231 Diseases of the Aorta
|
|
|
- Samson Hampton
- 6 years ago
- Views:
Transcription
1 Página 1 de Diseases of the Aorta Victor J. Dzau Mark A. Creager The aorta is the conduit through which the blood ejected from the left ventricle is delivered to the systemic arterial bed. In adults, its diameter is approximately 3 cm at the origin, 2.5 cm in the descending portion in the thorax, and 1.8 to 2 cm in the abdomen. The aortic wall consists of a thin intima composed of endothelium, subendothelial connective tissue, and an internal elastic lamina; a thick tunica media composed of smooth-muscle cells and extracellular matrix; and an adventitia composed primarily of connective tissue enclosing the vasa vasorum and nervi vascularis. In addition to its conduit function, the viscoelastic and compliant properties of the aorta also subserve a buffering function. The aorta is distended during systole to enable a portion of the stroke volume to be stored, and it recoils during diastole so that blood continues to flow to the periphery. Because of its continuous exposure to high pulsatile pressure and shear stress, the aorta is particularly prone to injury and disease resulting from mechanical trauma (Table 231-1). The aorta is also more prone to rupture than any other vessel, especially with the development of aneurysmal dilatation, since its wall tension, as governed by Laplace's law (i.e., proportional to the product of pressure and radius), would be increased. TABLE Diseases of the Aorta: Etiology and Associated Factors Aortic aneurysm Atherosclerosis Cystic medial necrosis Tuberculosis Syphilitic infection Mycotic infection Rheumatic aortitis
2 Página 2 de 13 Trauma Aortic dissection Cystic medial necrosis Systemic hypertension Atherosclerosis Takayasu's arteritis Giant cell arteritis Aortic occlusion Atherosclerosis Thromboembolism Aortitis Syphilitic aortitis Rheumatic aortitis Takayasu's arteritis Giant cell arteritis AORTIC ANEURYSM An aneurysm is defined as a pathologic dilatation of a segment of a blood vessel. A true aneurysm involves all three layers of the vessel wall and is distinguished from a pseudoaneurysm, in which the intimal and medial layers are disrupted and the dilatation is
3 Página 3 de 13 lined by adventitia only and sometimes by perivascular clot. Aneurysms may also be classified according to their gross appearance. A fusiform aneurysm affects the entire circumference of a segment of the vessel, resulting in a diffusely dilated lesion. In contrast, a saccular aneurysm involves only a portion of the circumference, resulting in an outpouching of the vessel wall. Aortic aneurysms are also classified according to location, i.e., abdominal versus thoracic. Aneurysms of the descending thoracic aorta are usually contiguous with infradiaphragmatic aneurysms and are referred to as thoracoabdominal aortic aneurysms. ETIOLOGY The most common pathologic condition associated with aortic aneurysm is atherosclerosis. It is controversial whether atherosclerosis itself actually causes aortic aneurysms or whether atherosclerosis develops as a secondary event in the dilated aorta. Causality is implied by studies that have shown that many patients with aortic aneurysms have coexisting risk factors for atherosclerosis (Chap. 224), particularly cigarette smoking, as well as atherosclerosis in other blood vessels. Seventy-five percent of atherosclerotic aneurysms are located in the distal abdominal aorta, below the renal arteries. Cystic medial necrosis is the term used to describe the degeneration of collagen and elastic fibers in the tunica media of the aorta, as well as the loss of medial cells that are replaced by multiple clefts of mucoid material. Cystic medial necrosis characteristically affects the proximal aorta, results in circumferential weakness and dilatation, and leads to development of fusiform aneurysms involving the ascending aorta and the sinuses of Valsalva. This condition is particularly prevalent in patients with Marfan syndrome and Ehlers-Danlos syndrome type IV (Chap. 342) but also occurs in pregnant women, in patients with hypertension, and in those with valvular heart disease. Sometimes it appears as an isolated condition in patients without any other apparent disease. Familial clusterings of aortic aneurysms occur in 20% of patients, suggesting a hereditary basis of the disease. Mutations of the genes encoding fibrillin-1 and type III procollagen have been implicated in some cases. Linkage analysis has identified loci on chromosomes 5q13-14 and 11q23.3- q24 in several families, although the specific culprit genes have not been described. Syphilis (Chap. 153) is a relatively uncommon cause of aortic aneurysm. Syphilitic periaortitis and mesoaortitis damage elastic fibers, resulting in thickening and weakening of the aortic wall. Approximately 90% of syphilitic aneurysms are located in the ascending aorta or aortic arch. Tuberculous aneurysms (Chap. 150) typically affect the thoracic aorta and result from direct extension of infection from hilar lymph nodes or contiguous abscesses or from bacterial seeding. Loss of aortic wall elasticity results from granulomatous destruction of the medial layer. A mycotic aneurysm is a rare condition that develops as a result of staphylococcal, streptococcal, or salmonella infections of the aorta, usually at an atherosclerotic plaque. These aneurysms are usually saccular. Blood cultures are often positive and reveal the nature of the infecting agent. Vasculitides associated with aortic aneurysm include Takayasu's arteritis and giant cell arteritis, which may cause aneurysms of the aortic arch and descending thoracic aorta. Spondyloarthropathies such as ankylosing spondylitis, rheumatoid arthritis, psoriatic arthritis, relapsing polychondritis and Reiter's syndrome are associated with dilatation of
4 Página 4 de 13 the ascending aorta. Behçet's disease (Chap. 307) causes thoracic and abdominal aortic aneurysms. Traumatic aneurysms may develop after penetrating or nonpenetrating chest trauma and most commonly affect the descending thoracic aorta just beyond the site of insertion of the ligamentum arteriosum. Congenital aortic aneurysms may be primary or associated with anomalies such as a bicuspid aortic valve or aortic coarctation. THORACIC AORTIC ANEURYSMS The clinical manifestations and natural history of thoracic aortic aneurysms depend on their location. Cystic medial necrosis is the most common cause of ascending aortic aneurysms, whereas atherosclerosis is the condition most frequently associated with aneurysms of the aortic arch and descending thoracic aorta. The average growth rate of thoracic aneurysms is 0.1 to 0.4 cm per year. The risk of rupture is related to the size of the aneurysm and the presence of symptoms; it increases substantially for ascending aortic aneurysms >6 cm and descending thoracic aneurysms >7 cm. Most thoracic aortic aneurysms are asymptomatic. However, compression or erosion of adjacent tissue by aneurysms may cause symptoms such as chest pain, shortness of breath, cough, hoarseness, or dysphagia. Aneurysmal dilatation of the ascending aorta may cause congestive heart failure as a consequence of aortic regurgitation; and compression of the superior vena cava may produce congestion of the head, neck, and upper extremities. P.1482 A chest x-ray may be the first test to suggest the diagnosis of a thoracic aortic aneurysm (Fig ). Findings include widening of the mediastinal shadow and displacement or compression of the trachea or left mainstem bronchus. Two-dimensional echocardiography, and particularly transesophageal echocardiography, can be used to assess the proximal ascending aorta and descending thoracic aorta. Both contrast-enhanced computed tomography (CT) and magnetic resonance imaging (MRI) are sensitive and specific tests for assessment of aneurysms of the thoracic aorta. In asymptomatic patients whose aneurysms are too small to justify surgery, noninvasive testing with either contrast-enhanced CT or MRI should be performed at least every 6 to 12 months to monitor expansion. Contrast aortography is frequently required preoperatively to assess the length of the aneurysm and involvement of branch vessels (Fig ). FIGURE A chest x-ray of a patient with a thoracic aortic aneurysm. FIGURE An aortogram demonstrating a large fusiform aneurysm of the descending thoracic aorta. Patients with thoracic aortic aneurysms, and particularly patients with Marfan syndrome who have evidence of aortic root dilatation, should receive long-term beta-blocker therapy. Additional medical therapy should be given, as necessary, to control hypertension.
