10RC2 - Berger. Resuscitation of the newborn
|
|
|
- Juliet Thompson
- 6 years ago
- Views:
Transcription
1 10RC2 - Berger Resuscitation of the newborn Thomas M. Berger Neonatal and Paediatric Intensive Care Unit Children s Hospital of Lucerne Lucerne, Switzerland Introduction The respiratory and cardiovascular changes that occur at birth are considerable and unparalleled by any other physiological events that may occur during extrauterine life. Transition from intrauterine to extrauterine life is a dangerous time in the life of a human being. Although neonatal mortality has decreased dramatically in industrialised countries over the past 50 years, deaths in the first week of life and in the first month of life account for the largest proportion of childhood mortality. The most common causes of death are related to prematurity, congenital malformations and perinatal asphyxia. Immediate and adequate support of newborn infants who fail to adapt normally in the delivery room is critically important for their prognosis. In many institutions, paediatricians or neonatologists are not immediately available in unexpected emergency situations and midwives, obstetricians or anaesthesiologists must initiate resuscitation of newborn infants. All parties who have the potential to be involved in neonatal resuscitation should be acquainted with the peculiarities of neonatal resuscitation in order to make adequate decisions in emergency situations. Neonatal resuscitation guidelines were recently revised and published by the International Liaison Committee on Resuscitation (IL- COR) [1,2] and adapted by the European Resuscitation Council (ERC) [3] and the American Heart Association (AHA) [4]. This review will focus on fetal physiology, normal neonatal adaptation and the most common causes of adaptation failure to provide a solid basis for understanding neonatal resuscitation guidelines. Fetal Physiology Secretion and absorption of fetal lung liquid In utero, the future air spaces are filled with fetal lung liquid. Its production is mediated by chloride (Clˉ) secretion by alveolar type II cells. Sodium (Na + ) follows passively and water flows down the osmotic gradient [5]. Around the time of birth, however, the lung liquid must be removed to allow the newborn infant to breathe air. Two mechanisms are believed to be involved in this process, both of which are at least in part linked to the process of labour. The first one involves surges of fetal hormones (epinephrine, cortisol, T 3 ) during labour and delivery. Thyroid and glucocorticoid hormones act synergistically to prime the lung to allow epinephrine to enhance transepithelial Na + absorption through an epithelial Na + channel. The second mechanism, thus far only demonstrated in sheep, is characterised by rhythmic fetal trunk muscle contractions, which frequently occur in synchrony with uterine contractions during active labour and lead to the expulsion of lung liquid [6]. More recently, researchers have been able to visualise lung aeration after birth using phase contrast X-ray imaging in newborn rabbits [7]. They have demonstrated that residual lung liquid clearance from the airways is closely associated with inspiratory activity, whereas between breaths, no significant distal movement of the air-liquid interface could be detected. They speculated that trans-pulmonary hydrostatic pressure generated by inspiration provides the predominant driving force for residual lung liquid clearance. When delivery occurs before the onset of labour (e.g. by elective Caesarean section), there are no surges of fetal stress hormones and lung liquid absorption is impaired. This may be coupled with a lack of lung liquid expulsion because of the absence of uterine contractions. These phenomena are likely explanations for the increased respiratory morbidity seen after Caesarean section deliveries that have occurred prior to labour
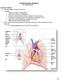
2 From fetal to neonatal circulation In utero, the placenta is responsible for fetal gas exchange. The fetal cotyledons are bathed in maternal blood in the intervillous space and CO 2 is removed from and O 2 taken up by the fetal blood. The partial pressure of oxygen (p uv O 2 ) in the umbilical vein only reaches 4 kpa (30 mmhg), but because of the properties of HbF still results in an oxygen saturation of 65-70%. This is the highest oxygen saturation that occurs in the foetus. The fetal blood is then collected in the umbilical vein, bypasses the liver through the ductus venosus Arantii and enters the inferior vena cava just below the right atrium. Mixed with blood from the lower body of the foetus, the umbilical venous blood is preferentially directed from the right atrium across the foramen ovale into the left atrium (intracardiac streaming) [8]. It is then ejected from the left ventricle into the ascending aorta. Thus, well-oxygenated fetal blood reaches the myocardium and the fetal brain. In contrast, deoxygenated blood from the superior vena cava is directed across the right atrium into the right ventricle and pumped into the pulmonary artery. Because pulmonary vascular resistance (PVR) is very high in utero, more than 85-90% of the right ventricular cardiac output bypasses the lung and flows through the ductus arteriosus Botalli into the descending aorta. Through admixture of this poorly oxygenated blood the lower part of the body is perfused with blood that only has an oxygen saturation of 45%. Vascular resistance of the placenta is low and approximately 50% of the combined right and left ventricular cardiac output flows through the internal iliac arteries into the umbilical arteries and eventually reaches the placenta via the umbilical cord [8] (Fig. 1). Figure 1. Fetal circulation: right ventricular output perfuses the descending aorta, the lower part of the body and the placenta, whereas the left ventricular output is directed toward the coronary and cerebral vascular beds with only a small portion crossing the aortic isthmus to perfuse the lower body. Therefore, the right and left ventricles function in parallel to perfuse the fetal body and the placenta (DAB: ductus arteriosus Botalli; DVA: ductus venosus Arantii; FO: foramen ovale; UA: umbilical artery; UV: umbilical vein). After birth, dramatic changes in the circulatory system occur that are vital for normal adaptation. When the umbilical cord is cut, the low resistance placental vascular bed is excluded from the circulation and the systemic vascular resistance (SVR) increases suddenly. At the same time, with the onset of air breathing, high concentrations of oxygen reach the pulmonary blood vessels (alveolar po 2 of 14.2 kpa (107 mmhg) when breathing room air) leading to vasodilatation via an NO-mediated mechanism. With the fall in PVR, pulmonary perfusion increases and pulmonary gas exchange can occur. Pulmonary venous return increases and, when left atrial pressure rises above right atrial pressure, the foramen ovale closes. As pressure in the pulmonary artery falls and pressure in the aorta increases, shunt across the ductus arteriosus Botalli changes from right-to-left to bidirectional and finally left-to-right. The smooth muscle cells of the ductus arteriosus Botalli respond to the increase in pao 2 with constriction, ultimately leading to functional and later anatomical closure of this shunt (Fig. 2)
