Therapeutic Hypothermia for Hypoxic Ischaemic Encephalopathy in Singapore General Hospital: Two Patient Case Series and Review Of Literature
|
|
|
- Eileen McLaughlin
- 5 years ago
- Views:
Transcription
1 case report Therapeutic Hypothermia for Hypoxic Ischaemic Encephalopathy in Singapore General Hospital: Two Patient Case Series and Review Of Literature Sridhar Arunachalam, MD, MRCPCH (UK); Woei Bing Poon, MRCPCH (UK), FAMS Neonatal and Developmental Medicine, Singapore General Hospital Abstract Neonatal encephalopathy affects 2 5/1000 live births and hypoxic ischaemic encephalopathy (HIE) is the major cause 1. Therapeutic hypothermia reduces brain injury and improves the neurodevelopmental outcome. We are sharing our local experience in therapeutic hypothermia in the form of a case series of two patients. Our incidence of moderate to severe HIE is 0.6/1000 live births. Both patients were cooled for 72 hours. The challenges faced were mainly in the time taken for achieving the target temperature and the time needed for re-warming, which varied from one to six hours and 4 24 hours, respectively. Complications like hyponatremia, hypokalemia, sinus bradycardia and thrombocytopenia were noted. Amplitude integrated electroencephalogram (aeeg) remained abnormal post cooling for both babies. Clinical markers, aeeg and MRI head findings combine to prognosticate well for the neurodevelopmental outcomes. We need to be familiar with the protocol for timely implementation of cooling, whichever the cooling method. Concentrating these high-risk cases in selected tertiary centres capable of instituting cooling as well as long-term follow-up will ensure better outcomes. Keywords: Encephalopathy, Neonate, Selective head cooling INTRODUCTION Hypoxic ischaemic encephalopathy (HIE) constitutes a major cause for neonatal encephalopathy. Until recently, management of a newborn with encephalopathy has consisted largely of supportive care to restore and maintain cerebral perfusion, provide adequate gas exchange and treat seizure activity. Hypothermia is the only available treatment for HIE presently. Neuronal death occurs in two phases which is immediate from cellular hypoxia and primary energy failure and delayed which occurs six hours later. The secondary phase continues over a period of several days leading to apoptosis or programmed cell death 2,3. The window of opportunity lies in the initial six hours before apoptosis sets in 4. It This Title was accepted as a Poster in the ISPPAC 2012 Conference, Singapore. has been shown that better neurodevelopmental outcome is expected if the intervention occurs in the first six hours of life. Cooling helps in reduced metabolic rate, reducing the excitatory amino acids and lowering production of nitric oxide and free radicals and ultimately reduce apoptosis. Cooling can be selective head cooling or whole body cooling. RCTs have shown that both are effective. Head cooling is preferred by some as the brain produces 70% of body heat whereas whole body cooling is preferred as core body temperature and deeper brain structures are of the same temperature 5. We initiated selective head cooling as we find it easier to manage the baby in terms of nursing and also maintenance of stable core temperature. 286 Proceedings of Singapore Healthcare Volume 21 Number
2 Therapeutic Hypothermia for HIE Our hospital s inclusion and exclusion criteria for initiating head cooling are as follows: Inclusion Criteria: Infants >35weeks gestation with one of the following: Apgar score <5 at 10 min after birth Continued need for resuscitation, at 10 min after birth Acidosis (cord ph/arterial ph with in 60 min of birth <7.00) Base deficit 12mmol/L {within 60 min of birth (arterial/ venous)} ph and base deficit of between mmol/l within 1st hour. Hypoxic Ischaemic Encephalopathy Score 7 based on HIE Scoring System by Thompson Abnormal aeeg <6 hours of life Exclusion criteria: Infants >6 hours at the start of cooling Major congenital abnormalities Imperforate anus (prevent rectal temperature recordings) Evidence of neurologically significant head trauma or skull fracture causing major intracranial haemorrhage. Subgaleal bleeding is a relative contraindication Coagulopathy with active bleeding Severe PPHN a relative contraindication Birth weight <1800g Infants in extremis (those infants for whom no other additional intensive management will be offered) Targets aimed for cooling: To begin within six hours of birth Initiate passive cooling at the earliest Target rectal temperature range for selective head cooling of degree Celsius. Rewarming to be initiated after 72 hours of cooling Passive rewarming over at least 6 12 hours (not >0.5 degree Celsius increment per hour) Investigations done during the process of cooling as per protocol are given below: ABG FBC, serum lactate, pyruvate, troponin, ammonia, CPK (total), electrolytes (icalcium, Mg, PO4, U/E/Creatinine), ALP: at 0, 12, 24, 48, 72hours or more frequently as indicated PT/PTT and LFT on admission, at 24, 48 and 72 hours Chest X-ray, ECG and 2D echocardiography as indicated (arrhythmia, prolonged QT, PPHN) Blood glucose monitoring and blood culture if indicated Cranial ultrasound on admission Continue investigations until 24 hours after rewarming is complete. We used Thompson scoring system 6 instead of Sarnat and Sarnat HIE scoring system from June 2011 as we found it easier to record with less variables and is effective in monitoring the neurological status in comparison to Sarnat and Sarnat s staging system. CASE 1 Case 1 is a one-year-old Malay boy, delivered by emergency crash Caesarean section for antepartum haemorrhage at 36+3/52 gestation, with maternal history of severe pre-eclampsia, on labetalol and alpha methyl dopa and maternal Group B Streptococcus, Candida positive in high vaginal swab culture. Placental histopathology 287
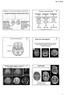
3 Case Report Fig. 1. aeeg at 5 hours of life in Case 1 showing burst suppression showed retroplacental haematoma with ischaemia. His birthweight was 2310 g. He was born flat at birth requiring intubation within one minute of life and external cardiac massage. Heart rate improved with intubation but he remained hypotonic without any spontaneous respiration. He was transported to NICU on neopuff, 18//5, FiO2 0.5, SpO2 100%. His Cord ph was 6.724, bicarbonate of 8.9 mmol/l and base deficit of His Apgar score being 2, 5, 5 at 1, 5 and 10 minutes. He was classified as having severe HIE based on Sarnat and Sarnat staging system. Selective head cooling was initiated at three hours of life with passive cooling being initiated at 20 minutes of life. Target temperature of degree Celsius was achieved in one hour of initiation and baby was cooled for 72 hours. Rewarming was done over a period of 24 hours in view of seizures noted during rewarming. Amplitude integrated EEG (aeeg) was used for this baby (fig. 1). Initially aeeg at five hours of life showed burst suppression pattern and did not normalise even after rewarming. Complications like seizures, hyponatremia and sinus bradycardia were noted during cooling. Standard EEG at 23 days of life was reported as abnormal, consistent with cerebral dysmaturity but with no obvious seizure activity. Cranial ultrasound done on day one and four was reported normal. MRI brain scan done on day 11 of life showed restricted diffusion of the genu and splenium of corpus callosum, bilateral cortico spinal tracts and lentiform nucleus, suggestive of HIE. His comorbidities at discharge were feeding difficulty which required tube feeding and seizures requiring phenobarbitone which was weaned off eventually at six weeks of age. He also manifests spastic quadriparesis requiring physiotherapy and occupational therapy. Initial hearing and visual screen were abnormal but on formal assessment at two months, shown to have normal hearing and visual assessments. His current developmental assessment reveals his gross motor age to be three to four months and fine motor, language and social fields at around four months, at his current age of one year. He also has microcephaly with a head circumference of 43 cm. CASE 2 Case 2 is a seven-months-old Chinese girl delivered by crash Caesarean section for fetal distress at term gestation. Her birthweight was 3920 g. Her mother had gestational diabetes mellitus, on diet control, 288
