9/10/2012. Chapter 49. Learning Objectives. Learning Objectives (Cont d) Thoracic Trauma
|
|
|
- Rachel Johnston
- 5 years ago
- Views:
Transcription
1 Chapter 49 Thoracic Trauma 1 Learning Objectives Explain relevance of thoracic injuries as part of the overall mortality rate from major trauma List thoracic injuries that may result in early death if left untreated by EMS Describe the incidence, morbidity, and mortality rates of thoracic injuries in trauma patients 2 Learning Objectives (Cont d) Discuss types of thoracic injuries Discuss A&P of organs and structures related to thoracic injuries Discuss pathophysiology of thoracic injuries Discuss assessment findings for thoracic injuries 3 1
2 Learning Objectives (Cont d) Discuss management of thoracic injuries Identify need for rapid intervention and transport of patient with thoracic injuries Discuss management of chest wall injuries Describe impact of rib fractures on oxygenation and ventilation 4 Learning Objectives (Cont d) Predict thoracic injuries on the basis of the mechanism of injury Discuss the pathophysiology of specific chest wall injuries, including: Rib fracture Flail segment Sternal fracture 5 Learning Objectives (Cont d) Discuss the management of lung injuries Explain the physiological consequences of flail chest Discuss assessment findings associated with chest wall injuries 6 2
3 Learning Objectives (Cont d) Identify the need for rapid intervention and transport of patient with lung injuries Discuss pathophysiology of traumatic asphyxia Discuss assessment findings associated with traumatic asphyxia 7 Learning Objectives (Cont d) Discuss the management of traumatic asphyxia Identify the need for rapid intervention and transport of patients with traumatic asphyxia Discuss assessment findings associated with lung injuries 8 Learning Objectives (Cont d) Discuss the pathophysiology of injury to the lung, including: Simple pneumothorax Open pneumothorax Tension pneumothorax Hemothorax Hemopneumothorax Pulmonary contusion 9 3
4 Learning Objectives (Cont d) Define pneumothorax and hemothorax List the signs and symptoms of tension pneumothorax Identify the need for rapid intervention and transport of patients with chest wall injuries 10 Learning Objectives (Cont d) Discuss the pathophysiology of tracheobronchial injuries Discuss assessment findings associated with tracheobronchial injuries Discuss the management of tracheobronchial injuries 11 Learning Objectives (Cont d) Identify the need for rapid intervention and transport of patients with tracheobronchial injuries Discuss the pathophysiology of myocardial injuries, including: Pericardial tamponade Myocardial contusion Myocardial rupture 12 4
5 Learning Objectives (Cont d) Discuss assessment findings for myocardial injuries Discuss management of myocardial injuries Define Beck s triad Identify need for rapid intervention and transport 13 Learning Objectives (Cont d) Describe pathophysiology of aortic rupture Discuss pathophysiology of vascular injuries, including injuries to: aorta, venae cavae, & pulmonary arteries and veins Discuss assessment findings for vascular injuries 14 Learning Objectives (Cont d) Discuss the management of vascular injuries Identify the need for rapid intervention and transport of patient with vascular injuries Discuss the pathophysiology of diaphragmatic injuries 15 5
6 Learning Objectives (Cont d) Discuss assessment findings associated with diaphragmatic injuries Discuss the management of diaphragmatic injuries Identify the need for rapid intervention and transport of patients with diaphragmatic injuries 16 Learning Objectives (Cont d) Discuss the pathophysiology of esophageal injuries Discuss assessment findings associated with esophageal injuries Discuss the management of esophageal injuries 17 Learning Objectives (Cont d) Identify the need for rapid intervention and transport of patients with esophageal injuries 18 6
7 Introduction Thoracic injuries directly account for 20 25% of trauma deaths Most common cause of injuries leading to accidental deaths in the United States is motor vehicles crashes 19 Chest Wall Injuries Most common injury of thorax Account for more than 50% of blunt trauma cases
8 Rib fracture Most common significant chest injury Fourth to ninth most commonly fractured thin and poorly protected First to third suggests high-velocity trauma Ninth to eleventh suggests intraabdominal injury 22 Rib fracture Left lower rib injury splenic injury Posterior rib fractures fifth to ninth most frequently fractured Lower posterior rib fractures spleen and kidney injury Open rib fracture visceral injury 2+ rib fractures internal injury 23 Rib fracture Multiple rib fractures possible results: Atelectasis Hypoventilation Inadequate cough Pneumonia 24 8
9 Rib fracture History and physical findings Tenderness Bony crepitus Ecchymosis Muscle spasm over ribs Localized pain Pain worsens with movement, deep breathing, coughing Splinting on respiration Anteroposterior pressure that elicits pain 25 Rib fracture Therapeutic interventions Transport to trauma center Monitor respiratory status Pain relief Maintain pulmonary function O 2, pulse oximeter, positive-pressure ventilation Capnography Encourage coughing, deep breathing No restrictive devices Administer opiate analgesics per local protocols 26 Sternal fracture and dislocation Caused by anterior blunt chest trauma Blow to chest Severe hyperflexion of thoracic cage Deceleration compression injury 27 9
10 Sternal fracture and dislocation Mortality rate of 25 45% Myocardial and pulmonary contusion Myocardial rupture Flail chest Vascular disruption of thoracic vessels Intraabdominal injuries Head injuries 28 Sternal fracture and dislocation History and physical findings Primary concerns Myocardial contusion Cardiac rupture Tamponade Pulmonary injury Point tenderness Crepitus Deformity Pain over sternum 29 Sternal fracture and dislocation Assessment findings History of blunt anterior chest trauma Localized anterior chest pain Point tenderness over sternum Soft tissue swelling Palpable deformity Crepitus Tachypnea ECG changes associated with myocardial contusion 30 10
11 Sternal fracture and dislocation Therapeutic interventions O 2, pulse oximeter, positive-pressure ventilation Capnography Cardiac monitor Opiate analgesics by IV per medical direction Flail chest 2+ adjacent ribs fractured at two points allowing freely moving segment of chest wall to move in paradoxic motion Common association with pulmonary contusion Flail segment moves inward with inspiration, outward with expiration 33 11
12 34 35 Flail chest History and physical findings Underlying pulmonary contusion Assessment findings Chest wall contusion Respiratory distress Paradoxic chest wall movement Pleuritic chest pain Crepitus Pain and splinting of affected side Tachypnea Tachycardia 36 12