3 Figure 2. Neonatal circulation after ligation of the umbilical cord: exclusion of the low resistance placental circulation rapidly increases SVR; at the same time PVR falls and pulmonary blood flow increases and pao2 more than doubles. As a consequence, the foramen ovale closes and the ductus arteriosus constricts, thus establishing serial circulations (DAB: ductus arteriosus Botalli; DVA: ductus venosus Arantii; FO: foramen ovale; UA: umbilical artery; UV: umbilical vein). Fetal response to intrauterine hypoxia In utero, fetal hypoxia stimulates a typical sequence of respiratory patterns. Following a period of rapid shallow breathing, a first period of apnoea occurs (i.e., primary apnoea). If intrauterine hypoxia is not corrected, the foetus will then develop gasping respirations followed by a second period of apnoea (secondary apnoea). When delivery occurs during primary apnoea, a newborn infant can be stimulated to restart breathing. In contrast, tactile stimulation alone will be insufficient to correct secondary apnoea and without adequate intervention (i.e. bag-mask ventilation) circulatory collapse will ensue (Fig. 3). Figure 3. Fetal response to hypoxia: Primary and secondary apnoea cannot be distinguished clinically. Since secondary apnoea is rapidly followed by cardiovascular collapse, any newborn not breathing after drying must be provided with positive pressure ventilation. Normal adaptation The most important prerequisite for normal adaptation is the initiation of breathing. With the first breaths, the remaining fetal lung liquid is replaced by air [7]. The forces that are required to establish an air-liquid-interface are surprisingly high (during the first breaths, animals generate intrapleural pressures between -40 to -60 cmh 2 O). Subsequently, compliance normalises to values around 3-5 ml/cmh 2 O so that a pressure gradient of 5-8 cmh 2 O will result in a normal tidal volume of 6 ml/kg in a term infant with a birth weight of 4 kg. Lung aeration and maintenance of a stable functional residual capacity (FRC) are important prerequisites for pulmonary vasodilatation after delivery. Apart from changes in pulmonary vascular geometry, oxygen plays a major role because the increase in alveolar po 2 stimulates endothelial NO synthetase leading to vasodilatation
4 Normally, a healthy newborn starts to breathe or cry within seconds after delivery. Preductal oxygen saturation increases from a fetal value of 65% to more than 90% within the first 10 minutes of life [9-11]. During transition from fetal to neonatal circulation venous admixture through a patent ductus arteriosus into the descending aorta can occur and postductal oxygen saturations can be significantly lower than values measured in preductal positions. Therefore, during resuscitation in the delivery room, oxygen saturation should be measured at the right hand in a preductal position to monitor the infant s heart rate and document the expected increase in oxygen saturation over the first minutes of life. Impaired adaptation There are numerous maternal and fetal conditions that are associated with an increased risk of impaired adaptation. Many of these conditions can be recognised antenatally and the need for resuscitative measures can be anticipated. However, some complications occur unexpectedly (e.g., placental abruption, cord prolapse, uterine rupture, etc.) and can affect individual or all aspects of neonatal adaptation. Impairment of lung liquid clearance Delayed or insufficient clearance of lung liquid can occur after elective Caesarean sections, following rapid deliveries or in premature infants. As long as the newborn infant has an adequate respiratory drive, impairment of lung liquid clearance will manifest as respiratory distress with tachypnoea (respiratory rate above 60/minute), retractions, flaring, grunting and possibly cyanosis. Impairment of respiratory drive The two most common scenarios in which respiratory drive is impaired after delivery are perinatal asphyxia and prematurity. In rare cases, drugs that have been administered to the mother during labour can affect the infant s respiratory centre (e.g., opiates) or weaken its muscular strength (e.g. infusion of magnesium sulphate for preeclampsia). Impairment of circulatory adaptation Impaired circulatory adaptation and thus persistence of fetal circulation can occur after perinatal asphyxia and meconium aspiration, following prolonged rupture of membranes with oligohydramnios and consecutive pulmonary hypoplasia, or in the setting of severe sepsis. Even after successful initial transition, a newborn infant can fall back into a fetal circulatory state, particularly when there is hypoxaemia and/or severe acidosis (i.e., conditions that cause pulmonary vasoconstriction). Epidemiology of neonatal resuscitation Approximately 10% of all newborn infants require some minor interventions after delivery (i.e., tactile stimulation, proper positioning and suctioning of mouth and nose, supplemental oxygen); more advanced resuscitative measures are necessary in about 1% of all deliveries and 80% of these neonates will respond to bag-mask ventilation. In term infants, extensive resuscitation with intubation, chest compressions and administration of resuscitation drugs is very rarely required (about in 1:1000 deliveries). Neonatal resuscitation algorithm It is important that midwives, obstetricians, neonatologists and anaesthetists communicate well to facilitate anticipation of potential problems the newborn infant might present with. A well-organised resuscitation team with clearly defined roles for each team member, including the designation of an experienced team leader, as well as the preparation of proper resuscitation equipment are prerequisites for successful resuscitation
5 Once it has been recognised that an infant might be compromised, the infant should be placed on a resuscitation unit without delay as soon as the cord has been cut. Initial measures include drying of the infant to prevent heat loss and to provide tactile stimulation, correct positioning of the head (i.e. in a sniffing position) and clearing the airway by suctioning of mouth and nose if necessary. This is followed by the assessment of both breathing effort and heart rate, and less importantly tone (note that colour is no longer assessed at this point). If the infant is gasping or not breathing at all, or their heart rate is less than 100 beats/minute, positive pressure ventilation (PPV) must be provided (Fig. 4). Since it is impossible to distinguish primary from secondary apnoea (see above), the more serious condition must be considered and no time should be wasted with further stimulation of the infant. Positive pressure ventilation should be initiated with room air (see below). Figure 4. Bag-mask ventilation using a self-inflating bag; alternatively, a flow-inflating bag or a T-piece resuscitator can be used. In the delivery room, either