5 Página 5 de 13 Operative repair with placement of a prosthetic graft is indicated in patients with symptomatic thoracic aortic aneurysms, and in those in whom the aortic diameter is >6 cm or has increased by >1 cm per year. In patients with Marfan syndrome, thoracic aortic aneurysms >5 cm should be considered for surgery. ABDOMINAL AORTIC ANEURYSMS Abdominal aortic aneurysms occur more frequently in males than in females, and the incidence increases with age. Abdominal aortic aneurysms may affect 1 to 2% of men older than 50 years. At least 90% of all abdominal aortic aneurysms >4.0 cm are affected by atherosclerosis, and most of these aneurysms are below the level of the renal arteries. Prognosis is related to both the size of the aneurysm and the severity of coexisting coronary artery and cerebrovascular disease. The risk of rupture increases with the size of the aneurysm. The 5-year risk of rupture for aneurysms <5 cm is 1 to 2%, whereas it is 20 to 40% for aneurysms >5 cm in diameter. The formation of mural thrombi within the aneurysm may predispose to peripheral embolization. An abdominal aortic aneurysm commonly produces no symptoms. It is usually detected on routine examination as a palpable, pulsatile, and nontender mass, or it is an incidental finding during an abdominal x-ray or ultrasound performed for other reasons. However, as abdominal aortic aneurysms expand, they may become painful. Some patients complain of strong pulsations in the abdomen; others experience pain in the chest, lower back, or scrotum. Aneurysmal pain is usually a harbinger of rupture and represents a medical emergency. More often, acute rupture occurs without any prior warning, and this complication is always life-threatening. Rarely, there is leakage of the aneurysm with severe pain and tenderness. Acute pain and hypotension occur with rupture of the aneurysm, which requires emergency operation. Abdominal radiography may demonstrate the calcified outline of the aneurysm. However, about 25% of aneurysms are not calcified and cannot be visualized by plain x-ray. An abdominal ultrasound can delineate the transverse and longitudinal dimensions of an abdominal aortic aneurysm and may detect mural thrombus. Abdominal ultrasound is useful for serial documentation of aneurysm size and can be used to screen patients at risk for developing aortic aneurysm, such as those with affected siblings, peripheral atherosclerosis, or peripheral artery aneurysms. In one larger study, ultrasound screening of men aged 65 to 74 years was associated with a risk reduction in aneurysm-related death by 42%. CT with contrast and MRI are accurate, noninvasive tests to determine the location and size of abdominal aortic aneurysms (Fig ). Contrast aortography is used for the evaluation of patients with aneurysms before surgery, but the procedure carries a small risk of complications, such as bleeding, allergic reactions, and atheroembolism. This technique is useful in documenting the length of the aneurysm, especially its upper and lower limits, and the extent of associated atherosclerotic vascular disease. However, since the presence of mural clots may reduce the luminal size, aortography may underestimate the diameter of an aneurysm. FIGURE A computed tomographic angiogram (CTA) depicting a fusiform abdominal aortic
6 Página 6 de 13 aneurysm that has been treated with a bifurcated stent graft. P.1483 TREATMENT Operative repair of the aneurysm and insertion of a prosthetic graft is indicated for abdominal aortic aneurysms of any size that are expanding rapidly or are associated with symptoms. For asymptomatic aneurysms, operation is indicated if the diameter is >5.5 cm. Operation may be recommended in patients with aneurysm diameters of 4 to 5 cm, except for patients with exceptionally high operative risk. However, in recent randomized trials of patients with abdominal aortic aneurysms <5.5 cm, there was no difference in the long-term (5- to 8-year) mortality rate between those followed with ultrasound surveillance and those undergoing elective aneurysm repair. Thus, serial noninvasive follow-up of smaller aneurysms (<5 cm) is an alternative to immediate surgery. Percutaneous placement of endovascular stent grafts (Fig ) for treatment of infrarenal abdominal aortic aneurysms is currently available for selected patients, and initial reports have been favorable. In surgical candidates, careful preoperative cardiac and general medical evaluations (followed by appropriate therapy of complicating conditions) are essential. Preexisting coronary artery disease, congestive heart failure, pulmonary disease, diabetes, and advanced age add to the risk of surgery. Perioperative management should include the placement of a Swan-Ganz catheter and arterial line to monitor and optimize left ventricular filling pressure, cardiac output, and arterial pressure, especially during clamping and unclamping of the aorta, as well as during the immediate postoperative period. With careful preoperative cardiac evaluation and postoperative care, the operative mortality rate approximates 1 to 2%. After acute rupture, the mortality rate of emergent operation generally exceeds 50%. AORTIC DISSECTION Aortic dissection is caused by a circumferential or, less frequently, transverse tear of the intima. It often occurs along the right lateral wall of the ascending aorta where the hydraulic shear stress is high. Another common site is the descending thoracic aorta just below the ligamentum arteriosum. The initiating event is either a primary intimal tear with secondary dissection into the media or a medial hemorrhage that dissects into and disrupts the intima. The pulsatile aortic flow then dissects along the elastic lamellar plates of the aorta and creates a false lumen. The dissection usually propagates distally down the descending aorta and into its major branches, but it may also propagate proximally. In some cases, a secondary distal intimal disruption occurs, resulting in the reentry of blood from the false to the true lumen. There are at least two important pathologic and radiologic variants: intramural hematoma
7 Página 7 de 13 without an intimal flap and penetrating atherosclerotic ulcer. The clinical picture and therapeutic management of intramural hematoma are similar to those for classic aortic dissection. By contrast, penetrating ulcers are usually localized and are not associated with extensive propagation. They are primarily found in the mid and distal portions of the descending thoracic aorta and are associated with extensive atherosclerotic disease. The ulcer can erode beyond the intimal border, leading to medial hematoma, and may progress to false aneurysm formation or rupture. DeBakey and coworkers initially classified aortic dissections as type I, in which an intimal tear occurs in the ascending aorta but which involves the descending aorta as well; type II, in which the dissection is limited to the ascending aorta; and type III, in which the intimal tear is located in the descending area with distal propagation of the dissection (Fig ). Another classification (Stanford) is that of type A, in which the dissection involves the ascending aorta (proximal dissection), and type B, in which it is limited to the descending aorta (distal dissection). From a management standpoint, classification into type A or B is more practical and useful, since DeBakey types I and II are managed in a similar manner. FIGURE Classification of aortic dissections. Stanford classification: Type A dissections (top panels) involve the ascending aorta independent of site of tear and distal extension; type B dissections (bottom panels) involve transverse and/or descending aorta without involvement of the ascending aorta. DeBakey classification: Type I dissection involves ascending to descending aorta (top left); type II dissection is limited to ascending or transverse aorta, without descending aorta (top center + top right); type III dissection involves descending aorta only (bottom left). [From DC Miller, in RM Doroghazi, EE Slater (eds): Aortic Dissection. New York, McGraw-Hill, 1983, with permission.] The factors that predispose to aortic dissection include systemic hypertension, a coexisting condition in 70% of patients, and cystic medial necrosis. Aortic dissection is the major cause of morbidity and mortality in patients with Marfan syndrome (Chap. 342) and similarly may affect patients with Ehlers-Danlos syndrome. The incidence is also increased in patients with inflammatory aortitis (i.e., Takayasu's arteritis, giant cell arteritis), congenital aortic valve anomalies (e.g., bicuspid valve), in those with coarctation of the aorta, and in otherwise normal women during the third trimester of pregnancy. P.1484 CLINICAL MANIFESTATIONS The peak incidence is in the sixth and seventh decades. Men are more affected than women by a ratio of 2:1. The presentations of aortic dissection and its variants are the consequences of intimal tear, dissecting hematoma, occlusion of involved arteries, and compression of adjacent tissues. Acute aortic dissection presents with the sudden onset of pain (Chap. 12), which is often described as very severe and tearing and is associated with diaphoresis. The pain may be localized to the front or back of the chest, often the interscapular region, and typically migrates with propagation of the dissection. Other symptoms include syncope, dyspnea, and weakness. Physical findings may include hypertension or hypotension, loss of pulses, aortic regurgitation, pulmonary edema, and neurologic findings due to carotid artery obstruction (hemiplegia, hemianesthesia) or spinal
8 Página 8 de 13 cord ischemia (paraplegia). Bowel ischemia, hematuria, and myocardial ischemia have all been observed. These clinical manifestations reflect complications resulting from the dissection occluding the major arteries. Furthermore, clinical manifestations may result from the compression of adjacent structures (e.g., superior cervical ganglia, superior vena cava, bronchus, esophagus) by the expanding dissection causing aneurysmal dilatation, and include Horner's syndrome, superior vena caval syndrome, hoarseness, dysphagia, and airway compromise. Hemopericardium and cardiac tamponade may complicate a type A lesion with retrograde dissection. Acute aortic regurgitation is an important and common (>50%) complication of proximal dissection. It is the outcome of either a circumferential tear that widens the aortic root or a disruption of the annulus by dissecting hematoma that tears a leaflet(s) or displaces it below the line of closure. Signs of aortic regurgitation include bounding pulses, a wide pulse pressure, a diastolic murmur often radiating along the right sternal border, and evidence of congestive heart failure. The clinical manifestation depends on the severity of the regurgitation. In dissections involving the ascending aorta, the chest x-ray often reveals a widened superior mediastinum. A pleural effusion (usually left-sided) may also be present. This effusion is typically serosanguineous and not indicative of rupture unless accompanied by hypotension and falling hematocrit. In dissections of the descending thoracic aorta, a widened mediastinum may also be observed on chest x-ray. In addition, the descending aorta may appear to be wider than the ascending portion. An electrocardiogram that shows no evidence of myocardial ischemia is helpful in distinguishing aortic dissection from myocardial infarction. Rarely, the dissection involves the right or left coronary ostium and causes acute myocardial infarction. The diagnosis of aortic dissection can be established by aortography or by the use of noninvasive techniques such as echocardiography, CT, or MRI. Aortography may be used to document the diagnosis; to identify the entry point, the intimal flap, and the false and true lumina; and to establish the extent of dissection into the major arteries. Coronary angiography may be performed concomitantly in high-risk patients in the evaluation and preparation for surgery. The sensitivity of aortography is 70% for visualizing an intimal flap, 56% for the site of intimal tear, and 87% for false lumen. It is unable to recognize intramural hemorrhage. Transthoracic echocardiography can be performed simply and rapidly and has an overall sensitivity of 60 to 85%. For diagnosing proximal ascending aortic dissections, its sensitivity exceeds 80%; it is less useful for detecting dissection of the arch and descending thoracic aorta. Transesophageal echocardiography requires greater skill and patient cooperation but is very accurate in identifying dissections of the ascending and descending thoracic aorta, but not the arch, achieving 98% sensitivity and approximately 90% specificity. Echocardiography also provides important information regarding the presence and severity of aortic regurgitation and pericardial effusion. CT and MRI are both highly accurate in identifying the intimal flap and the extent of the dissection; each has a sensitivity and specificity >90%. They are useful in recognizing intramural hemorrhage and penetrating ulcers. MRI can also detect blood flow, which may be useful in characterizing antegrade versus retrograde dissection. Transesophageal echocardiography, CT, and MRI are the diagnostic procedures of choice over contrast aortography. Their relative utility depends on the availability and expertise in individual institutions as well as on the hemodynamic stability of the patient, with CT and MRI obviously less suitable for unstable patients.
