Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences Neurology
|
|
|
- Aubrey McCarthy
- 5 years ago
- Views:
Transcription
1 Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences Neurology - Hypotonia: Definition: decreased resistance of movement when muscles of the child are PSSIVELY stretched. Notice that weakness is the decreased force generated by ACTIVE contraction of the muscle. Classification: Central hypotonia: upper motor neurons are affected. Peripheral hypotonia: lower motor neurons are affected. Etiology: Central hypotonia: Congenital: Cerebral malformation, Down syndrome or Prader-Willi syndrome. Acquired: Hypoxic-ischemic encephalopathy, trauma, infection (e.g. sepsis or meningitis), intracranial hemorrhage or electrolytes abnormalities. Peripheral hypotonia: Spinal cord: spinal muscular atrophy. Peripheral nerve: familial dysautonomia. Neuromuscular junction: neonatal myasthenia or botulism. Muscle: congenital muscular dystrophy or congenital myotonic dystrophy. Clinical features: Weak cry, decreased spontaneous movements and frog-leg posture. Central hypotonia: Seizures in neonatal period, increased deep tendon reflexes and ankle clonus. Peripheral hypotonia: History of decreased fetal movements + breech presentation, decreased muscle bulk and deep tendon reflexes. Investigation: Central hypotonia: head CT (looking for lesions), serum electrolytes and FISH/karyotyping (detecting genetic disorders). Peripheral hypotonia: EMG, muscle biopsy, DNA test for spinal muscular atrophy and serum CK. Types of peripheral hypotonia: Definition: degeneration of anterior horn cells. AR disorder in which mutation is affecting chromosome 5 (SMN1 gene). 2 nd most common neuromuscular disorders after Duchenne. Classification: infantile (> 6 months); intermediate (6- Spinal muscular 12 months); juvenile (> 3 years). atrophy Clinical features: tongue fasciculations, Bell-shaped chest and frog-leg posture. Diagnosis: DNA testing. Management: supportive. Prognosis: infantile (survival beyond 1 st year unusual); intermediate (survival to adolescence); juvenile (survival to adulthood).
2 Infantile botulism Congenital myotonic dystrophy - Hydrocephalus: Definition: bulbar weakness and paralysis due to ingestion of Clostridium botilinum spores (botulinum toxin). Commonly from contaminated HONEY thus inhibiting pre-synaptic release of Ach in neuromuscular junction. Clinical features (12-48 hours after ingestion of toxin): constipation (1 st most common symptoms); loss of previously obtained motor milestones; ophthalmoplegia and hyporeflexia. Notice that paralysis is symmetrical and descending. Diagnosis: detect bacteria/toxin in stool; EMG. Management: supportive. Prognosis: Excellent (with complete recovery). Definition: AD disorder characterized by inability to relax contracted muscles. Etiology: chromosome 19 is affected; there is trinucleotide repeat commonly transmitted to affected infants through affected MOTHERS. Clinical features: neonatal feeding and respiratory problems; myotonia is not present until the AGE OF 5 YEARS; myotonic fascies; ptosis; stiff-straight smile and inability to release the grip after hand shaking. Diagnosis: DNA testing. Management: supportive. Prognosis: all survivals have mental retardation. Definition: increased CSF under pressure within ventricles of the brain which is caused by: Increased production of CSF. Blockage of CSF flow. Decreased absorption of CSF. Types: Noncommunicating aqueductal stenosis). Enlarged ventricles due to blockage of CSF flow (e.g. Enlarged ventricles due to increased production of CSF (e.g. Communicating tumors) or decreased absorption of CSF (e.g. bacterial meningitis). NOT TRUE HYDROCEPHALUS; ventricles are enlarged Ex vacuo due to brain atrophy Congenital causes: Chiari type-ii malformation: downward displacement of cerebellum and medulla through foramen magnum causing obstruction of CSF flow. Dandy-Walker malformation: combination of absent cerebellar vermis and enlarged 4 th ventricle causing obstruction of CSF flow. Congenital aquiductal stenosis: X-linked trait. Clinical features: Increased head circumference. Infants: bulging fontanelles, wide sutures and sunset sign (downward deviation of both eyes).
3 Older children: S&S of increased intracranial pressure (e.g. headache, nausea/vomiting and papilledema). Diagnosis: head CT-scan. Management: VENTRICULO-PERITONEAL SHUNT. Complications are: shunt infection or obstruction. - Spina bifida: Definitions: Spina bifida Failure of bone fusion in posterior midline of vertebral column Herniation of meninges only; NOT associated with neural Meningocele deficits Herniation of meninges and spinal cord; MORE COMMON Meningomyelocele THAN MENINGOCELE Epidemiology: HIGHEST incidence in Ireland; LOWEST in Japan. Etiology: it is associated with folic acid deficiency and exposure to teratogens (e.g. valproic acid and phenytoin). Clinical features: Spinal bifida occulta: hairy patch covering the area in lumbar region; no neurologic deficits. Meningocele: transilluminated mass filled with CSF; usually no neurologic deficits. Meningomyelocele: Neurologic defects: complete paraplegia (above L3); bladder/bowel incontinence (S3 and below). Associated complication: hydrocephalus and lower extremity fractures due to loss of sensation. Diagnosis: Pre-natal diagnosis (common): maternal serum alpha fetoprotein; ultrasound. Spina bifida occulta: presence of skin abnormality and confirmed by spinal radiographs. Meningocele & meningomyelocele: physical examination. Management: Spina bifida occulta: no intervention needed. Meningocele and myningomyelocele: surgical repair which must be done within 24 hours (in meningomyelocele) to prevent further trauma to exposed neural tissue. Prognosis: Spina bifida occulta and meningocele: EXCELLENT. Meningomyelocele: wheelchair dependency; bladder/bowel incontinence and mental retardation. - Seizure: Definitions: Seizure: it is excessive electrical discharge from a group of cerebral neurons. Epilepsy: occurrence of 2 spontaneous seizures with no precipitating factors. Status epilepticus: seizure lasting 30 minutes during which patient does not regain consciousness. Etiology (UNKNOWN in 60-70% of cases): hypoxic-ischemic encephalopathy; trauma (e.g. subdural hematoma); tumor (e.g. astrocytoma); infection (e.g. meningitis/encephalitis); hemorrhage (e.g. intracranial hemorrhage); electrolyte disturbances (e.g. hypoglycemia, hypocalcemia, hypomagensemia or hypo/hypernatremia).
