Renal Physiology. April, J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine.
|
|
|
- Hilary Townsend
- 5 years ago
- Views:
Transcription
1 Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010). Berne & Levy Physiology. 6th Edition. Mosby, Elsevier. Marieb, E. & Hoehn, K. (2010). Human Anatomy & Physiology. 8th Edition, Pearson, Benjamin Cummings. Stanfield, C.L. & Germann W.J. (2008). Principles of Human Physiology. 3rd Edition, Pearson, Benjamin Cummings. Hall, J.E. (2011). Guyton and Hall Textbook of Medical Physiology. 12th Edition, Elsevier, Saunders. April 04-07,
2 Physiology Objectives Objectives 1-5, PBL Booklet (See next page) Topics Body Fluid Compartments, Osmolarity, Osmolality & Tonicity and Membrane Transport Mechanisms. Review Ch. 1 : Principles of Cell Function Mechanisms of Membrane Transport, p 7-19 Ch. 2 : Homeostasis of Body Fluids Physiology Objectives Classify body fluid compartments with regard to their volume, relative percentages and percentage of body weight. Quantify the ionic components of the major body fluid compartments. Define osmolarity, osmolality and tonicity with respect to movement between intracellular and extracellular body fluid compartments. Review the various types of membrane transport (active transport, facilitated diffusion etc.) Explain the resultant effects on red blood cells which are added to hypotonic and hypertonic solutions. April 04-07,
3 Physiology Objectives cont d... Objectives 6-8, PBL Booklet Ch 32, Topic Functional Anatomy of the Kidneys, Physiology Objectives cont d... Review the gross and microscopic structure of the kidney and nephrons. Describe in detail the vascular arrangement of the kidneys. Give a detailed description of the structures encountered during the passage of the ultrafiltrate from the Bowman s capsule through the tubular segments into the renal pelvis. April 04-07,
4 Today s Topics Overview of ultrastructure of the Nephron, Renal Corpuscle, & Juxtaglomerular apparatus. Renal Clearance. Glomerular Filtration (GFR). Estimation of GFR- creatinine clearance. Clinical Importance. Composition of Ultrafiltrate. Determinants of Ultrafiltration. Dynamics of Ultrafiltration. Renal Blood Flow (RBF). Renal Autoregulation Mechanisms of Autoregulation Extrinsic Regulation of RBF & GFR (nerves & hormones). Functions of the Kidneys Regulatory 1. body fluid osmolality and volumes importance? 2. electrolyte balance importance? 3. acid-base balance importance? Excretory 1. metabolic products and foreign substances e.g. urea, uric acid, creatinine, Hb metabolism, hormone metabolites, drugs Endocrine 1. produce and secrete hormones e.g. renin, calcitriol, erythropoetin April 04-07,
5 Mechanisms of Urine Formation Urine formation and adjustment of blood composition involves three major processes Glomerular filtration Tubular reabsorption Secretion Figure 25.10; Marieb & Hoehn, 2010 Nephrons are the structural and functional units that form urine, consisting of: Renal Corpuscle Proximal Convoluted Tubule Loop of Henle Distal Convoluted Tubule Collecting Duct System The Nephron Figure 32.3, Koeppen & Stanton, 2010 April 04-07,
6 The Nephron Renal Corpuscle : Glomerulus a tuft of capillaries associated with a renal tubule Bowman s capsule blind, cup-shaped end of a renal tubule that completely surrounds the glomerulus The Nephron Unique cells in each nephron segment Figure 32.3; Koeppen & Stanton, 2010 April 04-07,
7 The Nephron All cells, (except intercalated cells), have in their apical plasma membrane a single nonmotile primary cilium that protrudes into the tubule fluid mechanosensors chemosensors initiate Ca2+-dependent signaling pathways, e.g. those that control kidney cell function, proliferation, differentiation, and apoptosis Types of Nephrons Cortical nephrons 85% of nephrons; located superficially in the cortex short LoH efferent arteriole peritubular capillaries nutrients delivers substances to the nephron for secretion path for return of reabsorbed H 20 & solutes to blood Figure 25.7; Marieb & Hoehn, 2010 April 04-07,
8 Types of Nephrons Juxtamedullary nephrons: located at the cortexmedulla junction long LoH efferent arteriole series of vascular loops called the vasa recta functions of peritubular capillaries + involved in the production of concentrated urine Figure 25.7; Marieb & Hoehn, 2010 Ultrastructure of the Renal Corpuscle first step in urine formation : passive movement of a plasma ultrafiltrate from glomerular capillaries Bowman's space ultrafiltration : passive movement of an essentially protein-free fluid from the glomerular capillaries Bowman's space April 04-07,
9 Ultrastructure of the Renal Corpuscle the glomerulus : network of capillaries supplied by the afferent arteriole and drained by the efferent arteriole capillaries covered by epithelial cells called podocytes (visceral layer of Bowman's capsule) visceral cells face outward at the vascular pole to form the parietal layer of Bowman's capsule space between the visceral layer and the parietal layer - Bowman's space - lumen of the PCT Figure 32.5; Koeppen & Stanton, 2010 Ultrastructure of the Renal Corpuscle Figure 25.9; Marieb & Hoehn, 2010 April 04-07,
