NORTHERN IRELAND GUIDELINES FOR MANAGEMENT OF CHRONIC KIDNEY DISEASE
|
|
|
- Marsha Powers
- 6 years ago
- Views:
Transcription
1 NORTHERN IRELAND GUIDELINES FOR MANAGEMENT OF CHRONIC KIDNEY DISEASE Practical points for use of estimated GFR + quality outcome framework indicators Developed by GAIN and the Northern Ireland Nephrology Forum February 2010
2
3 PREFACE Northern Ireland Guidelines for Management of Chronic Kidney Disease. These guidelines have been published by the Guidelines & Audit Implementation Network (GAIN), which is a team of health care professionals established under the auspices of the Department of Health, Social Services & Public Safety in The aim of GAIN is to promote quality in the Health Service in Northern Ireland, through audit and guidelines, while ensuring the highest possible standard of clinical practice is maintained. This guideline was produced by a sub-group of health care professionals from varied backgrounds and was chaired by Professor Peter Maxwell, Consultant in the Belfast HSC Trust. This guideline revises and updates the original guideline on Chronic Kidney Disease published in July 2006 under the auspices of CREST (Clinical Efficiency Support Team), the predecessor to GAIN. GAIN wishes to thank clinicians from the Northern Ireland Nephrology Forum, General Practice, and all those who contributed in any way to the development of these guidelines. Dr T Trinick Chairman of GAIN 1
4
5 CONTENTS Foreword 5 Introduction 6 What is CKD and egfr (estimated Glomerular 7 Filtration Rate)? What causes CKD? 9 Why does it matter? 9 What baseline investigations should I do in CKD? 10 How do I test for proteinuria? 11 What should I do if haematuria is present? 12 Which CKD patients should I consider 14 referring to the Renal Services? When should a kidney ultrasound be 15 performed in persons with CKD? What treatments are appropriate for CKD? 16 How should I monitor non-referred CKD? 17 What about a rise in serum creatinine 18 or a fall in egfr? Do I need to screen anyone for CKD? 19 3
6 Urgency of referral to a nephrology service 20 Valuable information to include with 22 a hospital referral Appendix Where can I get more information? 24 Who may I contact for further advice? 26 Management of chronic kidney disease: summary table 27 Abbreviations ACEi: angiotensin converting enzyme inhibitor ACR: urine albumin/creatinine ratio ARB: angiotensin-ii receptor blocker PCR: urine protein/creatinine ratio NSAIDs: non-steroidal anti-inflammatory drugs egfr: estimated glomerular filtration rate MDRD: modification of diet in renal disease 4
7 FOREWORD Chronic kidney disease is common with approximately 5% of adults having an abnormal glomerular filtration rate of less than 60 ml/min/1.73m 2. Recognition of chronic kidney disease has improved with the routine reporting of an estimated glomerular filtration rate (egfr) each time serum creatinine is measured. The introduction of kidney specific Quality Outcome Framework (QOF) indicators has helped to increase awareness of chronic kidney disease in primary care. The QOF indicators emphasize the importance of identifying persons with chronic kidney disease and treating associated risk factors for progressive kidney failure such as diabetes and hypertension. These guidelines update the previous 2006 CREST Guidelines for the Management of Chronic Kidney Disease in Adults. The changes in the updated document reflect current NICE guidance and include advice on assessment of chronic kidney disease, appropriate referral of patients with declining kidney function for specialist help and the use of quantitative measures of proteinuria. I would like to thank clinicians from the Northern Ireland Nephrology Forum, GP colleagues, Dr Joanne Shields, Specialist Registrar in Renal Medicine and the staff from GAIN for their enthusiastic help in producing this updated guidance. Prof Peter Maxwell Professor of Renal Medicine / Consultant Nephrologist 5
8 INTRODUCTION Chronic kidney disease (CKD) is common, usually unrecognised and often exists in association with other conditions such as diabetes and cardiovascular disease. CKD has emerged as a significant public health problem with up to 10% of adults having evidence of underlying CKD or risk factors for CKD. There is evidence that earlier treatment may delay or prevent progression of CKD. One challenging issue is that CKD is often not diagnosed because persons with kidney disease usually have no specific symptoms. Late diagnosis of advanced CKD is associated with increased morbidity and mortality. CKD is now incorporated in the General Practice Quality and Outcomes Framework (QOF) with an increase in both the number and value of CKD QOFs since April Specifically five QOF indicators (accounting for 38 points) are recorded based upon generation of a register of patients with chronic kidney disease, measurement of blood pressure, treatment of blood pressure to target, use (if appropriate) of ACEi or ARB medication in patients with CKD and quantitative assessment of proteinuria. This booklet provides brief guidance on investigation, monitoring and management of CKD in adults. It replaces the Northern Ireland CREST guidelines on the management of chronic kidney disease published in Approximate equivalent values of ACR, PCR and urinary protein excretion ACR (mg/mmol) PCR (mg/mmol) Urinary protein excretion (g/24h)
9 WHAT IS CKD AND egfr (ESTIMATED GLOMERULAR FILTRATION RATE)? CKD can manifest as either reduced kidney function (reduced GFR) or urinary abnormalities (haematuria/proteinuria) or a combination of both. The international classification of CKD, based largely on estimated Glomerular Filtration Rate (egfr), has 5 classes of CKD. Patients with an egfr < 60 ml/min/1.73m 2 have CKD stage 3, 4 or 5 and are the focus of these guidelines and the revised QOF indicators. GFR in healthy young adults is approximately 100 ml/min/1.73m 2. An egfr result can be explained to patients as an approximate percentage of normal kidney function. egfr is an estimate of renal function (GFR) based on serum creatinine but also accounting for differences in gender, ethnicity and age. Laboratories report it whenever any creatinine is requested. If the egfr is 60 ml/min/1.73m 2 or greater, the diagnosis of CKD requires the presence of other kidney damage e.g. persistent proteinuria (albumin-creatinine ratio >30 mg/mmol), persistent non-visible (microscopic) haematuria or structural kidney disease e.g. polycystic kidney disease. 7
10 In Northern Ireland laboratories do not routinely report egfr > 60ml/min/1.73m 2. Thus, CKD stages 1 and 2 would require urinalysis or renal imaging to allow CKD definition. Stage Description egfr (ml/min/1.73m 2 ) Population Prevalence 1 CKD with normal GFR >90 3.3% + other kidney damage 2 Mild CKD and other kidney % damage 3a Mild to Moderate CKD % 3b Moderate to Severe CKD Severe CKD % 5 Established renal failure <15 or on 0.2% dialysis 8
11 WHAT CAUSES CKD? No specific cause is found in the majority of patients. Specific causes include conditions such as diabetes, atheromatous renal vascular disease, glomerulonephritis, pyelonephritis and polycystic kidney disease. In the absence of a specific diagnosis, it is most likely related to hypertensive or ischaemic kidney damage both of which become more common with advancing age. WHY DOES IT MATTER? The CKD staging system recognizes that patients with progressive kidney failure pass through a number of stages before reaching end-stage renal disease. Recognition of CKD allows earlier intervention to prevent dialysis and cardiovascular events. Persons with CKD stages 4 and 5 have higher risks for hospitalisation, cardiovascular events and premature death. Most persons with CKD stage 1-3 will be entirely asymptomatic. Very few persons with CKD 1-3 will end up on dialysis. Those at most risk of progression of kidney disease have higher blood pressure and more proteinuria. However, there is a substantial increased risk of cardiovascular events and premature death. 9
12 WHAT BASELINE INVESTIGATIONS SHOULD I DO IN CKD? In patients with newly identified reduced egfr (i.e. <60 ml/min/1.73m 2 ), the first step is to exclude acute kidney failure. Review of previous serum creatinine tests may allow confirmation that this is chronic disease. Otherwise the patient should have a repeat creatinine (egfr) within one week. Rapidly declining kidney function (over days to weeks) is acute kidney failure and urgent referral for assessment is advised. In all newly identified CKD patients the following should be checked at the earliest opportunity: blood pressure dipstick urinalysis random urine albumin-creatinine ratio or urine protein-creatinine ratio glucose, cholesterol and full blood count. 10
