Posterior vaginal compartment repairs: Where are the main anatomical defects?
|
|
|
- Vivien Davis
- 5 years ago
- Views:
Transcription
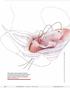
1 Int Urogynecol J (2016) 27: DOI /s ORIGINAL ARTICLE Posterior vaginal compartment repairs: Where are the main anatomical defects? Bernard T. Haylen 1 & Sushen Naidoo 2 & Stephen J. Kerr 3 & Chin H. Yong 2 & Warwick Birrell 4 Received: 1 August 2015 /Accepted: 16 October 2015 /Published online: 12 November 2015 # The International Urogynecological Association 2015 Abstract Introduction and hypothesis Traditionally, it has been believed that posterior vaginal compartment prolapse was largely due to defects in the rectovaginal fascia, with surgical repairs concentrating on addressing this defect. We aimed to determine the relative size of defects at the different vaginal levels (I III) following a large number of posterior vaginal compartment repairs (PRs) to determine whether this traditional viewpoint is still appropriate. Methods In a cross-sectional study of 300 consecutive PRs, mostly following prior or concomitant hysterectomy, two sets of markers of posterior compartment prolapse were used to measure anatomical defects at levels I III: (i) from Pelvic Organ Prolapse Quantification (POP-Q) system points C, Ap, Bp, and genital hiatus (GH), and from Posterior Repair Quantification (PR-Q) perineal gap (PG), posterior vaginalvault descent (PVVD), midvaginal laxity (MVL) vault undisplaced, and rectovaginal fascial laxity (RVFL). Results The largest defects were found at level I (PVVD: mean 6.0 cm; point C, mean minus 0.9 cm), and level III (PG, mean 2.9 cm; GH, mean 3.7 cm). Level II defects Electronic supplementary material The online version of this article (doi: /s ) contains supplementary material, which is available to authorized users. * Bernard T. Haylen bernard@haylen.co St. Vincent s Clinic, Suite 904, 438 Victoria Street, Darlinghurst 2010, NSW, Australia St. Vincent s Hospital, Darlinghurst, NSW, Australia Kirby Institute, University of New South Wales, Kensington, NSW, Australia Mater Hospital, North Sydney, NSW, Australia (MVL vault undisplaced, mean 1.3 cm; RVFL, mean 1.1 cm; points Ap, Bp, both mean 1.0 cm) were relatively small. Conclusions This study suggests that the defects found at surgery for posterior vaginal compartment prolapse were more frequent at the vaginal vault (level I) and vaginal introitus (level III) than at midvagina (level II). These findings should have implications for surgical planning. Keywords Prolapsesurgery. Posterior vaginal compartment. Pelvic organ prolapse. Key anatomical indicators (KAI). Anatomical defects. Posterior Repair Quantification (PR-Q) Introduction Traditionally, it has been believed that posterior vaginal compartment prolapse was largely due to defects in the rectovaginal fascia (level II [1]). Surgical repairs have tended to concentrate on addressing these defects [2 4] by using either native tissues or augmentation with a prosthesis. Attention to the vaginal introitus (level III [1]) was generally included, although there were uncertainties [2, 3] as to whether the repair at this level should commence at or below the hymen. There has been some evidence for the contribution of vaginal vault defects to anterior level II compartment defects [5]. The main anatomical defects at posterior vaginal compartment repairs (PR) have not, to date, been clearly identified in the literature, leaving uncertainty regarding optimum surgical approaches. Our recent preliminary report [6] of 50 cases examining additional intraoperative measurements at PR [Posterior Repair Quantification (PR-Q)] [6] suggested that the defects at PR seemed to be more frequent at levels I and III than at level II [1].
