Cerebral Monitoring of the Term Infant
|
|
|
- Derrick Carter
- 6 years ago
- Views:
Transcription
1 Cerebral Monitoring of the Term Infant Shelly V. Lavery, RN, BaHSc Kathi S. Randall, RN, MSN, CNS, NNP-BC Cerebral injury can have devastating consequences for long-term neurologic development. In some countries, limited-channel continuous bedside cerebral monitoring of infants at risk of cerebral injury has become part of routine clinical care in the NICU. 1 Most NICUs in the U.S. do not yet routinely monitor brain function continuously at the bedside. New technologies are changing this practice and can provide the ability to gain further insights into brain function beginning upon admission. In most NICUs, sick infants who have suffered a hypoxicischemic event are monitored from the moment of birth using invasive and noninvasive devices. It is not uncommon to quickly apply one or two oxygen saturation probes, three electrocardiogram (ECG) leads, a temperature probe, and a blood pressure cuff on an arm or leg. Often umbilical lines are inserted and attached to blood pressure transducers, and flow detectors are secured to ventilator circuits and endotracheal tubes. These devices have become so routine that many NICU nurses believe they could not adequately provide care without them. But often there is no continuous bedside monitoring of the organ most at risk of injury the brain. In this article, we review the evidence for current clinical uses of continuous bedside brain monitors in the NICU. We also describe the nurse s role in applying and using these Accepted for publication January Revised April Abs t r a c t Continuously monitoring brain function at the bedside in the NICU for term infants at risk of brain injury has become part of routine clinical practice in many countries. These monitors offer invaluable information about the sick infant s neurologic status by providing real-time measurements of the brain s electrical activity and identifying or confirming seizure activity. With the increasing availability of bedside electroencephalogram technology, it is essential for neonatal intensive care nursing staff to understand the rationale for its use, as well as the fundamentals of application and interpretation of this new technology. monitors. And an introduction to the interpretation of the more common patterns seen on these tools will assist the bedside nurse to appropriately refer abnormal brain activity for further evaluation. Conventional EEG The conventional electroencephalographic (ceeg) signal at the scalp represents the sum of the excitatory and inhibitory postsynaptic potentials from the neurons in the cerebral cortex. This creates small electrical impulses that can be measured by placing surface electrodes on the scalp. The ceeg displays a magnified raw/unprocessed waveform that correlates with the electrical impulses. In the presence of hypoxic or ischemic brain injury, there is reduced or abnormal cortical electrical activity. ceeg is most commonly used to measure the impact of a neurologic insult on the brain and to detect the presence of seizure activity. ceeg sensors are applied by specialized technicians using sensors, creating multiple channels between the sensors where the electrical activity can be measured. 2 In the acute clinical setting, ceeg is usually recorded for minutes by the EEG technician, this is sometimes known as a multichannel EEG tracing. Funding and salary support have been contributed by BrainZ Instruments (New Zealand). VOL. 27, NO. 5, September/october
2 FIGURE 1 n Neonate with bedside brain monitoring. real-time interpretation of the level of electrical activity of the brain at the bedside and visualization of changes in brain activity over extended periods of time. Today a number of bedside cerebral monitoring tools incorporate aeeg (Figure 1). Historically, these bedside aeeg monitors used a single biparietal channel (two sensors). The newer aeeg monitors use two channels (four sensors) in the parietal and central positions. The simplicity of these monitors allows them to be maintained by the bedside nurse and used as clinically required. The need for continuous brain monitoring Courtesy of Royal Children s Hospital, Melbourne, Australia. When neurologists analyze the output from a multichannel EEG tracing, they consider the individual morphology, frequency, amplitude, and evolution of the waveforms in relation to multiple channels. This information may assist in identifying abnormal levels of cortical electrical brain activity generally or focally, the existence of potentially epileptogenic foci, or ongoing seizures. The ceeg also assists in determining brain maturation, sleep state development, and the presence of artifact. Although it represents a short period of time, the ceeg provides comprehensive and subtle information about the whole cerebral cortex. However, the process of ordering a ceeg, arranging for a specialized technician to apply the EEG, and having a neurologist review and report on the ceeg may involve considerable delay. Amplitude Integrated EEG Amplitude integrated EEG (aeeg) was developed in the late 1960s to continuously monitor adult patients during anesthesia and in intensive care. The aeeg measures, filters, and time-compresses the raw EEG signal to create a simplified pattern that is easy to interpret. 3 This pattern permits Hypoxic-ischemic Encephalopathy Hypoxic-ischemic encephalopathy (HIE), affects 1 6 per 1,000 live births. 4 HIE can result in alterations of cerebral metabolism and reduction or derangement of cerebral electrical activity. Currently, the neurologic evaluation of encephalopathic infants relies heavily on clinical examination, which can be altered by the administration of sedatives, muscle relaxants, and antiepileptic drugs (AEDs). Other evaluation methods include multichannel EEG, cranial ultrasound, computed tomography (CT), and magnetic resonance imaging (MRI). Each of these offers a detailed static snapshot of the newborn brain, but they also require skill in application and interpretation. Additionally, transporting sick infants away from the unit to complete these neurologic examinations poses logistical challenges and inherent risks. With the promise of therapeutic interventions to improve the outcome from cerebral injury, the need is increasing for early bedside neurologic evaluation in the term encephalopathic infant. In term infants, aeeg has been shown to be very reliable in evaluating brain function after hypoxic-ischemic events. Studies have shown that patterns on aeeg have a high concordance with conventional 16-lead neonatal EEG 5,6 and MRI. 7 Other studies have demonstrated that aeeg patterns recorded in the first three to six hours of life are predictive of later neurodevelopmental outcomes in term encephalopathic infants. 8,9 A study by Eken and colleagues recruited 34 term infants with HIE within six hours of delivery. Bedside neurologic evaluations included cranial ultrasonography, Doppler ultrasonography, somatosensory evoked potentials, visual evoked potentials, and a single-channel aeeg brain monitor. These infants were followed up at 3, 9, 18, and 24 months of age. The aeeg monitor had the highest positive predictive value (PPV), 84.2 percent, and the highest negative predictive value (NPV), 91.7 percent, for an abnormal neurodevelopmental outcome (developmental quotient below 85 on the Griffths scale or cerebral palsy). Of the 12 infants with a normal aeeg pattern, all but 1 had a good outcome. 8 Toet and coworkers studied a larger cohort of 73 term infants treated for perinatal asphyxia, of which 68 were followed up for more than 12 months (range 12 months to six years). The 330 September/october 2008, VOL. 27, NO. 5
3 FIGURE 2 n aeeg of infant with unilateral cerebral injury. Note abnormal reduction of waveform activity on the EEG right channel, reflected in the aeeg right channel (lower band). FIGURE 3 n Normal aeeg, with lower margin predominantly above 5 microvolts and upper margin above 10 microvolts. Sleep/wake cycling wide part of band represents quiet sleep, and narrow part of band represents active sleep/awake. single-channel aeeg was classified at three and six hours of age. The PPV was 78 percent, and NPV was 84 percent three hours after birth. At six hours, the PPV was 86 percent, and the NPV was 91 percent. 9 Based on these predictive capabilities, abnormalities on aeeg recordings were used as a selection criterion for entry into published and ongoing large randomized hypothermia trials and may be utilized alongside future neuroprotective strategies. 10,11 Further prognostic information can be derived from the evolution of or recovery from cerebral injury. One study reviewed the aeegs of 160 term infants with signs of perinatal asphyxia and concluded that if a severely abnormal aeeg pattern returns to normal within 24 hours of life, an infant has a 61 percent chance of surviving with mild or no disability. 12 If the aeeg remains severely abnormal after 48 hours of life, the long-term prognosis is very poor. 13 Cerebral assessment by aeeg, in conjunction with a neurologic clinical examination, has been demonstrated to yield a higher PPV of short-term outcome than clinical assessments alone. 14 Thus, aeeg promises to improve the accuracy of identifying at-risk infants who can benefit from timely therapeutic intervention while reducing unnecessary treatment of infants not at risk. Neonatal cerebral infarction, or stroke, may present in an otherwise healthy infant with subtle neurologic abnormalities such as poor feeding skills or clinical seizures. Cerebral infarctions have historically been underdiagnosed or diagnosed late. However, with neuroimaging becoming more accessible to the neonatal population, the diagnosis of perinatal and neonatal stroke is becoming more common. 15 Cerebral infarction accounts for as much as 20 percent of cerebral injury in the term infant with encephalopathy. 16,17 Thrombolytic and rehabilitation therapies have been developed for neonates with stroke-like lesions and may improve outcomes. 18,19 These interventions may require early recognition and diagnosis for greatest effectiveness. At the very least, early diagnosis would allow at-risk infants to be eligible to receive timely early intervention and rehabilitation service. The newer aeeg brain monitor tools offer two or more channels to allow for comparison of electrical activity between cerebral hemispheres, helping to identify unilateral or focal injury (Figure 2). 20 Although most studies have focused on infants with HIE, more recent studies are exploring the prognostic value of aeeg for other neurologic disorders, using similar aeeg classifications as the studies that have been previously described. One of these studies reported on 86 encephalopathic infants of varying etiologies including meningitis, metabolic disorders, and cerebral vascular infarction. The infants had aeeg monitoring in the first three days of life and an MRI within the primary admission. Despite the varying timing of monitoring and the differing diagnoses, a strong correlation was demonstrated between an abnormal aeeg and cerebral injury as shown on MRI. 7 There is also increasing interest in aeeg monitoring of other infants who are at risk of cerebral injury, for example infants undergoing extracorporeal membrane oxygenation, 21 and in ongoing trials monitoring neonates with congenital heart disease undergoing cardiopulmonary bypass (in Melbourne, Australia, and Auckland, New Zealand). 22 Sleep/wake cycling can be identified on the aeeg pattern (Figure 3). This capability may help the bedside clinician VOL. 27, NO. 5, September/october
