Journal of the American College of Cardiology Vol. 48, No. 5, by the American College of Cardiology Foundation ISSN /06/$32.
|
|
|
- Robert Davidson
- 5 years ago
- Views:
Transcription
1 Journal of the American College of Cardiology Vol. 48, No. 5, by the American College of Cardiology Foundation ISSN /06/$32.00 Published by Elsevier Inc. doi: /j.jacc Lack of Inertia Force of Late Systolic Aortic Flow Is a Cause of Left Ventricular Isolated Diastolic Dysfunction in Patients With Coronary Artery Disease Cardiac Function Takayuki Yoshida, MD, Nobuyuki Ohte, MD, FACC, Hitomi Narita, MD, Seiichiro Sakata, MD, Kazuaki Wakami, MD, Kaoru Asada, MD, Hiromichi Miyabe, MD, Tomoaki Saeki, MD, Genjiro Kimura, MD Nagoya, Japan OBJECTIVES BACKGROUND METHODS RESULTS CONCLUSIONS We investigated whether a lack of inertia force of late systolic aortic flow and/or apical asynergy provoke early diastolic dysfunction in patients with coronary artery disease (CAD). Left ventricular (LV) isolated diastolic dysfunction is a well-recognized cause of heart failure. We evaluated LV apical wall motion and obtained left ventricular ejection fraction (LVEF) by left ventriculography in 101 patients who underwent cardiac catheterization to assess CAD. We also computed the LV relaxation time constant (Tp) and the inertia force of late systolic aortic flow from the LV pressure (P) first derivative of left ventricular pressure (dp/dt) relation. Using color Doppler echocardiography, we measured the propagation velocity of LV early diastolic filling flow (Vp). Patients with LVEF 50% (preserved systolic function [PSF], n 83) were divided into 2 subgroups: patients with inertia force (n 53) and without inertia force (n 30). No patient with systolic dysfunction (SDF) (LVEF 50%) had inertia force (n 18). The Tp was significantly longer in patients with SDF ( ms) and with PSF without inertia force ( ms) than in those with PSF with inertia force ( ms) (p 0.001). The Vp was significantly less in the former 2 groups than in the last group. In patients with PSF, LV apical wall motion abnormality was less frequently observed in those with inertia force than in those without (p ). An absence of inertia force in patients with PSF is one of the causes of isolated diastolic dysfunction in patients with CAD. Normal LV apical wall motion is substantial enough to give inertia to late systolic aortic flow. (J Am Coll Cardiol 2006;48:983 91) 2006 by the American College of Cardiology Foundation More than 40% of patients suffering from congestive heart failure have preserved left ventricular ejection fraction (LVEF) (1 3). An elevated left atrial pressure with left ventricular (LV) diastolic dysfunction causes symptoms of heart failure at rest and during exercise (4 7). Several pathophysiological conditions, such as myocardial hypertrophy, myocardial ischemia, interstitial fibrosis of the LV wall, and abnormal Ca 2 handling in myocytes, are seen in patients with diastolic dysfunction (8 12). The role of hypertension as a cause of diastolic heart failure has been well recognized (13,14). In contrast, coronary artery disease (CAD), especially with prior myocardial infarction (MI), is acknowledged as the most common cause of systolic heart failure (13). Although patients suffering from diastolic heart failure have a high incidence of CAD, including MI (1,14,15), CAD s role as a cause of diastolic heart failure has not been fully elucidated. Accordingly, in patients with CAD, we hypothesized that mild LV systolic dysfunction and/or LV apical asynergy may be associated with LV abnormal relaxation and impaired early diastolic filling. From the Department of Internal Medicine and Pathophysiology, Nagoya City University Graduate School of Medical Sciences, Nagoya, Japan. Manuscript received January 23, 2006; revised manuscript received April 14, 2006, accepted April 17, METHODS Study subjects. Study subjects consisted of 101 consecutive patients with suspected CAD who underwent cardiac catheterization. Patients with an acute coronary syndrome, primary valvular heart disease, atrial fibrillation, or intraventricular conduction disturbance were excluded from the study. According to the findings of cardiac catheterization, 91 patients had CAD, 36 without prior MI and 55 with prior MI. Coronary artery disease was defined as a narrowing of at least 50% in luminal diameter of 1 or more of the major coronary arteries as determined by selective coronary angiography. Prior MI was diagnosed on the finding of localized LV wall motion abnormality using biplane contrast left ventriculography with related electrocardiographic changes. Of the 55 MI patients, 37 had anteriorwall MI, 11 had inferior-wall MI, and 7 had combined anterior- and inferior-wall MI. The remaining 10 patients (those not identified as having CAD) had neither significant coronary stenosis nor LV wall motion abnormality, but had atypical chest pain. On the basis of the LVEF obtained by biplane left ventriculography, patients were divided into 2 groups: the preserved LV systolic function (PSF) group, which had LVEFs 50% (n
2 984 Yoshida et al. JACC Vol. 48, No. 5, 2006 Diastolic Dysfunction in Coronary Artery Disease September 5, 2006: Abbreviations and Acronyms CAD coronary artery disease dp/dt first derivative of left ventricular pressure E/A ratio of peak flow velocity during early diastole to peak flow velocity during atrial contraction Em peak mitral annular velocity during early diastole IQR interquartile range LV left ventricle/ventricular LVEF left ventricular ejection fraction MI myocardial infarction PSF preserved systolic function SDF systolic dysfunction Sm peak mitral annular velocity during systole Tp LV relaxation time constant obtained from LV pressure dp/dt relation Tw LV relaxation time constant obtained by the method proposed by Weiss et al. (18) Vp propagation velocity of early diastolic filling flow 83), and the LV systolic dysfunction (SDF) group, which had ejection fractions 50% (n 18). Details of study patients are shown in Table 1, and a flow diagram of their classification is shown in Figure 1. All patients were in New York Heart Association functional class II, and no patient had decompensated heart failure at the time of catheterization. Thus, this study was designed to investigate not the background of diastolic heart failure but the cause of diastolic dysfunction (8). Then, we reclassified the patients according to the definite criteria for isolated diastolic dysfunction on the basis of the invasive data (LVEF 50% as an index of preserved LV systolic function and time constant of LV pressure decay during isovolumic relaxation [Tw] 48 ms as a definition of abnormal LV relaxation) presented by Zile and Brutsaert (8) and the European Study Group on Diastolic Heart Failure (16). We retrospectively reanalyzed whether patients with PSF without inertia force belonged to the definite criteria for diastolic dysfunction. All studies were performed while patients were receiving cardiac medications. All subjects gave written informed consent to participate in the study, and the study was performed according to the regulations proposed by the Ethical Guidelines Committee of the Nagoya City University Graduate School of Medical Sciences. Doppler echocardiography. All patients were examined at rest lying in the left semilateral decubitus position. Doppler measurements were made using a Power Vision-6000 or (Toshiba Medical Co., Tokyo, Japan) echocardiographic system with a 2.5-MHz transducer. The acquisition of Doppler data was performed by 1 observer throughout the study. The transmitral flow velocity waveform at the mitral orifice was obtained by pulsed Doppler echocardiography, and the ratio of peak flow velocity during early diastole to that during atrial contraction (E/A) was calculated. As Doppler parameters of LV systolic and early diastolic function, which are relatively independent of preload to the LV, peak mitral annular velocity during systole (Sm) and that during early diastole (Em) were also measured at the septal and lateral corners of the mitral annulus using pulsed tissue Doppler imaging. The mean value of velocities at both sides was used in statistical analysis. The propagation of the peak of the early diastolic flow velocity wave in the LV (Vp) was imaged by appropriately changing the first aliasing limit of the color M-mode Doppler signals. The time-distance slope of the peak velocity tracing was measured as Vp; the reproducibility of these measurements in our hospital was as reported elsewhere (17). Cardiac catheterization. Diagnostic cardiac catheterization was performed within 2 h after echocardiography. Before contrast material was injected into the LV or coronary artery, LV pressure was obtained using a cathetertipped micromanometer (SPC-454D, Millar Instrument Co., Houston, Texas) and recorded on a polygraph system (RMC-2000, Nihon Kohden Inc., Tokyo, Japan) and also on a digital data recorder (NR-2000, Keyence, Osaka, Japan). The offset of pressure waves obtained using a catheter-tipped micromanometer was adjusted to that obtained using a fluid-filled system. From the recorded pressure waves, the peak negative first derivative of left ventricular pressure (dp/dt) was determined, and then Tw was calculated using the method proposed by Weiss et al. (18). In the calculation of Tw, the following assumption is applied: a monoexponential curve fitting with LV pressure decay after the phase of peak negative dp/dt has a zero asymptote. This assumption may bring a possibility that Tw is dependent on LV contraction phase and less sensitive to the deterioration of LV relaxation. Another LV relaxation time constant (Tp), which is relatively independent of LV Table 1. Clinical Information in the Subjects, Classified According to Left Ventricular Systolic Function and Inertia Force Total Number of Patients Atypical Chest Pain CAD Without MI Underlying Disease CAD With MI Anterior Inferior Combined Male/ Female Clinical Characteristics Age (yrs) HR (beats/min) MAP (mm Hg) PSF with IF / PSF without IF / SDF / CAD coronary artery disease; HR heart rate; IF inertia force; MAP mean arterial pressure; MI myocardial infarction; PSF preserved left ventricular systolic function; SDF left ventricular systolic dysfunction.
3 JACC Vol. 48, No. 5, 2006 September 5, 2006: Yoshida et al. Diastolic Dysfunction in Coronary Artery Disease 985 Figure 1. A flow diagram of patients classification. (A) Patients classification from the viewpoint of baseline disease. (B) Patients classification from the standpoint of left ventricular function. CAD coronary artery disease; Combined MI anterior myocardial infarction plus inferior MI; LVEF left ventricular ejection fraction. contractile phase and has a floating asymptote, was calculated from the LV pressure (P) dp/dt relation (phase loop) according to the method proposed by Sugawara et al. (19). From the phase loops, we also computed the inertia force of late systolic aortic flow (19). Details of the calculations are indicated in Figure 2. Little fluctuation was observed on the obtained phase loops, so that small amount of inertia force may be erroneously calculated in some patients without having an apparently observed bump (red area in Fig. 2A) in those loops around the phase of peak negative dp/dt. The consensus we reached by reviewing the phase loops in all patients was that we could confirm the existence of the Figure 2. Left ventricular pressure (LVP) first derivative of left ventricular pressure (dp/dt) relationship (phase loop). (A) A loop obtained from a patient with inertia force. (B) A loop obtained from a patient without inertia force. The negative inverse slope of the best linear-fitting line between the points a and b is equal to the time constant of exponential pressure decay during isovolumic relaxation (Tp). The Tp was 56.3 ms in A and 83.1 ms in B. The area in red divided by the vertical distance between P 0,0 and point d is equal to the amount of pressure decay augmented by the effect of the inertia of blood flowing out of the LV, and is defined as the inertia force. The inertia force in A was 3.6 mm Hg, and 0.12 mm Hg in B.
