OBG. Augmenting pelvic floor repairs. The use of mesh or grafts to augment surgical NEW MATERIALS AND TECHNIQUES MANAGEMENT
|
|
|
- Junior Davidson
- 6 years ago
- Views:
Transcription
1 Available at OBG MANAGEMENT January 2006 Augmenting pelvic floor repairs NEW MATERIALS AND TECHNIQUES Neeraj Kohli, MD, MBA, Editor Director, Division of Urogynecology Brigham and Women s Hospital Harvard Medical School Boston, Massachusetts Roger Goldberg, MD, MPH Assistant Professor of Obstetrics and Gynecology Northwestern University Chicago, Illinois Director of Research, Urogynecology Evanston Continence Center Evanston, Illinois Joseph Maccarone, MD Head, Division of Female Pelvic Medicine and Reconstructive Surgery Cooper Health System Camden, New Jersey The faculty have reported the following relationships with pharmaceutical companies or device manufacturers: Dr Goldberg is a consultant to Boston Scientific Corporation. Dr Kohli is a consultant to Boston Scientific and is on the speakers bureau of Bard, Pfizer, Novartis, and Yamanouchi. He receives research support from American Medical Systems. Dr Maccarone has received grants/research support from Boston Scientific, Bard, and Pfizer. He is on the speakers bureau of Pfizer, Indevus, Astellas, Bard, and Boston Scientific Corporation. Supported by a grant from Boston Scientific Corporation The use of mesh or grafts to augment surgical repairs is an established technique in many settings. In gynecologic surgery, mesh or grafts help correct paravaginal anterior or posterior compartment defects in patients for whom traditional prolapse repair techniques are inadequate or in patients who are recurrent or complicated cases. Traditional anterior repairs have been marked by failure rates between 25% and 52%. 1-4 Mesh or graft augmentation corrects both central and site-specific defects and restores correct anatomic support. It may provide additional stability to traditional repair, decreasing recurrence and the need for future procedures. Graft and mesh materials are readily available, but clinicians should be well informed as to the characteristics, safety profile, and clinical outcomes associated with their materials of choice. A trocar-free technique, the focus of this publication, minimizes the potential for bowel and vascular injuries associated with blind needle insertion. Thus, the risk for perforation of the gluteal, levator ani, or obturator muscles is avoided. The mesh augmentation procedures themselves are performed quickly and easily through the same incision utilized for traditional colporrhaphy. They may reduce operating-room time or add no more than 10 to 20 minutes to procedures. Disadvantages include the introduction of foreign material and the potential for complications, such as erosion. Costs are increased as well. While long-term data currently are being collected, short-term results are marked by encouraging rates of success. This monograph will review currently available materials, surgical technique, preliminary outcomes of clinical trials, and physician preferences. COPYRIGHT 2006 DOWDEN HEALTH MEDIA January 2006 Supplement to OBG Management S1
2 Augmenting pelvic floor repairs New materials and techniques As surgeons, we need to remember that prolapse results not from failure of the pelvic organs themselves but rather from defects in the vaginal connective tissues and ligaments that support the bladder, rectum, or bowel. In the anterior compartment, displacement of these organs may occur through distension injuries, such as a central cystocele with attenuation of the midline connective tissues that still remain attached to their fixed side-wall attachment points. Also possible are detachment injuries, such as a paravaginal defect in the anterior compartment, whereby vaginal connective tissues avulse from fixed anchoring points. Some patients can have a combination of both injuries. Displacement or distension injuries may also result from tears in posterior or apical connective tissue structures. When should augmentation be considered? Mesh or graft repairs are not substitutes for traditional colporrhaphy, which depends on adequate tissue for a strong repair. Instead, these techniques replace existing (and typically insufficient) tissue with a stronger material. These repairs are appropriate for patients: for whom previous reconstructive surgery has failed; the risk of needing reoperation for recurrent prolapse is 29.2%. 1 in whom dissection reveals inadequate tissue who are elderly and benefit from speedy procedures, which may result from the use of graft/mesh repairs who are young and with significant prolapse, suggesting congenital collagen deficiency with risk factors for recurrence (obesity, chronic cough, constipation, or Valsalva, or occupational risk factors associated with straining and heavy lifting) Failures of traditional approaches often are associated with suturing of poor tissue to poor tissue (a fundamentally flawed concept), insufficient support by the levator plate and weak attachments to the pelvic side wall and apex, and the composition of tissues in the anterior compartment (less dense and more elastic). A recent review of the literature and gross/microscopic evaluation of full-thickness bladder and vaginal-wall specimens revealed a complex support structure that maintains the position of important structures. 2 Identifying anatomic landmarks for correct graft/mesh placement Correct placement of mesh/graft materials depends on accurate identification of anatomic points for suture attachment. Bony structures serve as landmarks and guide the surgeon to the connective tissue and muscles that are the specific repair sites. These landmarks are consistent in every patient, regardless of the soft tissue structure. Anterior compartment repairs For cystocele repair, the essential bony landmarks are the sacral promontory, ischial spine, and pubic tubercle. These bones provide a reliable reference to the muscles/ligaments that splay out to each side and which serve as attachment points to anchor grafts. All structures are accessible vaginally. The sacrospinous ligament (important for apical suspension and for cystocele or rectocele repair) stretches from the ischial spine back to the sacrum. It is located at the front of the coccygeus muscle. The arcus tendineus fascia pelvis, also known as the white line, is a connective tissue remnant lying on the obturator internus muscle and extends from the ischial spine to the pubic tubercle. The iliococcygeus muscle lies medial to the arcus tendineus and is a shelf-like levator muscle that is utilized for posterior graft augmentation and also as a substitute for the sacrospinous ligament during repair of vaginal vault prolapse. Posterior compartment repairs Rectocele repair focuses on repair of the connective tissue layer that separates the rectum from the vaginal epithelium. Essential anatomic boundaries are the vaginal apex (proximal), the superior fascia of the levator ani (lateral), and the perineal body (distal). Unlike anterior compartment repairs, standard posterior colporrhaphy is associated with relatively high success rates, even for large rectoceles, but may be associated with dyspareunia due to levator plication. However, graft/mesh augmented repairs may be of benefit when the tissue layer is insufficient to reunite the fascial edge with its apical attachment or when individuals have had failed surgical repairs. In this type of repair, a rectangular graft is extended from the level of the ischial spine to the perineal body, anchoring laterally to the levator (iliococcygeus) muscle surface. As with the anterior compartment grafts, use of the Capio Ligature Carrier (Boston Scientific S2 Supplement to OBG Management January 2006