9 Página 9 de 13 TREATMENT Medical therapy should be initiated as soon as the diagnosis is considered. The patient should be admitted to an intensive care unit for monitoring hemodynamics and urine output. Unless hypotension is present, therapy should be aimed at reducing cardiac contractility and systemic arterial pressure, and thereby shear stress. For acute dissection, unless contraindicated, β-adrenergic blockers should be administered parenterally, using intravenous propranolol, metoprolol, or the short-acting esmolol to achieve a heart rate of approximately 60 beats/min. This should be accompanied by sodium nitroprusside infusion to lower systolic blood pressure to 120 mmhg. Labetalol (Chap. 230), a drug with both β- and α-adrenergic blocking properties, is also used as a parenteral agent in the acute therapy of dissection. The calcium channel antagonists, verapamil and diltiazem, may be used intravenously if nitroprusside or labetalol cannot be employed. The addition of a parenteral angiotensinconverting enzyme (ACE) inhibitor, such as enalaprilat, to a β-adrenergic blocker may also be considered. Isolated use of direct vasodilators, such as diazoxide and hydralazine, is contraindicated because these agents can increase hydraulic shear and may propagate dissection. Emergent or urgent surgical correction is the preferred treatment for ascending aortic dissections (type A) and complicated type B dissections including those characterized by propagation, compromise of major aortic branches, impending rupture, or continued pain. Surgery involves excision of the intimal flap, obliteration of the false lumen, and placement of an interposition graft. A composite valve-graft conduit is used if the aortic valve is disrupted. The overall in-hospital mortality rate after surgical treatment of patients with aortic dissection is reported to be 15 to 25%. The major causes of perioperative mortality and morbidity include myocardial infarction, paraplegia, renal failure, tamponade, hemorrhage, and sepsis. Reports of the use of endoluminal stent grafts in selected patients with type B dissection are encouraging. Other transcatheter techniques, such as fenestration of the intimal flaps and stenting of narrowed branch vessels to increase flow to compromised organs, are also under investigation. For uncomplicated and stable distal dissection (type B), medical therapy is the preferred treatment. The in-hospital mortality rate of medically treated patients with type B dissection is 10 to 20%. Long-term therapy for patients with aortic dissection (with or without surgery) consists of the control of hypertension and reduction of cardiac contractility with the use of beta blockers plus other antihypertensive agents such as ACE inhibitors or calcium antagonists. Patients with chronic type B dissection should be followed on an outpatient basis every 6 to 12 months by contrast-enhanced CT or MRI to detect propagation or expansion. Patients with Marfan syndrome are at high risk for postdissection complications. The long-term prognosis for patients with treated dissections is generally good with careful follow-up; the 10-year survival rate is approximately 60%. AORTIC OCCLUSION
10 Página 10 de 13 CHRONIC ATHEROSCLEROTIC OCCLUSIVE DISEASE Atherosclerosis may affect the thoracic and abdominal aorta. Occlusive aortic disease caused by atherosclerosis is usually confined to the distal abdominal aorta below the renal arteries. Frequently the disease extends to the iliac arteries (Chap. 232). Claudication characteristically involves the lower back, buttocks, and thighs and may be associated with impotence in males (Leriche syndrome). The severity of the symptoms depends on the adequacy of collaterals. With sufficient collateral blood flow, a complete occlusion of the abdominal aorta may occur without the development of ischemic symptoms. The physical findings include absence of femoral and other distal pulses bilaterally and the detection of an audible bruit over the abdomen (usually at or below the umbilicus) and the common femoral arteries. Atrophic skin, loss of hair, and coolness of the lower extremities are usually observed. In advanced ischemia, rubor on dependency and pallor on elevation can be seen. P.1485 The diagnosis is usually established by the physical examination and noninvasive testing, including leg pressure measurements, Doppler velocity analysis, pulse volume recordings, and duplex ultrasonography. The anatomy may be defined by MRI, CT or conventional aortography before revascularization. Operative treatment is indicated in patients with debilitating symptoms and/or with the development of leg ischemia. ACUTE OCCLUSION Acute occlusion in the distal abdominal aorta represents a medical emergency because it threatens the viability of the lower extremities. It usually results from an occlusive embolus that almost always originates from the heart. Rarely, acute occlusion may occur as the result of in situ thrombosis in a preexisting severely narrowed segment of the aorta or plaque rupture and hemorrhage into such an area. The clinical picture is one of acute ischemia of the lower extremities. Severe rest pain, coolness, and pallor of the lower extremities and the absence of distal pulses bilaterally are the usual manifestations. Diagnosis should be established rapidly by aortography. Emergency thrombectomy or revascularization is indicated. AORTITIS Aortitis frequently affects the thoracic aorta and may result in aneurysmal dilatation and aortic regurgitation; it occasionally obstructs branch vessels of the aorta. SYPHILITIC AORTITIS This late manifestation of luetic infection (Chap. 153) usually affects the proximal ascending aorta, particularly the aortic root, resulting in aortic dilatation and aneurysm formation. Syphilitic aortitis may occasionally involve the aortic arch or the descending aorta. The aneurysms may be saccular or fusiform and are usually asymptomatic, but compression of and erosion into adjacent structures may result in symptoms; rupture may
11 Página 11 de 13 also occur. The initial lesion is an obliterative endarteritis of the vasa vasorum, especially in the adventitia. This is an inflammatory response to the invasion of the adventitia by the spirochetes. Destruction of the aortic media occurs as the spirochetes spread into this layer, usually via the lymphatics accompanying the vasa vasorum. Destruction of collagen and elastic tissues leads to dilation of the aorta, scar formation, and calcification. These changes account for the characteristic radiographic appearance of a calcified ascending aortic aneurysm. The disease typically presents as an incidental chest radiographic finding 15 to 30 years after initial infection. Symptoms may result from aortic regurgitation, narrowing of coronary ostia due to syphilitic aortitis, compression of adjacent structures (e.g., esophagus), or rupture. Diagnosis is established by a positive serologic test, i.e., rapid plasmin reagin (RPR) or fluorescent treponemal antibody. Treatment includes penicillin and surgical excision and repair. RHEUMATIC AORTITIS Rheumatoid arthritis (Chap. 301), ankylosing spondylitis (Chap. 305), psoriatic arthritis (Chap. 305), Reiter's syndrome (Chap. 305), relapsing polychondritis, and inflammatory bowel disorders may all be associated with aortitis involving the ascending aorta. The inflammatory lesions usually involve the ascending aorta and may extend to the sinuses of Valsalva, the mitral valve leaflets, and adjacent myocardium. The clinical manifestations are aneurysm, aortic regurgitation, and involvement of the cardiac conduction system. TAKAYASU'S ARTERITIS This inflammatory disease often affects the ascending aorta and aortic arch causing obstruction of the aorta and its major arteries. Takayasu's arteritis is also termed pulseless disease because of the frequent occlusion of the large arteries originating from the aorta. It may also involve the descending thoracic and abdominal aorta and occlude large branches such as the renal arteries. Aortic aneurysms may also occur. The pathology is a panarteritis, characterized by mononuclear cells and occasionally giant cells, with marked intimal hyperplasia, medial and adventitial thickening, and, in chronic form, fibrotic occlusion. The disease is most prevalent in young females of Asian descent but does occur in women of other geographic and ethnic origins and also in young men. During the acute stage, fever, malaise, weight loss, and other systemic symptoms may be evident. An elevation of the erythrocyte sedimentation rate is common. The chronic stages of the disease present with symptoms related to large artery occlusion, such as upper extremity claudication, cerebral ischemia, and syncope. The chronic disease is intermittently active. Since the process is progressive and there is no definitive therapy, the prognosis is usually poor. Glucocorticoids and immunosuppressive agents have been reported to be effective in some patients during the acute phase. Occasionally, anticoagulation prevents thrombosis and complete occlusion of a large artery. Surgical bypass or endovascular intervention of a critically stenotic artery may be necessary.