10 Filtration Membrane endothelial cells of glomerular capillaries are covered by a basement membrane that is surrounded by podocytes capillary endothelium, basement membrane & foot processes of podocytes form the filtration barrier/membrane Figure 25.9; Marieb & Hoehn, 2010 Endothelium fenestrated - contains 700 Å holes, where 1 Å = m freely permeable to H 2 0, small solutes (such as Na+, urea, & glucose) & most proteins not permeable to RBC, WBC or platelets Filtration Membrane endothelial cells express negatively charged glycoproteins on their surface retard filtration of large anionic proteins into Bowman's space Figure 25.9; Marieb & Hoehn, 2010 April 04-07,
11 Filtration Membrane Basement membrane porous matrix of negatively charged proteins, ( type IV collagen, laminin, proteoglycans agrin & perlecan, & fibronectin) important filtration barrier to plasma proteins charge-selective filter Figure 25.9; Marieb & Hoehn, 2010 Filtration Membrane Podocytes long finger-like processes that completely encircle the outer surface of the capillaries processes of the podocytes interdigitate to cover the basement membrane separated by apparent gaps called filtration slits Figure 25.9; Marieb & Hoehn, 2010 April 04-07,
12 Filtration Membrane Filtration Slits each filtration slit bridged by a thin diaphragm that contains pores Å filtration slit diaphragm composed of several proteins nephrin (NPHS1), NEPH-1, podocin (NPHS2), α- actinin 4 (ACTN4) & CD2-AP function primarily as a sizeselective filter Figure 32.7; Koeppen & Stanton, 2010 Ultrastructure of the Renal Corpuscle Mesangium mesangial cells & matrix mesangial cells possess many properties of smooth muscle cells surround the glomerular capillaries provide structural support for the glomerular capillaries secrete the extracellular matrix Figure 32.5; Koeppen & Stanton, 2010 April 04-07,
13 Ultrastructure of the Renal Corpuscle Mesangium cont d... exhibit phagocytic activity by removing macromolecules from the mesangium secrete prostaglandins & proinflammatory cytokines mesangial cells contract & are adjacent to glomerular capillaries may influence the GFR by regulating blood flow through the glomerular capillaries or by altering the capillary surface area mesangial cells located outside the glomerulus - extraglomerular mesangial cells Ultrastructure of the Juxtaglomerular Apparatus JGA Involved in: tubulo-glomerular feedback mechanism (autoregulation of RBF and GFR) Comprises : 1. macula densa 2. extraglomerular mesangial cells 3. granular cells of the afferent arteriole (renin) Figure 32.5; Koeppen & Stanton, 2010 April 04-07,
14 Ultrastructure of the Juxtaglomerular Apparatus macula densa morphologically distinct region of the thick ascending limb (dct?) passes through the angle formed by the afferent and efferent arterioles of the same nephron cells contact the extraglomerular mesangial cells & granular cells of the afferent arterioles Figure 32.5; Koeppen & Stanton, 2010 Ultrastructure of the Juxtaglomerular Apparatus Granular cells manufacture, store & release renin contain smooth muscle myofilaments Figure 32.5; Koeppen & Stanton, 2010 April 04-07,
15 Innervation of the Kidneys renal nerves regulate RBF, GFR & salt & water reabsorption by the nephron sympathetic nerve fibers; no parasympathetic adrenergic fibers release norepinephrine & dopamine adrenergic fibers lie adjacent to the smooth muscle cells of the major branches of the renal artery & the afferent & efferent arterioles also, sympathetic nerves innervate the renin-producing granular cells of the afferent arterioles renin secretion nerve fibers also to PCT, LoH, DCT & collecting duct; Na+ reabsorption by these nephron segments Today s Topics Overview of ultrastructure of the Nephron, Renal Corpuscle, & Juxtaglomerular apparatus. Renal Clearance. Glomerular Filtration (GFR). Estimation of GFR- creatinine clearance. Clinical Importance. Composition of Ultrafiltrate. Determinants of Ultrafiltration. Dynamics of Ultrafiltration. Renal Blood Flow (RBF). Renal Autoregulation Mechanisms of Autoregulation Extrinsic Regulation of RBF & GFR (nerves & hormones). April 04-07,
16 Assessment of Renal Function The coordinated actions of the nephron's various segments determine the amount of a substance that appears in urine Depends on 3 processes : (1) glomerular filtration (2) reabsorption of the substance from tubular fluid back into blood (3) (in some cases) secretion of the substance from blood into tubule fluid Renal Clearance Renal clearance : theoretical basis for measurement of GFR & RBF based on the Fick principle (i.e., mass balance or conservation of mass) i.e. the amt substance entering organ= amt leaving organ, assuming no synthesis /degradation of substance by organ the renal artery is the single input source to the kidney, whereas the renal vein & ureter are the two output routes Figure 32.12; Koeppen & Stanton, 2010 April 04-07,
17 Renal Clearance P a x & P v x = concentrations of substance x in the renal artery & renal vein plasma, respectively RPFa & RPFv = renal plasma flow rates in the artery & vein, respectively U x = concentration of substance x in urine V (dot) = urine flow rate Figure 32.12; Koeppen & Stanton, 2010 Renal Clearance For any substance that is neither synthesized nor metabolized, the amount that enters the kidneys is = the amount that leaves the kidneys in urine + the amount that leaves the kidneys in renal venous blood allows measurement of the amount of substance x excreted in urine vs the amount returned to the systemic circulation in renal venous blood Figure 32.12; Koeppen & Stanton, 2010 April 04-07,