4 Classification: Febrile seizure: Definition: it is a benign type of seizure which is associated with fever and there is no CNS cause. It occurs in children between 6 months 6 years of age. Classification: Simple: generalized seizure lasting < 15 minutes. Complex: focal seizure lasting > 15 minutes and recurs within 24 hours. Diagnosis: HISTORY WITH NORMAL NEUROLOGIC EXAM AND NO CNS INFECTION ARE ENOUGH FOR DIAGNOSIS. There is no need for EEG or head CT/MRI. Management: First time or occasional febrile seizure: NO NEED FOR ANTICONVULSANTS, but treat subsequent febrile illness aggressively with anti-pyretics to prevent the occurrence of another febrile seizure. Frequent, recurrent febrile seizure: abortive treatment with rectal diazepam and daily anticonvulsant prophylaxis. Prognosis: 30% of patients with ONE febrile seizure will have recurrence. Risk of epilepsy is low (2%). Afebrile seizure: Partial (affecting ONE hemisphere): Simple: consciousness NOT impaired. Complex: consciousness IMPAIRED. Generalized (affecting BOTH hemispheres): Tonic-clonic (most common): body becomes stiff followed by jerky movements, upward rolling of the eyes, incontinence, tongue biting, decreased consciousness and postictal state. Absence (5-9 years): autosomal dominant (AD) characterized by staring with minor motor manifestations (e.g. eye blinking or mouthing movements) lasting < 15 seconds with no postictal state. EEG is characterized by 3-Hz spike and wave discharge. Prognosis is VERY GOOD. Diagnosis: History, physical examination, serum electrolytes, head CT-MRI and EEG (NOTICE THAT A NORMAL EEG DOES NOT EXCLUDE THE DIAGNOSIS OF SEIZURE/EPILEPSY). Management: Treatment of status epilepticus: starts with a benzodiazepine (e.g. lorazepam/diazepam) no response loading dose of Phenobarbital or phenytoin no response anesthesia (with propofol). Treatment of epilepsy: Pharmacotherapy: Partial epilepsy: carbamazepine. Generalized epilepsy: valproic acid. Absence epilepsy: ethosuximide. Surgery: in which there will be removal of epileptic tissue; best results for those with TEMPORAL LOBE LESIONS. Prognosis: EPILEPSY IS NOT A LIFE-LONG DISORDER. 70% of epileptic children can stop medications after 2 years seizure-free period with normalization of their EEG.
5 Infantile spasm (West syndrome): Etiology: it occurs in infants between 3-8 months of age mostly due to TUBEROUS SCLEROSIS. Other causes include: hypoxic ischemic injury, intraventricular hemorrhage or infection (e.g. meningitis/encephalitis). Clinical features: brief myoclonic jerks lasting 1-2 seconds each, occurring in clusters of 5-10 seizures spread over 3-5 minutes. Diagnosis: EEG shows HYPSARRHYTHMIA PATTERN. Management: ACTH IM injection for 4-6 weeks. Notice that VIGABATRIN is the most effective drig for patients with infantile spasms caused by tuberous sclerosis. Valproic acid is the 2 nd line drug of choice. Prognosis: POOR (children often develop moderate-severe mental retardation). Benign rolandic epilepsy: Definition: it is an autosomal dominant (AD) nocturnal partial seizure with secondary generalization. Epidemiology: it is considered as the most common partial seizure in childhood occurring between 3-13 years of age and found more among boys. Clinical features: oral-buccal manifestations (e.g. pooling of saliva) in early morning hours which then generalize to tonic-clonic seizures. Diagnosis: EEG shows spike and sharp waves disturbance in mid-temporal and central regions. Management: valproic acid. Prognosis: EXCELLENT. - Unsteady gait: Definition: ataxia is the inability to coordinate muscle activity during voluntary movements due to: cerebellar or proprioceptive dysfunction. What are your differential diagnoses for ataxia? Cerebellar ataxia: which is characterized by unsteady, wide-base gait with irregular steps and deviation to one side or the other. Vertigo. Vision problems. Head trauma, drug overdose or infection. During seizure and postictal state. Weakness (e.g. Guillain-Barre syndrome). Acute cerebellar ataxia of childhood: It is the most common cause of ataxia in children between 18 months 7 years that is caused by: Immune complex deposition in the cerebellum. Preceding infections: EBV, influenza, varicella or mycoplasma. Clinical features: Truncal ataxia with deterioration of gait. Slurred speech and nystagmus are often present. FEVER IS ABSENT. Diagnosis: History & physical examination + head CT-scan (which will be NORMAL!). Management: SUPPORITVE (symptoms will resolve within 2-3 months). Guillain-Barre syndrome: Definition: it is a demyelinating polyneuritis characterized by: ASCENDING weakness, AREFLEXIA, but INTACT sensation. It is commonly associated with Campylobacter jejuni infection. There will be cellmediated immune response to the infectious agent that cross-react with Schwann cell membrane of peripheral nerves.
6 Clinical features: Ascending, symmetric paralysis and areflexia which might progress to respiratory arrest (if involving the diaphragm). NO SENSORY LOSS. Cranial nerve involvement: facial weakness in 50% of patients. Diagnosis: Lumbar puncture: there is increased CSF protein. EMG: shows decreased nerve conduction velocity of conduction block. Management: IVIG (preferred treatment in children) or plasmapheresis for 4 days. There is complete recovery from the disease in children. - Duchenne and Becker muscular dystrophies (DMD, BMD): Definition: they are progressive, X-linked myopathies characterized by myofiber degeneration. NOTICE THAT DMD IS MORE SEVERE THAN BMD. The onset of symptoms is between 2-5 years of age. Pathophysiology: the absence of dystrophin gene leads to rupture of plasma membrane and subsequent degeneration of muscle fibers. Under light microscopy, there will be infiltration by lymphocytes and replacement of damaged muscle fibers with fibroblasts and lipid deposits. Clinical features: Children with DMD lose the ability to walk by 10 years of age while children with BMD lose the ability to walk by 20 years of age. Slow, progressive muscle weakness affecting LEGS FIRST (+ Gower s sign). Pseudohypertrophy of calves (due to deposition of lipids; MORE IN DMD). Cardiac involvement in 50% of patients. DMD mild cognitive impairment; NO cognitive impairment in BMD. Diagnosis: CLINICAL PICTURE IS SUGGESTIVE (a young boy with enlarged calves and muscle weakness). EMG. Muscle biopsy. DNA testing (showing the gene deletion). CK levels are VERY HIGH. Management and prognosis: THERE IS NO CURE. Patients with DMD will die in their late teens due to respiratory failure. Patients with BMD have a life expectancy until 50 s. - Myesthenia gravis: Definition: it is an autoimmune disorder in which there are antibodies directed against acetyl choline receptor at the neuromuscular junction and is found more among girls. Classification: Neonatal: in which there is transient weakness due to transplacental transfer of antibodies from a mother with myasthenia gravis. Juvenile: there is formation of AChR antibodies. Clinical features: BILATERAL PTOSIS IS THE MOST COMMON PRESENTING SIGN; Progressive muscle weakness especially late in the day with repetitive muscle activity; Diplopia (due to decreased movement of extraocular muscles). Diagnosis: Detection of AChR antibodies. EMG: shows decreased muscle contraction with repetitive nerve stimulation. Tensilon test: in which edrophonium chloride (cholinesterase inhibitor) is injected and producing transient improvement in ptosis. Management: cholinesterase inhibitor is the mainstay of therapy (pyridostigmine) if fails corticosteroids/plasmapheresis/ivig. Notice that thymectomy is often performed.