4 Clinical Application of aeeg Bedside Monitors in the NICU Pot e n t i a l b e n e f i t s o f aeeg m o n i t o r i n g : Ba c k g r o u n d (le v e l o f b r a i n a c t i v i t y) Assist in prognosis of long-term outcome in the encephalopathic term infant Assist in appropriate timing of referral for further neurologic investigations Aid in selecting infants at risk of cerebral injury who may benefit from neuroprotective strategies Identify electrical symmetry between the cerebral hemispheres in babies at risk of cerebral injury to identify focal or unilateral cerebral injury for appropriate referral Identify presence or absence of sleep/ wake cycling Pot e n t i a l b e n e f i t s o f aeeg m o n i t o r i n g : Se i z u r e s Identify the presence of seizures to alert clinicians of cerebral dysfunction Identify subclinical seizures that would be undetectable without monitoring Aid pharmacologic management of seizures Differentiate abnormal movements that are not associated with electroencephalographic seizures recognize the sleep states of the neonate and may also have implications for developmental care and nursing research. 23 Clinically assessing sleep states of a sick infant can be extremely challenging, leaving many unanswered questions: How much sleep are sick infants getting in a busy NICU? What are the barriers to sleep? Could a monitoring tool that identifies sleep states assist nurses to choose the best timing for nursing care? Do developmental care practices affect the quality or quantity of sleep patterns in the NICU? Does protecting sleep optimize neurodevelopmental outcomes? A tool that objectively measures sleep, at the bedside, in the NICU can help answer many important research questions that may potentially influence day-to-day NICU care practices. 24 Seizures One of the main signs of cerebral dysfunction is seizure activity. 25 Depending on etiology, neonatal seizures are associated with high mortality and neurodevelopmental delay. 26,27 In addition, an animal study demonstrated that the experimental induction of repeated seizures with existing hypoxic-ischemic injury may exacerbate cerebral injury. 28 These results highlight the concern that unrecognized and untreated seizures may cause further injury in infants with an existing hypoxic-ischemic injury. Clinical assessment of seizures alone may be unreliable. 29 Neonatal seizures often have subtle signs, e.g. apnea, lip smacking, tongue thrusting, changes in heart rate or blood pressure, that make recognition of them challenging. Two video ceeg studies documented that more than 50 percent of neonatal seizures are subclinical (electrographic seizures with an absence of visible clinical signs). 30,31 Most commonly used anticonvulsant medications may be inadequate, effectively treating only 50 percent of seizures and often initiating electroclinical or electromechanical dissociation in which the clinical manifestation of a seizure ceases after treatment with AEDs but electrically the seizure continues. 32,33 Bedside aeeg monitoring can be a useful tool in infants at risk of seizure activity by enhancing the ability to diagnose subclinical seizures and evaluating the electrical encephalographic response to antiepileptic therapy. 34 Bedside aeeg monitoring may also help to identify infants with abnormal movements that are not associated with electroencephalographic seizures. Boylan and colleagues evaluated 24 infants with ceeg monitoring where there was a clinical suspicion of neonatal seizures or high risk of developing seizures. Seven of these infants had clinical seizures with no corresponding seizure activity on ceeg. Of these 7 infants, 6 had a normal ceeg background and a normal MRI, and 5 were categorized with a normal outcome at one year of age. 30 Accurately identifying which abnormal movements are not seizure activity helps ensure that infants are not treated with AEDs unnecessarily. A study by Toet and colleagues published in 2005, demonstrated that treating all clinical and subclinical seizures identified by aeeg positively affected outcome. These investigators evaluated 206 term infants who were treated with AEDs for neonatal seizures that were detected by aeeg. They received AEDs for clinical as well as subclinical neonatal seizures. Eighty percent of the infants had a diagnosis of HIE, with the remaining diagnosed with intracranial hemorrhage or perinatal arterial stroke. 35 Follow-up data from five assessments (at 3, 9, and 15 months, and at three and five years) analyzed for their neuro developmental outcome and the presence of postneonatal epilepsy showed that the incidence of postnatal epilepsy was reduced to 9.4 percent. This is less than the percent incidence reported earlier in children who received treatment only for clinical 332 September/october 2008, VOL. 27, NO. 5
5 seizures. 36 Toet and colleagues study demonstrated how continuous bedside brain monitoring for seizure identification and treatment of clinical and subclinical seizures may improve an infant s outcome. In a busy NICU environment, subtle seizures may go unobserved. Most neonatal nurses have experienced the frustration of witnessing abnormal movements that are not repeated in the presence of medical personnel or during a ceeg recording. Long-term bedside brain monitoring can be a useful tool to increase accurate recognition of both clinical and subclinical seizures to identify cerebral dysfunction and prompt further investigation. It may also assist in evaluating the effect of therapies in the presence of electromechanical dissociation. Continuous brain monitoring can help the bedside nurse distinguish abnormal movements from seizure activity, ensuring that infants are not unnecessarily treated with AEDs (See: Clinical Application of aeeg Bedside Monitors in the NICU). Case Example Baby Jones is a 42-week infant, born by emergency cesarean birth for a presumed placental abruption. There was meconium-stained fluid present, and several prolonged late decelerations were recorded prior to delivery. He required resuscitation and mechanical ventilation, with Apgar scores of 1, 1, 3, 5, and 7 at 1, 5, 10, 15, and 20 minutes, respectively. He was admitted to the NICU on a Saturday night at 9 pm, pale, flaccid, tachycardic, and hypotensive. At midnight, you observe repetitive, rhythmic, clonic movements of both arms that do not stop on containment. These movements are noted several more times in the next hour; you page the neonatal nurse practitioner to the bedside. Baby Jones is given a 20 mg/kg loading dose of phenobarbital, and the seizurelike movements cease during the next hour. He will now be well sedated, which influences the results of any clinical examinations; yet subclinical seizures may still be occurring. Furthermore, the overall level of brain activity may contribute to determining his prognosis, which could assist with direction of treatment. Continuous aeeg brain monitoring could make this important information immediately available to the bedside clinicians caring for Baby Jones. Monitors can be applied at any time of the day or night, continued over long periods of time, and provide information immediately at the bedside. Bedside aeeg monitoring should be used in conjunction with other neurodiagnostic examinations whenever possible, such as MRI, CT, ultrasound, and ceeg; together they provide a comprehensive view of altered brain function and structure. Bedside brain monitors do not replace other technologies, but they do assist with early recognition of altered brain function, aid in the decision to pursue additional diagnostic tests, and give clinicians the ability to monitor the effectiveness of some interventions. To further illustrate this point, consider a comparison between brain monitoring and cardiac monitoring. When an infant on a cardiac monitor is noted to have an arrhythmia pattern, the medical team is notified and may order a 12-lead ECG, serum electrolytes, an echocardiogram, and even a cardiology consult to assist in the infant s management. Similarly, if abnormal brain activity is identified on the bedside brain monitor, the medical team may order further neurologic investigations to discover the cause and possibly order a consultation with a neurologist. Electrolytes and blood glucose levels may be reviewed, and a cranial ultrasound might be obtained to look for structural problems or intracranial bleeding. If CT and MRI are available, scans may be done to investigate brain structure and possible cerebral injury in greater detail. the Nurse s Role The nurse s role and responsibilities in regard to bedside brain monitoring are usually defined by individual NICU policies. However, application and maintenance of sensors, navigation of the monitor interface, and interpretation of the aeeg pattern are within the expertise of the NICU nurse. The nurse s role in documenting medication that affects the central nervous system is invaluable for optimal interpretation of the aeeg pattern. The nurse also needs to document any events that may cause a change in recording and possible identification of artifacts. As she must with any bedside monitoring system, the nurse needs to be aware of what is normal and abnormal for appropriate referral to the intensive care team. Application of Sensors The more opportunities that nurses have to apply the sensors, the quicker they will become skilled with the application. Most aeeg monitors use two to four soft hydrogel adhesive sensors (similar to ECG electrodes) that are applied to the scalp over each parietal and the central regions of the brain. These are noninvasive and are unlikely to cause irritation or pressure with prolonged use. However, the skin needs to be adequately prepared to ensure good contact. This involves cleaning, gentle abrasion with an exfoliant, and parting the hair to enable maximal scalp exposure to the gel sensors. Some NICUs may allow shaving of a small section of hair if contact remains problematic. Small, subdermal needle sensors are also available and are used routinely in some units. Needle sensors have the advantage of being quicker to apply, but they incur the potential problems of any invasive procedure. Once the sensors are applied, most brain monitors have a visual alarm to alert the bedside nurse that a sensor may need to be reapplied. Interpretation of aeeg in Term Infants Assessment of the aeeg tracing takes only a small amount of training and basic pattern recognition skills. NICU nurses are already extremely skilled at applying pattern recognition skills and observing for trends as they constantly review incoming data such as ECG information and ventilator loops. VOL. 27, NO. 5, September/october