4 986 Yoshida et al. JACC Vol. 48, No. 5, 2006 Diastolic Dysfunction in Coronary Artery Disease September 5, 2006: bump of phase loops in patients with computed inertia force 0.5 mm Hg. Thus, we defined the patients with computed inertia force 0.5 mm Hg as those with inertia force, and the patients with calculated inertia force 0.5 mm Hg as those without inertia force. We then divided the patients with PSF into 2 subgroups: patients with inertia force (n 53) and those without inertia force (n 30). No patient with SDF had inertia force (Fig. 1). Immediately after the pressure measurements, biplane contrast left ventriculography was performed. Left ventricular end-systolic and end-diastolic volumes were calculated using the method of Chapman et al. (20), using a cardiac image analyzer. The LVEF was then determined. The LV end-systolic volume was divided by the body surface area of each patient and expressed as an LV end-systolic volume index to normalize body size. Regional LV wall motion was evaluated using the centerline method (21), which is a reliable method to assess LV regional wall motion from contrast left ventriculography. As we reported previously (22), LV apical wall motion abnormality was confirmed when wall motion deteriorated by more than 2 standard deviations from the normal wall-motion amplitude on at least 20 lines that formed the apex of the 200 equidistant lines, which were drawn perpendicular to the centerline extending from the end-diastolic to the endsystolic counter in each 30 right anterior oblique (100 lines) and 60 left anterior oblique (100 lines) projection. Data related to LV pressure waves were analyzed by 1 observer, and data concerned with left ventriculography were independently analyzed by another observer through the study. Both observers were blinded to the Doppler data. Statistical analysis. Normally distributed continuous data are expressed as mean SD. The inertia force is presented as the median with interquartile range (IQR) (25th to 75th percentiles). Relationships between 2 parameters were evaluated using Spearman s correlation coefficients by ranks. Differences in parameters between 2 groups were compared Table 2. Summary of Hemodynamic Variables of the Subjects in Each Group PSF With Inertia Force PSF Without Inertia Force SDF LVEF (%) * * LV ESVI (ml/m 2 ) * * Sm (cm/s) Tp (ms) * * Tw (ms) * * Peak negative dp/dt 1, , , (mm Hg/s) E/A Em * Vp (cm/s) * * p values are those after Bonferroni adjustment among 3 comparisons. *p 0.001; p 0.01; p 0.05 (vs. PSF with inertia force). dp/dt first derivative of left ventricular pressure; E/A the ratio of transmitral flow velocity during early diastole to that during atrial contraction; Em peak mitral annular velocity during early diastole; LVEF left ventricular ejection fraction; LV ESVI left ventricular end-systolic volume index; Sm peak mitral annular velocity during systole; Tp left ventricular relaxation time constant calculated from phase loop; Tw left ventricular relaxation time constant calculated by Weiss method (18); Vp propagation velocity of left ventricular early diastolic filling flow; other abbreviations as in Table 1. using the unpaired Student t test. Differences between 3 groups were evaluated using 1-way analysis of variance with a Bonferroni adjustment. The p values shown in Table 2 are those after Bonferroni adjustment among 3 comparisons. A difference in incidence was compared using the chi-square test. Differences with p values 0.05 were considered significant. RESULTS The median of calculated inertia force was 1.19 (IQR 0.19 to 3.98) mm Hg and ranged from to 12.0 mm Hg. The inertia force significantly correlated with the LV systolic function parameters, such as LVEF and LV endsystolic volume index (r 0.72, p and r 0.68, p , respectively) (Fig. 3). It also significantly correlated with the parameters of LV relaxation, Tp, and of LV early diastolic filling, Vp (r 0.31, p and r 0.73, p , respectively) (Fig. 4). The correlation coefficient was greater in the relation between the inertia force and Vp than in that between the inertia force and Tp. No significant differences were found in age, heart rate, or mean blood pressure between the patients with PSF with or without inertia force and those with SDF (Table 1). Time constants of LV relaxation were significantly greater in patients with SDF and with PSF without inertia force than in those with PSF with inertia force. The peak negative dp/dt was significantly less in patients with SDF and with PSF without inertia force than in those with PSF with inertia force. Propagation velocity of early diastolic filling flow was also significantly less in the first 2 groups than in the last group. There were no significant differences in Tp, Tw, peak negative dp/dt, or Vp between patients with SDF and those with PSF without inertia force (Figs. 5 and 6). The E/A ratio of the transmitral flow velocity waveform also was not significantly different between the groups. In contrast, Em was significantly less in patients with SDF and with PSF without inertia force than in those with PSF with inertia force. No significant difference was found in Em between patients with SDF and those with PSF without inertia force (Fig. 6). Left ventricular ejection fraction was greater in patients with PSF with inertia force than in those with PSF without inertia force. Similarly, Sm was also significantly greater in the former than in the latter. Left ventricular end-systolic volume index was significantly lower in the former than in the latter (Fig. 7). These data are summarized in Table 2. In 53 patients with PSF with inertia force, 5 had LV apical asynergy and 48 did not. On the other hand, in 30 patients with PSF without inertia force, 26 had apical asynergy and 4 did not. The incidence of LV apical asynergy was significantly higher in patients without inertia force than in those with inertia force (chi square 48.8, p ).
5 JACC Vol. 48, No. 5, 2006 September 5, 2006: Yoshida et al. Diastolic Dysfunction in Coronary Artery Disease 987 Figure 3. Relationships between inertia force and left ventricular (LV) systolic function parameters. (A) Relation of inertia force to LV ejection fraction (LVEF). A significant positive correlation is observed. (B) Relation of inertia force to LV end-systolic volume index (ESVI). A significant inverse correlation is found. Circles patients with preserved systolic function with inertia force; squares patients with preserved systolic function without inertia force; X patients with systolic dysfunction. In 22 patients with PSF and a time constant Tw 48 ms, who met the definite criteria for isolated diastolic dysfunction, 1 had inertia force and 21 did not. In contrast, in 61 patients with PSF and a time constant Tw 48 ms, 52 had inertia force and 9 did not. The rate at which patients did not have inertia force was significantly greater in those who satisfied the definite criteria for isolated diastolic dysfunction (chi square 45.6, p ). DISCUSSION The present study indicates that patients with PSF without inertia force have similar levels of deterioration in LV relaxation and Vp compared with those in patients with SDF. The lack of inertia force in patients with PSF impairs LV relaxation and early diastolic filling and it may be one of the causes of isolated diastolic dysfunction in CAD patients. Normal LV apical wall motion appears to be substantial enough to give inertia to late systolic aortic flow. Coupling of LV systolic and diastolic function mediated by inertia force. From the viewpoint of cardiac mechanics, Gilbert and Glantz (23) reported that LVs with good systolic function have relatively smaller LV end-systolic volumes, producing a greater magnitude of LV rearrangement at the isovolumic relaxation phase by releasing elastic energy stored during systole. This phenomenon, called LV elastic recoil, speeds LV relaxation independently of the Ca 2 reuptake process by the sarcoplasmic reticulum (19, 23). Figure 4. Relationships between inertia force and parameters of left ventricular relaxation (Tp) and left ventricular early diastolic filling (Vp). A Relation of inertia force to Tp. A significant inverse correlation is observed. B Relation of inertia force to Vp. A significant positive correlation is found. Symbols are as in Figure 3; other abbreviations as in Figure 1.
6 988 Yoshida et al. JACC Vol. 48, No. 5, 2006 Diastolic Dysfunction in Coronary Artery Disease September 5, 2006: Figure 5. Comparisons of parameters regarding left ventricular relaxation between patients with preserved systolic function (PSF) with or without inertia force and those with systolic dysfunction (SDF). (A, B) The time constant Tp from phase loops and the time constant Tw obtained by the method of Weiss et al. (18) were significantly greater in patients with SDF and with PSF without inertia force than in those with PSF with inertia force. (C) The peak negative dp/dt was significantly less in the first 2 groups than in the last group. *p 0.001; p 0.01; p Other abbreviations as in Figure 4. Eichhorn et al. (24) demonstrated that a hyperbolic rather than a linear relationship was observed between LV contractile function as shown by end-systolic elastance and LV relaxation as shown by the slope of the time constant to the LV end-systolic pressure relation. The concept that LV myocardial contraction and ejection dynamics are intimately linked to LV relaxation has been established (25 27). In addition, Sugawara et al. (19) reported that late systolic aortic flow ejected from a LV with good contraction has inertia force. The blood, once set in motion, will continue in motion because of its inertia until the heart stops it (28). In late systole, when LV muscle shortening has reached a limit but its tension-bearing ability is still maintained, the inertia of the blood flowing out of the LV causes swift end-systolic unloading of the LV, producing a much smaller LV end-systolic volume and much greater elastic recoil force (19,22,29). The schematic diagram that demonstrates the idea that inertia force of late systolic aortic flow enhances LV elastic recoil is shown in Figure 8. Thus, the enhanced LV elastic recoil brought by the inertia force of late systolic aortic flow in patients with good LV contraction may produce faster LV relaxation (30). Furthermore, we demonstrated that the direct effect of LV end-systolic volume index on Vp was much greater than that of LV relaxation time constant on Vp (17). Smaller LV end-systolic volume, which is usually accompanied by a marked ellipsoidal LV cavity shape during the isovolumic relaxation phase, produces a greater intraventricular pressure gradient between the LV base and apex during the early diastolic filling phase and increases Vp (31). Thus, in addition to LV relaxation, LV elastic recoil itself also has a striking effect on Vp. As we demonstrated in this study, the magnitude of inertia force significantly and positively correlated with LV ejection fraction and inversely with LV end-systolic volume index, supporting the hypothesis shown in Figure 8. The finding that the inertia force showed a much closer relationship with Vp than with Tp may indicate that enhanced LV elastic recoil directly speeds Vp in addition to the effect through accelerated LV relaxation, similar to our previous report (17). Thus, the concept of hemodynamically induced inertia force may contribute further to the understanding of LV contraction-relaxation coupling, which has been mainly considered from the viewpoint of LV mechanics (25 27). If the LV does not have inertia force even though LVEF is more than 50%, it would not have enough elastic recoil to speed LV relaxation and Vp. One of the main messages of the present study that the lack of inertia force deteriorates LV relaxation was also confirmed by the finding that the patients with PSF without inertia force had a decreased Em (32,33). We found more significant decreases in LVEF and Sm in patients with PSF without inertia force than in those with PSF with inertia force, and we also found a more significant increase
7 JACC Vol. 48, No. 5, 2006 September 5, 2006: Yoshida et al. Diastolic Dysfunction in Coronary Artery Disease 989 Figure 6. Comparisons of the mitral annular velocity during early diastole (Em) and the propagation velocity of left ventricular early diastolic flow (Vp) between the patient groups. (A) Em was significantly lower both in patients with SDF and in those with PSF without inertia force than in those with PSF with inertia force. (B) Vp was also significantly less in the first 2 groups than in the last group. *p 0.001; p Other abbreviations as in Figure 5. in LV end-systolic volume index in the former patients than in the latter. These findings suggest that patients with PSF without inertia force have mild LV systolic dysfunction. Calculation of inertia force. Inertia force can be calculated from the LV P-dP/dt relation (phase loop) (19). Left ventricular pressure decay during the isovolumic relaxation phase can be assumed to be exponential if this process only depends on Ca 2 reuptake by the sarcoplasmic reticulum in myocytes (23). In the LV P-dP/dt plane, the exponential relationship is shown as a straight line. However, enhanced elastic recoil produced by inertia force observed in a LV with good contraction may shift such an exponential decay Figure 7. Comparisons of left ventricular systolic function parameters between patients with PSF with inertia force and those with PSF without inertia force. (A) Left ventricular ESVI was significantly smaller in patients with PSF with inertia force than in those with PSF without inertia force. (B) Left ventricular ejection fraction (LVEF) was significantly greater in the former than in the latter. (C) Peak mitral annular velocity during systole (Sm) was also significantly greater in the former than in the latter. *p 0.001; p Other abbreviations as Figures 3 and 5.