Neonatal Hypotonia. Encephalopathy acute No encephalopathy. Neurology Chapter of IAP
 The floppy infant assumes a frog legged position. On ventral suspension, the baby can not maintain limb posture against gravity and assumes the position of a rag doll. Encephalopathy acute No encephalopathy
The floppy infant assumes a frog legged position. On ventral suspension, the baby can not maintain limb posture against gravity and assumes the position of a rag doll. Encephalopathy acute No encephalopathy
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012
 Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
Neurology Clerkship Learning Objectives
 Neurology Clerkship Learning Objectives Clinical skills Perform a neurological screening examination of the cranial nerves, motor system, reflexes, and sensory system under the observation and guidance
Neurology Clerkship Learning Objectives Clinical skills Perform a neurological screening examination of the cranial nerves, motor system, reflexes, and sensory system under the observation and guidance
Pediatrics. Convulsive Disorders in Childhood
 Pediatrics Convulsive Disorders in Childhood Definition Convulsion o A sudden, violent, irregular movement of a limb or of the body o Caused by involuntary contraction of muscles and associated especially
Pediatrics Convulsive Disorders in Childhood Definition Convulsion o A sudden, violent, irregular movement of a limb or of the body o Caused by involuntary contraction of muscles and associated especially
Dr. Dafalla Ahmed Babiker Jazan University
 Dr. Dafalla Ahmed Babiker Jazan University change in motor activity and/or behaviour due to abnormal electrical activity in the brain. seizures in children either - provoked by somatic disorders originating
Dr. Dafalla Ahmed Babiker Jazan University change in motor activity and/or behaviour due to abnormal electrical activity in the brain. seizures in children either - provoked by somatic disorders originating
Movement Disorders. Psychology 372 Physiological Psychology. Background. Myasthenia Gravis. Many Types
 Background Movement Disorders Psychology 372 Physiological Psychology Steven E. Meier, Ph.D. Listen to the audio lecture while viewing these slides Early Studies Found some patients with progressive weakness
Background Movement Disorders Psychology 372 Physiological Psychology Steven E. Meier, Ph.D. Listen to the audio lecture while viewing these slides Early Studies Found some patients with progressive weakness
DISORDERS OF THE NERVOUS SYSTEM
 DISORDERS OF THE NERVOUS SYSTEM Bell Work What s your reaction time? Go to this website and check it out: https://www.justpark.com/creative/reaction-timetest/ Read the following brief article and summarize
DISORDERS OF THE NERVOUS SYSTEM Bell Work What s your reaction time? Go to this website and check it out: https://www.justpark.com/creative/reaction-timetest/ Read the following brief article and summarize
There are several types of epilepsy. Each of them have different causes, symptoms and treatment.
 1 EPILEPSY Epilepsy is a group of neurological diseases where the nerve cell activity in the brain is disrupted, causing seizures of unusual sensations, behavior and sometimes loss of consciousness. Epileptic
1 EPILEPSY Epilepsy is a group of neurological diseases where the nerve cell activity in the brain is disrupted, causing seizures of unusual sensations, behavior and sometimes loss of consciousness. Epileptic
Evaluation of the Hypotonic Infant and Child
 Evaluation of the Hypotonic Infant and Child Basil T. Darras, M.D. Neuromuscular Program Boston Children s Hospital Harvard Medical School Boston, MA, USA Classification and General Clinical Evaluation
Evaluation of the Hypotonic Infant and Child Basil T. Darras, M.D. Neuromuscular Program Boston Children s Hospital Harvard Medical School Boston, MA, USA Classification and General Clinical Evaluation
The Fitting Child. A/Prof Alex Tang
 The Fitting Child A/Prof Alex Tang Objective Define relevant history taking and physical examination Classify the types of epilepsy in children Demonstrate the usefulness of investigations Define treatment
The Fitting Child A/Prof Alex Tang Objective Define relevant history taking and physical examination Classify the types of epilepsy in children Demonstrate the usefulness of investigations Define treatment
Neuromuscular Disease(2) Epilepsy. Department of Pediatrics Soochow University Affiliated Children s Hospital
 Neuromuscular Disease(2) Epilepsy Department of Pediatrics Soochow University Affiliated Children s Hospital Seizures (p130) Main contents: 1) Emphasize the clinical features of epileptic seizure and epilepsy.
Neuromuscular Disease(2) Epilepsy Department of Pediatrics Soochow University Affiliated Children s Hospital Seizures (p130) Main contents: 1) Emphasize the clinical features of epileptic seizure and epilepsy.