self-inflating, flow-inflating bags or T-piece resuscitators can be used for respiratory support. Positive end-expiratory pressure (PEEP) may be useful to stabilise the infant s labile FRC, particularly in preterm infants. Successful ventilation requires a proper fit of the mask, an open airway and sufficient inflation pressures. Expansion of the chest should be recognisable but not excessive to avoid volutrauma. The heart rate should readily increase above 100 beats/minute and preductal oxygen saturation should reach values above 90% by the age of 10 minutes. In neonatal resuscitation, successful ventilation is the most important intervention and will suffice in the majority of patients. If the heart rate falls to less than 60 beats/minute despite adequate ventilation, more advanced life support measures are indicated. In this situation, chest compressions at a rate of 90/minute must be coordinated with positive pressure ventilations at a rate of 30/minute with a compression to ventilation ratio of 3:1. Chest compressions are applied over the lower third of the sternum and should compress the chest one third of the anterior-posterior diameter. It is important that chest compressions are only briefly interrupted to deliver positive pressure ventilation. The so-called two thumb-encircling hands method is the preferred mode (Fig. 5), however, the two-finger method (Fig. 6) can be used transiently to facilitate the insertion of an umbilical venous catheter. Figure 5: Chest compressions using two thumb-encircling hands method. Figure 6. Chest compressions using the two-finger method
6 Whenever advanced methods of life support must be provided, it is important to gain vascular access rapidly to administer drugs and isotonic crystalloid solutions (i.e. normal saline, Ringer s lactate) for volume expansion. In depressed neonates, cannulation of peripheral veins is difficult and it is easiest to gain access through the umbilical vein (Fig. 7). In most cases, blood can be aspirated from an umbilical venous line and blood gas analyses and glucose measurements can be performed. If positive pressure ventilation and chest compressions are unsuccessful to restore spontaneous circulation after 30 seconds, intravenous epinephrine should be given at a dose of ug/kg. If no venous access is available but the infant is intubated, epinephrine can be given intratracheally at a dose of ug/kg, however, the efficacy of this route is likely to be inferior to intravenous administration [1-4]. Figure7. Insertion of an umbilical venous catheter: A) using an aseptic technique, the umbilical cord is cut approximately cm above the skin (in case of bleeding, the tape wrapped around the base of the umbilicus can be tightened); B) three vessels can be identified: two small, thick-walled arteries and one larger, thin-walled vein; C) grasping the umbilical cord with a curved forceps, the gaping lumen of the umbilical vein can be seen; D) insertion of the umbilical venous catheter. If the interventions described are unsuccessful or if a stabilised infant deteriorates again, a pneumothorax must be excluded. Its diagnosis can be challenging: unilaterally decreased breath sounds and lateralisation of the heart sounds to the opposite side are the best clinical signs. If the resuscitation area can be darkened, transillumination of the chest with a high intensity light source can be helpful to identify a pneumothorax. The essential steps of neonatal resuscitation are summarised in Fig. 8. Figure 8. Neonatal resuscitation algorithm
7 Oxygen supplementation in the delivery room FiO 2 to be used to start resuscitation For more than 200 years, 100% oxygen has been used in neonatal resuscitation and has remained undisputed until very recently. Although concerns about the ability of newborn infants to cope with oxidative stress and epidemiological reports of potential long-term consequences of perinatal exposure to high oxygen concentrations (i.e. increased risk of developing childhood cancer) have been discussed for many years, the 2005 recommendations for neonatal resuscitation published by the ILCOR, the ERC and AHA still maintained that resuscitation should in general be started with 100% oxygen. They conceded, however, that lower oxygen concentrations and even room air could be chosen as well [12-14]. Based on several meta-analyses [15-19] of prospective randomised controlled trials that demonstrated non-superiority or even a detrimental effect (i.e. increased mortality with a number needed to harm of 20 [19] to 36 [17] associated with resuscitation with 100% oxygen) (Table 3), the revised ILCOR and ERC guidelines of 2010 now uniformly recommend the use of room air rather than 100% oxygen in the resuscitation of term infants [1,2]. In contrast, the 2010 recommendations by the AHA state more conservatively that air or blended oxygen can be used to achieve oxygen saturations in the interquartile range of preductal saturations measured in healthy term infants (Fig. 8). If blended oxygen is not available, resuscitation should begin with room air [1, 2]. In infants who do not respond to resuscitation with room air, the FiO 2 should be increased. The ILCOR and ERC recommendations fail to provide details but simply state [1-3]: If despite effective ventilation there is no increase in heart rate or if oxygenation (guided by oximetry) remains unacceptable, use of a higher concentration of oxygen should be considered. The AHA recommendations are more specific and suggest [4]: If the baby is bradycardic (heart rate < 60 per minute) after 90 seconds of resuscitation with a lower concentration of oxygen, the oxygen concentration should be increased to 100% until recovery of a normal heart rate. Pulse oximetry As discussed previously, changes in oxygen saturation in the first minutes of life are gradual and it takes several minutes before healthy term infants achieve oxygen saturations above 90% [9-11]. Pulse oximetry is the best method to follow this trend. During transition, a preductal location of the oxygen sensor is important since preductal SaO 2 values may be 10-15% higher than postductal SaO 2 values [10]. Pulse oximetry also provides continuous information on heart rate and thus helps to guide resuscitation. Key learning points Up to 10% of all newborn infants require some form of assistance after birth, but more advanced measures of life support are only required by 1% of all neonates Normal adaptation requires timely clearance (absorption, expulsion) of lung liquid, adequate respiratory drive and successful transition from fetal to neonatal circulation Effective ventilation, indicated by chest movement and an increasing heart rate, is the most important intervention in neonatal resuscitation According to updated international resuscitation guidelines, resuscitation of term neonates should be started with room air Supplemental oxygen should only be used if, despite effective ventilation with room air, there is no increase in heart rate or oxygenation remains unacceptably low - 7 -