8 990 Yoshida et al. JACC Vol. 48, No. 5, 2006 Diastolic Dysfunction in Coronary Artery Disease September 5, 2006: Figure 8. Schematic diagram demonstrating the concept that inertia force of late systolic aortic flow enhances left ventricular (LV) elastic recoil. (A) Left ventricles with relatively better LV systolic function give inertia to the late systolic aortic flow. In late systole, when LV muscle shortening has reached a limit but its tension-bearing ability is still maintained, the inertia of the blood flowing out of the LV causes swift end-systolic unloading of the LV, producing additional LV muscle shortening and hence smaller LV end-systolic volume. The resulting greater elastic recoil force brings faster LV relaxation. (B) Left ventricles with impaired contractile function do not give inertia to the late systolic aortic flow. Hence, the swift LV end-systolic unloading caused by the inertia force does not occur. LV relaxation is slow because of the lack of LV elastic recoil. downward at the beginning of relaxation, as shown in Figure 2. In accord with the method proposed by Sugawara et al. (19), we calculated the inertia force as a deviation of the LV P-dP/dt relation during the isovolumic relaxation phase from the expected straight line, which would be observed in a LV without significant elastic recoil. LV apical asynergy and inertia force. In the present study, we demonstrated that the lack of inertia force of late systolic aortic flow has a significant relation with LV apical asynergy. We also previously reported that in patients with CAD, apically directed flow during isovolumic relaxation observed in the LV with good EF helps to facilitate LV early diastolic filling; however, such flow was not observed in patients with LV apical asynergy (22,34). Normal LV apical contraction should play an important role in producing the inertia force of late systolic aortic flow, and then maintain normal LV behavior from isovolumic relaxation to early diastolic filling. Comparison to previous studies. Baicu et al. (35) have recently indicated that no significant differences are found in LVEF, pre-load recruitable stroke work, or peak dp/dt between normal control subjects and patients with diastolic heart failure (LVEF 50%). They concluded that the pathophysiology of diastolic heart failure does not appear to be due to significant abnormalities in LV systolic properties. In contrast, using tissue Doppler imaging of the mitral annulus, Brucks et al. (14) have demonstrated that heart failure with preserved LVEF is associated with mild systolic dysfunction in addition to diastolic dysfunction, which is inconsistent with the study by Baicu et al. (35). Our results regarding LVEF, LV end-systolic volume index, and Sm support the finding reported by Brucks et al. (14). They also reported that 60% to 70% of their subjects had CAD. Furthermore, Tsutsui et al. (15) reported 34% of their patients suffering from heart failure with preserved LV systolic function had MI. Thus, in the pathophysiology of isolated diastolic heart failure in CAD patients, LV apical wall motion abnormality due to prior MI may be important. From the viewpoint of the definite criteria for isolated diastolic dysfunction, we reanalyzed the data of our patients with PSF. We then demonstrated that most patients who satisfied the criteria did not have inertia force, whereas a majority of patients who did not meet the criteria had inertia force. These findings suggest that a lack of inertia force of late systolic aortic flow is one of the aspects of isolated diastolic dysfunction. Clinical implications. An absence of inertia force of late systolic aortic flow causes both LV relaxation and early diastolic filling to be impaired in patients with PSF. Thus, an evaluation to determine whether such patients have inertia force should be important for the assessment of their LV early diastolic function. However, an invasive examination is needed for this issue. Our present study indicates that LV apical asynergy observed in CAD patients frequently accompanies the lack of inertia force. One could noninvasively evaluate whether patients with CAD have isolated diastolic dysfunction by observing their LV apical wall motion using echocardiography. CONCLUSIONS The lack of inertia force of late systolic aortic flow plays a substantial role in provoking isolated diastolic dysfunction in patients with CAD. Mild LV systolic dysfunction and LV apical asynergy may be related to this pathophysiology. Reprint requests and correspondence: Dr. Nobuyuki Ohte, Department of Internal Medicine and Pathophysiology, Nagoya City University Graduate School of Medical Sciences, 1 Kawasumi, Mizuho-cho, Mizuho-ku, Nagoya , Japan. ohte@med.nagoya-cu.ac.jp. REFERENCES 1. Senni M, Tribouilloy CM, Rodeheffer RJ, et al. Congestive heart failure in the community: a study of all incident cases in Olmsted County, Minnesota, in Circulation 1998;98: Kitzman DW, Little WC, Brubaker PH, et al. Pathophysiological characterization of isolated diastolic heart failure in comparison to systolic heart failure. JAMA 2002;288: Smith GL, Masoudi FA, Vaccarino V, Radford MJ, Krumholz HM. Outcomes in heart failure patients with preserved ejection fraction: mortality, readmission, and functional decline. J Am Coll Cardiol 2003;41: Packer M. Abnormalities of diastolic function as a potential cause of exercise intolerance in chronic heart failure. Circulation 1990;81 Suppl 2:III Davies SW, Fussell AL, Jordan SL, Poole-Wilson PA, Lipkin DP. Abnormal diastolic filling patterns in chronic heart failure relationship to exercise capacity. Eur Heart J 1992;13:
9 JACC Vol. 48, No. 5, 2006 September 5, 2006: Yoshida et al. Diastolic Dysfunction in Coronary Artery Disease Wheeldon NM, Clarkson P, MacDonald TM. Diastolic heart failure. Eur Heart J 1994;15: Little WC, Kitzman DW, Cheng CP. Diastolic dysfunction as a cause of exercise intolerance. Heart Fail Rev 2000;5: Zile MR, Brutsaert DL. New concepts in diastolic dysfunction and diastolic heart failure: Part I: diagnosis, prognosis, and measurements of diastolic function. Circulation 2002;105: Dougherty AH, Naccarelli GV, Gray EL, Hicks CH, Goldstein RA. Congestive heart failure with normal systolic function. Am J Cardiol 1984;54: Grossman W. Diastolic dysfunction in congestive heart failure. N Engl J Med 1991;325: Brutsaert DL, Sys SU, Gillebert TC. Diastolic failure: pathophysiology and therapeutic implications. J Am Coll Cardiol 1993;22: Lenihan DJ, Gerson MC, Hoit BD, Walsh RA. Mechanisms, diagnosis, and treatment of diastolic heart failure. Am Heart J 1995;130: Kitzman DW. Diastolic heart failure in the elderly. Heart Fail Rev 2002;7: Brucks S, Little WC, Chao T, et al. Contribution of left ventricular diastolic dysfunction to heart failure regardless of ejection fraction. Am J Cardiol 2005;95: Tsutsui H, Tsuchihashi M, Takeshita A. Mortality and readmission of hospitalized patients with congestive heart failure and preserved versus depressed systolic function. Am J Cardiol 2001;88: European Study Group on Diastolic Heart Failure. How to diagnose diastolic heart failure. Eur Heart J 1998;19: Ohte N, Narita H, Akita S, Kurokawa K, Hayano J, Kimura G. Striking effect of left ventricular systolic performance on propagation velocity of left ventricular early diastolic filling flow. J Am Soc Echocardiogr 2001;14: Weiss JL, Frederiksen JW, Weisfeldt ML. Hemodynamic determinants of the time-course of fall in canine left ventricular pressure. J Clin Invest 1976;58: Sugawara M, Uchida K, Kondoh Y, et al. Aortic blood momentum the more the better for the ejecting heart in vivo? Cardiovasc Res 1997;33: Chapman CB, Baker O, Reynolds J, Bonte FJ. Use of biplane cinefluorography for measurement of ventricular volume. Circulation 1958;18: Sheehan FH, Bolson EL, Dodge HT, Mathey DG, Schofer J, Woo HW. Advantages and applications of the centerline method for characterizing regional ventricular function. Circulation 1986; 74: Ohte N, Narita H, Akita S, et al. The mechanism of emergence and clinical significance of apically directed intraventricular flow during isovolumic relaxation. J Am Soc Echocardiogr 2002;15: Gilbert JC, Glantz SA. Determinants of left ventricular filling and of the diastolic pressure-volume relation. Circ Res 1989;64: Eichhorn EJ, Willard JE, Alvarez L, et al. Are contraction and relaxation coupled in patients with and without congestive heart failure? Circulation 1992;85: Brutsaert DL, Sys SU. Relaxation and diastole of the heart. Physiol Rev 1989;69: Burkhoff D, de Tombe PP, Hunter WC. Impact of ejection on magnitude and time course of ventricular pressure-generating capacity. Am J Physiol (Heart Circ Physiol) 1993;265:H Brutsaert DL, Sys SU. Diastolic dysfunction in heart failure. J Card Fail 1997;3: Noble MI. The contribution of blood momentum to left ventricular ejection in the dog. Circ Res 1968;23: Sugawara M, Uchida K, Kondoh Y, Jones CJH. Cardiac utilization of the momentum of blood. In: Sasayama S, editor. New Horizons for Failing Heart Syndrome. Tokyo: Springer, 1996: Ohte N, Narita H, Sugawara M, et al. Clinical usefulness of carotid arterial wave intensity in assessing left ventricular systolic and early diastolic performance. Heart Vessels 2003;18: Nikolic SD, Feneley MP, Pajaro OE, Rankin JS, Yellin EL. Origin of regional pressure gradients in the left ventricle during early diastole. Am J Physiol 1995;268:H Oki T, Tabata T, Yamada H, et al. Clinical application of pulsed Doppler tissue imaging for assessing abnormal left ventricular relaxation. Am J Cardiol 1997;79: Ohte N, Narita H, Hashimoto T, Akita S, Kurokawa K, Fujinami T. Evaluation of left ventricular early diastolic performance by color tissue Doppler imaging of the mitral annulus. Am J Cardiol 1998;82: Yanada A, Ohte N, Narita H, et al. The role of apically directed intraventricular isovolumic relaxation flow in speeding early diastolic left ventricular filling. J Am Soc Echocardiogr 2003;16: Baicu CF, Zile MR, Aurigemma GP, Gaasch WH. Left ventricular systolic performance, function, and contractility in patients with diastolic heart failure. Circulation 2005;111:
Mechanisms of heart failure with normal EF Arterial stiffness and ventricular-arterial coupling. What is the pathophysiology at presentation?