2 742 Int Urogynecol J (2016) 27: We employed a larger study to determine with more certainty the relative size of anatomical defects at the different vaginal levels (I III) at PR. We used two sets of available measurements: (i) Pelvic Organ Prolapse Quantification (POP-Q) [7] and (ii) PR-Q, the latter having recently been described [6]. Patients and methods This was a cross-sectional study of 300 consecutive PRs, mostly following prior or concomitant hysterectomy and concomitant anterior colporrhaphy and was an extension of the study of 50 PR cases used in our preliminary report [6] but focussing on anatomical defects. Data collection was from December 2013 to December 2014 at St. Vincent s and Mater Hospitals, Sydney. Patients were assessed clinically in their rooms using the POP-Q [7] to determine the need for prolapse surgery. All POP-Q [7] and PR-Q [6] measurements were taken immediately prior to the PR and at the end of any concomitant prolapse surgeries. No patients were excluded from PR. Postoperative measurements were not included, as the study objective was to identify the relative size of preoperative anatomical defects at different vaginal levels. The following posterior prolapse markers were measured: (i) from POP-Q [7], points C, Ap, and Bp (point D not included, as the vast majority were posthysterectomy), and genital hiatus (GH); and from PR-Q [6], perineal gap (PG), posterior vaginal-vault descent (PVVD), midvaginal laxity (MVL) vault undisplaced, and rectovaginal fascial laxity (RVFL); MVL vault displaced [6] (by traction) was also measured. Each measurement by the primary surgeon received visual confirmation by an observer/surgical assistant. The bladder was re-emptied prior to this examination to prevent any limitation of aspects of prolapse extent [8]. The four PR-Q markers possibly less familiar to readers are described [6]. 1. Perineal gap: level III The line of the labia minora was visually followed posteriorly until the perineum was reached on either side. At this point, Moynihan (Littlewood) forceps were applied on each side of the labia. Gentle bilateral traction will show any deficient anterior perineum. Closer inspection allows marking (by surgical marker) of the junction of the much-thinned-out area medially and the start of thicker perineal tissue laterally, closer to the forceps. This section between surgical marks is the PG, which was measured with a surgical ruler in centimeters to one decimal point. Figure 1 shows how the PG might be assessed and its width measured. 2. Posterior vaginal-vault descent: level I [1] Total posterior vaginal length (TPVL) [6] was measured from the center of the PG to the vaginal vault. A Fig. 1 Perineal gap (PG): thinned-out medial area (cm) between Moynihan forceps placed bilaterally where the line of the labia minora meets the perineum Moynihan forceps, oriented horizontally, was applied in the midline 1 cm below and posterior to the vaginal-vault line (prior hysterectomy) or junction of the cervix and posterior vaginal vault if the uterus remained in situ. Gentle inferior traction was then placed on the forceps to assess vaginal-vault descent. The distance between the PG and the point of attachment of the Moynihan forceps under maximum displacement was called the perineal gap Moynihan (PGMOYN) distance. PVVD was then calculated using the formula below: PVVD ¼ TPVL PGMOYN Figure 2a shows the TPVL from which the PGMOYN distance (Fig. 2b) needs to be subtracted to determine PVVD. 3. Midvaginal laxity vault undisplaced (level II) [1] Gentle inferior traction on the Moynihan forceps was replaced by slight superior tension toward the vaginal vault steadied by a surgical assistant. This served to stabilize the vaginal vault. The surgeon then placed anterior traction perpendicular to the middle of the posterior vaginal wall using Gillies forceps to determine MVL vault undisplaced, determined by the length (cm) of the anteriorly displaced midvagina over the lateral vagina. Figure 3a demonstrates this measurement technique. Further measurement of the MVL was performed with the vaginal vault in traction, as in Fig. 2b. This was termed MVL vault displaced). 4 Rectovaginal fascial laxity (level II) This potential defect was assessed once posterior vaginal surgery was commenced. Once the PG had been excised, the posterior vaginal wall was opened in the midline up to the Moynihan forceps. Artery forceps were used to support both sides of the incision. The forceps at the apex
3 Int Urogynecol J (2016) 27: Fig. 2 a, b Posterior vaginal-vault descent (PVVD): subtract distance from inferiorly displaced vaginal vault and perineal gap (PG) (b) from total posterior vaginal length (TPVL) (a) of the incision was again held under slight tension toward the vaginal vault for stabilization. RVFL was measured in a similar way to MVL. A gentle anterior traction on the fascia was applied, and fascia laxity was measured from the midvagina level. Figure 3b demonstrates measurement technique (artery forceps not shown). Baseline demographic and surgical factors assessed were age, parity, weight, height, body mass index (BMI), menopause status, and prior hysterectomy. Surgical initiatives in response to defects were excision of the perineal defect (PG), vaginal-vault suspension with sacrospinous colpopexy (SSC), excision of excess posterior vaginal skin, and rectovaginal fascial plications. These initiatives were performed as per the previous study [6]: 1. Excision of the entire PG 2. SSC if PVVD >5 cm Fig. 3 Midvaginal laxity (MVL) vault undisplaced (a) Vault is held in undisplaced position by Moynihan forceps while anterior traction on the midpoint of the vaginal superoinferiorly is used to demonstrate MVL (cm). Rectovaginal fascial laxity (RVFL): Similar