Practical neurology 7 Recurrent headaches with visual disturbance
|
|
|
- Estella Abigayle Hunter
- 6 years ago
- Views:
Transcription
1 Practical neurology 7 Recurrent headaches with visual disturbance lessandro S Zagami MB BS, MD, FRCP, Neurologist, 1 and Conjoint ssociate Professor 2 Sian L Goddard BSc, MB BS, Basic Physician Trainee 1 1 Institute of Neurological Sciences, Prince of Wales Hospital, Sydney, NSW. 2 Prince of Wales Clinical School, University of New South Wales, Sydney, NSW. a.zagami@unsw.edu.au MJ 2012; 196: doi: /mja Rachel s story Rachel, who is aged 29 years, has had recurrent headaches and visual disturbance every 2 weeks or so for the past 8 years. Her headaches are usually one sided, in the frontotemporal region, but can affect either side and can even change sides during an attack. She describes them as throbbing. She always has associated nausea and often vomits when she takes oral medication. In addition, she is averse to light (photophobia), sound (phonophobia) and smells (osmophobia) during attacks. Most attacks wake her around 3 or 4 am. With daytime attacks, a visual disturbance is the first sign, which she describes as a patch of missing vision that enlarges into an arc like a bright shimmering light with a jagged edge. This can occur on the same or other side to the headache, and lasts 20 minutes. On some occasions, she develops numbness on one side of her body, which slowly spreads from her hand and arm up to the side of her face, lips and tongue, and similarly lasts about 20 minutes. Occasionally, she has difficulty with speech, concentration and decision making. The headaches start as these symptoms resolve; they usually last about a day (but up to 3 days) and they leave her feeling washed out for a day or so after. Rachel first developed her headaches around the time of menarche. She was initially treated with the combined oral contraceptive pill because of bad headaches with her periods, but the pill worsened the headaches and was withdrawn. Stress is also a trigger. In addition, she has other (more frequent) headaches without aura, which she treats with ibuprofen. She has difficulty telling whether one of these will develop into one of the more severe headaches. Because of the frequent and severe headaches, she has been avoiding going out and feels that her headaches are ruling her life. She smokes 6 10 cigarettes per day but rarely drinks alcohol. Her mother and brother suffer from migraine. Results of her neurological examination are normal. Her body mass index is 26 kg/m 2. PPROCH TO THE PROBLEM Making the diagnosis Headache, particularly migraine, is the commonest neurological problem with which patients present to general Previous article in this series Memory loss in practitioners and neurologists. Comprehensive historytaking offers the best chance of establishing whether a MJ 2012; 196: headache is primary (idiopathic) or secondary to an underlying condition. Most headaches encountered in practice The grading system for are primary, either migraine headache or tension-type recommendations The Medical in Journal headache. of ustralia Less common ISSN: primary headaches include cluster 2012 headache, primary cough and exertional headache, this article is described 729X 20 February in MJ 2011; 195: 328 The Medical primary Journal sex of headache ustralia and 2012 primary thunderclap headache. The second edition of The international classification of Clinical focus Neurology Series Editors Craig S nderson MB BS, PhD, FRCP Leo Davies MB BS, MD, FRCP headache disorders provides a comprehensive description of the many types of headache. 1 Important features in the patient history are: location, temporal pattern and quality of the pain; presence of associated symptoms; and presence of specific triggers (eg, Summary Headache, particularly migraine, is the commonest neurological problem with which patients present to general practitioners and neurologists. Episodic migraine affects up to 18% of women and 6% of men. cute migraine attacks can be severely disabling and chronic migraine is even more disabling. Of the mental and neurological disorders, migraine ranks eighth worldwide in terms of disability. Migraine is one of the primary headaches and may occur with or without aura. Differentiation from other severe primary headaches, such as cluster headache, is important for management. The vast majority of patients with migraine can be satisfactorily helped and treated. This involves acute and prophylactic drug therapy and management of triggers. In patients with migraine, medication overuse headache and chronic migraine need to be identified and treated. exertion, coughing, sneezing). Red flags that may indicate a secondary headache are summarised by the mnemonic SNOOP4 (Box 1). 2 When any of these red flags are present, brain imaging is mandatory (computed tomography or magnetic resonance, depending on how or when the patient presents, resource availability and clinical urgency). However, for most patients with migraine, brain imaging is not necessary. Recognising the features of migraine headache Migraine headache is defined by the features of the headache and the presence of associated symptoms (Box 2). 1 Migraine is considered a primary disorder of the central nervous system (CNS). It is a chronic disorder with episodic manifestations, and it is often familial and has a strong genetic component. Episodic migraine affects up to 18% of women and 6% of men. Neck pain is also very common in migraine up to 60% of patients complain of occipital or neck pain during their migraine attacks and this is nearly always a referred pain. Pathological conditions of the upper cervical spine, which are uncommon, can cause headache; however, disorders of the cervical spine are not a common cause of migraine. The manifestations of migraine are believed to be due to increased cortical neuronal excitability, owing to defective modulatory pathways in the brainstem and possibly other structures in the CNS. In particular, the aura of migraine is not due to vasospasm it is due to altered neuronal activity called cortical spreading depression. 3-5 For Rachel, the other features of her attacks that make the diagnosis of migraine definite are the change in sides of both the headache and aura. In addition to the headache 178
2 1 SNOOP4 headache red flags* 1 Systemic symptoms (fever, weight loss) or secondary risk factors (HIV, cancer) Neurological symptoms or abnormal signs (confusion, impaired alertness or consciousness) Onset sudden, abrupt or split second ( thunderclap ) Older new onset or progressive headache, especially in patients older than 50 years (giant cell arteritis) Previous headache history first headache or different headache (change in attack frequency, severity or clinical features) Postural or positional aggravation Precipitated by a Valsalva manoeuvre or exertion Papilloedema * Indicating that secondary causes should be considered. 3 Typical locations of primary and secondary headaches 2 Diagnostic criteria for migraine without aura t least five attacks Headaches last 4 72 hours t least two of the following headache characteristics: unilateral pulsating moderate to severe pain aggravated by, or causes avoidance of, routine physical activity t least one of the following during headaches: nausea and/or vomiting photophobia and phonophobia phase, there are often premonitory and resolution phases. 3,6 In some patients with migraine, nausea and vomiting are the most disabling features; in others, it is the aura or the severity of the headache. cute migraine attacks can be severely disabling, and chronic migraine is even more disabling. The World Health Organization ranks migraine as 19th worldwide of all the causes of years lived with a disability due to a medical condition and eighth of the mental and neurological disorders in terms of disability. In high-income countries such as ustralia, the total disability due to migraine is said to be more than 1.5 times that due to multiple sclerosis and Parkinson disease combined and almost three times that due to epilepsy. 7 However, it is considerably under-recognised, underdiagnosed and undertreated worldwide. DIFFERENTIL DIGNOSES The locations of migraine headache and other types of primary and secondary headaches are shown in Box 3. It is important to distinguish migraine headache from cluster headache, as the approaches to management differ significantly. Cluster headache is one of the trigeminal autonomic cephalalgias, 1 which are characterised by strictly unilateral headaches with autonomic features. It is differentiated from migraine by the duration and frequency of attacks. Cluster headache has such a dramatic presentation, and the headache is so excruciating, that it should never be missed. Patients can have up to eight attacks per day, with attacks lasting minutes each. Nocturnal attacks that wake the patient are common. The patient is usually agitated and will pace about (in contrast to migraine, where the The usual intensity of the headache in the various locations is denoted by the density of the shading. The discomfort in tension-type headache is usually described as a weight on the head or a tight band around the whole head. The pain of trigeminal neuralgia is lancinating and shock-like and is usually felt in the second or third divisions of the trigeminal nerve. Reproduced with permission from James W Lance. patient will lie still). Cluster headache is accompanied by redness or tearing of the eye, drooping of the eyelid and constriction of the pupil (Horner syndrome) on the ipsilateral side, and blockage or running of the nostril (autonomic features) on the ipsilateral side. Management of cluster headaches includes inhaled oxygen (100%, 12 L/minute, 15 minutes, grade evidence) 8 or acute sumatriptan therapy (6 mg, subcutaneous injection, grade evidence), and oral verapamil for prophylaxis (grade evidence). 