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Neurology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
NEONATAL SEIZURES-PGPYREXIA REVIEW
 NEONATAL SEIZURES-PGPYREXIA REVIEW This is a very important Postgraduate topics will few Q asked in undergraduation also. Lets see them in detail. References: 1.Volpe s Neurology of newborn 2.Nelson s
NEONATAL SEIZURES-PGPYREXIA REVIEW This is a very important Postgraduate topics will few Q asked in undergraduation also. Lets see them in detail. References: 1.Volpe s Neurology of newborn 2.Nelson s
Provide specific counseling to parents and patients with neurological disorders, addressing:
 Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Child Neurology Elective PL1 Rotation
 PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
Approach to a Neurologic Diagnosis
 Approach to a Neurologic Diagnosis Neurologic Diagnosis History Physical & Neurological Examination Ancillary Procedures 3 Questions Asked Focal neurologic deficits Increased intracranial pressure Signs
Approach to a Neurologic Diagnosis Neurologic Diagnosis History Physical & Neurological Examination Ancillary Procedures 3 Questions Asked Focal neurologic deficits Increased intracranial pressure Signs
Disclosure. Outline. Pediatric Epilepsy And Conditions That Mimic Seizures 9/20/2016. Bassem El-Nabbout, MD
 Pediatric Epilepsy And Conditions That Mimic Seizures Bassem El-Nabbout, MD Assistant Professor, Pediatric Neurology Board Certified in Neurology, and Headache Medicine. Disclosure I have no actual or
Pediatric Epilepsy And Conditions That Mimic Seizures Bassem El-Nabbout, MD Assistant Professor, Pediatric Neurology Board Certified in Neurology, and Headache Medicine. Disclosure I have no actual or
Neonatal Seizure. Dr.Nawar Yahya. Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan. Supervised by:
 Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Problems of Neurological Function. Unit 10
 Problems of Neurological Function Unit 10 Independent Student Review Brain Anatomy and physiology of cerebral hemispheres, diencephalon, brain stem, and cerebellum Meninges, ventricles, flow of CSF Blood
Problems of Neurological Function Unit 10 Independent Student Review Brain Anatomy and physiology of cerebral hemispheres, diencephalon, brain stem, and cerebellum Meninges, ventricles, flow of CSF Blood
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Absence seizures, 6 in childhood, 95 Adults, seizures and status epilepticus in, management of, 34 35 with first-time seizures. See Seizure(s),
Index Note: Page numbers of article titles are in boldface type. A Absence seizures, 6 in childhood, 95 Adults, seizures and status epilepticus in, management of, 34 35 with first-time seizures. See Seizure(s),
Anticonvulsants Antiseizure
 Anticonvulsants Antiseizure Seizure disorders Head trauma Stroke Drugs (overdose, withdrawal) Brain tumor Encephalitis/ Meningitis High fever Hypoglycemia Hypocalcemia Hypoxia genetic factors Epileptic
Anticonvulsants Antiseizure Seizure disorders Head trauma Stroke Drugs (overdose, withdrawal) Brain tumor Encephalitis/ Meningitis High fever Hypoglycemia Hypocalcemia Hypoxia genetic factors Epileptic
Classification of Seizures. Generalized Epilepsies. Classification of Seizures. Classification of Seizures. Bassel F. Shneker
 Classification of Seizures Generalized Epilepsies Bassel F. Shneker Traditionally divided into grand mal and petit mal seizures ILAE classification of epileptic seizures in 1981 based on clinical observation
Classification of Seizures Generalized Epilepsies Bassel F. Shneker Traditionally divided into grand mal and petit mal seizures ILAE classification of epileptic seizures in 1981 based on clinical observation
High Yield Neurological Examination
 High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
Disorders of the Nervous System. Disorders of the Neurological System. General Endpoints of CNS Disease. General Endpoints of CNS Disease
 HD in Nursing-Pathophysiology Disorders of the Nervous System What are some disorders of the nervous system? Disorders of the Neurological System Dr. C.H. Lai The nervous system is vulnerable to various
HD in Nursing-Pathophysiology Disorders of the Nervous System What are some disorders of the nervous system? Disorders of the Neurological System Dr. C.H. Lai The nervous system is vulnerable to various
1/31/2009. Paroxysmal, uncontrolled electrical discharge of neurons in brain interrupting normal function
 Paroxysmal, uncontrolled electrical discharge of neurons in brain interrupting normal function In epilepsy abnormal neurons undergo spontaneous firing Cause of abnormal firing is unclear Firing spreads
Paroxysmal, uncontrolled electrical discharge of neurons in brain interrupting normal function In epilepsy abnormal neurons undergo spontaneous firing Cause of abnormal firing is unclear Firing spreads
Vascular Disorders. Nervous System Disorders (Part B-1) Module 8 -Chapter 14. Cerebrovascular disease S/S 1/9/2013
 Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level
 Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level Prerequisites: Any prior pediatric rotations and experience Primary Goals for this
Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level Prerequisites: Any prior pediatric rotations and experience Primary Goals for this
Neurologic Examination
 John W. Engstrom, MD October 16, 2015 Neurologic Examination Overview The Neurologic Examination Neurologic Examination John W. Engstrom, M.D. Dept. of Neurology University of California, San Francisco
John W. Engstrom, MD October 16, 2015 Neurologic Examination Overview The Neurologic Examination Neurologic Examination John W. Engstrom, M.D. Dept. of Neurology University of California, San Francisco
Fetal Medicine. Case Presentations. Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital. October 2003
 Case Presentations Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital October 2003 Case 1 Ms A M 22year old P0 G1 Referred from Sebokeng Hospital at 36w for polyhydramnios On Ultrasound:
Case Presentations Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital October 2003 Case 1 Ms A M 22year old P0 G1 Referred from Sebokeng Hospital at 36w for polyhydramnios On Ultrasound:
Neuromuscular in the Pediatric Clinic: Recognition and Referral
 Neuromuscular in the Pediatric Clinic: Recognition and Referral Matthew Harmelink, MD Assistant Professor, Pediatric Neurology Medical College of Wisconsin Objectives: 1. Understand common presentations
Neuromuscular in the Pediatric Clinic: Recognition and Referral Matthew Harmelink, MD Assistant Professor, Pediatric Neurology Medical College of Wisconsin Objectives: 1. Understand common presentations
Central nervous system
 Central nervous system By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 7 th Lecture Lecture outline Review of structure & function. Symptoms, signs & tests. Specific diseases. Review of structure
Central nervous system By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 7 th Lecture Lecture outline Review of structure & function. Symptoms, signs & tests. Specific diseases. Review of structure
A Hypothesis Driven Approach to the Neurological Exam
 A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
PRIMARY DISEASES OF MYELIN. By: Shifaa Al Qa qa
 PRIMARY DISEASES OF MYELIN By: Shifaa Al Qa qa Most diseases of myelin are primarily white matter disorders??? Myelinated axons most diseases of CNS myelin do not involve the peripheral nerves to any significant
PRIMARY DISEASES OF MYELIN By: Shifaa Al Qa qa Most diseases of myelin are primarily white matter disorders??? Myelinated axons most diseases of CNS myelin do not involve the peripheral nerves to any significant
Neuro. Development. Judy Philbrook, NNP-BC. ! Primary neurulation! Prosencepahlic! Neuronal proliferation. ! 3-4 weeks! 2-3 months!
 Neuro Judy Philbrook, NNP-BC Microsoft clip art Development! Primary neurulation! Prosencepahlic! Neuronal proliferation! Neuronal migration! Organization! Myelination! 3-4 weeks! 2-3 months! 3-4 months!
Neuro Judy Philbrook, NNP-BC Microsoft clip art Development! Primary neurulation! Prosencepahlic! Neuronal proliferation! Neuronal migration! Organization! Myelination! 3-4 weeks! 2-3 months! 3-4 months!
*Pathophysiology of. Epilepsy
 *Pathophysiology of Epilepsy *Objectives * At the end of this lecture the students should be able to:- 1.Define Epilepsy 2.Etio-pathology of Epilepsy 3.Types of Epilepsy 4.Role of Genetic in Epilepsy 5.Clinical
*Pathophysiology of Epilepsy *Objectives * At the end of this lecture the students should be able to:- 1.Define Epilepsy 2.Etio-pathology of Epilepsy 3.Types of Epilepsy 4.Role of Genetic in Epilepsy 5.Clinical
The Floppy Baby. Clare Betteridge
 The Floppy Baby Clare Betteridge The floppy baby Identification Evaluation Investigation Diagnosis Examples What is a floppy baby? Elbows and knees loosely extended. Head control is usually poor or absent.