12 Página 12 de 13 GIANT CELL ARTERITIS (See also Chap. 306) This vasculitis occurs in older individuals and affects women more often than men. Primarily large and medium-sized arteries are affected. The pathology is that of focal granulomatous lesions involving the entire arterial wall. It may be associated with polymyalgia rheumatica. Obstruction of medium-sized arteries (e.g., temporal and ophthalmic arteries) and of major branches of the aorta and the development of aortitis and aortic regurgitation are some of the complications of the disease. High-dose glucocorticoid therapy may be effective when given early. FURTHER READING THE ANEURYSM DETECTION AND MANAGEMENT VETERANS AFFAIRS COOPERATIVE STUDY GROUP: Immediate repair compared with surveillance of small abdominal aortic aneurysms. N Engl J Med 346:1437, 2002 GANAHA F et al: Prognosis of aortic intramural hematoma with and without penetrating atherosclerotic ulcer. A clinical and radiological analysis. Circulation 106:342, 2002 GUO D et al: Familial thoracic aortic aneurysms and dissections: Genetic heterogeneity with a major locus mapping to 5q Circulation 103:2461, 2001 HAGAN PG et al: The International Registry of Acute Aortic Dissection (IRAD): New insights into an old disease. JAMA 283:897, 2000 HASHIMOTO H: Takayasu's arteritis and giant cell (temporal or cranial) arteritis. Intern Med 39:4, 2000 ISSELBACHER EM et al: Diseases of the aorta, in Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine, 7th ed, DP Zipes et al (eds). Philadelphia, Saunders, 2005 THE MULTICENTRE ANEURYSM SCREENING STUDY GROUP: The Multicentre Aneurysm Screening Study (MASS) into the effect of abdominal aortic aneurysm screening on mortality in men: A randomized controlled trial. Lancet 360:1531, 2002 PARODI JC et al: Endovascular treatment of aneurysmal disease. Cardiol Clin 20:579, 2002
13 Página 13 de 13 THE UK SMALL ANEURYSM TRIAL PARTICIPANTS: Long-term outcomes of immediate repair compared with surveillance of small abdominal aortic aneurysms. N Engl J Med 346:1445, 2002 VAUGHAN CJ et al: Identification of a chromosome 11q23.2-q24 locus for familial aortic aneurysm disease, a genetically heterogeneous disorder. Circulation 103:2469, 2001 BIBLIOGRAPHY BLANCHARD JF et al: Risk factors for abdominal aortic aneurysm: Results of a casecontrol study. Am J Epidemiol 151:575, 2000 BLUM U et al: Endoluminal stent-grafts for infrarenal abdominal aortic aneurysms. N Engl J Med 336:13, 1997 LEDERLE FA et al: Abdominal aortic aneurysm in women. J Vasc Surg 34:122, 2001 NIENABER CA et al: Nonsurgical reconstruction of thoracic aortic dissection by stentgraft placement. N Engl J Med 340:1539, 1999 Copyright (c) Ovid Technologies, Inc. Version: rel9.2.0, SourceID
AORTIC DISSECTION. DISSECTING ANEURYSMS OF THE AORTA or CLASSIFICATION
 DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial
 An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial wall (intima, media, and adventitia) or the attenuated
An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial wall (intima, media, and adventitia) or the attenuated
CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D.
 CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D. Thoracic Aortic Aneurysms Atherosclerotic Dissection Penetrating ulcer Mycotic Inflammatory (vasculitis) Traumatic Aortic Imaging Options Catheter
CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D. Thoracic Aortic Aneurysms Atherosclerotic Dissection Penetrating ulcer Mycotic Inflammatory (vasculitis) Traumatic Aortic Imaging Options Catheter
Diseases of the aorta
 Diseases of the aorta Aneurysm, dissection and aortitis are the main pathologies (Fig. 18.79 ). data:text/html;charset=utf-8,%3ch2%20id%3d%22cc5a0836d6aa490ca26dd7c15632b559%22%20style%3d%22margin%3a%201.3em%200px%200.5em%3b%20padding%3a%200px%3b%20border%3a%200px%3b%20font-fa
Diseases of the aorta Aneurysm, dissection and aortitis are the main pathologies (Fig. 18.79 ). data:text/html;charset=utf-8,%3ch2%20id%3d%22cc5a0836d6aa490ca26dd7c15632b559%22%20style%3d%22margin%3a%201.3em%200px%200.5em%3b%20padding%3a%200px%3b%20border%3a%200px%3b%20font-fa
Aneurysms & a Brief Discussion on Embolism
 Aneurysms & a Brief Discussion on Embolism Aneurysms, overview = congenital or acquired dilations of blood vessels or the heart True aneurysms -involve all three layers of the artery (intima, media, and
Aneurysms & a Brief Discussion on Embolism Aneurysms, overview = congenital or acquired dilations of blood vessels or the heart True aneurysms -involve all three layers of the artery (intima, media, and
Diseases of the Aorta
 Diseases of the Aorta ASE Review 2018 Susan E Wiegers, MD, FASE, FACC Professor of Medicine My great friend Dr. Roberto Lang Disclosure None related to this presentation 1 Objectives Aneurysm Dissection
Diseases of the Aorta ASE Review 2018 Susan E Wiegers, MD, FASE, FACC Professor of Medicine My great friend Dr. Roberto Lang Disclosure None related to this presentation 1 Objectives Aneurysm Dissection
THORACIC AORTIC DISSECTION
 The Essence of Aortic Dissection THORACIC AORTIC DISSECTION Aortic dissection can be classified as acute if it s onset has been less than 14 days or chronic if its onset has been more than 14 days. Mortality
The Essence of Aortic Dissection THORACIC AORTIC DISSECTION Aortic dissection can be classified as acute if it s onset has been less than 14 days or chronic if its onset has been more than 14 days. Mortality
, David Stultz, MD. Aortic Dissection. David Stultz, MD October 7, 2003
 Aortic Dissection David Stultz, MD October 7, 2003 Background Incidence of 1 in 2000 in US Early mortality of 1%/hour for proximal dissection Two theories of formation Breach of intimal layer of aorta
Aortic Dissection David Stultz, MD October 7, 2003 Background Incidence of 1 in 2000 in US Early mortality of 1%/hour for proximal dissection Two theories of formation Breach of intimal layer of aorta
ACUTE AORTIC SYNDROMES
 ACUTE AORTIC SYNDROMES AGNETA FLINCK MD, PhD Dept. of Thoracic Radiology Sahlgrenska University Hospital ACUTE AORTIC SYNDROMES Aortic dissection Intramural hematoma (IMH) 5-20% Penetrating atherosclerotic
ACUTE AORTIC SYNDROMES AGNETA FLINCK MD, PhD Dept. of Thoracic Radiology Sahlgrenska University Hospital ACUTE AORTIC SYNDROMES Aortic dissection Intramural hematoma (IMH) 5-20% Penetrating atherosclerotic
Acute Aortic Syndromes
 Acute Aortic Syndromes None Disclosures Smita Patel, M.B.B.S., M.R.C.P., F.R.C.R. Associate Professor, University of Michigan Ann Arbor, MI Objectives To review common CTA findings of acute aortic syndromes
Acute Aortic Syndromes None Disclosures Smita Patel, M.B.B.S., M.R.C.P., F.R.C.R. Associate Professor, University of Michigan Ann Arbor, MI Objectives To review common CTA findings of acute aortic syndromes
AORTIC DISSECTIONS Current Management. TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida
 AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
Aortic arch pathology. Cerebral ischemia following carotid artery stenosis.
 Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Χρόνιος διαχωρισμός. υπερηχοκαρδιογραφική. αορτής. παρακολούθηση ή άλλη; Α. Παπασπυρόπουλος ΕΠΙΜΕΛΗΤΗΣ ΓΝ.ΝΙΚΑΙΑΣ ΠΕΜΠΤΗ
 Χρόνιος διαχωρισμός αορτής υπερηχοκαρδιογραφική παρακολούθηση ή άλλη; Α. Παπασπυρόπουλος ΕΠΙΜΕΛΗΤΗΣ ΓΝ.ΝΙΚΑΙΑΣ ΠΕΜΠΤΗ 8-2-2018 The Normal Aorta (conduit function + control ) *Aortic expansion is about
Χρόνιος διαχωρισμός αορτής υπερηχοκαρδιογραφική παρακολούθηση ή άλλη; Α. Παπασπυρόπουλος ΕΠΙΜΕΛΗΤΗΣ ΓΝ.ΝΙΚΑΙΑΣ ΠΕΜΠΤΗ 8-2-2018 The Normal Aorta (conduit function + control ) *Aortic expansion is about
Acute Aortic Syndromes
 Acute Aortic Syndromes Carole J. Dennie, MD Acute Thoracic Aortic Syndromes Background Non-Traumatic Acute Thoracic Aortic Syndromes Carole Dennie MD FRCPC Associate Professor of Radiology and Cardiology
Acute Aortic Syndromes Carole J. Dennie, MD Acute Thoracic Aortic Syndromes Background Non-Traumatic Acute Thoracic Aortic Syndromes Carole Dennie MD FRCPC Associate Professor of Radiology and Cardiology
Multimodality Imaging of the Thoracic Aorta
 Multimodality Imaging of the Thoracic Aorta Steven Goldstein MD, FACC Director Noninvasive Cardiology MedStar Heart and Vascular Institute Washington Hospital Center Saturday, October 8, 2016 DISCLOSURE
Multimodality Imaging of the Thoracic Aorta Steven Goldstein MD, FACC Director Noninvasive Cardiology MedStar Heart and Vascular Institute Washington Hospital Center Saturday, October 8, 2016 DISCLOSURE
NON-ATHEROSCLEROTIC PATHOLOGY OF THE CAROTID ARTERIES
 NON-ATHEROSCLEROTIC PATHOLOGY OF THE CAROTID ARTERIES Leslie M. Scoutt, MD, FACR Professor of Diagnostic Radiology & Surgery Vice Chair, Dept of Radiology & Biomedical Imaging Chief, Ultrasound Section
NON-ATHEROSCLEROTIC PATHOLOGY OF THE CAROTID ARTERIES Leslie M. Scoutt, MD, FACR Professor of Diagnostic Radiology & Surgery Vice Chair, Dept of Radiology & Biomedical Imaging Chief, Ultrasound Section
Update on Acute Aortic Syndrome
 SUNDAY Update on Acute Aortic Syndrome Diana Litmanovich, MD Learning objectives To be familiar with the definition, natural history, and imaging findings of acute aortic syndrome, including: I. Aortic
SUNDAY Update on Acute Aortic Syndrome Diana Litmanovich, MD Learning objectives To be familiar with the definition, natural history, and imaging findings of acute aortic syndrome, including: I. Aortic
Disclosures: Acute Aortic Syndrome. A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO
 Acute Aortic Syndrome Disclosures: A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO No financial relationships to disclose 1 Acute Aortic
Acute Aortic Syndrome Disclosures: A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO No financial relationships to disclose 1 Acute Aortic
Aortic CT: Intramural Hematoma. Leslie E. Quint, M.D.
 Aortic CT: Intramural Hematoma Leslie E. Quint, M.D. 43 M Mid back pain X several months What type of aortic disease? A. Aneurysm with intraluminal thrombus B. Chronic dissection with thrombosed false
Aortic CT: Intramural Hematoma Leslie E. Quint, M.D. 43 M Mid back pain X several months What type of aortic disease? A. Aneurysm with intraluminal thrombus B. Chronic dissection with thrombosed false
Case Acute ascending thoracic aortic rupture due to penetrating atherosclerotic ulcer
 Case 12305 Acute ascending thoracic aortic rupture due to penetrating atherosclerotic ulcer Lopes Dias J, Costa NV, Leal C, Alves P, Bilhim T Section: Chest Imaging Published: 2014, Dec. 19 Patient: 68
Case 12305 Acute ascending thoracic aortic rupture due to penetrating atherosclerotic ulcer Lopes Dias J, Costa NV, Leal C, Alves P, Bilhim T Section: Chest Imaging Published: 2014, Dec. 19 Patient: 68
PERPHERAL ARTERY ANEURYSM. By Pooja Sharma and Susanna Sebastianpillai
 PERPHERAL ARTERY ANEURYSM By Pooja Sharma and Susanna Sebastianpillai Defintions True Aneurysm Involves all three layers of the vessel. Have two basic shapes; Fusiform = symmetric widening of the vessels
PERPHERAL ARTERY ANEURYSM By Pooja Sharma and Susanna Sebastianpillai Defintions True Aneurysm Involves all three layers of the vessel. Have two basic shapes; Fusiform = symmetric widening of the vessels
Animesh Rathore, MD 4/21/17. Penetrating atherosclerotic ulcers of aorta
 Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
AORTIC ANEURYSM. howmed.net
 AORTIC ANEURYSM howmed.net ANATOMY It is important to understand the anatomy of the aorta Need to know the extent of the aneurysm Need to know the vessels involved This helps with Medical or Surgical management
AORTIC ANEURYSM howmed.net ANATOMY It is important to understand the anatomy of the aorta Need to know the extent of the aneurysm Need to know the vessels involved This helps with Medical or Surgical management
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
From Valve to Arch: How s Your Aorta? March 7, 2011
 From Valve to Arch: How s Your Aorta? March 7, 2011 Susan Housholder-Hughes, RN, MSN, ANP-BC, FAHA, AACC Nurse Practitioner, Multidisciplinary Aortic Program Cardiovascular Center Adjunct Clinical Instructor,
From Valve to Arch: How s Your Aorta? March 7, 2011 Susan Housholder-Hughes, RN, MSN, ANP-BC, FAHA, AACC Nurse Practitioner, Multidisciplinary Aortic Program Cardiovascular Center Adjunct Clinical Instructor,
Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias. UCSF Vascular Symposium April 7-9, Acute Aortic Dissection
 Aortic Dissection: Natural History What is the Natural History of Aortic Dissection? UCSF Vascular Symposium April 7-9, 2011 Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias Stephen
Aortic Dissection: Natural History What is the Natural History of Aortic Dissection? UCSF Vascular Symposium April 7-9, 2011 Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias Stephen
Vascular Emergencies. Scott M Surowiec, MD Assistant Professor of Surgery Upstate Vascular and Crouse Hospital September 29, 2015
 Vascular Emergencies Scott M Surowiec, MD Assistant Professor of Surgery Upstate Vascular and Crouse Hospital September 29, 2015 Introduction Main vascular emergencies include Ruptured Abdominal Aortic
Vascular Emergencies Scott M Surowiec, MD Assistant Professor of Surgery Upstate Vascular and Crouse Hospital September 29, 2015 Introduction Main vascular emergencies include Ruptured Abdominal Aortic
3 : 37. Kirit Patel, USA CLASSIFICATION DIAGNOSIS
 3 : 37 Management of Aortic Aneurysms Clinical features and diagnosis of thoracic aortic aneurysm An aneurysm is currently defined as a localized dilatation of the aorta, 50 percent over the normal diameter,
3 : 37 Management of Aortic Aneurysms Clinical features and diagnosis of thoracic aortic aneurysm An aneurysm is currently defined as a localized dilatation of the aorta, 50 percent over the normal diameter,
IMAGING the AORTA. Mirvat Alasnag FACP, FSCAI, FSCCT, FASE June 1 st, 2011
 IMAGING the AORTA Mirvat Alasnag FACP, FSCAI, FSCCT, FASE June 1 st, 2011 September 11, 2003 Family is asking $67 million in damages from two doctors Is it an aneurysm? Is it a dissection? What type of
IMAGING the AORTA Mirvat Alasnag FACP, FSCAI, FSCCT, FASE June 1 st, 2011 September 11, 2003 Family is asking $67 million in damages from two doctors Is it an aneurysm? Is it a dissection? What type of
CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns
 CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns Eneva M. St. Ekaterna University Hospital Report objectives 1. Review malperfusion
CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns Eneva M. St. Ekaterna University Hospital Report objectives 1. Review malperfusion
Descending aorta replacement through median sternotomy
 Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Acute Aortic Syndromes
 Acute Aortic Syndromes Michael H. Picard, M.D. Massachusetts General Hospital Harvard Medical School No disclosures For everything you need to know about the aorta see Circulation 2010;121:e266-e369 And.
