2016 Monica Beaulieu, MD FRCPC MHA CHAIR PROVINCIAL KIDNEY CARE COMMITTEE
Faculty/Presenter Disclosure
 CSI for CKD Unravelling the myths surrounding chronic kidney disease Practical Evidence for Informed Practice Oct 21 2016 Dr. Scott Klarenbach University of Alberta Slide 1: Option B (Presenter with NO
CSI for CKD Unravelling the myths surrounding chronic kidney disease Practical Evidence for Informed Practice Oct 21 2016 Dr. Scott Klarenbach University of Alberta Slide 1: Option B (Presenter with NO
CKD and risk management : NICE guideline
 CKD and risk management : NICE guideline 2008-2014 Shahed Ahmed Consultant Nephrologist shahed.ahmed@rlbuht.nhs.uk Key points : Changing parameters of CKD and NICE guidance CKD and age related change of
CKD and risk management : NICE guideline 2008-2014 Shahed Ahmed Consultant Nephrologist shahed.ahmed@rlbuht.nhs.uk Key points : Changing parameters of CKD and NICE guidance CKD and age related change of
Bulletin Independent prescribing information for NHS Wales
 Bulletin Independent prescribing information for NHS Wales October 2017 Chronic kidney disease Chronic kidney disease (CKD) is a long-term irreversible deterioration in the function of the kidneys, often
Bulletin Independent prescribing information for NHS Wales October 2017 Chronic kidney disease Chronic kidney disease (CKD) is a long-term irreversible deterioration in the function of the kidneys, often
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012
 Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
CKD FOR INTERNISTS. Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College
 CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
Elevation of Serum Creatinine: When to Screen, When to Refer. Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC
 Elevation of Serum Creatinine: When to Screen, When to Refer Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC Presented at the University of Calgary s CME and Professional Development 2006-2007
Elevation of Serum Creatinine: When to Screen, When to Refer Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC Presented at the University of Calgary s CME and Professional Development 2006-2007
Management of New-Onset Proteinuria in the Ambulatory Care Setting. Akinlolu Ojo, MD, PhD, MBA
 Management of New-Onset Proteinuria in the Ambulatory Care Setting Akinlolu Ojo, MD, PhD, MBA Urine dipstick results Negative Trace between 15 and 30 mg/dl 1+ between 30 and 100 mg/dl 2+ between 100 and
Management of New-Onset Proteinuria in the Ambulatory Care Setting Akinlolu Ojo, MD, PhD, MBA Urine dipstick results Negative Trace between 15 and 30 mg/dl 1+ between 30 and 100 mg/dl 2+ between 100 and
Lower Urinary Tract Infection (UTI) in Males
 Lower Urinary Tract Infection (UTI) in Males Clinical presentation For patients in care homes see UTI in adults where IV Antibiotics in the community may be appropriate (under development) History and
Lower Urinary Tract Infection (UTI) in Males Clinical presentation For patients in care homes see UTI in adults where IV Antibiotics in the community may be appropriate (under development) History and
Identifying and Managing Chronic Kidney Disease: A Practical Approach
 Identifying and Managing Chronic Kidney Disease: A Practical Approach S. Neil Finkle, MD, FRCPC Associate Professor Division of Nephrology, Department of Medicine, Dalhousie University Program Director,
Identifying and Managing Chronic Kidney Disease: A Practical Approach S. Neil Finkle, MD, FRCPC Associate Professor Division of Nephrology, Department of Medicine, Dalhousie University Program Director,
CHRONIC KIDNEY DISEASE DIAGNOSIS
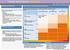 CHRONIC KIDNEY DISEASE DIAGSIS GFR categories, description and range WHO SHOULD BE TESTED FOR CKD CLASSIFICATION OF CKD USING egfr AND ACR CATEGORIES Offer testing for CKD using egfr, creatinine and ACR
CHRONIC KIDNEY DISEASE DIAGSIS GFR categories, description and range WHO SHOULD BE TESTED FOR CKD CLASSIFICATION OF CKD USING egfr AND ACR CATEGORIES Offer testing for CKD using egfr, creatinine and ACR
SERVICE SPECIFICATION 6 Conservative Management & End of Life Care
 SERVICE SPECIFICATION 6 Conservative Management & End of Life Care Table of Contents Page 1 Key Messages 2 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies
SERVICE SPECIFICATION 6 Conservative Management & End of Life Care Table of Contents Page 1 Key Messages 2 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies
CKD at the primary and secondary care interface. Paul Cockwell Consultant Nephrologist Clinical Service Lead Renal Medicine, QEHB
 CKD at the primary and secondary care interface Paul Cockwell Consultant Nephrologist Clinical Service Lead Renal Medicine, QEHB The Health improvement Network (THIN): 6.7 million patients from 426 primary