13 HOW DO I TEST FOR PROTEINURIA? Reagent strips for dipstick urinalysis provide a simple screening test but are not an accurate method of quantifying proteinuria. Reagent strips cannot detect low concentrations of albumin in the urine. Use a random urine albumin-creatinine ratio (ACR) to detect albuminuria. The urine ACR result may be normal (< 3 mg/mmol). The urine ACR may indicate microalbuminuria (3-30mg/mmol). Persistent microalbuminuria is the earliest clinical indicator of development of nephropathy in persons with diabetes. The urine ACR may indicate dipstick positive proteinuria (>30mg/mmol). A urine protein-creatinine ratio (PCR) >50mg/mmol also indicates dipstick positive proteinuria. Progression of renal failure (decline in GFR) and cardiovascular events are more common if albuminuria (or proteinuria) is present. Approximate equivalent values of ACR, PCR and urinary protein excretion ACR (mg/mmol) PCR (mg/mmol) Urinary protein excretion (g/24h)
14 WHAT SHOULD I DO IF HAEMATURIA IS PRESENT? Haematuria is a very common presentation in general practice with a prevalence of 2%. There is currently no evidence to justify screening of the general population. In 2008, excellent short clinical guidelines on assessment of haematuria were published by the British Association of Urological Surgeons and Renal Association and should be read in association with the summary in this GAIN document (web link listed in Appendix). The causes of haematuria vary with clinical presentation and age and in many such patients, particularly young adults, haematuria is transient and may be of no consequence. The most common causes are urological such as kidney or urinary tract malignancy, stones, inflammation, infection or hyperplasia of the prostate or bladder. Only 10% of patients with haematuria will have a renal parenchymal cause. In up to 60% no diagnosis will be found despite complete assessment. The following steps should be taken in the assessment of patients with haematuria: 1) Urinary tract infection should be excluded by absence of nitrite and leucocyte on dipstick and negative MSU. Urinalysis should be repeated following treatment of a UTI to ensure haematuria is not persistent. 2) History/Examination are there any findings that suggest a particular diagnosis? 3) Investigations: serum creatinine /egfr, urinary ACR, bone profile. 12
15 4) Referral criteria: Referral for urological evaluation including renal imaging and cystoscopy is required in all patients with significant haematuria as defined by: a) Any single episode of Visible Haematuria, otherwise known as macroscopic or gross haematuria, at any age. b) Non-Visible Haematuria, otherwise referred to as microscopic or dipstick positive haematuria, is significant if a single episode is symptomatic at any age (hesitancy, frequency, urgency, dysuria) or if it is persistent (defined as 2 out of 3 dipsticks positive) and aged over 40. If a urological cause is excluded a nephrology referral should be considered if the patient meets any of the CKD criteria for referral or has: Significant proteinuria (ACR >30mg/mmol or PCR >50mg/mmol =0.5g/24hr). Evidence of declining GFR (by >10ml/min at any stage within the previous 5 years or by >5ml/min within the last 1 year). Stage 4 or 5 CKD (egfr <30ml/min). Isolated haematuria (i.e. in the absence of significant proteinuria) with hypertension in those aged <40. Visible haematuria coinciding with intercurrent (usually upper respiratory tract) infection. In the event the above criteria are not met, haematuria itself (visible or non-visible) does not require nephrology referral. 13
16 WHICH CKD PATIENTS SHOULD I CONSIDER REFERRING TO THE RENAL SERVICE? General points Take into account the individual s wishes and comorbidities when considering referral to a specialist. Some individuals with advanced CKD (and their families) would not wish to consider renal replacement therapy e.g. dialysis and therefore referral may not be appropriate. Consider discussing management issues with a specialist (virtual referral) where it may not be necessary for a patient to attend for hospital-based assessment. Patients who seem too frail for dialysis may still be discussed as there are some non-dialytic management options. Based on egfr Patients with new CKD 5 (egfr <15 ml/min) should be discussed immediately. Patients with new CKD 4 (egfr ml/min) should be referred or discussed. Patients with deteriorating renal function confirmed on repeat testing (egfr decline by > 5 ml/min/1.73m 2 within 1 year or > 10 ml/min/1.73 m 2 within 5 years) should be referred routinely. Patients with egfr <60 ml/min/1.73m 2 + inadequately controlled blood pressure despite 2-3 antihypertensive agents should be referred routinely. 14
17 Based on proteinuria Patients with an ACR or PCR >300 mg/mmol and/or the nephrotic syndrome should be referred urgently. Patients with an ACR or PCR mg/mmol should be referred routinely. Patients with an ACR or PCR mg/mmol AND haematuria should be referred routinely. Clinical judgement may suggest other patients who should be referred, or a different degree of urgency. WHEN SHOULD A KIDNEY ULTRASOUND BE PERFORMED IN PERSONS WITH CKD? A kidney ultrasound is recommended for persons with CKD who: have progressive CKD have visible or non-visible haematuria have symptoms of urinary tract obstruction, have a family history of polycystic kidney disease and are aged over 20 have stage 4 or 5 CKD. 15
18 WHAT TREATMENTS ARE APPROPRIATE FOR CKD? Review existing medication. Stop NSAIDs. Adjust other medication dose(s) according to egfr using Appendix 3 in BNF. Treat blood pressure ideally to <130/80 mmhg. Multiple agents may be required and the threshold for starting treatment is 140/90 mmhg [140/85 mmhg is QOF target]. If urine albumin-creatinine ratio >100 mg/mmol treat blood pressure ideally to <125/75 mmhg. ACEi/ARBs are first choice therapy. Serum creatinine/egfr should be checked 7-10 days after starting, or increasing the dose of an ACE-i / ARB. These drugs may cause a rise in serum creatinine or fall in egfr. If serum creatinine increase is < 30% or egfr decrease is < 25% then the current dose can be tolerated, as long as it stabilises thereafter. Serum potassium up to 5.9 mmol/l can also be tolerated. Consider anti-platelet agents and statins to reduce cardiovascular risk. Standard cardiovascular risk tables markedly underestimate risk in CKD. Treat as an equivalent CHD risk factor as having diabetes. Advise lifestyle changes as appropriate: smoking cessation, reduction of obesity, increased exercise and reduce dietary salt intake to < 6 grams/day. In patients with diabetes mellitus HbA1c ideally should be <7%. 16
19 A NOTE OF CAUTION: Decline in GFR with age is incompletely understood at present and there is a need to refine and validate the MDRD based egfr equation especially when considering elderly (> 70 yr) patients with low egfr. The new CKD classification system will identify many elderly subjects with low egfr who do not have "true" kidney disease (as defined by steadily progressive kidney failure in association with other abnormal features such as proteinuria). Most CKD in the elderly is due to the cumulative effect of other disease states, especially hypertension and atherosclerosis. It is important not to unduly alarm elderly patients with a misplaced diagnosis of advanced kidney failure. HOW SHOULD I MONITOR NON-REFERRED CKD? A majority of patients with CKD do not need to be referred and are well managed in primary care. A CKD register should be established for CKD stages 3, 4 and 5 (QOF indicator) to allow re-call arrangements. This would include patients with mild proteinuria (ACR mg/mmol or PCR mg/mmol), isolated non-visible haematuria (after assessment by urology if appropriate see RA/BAUS guidelines 2008) and stable CKD 3/4. The attached table indicates suggested monitoring for these patients and some of the associated targets. 17