3 OBG MANAGEMENT Corporation, Natick, Mass) posteriorly allows for fixation rather than perforation of the levator ani muscle and apical fixation point. Apically, the graft is sutured either into the sacrospinous muscle or just distal and lateral to the spine into the iliococcygeus. FIGURE 1 The Capio Ligature Device Practical pearls for performing graft/mesh augmentation Surgeons who are competently trained in anterior compartment repairs have most of the skills needed to perform mesh/graft augmentation. The procedure requires a standard colporrhaphy incision, palpation of bony landmarks to locate the muscles, use of a device to place sutures, and graft materials. Patients presenting with a grade 3 or 4 prolapse, those with a history of previous surgical failure, or those with risk factors for recurrence are the typical patients selected for possible graft augmentation. Dissection. The gentle dissection from the pubic tubercle to the ischial spine differs slightly from traditional approaches used for colporrhaphy: the dissection is made 1 cm to 2 cm lateral to the normal cystocele dissection. With blunt dissection, the obturator internus muscle (and in many cases, the overlying arcus tendineus) can be felt, just lateral to the descending pubic ramus on each side. During fascial dissection, most surgeons are taught to keep the fascia on the bladder side (ie, make the vaginal flaps thinner). Now that surgeons use the mesh to replace the fascia, it is important to place a thicker layer of epithelial and connective tissue over the mesh to avoid erosion. Palpation. The operator then locates the bony landmarks by tracing a line between the pubic tubercle and ischial spine. If direct visualization is desired, Breisky-Navratil retractors are well suited for exposing the arcus tendineus, coccygeus muscle, and sacrospinous ligament without obstructing the surgical field. Some surgeons use retractors or suction devices mounted with a fiberoptic light source to identify the retropubic anatomy. However, the Capio suture device allows accurate suture placement by palpation, minimizing the need for extensive dissection or retractor use. Device selection for suture placement. Various tools can be used for suture placement, including the Deschamps ligature carrier, Miya Hook TM (CooperSurgical, Inc, Trumbull, Conn), and Capio device. Some surgeons also use a standard long The long narrow tool catches and passes sutures easily, allowing deep suture throws without excessive dissection. curved needle holder. The Capio is ideal for suturing into the sacrospinous ligament (via cystocele or rectocele repair), the arcus tendineus, obturator internus, or iliococcygeus. The long, narrow tool catches and passes the sutures easily, allowing deep suture throws without excessive dissection (FIGURE 1). It allows for placement of sutures based on direct visualization or palpation and provides a consistent depth of suture placement. Importantly, the device permits fixation not perforation of the suture into musculature and can be used to place both apical and basal stitches; basal stitches may also be placed free-form. Suture placement. The first sutures are placed at the apex; with the Capio, a 30-to-45º angle between the needle catch and the ligament provides adequate suture fixation. Additionally, as the ligament lies within the muscle, sutures should not be placed around the sacrospinous ligament. Instead, sutures should be placed into the front side of the coccygeus muscle and sacrospinous ligament to avoid pudendal or major vascular injury. Mesh characteristics. The nuances of mesh/ graft size and specific placement will be described subsequently with respect to various available meshes. In all procedures, however, it is important that the mesh be adjusted loosely (this varies with the type of mesh/graft) and with January 2006 Supplement to OBG Management S3
4 Augmenting pelvic floor repairs New materials and techniques TABLE 1 Repair With Synthetic Mesh AUTHOR N MESH COMPLICATIONS RESULTS FOLLOW-UP (mo) Watson 9 Polypropylene 11% wound infection Not stated 29 et al, Transperineal Dwyer and 67 Polypropylene 12% erosion 0% 24 O Reilly, (Atrium) 1 RVF dyspareunia Salvatore 31 Prolene 13% erosion et al, Plus Colpor. Dyspareunia 6 69% Mercer-Jones 22 Prolene 3 infections 75% improved 12 et al, rectal perforations a minimum of folds. Overly tight attachments may result in patient pain and increased possibility of erosions. Coding and reimbursement. In coding for graft and mesh repairs, surgeons may want to note that graft repairs can be coded for each incision; the use of 2 incisions permits coding for 2 repairs. A recently introduced current procedural terminology (CPT) code is used as an add-on code to reimburse surgeons for the added work/complexity associated with graft/mesh prolapse augmented repairs. Follow-up to monitor for erosions. Evidence of erosions should be assessed at 2 weeks and 6 weeks after the procedure and at 6-month intervals for 2 years thereafter. If evidence of erosion is seen, prescription of an estrogen cream, office-based excision, and 6 weeks of pelvic rest generally are effective. Materials for prolapse repair Currently available materials include synthetic mesh, allografts, or xenografts. Long-term outcomes data are lacking, although a randomized, case-controlled clinical trial is in progress. At present, however, insufficient data exist regarding terms of functional outcomes and prevalence of dyspareunia. While the ideal material for repair of prolapse has not been identified, new products and refinement of surgical technique offer significant hope for future successes and may improve outcomes for patients. Use of synthetics in pelvic repair Bioengineered mesh materials are permanent and feature elasticity, flexibility, and tensile strength. Mesh is readily available and features a consistent manufacturing process, which offers reproducibility with consistent strength and tissue response. Mesh typically allows tissue in-growth with resulting fixation and continued support. There is a low risk for infection transmission, but erosion can occur and patients with vaginal atrophy or thin vaginal walls, now or in the future, may be at increased risk. Historically, erosion rates as high as 13% have been reported. 