CKD at the primary and secondary care interface Paul Cockwell Consultant Nephrologist Clinical Service Lead Renal Medicine, QEHB The Health improvement Network (THIN): 6.7 million patients from 426 primary
What should you do next? Presenter Disclosure Information. Learning Objectives. Case: George
 2:45 3:45pm Optimizing the Management of Patients with Chronic Kidney Disease SPEAKER Jay B. Wish, MD, FACP Presenter Disclosure Information The following relationships exist related to this presentation:
2:45 3:45pm Optimizing the Management of Patients with Chronic Kidney Disease SPEAKER Jay B. Wish, MD, FACP Presenter Disclosure Information The following relationships exist related to this presentation:
Outpatient Management of Chronic Kidney Disease for the Internist
 Outpatient Management of Chronic Kidney Disease for the Internist Annual Meeting of Maryland Chapter of the American College of Physicians February 3, 2018 MARY (TESSIE) BEHRENS, MD, FACP, FASN, FNKF MID-ATLANTIC
Outpatient Management of Chronic Kidney Disease for the Internist Annual Meeting of Maryland Chapter of the American College of Physicians February 3, 2018 MARY (TESSIE) BEHRENS, MD, FACP, FASN, FNKF MID-ATLANTIC
CKD & HT. Anne-Marie Angus
 CKD & HT Anne-Marie Angus Hypertension definitions Persisting BP >140/90 and HBPM >135/85 Stage 1 >140/90 (HBPM >135/85) Stage 2 >160/100 (HBPM >150/90) Severe >180/100 White coat HT Why treat? A major
CKD & HT Anne-Marie Angus Hypertension definitions Persisting BP >140/90 and HBPM >135/85 Stage 1 >140/90 (HBPM >135/85) Stage 2 >160/100 (HBPM >150/90) Severe >180/100 White coat HT Why treat? A major
CKDinform: A PCP s Guide to CKD Detection and Delaying Progression
 CKDinform: A PCP s Guide to CKD Detection and Delaying Progression Learning Objectives Describe suitable screening tools, such as GFR and ACR, for proper utilization in clinical practice related to the
CKDinform: A PCP s Guide to CKD Detection and Delaying Progression Learning Objectives Describe suitable screening tools, such as GFR and ACR, for proper utilization in clinical practice related to the
Clinical guideline Published: 23 July 2014 nice.org.uk/guidance/cg182
 Chronic kidney disease in adults: assessment and management Clinical guideline Published: 23 July 2014 nice.org.uk/guidance/cg182 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Chronic kidney disease in adults: assessment and management Clinical guideline Published: 23 July 2014 nice.org.uk/guidance/cg182 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
National Chronic Kidney Disease Audit
 National Chronic Kidney Disease Audit // National Report: Part 2 December 2017 Commissioned by: Delivered by: // Foreword by Fiona Loud And if, as part of good, patient-centred care, a record of your condition(s),
National Chronic Kidney Disease Audit // National Report: Part 2 December 2017 Commissioned by: Delivered by: // Foreword by Fiona Loud And if, as part of good, patient-centred care, a record of your condition(s),
The role of the Nephrologist in Acute Kidney Injury. Rebecca Brown Consultant Nephrologist Royal Liverpool University Hospital
 The role of the Nephrologist in Acute Kidney Injury Rebecca Brown Consultant Nephrologist Royal Liverpool University Hospital Overview Impact of AKI Need for change Who needs a Nephrologist Are we making
The role of the Nephrologist in Acute Kidney Injury Rebecca Brown Consultant Nephrologist Royal Liverpool University Hospital Overview Impact of AKI Need for change Who needs a Nephrologist Are we making
Doncaster & Bassetlaw. AKI guidelines for primary care
 Doncaster & Bassetlaw AKI guidelines for primary care Contents: FLOW DIAGRAM: MANAGEMENT OF PATIENTS WITH AKI DETECTED IN PRIMARY CARE... 2 FLOW DIAGRAM: MANAGEMENT OF HYPERKALAEMIA.... 3 FLOW DIAGRAM:
Doncaster & Bassetlaw AKI guidelines for primary care Contents: FLOW DIAGRAM: MANAGEMENT OF PATIENTS WITH AKI DETECTED IN PRIMARY CARE... 2 FLOW DIAGRAM: MANAGEMENT OF HYPERKALAEMIA.... 3 FLOW DIAGRAM:
Chronic Kidney Disease
 Chronic Kidney Disease Chronic Kidney Disease (CKD) Educational Objectives Outline Demographics Propose Strategies to slow progression and improve outcomes Plan for treatment of CKD Chronic Kidney Disease
Chronic Kidney Disease Chronic Kidney Disease (CKD) Educational Objectives Outline Demographics Propose Strategies to slow progression and improve outcomes Plan for treatment of CKD Chronic Kidney Disease
The Health Problem: Guidelines: NHS Priority:
 PRIORITY BRIEFING The purpose of this briefing paper is to aid Stakeholders in prioritising topics to be taken further by PenCLAHRC as the basis for a specific evaluation or implementation research project.