20 WHAT ABOUT A RISE IN SERUM CREATININE OR A FALL IN egfr? Large rises in creatinine (>30%) and the commensurate fall in egfr are associated with underlying renal vascular disease, heart failure treatment and the elderly. A falling egfr will require closer monitoring. A sustained fall in egfr (reduction of >10 ml/min/1.73m 2 ) should be confirmed by repeating serum creatinine/egfr within 1 month. Progressive CKD is usually defined by at least 3 egfrs over at least 90 days. Many CKD patients exhibit minor fluctuations in their serum creatinine/egfr (often linked to diuretic / ACE or ARB therapy or inter-current illness). Temporary cessation of ACEi or ARBs can often correct these changes if the patient is at risk of dehydration. However these agents are protective and should not be stopped indefinitely if vascular or renal protection is indicated. Chronic use of NSAIDs may be associated with progressive CKD; only use with caution and ideally only for short term. Patients with CKD should be referred if they have a SUSTAINED fall in GFR of > 5 ml/min/1.73m 2 per year. 18
21 DO I NEED TO SCREEN ANYONE FOR CKD? Any patient with diabetes mellitus, hypertension, ischaemic heart disease, heart failure, peripheral vascular disease, cerebrovascular disease or urinary tract abnormalities are more likely to have CKD and ideally should have their egfr checked annually. Urinalysis should be checked in the initial assessment of hypertension, diabetes, peripheral oedema, heart failure and multi-system disease. Urine ACR should be checked annually in diabetes patients. If urinalysis shows one or more plus proteinuria, a spot sample in a plain (white cap) tube should be sent for ACR or PCR. A 24h urine collection is not required. 19
22 URGENCY OF REFERRAL TO A NEPHROLOGY SERVICE All nephrology services should offer 24 h telephone access to qualified advice. A guide to referral urgency is below: Immediate Suspected ARF. ARF superimposed on CKD. Newly detected stage 5 CKD (GFR < 15 ml/min/1.73 m 2 ). Accelerated or malignant phase hypertension with suspicion of underlying kidney disease (or if there is no specialist hypertension service available locally). Hyperkalaemia, serum potassium >7.0 mmol/l. Urgent outpatient Nephrotic syndrome. Newly detected stage 4 CKD (unless known to be stable) or stable stage 5 CKD. Multisystem disease (e.g. SLE, systemic vasculitis) with evidence of kidney disease. Hyperkalaemia, serum potassium mmol/l (after exclusion of artefactual and treatable causes). 20
23 Routine outpatient Refractory hypertension (defined as sustained BP >160/90 mm Hg despite combination therapy with 3 drugs from complementary classes). Acute deterioration in kidney function (defined as a fall of egfr of >25% or rise of serum creatinine concentration of >30% from baseline) associated with use of ACEIs or ARBs. Proteinuria (urine protein:creatinine ratio >100 mg/mmol) without nephrotic syndrome. Proteinuria with haematuria. Stage 3 CKD with haematuria. Urologically unexplained visible (macroscopic) haematuria (with or without proteinuria). Stable stage 4 CKD. GP care +/- virtual nephrology support/advice Stable CKD stages 1, 2 and 3. Isolated non-visible (microscopic) haematuria (after negative urological evaluation). Isolated microalbuminuria in diabetes (albumin: creatinine ratio < 30mg/mmol). 21
24 VALUABLE INFORMATION TO INCLUDE WITH A HOSPITAL REFERRAL General medical history - particularly noting urinary symptoms, previous blood pressures, urine testing. Information on the patient s functional status and cognitive function is especially relevant if dialysis is being considered as a treatment option. Medication history. Examination e.g. blood pressure, presence of oedema, vascular disease findings. Urine dipstick result - and quantitation of dipstick positive proteinuria by urine albumin/creatinine ratio or protein/creatinine ratio. Blood tests - Full blood count, urea and electrolytes, calcium, albumin, phosphate, cholesterol. HbA1c (in diabetes). Previous tests of renal function with dates. Imaging:- results of renal imaging if undertaken (according to local circumstances, pre-ordering may speed assessment). 22
25 APPENDIX
26 WHERE CAN I GET MORE INFORMATION? National Institute for Health and Clinical Excellence guidelines for Chronic Kidney Disease (2008). Renal Association CKD eguide that is derived from NICE, SIGN and Renal Association guidelines. Easy to navigate website with multiple useful points about CKD. Renal Association website quick access to info about egfr and CKD stages with links to management. Website of the Edinburgh Renal Unit with may helpful articles on kidney disease that are suitable for both health care professionals and patients. BAUS%20Haematuria%20consensus%20guidelines%20July% pdf British Association of Urological Surgeons / Renal Association: Initial assessment of haematuria. Access to these guidelines and any future updates Guidelines and Audit Implementation Network (Northern Ireland). 24
27 The Guidelines and Audit Implementation Network (GAIN) website also displays other topic guidelines with relevance to the management of chronic kidney disease. These include: Guidance on the management of hypertension FAQs (CREST 2007) Guidelines on the use of the laboratory (GAIN 2008) Hyperkalaemia guidelines (GAIN 2009). 25
28 WHO MAY I CONTACT FOR FURTHER ADVICE? Contact your local nephrologist as listed below Altnagelvin and Tyrone County Hospitals: Dr PJ Garrett Tel peter.garrett@westerntrust.hscni.net Dr Y Kuan Tel ying.kuan@westerntrust.hscni.net Dr F Kelly Tel frank.kelly@westerntrust.hscni.net Dr M Elawad Tel mamoun.elawad@westerntrust.hscni.net Antrim Area Hospital: Dr JC Harron Tel camille.harron@northerntrust.hscni.net Dr RN Mullan Tel robert.mullan@northerntrust.hscni.net Dr R Cunningham Tel ronan.cunningham@northerntrust.hscni.net Belfast City Hospital: Dr JH Brown Tel henry.brown@belfasttrust.hscni.net Dr AE Courtney Tel aisling.courtney@belfasttrust.hscni.net Dr DG Fogarty Tel damian.fogarty@belfasttrust.hscni.net Dr PT McNamee Tel peter.mcnamee@belfasttrust.hscni.net Prof AP Maxwell Tel peter.maxwell@belfasttrust.hscni.net Dr WE Nelson Tel william.nelson@belfasttrust.hscni.net Dr JD Woods Tel jd.woods@belfasttrust.hscni.net Daisy Hill Hospital: Dr JC Harty Tel john.harty@southerntrust.hscni.net Dr PJ McKeveney Tel paul.mckeveney@southerntrust.hscni.net Dr NA Morgan Tel neal.morgan@southerntrust.hscni.net Ulster Hospital Dundonald: Dr JS Smyth Tel john.smyth@setrust.hscni.net Dr N Leonard Tel niall.leonard@setrust.hscni.net Dr AM Woodman Tel alastair.woodman@setrust.hscni.net 26
29 MANAGEMENT OF CHRONIC KIDNEY DISEASE (CKD) A diagnosis of CKD should not be made on the basis of a single biochemistry value or an acute rise in serum creatinine. Likewise if a patient is unwell, with rapidly deteriorating kidney function, they should be discussed or referred urgently. Stage egfr mls/min/1.73m 2 > 90 + albuminuria or haematuria albuminuria or haematuria Tests Annual U+E (including egfr) Annual urine ACR <15 As before but Check U&E now 3 monthly 6 weekly Treatment Treat BP to a target of < 130/80 (threshold to treat is 140/90 mmhg) ACEi or ARB if urine ACR > 30 mg/mmol in non-diabetic individual or ACR >3 in person with diabetes Statin if cardiovascular disease risk > 20% over 10 years Aspirin 75mg (if no contraindication) Advise lifestyle changes as appropriate Referral Fall in egfr by >5 ml/min/1.73m 2 per year Rise in serum creatinine >20% per year ± Urine ACR > 70 mg/mmol ± Systolic BP > 160 mmhg (despite treatment with multiple agents) Discussion with or referral to renal unit is usual Usually automatic (Unless not for active treatment based co-morbidity) Approximate equivalent values of ACR, PCR and urinary protein excretion ACR (mg/mmol) PCR (mg/mmol) Urinary protein excretion (g/24h)
30 NOTES 28
31
32 Further copies available from: GAIN Office Room C4.17, Castle Buildings, Stormont BELFAST, BT4 3SQ Tel: (028) Website: ISBN:
UPDATE. Northern Ireland Guidelines for the Management of Chronic Kidney Disease (CKD)
 UPDATE Northern Ireland Guidelines for the Management of Chronic Kidney Disease (CKD) Practical Points for Use of Estimated GFR and Albuminuria (ACR) in Assessing CKD Developed by GAIN and the Northern
UPDATE Northern Ireland Guidelines for the Management of Chronic Kidney Disease (CKD) Practical Points for Use of Estimated GFR and Albuminuria (ACR) in Assessing CKD Developed by GAIN and the Northern
QUICK REFERENCE FOR HEALTHCARE PROVIDERS
 KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus
 Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus 1 Contents Executive Summary... 3 How to Screen for Diabetic Nephropathy... 4 What to Measure... 4 Frequency
Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus 1 Contents Executive Summary... 3 How to Screen for Diabetic Nephropathy... 4 What to Measure... 4 Frequency
Chronic kidney disease (CKD) (Southampton pathway)
 Background information Patient information Key messages for this pathway Definitions and abbreviations used in this pathway Classification of CKD Diagnosis of CKD Summary of referral criteria Screening
Background information Patient information Key messages for this pathway Definitions and abbreviations used in this pathway Classification of CKD Diagnosis of CKD Summary of referral criteria Screening
Elevation of Serum Creatinine: When to Screen, When to Refer. Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC
 Elevation of Serum Creatinine: When to Screen, When to Refer Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC Presented at the University of Calgary s CME and Professional Development 2006-2007
Elevation of Serum Creatinine: When to Screen, When to Refer Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC Presented at the University of Calgary s CME and Professional Development 2006-2007
Management of early chronic kidney disease
 Management of early chronic kidney disease GREENLANE SUMMER GP SYMPOSIUM 2018 Jonathan Hsiao Renal and General Physician Introduction A growing public health problem in NZ and throughout the world. Unknown
Management of early chronic kidney disease GREENLANE SUMMER GP SYMPOSIUM 2018 Jonathan Hsiao Renal and General Physician Introduction A growing public health problem in NZ and throughout the world. Unknown
Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma. Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree
 Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree Topics CKD background egfr background Patient with egfr Referral Guidelines
Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree Topics CKD background egfr background Patient with egfr Referral Guidelines
CKD and risk management : NICE guideline
 CKD and risk management : NICE guideline 2008-2014 Shahed Ahmed Consultant Nephrologist shahed.ahmed@rlbuht.nhs.uk Key points : Changing parameters of CKD and NICE guidance CKD and age related change of
CKD and risk management : NICE guideline 2008-2014 Shahed Ahmed Consultant Nephrologist shahed.ahmed@rlbuht.nhs.uk Key points : Changing parameters of CKD and NICE guidance CKD and age related change of
CHRONIC KIDNEY DISEASE DIAGNOSIS
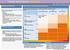 CHRONIC KIDNEY DISEASE DIAGSIS GFR categories, description and range WHO SHOULD BE TESTED FOR CKD CLASSIFICATION OF CKD USING egfr AND ACR CATEGORIES Offer testing for CKD using egfr, creatinine and ACR
CHRONIC KIDNEY DISEASE DIAGSIS GFR categories, description and range WHO SHOULD BE TESTED FOR CKD CLASSIFICATION OF CKD USING egfr AND ACR CATEGORIES Offer testing for CKD using egfr, creatinine and ACR
The National Quality Standards for Chronic Kidney Disease
 The National Quality Standards for Chronic Kidney Disease Dr Robert Lewis Chief of Service, Wessex Kidney Centre, Portsmouth Specialist Committee Member Quality Standard for Chronic Kidney Disease, NICE
The National Quality Standards for Chronic Kidney Disease Dr Robert Lewis Chief of Service, Wessex Kidney Centre, Portsmouth Specialist Committee Member Quality Standard for Chronic Kidney Disease, NICE
Identification, management and referral of adults with chronic kidney disease: concise guidelines
 Identification, management and referral of adults with chronic kidney disease: concise guidelines Abstract Chronic Kidney Disease (CKD) is often thought to be a relatively rare condition requiring specialist
Identification, management and referral of adults with chronic kidney disease: concise guidelines Abstract Chronic Kidney Disease (CKD) is often thought to be a relatively rare condition requiring specialist
Nice CKD Clinical Guidelines 2014 The challenges and benefits they may bring toprimary care
 Nice CKD Clinical Guidelines 2014 The challenges and benefits they may bring toprimary care Paula D Souza Senior CKD Nurse Specialist Royal Devon and Exeter Healthcare Trust Introduction Background What
Nice CKD Clinical Guidelines 2014 The challenges and benefits they may bring toprimary care Paula D Souza Senior CKD Nurse Specialist Royal Devon and Exeter Healthcare Trust Introduction Background What
Southern Derbyshire Shared Care Pathology Guidelines. AKI guidelines for primary care
 Southern Derbyshire Shared Care Pathology Guidelines AKI guidelines for primary care Contents: Flow Diagram: Recommended response time to AKI warning stage test results for adults in primary care 2 Table
Southern Derbyshire Shared Care Pathology Guidelines AKI guidelines for primary care Contents: Flow Diagram: Recommended response time to AKI warning stage test results for adults in primary care 2 Table
H(a)ematuria. FX Keeley Consultant Urologist Bristol Urological Institute
 H(a)ematuria FX Keeley Consultant Urologist Bristol Urological Institute From Philadelphia to Bristol, England Southmead Hospital, 1916 Southmead Hospital, 2013 Southmead Hospital, 2014 H(a)ematuria Blood
H(a)ematuria FX Keeley Consultant Urologist Bristol Urological Institute From Philadelphia to Bristol, England Southmead Hospital, 1916 Southmead Hospital, 2013 Southmead Hospital, 2014 H(a)ematuria Blood
Office Management of Reduced GFR Practical advice for the management of CKD
 Office Management of Reduced GFR Practical advice for the management of CKD CKD Online Education CME for Primary Care April 27, 2016 Monica Beaulieu, MD FRCPC MHA CHAIR PROVINCIAL KIDNEY CARE COMMITTEE
Office Management of Reduced GFR Practical advice for the management of CKD CKD Online Education CME for Primary Care April 27, 2016 Monica Beaulieu, MD FRCPC MHA CHAIR PROVINCIAL KIDNEY CARE COMMITTEE
5.2 Key priorities for implementation
 5.2 Key priorities for implementation From the full set of recommendations, the GDG selected ten key priorities for implementation. The criteria used for selecting these recommendations are listed in detail
5.2 Key priorities for implementation From the full set of recommendations, the GDG selected ten key priorities for implementation. The criteria used for selecting these recommendations are listed in detail
CHRONIC KIDNEY DISEASE DIAGNOSIS
 CHRONIC KIDNEY DISEASE DIAGSIS WHO SHOULD BE TESTED FOR CKD Offer testing for CKD using egfr, serum creatinine and urinary ACR to people with any of the following risk factors: diabetes hypertension acute
CHRONIC KIDNEY DISEASE DIAGSIS WHO SHOULD BE TESTED FOR CKD Offer testing for CKD using egfr, serum creatinine and urinary ACR to people with any of the following risk factors: diabetes hypertension acute
Professor Suetonia Palmer
 Professor Suetonia Palmer Department of Medicine Nephrologist Christchurch Hospital Christchurch 14:00-14:55 WS #108: The Kidney Test - When To Test and When to Refer ( and When Not To) 15:05-16:00 WS
Professor Suetonia Palmer Department of Medicine Nephrologist Christchurch Hospital Christchurch 14:00-14:55 WS #108: The Kidney Test - When To Test and When to Refer ( and When Not To) 15:05-16:00 WS
VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERENCE CARDS Chronic Kidney Disease
 VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERECE CARDS Chronic Kidney Disease CKD VA/DoD Clinical Practice Guideline for the Management
VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERECE CARDS Chronic Kidney Disease CKD VA/DoD Clinical Practice Guideline for the Management
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
CKD FOR INTERNISTS. Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College
 CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CKDinform: A PCP s Guide to CKD Detection and Delaying Progression
 CKDinform: A PCP s Guide to CKD Detection and Delaying Progression Learning Objectives Describe suitable screening tools, such as GFR and ACR, for proper utilization in clinical practice related to the
CKDinform: A PCP s Guide to CKD Detection and Delaying Progression Learning Objectives Describe suitable screening tools, such as GFR and ACR, for proper utilization in clinical practice related to the
Younger adults with a family history of premature artherosclerotic disease should have their cardiovascular risk factors measured.