5-8 Some institutions, however, report erosion rates of less than 5% with a 20% reduction in recurrent prolapse (Kohli, personal communication). (SEE ONE SURGEON S TECHNIQUE: USE OF SYNTHETIC MATERI- ALS, PAGE 7) The risk for erosion may be minimized by selection of the appropriate mesh material (soft, pliable, macropore meshes) and surgical technique (dissection, fixation, hemostasis, and vaginal packing). Additionally, a surgeon s technique of ensuring that the mesh attachment is laced without tension is important to prevent erosions and ensure good outcomes. Currently available products feature pore sizes sufficient to allow tissue in-growth and to fight infection; therefore, the risk for breakdown of materials is eliminated. New materials offer increased thinness and allow sufficient stretch to accommodate the vagina as a dynamic organ that needs to expand during sexual activity. More rigid materials may not permit vaginal expansion and also may increase the risk for erosion as the vaginal wall thins during the menopause. The results of trials using various forms of mesh 5-8 are shown in TABLE 1. A new product, Polyform (Boston Scientific Corporation, Natick, Mass), (FIGURE 2) offers an important option for clinicians (TABLE 2). It is characteristic of the technical advances in materials that are continually being made. S4 Supplement to OBG Management January 2006
5 OBG MANAGEMENT A recent pre-clinical review compared the in vivo repair processes of Polyform and Gynemesh (GYNECARE WORLDWIDE, Somerville, NJ) in an animal model at 1, 3, 6, and 12 weeks. Collagen deposition and wound-healing properties and processes were evaluated. 9 Neither product led to encapsulation. Wound healing was characterized by collagen deposition and tissue integration rather than fibrous capsule isolation. Both materials behaved similarly at all time points with respect to the inflammatory and wound-healing response and collagen-deposition characteristics. Physician-dependent factors also affect outcomes. These include musculofascial dissection, tension-free application, use of strong attachment points, minimization of folds, good hemostasis, absence of tension on the suture line, and vaginal packing. Use of allografts in pelvic repair Repairs using allograft materials avoid many of the problems associated with traditional repairs, including the use of trocars and the risk for muscle perforation. They also avoid the potential for stray mesh arms and thereby reduce the potential for erosion. (SEE ONE SURGEON S TECHNIQUE: USE OF ALLOGRAFT MATERIALS, PAGE 7) As is true with synthetic materials, allograft materials are marked by continual innovations in the marketplace. Allograft materials are composed of acellular cadaveric dermis, an extracellular matrix of connective tissue. Tissue is procured from the American Association of Tissue Banks. The graft allows the body to regenerate its own tissue onto the scaffolding provided by the matrix. The transition from graft to functional host tissue mirrors what we see in native tissue: A recent trial with Repliform (LifeCell Corporation, Branchburg, NJ), demonstrated that, within 12 weeks, typically, graft material can no longer be distinguished from the patient s native skin borders. Histology confirmed robust, vital, and intact collagen with normal cell density at 12 months. Safety has been confirmed: in 12 years of clinical experience, more than 750,000 grafts have been performed, with no reported disease transmissions. 10 Outcomes associated with colporrhaphy plus arcus-to-arcus graft (Repliform) versus colporrhaphy without graft were compared in 84 patients. In the resolution of grades 3 and 4 cystoceles, the results revealed that a 78% reduction of recurrence was associated with the use of graft materials at 12 weeks. Recurrence rates in patients who received grafts were 5% in patients vs FIGURE 2 Polyform TM mesh Important mesh characteristics include softness, pliability, and macropore construction. 14% in those who received colporrhaphy alone. Equally, if not more important, not a single adverse outcome, erosion, graft exposure, or explant has been associated with the use of Repliform graft augmentation in our cohort to date. No patient reactions to the grafts were seen. 11 Currently, a prospective, randomized controlled trial of Repliform augmentation versus traditional colporrhaphy is being conducted at our center in Evanston, Illinois. Other outcomes data from small short-term, uncontrolled studies demonstrate that posterior allograft repairs are safe and well tolerated and thus represent a promising alternative to colporrhaphy. 12,13 Oster and colleagues reported a subjective success rate in all 15 patients treated with a dermal allograft; 13% of patients, however, experienced de novo dyspareunia. Kohli and Miklos 14 reported that after site-specific repairs, a dermal allograft was associated with anatomic fixation and permanent sutures. For the 30 or 43 women available for follow-up, a 93% objective cure rate was reported. Use of xenografts in pelvic repair These products, harvested from porcine or bovine sources, provide minimal risk for erosion or rejection. The bovine model featured in Xenform TM (Boston Scientific Corporation, Natick, Mass), for example, consists of regenerative tissue matrix derived from a fetal cow that remodels easily into new, native tissues. It consists of a non-denatured, non-crosslinked collagen matrix scaf- January 2006 Supplement to OBG Management S5
6 Augmenting pelvic floor repairs New materials and techniques TABLE 2 Polyform vs Gynemesh : Technical Comparison Within key criteria, compared with Gynemesh PS Mesh, Polyform Mesh is: 40% softer (reduction in rigidity/stiffness) 55% thinner (reduction in thickness) 35% smoother (reduction in coefficient of friction) 20% lighter (reduction in basis weight) 3x greater stretch (blended reduction in force V displacement) CHARACTERISTIC POLYFORM MESH GYNEMESH PS Composition Monofilament, Polypropylene Monofilament, Polypropylene Pore Size (microns) Macroporous 1450 Macroporous 2500 Fiber Diameter (microns) Basis Weight (g/m 2 ) Thickness (microns) Coefficient of Friction (u 2 ) Flexural Rigidity/Stiffness (F max N) Ball Burst F max N) Elongation Machine F max N) Elongation Transverse F max N) Size 10 cm x 15 cm 10 cm x 15 cm Data on file. Boston Scientific Corporation. fold. Because this product is not cross-linked, it likely retains important biologic information that aids in the regenerative process. The intrinsic collagen biologic information is not interrupted. The product, as do others in this class, offers biocompatibility