PRIORITY BRIEFING The purpose of this briefing paper is to aid Stakeholders in prioritising topics to be taken further by PenCLAHRC as the basis for a specific evaluation or implementation research project.
Management of early chronic kidney disease
 Management of early chronic kidney disease GREENLANE SUMMER GP SYMPOSIUM 2018 Jonathan Hsiao Renal and General Physician Introduction A growing public health problem in NZ and throughout the world. Unknown
Management of early chronic kidney disease GREENLANE SUMMER GP SYMPOSIUM 2018 Jonathan Hsiao Renal and General Physician Introduction A growing public health problem in NZ and throughout the world. Unknown
Southern Derbyshire Shared Care Pathology Guidelines. AKI guidelines for primary care
 Southern Derbyshire Shared Care Pathology Guidelines AKI guidelines for primary care Contents: Flow Diagram: Recommended response time to AKI warning stage test results for adults in primary care 2 Table
Southern Derbyshire Shared Care Pathology Guidelines AKI guidelines for primary care Contents: Flow Diagram: Recommended response time to AKI warning stage test results for adults in primary care 2 Table
H(a)ematuria. FX Keeley Consultant Urologist Bristol Urological Institute
 H(a)ematuria FX Keeley Consultant Urologist Bristol Urological Institute From Philadelphia to Bristol, England Southmead Hospital, 1916 Southmead Hospital, 2013 Southmead Hospital, 2014 H(a)ematuria Blood
H(a)ematuria FX Keeley Consultant Urologist Bristol Urological Institute From Philadelphia to Bristol, England Southmead Hospital, 1916 Southmead Hospital, 2013 Southmead Hospital, 2014 H(a)ematuria Blood
Nephrology. 3 rd Year Revision Session 06/05/17 Cathal Hannan
 Nephrology 3 rd Year Revision Session 06/05/17 Cathal Hannan Aims Acute Kidney Injury-recognition and management Sample OSCE Station Clinically relevant renal physiology Aetiology of Chronic Kidney Disease
Nephrology 3 rd Year Revision Session 06/05/17 Cathal Hannan Aims Acute Kidney Injury-recognition and management Sample OSCE Station Clinically relevant renal physiology Aetiology of Chronic Kidney Disease
Primary Care Physicians and Clinicians. XXX on behalf of the Upper Midwest Fistula First Coalition. Chronic Kidney Disease (CKD) Resources
 August 10, 2007 To: From: RE: Primary Care Physicians and Clinicians XXX on behalf of the Upper Midwest Fistula First Coalition Chronic Kidney Disease (CKD) Resources Caring for patients with chronic kidney
August 10, 2007 To: From: RE: Primary Care Physicians and Clinicians XXX on behalf of the Upper Midwest Fistula First Coalition Chronic Kidney Disease (CKD) Resources Caring for patients with chronic kidney
Online clinical pathway for chronic kidney disease (CKD) in primary care. February 27, 2015 Dr. Kerry McBrien University of Calgary
 Online clinical pathway for chronic kidney disease (CKD) in primary care February 27, 2015 Dr. Kerry McBrien University of Calgary FACULTY/PRESENTER DISCLOSURE Faculty: Kerry McBrien Relationships with
Online clinical pathway for chronic kidney disease (CKD) in primary care February 27, 2015 Dr. Kerry McBrien University of Calgary FACULTY/PRESENTER DISCLOSURE Faculty: Kerry McBrien Relationships with
THE KIDNEY AND SLE LUPUS NEPHRITIS
 THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009
 The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
CHRONIC KIDNEY DISEASE DIAGNOSIS
 CHRONIC KIDNEY DISEASE DIAGSIS WHO SHOULD BE TESTED FOR CKD Offer testing for CKD using egfr, serum creatinine and urinary ACR to people with any of the following risk factors: diabetes hypertension acute
CHRONIC KIDNEY DISEASE DIAGSIS WHO SHOULD BE TESTED FOR CKD Offer testing for CKD using egfr, serum creatinine and urinary ACR to people with any of the following risk factors: diabetes hypertension acute
Special Challenges and Co-Morbidities
 Special Challenges and Co-Morbidities Renal Disease/ Hypertension/ Diabetes in African-Americans M. Keith Rawlings, MD Medical Director Peabody Health Center AIDS Arms, Inc Dallas, TX Chair, Internal Medicine
Special Challenges and Co-Morbidities Renal Disease/ Hypertension/ Diabetes in African-Americans M. Keith Rawlings, MD Medical Director Peabody Health Center AIDS Arms, Inc Dallas, TX Chair, Internal Medicine