 Appendix 2A - Guidance on Management of Hypertension Measurement of blood pressure All adults from 40 years should have blood pressure measured as part of opportunistic cardiovascular risk assessment.
Appendix 2A - Guidance on Management of Hypertension Measurement of blood pressure All adults from 40 years should have blood pressure measured as part of opportunistic cardiovascular risk assessment.
Online clinical pathway for chronic kidney disease (CKD) in primary care. February 27, 2015 Dr. Kerry McBrien University of Calgary
 Online clinical pathway for chronic kidney disease (CKD) in primary care February 27, 2015 Dr. Kerry McBrien University of Calgary FACULTY/PRESENTER DISCLOSURE Faculty: Kerry McBrien Relationships with
Online clinical pathway for chronic kidney disease (CKD) in primary care February 27, 2015 Dr. Kerry McBrien University of Calgary FACULTY/PRESENTER DISCLOSURE Faculty: Kerry McBrien Relationships with
Chronic Kidney Disease: Optimal and Coordinated Management
 Chronic Kidney Disease: Optimal and Coordinated Management Michael Copland, MD, FRCPC Presented at University of British Columbia s 42nd Annual Post Graduate Review in Family Medicine Conference, Vancouver,
Chronic Kidney Disease: Optimal and Coordinated Management Michael Copland, MD, FRCPC Presented at University of British Columbia s 42nd Annual Post Graduate Review in Family Medicine Conference, Vancouver,
Summary of Recommendation Statements Kidney International Supplements (2013) 3, 5 14; doi: /kisup
 http://www.kidney-international.org & 2013 DIGO Summary of Recommendation Statements idney International Supplements (2013) 3, 5 14; doi:10.1038/kisup.2012.77 Chapter 1: Definition and classification of
http://www.kidney-international.org & 2013 DIGO Summary of Recommendation Statements idney International Supplements (2013) 3, 5 14; doi:10.1038/kisup.2012.77 Chapter 1: Definition and classification of
Doncaster & Bassetlaw. AKI guidelines for primary care
 Doncaster & Bassetlaw AKI guidelines for primary care Contents: FLOW DIAGRAM: MANAGEMENT OF PATIENTS WITH AKI DETECTED IN PRIMARY CARE... 2 FLOW DIAGRAM: MANAGEMENT OF HYPERKALAEMIA.... 3 FLOW DIAGRAM:
Doncaster & Bassetlaw AKI guidelines for primary care Contents: FLOW DIAGRAM: MANAGEMENT OF PATIENTS WITH AKI DETECTED IN PRIMARY CARE... 2 FLOW DIAGRAM: MANAGEMENT OF HYPERKALAEMIA.... 3 FLOW DIAGRAM:
CKD at the primary and secondary care interface. Paul Cockwell Consultant Nephrologist Clinical Service Lead Renal Medicine, QEHB
 CKD at the primary and secondary care interface Paul Cockwell Consultant Nephrologist Clinical Service Lead Renal Medicine, QEHB The Health improvement Network (THIN): 6.7 million patients from 426 primary
CKD at the primary and secondary care interface Paul Cockwell Consultant Nephrologist Clinical Service Lead Renal Medicine, QEHB The Health improvement Network (THIN): 6.7 million patients from 426 primary
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012
 Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Chronic kidney disease screening and assessment
 Care map information Information resources for patients and carers Aboriginal and Torres Strait Islanders DEFINITION OF CKD egfr
Care map information Information resources for patients and carers Aboriginal and Torres Strait Islanders DEFINITION OF CKD egfr
Lower Urinary Tract Infection (UTI) in Males
 Lower Urinary Tract Infection (UTI) in Males Clinical presentation For patients in care homes see UTI in adults where IV Antibiotics in the community may be appropriate (under development) History and
Lower Urinary Tract Infection (UTI) in Males Clinical presentation For patients in care homes see UTI in adults where IV Antibiotics in the community may be appropriate (under development) History and
Primary Care Approach to Management of CKD
 Primary Care Approach to Management of CKD This PowerPoint was developed through a collaboration between the National Kidney Foundation and ASCP. Copyright 2018 National Kidney Foundation and ASCP Low
Primary Care Approach to Management of CKD This PowerPoint was developed through a collaboration between the National Kidney Foundation and ASCP. Copyright 2018 National Kidney Foundation and ASCP Low
Faculty/Presenter Disclosure
 CSI for CKD Unravelling the myths surrounding chronic kidney disease Practical Evidence for Informed Practice Oct 21 2016 Dr. Scott Klarenbach University of Alberta Slide 1: Option B (Presenter with NO
CSI for CKD Unravelling the myths surrounding chronic kidney disease Practical Evidence for Informed Practice Oct 21 2016 Dr. Scott Klarenbach University of Alberta Slide 1: Option B (Presenter with NO
Clinical guideline Published: 23 July 2014 nice.org.uk/guidance/cg182
 Chronic kidney disease in adults: assessment and management Clinical guideline Published: 23 July 2014 nice.org.uk/guidance/cg182 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Chronic kidney disease in adults: assessment and management Clinical guideline Published: 23 July 2014 nice.org.uk/guidance/cg182 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Chronic Kidney Disease
 Chronic Kidney Disease Presence of kidney damage or decreased kidney function for three or more months, - necessary to distinguish CKD from acute kidney disease. Ascertained either by kidney biopsy or
Chronic Kidney Disease Presence of kidney damage or decreased kidney function for three or more months, - necessary to distinguish CKD from acute kidney disease. Ascertained either by kidney biopsy or
Diabetes in Renal Patients. Contents. Understanding Diabetic Nephropathy
 Diabetes in Renal Patients Contents Understanding Diabetic Nephropathy What effect does CKD have on a patient s diabetic control? Diabetic Drugs in CKD and Dialysis Patients Hyper and Hypoglycaemia in
Diabetes in Renal Patients Contents Understanding Diabetic Nephropathy What effect does CKD have on a patient s diabetic control? Diabetic Drugs in CKD and Dialysis Patients Hyper and Hypoglycaemia in
Bulletin Independent prescribing information for NHS Wales
 Bulletin Independent prescribing information for NHS Wales October 2017 Chronic kidney disease Chronic kidney disease (CKD) is a long-term irreversible deterioration in the function of the kidneys, often
Bulletin Independent prescribing information for NHS Wales October 2017 Chronic kidney disease Chronic kidney disease (CKD) is a long-term irreversible deterioration in the function of the kidneys, often
Diabetes and Hypertension
 Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Diabetic Nephropathy. Objectives:
 There are, in truth, no specialties in medicine, since to know fully many of the most important diseases a man must be familiar with their manifestations in many organs. William Osler 1894. Objectives:
There are, in truth, no specialties in medicine, since to know fully many of the most important diseases a man must be familiar with their manifestations in many organs. William Osler 1894. Objectives:
Managing Patients with CKD in Primary Care: A Shared Care Pathway. 5 th April 2018
 Managing Patients with CKD in Primary Care: A Shared Care Pathway 5 th April 2018 Learning Objectives 1) What health risks does CKD represent? 2) Why change how we manage CKD in NWL? 1) How do we improve
Managing Patients with CKD in Primary Care: A Shared Care Pathway 5 th April 2018 Learning Objectives 1) What health risks does CKD represent? 2) Why change how we manage CKD in NWL? 1) How do we improve
Identifying and Managing Chronic Kidney Disease: A Practical Approach
 Identifying and Managing Chronic Kidney Disease: A Practical Approach S. Neil Finkle, MD, FRCPC Associate Professor Division of Nephrology, Department of Medicine, Dalhousie University Program Director,
Identifying and Managing Chronic Kidney Disease: A Practical Approach S. Neil Finkle, MD, FRCPC Associate Professor Division of Nephrology, Department of Medicine, Dalhousie University Program Director,
Haematuria and Modern Bladder Cancer Treatment
 Haematuria and Modern Bladder Cancer Treatment Mr Nikhil Vasdev MBBS MRCS MCh(Urol) FRCS(Urol) RCSEng/BAUS Robotic Fellowship Accredited and Trained Consultant Urological and Robotic Surgeon Hertfordshire
Haematuria and Modern Bladder Cancer Treatment Mr Nikhil Vasdev MBBS MRCS MCh(Urol) FRCS(Urol) RCSEng/BAUS Robotic Fellowship Accredited and Trained Consultant Urological and Robotic Surgeon Hertfordshire
REFERRAL GUIDELINES: RENAL MEDICINE
 Outpatient Page 1 1 REFERRAL GUIDELINES: RENAL MEDICINE Demographic Clinical Date of birth Reason for referral Contact details (including mobile phone) Duration of symptoms Essential Referring GP details
Outpatient Page 1 1 REFERRAL GUIDELINES: RENAL MEDICINE Demographic Clinical Date of birth Reason for referral Contact details (including mobile phone) Duration of symptoms Essential Referring GP details
CLINICAL GUIDELINE. Document No:CG38 *All Sites Management of adult patients referred to South Tees University Hospitals for hypertension.