8 References 1. Perlman JM, Wyllie J, Kattwinkel J, et al. Part 11: Neonatal resuscitation: 2010 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science With Treatment Recommendations. Circulation 2010; 122: S Wyllie J, Perlman JM, Kattwinkel J, et al. Part 11: Neonatal resuscitation: 2010 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations. Resuscitation 2010; 81 Suppl 1: e Richmond S and Wyllie J. European Resuscitation Council Guidelines for Resuscitation 2010 Section 7. Resuscitation of babies at birth. Resuscitation 2010; 81: Kattwinkel J, Perlman JM, Aziz K, et al. Part 15: neonatal resuscitation: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010; 122: S Olver RE, Walters DV and S MW. Developmental regulation of lung liquid transport. Annual Review of Physiology 2004; 66: Stockx EM, Pfister RE, Kyriakides MA, et al. Expulsion of liquid from the fetal lung during labour in sheep. Respiratory Physiology and Neurobioogy 2007; 157: Hooper SB, Kitchen MJ, Wallace MJ, et al. Imaging lung aeration and lung liquid clearance at birth. Faseb Journal 2007; 21: Rychik J. Fetal cardiovascular physiology. Pediaticr Cardiology 2004; 25: Kamlin CO, O Donnell CP, Davis PG, et al. Oxygen saturation in healthy infants immediately after birth. Journal of Pediatrics 2006; 148: Mariani G, Dik PB, Ezquer A, et al. Pre-ductal and post-ductal O2 saturation in healthy term neonates after birth. Journal of Pediatrics 2007; 150: Rabi Y, Yee W, Chen SY, et al. Oxygen saturation trends immediately after birth. Journal of Pediatrics 2006; 148: International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations. Part 7: Neonatal resuscitation. Resuscitation 2005; 67: American Heart Association (AHA) guidelines for cardiopulmonary resuscitation (CPR) and emergency cardiovascular care (ECC) of pediatric and neonatal patients: neonatal resuscitation guidelines. Pediatrics 2006; 117: e The International Liaison Committee on Resuscitation (ILCOR) consensus on science with treatment recommendations for pediatric and neonatal patients: neonatal resuscitation. Pediatrics 2006; 117: e Davis PG, Tan A, O Donnell CP, et al. Resuscitation of newborn infants with 100% oxygen or air: a systematic review and metaanalysis. Lancet 2004; 364: Rabi Y, Rabi D and Yee W. Room air resuscitation of the depressed newborn: a systematic review and meta-analysis. Resuscitation 2007; 72: Saugstad OD, Ramji S, Soll RF, et al. Resuscitation of Newborn Infants with 21% or 100% Oxygen: An Updated Systematic Review and Meta-Analysis. Neonatology 2008; 94: Saugstad OD, Ramji S and Vento M. Resuscitation of depressed newborn infants with ambient air or pure oxygen: a metaanalysis. Biology of the Neonate 2005; 87: Tan A, Schulze A, O Donnell CP, et al. Air versus oxygen for resuscitation of infants at birth. Cochrane Database of Systematic Reviews 2005: CD
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA
 GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
TRAINING NEONATOLOGY SILVANA PARIS
 TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
The Physiology of the Fetal Cardiovascular System
 The Physiology of the Fetal Cardiovascular System Jeff Vergales, MD, MS Department of Pediatrics Division of Pediatric Cardiology jvergales@virginia.edu Disclosures I serve as the medical director for
The Physiology of the Fetal Cardiovascular System Jeff Vergales, MD, MS Department of Pediatrics Division of Pediatric Cardiology jvergales@virginia.edu Disclosures I serve as the medical director for
5 Million neonatal deaths each year worldwide. 20% caused by neonatal asphyxia. Improvement of the outcome of 1 million newborns every year
 1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني
 Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
Neonatal Resuscitation. Dustin Coyle, M.D. Anesthesiology
 Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
NRP Raising the Bar for Providers and Instructors
 NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
FANNP 28TH NATIONAL NNP SYMPOSIUM: CLINICAL UPDATE AND REVIEW OCTOBER 17-21, 2017
 Pulse Oximetry in the Delivery Room: Principles and Practice GS2 3 Jonathan P. Mintzer, MD, FAAP Assistant Professor of Pediatrics Stony Brook Children s Hospital, Division of Neonatal-Perinatal Medicine,
Pulse Oximetry in the Delivery Room: Principles and Practice GS2 3 Jonathan P. Mintzer, MD, FAAP Assistant Professor of Pediatrics Stony Brook Children s Hospital, Division of Neonatal-Perinatal Medicine,
 NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3-
 1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
The fetal circulation
 Peter John Murphy MB ChB DA FRCA The fetal circulation (Fig. 1) is markedly different from the adult circulation. In the fetus, gas exchange does not occur in the lungs but in the placenta. The placenta
Peter John Murphy MB ChB DA FRCA The fetal circulation (Fig. 1) is markedly different from the adult circulation. In the fetus, gas exchange does not occur in the lungs but in the placenta. The placenta
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영
 When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영 The Korean Society of Cardiology COI Disclosure Eun-Young Choi The author have no financial conflicts of interest to disclose
When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영 The Korean Society of Cardiology COI Disclosure Eun-Young Choi The author have no financial conflicts of interest to disclose
Neonatal Resuscitation in What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011
 Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
PIAF study: Placental insufficiency and aortic isthmus flow Jean-Claude Fouron, MD
 Dear colleagues, I would like to thank you very sincerely for agreeing to participate in our multicentre study on the clinical significance of recording fetal aortic isthmus flow during placental circulatory
Dear colleagues, I would like to thank you very sincerely for agreeing to participate in our multicentre study on the clinical significance of recording fetal aortic isthmus flow during placental circulatory
The Blue Baby. Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin
 The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
10/13/2017. Newborn Care. Objectives. Cardiac Anatomy. Managing Transitional Physiology
 Newborn Care Managing Transitional Physiology Mary Coughlin MS, NNP, RNC-E President and Founder Caring Essentials Collaborative Boston, MA Objectives Upon completion of the learning session participants
Newborn Care Managing Transitional Physiology Mary Coughlin MS, NNP, RNC-E President and Founder Caring Essentials Collaborative Boston, MA Objectives Upon completion of the learning session participants
THE CIRCULATORY SYSTEM
 Biology 30S THE CIRCULATORY SYSTEM Name: This module adapted from bblearn.merlin.mb.ca 1 Introduction to Circulation The first organ to form, and the last organ to die. The heart is the pump of life. The
Biology 30S THE CIRCULATORY SYSTEM Name: This module adapted from bblearn.merlin.mb.ca 1 Introduction to Circulation The first organ to form, and the last organ to die. The heart is the pump of life. The
Table 1: The major changes in AHA / AAP neonatal resuscitation guidelines2010 compared to previous recommendations in 2005
 Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