to a, though measurement of the RVFL occurs once the posterior vaginal wall has been opened to the apical Moynihan forceps (b ) 3. Vaginal skin excision under half MVL vault undisplaced 4. Rectovaginal fascial plication if RVFL >0.5 cm Surgical materials and techniques used were identical for all 300 patients. The posterior vaginal skin was sutured down to the surgical marks for the PG using a 1/0 Vicryl suture. For perineorrhaphy, 2/0 Vicryl rapide was used, with 0/0 Vicryl used for rectovaginal fascial plication, if indicated. Dissection in the rectovaginal space was minimalized. Levator or levator fascial plication was not used in this study as a result of the minimalized dissection. A Capio device (Boston Scientific) was used to insert the size 0 Ethibond sacrospinous colpopexy sutures. Institutional ethical approval was received for the study. All patients gave informed consent as part of this audit of surgical practice. Methods, definitions, and units conform to standards jointly recommended by the
4 744 Int Urogynecol J (2016) 27: International Continence Society and the International Urogynecological Society, except where specifically noted [9]. Statistical analysis was conducted with Stata version 13.1 (College Station, TX, USA). Results Table 1 shows the parameter distribution summary. Of the 300 women, 39 (13.0 %) were premenopausal and 261 (87.0 %) were menopausal; (ii) 139 (46.3 %) had a prior hysterectomy, 128 (42.7 %) had a concomitant hysterectomy, and in 33 (11.0 %) the uterus was in situ. The largest defects were found at level I (PVVD, mean 6.0 cm; point C, mean minus 0.9 cm) and level III (PG, mean 2.9 cm; GH, mean 3.7 cm). Level II defects (MVL vault undisplaced, mean 1.3 cm; RVFL, mean 1.1 cm; points Ap, Bp, both mean 1.0 cm) were relatively small. Mean preoperative MVL vault displaced was 2.8 cm and mean preoperative MVL vault undisplaced was 1.3 cm. From this finding, it can be interpreted that 1.5 cm (55 %) of preoperative MVL vault displaced was due to vaginal-vault laxity. SSC was required in 84 % of cases to restore level I support. Vaginal skin excision occurred in 96 % cases, with 67 % requiring only up to 0.5-cm bilateral excision. Fascial suturing occurred in 76 %. Table 1 Preoperative baseline patient characteristics and the two sets of posterior prolapse markers: (i) PR-Q; (ii) POP-Q Variable Mean SD Min Max Age (years) Weight (kg) Height (cm) BMI (kg/m 2 ) Parity PR-Q posterior prolapse markers PG (cm) PVVD (cm) MVL vault undisplaced (cm) RVFL (cm) POP-Q posterior prolapse markers Preop point C (cm) Preop point Ap (cm) Preop point Bp (cm) Genital hiatus preop (cm) PR-Q Posterior Repair Quantification, POP-Q Pelvic Organ Prolapse Quantification, BMI body mass index, PG perineal gap, PVVD posterior vaginal-vault descent, MVL midvaginal laxity, RVFL rectovaginal fascial laxity, SD standard deviation Discussion This study confirmed and strengthened our preliminary findings [6] that the anatomical defects found at surgery for posterior vaginal compartment prolapse were more at the vaginal vault (level I) and vaginal introitus (level III) rather than at the midvagina (level II). A majority (55 %) of midvaginal laxity was due to vaginal-vault descent. These results indicate the presence of significant posterior vaginal-vault laxity in the majority of the women undergoing PR. The majority of vaginal-vault support obtained during hysterectomy (prior or concomitant) by using the two supportive uterine ligaments uterosacral and cardinal is directed toward the anterior vaginal vault and wall with very little influence on the posterior vaginal vault and wall [10 12]. Additional posterior vaginalvault support provided by SSC was required in 84 % of cases. We acknowledge that an SSC is not the only vaginal-vault supportive procedure [13, 14]. We adopted a cutoff of 5.0 cm for PVVD level, requiring posterior vaginal-vault fixation, e.g., by a SSC. Our rationale for this arbitrary figure is that: (i) for PVVD >5.0 cm, an SSC is more anatomically and surgically desirable; (ii) for PVVD <5.0 cm, posterior vaginal-vault support is less in question, and it is much harder for the vaginal vault to reach the sacrospinous ligament via the usual posterior approach. We acknowledge that some surgeons believe it is not necessary for the vaginal vault to be in contact with the SSL at SSC. Our results tend to challenge the traditional concept of a rectocele as a level II defect of rectovaginal fascia (septum) [15 17] and accompanying vaginal skin laxity. Overall mean MVL vault undisplaced was only 1.3 cm and mean RVFL only 1.1 cm (Ap and Bp, both 1.0 cm). These results also highlighted the bigger issues in the posterior vaginal compartment were, in fact, at the perineum (level III overall mean PG 2.9 cm; GH mean 3.7 cm) and vaginal vault (level I overall mean PVVD 6.0 cm; point C mean 0.9 cm). Surgical implication in the traditional posterior repair is that to date, the midvagina (level II) may have received more intervention than required, with the vaginal vault and perineum perhaps receiving less surgical attention than needed. MRI evidence [18] supports the view that there is overall weakening and generalized deformation of pelvic floor tissues rather than specific fascial defects, perhaps indicating a reason for the relatively modest success rates of posterior vaginal repairs [16 18]. Results for GH between this series and our preliminary report were essentially similar: 3.7 cm vs 3.6 cm [6]. GH has a strong correlation with prolapse severity [19]. The different anatomical benefits of PG excision have been previously outlined [20]. These include: 1. A 100 % excision of thinned-out perineal skin 2. A 24 % increase in vaginal length over PR commenced at the hymen