 Mechanisms of heart failure with normal EF Arterial stiffness and ventricular-arterial coupling What is the pathophysiology at presentation? Ventricular-arterial coupling elastance Central arterial pressure
Mechanisms of heart failure with normal EF Arterial stiffness and ventricular-arterial coupling What is the pathophysiology at presentation? Ventricular-arterial coupling elastance Central arterial pressure
Diastology Disclosures: None. Dias2011:1
 Diastology 2011 James D. Thomas, M.D., F.A.C.C. Cardiovascular Imaging Center Department of Cardiology Cleveland Clinic Foundation Cleveland, Ohio, USA Disclosures: None Dias2011:1 Is EVERYBODY a member!?!
Diastology 2011 James D. Thomas, M.D., F.A.C.C. Cardiovascular Imaging Center Department of Cardiology Cleveland Clinic Foundation Cleveland, Ohio, USA Disclosures: None Dias2011:1 Is EVERYBODY a member!?!
LV geometric and functional changes in VHD: How to assess? Mi-Seung Shin M.D., Ph.D. Gachon University Gil Hospital
 LV geometric and functional changes in VHD: How to assess? Mi-Seung Shin M.D., Ph.D. Gachon University Gil Hospital LV inflow across MV LV LV outflow across AV LV LV geometric changes Pressure overload
LV geometric and functional changes in VHD: How to assess? Mi-Seung Shin M.D., Ph.D. Gachon University Gil Hospital LV inflow across MV LV LV outflow across AV LV LV geometric changes Pressure overload
Research Article Prognostic Value of Left Ventricular Diastolic Dysfunction in Patients Undergoing Cardiac Catheterization for Coronary Artery Disease
 Cardiology Research and Practice Volume 2012, Article ID 243735, 8 pages doi:10.1155/2012/243735 Research Article Prognostic Value of Left Ventricular Diastolic Dysfunction in Patients Undergoing Cardiac
Cardiology Research and Practice Volume 2012, Article ID 243735, 8 pages doi:10.1155/2012/243735 Research Article Prognostic Value of Left Ventricular Diastolic Dysfunction in Patients Undergoing Cardiac
Basic Approach to the Echocardiographic Evaluation of Ventricular Diastolic Function
 Basic Approach to the Echocardiographic Evaluation of Ventricular Diastolic Function J A F E R A L I, M D U N I V E R S I T Y H O S P I T A L S C A S E M E D I C A L C E N T E R S T A F F C A R D I O T
Basic Approach to the Echocardiographic Evaluation of Ventricular Diastolic Function J A F E R A L I, M D U N I V E R S I T Y H O S P I T A L S C A S E M E D I C A L C E N T E R S T A F F C A R D I O T
The Patient with Atrial Fibrilation
 Assessment of Diastolic Function The Patient with Atrial Fibrilation Assoc. Prof. Adriana Ilieşiu, FESC University of Medicine Carol Davila Bucharest, Romania Associated Conditions with Atrial Fibrillation
Assessment of Diastolic Function The Patient with Atrial Fibrilation Assoc. Prof. Adriana Ilieşiu, FESC University of Medicine Carol Davila Bucharest, Romania Associated Conditions with Atrial Fibrillation
Left Ventricular Diastolic Dysfunction in South Indian Essential Hypertensive Patient
 Left Ventricular Diastolic Dysfunction in South Indian Essential Hypertensive Patient Dr. Peersab.M. Pinjar 1, Dr Praveenkumar Devarbahvi 1 and Dr Vasudeva Murthy.C.R 2, Dr.S.S.Bhat 1, Dr.Jayaraj S G 1
Left Ventricular Diastolic Dysfunction in South Indian Essential Hypertensive Patient Dr. Peersab.M. Pinjar 1, Dr Praveenkumar Devarbahvi 1 and Dr Vasudeva Murthy.C.R 2, Dr.S.S.Bhat 1, Dr.Jayaraj S G 1
좌심실수축기능평가 Cardiac Function
 Basic Echo Review Course 좌심실수축기능평가 Cardiac Function Seonghoon Choi Cardiology Hallym university LV systolic function Systolic function 좌심실수축기능 - 심근의수축으로심실에서혈액을대동맥으로박출하는기능 실제임상에서 LV function 의의미 1Diagnosis
Basic Echo Review Course 좌심실수축기능평가 Cardiac Function Seonghoon Choi Cardiology Hallym university LV systolic function Systolic function 좌심실수축기능 - 심근의수축으로심실에서혈액을대동맥으로박출하는기능 실제임상에서 LV function 의의미 1Diagnosis
Diastolic Heart Failure
 Chronic Heart Failure Prevalence overall = 2-3 % Diastolic Heart Failure Patrick Wouters University Hospital Ghent Belgium (Heart Failure + Asymptomatic Ventricular Dysfunction) Prevalence > 70 y = 10-20
Chronic Heart Failure Prevalence overall = 2-3 % Diastolic Heart Failure Patrick Wouters University Hospital Ghent Belgium (Heart Failure + Asymptomatic Ventricular Dysfunction) Prevalence > 70 y = 10-20
Introduction. Toshihiko Goto 1 Kazuaki Wakami 1 Hidekatsu Fukuta 1 Hiroshi Fujita 1 Tomomitsu Tani 1 Nobuyuki Ohte 1
 DOI 10.1007/s00380-015-0657-1 ORIGINAL ARTICLE Patients with left ventricular ejection fraction greater than 58 % have fewer incidences of future acute decompensated heart failure admission and all cause
DOI 10.1007/s00380-015-0657-1 ORIGINAL ARTICLE Patients with left ventricular ejection fraction greater than 58 % have fewer incidences of future acute decompensated heart failure admission and all cause
Advance Publication by-j-stage
 Circulation Journal Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp Relationship Between Effective Arterial Elastance, Total Vascular Resistance, and Augmentation Index at
Circulation Journal Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp Relationship Between Effective Arterial Elastance, Total Vascular Resistance, and Augmentation Index at
Evalua&on)of)Le-)Ventricular)Diastolic) Dysfunc&on)by)Echocardiography:) Role)of)Ejec&on)Frac&on)
 Evalua&on)of)Le-)Ventricular)Diastolic) Dysfunc&on)by)Echocardiography:) Role)of)Ejec&on)Frac&on) N.Koutsogiannis) Department)of)Cardiology) University)Hospital)of)Patras)! I have no conflicts of interest
Evalua&on)of)Le-)Ventricular)Diastolic) Dysfunc&on)by)Echocardiography:) Role)of)Ejec&on)Frac&on) N.Koutsogiannis) Department)of)Cardiology) University)Hospital)of)Patras)! I have no conflicts of interest
Strain/Untwisting/Diastolic Suction
 What Is Diastole and How to Assess It? Strain/Untwisting/Diastolic Suction James D. Thomas, M.D., F.A.C.C. Cardiovascular Imaging Center Department of Cardiology Cleveland Clinic Foundation Cleveland,
What Is Diastole and How to Assess It? Strain/Untwisting/Diastolic Suction James D. Thomas, M.D., F.A.C.C. Cardiovascular Imaging Center Department of Cardiology Cleveland Clinic Foundation Cleveland,
ECHO HAWAII. Role of Stress Echo in Valvular Heart Disease. Not only ischemia! Cardiomyopathy. Prosthetic Valve. Diastolic Dysfunction
 Role of Stress Echo in Valvular Heart Disease ECHO HAWAII January 15 19, 2018 Kenya Kusunose, MD, PhD, FASE Tokushima University Hospital Japan Not only ischemia! Cardiomyopathy Prosthetic Valve Diastolic
Role of Stress Echo in Valvular Heart Disease ECHO HAWAII January 15 19, 2018 Kenya Kusunose, MD, PhD, FASE Tokushima University Hospital Japan Not only ischemia! Cardiomyopathy Prosthetic Valve Diastolic
Evaluation of Native Left Ventricular Function During Mechanical Circulatory Support.: Theoretical Basis and Clinical Limitations
 Review Evaluation of Native Left Ventricular Function During Mechanical Circulatory Support.: Theoretical Basis and Clinical Limitations Tohru Sakamoto, MD, PhD Left ventricular function on patients with
Review Evaluation of Native Left Ventricular Function During Mechanical Circulatory Support.: Theoretical Basis and Clinical Limitations Tohru Sakamoto, MD, PhD Left ventricular function on patients with
Coronary artery disease (CAD) risk factors
 Background Coronary artery disease (CAD) risk factors CAD Risk factors Hypertension Insulin resistance /diabetes Dyslipidemia Smoking /Obesity Male gender/ Old age Atherosclerosis Arterial stiffness precedes
Background Coronary artery disease (CAD) risk factors CAD Risk factors Hypertension Insulin resistance /diabetes Dyslipidemia Smoking /Obesity Male gender/ Old age Atherosclerosis Arterial stiffness precedes
Myocardial performance index, Tissue Doppler echocardiography
 Value of Measuring Myocardial Performance Index by Tissue Doppler Echocardiography in Normal and Diseased Heart Tarkan TEKTEN, 1 MD, Alper O. ONBASILI, 1 MD, Ceyhun CEYHAN, 1 MD, Selim ÜNAL, 1 MD, and
Value of Measuring Myocardial Performance Index by Tissue Doppler Echocardiography in Normal and Diseased Heart Tarkan TEKTEN, 1 MD, Alper O. ONBASILI, 1 MD, Ceyhun CEYHAN, 1 MD, Selim ÜNAL, 1 MD, and
Value of echocardiography in chronic dyspnea
 Value of echocardiography in chronic dyspnea Jahrestagung Schweizerische Gesellschaft für /Schweizerische Gesellschaft für Pneumologie B. Kaufmann 16.06.2016 Chronic dyspnea Shortness of breath lasting
Value of echocardiography in chronic dyspnea Jahrestagung Schweizerische Gesellschaft für /Schweizerische Gesellschaft für Pneumologie B. Kaufmann 16.06.2016 Chronic dyspnea Shortness of breath lasting
Evaluation of Left Ventricular Diastolic Dysfunction by Doppler and 2D Speckle-tracking Imaging in Patients with Primary Pulmonary Hypertension
 ESC Congress 2011.No 85975 Evaluation of Left Ventricular Diastolic Dysfunction by Doppler and 2D Speckle-tracking Imaging in Patients with Primary Pulmonary Hypertension Second Department of Internal
ESC Congress 2011.No 85975 Evaluation of Left Ventricular Diastolic Dysfunction by Doppler and 2D Speckle-tracking Imaging in Patients with Primary Pulmonary Hypertension Second Department of Internal
Noninvasive assessment of left ventricular (LV)
 Comparative Value of Tissue Doppler Imaging and M-Mode Color Doppler Mitral Flow Propagation Velocity for the Evaluation of Left Ventricular Filling Pressure* Michal Kidawa, MD; Lisa Coignard, MD; Gérard
Comparative Value of Tissue Doppler Imaging and M-Mode Color Doppler Mitral Flow Propagation Velocity for the Evaluation of Left Ventricular Filling Pressure* Michal Kidawa, MD; Lisa Coignard, MD; Gérard
Echo-Doppler evaluation of left ventricular diastolic function. Michel Slama Amiens France
 Echo-Doppler evaluation of left ventricular diastolic function Michel Slama Amiens France Left ventricular pressure Pressure A wave [ LVEDP LVEDP préa Congestive cardiac failure with preserved systolic
Echo-Doppler evaluation of left ventricular diastolic function Michel Slama Amiens France Left ventricular pressure Pressure A wave [ LVEDP LVEDP préa Congestive cardiac failure with preserved systolic
Diastolic Function Overview
 Diastolic Function Overview Richard Palma BS, RDCS, RCS, APS, FASE Director and Clinical Coordinator The Hoffman Heart and Vascular Institute School of Cardiac Ultrasound None Disclosures Learning Objectives
Diastolic Function Overview Richard Palma BS, RDCS, RCS, APS, FASE Director and Clinical Coordinator The Hoffman Heart and Vascular Institute School of Cardiac Ultrasound None Disclosures Learning Objectives
Objectives. Systolic Heart Failure: Definitions. Heart Failure: Historical Perspective 2/7/2009
 Objectives Diastolic Heart Failure and Indications for Echocardiography in the Asian Population Damon M. Kwan, MD UCSF Asian Heart & Vascular Symposium 02.07.09 Define diastolic heart failure and differentiate
Objectives Diastolic Heart Failure and Indications for Echocardiography in the Asian Population Damon M. Kwan, MD UCSF Asian Heart & Vascular Symposium 02.07.09 Define diastolic heart failure and differentiate
E/Ea is NOT an essential estimator of LV filling pressures
 Euroecho Kopenhagen Echo in Resynchronization in 2010 E/Ea is NOT an essential estimator of LV filling pressures Wilfried Mullens, MD, PhD December 10, 2010 Ziekenhuis Oost Limburg Genk University Hasselt
Euroecho Kopenhagen Echo in Resynchronization in 2010 E/Ea is NOT an essential estimator of LV filling pressures Wilfried Mullens, MD, PhD December 10, 2010 Ziekenhuis Oost Limburg Genk University Hasselt
Tissue Doppler Imaging in Congenital Heart Disease
 Tissue Doppler Imaging in Congenital Heart Disease L. Youngmin Eun, M.D. Department of Pediatrics, Division of Pediatric Cardiology, Kwandong University College of Medicine The potential advantage of ultrasound
Tissue Doppler Imaging in Congenital Heart Disease L. Youngmin Eun, M.D. Department of Pediatrics, Division of Pediatric Cardiology, Kwandong University College of Medicine The potential advantage of ultrasound
Journal of the American College of Cardiology Vol. 44, No. 9, by the American College of Cardiology Foundation ISSN /04/$30.