Managing Patients with CKD in Primary Care: A Shared Care Pathway. 5 th April 2018
 Managing Patients with CKD in Primary Care: A Shared Care Pathway 5 th April 2018 Learning Objectives 1) What health risks does CKD represent? 2) Why change how we manage CKD in NWL? 1) How do we improve
Managing Patients with CKD in Primary Care: A Shared Care Pathway 5 th April 2018 Learning Objectives 1) What health risks does CKD represent? 2) Why change how we manage CKD in NWL? 1) How do we improve
Concept and General Objectives of the Conference: Prognosis Matters. Andrew S. Levey, MD Tufts Medical Center Boston, MA
 Concept and General Objectives of the Conference: Prognosis Matters Andrew S. Levey, MD Tufts Medical Center Boston, MA General Objectives Topics to discuss What are the key outcomes of CKD? What progress
Concept and General Objectives of the Conference: Prognosis Matters Andrew S. Levey, MD Tufts Medical Center Boston, MA General Objectives Topics to discuss What are the key outcomes of CKD? What progress
LRI Children s Hospital
 LRI Children s Hospital Management of Henoch Schönlein Purpura (HSP) in children Staff relevant to: Clinical staff working within the UHL Children s Hospital. Team approval date: July 2017 Version: V 3
LRI Children s Hospital Management of Henoch Schönlein Purpura (HSP) in children Staff relevant to: Clinical staff working within the UHL Children s Hospital. Team approval date: July 2017 Version: V 3
REFERRAL GUIDELINES: RENAL MEDICINE
 Outpatient Page 1 1 REFERRAL GUIDELINES: RENAL MEDICINE Demographic Clinical Date of birth Reason for referral Contact details (including mobile phone) Duration of symptoms Essential Referring GP details
Outpatient Page 1 1 REFERRAL GUIDELINES: RENAL MEDICINE Demographic Clinical Date of birth Reason for referral Contact details (including mobile phone) Duration of symptoms Essential Referring GP details
Objectives. Pre-dialysis CKD: The Problem. Pre-dialysis CKD: The Problem. Objectives
 The Role of the Primary Physician and the Nephrologist in the Management of Chronic Kidney Disease () By Brian Young, M.D. Assistant Clinical Professor of Medicine David Geffen School of Medicine at UCLA
The Role of the Primary Physician and the Nephrologist in the Management of Chronic Kidney Disease () By Brian Young, M.D. Assistant Clinical Professor of Medicine David Geffen School of Medicine at UCLA
Figure 1 LVH: Allowed Cost by Claim Volume (Data generated from a Populytics analysis).
 Chronic Kidney Disease (CKD): The New Silent Killer Nelson Kopyt D.O. Chief of Nephrology, LVH Valley Kidney Specialists For the past several decades, the health care needs of Americans have shifted from
Chronic Kidney Disease (CKD): The New Silent Killer Nelson Kopyt D.O. Chief of Nephrology, LVH Valley Kidney Specialists For the past several decades, the health care needs of Americans have shifted from
Diabetes and Kidney Disease. Kris Bentley Renal Nurse practitioner 2018
 Diabetes and Kidney Disease Kris Bentley Renal Nurse practitioner 2018 Aims Develop an understanding of Chronic Kidney Disease Understand how diabetes impacts on your kidneys Be able to recognise the risk
Diabetes and Kidney Disease Kris Bentley Renal Nurse practitioner 2018 Aims Develop an understanding of Chronic Kidney Disease Understand how diabetes impacts on your kidneys Be able to recognise the risk
Outline. Outline CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW 7/23/2013. Question 1: Which of these patients has CKD?
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Session 9: Optimizing the Management of Patients with Chronic Kidney Disease Learning Objectives
 Session 9: Optimizing the Management of Patients with Chronic Kidney Disease Learning Objectives 1. Understand the impact of chronic kidney disease (CKD) as a common condition of the adult US population.
Session 9: Optimizing the Management of Patients with Chronic Kidney Disease Learning Objectives 1. Understand the impact of chronic kidney disease (CKD) as a common condition of the adult US population.
