STS Care of Thermal Burns 20% Total Body Surface Area
|
|
|
- Emil Nash
- 5 years ago
- Views:
Transcription
1 Temp Regulation Transfer Pain Fluids Airway Initial Assessment STS Care of Thermal Burns 20% Total Body Surface Area Remove burned clothing, rings, watches, and jewelry Cervical spine precautions (if history of blast injury or other significant trauma) Estimate total body surface area (TBSA) with partial and full thickness burns using the Shriners burn diagram (see accompanying page) Check temperature and begin continuous temperature monitoring if indicated (see burn FAQ sheet) 20% TBSA Initiate 100% FiO 2 by non-rebreathing face mask with noninvasive EtCO 2 monitor in place for all burns related to fire (can omit for scald and non-fire-related thermal burns) Manage airway if indicated (see box to right) Pitfalls to Avoid Overestimation of TBSA Over/under resuscitation with IV fluids Endotracheal intubation when not indicated Inadequate temp monitoring and hypothermia Indications for emergent airway management in a burn patient Obtundation with absent airway reflexes (no cough/no gag) Hoarse voice or cry, stridor, drooling, difficulty speaking, respiratory distress, obvious swelling of the oropharynx Extensive (> 40%) TBSA burns In the absence of the above findings, emergent intubation may not be indicated. Flash facial burns, singed nasal/facial hair, and carbonaceous material (soot) in the naso/ oropharynx are not absolute indications for emergent intubation as long as the patient is breathing comfortably. Establish IV access (2 large bore IVs for burns 20% TBSA) Initiate normal saline or Ringer s lactate infusion according to fluid administration recommendations (see box to right) Do not bolus (avoid fluid creep ) Insert Foley catheter for urine output monitoring (goal 1 ml/kg/hr) Pain control with IV morphine 0.1 mg/kg/dose (max 10 mg/dose) or IV fentanyl 1-2 mcg/kg/dose (max 200 mcg/dose) Avoid IM administration due to erratic absorption Call Shriners at and ask to speak with the charge nurse Key information to convey: Mechanism of burn including whether it occurred in a closed space TBSA with partial/full thickness burns Summary of interventions (fluid rate, Foley, airway interventions, pain management, temperature) Fluid administration recommendations Use normal saline or Ringer s lactate 5 years or less: 125 ml/hr 6-13 years: 250 ml/hr 14 years or older: 500 ml/hr Labs/Studies to Consider I Stat (Shriners requests this if intubated) Renal profile and CBC Noninvasive carbon monoxide measurement Venous co-oximetry (ie carboxyhemoglobin level) Lactic Acid (Stat) Cyanide level Urine or blood hcg (if post-menarchal) CXR and Type and Screen (if history of blast injury or other significant trauma) Dress the burns with dry, sterile gauze or cover the patient with a dry sheet if the burns are extensive Keep the patient warm (blankets, turn up ambient room temperature, warmed IV fluids, head covering, Bair Hugger )
2 1 Burn Management Frequently Asked Questions (FAQ) Initial Assessment How do I assess for PULSES in a circumferentially burned extremity? Doppler examination can be used to determine whether there is a circulation deficit in a circumferentially burned extremity.[1] Capillary refill time, warmth/coolness of the distal extremity, and palpation of pulses may be of limited utility in assessing the adequacy of circulation in this situation. What should I expect a burn patient s MENTAL STATUS to be like? Typically, a burn patient is alert and oriented and may be in a significant amount of pain. If the patient is not alert, consider associated trauma/injury, carbon monoxide poisoning, cyanide poisoning, hypoxia, and hypoglycemia.[1, 2] What is the most accurate way to estimate TBSA in burns that are SCATTERED or IRREGULARLY SHAPED? The palmar surface of the patient s hand including the fingers represents approximately 1% of the patient s total body surface area. Assessment of the size of the palmar surface of the patient s hand and approximating it to the burn areas can aid in estimating the TBSA when burns are scattered or irregularly-shaped.[1] Do burn patients need a C-COLLAR? If the burn injury is a result of an explosion, blast, motor vehicle crash, or mechanism that puts the patient at risk for spinal cord injury, then immobilization of the cervical spine with a collar is warranted. How do I assess for INHALATION injury? There are 3 distinguishable types of airway inhalation injury: 1) carbon monoxide poisoning; 2) inhalation (thermal) injury above the glottis; and 3) inhalation (chemical and irritant) injury below the glottis. Carboxyhemoglobin levels of 5-10% can be found in smokers. Levels of 15-40% cause central