COPYRIGHTED MATERIAL. The fetal circulation CHAPTER 1. Postnatal circulation
 1 CHAPTER 1 The fetal circulation The circulation in the fetus differs from that in the adult. Knowledge of the course and distribution of the fetal circulation is important to our understanding of the
1 CHAPTER 1 The fetal circulation The circulation in the fetus differs from that in the adult. Knowledge of the course and distribution of the fetal circulation is important to our understanding of the
Blood Vessels. Types of Blood Vessels Arteries carry blood away from the heart Capillaries smallest blood vessels. Veins carry blood toward the heart
 C H A P T E R Blood Vessels 20 Types of Blood Vessels Arteries carry blood away from the heart Capillaries smallest blood vessels The site of exchange of molecules between blood and tissue fluid Veins
C H A P T E R Blood Vessels 20 Types of Blood Vessels Arteries carry blood away from the heart Capillaries smallest blood vessels The site of exchange of molecules between blood and tissue fluid Veins
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
Steven Ringer MD PhD April 5, 2011
 Steven Ringer MD PhD April 5, 2011 Disclaimer Mead Johnson sponsors programs such as this to give healthcare professionals access to scientific and educational information provided by experts. The presenter
Steven Ringer MD PhD April 5, 2011 Disclaimer Mead Johnson sponsors programs such as this to give healthcare professionals access to scientific and educational information provided by experts. The presenter
CONGENITAL HEART DISEASE (CHD)
 CONGENITAL HEART DISEASE (CHD) DEFINITION It is the result of a structural or functional abnormality of the cardiovascular system at birth GENERAL FEATURES OF CHD Structural defects due to specific disturbance
CONGENITAL HEART DISEASE (CHD) DEFINITION It is the result of a structural or functional abnormality of the cardiovascular system at birth GENERAL FEATURES OF CHD Structural defects due to specific disturbance
The Cardiovascular System. The Structure of Blood Vessels. The Structure of Blood Vessels. The Blood Vessels. Blood Vessel Review
 The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
Pathophysiology: Left To Right Shunts
 Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
Congenital Heart Disease. CCCHD In WI. Critical Congenital Heart Disease. Why Screen? 4/20/2018. Early Detection = Better Outcomes
 Congenital Heart Disease A Positive Screen? What Does it Mean? A Review of Pulse Oximetry Screening for Critical Congenital Heart Disease Elizabeth Goetz MD MPH 8-10/1000 livebirths 3% of all infant mortality
Congenital Heart Disease A Positive Screen? What Does it Mean? A Review of Pulse Oximetry Screening for Critical Congenital Heart Disease Elizabeth Goetz MD MPH 8-10/1000 livebirths 3% of all infant mortality
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
The blue baby. Case 4
 Case 4 The blue baby Mrs Smith has brought her baby to A&E because she says he has started turning blue. What are your immediate differential diagnoses? 1 Respiratory causes: Congenital respiratory disorder.
Case 4 The blue baby Mrs Smith has brought her baby to A&E because she says he has started turning blue. What are your immediate differential diagnoses? 1 Respiratory causes: Congenital respiratory disorder.
Pulse Oximetry Screening in Newborns to Enhance the Detection Of Critical Congenital Heart Disease. Frequently Asked Questions
 Pulse Oximetry Screening in Newborns to Enhance the Detection Of Critical Congenital Heart Disease Frequently Asked Questions Current Recommendation: The current recommendation from the Canadian Cardiovascular
Pulse Oximetry Screening in Newborns to Enhance the Detection Of Critical Congenital Heart Disease Frequently Asked Questions Current Recommendation: The current recommendation from the Canadian Cardiovascular
Pathophysiology: Left To Right Shunts
 Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Lecture Notes. Chapter 2: Introduction to Respiratory Failure
 Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
NRP 2018 Current Issues Seminar Science behind NRP. Myra Wyckoff, MD, FAAP Marya Strand, MD, MS, FAAP
 NRP 2018 Current Issues Seminar Science behind NRP Myra Wyckoff, MD, FAAP Marya Strand, MD, MS, FAAP Faculty Disclosure Information In the past 12 months, we have had no relevant financial relationships
NRP 2018 Current Issues Seminar Science behind NRP Myra Wyckoff, MD, FAAP Marya Strand, MD, MS, FAAP Faculty Disclosure Information In the past 12 months, we have had no relevant financial relationships
Scope This guideline is aimed at all Health care professionals involved in the care of infants within the Neonatal Service.
 Management of Newborn Infants born through Meconium-stained liquor University Hospitals of Leicester NHS NHS Trust March 2018 March 2021 Scope This guideline is aimed at all Health care professionals involved
Management of Newborn Infants born through Meconium-stained liquor University Hospitals of Leicester NHS NHS Trust March 2018 March 2021 Scope This guideline is aimed at all Health care professionals involved
2. capillaries - allow exchange of materials between blood and tissue fluid
 Chapter 19 - Vascular System A. categories and general functions: 1. arteries - carry blood away from heart 2. capillaries - allow exchange of materials between blood and tissue fluid 3. veins - return
Chapter 19 - Vascular System A. categories and general functions: 1. arteries - carry blood away from heart 2. capillaries - allow exchange of materials between blood and tissue fluid 3. veins - return
Development of Blood Vessels and Fetal Circulation *
 OpenStax-CNX module: m46610 1 Development of Blood Vessels and Fetal Circulation * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the
OpenStax-CNX module: m46610 1 Development of Blood Vessels and Fetal Circulation * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Cardiovascular System Blood Vessels
 Cardiovascular System Blood Vessels Structure of Blood Vessels The three layers (tunics) Tunica intima composed of simple squamous epithelium Tunica media sheets of smooth muscle Contraction vasoconstriction
Cardiovascular System Blood Vessels Structure of Blood Vessels The three layers (tunics) Tunica intima composed of simple squamous epithelium Tunica media sheets of smooth muscle Contraction vasoconstriction
Large Arteries of Heart
 Cardiovascular System (Part A-2) Module 5 -Chapter 8 Overview Arteries Capillaries Veins Heart Anatomy Conduction System Blood pressure Fetal circulation Susie Turner, M.D. 1/5/13 Large Arteries of Heart
Cardiovascular System (Part A-2) Module 5 -Chapter 8 Overview Arteries Capillaries Veins Heart Anatomy Conduction System Blood pressure Fetal circulation Susie Turner, M.D. 1/5/13 Large Arteries of Heart
1
 1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Pediatrics. Blue Baby Syndrome (Cyanotic Newborn) and Hyperoxia Test. Definition. See online here
 Pediatrics Blue Baby Syndrome (Cyanotic Newborn) and Hyperoxia Test See online here Blue babies lack sufficient hemoglobin, resulting in the bluish discoloration of tissues, a term referred to as cyanosis.