13 Flail chest Therapeutic interventions High-flow O 2 Cardiac monitor, pulse oximetry Monitor for respiratory failure ET Continuous positive airway pressure by mask may be in place of ET 37 Nonpenetrating ballistic injury Body armor Can produce significant injury without penetration Heart Liver Spleen Lung Spinal cord 38 Nonpenetrating ballistic injury History and physical findings Redness Bruising Marked tenderness to palpation Palpate surrounding structures for subcutaneous emphysema, crepitus, bony step-offs Therapeutic interventions Transport Possible underlying injury 39 13
14 Traumatic asphyxia Deep purple skin color of head and neck Bilateral subconjunctival hemorrhage Petechiae Facial edema 40 Traumatic asphyxia Caused by severe compression of chest by extremely heavy object Marked increase in pressure in chest and superior vena cava Backflow of blood from right heart to great veins of head and neck Pressure transmitted to capillaries of head and neck, engorge with blood Blood stagnates Skin becomes purple 41 Traumatic asphyxia History and physical findings Benign condition, self-limiting Possible intrathoracic injury Chest wall and pulmonary injuries most common Visual disturbances 42 14
15 Traumatic asphyxia Assessment findings Cyanosis to face and upper neck Jugular venous distention Facial swelling Swelling or hemorrhage of conjunctiva Skin below compressed area remains pink Hypotension when compressive force is released 43 Traumatic asphyxia Therapeutic interventions Trauma center evaluation High-flow O 2 Cardiac monitor, pulse oximetry IV access 44 Pulmonary Injuries Subcutaneous emphysema Presence of air in soft tissue space Up to the neck and down to groin 45 15
16 Subcutaneous emphysema History and physical findings Over chest wall indicates pneumothorax Crunching sensation on chest wall palpation Esophageal tear from penetrating injury produces pneumomediastinum Massive accumulation uncomfortable Therapeutic interventions Consider transport No prehospital treatment 46 Pulmonary contusion Direct bruise of the lung tissue Bleeding and edema in alveolar spaces Buildup of blood, fluid, inflammatory components impairs oxygenation, causes respiratory distress Great force needed 47 Pulmonary contusion History and physical findings Present with varying degrees of dyspnea Crackles Diminished breath sounds Absent breath on auscultation over affected area Possible rib fractures 48 16
17 Pulmonary contusion History and physical findings Blunt trauma cases: Hematomas Ecchymoses Tenderness Abrasions Lacerations 49 Pulmonary contusion History and physical findings Assessment findings Tachypnea Tachycardia Cough Hemoptysis Apprehension Respiratory distress Dyspnea Cyanosis Chest wall bruising 50 Pulmonary contusion Therapeutic interventions Do not focus on more dramatic injuries and overlook pulmonary contusion Hypoxic High-flow O 2 Pulse oximeter, cardiac monitor Capnography IV access Rapid transport 51 17
18 Accumulation of air in pleural space Common complication of chest trauma Present in 15 50% of penetrating trauma 52 Simple pneumothorax When no communication with atmosphere exists Mediastinum/diaphragm has not shifted as result of air 53 Simple pneumothorax History and physical findings Small tears may resolve on own Assessment findings Tachypnea Tachycardia Respiratory distress Absent or decreased breath sounds on affected side Hyperresonance Decreased chest wall movement Dyspnea Chest pain referred to shoulder or arm on affected side Slight pleuritic chest pain 54 18
19 Simple pneumothorax Therapeutic interventions Oxygenation and ventilation Pulse oximeter, cardiac monitor IV access Capnography Spinal stabilization if warranted Open pneumothorax Injury penetrates chest wall and pleura Enters pleural cavity Lung collapse Open connection between pleural space and environment 57 19
20 Open pneumothorax Assessment findings Defect in chest wall To-and-fro air motion out of defect Penetrating injury to chest, does not seal itself Sucking sound on inhalation (sucking chest wound) Tachypnea Tachycardia Respiratory distress Subcutaneous emphysema Decreased breath sounds on affected side 58 Open pneumothorax Therapeutic interventions Recognition critical Occlusive dressing Never pack wound Tape on three sides Oxygenation and ventilation Pulse oximeter, cardiac monitor, capnography IV access Spinal mobilization if warranted Observe for developing tension pneumothorax
21 Tension pneumothorax Progressive accumulation of air under pressure within the pleural cavity Shifts chest contents to the opposite side Opposite lung and great vessels compression Acts as one-way valve, prevents free bilateral communication Increase in intrapleural pressure 61 Tension pneumothorax Air enters on inspiration, cannot exit with expiration Compresses venae cavae Decreases filling of heart, decreased cardiac output Hypoxia Respiratory distress Shock Can progress to prevent heart from contracting or opposite lung moving air Suffocation 62 Tension pneumothorax Assessment findings Hyperinflation of affected side Poor ventilation despite open airway Restlessness, agitation, extreme anxiety Increased airway resistance on ventilating patient Respiratory distress Neck vein distention Decreased or absent breath sounds on affected side 63 21
22 Tension pneumothorax Assessment findings Tympany (hyperresonance) to percussion on affected side Tachycardia Signs of shock Tracheal deviation away from side of injury Cyanosis Bulging of intercostal muscles Narrow pulse pressure Subcutaneous emphysema 64 Tension pneumothorax Therapeutic interventions High-flow O 2 Pulse oximeter, cardiac monitor Capnography IV access Emergent needle compression on affected lung
23 67 Skill 49-1: Needle Decompression Standard precautions Prepare necessary equipment for needle thoracostomy 68 Skill 49-1: Needle Decompression (Cont d) Expose chest and identify landmarks Palpate from angle of Louis across second rib and locate third rib at mid-clavicular line 69 23
24 Skill 49-1: Needle Decompression (Cont d) Cleanse site Insert 14- or 16- gauge over-theneedle catheter to skin over top of third rib and into second intercostal space, midclavicular line 70 Skill 49-1: Needle Decompression (Cont d) 71 Skill 49-1: Needle Decompression (Cont d) Attach flutter valve to catheter hub Secure catheter to patient s chest wall with dressing and tape 72 24
25 Skill 49-1: Needle Decompression (Cont d) Reassess breath sounds, respiratory status and vital signs Notify medical direction of procedure 73 Pulmonary Injuries Hemothorax Collection of blood within pleural cavity Caused by blunt or penetrating trauma to chest Capillaries or small blood vessels bleed into pleural cavity Blood displaces lung, reduces air space Possible hypovolemic shock Compromised ventilation 74 Hemothorax History and physical findings Patient complains of initial injury, does not notice dyspnea Nontraumatic hemothorax uncommon Auscultation reveals decreased breath sounds in lower lobes when patient is sitting up 75 25