as required under FDA guidelines to ensure biocompatibility with the host. Xenograft materials are processed with effective viral and prion inactivation steps, eliminating the risk for bovine disease transmission. They are available in a wide range of sizes with uniform thickness, providing consistency of graft materials and ensuring that the graft will conform to the site. Material is packaged dry and achieves hydration in a room-temperature saline solution in less than 1 minute. Preparation and packaging provides consistency in terms of hydration, long shelf-life, and ease of use. Techniques are discussed in ONE SURGEON S TECHNIQUE: USE OF XENOGRAFT MATERIALS, PAGE 8. The repair process has been well documented. In pre-clinical and clinical reviews using a rodent softtissue repair model with Xenform, the regenerative tissue matrix has been shown to be populated by host cells and vessels in as little as 3 weeks following the procedure. Within 9 months, the graft has been remodeled into strong host connective tissue and the graft cannot be distinguished from host tissue. At 15 months, there was no evidence of an elicited foreign body response, no surgical adhesions, and no herniation. 15 Thus, a key benefit of using this modality is the reduced risk of erosion or encapsulation. A 1-year prospective, case-controlled trial is in process and nearing completion to evaluate sexual function and pelvic floor distress in women who have been treated with Xenform. The trial also will assess anatomic outcomes. Conclusions Mesh or graft augmentation offers an important resource for surgeons who strive to restore normal pelvic function to their patients. New products and technical advances offer important options with promising initial outcomes. Surgeons interested in these newer techniques should consider the safety and efficacy of the specific graft/mesh material being implanted, as well as the delivery system. The Capio anchoring technique described in this monograph requires a smaller amount of dissection than that of a traditional repair, eliminating the unique risks associated with blind trocar insertion. Currently, large, randomized, prospective, case-controlled clinical trials are underway to assess outcomes associated with currently available products. S6 Supplement to OBG Management January 2006
7 OBG MANAGEMENT One surgeon s technique: Use of synthetic materials We need to remember that the vagina is a dynamic organ and needs to stretch with sexual activity. Bioengineered mesh materials can provide that degree of flexibility. Pore size is an issue, so I select a product that, over time, will allow tissue in-growth and hold the mesh in place. Additionally, I choose the smoothest, thinnest product available. In my mesh repairs, I use the Capio device and make a transverse or midline incision and dissect underneath, using a very small level of dissection to reduce the amount of incision exposed to the mesh. For anterior repairs, I use a 4-point attachment, with sutures at the apex (sacrospinous ligament, arcus tendineus, or coccygeus muscle) and pubourethral ligament (for anterior support) or perineal body (for posterior support). I like to attach the mesh to the vaginal apex using a suspension suture. That will fix the vaginal apex underneath the mesh, provide apical support, prevent enterocele formation, and allow me to code for a vaginal vault suspension. I cut the mesh to size, depending on the specific attachment points required for the individual patient. If I attach the mesh at the arcus or coccygeus, I use a 12-cm piece (not a 10-cm piece) to avoid tension. I use an 8-mm to 10-mm piece for an attachment to the sacrospinous ligament, stopping short of the bladder neck. We have done numerous total vaginal mesh reconstructions using a piece of mesh 15 cm in length, with a 9-cm extension posteriorly and a 6-cm extension. I avoid placing small pieces of mesh that may not extend into important areas. The procedure can be combined with other procedures, such as suburethral slings. Neeraj Kohli, MD, MBA One surgeon s technique: Use of allograft materials Iuse Repliform for the majority of my graft augmentations at this time, primarily because these grafts have been associated with no adverse patient reactions, while offering promising results to date. Thus, in my view, these procedures conform to the first do no harm mandate under which we all need to practice, as we seek to eventually determine the overall best material and technique through well-designed studies. I am concerned about the permanence of mesh materials: Traditionally, they have been associated with a risk for erosion. Will mesh contract over time? Or are the traditional rates of erosion associated with surgeon technique, ie, suturing too tightly? What is the risk for dyspareunia? In assessing outcomes, I am particularly interested in safety and tolerability, in addition to effectiveness. When counseling patients, I always think: is this something I would recommend to my mother? I want to feel completely comfortable with the recommendations I make to my patients, a challenge when I know that, in terms of these materials, we do not have all the answers. With respect to technique for anterior repairs, I prefer a 6-point suspension to the arcus tendineus and underlying obturator internus muscle, spanning from pubic tubercle to ischial spine. This arcus-to-arcus graft addresses both central (distension) and paravaginal (detachment) aspects of a cystocele. The graft supports the entire bladder along its original anatomically correct attachment points. I use a standard midline dissection, about 1 cm to 2 cm to the east and west from our normal lateral boundaries of cystocele dissection. I do not rely on being able to see or feel the arcus, although we find that it is clearly visible and/or palpable about 50% of the time. Whether this connective tissue remnant is present or not, I am confident in placing my sutures because I know that the appropriate span of obturator internus muscle is located between the tubercle and ischial spine. I use a Capio device, which allows me to fixate rather than blindly perforate the pelvic floor muscles. In my view, the addition of trocar perforations and stray mesh arms introduce unnecessary risk, with no proven benefit at this stage. The Capio s placement, very close to the sacrospinous, makes it easy to do a concurrent vault suspension, if indicated. For suturing, I prefer to use a Gore-Tex #0; I like its feel and find it easy to work with, although no data suggest that any 1 suture material is superior to another. The Repliform graft is trimmed into a trapezoid shape, 9 cm across at the apex, tapering down to 4 cm. I use a free needle to place the suture ends at appropriate positions along the graft. The Repliform graft will be placed somewhat more tautly than will a synthetic, as no significant scarring or contraction appears to occur, and also because putting the graft on stretch helps to stimulate native tissue growth. Thus, unlike the desired loose appearance of a polypropylene mesh insert at the time of closure, the Repliform allograft should have no excessive laxity, but rather should look like a firm, supported sheet. Roger Goldberg, MD, MPH January 2006 Supplement to OBG Management S7