Pediatrics Blue Baby Syndrome (Cyanotic Newborn) and Hyperoxia Test See online here Blue babies lack sufficient hemoglobin, resulting in the bluish discoloration of tissues, a term referred to as cyanosis.
Circulatory System Review
 Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
Resuscitation efforts for Mom & Baby
 Resuscitation efforts for Mom & Baby Beth Ann Clayton, CRNA, MS AmSol Obstetric Anesthesia CRNA Educator Obstetric Anesthesia Clinical Coordinator Mercy Health-Fairfield Hospital Assistant Professor, University
Resuscitation efforts for Mom & Baby Beth Ann Clayton, CRNA, MS AmSol Obstetric Anesthesia CRNA Educator Obstetric Anesthesia Clinical Coordinator Mercy Health-Fairfield Hospital Assistant Professor, University
Hyaline membrane disease. By : Dr. Ch Sarishma Peadiatric Pg
 Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Foetal Cardiology: How to predict perinatal problems. Prof. I.Witters Prof.M.Gewillig UZ Leuven
 Foetal Cardiology: How to predict perinatal problems Prof. I.Witters Prof.M.Gewillig UZ Leuven Cardiopathies Incidence : 8-12 / 1000 births ( 1% ) Most frequent - Ventricle Septum Defect 20% - Atrium Septum
Foetal Cardiology: How to predict perinatal problems Prof. I.Witters Prof.M.Gewillig UZ Leuven Cardiopathies Incidence : 8-12 / 1000 births ( 1% ) Most frequent - Ventricle Septum Defect 20% - Atrium Septum
Chronic Obstructive Pulmonary Disease
 136 PHYSIOLOGY CASES AND PROBLEMS Case 24 Chronic Obstructive Pulmonary Disease Bernice Betweiler is a 73-year-old retired seamstress who has never been married. She worked in the alterations department
136 PHYSIOLOGY CASES AND PROBLEMS Case 24 Chronic Obstructive Pulmonary Disease Bernice Betweiler is a 73-year-old retired seamstress who has never been married. She worked in the alterations department
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Skeletal muscle. Flow increases and decreases with each muscular contraction - as a result of compression of the blood vessels by contracted muscle
 Regional blood flow Skeletal muscle Extreme increases during exercises Flow increases and decreases with each muscular contraction - as a result of compression of the blood vessels by contracted muscle
Regional blood flow Skeletal muscle Extreme increases during exercises Flow increases and decreases with each muscular contraction - as a result of compression of the blood vessels by contracted muscle
Paediatric Cardiology. Acyanotic CHD. Prof F F Takawira
 Paediatric Cardiology Acyanotic CHD Prof F F Takawira Aetiology Chromosomal Down syndrome, T13, T18 Genetic syndromes (gene defects) Velo-Cardio-facial (22 del) Genetic syndromes (undefined aetiology)
Paediatric Cardiology Acyanotic CHD Prof F F Takawira Aetiology Chromosomal Down syndrome, T13, T18 Genetic syndromes (gene defects) Velo-Cardio-facial (22 del) Genetic syndromes (undefined aetiology)
Birth Resuscitation. Jon Palmer, VMD, DACVIM New Bolton Center University on Pennsylvania USA
 Birth Resuscitation Jon Palmer, VMD, DACVIM New Bolton Center University on Pennsylvania USA Resuscitation Fetal Resuscitation Intranatal Resuscitation EXIT Procedures Birth Resuscitation Birth Transition
Birth Resuscitation Jon Palmer, VMD, DACVIM New Bolton Center University on Pennsylvania USA Resuscitation Fetal Resuscitation Intranatal Resuscitation EXIT Procedures Birth Resuscitation Birth Transition
Cardiac Emergencies in Infants. Michael Luceri, DO
 Cardiac Emergencies in Infants Michael Luceri, DO October 7, 2017 I have no financial obligations or conflicts of interest to disclose. Objectives Understand the scope of congenital heart disease Recognize
Cardiac Emergencies in Infants Michael Luceri, DO October 7, 2017 I have no financial obligations or conflicts of interest to disclose. Objectives Understand the scope of congenital heart disease Recognize
Protocol for performing chest clearance techniques by nursing staff
 Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
Neonatal/Pediatric Cardiopulmonary Care
 Neonatal/Pediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate Need usually related Combination of Can occur in 3 Causes of Fetal Asphyxia 1 4 Apnea Hypoxia Stimulates chemoreceptors & baroreceptors
Neonatal/Pediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate Need usually related Combination of Can occur in 3 Causes of Fetal Asphyxia 1 4 Apnea Hypoxia Stimulates chemoreceptors & baroreceptors
NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY
 Background NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY A perinatal hypoxic-ischaemic insult may present with varying degrees of neonatal encephalopathy, neurological disorder and
Background NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY A perinatal hypoxic-ischaemic insult may present with varying degrees of neonatal encephalopathy, neurological disorder and
INDEPENDENT LUNG VENTILATION
 INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary.
 CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
A SYNOPSIS BY ILCOR PEDIATRIC TASK FORCE. Pediatric Basic Life Support, Pediatric Advanced Life Support and Neonatal Resuscitation 2015
 Vol. 2 - No.4 October - December 2015 83 Vol. 2 - No.4 October - December 2015 84 There is new evidence that when treating pediatric septic shock in specific settings, the use of restricted volume of isotonic
Vol. 2 - No.4 October - December 2015 83 Vol. 2 - No.4 October - December 2015 84 There is new evidence that when treating pediatric septic shock in specific settings, the use of restricted volume of isotonic
² C Y E N G R E M E ssignac Cardiac Arrest Resuscitation Device uob
 E M E R G E N C Y Boussignac Cardiac Arrest Resuscitation Device ² What is b-card? b-card Boussignac Cardiac Arrest Resuscitation Device has been designed specifically for the treatment of cardiac arrest.
E M E R G E N C Y Boussignac Cardiac Arrest Resuscitation Device ² What is b-card? b-card Boussignac Cardiac Arrest Resuscitation Device has been designed specifically for the treatment of cardiac arrest.
Cardiovascular Physiology
 Cardiovascular Physiology Lecture 1 objectives Explain the basic anatomy of the heart and its arrangement into 4 chambers. Appreciate that blood flows in series through the systemic and pulmonary circulations.
Cardiovascular Physiology Lecture 1 objectives Explain the basic anatomy of the heart and its arrangement into 4 chambers. Appreciate that blood flows in series through the systemic and pulmonary circulations.
Surfactant Administration
 Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Pulmonary circulation. Lung Blood supply : lungs have a unique blood supply system :
 Dr. Ali Naji Pulmonary circulation Lung Blood supply : lungs have a unique blood supply system : 1. Pulmonary circulation 2. Bronchial circulation 1- Pulmonary circulation : receives the whole cardiac
Dr. Ali Naji Pulmonary circulation Lung Blood supply : lungs have a unique blood supply system : 1. Pulmonary circulation 2. Bronchial circulation 1- Pulmonary circulation : receives the whole cardiac
Simulation 08: Cyanotic Preterm Infant in Respiratory Distress
 Flow Chart Simulation 08: Cyanotic Preterm Infant in Respiratory Distress Opening Scenario Section 1 Type: DM As staff therapist assigned to a Level 2 NICU in a 250 bed rural medical center you are called
Flow Chart Simulation 08: Cyanotic Preterm Infant in Respiratory Distress Opening Scenario Section 1 Type: DM As staff therapist assigned to a Level 2 NICU in a 250 bed rural medical center you are called
Trust Guideline on Routine Oxygen Saturation Measurement on the New-born (Pulse Oximetry)
 Trust Guideline on Routine Oxygen Saturation Measurement on the New-born For Use in: By: For: Division responsible for document: Key words: Name and job title of document author: Name and job title of
Trust Guideline on Routine Oxygen Saturation Measurement on the New-born For Use in: By: For: Division responsible for document: Key words: Name and job title of document author: Name and job title of
A physiological approach to the timing of umbilical cord clamping at birth
 1 Ritchie Centre, MIMR-PHI Institute of Medical Research, Monash University, Melbourne, Victoria, Australia 2 Department of Obstetrics & Gynaecology, Monash University, Melbourne, Victoria, Australia 3
1 Ritchie Centre, MIMR-PHI Institute of Medical Research, Monash University, Melbourne, Victoria, Australia 2 Department of Obstetrics & Gynaecology, Monash University, Melbourne, Victoria, Australia 3
1 Pediatric Advanced Life Support Science Update What s New for 2010? 3 CPR. 4 4 Steps of BLS Survey 5 CPR 6 CPR.
 1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Function: Transportation of. Oxygen Nutrients Waste Hormones gases
 Function: Transportation of Oxygen Nutrients Waste Hormones gases Pericardium: double sac of serous membrane filled with fluid (pericardial fluid to be exact) that surrounds the heart. Parietal pericardium:
Function: Transportation of Oxygen Nutrients Waste Hormones gases Pericardium: double sac of serous membrane filled with fluid (pericardial fluid to be exact) that surrounds the heart. Parietal pericardium:
4/19/2018. St. Cloud Hospital Perinatology Kristin Olson, RDMS, RVT
 St. Cloud Hospital Perinatology Kristin Olson, RDMS, RVT Review Fetal Circulation Provide Indications for Umbilical Artery, Middle Cerebral Artery, and Ductus Venosus Doppler studies. Demonstrate normal
St. Cloud Hospital Perinatology Kristin Olson, RDMS, RVT Review Fetal Circulation Provide Indications for Umbilical Artery, Middle Cerebral Artery, and Ductus Venosus Doppler studies. Demonstrate normal
PALS Case Scenario Testing Checklist Respiratory Case Scenario 1 Upper Airway Obstruction
 Respiratory Case Scenario 1 Upper Airway Obstruction Directs administration of 100% oxygen or supplementary oxygen as needed to support oxygenation Identifies signs and symptoms of upper airway obstruction
Respiratory Case Scenario 1 Upper Airway Obstruction Directs administration of 100% oxygen or supplementary oxygen as needed to support oxygenation Identifies signs and symptoms of upper airway obstruction
Congenital Heart Defects
 Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
End tidal carbon dioxide (ETCO2) and peripheral pulse oximetry (SpO2) trends and right-to-left shunting in neonates undergoing
 End tidal carbon dioxide (ETCO2) and peripheral pulse oximetry (SpO2) trends and right-to-left shunting in neonates undergoing non cardiac surgery under general anesthesia C. Goonasekera, G. Kunst, M.
End tidal carbon dioxide (ETCO2) and peripheral pulse oximetry (SpO2) trends and right-to-left shunting in neonates undergoing non cardiac surgery under general anesthesia C. Goonasekera, G. Kunst, M.
Portal vein catheterization and selective angiography in diagnosis of total anomalous pulmonary venous connexion
 British Heart journal, 974, 36, 155-59. Portal vein catheterization and selective angiography in diagnosis of total anomalous pulmonary venous connexion Michael Tynan, D. Behrendt, W. Urquhart, and G.
British Heart journal, 974, 36, 155-59. Portal vein catheterization and selective angiography in diagnosis of total anomalous pulmonary venous connexion Michael Tynan, D. Behrendt, W. Urquhart, and G.