9 MIGRINE UR Migraine aura, which is almost always (in more than 95% of cases) visual but sometimes involves other senses or speech, occurs in up to 30% of patients with migraine (Box 4). 1 True weakness does not occur in typical migraine with aura, but may occur in hemiplegic migraine and basilar-type migraine, which are very rare. 1 ura symptoms usually consist of positive features (eg, flickering lights) and negative features (eg, scotomata). The symptoms develop over several minutes and spread gradually, but usually resolve within 60 minutes. The visual aura can be in one or both visual fields, although many patients describe it as being in one eye unless prompted to do the cover test (where the patient covers each eye in turn to observe whether the aura persists). The visual aura can be simple (unformed flashes or phosphenes) or complex (classical fortification spectra), as experienced by Rachel. Other sensory aura symptoms are usually unilateral and on the contralateral side to the headache, but they can sometimes be ipsilateral, as can visual aura. ura symptoms may also alternate sides from one attack to the next. These characteristics help distinguish them from the symptoms of a transient ischaemic attack. 179
3 4 Diagnostic criteria for migraine with typical aura 4 t least two attacks One or more fully reversible aura symptoms indicating focal cortical and/or brainstem dysfunction, such as flickering lights or loss of vision, and unilateral pins and needles or numbness No aura symptom lasts longer than 60 minutes Headache follows aura with a headache-free interval of less than 60 minutes 5 Complicating issues and treatment options Nausea and vomiting: use antiemetics; consider non-oral medications (rizatriptan wafers, sumatriptan nasal spray or injection, rectal diclofenac, rectal indomethacin, rectal prochlorperazine) Frequent nocturnal onset: consider prophylaxis, even if frequency is not high; identify the presence of any warning the night before and consider pre-emptive treatment (ie, treatment given in the evening, such as an NSID) Frequent recurrence after initial relief of headache: consider an ergot preparation, naratriptan (as the incidence of recurrence is lower than for other triptans) or a triptan with a long-acting NSID 16 Severe perimenstrual attacks: consider perimenstrual pre-emptive treatment (eg, ergot preparation or NSID therapy) (need diary) or prophylaxis, as menstrually related 16, 17 attacks are often severe and refractory to acute treatment Elevated body mass index: avoid agents likely to cause increased appetite and weight gain (amitripyline, pizotifen, sodium valproate); consider topiramate (warn patient of, and monitor for, potentially serious adverse effects) Concomitant SSRI or SNRI use: warn patient about, and monitor for, potential serotonergic adverse effects (eg, confusion, autonomic effects, tremor) if serotonergic antimigraine medication (ergot preparations, methysergide, triptans) is prescribed Triptan failure: if ineffective, try another; if adverse effects, try naratriptan (which has the best side-effect profile of the triptans available in ustralia) Intolerance to, failure of, or reticence to use, pharmacological treatments: consider non-pharmacological approaches (eg, behavioural treatment and acupuncture) 16,18,19 Medication overuse headache: identify and manage (see main text) Comorbidities (eg, depression): identify and manage NSID = non-steroidal anti-inflammatory drug. SNRI = serotonin and noradrenaline reuptake inhibitor. SSRI =selective serotonin reuptake inhibitor. Patients who suffer migraine with aura can go on to have visual aura without headache in later years. lso, migraine aura without headache can occur for the first time in later life the so called transient migrainous accompaniments. 4 Such symptoms must firstly be considered as possibly being due to another neurological problem, such as a transient ischaemic attack or giant cell arteritis. Hence, patients with strictly unilateral headaches and contralateral aura, atypical aura, or first visual or other neurological disturbance with or without headache at over 50 years of age should be referred to a neurologist for urgent assessment and brain imaging, preferably with magnetic resonance imaging. COMPLICTIONS OF MIGRINE Chronic migraine Chronic migraine is diagnosed when a patient known to have migraine without aura has headaches on 15 or more days per month for at least 3 months, of which eight or more per month meet the criteria for migraine without aura or respond to migraine-specific acute medication (triptans or ergot preparations). 10 Its prevalence is 2% worldwide 11 and patients with chronic migraine are more disabled, have a lower quality of life, have a higher rate of psychiatric comorbidity and use significantly more health care resources than patients with episodic migraine. 12 bout 2.5% of patients with episodic migraine will progress to FINL DIGNOSIS Migraine with aura chronic migraine over a year. Risk factors for progression include female sex, lower socioeconomic status and increased caffeine intake. 11 Medication overuse is also an important contributor to development of chronic migraine. Medication overuse headache (MOH) MOH is likely in patients who have headache on 15 or more days per month for more than 3 months, have been using acute medication therapies frequently and have had worsening of the headaches while using the acute medication. 13 Frequent use of ergot preparations, opiates, triptans or combination analgesics is defined as 10 or more days per month and for simple analgesics 15 or more days per month. Many patients with MOH have daily headaches and take acute medication every day or nearly every day. Prophylactic therapies are usually ineffective for migraine if MOH is present, and MOH is a risk factor for progression from episodic migraine to chronic migraine. n accurate patient history of all acute medication use (including paracetamol) and caffeine is needed. Some agents, including triptans, can lead to MOH and chronic migraine more quickly than others, such as simple analgesics or nonsteroidal anti-inflammatory drugs (NSIDs). In ustralia, overuse of codeine-containing agents is particularly common and carries the added potential risk of dependency. Management of MOH involves education of the patient, appropriate prophylactic medication and withdrawal of the offending acute medication therapy. MOH can usually be managed in the outpatient setting, but hospital admission is sometimes needed for a dihydroergotamine (DHE) or lignocaine infusion. Risk of stroke in migraine The risk of stroke is increased in patients with migraine. ccording to a recent meta-analysis, there is a twofold increased risk of ischaemic stroke which occurs in patients with migraine with aura but not in patients with migraine without aura. 14 Women are more at risk, particularly if they are young (under 45 years), smokers and taking the oral contraceptive pill. The overall absolute risk is, however, quite low, and stroke in young patients with migraine is rare. 15 Rachel has migraine with aura, nocturnal severe migraine and other headaches of the tension type. Because of her frequent use of NSIDs, the possibility of MOH was discussed and she was asked to start keeping a simple headache diary. For daytime attacks with aura, she was asked to take diclofenac potassium 50 mg tablets with domperidone mg at the onset of her aura or as soon as she developed a migraine headache without aura. If she went on to develop a headache despite taking diclofenac at the onset of aura, she was to repeat the dose of diclofenac. She was encouraged to avoid using anything for milder headaches. For nocturnal attacks, she was asked to try ondansetron wafers and an indomethacin suppository (as oral therapy was futile). Rachel required prophylaxis, but was reticent to accept such therapy because a previous trial of pizotifen had led to 8 kg of weight gain. Because of her frequent aura attacks, -blocker therapy was not recommended. She agreed to start on low-dose amitriptyline (10 mg at night) in the first instance. The risk of stroke in migraine was discussed. The greatest risk is in younger women who suffer migraine with aura, and who smoke and use the combined oral contraceptive pill. She agreed to cease smoking. 180