8 Augmenting pelvic floor repairs New materials and techniques One surgeon s technique: Use of xenograft materials As a new product, Xenform provides many of the benefits of products already in the marketplace. However, as is true of all developments in graft/mesh technology, new products have been developed to create materials that are best suited to use in gynecologic surgery. In any graft material, I look for softness and pliability, which aid in restoration of vaginal form and function. I compare the feel of products: some have a stiff, leathery feel. I am concerned that this will translate into lack of flexibility in the vaginal wall, which could result in lessthan-ideal function. I want a product that encourages cellular in-growth, and reduces the likelihood of encapsulation. I am concerned that chemically crosslinked products may reduce in-growth and negatively affect a patient s return to normal sexual function. In follow-up examinations of repairs made with more rigid products, the surgeon may notice a ridge in the midto-upper vagina, where it should be softer and more pliable. I believe that the rate of incorporation of the collagen matrix into the native tissue reduces the risk for wound separation and allows healing of the suture line, the most common site of erosions. In using Xenform, it is important to hydrate with room-temperature saline: use of hot liquid will denature the collagen. Our anterior repair technique utilizes an 8 cm x 12 cm piece of Xenform, which is fashioned into a trapezoidal shape that is 12 cm at the base and 7 cm at the apex. The open-access Capio needle passer is loaded with 2-0 Gore-Tex suture and aided by Miyazaki lighted vaginal retractors (Marina Medical, Hollywood, Fla). Four sutures are placed into each arcus from ischial spine to just behind the pubis.this is done under direct vision.the graft edges then are attached to these sutures, and the graft tied into position. Any central defect can be corrected by placation if desired prior to this step, or it simply can be ignored, as usually is our custom. The graft is anchored in the midline, at the level of the bladder base, with 2 interrupted delayed absorbable sutures to help with enterocele prophylaxis. Posteriorly, in an effort to protect the vault, we use a graft as well. Again, the approach begins like a standard posterior repair, but dissection continues to both sacrospinous ligaments. The Capio device, again with Gore-Tex suture, is passed twice into each ligament. An 8 cm x 12 cm graft,12 cm across and 8 cm front to back, is attached to the medial of the 2 sutures. Two delayed absorbable sutures are placed into the midline of the graft at the uppermost/innermost edge, and attached into the vaginal epithelium, again to help prevent enterocele. Site-specific defects may be corrected at this time, if desired. Often no usable tissue is found. The graft is tied in place, and secured laterally and anteriorly (to levator fascia and perineal body) with a running delayed absorbable suture. The remaining sacrospinous sutures are attached to the vaginal vault to complete a bilateral vault suspension. (A procedural video is available from the American College of Obstetricians and Gynecologists video library.) Joseph Maccarone, MD References 1. Olsen AL, Smith VJ, Bergstrom JO, et al. Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol. 1997;89: Weber AM, Walters MD, Piedmonte MR, et al. Anterior colporrhaphy: a randomized trial of three surgical techniques. Am J Obstet Gynecol. 2001;185: Kohli N, Sze EHM, Roat TW, et al. Incidence of recurrent cystocele after anterior colporrhaphy with and without concomitant transvaginal needle suspension. Am J Obstet Gynecol. 1996;175: Sand PK, Koduri S, Lobel RW, et al. Prospective, randomized trial of polyglactin 910 mesh to prevent recurrence of cystoceles and rectoceles. Am J Obstet Gynecol. 2001;184: Watson SJ, Loder PB, Halligan S, et al. Transperineal repair of symptomatic rectocele with Marlex mesh: a clinical, physiological and radiologic assessment of treatment. J Am Coll Surg. 1996;183: Dwyer PL, O Reilly BA. Transvaginal repair of anterior and posterior compartment prolapse with Atrium polypropylene mesh. BJOG. 2004;111: Salvatore S, Soligo M, Meschia M, et al. Prosthetic surgery for genital prolapse: functional outcome. Paper presented at: International Continence Society Congress; 2002; Heidelberg, Germany. Abstract Mercer-Jones MA, Sprowson A, Varma JS. Outcome after transperineal mesh repair of rectocele: a case series. Dis Colon Rectum. 2004;47: Data on file. GYNECARE WORLDWIDE, Somerville, NJ. 10. Data on file. LifeCell Corporation, Branchburg, NJ. 11. Batros S, Goldberg ERP. Adjuvant dermal graft for advanced anterior compartment prolapse: Comparison to standard anterior colporrhaphy. American Urologynecologic Society Annual Meeting. Atlanta, Georgia. International Urogynecology Society 30th Annual Meeting Copenhagen, Denmark. 12. Oster S, Astrup A. A new vaginal operation for recurrent and large rectocele using dermis transplant. Acta Obstet Gynecol Scand. 1981;60: Abramov Y, Gandhi S, Goldberg RP, et al. Site-specific rectocele repair compared with standard posterior colporrhaphy. Obstet Gynecol. 2005;105: Kohli N, Miklos JR. Dermal graft-augmented rectocele repair. Int Urogynecol J Pelvic Floor Dysfunct. 2003;14: Data on file. Boston Scientific Corporation, Natick, Mass. S8 Supplement to OBG Management January 2006 RVU2400
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
ig. 2. The organs and their outlet tubes.
 Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
Women s Health. Product innovation. Commitment. We are committed to you... and advancing the quality of your patient care.
 II Commitment We are committed to you... and advancing the quality of your patient care. Boston Scientific is always there for you, your physicians and your patients. We are anchored in our guiding principle
II Commitment We are committed to you... and advancing the quality of your patient care. Boston Scientific is always there for you, your physicians and your patients. We are anchored in our guiding principle
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation
 Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Anterior vaginal wall prolapse occurs commonly
 Anterior vaginal wall prolapse: Innovative surgical approaches MARK D. WALTERS, MD, AND MARIE FIDELA R. PARAISO, MD Anterior vaginal wall prolapse occurs commonly and may coexist with disorders of micturition.