18 Renal Clearance C x = U x X V P x ml/min represents a volume of plasma from which all of substance x has been removed and excreted into urine per unit time i.e. rate of removal of substance x from plasma by kidneys Note : ratio of the amount of x excreted in urine to the amount of x in plasma Renal Clearance C x = U x X V Pa x ml/min E.g. if Ux = 100 mg/ml; V= 1 ml/min Then excretion rate of x = 100 mg/ml x 1 ml/min = 100 mg/min If Px = 1 mg.ml, then Cx = 100 mg/min 1 mg/ml = 100 ml/min April 04-07,
19 Today s Topics Overview of ultrastructure of the Nephron, Renal Corpuscle, & Juxtaglomerular apparatus. Renal Clearance. Glomerular Filtration (GFR). Estimation of GFR- creatinine clearance. Clinical Importance. Composition of Ultrafiltrate. Determinants of Ultrafiltration. Dynamics of Ultrafiltration. Renal Blood Flow (RBF). Renal Autoregulation Mechanisms of Autoregulation Extrinsic Regulation of RBF & GFR (nerves & hormones). Mechanisms of Urine Formation Urine formation and adjustment of blood composition involves three major processes Glomerular filtration Tubular reabsorption Secretion Figure 25.10; Marieb & Hoehn, 2010 April 04-07,
20 GFR Glomerular Filtration Rate (GFR) the sum of the filtration rates of all functioning nephrons index of kidney function quantity of glomerular filtrate formed each minute in all nephrons of both kidneys in normal adult male : ml/min in normal adult female : ml/min So, in 24 hours or 1 day, as much as 180 L of plasma is filtered by the glomeruli can be estimated using creatinine clearance test Estimation of GFR Creatinine byproduct of skeletal muscle creatine metabolism freely filtered across the glomerulus into Bowman's space not reabsorbed, secreted, or metabolized by the cells of the nephron April 04-07,
21 Estimation of GFR the amount of creatinine excreted in urine per minute = the amount of creatinine filtered at the glomerulus each minute where : P Cr = [plasma] creatinine U Cr = [urine] creatinine V = urine flow Figure 32.13; Koeppen & Stanton, 2010 Estimation of GFR From equation : GFR = U Cr X V P Cr where : P Cr = [plasma] creatinine U Cr = [urine] creatinine V = urine flow Figure 32.13; Koeppen & Stanton, 2010 April 04-07,
22 Estimation of GFR NB: this equation is the same form as that for clearance So, clearance of creatinine provides a means for determining the GFR Figure 32.13; Koeppen & Stanton, 2010 Estimation of GFR Creatinine is not the only substance that can be used to measure GFR Any substance that meets the following criteria can serve as an appropriate marker for the measurement of GFR The substance must: 1. Be freely filtered across the glomerulus into Bowman's space 2. Not be reabsorbed or secreted by the nephron 3. Not be metabolized or produced by the kidney 4. Not alter the GFR e.g. Inulin - fructose polymer- its clearance measures GFR April 04-07,
23 Filtration Fraction not all of the plasma coming into the kidneys is filtered approximately 10% of plasma that enters the kidneys in the renal artery does not pass through the glomerulus the portion of filtered plasma = filtration fraction Filtration Fraction = GFR RPF ~ Glomerular Filtration Rate Clinical Importance of GFR : measuring GFR is important when kidney disease is suspected : GFR may be the first & only clinical sign of kidney disease knowledge of the patient's GFR is essential in evaluating the severity and course of kidney disease GFR kidney disease is progressing GFR recuperation a 50% loss of functioning nephrons reduces the GFR only by about 25%; the decline in GFR is not 50% because the remaining nephrons compensate April 04-07,
24 Glomerular Filtration Rate Because measurements of GFR are cumbersome, kidney function is usually assessed in the clinical setting by measuring P Cr, which is inversely related to GFR BUT changes in P Cr are small : GFR from ml/min (~ 20%) is accompanied by an increase in P Cr from 1.0 to 1.2 mg/dl Figure 32.14; Koeppen & Stanton, 2010 Composition of Glomerular Filtrate first step in the formation of urine is ultrafiltration of plasma by the glomerulus the plasma ultrafiltrate = glomerular filtrate no cellular elements (i.e., RBC, WBC & platelets) no proteins [salts & organic molecules], e.g. glucose and amino acids, is similar to plasma Starling forces drive ultrafiltration across the glomerular capillaries and changes in these forces alter the GFR April 04-07,
25 Determinants of Ultrafiltrate Composition the glomerular filtration barrier determines the composition of the plasma ultrafiltrate it restricts the filtration of molecules on the basis of both size & electrical charge neutral molecules with a radius < 20 Å are filtered freely molecules > 42 Å are not filtered molecules between Å are filtered to various degrees, depending on their electrical charge e.g. cations Eg: serum albumin : an anionic protein molecular radius of 35.5 Å, (i.e. < 42 Å) BUT is filtered poorly (because of negative charges on it) Determinants of Ultrafiltrate Composition Clinical importance of the negative charges on the filtration barrier in restricting the filtration of plasma proteins : removal of the negative charges from the filtration barrier proteins filtered solely on the basis of their size at sizes between Å, filtration of polyanionic proteins > the filtration in the normal state E.g. glomerular diseases the negative charges on the filtration barrier are reduced because of immunological damage and inflammation filtration of proteins proteins appear in urine (proteinuria) April 04-07,