26 Hemothorax Therapeutic interventions Adequate oxygenation and ventilation Pulse oximeter, cardiac monitor IV access, minimize fluids Capnography Spinal immobilization only when necessary 76 Hemopneumothorax with bleeding in pleural space Usually caused by penetrating trauma Similar signs and symptoms as hemothorax Similar treatment as hemothorax Watch for development of possible tension pneumothorax 77 Hemopneumothorax History and physical findings Dyspnea Tachypnea Tachycardia Hypotension Shock Rib crepitus Flail segments Subcutaneous emphysema Absent breath sounds Hyperresonance on percussion 78 26
27 Hemopneumothorax Therapeutic interventions Airway control and oxygenation 100% O 2 by nonrebreather mask IV access Pulse oximeter, cardiac monitor Capnography 79 Hemopneumothorax Watch for tension pneumothorax Increasing distress Dropping BP Increasing tachycardia Dropping O 2 saturations Rapid transport 80 Tracheobronchial injury Blunt or penetrating trauma of neck or chest Direct blow to neck may transect tracheal rings or cricoids cartilage Respiratory distress Hypoxia Hemoptysis Subcutaneous emphysema 81 27
28 Tracheobronchial injury History and physical findings Wound opens into pleural space, produces large pneumothorax Complete transaction of tracheobronchial tree, no communication with pleural space 82 Tracheobronchial injury Therapeutic interventions Rapid transport Caution if blind intubation, ET tube through transected airway 83 Cardiovascular Trauma Cardiac contusion Large force applied to chest wall High-speed deceleration injuries Sternum displaced posteriorly Heart compressed between sternum and chest 84 28
29 Cardiovascular Trauma (Cont d) Cardiac contusion History and physical findings Varied, nonspecific Pain and shock or benign Blunt cardiac injury likely has additional abdominal, skeletal, or CNS injury 85 Cardiovascular Trauma (Cont d) Cardiac contusion History and physical findings Associated injuries Pulmonary contusion Pneumothorax Hemothorax External fracture Great vessel injury Cardiac output reduction may manifest as shock 86 Cardiovascular Trauma (Cont d) Cardiac contusion History and physical findings Right ventricle more likely injured Least specific sign: sinus tachycardia ECG: right bundle branch block 87 29
30 Cardiovascular Trauma (Cont d) Cardiac contusion History and physical findings Information to ED MOI Status of motor vehicle Steering wheel/dashboard damage Seatbelt use Air bag deployment Estimated speed of vehicle before crash Position of patient when found 88 Cardiovascular Trauma (Cont d) Cardiac contusion Therapeutic intervention Rapid transport High-flow O 2 Cardiac monitor IV access en route, analgesic agents Fibrinolytic agents and aspirin contraindicated 89 Cardiovascular Trauma (Cont d) Pericardial tamponade Accumulation of fluid (blood) in pericardial space that impedes cardiac filling and cardiac output Pericardial fluid volume increases, ventricles restrict and are unable to fill Decreased cardiac output Decreased systolic BP Pulse pressure decreased Suspect pericardial tamponade in penetrating or blunt trauma to chest/upper abdomen 90 30
31 Cardiovascular Trauma (Cont d) Pericardial tamponade History and physical findings Hypotension Distended neck veins Distant muffled heart tones Significant blood loss from other injuries precludes jugular venous distention (JVD) Most reliable signs: JVD in association with hypotension and tachycardia Pulsus paradoxus 91 Cardiovascular Trauma (Cont d) Cardiac rupture Acute traumatic perforation of ventricles or atria High-speed MVCs Most common cause of death in nonpenetrating cardiac injuries One-third multiple chamber rupture One-quarter ascending aortic rupture 92 Cardiovascular Trauma (Cont d) Cardiac rupture Epidemiology and demographics Almost always immediately fatal 15% of fatal thoracic injuries Most survivors from atrial rupture Multisystem injuries common 93 31
32 Cardiovascular Trauma (Cont d) Cardiac rupture History and physical findings Hypotension Tachycardia Distended neck veins Cyanosis of head, neck, arms, upper chest Unresponsiveness Distant heart sounds Chest injuries 94 Cardiovascular Trauma (Cont d) Cardiac rupture Therapeutic interventions Oxygenation and ventilation Pulse oximeter Capnography IV access Cardiac monitor Rapid transport 95 Injury to Great Vessels Aortic rupture Thoracic aorta is most common vessel injured by blunt trauma 80 90% occur in descending aorta, distal to left subclavian artery Pericardial tamponade Aortic valve tears Myocardial contusion Coronary artery injuries Rarely survive 96 32
33 Injury to Great Vessels (Cont d) Aortic rupture History and physical findings High-speed MVC deceleration Vertical deceleration Associated injuries Pulmonary Neurological Orthopedic Facial Abdominal 97 Injury to Great Vessels (Cont d) Aortic rupture History and physical findings Symptoms Interscapular or retrosternal pain Dyspnea Stridor or hoarseness Dysphagia Extremity pain Hypertension Pseudocoarctation syndrome 98 Injury to Great Vessels (Cont d) Aortic rupture Therapeutic interventions Find MOI compatible with aortic rupture Treat hypotension, tension pneumothorax, cardiac tamponade Relay information to ED Rapid transport 99 33
34 Injury to Great Vessels (Cont d) Injury to venae cavae or pulmonary vessels Associated with injuries to chest, abdomen, or neck Injuries to vena cava, inferior vena cava, pulmonary arteries, four main pulmonary veins accompanied by: Massive hemothorax Hypovolemic shock Cardiac tamponade 100 Diaphragmatic Injuries Description and definition Direct penetration of diaphragm Blunt forces to chest or abdomen Therapeutic interventions Awareness of injury Transport 101 Esophageal Injuries Description and definition Usually not isolated injury Cervical esophageal injuries most common Trachea most common site of injury
35 Esophageal Injuries (Cont d) History and physical findings Neck pain Difficulty swallowing Cough Voice changes Hematemesis 103 Esophageal Injuries (Cont d) History and physical findings Physical findings Neck tenderness Resistance to flexion Crepitus Stridor Airway compromise 104 Esophageal Injuries (Cont d) Therapeutic interventions Rapid-sequence intubation Surgical airway Rapid transport
36 Chapter Summary Thoracic trauma includes a wide range of injuries, many of which may result in death if not recognized early Must be able to identify and treat these injuries rapidly to provide potentially lifesaving care 106 Questions?