 GUIDELINE CLINICAL GUIDELINE Document No:CG38 *All Sites Management of adult patients referred to South Tees University Hospitals for hypertension. TITLE Management of adult patients referred to South
GUIDELINE CLINICAL GUIDELINE Document No:CG38 *All Sites Management of adult patients referred to South Tees University Hospitals for hypertension. TITLE Management of adult patients referred to South
Type 2 Diabetes. Stopping Smoking. Consider referral to smoking cessation. Consider referring for weight management advice.
 Type 2 Diabetes Stopping Smoking Consider referral to smoking cessation BMI > 25 kg m² Set a weight loss target of a 5-10% reduction Consider referring for weight management advice Control BP to
Type 2 Diabetes Stopping Smoking Consider referral to smoking cessation BMI > 25 kg m² Set a weight loss target of a 5-10% reduction Consider referring for weight management advice Control BP to
POTENTIAL LINKAGES BETWEEN THE QUALITY AND OUTCOMES FRAMEWORK (QOF) AND THE NHS HEALTH CHECK
 POTENTIAL LINKAGES BETWEEN THE QUALITY AND OUTCOMES FRAMEWORK (QOF) AND THE NHS HEALTH CHECK Author: CHARLOTTE SIMPSON, SPECIALTY REGISTAR PUBLIC HEALTH (ST3), CHESHIRE EAST COUNCIL/MERSEY DEANERY SUMMARY
POTENTIAL LINKAGES BETWEEN THE QUALITY AND OUTCOMES FRAMEWORK (QOF) AND THE NHS HEALTH CHECK Author: CHARLOTTE SIMPSON, SPECIALTY REGISTAR PUBLIC HEALTH (ST3), CHESHIRE EAST COUNCIL/MERSEY DEANERY SUMMARY
CKD & HT. Anne-Marie Angus
 CKD & HT Anne-Marie Angus Hypertension definitions Persisting BP >140/90 and HBPM >135/85 Stage 1 >140/90 (HBPM >135/85) Stage 2 >160/100 (HBPM >150/90) Severe >180/100 White coat HT Why treat? A major
CKD & HT Anne-Marie Angus Hypertension definitions Persisting BP >140/90 and HBPM >135/85 Stage 1 >140/90 (HBPM >135/85) Stage 2 >160/100 (HBPM >150/90) Severe >180/100 White coat HT Why treat? A major
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009
 The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
Supplement: Summary of Recommendation Statements CHAPTER 1: DEFINITION AND CLASSIFICATION OF CKD
 Supplement: Summary of Recommendation Statements CHAPTER 1: DEFINITION AND CLASSIFICATION OF CKD 1.1 DEFINITION OF CKD 1.1.1: CKD is defined as abnormalities of kidney structure or function, present for
Supplement: Summary of Recommendation Statements CHAPTER 1: DEFINITION AND CLASSIFICATION OF CKD 1.1 DEFINITION OF CKD 1.1.1: CKD is defined as abnormalities of kidney structure or function, present for
Primary hypertension in adults
 Primary hypertension in adults NICE provided the content for this booklet which is independent of any company or product advertised Hypertension Welcome NICE published an updated guideline on the diagnosis
Primary hypertension in adults NICE provided the content for this booklet which is independent of any company or product advertised Hypertension Welcome NICE published an updated guideline on the diagnosis
Nephrology. 3 rd Year Revision Session 06/05/17 Cathal Hannan
 Nephrology 3 rd Year Revision Session 06/05/17 Cathal Hannan Aims Acute Kidney Injury-recognition and management Sample OSCE Station Clinically relevant renal physiology Aetiology of Chronic Kidney Disease
Nephrology 3 rd Year Revision Session 06/05/17 Cathal Hannan Aims Acute Kidney Injury-recognition and management Sample OSCE Station Clinically relevant renal physiology Aetiology of Chronic Kidney Disease
Outline. Outline CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW 7/23/2013. Question 1: Which of these patients has CKD?
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Stages of Chronic Kidney Disease (CKD)
 Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Management of Hypertension. M Misra MD MRCP (UK) Division of Nephrology University of Missouri School of Medicine
 Management of Hypertension M Misra MD MRCP (UK) Division of Nephrology University of Missouri School of Medicine Disturbing Trends in Hypertension HTN awareness, treatment and control rates are decreasing
Management of Hypertension M Misra MD MRCP (UK) Division of Nephrology University of Missouri School of Medicine Disturbing Trends in Hypertension HTN awareness, treatment and control rates are decreasing
What should you do next? Presenter Disclosure Information. Learning Objectives. Case: George
 2:45 3:45pm Optimizing the Management of Patients with Chronic Kidney Disease SPEAKER Jay B. Wish, MD, FACP Presenter Disclosure Information The following relationships exist related to this presentation:
2:45 3:45pm Optimizing the Management of Patients with Chronic Kidney Disease SPEAKER Jay B. Wish, MD, FACP Presenter Disclosure Information The following relationships exist related to this presentation:
Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease
 Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease Investigator Meeting 12 th September 2017 - Sheffield Prof Sunil Bhandari Consultant
Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease Investigator Meeting 12 th September 2017 - Sheffield Prof Sunil Bhandari Consultant
The evidence base for interventions to slow the progression of chronic kidney disease: Medical interventions. Jonathan Evans Paediatric Nephrologist
 The evidence base for interventions to slow the progression of chronic kidney disease: Medical interventions Jonathan Evans Paediatric Nephrologist CKD in adults Often unrecognised Preventable Major cardiovascular
The evidence base for interventions to slow the progression of chronic kidney disease: Medical interventions Jonathan Evans Paediatric Nephrologist CKD in adults Often unrecognised Preventable Major cardiovascular
ABCD and Renal Association Clinical Guidelines for Diabetic Nephropathy-CKD. Management of Dyslipidaemia and Hypertension in Adults Dr Peter Winocour
 ABCD and Renal Association Clinical Guidelines for Diabetic Nephropathy-CKD. Management of Dyslipidaemia and Hypertension in Adults Dr Peter Winocour Dr Indranil Dasgupta Rationale No national practical
ABCD and Renal Association Clinical Guidelines for Diabetic Nephropathy-CKD. Management of Dyslipidaemia and Hypertension in Adults Dr Peter Winocour Dr Indranil Dasgupta Rationale No national practical
Objectives. Pre-dialysis CKD: The Problem. Pre-dialysis CKD: The Problem. Objectives
 The Role of the Primary Physician and the Nephrologist in the Management of Chronic Kidney Disease () By Brian Young, M.D. Assistant Clinical Professor of Medicine David Geffen School of Medicine at UCLA
The Role of the Primary Physician and the Nephrologist in the Management of Chronic Kidney Disease () By Brian Young, M.D. Assistant Clinical Professor of Medicine David Geffen School of Medicine at UCLA
Management of New-Onset Proteinuria in the Ambulatory Care Setting. Akinlolu Ojo, MD, PhD, MBA
 Management of New-Onset Proteinuria in the Ambulatory Care Setting Akinlolu Ojo, MD, PhD, MBA Urine dipstick results Negative Trace between 15 and 30 mg/dl 1+ between 30 and 100 mg/dl 2+ between 100 and
Management of New-Onset Proteinuria in the Ambulatory Care Setting Akinlolu Ojo, MD, PhD, MBA Urine dipstick results Negative Trace between 15 and 30 mg/dl 1+ between 30 and 100 mg/dl 2+ between 100 and
Outline. Outline CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW. Question 1: Which of these patients has CKD?