Acute Aortic Syndromes Michael H. Picard, M.D. Massachusetts General Hospital Harvard Medical School No disclosures For everything you need to know about the aorta see Circulation 2010;121:e266-e369 And.
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Case 9799 Stanford type A aortic dissection: US and CT findings
 Case 9799 Stanford type A aortic dissection: US and CT findings Accogli S, Aringhieri G, Scalise P, Angelini G, Pancrazi F, Bemi P, Bartolozzi C Department of Diagnostic and Interventional Radiology, University
Case 9799 Stanford type A aortic dissection: US and CT findings Accogli S, Aringhieri G, Scalise P, Angelini G, Pancrazi F, Bemi P, Bartolozzi C Department of Diagnostic and Interventional Radiology, University
Penetrating Atherosclerotic Ulcer
 April 2016 Penetrating Atherosclerotic Ulcer Michael Nguyen, Harvard Medical School Year III Outline Introduction to Penetrating Atherosclerotic Ulcers Radiographic Features Treatment and Prognosis Patient
April 2016 Penetrating Atherosclerotic Ulcer Michael Nguyen, Harvard Medical School Year III Outline Introduction to Penetrating Atherosclerotic Ulcers Radiographic Features Treatment and Prognosis Patient
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when?
 Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
VASCULAR SURGERY, PART I VOLUME
 CME Pretest VASCULAR SURGERY, PART I VOLUME 42 7 2016 To earn CME credit, completing the pretest is a mandatory requirement. The pretest should be completed BEFORE reading the overview and taking the posttest.
CME Pretest VASCULAR SURGERY, PART I VOLUME 42 7 2016 To earn CME credit, completing the pretest is a mandatory requirement. The pretest should be completed BEFORE reading the overview and taking the posttest.
Echocardiographic Evaluation of the Aorta
 Echocardiographic Evaluation of the Aorta William F. Armstrong M.D. Director Echocardiography Laboratory Professor of Medicine University of Michigan The Aorta: What to Evaluate Dimensions / shape Atherosclerotic
Echocardiographic Evaluation of the Aorta William F. Armstrong M.D. Director Echocardiography Laboratory Professor of Medicine University of Michigan The Aorta: What to Evaluate Dimensions / shape Atherosclerotic
Abdominal Aortic Aneurysms. A Surgeons Perspective Dr. Derek D. Muehrcke
 Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
THE BLOOD VESSELS. Manar hajeer, MD University of Jordan Faculty of medicine, pathology department.
 THE BLOOD VESSELS Manar hajeer, MD University of Jordan Faculty of medicine, pathology department. Vascular pathology: 1- Narrowing or complete obstruction of vessel lumina, either progressively (e.g.,
THE BLOOD VESSELS Manar hajeer, MD University of Jordan Faculty of medicine, pathology department. Vascular pathology: 1- Narrowing or complete obstruction of vessel lumina, either progressively (e.g.,
Detailed Order Request Checklists for Cardiology
 Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
ISPUB.COM. A pulled muscle," - Aortic Dissection. A Bhagra, N Anand, M Fernanda Bellolio INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Radiology Volume 9 Number 1 A pulled muscle," - Aortic Dissection A Bhagra, N Anand, M Fernanda Bellolio Citation A Bhagra, N Anand, M Fernanda Bellolio. A pulled muscle,"
ISPUB.COM The Internet Journal of Radiology Volume 9 Number 1 A pulled muscle," - Aortic Dissection A Bhagra, N Anand, M Fernanda Bellolio Citation A Bhagra, N Anand, M Fernanda Bellolio. A pulled muscle,"
Case Presentation VASCULITIS. Case Presentation. Case Presentation. Vasculitis
 Case Presentation VASCULITIS The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Case Presentation VASCULITIS The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Infected Lower Extremity Aneurysms C. Stefan Kénel-Pierre, MD
 Infected Lower Extremity Aneurysms C. Stefan Kénel-Pierre, MD University Hospital of Brooklyn Department of Surgery History 52F c PMHx of HTN, asthma p/w fever, malaise s/p one week of ABx for presumed
Infected Lower Extremity Aneurysms C. Stefan Kénel-Pierre, MD University Hospital of Brooklyn Department of Surgery History 52F c PMHx of HTN, asthma p/w fever, malaise s/p one week of ABx for presumed
Treatment of acute type B aortic dissection: Current status
 MEET Cannes, 18. - 21.06.2009 Treatment of acute type B aortic dissection: Current status Christoph A. Nienaber, MD, FACC University of Rostock Department of Internal Medicine, Cardiology christoph.nienaber@med.uni-rostock.de
MEET Cannes, 18. - 21.06.2009 Treatment of acute type B aortic dissection: Current status Christoph A. Nienaber, MD, FACC University of Rostock Department of Internal Medicine, Cardiology christoph.nienaber@med.uni-rostock.de
VASCULITIS. Case Presentation. Case Presentation
 VASCULITIS Case Presentation The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
VASCULITIS Case Presentation The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Takayasu s Arteritis: A Case Report With Global Arterial Involvement
 1 Case Report Takayasu s Arteritis: A Case Report With Global Arterial Involvement Waqas Ahmed, Zeeshan Ahmad* From Shifa International Hospital H-8/4, Islamabad, Pakistan Correspondence: Dr Waqas Ahmed,
1 Case Report Takayasu s Arteritis: A Case Report With Global Arterial Involvement Waqas Ahmed, Zeeshan Ahmad* From Shifa International Hospital H-8/4, Islamabad, Pakistan Correspondence: Dr Waqas Ahmed,
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
SUPPLEMENTAL MATERIAL
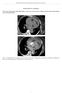 SUPPLEMENTL MTERIL Marie erna, Martin Kocher, Rohit Philip Thomas. cute aorta, overview of acute T findings and endovascular treatment options (doi: 10.5507/bp.2016.060) Fig. 1. : Non-enhanced T, hemopericardium
SUPPLEMENTL MTERIL Marie erna, Martin Kocher, Rohit Philip Thomas. cute aorta, overview of acute T findings and endovascular treatment options (doi: 10.5507/bp.2016.060) Fig. 1. : Non-enhanced T, hemopericardium
Acute dissections of the descending thoracic aorta (Debakey
 Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Ischemic heart disease
 Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Beyond Stenosis Severity: Top 5 Important Duplex Characteristics to Identify in a Patient with Carotid Disease
 Beyond Stenosis Severity: Top 5 Important Duplex Characteristics to Identify in a Patient with Carotid Disease Jan M. Sloves RVT, RCS, FASE Technical Director New York Cardiovascular Associates Disclosures
Beyond Stenosis Severity: Top 5 Important Duplex Characteristics to Identify in a Patient with Carotid Disease Jan M. Sloves RVT, RCS, FASE Technical Director New York Cardiovascular Associates Disclosures
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
New ASE Guidelines: What you must know
 New ASE Guidelines: What you must know Federico M Asch MD, FASE, FACC Chair, ASE Guidelines and Standards Committee Medstar Washington Hospital Center Medstar Health Research Institute Georgetown University
New ASE Guidelines: What you must know Federico M Asch MD, FASE, FACC Chair, ASE Guidelines and Standards Committee Medstar Washington Hospital Center Medstar Health Research Institute Georgetown University
Objectives. Abdominal Aortic Aneuryms 11/16/2017. The Vascular Patient: Diagnosis and Conservative Treatment
 The Vascular Patient: Diagnosis and Conservative Treatment Ferrell-Duncan Clinic Zachary C. Schmittling, M.D., F.A.C.S. Vascular and General Surgery Ferrell-Duncan Clinic Cox Health Systems Objectives
The Vascular Patient: Diagnosis and Conservative Treatment Ferrell-Duncan Clinic Zachary C. Schmittling, M.D., F.A.C.S. Vascular and General Surgery Ferrell-Duncan Clinic Cox Health Systems Objectives