4 6 Recommended drugs for the acute treatment of migraine Drug Dose Specific considerations PBS status* Grade of evidence 17,21 Common or serious adverse effects, interactions and warnings Simple analgesics and NSIDs spirin Diclofenac potassium Ibuprofen mg mg mg No Yes Yes Caution needed in patients with asthma and those with renal impairment ll can cause peptic ulceration and excessive bleeding Naproxen sodium mg Yes Indomethacin 100 mg Suppository; useful if severe nausea or No B vomiting is present Diclofenac sodium mg Suppository; useful if severe nausea or vomiting is present No B Triptans Eletriptan mg Lower incidence of recurrence; potent CYP34 inhibitor Naratriptan 2.5 mg Best tolerated triptan of those available in ustralia but slower to be effective; lower incidence of recurrence Rizatriptan 10 mg Wafer form; consider if nausea or vomiting are prominent or if patient is unable to take tablets; possible interaction with propranolol Sumatriptan 50 mg Tablets Yes, S mg Nasal spray Yes, S 6 mg Subcutaneous injection Yes Zolmitriptan mg CYP450 interaction Yes, R, X NSIDs are not suitable for patients with a high cardiovascular risk profile or those who are pregnant Yes, S Yes, R, X Yes, S class adverse effect of all triptans is the presence of atypical sensations over the chest, neck or throat, including heaviness, paraesthesias, pressure or tightness Other adverse effects include dizziness, palpitations, somnolence and tingling Contraindicated in patients with peripheral vascular, cerebrovascular and ischaemic heart disease, and in those with uncontrolled hypertension Not to be used concurrently with ergot derivatives (including methysergide) or MOIs ( 2 weeks) Potential interactions with SSRIs, SNRIs and St John s Wort R = authority required. S = authority required (Streamlined uthority Code 3233). X = authority required, indication(s) to waive special patient contribution. CYP34 = cytochrome P450 subtype. CYP450 = cytochrome P450. MOI = monoamine oxidase inhibitor. NSID = non-steroidal anti-inflammatory drug. PBS = Pharmaceutical Benefits Scheme. SNRI = serotonin and noradrenaline reuptake inhibitor. SSRI = selective serotonin reuptake inhibitor. * Yes means a PBS indication for migraine, No means no PBS indication for migraine. These apply to group as a whole, unless otherwise specified. MNGEMENT Management of episodic migraine Patients with episodic migraine need to be given an explanation of the condition and a treatment plan, and the treatment goals need to be discussed. Online resources for patients are available from Headache ustralia ( headacheaustralia.org.au, see the imanage Migraine app), the World Headache lliance ( and the BMJ ( 05/migraine-pain-and-pressure). Treatment options for complicating factors are shown in Box 5. Keeping a diary: headache diary is invaluable for establishing baseline headache frequency, identifying patterns (such as an association of migraine attacks with menstruation), quantifying lost work time, monitoring treatment response, and identifying MOH. Identifying triggers: The commonest triggers in migraine without aura are stress, foods (eg, alcohol, chocolate, dairy foods [particularly cheese]) and menstruation. 6 In migraine with aura, a visual stimulus (eg, flickering light) is a common trigger. Triggers should generally be avoided, although an alternative behavioural approach of trying to cope with some triggers has been suggested. 19 However, many patients cannot identify triggers, and some triggers may be complex (eg, a period of stress coinciding with menstruation). Only about 10% of women with migraine have pure menstrual migraine, where they only have attacks during menstruation. cute treatment: It is important to tailor the acute treatment to both the individual patient and to the different attacks experienced by the individual patient. cute medication therapies in migraine are either non-specific (paracetamol, aspirin or other NSIDs) or migrainespecific (ergot preparations and triptans) (Box 6). Initial treatment should be with simple analgesics and NSIDs, taken at the earliest possible time (at onset of aura, if present). Suppositories can be helpful in patients with significant nausea or those who are already vomiting. ntiemetic and prokinetic drugs are helpful in treating associated nausea and may improve the efficacy of analgesics, NSIDs and triptans by overcoming associated gastroparesis. ntiemetics may also reduce the severity of the headache and should always be used if there is nausea. Local guidelines list oral domperidone mg (grade B evidence), metoclopramide mg (grade B evidence) and prochlorperazine 10 mg, and prochlorperazine 25 mg suppositories. 17 Domperidone is much less likely than metoclopramide or prochlorperazine to cause a dystonic reaction or akathisia. lthough only PBS listed for cytotoxic chemotherapy-related nausea and vomiting, ondansetron wafers are often the most effective antiemetic for some patients; however, cost is an issue. Second-line agents for acute treatment are ergot preparations and triptans. No oral or rectal ergot preparations are commercially available in ustralia, but compounded ergot preparations can be obtained. Triptans should be used if first-line agents have been ineffective after 1 2 hours or ineffective in previous attacks. Unlike the other acute medication therapies, triptans are generally ineffective 181
5 7 Drugs recommended for the prophylactic treatment of migraine* Drug Dose Class of drug TG status PBS status Grade of evidence 21,23 Common or serious adverse effects First choice Propranolol mg twice daily -blocker Yes Yes Hypotension, fatigue, insomnia mitriptyline mg nightly Tricyclic antidepressant Yes No Sedation, dry mouth, weight gain Pizotifen mg nightly Serotonin antagonist Yes Yes B Sedation, weight gain Metoprolol mg twice daily -blocker Yes Yes B Hypotension, bradycardia Second choice Sodium valproate mg twice daily nticonvulsant No No Weight gain, tremor, hair loss Topiramate mg twice daily nticonvulsant Yes Yes, S Paraesthesias, cognitive impairment, mood and personality changes, weight loss Verapamil mg daily Calcium-channel blocker No No B Constipation, swollen ankles, flushing Gabapentin mg daily nticonvulsant No No C Dizziness, sedation S = uthority required (Streamlined uthority Code 2799). PBS = Pharmaceutical Benefits Scheme. TG = Therapeutic Goods dministration. * Third choice drugs are flunarizine, methysergide, lisinopril, cyproheptadine, candesartan, magnesium and riboflavin. Yes means TG approved for migraine, No means not TG approved for migraine. Yes means a PBS indication for migraine, No means no PBS indication for migraine. if taken at the aura stage, but are effective during the headache phase. Parenteral agents may be required for patients whose condition fails to respond to oral agents or who are vomiting and cannot tolerate oral agents. DHE mg can be given by subcutaneous, intramuscular or intravenous injection always with an antiemetic or sumatriptan 6 mg can be given by subcutaneous injection. Emerging treatments: With new treatments emerging, this is an exciting time in the field of migraine management. On the horizon are new classes of non-vasoconstrictor drugs, calcitonin gene-related peptide (CGRP) antagonists ( gepants ) and serotonin 1F receptor agonists, as well as novel neuromodulation techniques such as occipital nerve stimulators and transcranial magnetic stimulation. 20 Treatment of status migrainosus Status migrainosus is a debilitating migraine attack that lasts more than 72 hours and is refractory to the patient s usual treatments. 1 Hospital admission and treatment of dehydration with intravenous fluids are usually necessary. Parenteral administration of DHE, with an antiemetic, can be effective in this situation. Some guidelines suggest using 8-hourly intravenous injections of mg DHE. 17 However, in our experience, it is better tolerated as an infusion of 3mg DHE over 24 hours (which can be titrated up or down according to response and adverse effects). Other options include parenteral chlorpromazine, droperidol, prochlorperazine and sumatriptan. 17 Prophylaxis of episodic migraine Patients who have three or more migraine attacks per month are usually considered as being suitable for prophylaxis. However, prophylaxis may also be warranted in patients who have fewer attacks for example, if the attacks last days, do not respond to acute treatment, cause lost work time or are otherwise disabling. Conversely, patients who have more than three attacks per month FCT OR FICTION? that are all reliably aborted by acute treatment may not need prophylaxis. The aim of prophylactic treatment is not only to reduce the frequency of attacks but also to reduce severity and duration of the attacks and to render the attacks more amenable to acute treatment. The initial choice of prophylactic agent is usually based on sideeffect profiles and patient characteristics. First-line prophylactic agents are serotonin reuptake inhibitors such as amitriptyline, other tricyclic antidepressants, 5-HT 2 - receptor antagonists (pizotifen) and -blockers (propranolol and metoprolol) (Box 7). 17,21-23 The -blockers, however, are best avoided in patients who have frequent migraine with aura as they can worsen the aura. It is appropriate for a general practitioner or other physician to initiate prophylaxis with first-line agents, but, if these are ineffective or cause adverse effects, referral to a neurologist is appropriate. Prophylactic agents should be trialled for at least a month at the highest tolerated dose before being deemed ineffective. Once good control has been achieved for at least 6 months, it may be possible to wean the patient off the drug. In more severely affected patients (eg, those with a longstanding history of very frequent attacks), a longer period of prophylactic therapy or combination prophylactic therapy may be needed. Management of chronic migraine In some patients with chronic migraine, the condition responds to treatment with topiramate 11 or repeated injection of onabotulinumtoxin into multiple sites in the head and neck. 24 multidisciplinary approach, including behavioural pain management, to chronic migraine and other refractory headaches (eg, in a dedicated headache clinic) is more likely to be successful than other approaches. 25 FCT: It is true that the risk of stroke is increased in patients who suffer migraine with aura. FICTION: It is not true that disorders of the cervical spine are commonly a cause for migraine (although neck pain is very common). 182