4 Therapeutic Hypothermia for HIE Fig.2. MRI brain image with Proton spectroscopy in Case 2. Metabolites like Myoinositol, Creatine, Choline, Nacetylaspartate (NAA) and lactate are used as markers for brain insult in MR spectroscopy. Abnormal lactate production at 1.31 ppm in the watershed areas is noted in this image and noted to have decreased fetal movements but sought medical attention after two days. Placental histopathology showed placental infarction with dystrophic calcification laden with pigment laden macrophages and nucleated RBCs indicative of fetal distress. At birth, there was thick meconium stained liquor which was aspirated and she was intubated at one minute of life as there was no respiratory effort. She was also given external cardiac massage and the umbilical venous line was inserted to give five doses of adrenaline, one dose of sodium bicarbonate, and two boluses of normal saline and finally heart beat was recordable at 20 minutes of life. Apgar scores were 0 at 1, 5, 10 minutes and 3 at 20 minutes and 4 at 25 minutes. She was transported to NICU on Neopuff on pressures of 20/5, FiO2 of 1, SpO2 of 84-95%. Cord ph was 7.182, bicarbonate of 18.9 mmol/l, base deficit of 6.1. She was diagnosed to have a Thompson s score of 17 indicating severe HIE. Passive cooling was initiated at 20 minutes of life and selective head cooling was initiated at two hours of life. Target temperature aimed was 34 to 35 degree Celsius and was achieved in six hours from the time of initiation. Rewarming was started at 72 hours of life and was achieved in 12 hours time. Amplitude integrated EEG (aeeg) was used for monitoring in her. Initial aeeg at six hours of life was that of burst suppression and normal aeeg was established by day seven of life. She also had persistent pulmonary hypertension requiring magnesium sulphate infusion which was weaned off over four days from day one. Complications noted during cooling were thrombocytopenia, hypotension (requiring 3 inotropes: dopamine, dobutamine & adrenaline), and coagulopathy. She underwent standard EEG on day 14 which was abnormal with spikes over frontal region and absence of delta brush activity. Cranial ultrasound was normal on days one and four. MRI brain with proton MR spectroscopy was performed on day nine of life (fig. 2) which revealed restricted diffusion in sub-cortical white matter extending into watershed areas suggestive of mild to moderate HIE. Abnormal lactate doublet with decreased apparent diffusion co-efficient in watershed areas were noted. Co-morbidities noted were feeding difficulty in the form of suck swallow and breathing in coordination which resolved at discharge and failed hearing screen which was re-evaluated formally and found to have impairment for higher frequencies. Neurological examination and eye screening were 289
5 Case Report normal at discharge. Her head circumference is on the 3rd centile and her developmental milestones in all fields range from four to six months at her current age of seven months. She is off phenobarbitone at three months of age and currently managed by a multidisciplinary team of paediatrician, neurologist and therapists. DISCUSSION Cooling in neonatal HIE has been studied widely in the last decade and studies have shown that there is definite benefit. Recent updated systematic review and meta-analysis 7 showed that cooling reduced the mortality and major disability at 18 months of age, especially in the moderate to severe HIE group. Six moderately asphyxiated newborns or seven severely asphyxiated newborns need to be treated to save one newborn from death or major disability. Cooling is said to be more beneficial in the moderate HIE group than the severe HIE group. Mild HIE group of babies would not benefit from this intervention but Jacobs et al 8 showed that the clinical classification alone would not be sufficient to diagnose severity accurately. Hence the use of aeeg would be of help to accurately diagnose moderate to severe HIE. Cerebral palsy and developmental delay were significantly reduced but blindness and deafness showed a trend towards reduction though not statistically significant. Evidence in the last decade in favour of cooling 9,10 in moderate to severe HIE in neonates encouraged us to initiate cooling in our hospital in the year We share our experience to aid other similar tertiary neonatal units in this region to understand the feasibility and difficulties involved in its implementation. Both babies had significant antenatal events which predisposed them for higher risk at the point of delivery requiring emergency Caesarean section. They needed active to even extensive resuscitation as in the baby in Case 2. We went ahead with cooling the baby in Case 2, although he showed response only at 20 minutes of resuscitation, after discussion with parents about long-term survival, morbidities and consequences of doing so. There were difficulties in incorporating cooling both at initiation, to achieve target temperature, and also at completion and rewarming. Each baby varied in their time to achieve target temperatures from one to six hours and rewarming extended from 4 to 24 hours (24 hours due to recurrent seizures at the time of rewarming in the baby in Case 1). Both babies were monitored for complications and laboratory investigations were done according to the protocol. Electrolyte abnormalities (hyponatremia) and thrombocytopenia were noted during cooling. Amplitude integrated EEG was used in both babies. The baby in Case 1 remained abnormal throughout the monitoring period whereas the baby in Case 2 normalised on day seven of life. MRI findings were suggestive of HIE in both babies and the addition of spectroscopy in the baby in Case 2 added support to the findings. Co-morbidities were seen in the form of feeding difficulties in both the severely affected babies; though the baby in Case 2 improved at the time of discharge but went on to develop hearing impairment. Both these babies were also on follow-up noted to have global developmental delay with microcephaly, with it being more severe in the baby in Case 1. Prognosis in babies with HIE would be detrimental if it is scored as severe, has early onset of seizures 11, needs more than 30 minutes for initiation of spontaneous respiration 12, has abnormal aeeg and return of sleep wake cycle occurs after 36 hours and MRI/MR Spectroscopy done at 7 10 days shows grade 3 changes 13 (>30% central or peripheral brain matter involvement). Both babies in our report were categorised as severe HIE, needed >30 minutes to achieve spontaneous respiration, had abnormal aeeg 14,15,16 <6hours and return of sleep wake cycle was >36 hours, although it never normalised in the baby in Case 1. MRI changes were suggestive of HIE although not graded as above. Based on the above risk factors, the neurodevelopmental prognosis seems to be guarded in both these babies. Since August 2010, studies have been carried out by the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) to further refine the hypothermia intervention in the form of late initiation of cooling (6 24 hours) and use of varying depth of cooling 33.5 versus 32 degree Celsius and changing the duration to