6 Background/Brain Activity Care must be taken with interpretation in the presence of AEDs and sedation, which may depress the EEG signal and, in turn, the aeeg. Ideally, brain monitoring should be initiated on admission, providing a baseline before medication begins. It is important to document the administration of these medications so their effect on the aeeg will be evident. Visualization of the unprocessed/raw EEG signal assists in the identification of artifacts that may elevate the baseline, such as muscle artifact and extra waveforms caused by rapid ventilation. The aeeg is presented as a dense band charted on a semilogarithmic microvoltage scale (Figure 4). The position of this band reflects the amount of electrical brain activity; that is, the lower the brain activity, the lower the voltage reading, thus the lower the level of the band. This band is plotted over time on the x-axis. Various aeeg classifications have been described. 5,9,37,38 Perhaps the easiest for clinical application is based on the voltage levels of the lower and upper margins of the band (see Figure 4). 5 Normal Patterns The normal neonatal brain activity pattern with sleep/wake cycling present is called continuous. The lower margin of the dense band sits predominantly above 5 microvolts, and the upper margin of the band is above 10 microvolts. When the infant is in a quiet sleep, the band usually widens with the lower margin dropping. When the infant is in active sleep or awake, the activity becomes more continuous, and the band narrows with the lower margin rising (see Figure 3). In term infants, this is usually a 20-minute cyclical pattern. 39 Moderately Abnormal Pattern When there is a mixture of low activity and higher activity, the pattern is called discontinuous. It is displayed as a wide aeeg band due to the variable levels of brain activity and waveforms. The lower margin is variable, but is consistently less than 5 microvolts, reflecting the lower activity of the brain. The upper margin, as with the normal pattern, remains above 10 microvolts, representing the presence of some higher levels of activity (Figure 5). This pattern may be seen after the administration of anticonvulsant medications and after mild hypoxic events. 39 FIGURE 4 n Lower (yellow) and upper (red) margin of aeeg band. Severely Abnormal Patterns Burst suppression, continuous low voltage, and isoelectric or flat traces are all examples of severely abnormal aeeg patterns. Their common thread is that most of the brain activity is low, causing the aeeg lower margin to be consistently less than 5 microvolts and straight. As the brain becomes energy depleted, the top margin of the aeeg progresses toward values less than 10 microvolts (continuous low voltage) (Figure 6). 39 Burst suppression is classified as a severely abnormal pattern. The raw EEG is characterized by mostly suppressed activity with brief abnormal bursts of brain activity. The suppressed sections of the EEG give the aeeg pattern a straight and low bottom margin, but the brief bursts of high-amplitude waves create spikes on the aeeg greater than 25 microvolts (Figure 7). 37 Seizures Seizures are characterized by increasing brain activity. This causes a rise in the lower margin and usually the upper margin of the aeeg band, creating an arch in the aeeg record (Figure 8). 39 This feature enables the clinician to quickly scan for areas where the raw EEG signal should be Unprocessed/raw EEG (Left cerebral hemisphere) Unprocessed/raw EEG (Right cerebral hemisphere) aeeg (Left cerebral hemisphere) aeeg (Right cerebral hemisphere) FIGURE 5 n Moderately abnormal (discontinuous) aeeg with lower margin predominantly below 5 microvolts and upper margin above 10 microvolts. Lower margin is less than 5 µv Lower margin is less than 5 µv 334 September/october 2008, VOL. 27, NO. 5
7 FIGURE 6 n Severely abnormal (continuous low voltage) aeeg, with lower margin below 5 microvolts and upper margin below 10 microvolts. FIGURE 7 n Severely abnormal (burst suppression) aeeg with lower margin below 5 microvolts and high-voltage spikes greater than 25 microvolts. Upper margin is less than 10 µv Lower margin is less than 5 µv Upper margin is less than 10 µv Lower margin is less than 5 µv more closely examined to confirm seizure activity. Neonatal seizures on the raw EEG signal have been described as rhythmic, sharp, or spiky waveforms that are similar in morphology and last longer than ten seconds. 2 Suspected seizures on the aeeg must be confirmed by reviewing the raw EEG signal because some artifacts (such as muscle artifact) may also cause an intermittent rise in the aeeg (Figure 9). Nurses play a crucial role in the identification of artifact. Diligent documentation of clinical events and nursing interventions will aid in the identification of artifact, such as patting or chest physiotherapy, that can simulate a seizure pattern. Using aeeg as a screening tool for seizures has its limitations. 40 Seizures typically evolve, meaning that they have a beginning, middle, and end, and they can migrate from one area of the brain to another. On limited-channel monitors, this evolution and migration of seizures may not be as clearly evident. Limited channels can also miss focal seizures that do not migrate to the monitored area. For these reasons, a full multichannel ceeg is necessary for a comprehensive look at the whole cortical area. Because aeeg is a compressed record, brief seizures may not be detected, and low-amplitude seizures may not cause a rise in the aeeg. Online tools to detect spikes in the raw EEG pattern are being developed to address these limitations. 41 Conclusion In the case of Baby Jones, with bedside brain monitoring available, NICU staff could initiate monitoring at the time of admission. An abnormal aeeg pattern would provide the neonatal staff with valuable prognostic information. Seizures continuing on the bedside brain monitor, after administration of phenobarbital, would give valuable feedback on the efficacy of the treatment regimen. The information provided by an early aeeg may justify an emergency consultation with the pediatric neurologist and a ceeg during the weekend or at other off-peak times. As researchers explore potential neuroprotective strategies, it is essential to have the technology to identify infants who may benefit and then to monitor the effect of experimental therapies. If the decision in the NICU is to treat seizures, we must attempt to identify both clinical and subclinical seizures, then adequately treat them by monitoring the response to AEDs. As one neurologist pointed out, we would not consider treating a cardiac electrical disturbance (arrhythmia) without monitoring the heart, FIGURE 8 n Electroencephalographic seizure causing a rise in the lower margin and usually the upper margin, creating an arch in the aeeg band. FIGURE 9 n Example of artifact (arrows) raising the aeeg band. VOL. 27, NO. 5, September/october
8 yet we continue to treat cerebral electrical disturbances (seizures) without routinely monitoring the brain. 42 At the very least, it is still essential to identify seizures for further investigation. Bedside aeeg technology provides NICU clinicians the opportunity to gain further insights into neonatal brain function and optimize care to ensure the best outcome for their patients. References 1. Filan, P. M., Inder, T. E., Anderson, P. J., Doyle, L. W., & Hunt, R. W. (2007). Monitoring the neonatal brain: A survey of current practice among Australian and New Zealand neonatologists. Journal of Paediatrics and Child Health, 43, Koszer, S. E., Moshe, S. L., & Holmes, G. L. (2006). Visual analysis of the neonatal electoencephalogram. In G. L. Holmes, S. L. Moshe, & H. R. Jones, Jr (Eds.), Clinical neurophysiology of infancy, childhood, and adolescence (pp ). Philadelphia: Butterworth Heinemann. 3. Prior, P. F., Maynard, D. E., Sheaff, P. C., Simpson, B. R., Strunin, L., Weaver, E. J., et al. (1971). Monitoring cerebral function: Clinical experience with new device for continuous recording of electrical activity of brain. British Medical Journal, 2, Hagberg, B., & Hagberg, G. (1996). The changing panorama of cerebral palsy bilateral spastic forms in particular. Acta Paediatrica, 416 (Suppl.), al Naqeeb, N., Edwards, A. D., Cowan, F. M., & Azzopardi, D. (1999). Assessment of neonatal encephalopathy by amplitude-integrated electroencephalography. Pediatrics, 103, Toet, M. C., van der Meij, W., de Vries, L. S., Uiterwaal, C. S., & van Huffelen, K. C. (2002). Comparison between simultaneously recorded amplitude integrated electroencephalogram (cerebral function monitor) and standard electroencephalogram in neonates. Pediatrics, 109, Shah, D. K., Lavery, S., Doyle, L. W., Wong, C., McDougall, P., & Inder, T. E. (2006). Use of 2-channel bedside electroencephalogram monitoring in term-born encephalopathic infants related to cerebral injury defined by magnetic resonance imaging. Pediatrics, 118, Eken, P., Toet, M. C., Groenendaal, F., & de Vries, L. S. (1995). Predictive value of early neuroimaging, pulsed Doppler and neurophysiology in full term infants with hypoxic-ischaemic encephalopathy. Archives of Disease in Childhood. Fetal and Neonatal Edition, 73, F75 F Toet, M. C., Hellstrom-Westas, L., Groenendaal, F., Eken, P., & de Vries, L. S. (1999). Amplitude integrated EEG 3 and 6 hours after birth in full term neonates with hypoxic-ischaemic encephalopathy. Archives of Disease in Childhood. Fetal and Neonatal Edition, 81, F19 F Azzopardi, D., Robertson, N. J., Cowan, F. M., Rutherford, M. A., Rampling, M., & Edwards, A. D. (2000). Pilot study of treatment with whole body hypothermia for neonatal encephalopathy. Pediatrics, 106, Gluckman, P. D., Wyatt, J. S., Azzopardi, D., Ballard, R., Edwards, A. D., Ferriero, D. M., et al. (2005). Selective head cooling with mild systemic hypothermia after neonatal encephalopathy: Multicentre randomised trial. Lancet, 365(9460), van Rooij, L. G., Toet, M. C., Osredkar, D., van Huffelen, A. C., Groenendaal, F., & de Vries, L. S. (2005). Recovery of amplitude integrated electroencephalographic background patterns within 24 hours of perinatal asphyxia. Archives of Disease in Childhood. Fetal and Neonatal Edition, 90, F245 F ter Horst, H. J., Sommer, C., Bergman, K. A., Fock, J. M., van Weerden, T. W., & Bos, A. F. (2006). Prognostic significance of amplitudeintegrated EEG during the first 72 hours after birth in severely asphyxiated neonates. Pediatric Research, 55, Shalak, L. F., Laptook, A. R., Velaphi, S. C., & Perlman, J. M. (2003). Amplitude-integrated electroencephalography coupled with an early neurologic examination enhances prediction of term infants at risk for persistent encephalopathy. Pediatrics, 111, Hunt, R. W., & Inder, T. E. (2006). Perinatal and neonatal ischaemic stroke: A review. Thrombosis Research, 118(1), Mercuri, E., Cowan, F., Rutherford, M., Acolet, D., Pennock, J., & Dubowitz, L. (1995). Ischaemic and haemorrhagic brain