5 Int Urogynecol J (2016) 27: Mean 31 % decrease in GH 4. Mean 28 % increase in perineal length 5. Mean 57 % increase in midperineal thickness Postoperative anatomical results were discussed in the preliminary report [6], though they are not a specific part of this particular report. We believe that the strengths of this study were it focus of attention on the defects present at the different levels of the posterior vaginal compartment. We have shown that defects are different from those traditionally thought to be present. These may then be used to guide appropriate surgical measures on a case-specific basis, rather than employing a onesize-fits-all standardized repair. The latter, by not being individualized to the patient s anatomy, might leave some defects unresolved. It also has the potential to create new defects [3]. A weakness of the study is that it does not, at this stage, include further short- and longer-term follow-up data, including rate of recurrent cystocele with increased use of posterior SSC. Part of the future difficulty in creating follow-up data is the need for PR-Q measurements to be performed under anesthesia. In this study, we did not want to confuse or compromise the key message. Other validation studies, including interobserver reliability studies are planned to determine PR-Q prolapse markers. Acknowledgments The authors thank the theater teams at St. Vincent s and Mater Hospitals, Sydney, for providing support and facilitating this study. We acknowledge surgical assistant Dr. John McNamara as an additional observer to measurements, anesthetists for their support and patience, associate professor Alan Molloy and Drs. Colleen Kane, Simon Adamo, Luke Vyvyan, and Alex Wang, who recorded most measurements. Compliance with ethical standards Conflicts of interest References None. 1. DeLancey JOL (1992) Anatomic aspects of vaginal eversion after hysterectomy. Am J Obstet Gynecol 166: Fowler GE, Richmond DH (2011) Operations for pelvic organ prolapse. In: Lopes T, Spirtos NM, Naik R, Monaghan JM Bonney s Gynaecological Surgery, 11th edn. Wiley-Blackwell London. Chapter 16. P Nichols DH, Randall CL (1996) Posterior colporrhaphy and perineorrhaphy. In Nichols DH, Randall CL Vaginal surgery, 4th edn. Williams & Wilkins. Baltimore. Chapter 11 p Karram MM, Maher C (2013) Surgery for posterior vaginal wall prolapse. Int Urogynecol J 24(1835 1): Summers A, Winkel LA, Hussain HK, DeLancey JOL (2006) The relationship between anterior and apical compartment support. Am J Obstet Gynecol 194: Haylen BT, Avery D, Chiu TL, Birrell W (2014) Posterior repair quantification (PR-Q) using key anatomical indicators (KAI) Preliminary Report. Int Urogynecol J 2014(25): Bump RC, Mattiasson A, Bo K, Brubaker LP et al (1996) The standardization of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175(1): Yang A, Mostwin J, Genadry R, Sanders R (1993) Patterns of prolapse demonstrated with dynamic fastscan MRI; reassessment of conventional concepts of pelvic floor weaknesses. Neurourol Urodyn 12(4): Haylen BT, Freeman RM, de Ridder D, Swift SE, Berghmans B, Lee J, Monga A, Petri E, Rizk D, Sand P, Schaer G (2010). An International Urogynecological Association (IUGA) International Continence Society (ICS) Joint Report into the Terminology for Female Pelvic Floor Dysfunction. Neurourol Urodyn 29:4 20. Int Urogynecol J 21: Haylen BT, Vu D, Birrell W, Vashevnik S, Tse K (2012) A preliminary anatomical basis for dual (uterosacral and sacrospinous ligaments) vaginal vault support at colporrhaphy. Int Urogynecol J 23: Samaan A, Vu D, Haylen BT, Tse K (2014) Cardinal ligament surgical anatomy: cardinal points at hysterectomy. Int Urogynecol J 25(2): Vu D, Haylen BT, Tse K, Farnsworth A (2010) Surgical anatomy of the uterosacral ligament. Int Urogynecol J 21: McCall ML (1957) Posterior culdoplasty: surgical correction of enterocoele during vaginal hysterectomy; a preliminary report. Obstet Gynecol 10: Montella JM, Morrill MY (2005) Effectiveness of the McCall culdeplasty in maintaining support after vaginal hysterectomy. Int Urogynecol J 16: Francis WFA, Jeffcoate TNA (1961) Dyspareunia following vaginal operations. J Obstet Gynaecol Br Commonw 68: Richardson AC (1993) The rectovaginal septum revisited: its relationship to rectocele and its importance in rectocele repair. Clin Obstet Gynecol 36: Richardson AC (1995) The anatomic defects in rectocele and enterocele. J Pelvic Surg 1: Lewicky-Gaupp C, Yousuf A, Larson KA, Fenner DE, DeLancey JOL (2010) Structural position of the posterior vagina and pelvic floor in women with and without posterior vaginal prolapse. Am J Obstet Gynecol 202(5): Ghetti C, Grerory WT, Edwards SR, Otto LN, Clark AL (2005) Severity of pelvic organ prolapse associated with measurements of pelvic floor function. Int Urogynecol J 16: Haylen BT, Birrell W, Naidoo S, Younis M (2014) Perineorrhaphy quantitative assessment (Pe-QA). Int Urogynecol J 26(4):
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments?
 Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after vaginal hysterectomy
 Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR SURGICAL PROCEDURES TO
 AN AMERICAN UROGYNECOLOGIC SOCIETY (AUGS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR SURGICAL PROCEDURES TO TREAT PELVIC ORGAN PROLAPSE NEED FOR A WORKING
AN AMERICAN UROGYNECOLOGIC SOCIETY (AUGS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR SURGICAL PROCEDURES TO TREAT PELVIC ORGAN PROLAPSE NEED FOR A WORKING
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Original article J Bas Res Med Sci 2015; 2(2): The incidence of recurrent pelvic organ prolapse: A cross sectional study
 The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
How to use the Pelvic Organ Prolapse Quantification (POP-Q) system?