26 Determinants of Ultrafiltrate Composition Figure 32.16; Koeppen & Stanton, 2010 Dynamics of Ultrafiltration Ultrafiltration occurs because the Starling forces (i.e., hydrostatic and oncotic pressure) drive fluid from the lumen of glomerular capillaries, across the filtration barrier Bowman's space Figure 32.17; Koeppen & Stanton, 2010 April 04-07,
27 Dynamics of Ultrafiltration GFR is proportional to the sum of the Starling forces that exist across the capillaries [(PGC - PBS) σ (πgc - πbs)] multiplied by the ultrafiltration coefficient (Kf) GFR = Kf [(P GC - P BS) σ (π GC - π BS)] GFR = Kf x Net Filtration Pressure (NFP) Kf = the product of the intrinsic permeability of the glomerular capillary and the glomerular surface area available for filtration σ = reflection coefficient for proteins across the glomerular capillary = 1 Dynamics of Ultrafiltration the rate of glomerular filtration is > in glomerular capillaries than in systemic capillaries, mainly because Kf is approximately 100 times > in glomerular capillaries Also, P GC is approximately twice as great as the hydrostatic pressure in systemic capillaries April 04-07,
28 Dynamics of Ultrafiltration GFR can be altered by changing Kf or by changing any of the Starling forces ( NFP) In normal individuals, the GFR is regulated by alterations in P GC that are mediated mainly by changes in afferent or efferent arteriolar resistance P GC is affected in 3 ways: 1. Changes in afferent arteriolar resistance : resistance increases P GC & GFR (See D) resistance decreases P GC & GFR (See A) Dynamics of Ultrafiltration 2. Changes in efferent arteriolar resistance : resistance decreases P GC & GFR (See C) resistance increases P GC & GFR (See B) 3. Changes in renal arteriolar pressure : pressure transiently increases P GC GFR pressure transiently decreases P GC GFR Figure 32.21; Koeppen & Stanton, 2010 April 04-07,
29 Today s Topics Overview of ultrastructure of the Nephron, Renal Corpuscle, & Juxtaglomerular apparatus. Renal Clearance. Glomerular Filtration (GFR). Estimation of GFR- creatinine clearance. Clinical Importance. Composition of Ultrafiltrate. Determinants of Ultrafiltration. Dynamics of Ultrafiltration. Renal Blood Flow (RBF). Renal Autoregulation Mechanisms of Autoregulation Extrinsic Regulation of RBF & GFR (nerves & hormones). Renal Blood Flow Blood flow through the kidneys serves several important functions : 1. Indirectly determines the GFR 2. Modifies the rate of solute & H 2 0 reabsorption by the PCT 3. Participates in the concentration and dilution of urine 4. Delivers O 2, nutrients, and hormones to the cells of the nephron and returns CO 2 and reabsorbed fluid and solutes to the general circulation 5. Delivers substrates for excretion in urine April 04-07,
30 Renal Blood Flow Blood flow through any organ may be represented by : Q = P R where : Q = blood flow P = mean arterial pressure minus venous pressure for that organ R = resistance to flow through that organ Renal Blood Flow Renal Blood Flow (RBF) is equal to the pressure difference between the renal artery and the renal vein divided by renal vascular resistance: RBF = Aortic pressure renal venous pressure Renal vascular resistance April 04-07,
31 Renal Blood Flow arterial pressure RBF = Aortic pressure Renal venous pressure Renal vascular resistance afferent arteriole efferent arteriole interlobular artery RBF remains relatively constant ABP = mm Hg GFR is also regulated over the same range of ABP the phenomenon whereby RBF and GFR are maintained relatively constant = autoregulation achieved by in vascular resistance (afferent arterioles) Renal Blood Flow Figure 32.18; Koeppen & Stanton, 2010 April 04-07,
32 Autoregulation of RBF & GFR Two mechanisms : 1. Responds to changes in arterial pressure 2. Responds to changes in [NaCl] in tubular fluid Autoregulation of RBF & GFR Pressure mechanism : Myogenic Mechanism intrinsic property of vascular smooth muscle: the tendency to contract when stretched when arterial pressure rises and the renal afferent arteriole is stretched, the smooth muscle contracts Because the increase in resistance of the arteriole offsets the increase in pressure, RBF & therefore GFR remain constant (See equation for Renal Blood Flow) April 04-07,
33 Autoregulation of RBF & GFR [NaCl]-dependent mechanism : Tubuloglomerular Feedback [NaCl] in tubular fluid is sensed by the macula densa of the JGA & converted into a signal that affect afferent arteriolar resistance GFR Autoregulation of RBF & GFR formation & release of ATP & ADO vasoconstriction of afferent arteriole GFR to normal levels GFR [NaCl] NaCl enters the macula densa cells ATP & ADO production & release vasodilation of the afferent arteriole GFR Figure 32.19; Koeppen & Stanton, 2010 April 04-07,