Atlas of the Vasculitic Syndromes
 CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
Imaging abdominal vascular emergencies. V.Stoynova
 Imaging abdominal vascular emergencies V.Stoynova Abdominal vessels V. Stoynova 2 Acute liver bleeding trauma anticoagulant therapy liver disease : HCC, adenoma, meta, FNH, Hemangioma Diagnosis :CT angiography
Imaging abdominal vascular emergencies V.Stoynova Abdominal vessels V. Stoynova 2 Acute liver bleeding trauma anticoagulant therapy liver disease : HCC, adenoma, meta, FNH, Hemangioma Diagnosis :CT angiography
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
ADVANCED CARDIOVASCULAR IMAGING. Medical Knowledge. Goals and Objectives PF EF MF LF Aspirational
 Medical Knowledge Goals and Objectives PF EF MF LF Aspirational Know the basic principles of magnetic resonance imaging (MRI) including the role of the magnetic fields and gradient coil systems, generation
Medical Knowledge Goals and Objectives PF EF MF LF Aspirational Know the basic principles of magnetic resonance imaging (MRI) including the role of the magnetic fields and gradient coil systems, generation
FMD 101. Esther S.H. Kim, MD, MPH, FACC, FSVM FMDSA Annual Meeting 18 May 2013
 FMD 101 Esther S.H. Kim, MD, MPH, FACC, FSVM FMDSA Annual Meeting 18 May 2013 Back to basics Blood Bodily fluid that transports necessary substances (oxygen, nutrients, antibodies, hormones, etc) and waste
FMD 101 Esther S.H. Kim, MD, MPH, FACC, FSVM FMDSA Annual Meeting 18 May 2013 Back to basics Blood Bodily fluid that transports necessary substances (oxygen, nutrients, antibodies, hormones, etc) and waste
Open fenestration for complicated acute aortic B dissection
 Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Management of Ascending Aortic
 Management of Ascending Aortic Aneurysm Complicating Coarctation of the Aorta Ramanathan Sampath, M.D., William N. O'Connor, M.D., Jacqueline A. Noonan, M.D., and Edward P. Todd, M.D., Ph.D. ABSTRACT Four
Management of Ascending Aortic Aneurysm Complicating Coarctation of the Aorta Ramanathan Sampath, M.D., William N. O'Connor, M.D., Jacqueline A. Noonan, M.D., and Edward P. Todd, M.D., Ph.D. ABSTRACT Four
Surgical indications in ascending aorta aneurysms: What do we know? Jean-Luc MONIN, MD, PhD. Institut Mutualiste Montsouris, Paris, FRANCE
 Surgical indications in ascending aorta aneurysms: What do we know? Jean-Luc MONIN, MD, PhD. Institut Mutualiste Montsouris, Paris, FRANCE Disclosures related to this talk : NONE 2 Clinical case A 40 year-old
Surgical indications in ascending aorta aneurysms: What do we know? Jean-Luc MONIN, MD, PhD. Institut Mutualiste Montsouris, Paris, FRANCE Disclosures related to this talk : NONE 2 Clinical case A 40 year-old
MAGNETIC RESONANCE LATE GADOLINIUM ENHANCEMENT DETECTS ACUTE AORTIC INTRAMURAL HEMATOMA
 MAGNETIC RESONANCE LATE GADOLINIUM ENHANCEMENT DETECTS ACUTE AORTIC INTRAMURAL HEMATOMA Diego Perez de Arenaza, Santiago del Castillo, Marcelo Pietrani, Mariano Falconi, Juan Benger, Ezequiel Levy Yeyati,
MAGNETIC RESONANCE LATE GADOLINIUM ENHANCEMENT DETECTS ACUTE AORTIC INTRAMURAL HEMATOMA Diego Perez de Arenaza, Santiago del Castillo, Marcelo Pietrani, Mariano Falconi, Juan Benger, Ezequiel Levy Yeyati,
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion
 Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Deb Coghlan AMS (Vascular and General ) Brisbane, Australia
 Deb Coghlan AMS (Vascular and General ) Brisbane, Australia ANEURYSMAL DIISEASE The infrarenal aorta enlarges with age, and is the commonest site for arterial aneurysms. An aneurysm is a permanent focal
Deb Coghlan AMS (Vascular and General ) Brisbane, Australia ANEURYSMAL DIISEASE The infrarenal aorta enlarges with age, and is the commonest site for arterial aneurysms. An aneurysm is a permanent focal
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
Current treatment of Aortic Aneurysms and Dissections. Adam Keefer, MD, FACS Sean Hislop, MD, FACS
 Current treatment of Aortic Aneurysms and Dissections Adam Keefer, MD, FACS Sean Hislop, MD, FACS Patient 1 69 year old well-educated man with reoccurring pain in his upper abdomen and a pulsatile mass.
Current treatment of Aortic Aneurysms and Dissections Adam Keefer, MD, FACS Sean Hislop, MD, FACS Patient 1 69 year old well-educated man with reoccurring pain in his upper abdomen and a pulsatile mass.
Debate in Management of native COA; Balloon Versus Surgery
 Debate in Management of native COA; Balloon Versus Surgery Dr. Amira Esmat, El Tantawy, MD Professor of Pediatrics Consultant Pediatric Cardiac Interventionist Faculty of Medicine Cairo University 23/2/2017
Debate in Management of native COA; Balloon Versus Surgery Dr. Amira Esmat, El Tantawy, MD Professor of Pediatrics Consultant Pediatric Cardiac Interventionist Faculty of Medicine Cairo University 23/2/2017
Case 1. Aortic Disasters. Case 2. Case 3. Diagnosis, Imaging Techniques and Management
 Aortic Disasters Diagnosis, Imaging Techniques and Management Eric R. Snoey, MD Alameda County Medical Center Oakland, CA 1 Case 1 51 yo female presents with sharp anterior chest pain while at rest. She
Aortic Disasters Diagnosis, Imaging Techniques and Management Eric R. Snoey, MD Alameda County Medical Center Oakland, CA 1 Case 1 51 yo female presents with sharp anterior chest pain while at rest. She
New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor. Cardiothoracic Radiology
 New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor Cardiothoracic Radiology Disclosure I have no disclosure pertinent to this presentation.
New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor Cardiothoracic Radiology Disclosure I have no disclosure pertinent to this presentation.
Type B Aortic Dissection: Management in a Young Man With Neurologic Sequelae
 C a s e S t u d i e s i n H y p e r t e n s i o n J o e l H a n d l e r, M D, S e c t i o n E d i t o r Type B Aortic Dissection: Management in a Young Man With Neurologic Sequelae Joel Handler, MD 39-year-old
C a s e S t u d i e s i n H y p e r t e n s i o n J o e l H a n d l e r, M D, S e c t i o n E d i t o r Type B Aortic Dissection: Management in a Young Man With Neurologic Sequelae Joel Handler, MD 39-year-old
Cardiac Imaging Tests
 Cardiac Imaging Tests http://www.medpagetoday.com/upload/2010/11/15/23347.jpg Standard imaging tests include echocardiography, chest x-ray, CT, MRI, and various radionuclide techniques. Standard CT and
Cardiac Imaging Tests http://www.medpagetoday.com/upload/2010/11/15/23347.jpg Standard imaging tests include echocardiography, chest x-ray, CT, MRI, and various radionuclide techniques. Standard CT and
GENERAL DATA GENERAL HISTORY. NAME : 賴 X 禎 AGE : 52-year-old SEX : Male NATIVE : Taiwanese EDUCATION : Junior high school OCCUPATION : 失業中
 GENERAL HISTORY GENERAL DATA GENERAL HISTORY NAME : 賴 X 禎 AGE : 52-year-old SEX : Male NATIVE : Taiwanese EDUCATION : Junior high school OCCUPATION : 失業中 GENERAL HISTORY PRESENT ILLNESS SUMMARY This 52-year-old
GENERAL HISTORY GENERAL DATA GENERAL HISTORY NAME : 賴 X 禎 AGE : 52-year-old SEX : Male NATIVE : Taiwanese EDUCATION : Junior high school OCCUPATION : 失業中 GENERAL HISTORY PRESENT ILLNESS SUMMARY This 52-year-old
CORONARY ARTERY DISEASES
 CORONARY ARTERY DISEASES It has been estimated that over one third of the population eventually will die of CAD, and 20% will develop symptoms when younger than age 60 years. ANATOMY OF THE CORONARY ARTERIES
CORONARY ARTERY DISEASES It has been estimated that over one third of the population eventually will die of CAD, and 20% will develop symptoms when younger than age 60 years. ANATOMY OF THE CORONARY ARTERIES
(For items 1-12, each question specifies mark one or mark all that apply.)