Anterior vaginal wall prolapse: Innovative surgical approaches MARK D. WALTERS, MD, AND MARIE FIDELA R. PARAISO, MD Anterior vaginal wall prolapse occurs commonly and may coexist with disorders of micturition.
Prolapse & Stress Incontinence
 Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
Bard: Continence Therapy. Stress Urinary Incontinence. Regaining Control. Restoring Your Lifestyle.
 Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Desara TV and Desara Blue TV
 Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
ORIENTING TO BISECTED SPECIMENS ON THE PELVIS PRACTICAL
 ORIENTING TO BISECTED SPECIMENS ON THE PELVIS PRACTICAL The Pelvis is just about as complicated as head and neck and considerably more mysterious. You have to be able to visualize (imagine) the underlying
ORIENTING TO BISECTED SPECIMENS ON THE PELVIS PRACTICAL The Pelvis is just about as complicated as head and neck and considerably more mysterious. You have to be able to visualize (imagine) the underlying
Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience with Prolift Mesh in 84 Women with Complicated Pelvic Prolapses
 Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Pelvic Floor. Reimbursement & Coding Guide
 Pelvic Floor Reimbursement & Coding Guide Pelvic Floor Reimbursement and Coding Guide ACell Pelvic Floor Matrix products are biologically-derived devices comprised of porcine Urinary Bladder Matrix (UBM),
Pelvic Floor Reimbursement & Coding Guide Pelvic Floor Reimbursement and Coding Guide ACell Pelvic Floor Matrix products are biologically-derived devices comprised of porcine Urinary Bladder Matrix (UBM),
Strength and Predictability. Zimmer Collagen Repair Patch
 Strength and Predictability Zimmer Collagen Repair Patch Durable Reinforcement The Zimmer Collagen Repair Patch is a biological implant consisting of an acellular scaffold of collagen and elastin, derived
Strength and Predictability Zimmer Collagen Repair Patch Durable Reinforcement The Zimmer Collagen Repair Patch is a biological implant consisting of an acellular scaffold of collagen and elastin, derived
TissueMend. Arthroscopic Surgical Technique. Arthroscopic Insertion of a Biologic Rotator Cuff Tissue Augment After Rotator Cuff Repair
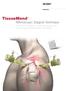 TissueMend Arthroscopic Surgical Technique Arthroscopic Insertion of a Biologic Rotator Cuff Tissue Augment After Rotator Cuff Repair Table of Contents Placement of suture anchors Placement of anteromedial
TissueMend Arthroscopic Surgical Technique Arthroscopic Insertion of a Biologic Rotator Cuff Tissue Augment After Rotator Cuff Repair Table of Contents Placement of suture anchors Placement of anteromedial
Titanised mesh implants for urogynaecology Transvaginal multi-arm meshes Incontinence tapes Instruments Laparoscopic meshes
 Quality and Experience Titanised mesh implants for urogynaecology Transvaginal multi-arm meshes Incontinence tapes Instruments Laparoscopic meshes www.pfmmedical.com 1 Titanised Mesh Implants for Urogynaecology
Quality and Experience Titanised mesh implants for urogynaecology Transvaginal multi-arm meshes Incontinence tapes Instruments Laparoscopic meshes www.pfmmedical.com 1 Titanised Mesh Implants for Urogynaecology
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
II.- PLUG. NAME of the products. Premilene Mesh Plug MANUFACTURER. B Braun DESCRIPTION. Polypropylene mesh for plug technique
 II.- PLUG Premilene Mesh Plug B Braun Polypropylene mesh for plug technique Premilene Mesh Plug is a monofilament polypropylene mesh plug designed for the repair of recurrent hernias and can also be used
II.- PLUG Premilene Mesh Plug B Braun Polypropylene mesh for plug technique Premilene Mesh Plug is a monofilament polypropylene mesh plug designed for the repair of recurrent hernias and can also be used
Strattice Reconstructive Tissue Matrix used in the repair of rippling
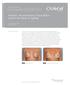 Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Ventralex ST Hernia Patch featuring Sepra Technology
 Ventralex ST Hernia Patch featuring Sepra Technology Proven Sepra Technology in a Low Profile, Lightweight Mesh Sepra Technology An extensively studied barrier with more than 10 publications and used clinically
Ventralex ST Hernia Patch featuring Sepra Technology Proven Sepra Technology in a Low Profile, Lightweight Mesh Sepra Technology An extensively studied barrier with more than 10 publications and used clinically
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
Urethrolysis; When, Why & How. M Karram Professor of Ob/Gyn & Urology University of Cincinnati
 Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander.
 Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Technique Guide. Bard MK Hernia Repair. Featuring Modified Onflex Mesh SOFT TISSUE REPAIR. Anterior Approach to a Preperitoneal Inguinal Hernia Repair
 Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
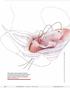 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
Introduction. Regarding the Section of the UPDATE Entitled Purpose
 Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy
 Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
CorMatrix ECM Bioscaffold
 CorMatrix ECM Bioscaffold REMODEL. REGROW. RESTORE. CorMatrix ECM Bioscaffold provides a natural bioscaffold matrix that enables the body s own cells to repair and remodel damaged cardio-vascular tissue.
CorMatrix ECM Bioscaffold REMODEL. REGROW. RESTORE. CorMatrix ECM Bioscaffold provides a natural bioscaffold matrix that enables the body s own cells to repair and remodel damaged cardio-vascular tissue.