lesions in newborns with seizures and normal Apgar scores. Archives of Disease in Childhood. Fetal and Neonatal Edition, 73, F67 F Rutherford, M., Pennock, J., Schwieso, J., Cowan, F., & Dubowitz, L. (1996). Hypoxic-ischaemic encephalopathy: Early and late magnetic resonance imaging findings in relation to outcome. Archives of Disease in Childhood. Fetal and Neonatal Edition, 75, F145 F Pohl, M., Zimmerhackl, L. B., Heinen, F., Sutor, A. H., Schneppenheim, R., & Brandis, M. (1998). Bilateral renal vein thrombosis and venous sinus thrombosis in a neonate with factor V mutation (FV Leiden). The Journal of Pediatrics, 132, Eliasson, A. C., Bonnier, B., & Krumlinde-Sundholm, L. (2003). Clinical experience of constraint induced movement therapy in adolescents with hemiplegic cerebral palsy -a day camp model. Developmental Medicine and Child Neurology, 45, Lavery, S., Shah, D. K., Hunt, R. W., Filan, P. M., Doyle, L. W., & Inder, T. E. (2008). Single versus bihemispheric amplitude-integrated electroencephalography in relation to cerebral injury and outcome in the term encephalopathic infant. Journal of Paediatrics and Child Health, 44, Pappas, A., Shankaran, S., Stockmann, P. T., & Bara, R. (2006). Changes in amplitude-integrated electroencephalography in neonates treated with extracorporeal membrane oxygenation: A pilot study. The Journal of Pediatrics, 148, Gunn, J., Hunt, R. W., Lavery, S., McKeever, S., Delzoppo, C.,Goldsworthy, M., et al. (2008). Amplitude integrated electroencephalograph (aeeg) changes with hypothermia for neuroprotection during neonatal cardiac surgery. Paper presented at the Perinatal Society of Australia and New Zealand, Gold Coast, Queensland, Australia. 23. Hellstrom-Westas, L., Inghammar, M., Isaksson, K., Rosen, I., & Stjernqvist, K. (2001). Short-term effects of incubator covers on quiet sleep in stable premature infants. Acta Paediatrica, 90, Bertelle, V., Sevestre, A., Laou-Hap, K., Nagahapitiye, M. C., & Sizun, J. (2007). Sleep in the neonatal intensive care unit. The Journal of Perinatal & Neonatal Nursing, 21, Volpe, J. (2001). Neurology of the newborn (4th ed.). Philadelphia: WB Saunders. 26. McBride, M. C., Laroia, N., & Guillet, R. (2000). Electrographic seizures in neonates correlate with poor neurodevelopmental outcome. Neurology, 55, Scher, M. S., Painter, M. J., Bergman, I., Barmada, M. A., & Brunberg, J. (1989). EEG diagnoses of neonatal seizures: Clinical correlations and outcome. Pediatric Neurology, 5, Wirrell, E. C., Armstrong, E. A., Osman, L. D., & Yager, J. Y. (2001). Prolonged seizures exacerbate perinatal hypoxic-ischemic brain damage. Pediatric Research, 50, Levene, M. (2002). The clinical conundrum of neonatal seizures. Archives of Disease in Childhood. Fetal and Neonatal Edition, 86, F75 F Boylan, G. B., Pressler, R. M., Rennie, J. M., Morton, M., Leow, P. L., Hughes, R., et al. (1999). Outcome of electroclinical, electrographic, and clinical seizures in the newborn infant. Developmental Medicine and Child Neurology, 41, Scher, M. S., Aso, K., Beggarly, M. E., Hamid, M. Y., Steppe, D. A., & Painter, M. J. (1993). Electrographic seizures in preterm and fullterm neonates: Clinical correlates, associated brain lesions, and risk for neurologic sequelae. Pediatrics, 91, September/october 2008, VOL. 27, NO. 5
9 32. Boylan, G. B., Rennie, J. M., Chorley, G., Pressler, R. M., Fox, G. F., Farrer, K., et al. (2004). Second-line anticonvulsant treatment of neonatal seizures: A video-eeg monitoring study. Neurology, 62, Scher, M. S., Alvin, J., Gaus, L., Minnigh, B., & Painter, M. J. (2003). Uncoupling of EEG-clinical neonatal seizures after antiepileptic drug use. Pediatric Neurology, 28, de Vries, L. S., & Hellstrom-Westas, L. (2005). Role of cerebral function monitoring in the newborn. Archives of Disease in Childhood. Fetal and Neonatal Edition, 90, F201 F Toet, M. C., Groenendaal, F., Osredkar, D., van Huffelen, A. C., & de Vries, L. S. (2005). Postneonatal epilepsy following amplitude-integrated EEG-detected neonatal seizures. Pediatric Neurology, 32, Clancy, R. R., & Legido, A. (1991). Postnatal epilepsy after EEGconfirmed neonatal seizures. Epilepsia, 32, Hellstrom-Westas, L., Rosen, I., de Vries, L. S., & Greisen, G. (2007). Amplitude-integrated EEG classification and interpretation in preterm and term infants. Neoreviews, 7(2), Hellstrom-Westas, L., Rosen, I., & Svenningsen, N. W. (1995). Predictive value of early continuous amplitude integrated EEG recordings on outcome after severe birth asphyxia in full term infants. Archives of Disease in Childhood. Fetal and Neonatal Edition, 72, F34 F Hellstrom-Westas, L., de Vries, L. S., & Rosen, I. (2003). An atlas of amplitude-integrated EEGs in the newborn (1st ed.). London: Parthenon Publishing. 40. Rennie, J. M., Chorley, G., Boylan, G. B., Pressler, R., Nguyen, Y., & Hooper, R. (2004). Non-expert use of the cerebral function monitor for neonatal seizure detection. Archives of Disease in Childhood. Fetal and Neonatal Edition, 89, F37 F Navakatikyan, M. A., Colditz, P. B., Burke, C. J., Inder, T. E., Richmond, J., & Williams, C. E. (2006). Seizure detection algorithm for neonates based on wave-sequence analysis. Clinical Neurophysiology, 117, Vespa, P. (2005). Continuous EEG monitoring for the detection of seizures in traumatic brain injury, infarction, and intracerebral hemorrhage: To detect and protect. Journal of Clinical Neurophysiology, 22, About the Authors Shelly V. Lavery is currently a research nurse with the Victorian Infant Brain Study Group (VIBeS), Melbourne, Australia. She was previously employed as an associate unit manager of the neonatal ICU, Royal Children s Hospital, Melbourne. Shelly received her midwifery certificate at Bellshill, Scotland, and neonatal ICU certificate at Latrobe University, Melbourne. Kathi S. Randall has held a variety of positions in the NICU at Loma Linda University Medical Center over the last 14 years. At the time of writing this article, she was practicing as an NNP in their 80-bed Level III plus ECMO referral center. Kathi has a passion for education of both NICU staff and families. She lectures throughout the U.S. and internationally on a variety of neonatal topics. In addition to her clinical practice, Kathi provides education consultation services to medical device companies and has been a consultant to BrainZ Instruments, the manufacturer of the BRM bedside aeeg device, since they received FDA approval in We thank Barbara Mordue (Loma Linda University Medical Center), Brenda Smith (Utah Valley Regional Medical Center in Provo), and Tom Pantano (BrainZ Instruments) for their critique and helpful comments. For further information, please contact: Shelly V. Lavery, RN, BaHSc Victorian Infant Brain Study Group (VIBeS) Royal Children s Hospital Flemington Road Melbourne, Australia shelly.lavery@rch.org.au VOL. 27, NO. 5, September/october
7 Simple Steps to Assess & Document any Neonatal aeeg
 7 Simple Steps to Assess & Document any Neonatal aeeg Created for you by: www.aeegcoach.com How to use the Seven Simple Steps Checklist Hi! It s Kathi Randall here Your aeeg coach. I m so excited to share
7 Simple Steps to Assess & Document any Neonatal aeeg Created for you by: www.aeegcoach.com How to use the Seven Simple Steps Checklist Hi! It s Kathi Randall here Your aeeg coach. I m so excited to share
Nurses & Bedside Brain Monitoring
 Nurses & Bedside Brain Monitoring Kathi S. Randall MSN, CNS, NNP BC www.synapsecare.com/neocon kathi@synapsecare.com What you have already learned Pros & Cons of aeeg How to Read aeeg Populations for Potential
Nurses & Bedside Brain Monitoring Kathi S. Randall MSN, CNS, NNP BC www.synapsecare.com/neocon kathi@synapsecare.com What you have already learned Pros & Cons of aeeg How to Read aeeg Populations for Potential
CEREBRAL FUNCTION MONITORING
 CEREBRAL FUNCTION MONITORING Introduction and Definitions The term amplitude integrated electroencephalography (aeeg) is used to denote a method for electro-cortical monitoring whereas cerebral function
CEREBRAL FUNCTION MONITORING Introduction and Definitions The term amplitude integrated electroencephalography (aeeg) is used to denote a method for electro-cortical monitoring whereas cerebral function
Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline
 Original Article Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline Stephen Attard, Doriette Soler, Paul Soler Introduction: Cerebral
Original Article Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline Stephen Attard, Doriette Soler, Paul Soler Introduction: Cerebral
Hypoxic-ischemic encephalopathy has an incidence of
 Original Article Amplitude-Integrated EEG Is Useful in Predicting Neurodevelopmental Outcome in Full-Term Infants With Hypoxic-Ischemic Encephalopathy: A Meta-Analysis Journal of Child Neurology Volume
Original Article Amplitude-Integrated EEG Is Useful in Predicting Neurodevelopmental Outcome in Full-Term Infants With Hypoxic-Ischemic Encephalopathy: A Meta-Analysis Journal of Child Neurology Volume
I have no relevant financial relationships with the manufacturers of any commercial products or provider of commercial CME services discussed in this
 Neonatal Seizures Dennis J. Dlugos, MD Pediatric Regional Epilepsy Program The Children s Hospital of Philadelphia Perelman School of Medicine at the University of Pennsylvania I have no relevant financial
Neonatal Seizures Dennis J. Dlugos, MD Pediatric Regional Epilepsy Program The Children s Hospital of Philadelphia Perelman School of Medicine at the University of Pennsylvania I have no relevant financial
05/14/2012. I have been a paid speaker for Natus
 I have been a paid speaker for Natus Robert White, MD Medical Director, Pediatrix Medical Group Memorial Hospital, South Bend, IN For diagnosis/prognosis following HIE For seizure detection and monitoring
I have been a paid speaker for Natus Robert White, MD Medical Director, Pediatrix Medical Group Memorial Hospital, South Bend, IN For diagnosis/prognosis following HIE For seizure detection and monitoring
TOBY Cerebral Function Monitoring Addition to CFM handbook for users of the Olympic CFM 6000
 ISRCTN 89547571 TOBY Cerebral Function Monitoring Addition to CFM handbook for users of the Olympic CFM 6000 2 The contents of this booklet were originally produced for the website http://www.azzopardi.freeserve.co.uk/cfm
ISRCTN 89547571 TOBY Cerebral Function Monitoring Addition to CFM handbook for users of the Olympic CFM 6000 2 The contents of this booklet were originally produced for the website http://www.azzopardi.freeserve.co.uk/cfm
Treating EEG Seizures in Hypoxic Ischemic Encephalopathy: A Randomized Controlled Trial
 Treating EEG Seizures in Hypoxic Ischemic Encephalopathy: A Randomized Controlled Trial Preethi Srinivasakumar, MD a, John Zempel, MD, PhD b, Shamik Trivedi, MD a, Michael Wallendorf, PhD c, Rakesh Rao,
Treating EEG Seizures in Hypoxic Ischemic Encephalopathy: A Randomized Controlled Trial Preethi Srinivasakumar, MD a, John Zempel, MD, PhD b, Shamik Trivedi, MD a, Michael Wallendorf, PhD c, Rakesh Rao,
When? Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group.
 Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group. Standard EEG 2,3% 8.6% Standard EEG + aeeg Scher MS et al; Pediatrics
Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group. Standard EEG 2,3% 8.6% Standard EEG + aeeg Scher MS et al; Pediatrics
The Prognostic Value of Amplitude-Integrated EEG in Full-Term Neonates with Seizures
 The Prognostic Value of Amplitude-Integrated EEG in Full-Term Neonates with Seizures Dandan Zhang 1., Haiyan Ding 2., Lili Liu 3, Xinlin Hou 3 *, Guoyu Sun 3, Lei Li 4, Yunzhe Liu 1, Congle Zhou 3, Ruolei
The Prognostic Value of Amplitude-Integrated EEG in Full-Term Neonates with Seizures Dandan Zhang 1., Haiyan Ding 2., Lili Liu 3, Xinlin Hou 3 *, Guoyu Sun 3, Lei Li 4, Yunzhe Liu 1, Congle Zhou 3, Ruolei
The Clinical Spectrum and Prediction of Outcome in Hypoxic-Ischemic Encephalopathy
 Article neurology The Clinical Spectrum and Prediction of Outcome in Hypoxic-Ischemic Encephalopathy Walter C. Allan, MD* Objectives After completing this article, readers should be able to: 1. List the
Article neurology The Clinical Spectrum and Prediction of Outcome in Hypoxic-Ischemic Encephalopathy Walter C. Allan, MD* Objectives After completing this article, readers should be able to: 1. List the
Objectives. Birth Depression Management. Birth Depression Terms
 Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Neonatal seizures are an emergency
 VOLUME 46 November - December 2006 NUMBER 11-12 Original Article Neonatal seizures: clinical manifestations and etiology Daisy Widiastuti, Irawan Mangunatmadja, Taralan Tambunan, Rulina Suradi ABSTRACT
VOLUME 46 November - December 2006 NUMBER 11-12 Original Article Neonatal seizures: clinical manifestations and etiology Daisy Widiastuti, Irawan Mangunatmadja, Taralan Tambunan, Rulina Suradi ABSTRACT
Predicting Outcomes in HIE. Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016
 Predicting Outcomes in HIE Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016 Interactive please! Case 1 Term, 3.5 kg Antenatal: Breech Labour/Delivery: Em CS failure to progress, mec
Predicting Outcomes in HIE Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016 Interactive please! Case 1 Term, 3.5 kg Antenatal: Breech Labour/Delivery: Em CS failure to progress, mec
Enhancing patient care in the ICU with NeuroMonitoring
 Enhancing patient care in the ICU with NeuroMonitoring In the ICU, several patient vital signs are monitored continuously. But what about the brain? Hemodynamics Heart rate Non invasive blood pressure
Enhancing patient care in the ICU with NeuroMonitoring In the ICU, several patient vital signs are monitored continuously. But what about the brain? Hemodynamics Heart rate Non invasive blood pressure
P henobarbitone remains the most frequently used first line
 F165 ORIGINAL ARTICLE Phenobarbitone, neonatal seizures, and video-eeg G B Boylan, J M Rennie, R M Pressler, G Wilson, M Morton, C D Binnie... See end of article for authors affiliations... Correspondence
F165 ORIGINAL ARTICLE Phenobarbitone, neonatal seizures, and video-eeg G B Boylan, J M Rennie, R M Pressler, G Wilson, M Morton, C D Binnie... See end of article for authors affiliations... Correspondence
Continuous EEG monitoring of the premature infant in the NICU
 Continuous EEG monitoring of the premature infant in the NICU Tom Stiris Oslo University Hospital, NICU CIP, Paris 2011 Background A method that at a very early stage diagnose those babies which would
Continuous EEG monitoring of the premature infant in the NICU Tom Stiris Oslo University Hospital, NICU CIP, Paris 2011 Background A method that at a very early stage diagnose those babies which would
Incidence and diagnosis of unilateral arterial cerebral infarction in newborn infants *
 J. Perinat. Med. 33 (2005) 170 175 Copyright by Walter de Gruyter Berlin New York. DOI 10.1515/JPM.2005.032 Short communication Incidence and diagnosis of unilateral arterial cerebral infarction in newborn
J. Perinat. Med. 33 (2005) 170 175 Copyright by Walter de Gruyter Berlin New York. DOI 10.1515/JPM.2005.032 Short communication Incidence and diagnosis of unilateral arterial cerebral infarction in newborn
Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy
 Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Developmental Changes Including Neonatal EEG. Gregory L. Holmes, MD
 Developmental Changes Including Neonatal EEG Gregory L. Holmes, MD A A + B =: B + A.Dravet Syndrome B.Menkes syndrome C.West syndrome D.Ohtahara shyndrome The Difficult Delivery 1 day old male transferred
Developmental Changes Including Neonatal EEG Gregory L. Holmes, MD A A + B =: B + A.Dravet Syndrome B.Menkes syndrome C.West syndrome D.Ohtahara shyndrome The Difficult Delivery 1 day old male transferred
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Automated EEG discontinuity in cooled newborns predicts cerebral MRI and neurodevelopmental outcome
 Automated EEG discontinuity in cooled newborns predicts cerebral MRI and neurodevelopmental outcome Jonathan M Dunne 1, David Wertheim MA, PhD 2 ; Paul Clarke MD, FRCPCH 3 ; Olga Kapellou MRCPCH, MD, PhD
Automated EEG discontinuity in cooled newborns predicts cerebral MRI and neurodevelopmental outcome Jonathan M Dunne 1, David Wertheim MA, PhD 2 ; Paul Clarke MD, FRCPCH 3 ; Olga Kapellou MRCPCH, MD, PhD
This lecture will provide an overview of the neurologic exam of a neonate in the context of clinical cases.
 A11a Neuro Nuggets from the Trenches Michael D. Weiss, MD Associate Professor Department of Pediatrics, Division of Neonatology University of Florida, Gainesville, FL The speaker has signed a disclosure
A11a Neuro Nuggets from the Trenches Michael D. Weiss, MD Associate Professor Department of Pediatrics, Division of Neonatology University of Florida, Gainesville, FL The speaker has signed a disclosure
Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia
 Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia D H Karunatilaka 1, G W D S Amaratunga 2, K D N I Perera 3, V Caldera 4
Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia D H Karunatilaka 1, G W D S Amaratunga 2, K D N I Perera 3, V Caldera 4
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants
 Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO
 TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO DISCLOSURE I have no relationships with commercial companies
TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO DISCLOSURE I have no relationships with commercial companies
Too Cool? Hypoxic Ischemic Encephalopathy and Therapeutic Hypothermia. Lauren Sacco DNP, ARNP, NNP-BC
 Too Cool? Hypoxic Ischemic Encephalopathy and Therapeutic Hypothermia Lauren Sacco DNP, ARNP, NNP-BC Pathophysiology of HIE Occurs in two energy failure phases: First phase happens during the initial insult
Too Cool? Hypoxic Ischemic Encephalopathy and Therapeutic Hypothermia Lauren Sacco DNP, ARNP, NNP-BC Pathophysiology of HIE Occurs in two energy failure phases: First phase happens during the initial insult
Automated System for Detecting Neonatal Brain Injuries
 Snapshots of Postgraduate Research at University College Cork 2016 Automated System for Detecting Neonatal Brain Injuries Rehan Ahmed Dept. of Electrical and Electronics Engineering,, UCC The most dangerous
Snapshots of Postgraduate Research at University College Cork 2016 Automated System for Detecting Neonatal Brain Injuries Rehan Ahmed Dept. of Electrical and Electronics Engineering,, UCC The most dangerous
Prognostic Significance of Amplitude-Integrated EEG during the First 72 Hours after Birth in Severely Asphyxiated Neonates
 0031-3998/04/5506-1026 PEDIATRIC RESEARCH Vol. 55, No. 6, 2004 Copyright 2004 International Pediatric Research Foundation, Inc. Printed in U.S.A. Prognostic Significance of Amplitude-Integrated EEG during
0031-3998/04/5506-1026 PEDIATRIC RESEARCH Vol. 55, No. 6, 2004 Copyright 2004 International Pediatric Research Foundation, Inc. Printed in U.S.A. Prognostic Significance of Amplitude-Integrated EEG during
No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on Needed to be resuscitated at birth
 No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on 9-16-2011 Needed to be resuscitated at birth (included assisted vent) Had generalized edema and possible
No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on 9-16-2011 Needed to be resuscitated at birth (included assisted vent) Had generalized edema and possible
Management of Neonatal Seizures
 Management of Neonatal Seizures Manal E. Moustafa Assistant Professor of Pediatric Neurology and Epilepsy Children s Healthcare of Atlanta/Emory University Disclosures I have none! 1 Objectives Recognition
Management of Neonatal Seizures Manal E. Moustafa Assistant Professor of Pediatric Neurology and Epilepsy Children s Healthcare of Atlanta/Emory University Disclosures I have none! 1 Objectives Recognition
Queen Charlotte Hospital
 Queen Charlotte Hospital Neuroprotection for neonatal encephalopathy Neonatal encephalopathy accounts for 1 million deaths worldwide and even greater numbers of disabled survivors In countries with
Queen Charlotte Hospital Neuroprotection for neonatal encephalopathy Neonatal encephalopathy accounts for 1 million deaths worldwide and even greater numbers of disabled survivors In countries with
Hypoxic-Ischemic Encephalopathy. TW de Witt University of Pretoria Department of Paediatrics Neonatology
 Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Developing a Neuro NICU. Courtney Wusthoff, MD MS Assistant Professor, Neurology Neurology Director, LPCH Neuro NICU
 Developing a Neuro NICU Courtney Wusthoff, MD MS Assistant Professor, Neurology Neurology Director, LPCH Neuro NICU Acknowledgments Frances Cowan Miriam Martinez-Biarge Susan Hintz Kathi Randall Sonia
Developing a Neuro NICU Courtney Wusthoff, MD MS Assistant Professor, Neurology Neurology Director, LPCH Neuro NICU Acknowledgments Frances Cowan Miriam Martinez-Biarge Susan Hintz Kathi Randall Sonia
Continuous EEG: A Standard in Canada?