 Journal of the American College of Cardiology Vol. 44, 9, 2004 2004 by the American College of Cardiology Foundation ISSN 0735-1097/04/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.04.062 Relation
Journal of the American College of Cardiology Vol. 44, 9, 2004 2004 by the American College of Cardiology Foundation ISSN 0735-1097/04/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.04.062 Relation
Mechanisms of False Positive Exercise Electrocardiography: Is False Positive Test Truly False?
 Mechanisms of False Positive Exercise Electrocardiography: Is False Positive Test Truly False? Masaki Izumo a, Kengo Suzuki b, Hidekazu Kikuchi b, Seisyo Kou b, Keisuke Kida b, Yu Eguchi b, Nobuyuki Azuma
Mechanisms of False Positive Exercise Electrocardiography: Is False Positive Test Truly False? Masaki Izumo a, Kengo Suzuki b, Hidekazu Kikuchi b, Seisyo Kou b, Keisuke Kida b, Yu Eguchi b, Nobuyuki Azuma
Index of subjects. effect on ventricular tachycardia 30 treatment with 101, 116 boosterpump 80 Brockenbrough phenomenon 55, 125
 145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
Advanced imaging of the left atrium - strain, CT, 3D, MRI -
 Advanced imaging of the left atrium - strain, CT, 3D, MRI - Monica Rosca, MD Carol Davila University of Medicine and Pharmacy, Bucharest, Romania Declaration of interest: I have nothing to declare Case
Advanced imaging of the left atrium - strain, CT, 3D, MRI - Monica Rosca, MD Carol Davila University of Medicine and Pharmacy, Bucharest, Romania Declaration of interest: I have nothing to declare Case
Left ventricular diastolic function and filling pressure in patients with dilated cardiomyopathy
 Left ventricular diastolic function and filling pressure in patients with dilated cardiomyopathy Bogdan A. Popescu University of Medicine and Pharmacy Bucharest, Romania My conflicts of interest: I have
Left ventricular diastolic function and filling pressure in patients with dilated cardiomyopathy Bogdan A. Popescu University of Medicine and Pharmacy Bucharest, Romania My conflicts of interest: I have
Carlos Eduardo Suaide Silva, Luiz Darcy Cortez Ferreira, Luciana Braz Peixoto, Claudia Gianini Monaco, Manuel Adán Gil, Juarez Ortiz
 Silva et al Original Article Arq Bras Cardiol Study of the Myocardial Contraction and Relaxation Velocities through Doppler Tissue Imaging Echocardiography. A New Alternative in the Assessment of the Segmental
Silva et al Original Article Arq Bras Cardiol Study of the Myocardial Contraction and Relaxation Velocities through Doppler Tissue Imaging Echocardiography. A New Alternative in the Assessment of the Segmental
LV FUNCTION ASSESSMENT: WHAT IS BEYOND EJECTION FRACTION
 LV FUNCTION ASSESSMENT: WHAT IS BEYOND EJECTION FRACTION Jamilah S AlRahimi Assistant Professor, KSU-HS Consultant Noninvasive Cardiology KFCC, MNGHA-WR Introduction LV function assessment in Heart Failure:
LV FUNCTION ASSESSMENT: WHAT IS BEYOND EJECTION FRACTION Jamilah S AlRahimi Assistant Professor, KSU-HS Consultant Noninvasive Cardiology KFCC, MNGHA-WR Introduction LV function assessment in Heart Failure:
Objectives. Diastology: What the Radiologist Needs to Know. LV Diastolic Function: Introduction. LV Diastolic Function: Introduction
 Objectives Diastology: What the Radiologist Needs to Know. Jacobo Kirsch, MD Cardiopulmonary Imaging, Section Head Division of Radiology Cleveland Clinic Florida Weston, FL To review the physiology and
Objectives Diastology: What the Radiologist Needs to Know. Jacobo Kirsch, MD Cardiopulmonary Imaging, Section Head Division of Radiology Cleveland Clinic Florida Weston, FL To review the physiology and
Degenerative Mitral Regurgitation: Etiology and Natural History of Disease and Triggers for Intervention
 Degenerative Mitral Regurgitation: Etiology and Natural History of Disease and Triggers for Intervention John N. Hamaty D.O. FACC, FACOI November 17 th 2017 I have no financial disclosures Primary Mitral
Degenerative Mitral Regurgitation: Etiology and Natural History of Disease and Triggers for Intervention John N. Hamaty D.O. FACC, FACOI November 17 th 2017 I have no financial disclosures Primary Mitral
ΕΚΤΙΜΗΣΗ ΤΗΣ ΑΡΙΣΤΕΡΗΣ ΚΟΙΛΙΑΣ ΜΕ ΜΕΘΟΔΟΥΣ ΚΛΑΣΣΙΚΗΣ ΑΓΓΕΙΟΓΡΑΦΙΑΣ
 ΕΚΤΙΜΗΣΗ ΤΗΣ ΑΡΙΣΤΕΡΗΣ ΚΟΙΛΙΑΣ ΜΕ ΜΕΘΟΔΟΥΣ ΚΛΑΣΣΙΚΗΣ ΑΓΓΕΙΟΓΡΑΦΙΑΣ Α.-Δ. ΜΑΥΡΟΓΙΑΝΝΗ ΚΑΡΔΙΟΛΟΓΟΣ AIMOΔΥΝΑΜIΚΟ ΕΡΓΑΣΤΗΡΙΟ Γ.Ν.Θ. «Γ.ΠΑΠΑΝΙΚΟΛΑΟΥ» ΘΕΣΣΑΛΟΝΙΚΗ Disclosure Statement of Financial Interest None
ΕΚΤΙΜΗΣΗ ΤΗΣ ΑΡΙΣΤΕΡΗΣ ΚΟΙΛΙΑΣ ΜΕ ΜΕΘΟΔΟΥΣ ΚΛΑΣΣΙΚΗΣ ΑΓΓΕΙΟΓΡΑΦΙΑΣ Α.-Δ. ΜΑΥΡΟΓΙΑΝΝΗ ΚΑΡΔΙΟΛΟΓΟΣ AIMOΔΥΝΑΜIΚΟ ΕΡΓΑΣΤΗΡΙΟ Γ.Ν.Θ. «Γ.ΠΑΠΑΝΙΚΟΛΑΟΥ» ΘΕΣΣΑΛΟΝΙΚΗ Disclosure Statement of Financial Interest None
Μαρία Μπόνου Διευθύντρια ΕΣΥ, ΓΝΑ Λαϊκό
 Μαρία Μπόνου Διευθύντρια ΕΣΥ, ΓΝΑ Λαϊκό Diastolic HF DD: Diastolic Dysfunction DHF: Diastolic HF HFpEF: HF with preserved EF DD Pathophysiologic condition: impaired relaxation, LV compliance, LV filling
Μαρία Μπόνου Διευθύντρια ΕΣΥ, ΓΝΑ Λαϊκό Diastolic HF DD: Diastolic Dysfunction DHF: Diastolic HF HFpEF: HF with preserved EF DD Pathophysiologic condition: impaired relaxation, LV compliance, LV filling
Evaluation of Left Ventricular Function and Hypertrophy Gerard P. Aurigemma MD
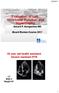 Evaluation of Left Ventricular Function and Hypertrophy Gerard P. Aurigemma MD Board Review Course 2017 43 year old health assistant Severe resistant HTN LT BSA 2 Height 64 1 Here is the M mode echocardiogram
Evaluation of Left Ventricular Function and Hypertrophy Gerard P. Aurigemma MD Board Review Course 2017 43 year old health assistant Severe resistant HTN LT BSA 2 Height 64 1 Here is the M mode echocardiogram
An Integrated Approach to Study LV Diastolic Function
 An Integrated Approach to Study LV Diastolic Function Assoc. Prof. Adriana Ilieşiu, FESC University of Medicine Carol Davila Bucharest, Romania LV Diastolic Dysfunction impaired relaxation (early diastole)
An Integrated Approach to Study LV Diastolic Function Assoc. Prof. Adriana Ilieşiu, FESC University of Medicine Carol Davila Bucharest, Romania LV Diastolic Dysfunction impaired relaxation (early diastole)
Characteristics of Left Ventricular Diastolic Function in Patients with Systolic Heart Failure: A Doppler Tissue Imaging Study
 Characteristics of Left Ventricular Diastolic Function in Patients with Systolic Heart Failure: A Doppler Tissue Imaging Study Bassem A. Samad, MD, PhD, Jens M. Olson, MD, and Mahbubul Alam, MD, PhD, FESC,
Characteristics of Left Ventricular Diastolic Function in Patients with Systolic Heart Failure: A Doppler Tissue Imaging Study Bassem A. Samad, MD, PhD, Jens M. Olson, MD, and Mahbubul Alam, MD, PhD, FESC,
Load and Function - Valvular Heart Disease. Tom Marwick, Cardiovascular Imaging Cleveland Clinic
 Load and Function - Valvular Heart Disease Tom Marwick, Cardiovascular Imaging Cleveland Clinic Indications for surgery in common valve lesions Risks Operative mortality Failed repair - to MVR Operative
Load and Function - Valvular Heart Disease Tom Marwick, Cardiovascular Imaging Cleveland Clinic Indications for surgery in common valve lesions Risks Operative mortality Failed repair - to MVR Operative
The importance of left atrium in LV diastolic function
 II Baltic Heart Failure Meeting and Congress of Latvian Society of Cardiology The importance of left atrium in LV diastolic function Dr. Artem Kalinin Eastern Clinical University Hospital Riga 30.09.2010.