Medical NREMT-PTE. NREMT Paramedic Trauma Exam.
 Medical NREMT-PTE NREMT Paramedic Trauma Exam https://killexams.com/pass4sure/exam-detail/nremt-pte Question: 41 Which of the following most accurately describes the finding of jugular venous distension
Medical NREMT-PTE NREMT Paramedic Trauma Exam https://killexams.com/pass4sure/exam-detail/nremt-pte Question: 41 Which of the following most accurately describes the finding of jugular venous distension
Chest Trauma.
 Chest Trauma www.fisiokinesiterapia.biz Objectives Anatomy of Thorax Main Causes of Chest Injuries S/S of Chest Injuries Different Types of Chest Injuries Treatments of Chest Injuries Anatomy of the chest
Chest Trauma www.fisiokinesiterapia.biz Objectives Anatomy of Thorax Main Causes of Chest Injuries S/S of Chest Injuries Different Types of Chest Injuries Treatments of Chest Injuries Anatomy of the chest
Chapter 29 - Chest Injuries
 1 2 3 4 5 6 7 8 9 National EMS Education Standard Competencies (1 of 5) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
1 2 3 4 5 6 7 8 9 National EMS Education Standard Competencies (1 of 5) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
CHEST TRAUMA. Dr Naeem Zia FCPS,FACS,FRCS
 CHEST TRAUMA Dr Naeem Zia FCPS,FACS,FRCS Learning objectives Anatomy of chest wall and thoracic viscera Physiology of respiration and nerve pathways for pain Enumerate different thoracic conditions requiring
CHEST TRAUMA Dr Naeem Zia FCPS,FACS,FRCS Learning objectives Anatomy of chest wall and thoracic viscera Physiology of respiration and nerve pathways for pain Enumerate different thoracic conditions requiring
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
Chapter 29 - Chest_and_Abdominal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 29.1 Define key terms introduced in this chapter. Slides 11, 15, 18, 27 29.2 Describe mechanisms of injury commonly associated with chest injuries. Slides
Introduction to Emergency Medical Care 1 OBJECTIVES 29.1 Define key terms introduced in this chapter. Slides 11, 15, 18, 27 29.2 Describe mechanisms of injury commonly associated with chest injuries. Slides
PRE-HOSPITAL EMERGENCY CARE COURSE.
 PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
The Management of Chest Trauma. Tom Scaletta, MD FAAEM Immediate Past President, AAEM
 The Management of Chest Trauma Tom Scaletta, MD FAAEM Immediate Past President, AAEM Trichotomizing Rib Fractures Upper 1-3 vascular injuries Middle 4-9 Lower 10-12 12 liver/spleen injuries Management
The Management of Chest Trauma Tom Scaletta, MD FAAEM Immediate Past President, AAEM Trichotomizing Rib Fractures Upper 1-3 vascular injuries Middle 4-9 Lower 10-12 12 liver/spleen injuries Management
The ABC s of Chest Trauma
 The ABC s of Chest Trauma J Bradley Pickhardt MD, FACS Providence St Patrick Hospital What s the Problem? 2/3 of trauma patients have chest trauma Responsible for 25% of all trauma deaths Most injuries
The ABC s of Chest Trauma J Bradley Pickhardt MD, FACS Providence St Patrick Hospital What s the Problem? 2/3 of trauma patients have chest trauma Responsible for 25% of all trauma deaths Most injuries
In ESH we usually see blunt chest trauma but penetrating injuries also treated here (usually as single injuries, like stab wound)
 Chest Trauma Dr Csaba Dioszeghy MD PhD FRCEM FFICM FERC East Surrey Hospital Emergency Department Scope Thoracic injuries are common and can be life threatening In ESH we usually see blunt chest trauma
Chest Trauma Dr Csaba Dioszeghy MD PhD FRCEM FFICM FERC East Surrey Hospital Emergency Department Scope Thoracic injuries are common and can be life threatening In ESH we usually see blunt chest trauma
Chapter 34. Objectives. Objectives 01/09/2013. Chest Trauma
 Chapter 34 Chest Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced
Chapter 34 Chest Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced
Imaging of Thoracic Trauma: Tips and Traps. Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania
 Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Chapter 13. Injuries to the Thorax and Abdomen
 Chapter 13 Injuries to the Thorax and Abdomen Anatomy Review Thoracic cage has 12 pairs of ribs. The first 7 pairs connect directly to sternum. Pairs 8 through 10 connect via common costal cartilage. Pairs
Chapter 13 Injuries to the Thorax and Abdomen Anatomy Review Thoracic cage has 12 pairs of ribs. The first 7 pairs connect directly to sternum. Pairs 8 through 10 connect via common costal cartilage. Pairs
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Aurora Health Care EMS Continuing Education Spring 2011 Packet THORACIC TRAUMA THE PREHOSPITAL APPROACH TO CHEST INJURY MANAGEMENT
 Aurora Health Care EMS Continuing Education Spring 2011 Packet THORACIC TRAUMA Chest injuries are significant contributors to death from major trauma and can be difficult to assess adequately in the pre-hospital
Aurora Health Care EMS Continuing Education Spring 2011 Packet THORACIC TRAUMA Chest injuries are significant contributors to death from major trauma and can be difficult to assess adequately in the pre-hospital
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma Penetrating neck injury (PNI) comprises 5 to 10 percent of traumatic injuries
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma Penetrating neck injury (PNI) comprises 5 to 10 percent of traumatic injuries
ITLS Advanced Pre-Test Annotated Key 8 th Edition
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D.