 Received: 30 April 2018 Accepted: 17 May 2018 DOI: 10.1002/nau.23740 SOUNDING BOARD How to use the Pelvic Organ Prolapse Quantification (POP-Q) system? Chendrimada Madhu 1 Steven Swift 2 Sophie Moloney-Geany
Received: 30 April 2018 Accepted: 17 May 2018 DOI: 10.1002/nau.23740 SOUNDING BOARD How to use the Pelvic Organ Prolapse Quantification (POP-Q) system? Chendrimada Madhu 1 Steven Swift 2 Sophie Moloney-Geany
Gökmen Sukgen, 1 Esra SaygJlJ YJlmaz, 2 and Eralp BaGer Introduction. 2. Case Presentation
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
The UK National Prolapse Survey: 10 years on
 Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
What are we talking about? Symptoms. Prolapse Risk Factors. Vaginal bulge 1 Splinting. ?? Pelvic pressure Back pain 1 Urinary complaints 2
 Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Site-specific fascial defects in the diagnosis and surgical management of enterocele
 Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy
 Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Association between ICS POP-Q coordinates and translabial ultrasound findings: implications for definition of normal pelvic organ support
 Ultrasound Obstet Gynecol 216; 47: 36368 Published online 29 January 216 in Wiley Online Library (wileyonlinelibrary.com). DOI: 1.12/uog.14872 Association between ICS POP-Q coordinates and translabial
Ultrasound Obstet Gynecol 216; 47: 36368 Published online 29 January 216 in Wiley Online Library (wileyonlinelibrary.com). DOI: 1.12/uog.14872 Association between ICS POP-Q coordinates and translabial
Prolapse & Stress Incontinence
 Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
Vaginal McCall culdoplasty versus laparoscopic uterosacral plication to prophylactically address vaginal vault prolapse
 Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Laparoscopic sacrocolpopexy: how low does the mesh go?
 Ultrasound Obstet Gynecol 2017; 49: 404 408 Published online 7 February 2017 in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.15882 Laparoscopic sacrocolpopexy: how low does the mesh
Ultrasound Obstet Gynecol 2017; 49: 404 408 Published online 7 February 2017 in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.15882 Laparoscopic sacrocolpopexy: how low does the mesh
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
Study of correlation between symptoms and signs in women with anterior vaginal wall prolapse
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Bijwe SA et al. Int J Reprod Contracept Obstet Gynecol. 2017 Jul;6(7):3155-3159 www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20172953
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Bijwe SA et al. Int J Reprod Contracept Obstet Gynecol. 2017 Jul;6(7):3155-3159 www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20172953
SACROSPINOUS LIGAMENT FIXATION, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE
 Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks
 T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
Imaging of Pelvic Floor Weakness. Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne
 Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Use of a visual analog scale for evaluation of bother from pelvic organ prolapse
 Ultrasound Obstet Gynecol 2014; 43: 693 697 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.13222 Use of a visual analog scale for evaluation of bother from pelvic organ
Ultrasound Obstet Gynecol 2014; 43: 693 697 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.13222 Use of a visual analog scale for evaluation of bother from pelvic organ
ISSN (o): Sacrospinous fixation: an efficient technique for prevention and treatment of vault prolapse
 Original article www.ijrhs.com ISSN (o):2321 7251 Sacrospinous fixation: an efficient technique for prevention and treatment of vault Rajshree dayanand katke 1, Usha kiran. 2 1M.D.(Obstetrics & Gynecology),
Original article www.ijrhs.com ISSN (o):2321 7251 Sacrospinous fixation: an efficient technique for prevention and treatment of vault Rajshree dayanand katke 1, Usha kiran. 2 1M.D.(Obstetrics & Gynecology),
Diagnosis of cystocele type by clinical examination and pelvic floor ultrasound
 Ultrasound Obstet Gynecol 2012; 39: 710 714 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.10156 Diagnosis of cystocele type by clinical examination and pelvic floor
Ultrasound Obstet Gynecol 2012; 39: 710 714 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.10156 Diagnosis of cystocele type by clinical examination and pelvic floor
JMSCR Volume 03 Issue 03 Page March 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes
 DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
Predicting Treatment Choice for Patients With Pelvic Organ Prolapse
 Predicting Treatment Choice for Patients With Pelvic Organ Prolapse Michael Heit, MD, MSPH, Chris Rosenquist, MD, Patrick Culligan, MD, Carol Graham, MD, Miles Murphy, MD, and Susan Shott, PhD OBJECTIVE:
Predicting Treatment Choice for Patients With Pelvic Organ Prolapse Michael Heit, MD, MSPH, Chris Rosenquist, MD, Patrick Culligan, MD, Carol Graham, MD, Miles Murphy, MD, and Susan Shott, PhD OBJECTIVE:
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
High success rate and considerable adverse events of pelvic prolapse surgery with Prolift: A single center experience
 Available online at www.sciencedirect.com ScienceDirect Taiwanese Journal of Obstetrics & Gynecology 52 (2013) 389e394 Short Communication High success rate and considerable adverse events of pelvic prolapse
Available online at www.sciencedirect.com ScienceDirect Taiwanese Journal of Obstetrics & Gynecology 52 (2013) 389e394 Short Communication High success rate and considerable adverse events of pelvic prolapse
Index. Cyclical pelvic pain, 37 Cystocele, 22, 23, 25, 48, 51, 52, 54, 56, 124, 148, 160
 A Abdominal approach, 141 Abdominal hernia s surgery, 123, 124 Abdominal sacrocolpopexy (ASC), 116, 117 Abnormal uterine bleeding, 96 Anterior compartment repair, 101, 102 Apical compartment repair, 96
A Abdominal approach, 141 Abdominal hernia s surgery, 123, 124 Abdominal sacrocolpopexy (ASC), 116, 117 Abnormal uterine bleeding, 96 Anterior compartment repair, 101, 102 Apical compartment repair, 96
Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience with Prolift Mesh in 84 Women with Complicated Pelvic Prolapses
 Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Pelvic Floor Reconstruction
 3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Keywords De novo prolapse, mesh, surgery, untreated compartment,
 DOI: 10.1111/j.1471-0528.2011.03231.x www.bjog.org Urogynaecology Development of de novo prolapse in untreated vaginal compartments after prolapse repair with and without mesh: a secondary analysis of
DOI: 10.1111/j.1471-0528.2011.03231.x www.bjog.org Urogynaecology Development of de novo prolapse in untreated vaginal compartments after prolapse repair with and without mesh: a secondary analysis of
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation
 Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
University of Bristol - Explore Bristol Research
 O'brien, S., Dua, A., & Vij, M. (2016). Practices in pelvic organ prolapse operations among surgeons: an international survey identifying needs for further research. International Urogynecology Journal,
O'brien, S., Dua, A., & Vij, M. (2016). Practices in pelvic organ prolapse operations among surgeons: an international survey identifying needs for further research. International Urogynecology Journal,
Safe and effective intervention surgery for pelvic organ prolapse with CR-Mesh kit: a comparative study from United Kingdom and Italy
 Original article Safe and effective intervention surgery for pelvic organ prolapse with CR-Mesh kit: a comparative study from United Kingdom and Italy NARMADA KATAKAM 1, DAVIDE DE VITA 2, KV CHIA 1 1 Royal
Original article Safe and effective intervention surgery for pelvic organ prolapse with CR-Mesh kit: a comparative study from United Kingdom and Italy NARMADA KATAKAM 1, DAVIDE DE VITA 2, KV CHIA 1 1 Royal
Guest Editorial Seeing the future by appreciating the past
 Volume 2, Issue 3 SEPTEMBER 2014 Editorial Peter de Jong Congratulations to Etienne Henn who produced this Edition of the SAUGA Newsletter. Short and to the point as always. His editorial is appropriate
Volume 2, Issue 3 SEPTEMBER 2014 Editorial Peter de Jong Congratulations to Etienne Henn who produced this Edition of the SAUGA Newsletter. Short and to the point as always. His editorial is appropriate
ig. 2. The organs and their outlet tubes.
 Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
Aetiology 1998 Bump & Norton Theoretical model
 Kate Lough MSc MCSP Handout IUGA Nice 2015 Physiotherapy and the Provision of Pelvic Floor Muscle Training and Lifestyle Intervention in the Conservative Management of Pelvic Organ Prolapse an evidence
Kate Lough MSc MCSP Handout IUGA Nice 2015 Physiotherapy and the Provision of Pelvic Floor Muscle Training and Lifestyle Intervention in the Conservative Management of Pelvic Organ Prolapse an evidence
American Journal of Obstetrics and Gynecology
 American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
Pelvic organ prolapse: A primer for urologists
 review Pelvic organ prolapse: A primer for urologists Michel Bureau, MD; Kevin V. Carlson, MD Section of Urology, Department of Surgery, University of Calgary, Calgary, AB, Canada Cite as: Can Urol Assoc
review Pelvic organ prolapse: A primer for urologists Michel Bureau, MD; Kevin V. Carlson, MD Section of Urology, Department of Surgery, University of Calgary, Calgary, AB, Canada Cite as: Can Urol Assoc
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Le fort s operation for prolapse uterus: A forgotten procedure
 2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Complications from permanent synthetic mesh
 Original Research Symptom Resolution After Operative Management of Complications From Transvaginal Mesh Erin C. Crosby, MD, Melinda Abernethy, MD, MPH, Mitchell B. Berger, MD, PhD, John O. DeLancey, MD,
Original Research Symptom Resolution After Operative Management of Complications From Transvaginal Mesh Erin C. Crosby, MD, Melinda Abernethy, MD, MPH, Mitchell B. Berger, MD, PhD, John O. DeLancey, MD,
Female Urology. Young-Suk Lee, Deok Hyun Han, Ji Youl Lee 1, Joon Chul Kim 2, Myung-Soo Choo 3, Kyu-Sung Lee