 Continuous EEG: A Standard in Canada? Victoria McCredie MBChB Neurointensivist Sunnybrook Health Sciences Centre Critical Care Canada Forum 28 th October 2015 No conflicts of interest to disclose. Outline
Continuous EEG: A Standard in Canada? Victoria McCredie MBChB Neurointensivist Sunnybrook Health Sciences Centre Critical Care Canada Forum 28 th October 2015 No conflicts of interest to disclose. Outline
Running title: EEG, MRI and neurodevelopmental outcome in HIE. Word count manuscript body: Word count abstract: 226. Address correspondence to:
 Role of EEG background activity, seizure burden and MRI in predicting neurodevelopmental outcome in full-term infants with hypoxic-ischaemic encephalopathy in the era of therapeutic hypothermia. Lauren
Role of EEG background activity, seizure burden and MRI in predicting neurodevelopmental outcome in full-term infants with hypoxic-ischaemic encephalopathy in the era of therapeutic hypothermia. Lauren
The NeuroNICU From Concept to Clinical Service. MJ Harbert, MD Co-Director, NeuroNICU Service Rady Children s Hospital San Diego
 The NeuroNICU From Concept to Clinical Service MJ Harbert, MD Co-Director, NeuroNICU Service Rady Children s Hospital San Diego What is a NeuroNICU? Collaboration between Neonatology and Neurology Neonatal
The NeuroNICU From Concept to Clinical Service MJ Harbert, MD Co-Director, NeuroNICU Service Rady Children s Hospital San Diego What is a NeuroNICU? Collaboration between Neonatology and Neurology Neonatal
Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1
 Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1 Therapeutic Hypothermia for Neonatal Encephalopathy: Preparation for Transport to Cooling Center Teresa Z. Baker, DNP-S Annie L. Addison, FNP-S NURS
Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1 Therapeutic Hypothermia for Neonatal Encephalopathy: Preparation for Transport to Cooling Center Teresa Z. Baker, DNP-S Annie L. Addison, FNP-S NURS
withdrawal of antiepileptic treatment in the neonatal period
 Archives of Disease in Childhood 1995; 72: F97-F1l1 Department of Paediatrics L Hellstrom-Westas G Blennow M Iindroth N W Svenningsen Department of Clinical Neurophysiology I Rosen Neonatal Intensive Care
Archives of Disease in Childhood 1995; 72: F97-F1l1 Department of Paediatrics L Hellstrom-Westas G Blennow M Iindroth N W Svenningsen Department of Clinical Neurophysiology I Rosen Neonatal Intensive Care
State of Florida Systemic Supportive Care Guidelines. Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology
 State of Florida Systemic Supportive Care Guidelines Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. FEN 1. What intravenous fluids should be initiated upon admission
State of Florida Systemic Supportive Care Guidelines Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. FEN 1. What intravenous fluids should be initiated upon admission
I t is increasingly recognised that arterial cerebral infarction
 F252 ORIGINAL ARTICLE Does cranial ultrasound imaging identify arterial cerebral infarction in term neonates? F Cowan, E Mercuri, F Groenendaal, L Bassi, D Ricci, M Rutherford, L de Vries... See end of
F252 ORIGINAL ARTICLE Does cranial ultrasound imaging identify arterial cerebral infarction in term neonates? F Cowan, E Mercuri, F Groenendaal, L Bassi, D Ricci, M Rutherford, L de Vries... See end of
Early instrumental predictors of long term neurodevelopmental impairment in newborns with perinatal asphyxia treated with therapeutic hypothermia
 SIGNA VITAE 218; 14(1): 81-85 Early instrumental predictors of long term neurodevelopmental impairment in newborns with perinatal asphyxia treated with therapeutic hypothermia ALICE MONZANI 1, GIANLUCA
SIGNA VITAE 218; 14(1): 81-85 Early instrumental predictors of long term neurodevelopmental impairment in newborns with perinatal asphyxia treated with therapeutic hypothermia ALICE MONZANI 1, GIANLUCA
There are several types of epilepsy. Each of them have different causes, symptoms and treatment.
 1 EPILEPSY Epilepsy is a group of neurological diseases where the nerve cell activity in the brain is disrupted, causing seizures of unusual sensations, behavior and sometimes loss of consciousness. Epileptic
1 EPILEPSY Epilepsy is a group of neurological diseases where the nerve cell activity in the brain is disrupted, causing seizures of unusual sensations, behavior and sometimes loss of consciousness. Epileptic
EEG in the ICU: Part I
 EEG in the ICU: Part I Teneille E. Gofton July 2012 Objectives To outline the importance of EEG monitoring in the ICU To briefly review the neurophysiological basis of EEG To introduce formal EEG and subhairline
EEG in the ICU: Part I Teneille E. Gofton July 2012 Objectives To outline the importance of EEG monitoring in the ICU To briefly review the neurophysiological basis of EEG To introduce formal EEG and subhairline
Wales Neonatal Network Guideline Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling.
 Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling. (Including flowchart for infants fulfilling A criteria or A and B criteria only) Perinatal asphyxia
Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling. (Including flowchart for infants fulfilling A criteria or A and B criteria only) Perinatal asphyxia
TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised by P.
 TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised 05-13-13 by P. Joe SCREENING FOR POTENTIAL COOLING PATIENTS Patients who are >
TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised 05-13-13 by P. Joe SCREENING FOR POTENTIAL COOLING PATIENTS Patients who are >
NEUROPROTECTIVE CARE IN ACTION:
 NEUROPROTECTIVE CARE IN ACTION: aeeg & NIRS monitoring No Disclosures or Conflicts of Interest Alexis Davis, MD, MS Epi Care of the Newborn Brain Symposium September 14, 2017 Overview aeeg Understanding
NEUROPROTECTIVE CARE IN ACTION: aeeg & NIRS monitoring No Disclosures or Conflicts of Interest Alexis Davis, MD, MS Epi Care of the Newborn Brain Symposium September 14, 2017 Overview aeeg Understanding
NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY
 Background NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY A perinatal hypoxic-ischaemic insult may present with varying degrees of neonatal encephalopathy, neurological disorder and
Background NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY A perinatal hypoxic-ischaemic insult may present with varying degrees of neonatal encephalopathy, neurological disorder and
Imaging the Premature Brain- New Knowledge
 Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Neonatal Seizures: Etiology and Hospital Outcome
 Neonatal Seizures: Etiology and Hospital Outcome *Sarker SA, 1 Ahmed SF, 2 Rahman MM, 3 Ali SS, 4 Rehana Z, 5 Ahmed S, 6 Farzana F, 7 Bose BK, 8 Begum J 9 Neonatal seizures are a manifestation of neurological
Neonatal Seizures: Etiology and Hospital Outcome *Sarker SA, 1 Ahmed SF, 2 Rahman MM, 3 Ali SS, 4 Rehana Z, 5 Ahmed S, 6 Farzana F, 7 Bose BK, 8 Begum J 9 Neonatal seizures are a manifestation of neurological
Advancing Neurologic Care in the Intensive Care Nursery
 Article neurology Advancing Neurologic Care in the Intensive Care Nursery Hannah C. Glass, MDCM* AUTHOR DISCLOSURE Dr Glass has disclosed that she is supported by grant K23NS066137 from the National Institute
Article neurology Advancing Neurologic Care in the Intensive Care Nursery Hannah C. Glass, MDCM* AUTHOR DISCLOSURE Dr Glass has disclosed that she is supported by grant K23NS066137 from the National Institute
Inclusion criteria for cooling: Babies should be assessed for 3 criteria: A, B and C. See Appendix 1 for a decision making flowchart.
 Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling. (Including flowchart for infants fulfilling A criteria or A and B criteria only) Perinatal asphyxia
Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling. (Including flowchart for infants fulfilling A criteria or A and B criteria only) Perinatal asphyxia
Perlman J, Clinics Perinatol 2006; 33: Underlying causal pathways. Antenatal Intrapartum Postpartum. Acute near total asphyxia
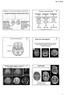 Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Perinatal asphyxia: Pathophysiology and therapy
 Perinatal asphyxia: Pathophysiology and therapy Peter Davis Melbourne Australia With thanks to Dr Sue Jacobs Moderate or severe HIE Complicates ~1/1000 term live births: Mortality: >25% Major neurological
Perinatal asphyxia: Pathophysiology and therapy Peter Davis Melbourne Australia With thanks to Dr Sue Jacobs Moderate or severe HIE Complicates ~1/1000 term live births: Mortality: >25% Major neurological
Seizure burden and neurodevelopmental outcome in neonates with hypoxic ischemic encephalopathy
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Seizure burden and neurodevelopmental outcome in neonates with hypoxic ischemic encephalopathy LIUDMILA KHAROSHANKAYA 1,2 NATHAN J STEVENSON 1
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Seizure burden and neurodevelopmental outcome in neonates with hypoxic ischemic encephalopathy LIUDMILA KHAROSHANKAYA 1,2 NATHAN J STEVENSON 1
Effect of prophylactic phenobarbital on seizures, encephalopathy and mortality in neonates with perinatal asphyxia
 of Journal Child Health Health SA RESEARCH Effect of prophylactic phenobarbital on seizures, encephalopathy and mortality in neonates with perinatal asphyxia S Velaphi, M Mokhachane, R Mphahlele, E Beckh-Arnold
of Journal Child Health Health SA RESEARCH Effect of prophylactic phenobarbital on seizures, encephalopathy and mortality in neonates with perinatal asphyxia S Velaphi, M Mokhachane, R Mphahlele, E Beckh-Arnold
COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY
 COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY Roger F. Soll H. Wallace Professor of Neonatology University of Vermont 19 th International Symposium on Neonatology Sao Paulo, Brazil DISCLOSURE Roger F. Soll
COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY Roger F. Soll H. Wallace Professor of Neonatology University of Vermont 19 th International Symposium on Neonatology Sao Paulo, Brazil DISCLOSURE Roger F. Soll
Neonatal Seizures The Tip of the Iceberg. Courtney Wusthoff, MD MS Assistant Professor, Neurology Neurology Director, LPCH Neuro NICU
 Neonatal Seizures The Tip of the Iceberg Courtney Wusthoff, MD MS Assistant Professor, Neurology Neurology Director, LPCH Neuro NICU Disclosures I have no conflicts of interest I will discuss off-label
Neonatal Seizures The Tip of the Iceberg Courtney Wusthoff, MD MS Assistant Professor, Neurology Neurology Director, LPCH Neuro NICU Disclosures I have no conflicts of interest I will discuss off-label
RESEARCH BRIEF. Prognostic Value of Resistive Index in Neonates with Hypoxic Ischemic
 RESEARCH BRIEF Prognostic Value of Resistive Index in Neonates with Hypoxic Ischemic A Senthil Kumar, Aparna Chandrasekaran, Rajamannar Asokan and *Kathirvelu Gopinathan From the Department of Neonatology,
RESEARCH BRIEF Prognostic Value of Resistive Index in Neonates with Hypoxic Ischemic A Senthil Kumar, Aparna Chandrasekaran, Rajamannar Asokan and *Kathirvelu Gopinathan From the Department of Neonatology,
Neurological Prognosis after Cardiac Arrest Guideline
 Neurological Prognosis after Cardiac Arrest Guideline I. Associated Guidelines and Appendices 1. Therapeutic Hypothermia after Cardiac Arrest 2. Hypothermia after Cardiac Arrest Algorithm II. Rationale
Neurological Prognosis after Cardiac Arrest Guideline I. Associated Guidelines and Appendices 1. Therapeutic Hypothermia after Cardiac Arrest 2. Hypothermia after Cardiac Arrest Algorithm II. Rationale
Neurodevelopmental Follow Up After Therapeutic Hypothermia for Perinatal Asphyxia
 ORIGINAL PAPER doi: 10.5455/medarh.2015.69.362-366 Med Arh. 2015 Dec; 69(6): 362-366 Received: August 25th 2015 Accepted: November 05th 2015 2015 Smail Zubcevic, Suada Heljic, Feriha Catibusic, Sajra Uzicanin,
ORIGINAL PAPER doi: 10.5455/medarh.2015.69.362-366 Med Arh. 2015 Dec; 69(6): 362-366 Received: August 25th 2015 Accepted: November 05th 2015 2015 Smail Zubcevic, Suada Heljic, Feriha Catibusic, Sajra Uzicanin,
CHAPTER 6 INTERFERENCE CANCELLATION IN EEG SIGNAL
 116 CHAPTER 6 INTERFERENCE CANCELLATION IN EEG SIGNAL 6.1 INTRODUCTION Electrical impulses generated by nerve firings in the brain pass through the head and represent the electroencephalogram (EEG). Electrical
116 CHAPTER 6 INTERFERENCE CANCELLATION IN EEG SIGNAL 6.1 INTRODUCTION Electrical impulses generated by nerve firings in the brain pass through the head and represent the electroencephalogram (EEG). Electrical
Electroencephalography. Role of EEG in NCSE. Continuous EEG in ICU 25/05/59. EEG pattern in status epilepticus
 EEG: ICU monitoring & 2 interesting cases Electroencephalography Techniques Paper EEG digital video electroencephalography Dr. Pasiri Sithinamsuwan PMK Hospital Routine EEG long term monitoring Continuous
EEG: ICU monitoring & 2 interesting cases Electroencephalography Techniques Paper EEG digital video electroencephalography Dr. Pasiri Sithinamsuwan PMK Hospital Routine EEG long term monitoring Continuous
State of Florida Hypothermia Protocol. Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology
 State of Florida Hypothermia Protocol Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. Entry Criteria 1. Gestational Age greater than or equal to 35 weeks gestation
State of Florida Hypothermia Protocol Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. Entry Criteria 1. Gestational Age greater than or equal to 35 weeks gestation
Prognosis in. Encephalopathy. Hypoxic-Ischemic. Özge Aydemİr MD
 Prognosis in Hypoxic-Ischemic Encephalopathy Özge Aydemİr MD Major problems we have to face while caring infants with HIE are; Øto provide families with reliable information about outcome. Øto decide how
Prognosis in Hypoxic-Ischemic Encephalopathy Özge Aydemİr MD Major problems we have to face while caring infants with HIE are; Øto provide families with reliable information about outcome. Øto decide how
Therapeutic Hypothermia for Hypoxic Ischaemic Encephalopathy in Singapore General Hospital: Two Patient Case Series and Review Of Literature
 case report Therapeutic Hypothermia for Hypoxic Ischaemic Encephalopathy in Singapore General Hospital: Two Patient Case Series and Review Of Literature Sridhar Arunachalam, MD, MRCPCH (UK); Woei Bing
case report Therapeutic Hypothermia for Hypoxic Ischaemic Encephalopathy in Singapore General Hospital: Two Patient Case Series and Review Of Literature Sridhar Arunachalam, MD, MRCPCH (UK); Woei Bing
Newborn Hypoxic Ischemic Brain Injury. Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford
 Newborn Hypoxic Ischemic Brain Injury Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford NO DISCLOSURES INTRODUCTION Neonatal hypoxic-ischemic encephalopathy (HIE) is a major cause
Newborn Hypoxic Ischemic Brain Injury Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford NO DISCLOSURES INTRODUCTION Neonatal hypoxic-ischemic encephalopathy (HIE) is a major cause
Clinical Neurophysiology
 Clinical Neurophysiology 120 (2009) 1046 1053 Contents lists available at ScienceDirect Clinical Neurophysiology journal homepage: www.elsevier.com/locate/clinph EEG in the healthy term newborn within
Clinical Neurophysiology 120 (2009) 1046 1053 Contents lists available at ScienceDirect Clinical Neurophysiology journal homepage: www.elsevier.com/locate/clinph EEG in the healthy term newborn within
Hypothermia: Neuroprotective Treatment of Hypoxic-Ischemic Encephalopathy. Serious perinatal asphyxia. Therapeutic hypothermia
 Therapeutic hypothermia Hypothermia: Neuroprotective Treatment of Hypoxic-Ischemic Encephalopathy Background of hypothermia Clinical application Floris Groenendaal Department of Neonatology Complications
Therapeutic hypothermia Hypothermia: Neuroprotective Treatment of Hypoxic-Ischemic Encephalopathy Background of hypothermia Clinical application Floris Groenendaal Department of Neonatology Complications
Neonatal Therapeutic Hypothermia. A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi
 Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Neonatal Seizure. Dr.Nawar Yahya. Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan. Supervised by:
 Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Hypoxic ischaemic encephalopathy
 Hypoxic ischaemic encephalopathy Frances Cowan Denis Azzopardi Abstract Encephalopathy occurring soon after birth continues to be a major complication in near- and full-term newborn infants. Early neonatal
Hypoxic ischaemic encephalopathy Frances Cowan Denis Azzopardi Abstract Encephalopathy occurring soon after birth continues to be a major complication in near- and full-term newborn infants. Early neonatal
Electroencephalography
 The electroencephalogram (EEG) is a measure of brain waves. It is a readily available test that provides evidence of how the brain functions over time. The EEG is used in the evaluation of brain disorders.
The electroencephalogram (EEG) is a measure of brain waves. It is a readily available test that provides evidence of how the brain functions over time. The EEG is used in the evaluation of brain disorders.
Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia
 International Pediatrics Volume 2011, Article ID 848413, 5 pages doi:10.1155/2011/848413 Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia Pia Wintermark Division of Newborn
International Pediatrics Volume 2011, Article ID 848413, 5 pages doi:10.1155/2011/848413 Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia Pia Wintermark Division of Newborn
Serum Lactate, Brain Magnetic Resonance Imaging and Outcome of Neonatal Hypoxic Ischemic Encephalopathy after Therapeutic Hypothermia
 Pediatrics and Neonatology (2016) 57, 35e40 Available online at www.sciencedirect.com ScienceDirect journal homepage: http://www.pediatr-neonatol.com ORIGINAL ARTICLE Serum Lactate, Brain Magnetic Resonance
Pediatrics and Neonatology (2016) 57, 35e40 Available online at www.sciencedirect.com ScienceDirect journal homepage: http://www.pediatr-neonatol.com ORIGINAL ARTICLE Serum Lactate, Brain Magnetic Resonance
Chapter 7 Heart Rate Variability in Newborns with Hypoxic Brain Injury
 Chapter 7 Heart Rate Variability in Newborns with Hypoxic Brain Injury Vladimir Matić, Perumpillichira J. Cherian, Devy Widjaja, Katrien Jansen, Gunnar Naulaers, Sabine Van Huffel, and Maarten De Vos Abstract
Chapter 7 Heart Rate Variability in Newborns with Hypoxic Brain Injury Vladimir Matić, Perumpillichira J. Cherian, Devy Widjaja, Katrien Jansen, Gunnar Naulaers, Sabine Van Huffel, and Maarten De Vos Abstract
EEG workshop. Epileptiform abnormalities. Definitions. Dr. Suthida Yenjun
 EEG workshop Epileptiform abnormalities Paroxysmal EEG activities ( focal or generalized) are often termed epileptiform activities EEG hallmark of epilepsy Dr. Suthida Yenjun Epileptiform abnormalities
EEG workshop Epileptiform abnormalities Paroxysmal EEG activities ( focal or generalized) are often termed epileptiform activities EEG hallmark of epilepsy Dr. Suthida Yenjun Epileptiform abnormalities
RESULTS: Seizures Primary Outcomes Survey AUGUST 2016
 RESULTS: Seizures Primary Outcomes Survey AUGUST 2016 1 Statistical analysis Descriptive statistics were used to describe the characteristics and responses of the respondents overall and split by specialty
RESULTS: Seizures Primary Outcomes Survey AUGUST 2016 1 Statistical analysis Descriptive statistics were used to describe the characteristics and responses of the respondents overall and split by specialty
CEREBRAL OXIMETRY IN INFANTS WITH HIE DAPHNA YASOVA BARBEAU, MD FN3 MEETING 2018
 CEREBRAL OXIMETRY IN INFANTS WITH HIE DAPHNA YASOVA BARBEAU, MD FN3 MEETING 2018 OBJECTIVES 1. Understand how cerebral oximetry works 2. Understand how cerebral oximetry may guide intervention 3. Learn