6 Rachel returned 2 months later with her diary. Overall, she felt that there had been some improvement. ccording to her diary, she had had 17 headache days, more than she thought she was having before keeping the diary. Some of her less severe headaches resolved without treatment, which surprised her. She had had three daytime-onset migraine attacks with aura, two of which responded to diclofenac and domperidone. She had had two full-blown nocturnal-onset attacks, one of which occurred during her period; the attack during her period did not respond to ondansetron and indomethacin but the other did, and this was the first time she had ever been able to abort a fullblown attack. However, she had put on more weight despite taking only a low dose of amitriptyline. Topiramate 25 mg at night was added to Rachel s prophylactic therapy regimen, and she was given a schedule to gradually increase the dose. She was advised to use rizatriptan wafers for attacks that did not respond to initial treatment. Rachel returned 3 months later and was pleased to show us her diary. She was taking topiramate (25 mg in the morning and 50 mg at night) and amitriptyline. She was experiencing pins and needles in her hands and feet but these were resolving and she had managed to lose weight (several kilograms). She had had only one nocturnalonset attack, which responded to treatment, and no vomiting. She had had five daytime-onset attacks of migraine with aura, which had also responded to treatment, although she needed to use rizatriptan on two occasions. She had not missed any work days due to migraines, had started going out again and felt that she was finally getting her life back on track. Since she was responding to the topiramate without significant adverse effects, she was asked to increase it to 50 mg twice daily and to cease amitriptyline. t her last review, Rachel was very happy with her situation. She had had no nocturnal-onset attacks and infrequent daytime-onset attacks with aura, which she reliably aborted. She had already started weaning herself off topiramate. It was agreed that she should come off topiramate as she no longer needed prophylaxis. She rang 6 months later to say that she remained essentially migraine-free. Competing interests: lessandro Zagami receives financial support from the National Health and Medical Research Council and the ustralian Brain Foundation. Provenance: Commissioned; externally peer reviewed. 1 International Headache Society. IHS Classification ICHD-II. (accessed Feb 2012). 2 Lipton RB, Silberstein SD, Dodick DW. Overview of diagnosis and classification. In: Silberstein SD, Lipton RB, Dodick DW, editors. Wolff's headache and other head pain. 8th ed. New York: Oxford University Press, 2008: Silberstein SD. Migraine. Lancet 2004; 363: Lance JW, Goadsby PJ. Mechanism and management of headache. 7th ed. Philadelphia: Elsevier, Goadsby PJ. Pathophysiology of migraine. Neurologic Clinics 2009; 27: Zagami S, Bahra. Symptomatology of migraines without aura. In: Olesen J, Goadsby PJ, Ramadan NM, et al, editors. The headaches. 3rd ed. Philadelphia: Lippincott Williams and Williams, 2006: Collins PY, Patel V. Grand challenges in global mental health. Nature 2011; 475: Cohen S, Burns B, Goadsby PJ. High-flow oxygen for treatment of cluster headache: a randomized trial. JM 2009; 302: May, Leone M, fra J, et al. EFNS guidelines on the treatment of cluster headache and other trigeminal-autonomic cephalalgias. Eur J Neurol 2006; 13: Olesen J, Bousser M-G, Diener H-C, et al. New appendix criteria open for a broader concept of chronic migraine. Cephalalgia 2006; 26: Vargas BB, Dodick DW. The face of chronic migraine: epidemiology, demographics, and treatment strategies. Neurol Clin 2009; 27: Blumenfeld M, Varon SF, Wilcox TK, et al. Disability, HRQoL and resource use among chronic and episodic migraineurs: results from the International Burden of Migraine Study (IBMS). Cephalalgia 2011; 31: Silberstein SD, Olesen J, Bousser M-G, et al. The international classification of headache disorders, 2nd edition (ICDH-II) revision of criteria for 8.2 Medication-overuse headache. Cephalalgia 2005; 25: Schurks M, Rist P, Bigal M, et al. Migraine and cardiovascular disease: systemic review and meta-analysis. BMJ 2009; 339: b Kurth T, Chabrait H, Bousser M-G. Migraine and stroke: a complex association with clinical implications. Lancet Neurol 2012; 11: Goadsby PJ, Sprenger T. Current practice and future directions in the prevention and acute management of migraine. Lancet Neurol 2010; 9: Neurology Expert Group. Therapeutic guidelines: neurology. Version 4. Melbourne: Therapeutic Guidelines, 2011: Sun-Edelstein C, Mauskop. lternative headache treatments: neutraceuticals, behavioural and physical treatments. Headache 2011; 51: Martin PR, MacLeod C. Behavioral management of headache triggers: avoidance of triggers is an inadequate strategy. Clin Psychol Rev 2009; 29: Magis D, Schoenen J. Treatment of migraine: update on new therapies. Curr Opin Neurol 2011; 24: Evers S, fra J, Frese, et al. EFNS guideline on the drug treatment of migraine-revised report of an EFNS task force. Eur J Neurol 2009; 16: Stark RJ, Stark CD. Migraine prophylaxis. Med J ust 2008; 189: Fenstermacher N, Levin M, Ward T. Pharmacological prevention of migraine. BMJ 2011; 342: d urora SK, Winner P, Freeman MC, et al. Onabotulinumtoxin for treatment of chronic migraine: pooled analyses of the 56-week PREEMPT clinical program. Headache 2011; 51: Diener H-C, Gaul C, Jensen R, et al. Integrated headache care. Cephalalgia 2011; 31:
How do we treat migraine? New SIGN Guidelines
 How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
Treatments for migraine
 Treatments for migraine Information for patients and carers Department of Neurology Aberdeen Royal Infirmary Contents Page About this leaflet Abortive medication for migraine Painkillers Antisickness medication
Treatments for migraine Information for patients and carers Department of Neurology Aberdeen Royal Infirmary Contents Page About this leaflet Abortive medication for migraine Painkillers Antisickness medication
HMFP Comprehensive Headache Center Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center Instructor in
 HMFP Comprehensive Headache Center Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center Instructor in Anesthesia and Neurology Harvard Medical School Limited time
HMFP Comprehensive Headache Center Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center Instructor in Anesthesia and Neurology Harvard Medical School Limited time
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline. Scottish intercollegiate Guidelines Network SIGN
 A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
Migraine Management. Jane Melling Headache nurse Mater Misericordiae Hospital
 Migraine Management Jane Melling Headache nurse Mater Misericordiae Hospital Migraine facts Among the most common disorders of the nervous system 3 rd most prevalent medical disorder on the planet (lancet
Migraine Management Jane Melling Headache nurse Mater Misericordiae Hospital Migraine facts Among the most common disorders of the nervous system 3 rd most prevalent medical disorder on the planet (lancet
Update on Diagnosis and Management of Migraines
 Update on Diagnosis and Management of Migraines Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Learning Objectives To distinguish
Update on Diagnosis and Management of Migraines Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Learning Objectives To distinguish
ADVANCES IN MIGRAINE MANAGEMENT
 ADVANCES IN MIGRAINE MANAGEMENT Joanna Girard Katzman, M.D.MSPH Assistant Professor, Dept. of Neurology Project ECHO, Chronic Pain Program University of New Mexico Outline Migraine throughout the decades
ADVANCES IN MIGRAINE MANAGEMENT Joanna Girard Katzman, M.D.MSPH Assistant Professor, Dept. of Neurology Project ECHO, Chronic Pain Program University of New Mexico Outline Migraine throughout the decades
Management of headache
 Management of headache TJ Steiner Imperial College London Based on European principles of management of common headache disorders TJ Steiner, K Paemeleire, R Jensen, D Valade, L Savi, MJA Lainez, H-C Diener,
Management of headache TJ Steiner Imperial College London Based on European principles of management of common headache disorders TJ Steiner, K Paemeleire, R Jensen, D Valade, L Savi, MJA Lainez, H-C Diener,
MIGRAINE A MYSTERY HEADACHE
 MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
COMBINATION THERAPIES PREVENTATIVE THERAPIES BETA BLOCKERS
 ACUTE THEAPIES TIPTANS TICYCLIC ANTIDEPESSANTS When starting acute treatment, healthcare professionals should warn patients about the risk of developing medication-overuse headache. ASPIIN Aspirin (900
ACUTE THEAPIES TIPTANS TICYCLIC ANTIDEPESSANTS When starting acute treatment, healthcare professionals should warn patients about the risk of developing medication-overuse headache. ASPIIN Aspirin (900
Reflections on NICE Headache Guideline. Dr Kay Kennis GPwSI in Headache, Bradford
 Reflections on NICE Headache Guideline Dr Kay Kennis GPwSI in Headache, Bradford Overview The process of guideline development illustrated with the headache guideline Reflections on the process Key recommendations
Reflections on NICE Headache Guideline Dr Kay Kennis GPwSI in Headache, Bradford Overview The process of guideline development illustrated with the headache guideline Reflections on the process Key recommendations
MIGRAINE UPDATE. Objectives & Disclosures. Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment.