3 2 nervous system dysfunction % carboxyhemoglobin causes obtundation and loss of consciousness. Blood gas analysis is normal in carbon monoxide poisoning because the amount of oxygen dissolved in the plasma (PaO 2 ) is unaffected. Oxygen saturation is also usually normal because a standard pulse oximeter cannot differentiate between carboxyhemoglobin and regular oxygenated hemoglobin. Thermal burns to the respiratory tract are limited to the upper airway above the glottis (nasopharynx, oropharynx, and larynx) because the respiratory tract s heat exchange capability is very efficient so absorption of heat and damage occurs above the vocal cords. Supraglottic edema may be delayed until fluid resuscitation is underway. Generalized edema developing in the upper airway related to the size of burns can occur without direct thermal injury to the upper airway. Inhalation injury below the glottis is almost always chemical in nature. The severity of inhalation injury and the extent of damage are clinically unpredictable based on history and initial exam. Chest x-ray is often normal at the time of initial presentation. Onset of symptoms is also unpredictable. 24 hours of observation is recommended if inhalation injury is suspected. Both inadequate volume of fluid resuscitation and excess fluid resuscitation are damaging to pulmonary function post burn.[1-3] What is considered a CONFINED/CLOSED SPACE? A confined/closed space is an area where smoke and heat cannot readily escape thereby increasing the risk of an inhalation injury. Airway Management How do I know if I need to INTUBATE? Stridor, hoarseness of voice or cry, drooling, difficulty speaking, respiratory distress, and obvious swelling of the oropharynx are indications for emergent intubation. An obtunded patient or a patient with absent airway reflexes mandates emergent intubation. Extensive total body surface area burns (> 40%) will also require intubation.[1, 2] Flash facial burns, singed nasal/facial hair, and carbonaceous material (soot) in the nasopharynx or oropharynx are not absolute indications for emergent intubation as long as the patient is breathing comfortably and does not display any of the above mentioned signs. How do I SECURE an ETT? Adhesive tape sticks poorly to burned skin. The endotracheal tube should be secured with endotracheal tube ties (1/2 inch cotton ties) passed around the head/neck.[2] Which burn patients require an NG TUBE? Ileus is common with burns of more than 20% TBSA. Gastric dilatation can ensue.[1] In addition, any patient with an endotracheal tube in place should have an NG tube to decompress the stomach to facilitate ventilation.
4 3 Vascular Access WHERE should I place an IV? Preferably through unburned skin, but vessels underlying burned skin can be used if necessary.[1] Preparation of the skin or burned tissue overlying the vessel to be cannulated should follow the same protocol as typical IV placement. If peripheral venous access cannot be obtained, a central venous catheter should be placed using unburned areas if possible. Intraosseous lines can serve as temporizing measures until venous access is achieved. How do I SECURE an IV? Adhesive tape sticks poorly to burned skin. IV catheters can be secured using a gauze roll or Coban Self-Adherent Wrap if available. Monitoring How do I SECURE the cardiorespiratory and pulse oximeter MONITORING PROBES to the patient? Apply over unburned skin if possible. If there are no unburned areas available for application, apply probe and secure with 1-inch gauze. When is CONTINUOUS RECTAL TEMPERATURE monitoring INDICATED? Temperature monitoring should be performed hourly in order to prevent hypothermia. In the obtunded or intubated and sedated patient, continuous rectal or esophageal temperature monitoring can be employed for burns 30% TBSA. Otherwise, noninvasive temperature measurement is adequate. WHERE is the TEMPERATURE monitoring PROBE located, and how do I hook it up? The brown thermometer cables are attached to the monitor and the Mon-a-therm rectal probe is located in the bedside carts. No calibration is necessary. Monitoring can be performed using transport or in-room monitors. 1. Lubricate the end of the rectal sensor/probe with a small amount of water-soluble lubricant. 2. Insert the rectal sensor/probe two inches into the rectum. 3. Secure the exposed sensor/probe tubing with tape or Tegaderm to the buttocks and upper thighs. 4. Insert the Mon-a-therm rectal sensor/probe into the thermometer cable. 5. The core body temperature will automatically and continuously display.