 1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
CHEST INJURIES. Jacek Piątkowski M.D., Ph. D.
 CHEST INJURIES Jacek Piątkowski M.D., Ph. D. CHEST INJURIES 3-4% of all injuries 8% of patients hospitalized due to injuries 65% of patients who died at the accident place CLASSIFICATION OF THE CHEST INJURIES
CHEST INJURIES Jacek Piątkowski M.D., Ph. D. CHEST INJURIES 3-4% of all injuries 8% of patients hospitalized due to injuries 65% of patients who died at the accident place CLASSIFICATION OF THE CHEST INJURIES
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
Focused History and Physical Examination of the
 Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Critical Care Monitoring. Indications. Pleural Space. Chest Drainage. Chest Drainage. Potential space. Contains fluid lubricant
 Critical Care Monitoring Indications 1-2- 2 Pleural Space Potential space Contains fluid lubricant Can fill with air, blood, plasma, serum, lymph, pus 3 1 Pleural Space Problems when contain abnormal substances:
Critical Care Monitoring Indications 1-2- 2 Pleural Space Potential space Contains fluid lubricant Can fill with air, blood, plasma, serum, lymph, pus 3 1 Pleural Space Problems when contain abnormal substances:
Northwest Community EMS System September 2017: Head and Chest Trauma Credit Questions
 NWC EMSS Sept 2017 CE: Head & Chest Trauma. Credit Questions - page 1 Northwest Community EMS System September 2017: Head and Chest Trauma Credit Questions Name: EMS Agency EMSC/Educator reviewer: Date
NWC EMSS Sept 2017 CE: Head & Chest Trauma. Credit Questions - page 1 Northwest Community EMS System September 2017: Head and Chest Trauma Credit Questions Name: EMS Agency EMSC/Educator reviewer: Date
Purpose This Operating Procedure provides guidance on the management of blunt thoracic traumatic injury
 Blunt Thoracic Trauma HELI.CLI.09 Purpose This Operating Procedure provides guidance on the management of blunt thoracic traumatic injury Procedure Management of Blunt Thoracic Traumatic Injury For Review
Blunt Thoracic Trauma HELI.CLI.09 Purpose This Operating Procedure provides guidance on the management of blunt thoracic traumatic injury Procedure Management of Blunt Thoracic Traumatic Injury For Review
Chapter 3: Thorax. Thorax
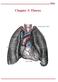 Chapter 3: Thorax Thorax Thoracic Cage I. Thoracic Cage Osteology A. Thoracic Vertebrae Basic structure: vertebral body, pedicles, laminae, spinous processes and transverse processes Natural kyphotic shape,
Chapter 3: Thorax Thorax Thoracic Cage I. Thoracic Cage Osteology A. Thoracic Vertebrae Basic structure: vertebral body, pedicles, laminae, spinous processes and transverse processes Natural kyphotic shape,
The Primary Survey. C. Clay Cothren, MD FACS. Attending Surgeon, Denver Health Medical Center Assistant Professor of Surgery, University of Colorado
 The Primary Survey C. Clay Cothren, MD FACS Attending Surgeon, Denver Health Medical Center Assistant Professor of Surgery, University of Colorado Outlining the ABCs Why do we need such an approach? The
The Primary Survey C. Clay Cothren, MD FACS Attending Surgeon, Denver Health Medical Center Assistant Professor of Surgery, University of Colorado Outlining the ABCs Why do we need such an approach? The
Professional Development & Training MM3. Firefighter Prehospital Care Program. Maintenance Module 3 Course Mill Version
 Professional Development & Training MM3 Firefighter Prehospital Care Program F T Maintenance Module 3 Course Mill Version S Objectives Upon successful completion of the Firefighter Prehospital Care Maintenance
Professional Development & Training MM3 Firefighter Prehospital Care Program F T Maintenance Module 3 Course Mill Version S Objectives Upon successful completion of the Firefighter Prehospital Care Maintenance
PEDIATRIC TRAUMA: Implications for Respiratory Care
 PEDIATRIC TRAUMA: Implications for Respiratory Care 17 th Annual Rainbow Respiratory Conference - September 4, 2015 Mike Dingeldein, MD Pediatric Surgeon Pediatric Trauma Medical Director Disclosures none
PEDIATRIC TRAUMA: Implications for Respiratory Care 17 th Annual Rainbow Respiratory Conference - September 4, 2015 Mike Dingeldein, MD Pediatric Surgeon Pediatric Trauma Medical Director Disclosures none
oriented evaluation of your patient and establishing priorities of care based on existing and
 1 Chapter 12: Patient Assessment in the Field 2 Patient assessment means conducting a - oriented evaluation of your patient and establishing priorities of care based on existing and potential threats to
1 Chapter 12: Patient Assessment in the Field 2 Patient assessment means conducting a - oriented evaluation of your patient and establishing priorities of care based on existing and potential threats to
 55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
INJURIES CHEST, ABDOMEN, LIMBS. FN Brno November 2011
 INJURIES CHEST, ABDOMEN, LIMBS FN Brno November 2011 Injury Chest Abdomen Limbs Injury to the rib cage Fractured one or more ribs Sharp pain at the site of fracture Pain on taking a deep breath Shallow
INJURIES CHEST, ABDOMEN, LIMBS FN Brno November 2011 Injury Chest Abdomen Limbs Injury to the rib cage Fractured one or more ribs Sharp pain at the site of fracture Pain on taking a deep breath Shallow
BIOE221. Session 5. Examination of Thorax- Respiratory system. Bioscience Department. Endeavour College of Natural Health endeavour.edu.