Supplement: Summary of Recommendation Statements CHAPTER 1: DEFINITION AND CLASSIFICATION OF CKD
 Supplement: Summary of Recommendation Statements CHAPTER 1: DEFINITION AND CLASSIFICATION OF CKD 1.1 DEFINITION OF CKD 1.1.1: CKD is defined as abnormalities of kidney structure or function, present for
Supplement: Summary of Recommendation Statements CHAPTER 1: DEFINITION AND CLASSIFICATION OF CKD 1.1 DEFINITION OF CKD 1.1.1: CKD is defined as abnormalities of kidney structure or function, present for
UPDATE. Northern Ireland Guidelines for the Management of Chronic Kidney Disease (CKD)
 UPDATE Northern Ireland Guidelines for the Management of Chronic Kidney Disease (CKD) Practical Points for Use of Estimated GFR and Albuminuria (ACR) in Assessing CKD Developed by GAIN and the Northern
UPDATE Northern Ireland Guidelines for the Management of Chronic Kidney Disease (CKD) Practical Points for Use of Estimated GFR and Albuminuria (ACR) in Assessing CKD Developed by GAIN and the Northern
Haematuria and Modern Bladder Cancer Treatment
 Haematuria and Modern Bladder Cancer Treatment Mr Nikhil Vasdev MBBS MRCS MCh(Urol) FRCS(Urol) RCSEng/BAUS Robotic Fellowship Accredited and Trained Consultant Urological and Robotic Surgeon Hertfordshire
Haematuria and Modern Bladder Cancer Treatment Mr Nikhil Vasdev MBBS MRCS MCh(Urol) FRCS(Urol) RCSEng/BAUS Robotic Fellowship Accredited and Trained Consultant Urological and Robotic Surgeon Hertfordshire
London Strategic Clinical Networks. My AKI. Guidance for patients with, or recovering from, acute kidney injury
 London Strategic Clinical Networks My AKI Guidance for patients with, or recovering from, acute kidney injury Supporting the delivery of equitable, high quality AKI care through collaboration www.londonaki.net
London Strategic Clinical Networks My AKI Guidance for patients with, or recovering from, acute kidney injury Supporting the delivery of equitable, high quality AKI care through collaboration www.londonaki.net
5/10/2014. Observation, control of blood pressure. Observation, control of blood pressure and risk factors.
 Overview The Kidneys Nicola Barlow Clinical Biochemistry Department City Hospital Renal physiology Renal pathophysiology Acute kidney injury Chronic kidney disease Assessing renal function GFR Proteinuria
Overview The Kidneys Nicola Barlow Clinical Biochemistry Department City Hospital Renal physiology Renal pathophysiology Acute kidney injury Chronic kidney disease Assessing renal function GFR Proteinuria
Outline. Outline CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW. Question 1: Which of these patients has CKD?
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Appendix C: Renal Services Described for Non-physicians
 Appendix C: Renal Services Described for Non-physicians (Reproduced from the third edition of the Renal Association Standards document, August 2002.) This appendix provides information on the issues discussed
Appendix C: Renal Services Described for Non-physicians (Reproduced from the third edition of the Renal Association Standards document, August 2002.) This appendix provides information on the issues discussed
OUTLINE INTRODUCTION EPIDEMIOLOGY CLASSIFICATION DIAGNOSIS AETIOLOGY MANAGEMENT FINANCIAL BURDEN OF ESRD SCREENIG GUIDELINE CONCLUSION
 Dr O. A ADEJUMO OUTLINE INTRODUCTION EPIDEMIOLOGY CLASSIFICATION DIAGNOSIS AETIOLOGY MANAGEMENT FINANCIAL BURDEN OF ESRD SCREENIG GUIDELINE CONCLUSION Introduction Chronic Kidney Disease is defined as
Dr O. A ADEJUMO OUTLINE INTRODUCTION EPIDEMIOLOGY CLASSIFICATION DIAGNOSIS AETIOLOGY MANAGEMENT FINANCIAL BURDEN OF ESRD SCREENIG GUIDELINE CONCLUSION Introduction Chronic Kidney Disease is defined as
Acute Kidney Injury (AKI) Undergraduate nurse education
 Acute Kidney Injury (AKI) Undergraduate nurse education Year Three Developed Summer 2017 Objectives Understand Acute Kidney Injury and its relevance to patient care. Brief revision of the Anatomy and physiology
Acute Kidney Injury (AKI) Undergraduate nurse education Year Three Developed Summer 2017 Objectives Understand Acute Kidney Injury and its relevance to patient care. Brief revision of the Anatomy and physiology
Chronic Kidney Disease. Paul Cockwell Queen Elizabeth Hospital Birmingham
 Chronic Kidney Disease Paul Cockwell Queen Elizabeth Hospital Birmingham Paradigms for chronic disease 1. Acute and chronic disease is closely linked 2. Stratify risk and tailor interventions around failure
Chronic Kidney Disease Paul Cockwell Queen Elizabeth Hospital Birmingham Paradigms for chronic disease 1. Acute and chronic disease is closely linked 2. Stratify risk and tailor interventions around failure
Summary of Recommendation Statements Kidney International Supplements (2013) 3, 5 14; doi: /kisup
 http://www.kidney-international.org & 2013 DIGO Summary of Recommendation Statements idney International Supplements (2013) 3, 5 14; doi:10.1038/kisup.2012.77 Chapter 1: Definition and classification of
http://www.kidney-international.org & 2013 DIGO Summary of Recommendation Statements idney International Supplements (2013) 3, 5 14; doi:10.1038/kisup.2012.77 Chapter 1: Definition and classification of
Nephrology referral - Does my patient need it? Disclosure