Desara and Desara Blue
 Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Uphold LITE Vaginal Support System 2015 Coding & Quick Reference Guide
 Hospital Outpatient Coding Scenarios This guide contains specific information for two (2) common coding/reimbursement scenarios related to the use of the Uphold LITE Vaginal Support System when performed
Hospital Outpatient Coding Scenarios This guide contains specific information for two (2) common coding/reimbursement scenarios related to the use of the Uphold LITE Vaginal Support System when performed
High risk of complications with a single incision pelvic floor repair kit: results of a retrospective case series
 Int Urogynecol J (2014) 25:109 116 DOI 10.1007/s00192-013-2156-1 ORIGINAL ARTICLE High risk of complications with a single incision pelvic floor repair kit: results of a retrospective case series Stephen
Int Urogynecol J (2014) 25:109 116 DOI 10.1007/s00192-013-2156-1 ORIGINAL ARTICLE High risk of complications with a single incision pelvic floor repair kit: results of a retrospective case series Stephen
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
Management of Vaginal Prolapse
 Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
INSTRUCTIONS FOR USE FOR:
 INSTRUCTIONS FOR USE FOR: en English INSTRUCTIONS FOR USE GORE ENFORM PREPERITONEAL BIOMATERIAL Carefully read all instructions prior to use. Observe all instructions, warnings, and precautions noted throughout.
INSTRUCTIONS FOR USE FOR: en English INSTRUCTIONS FOR USE GORE ENFORM PREPERITONEAL BIOMATERIAL Carefully read all instructions prior to use. Observe all instructions, warnings, and precautions noted throughout.
q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE
 493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics.
 NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics. Anatomy above the arcuate line Skin Camper s fascia Scarpa s fascia External oblique
NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics. Anatomy above the arcuate line Skin Camper s fascia Scarpa s fascia External oblique
Tension Free Monofilament Macropore Polypropylene Mesh (Gynemesh PS) in Female Genital Prolapse Repair
 Clinical Urology Gynemesh PS in Female Genital Prolapse Repair International Braz J Urol Vol. 32 (4): 410-415, July - August, 2006 Tension Free Monofilament Macropore Polypropylene Mesh (Gynemesh PS) in
Clinical Urology Gynemesh PS in Female Genital Prolapse Repair International Braz J Urol Vol. 32 (4): 410-415, July - August, 2006 Tension Free Monofilament Macropore Polypropylene Mesh (Gynemesh PS) in
INJ. Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple Sutures: Surgical Technique and Results.
 Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
ROBOTIC MESH SACROCOLPOPEXY
 ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
9/24/2015. Pelvic Floor Disorders. Agenda. What is the Pelvic Floor? Pelvic Floor Problems
 Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Dana Alrafaiah. - Amani Nofal. - Ahmad Alsalman. 1 P a g e
 - 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
- 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
A wide variety of membrane options
 A wide variety of membrane options BOVINE Bovine collagen membrane Neomem is a resorbable collagen membrane derived from highly purified type I collagen fibres from bovine Achilles tendon. The macromolecular
A wide variety of membrane options BOVINE Bovine collagen membrane Neomem is a resorbable collagen membrane derived from highly purified type I collagen fibres from bovine Achilles tendon. The macromolecular
THE USE OF PROSTHESES IN PELVIC RECONSTRUCTIVE SURGERY: JOY OR TOY?
 REVIEW ARTICLE THE USE OF PROSTHESES IN PELVIC RECONSTRUCTIVE SURGERY: JOY OR TOY? Ming-Ping Wu 1,2 * 1 Division of Urogynecology and Pelvic Floor Reconstruction, Department of Obstetrics and Gynecology,
REVIEW ARTICLE THE USE OF PROSTHESES IN PELVIC RECONSTRUCTIVE SURGERY: JOY OR TOY? Ming-Ping Wu 1,2 * 1 Division of Urogynecology and Pelvic Floor Reconstruction, Department of Obstetrics and Gynecology,
New Insights in the Surgical Management of Stress Urinary Incontinence in Women
 New Insights in the Surgical Management of Stress Urinary Incontinence in Women Gabriel Gillon MD Dept. of Urology Rabin Med. Cent. /Beilinson Incontinence and LUTS 25/6/2009 Symposium Ramat Aviv New Insights
New Insights in the Surgical Management of Stress Urinary Incontinence in Women Gabriel Gillon MD Dept. of Urology Rabin Med. Cent. /Beilinson Incontinence and LUTS 25/6/2009 Symposium Ramat Aviv New Insights
Imaging of Pelvic Floor Weakness. Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne
 Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Recent advances in POP. Dr. Bernhard Uhl Department for Obstetrics and Gynecology St. Vinzenz-Hospital Dinslaken Germany
 Recent advances in POP Dr. Bernhard Uhl Department for Obstetrics and Gynecology St. Vinzenz-Hospital Dinslaken Germany Level of pelvic floor support Level I apical Level II transverse/ horizontal Level
Recent advances in POP Dr. Bernhard Uhl Department for Obstetrics and Gynecology St. Vinzenz-Hospital Dinslaken Germany Level of pelvic floor support Level I apical Level II transverse/ horizontal Level
Figure 13 1 Technique of anterior repair with plication of the pubocervical fascia for cystocele repair.