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
New indicators to be added to the NICE menu for the QOF and amendments to existing indicators
 New indicators to be added to the for the QOF and amendments to existing indicators 1 st September 2015 Version 1.1 This document was originally published on 3 rd August 2015, it has since been updated.
New indicators to be added to the for the QOF and amendments to existing indicators 1 st September 2015 Version 1.1 This document was originally published on 3 rd August 2015, it has since been updated.
Diabetes Mellitus. Eiman Ali Basheir. Mob: /1/2019
 Diabetes Mellitus Eiman Ali Basheir Mob: 091520385 27/1/2019 Learning Outcomes Discuss the WHO criteria for Diabetes Mellitus diagnosis Describe the steps taken to confirm diagnosis Interpret GTT. Discuss
Diabetes Mellitus Eiman Ali Basheir Mob: 091520385 27/1/2019 Learning Outcomes Discuss the WHO criteria for Diabetes Mellitus diagnosis Describe the steps taken to confirm diagnosis Interpret GTT. Discuss
Quality ID #119 (NQF 0062): Diabetes: Medical Attention for Nephropathy National Quality Strategy Domain: Effective Clinical Care
 Quality ID #119 (NQF 0062): Diabetes: Medical Attention for Nephropathy National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS F INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process
Quality ID #119 (NQF 0062): Diabetes: Medical Attention for Nephropathy National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS F INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Process
 Quality ID #119 (NQF 0062): Diabetes: Medical Attention for Nephropathy National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Management of Chronic Conditions 2019 COLLECTION
Quality ID #119 (NQF 0062): Diabetes: Medical Attention for Nephropathy National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Management of Chronic Conditions 2019 COLLECTION
Outline. Outline. Introduction CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW 8/11/2011
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
SERVICE SPECIFICATION 6 Conservative Management & End of Life Care
 SERVICE SPECIFICATION 6 Conservative Management & End of Life Care Table of Contents Page 1 Key Messages 2 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies
SERVICE SPECIFICATION 6 Conservative Management & End of Life Care Table of Contents Page 1 Key Messages 2 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies
Chronic Kidney Disease. Paul Cockwell Queen Elizabeth Hospital Birmingham
 Chronic Kidney Disease Paul Cockwell Queen Elizabeth Hospital Birmingham Paradigms for chronic disease 1. Acute and chronic disease is closely linked 2. Stratify risk and tailor interventions around failure
Chronic Kidney Disease Paul Cockwell Queen Elizabeth Hospital Birmingham Paradigms for chronic disease 1. Acute and chronic disease is closely linked 2. Stratify risk and tailor interventions around failure
Diabetes and Kidney Disease. Kris Bentley Renal Nurse practitioner 2018
 Diabetes and Kidney Disease Kris Bentley Renal Nurse practitioner 2018 Aims Develop an understanding of Chronic Kidney Disease Understand how diabetes impacts on your kidneys Be able to recognise the risk
Diabetes and Kidney Disease Kris Bentley Renal Nurse practitioner 2018 Aims Develop an understanding of Chronic Kidney Disease Understand how diabetes impacts on your kidneys Be able to recognise the risk
Reframe the Paradigm of Hypertension treatment Focus on Diabetes
 Reframe the Paradigm of Hypertension treatment Focus on Diabetes Paola Atallah, MD Lecturer of Clinical Medicine SGUMC EDL monthly meeting October 25,2016 Overview Physiopathology of hypertension Classification
Reframe the Paradigm of Hypertension treatment Focus on Diabetes Paola Atallah, MD Lecturer of Clinical Medicine SGUMC EDL monthly meeting October 25,2016 Overview Physiopathology of hypertension Classification
Outline. Outline 10/14/2014 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW. Question 1: Which of these patients has CKD?
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Diabetic Kidney Disease: Update. GKA Master Class. Istanbul 2011
 Diabetic Kidney Disease: Update GKA Master Class Istanbul 2011 DKD: Challenging dogmas Old Dogmas Type 1 and Type 2 DN have the same natural history Microalbuminuria is an early stage of DN Tight Glycemia
Diabetic Kidney Disease: Update GKA Master Class Istanbul 2011 DKD: Challenging dogmas Old Dogmas Type 1 and Type 2 DN have the same natural history Microalbuminuria is an early stage of DN Tight Glycemia
Hypertension Clinical case scenarios for primary care
 Hypertension Clinical case scenarios for primary care Implementing NICE guidance August 2011 NICE clinical guideline 127 What this presentation covers Five clinical case scenarios, including: presentation
Hypertension Clinical case scenarios for primary care Implementing NICE guidance August 2011 NICE clinical guideline 127 What this presentation covers Five clinical case scenarios, including: presentation
Outline. Introduction. Outline CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW 6/26/2012
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Screen annually for patients with any of the following risk factors:
 CASE DEFINITION Chronic Kidney Disease (CKD) is either of the following, persisting for at least three months, repeated on at least two occasions: 1. Markers of kidney damage (e.g. proteinuria, haematuria
CASE DEFINITION Chronic Kidney Disease (CKD) is either of the following, persisting for at least three months, repeated on at least two occasions: 1. Markers of kidney damage (e.g. proteinuria, haematuria
WEEK. MPharm Programme. Acute Kidney Injury. Alan M. Green MPHM13: Acute Kidney Injury. Slide 1 of 47
 MPharm Programme Acute Kidney Injury Alan M. Green 2017 Slide 1 of 47 Overview Renal Function What is it? Why does it matter? What causes it? Who is at risk? What can we (Pharmacists) do? How do you recognise
MPharm Programme Acute Kidney Injury Alan M. Green 2017 Slide 1 of 47 Overview Renal Function What is it? Why does it matter? What causes it? Who is at risk? What can we (Pharmacists) do? How do you recognise
Hypertension diagnosis (see detail document) Diabetic. Target less than 130/80mmHg
 Hypertension diagnosis (see detail document) Non-diabetic Diabetic Very elderly (older than 80 years) Target less than 140/90mmHg Target less than 130/80mmHg Consider SBP target less than 150mmHg Non-diabetic
Hypertension diagnosis (see detail document) Non-diabetic Diabetic Very elderly (older than 80 years) Target less than 140/90mmHg Target less than 130/80mmHg Consider SBP target less than 150mmHg Non-diabetic
New Hypertension Guideline Recommendations for Adults July 7, :45-9:30am
 Advances in Cardiovascular Disease 30 th Annual Convention and Reunion UERM-CMAA, Inc. Annual Convention and Scientific Meeting July 5-8, 2018 New Hypertension Guideline Recommendations for Adults July
Advances in Cardiovascular Disease 30 th Annual Convention and Reunion UERM-CMAA, Inc. Annual Convention and Scientific Meeting July 5-8, 2018 New Hypertension Guideline Recommendations for Adults July
Renal Protection Staying on Target
 Update Staying on Target James Barton, MD, FRCPC As presented at the University of Saskatchewan's Management of Diabetes & Its Complications (May 2004) Gwen s case Gwen, 49, asks you to take on her primary
Update Staying on Target James Barton, MD, FRCPC As presented at the University of Saskatchewan's Management of Diabetes & Its Complications (May 2004) Gwen s case Gwen, 49, asks you to take on her primary
5/10/2014. Observation, control of blood pressure. Observation, control of blood pressure and risk factors.