 Nephrology referral - Does my patient need it? Sophia Chou, MD MSc March 10, 2018 Faculty: Sophia Chou Disclosure Relationships with commercial interest: None Potential conflict of interest: None 1 Objectives
Nephrology referral - Does my patient need it? Sophia Chou, MD MSc March 10, 2018 Faculty: Sophia Chou Disclosure Relationships with commercial interest: None Potential conflict of interest: None 1 Objectives
CKD IN THE CLINIC. Session Content. Recommendations for commonly used medications in CKD. CKD screening and referral
 CKD IN THE CLINIC Family Physician Refresher Course Lisa M. Antes, MD April 19, 2017 No disclosures Session Content 1. 2. Recommendations for commonly used medications in CKD Basic principles /patient
CKD IN THE CLINIC Family Physician Refresher Course Lisa M. Antes, MD April 19, 2017 No disclosures Session Content 1. 2. Recommendations for commonly used medications in CKD Basic principles /patient
Update on HIV-Related Kidney Diseases. Agenda
 Update on HIV-Related Kidney Diseases ANDY CHOI THE MEDICAL MANAGEMENT OF HIV/AIDS DECEMBER 15, 2006 Agenda 1. EPIDEMIOLOGY: A) END STAGE RENAL DISEASE (ESRD) B) CHRONIC KIDNEY DISEASE (CKD) 2. HIV-ASSOCIATED
Update on HIV-Related Kidney Diseases ANDY CHOI THE MEDICAL MANAGEMENT OF HIV/AIDS DECEMBER 15, 2006 Agenda 1. EPIDEMIOLOGY: A) END STAGE RENAL DISEASE (ESRD) B) CHRONIC KIDNEY DISEASE (CKD) 2. HIV-ASSOCIATED
WEEK. MPharm Programme. Acute Kidney Injury. Alan M. Green MPHM13: Acute Kidney Injury. Slide 1 of 47
 MPharm Programme Acute Kidney Injury Alan M. Green 2017 Slide 1 of 47 Overview Renal Function What is it? Why does it matter? What causes it? Who is at risk? What can we (Pharmacists) do? How do you recognise
MPharm Programme Acute Kidney Injury Alan M. Green 2017 Slide 1 of 47 Overview Renal Function What is it? Why does it matter? What causes it? Who is at risk? What can we (Pharmacists) do? How do you recognise
TREAT THE KIDNEY TO SAVE THE HEART. Leanna Tyshler, MD Chronic Kidney Disease Medical Advisor Northwest Kidney Centers February 2 nd, 2009
 TREAT THE KIDNEY TO SAVE THE HEART Leanna Tyshler, MD Chronic Kidney Disease Medical Advisor Northwest Kidney Centers February 2 nd, 2009 1 ESRD Prevalent Rates in 1996 per million population December
TREAT THE KIDNEY TO SAVE THE HEART Leanna Tyshler, MD Chronic Kidney Disease Medical Advisor Northwest Kidney Centers February 2 nd, 2009 1 ESRD Prevalent Rates in 1996 per million population December
Evaluation of Chronic Kidney Disease KDIGO. Paul E de Jong University Medical Center Groningen The Netherlands
 Evaluation of Chronic Kidney Disease Paul E de Jong University Medical Center Groningen The Netherlands Evaluation and Management of CKD 1. Definition and classification of CKD 2. Definition and impact
Evaluation of Chronic Kidney Disease Paul E de Jong University Medical Center Groningen The Netherlands Evaluation and Management of CKD 1. Definition and classification of CKD 2. Definition and impact
Outline. Outline. Introduction CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW 8/11/2011
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Autosomal Dominant Polycystic Kidney Disease
 I want to know more about... Autosomal Dominant Polycystic Kidney Disease together the answer This booklet is about autosomal dominant polycystic kidney disease (ADPKD). It is intended as a general guide
I want to know more about... Autosomal Dominant Polycystic Kidney Disease together the answer This booklet is about autosomal dominant polycystic kidney disease (ADPKD). It is intended as a general guide
Applying clinical guidelines treating and managing CKD
 Applying clinical guidelines treating and managing CKD Develop patient treatment plan according to level of severity. Source: Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012
Applying clinical guidelines treating and managing CKD Develop patient treatment plan according to level of severity. Source: Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012
ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS. Myriam Farah, MD, FRCPC
 ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS Myriam Farah, MD, FRCPC Clinical Assistant Professor Division of Nephrology, University of British Columbia November 2016 1. How to recognize acute
ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS Myriam Farah, MD, FRCPC Clinical Assistant Professor Division of Nephrology, University of British Columbia November 2016 1. How to recognize acute
Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease
 Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease Investigator Meeting 12 th September 2017 - Sheffield Prof Sunil Bhandari Consultant
Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease Investigator Meeting 12 th September 2017 - Sheffield Prof Sunil Bhandari Consultant
Reducing proteinuria
 Date written: May 2005 Final submission: October 2005 Author: Adrian Gillin Reducing proteinuria GUIDELINES a. The beneficial effect of treatment regimens that include angiotensinconverting enzyme inhibitors
Date written: May 2005 Final submission: October 2005 Author: Adrian Gillin Reducing proteinuria GUIDELINES a. The beneficial effect of treatment regimens that include angiotensinconverting enzyme inhibitors
Outline. Outline 10/14/2014 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW. Question 1: Which of these patients has CKD?