 MIGRAINE UPDATE Karen L. Bremer, MD November 16, 2018 Objectives & Disclosures Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment. Disclosure: I am
MIGRAINE UPDATE Karen L. Bremer, MD November 16, 2018 Objectives & Disclosures Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment. Disclosure: I am
How could I be having migraine when I don't have a headache?
 Migraine Your doctor thinks you may have migraine. Classic migraine attacks start with visual symptoms (often zig-zag colored lights or flashes of light expanding to one side over 10-30 minutes) followed
Migraine Your doctor thinks you may have migraine. Classic migraine attacks start with visual symptoms (often zig-zag colored lights or flashes of light expanding to one side over 10-30 minutes) followed
Management options for Migraine. Prof. Dr. Khwaja Nazimuddin Head Dept. of Internal Medicine BIRDEM
 Management options for Migraine Prof. Dr. Khwaja Nazimuddin Head Dept. of Internal Medicine BIRDEM Assessment The Migraine Disability Assessment Score MIDAS Complete loss of work Partial loss of work Off
Management options for Migraine Prof. Dr. Khwaja Nazimuddin Head Dept. of Internal Medicine BIRDEM Assessment The Migraine Disability Assessment Score MIDAS Complete loss of work Partial loss of work Off
M0BCore Safety Profile. Pharmaceutical form(s)/strength: ordispersible tablet SE/H/PSUR/0022/002 Date of FAR:
 M0BCore Safety Profile Active substance: Zolmitriptan Pharmaceutical form(s)/strength: ordispersible tablet P-RMS: SE/H/PSUR/0022/002 Date of FAR: 15.03.2014 4.3 Contraindications Zolmitriptan is contraindicated
M0BCore Safety Profile Active substance: Zolmitriptan Pharmaceutical form(s)/strength: ordispersible tablet P-RMS: SE/H/PSUR/0022/002 Date of FAR: 15.03.2014 4.3 Contraindications Zolmitriptan is contraindicated
SIGN on the pharmacological management of migraine
 GUIDELINES SIGN on the pharmacological management of migraine STEVE CHAPLIN In February 2018, the Scottish Intercollegiate Guidelines Network (SIGN) published a new guideline on the pharmacological management
GUIDELINES SIGN on the pharmacological management of migraine STEVE CHAPLIN In February 2018, the Scottish Intercollegiate Guidelines Network (SIGN) published a new guideline on the pharmacological management
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Primary Care Adult Headache Management Pathway (formerly North West Headache Management Guideline for Adults) Version 1.0
 Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
Disclosures. Triptans for Kids 5/16/13
 5/16/13 Disclosures Triptans for Kids Amy A. Gelfand, MD GelfandA@neuropeds.ucsf.edu Departments of Neurology and Pediatrics UCSF Child Neurology and Headache Center I receive grant funding from: NIH/NINDS
5/16/13 Disclosures Triptans for Kids Amy A. Gelfand, MD GelfandA@neuropeds.ucsf.edu Departments of Neurology and Pediatrics UCSF Child Neurology and Headache Center I receive grant funding from: NIH/NINDS
What is new in the migraine world! Modar Khalil Consultant neurologist Hull Royal Infirmary
 What is new in the migraine world! Modar Khalil Consultant neurologist Hull Royal Infirmary Overview Understanding the burden Commonly used terms Acute therapy What we currently have What we are going
What is new in the migraine world! Modar Khalil Consultant neurologist Hull Royal Infirmary Overview Understanding the burden Commonly used terms Acute therapy What we currently have What we are going
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert
 Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE
 Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE IHS Classification 1989 (updated 2004) Primary Headaches 4 categories Migraine Tension-type Cluster and other trigeminal
Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE IHS Classification 1989 (updated 2004) Primary Headaches 4 categories Migraine Tension-type Cluster and other trigeminal
Headache. Section 1. Migraine headache. Clinical presentation
 Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
Migraine Management. Dr Helen Brown Director of Neurology and Stroke The Princess Alexandra Hospital
 Migraine Management Dr Helen Brown Director of Neurology and Stroke The Princess Alexandra Hospital Referral Criteria for Migraine Migraine Management Migraine Diagnosis Spot on Health Migraine pathway
Migraine Management Dr Helen Brown Director of Neurology and Stroke The Princess Alexandra Hospital Referral Criteria for Migraine Migraine Management Migraine Diagnosis Spot on Health Migraine pathway
ONZETRA XSAIL (sumatriptan) nasal powder
 ONZETRA XSAIL (sumatriptan) nasal powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
ONZETRA XSAIL (sumatriptan) nasal powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy
 HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
New Zealand Data Sheet
 Arrow - Sumatriptan Sumatriptan Injection 6mg/0.5mL Presentation New Zealand Data Sheet ARROW SUMATRIPTAN Injection 6mg/0.5mL is a clear, colourless to pale yellow solution in a prefilled syringe. Uses
Arrow - Sumatriptan Sumatriptan Injection 6mg/0.5mL Presentation New Zealand Data Sheet ARROW SUMATRIPTAN Injection 6mg/0.5mL is a clear, colourless to pale yellow solution in a prefilled syringe. Uses
MIGRAINE ASSOCIATION OF IRELAND
 MIGRAINE ASSOCIATION OF IRELAND HEADACHE IN MEN: THE FACTS This leaflet was composed by Paolo Rossi M.D., Ph.D. of the European Headache Alliance to mark European Migraine Day of Action 2014. Why a leaflet
MIGRAINE ASSOCIATION OF IRELAND HEADACHE IN MEN: THE FACTS This leaflet was composed by Paolo Rossi M.D., Ph.D. of the European Headache Alliance to mark European Migraine Day of Action 2014. Why a leaflet
Index. Prim Care Clin Office Pract 31 (2004) Note: Page numbers of article titles are in boldface type.
 Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache
 MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache Measure Description Percentage of patients age 18 years old and older diagnosed with migraine headache whose migraine frequency is 4 migraine
MEASURE #3: PREVENTIVE MIGRAINE MEDICATION PRESCRIBED Headache Measure Description Percentage of patients age 18 years old and older diagnosed with migraine headache whose migraine frequency is 4 migraine
HEADACHE. Dr Nick Pendleton. September Headache
 HEADACHE Dr Nick Pendleton September 2017 Headache Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache Raised ICP
HEADACHE Dr Nick Pendleton September 2017 Headache Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache Raised ICP
Headache A Practical Approach
 Headache A Practical Approach Integrated Pain Symposium December 1, 2017 Alyssa Lettich. MD Neurosciences Institute/Neurosciences Clinical Program Medical Director Headache and Pain Development Teams Disclosures:
Headache A Practical Approach Integrated Pain Symposium December 1, 2017 Alyssa Lettich. MD Neurosciences Institute/Neurosciences Clinical Program Medical Director Headache and Pain Development Teams Disclosures:
Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE
 Headache in children and adolescents Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE Dept. of Psychiatry of Childhood and Adolescence Medical University of Vienna, Vienna, Austria Impact
Headache in children and adolescents Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE Dept. of Psychiatry of Childhood and Adolescence Medical University of Vienna, Vienna, Austria Impact
Clinical Learning Days November 10, 2017
 Migraine Clinical Learning Days November 10, 2017 Alyssa Lettich. MD Neurosciences Institute/Neurosciences Clinical Program Medical Director Headache Disclosures: none Learning Objectives: At the conclusion
Migraine Clinical Learning Days November 10, 2017 Alyssa Lettich. MD Neurosciences Institute/Neurosciences Clinical Program Medical Director Headache Disclosures: none Learning Objectives: At the conclusion
Current Migraine Treatment Therapy. Daniel Kassicieh, DO, FAAN
 Current Migraine Treatment Therapy Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraines are a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality
Current Migraine Treatment Therapy Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraines are a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality
25/09/2018 HEADACHE. Dr Nick Pendleton
 HEADACHE Dr Nick Pendleton September 2018 1 Small Group Work Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache
HEADACHE Dr Nick Pendleton September 2018 1 Small Group Work Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache
Strategies in Migraine Care
 Strategies in Migraine Care Julie L. Roth, MD Rhode Island Hospital Assistant Professor, Neurology The Warren Alpert Medical School of Brown University March 28, 2015 Financial Disclosures None. Objectives
Strategies in Migraine Care Julie L. Roth, MD Rhode Island Hospital Assistant Professor, Neurology The Warren Alpert Medical School of Brown University March 28, 2015 Financial Disclosures None. Objectives
A case of a patient with chronic headache. Focus on Migraine. None related to the presentation Grants to conduct clinical trials from: Speaker bureau:
 Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Disclosures. Objectives 6/2/2017
 Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Faculty Disclosure. Karen L. Bremer, MD. Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest.
 Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation.
 I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
Case Presentation. Case Presentation. Case Presentation. Truths about Headaches (2017) Most headaches were muscle-tension headaches
 Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
HEADACHES THE RED FLAGS
 HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
Long-Term Care Updates
 Long-Term Care Updates September 2017 By Lindsay Slowiczek, PharmD Migraines are often considered to be a condition affecting younger or middle-aged patients, during which patients experience episodic,
Long-Term Care Updates September 2017 By Lindsay Slowiczek, PharmD Migraines are often considered to be a condition affecting younger or middle-aged patients, during which patients experience episodic,
Headache Questionnaire
 Date: All Headache Patients We would appreciate your cooperation in filling out this form. In our evaluation of headache, your history is typically our most valuable tool for diagnosis and subsequent treatment.
Date: All Headache Patients We would appreciate your cooperation in filling out this form. In our evaluation of headache, your history is typically our most valuable tool for diagnosis and subsequent treatment.
Migraine. What are the symptoms of a migraine attack?
 Migraine Migraine causes attacks of headaches, often with feeling sick or vomiting. Treatment options include: avoiding possible 'triggers', painkillers, antiinflammatory painkillers, anti-sickness medicines,
Migraine Migraine causes attacks of headaches, often with feeling sick or vomiting. Treatment options include: avoiding possible 'triggers', painkillers, antiinflammatory painkillers, anti-sickness medicines,
Neuralgias tend to be sudden, brief, intermittent severe, stabbing or lightning pains or electric shock sensations.
 Neuralgia is the term used to describe pain arising from a nerve. There are many different neuralgias which have been described in the medical literature, but I will only touch upon a few more common ones.
Neuralgia is the term used to describe pain arising from a nerve. There are many different neuralgias which have been described in the medical literature, but I will only touch upon a few more common ones.
10/13/17. Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD
 Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD } Depomed Consultant 2014 to present } Avanir Consultant 2014 to present } Amgen
Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD } Depomed Consultant 2014 to present } Avanir Consultant 2014 to present } Amgen
Regulatory Status FDA approved indication: Migranal Nasal Spray is indicated for the acute treatment of migraine headaches with or without aura (1).
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.60 Subject: Migranal Nasal Spray Page: 1 of 5 Last Review Date: November 30, 2018 Migranal Nasal Spray
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.60 Subject: Migranal Nasal Spray Page: 1 of 5 Last Review Date: November 30, 2018 Migranal Nasal Spray
Headache and Facial Pain. Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology
 Headache and Facial Pain Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology Introduction It is the most common neurologic complain The diagnosis usually
Headache and Facial Pain Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology Introduction It is the most common neurologic complain The diagnosis usually
Clinical case. Clinical case 3/15/2018 OVERVIEW. Refractory headaches and update on novel treatment. Refractory headache.
 OVERVIEW Refractory headaches and update on novel treatment Definition of refractory headache Treatment approach Medications Neuromodulation In the pipeline Juliette Preston, MD OHSU Headache Center Refractory
OVERVIEW Refractory headaches and update on novel treatment Definition of refractory headache Treatment approach Medications Neuromodulation In the pipeline Juliette Preston, MD OHSU Headache Center Refractory
Chronic Daily Headaches
 Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Faculty Disclosures. Learning Objectives. Acute Treatment Strategies
 WWW.AMERICANHEADACHESOCIETY.ORG Acute Treatment Strategies Content developed by: Lawrence C. Newman, MD, FAHS Donna Gutterman, PharmD Faculty Disclosures LAWRENCE C. NEWMAN, MD, FAHS Dr. Newman has received
WWW.AMERICANHEADACHESOCIETY.ORG Acute Treatment Strategies Content developed by: Lawrence C. Newman, MD, FAHS Donna Gutterman, PharmD Faculty Disclosures LAWRENCE C. NEWMAN, MD, FAHS Dr. Newman has received
SUMAVEL DOSEPRO (sumatriptan succinate) solution for injection
 SUMAVEL DOSEPRO (sumatriptan succinate) solution for injection Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit
SUMAVEL DOSEPRO (sumatriptan succinate) solution for injection Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา
 ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
Controlling Migraine Pain
 Migraine Stats Controlling Migraine Pain Alan Zacharias, M.D. Associated Neurologists, Boulder Community Health 303-622-3365 Women 15% Men 5% Usually starts in 2 nd and 3 rd Decade Major Impact on days
Migraine Stats Controlling Migraine Pain Alan Zacharias, M.D. Associated Neurologists, Boulder Community Health 303-622-3365 Women 15% Men 5% Usually starts in 2 nd and 3 rd Decade Major Impact on days
Core Safety Profile. Pharmaceutical form(s)/strength: Tablets and Oral lyophilisates (wafers) 5 and 10 mg NL/H/PSUR/0002/001 Date of FAR:
 Core Safety Profile Active substance: Rizatriptan Pharmaceutical form(s)/strength: Tablets and Oral lyophilisates (wafers) 5 and 10 mg P RMS: NL/H/PSUR/0002/001 Date of FAR: 23.05.2011 4.3 Contraindications
Core Safety Profile Active substance: Rizatriptan Pharmaceutical form(s)/strength: Tablets and Oral lyophilisates (wafers) 5 and 10 mg P RMS: NL/H/PSUR/0002/001 Date of FAR: 23.05.2011 4.3 Contraindications
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centers: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Medication For Migraine Chart: Table 1: Acute Treatment when the attack begins
 Medication For Migraine Chart: Table 1: Acute Treatment when the attack begins Page a Analgesics (painkillers) Non-steroidal antiinflammatory drugs (NSAIDs) Prescription required Brand Name Formulation
Medication For Migraine Chart: Table 1: Acute Treatment when the attack begins Page a Analgesics (painkillers) Non-steroidal antiinflammatory drugs (NSAIDs) Prescription required Brand Name Formulation
Prevention and Treatment of Migraines CAITLIN BARNES, PHARM.D. CANDIDATE AMBULATORY CARE JOE CAMMILLERI, PHARM.D. NATOHYA MALLORY, PHARM.D.
 Prevention and Treatment of Migraines CAITLIN BARNES, PHARM.D. CANDIDATE AMBULATORY CARE JOE CAMMILLERI, PHARM.D. NATOHYA MALLORY, PHARM.D. Objectives Present patient case Review epidemiology/pathophysiology
Prevention and Treatment of Migraines CAITLIN BARNES, PHARM.D. CANDIDATE AMBULATORY CARE JOE CAMMILLERI, PHARM.D. NATOHYA MALLORY, PHARM.D. Objectives Present patient case Review epidemiology/pathophysiology
Do you suffer from Headaches? - November/Dec 2011
 Do you suffer from Headaches? - November/Dec 2011 Inside this month's issue Headaches Acute single headaches Recurring Headaches: Migraine What causes Migraine? Treatments for migraine & prevention Headaches
Do you suffer from Headaches? - November/Dec 2011 Inside this month's issue Headaches Acute single headaches Recurring Headaches: Migraine What causes Migraine? Treatments for migraine & prevention Headaches
Headache Assessment In Primary Eye Care
 Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
PAEDIATRIC ACUTE CARE GUIDELINE. Headache. This document should be read in conjunction with this DISCLAIMER
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Headaches. Mini Medical School. November 10, A. Laine Green MSc, MD FRCP(C) Assistant Professor Department of Medicine (Neurology)
 Headaches. Mini Medical School. November 10, 2016 A. Laine Green MSc, MD FRCP(C) Assistant Professor Department of Medicine (Neurology) Artist Agnes Cecile Disclosures I have received an honorarium from
Headaches. Mini Medical School. November 10, 2016 A. Laine Green MSc, MD FRCP(C) Assistant Professor Department of Medicine (Neurology) Artist Agnes Cecile Disclosures I have received an honorarium from
The recommended dose of Imigran Suppositories for the acute treatment of a migraine attack is one 25mg suppository administered rectally.