34 Autoregulation of RBF & GFR Figure 32.20; Koeppen & Stanton, 2010 Autoregulation of RBF & GFR GFR [NaCl] in tubule fluid at the macula densa uptake of NaCl across the apical cell membrane of macula densa cells via the 1Na+-1K+-2Cl- (NKCC2) symporter [ATP] & [adenosine] (ADO) ATP binds to P2X receptors & ADO binds to adenosine A1 receptors in the plasma membrane of smooth muscle cells in afferent arteriole intracellular [Ca2+] vasoconstriction of the afferent GFR ATP & ADO also renin release by granular cells in the afferent arteriole via intracellular [Ca2+] in vascular smooth muscle (VSM) cells April 04-07,
35 Autoregulation of RBF & GFR GFR [NaCl] in tubule fluid uptake of NaCl into macula densa cells release of ATP & ADO intracellular [Ca2+] GFR release of ATP & ADO release of renin by granular cells Also, entry of NaCl into macula densa cells production of PGE2 renin secretion by granular cells NB: although ADO is a vasodilator in most other vascular beds, it constricts the afferent arteriole in the kidney Importance of Autoregulation many activities can change arterial blood pressure, so, we need mechanisms that maintain RBF & GFR relatively constant despite changes in arterial pressure if RBF & GFR or suddenly in proportion to changes in blood pressure urinary excretion of fluid and solute would also change suddenly; if no corresponding intake fluid & electrolyte imbalance autoregulation of RBF & GFR : provides an effective means for uncoupling renal function from arterial pressure ensures that fluid and solute excretion remain constant April 04-07,
36 Autoregulation of RBF & GFR 3 points concerning autoregulation should be noted : 1. Autoregulation is absent when arterial pressure is < 90 mm Hg 2. Autoregulation is not perfect; RBF & GFR do change slightly as arterial blood pressure varies 3. Despite autoregulation, RBF & GFR can be changed by certain hormones and by changes in sympathetic nerve activity Regulation of RBF & GFR Table 32-1; Koeppen & Stanton, 2010 April 04-07,
37 Can you predict the effect of these changes in afferent & efferent arterioles on P GC, GFR & RBF? Figure 32.21; Koeppen & Stanton, 2010 Regulation of RBF & GFR Constriction of the afferent arteriole (A) decreases PGC because less of the arterial pressure is transmitted to the glomerulus, thereby reducing GFR Constriction of the efferent arteriole (B) elevates PGC and thus increases GFR Dilation of the efferent arteriole (C) decreases PGC and thus decreases GFR Dilation of the afferent arteriole (D) increases PGC because more of the arterial pressure is transmitted to the glomerulus, thereby increasing GFR Figure 32.21; Koeppen & Stanton, 2010 April 04-07,
38 Sympathetic Nerves Regulation of RBF & GFR Dehydration or strong emotional stimuli, such as fear and pain sympathetic activity afferent & efferent arterioles innervated by sympathetic neurons sympathetic nerves release NE & dopamine circulating E secreted by adrenal medulla NE & E vasoconstriction by binding to α1-adrenoceptors mainly on afferent arterioles GFR & RBF Renalase from kidneys facilitates degradation of catecholamines Regulation of RBF & GFR Angiotensin II Ag II is produced systemically and locally within the kidneys constricts the afferent & efferent arterioles and decreases RBF & GFR efferent arteriole more sensitive to Ag II than afferent arteriole, so low [Ag II] constriction of efferent arteriole GFR & RBF high [Ag II] constriction of afferent & efferent arteriole GFR & RBF April 04-07,
39 Regulation of RBF & GFR blood vol ABP Figure 32.22; Koeppen & Stanton, 2010 Regulation of RBF & GFR Prostaglandins (PGs) : clinical importance PGs do not play a major role in regulating RBF in healthy, resting people However, during pathophysiological conditions e.g. hemorrhage, there is production of PGs (PGI2, PGE1 & PGE2) by kidneys ; PGs RBF without changing GFR PGs RBF by dampening the vasoconstrictor effects of sympathetic nerves & Ag II prevents severe & potentially harmful vasoconstriction & renal ischemia dehydration & stress (e.g., surgery, anesthesia), Ag II, & sympathetic nerves synthesis of PGs April 04-07,
40 Regulation of RBF & GFR Prostaglandins (PGs) : clinical importance non-steroidal anti-inflammatory drugs (NSAIDs), e.g. aspirin & ibuprofen synthesis of PGs administration of NSAIDs during renal ischemia and hemorrhagic shock is contraindicated because by blocking the production of prostaglandins, they decrease RBF & increase renal ischemia PGs play an increasingly important role in maintaining RBF & GFR as individuals age, so NSAIDs can significantly RBF & GFR in the elderly Nitric Oxide Regulation of RBF & GFR NO : an endothelium-derived relaxing factor (EDRF) important vasodilator under basal conditions counteracts vasoconstriction produced by Ag II & catecholamines blood flow increases greater shear force on endothelial cells in the arterioles production of NO ACh, histamine, bradykinin, & ATP facilitate release of NO from endothelial cells NO dilation of the afferent and efferent arterioles in the kidneys NO total peripheral resistance (TPR) NO TPR April 04-07,