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Management of Nephrotic Syndrome
 Management of Nephrotic Syndrome 1. Introduction Incidence 2-4/100,000. Boys > girls 3:2; age of onset 2-6 years 80% of cases in children is due to minimal change (MCD) of which 80% will respond to steroid
Management of Nephrotic Syndrome 1. Introduction Incidence 2-4/100,000. Boys > girls 3:2; age of onset 2-6 years 80% of cases in children is due to minimal change (MCD) of which 80% will respond to steroid
DIABETES AND CHRONIC KIDNEY DISEASE
 DIABETES AND CHRONIC KIDNEY DISEASE Stages 1 4 www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes
DIABETES AND CHRONIC KIDNEY DISEASE Stages 1 4 www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes
Hot Topics in Diabetic Kidney Disease a primary care perspective
 Hot Topics in Diabetic Kidney Disease a primary care perspective DR SARAH DAVIES GP PARTNER WITH SPECIAL INTEREST IN DIABETES, CARDIFF DUK CLINICAL CHAMPION NB MEDICAL HOT TOPICS PRESENTER AND DIABETES
Hot Topics in Diabetic Kidney Disease a primary care perspective DR SARAH DAVIES GP PARTNER WITH SPECIAL INTEREST IN DIABETES, CARDIFF DUK CLINICAL CHAMPION NB MEDICAL HOT TOPICS PRESENTER AND DIABETES
Stages of Chronic Kidney Disease (CKD)
 Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Diabetes Mellitus. Eiman Ali Basheir. Mob: /1/2019
 Diabetes Mellitus Eiman Ali Basheir Mob: 091520385 27/1/2019 Learning Outcomes Discuss the WHO criteria for Diabetes Mellitus diagnosis Describe the steps taken to confirm diagnosis Interpret GTT. Discuss
Diabetes Mellitus Eiman Ali Basheir Mob: 091520385 27/1/2019 Learning Outcomes Discuss the WHO criteria for Diabetes Mellitus diagnosis Describe the steps taken to confirm diagnosis Interpret GTT. Discuss
Creatinine & egfr A Clinical Perspective. Suheir Assady MD, PhD Dept. of Nephrology & Hypertension RHCC
 Creatinine & egfr A Clinical Perspective Suheir Assady MD, PhD Dept. of Nephrology & Hypertension RHCC CLINICAL CONDITIONS WHERE ASSESSMENT OF GFR IS IMPORTANT Stevens et al. J Am Soc Nephrol 20: 2305
Creatinine & egfr A Clinical Perspective Suheir Assady MD, PhD Dept. of Nephrology & Hypertension RHCC CLINICAL CONDITIONS WHERE ASSESSMENT OF GFR IS IMPORTANT Stevens et al. J Am Soc Nephrol 20: 2305
6/10/2014. Chronic Kidney Disease - General management and standard of care. Management of CKD according to stage (KDOQI 2002)
 Chronic Kidney Disease - General management and standard of care Dr Nathalie Demoulin, Prof Michel Jadoul Cliniques universitaires Saint-Luc Université Catholique de Louvain What should and can be done
Chronic Kidney Disease - General management and standard of care Dr Nathalie Demoulin, Prof Michel Jadoul Cliniques universitaires Saint-Luc Université Catholique de Louvain What should and can be done
CKD: An update on recent developments. Robert Lewis Wessex Kidney Centre
 CKD: An update on recent developments Robert Lewis Wessex Kidney Centre Anatomy and functions of the kidney Calyces Key functions of the kidney Renal artery Renal vein Ureter Cortex Renal pelvis Medulla
CKD: An update on recent developments Robert Lewis Wessex Kidney Centre Anatomy and functions of the kidney Calyces Key functions of the kidney Renal artery Renal vein Ureter Cortex Renal pelvis Medulla
NICE Clinical Guideline 169 Acute Kidney Injury Local Implementation Gap Analysis
 NICE Clinical Guideline 169 Acute Kidney Injury Local Implementation Gap Analysis Please tick appropriate box in response to questions below and return to Michelle Timoney (michelle.timoney@nhs.net) by
NICE Clinical Guideline 169 Acute Kidney Injury Local Implementation Gap Analysis Please tick appropriate box in response to questions below and return to Michelle Timoney (michelle.timoney@nhs.net) by
Outline. Introduction. Outline CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW 6/26/2012
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Younger adults with a family history of premature artherosclerotic disease should have their cardiovascular risk factors measured.