 BIOE221 Session 5 Examination of Thorax- Respiratory system Bioscience Department Session Objectives Understand the structure of the thorax and the organs contained in this cavity Understand the importance
BIOE221 Session 5 Examination of Thorax- Respiratory system Bioscience Department Session Objectives Understand the structure of the thorax and the organs contained in this cavity Understand the importance
CHEST INJURY PULMONARY CONTUSION
 CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
Adult Intubation Skill Sheet
 Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Hypotension / Shock. Adult Medical Section Protocols. Protocol 30
 Hypotension / Shock History Blood loss - vaginal or gastrointestinal bleeding, AAA, ectopic Fluid loss - vomiting, diarrhea, fever nfection Cardiac ischemia (M, CHF) Medications Allergic reaction regnancy
Hypotension / Shock History Blood loss - vaginal or gastrointestinal bleeding, AAA, ectopic Fluid loss - vomiting, diarrhea, fever nfection Cardiac ischemia (M, CHF) Medications Allergic reaction regnancy
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT NC ITLS Rev. 2/18 STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT What to wear ITLS is a practical course that stresses hands-on teaching. You should wear comfortable
INTERNATIONAL TRAUMA LIFE SUPPORT NC ITLS Rev. 2/18 STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT What to wear ITLS is a practical course that stresses hands-on teaching. You should wear comfortable
Thoracic Trauma The Spectrum
 Thoracic Trauma The Spectrum Joseph Mathew Consultant, s & Emergency dept. 2 Thoracic Trauma Responsible for 20-25% of all deaths attributed to trauma. Contributing cause of death in an additional 25%
Thoracic Trauma The Spectrum Joseph Mathew Consultant, s & Emergency dept. 2 Thoracic Trauma Responsible for 20-25% of all deaths attributed to trauma. Contributing cause of death in an additional 25%
Introduction (1 of 3)
 Chapter 10 Shock Introduction (1 of 3) Shock (hypoperfusion) means a state of collapse and failure of the cardiovascular system. In the early stages, the body attempts to maintain homeostasis. As shock
Chapter 10 Shock Introduction (1 of 3) Shock (hypoperfusion) means a state of collapse and failure of the cardiovascular system. In the early stages, the body attempts to maintain homeostasis. As shock
Face and Throat Injuries. Chapter 26
 Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
1. Which of the following organs is contained in the retroperitoneal region of the abdomen? A. Stomach B. Liver C. Kidney D.
 1. Which of the following organs is contained in the retroperitoneal region of the abdomen? A. Stomach B. Liver C. Kidney D. Uterus 2. What is Sellick's maneuver? A. A method allowing the rescuer to hold
1. Which of the following organs is contained in the retroperitoneal region of the abdomen? A. Stomach B. Liver C. Kidney D. Uterus 2. What is Sellick's maneuver? A. A method allowing the rescuer to hold
PARA107 Summary. Page 1-3: Page 4-6: Page 7-10: Page 11-13: Page 14-17: Page 18-21: Page 22-25: Page 26-28: Page 29-33: Page 34-36: Page 37-38:
 PARA107 Summary Page 1-3: Page 4-6: Page 7-10: Page 11-13: Page 14-17: Page 18-21: Page 22-25: Page 26-28: Page 29-33: Page 34-36: Page 37-38: Injury, Mechanisms of Injury, Time Critical Guidelines Musculoskeletal
PARA107 Summary Page 1-3: Page 4-6: Page 7-10: Page 11-13: Page 14-17: Page 18-21: Page 22-25: Page 26-28: Page 29-33: Page 34-36: Page 37-38: Injury, Mechanisms of Injury, Time Critical Guidelines Musculoskeletal
Internal Injury Documentation Guidelines
 Internal Injury Documentation Guidelines General Open Wound of Thorax Injury to Heart Identify episode of care Initial Subsequent Sequela Laterality Sequela of injury Place of occurrence of injury Activity
Internal Injury Documentation Guidelines General Open Wound of Thorax Injury to Heart Identify episode of care Initial Subsequent Sequela Laterality Sequela of injury Place of occurrence of injury Activity
Techniques of examination of the thorax and lungs. Dr. Szathmári Miklós Semmelweis University First Department of Medicine 24. Sept
 Techniques of examination of the thorax and lungs Dr. Szathmári Miklós Semmelweis University First Department of Medicine 24. Sept. 2013. Inspection of the thorax Observe: the shape of chest Deformities
Techniques of examination of the thorax and lungs Dr. Szathmári Miklós Semmelweis University First Department of Medicine 24. Sept. 2013. Inspection of the thorax Observe: the shape of chest Deformities
Thoracic trauma. 1 The majority of deaths occur after the. FEBRUARY 2001 The Surgical Technologist
 Thoracic trauma Richard Wills, MD, MBA, ACSM, Michael Norton, DC, and Kathryn DeLaney Approximately 25% of nonmilitary trauma-related deaths are due to thoracic trauma. 1 The majority of deaths occur after
Thoracic trauma Richard Wills, MD, MBA, ACSM, Michael Norton, DC, and Kathryn DeLaney Approximately 25% of nonmilitary trauma-related deaths are due to thoracic trauma. 1 The majority of deaths occur after
5/2/2018. Notice. Putting Humpty Dumpty Back Together Again
 Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
HEALTH ASSESSMENT. Afnan Tunsi BSN, RN, MSc.
 HEALTH ASSESSMENT Afnan Tunsi BSN, RN, MSc. Learning Outcomes 2 After completion of this lecture, the student will be able to: Describe suggested sequencing to conduct a thorax and lungs physical health
HEALTH ASSESSMENT Afnan Tunsi BSN, RN, MSc. Learning Outcomes 2 After completion of this lecture, the student will be able to: Describe suggested sequencing to conduct a thorax and lungs physical health
Dana Alrafaiah. - Moayyad Al-Shafei. -Mohammad H. Al-Mohtaseb. 1 P a g e
 - 6 - Dana Alrafaiah - Moayyad Al-Shafei -Mohammad H. Al-Mohtaseb 1 P a g e Quick recap: Both lungs have an apex, base, mediastinal and costal surfaces, anterior and posterior borders. The right lung,
- 6 - Dana Alrafaiah - Moayyad Al-Shafei -Mohammad H. Al-Mohtaseb 1 P a g e Quick recap: Both lungs have an apex, base, mediastinal and costal surfaces, anterior and posterior borders. The right lung,
Shot Through the Heart (And You re to Blame): Penetrating Cardiac Trauma
 Shot Through the Heart (And You re to Blame): Penetrating Cardiac Trauma Yalaunda M. Thomas, MD, FACS The American College of Osteopathic Emergency Physicians Spring Seminar April 5, 2018 Disclosures I
Shot Through the Heart (And You re to Blame): Penetrating Cardiac Trauma Yalaunda M. Thomas, MD, FACS The American College of Osteopathic Emergency Physicians Spring Seminar April 5, 2018 Disclosures I
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
The Primary Survey. Clay Cothren Burlew, MD FACS
 The Primary Survey Clay Cothren Burlew, MD FACS Director, Surgical Intensive Care Unit Attending Surgeon, Denver Health Medical Center Associate Professor of Surgery, University of Colorado Outlining the
The Primary Survey Clay Cothren Burlew, MD FACS Director, Surgical Intensive Care Unit Attending Surgeon, Denver Health Medical Center Associate Professor of Surgery, University of Colorado Outlining the
Advances in MDCT of Thoracic Trauma
 Baltic Congress of Radiology, Riga 2010 Advances in MDCT of Thoracic Trauma Robert A. Novelline, MD Professor of Radiology, Harvard Medical School Director of Emergency Radiology, Massachusetts General
Baltic Congress of Radiology, Riga 2010 Advances in MDCT of Thoracic Trauma Robert A. Novelline, MD Professor of Radiology, Harvard Medical School Director of Emergency Radiology, Massachusetts General
7. Hypovolemic shock caused by severe burns is the result of a loss of: A) plasma. B) platelets. C) whole blood. D) red blood cells.