CEREBRAL OXIMETRY IN INFANTS WITH HIE DAPHNA YASOVA BARBEAU, MD FN3 MEETING 2018 OBJECTIVES 1. Understand how cerebral oximetry works 2. Understand how cerebral oximetry may guide intervention 3. Learn
A study of clinico-biochemical profile of neonatal seizure: A tertiary care hospital study
 Original Research Article A study of clinico-biochemical profile of neonatal seizure: A tertiary care hospital study Wakil Paswan 1*, Bankey Behari Singh 2 1 Assistant Professor, 2 Associate Professor
Original Research Article A study of clinico-biochemical profile of neonatal seizure: A tertiary care hospital study Wakil Paswan 1*, Bankey Behari Singh 2 1 Assistant Professor, 2 Associate Professor
Natalia Gorelik 1, Ricardo Faingold 2, Alan Daneman 3, Monica Epelman 3,4. Original Article
 Original Article Intraventricular hemorrhage in term neonates with hypoxicischemic encephalopathy: a comparison study between neonates treated with and without hypothermia Natalia Gorelik 1, Ricardo Faingold
Original Article Intraventricular hemorrhage in term neonates with hypoxicischemic encephalopathy: a comparison study between neonates treated with and without hypothermia Natalia Gorelik 1, Ricardo Faingold
Effect of Sedation and Analgesia on Postoperative Amplitude-Integrated EEG in Newborn Cardiac Patients
 0031-3998/10/6706-0650 PEDIATRIC RESEARCH Copyright 2010 International Pediatric Research Foundation, Inc. Vol. 67, No. 6, 2010 Printed in U.S.A. Effect of Sedation and Analgesia on Postoperative Amplitude-Integrated
0031-3998/10/6706-0650 PEDIATRIC RESEARCH Copyright 2010 International Pediatric Research Foundation, Inc. Vol. 67, No. 6, 2010 Printed in U.S.A. Effect of Sedation and Analgesia on Postoperative Amplitude-Integrated
EEG in Medical Practice
 EEG in Medical Practice Dr. Md. Mahmudur Rahman Siddiqui MBBS, FCPS, FACP, FCCP Associate Professor, Dept. of Medicine Anwer Khan Modern Medical College What is the EEG? The brain normally produces tiny
EEG in Medical Practice Dr. Md. Mahmudur Rahman Siddiqui MBBS, FCPS, FACP, FCCP Associate Professor, Dept. of Medicine Anwer Khan Modern Medical College What is the EEG? The brain normally produces tiny
This is a repository copy of An introduction to neonatal EEG. White Rose Research Online URL for this paper:
 This is a repository copy of An introduction to neonatal EEG. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/124766/ Version: Accepted Version Article: Alix, J.J.P. orcid.org/0000-0001-8391-9749,
This is a repository copy of An introduction to neonatal EEG. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/124766/ Version: Accepted Version Article: Alix, J.J.P. orcid.org/0000-0001-8391-9749,
Periodic and Rhythmic Patterns. Suzette M LaRoche, MD Mission Health Epilepsy Center Asheville, North Carolina
 Periodic and Rhythmic Patterns Suzette M LaRoche, MD Mission Health Epilepsy Center Asheville, North Carolina Continuum of EEG Activity Neuronal Injury LRDA GPDs SIRPIDs LPDs + NCS Burst-Suppression LPDs
Periodic and Rhythmic Patterns Suzette M LaRoche, MD Mission Health Epilepsy Center Asheville, North Carolina Continuum of EEG Activity Neuronal Injury LRDA GPDs SIRPIDs LPDs + NCS Burst-Suppression LPDs
Int J Clin Exp Med 2014;7(4): /ISSN: /IJCEM
 Int J Clin Exp Med 2014;7(4):1099-1104 www.ijcem.com /ISSN:1940-5901/IJCEM0000283 Original Article Value of amplitude-integrated electroencephalograph in early diagnosis and prognosis prediction of neonatal
Int J Clin Exp Med 2014;7(4):1099-1104 www.ijcem.com /ISSN:1940-5901/IJCEM0000283 Original Article Value of amplitude-integrated electroencephalograph in early diagnosis and prognosis prediction of neonatal
VALIDATION OF AN AUTOMATED SEIZURE DETECTION SYSTEM ON HEALTHY BABIES Histogram-based Energy Normalization for Montage Mismatch Compensation
 VALIDATION OF AN AUTOMATED SEIZURE DETECTION SYSTEM ON HEALTHY BABIES Histogram-based Energy Normalization for Montage Mismatch Compensation A. Temko 1, I. Korotchikova 2, W. Marnane 1, G. Lightbody 1
VALIDATION OF AN AUTOMATED SEIZURE DETECTION SYSTEM ON HEALTHY BABIES Histogram-based Energy Normalization for Montage Mismatch Compensation A. Temko 1, I. Korotchikova 2, W. Marnane 1, G. Lightbody 1
Disclosures. Objectives. Definition: HIE. HIE: Incidence. Impact 9/10/2018. Hypoxic Ischemic Encephalopathy in the Neonate
 Disclosures Hypoxic Ischemic Encephalopathy in the Neonate No relevant financial relationships or conflicts of interest to disclose Franscesca Miquel-Verges MD 2018 Review therapies currently under research
Disclosures Hypoxic Ischemic Encephalopathy in the Neonate No relevant financial relationships or conflicts of interest to disclose Franscesca Miquel-Verges MD 2018 Review therapies currently under research
FANNP 28TH NATIONAL NNP SYMPOSIUM: CLINICAL UPDATE AND REVIEW OCTOBER 17-21, 2017
 Pulse Oximetry in the Delivery Room: Principles and Practice GS2 3 Jonathan P. Mintzer, MD, FAAP Assistant Professor of Pediatrics Stony Brook Children s Hospital, Division of Neonatal-Perinatal Medicine,
Pulse Oximetry in the Delivery Room: Principles and Practice GS2 3 Jonathan P. Mintzer, MD, FAAP Assistant Professor of Pediatrics Stony Brook Children s Hospital, Division of Neonatal-Perinatal Medicine,
Chapter 7. Neuropediatrics 2007; 38 (5): Lara Leijser Alla Vein Lishya Liauw Tzipi Strauss Sylvia Veen Gerda van Wezel-Meijler
 Chapter 7 Prediction of short-term neurological outcome in full-term neonates with hypoxic-ischaemic encephalopathy based on combined use of electroencephalogram and neuro-imaging Lara Leijser Alla Vein
Chapter 7 Prediction of short-term neurological outcome in full-term neonates with hypoxic-ischaemic encephalopathy based on combined use of electroencephalogram and neuro-imaging Lara Leijser Alla Vein
Neonatal EEG Maturation
 Neonatal EEG Maturation Cindy Jenkinson, R. EEG T., CLTM October 7, 2017 Fissure Development 3 http://www.hhmi.org/biointeractive/develop ment-human-embryonic-brain 4 WHAT IS IMPORTANT TO KNOW BEFORE I
Neonatal EEG Maturation Cindy Jenkinson, R. EEG T., CLTM October 7, 2017 Fissure Development 3 http://www.hhmi.org/biointeractive/develop ment-human-embryonic-brain 4 WHAT IS IMPORTANT TO KNOW BEFORE I
HIE (Hypoxic Ischaemic Encephalopathy)
 HIE (Hypoxic Ischaemic Encephalopathy) Document Title and Reference : HIE (Hypoxic Ischaemic Encephalopathy Main Auth (s) Kiran Yajamanyam Consultant LWH Ratified by: CM NSG Date Ratified: May 2017 Review
HIE (Hypoxic Ischaemic Encephalopathy) Document Title and Reference : HIE (Hypoxic Ischaemic Encephalopathy Main Auth (s) Kiran Yajamanyam Consultant LWH Ratified by: CM NSG Date Ratified: May 2017 Review
Study of renal functions in neonatal asphyxia
 Original article: Study of renal functions in neonatal asphyxia *Dr. D.Y.Shrikhande, **Dr. Vivek Singh, **Dr. Amit Garg *Professor and Head, **Senior Resident Department of Pediatrics, Pravara Institute
Original article: Study of renal functions in neonatal asphyxia *Dr. D.Y.Shrikhande, **Dr. Vivek Singh, **Dr. Amit Garg *Professor and Head, **Senior Resident Department of Pediatrics, Pravara Institute
NEONATAL SEIZURES-PGPYREXIA REVIEW
 NEONATAL SEIZURES-PGPYREXIA REVIEW This is a very important Postgraduate topics will few Q asked in undergraduation also. Lets see them in detail. References: 1.Volpe s Neurology of newborn 2.Nelson s
NEONATAL SEIZURES-PGPYREXIA REVIEW This is a very important Postgraduate topics will few Q asked in undergraduation also. Lets see them in detail. References: 1.Volpe s Neurology of newborn 2.Nelson s
Outcome of infants with hypoxic ischemic encephalopathy treated with brain hypothermia
 bs_bs_banner doi:10.1111/jog.12520 J. Obstet. Gynaecol. Res. Vol. 41, No. 2: 229 237, February 2015 Outcome of infants with hypoxic ischemic encephalopathy treated with brain hypothermia Takuya Tokuhisa
bs_bs_banner doi:10.1111/jog.12520 J. Obstet. Gynaecol. Res. Vol. 41, No. 2: 229 237, February 2015 Outcome of infants with hypoxic ischemic encephalopathy treated with brain hypothermia Takuya Tokuhisa
Unilateral neonatal cerebral infarction in full term infants
 F88 Department of Paediatrics, John RadcliVe Hospital, Oxford, OX3 9DU J Estan P Hope Correspondence to: Dr Peter Hope. Accepted 11 December 1996 Unilateral neonatal cerebral infarction in full term infants
F88 Department of Paediatrics, John RadcliVe Hospital, Oxford, OX3 9DU J Estan P Hope Correspondence to: Dr Peter Hope. Accepted 11 December 1996 Unilateral neonatal cerebral infarction in full term infants
Epilepsy in children with cerebral palsy
 Seizure 2003; 12: 110 114 doi:10.1016/s1059 1311(02)00255-8 Epilepsy in children with cerebral palsy A.K. GURURAJ, L. SZTRIHA, A. BENER,A.DAWODU & V. EAPEN Departments of Paediatrics, Community Medicine
Seizure 2003; 12: 110 114 doi:10.1016/s1059 1311(02)00255-8 Epilepsy in children with cerebral palsy A.K. GURURAJ, L. SZTRIHA, A. BENER,A.DAWODU & V. EAPEN Departments of Paediatrics, Community Medicine
Early predictors of outcome in infants treated with hypothermia for hypoxic ischaemic encephalopathy
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Early predictors of outcome in infants treated with hypothermia for hypoxic ischaemic encephalopathy NAZAKAT MERCHANT 1,2 DENIS AZZOPARDI 1 1 Centre
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Early predictors of outcome in infants treated with hypothermia for hypoxic ischaemic encephalopathy NAZAKAT MERCHANT 1,2 DENIS AZZOPARDI 1 1 Centre
HHS Public Access Author manuscript Pediatr Res. Author manuscript; available in PMC 2014 October 01.
 Early Electrographic Seizures, Brain Injury an Neurodevelopmental Risk in the Very Preterm Infant Zachary A. Vesoulis 1, Terrie E. Inder 1, Lianne J. Woodward 1, Bradley Buse 2, Claudine Vavasseur 3, and
Early Electrographic Seizures, Brain Injury an Neurodevelopmental Risk in the Very Preterm Infant Zachary A. Vesoulis 1, Terrie E. Inder 1, Lianne J. Woodward 1, Bradley Buse 2, Claudine Vavasseur 3, and