II Baltic Heart Failure Meeting and Congress of Latvian Society of Cardiology The importance of left atrium in LV diastolic function Dr. Artem Kalinin Eastern Clinical University Hospital Riga 30.09.2010.
Affecting the elderly Requiring new approaches. Echocardiographic Evaluation of Hemodynamic Severity. Increasing prevalence Mostly degenerative
 Echocardiographic Evaluation of Hemodynamic Severity Steven J. Lester MD, FACC, FRCP(C), FASE Mayo Clinic, Arizona Relevant Financial Relationship(s) None Off Label Usage None A re-emerging public-health
Echocardiographic Evaluation of Hemodynamic Severity Steven J. Lester MD, FACC, FRCP(C), FASE Mayo Clinic, Arizona Relevant Financial Relationship(s) None Off Label Usage None A re-emerging public-health
Echocardiographic assessment of the right ventricle in paediatric pulmonary hypertension.
 Echocardiographic assessment of the right ventricle in paediatric pulmonary hypertension. Mark K. Friedberg, MD No disclosures Outline RV response to increased afterload Echo assessment of RV function
Echocardiographic assessment of the right ventricle in paediatric pulmonary hypertension. Mark K. Friedberg, MD No disclosures Outline RV response to increased afterload Echo assessment of RV function
Left Atrial Deformation Predicts Pulmonary Capillary Wedge Pressure in Pediatric Heart Transplant Recipients
 DOI: 10.1111/echo.12679 2014, Wiley Periodicals, Inc. Echocardiography Left Atrial Deformation Predicts Pulmonary Capillary Wedge Pressure in Pediatric Heart Transplant Recipients Jay Yeh, M.D.,* Ranjit
DOI: 10.1111/echo.12679 2014, Wiley Periodicals, Inc. Echocardiography Left Atrial Deformation Predicts Pulmonary Capillary Wedge Pressure in Pediatric Heart Transplant Recipients Jay Yeh, M.D.,* Ranjit
Influence of Preload Reduction on Left Ventricular Diastolic Function in Hemodialysis Patients with Left Ventricular Hypertrophy
 93 Original Article St. Marianna Med. J. Vol. 35, pp. 93 99, 2007 Influence of Preload Reduction on Left Ventricular Diastolic Function in Hemodialysis Patients with Left Ventricular Hypertrophy Sachihiko
93 Original Article St. Marianna Med. J. Vol. 35, pp. 93 99, 2007 Influence of Preload Reduction on Left Ventricular Diastolic Function in Hemodialysis Patients with Left Ventricular Hypertrophy Sachihiko
Articles in PresS. J Appl Physiol (September 29, 2005). doi: /japplphysiol
 Articles in PresS. J Appl Physiol (September 29, 2005). doi:10.1152/japplphysiol.00671.2005 Assessment of Left Ventricular Diastolic Function by Early Diastolic Mitral Annulus Peak Acceleration Rate: Experimental
Articles in PresS. J Appl Physiol (September 29, 2005). doi:10.1152/japplphysiol.00671.2005 Assessment of Left Ventricular Diastolic Function by Early Diastolic Mitral Annulus Peak Acceleration Rate: Experimental
Hemodynamic Assessment. Assessment of Systolic Function Doppler Hemodynamics
 Hemodynamic Assessment Matt M. Umland, RDCS, FASE Aurora Medical Group Milwaukee, WI Assessment of Systolic Function Doppler Hemodynamics Stroke Volume Cardiac Output Cardiac Index Tei Index/Index of myocardial
Hemodynamic Assessment Matt M. Umland, RDCS, FASE Aurora Medical Group Milwaukee, WI Assessment of Systolic Function Doppler Hemodynamics Stroke Volume Cardiac Output Cardiac Index Tei Index/Index of myocardial
How to Assess Diastolic Dysfunction?
 How to Assess Diastolic Dysfunction? Fausto J Pinto, MD, PhD, FESC, FACC, FASE Lisbon University Dyastolic Dysfunction Impaired relaxation Elevated filling pressures Ischemic heart disease Cardiomyopathies
How to Assess Diastolic Dysfunction? Fausto J Pinto, MD, PhD, FESC, FACC, FASE Lisbon University Dyastolic Dysfunction Impaired relaxation Elevated filling pressures Ischemic heart disease Cardiomyopathies
Diastolic Heart Failure Abnormalities in Active Relaxation and Passive Stiffness of the Left Ventricle
 original article Diastolic Heart Failure Abnormalities in Active Relaxation and Passive Stiffness of the Left Ventricle Michael R. Zile, M.D., Catalin F. Baicu, Ph.D., and William H. Gaasch, M.D. abstract
original article Diastolic Heart Failure Abnormalities in Active Relaxation and Passive Stiffness of the Left Ventricle Michael R. Zile, M.D., Catalin F. Baicu, Ph.D., and William H. Gaasch, M.D. abstract
Aortic stenosis (AS) is common with the aging population.
 New Insights Into the Progression of Aortic Stenosis Implications for Secondary Prevention Sanjeev Palta, MD; Anita M. Pai, MD; Kanwaljit S. Gill, MD; Ramdas G. Pai, MD Background The risk factors affecting
New Insights Into the Progression of Aortic Stenosis Implications for Secondary Prevention Sanjeev Palta, MD; Anita M. Pai, MD; Kanwaljit S. Gill, MD; Ramdas G. Pai, MD Background The risk factors affecting
Chamber Quantitation Guidelines: What is New?
 Chamber Quantitation Guidelines: What is New? Roberto M Lang, MD J AM Soc Echocardiogr 2005; 18:1440-1463 1 Approximately 10,000 citations iase in itune Cardiac Chamber Quantification: What is New? Database
Chamber Quantitation Guidelines: What is New? Roberto M Lang, MD J AM Soc Echocardiogr 2005; 18:1440-1463 1 Approximately 10,000 citations iase in itune Cardiac Chamber Quantification: What is New? Database
Peak Early Diastolic Mitral Annulus Velocity by Tissue Doppler Imaging Adds Independent and Incremental Prognostic Value
 Journal of the American College of Cardiology Vol. 41, No. 5, 2003 2003 by the American College of Cardiology Foundation ISSN 0735-1097/03/$30.00 Published by Elsevier Science Inc. doi:10.1016/s0735-1097(02)02921-2
Journal of the American College of Cardiology Vol. 41, No. 5, 2003 2003 by the American College of Cardiology Foundation ISSN 0735-1097/03/$30.00 Published by Elsevier Science Inc. doi:10.1016/s0735-1097(02)02921-2
Aortic Root Dilatation as a Marker of Subclinical Left Ventricular Diastolic Dysfunction in Patients with Cardiovascular Risk Factors
 The Journal of International Medical Research 2011; 39: 64 70 Aortic Root Dilatation as a Marker of Subclinical Left Ventricular Diastolic Dysfunction in Patients with Cardiovascular Risk Factors H MASUGATA,
The Journal of International Medical Research 2011; 39: 64 70 Aortic Root Dilatation as a Marker of Subclinical Left Ventricular Diastolic Dysfunction in Patients with Cardiovascular Risk Factors H MASUGATA,
How to assess ischaemic MR?
 ESC 2012 How to assess ischaemic MR? Luc A. Pierard, MD, PhD, FESC, FACC Professor of Medicine Head, Department of Cardiology University Hospital Sart Tilman, Liège ESC 2012 No conflict of interest Luc
ESC 2012 How to assess ischaemic MR? Luc A. Pierard, MD, PhD, FESC, FACC Professor of Medicine Head, Department of Cardiology University Hospital Sart Tilman, Liège ESC 2012 No conflict of interest Luc
Diastology State of The Art Assessment
 Diastology State of The Art Assessment Dr. Mohammad AlGhamdi Assistant professor, KSAU-HS Consultant Cardiologist King AbdulAziz Cardiac Center Ministry of National Guard Health Affairs Diagnostic Clinical
Diastology State of The Art Assessment Dr. Mohammad AlGhamdi Assistant professor, KSAU-HS Consultant Cardiologist King AbdulAziz Cardiac Center Ministry of National Guard Health Affairs Diagnostic Clinical
Stephen Glen ISCHAEMIC HEART DISEASE AND LEFT VENTRICULAR FUNCTION
 Stephen Glen ISCHAEMIC HEART DISEASE AND LEFT VENTRICULAR FUNCTION Overview Coronary arteries Terminology to describe contractility Measuring ventricular function Systolic dysfunction Practice cases- LV
Stephen Glen ISCHAEMIC HEART DISEASE AND LEFT VENTRICULAR FUNCTION Overview Coronary arteries Terminology to describe contractility Measuring ventricular function Systolic dysfunction Practice cases- LV
THE PATHOGENESIS OF ACUTE PULMONARY EDEMA ASSOCIATED WITH HYPERTENSION THE PATHOGENESIS OF ACUTE PULMONARY EDEMA ASSOCIATED WITH HYPERTENSION
 THE PATHOGENESIS OF ACUTE PULMONARY EDEMA ASSOCIATED WITH HYPERTENSION THE PATHOGENESIS OF ACUTE PULMONARY EDEMA ASSOCIATED WITH HYPERTENSION SANJAY K. GANDHI, M.D., JOHN C. POWERS, M.D., ABDEL-MOHSEN
THE PATHOGENESIS OF ACUTE PULMONARY EDEMA ASSOCIATED WITH HYPERTENSION THE PATHOGENESIS OF ACUTE PULMONARY EDEMA ASSOCIATED WITH HYPERTENSION SANJAY K. GANDHI, M.D., JOHN C. POWERS, M.D., ABDEL-MOHSEN
Diagnosis is it really Heart Failure?