6 Therapeutic Hypothermia for HIE Comparison of Salient Features of Two Babies with HIE on Therapeutic Hypothermia. Salient Features 1st baby ( 1 year old) 2nd baby (7 months old) Method of cooling Selective Head cooling Selective Head cooling Time to achieve target temperature 1 hour 6 hours Time to re-warm 24 hours 12 hours Complications during cooling Seizures, Hyponatremia and Sinus bradycardia Thrombocytopenia, hypotension and coagulopathy Time taken to achieve normal aeeg Never normalised even after 1 week Normalised on day 7 of life. MRI findings Neurodevelopmental outcome including co-morbidities Slight restricted diffusion of the genu & splenium of corpus callosum, bilateral cortico spinal tracts and lentiform nucleus suggestive of HIE. Global developmental delay 4 months in all fields and still being tube fed. Restricted diffusion in sub cortical white matter extending into watershed areas suggestive of mild to moderate HIE. Global developmental delay 4-6 months in all fields. She has hearing impairment for higher frequencies hours from 72 hours. Cooling in preterm babies is also being considered. The other treatment modalities as adjuvant to cooling currently under study are Topiramate, Xenon, N-acetyl cysteine, Clonidine, Melatonin, Allopurinol, Cannabinoids, Stem cells and erythropoietin1. IN CONCLUSION: Therapeutic hypothermia improves outcome after moderate to severe HIE, Whole body and selective head cooling are both effective, Long-term benefits outweigh the short-term complications faced during cooling, Regional guidelines and updates are imperative for early institution of cooling and cooling during transport 17, Medical and para-medical staff need to be well-versed with the cooling technique to initiate early cooling, as earlier institution would benefit more severely affected babies. REFERENCES 1. Pfister RH, Soll RF. Hypothermia for the treatment of infants with hypoxic ischemic Encephalopath. Journal of Perinatology 2010(30): S82 S Ferriero DM. Neonatal brain injury. N Engl J Med 2004;351(19): Nakajima W, Ishida A, Lange MS, Gabrielson KL, Wilson MA, Martin LJ, et al. Apoptosis has a prolonged role in the neurodegeneration after hypoxic ischemia in the newbornrat. J Neurosci 2000;20(21): Vannucci RC, Perlman JM. Interventions for perinatal hypoxic-ischemic encephalopathy. Pediatrics 1997;100(6): Laptook AR, Shalak L, Corbett JT. Differences in brain temperature and cerebral blood flow during selective head versus whole-body cooling. Pediatrics 2001;108: Thompson CM, Puterman AS, Linley LL, Hann FM, van der Elst CW, Molteno CD, et al. The value of a scoring system for hypoxic ischaemic encephalopathy in predicting neurodevelopmental outcome. Acta Paediatr 1997;86: Tagin MA, Woolcott CG, Vincer MJ, Whyte RK, Stinson DA. Hypothermia for neonatal hypoxic ischemic encephalopathy, an updated systematic review and metaanalysis. Arch Pediatr Adolesc Med 2012;166(6): Jacobs SE, Stewart MJ, Smith KR, Inder TE, Doyle LW, Morley C, et al. The ICE randomized trial of whole body hypothermia for hypoxic-ischemic encephalopathy (HIE). Arch Pediatr Adolesc Med2011Aug;165(8): Gluckman P, Wyatt J, Azzopardi D, Ballard R, Edwards A, Ferriero D, et al. Selective head cooling with mild systemic hypothermia after neonatal encephalopathy: multicentre randomised trial. Lancet 2005;365(9460):
7 Case Report 10. Spitzmiller RE, Phillips T, Meinzen-Derr J, Hoath SB. Amplitude-integrated EEG is useful in predicting neurodevelopmental outcome in full-term infants with hypoxic-ischemic encephalopathy: a meta-analysis. J Child Neurol 2007;22(9): Glass HC, Glidden D, Jeremy RJ, Barkovich AJ, Ferriero DM, Miller SP. Clinical neonatal seizures are independently associated with outcome in infants at risk for hypoxicischemic brain injury. J Pediatr 2009;155(3): Perlman JM, Risser R. Can asphyxiated infants at risk for neonatal seizures be rapidly identified by current highrisk markers? Pediatrics 1996;97(4): Jyoti R, O Neil R, Hurrion E. Predicting outcome in term neonates with hypoxic-ischaemic encephalopathy using simplified MR criteria. Pediatr Radiol 2006;36(1): Azzopardi D, Guarino I, Brayshaw C, Cowan F, Price- Williams D, Edwards AD, et al. Prediction of neurological outcome after birth asphyxia from early continuous two-channel electroencephalography. Early Hum Dev 1999;55(2): Van Rooij LG, Toet MC, Osredkar D, van Huffelen AC, Groenendaal F, de Vries LS. Recovery of amplitude integrated electroencephalographic background patterns within 24 hours of perinatal asphyxia. Arch Dis Child Fetal Neonatal Ed 2005;90(3):F Ter Horst HJ, Sommer C, Bergman KA, Fock JM, van Weerden TW, Bos AF. Prognostic significance of amplitude-integrated EEG during the first 72 hours after birth in severely asphyxiated neonates. Pediatr Res 2004;55(6): Fairchild K, Sokora D, Scott J, Zanelli S. Therapeutic hypothermia on neonatal transport: 4-year experience in a single NICU. Journal of Perinatology 2010;30:
Neonatal Therapeutic Hypothermia. A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi
 Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Objectives. Birth Depression Management. Birth Depression Terms
 Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Perinatal asphyxia: Pathophysiology and therapy
 Perinatal asphyxia: Pathophysiology and therapy Peter Davis Melbourne Australia With thanks to Dr Sue Jacobs Moderate or severe HIE Complicates ~1/1000 term live births: Mortality: >25% Major neurological
Perinatal asphyxia: Pathophysiology and therapy Peter Davis Melbourne Australia With thanks to Dr Sue Jacobs Moderate or severe HIE Complicates ~1/1000 term live births: Mortality: >25% Major neurological
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY
 Background NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY A perinatal hypoxic-ischaemic insult may present with varying degrees of neonatal encephalopathy, neurological disorder and
Background NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY A perinatal hypoxic-ischaemic insult may present with varying degrees of neonatal encephalopathy, neurological disorder and
7 Simple Steps to Assess & Document any Neonatal aeeg
 7 Simple Steps to Assess & Document any Neonatal aeeg Created for you by: www.aeegcoach.com How to use the Seven Simple Steps Checklist Hi! It s Kathi Randall here Your aeeg coach. I m so excited to share
7 Simple Steps to Assess & Document any Neonatal aeeg Created for you by: www.aeegcoach.com How to use the Seven Simple Steps Checklist Hi! It s Kathi Randall here Your aeeg coach. I m so excited to share
Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1
 Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1 Therapeutic Hypothermia for Neonatal Encephalopathy: Preparation for Transport to Cooling Center Teresa Z. Baker, DNP-S Annie L. Addison, FNP-S NURS
Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1 Therapeutic Hypothermia for Neonatal Encephalopathy: Preparation for Transport to Cooling Center Teresa Z. Baker, DNP-S Annie L. Addison, FNP-S NURS
Disclosures. Objectives. Definition: HIE. HIE: Incidence. Impact 9/10/2018. Hypoxic Ischemic Encephalopathy in the Neonate
 Disclosures Hypoxic Ischemic Encephalopathy in the Neonate No relevant financial relationships or conflicts of interest to disclose Franscesca Miquel-Verges MD 2018 Review therapies currently under research
Disclosures Hypoxic Ischemic Encephalopathy in the Neonate No relevant financial relationships or conflicts of interest to disclose Franscesca Miquel-Verges MD 2018 Review therapies currently under research
Queen Charlotte Hospital
 Queen Charlotte Hospital Neuroprotection for neonatal encephalopathy Neonatal encephalopathy accounts for 1 million deaths worldwide and even greater numbers of disabled survivors In countries with
Queen Charlotte Hospital Neuroprotection for neonatal encephalopathy Neonatal encephalopathy accounts for 1 million deaths worldwide and even greater numbers of disabled survivors In countries with
Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline
 Original Article Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline Stephen Attard, Doriette Soler, Paul Soler Introduction: Cerebral
Original Article Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline Stephen Attard, Doriette Soler, Paul Soler Introduction: Cerebral
No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on Needed to be resuscitated at birth
 No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on 9-16-2011 Needed to be resuscitated at birth (included assisted vent) Had generalized edema and possible
No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on 9-16-2011 Needed to be resuscitated at birth (included assisted vent) Had generalized edema and possible
COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY
 COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY Roger F. Soll H. Wallace Professor of Neonatology University of Vermont 19 th International Symposium on Neonatology Sao Paulo, Brazil DISCLOSURE Roger F. Soll
COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY Roger F. Soll H. Wallace Professor of Neonatology University of Vermont 19 th International Symposium on Neonatology Sao Paulo, Brazil DISCLOSURE Roger F. Soll
TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO
 TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO DISCLOSURE I have no relationships with commercial companies
TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO DISCLOSURE I have no relationships with commercial companies
When? Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group.
 Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group. Standard EEG 2,3% 8.6% Standard EEG + aeeg Scher MS et al; Pediatrics
Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group. Standard EEG 2,3% 8.6% Standard EEG + aeeg Scher MS et al; Pediatrics
State of Florida Hypothermia Protocol. Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology
 State of Florida Hypothermia Protocol Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. Entry Criteria 1. Gestational Age greater than or equal to 35 weeks gestation
State of Florida Hypothermia Protocol Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. Entry Criteria 1. Gestational Age greater than or equal to 35 weeks gestation
Wales Neonatal Network Guideline Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling.
 Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling. (Including flowchart for infants fulfilling A criteria or A and B criteria only) Perinatal asphyxia
Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling. (Including flowchart for infants fulfilling A criteria or A and B criteria only) Perinatal asphyxia
Inclusion criteria for cooling: Babies should be assessed for 3 criteria: A, B and C. See Appendix 1 for a decision making flowchart.
 Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling. (Including flowchart for infants fulfilling A criteria or A and B criteria only) Perinatal asphyxia
Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling. (Including flowchart for infants fulfilling A criteria or A and B criteria only) Perinatal asphyxia
Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy
 Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Hypoxic-ischemic encephalopathy has an incidence of
 Original Article Amplitude-Integrated EEG Is Useful in Predicting Neurodevelopmental Outcome in Full-Term Infants With Hypoxic-Ischemic Encephalopathy: A Meta-Analysis Journal of Child Neurology Volume
Original Article Amplitude-Integrated EEG Is Useful in Predicting Neurodevelopmental Outcome in Full-Term Infants With Hypoxic-Ischemic Encephalopathy: A Meta-Analysis Journal of Child Neurology Volume
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Hypoxic Ischemic Encephalopathy. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Hypoxic Ischemic Encephalopathy. These podcasts are designed to give medical students an overview of key topics in pediatrics.
Too Cool? Hypoxic Ischemic Encephalopathy and Therapeutic Hypothermia. Lauren Sacco DNP, ARNP, NNP-BC
 Too Cool? Hypoxic Ischemic Encephalopathy and Therapeutic Hypothermia Lauren Sacco DNP, ARNP, NNP-BC Pathophysiology of HIE Occurs in two energy failure phases: First phase happens during the initial insult
Too Cool? Hypoxic Ischemic Encephalopathy and Therapeutic Hypothermia Lauren Sacco DNP, ARNP, NNP-BC Pathophysiology of HIE Occurs in two energy failure phases: First phase happens during the initial insult
Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia
 Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia D H Karunatilaka 1, G W D S Amaratunga 2, K D N I Perera 3, V Caldera 4
Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia D H Karunatilaka 1, G W D S Amaratunga 2, K D N I Perera 3, V Caldera 4
Hypoxic-Ischemic Encephalopathy. TW de Witt University of Pretoria Department of Paediatrics Neonatology
 Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Therapeutic Hypothermia for infants > 35 wks with moderate or severe Hypoxic Ischaemic Encephalopathy (HIE) Clinical Guideline Reference Number:
 This is an official Northern Trust policy and should not be edited in any way Therapeutic Hypothermia for infants > 35 wks with moderate or severe Hypoxic Ischaemic Encephalopathy (HIE) Clinical Guideline
This is an official Northern Trust policy and should not be edited in any way Therapeutic Hypothermia for infants > 35 wks with moderate or severe Hypoxic Ischaemic Encephalopathy (HIE) Clinical Guideline
Predicting Outcomes in HIE. Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016
 Predicting Outcomes in HIE Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016 Interactive please! Case 1 Term, 3.5 kg Antenatal: Breech Labour/Delivery: Em CS failure to progress, mec
Predicting Outcomes in HIE Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016 Interactive please! Case 1 Term, 3.5 kg Antenatal: Breech Labour/Delivery: Em CS failure to progress, mec
State of Florida Systemic Supportive Care Guidelines. Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology
 State of Florida Systemic Supportive Care Guidelines Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. FEN 1. What intravenous fluids should be initiated upon admission
State of Florida Systemic Supportive Care Guidelines Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. FEN 1. What intravenous fluids should be initiated upon admission
Therapeutic hypothermia for hypoxic ischemic encephalopathy using low-technology methods: A systematic review and meta-analysis
 Therapeutic hypothermia for hypoxic ischemic encephalopathy using low-technology methods: A systematic review and meta-analysis Rossouw G 1, Irlam J 2, Horn AR 1 1)Division of Neonatal Medicine, Department
Therapeutic hypothermia for hypoxic ischemic encephalopathy using low-technology methods: A systematic review and meta-analysis Rossouw G 1, Irlam J 2, Horn AR 1 1)Division of Neonatal Medicine, Department
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants
 Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Pathophysiology Review. Hypoxic-Ischemic Encephalopathy & Therapeutic Hypothermia. Objectives. What is Hypoxic-Ischemic Encephalopathy?
 Hypoxic-Ischemic Encephalopathy & Therapeutic Hypothermia Nancy Couto Nurse Practitioner, NICU London Health Sciences Centre, Children s Hospital nancy.couto@lhsc.on.ca 2014 12 17 Objectives Review Pathophysiology
Hypoxic-Ischemic Encephalopathy & Therapeutic Hypothermia Nancy Couto Nurse Practitioner, NICU London Health Sciences Centre, Children s Hospital nancy.couto@lhsc.on.ca 2014 12 17 Objectives Review Pathophysiology
TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised by P.
 TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised 05-13-13 by P. Joe SCREENING FOR POTENTIAL COOLING PATIENTS Patients who are >
TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised 05-13-13 by P. Joe SCREENING FOR POTENTIAL COOLING PATIENTS Patients who are >
Fetal Heart Rate Monitoring Myths and Misperceptions s: Electronic Fetal Heart Rate Monitoring (EFM): Baseline Assumptions.
 Can FHR Monitoring Prevent Hypoxic-Ischemic Encephalopathy in the Newborn? Fetal Heart Rate Monitoring Myths and Misperceptions 1. Yes 2. No 72% Tekoa L. King CNM, MPH June 6, 2008 28% Yes No Objectives
Can FHR Monitoring Prevent Hypoxic-Ischemic Encephalopathy in the Newborn? Fetal Heart Rate Monitoring Myths and Misperceptions 1. Yes 2. No 72% Tekoa L. King CNM, MPH June 6, 2008 28% Yes No Objectives
Dysphagia in Encephalopathic Neonates Treated with Hypothermia
 Dysphagia in Encephalopathic Neonates Treated with Hypothermia A thesis submitted to the University of Arizona College of Medicine -- Phoenix in partial fulfillment of the requirements for the degree of
Dysphagia in Encephalopathic Neonates Treated with Hypothermia A thesis submitted to the University of Arizona College of Medicine -- Phoenix in partial fulfillment of the requirements for the degree of
Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia
 International Pediatrics Volume 2011, Article ID 848413, 5 pages doi:10.1155/2011/848413 Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia Pia Wintermark Division of Newborn
International Pediatrics Volume 2011, Article ID 848413, 5 pages doi:10.1155/2011/848413 Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia Pia Wintermark Division of Newborn
Newborn Hypoxic Ischemic Brain Injury. Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford
 Newborn Hypoxic Ischemic Brain Injury Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford NO DISCLOSURES INTRODUCTION Neonatal hypoxic-ischemic encephalopathy (HIE) is a major cause
Newborn Hypoxic Ischemic Brain Injury Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford NO DISCLOSURES INTRODUCTION Neonatal hypoxic-ischemic encephalopathy (HIE) is a major cause
TLC March 27, Shawn Hollinger-Neonatal Fellow CHEO
 TLC March 27, 2013 Presented/Prepared by: Shawn Hollinger, PGY5 Neonatal-Perinatal Medicine Resident - University of Ottawa With slides/images from Dr. Brigitte Lemyre Associate Professor of Pediatrics
TLC March 27, 2013 Presented/Prepared by: Shawn Hollinger, PGY5 Neonatal-Perinatal Medicine Resident - University of Ottawa With slides/images from Dr. Brigitte Lemyre Associate Professor of Pediatrics
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of therapeutic hypothermia with intracorporeal temperature monitoring for hypoxic
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of therapeutic hypothermia with intracorporeal temperature monitoring for hypoxic
Therapeutic hypothermia in neonatal asphyxia
 FVV IN OBGYN, 2012, 4 (2): 133-139 New perspective Therapeutic hypothermia in neonatal asphyxia L. CORNETTE Head Department Neonatology, AZ Sint Jan Brugge-Oostende AV Ruddershove 10, 8000 Brugge, Belgium.
FVV IN OBGYN, 2012, 4 (2): 133-139 New perspective Therapeutic hypothermia in neonatal asphyxia L. CORNETTE Head Department Neonatology, AZ Sint Jan Brugge-Oostende AV Ruddershove 10, 8000 Brugge, Belgium.
1/29/2014. Kimberly Johnson Hatchett, MD PGY-4 11/15/13
 Kimberly Johnson Hatchett, MD PGY-4 11/15/13 History of Present Illness 14 month old previously healthy infant boy presented via EMS after being found by his mother to be breathing loudly and non-responsive.
Kimberly Johnson Hatchett, MD PGY-4 11/15/13 History of Present Illness 14 month old previously healthy infant boy presented via EMS after being found by his mother to be breathing loudly and non-responsive.
Hypothermia: Neuroprotective Treatment of Hypoxic-Ischemic Encephalopathy. Serious perinatal asphyxia. Therapeutic hypothermia
 Therapeutic hypothermia Hypothermia: Neuroprotective Treatment of Hypoxic-Ischemic Encephalopathy Background of hypothermia Clinical application Floris Groenendaal Department of Neonatology Complications
Therapeutic hypothermia Hypothermia: Neuroprotective Treatment of Hypoxic-Ischemic Encephalopathy Background of hypothermia Clinical application Floris Groenendaal Department of Neonatology Complications
This lecture will provide an overview of the neurologic exam of a neonate in the context of clinical cases.
 A11a Neuro Nuggets from the Trenches Michael D. Weiss, MD Associate Professor Department of Pediatrics, Division of Neonatology University of Florida, Gainesville, FL The speaker has signed a disclosure
A11a Neuro Nuggets from the Trenches Michael D. Weiss, MD Associate Professor Department of Pediatrics, Division of Neonatology University of Florida, Gainesville, FL The speaker has signed a disclosure
RESEARCH BRIEF. Prognostic Value of Resistive Index in Neonates with Hypoxic Ischemic
 RESEARCH BRIEF Prognostic Value of Resistive Index in Neonates with Hypoxic Ischemic A Senthil Kumar, Aparna Chandrasekaran, Rajamannar Asokan and *Kathirvelu Gopinathan From the Department of Neonatology,
RESEARCH BRIEF Prognostic Value of Resistive Index in Neonates with Hypoxic Ischemic A Senthil Kumar, Aparna Chandrasekaran, Rajamannar Asokan and *Kathirvelu Gopinathan From the Department of Neonatology,
Effect of ALlopurinol in addition to hypothermia for hypoxic-ischemic Brain Injury on Neurocognitive Outcome. Axel Franz, Tübingen
 Effect of ALlopurinol in addition to hypothermia for hypoxic-ischemic Brain Injury on Neurocognitive Outcome Axel Franz, Tübingen Hypoxic-ischemic encephalopathy 1-2 / 1000 newborn suffer from moderate
Effect of ALlopurinol in addition to hypothermia for hypoxic-ischemic Brain Injury on Neurocognitive Outcome Axel Franz, Tübingen Hypoxic-ischemic encephalopathy 1-2 / 1000 newborn suffer from moderate
Running head: CASE STUDY NEONATAL HEAD COOLING 1
 Running head: CASE STUDY NEONATAL HEAD COOLING 1 Case Study 1: Head Cooling as Treatment for Neonatal Encephalopathy NURS 6035 Practicum I Teresa Z. Baker Texas Woman s University CASE STUDY NEONATAL HEAD
Running head: CASE STUDY NEONATAL HEAD COOLING 1 Case Study 1: Head Cooling as Treatment for Neonatal Encephalopathy NURS 6035 Practicum I Teresa Z. Baker Texas Woman s University CASE STUDY NEONATAL HEAD
Case Presentations. Anamika B. Mukherjee, MD September 13, 2017
 Case Presentations Anamika B. Mukherjee, MD September 13, 2017 Nothing to disclose Disclosures Learning Objectives Use the CPQCC Toolkit for therapeutic hypothermia to apply the guidelines for screening
Case Presentations Anamika B. Mukherjee, MD September 13, 2017 Nothing to disclose Disclosures Learning Objectives Use the CPQCC Toolkit for therapeutic hypothermia to apply the guidelines for screening