5 4 What is the UTILITY of TEMPORAL THERMOMETRY in measuring body temperature in burn patients? Temporal thermometers should be avoided in burn patients. When trialed at Shriners, temporal thermometers were found to be inaccurate. What are the LIMITATIONS of traditional MONITORING techniques in the burn patient? In circumferential extremity burns, edema develops in the tissue under the eschar and may gradually impair venous return.[1] This may limit the ability to assess for adequate perfusion by palpation of distal pulses, determination of capillary refill time, and measurement blood pressure. Burn injury also triggers the systemic inflammatory response syndrome which is, in part, characterized by tachycardia.[2] Tachycardia is a common finding in the burn patient and cannot be utilized as a reliable indicator of intravascular volume depletion. Standard pulse oximetry may be falsely reassuring with an oxygen saturation of 100% in the presence of clinically significant carbon monoxide poisoning. Fluid Management/Resuscitation WHO needs a FLUID BOLUS? Routine fluid boluses should be avoided in order to prevent fluid overload (ie fluid creep ) that will exacerbate generalized edema and contribute to respiratory distress syndrome. If there is a history of acute blood loss secondary to trauma, a fluid bolus to replace intravascular volume would be reasonable as in any trauma patient. In the absence of a history of acute blood loss, initiate resuscitation fluids at the recommended rate (see burn algorithm). What is FLUID CREEP? Fluid creep refers to fluid overload that may result from overestimation of burn size, under appreciation of the limitations of standard hemodynamic monitoring methods in the burn patient, and inadequate reduction of fluid infusion in response to excessive urine output.[3] What are the GOALS for FLUID RESUSCITATION in a burn patient? Fluid resuscitation should be aimed at maintaining tissue perfusion and organ function while avoiding the complications of inadequate or excessive fluid therapy. Peripheral vascular resistance markedly increases and cardiac output decreases in the early stages after thermal injury.[1] Tissue blood flow is diminished and redistributed. Cardiac output usually returns to predicted normal levels between hours post burn. The edema that forms in injured tissue reaches its maximum in the second 24 hours post burn. Excessive volume of resuscitation fluid exaggerates edema formation leading to compromised local blood supply as well as contributing to worsened respiratory distress syndrome and prolonged time on the ventilator. Inadequate resuscitation can lead to shock and organ failure, most commonly acute renal failure.[1]
6 5 Which burn patients REQUIRE a FOLEY CATHETER? A patient with TBSA burns of 20% or more should have a Foley catheter placed in order to monitor urine output. What is the best way to know that I am RESUSCITATING EFFECTIVELY? Urine output is the best guide for ensuring the appropriateness of fluid resuscitation.[1] Insertion of a Foley catheter allows for the calculation of hourly urine output. Goal urine output: adults = ml/hr; children < 30 kg = 1 ml/kg/hr.[1-3] Does the recommended fluid administration rate include MAINTENANCE FLUID REQUIREMENTS? No. Infants and young children should receive maintenance IV fluid with 5% dextrose in addition to the recommended resuscitation fluid rate.[1] Is RINGER S LACTATE or NORMAL SALINE better for a burn patient? Either fluid can used depending on ease of availability. If a burn patient has metabolic acidosis or is hyperchloremic or hypernatremic, Ringer s lactate would be preferred. Pain Management What is the best way to control a burn patient s PAIN? IV morphine (0.1 mg/kg/dose, max 10 mg/dose) or fentanyl (1-2 mcg/kg/dose, max 200 mcg/dose) is indicated for control of pain associated with moderate to severe burns. Alterations in tissue blood flow resulting from the systemic inflammatory response syndrome associated with the burn make absorption of intramuscular or subcutaneous injections unpredictable.[1] The use of IM injections is therefore not recommended due to this variable absorption and lag time to peak effect. IV administration is the recommended route. Oral morphine may be administered to those patients who are awake, protecting their airway, and require pain control prior to attainment of IV access. The dose is 0.3 mg/kg/dose (max 20 mg/dose).
7 6 Threats/Pitfalls What are the MOST COMMON THREATS/PITFALLS in the management of burns 20% TBSA? Over/under resuscitation with IV fluids, endotracheal intubation when it is not necessarily indicated, lack of adequate temperature monitoring and warming resulting in hypothermia, inadequate measurement of the response to resuscitation with early placement of a Foley catheter and measurement of hourly urine output.[1, 3] Maintaining the patient s temperature is a priority. The room should be warmed, and the patient should be covered with dry sheets and blankets to prevent hypothermia. Warmed IV fluid (37-40 C) may be used for resuscitation.[1] Toxicology Considerations Which burn patients require DECONTAMINATION? Indications for decontamination of a burn patient are the same as for other patients and include, but are not limited to, exposure to corrosive agents on the clothes or skin and volatile fumes emanating from the patient or the patient s clothing (e.g. gasoline). Clothing should be removed and the patient s skin flushed with copious amounts of lukewarm water. What is the recommended TREATMENT for CARBON MONOXIDE poisoning? Humidified 100% oxygen should be administered by nonrebreathing face mask or endotracheal tube until carboxyhemoglobin levels of less than 5% are achieved.[1, 3, 4] The approximate half-life of elimination of carboxyhemoglobin during treatment with high-flow oxygen by tight-fitting mask or endotracheal tube is 74 minutes (range minutes). In room air, the approximate half-life is as much as 200 minutes.