 ESC Congress Munich - 25-29 August 2012 Heart Failure with Preserved Ejection Fraction From Bench to Bedside Diagnosis is it really Heart Failure? Prof. Burkert Pieske Department of Cardiology Med.University
ESC Congress Munich - 25-29 August 2012 Heart Failure with Preserved Ejection Fraction From Bench to Bedside Diagnosis is it really Heart Failure? Prof. Burkert Pieske Department of Cardiology Med.University
Aortic Stenosis and Perioperative Risk With Non-cardiac Surgery
 Aortic Stenosis and Perioperative Risk With Non-cardiac Surgery Aortic stenosis (AS) is characterized as a high-risk index for cardiac complications during non-cardiac surgery. A critical analysis of old
Aortic Stenosis and Perioperative Risk With Non-cardiac Surgery Aortic stenosis (AS) is characterized as a high-risk index for cardiac complications during non-cardiac surgery. A critical analysis of old
Cardiac Cycle MCQ. Professor of Cardiovascular Physiology. Cairo University 2007
 Cardiac Cycle MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Regarding the length of systole and diastole: a- At heart rate 75 b/min, the duration of
Cardiac Cycle MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Regarding the length of systole and diastole: a- At heart rate 75 b/min, the duration of
DOPPLER HEMODYNAMICS (1) QUANTIFICATION OF PRESSURE GRADIENTS and INTRACARDIAC PRESSURES
 THORAXCENTRE DOPPLER HEMODYNAMICS (1) QUANTIFICATION OF PRESSURE GRADIENTS and INTRACARDIAC PRESSURES J. Roelandt DOPPLER HEMODYNAMICS Intracardiac pressures and pressure gradients Volumetric measurement
THORAXCENTRE DOPPLER HEMODYNAMICS (1) QUANTIFICATION OF PRESSURE GRADIENTS and INTRACARDIAC PRESSURES J. Roelandt DOPPLER HEMODYNAMICS Intracardiac pressures and pressure gradients Volumetric measurement
Jong-Won Ha*, Jeong-Ah Ahn, Jae-Yun Moon, Hye-Sun Suh, Seok-Min Kang, Se-Joong Rim, Yangsoo Jang, Namsik Chung, Won-Heum Shim, Seung-Yun Cho
 Eur J Echocardiography (2006) 7, 16e21 CLINICAL/ORIGINAL PAPERS Triphasic mitral inflow velocity with mid-diastolic flow: The presence of mid-diastolic mitral annular velocity indicates advanced diastolic
Eur J Echocardiography (2006) 7, 16e21 CLINICAL/ORIGINAL PAPERS Triphasic mitral inflow velocity with mid-diastolic flow: The presence of mid-diastolic mitral annular velocity indicates advanced diastolic
Rownak Jahan Tamanna 1, Rowshan Jahan 2, Abduz Zaher 3 and Abdul Kader Akhanda. 3 ORIGINAL ARTICLES
 University Heart Journal Vol. 4 No. 2 July 2008 ORIGINAL ARTICLES Correlation of Doppler echocardiography with cardiac catheterization in estimating pulmonary capillary wedge pressure: A tertiary level
University Heart Journal Vol. 4 No. 2 July 2008 ORIGINAL ARTICLES Correlation of Doppler echocardiography with cardiac catheterization in estimating pulmonary capillary wedge pressure: A tertiary level
Incorporating the New Echo Guidelines Into Everyday Practice
 Incorporating the New Echo Guidelines Into Everyday Practice Clinical Case RIGHT VENTRICULAR FAILURE Gustavo Restrepo MD President Elect Interamerican Society of Cardiology Director Fellowship Training
Incorporating the New Echo Guidelines Into Everyday Practice Clinical Case RIGHT VENTRICULAR FAILURE Gustavo Restrepo MD President Elect Interamerican Society of Cardiology Director Fellowship Training
Segmental Tissue Doppler Image-Derived Tei Index in Patients With Regional Wall Motion Abnormalities
 ORIGINAL ARTICLE DOI 10.4070 / kcj.2010.40.3.114 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2010 The Korean Society of Cardiology Open Access Segmental Tissue Doppler Image-Derived Tei Index
ORIGINAL ARTICLE DOI 10.4070 / kcj.2010.40.3.114 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2010 The Korean Society of Cardiology Open Access Segmental Tissue Doppler Image-Derived Tei Index
The impact of hypertension on systolic and diastolic left ventricular function. A tissue Doppler echocardiographic study
 The impact of hypertension on systolic and diastolic left ventricular function. A tissue Doppler echocardiographic study Manolis Bountioukos, MD, PhD, a Arend F.L. Schinkel, MD, PhD, a Jeroen J. Bax, MD,
The impact of hypertension on systolic and diastolic left ventricular function. A tissue Doppler echocardiographic study Manolis Bountioukos, MD, PhD, a Arend F.L. Schinkel, MD, PhD, a Jeroen J. Bax, MD,
Diastolic Dysfunction: Hypertension to Hypertrophy to Heart Failure
 Diastolic Dysfunction: Hypertension to Hypertrophy to Heart Failure Dr. Shelley Zieroth FRCPC Assistant Professor, Cardiology, University of Manitoba Director of Cardiac Transplant and Heart Failure Clinics
Diastolic Dysfunction: Hypertension to Hypertrophy to Heart Failure Dr. Shelley Zieroth FRCPC Assistant Professor, Cardiology, University of Manitoba Director of Cardiac Transplant and Heart Failure Clinics
The Impact of Autonomic Neuropathy on Left Ventricular Function in Normotensive Type 1 Diabetic Patients: a Tissue Doppler Echocardiographic Study
 Diabetes Care Publish Ahead of Print, published online November 13, 2007 The Impact of Autonomic Neuropathy on Left Ventricular Function in Normotensive Type 1 Diabetic Patients: a Tissue Doppler Echocardiographic
Diabetes Care Publish Ahead of Print, published online November 13, 2007 The Impact of Autonomic Neuropathy on Left Ventricular Function in Normotensive Type 1 Diabetic Patients: a Tissue Doppler Echocardiographic
Elevated LV filling pressure is a major determinant of cardiac symptoms and
 LEFT VENTRICULAR FILLING PRESSURE, DIASTOLIC FUNCTION, AND HEART RATE PATRIZIO LANCELLOTTI, MD, PhD, FESC PERSPECTIVES Author affiliations: University of Liège hospital, GIGA Cardiovascular Science, Heart
LEFT VENTRICULAR FILLING PRESSURE, DIASTOLIC FUNCTION, AND HEART RATE PATRIZIO LANCELLOTTI, MD, PhD, FESC PERSPECTIVES Author affiliations: University of Liège hospital, GIGA Cardiovascular Science, Heart
Postsystolic shortening of ischemic myocardium: a mechanism of abnormal intraventricular filling
 Am J Physiol Heart Circ Physiol 284: H2343 H2350, 2003. First published February 6, 2003; 10.1152/ajpheart.00320.2002. Postsystolic shortening of ischemic myocardium: a mechanism of abnormal intraventricular
Am J Physiol Heart Circ Physiol 284: H2343 H2350, 2003. First published February 6, 2003; 10.1152/ajpheart.00320.2002. Postsystolic shortening of ischemic myocardium: a mechanism of abnormal intraventricular
Appendix II: ECHOCARDIOGRAPHY ANALYSIS
 Appendix II: ECHOCARDIOGRAPHY ANALYSIS Two-Dimensional (2D) imaging was performed using the Vivid 7 Advantage cardiovascular ultrasound system (GE Medical Systems, Milwaukee) with a frame rate of 400 frames
Appendix II: ECHOCARDIOGRAPHY ANALYSIS Two-Dimensional (2D) imaging was performed using the Vivid 7 Advantage cardiovascular ultrasound system (GE Medical Systems, Milwaukee) with a frame rate of 400 frames
RIGHT VENTRICULAR SIZE AND FUNCTION
 RIGHT VENTRICULAR SIZE AND FUNCTION Edwin S. Tucay, MD, FPCC, FPCC, FPSE Philippine Society of Echocardiography Quezon City, Philippines Echo Mission, BRTTH, Legaspi City, July 1-2, 2016 NO DISCLOSURE
RIGHT VENTRICULAR SIZE AND FUNCTION Edwin S. Tucay, MD, FPCC, FPCC, FPSE Philippine Society of Echocardiography Quezon City, Philippines Echo Mission, BRTTH, Legaspi City, July 1-2, 2016 NO DISCLOSURE
Diastolic Function Assessment Practical Ways to Incorporate into Every Echo
 Diastolic Function Assessment Practical Ways to Incorporate into Every Echo Jae K. Oh, MD Echo Hawaii 2018 2018 MFMER 3712003-1 Learning Objectives My presentation will help you to Appreciate the importance
Diastolic Function Assessment Practical Ways to Incorporate into Every Echo Jae K. Oh, MD Echo Hawaii 2018 2018 MFMER 3712003-1 Learning Objectives My presentation will help you to Appreciate the importance
Heart Failure with Preserved Left Ventricular Ejection Fraction. (HFpEF)
 Thessaloniki, May 27, 2017 Heart Failure with Preserved Left Ventricular Ejection Fraction Filippos Triposkiadis, MD, FESC, FACC Professor of Cardiology Director, Department of Cardiology Larissa University
Thessaloniki, May 27, 2017 Heart Failure with Preserved Left Ventricular Ejection Fraction Filippos Triposkiadis, MD, FESC, FACC Professor of Cardiology Director, Department of Cardiology Larissa University
Advanced Multi-Layer Speckle Strain Permits Transmural Myocardial Function Analysis in Health and Disease:
 Advanced Multi-Layer Speckle Strain Permits Transmural Myocardial Function Analysis in Health and Disease: Clinical Case Examples Jeffrey C. Hill, BS, RDCS Echocardiography Laboratory, University of Massachusetts
Advanced Multi-Layer Speckle Strain Permits Transmural Myocardial Function Analysis in Health and Disease: Clinical Case Examples Jeffrey C. Hill, BS, RDCS Echocardiography Laboratory, University of Massachusetts
Left atrial function. Aliakbar Arvandi MD
 In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
Ref 1. Ref 2. Ref 3. Ref 4. See graph
 Ref 1 Ref 2 Ref 3 1. Ages 6-23 y/o 2. Significant LVM differences by gender 3. For males 95 th percentiles: a. LVM/BSA = 103 b. LVM/height = 100 4. For females 95 th percentiles: a. LVM/BSA = 84 b. LVM/height
Ref 1 Ref 2 Ref 3 1. Ages 6-23 y/o 2. Significant LVM differences by gender 3. For males 95 th percentiles: a. LVM/BSA = 103 b. LVM/height = 100 4. For females 95 th percentiles: a. LVM/BSA = 84 b. LVM/height
Losartan Improves Exercise Tolerance in Patients With Diastolic Dysfunction and a Hypertensive Response to Exercise
 Journal of the American College of Cardiology Vol. 33, No. 6, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00048-0 Losartan
Journal of the American College of Cardiology Vol. 33, No. 6, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00048-0 Losartan
Effect of physiological heart rate changes on left ventricular dimensions and mitral blood flow velocities in the normal fetus