Birth Asphyxia - Summary of the previous meeting and protocol overview
 Birth Asphyxia - Summary of the previous meeting and protocol overview Dr Ornella Lincetto, WHO Geneve Milano, 11June 2007 Vilka är Personality egenskaper med den astrologiska Tvillingarna? Objective of
Birth Asphyxia - Summary of the previous meeting and protocol overview Dr Ornella Lincetto, WHO Geneve Milano, 11June 2007 Vilka är Personality egenskaper med den astrologiska Tvillingarna? Objective of
COOLING FOR NEONATAL HYPOXIC ISCHAEMIC ENCEPHALOPATHY (HIE) - GUIDELINE
 Background Objective Equipment Indications Contraindications When to initiate cooling in NPICU Procedure for therapeutic cooling NETS Transfer Issues Follow-up References Acknowledgements Related Documents
Background Objective Equipment Indications Contraindications When to initiate cooling in NPICU Procedure for therapeutic cooling NETS Transfer Issues Follow-up References Acknowledgements Related Documents
The Pharmacokinetics of Antiepileptics Drugs in Neonates with Hypoxic Ischemic Encephalopathy
 The Pharmacokinetics of Antiepileptics Drugs in Neonates with Hypoxic Ischemic Encephalopathy KELIANA O MARA, PHARMD FLORIDA NEONATAL NEUROLOGIC NETWORK STATE MEETING Objectives Describe seizures in hypoxic
The Pharmacokinetics of Antiepileptics Drugs in Neonates with Hypoxic Ischemic Encephalopathy KELIANA O MARA, PHARMD FLORIDA NEONATAL NEUROLOGIC NETWORK STATE MEETING Objectives Describe seizures in hypoxic
Perlman J, Clinics Perinatol 2006; 33: Underlying causal pathways. Antenatal Intrapartum Postpartum. Acute near total asphyxia
 Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Initiation of passive cooling at referring centre is most predictive of achieving early therapeutic hypothermia in asphyxiated newborns
 Paediatrics & Child Health, 2017, 264 268 doi: 10.1093/pch/pxx062 Original Article Advance Access publication 23 May 2017 Original Article Initiation of passive cooling at referring centre is most predictive
Paediatrics & Child Health, 2017, 264 268 doi: 10.1093/pch/pxx062 Original Article Advance Access publication 23 May 2017 Original Article Initiation of passive cooling at referring centre is most predictive
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY
 ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
Temperature Correction of Blood Gas Measurements during Therapeutic Hypothermia: Is it Time to Chill Out?
 Temperature Correction of Blood Gas Measurements during Therapeutic Hypothermia: Is it Time to Chill Out? Dr. Elizabeth Zorn Dr. Gwenyth Fischer Dr. Martha Lyon Disclosures (ML) Speaking Honoraria Radiometer
Temperature Correction of Blood Gas Measurements during Therapeutic Hypothermia: Is it Time to Chill Out? Dr. Elizabeth Zorn Dr. Gwenyth Fischer Dr. Martha Lyon Disclosures (ML) Speaking Honoraria Radiometer
Number: Policy *Please see amendment for Pennsylvania Medicaid at the end of this CPB.
 Number: 0812 Policy *Please see amendment for Pennsylvania Medicaid at the end of this CPB. Aetna considers total body cooling (TBC, also known as whole body cooling) and/or selective head cooling (SHC)
Number: 0812 Policy *Please see amendment for Pennsylvania Medicaid at the end of this CPB. Aetna considers total body cooling (TBC, also known as whole body cooling) and/or selective head cooling (SHC)
Therapeutichypothermia headcooling and its Adverse Effects in Newborns with PerinatalAsphyxia
 International Research Journal of Applied and Basic Sciences 2013 Available online at www.irjabs.com ISSN 2251-838X / Vol, 5 (12): 1546-1551 Science Explorer Publications Therapeutichypothermia headcooling
International Research Journal of Applied and Basic Sciences 2013 Available online at www.irjabs.com ISSN 2251-838X / Vol, 5 (12): 1546-1551 Science Explorer Publications Therapeutichypothermia headcooling
Neurodevelopmental Follow Up After Therapeutic Hypothermia for Perinatal Asphyxia
 ORIGINAL PAPER doi: 10.5455/medarh.2015.69.362-366 Med Arh. 2015 Dec; 69(6): 362-366 Received: August 25th 2015 Accepted: November 05th 2015 2015 Smail Zubcevic, Suada Heljic, Feriha Catibusic, Sajra Uzicanin,
ORIGINAL PAPER doi: 10.5455/medarh.2015.69.362-366 Med Arh. 2015 Dec; 69(6): 362-366 Received: August 25th 2015 Accepted: November 05th 2015 2015 Smail Zubcevic, Suada Heljic, Feriha Catibusic, Sajra Uzicanin,
Total Body Cooling & Hypoxic Ischemic Encephalopathy in the Neonate Kaleidoscope 2017
 Total Body Cooling & Hypoxic Ischemic Encephalopathy in the Neonate Kaleidoscope 2017 LEIGH ANN CATES PHD, APRN, NNP -BC, RRT-NPS, CHSE N E O N ATA L N U R S E P R A C T I T I O N E R - T E X A S C H I
Total Body Cooling & Hypoxic Ischemic Encephalopathy in the Neonate Kaleidoscope 2017 LEIGH ANN CATES PHD, APRN, NNP -BC, RRT-NPS, CHSE N E O N ATA L N U R S E P R A C T I T I O N E R - T E X A S C H I
University of Bristol - Explore Bristol Research
 Elstad, M., Liu, X., & Thoresen, M. (2016). Heart rate response to therapeutic hypothermia in infants with hypoxic-ischaemic encephalopathy. Resuscitation, 106, 53-57. DOI: 10.1016/j.resuscitation.2016.06.023
Elstad, M., Liu, X., & Thoresen, M. (2016). Heart rate response to therapeutic hypothermia in infants with hypoxic-ischaemic encephalopathy. Resuscitation, 106, 53-57. DOI: 10.1016/j.resuscitation.2016.06.023
PEER REVIEW HISTORY ARTICLE DETAILS TITLE (PROVISIONAL)
 PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
Admission/Discharge Form for Infants Born in Please DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
Too or Too Cold. Too Cold...Too Hot...Just Right. Temperature Control in Newborns. Temperature Balance in Newborns. Basics in the Delivery Room
 Too or Too Cold Neonatology Rediscovers Temperature Control Advances and Controversies in Clinical Pediatrics May 31, 2007 Terri A. Slagle Neonatology, CPMC Too Cold...Too Hot...Just Right Too Cold = Issues
Too or Too Cold Neonatology Rediscovers Temperature Control Advances and Controversies in Clinical Pediatrics May 31, 2007 Terri A. Slagle Neonatology, CPMC Too Cold...Too Hot...Just Right Too Cold = Issues
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
NEONATAL SEIZURE. IAP UG Teaching slides
 NEONATAL SEIZURE 1 INTRODUCTION One of the important neonatal neurological emergencies requiring immediate medical care. Contribute to significant morbidity and mortality Incidence is around 0.5 to 0.8%
NEONATAL SEIZURE 1 INTRODUCTION One of the important neonatal neurological emergencies requiring immediate medical care. Contribute to significant morbidity and mortality Incidence is around 0.5 to 0.8%
1
 1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
Brain injury and Resuscitation! Turning Back the Clock!