 Appendix 2A - Guidance on Management of Hypertension Measurement of blood pressure All adults from 40 years should have blood pressure measured as part of opportunistic cardiovascular risk assessment.
Appendix 2A - Guidance on Management of Hypertension Measurement of blood pressure All adults from 40 years should have blood pressure measured as part of opportunistic cardiovascular risk assessment.
The CARI Guidelines Caring for Australians with Renal Impairment. 5. Classification of chronic kidney disease based on evaluation of kidney function
 5. Classification of chronic kidney disease based on evaluation of kidney function Date written: April 2005 Final submission: May 2005 GUIDELINES No recommendations possible based on Level I or II evidence
5. Classification of chronic kidney disease based on evaluation of kidney function Date written: April 2005 Final submission: May 2005 GUIDELINES No recommendations possible based on Level I or II evidence
Chronic Kidney Disease
 Page 1 of 10 View this article online at: patient.info/doctor/chronic-kidney-disease-pro Chronic Kidney Disease Synonym: chronic renal failure Chronic kidney disease (CKD) describes abnormal kidney function
Page 1 of 10 View this article online at: patient.info/doctor/chronic-kidney-disease-pro Chronic Kidney Disease Synonym: chronic renal failure Chronic kidney disease (CKD) describes abnormal kidney function
Children s Services Medical Guideline
 See also: NICE Guidelines These local guidelines are in conjunction with NICE UTI Algorithms Renal scarring and subsequent nephropathy are important causes of later hypertension and renal failure. Early
See also: NICE Guidelines These local guidelines are in conjunction with NICE UTI Algorithms Renal scarring and subsequent nephropathy are important causes of later hypertension and renal failure. Early
Chronic Kidney Disease. Basics of CKD Terms Diagnosis Management
 Chronic Kidney Disease Basics of CKD Terms Diagnosis Management Review the prevalence of chronic kidney disease (CKD) Review how CKD develops Review populations at risk for CKD Review CKD diagnosis Objectives
Chronic Kidney Disease Basics of CKD Terms Diagnosis Management Review the prevalence of chronic kidney disease (CKD) Review how CKD develops Review populations at risk for CKD Review CKD diagnosis Objectives
Chronic Kidney Disease due to Diabetes (Diabetic Nephropathy)
 Chronic Kidney Disease due to Diabetes (Diabetic Nephropathy) Patient information Oxford Kidney Unit If you have been told you have chronic kidney disease (CKD) due to diabetic nephropathy this leaflet
Chronic Kidney Disease due to Diabetes (Diabetic Nephropathy) Patient information Oxford Kidney Unit If you have been told you have chronic kidney disease (CKD) due to diabetic nephropathy this leaflet
Proteinuria (Protein in the Urine) Basics
 Proteinuria (Protein in the Urine) Basics OVERVIEW Proteinuria is the medical term for protein in the urine Urinary protein is detected by urine dipstick analysis, urinary protein: creatinine ratio (UP:C
Proteinuria (Protein in the Urine) Basics OVERVIEW Proteinuria is the medical term for protein in the urine Urinary protein is detected by urine dipstick analysis, urinary protein: creatinine ratio (UP:C
National Audit of CKD in Primary Care
 National Audit of CKD in Primary Care David C Wheeler Royal Free Campus University College London d.wheeler@ucl.ac.uk Kidney for General Physicians RCP London 24 th November 2017 Who looks after CKD patients
National Audit of CKD in Primary Care David C Wheeler Royal Free Campus University College London d.wheeler@ucl.ac.uk Kidney for General Physicians RCP London 24 th November 2017 Who looks after CKD patients
Mr PA. Clinical assessment of hydration. Poor urine output Sunken eyes Moistness of mucosa Cool peripheries Reduction in weight Postural hypotension
 X Anthony Warrens Mr PA 54 years old Previously well Went to Thailand Developed serious diarrhoea and vomiting two days before coming home 24 hours after return, still unwell GP found: urea 24 mmol/l creatinine
X Anthony Warrens Mr PA 54 years old Previously well Went to Thailand Developed serious diarrhoea and vomiting two days before coming home 24 hours after return, still unwell GP found: urea 24 mmol/l creatinine

 www.usrds.org www.usrds.org 1 1,749 + (2,032) 1,563 to
www.usrds.org www.usrds.org 1 1,749 + (2,032) 1,563 to