[5] Existing evidence does not establish whether treatment with hyperbaric oxygen therapy reduces adverse neurologic outcomes in carbon monoxide poisoning.[6] Due to the challenges in transporting a burned patient to a hyperbaric oxygen therapy chamber and providing resuscitative care in the chamber, hyperbaric oxygen therapy is not recommended.[2] WHO should receive the CYANOKIT? Cyanide poisoning usually results in sustained loss of consciousness, persistent, severe lactic acidosis, and hypotension. Seizures may also be seen. It is reasonable to consider administration of the Cyanokit to a patient with persistent, severe lactic acidosis and altered mental status of unclear etiology despite adequate oxygenation and ventilation. However, administration of the Cyanokit interferes with laboratory testing performed by colorimetric assay (eg AST, creatinine, magnesium, and bilirubin) and may also interfere with the ability to dialyze a patient due to false detection of a
8 7 blood leak from the blood-like appearance of the solution (see Cyanokit package insert for additional details).[7-9] Therefore, the risks and benefits should be weighed carefully before administering the Cyanokit. Urine, sweat, tears, and other secretions become pink or red after Cyanokit administration.[5] HOW is the CYANOKIT DOSED? 70 mg/kg (maximum dose 5000 mg) IV over 15 minutes[5] WHERE is the CYANOKIT STORED? The Cyanokit is stored in the STS Pyxis machine (Trauma 2) and in the Big Room. Additional doses are stored in the inpatient pharmacies at Burnet and Liberty. Transfer Considerations How do I know who to TRANSFER TO SHRINERS? The American Burn Association has identified injuries usually requiring referral to a burn center.[1] See the back of the Shriners burn diagram for a comprehensive list of reasons for referral. You can also call and ask to speak with the charge nurse to review the history and findings and decide on the necessity and appropriate timing for referral. What RESOURCES does SHRINERS have available when the patient arrives to their floor? There is a surgery resident in house 24 hours/day. Anesthesia and burn surgery attendings are available on an as needed basis dictated by patient condition. This determination is made prior to admission. The Shriners burn surgery attending speaks to the attending at the referring facility prior to transport. What is the best way to DRESS THE BURNS? Cover the burn area with a clean, dry sheet. Covering burn wounds prevents air currents from causing pain in partial thickness burns. Ice or wet dressings should not be applied directly to the burn in order to avoid hypothermia and frostbite.[1] Do not apply topical antibiotic ointment if immediate transfer to Shriners is planned. If I receive a CALL FROM an OUTLYING HOSPITAL regarding a burn patient, does the patient need to come to the CCHMC ED first? No. The patient can be transferred directly to Shriners for definitive burn wound care. Tell the outlying hospital to call and ask to speak with the charge nurse to review the history and findings and decide on the necessity and appropriate timing for referral.
9 8 Healing What can I teach about expected scarring and TIME TO HEALING? A first-degree burn is limited to the epidermis. Injured cells will peel away within a few days revealing healed skin below with no scarring. Partial-thickness (second degree) burns involve the entire epidermis and variable portions of the dermis. Healing may require 2-3 weeks or even longer. Scarring is minimal if healing occurs within 2-3 weeks. Grafting may be necessary if the wound is open for a longer period of time.[1, 3] Non-Thermal Burn Considerations What about ELECTRICAL or CHEMICAL BURNS? Electrical burns serious dysrhythmias may occur even after a stable cardiac rhythm has been obtained. Continuous cardiac monitoring may be necessary during the first 24 hours post injury. There may also be occult severe, deep tissue injury.[1] Chemical burns copious amounts of water should be used to flush the chemical from the body surface. Powdered chemicals should be brushed from the skin prior to flushing. Chemical eye injuries should be irrigated until instructed otherwise by an ophthalmologist. References 1. Advanced Burn Life Support Course Provider Manual. 2007, Chicago, IL: American Burn Association. 2. Cancio, L.C., Airway management and smoke inhalation injury in the burn patient. Clinics in plastic surgery, (4): p Toussaint, J. and A. Singer, The evaluation and management of thermal injuries: 2014 update. Clinical and Experimental Emergency Medicine, (1): p Hoffman, R.S., et al., Goldfrank's Toxicologic Emergencies. Tenth edition. ed. 2015, New York: McGraw-Hill,. 5. Poisoning & Drug Overdose. 4th ed. 2004: McGraw-Hill. 6. Buckley, N.A., et al., Hyperbaric oxygen for carbon monoxide poisoning. Cochrane Database Syst Rev, 2011(4): p. CD Sutter, M.E., et al., Blood leak alarm interference by hydoxocobalamin is hemodialysis machine dependent. Clin Toxicol (Phila), (10): p Avila, J., et al., Pseudo-blood leak? A hemodialysis mystery. Clin Nephrol, (4): p Sutter, M., et al., Hemodialysis complications of hydroxocobalamin: a case report. J Med Toxicol, (2): p
Approved By: Airway and Breathing A. Initially give humidified high flow oxygen at 15 L (100%) using a nonrebreather
 Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
EmergencyKT: Management of Thermal Injury in Adult Patients
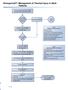 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
Burns. A Comprehensive Review Assessment & Management
 Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Objectives. Initial Burn Care and Fluid Resuscitation 6/5/2015 INITIAL MANAGEMENT
 Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
The immediate management of burns patients should be similar to management of trauma.
 CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
Management of Acute Burn Injuries: The First 24 Hours
 Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
BURNS MODULE. In the paediatric population consider non-accidental injury as a mechanism for burn injuries.
 BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
EMERGENCYROOM BURN MANAGEMENT
 EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
Burns Management in the Emergency Department
 Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
At the conclusion of this course the learner will be able to
 Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
INITIAL CARE AND TREATMENT OF BURN INJURIES. November 10,
 INITIAL CARE AND TREATMENT OF BURN INJURIES 2 11/10/2012 November 10, 2012 2 Oregon Burn Center Only burn center in Oregon and SW Washington New unit 16 beds, 20,000 square feet Opened in February 2002
INITIAL CARE AND TREATMENT OF BURN INJURIES 2 11/10/2012 November 10, 2012 2 Oregon Burn Center Only burn center in Oregon and SW Washington New unit 16 beds, 20,000 square feet Opened in February 2002
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test
 Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Burn injury. A : patent airway with smoking inhalation, stridor. D: E4V5M6,pupil 2mm RTLBE
 Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Applicable to. Team Members Performing
 Protocol: Pediatric Burn Inhalation Injury Category Clinical Practice Protocol Number Approval Date November 1, 2016 Due for review November 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations
Protocol: Pediatric Burn Inhalation Injury Category Clinical Practice Protocol Number Approval Date November 1, 2016 Due for review November 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations
Smoke inhalation damages the body by simple asphyxiation (lack of oxygen), chemical irritation, chemical asphyxiation, or a combination of these.
 Print Close 2011 WebMD, LLC. All rights reserved. Smoke Inhalation Recommend 13 Medical Author: Christopher P Holstege, MD Medical Editor: Melissa Conrad Stöppler, MD Smoke Inhalation Overview Smoke Inhalation
Print Close 2011 WebMD, LLC. All rights reserved. Smoke Inhalation Recommend 13 Medical Author: Christopher P Holstege, MD Medical Editor: Melissa Conrad Stöppler, MD Smoke Inhalation Overview Smoke Inhalation
Appendix D An unresponsive patient with shallow, gasping breaths at a rate of six per minute requires:
 Answer Key Appendix D-2 1. An unresponsive patient with shallow, gasping breaths at a rate of six per minute requires: a. oxygen given via nasal cannula b. immediate transport to a medical facility c.
Answer Key Appendix D-2 1. An unresponsive patient with shallow, gasping breaths at a rate of six per minute requires: a. oxygen given via nasal cannula b. immediate transport to a medical facility c.
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02
 PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
COBIS Management of airway burns and inhalation injury PAEDIATRIC
 COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose.
 Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. Debbie Harrell RN, MSN, Shriners Hospitals for Children Cincinnati Cincinnati, Ohio
Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. Debbie Harrell RN, MSN, Shriners Hospitals for Children Cincinnati Cincinnati, Ohio
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Chapter 29. Objectives. Objectives 01/09/2013. Burns
 Chapter 29 Burns Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced in
Chapter 29 Burns Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced in
Burn Injuries & Its Management M JARI.MD
 Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns.
 Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT
 PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Shruti Dholakia L Chigaru Author Position Fellow CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Shruti Dholakia L Chigaru Author Position Fellow CATS Consultant Document Owner E. Polke Document
Applicable to. Team Members Performing MD House Staff APRN/PA RN LPN
 Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Chapter 24 Soft Tissue Injuries Presentation Notes
 Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department
 Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES
 INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES 180801 1 Tactical Combat Casualty Care for Medical Personnel 1. August 2017 (Based on TCCC-MP Guidelines 180801 In this presentation, we
INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES 180801 1 Tactical Combat Casualty Care for Medical Personnel 1. August 2017 (Based on TCCC-MP Guidelines 180801 In this presentation, we
Pediatric Trauma Care
 2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
Current Trends in Burn Care
 Objectives Current Trends in Burn Care Jordan Murphy, BSN, CFRN Clinical Educator-KY/FL PHI Air Medical Describes normal skin anatomy. Differentiates pathophysiology related to etiology of injury. Identify
Objectives Current Trends in Burn Care Jordan Murphy, BSN, CFRN Clinical Educator-KY/FL PHI Air Medical Describes normal skin anatomy. Differentiates pathophysiology related to etiology of injury. Identify
MEDICAL KIT - ALGORITHMS
 MEDICAL KIT - ALGORITHMS Page 2 : BRONCHOSPASM / ASTHMA Page 3 : TENSION PNEUMOTHORAX Page 4 : Page 5 : Page 6 : CONGESTIVE HEART FAILURE/ PULMONARY EDEMA ANAPHYLACTIC SHOCK / ALLERGIC REACTION ANGINA
MEDICAL KIT - ALGORITHMS Page 2 : BRONCHOSPASM / ASTHMA Page 3 : TENSION PNEUMOTHORAX Page 4 : Page 5 : Page 6 : CONGESTIVE HEART FAILURE/ PULMONARY EDEMA ANAPHYLACTIC SHOCK / ALLERGIC REACTION ANGINA
HEAVY METALS : Review
 HEAVY METALS : Review INHALED TOXINS Dr. Tawfiq Almezeiny MBBS FRCPC (CCM) Introduction Airborne toxins typically produce local noxious effects on the airways and lungs. Examples of Inhalational exposure:
HEAVY METALS : Review INHALED TOXINS Dr. Tawfiq Almezeiny MBBS FRCPC (CCM) Introduction Airborne toxins typically produce local noxious effects on the airways and lungs. Examples of Inhalational exposure:
Management of Burns under Prolonged Field Care
 This Role 1, prolonged field care (PFC) guideline is intended to be used after TCCC Guidelines when evacuation to higher level of care is not immediately possible. A provider of PFC must first and foremost
This Role 1, prolonged field care (PFC) guideline is intended to be used after TCCC Guidelines when evacuation to higher level of care is not immediately possible. A provider of PFC must first and foremost
HeartCode PALS. PALS Actions Overview > Legend. Contents
 HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Poison (Toxicant): any substance or agent capable of producing a deleterious response in a biological system or living organism.