 Name: Date: 1. When parking your ambulance at the scene of a motor vehicle crash, you should position the ambulance: A) 50 past the scene on the opposite side of the road. B) 100 past the scene on the
Name: Date: 1. When parking your ambulance at the scene of a motor vehicle crash, you should position the ambulance: A) 50 past the scene on the opposite side of the road. B) 100 past the scene on the
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Basic Assessment and Treatment of Trauma
 Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Respiratory Assessment
 Module Four Physical examination of Respiratory Assessment 1 THORACIC CAGE: Anterior thoracic cage Posterior thoracic cage 2 Reference lines: Anterior vertical lines Lateral vertical line Posterior vertical
Module Four Physical examination of Respiratory Assessment 1 THORACIC CAGE: Anterior thoracic cage Posterior thoracic cage 2 Reference lines: Anterior vertical lines Lateral vertical line Posterior vertical
: TORSO & PELVIC TRAUMA
 INTRODUCTION Torso injuries include those involving the chest, back, flanks, and abdomen. This guideline also includes assessment and management of pelvic injuries. Neurological Trauma guideline and Management
INTRODUCTION Torso injuries include those involving the chest, back, flanks, and abdomen. This guideline also includes assessment and management of pelvic injuries. Neurological Trauma guideline and Management
Bronchoconstriction is also treated with medications that inhibit bronchiolar constriction such as: Ipratropium (Atrovent)
 Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Penetrating Trauma in Pediatric Patients. Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017
 Penetrating Trauma in Pediatric Patients Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017 Introduction Trauma is the leading cause of death between ages of 1-18 years Penetrating injury accounts
Penetrating Trauma in Pediatric Patients Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017 Introduction Trauma is the leading cause of death between ages of 1-18 years Penetrating injury accounts
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Advanced Assessment and Treatment of Trauma
 Advanced Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls
Advanced Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls
Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous structures - Significant thoracic inj
 PEDIATRIC CHEST TRAUMA Children are not small adults Role of imaging Spectrum of injury Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous
PEDIATRIC CHEST TRAUMA Children are not small adults Role of imaging Spectrum of injury Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous
Session Number 219 A BLUNT REVIEW OF THE PENETRATING ISSUES IN CHEST TRAUMA
 Session Number 219 A BLUNT REVIEW OF THE PENETRATING ISSUES IN CHEST TRAUMA Lisa C. Laphan-Morad, MSN, APN-C Administrative Director of Surgical & Ambulatory Services Nurse Practitioner Virtua Health Marlton,
Session Number 219 A BLUNT REVIEW OF THE PENETRATING ISSUES IN CHEST TRAUMA Lisa C. Laphan-Morad, MSN, APN-C Administrative Director of Surgical & Ambulatory Services Nurse Practitioner Virtua Health Marlton,
Anatomy notes-thorax.
 Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
This is not a required assignment but it is recommended.
 SU 12 Name: This is not a required assignment but it is recommended. BIO 116 - Anatomy & Physiology II Practice Assignment 2 - The Respiratory and Cardiovascular Systems 1. The exchange of oxygen and carbon
SU 12 Name: This is not a required assignment but it is recommended. BIO 116 - Anatomy & Physiology II Practice Assignment 2 - The Respiratory and Cardiovascular Systems 1. The exchange of oxygen and carbon
The Cardiovascular System. Chapter 15. Cardiovascular System FYI. Cardiology Closed systemof the heart & blood vessels. Functions
 Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
MANAGEMENT OF THORACIC TRAUMA. Luis H. Tello MV, MS DVM, COS Portland Hospital Classic Banfield Pet Hospital - USA
 MANAGEMENT OF THORACIC TRAUMA Luis H. Tello MV, MS DVM, COS Portland Hospital Classic Banfield Pet Hospital - USA luis.tello@banfield.com Chest Trauma: Big threat!!!! CAUSES OF THORACIC TRAUMA Blunt Trauma
MANAGEMENT OF THORACIC TRAUMA Luis H. Tello MV, MS DVM, COS Portland Hospital Classic Banfield Pet Hospital - USA luis.tello@banfield.com Chest Trauma: Big threat!!!! CAUSES OF THORACIC TRAUMA Blunt Trauma
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Cath Lab Essentials: Pericardial effusion & tamponade
 Cath Lab Essentials: Pericardial effusion & tamponade Pranav M. Patel, MD, FACC, FSCAI Chief, Division of Cardiology Director, Cardiac Cath Lab & CCU University of California, Irvine Division of Cardiology
Cath Lab Essentials: Pericardial effusion & tamponade Pranav M. Patel, MD, FACC, FSCAI Chief, Division of Cardiology Director, Cardiac Cath Lab & CCU University of California, Irvine Division of Cardiology
9/10/2012. Chapter 44. Learning Objectives. Learning Objectives (Cont d) Bleeding
 Chapter 44 Bleeding 1 Learning Objectives Describe the etiology, history, and physical findings of external bleeding Predict hemorrhage on the basis of the patient s mechanism of injury Distinguish between
Chapter 44 Bleeding 1 Learning Objectives Describe the etiology, history, and physical findings of external bleeding Predict hemorrhage on the basis of the patient s mechanism of injury Distinguish between
Northwest Community EMS System Continuing Education Class Credit Questions Respiratory Assessment January 2012
 Name (PRINT): Date submitted: Affiliation: Rating: [ ] Complete [ ] Incomplete Reminder: You must schedule to take the class post-test with your assigned hospital EMS Coordinator/educator or their designee
Name (PRINT): Date submitted: Affiliation: Rating: [ ] Complete [ ] Incomplete Reminder: You must schedule to take the class post-test with your assigned hospital EMS Coordinator/educator or their designee