 1. NAME OF THE MEDICINAL PRODUCT Imigran 25 mg Suppository. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Imigran 25 mg Suppository: contains 25 mg sumatriptan For a full list of excipients, see section
1. NAME OF THE MEDICINAL PRODUCT Imigran 25 mg Suppository. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Imigran 25 mg Suppository: contains 25 mg sumatriptan For a full list of excipients, see section
Dubai Standards of Care (Migraine)
 Dubai Standards of Care 2018 (Migraine) Preface Migraine is one of the most common problem dealt with in daily practice. In Dubai, the management of migraine is done through various different strategies.
Dubai Standards of Care 2018 (Migraine) Preface Migraine is one of the most common problem dealt with in daily practice. In Dubai, the management of migraine is done through various different strategies.
Jessica Ailani MD FAHS Director, Georgetown Headache Center Associate Professor Neurology Medstar Georgetown University Hospital
 Jessica Ailani MD FAHS Director, Georgetown Headache Center Associate Professor Neurology Medstar Georgetown University Hospital Honorarium from Current Pain and Headache Reports; Section Editor Unusual
Jessica Ailani MD FAHS Director, Georgetown Headache Center Associate Professor Neurology Medstar Georgetown University Hospital Honorarium from Current Pain and Headache Reports; Section Editor Unusual
WHY IS MIGRAINE IMPORTANT
 WHY IS MIGRAINE IMPORTANT Migraine is a complex disorder characterized by recurrent episodes of headache, most often unilateral and in some cases associated with visual or sensory symptoms collectively
WHY IS MIGRAINE IMPORTANT Migraine is a complex disorder characterized by recurrent episodes of headache, most often unilateral and in some cases associated with visual or sensory symptoms collectively
Goals. Primary Headache Syndromes. One-Year Prevalence of Common Headache Disorders
 Goals One-Year Prevalence of Common Headache Disorders Impact of primary headache syndromes Non pharmacologic Rx of migraine individualized to patient triggers Complementary and alternative Rx of migraine
Goals One-Year Prevalence of Common Headache Disorders Impact of primary headache syndromes Non pharmacologic Rx of migraine individualized to patient triggers Complementary and alternative Rx of migraine
Vestibular Migraine. Information for patients and carers. Department of Neurology and Otolaryngology Aberdeen Royal Infirmary
 Vestibular Migraine Information for patients and carers Department of Neurology and Otolaryngology Aberdeen Royal Infirmary What is vestibular migraine? Migraine is a disabling headache disorder that affects
Vestibular Migraine Information for patients and carers Department of Neurology and Otolaryngology Aberdeen Royal Infirmary What is vestibular migraine? Migraine is a disabling headache disorder that affects
...SELECTED ABSTRACTS...
 The following abstracts, from medical journals containing literature on migraine management, were selected for their relevance to this Special Report supplement. Two Sumatriptan Studies Two double-blind
The following abstracts, from medical journals containing literature on migraine management, were selected for their relevance to this Special Report supplement. Two Sumatriptan Studies Two double-blind
10/31/2017 PRIMARY CARE AND HEADACHE DISCLOSURES WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Primary Care 67%
 PRIMARY CARE AND HEADACHE Sonja Potrebic MD PhD Regional Headache Specialist Kaiser LAMC 1 WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Column1 Primary Care 67% Primary Care Headache Specialty Other
PRIMARY CARE AND HEADACHE Sonja Potrebic MD PhD Regional Headache Specialist Kaiser LAMC 1 WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Column1 Primary Care 67% Primary Care Headache Specialty Other
Transcutaneous stimulation of the cervical branch of the vagus nerve for cluster headache and migraine
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Transcutaneous stimulation of the cervical branch of the vagus nerve for cluster headache and migraine Cluster
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Transcutaneous stimulation of the cervical branch of the vagus nerve for cluster headache and migraine Cluster
Outpatient Headache Care Guideline
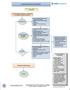 1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
Adult with headache. Problem-specific video guides to diagnosing patients and helping them with management and prevention
 Adult with headache Problem-specific video guides to diagnosing patients and helping them with management and prevention London Strategic Clinical Networks London Neuroscience Strategic Clinical Network
Adult with headache Problem-specific video guides to diagnosing patients and helping them with management and prevention London Strategic Clinical Networks London Neuroscience Strategic Clinical Network
Headache Mary D. Hughes, MD Neuroscience Associates
 Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
Migranal Nasal Spray. Migranal Nasal Spray (dihydroergotamine) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.60 Subject: Migranal Nasal Spray Page: 1 of 5 Last Review Date: June 22, 2017 Migranal Nasal Spray
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.60 Subject: Migranal Nasal Spray Page: 1 of 5 Last Review Date: June 22, 2017 Migranal Nasal Spray
Adult & Pediatric Patients. Stanford Health Care, Division Pain Medicine
 Acute Treatment Strategies in Adult & Pediatric Patients Theresa Mallick Searle, MS, RN BC, ANP BC Disclosures Speakers Bureau: Allergan, Depomed Acute Treatment Strategies in Adult & Pediatric Patients
Acute Treatment Strategies in Adult & Pediatric Patients Theresa Mallick Searle, MS, RN BC, ANP BC Disclosures Speakers Bureau: Allergan, Depomed Acute Treatment Strategies in Adult & Pediatric Patients
Sumatriptan Tablets, Nasal Spray (Imitrex), Nasal Powder (Onzetra Xsail), sumatriptan and naproxen sodium (Treximet tablets)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 0 Subject: Sumatriptan Page: 1 of 6 Last Review Date: November 30, 2018 Sumatriptan Description Sumatriptan
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 0 Subject: Sumatriptan Page: 1 of 6 Last Review Date: November 30, 2018 Sumatriptan Description Sumatriptan
Migraine Migraine Age Specific Prevalence in the United States. Headache International Headache Society Classification
 28 Primary Care Medicine Principles and Practice 29 October 28 Professor Peter J. Goadsby Peter.Goadsby@headache.ucsf.edu Department of Neurology Headache International Headache Society Classification
28 Primary Care Medicine Principles and Practice 29 October 28 Professor Peter J. Goadsby Peter.Goadsby@headache.ucsf.edu Department of Neurology Headache International Headache Society Classification
Chronic Migraine in Primary Care. December 11 th, 2017 Werner J. Becker University of Calgary
 Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
OH, MY ACHING HEAD! I HAVE NO DISCLOSURES OR CONFLICTS OF INTERESTS TO DECLARE MANAGING HEADACHE IN THE OUTPATIENT SETTING SECONDARY HEADACHES
 1 JUSTIN A. OSSMAN, MD CHATTANOOGA FAMILY MEDICINE UPDATE OH, MY ACHING HEAD! MANAGING HEADACHE IN THE OUTPATIENT SETTING 2 I HAVE NO DISCLOSURES OR CONFLICTS OF INTERESTS TO DECLARE OBJECTIVES International
1 JUSTIN A. OSSMAN, MD CHATTANOOGA FAMILY MEDICINE UPDATE OH, MY ACHING HEAD! MANAGING HEADACHE IN THE OUTPATIENT SETTING 2 I HAVE NO DISCLOSURES OR CONFLICTS OF INTERESTS TO DECLARE OBJECTIVES International
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Treatment Of Medication. Overuse Headache
 7 November 2012 BASH GPwSI Meeting Lecture title... Treatment Of Medication Dr... Overuse Headache Dr Marcus Lewis Dr... The National Migraine Centre International Headache Society Diagnostic criteria
7 November 2012 BASH GPwSI Meeting Lecture title... Treatment Of Medication Dr... Overuse Headache Dr Marcus Lewis Dr... The National Migraine Centre International Headache Society Diagnostic criteria
The best defense is a good offense. Optimizing the Acute Treatment of Migraine. Disclosures 11/10/2017
 Optimizing the Acute Treatment of Migraine Brian M. Plato, DO, FAHS Norton Neuroscience Institute Louisville, KY Disclosures Speakers Bureau (personal): Allergan, Depomed, Avanir Research Funding (paid
Optimizing the Acute Treatment of Migraine Brian M. Plato, DO, FAHS Norton Neuroscience Institute Louisville, KY Disclosures Speakers Bureau (personal): Allergan, Depomed, Avanir Research Funding (paid
Headache is the most common symptom in patients with Idiopathic Intracranial Hypertension (IIH). Not everybody with IIH gets headache.