 Poison (Toxicant): any substance or agent capable of producing a deleterious response in a biological system or living organism. Poisoning= overdose toxicity intoxication= toxicity due to foreign substance
Poison (Toxicant): any substance or agent capable of producing a deleterious response in a biological system or living organism. Poisoning= overdose toxicity intoxication= toxicity due to foreign substance
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
BLS, ILS, ALS OTEP BURNS BURN INTRODUCTION TYPES OF BURNS
 BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Resuscitation Patient Management Tool May 2015 MET Event
 OPTIONAL: Local Event ID: Date/Time MET was activated: Time Not Documented MET 2.1 Pre-Event Pre-Event Tab Was patient discharged from an Intensive Care Unit (ICU) at any point during this admission and
OPTIONAL: Local Event ID: Date/Time MET was activated: Time Not Documented MET 2.1 Pre-Event Pre-Event Tab Was patient discharged from an Intensive Care Unit (ICU) at any point during this admission and
TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised by P.
 TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised 05-13-13 by P. Joe SCREENING FOR POTENTIAL COOLING PATIENTS Patients who are >
TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised 05-13-13 by P. Joe SCREENING FOR POTENTIAL COOLING PATIENTS Patients who are >
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS
 CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
Clearing the air.. How to assist and rescue neck breathing patients. Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA
 Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy
 Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Nassau Regional Emergency Medical Services. Advanced Life Support Pediatric Protocol Manual
 Nassau Regional Emergency Medical Services Advanced Life Support Pediatric Protocol Manual 2014 PEDIATRIC ADVANCED LIFE SUPPORT PROTOCOLS TABLE OF CONTENTS Approved Effective Newborn Resuscitation P 1
Nassau Regional Emergency Medical Services Advanced Life Support Pediatric Protocol Manual 2014 PEDIATRIC ADVANCED LIFE SUPPORT PROTOCOLS TABLE OF CONTENTS Approved Effective Newborn Resuscitation P 1
PEPP Course: PEPP BLS Pretest
 PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
MICHIGAN. State Protocols. Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.
 MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Pediatric Code Blue. Goals of Resuscitation. Focus Conference November Ensure organ perfusion
 Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Fire Deaths. Dr Julie McAdam Consultant Forensic Pathologist Glasgow University
 Fire Deaths Dr Julie McAdam Consultant Forensic Pathologist Glasgow University Forensic investigation multidisciplinary fire officers, police officers, scientists, photographers, pathologist, procurator
Fire Deaths Dr Julie McAdam Consultant Forensic Pathologist Glasgow University Forensic investigation multidisciplinary fire officers, police officers, scientists, photographers, pathologist, procurator
10/17/2016 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT COURSE OBJECTIVES COMMON CAUSES OF RESPIRATORY FAILURE
 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
Post-Anesthesia Care In the ICU
 Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Adult Intubation Skill Sheet
 Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
BLS ROUTINE MEDICAL CARE
 BLS ROUTINE MEDICAL CARE Scene safety # Assure scene safety prior to patient contact C-spine # Perform manual cervical spine stabilization if indicated (Follow the cervical spine protocol.) ABCs # Assess
BLS ROUTINE MEDICAL CARE Scene safety # Assure scene safety prior to patient contact C-spine # Perform manual cervical spine stabilization if indicated (Follow the cervical spine protocol.) ABCs # Assess
Pediatric Advanced Life Support
 Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital. Mr Adam Bialostocki Plastic Surgeon, Tauranga
 Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital Mr Adam Bialostocki Plastic Surgeon, Tauranga Mr. Adam Bialostocki Plastic Surgeon Minor Burns First Aid Remove the burning agent / wet clothes
Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital Mr Adam Bialostocki Plastic Surgeon, Tauranga Mr. Adam Bialostocki Plastic Surgeon Minor Burns First Aid Remove the burning agent / wet clothes
Capnography 101. James A Temple BA, NRP, CCP
 Capnography 101 James A Temple BA, NRP, CCP Expected Outcomes 1. Gain a working knowledge of the physiology and science behind End-Tidal CO2. 2.Relate End-Tidal CO2 to ventilation, perfusion, and metabolism.