41 Regulation of RBF & GFR Endothelin potent vasoconstrictor secreted by endothelial cells of the renal vessels, mesangial cells, and distal tubular cells in response to Ag II, bradykinin, epinephrine, and endothelial shear stress profound vasoconstriction of the afferent & efferent arterioles decreases GFR & RBF production of endothelin in a number of glomerular disease states (e.g., renal disease associated with diabetes mellitus) Regulation of RBF & GFR Bradykinin vasodilator that acts by stimulating the release of NO & PGs increases GFR & RBF kallikrein = proteolytic enzyme produced in the kidneys cleaves circulating kininogen to bradykinin Adenosine (ADO) produced within the kidneys vasoconstriction of the afferent arteriole GFR & RBF (see tubuloglomerular feedback) April 04-07,
42 Regulation of RBF & GFR Natriuretic Peptides secretion of ANP by cardiac atria & BNP by cardiac ventricle when ECF ANP & BNP dilate afferent arteriole & constrict efferent arteriole ANP & BNP produce a modest increase in GFR with little change in RBF Regulation of RBF & GFR Adenosine Triphosphate cells release ATP into the renal interstitial fluid ATP has dual effects on GFR & RBF under some conditions, ATP constricts the afferent arteriole, reduces RBF & GFR (tubuloglomerular feedback) ATP also may NO production & GFR & RBF Glucocorticoids therapeutic doses of glucocorticoids GFR & RBF April 04-07,
43 Regulation of RBF & GFR Histamine local release of histamine modulates RBF during the resting state and during inflammation and injury resistance of afferent and efferent arterioles RBF without elevating GFR Dopamine produced by PT RBF & renin secretion Regulation of RBF & GFR Figure 32.23; Koeppen & Stanton, 2010 NB : role of Angiotensin-converting enzyme (ACE) located on the surface of endothelial cells lining the afferent arteriole & glomerular capillaries converts Ag I to Ag II GFR & RBF Ag II also produced locally in granular cells in the afferent arteriole & PT cells April 04-07,
44 Regulation of RBF & GFR Clinical Importance of ACE ACE degrades & thereby inactivates bradykinin converts Ag I to Ag II ACE Ag II levels & bradykinin levels Drugs : ACE inhibitors (e.g., enalapril, captopril), Ag II levels & bradykinin levels systemic vascular resistance BP Ag II levels & bradykinin levels renal vascular resistance GFR & RBF therefore used to systemic blood pressure in hypertensive patients Regulation of RBF & GFR Clinical Importance of AgII receptor antagonists Ag II receptor antagonists (e.g., losartan) are also used to treat high blood pressure block the binding of Ag II to the Ag II receptor (AT1) block the vasoconstrictor effects of angiotensin II on the afferent arteriole; GFR & RBF Ag II receptor antagonists do not inhibit kinin metabolism (e.g., bradykinin) as do ACE inhibitors April 04-07,
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY
 RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Glomerular filtration rate (GFR)
 LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
MAJOR FUNCTIONS OF THE KIDNEY
 MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences. Body fluids and.
 By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences Body fluids and Renal physiology 25 Volume and Osmolality of Extracellular and Intracellular Fluids
By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences Body fluids and Renal physiology 25 Volume and Osmolality of Extracellular and Intracellular Fluids
Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph
 The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
Functions of the kidney
 Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Basic Functions of the Kidneys
 Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Urinary bladder provides a temporary storage reservoir for urine
 Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 17 Urinary System 2 Glomerular Filtration Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Overview of Renal Physiology
BIOH122 Human Biological Science 2 Session 17 Urinary System 2 Glomerular Filtration Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Overview of Renal Physiology
Chapter 26 The Urinary System
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 16 Urinary System 1 The Kidneys Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Functions of Urinary system o The Kidneys:
BIOH122 Human Biological Science 2 Session 16 Urinary System 1 The Kidneys Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Functions of Urinary system o The Kidneys:
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM
 RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19
![QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19](/thumbs/77/74887026.jpg) QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion,
QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion,
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Renal Physiology - Lectures
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (1)
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (1) Dr. Attila Nagy 2017 Functional role of the kidney 1.Homeostasis of fluid compartments (isosmia, isovolemia, isoionia, isohydria,) 2. Elimination
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (1) Dr. Attila Nagy 2017 Functional role of the kidney 1.Homeostasis of fluid compartments (isosmia, isovolemia, isoionia, isohydria,) 2. Elimination
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION
 3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION
 LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
Renal Physiology. April, J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine.
 Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
CHAPTER 25 URINARY. Urinary system. Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1. functions
 CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Kidney Structure. Renal Lobe = renal pyramid & overlying cortex. Renal Lobule = medullary ray & surrounding cortical labryinth.
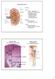 Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
URINARY SYSTEM. Primary functions. Major organs & structures
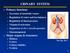 URINARY SYSTEM Primary functions Excretion of metabolic wastes Regulation of water and ion balances Regulation of blood pressure Vitamin D activation Regulation of rbc s (erythropoietin) Gluconeogenesis
URINARY SYSTEM Primary functions Excretion of metabolic wastes Regulation of water and ion balances Regulation of blood pressure Vitamin D activation Regulation of rbc s (erythropoietin) Gluconeogenesis
Lab Activity 31. Anatomy of the Urinary System. Portland Community College BI 233
 Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Functional morphology of kidneys Clearance
 Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Chapter 24: The Urinary System
 Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note
![Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note](/thumbs/77/75431210.jpg) Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Urinary System (Anatomy & Physiology)
 Urinary System (Anatomy & Physiology) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran The Urinary System
Urinary System (Anatomy & Physiology) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran The Urinary System
Urinary System kidneys, ureters, bladder & urethra
 Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Waste Products & Kidney Function
 Waste Products & Kidney Function urinary system principal means of metabolic waste removal urinary system is closely associated with reproductive system urogenital system share embryonic development share
Waste Products & Kidney Function urinary system principal means of metabolic waste removal urinary system is closely associated with reproductive system urogenital system share embryonic development share
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Chapter 23. The Nephron. (functional unit of the kidney
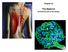 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
BLOCK REVIEW Renal Physiology. May 9, 2011 Koeppen & Stanton. EXAM May 12, Tubular Epithelium
 BLOCK REVIEW Renal Physiology Lisa M. HarrisonBernard, Ph.D. May 9, 2011 Koeppen & Stanton EXAM May 12, 2011 Tubular Epithelium Reabsorption Secretion 1 1. 20, 40, 60 rule for body fluid volumes 2. ECF
BLOCK REVIEW Renal Physiology Lisa M. HarrisonBernard, Ph.D. May 9, 2011 Koeppen & Stanton EXAM May 12, 2011 Tubular Epithelium Reabsorption Secretion 1 1. 20, 40, 60 rule for body fluid volumes 2. ECF
19. RENAL PHYSIOLOGY ROLE OF THE URINARY SYSTEM THE URINARY SYSTEM. Components and function. V BS 122 Physiology II 151 Class of 2011
 19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Urinary System kidneys, ureters, bladder & urethra
 Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Ch 19: The Kidneys. Functional unit of kidneys:?? Developed by John Gallagher, MS, DVM
 Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Urinary System. BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College
 Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Introduction to the kidney: regulation of sodium & glucose. Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health
 Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Chapter 25: Urinary System
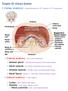 Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
2- Maintain the proper balance between water and. 3- Maintain the proper acid base balance. glucose by gluconeogenesis. pressure
 Filter ~180 liters of blood plasma daily, allowing toxins, metabolic wastes, and excess ions to leave the body in urine 1 Regulate volume and chemical composition of the blood 2 Maintain the proper balance
Filter ~180 liters of blood plasma daily, allowing toxins, metabolic wastes, and excess ions to leave the body in urine 1 Regulate volume and chemical composition of the blood 2 Maintain the proper balance
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (1)
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (1) Dr. Attila Nagy 2017 Functional roles of the kidney 1.Homeostasis of fluid compartments (isosmia, isovolemia, isoionia, isohydria,) 2. Elimination
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (1) Dr. Attila Nagy 2017 Functional roles of the kidney 1.Homeostasis of fluid compartments (isosmia, isovolemia, isoionia, isohydria,) 2. Elimination
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Urinary system. Urinary system
 INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
Collin College. BIOL Anatomy & Physiology WEEK 12. Urinary System INTRODUCTION. Main functions of the kidneys are
 Collin College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 INTRODUCTION Main functions of the kidneys are regulate blood volume, water content regulate blood composition e..g. Na, Cl, K, ph
Collin College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 INTRODUCTION Main functions of the kidneys are regulate blood volume, water content regulate blood composition e..g. Na, Cl, K, ph
Figure 26.1 An Introduction to the Urinary System
 Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
osmoregulation mechanisms in gills, salt glands, and kidneys