 Overview The Kidneys Nicola Barlow Clinical Biochemistry Department City Hospital Renal physiology Renal pathophysiology Acute kidney injury Chronic kidney disease Assessing renal function GFR Proteinuria
Overview The Kidneys Nicola Barlow Clinical Biochemistry Department City Hospital Renal physiology Renal pathophysiology Acute kidney injury Chronic kidney disease Assessing renal function GFR Proteinuria
1. Albuminuria an early sign of glomerular damage and renal disease. albuminuria
 1. Albuminuria an early sign of glomerular damage and renal disease albuminuria Cardio-renal continuum REGRESS Target organ damage Asymptomatic CKD New risk factors Atherosclerosis Target organ damage
1. Albuminuria an early sign of glomerular damage and renal disease albuminuria Cardio-renal continuum REGRESS Target organ damage Asymptomatic CKD New risk factors Atherosclerosis Target organ damage
Figure 1 LVH: Allowed Cost by Claim Volume (Data generated from a Populytics analysis).
 Chronic Kidney Disease (CKD): The New Silent Killer Nelson Kopyt D.O. Chief of Nephrology, LVH Valley Kidney Specialists For the past several decades, the health care needs of Americans have shifted from
Chronic Kidney Disease (CKD): The New Silent Killer Nelson Kopyt D.O. Chief of Nephrology, LVH Valley Kidney Specialists For the past several decades, the health care needs of Americans have shifted from
Metformin should be considered in all patients with type 2 diabetes unless contra-indicated
 November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Nephrology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Nephrology 1. GOAL: Understand the general pediatrician's role in diagnosis and management of hypertension in children.
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Nephrology 1. GOAL: Understand the general pediatrician's role in diagnosis and management of hypertension in children.
Applying clinical guidelines treating and managing CKD
 Applying clinical guidelines treating and managing CKD Develop patient treatment plan according to level of severity. Source: Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012
Applying clinical guidelines treating and managing CKD Develop patient treatment plan according to level of severity. Source: Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012
Clinical guideline Published: 24 August 2011 nice.org.uk/guidance/cg127
 Hypertension in adults: diagnosis and management Clinical guideline Published: 24 August 2011 nice.org.uk/guidance/cg127 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Hypertension in adults: diagnosis and management Clinical guideline Published: 24 August 2011 nice.org.uk/guidance/cg127 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
LRI Children s Hospital
 LRI Children s Hospital Management of Henoch Schönlein Purpura (HSP) in children Staff relevant to: Clinical staff working within the UHL Children s Hospital. Team approval date: July 2017 Version: V 3
LRI Children s Hospital Management of Henoch Schönlein Purpura (HSP) in children Staff relevant to: Clinical staff working within the UHL Children s Hospital. Team approval date: July 2017 Version: V 3
ACE. Inhibitors. Quiz feedback
 ACE Inhibitors Quiz feedback bpac nz better medicin e bpac nz Quiz feedback, ACE inhibitors, 2006 Best Practice Advocacy Centre ACE inhibitors quiz feedback bpac nz Development Team: Rachael Clarke Sonia
ACE Inhibitors Quiz feedback bpac nz better medicin e bpac nz Quiz feedback, ACE inhibitors, 2006 Best Practice Advocacy Centre ACE inhibitors quiz feedback bpac nz Development Team: Rachael Clarke Sonia
CKD: An update on recent developments. Robert Lewis Wessex Kidney Centre
 CKD: An update on recent developments Robert Lewis Wessex Kidney Centre Anatomy and functions of the kidney Calyces Key functions of the kidney Renal artery Renal vein Ureter Cortex Renal pelvis Medulla
CKD: An update on recent developments Robert Lewis Wessex Kidney Centre Anatomy and functions of the kidney Calyces Key functions of the kidney Renal artery Renal vein Ureter Cortex Renal pelvis Medulla
Primary Care Physicians and Clinicians. XXX on behalf of the Upper Midwest Fistula First Coalition. Chronic Kidney Disease (CKD) Resources
 August 10, 2007 To: From: RE: Primary Care Physicians and Clinicians XXX on behalf of the Upper Midwest Fistula First Coalition Chronic Kidney Disease (CKD) Resources Caring for patients with chronic kidney
August 10, 2007 To: From: RE: Primary Care Physicians and Clinicians XXX on behalf of the Upper Midwest Fistula First Coalition Chronic Kidney Disease (CKD) Resources Caring for patients with chronic kidney
Introduction to Clinical Diagnosis Nephrology
 Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
Kidney Failure- Are you at risk?? ( 腎功能衰竭 - 你是在高危險群嗎?)
 Kidney Failure- Are you at risk?? ( 腎功能衰竭 - 你是在高危險群嗎?) Dr Goh Heong Keong, Penang www.passpaces.com/kidney.htm Outline of Lecture Introduction( 介紹 ) Definition of Chronic kidney disease( 慢性肾脏病的定义 ) Stages
Kidney Failure- Are you at risk?? ( 腎功能衰竭 - 你是在高危險群嗎?) Dr Goh Heong Keong, Penang www.passpaces.com/kidney.htm Outline of Lecture Introduction( 介紹 ) Definition of Chronic kidney disease( 慢性肾脏病的定义 ) Stages
Special Challenges and Co-Morbidities
 Special Challenges and Co-Morbidities Renal Disease/ Hypertension/ Diabetes in African-Americans M. Keith Rawlings, MD Medical Director Peabody Health Center AIDS Arms, Inc Dallas, TX Chair, Internal Medicine
Special Challenges and Co-Morbidities Renal Disease/ Hypertension/ Diabetes in African-Americans M. Keith Rawlings, MD Medical Director Peabody Health Center AIDS Arms, Inc Dallas, TX Chair, Internal Medicine
ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS. Myriam Farah, MD, FRCPC
 ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS Myriam Farah, MD, FRCPC Clinical Assistant Professor Division of Nephrology, University of British Columbia November 2016 1. How to recognize acute
ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS Myriam Farah, MD, FRCPC Clinical Assistant Professor Division of Nephrology, University of British Columbia November 2016 1. How to recognize acute
Chronic Kidney Disease
 Chronic Kidney Disease Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Guideline for the Identification
Chronic Kidney Disease Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Guideline for the Identification
Dr.Nahid Osman Ahmed 1
 1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
Tread Carefully Because you Tread on my Nephrons. Prescribing Hints in Renal Disease
 Tread Carefully Because you Tread on my Nephrons Prescribing Hints in Renal Disease David WP Lappin,, MB PhD FRCPI Clinical Lecturer in Medicine and Consultant Nephrologist and General Physician, Merlin
Tread Carefully Because you Tread on my Nephrons Prescribing Hints in Renal Disease David WP Lappin,, MB PhD FRCPI Clinical Lecturer in Medicine and Consultant Nephrologist and General Physician, Merlin
London Strategic Clinical Networks. My AKI. Guidance for patients with, or recovering from, acute kidney injury
 London Strategic Clinical Networks My AKI Guidance for patients with, or recovering from, acute kidney injury Supporting the delivery of equitable, high quality AKI care through collaboration www.londonaki.net
London Strategic Clinical Networks My AKI Guidance for patients with, or recovering from, acute kidney injury Supporting the delivery of equitable, high quality AKI care through collaboration www.londonaki.net
CHRONIC RENAL FAILURE: WHAT THE PRIMARY CARE CAN OFFER. The annual conference of the Lebanese Society of Family Medicine October 2017 Dr Hiba AZAR
 CHRONIC RENAL FAILURE: WHAT THE PRIMARY CARE CAN OFFER The annual conference of the Lebanese Society of Family Medicine October 2017 Dr Hiba AZAR OUTLINE: A journey through CKD Screening for CKD: The why,
CHRONIC RENAL FAILURE: WHAT THE PRIMARY CARE CAN OFFER The annual conference of the Lebanese Society of Family Medicine October 2017 Dr Hiba AZAR OUTLINE: A journey through CKD Screening for CKD: The why,
Chapter 1: CKD in the General Population
 Chapter 1: CKD in the General Population Overall prevalence of CKD (Stages 1-5) in the U.S. adult general population was 14.8% in 2011-2014. CKD Stage 3 is the most prevalent (NHANES: Figure 1.2 and Table
Chapter 1: CKD in the General Population Overall prevalence of CKD (Stages 1-5) in the U.S. adult general population was 14.8% in 2011-2014. CKD Stage 3 is the most prevalent (NHANES: Figure 1.2 and Table