Capnography 101 James A Temple BA, NRP, CCP Expected Outcomes 1. Gain a working knowledge of the physiology and science behind End-Tidal CO2. 2.Relate End-Tidal CO2 to ventilation, perfusion, and metabolism.
Burn wounds - Determining the size and type degree
 1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1 2 Burn depth Most burns are a combination of superficial and deeper burns and the
1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1 2 Burn depth Most burns are a combination of superficial and deeper burns and the
(31189) Hypothermia Initiation Phase One
 Hypothermia Initiation Phase One Diagnosis Allergies For hypothermia tracking purposes only. Please do not uncheck.- Required Cardiac Emergency Tracking For hypothermia tracking purposes only. Consults
Hypothermia Initiation Phase One Diagnosis Allergies For hypothermia tracking purposes only. Please do not uncheck.- Required Cardiac Emergency Tracking For hypothermia tracking purposes only. Consults
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
IRECA BLS Challenge 2015 Scenario 1
 Scenario 1 Team Name Team Number Captain Name Judge 1 # Judge 2 # JUDGE S SHEET Overview: This scenario challenges the competitors to use basic triage techniques and then to do the most good for the most
Scenario 1 Team Name Team Number Captain Name Judge 1 # Judge 2 # JUDGE S SHEET Overview: This scenario challenges the competitors to use basic triage techniques and then to do the most good for the most
7. Hypovolemic shock caused by severe burns is the result of a loss of: A) plasma. B) platelets. C) whole blood. D) red blood cells.
 Name: Date: 1. When parking your ambulance at the scene of a motor vehicle crash, you should position the ambulance: A) 50 past the scene on the opposite side of the road. B) 100 past the scene on the
Name: Date: 1. When parking your ambulance at the scene of a motor vehicle crash, you should position the ambulance: A) 50 past the scene on the opposite side of the road. B) 100 past the scene on the
Guidelines Administrative Practice X Clinical Practice Professional Practice
 Guidelines Administrative Practice X Clinical Practice Professional Practice End Tidal CO 2 (EtCO2) Monitoring Using the Zoll Monitor/Defibrillator Page 1 of 4 Scope: Outcome: Respiratory Therapists (RT),
Guidelines Administrative Practice X Clinical Practice Professional Practice End Tidal CO 2 (EtCO2) Monitoring Using the Zoll Monitor/Defibrillator Page 1 of 4 Scope: Outcome: Respiratory Therapists (RT),
Frontline First Aid 2012 Emergency Care Manual Treatments
 Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
SEPSIS SYNDROME
 INTRODUCTION Sepsis has been defined as a life threatening condition that arises when the body s response to an infection injures its own tissues and organs. Sepsis may lead to shock, multiple organ failure
INTRODUCTION Sepsis has been defined as a life threatening condition that arises when the body s response to an infection injures its own tissues and organs. Sepsis may lead to shock, multiple organ failure
Staging Sepsis for the Emergency Department: Physician
 Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
SEMINOLE COUNTY EMS PROVISIONAL EMT SKILLS VERIFICATION
 The following individual has completed the Seminole County EMS Provisional EMT Skills Verification check in the following areas: Oxygen, Airway and Ventilation Skills ALS Assistance Trauma Management Medical
The following individual has completed the Seminole County EMS Provisional EMT Skills Verification check in the following areas: Oxygen, Airway and Ventilation Skills ALS Assistance Trauma Management Medical
Review. A. abrasion B. contusion C. hematoma D. avulsion
 Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Cellular and Tissue Effects. Pathophysiology of the Burn Wound. Special Topics: Thermal Burns & Smoke Inhalation
 Special Topics: Thermal Burns & Smoke Inhalation MEDICAL RESPONDER AND RECEIVER SEMINAR; EXPLOSION AND BLAST INJURIES Pathophysiology of the Burn Wound The burn wound is the source of virtually all ill
Special Topics: Thermal Burns & Smoke Inhalation MEDICAL RESPONDER AND RECEIVER SEMINAR; EXPLOSION AND BLAST INJURIES Pathophysiology of the Burn Wound The burn wound is the source of virtually all ill
ADVANCED PATIENT MONITORING DURING ANAESTHESIA: PART ONE
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk ADVANCED PATIENT MONITORING DURING ANAESTHESIA: PART ONE Author : CARL BRADBROOK Categories : Vets Date : October 7, 2013
Vet Times The website for the veterinary profession https://www.vettimes.co.uk ADVANCED PATIENT MONITORING DURING ANAESTHESIA: PART ONE Author : CARL BRADBROOK Categories : Vets Date : October 7, 2013
Where Emergency Medicine Meets Critical Care: Next Level Resuscitation
 Where Emergency Medicine Meets Critical Care: Next Level Resuscitation Rob Green, BSc, MD, DABEM, FRCPC, FRCP(Edin) Professor, Dalhousie University Departments of Emergency Medicine,Critical Care Medicine
Where Emergency Medicine Meets Critical Care: Next Level Resuscitation Rob Green, BSc, MD, DABEM, FRCPC, FRCP(Edin) Professor, Dalhousie University Departments of Emergency Medicine,Critical Care Medicine
Appendix E Choose the sign or symptom that best indicates severe respiratory distress.