 Headaches in Idiopathic Intracranial Hypertension Headache is the most common symptom in patients with Idiopathic Intracranial Hypertension (). Not everybody with gets headache. Headaches can be there
Headaches in Idiopathic Intracranial Hypertension Headache is the most common symptom in patients with Idiopathic Intracranial Hypertension (). Not everybody with gets headache. Headaches can be there
TABLE 1. Current Diagnostic Criteria for Migraine Without Aura 2 A. At least 5 attacks fulfilling criteria B-D B. Headache attacks lasting 4-72 hours
 ANSWERS CONCISE TO FREQUENTLY REVIEW ASKED QUESTIONS FOR CLINICIANS ABOUT MIGRAINE Answers to Frequently Asked Questions About Migraine IVAN GARZA, MD, AND JERRY W. SWANSON, MD Migraine is a common primary
ANSWERS CONCISE TO FREQUENTLY REVIEW ASKED QUESTIONS FOR CLINICIANS ABOUT MIGRAINE Answers to Frequently Asked Questions About Migraine IVAN GARZA, MD, AND JERRY W. SWANSON, MD Migraine is a common primary
July 2012 Target Population. Adult patients 18 years or older in primary care settings.
 Guideline for Primary Care Management of Headache in Adults July 2012 Target Population Adult patients 18 years or older in primary care settings. Exclusions: This guideline does not provide recommendations
Guideline for Primary Care Management of Headache in Adults July 2012 Target Population Adult patients 18 years or older in primary care settings. Exclusions: This guideline does not provide recommendations
HEADACHE. Summary of British Association on the Study of Headaches {click to visit}
 F:M=3:1 Affects 15% adults HEADACHE Summary of British Association on the Study of Headaches {click to visit} Primary: Migraine (with aura 1/3, without aura 2/3) Tension Cluster Other Secondary Neuralgia
F:M=3:1 Affects 15% adults HEADACHE Summary of British Association on the Study of Headaches {click to visit} Primary: Migraine (with aura 1/3, without aura 2/3) Tension Cluster Other Secondary Neuralgia
OCTOBER 7-10 PHILADELPHIA, PENNSYLVANIA
 OMED 17 OCTOBER 7-10 PHILADELPHIA, PENNSYLVANIA 29.5 Category 1-A CME credits anticipated ACOFP / AOA s 122 nd Annual Osteopathic Medical Conference & Exposition Joint Session with ACOFP, ACONP and AOAAM:
OMED 17 OCTOBER 7-10 PHILADELPHIA, PENNSYLVANIA 29.5 Category 1-A CME credits anticipated ACOFP / AOA s 122 nd Annual Osteopathic Medical Conference & Exposition Joint Session with ACOFP, ACONP and AOAAM:
Recognition and treatment of medication overuse headache
 Recognition and treatment of medication overuse headache Marcus Lewis MA, MRCGP, DRCOG, DFSRH 20 Mean weekly headache index 15 10 5 Medication overuse headache is a common condition responsible for a high
Recognition and treatment of medication overuse headache Marcus Lewis MA, MRCGP, DRCOG, DFSRH 20 Mean weekly headache index 15 10 5 Medication overuse headache is a common condition responsible for a high
UNDERSTANDING CHRONIC MIGRAINE. Learn about diagnosis, management, and treatment options for this headache condition
 UNDERSTANDING CHRONIC MIGRAINE Learn about diagnosis, management, and treatment options for this headache condition 1 What We re Going to Cover Today The symptoms and phases of migraine Differences between
UNDERSTANDING CHRONIC MIGRAINE Learn about diagnosis, management, and treatment options for this headache condition 1 What We re Going to Cover Today The symptoms and phases of migraine Differences between
Migrainous headache, the menstrual cycle and pregnancy. Dr Manuela Fontebasso Headache Specialist, Author and Headache Education Facilitator
 Migrainous headache, the menstrual cycle and pregnancy Dr Manuela Fontebasso Headache Specialist, Author and Headache Education Facilitator What sort of headaches? Migraine with and without aura Tension
Migrainous headache, the menstrual cycle and pregnancy Dr Manuela Fontebasso Headache Specialist, Author and Headache Education Facilitator What sort of headaches? Migraine with and without aura Tension
What You Should Know About Your HEADACHE. Learn more about headache types, triggers, and treatments, when to get help, and how to help yourself
 What You Should Know About Your HEADACHE Learn more about headache types, triggers, and treatments, when to get help, and how to help yourself Introduction The purpose of this brochure is to give you a
What You Should Know About Your HEADACHE Learn more about headache types, triggers, and treatments, when to get help, and how to help yourself Introduction The purpose of this brochure is to give you a
Sumatran Relief 50mg Tablets. Pharmacist General Migraine Information. Table of content
 Sumatran Relief 50mg Tablets Pharmacist General Migraine Information Table of content 1. Introduction 2. Sumatran Relief indication 3. Mechanism of action 4. Supply criteria 5. Migraine: Description, symptoms,
Sumatran Relief 50mg Tablets Pharmacist General Migraine Information Table of content 1. Introduction 2. Sumatran Relief indication 3. Mechanism of action 4. Supply criteria 5. Migraine: Description, symptoms,
Preventive treatment of migraine. Rebecca Burch, MD Brigham and Women s Faulkner Hospital Harvard Medical School Boston, MA
 Preventive treatment of migraine Rebecca Burch, MD Brigham and Women s Faulkner Hospital Harvard Medical School Boston, MA No disclosures Disclosures Many preventive treatments for migraine are not FDA-approved
Preventive treatment of migraine Rebecca Burch, MD Brigham and Women s Faulkner Hospital Harvard Medical School Boston, MA No disclosures Disclosures Many preventive treatments for migraine are not FDA-approved
Migraine. A booklet for people with migraine and their carers. Consultation. Consultation. draft. draft. Scottish guidelines
 Migraine Scottish guidelines A booklet for people with migraine and their carers Cover image courtesy of Migraine Action (migraineart.org.uk) Patient quotes kindly supplied by The Migraine Trust Scottish
Migraine Scottish guidelines A booklet for people with migraine and their carers Cover image courtesy of Migraine Action (migraineart.org.uk) Patient quotes kindly supplied by The Migraine Trust Scottish
NARAMIG QUALITATIVE AND QUANTITATIVE COMPOSITION
 NARAMIG Naratriptan QUALITATIVE AND QUANTITATIVE COMPOSITION Tablets containing 2.5 mg of naratriptan as naratriptan hydrochloride. PHARMACEUTICAL FORM Film coated tablets. CLINICAL PARTICULARS Indications
NARAMIG Naratriptan QUALITATIVE AND QUANTITATIVE COMPOSITION Tablets containing 2.5 mg of naratriptan as naratriptan hydrochloride. PHARMACEUTICAL FORM Film coated tablets. CLINICAL PARTICULARS Indications
Painless, progressive weakness Could this be Motor Neurone Disease?
 APPENDIX 1 Painless, progressive weakness Could this be Motor Neurone Disease? 1. Does the patient have one or more of these? Bulbar features Limb features Respiratory features Cognitive features (rare)
APPENDIX 1 Painless, progressive weakness Could this be Motor Neurone Disease? 1. Does the patient have one or more of these? Bulbar features Limb features Respiratory features Cognitive features (rare)