 Brain injury and Resuscitation! Turning Back the Clock! Dec 2008 Patrick J McNamara Learning Objectives Understand the benefits of Hypothermia and how it works? Identify patients who may benefit from treatment.
Brain injury and Resuscitation! Turning Back the Clock! Dec 2008 Patrick J McNamara Learning Objectives Understand the benefits of Hypothermia and how it works? Identify patients who may benefit from treatment.
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants?
 Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia
 Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Study of renal functions in neonatal asphyxia
 Original article: Study of renal functions in neonatal asphyxia *Dr. D.Y.Shrikhande, **Dr. Vivek Singh, **Dr. Amit Garg *Professor and Head, **Senior Resident Department of Pediatrics, Pravara Institute
Original article: Study of renal functions in neonatal asphyxia *Dr. D.Y.Shrikhande, **Dr. Vivek Singh, **Dr. Amit Garg *Professor and Head, **Senior Resident Department of Pediatrics, Pravara Institute
Retrospectıve analysıs for newborn ınfants wıth hypoxıc-ıschemıc encephalopathy
 Basic Research Journal of Medicine and Clinical Sciences ISSN 2315-6864 Vol. 1(2) pp. 19-24 September 2012 Available online http//www.basicresearchjournals.org Copyright 2012 Basic Research Journal Full
Basic Research Journal of Medicine and Clinical Sciences ISSN 2315-6864 Vol. 1(2) pp. 19-24 September 2012 Available online http//www.basicresearchjournals.org Copyright 2012 Basic Research Journal Full
Birth Asphyxia. Perinatal Depression. Birth Asphyxia. Risk Factors maternal. Risk Factors fetal. Risk Factors Intrapartum 2/12/2011
 Birth Asphyxia Perinatal Depression Sara Brown, ARNP Children s Hospital and Regional Medical Center May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood
Birth Asphyxia Perinatal Depression Sara Brown, ARNP Children s Hospital and Regional Medical Center May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Kimberly M. Thornton, 1,2 Hongying Dai, 3 Seth Septer, 2,4 and Joshua E. Petrikin 1,2. 1. Introduction
 International Pediatrics, Article ID 643689, 7 pages http://dx.doi.org/10.1155/2014/643689 Research Article Effects of Whole Body Therapeutic Hypothermia on Gastrointestinal Morbidity and Feeding Tolerance
International Pediatrics, Article ID 643689, 7 pages http://dx.doi.org/10.1155/2014/643689 Research Article Effects of Whole Body Therapeutic Hypothermia on Gastrointestinal Morbidity and Feeding Tolerance
Early seizures indicate quality of perinatal care
 Archives of Disease in Childhood, 1985, 6, 89-813 Early seizures indicate quality of perinatal care R J DERHAM, T G MATTHEWS, AND T A CLARKE Rotunda Hospital, Dublin, Ireland SUMMARY An analysis of antepartum,
Archives of Disease in Childhood, 1985, 6, 89-813 Early seizures indicate quality of perinatal care R J DERHAM, T G MATTHEWS, AND T A CLARKE Rotunda Hospital, Dublin, Ireland SUMMARY An analysis of antepartum,
NEONATAL SEIZURES. Introduction
 Introduction NEONATAL SEIZURES Definition: Sudden, paroxysmal depolarisation of a group of neurones with transient alteration in neurological state. Possibly abnormal motor, sensory or autonomic activity
Introduction NEONATAL SEIZURES Definition: Sudden, paroxysmal depolarisation of a group of neurones with transient alteration in neurological state. Possibly abnormal motor, sensory or autonomic activity
Neonatal Hypoxic-Ischemic Injury: Ultrasound and Dynamic Color Doppler Sonography perfusion of the Brain and Abdomen with pathologic correlation.
 Neonatal Hypoxic-Ischemic Injury: Ultrasound and Dynamic Color Doppler Sonography perfusion of the Brain and Abdomen with pathologic correlation. Ricardo Faingold,MD Montreal Children s Hospital Medical
Neonatal Hypoxic-Ischemic Injury: Ultrasound and Dynamic Color Doppler Sonography perfusion of the Brain and Abdomen with pathologic correlation. Ricardo Faingold,MD Montreal Children s Hospital Medical
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Swiss neonatal network and Follow up Group
 Swiss neonatal network and Follow up Group March 2011 Barbara Brotschi and Cornelia Hagmann Hypoxic ischaemic encephalopathy Neonatal encephalopathy due to perinatal hypoxiaischaemia: clinically defined
Swiss neonatal network and Follow up Group March 2011 Barbara Brotschi and Cornelia Hagmann Hypoxic ischaemic encephalopathy Neonatal encephalopathy due to perinatal hypoxiaischaemia: clinically defined
Is there a role for Sodium Bicarbonate in NICU? Stephen Wardle Consultant Neonatologist Nottingham University Hospitals
 Is there a role for Sodium Bicarbonate in NICU? Stephen Wardle Consultant Neonatologist Nottingham University Hospitals Aim / Objectives To persuade you:- there is no evidence in favour of using bicarbonate
Is there a role for Sodium Bicarbonate in NICU? Stephen Wardle Consultant Neonatologist Nottingham University Hospitals Aim / Objectives To persuade you:- there is no evidence in favour of using bicarbonate
Unilateral neonatal cerebral infarction in full term infants
 F88 Department of Paediatrics, John RadcliVe Hospital, Oxford, OX3 9DU J Estan P Hope Correspondence to: Dr Peter Hope. Accepted 11 December 1996 Unilateral neonatal cerebral infarction in full term infants
F88 Department of Paediatrics, John RadcliVe Hospital, Oxford, OX3 9DU J Estan P Hope Correspondence to: Dr Peter Hope. Accepted 11 December 1996 Unilateral neonatal cerebral infarction in full term infants
These signs should lead to the administration of high concentrations of
 Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
The Blue Baby. Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin
 The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
Serum Lactate, Brain Magnetic Resonance Imaging and Outcome of Neonatal Hypoxic Ischemic Encephalopathy after Therapeutic Hypothermia
 Pediatrics and Neonatology (2016) 57, 35e40 Available online at www.sciencedirect.com ScienceDirect journal homepage: http://www.pediatr-neonatol.com ORIGINAL ARTICLE Serum Lactate, Brain Magnetic Resonance
Pediatrics and Neonatology (2016) 57, 35e40 Available online at www.sciencedirect.com ScienceDirect journal homepage: http://www.pediatr-neonatol.com ORIGINAL ARTICLE Serum Lactate, Brain Magnetic Resonance
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
Post-Cardiac Arrest Syndrome. MICU Lecture Series
 Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