Chapter 22. Learning Objectives. Learning Objectives 9/18/2012. Chest and Abdominal Emergencies
 Chapter 22 and Abdominal Emergencies Learning Objectives Discuss emergency medical care considerations for patient with penetrating chest injury Differentiate care of an open wound to the chest from an
Chapter 22 and Abdominal Emergencies Learning Objectives Discuss emergency medical care considerations for patient with penetrating chest injury Differentiate care of an open wound to the chest from an
ADC ED/TRAUMA POLICY AND PROCEDURE Policy 270
 Section: ADC Trauma ADC ED/TRAUMA POLICY AND PROCEDURE Policy 270 Subject: Pediatric Trauma Resuscitation Protocol Trauma Coordinator UTMB respects the diverse culture needs, preferences, and expectations
Section: ADC Trauma ADC ED/TRAUMA POLICY AND PROCEDURE Policy 270 Subject: Pediatric Trauma Resuscitation Protocol Trauma Coordinator UTMB respects the diverse culture needs, preferences, and expectations
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Kinetic Energy Energy in Motion KE = Mass (weight) X Velocity (speed)² 2 Double Weight = Energy Double Speed = Energy IS THE GREATEST DETERMINANT
 1 Chapter 17 Blunt Trauma 2 Introduction to Blunt Trauma Most common cause of trauma death and disability exchange between an object and the human body, without intrusion through the skin 3 Blunt trauma
1 Chapter 17 Blunt Trauma 2 Introduction to Blunt Trauma Most common cause of trauma death and disability exchange between an object and the human body, without intrusion through the skin 3 Blunt trauma
Prehospital Resuscitation for the 21 st Century Simulation Case. VF/Asystole
 Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Thoracic Trauma: 5/19/2010. Keihan Golshani, MD, Assistant Professor of emergency Medicine, Isfahan Medical University,
 Thoracic Trauma: 1 Thoracic trauma: A significant cause of mortality. Many patients with thoracic trauma: die after reaching the hospital Many of them can be prevented by: Prompt diagnosis and treatment.
Thoracic Trauma: 1 Thoracic trauma: A significant cause of mortality. Many patients with thoracic trauma: die after reaching the hospital Many of them can be prevented by: Prompt diagnosis and treatment.
Trauma Activation 7/18/17
 Blunt Rupture of the Thoracic Duct after Severe Thoracic Trauma Samuel Brown, MD Trauma Activation 7/18/17 53 year old male, rear end MVC, exited vehicle and was struck by a semi truck. Denies LOC, complaints
Blunt Rupture of the Thoracic Duct after Severe Thoracic Trauma Samuel Brown, MD Trauma Activation 7/18/17 53 year old male, rear end MVC, exited vehicle and was struck by a semi truck. Denies LOC, complaints
Evaluation & Management of Penetrating Wounds to the NECK
 Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
RCH Trauma Guideline. Management of Traumatic Pneumothorax & Haemothorax. Trauma Service, Division of Surgery
 RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
Pediatric Trauma Care
 2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
Trauma Overview. Chapter 22
 Trauma Overview Chapter 22 Kinematics of Trauma Injuries are the leading cause of death among children and young adults. Kinematics introduces the basic physical concepts that dictate how injuries occur
Trauma Overview Chapter 22 Kinematics of Trauma Injuries are the leading cause of death among children and young adults. Kinematics introduces the basic physical concepts that dictate how injuries occur
Surface anatomy of Cardiovascular system
 Surface anatomy of Cardiovascular system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The lines cover the front, side, and back of the thorax Midsternal
Surface anatomy of Cardiovascular system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The lines cover the front, side, and back of the thorax Midsternal
Initial Assessment and Management of the Trauma Patient
 Initial Assessment and Management of the Trauma Patient 1 Epidemiology Road Traffic Accidents are major cause of long term morbidity and mortality in developing nations WHO predicts that by 2020, Road
Initial Assessment and Management of the Trauma Patient 1 Epidemiology Road Traffic Accidents are major cause of long term morbidity and mortality in developing nations WHO predicts that by 2020, Road
Abdomen and Genitalia Injuries. Chapter 28
 Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Review. A. abrasion B. contusion C. hematoma D. avulsion
 Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Condensed version.
 I m Stu 3 Condensed version smcvicar@uwhealth.org Listen 1. Snoring 2. Gurgling 3. Hoarseness 4. Stridor (inspiratory/expiratory) 5. Wheezing 6. Grunting Listen Crackles Wheezing Stridor Absent Crackles
I m Stu 3 Condensed version smcvicar@uwhealth.org Listen 1. Snoring 2. Gurgling 3. Hoarseness 4. Stridor (inspiratory/expiratory) 5. Wheezing 6. Grunting Listen Crackles Wheezing Stridor Absent Crackles
Dr.Kasturi Bhagawati Emergency Medicine Department
 Dr.Kasturi Bhagawati Emergency Medicine Department 16-04-2015 Introduction Chest trauma is often sudden and dramatic. Cardiac injuries can be catastrophic. Accounts for 25% of all trauma deaths 10% of
Dr.Kasturi Bhagawati Emergency Medicine Department 16-04-2015 Introduction Chest trauma is often sudden and dramatic. Cardiac injuries can be catastrophic. Accounts for 25% of all trauma deaths 10% of
Pneumothorax. Defined as air in the pleural space which can occur through a number of mechanisms
 Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing
 1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
APPROACH TO TRAUMA. Dr E.Memary Anesthesiologist Assistant Professor of SBMU
 APPROACH TO TRAUMA Dr E.Memary Anesthesiologist Assistant Professor of SBMU Objectives Describe the initial approach to the injured patient, including the primary and secondary surveys. Identify the types
APPROACH TO TRAUMA Dr E.Memary Anesthesiologist Assistant Professor of SBMU Objectives Describe the initial approach to the injured patient, including the primary and secondary surveys. Identify the types