The Floppy Baby Clare Betteridge The floppy baby Identification Evaluation Investigation Diagnosis Examples What is a floppy baby? Elbows and knees loosely extended. Head control is usually poor or absent.
EEG in Epileptic Syndrome
 EEG in Epileptic Syndrome Surachai Likasitwattanakul, M.D. Division of Neurology, Department of Pediatrics Faculty of Medicine, Siriraj Hospital Mahidol University Epileptic syndrome Electroclinical syndrome
EEG in Epileptic Syndrome Surachai Likasitwattanakul, M.D. Division of Neurology, Department of Pediatrics Faculty of Medicine, Siriraj Hospital Mahidol University Epileptic syndrome Electroclinical syndrome
Muscular System. Disorders & Conditions
 Muscular System Disorders & Conditions Fibromyalgia Fibromyalgia is a disorder characterized by widespread musculoskeletal pain accompanied by fatigue, sleep, memory and mood issues. Often is described
Muscular System Disorders & Conditions Fibromyalgia Fibromyalgia is a disorder characterized by widespread musculoskeletal pain accompanied by fatigue, sleep, memory and mood issues. Often is described
Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of
 Peripheral Nervous System Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of non-insulin dependent diabetes
Peripheral Nervous System Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of non-insulin dependent diabetes
Epilepsy 101. Russell P. Saneto, DO, PhD. Seattle Children s Hospital/University of Washington November 2011
 Epilepsy 101 Russell P. Saneto, DO, PhD Seattle Children s Hospital/University of Washington November 2011 Specific Aims How do we define epilepsy? Do seizures equal epilepsy? What are seizures? Seizure
Epilepsy 101 Russell P. Saneto, DO, PhD Seattle Children s Hospital/University of Washington November 2011 Specific Aims How do we define epilepsy? Do seizures equal epilepsy? What are seizures? Seizure
Status Epilepticus in Children
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
NEONATAL MUSCULAR HYPOTONIA
 NEONATAL MUSCULAR HYPOTONIA Differential Diagnosis Systemic causes of neonatal hypotonia should be identified rapidly as they are usually transient if treated appropriately. Major differential diagnoses
NEONATAL MUSCULAR HYPOTONIA Differential Diagnosis Systemic causes of neonatal hypotonia should be identified rapidly as they are usually transient if treated appropriately. Major differential diagnoses
LOCALIZATION NEUROLOGY EPISODE VI HEARING LOSS AND GAIT ATAXIA
 LOCALIZATION NEUROLOGY EPISODE VI HEARING LOSS AND GAIT ATAXIA EPISODE VI HEARING LOSS APPROACH and DIAGNOSIS 2 Cochlea and Auditory nerve Pons (superior olive) lateral lemniscus Inferior colliculus Thalamus
LOCALIZATION NEUROLOGY EPISODE VI HEARING LOSS AND GAIT ATAXIA EPISODE VI HEARING LOSS APPROACH and DIAGNOSIS 2 Cochlea and Auditory nerve Pons (superior olive) lateral lemniscus Inferior colliculus Thalamus
Epilepsy and Epileptic Seizures
 Epilepsy and Epileptic Seizures Petr Marusič Dpt. of Neurology Charles University, Second Faculty of Medicine Motol University Hospital Diagnosis Steps Differentiation of nonepileptic events Seizure classification
Epilepsy and Epileptic Seizures Petr Marusič Dpt. of Neurology Charles University, Second Faculty of Medicine Motol University Hospital Diagnosis Steps Differentiation of nonepileptic events Seizure classification
The Neurologic Examination. John W. Engstrom, M.D. University of California San Francisco School of Medicine
 The Neurologic Examination John W. Engstrom, M.D. University of California San Francisco School of Medicine Overview The Neurologic Examination Mental status demonstration/questions Cranial nerves demonstration/questions
The Neurologic Examination John W. Engstrom, M.D. University of California San Francisco School of Medicine Overview The Neurologic Examination Mental status demonstration/questions Cranial nerves demonstration/questions
5.1 Alex.
 5.1 Alex http://tinyurl.com/neuromakessense Alex is a 20-year-old full-time national serviceman. His only past medical history is asthma, presents to A&E with a 4-day history of bilateral finger weakness
5.1 Alex http://tinyurl.com/neuromakessense Alex is a 20-year-old full-time national serviceman. His only past medical history is asthma, presents to A&E with a 4-day history of bilateral finger weakness
Problems of Neurological Function
 Problems of Neurological Function Unit 10 Independent Student Review Brain Anatomy and physiology of cerebral hemispheres, diencephalon, brain stem, and cerebellum Meninges, ventricles, flow of CSF Blood
Problems of Neurological Function Unit 10 Independent Student Review Brain Anatomy and physiology of cerebral hemispheres, diencephalon, brain stem, and cerebellum Meninges, ventricles, flow of CSF Blood
David Dredge, MD MGH Child Neurology CME Course September 9, 2017
 David Dredge, MD MGH Child Neurology CME Course September 9, 2017 } 25-40,000 children experience their first nonfebrile seizure each year } AAN/CNS guidelines developed in early 2000s and subsequently
David Dredge, MD MGH Child Neurology CME Course September 9, 2017 } 25-40,000 children experience their first nonfebrile seizure each year } AAN/CNS guidelines developed in early 2000s and subsequently
Spinal Cord: Clinical Applications. Dr. Stuart Inglis
 Spinal Cord: Clinical Applications Dr. Stuart Inglis Tabes dorsalis, also known as syphilitic myelopathy, is a slow degeneration (specifically, demyelination) of the nerves in the dorsal funiculus of the
Spinal Cord: Clinical Applications Dr. Stuart Inglis Tabes dorsalis, also known as syphilitic myelopathy, is a slow degeneration (specifically, demyelination) of the nerves in the dorsal funiculus of the
Periodic and Rhythmic Patterns. Suzette M LaRoche, MD Mission Health Epilepsy Center Asheville, North Carolina