 www.kjurology.org DOI:1.4111/kju.21.51.3.187 Female Urology Anatomical and Functional Outcomes of Posterior Intravaginal Slingplasty for the Treatment of Vaginal Vault or Uterine Prolapse: A Prospective,
www.kjurology.org DOI:1.4111/kju.21.51.3.187 Female Urology Anatomical and Functional Outcomes of Posterior Intravaginal Slingplasty for the Treatment of Vaginal Vault or Uterine Prolapse: A Prospective,
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA
 AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
Medium-term follow-up on use of freeze-dried, irradiated donor fascia for sacrocolpopexy and sling procedures
 Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy
 Int Urogynecol J (2011) 22:577 584 DOI 10.1007/s00192-010-1325-8 ORIGINAL ARTICLE Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy Stergios K. Doumouchtsis
Int Urogynecol J (2011) 22:577 584 DOI 10.1007/s00192-010-1325-8 ORIGINAL ARTICLE Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy Stergios K. Doumouchtsis
New Directions in Restoration of Pelvic Structure and Function
 2 New Directions in Restoration of Pelvic Structure and Function Peter E. Petros and Bernhard Liedl The fundamental theme of this chapter is that structure and function are intimately related. Abnormal
2 New Directions in Restoration of Pelvic Structure and Function Peter E. Petros and Bernhard Liedl The fundamental theme of this chapter is that structure and function are intimately related. Abnormal
High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay
 High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay Poster No.: C-430 Congress: ECR 2009 Type: Educational Exhibit Topic: Abdominal and
High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay Poster No.: C-430 Congress: ECR 2009 Type: Educational Exhibit Topic: Abdominal and
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Recent advances in POP. Dr. Bernhard Uhl Department for Obstetrics and Gynecology St. Vinzenz-Hospital Dinslaken Germany
 Recent advances in POP Dr. Bernhard Uhl Department for Obstetrics and Gynecology St. Vinzenz-Hospital Dinslaken Germany Level of pelvic floor support Level I apical Level II transverse/ horizontal Level
Recent advances in POP Dr. Bernhard Uhl Department for Obstetrics and Gynecology St. Vinzenz-Hospital Dinslaken Germany Level of pelvic floor support Level I apical Level II transverse/ horizontal Level
Female Urology. The Results of Grade IV Cystocele Repair Using Mesh. Introduction ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M
 Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Ballooning of the levator hiatus
 Ultrasound Obstet Gynecol 2008; 31: 676 680 Published online 12 May 2008 in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/uog.5355 Ballooning of the levator hiatus H. P. DIETZ*, C. SHEK*,
Ultrasound Obstet Gynecol 2008; 31: 676 680 Published online 12 May 2008 in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/uog.5355 Ballooning of the levator hiatus H. P. DIETZ*, C. SHEK*,
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October :00-12:00
 W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
Pelvic Organ Prolapse: Diagnosis, Treatment, and Avoiding Complications
 Pelvic Organ Prolapse: Diagnosis, Treatment, and Avoiding Complications Christina Dancz and Morgan Fullerton Contents 1 Introduction... 2 2 Anatomy/Pathophysiology... 2 2.1 Level 1: The Cardinal and Uterosacral
Pelvic Organ Prolapse: Diagnosis, Treatment, and Avoiding Complications Christina Dancz and Morgan Fullerton Contents 1 Introduction... 2 2 Anatomy/Pathophysiology... 2 2.1 Level 1: The Cardinal and Uterosacral
Surgical treatments for vaginal apical prolapse
 Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Surgery for women with apical vaginal prolapse(review)
 Cochrane Database of Systematic Reviews (Review) Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J.. Cochrane Database
Cochrane Database of Systematic Reviews (Review) Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J.. Cochrane Database
Levator trauma is associated with pelvic organ prolapse
 DOI: 10.1111/j.1471-0528.2008.01751.x www.blackwellpublishing.com/bjog Urogynaecology Levator trauma is associated with pelvic organ prolapse HP Dietz, a JM Simpson b a Department of Obstetrics and Gynaecology,
DOI: 10.1111/j.1471-0528.2008.01751.x www.blackwellpublishing.com/bjog Urogynaecology Levator trauma is associated with pelvic organ prolapse HP Dietz, a JM Simpson b a Department of Obstetrics and Gynaecology,
Management of Urogenital Prolapse of Women in Primary Care. Lizzie McManus MBE RGN RMN Practice nurse Womens health practitioner
 Management of Urogenital Prolapse of Women in Primary Care Lizzie McManus MBE RGN RMN Practice nurse Womens health practitioner Primary Care Womens Health Forum www.pcwhf.org.uk Useful websites RCN genital
Management of Urogenital Prolapse of Women in Primary Care Lizzie McManus MBE RGN RMN Practice nurse Womens health practitioner Primary Care Womens Health Forum www.pcwhf.org.uk Useful websites RCN genital
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Prolaps: Anteriore Rektopexie nach D Hoore. Prof. Dr. med. F. Hetzer