 Form 121 - Report of Cardiovascular Outcome Ver. 9.2 COMMENTS -Affix label here- Member ID: - - To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: - Central Case No.:
Form 121 - Report of Cardiovascular Outcome Ver. 9.2 COMMENTS -Affix label here- Member ID: - - To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: - Central Case No.:
HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM
 REVIEW DATE REVIEWER'S ID HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM : DISCHARGE DATE: RECORDS FROM: Hospitalization ER Please check all that may apply: Myocardial Infarction Pages 2, 3,
REVIEW DATE REVIEWER'S ID HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM : DISCHARGE DATE: RECORDS FROM: Hospitalization ER Please check all that may apply: Myocardial Infarction Pages 2, 3,
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Ταξινόµηση οξέων αορτικών συνδρόµων
 !!!!!!!!!! ΕΑΑΑ Ταξινόµηση οξέων αορτικών συνδρόµων Acute aortic syndromes The common denominator of AAS is disruption of the media layer of the aorta with Bleeding within IMH, Bleeding along the aortic
!!!!!!!!!! ΕΑΑΑ Ταξινόµηση οξέων αορτικών συνδρόµων Acute aortic syndromes The common denominator of AAS is disruption of the media layer of the aorta with Bleeding within IMH, Bleeding along the aortic
Blood Vessels. Dr. Nabila Hamdi MD, PhD
 Blood Vessels Dr. Nabila Hamdi MD, PhD ILOs Understand the structure and function of blood vessels. Discuss the different mechanisms of blood pressure regulation. Compare and contrast the following types
Blood Vessels Dr. Nabila Hamdi MD, PhD ILOs Understand the structure and function of blood vessels. Discuss the different mechanisms of blood pressure regulation. Compare and contrast the following types
Case 8036 Multiple penetrating atherosclerotic ulcers
 Case 8036 Multiple penetrating atherosclerotic ulcers Santiago I, Seco M, Curvo-Semedo L Section: Cardiovascular Published: 2010, Feb. 22 Patient: 78 year(s), male Clinical History A 78-year-old hypertensive
Case 8036 Multiple penetrating atherosclerotic ulcers Santiago I, Seco M, Curvo-Semedo L Section: Cardiovascular Published: 2010, Feb. 22 Patient: 78 year(s), male Clinical History A 78-year-old hypertensive
Percutaneous Approaches to Aortic Disease in 2018
 Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Aortitis What does Radiologist need to know to help the Clinician?
 Aortitis What does Radiologist need to know to help the Clinician? Diana E. Litmanovich, MD Assistant Professor of Radiology Director of Cardiac CT Outline Background Imaging techniques Diseases Takayasu
Aortitis What does Radiologist need to know to help the Clinician? Diana E. Litmanovich, MD Assistant Professor of Radiology Director of Cardiac CT Outline Background Imaging techniques Diseases Takayasu
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Abdominal Aortic Aneurysm - Part 1. Learning Objectives. Disclosure. University of Toronto Division of Vascular Surgery
 University of Toronto Division of Vascular Surgery Abdominal Aortic Aneurysm - Part 1 Dr Mark Wheatcroft & Dr Elisa Greco Vascular Surgeon, St Michael s Hospital, Toronto & University of Toronto Disclosure
University of Toronto Division of Vascular Surgery Abdominal Aortic Aneurysm - Part 1 Dr Mark Wheatcroft & Dr Elisa Greco Vascular Surgeon, St Michael s Hospital, Toronto & University of Toronto Disclosure
Aneurysms of the aorta are at times evaluated and treated
 Contemporary Reviews in Cardiovascular Medicine Thoracic and Abdominal Aortic Aneurysms Eric M. Isselbacher, MD Aneurysms of the aorta are at times evaluated and treated by physicians from a number of
Contemporary Reviews in Cardiovascular Medicine Thoracic and Abdominal Aortic Aneurysms Eric M. Isselbacher, MD Aneurysms of the aorta are at times evaluated and treated by physicians from a number of
Acute arterial embolism
 Acute arterial embolism Definition Thrombus come from heart or blood vessel or other embolus such as tumor,air gas or fat flow with blood stream and occlude distal limb or visceral arteries which causes
Acute arterial embolism Definition Thrombus come from heart or blood vessel or other embolus such as tumor,air gas or fat flow with blood stream and occlude distal limb or visceral arteries which causes
Transluminal Stent-graft Placement endovascular surgery
 13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
An Extracardiac Unruptured Right Sinus of Valsalva Aneurysm Complicated with
 Page of An Extracardiac Unruptured Right Sinus of Valsalva Aneurysm Complicated with Atherothrombosis Jun Zhang, MD, Yani Liu, MD, PhD, Ligang Liu, MD, PhD, Youbin Deng, MD, PhD. Department of Medical
Page of An Extracardiac Unruptured Right Sinus of Valsalva Aneurysm Complicated with Atherothrombosis Jun Zhang, MD, Yani Liu, MD, PhD, Ligang Liu, MD, PhD, Youbin Deng, MD, PhD. Department of Medical
Ascending Thoracic Aorta: Postsurgical CT Evaluation
 Ascending Thoracic Aorta: Postsurgical CT Evaluation Santiago Martinez Jimenez, MD GOALS Ascending Thoracic Aorta: Postsurgical CT Evaluation Santiago Martínez MD smartinez-jimenez@saint-lukes.org Saint
Ascending Thoracic Aorta: Postsurgical CT Evaluation Santiago Martinez Jimenez, MD GOALS Ascending Thoracic Aorta: Postsurgical CT Evaluation Santiago Martínez MD smartinez-jimenez@saint-lukes.org Saint
Clinical management and treatment of thoracic aortic diseases. Evolution of IMH. Luigi Lovato
 Clinical management and treatment of thoracic aortic diseases Evolution of IMH Luigi Lovato Cardio-Thoracic and Vascular Department Cardio-Thoracic Radiology-University Hospital S. Orsola-Malpighi Bologna-Italy
Clinical management and treatment of thoracic aortic diseases Evolution of IMH Luigi Lovato Cardio-Thoracic and Vascular Department Cardio-Thoracic Radiology-University Hospital S. Orsola-Malpighi Bologna-Italy
Abdominal Aortic Aneurysms (AAA): Management in 2012
 Abdominal Aortic Aneurysms (AAA): Management in 2012 Matthew S. Edwards, MD, MS, FACS Associate Professor of Surgery and Public Health Sciences Department of Vascular and Endovascular Surgery General Considerations
Abdominal Aortic Aneurysms (AAA): Management in 2012 Matthew S. Edwards, MD, MS, FACS Associate Professor of Surgery and Public Health Sciences Department of Vascular and Endovascular Surgery General Considerations
Endovascular Repair o Abdominal. Aortic Aneurysms. Cesar E. Mendoza, M.D. Jackson Memorial Hospital Miami, Florida
 Endovascular Repair o Abdominal Aortic Aneurysms Cesar E. Mendoza, M.D. Jackson Memorial Hospital Miami, Florida Disclosure Nothing to disclose. 2 Mr. X AAA Mr. X. Is a 70 year old male who presented to
Endovascular Repair o Abdominal Aortic Aneurysms Cesar E. Mendoza, M.D. Jackson Memorial Hospital Miami, Florida Disclosure Nothing to disclose. 2 Mr. X AAA Mr. X. Is a 70 year old male who presented to
Internal Carotid Artery Dissection
 May 2011 Internal Carotid Artery Dissection Carolyn April, HMS IV Agenda Presentation of a clinical case Discussion of the clinical features of ICA dissection Discussion of the imaging modalities used
May 2011 Internal Carotid Artery Dissection Carolyn April, HMS IV Agenda Presentation of a clinical case Discussion of the clinical features of ICA dissection Discussion of the imaging modalities used
Case 47 Clinical Presentation
 93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
Intractable Vomiting: A Dissection in Disguise
 Intractable Vomiting: A Dissection in Disguise Jordan Hunter, OMSIII Scott Kirby, D.O. Charles Finch, D.O., FACOEP Jhunter85@midwestern.edu; skirby76@yahoo.com; cfinch@midwestern.edu Abstract Aortic dissection
Intractable Vomiting: A Dissection in Disguise Jordan Hunter, OMSIII Scott Kirby, D.O. Charles Finch, D.O., FACOEP Jhunter85@midwestern.edu; skirby76@yahoo.com; cfinch@midwestern.edu Abstract Aortic dissection
Looking Outside the Box: Incidental Extracardiac Finding in Echo
 Looking Outside the Box: Incidental Extracardiac Finding in Echo Dr. Aijaz Shah Head of Division, Adult Echocardiography Laboratory Prince Sultan Cardiac Centre Riyadh Case 1 17 year old boy presented
Looking Outside the Box: Incidental Extracardiac Finding in Echo Dr. Aijaz Shah Head of Division, Adult Echocardiography Laboratory Prince Sultan Cardiac Centre Riyadh Case 1 17 year old boy presented
Management of cervicocephalic arterial dissection. Ciro G. Randazzo, MD, MPH Thomas Jefferson University Hospital, Department of Neurosurgery
 Management of cervicocephalic arterial dissection Ciro G. Randazzo, MD, MPH Thomas Jefferson University Hospital, Department of Neurosurgery Definition Disruption of arterial wall, either at level of intima-media
Management of cervicocephalic arterial dissection Ciro G. Randazzo, MD, MPH Thomas Jefferson University Hospital, Department of Neurosurgery Definition Disruption of arterial wall, either at level of intima-media