 Appendix E-2 1. In Kansas EMT-B may monitor pulse oximetry: a. after they complete the EMT-B course b. when the service purchases the state approved pulse oximeters c. when the service director receives
Appendix E-2 1. In Kansas EMT-B may monitor pulse oximetry: a. after they complete the EMT-B course b. when the service purchases the state approved pulse oximeters c. when the service director receives
In accordance with protocols, this patient should be transported to which medical facility?
 NOTE: Please select the most appropriate answer based on the Westchester Regional On-Line Medical Control Physician (OLMC) Regional System Overview, as well as current regional and state EMS protocols
NOTE: Please select the most appropriate answer based on the Westchester Regional On-Line Medical Control Physician (OLMC) Regional System Overview, as well as current regional and state EMS protocols
Introduction (1 of 3)
 Chapter 10 Shock Introduction (1 of 3) Shock (hypoperfusion) means a state of collapse and failure of the cardiovascular system. In the early stages, the body attempts to maintain homeostasis. As shock
Chapter 10 Shock Introduction (1 of 3) Shock (hypoperfusion) means a state of collapse and failure of the cardiovascular system. In the early stages, the body attempts to maintain homeostasis. As shock
Ammonia (NH 3 ) B 1. Information and recommendations for paramedics and doctors at the site. BASF Chemical Emergency Medical Guidelines
 BASF Chemical Emergency Medical Guidelines Ammonia (NH 3 ) B 1 Information and recommendations for paramedics and doctors at the site Before approaching the patient the paramedics and doctors at the site
BASF Chemical Emergency Medical Guidelines Ammonia (NH 3 ) B 1 Information and recommendations for paramedics and doctors at the site Before approaching the patient the paramedics and doctors at the site
NRP Raising the Bar for Providers and Instructors
 NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
Table of Contents. Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings
 Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
table of contents pediatric treatment guidelines
 table of contents pediatric treatment guidelines P1 PEDIATRIC PATIENT CARE...70 P2 APPARENT LIFE-THREATENING EVENT (ALTE)...71 P3 CARDIAC ARREST INITIAL CARE AND CPR...72 73 P4 NEONATAL CARE AND RESUSCITATION...74
table of contents pediatric treatment guidelines P1 PEDIATRIC PATIENT CARE...70 P2 APPARENT LIFE-THREATENING EVENT (ALTE)...71 P3 CARDIAC ARREST INITIAL CARE AND CPR...72 73 P4 NEONATAL CARE AND RESUSCITATION...74
Wisecracks 1. What are the indications for an escharotomy 2. What are the primary considerations in mechanical ventilation of burn patients
 Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Facility Name: Name: Date: Tracheostomy Care Evaluation Checklist
 Name: Date: Tracheostomy Care Evaluation Checklist Objective: Learner will be able to demonstrate tracheostomy care with a disposable inner cannula. Review facility protocol for caring for Airway Management:
Name: Date: Tracheostomy Care Evaluation Checklist Objective: Learner will be able to demonstrate tracheostomy care with a disposable inner cannula. Review facility protocol for caring for Airway Management:
Advanced Paediatric Nursing. Burn Trauma. 26 April Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH
 Advanced Paediatric Nursing Burn Trauma 26 April 2016 Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH Objective: Understand burn trauma in children Understand Important nursing interventions in burn
Advanced Paediatric Nursing Burn Trauma 26 April 2016 Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH Objective: Understand burn trauma in children Understand Important nursing interventions in burn
Z19.2 Cross Reference to Patient Care Maps & Clinical Care Procedures
 2017-04-07 Old version G1 Code of Ethics G2 Scope and Function G3 Scene Assessment G4 Triage G5 Primary Survey G6 Shock G7 Load and Go G8 Secondary Survey G9 Unconscious Patient G10A Obstructed Airway
2017-04-07 Old version G1 Code of Ethics G2 Scope and Function G3 Scene Assessment G4 Triage G5 Primary Survey G6 Shock G7 Load and Go G8 Secondary Survey G9 Unconscious Patient G10A Obstructed Airway