 Prolaps: Anteriore Rektopexie nach D Hoore Prof. Dr. med. F. Hetzer franc.hetzer@spital-linth.ch Rectal prolapse pathophysiology 24 22 20 18 congenital female pathology (90%) 16 14 straining weakened pelvic
Prolaps: Anteriore Rektopexie nach D Hoore Prof. Dr. med. F. Hetzer franc.hetzer@spital-linth.ch Rectal prolapse pathophysiology 24 22 20 18 congenital female pathology (90%) 16 14 straining weakened pelvic
High risk of complications with a single incision pelvic floor repair kit: results of a retrospective case series
 Int Urogynecol J (2014) 25:109 116 DOI 10.1007/s00192-013-2156-1 ORIGINAL ARTICLE High risk of complications with a single incision pelvic floor repair kit: results of a retrospective case series Stephen
Int Urogynecol J (2014) 25:109 116 DOI 10.1007/s00192-013-2156-1 ORIGINAL ARTICLE High risk of complications with a single incision pelvic floor repair kit: results of a retrospective case series Stephen
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Bilateral sacrospinous fixation after second recurrence of vaginal vault prolapse:
 Bilateral sacrospinous fixation after second recurrence of vaginal vault prolapse: efficacy and impact on quality of life and sexuality. Salvatore Giovanni Vitale 1, Diego Rossetti 2, Marco Noventa 3,
Bilateral sacrospinous fixation after second recurrence of vaginal vault prolapse: efficacy and impact on quality of life and sexuality. Salvatore Giovanni Vitale 1, Diego Rossetti 2, Marco Noventa 3,
High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
 Int Urogynecol J (2010) 21:515 522 DOI 10.1007/s00192-009-1064-x ORIGINAL ARTICLE High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
Int Urogynecol J (2010) 21:515 522 DOI 10.1007/s00192-009-1064-x ORIGINAL ARTICLE High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy
 Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Stephen T Jeffery. University of Cape Town, South Africa
 Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
W12: Approaches to Pelvic Organ Prolapse Surgery Workshop Chair: Philippe Zimmern, United States 06 October :00-17:00
 W12: Approaches to Pelvic Organ Prolapse Surgery Workshop Chair: Philippe Zimmern, United States 06 October 2015 14:00-17:00 Start End Topic Speakers 14:00 14:30 Goals of repair and anatomical principles
W12: Approaches to Pelvic Organ Prolapse Surgery Workshop Chair: Philippe Zimmern, United States 06 October 2015 14:00-17:00 Start End Topic Speakers 14:00 14:30 Goals of repair and anatomical principles
Introduction. Regarding the Section of the UPDATE Entitled Purpose
 Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Functional Anatomy of the Pelvic Floor and Lower Urinary Tract
 CLINICAL OBSTETRICS AND GYNECOLOGY Volume 47, Number 1, 3 17 2004, Lippincott Williams & Wilkins, Inc. Functional Anatomy of the Pelvic Floor and Lower Urinary Tract JOHN T. WEI, MD* and JOHN O. L. DE
CLINICAL OBSTETRICS AND GYNECOLOGY Volume 47, Number 1, 3 17 2004, Lippincott Williams & Wilkins, Inc. Functional Anatomy of the Pelvic Floor and Lower Urinary Tract JOHN T. WEI, MD* and JOHN O. L. DE
Guide to Pelvic Floor Multicompartment Scanning
 Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Childbirth, chronic coughing, heavy lifting,
 OBG MANAGEMENT BY THOMAS JULIAN, MD Pelvic-support defects: a guide to anatomy and physiology Due to high postoperative failure rates, the traditional treatment for pelvic-organ prolapse hysterectomy with
OBG MANAGEMENT BY THOMAS JULIAN, MD Pelvic-support defects: a guide to anatomy and physiology Due to high postoperative failure rates, the traditional treatment for pelvic-organ prolapse hysterectomy with
Incidence rate and risk factors for vaginal vault prolapse repair after hysterectomy
 Int Urogynecol J (2008) 19:1623 1629 DOI 10.1007/s00192-008-0718-4 ORIGINAL ARTICLE Incidence rate and risk factors for vaginal vault prolapse repair after hysterectomy Patrick Dällenbach & Isabelle Kaelin-Gambirasio
Int Urogynecol J (2008) 19:1623 1629 DOI 10.1007/s00192-008-0718-4 ORIGINAL ARTICLE Incidence rate and risk factors for vaginal vault prolapse repair after hysterectomy Patrick Dällenbach & Isabelle Kaelin-Gambirasio
Glasgow Caledonian University
 ResearchOnline@GCU Glasgow Caledonian University Feasibility, inter- and intra-rater reliability of physiotherapists measuring prolapse using the pelvic organ prolapse quantification system Stark, Diane;
ResearchOnline@GCU Glasgow Caledonian University Feasibility, inter- and intra-rater reliability of physiotherapists measuring prolapse using the pelvic organ prolapse quantification system Stark, Diane;
Anterior six arms prolene mesh for high stage vaginal prolapse: five years follow-up
 ORIGINAL ARTICLE Vol. 43 (3): 525-532, May - June, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0482 Anterior six arms prolene mesh for high stage vaginal prolapse: five years follow-up Luis Gustavo M. de Toledo
ORIGINAL ARTICLE Vol. 43 (3): 525-532, May - June, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0482 Anterior six arms prolene mesh for high stage vaginal prolapse: five years follow-up Luis Gustavo M. de Toledo
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