The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the Edwards PreSep oximetry catheter
 1 2 The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the Edwards PreSep oximetry catheter for continuous central venous oximetry (ScvO2) 3
1 2 The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the Edwards PreSep oximetry catheter for continuous central venous oximetry (ScvO2) 3
Screening for Critical Congenital Heart Disease
 Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
DEVELOPMENT OF THE CIRCULATORY SYSTEM L E C T U R E 5
 DEVELOPMENT OF THE CIRCULATORY SYSTEM L E C T U R E 5 REVIEW OF CARDIAC ANATOMY Heart 4 chambers Base and apex Valves Pericardial sac 3 layers: epi, myo, endo cardium Major blood vessels Aorta and its
DEVELOPMENT OF THE CIRCULATORY SYSTEM L E C T U R E 5 REVIEW OF CARDIAC ANATOMY Heart 4 chambers Base and apex Valves Pericardial sac 3 layers: epi, myo, endo cardium Major blood vessels Aorta and its
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
How to Recognize a Suspected Cardiac Defect in the Neonate
 Neonatal Nursing Education Brief: How to Recognize a Suspected Cardiac Defect in the Neonate https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Neonatal Nursing Education Brief: How to Recognize a Suspected Cardiac Defect in the Neonate https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Delivery Room Resuscitation of Newborns with Congenital Anomalies
 Delivery Room Resuscitation of Newborns with Congenital Anomalies Anne Ades, MD, MSEd Director of Neonatal Education The Children s Hospital of Philadelphia Associate Professor of Clinical Pediatrics Perelman
Delivery Room Resuscitation of Newborns with Congenital Anomalies Anne Ades, MD, MSEd Director of Neonatal Education The Children s Hospital of Philadelphia Associate Professor of Clinical Pediatrics Perelman
Cardiovascular Anatomy Dr. Gary Mumaugh
 Cardiovascular Anatomy Dr. Gary Mumaugh Location of Heart Approximately the size of your fist Location o Superior surface of diaphragm o Left of the midline in mediastinum o Anterior to the vertebral column,
Cardiovascular Anatomy Dr. Gary Mumaugh Location of Heart Approximately the size of your fist Location o Superior surface of diaphragm o Left of the midline in mediastinum o Anterior to the vertebral column,
SWISS SOCIETY OF NEONATOLOGY. Prenatal closure of the ductus arteriosus
 SWISS SOCIETY OF NEONATOLOGY Prenatal closure of the ductus arteriosus March 2007 Leone A, Fasnacht M, Beinder E, Arlettaz R, Neonatal Intensive Care Unit (LA, AR), University Hospital Zurich, Cardiology
SWISS SOCIETY OF NEONATOLOGY Prenatal closure of the ductus arteriosus March 2007 Leone A, Fasnacht M, Beinder E, Arlettaz R, Neonatal Intensive Care Unit (LA, AR), University Hospital Zurich, Cardiology
INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2
 2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
Earlier Use of Inhaled Nitric Oxide in Term and Near-Term Neonates With Hypoxic Respiratory Failure (HRF) and Pulmonary Hypertension (PH)
 Earlier Use of Inhaled Nitric Oxide in Term and Near-Term Neonates With Hypoxic Respiratory Failure (HRF) and Pulmonary Hypertension (PH) 2013 Ikaria, Inc. 1 Disclosure Information This program is sponsored
Earlier Use of Inhaled Nitric Oxide in Term and Near-Term Neonates With Hypoxic Respiratory Failure (HRF) and Pulmonary Hypertension (PH) 2013 Ikaria, Inc. 1 Disclosure Information This program is sponsored
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by
 24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
Neonatal Resuscitation
 Neonatal Resuscitation High Risk Deliveries A person trained in neonatal resuscitation is usually called to be present for the following deliveries: 1. Antepartum factors Maternal diabetes Pregnancy induced
Neonatal Resuscitation High Risk Deliveries A person trained in neonatal resuscitation is usually called to be present for the following deliveries: 1. Antepartum factors Maternal diabetes Pregnancy induced
a. Describe the physiological consequences of intermittent positive pressure ventilation and positive end-expiratory pressure.
 B. 10 Applied Respiratory Physiology a. Describe the physiological consequences of intermittent positive pressure ventilation and positive end-expiratory pressure. Intermittent positive pressure ventilation
B. 10 Applied Respiratory Physiology a. Describe the physiological consequences of intermittent positive pressure ventilation and positive end-expiratory pressure. Intermittent positive pressure ventilation
Chapter 23. Circulation
 Chapter 23 Circulation Standards CORE: I can describe the components and function of blood. I can describe structure and function of blood vessels. I can compare and contrast systemic and pulmonary systems.
Chapter 23 Circulation Standards CORE: I can describe the components and function of blood. I can describe structure and function of blood vessels. I can compare and contrast systemic and pulmonary systems.
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen
 Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION
 CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
Neonatal/Pediatric Cardiopulmonary Care. Persistent Pulmonary Hypertension of the Neonate (PPHN) PPHN. Other. Other Diseases
 Neonatal/Pediatric Cardiopulmonary Care Other Diseases Persistent Pulmonary Hypertension of the Neonate (PPHN) PPHN 3 Also known as Persistent Fetal Circulation (PFC) Seen most frequently in term, post-term
Neonatal/Pediatric Cardiopulmonary Care Other Diseases Persistent Pulmonary Hypertension of the Neonate (PPHN) PPHN 3 Also known as Persistent Fetal Circulation (PFC) Seen most frequently in term, post-term
Patient Ductus Arteriosus (PDA)
 Patient Ductus Arteriosus (PDA) WINSTON HELEN Author: Paediatric Department Document Number: STHK7026 Version: 5 Review date: 30th June 2021 The Normal Heart The Heart is made up of four chambers: the
Patient Ductus Arteriosus (PDA) WINSTON HELEN Author: Paediatric Department Document Number: STHK7026 Version: 5 Review date: 30th June 2021 The Normal Heart The Heart is made up of four chambers: the
Handling Common Problems & Pitfalls During. Oxygen desaturation in patients receiving mechanical ventilation ACUTE SEVERE RESPIRATORY FAILURE
 Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