 Periodic and Rhythmic Patterns Suzette M LaRoche, MD Mission Health Epilepsy Center Asheville, North Carolina Continuum of EEG Activity Neuronal Injury LRDA GPDs SIRPIDs LPDs + NCS Burst-Suppression LPDs
Periodic and Rhythmic Patterns Suzette M LaRoche, MD Mission Health Epilepsy Center Asheville, North Carolina Continuum of EEG Activity Neuronal Injury LRDA GPDs SIRPIDs LPDs + NCS Burst-Suppression LPDs
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases
 Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM. Andrzej Sladkowski
 Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Unit VIII Problem 7 Pharmacology: Principles of Management of Seizure Disorders
 Unit VIII Problem 7 Pharmacology: Principles of Management of Seizure Disorders - Terminologies: Anti-convulsants: they are used to control convulsions seen in certain types of epilepsy. Convulsions may
Unit VIII Problem 7 Pharmacology: Principles of Management of Seizure Disorders - Terminologies: Anti-convulsants: they are used to control convulsions seen in certain types of epilepsy. Convulsions may
Neuromuscular Disease of Infants and Children. A Guide to Diagnosis of Genetic and Acquired Conditions
 Neuromuscular Disease of Infants and Children A Guide to Diagnosis of Genetic and Acquired Conditions Genetic Effects and Infant/Neonatal Neuromuscular Conditions Who did I get this from? Onset, progression,
Neuromuscular Disease of Infants and Children A Guide to Diagnosis of Genetic and Acquired Conditions Genetic Effects and Infant/Neonatal Neuromuscular Conditions Who did I get this from? Onset, progression,
Common Neurological Problems
 Common Neurological Problems Chapter 31 Common Neurological Problems Pediatric Neurological Examination Mental status Is the child alert? Is the child appropriately oriented (based on age)? Is the child
Common Neurological Problems Chapter 31 Common Neurological Problems Pediatric Neurological Examination Mental status Is the child alert? Is the child appropriately oriented (based on age)? Is the child
Febrile seizures. Olivier Dulac. Hôpital Necker-Enfants Malades, Université Paris V, INSERM U663
 Febrile seizures Olivier Dulac Hôpital Necker-Enfants Malades, Université Paris V, INSERM U663 olivier.dulac@nck.aphp.fr Definition Seizures precipitated by fever that is not due to an intracranial infection
Febrile seizures Olivier Dulac Hôpital Necker-Enfants Malades, Université Paris V, INSERM U663 olivier.dulac@nck.aphp.fr Definition Seizures precipitated by fever that is not due to an intracranial infection
Case #1. Inter-ictal EEG. Difficult Diagnosis Pediatrics. 15 mos girl with medically refractory infantile spasms 2/13/2010
 Difficult Diagnosis Pediatrics Joseph E. Sullivan M.D. Assistant Professor of Clinical Neurology & Pediatrics Director, UCSF Pediatric Epilepsy Center University of California San Francisco Case #1 15
Difficult Diagnosis Pediatrics Joseph E. Sullivan M.D. Assistant Professor of Clinical Neurology & Pediatrics Director, UCSF Pediatric Epilepsy Center University of California San Francisco Case #1 15
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Chapter 15 Neurological Emergencies Stroke (1 of 2) Stroke (2 of 2) Seizures Altered Mental Status (AMS)
 1 2 3 4 5 Chapter 15 Neurological Emergencies Stroke (1 of 2) Stroke is the leading cause of death in the United States. After heart disease and cancer It is common in geriatric patients. More than women
1 2 3 4 5 Chapter 15 Neurological Emergencies Stroke (1 of 2) Stroke is the leading cause of death in the United States. After heart disease and cancer It is common in geriatric patients. More than women
Diagnosing Epilepsy in Children and Adolescents
 2019 Annual Epilepsy Pediatric Patient Care Conference Diagnosing Epilepsy in Children and Adolescents Korwyn Williams, MD, PhD Staff Epileptologist, BNI at PCH Clinical Assistant Professor, Department
2019 Annual Epilepsy Pediatric Patient Care Conference Diagnosing Epilepsy in Children and Adolescents Korwyn Williams, MD, PhD Staff Epileptologist, BNI at PCH Clinical Assistant Professor, Department
EGI Clinical Data Collection Form Cover Page
 EGI Clinical Data Collection Form Cover Page Please find enclosed the EGI Clinical Data Form for my patient. This form was completed by: On (date): _ Page 1 of 14 EGI Clinical Data Form Patient Name: Date
EGI Clinical Data Collection Form Cover Page Please find enclosed the EGI Clinical Data Form for my patient. This form was completed by: On (date): _ Page 1 of 14 EGI Clinical Data Form Patient Name: Date
PEDIATRIC BRAIN CARE
 PEDIATRIC BRAIN CARE The brain matters most! OVERVIEW OF NEURO ASSESSMENT 1. Overall responsiveness/activity 2. The eyes 3.? Increased ICP 4. Movements 5.? Seizures 6. Other OVERALL RESPONSIVENESS/ ACTIVITY
PEDIATRIC BRAIN CARE The brain matters most! OVERVIEW OF NEURO ASSESSMENT 1. Overall responsiveness/activity 2. The eyes 3.? Increased ICP 4. Movements 5.? Seizures 6. Other OVERALL RESPONSIVENESS/ ACTIVITY
Stroke - Intracranial hemorrhage. Dr. Amitesh Aggarwal Associate Professor Department of Medicine
 Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
The Child with Alterations in Cerebral Function
 The Child with Alterations in Cerebral Function Neurologic Assessment VS HR, BP, Respirations, Temperature LOC Orientation Pediatric Glasgow Coma Scale Eyes Pupillary response and movement, extraoccular
The Child with Alterations in Cerebral Function Neurologic Assessment VS HR, BP, Respirations, Temperature LOC Orientation Pediatric Glasgow Coma Scale Eyes Pupillary response and movement, extraoccular
Chiari Malformations. Google. Objectives Seventh Annual NKY TBI Conference 3/22/13. Kerry R. Crone, M.D.
 Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chapter 15 Neurological Emergencies Stroke (1 of 2) Stroke (2 of 2) Seizures Altered Mental Status (AMS) Brain Structure and Function
 1 Chapter 15 Neurological Emergencies 2 Stroke (1 of 2) Stroke is the leading cause of death in the United States. After heart disease and cancer It is common in geriatric patients. More than women have
1 Chapter 15 Neurological Emergencies 2 Stroke (1 of 2) Stroke is the leading cause of death in the United States. After heart disease and cancer It is common in geriatric patients. More than women have
Clinical Summaries. CLN1 Disease, infantile onset and others
 Clinical Summaries CLN1 Disease, infantile onset and others The gene called CLN1 lies on chromosome 1. CLN1 disease is inherited as an autosomal recessive disorder, which means that both chromosomes carry
Clinical Summaries CLN1 Disease, infantile onset and others The gene called CLN1 lies on chromosome 1. CLN1 disease is inherited as an autosomal recessive disorder, which means that both chromosomes carry
Introduction. 1 person in 20 will have an epileptic seizure at some time in their life
 Introduction 1 person in 20 will have an epileptic seizure at some time in their life Epilepsy is diagnosed on the basis of two or more epileptic seizures. Around 450,000 people in the UK have epilepsy
Introduction 1 person in 20 will have an epileptic seizure at some time in their life Epilepsy is diagnosed on the basis of two or more epileptic seizures. Around 450,000 people in the UK have epilepsy
Neurodevelopment. Checkpoints in children with congenital heart disease
 Neurodevelopment Checkpoints in children with congenital heart disease Jeehun Lee, M.D., PhD. Pediatric Neurology Samsung Medical Center Sungkyunkwan University, School of Medicine Heart and Brain : Why
Neurodevelopment Checkpoints in children with congenital heart disease Jeehun Lee, M.D., PhD. Pediatric Neurology Samsung Medical Center Sungkyunkwan University, School of Medicine Heart and Brain : Why
The Cerebellum. Physiology #13 #CNS1
 Physiology #13 #CNS1 The cerebellum consists of cortex and deep nuclei, it is hugely condensed with gray mater (condensed with neurons (1/3 of the neurons of the brain)). Cerebellum contains 30 million
Physiology #13 #CNS1 The cerebellum consists of cortex and deep nuclei, it is hugely condensed with gray mater (condensed with neurons (1/3 of the neurons of the brain)). Cerebellum contains 30 million
Advanced Concept of Nursing- II
 In The Name of God (A PROJECT OF NEW LIFE HEALTH CARE SOCIETY, KARACHI) Advanced Concept of Nursing- II UNIT- VIII Advance Nursing Management Of neurovascular Diseases. Shahzad Bashir RN, BScN, DCHN,MScN
In The Name of God (A PROJECT OF NEW LIFE HEALTH CARE SOCIETY, KARACHI) Advanced Concept of Nursing- II UNIT- VIII Advance Nursing Management Of neurovascular Diseases. Shahzad Bashir RN, BScN, DCHN,MScN
42 y/o woman with unwitnessed episode of loss of consciousness and urinary incontinence
 Top Five Neurological Emergencies: When To Refer February 23, 2011 Jinny Tavee, MD Associate Professor Neurological Institute Cleveland Clinic Foundation 1 CASE 1 42 y/o woman with unwitnessed episode
Top Five Neurological Emergencies: When To Refer February 23, 2011 Jinny Tavee, MD Associate Professor Neurological Institute Cleveland Clinic Foundation 1 CASE 1 42 y/o woman with unwitnessed episode
NEONATAL SEIZURE. IAP UG Teaching slides
 NEONATAL SEIZURE 1 INTRODUCTION One of the important neonatal neurological emergencies requiring immediate medical care. Contribute to significant morbidity and mortality Incidence is around 0.5 to 0.8%
NEONATAL SEIZURE 1 INTRODUCTION One of the important neonatal neurological emergencies requiring immediate medical care. Contribute to significant morbidity and mortality Incidence is around 0.5 to 0.8%
Dravet syndrome : Clinical presentation, genetic investigation and anti-seizure medication. Bradley Osterman MD, FRCPC, CSCN
 Dravet syndrome : Clinical presentation, genetic investigation and anti-seizure medication Bradley Osterman MD, FRCPC, CSCN Objectives Learn about the typical early clinical presentation of Dravet syndrome
Dravet syndrome : Clinical presentation, genetic investigation and anti-seizure medication Bradley Osterman MD, FRCPC, CSCN Objectives Learn about the typical early clinical presentation of Dravet syndrome
How to Think like a Neurologist Review of Exam Process and Assessment Findings
 Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
Is it epilepsy? Does the patient need long-term therapy?
 Is it a seizure? Definition Transient occurrence of signs and/or symptoms due to abnormal excessive or synchronous neuronal activity in the brain Is it provoked or unprovoked? Is it epilepsy? Does the
Is it a seizure? Definition Transient occurrence of signs and/or symptoms due to abnormal excessive or synchronous neuronal activity in the brain Is it provoked or unprovoked? Is it epilepsy? Does the
Measures have been taken, by the Utah Department of Health, Bureau of Health Promotions, to ensure no conflict of interest in this activity
 Measures have been taken, by the Utah Department of Health, Bureau of Health Promotions, to ensure no conflict of interest in this activity Seizures in the School Setting Meghan Candee, MD MS Assistant
Measures have been taken, by the Utah Department of Health, Bureau of Health Promotions, to ensure no conflict of interest in this activity Seizures in the School Setting Meghan Candee, MD MS Assistant
The Diagnostic Detective: Epilepsy
 The Diagnostic Detective: Epilepsy Some Facts About Epilepsy and Its Causes Seizures are the most common neurologic disorders affecting children 5% of children have a seizure during childhood There are
The Diagnostic Detective: Epilepsy Some Facts About Epilepsy and Its Causes Seizures are the most common neurologic disorders affecting children 5% of children have a seizure during childhood There are
Neuroanatomy. Assistant Professor of Anatomy Faculty of Medicine The University of Jordan Dr Maha ELBeltagy
 Neuroanatomy Dr. Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018 Development of the Central Nervous System Development of the nervous system Development
Neuroanatomy Dr. Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018 Development of the Central Nervous System Development of the nervous system Development
Appendix 2 (as supplied by the authors): ICD codes to identify high-risk children
 Appendix 2 (as supplied by the authors): ICD codes to identify high-risk children ICD-9 codes to identify high risk children in physician claims database Category of condition Condition ICD-9 code Bacterial
Appendix 2 (as supplied by the authors): ICD codes to identify high-risk children ICD-9 codes to identify high risk children in physician claims database Category of condition Condition ICD-9 code Bacterial
Slide 1. Slide 2. Slide 3. Intro to Physical Therapy for Neuromuscular Conditions. PT Evaluation. PT Evaluation
 Slide 1 Intro to Physical Therapy for Neuromuscular Conditions PTA 103 Introduction to Clinical Practice 2 Slide 2 Mental status: consciousness, attention, orientation, cognition Communication: speech
Slide 1 Intro to Physical Therapy for Neuromuscular Conditions PTA 103 Introduction to Clinical Practice 2 Slide 2 Mental status: consciousness, attention, orientation, cognition Communication: speech
Pediatic Neurology Consult and Referral Guidelines
 Pediatic Neurology Consult and Referral Guidelines Introduction We see children and teens from birth to 18 years. The most common reasons patients are referred to pediatric neurology services include:
Pediatic Neurology Consult and Referral Guidelines Introduction We see children and teens from birth to 18 years. The most common reasons patients are referred to pediatric neurology services include:
Myasthenia Gravis. Mike Gilchrist 10/30/06
 Myasthenia Gravis Mike Gilchrist 10/30/06 Overview Background Pathogenesis Clinical Manifestations Diagnosis Treatment Associated Conditions Background Severe muscle disease Most common disorder of neuromuscular
Myasthenia Gravis Mike Gilchrist 10/30/06 Overview Background Pathogenesis Clinical Manifestations Diagnosis Treatment Associated Conditions Background Severe muscle disease Most common disorder of neuromuscular
Management of Complex Febrile Seizures
 Management of Complex Febrile Seizures An 13 month old girl presents to the ED after having a shaking episode at home. Mom describes shaking of both arms and legs, lasting 20 minutes. The child has no
Management of Complex Febrile Seizures An 13 month old girl presents to the ED after having a shaking episode at home. Mom describes shaking of both arms and legs, lasting 20 minutes. The child has no
Biology 3201 Nervous System # 7: Nervous System Disorders
 Biology 3201 Nervous System # 7: Nervous System Disorders Alzheimer's Disease first identified by German physician, Alois Alzheimer, in 1906 most common neurodegenerative disease two thirds of cases of
Biology 3201 Nervous System # 7: Nervous System Disorders Alzheimer's Disease first identified by German physician, Alois Alzheimer, in 1906 most common neurodegenerative disease two thirds of cases of
Initial Treatment of Seizures in Childhood
 Initial Treatment of Seizures in Childhood Roderic L. Smith, MD, Ph.D. Pediatric Neurology Clinic of Alaska,PC Incidence of Seizures Overall 5% by age 20 yrs. Lifetime risk= 5-10% CNS Infections= 5% TBI=10%
Initial Treatment of Seizures in Childhood Roderic L. Smith, MD, Ph.D. Pediatric Neurology Clinic of Alaska,PC Incidence of Seizures Overall 5% by age 20 yrs. Lifetime risk= 5-10% CNS Infections= 5% TBI=10%
Antiepileptic agents
 Antiepileptic agents Excessive excitability of neurons in the CNS Abnormal function of ion channels Spread through neural networks Abnormal neural activity leads to abnormal motor activity Suppression
Antiepileptic agents Excessive excitability of neurons in the CNS Abnormal function of ion channels Spread through neural networks Abnormal neural activity leads to abnormal motor activity Suppression
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Epilepsy. Epilepsy can be defined as:
 Epilepsy Epilepsy can be defined as: A neurological condition causing the tendency for repeated seizures of primary cerebral origin Epilepsy is currently defined as a tendency to have recurrent seizures
Epilepsy Epilepsy can be defined as: A neurological condition causing the tendency for repeated seizures of primary cerebral origin Epilepsy is currently defined as a tendency to have recurrent seizures
ROLE OF EEG IN EPILEPTIC SYNDROMES ASSOCIATED WITH MYOCLONUS
 Version 18 A Monthly Publication presented by Professor Yasser Metwally February 2010 ROLE OF EEG IN EPILEPTIC SYNDROMES ASSOCIATED WITH MYOCLONUS EEG is an essential component in the evaluation of epilepsy.
Version 18 A Monthly Publication presented by Professor Yasser Metwally February 2010 ROLE OF EEG IN EPILEPTIC SYNDROMES ASSOCIATED WITH MYOCLONUS EEG is an essential component in the evaluation of epilepsy.
Neurological Emergencies. Aaron J. Katz, AEMT-P, CIC
 Neurological Emergencies Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 1 Stroke ( CVA ) CerebroVascular Accident Brain Attack Brain damage caused by a blockage of blood to a specific area of the brain
Neurological Emergencies Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 1 Stroke ( CVA ) CerebroVascular Accident Brain Attack Brain damage caused by a blockage of blood to a specific area of the brain
Images have been removed from the PowerPoint slides in this handout due to copyright restrictions.
 Seizures Seizures & Status Epilepticus Seizures are episodes of disturbed brain activity that cause changes in attention or behavior. Donna Lindsay, MN RN, CNS-BC, CCRN, CNRN Neuroscience Clinical Nurse
Seizures Seizures & Status Epilepticus Seizures are episodes of disturbed brain activity that cause changes in attention or behavior. Donna Lindsay, MN RN, CNS-BC, CCRN, CNRN Neuroscience Clinical Nurse
intracranial anomalies
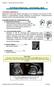 Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Neurology. Access Center 24/7 access for referring physicians (866) 353-KIDS (5437)
 Neurology The Neurology practice at Valley Children s provides diagnostic services, medical treatment, and followup care to infants, children, and adolescents who have suspected or confirmed neurological
Neurology The Neurology practice at Valley Children s provides diagnostic services, medical treatment, and followup care to infants, children, and adolescents who have suspected or confirmed neurological
Diseases of Muscle and Neuromuscular Junction
 Diseases of Muscle and Neuromuscular Junction Diseases of Muscle and Neuromuscular Junction Neuromuscular Junction Muscle Myastenia Gravis Eaton-Lambert Syndrome Toxic Infllammatory Denervation Atrophy
Diseases of Muscle and Neuromuscular Junction Diseases of Muscle and Neuromuscular Junction Neuromuscular Junction Muscle Myastenia Gravis Eaton-Lambert Syndrome Toxic Infllammatory Denervation Atrophy
Epilepsy 7/28/09! Definitions. Classification of epilepsy. Epidemiology of Seizures and Epilepsy. International classification of epilepsies
 Definitions Epilepsy Dr.Yotin Chinvarun M.D., Ph.D. Seizure: the clinical manifestation of an abnormal and excessive excitation of a population of cortical neurons Epilepsy: a tendency toward recurrent
Definitions Epilepsy Dr.Yotin Chinvarun M.D., Ph.D. Seizure: the clinical manifestation of an abnormal and excessive excitation of a population of cortical neurons Epilepsy: a tendency toward recurrent
Faculty Disclosure. Sanjay P. Singh, MD, FAAN. Dr. Singh has listed an affiliation with: Consultant Sun Pharma Speaker s Bureau Lundbeck, Sunovion
 Faculty Disclosure Sanjay P. Singh, MD, FAAN Dr. Singh has listed an affiliation with: Consultant Sun Pharma Speaker s Bureau Lundbeck, Sunovion however, no conflict of interest exists for this conference.
Faculty Disclosure Sanjay P. Singh, MD, FAAN Dr. Singh has listed an affiliation with: Consultant Sun Pharma Speaker s Bureau Lundbeck, Sunovion however, no conflict of interest exists for this conference.
Disorders of Muscle. Disorders of Muscle. Muscle Groups Involved in Myopathy. Needle Examination of EMG. History. Muscle Biopsy
 Disorders of Muscle Disorders of Muscle Zakia Bell, M.D. Associate Professor of Neurology and Physical Medicine & Rehabilitation Virginia Commonwealth University Cardinal symptom of diseases of the muscle
Disorders of Muscle Disorders of Muscle Zakia Bell, M.D. Associate Professor of Neurology and Physical Medicine & Rehabilitation Virginia Commonwealth University Cardinal symptom of diseases of the muscle
LIMP BABIES - WHAT MAY THAT MEAN?
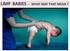 LIMP BABIES - WHAT MAY THAT MEAN? ARE WE LOOKING WHERE WE SHOULD? FLOPPY = LIMP = FLACCID = WEAK Poor head control when pulled C-posture sitting, or in ventral susp. Frog-leg lying Dropping arms Casey
LIMP BABIES - WHAT MAY THAT MEAN? ARE WE LOOKING WHERE WE SHOULD? FLOPPY = LIMP = FLACCID = WEAK Poor head control when pulled C-posture sitting, or in ventral susp. Frog-leg lying Dropping arms Casey