 ELSEVIER Early Human Development 40 (1995) 109-114 Effect of physiological heart rate changes on left ventricular dimensions and mitral blood flow velocities in the normal fetus P.B. Tsyvian a, K.V. Malkin
ELSEVIER Early Human Development 40 (1995) 109-114 Effect of physiological heart rate changes on left ventricular dimensions and mitral blood flow velocities in the normal fetus P.B. Tsyvian a, K.V. Malkin
Three-dimensional Wall Motion Tracking:
 Three-dimensional Wall Motion Tracking: A Novel Echocardiographic Method for the Assessment of Ventricular Volumes, Strain and Dyssynchrony Jeffrey C. Hill, BS, RDCS, FASE Jennifer L. Kane, RCS Gerard
Three-dimensional Wall Motion Tracking: A Novel Echocardiographic Method for the Assessment of Ventricular Volumes, Strain and Dyssynchrony Jeffrey C. Hill, BS, RDCS, FASE Jennifer L. Kane, RCS Gerard
Low fractional diastolic pressure in the ascending aorta increased the risk of coronary heart disease
 (2002) 16, 837 841 & 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Low fractional diastolic pressure in the ascending aorta increased the risk
(2002) 16, 837 841 & 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Low fractional diastolic pressure in the ascending aorta increased the risk
Assessment of LV systolic function
 Tutorial 5 - Assessment of LV systolic function Assessment of LV systolic function A knowledge of the LV systolic function is crucial in the undertanding of and management of unstable hemodynamics or a
Tutorial 5 - Assessment of LV systolic function Assessment of LV systolic function A knowledge of the LV systolic function is crucial in the undertanding of and management of unstable hemodynamics or a
Diagnostic approach to heart disease
 Diagnostic approach to heart disease Initial work up History Physical exam Chest radiographs ECG Special studies Echocardiography Cardiac catheterization Echocardiography principles Technique of producing
Diagnostic approach to heart disease Initial work up History Physical exam Chest radiographs ECG Special studies Echocardiography Cardiac catheterization Echocardiography principles Technique of producing
Diastole is Not a Single Entity Four Components of Diastolic Dysfunction
 Physiology of Diastolic Function Made Easy James D. Thomas, MD, FACC, FASE Director, Center for Heart Valve Disease Bluhm Cardiovascular Institute Professor of Medicine, Feinberg School of Medicine, Northwestern
Physiology of Diastolic Function Made Easy James D. Thomas, MD, FACC, FASE Director, Center for Heart Valve Disease Bluhm Cardiovascular Institute Professor of Medicine, Feinberg School of Medicine, Northwestern
Left Ventricular Function In Subclinical Hypothyroidism
 Clinical Proceedings. 2016;12(1):13-19 Original Article Left Ventricular Function In Subclinical Hypothyroidism NK Thulaseedharan, P Geetha, TM Padmaraj Department of Internal Medicine, Govt. Medical College
Clinical Proceedings. 2016;12(1):13-19 Original Article Left Ventricular Function In Subclinical Hypothyroidism NK Thulaseedharan, P Geetha, TM Padmaraj Department of Internal Medicine, Govt. Medical College
Significance of Left Atrial Pressure and Left Ventricular Relaxation as Determinants of Left Ventricular Early Diastolic Filling Flow in Man
 Significance of Left Atrial Pressure and Left Ventricular Relaxation as Determinants of Left Ventricular Early Diastolic Filling Flow in Man Toshiyuki TAKAHASHI, M.D., Masahiko IIZUKA, M.D., Takashi SERIZAWA,
Significance of Left Atrial Pressure and Left Ventricular Relaxation as Determinants of Left Ventricular Early Diastolic Filling Flow in Man Toshiyuki TAKAHASHI, M.D., Masahiko IIZUKA, M.D., Takashi SERIZAWA,
Effect of Heart Rate on Tissue Doppler Measures of E/E
 Cardiology Department of Bangkok Metropolitan Administration Medical College and Vajira Hospital, Bangkok, Thailand Abstract Background: Our aim was to study the independent effect of heart rate (HR) on
Cardiology Department of Bangkok Metropolitan Administration Medical College and Vajira Hospital, Bangkok, Thailand Abstract Background: Our aim was to study the independent effect of heart rate (HR) on
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Table S1: Number and percentage of patients by age category Distribution of age Age
SUPPLEMENTAL MATERIAL Table S1: Number and percentage of patients by age category Distribution of age Age
Prognostic Value of Left Atrial Size and Function
 Prognostic Value of Left Atrial Size and Function James D. Thomas, M.D., F.A.C.C. Cardiovascular Imaging Center Department of Cardiology Cleveland Clinic Foundation Cleveland, Ohio, USA Conflicts: None
Prognostic Value of Left Atrial Size and Function James D. Thomas, M.D., F.A.C.C. Cardiovascular Imaging Center Department of Cardiology Cleveland Clinic Foundation Cleveland, Ohio, USA Conflicts: None
Tissue Doppler-Derived Myocardial Acceleration for Evaluation of Left Ventricular Diastolic Function
 Journal of the American College of Cardiology Vol. 44, No. 7, 2004 2004 by the American College of Cardiology Foundation ISSN 0735-1097/04/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.06.067
Journal of the American College of Cardiology Vol. 44, No. 7, 2004 2004 by the American College of Cardiology Foundation ISSN 0735-1097/04/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.06.067
RV dysfunction and failure PATHOPHYSIOLOGY. Adam Torbicki MD, Dept Chest Medicine Institute of Tuberculosis and Lung Diseases Warszawa, Poland
 RV dysfunction and failure PATHOPHYSIOLOGY Adam Torbicki MD, Dept Chest Medicine Institute of Tuberculosis and Lung Diseases Warszawa, Poland Normal Right Ventricle (RV) Thinner wall Weaker myocytes Differences
RV dysfunction and failure PATHOPHYSIOLOGY Adam Torbicki MD, Dept Chest Medicine Institute of Tuberculosis and Lung Diseases Warszawa, Poland Normal Right Ventricle (RV) Thinner wall Weaker myocytes Differences
MITRAL STENOSIS. Joanne Cusack
 MITRAL STENOSIS Joanne Cusack BSE Breakdown Recognition of rheumatic mitral stenosis Qualitative description of valve and sub-valve calcification and fibrosis Measurement of orifice area by planimetry
MITRAL STENOSIS Joanne Cusack BSE Breakdown Recognition of rheumatic mitral stenosis Qualitative description of valve and sub-valve calcification and fibrosis Measurement of orifice area by planimetry
Disclosure Information : No conflict of interest
 Intravenous nicorandil improves symptoms and left ventricular diastolic function immediately in patients with acute heart failure : a randomized, controlled trial M. Shigekiyo, K. Harada, A. Okada, N.
Intravenous nicorandil improves symptoms and left ventricular diastolic function immediately in patients with acute heart failure : a randomized, controlled trial M. Shigekiyo, K. Harada, A. Okada, N.
Journal of the American College of Cardiology Vol. 34, No. 2, by the American College of Cardiology ISSN /99/$20.
 Journal of the American College of Cardiology Vol. 34, No. 2, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00230-2 Combined
Journal of the American College of Cardiology Vol. 34, No. 2, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00230-2 Combined
Echocardiographic and Doppler Assessment of Cardiac Functions in Patients of Non-Insulin Dependent Diabetes Mellitus
 ORIGINAL ARTICLE JIACM 2002; 3(2): 164-8 Echocardiographic and Doppler Assessment of Cardiac Functions in Patients of Non-Insulin Dependent Diabetes Mellitus Rajesh Rajput*, Jagdish**, SB Siwach***, A
ORIGINAL ARTICLE JIACM 2002; 3(2): 164-8 Echocardiographic and Doppler Assessment of Cardiac Functions in Patients of Non-Insulin Dependent Diabetes Mellitus Rajesh Rajput*, Jagdish**, SB Siwach***, A
Little is known about the degree and time course of
 Differential Changes in Regional Right Ventricular Function Before and After a Bilateral Lung Transplantation: An Ultrasonic Strain and Strain Rate Study Virginija Dambrauskaite, MD, Lieven Herbots, MD,
Differential Changes in Regional Right Ventricular Function Before and After a Bilateral Lung Transplantation: An Ultrasonic Strain and Strain Rate Study Virginija Dambrauskaite, MD, Lieven Herbots, MD,
HFPEF Echo with Strain vs. MRI T1 Mapping
 HFPEF Echo with Strain vs. MRI T1 Mapping Erik Schelbert, MD MS Director, Cardiovascular Magnetic Resonance Assistant Professor of Medicine Heart & Vascular Institute University of Pittsburgh Disclosures
HFPEF Echo with Strain vs. MRI T1 Mapping Erik Schelbert, MD MS Director, Cardiovascular Magnetic Resonance Assistant Professor of Medicine Heart & Vascular Institute University of Pittsburgh Disclosures
M. Hajahmadi Poorrafsanjani 1 & B. Rahimi Darabad 1
 Global Journal of Health Science; Vol. 6, No. 7; 2014 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Evaluate the Sensitivity and Specificity Echocardiography in
Global Journal of Health Science; Vol. 6, No. 7; 2014 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Evaluate the Sensitivity and Specificity Echocardiography in
가천의대길병원소아심장과최덕영 PA C IVS THE EVALUATION AND PRINCIPLES OF TREATMENT STRATEGY
 가천의대길병원소아심장과최덕영 PA C IVS THE EVALUATION AND PRINCIPLES OF TREATMENT STRATEGY PA c IVS (not only pulmonary valve disease) Edwards JE. Pathologic Alteration of the right heart. In: Konstam MA, Isner M, eds.
가천의대길병원소아심장과최덕영 PA C IVS THE EVALUATION AND PRINCIPLES OF TREATMENT STRATEGY PA c IVS (not only pulmonary valve disease) Edwards JE. Pathologic Alteration of the right heart. In: Konstam MA, Isner M, eds.
Research Article Changes in Mitral Annular Ascent with Worsening Echocardiographic Parameters of Left Ventricular Diastolic Function
 Scientifica Volume 216, Article ID 633815, 4 pages http://dx.doi.org/1.1155/216/633815 Research Article Changes in Mitral Annular Ascent with Worsening Echocardiographic Parameters of Left Ventricular
Scientifica Volume 216, Article ID 633815, 4 pages http://dx.doi.org/1.1155/216/633815 Research Article Changes in Mitral Annular Ascent with Worsening Echocardiographic Parameters of Left Ventricular