 Ionic & Osmotic Homeostasis osmoregulation mechanisms in gills, salt glands, and kidneys extracellular intracellular 22 23 Salt Secretion: recycle Figure in Box 26.2 Hill et al. 2004 active Down electrochemical
Ionic & Osmotic Homeostasis osmoregulation mechanisms in gills, salt glands, and kidneys extracellular intracellular 22 23 Salt Secretion: recycle Figure in Box 26.2 Hill et al. 2004 active Down electrochemical
Renal physiology II. Basic renal processes. Dr Alida Koorts BMS
 Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal Blood flow; Renal Clearance. Dr Sitelbanat
 Renal Blood flow; Renal Clearance Dr Sitelbanat Objectives At the end of this lecture student should be able to describe: Renal blood flow Autoregulation of GFR and RBF Regulation of GFR The Calcuation
Renal Blood flow; Renal Clearance Dr Sitelbanat Objectives At the end of this lecture student should be able to describe: Renal blood flow Autoregulation of GFR and RBF Regulation of GFR The Calcuation
Copyright 2010 Pearson Education, Inc. Urinary System
 Urinary System What are the organs that comprise the urinary system? Urinary System Organs Kidneys Urinary bladder Ureters Urethra Hepatic veins (cut) Esophagus (cut) Inferior vena cava Adrenal gland Aorta
Urinary System What are the organs that comprise the urinary system? Urinary System Organs Kidneys Urinary bladder Ureters Urethra Hepatic veins (cut) Esophagus (cut) Inferior vena cava Adrenal gland Aorta
PHGY210 Renal Physiology
 PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System Review Questions:
 Urinary System Review Questions: 1. This system would be lined with what type of membrane? 2. What type of epithelial tissue would line the opening of the urethra (the exit of the tract)? 3. What type
Urinary System Review Questions: 1. This system would be lined with what type of membrane? 2. What type of epithelial tissue would line the opening of the urethra (the exit of the tract)? 3. What type
Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
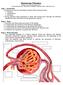 Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Formation of urine by the kidney involves
Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Formation of urine by the kidney involves
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
Overview of Kidney Function
 The Kidney Overview of Kidney Function osmolarity of the body fluids volume of ECF plasma ph waste products (urea, uric acid, creatinine, foreign compounds) synthesis of: - EPO, renin, kallikrein, prostaglandins,
The Kidney Overview of Kidney Function osmolarity of the body fluids volume of ECF plasma ph waste products (urea, uric acid, creatinine, foreign compounds) synthesis of: - EPO, renin, kallikrein, prostaglandins,
I. General Features of Renal Function -Objectives II. Blood Flow and Filtration -Objectives III. Tubular Anatomy and Function -Objectives IV.
 ORGANIZATION This syllabus is divided into ten sections or topics. Each section is divided into objectives. On the contents page, clicking on the section title takes you directly to that section. Clicking
ORGANIZATION This syllabus is divided into ten sections or topics. Each section is divided into objectives. On the contents page, clicking on the section title takes you directly to that section. Clicking
MOLECULAR SIZE, ELECTRICAL CHARGE, AND SHAPE DETERMINE THE FILTERABILITY OF SOLUTES ACROSS THE GLOMERULAR FILTRATION BARRIER
 MOLECULAR SIZE, ELECTRICAL CHARGE, AND SHAPE DETERMINE THE FILTERABILITY OF SOLUTES ACROSS THE GLOMERULAR FILTRATION BARRIER The glomerular filtration barrier consists of three elements: (1) endothelial
MOLECULAR SIZE, ELECTRICAL CHARGE, AND SHAPE DETERMINE THE FILTERABILITY OF SOLUTES ACROSS THE GLOMERULAR FILTRATION BARRIER The glomerular filtration barrier consists of three elements: (1) endothelial
Histology Urinary system
 Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Chapter 26 The Urinary System. Overview of Kidney Functions. External Anatomy of Kidney. External Anatomy of Kidney
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Renal Functions: Renal Functions: Renal Function: Produce Urine
 Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
A. Incorrect! The urinary system is involved in the regulation of blood ph. B. Correct! The urinary system is involved in the synthesis of vitamin D.
 Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Lecture 16: The Nephron
 Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
URINARY SYSTEM. Urinary System
 URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
Excretory Lecture Test Questions Set 1
 Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Chapter 17: Urinary System
 Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Histology / First stage The Urinary System: Introduction. Kidneys
 The Urinary System: Introduction The urinary system consists of the paired kidneys and ureters, the bladder, and the urethra. This system helps maintain homeostasis by a complex combination of processes
The Urinary System: Introduction The urinary system consists of the paired kidneys and ureters, the bladder, and the urethra. This system helps maintain homeostasis by a complex combination of processes
Excretory System-Training Handout
 Excretory System-Training Handout Karen L. Lancour National Rules Committee Chairman Life Science Excretion - Excretion is the removal of the metabolic wastes of an organism. Wastes that are removed include
Excretory System-Training Handout Karen L. Lancour National Rules Committee Chairman Life Science Excretion - Excretion is the removal of the metabolic wastes of an organism. Wastes that are removed include