HIE (Hypoxic Ischaemic Encephalopathy)
 HIE (Hypoxic Ischaemic Encephalopathy) Document Title and Reference : HIE (Hypoxic Ischaemic Encephalopathy Main Auth (s) Kiran Yajamanyam Consultant LWH Ratified by: CM NSG Date Ratified: May 2017 Review
HIE (Hypoxic Ischaemic Encephalopathy) Document Title and Reference : HIE (Hypoxic Ischaemic Encephalopathy Main Auth (s) Kiran Yajamanyam Consultant LWH Ratified by: CM NSG Date Ratified: May 2017 Review
Hypoxic ischemic brain injury in neonates - early MR imaging findings
 Hypoxic ischemic brain injury in neonates - early MR imaging findings Poster No.: C-1208 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit E.-M. Heursen, R. Reina Cubero, T. Guijo Hernandez,
Hypoxic ischemic brain injury in neonates - early MR imaging findings Poster No.: C-1208 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit E.-M. Heursen, R. Reina Cubero, T. Guijo Hernandez,
Incidence and diagnosis of unilateral arterial cerebral infarction in newborn infants *
 J. Perinat. Med. 33 (2005) 170 175 Copyright by Walter de Gruyter Berlin New York. DOI 10.1515/JPM.2005.032 Short communication Incidence and diagnosis of unilateral arterial cerebral infarction in newborn
J. Perinat. Med. 33 (2005) 170 175 Copyright by Walter de Gruyter Berlin New York. DOI 10.1515/JPM.2005.032 Short communication Incidence and diagnosis of unilateral arterial cerebral infarction in newborn
SWISS SOCIETY OF NEONATOLOGY. Bart s syndrome with severe newborn encephalopathy: a delayed diagnosis
 SWISS SOCIETY OF NEONATOLOGY Bart s syndrome with severe newborn encephalopathy: a delayed diagnosis May 2003 2 Buettiker V, Hogan P, Badawi N, Department of Neonatology (BV, NB), Department of Dermatology
SWISS SOCIETY OF NEONATOLOGY Bart s syndrome with severe newborn encephalopathy: a delayed diagnosis May 2003 2 Buettiker V, Hogan P, Badawi N, Department of Neonatology (BV, NB), Department of Dermatology
Resuscitating neonatal and infant organs and preserving function. GI Tract and Kidneys
 Resuscitating neonatal and infant organs and preserving function GI Tract and Kidneys Australian and New Zealand Resuscitation Council Joint Guidelines Outline Emphasis on the infant - PICU Kidney Gastrointestinal
Resuscitating neonatal and infant organs and preserving function GI Tract and Kidneys Australian and New Zealand Resuscitation Council Joint Guidelines Outline Emphasis on the infant - PICU Kidney Gastrointestinal
Increased Serum Malondialdehyde Level in Neonates with Hypoxic Ischaemic Encephalopathy: Prediction of Disease Severity
 The Journal of International Medical Research 2010; 38: 220 226 Increased Serum Malondialdehyde Level in Neonates with Hypoxic Ischaemic Encephalopathy: Prediction of Disease Severity E KIRIMI 1, E PEKER
The Journal of International Medical Research 2010; 38: 220 226 Increased Serum Malondialdehyde Level in Neonates with Hypoxic Ischaemic Encephalopathy: Prediction of Disease Severity E KIRIMI 1, E PEKER
Hypoglycaemia of the neonate. Dr. L.G. Lloyd Dept. Paediatrics
 Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
UK TOBY Cooling Register
 UK TOBY Cooling Register Patient identification number (PIN) Patient ospital number At centre, optional Cooling treatment provided at Name of Hospital Sex M F Mont and year of treatment M M / Y Y Gestational
UK TOBY Cooling Register Patient identification number (PIN) Patient ospital number At centre, optional Cooling treatment provided at Name of Hospital Sex M F Mont and year of treatment M M / Y Y Gestational
CEREBRAL FUNCTION MONITORING
 CEREBRAL FUNCTION MONITORING Introduction and Definitions The term amplitude integrated electroencephalography (aeeg) is used to denote a method for electro-cortical monitoring whereas cerebral function
CEREBRAL FUNCTION MONITORING Introduction and Definitions The term amplitude integrated electroencephalography (aeeg) is used to denote a method for electro-cortical monitoring whereas cerebral function
Outcome of infants with hypoxic ischemic encephalopathy treated with brain hypothermia
 bs_bs_banner doi:10.1111/jog.12520 J. Obstet. Gynaecol. Res. Vol. 41, No. 2: 229 237, February 2015 Outcome of infants with hypoxic ischemic encephalopathy treated with brain hypothermia Takuya Tokuhisa
bs_bs_banner doi:10.1111/jog.12520 J. Obstet. Gynaecol. Res. Vol. 41, No. 2: 229 237, February 2015 Outcome of infants with hypoxic ischemic encephalopathy treated with brain hypothermia Takuya Tokuhisa
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA
 GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
Ipotermia terapeutica nel bambino: manca l evidenza?
 Ipotermia terapeutica nel bambino: manca l evidenza? Andrea Moscatelli UOSD Terapia Intensiva Neonatale e Pediatrica Dipartimento Integrato di Alta Intensita` di Cura e Chirurgia Istituto Giannina Gaslini
Ipotermia terapeutica nel bambino: manca l evidenza? Andrea Moscatelli UOSD Terapia Intensiva Neonatale e Pediatrica Dipartimento Integrato di Alta Intensita` di Cura e Chirurgia Istituto Giannina Gaslini
Hypoxic ischaemic encephalopathy
 Hypoxic ischaemic encephalopathy Frances Cowan Denis Azzopardi Abstract Encephalopathy occurring soon after birth continues to be a major complication in near- and full-term newborn infants. Early neonatal
Hypoxic ischaemic encephalopathy Frances Cowan Denis Azzopardi Abstract Encephalopathy occurring soon after birth continues to be a major complication in near- and full-term newborn infants. Early neonatal
National follow-up program CPUP Pediatric Neurology paper form
 National follow-up program CPUP Pediatric Neurology paper form 110206 1 National Follow-Up program- CPUP Pediatric Neurology Personal nr (unique identifier): Last name: First name: Region child belongs
National follow-up program CPUP Pediatric Neurology paper form 110206 1 National Follow-Up program- CPUP Pediatric Neurology Personal nr (unique identifier): Last name: First name: Region child belongs
Therapeutic Hypothermia: Treatment for Hypoxic-Ischemic Encephalopathy in the NICU
 Therapeutic Hypothermia: Treatment for Hypoxic-Ischemic Encephalopathy in the NICU Denise M. Casey, RN, MS, CCRN, CPNP Nancy Tella, RN, BSN, CCRN Rachel Turesky, RN, BSN Michelle Labrecque, RN, MSN, CCRN
Therapeutic Hypothermia: Treatment for Hypoxic-Ischemic Encephalopathy in the NICU Denise M. Casey, RN, MS, CCRN, CPNP Nancy Tella, RN, BSN, CCRN Rachel Turesky, RN, BSN Michelle Labrecque, RN, MSN, CCRN