 Figure 13 1 Technique of anterior repair with plication of the pubocervical fascia for cystocele repair. Figure 13 2 Technique of posterior repair with plication of the recto-vaginal fascia for rectocele
Figure 13 1 Technique of anterior repair with plication of the pubocervical fascia for cystocele repair. Figure 13 2 Technique of posterior repair with plication of the recto-vaginal fascia for rectocele
Pelvic Organ Prolapse. Natural Solutions
 Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
NOTICE OF FILING. Details of Filing. Kathryn Gill & Ors v Ethicon Sarl & Ors NEW SOUTH WALES REGISTRY - FEDERAL COURT OF AUSTRALIA
 NOTICE OF FILING This document was lodged electronically in the FEDERAL COURT OF AUSTRALIA (FCA) on 13/04/2018 3:35:30 PM AEST and has been accepted for filing under the Court s Rules. Details of filing
NOTICE OF FILING This document was lodged electronically in the FEDERAL COURT OF AUSTRALIA (FCA) on 13/04/2018 3:35:30 PM AEST and has been accepted for filing under the Court s Rules. Details of filing
Thesis. Reference. To mesh or not to mesh: a review of pelvic organ reconstructive surgery. DAELLENBACH, Patrick Peter
 Thesis To mesh or not to mesh: a review of pelvic organ reconstructive surgery DAELLENBACH, Patrick Peter Abstract Pelvic organ prolapse (POP) is a major health issue with a lifetime risk of undergoing
Thesis To mesh or not to mesh: a review of pelvic organ reconstructive surgery DAELLENBACH, Patrick Peter Abstract Pelvic organ prolapse (POP) is a major health issue with a lifetime risk of undergoing
Gökmen Sukgen, 1 Esra SaygJlJ YJlmaz, 2 and Eralp BaGer Introduction. 2. Case Presentation
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Meshes. Meshes. Non-absorbable meshes. Absorbable meshes
 Meshes Meshes Non-absorbable meshes Absorbable meshes Non-absorbable meshes hernia Premilene Mesh Premilene Mesh Plug Optilene Mesh Optilene Mesh LP Optilene Mesh Elastic Omyra Mesh Non-absorbable meshes
Meshes Meshes Non-absorbable meshes Absorbable meshes Non-absorbable meshes hernia Premilene Mesh Premilene Mesh Plug Optilene Mesh Optilene Mesh LP Optilene Mesh Elastic Omyra Mesh Non-absorbable meshes
One Slim Needle One Incision. One Simple Solution for Stress Urinary Incontinence. The Difference is in the Data
 CONTINENCE SOLUTIONS One Slim Needle One Incision ordering information Description US International Order Number Order Number One Simple Solution for Stress Urinary Incontinence MiniArc Single-Incision
CONTINENCE SOLUTIONS One Slim Needle One Incision ordering information Description US International Order Number Order Number One Simple Solution for Stress Urinary Incontinence MiniArc Single-Incision
Desara Blue OV D I. Sling for Female Stress Urinary Incontinence. Instructions For Use
 Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments?
 Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Le fort s operation for prolapse uterus: A forgotten procedure
 2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Surgical Procedures for Treatment of Pelvic Organ Prolapse in Women PATIENT INFORMATION LEAFLET
 Patient Label Surgical Procedures for Treatment of Pelvic Organ Prolapse in Women PATIENT INFORMATION LEAFLET 1 About this leaflet: This leaflet gives you detailed information about the operations being
Patient Label Surgical Procedures for Treatment of Pelvic Organ Prolapse in Women PATIENT INFORMATION LEAFLET 1 About this leaflet: This leaflet gives you detailed information about the operations being
Positioning System. Laparoscopic ventral hernia repair KEY BENEFITS SOFT TISSUE REPAIR
 Echo PS Positioning System with Ventralight ST Mesh or Composix L/P Mesh Laparoscopic ventral hernia repair Echo PS Positioning System with Ventralight ST Mesh Echo PS Positioning System with Composix
Echo PS Positioning System with Ventralight ST Mesh or Composix L/P Mesh Laparoscopic ventral hernia repair Echo PS Positioning System with Ventralight ST Mesh Echo PS Positioning System with Composix
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May Dr. Annie Leong MBBS, FRANZCOG, CU
 EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
New Directions in Restoration of Pelvic Structure and Function
 2 New Directions in Restoration of Pelvic Structure and Function Peter E. Petros and Bernhard Liedl The fundamental theme of this chapter is that structure and function are intimately related. Abnormal
2 New Directions in Restoration of Pelvic Structure and Function Peter E. Petros and Bernhard Liedl The fundamental theme of this chapter is that structure and function are intimately related. Abnormal
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
SACROSPINOUS LIGAMENT FIXATION, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE
 Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Table 2. First Generated List of Expert Responses. Likert-Type Scale. Category or Criterion. Rationale or Comments (1) (2) (3) (4)
 Table 2. First Generated List of Expert Responses. Likert-Type Scale Category or Criterion Anatomical Structures and Features Skeletal Structures and Features (1) (2) (3) (4) Rationale or Comments 1. Bones
Table 2. First Generated List of Expert Responses. Likert-Type Scale Category or Criterion Anatomical Structures and Features Skeletal Structures and Features (1) (2) (3) (4) Rationale or Comments 1. Bones
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
I. Permission to publish. II. Offprint order. III. Copyright Transfer Statement (sign only if not submitted previously) Dear Beate Gärtner,
 Fax to: +49622148768905 Beate Gärtner Springer Heidelberg, 69121 Heidelberg From: Re: Authors: International Urogynecology Journal DOI 10.1007/s00192-004-1264-3 Translevator posterior intravaginal slingplasty:
Fax to: +49622148768905 Beate Gärtner Springer Heidelberg, 69121 Heidelberg From: Re: Authors: International Urogynecology Journal DOI 10.1007/s00192-004-1264-3 Translevator posterior intravaginal slingplasty:
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Tian-Ni Kuo 1, Ming-Ping Wu 1,2 *
 RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
Elevate Anterior/Apical: 12-Month Data Showing Safety and Efficacy in Surgical Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Elevate Anterior/Apical: 12-Month Data Showing Safety and Efficacy in Surgical Treatment of Pelvic Organ Prolapse Edward J. Stanford, MD, MS,* Robert D. Moore, DO,Þ Jan-Paul W.R. Roovers,
ORIGINAL ARTICLE Elevate Anterior/Apical: 12-Month Data Showing Safety and Efficacy in Surgical Treatment of Pelvic Organ Prolapse Edward J. Stanford, MD, MS,* Robert D. Moore, DO,Þ Jan-Paul W.R. Roovers,
Case Report. XCM Biologic Tissue Matrix. Components separation using sandwich technique for reconstruction of abdominal wall defect.
 Case Report XCM Biologic Tissue Matrix. Components separation using sandwich technique for reconstruction of abdominal wall defect. XCM Biologic Tissue Matrix. Components separation using sandwich technique
Case Report XCM Biologic Tissue Matrix. Components separation using sandwich technique for reconstruction of abdominal wall defect. XCM Biologic Tissue Matrix. Components separation using sandwich technique
OptiFix Absorbable Fixation System
 OptiFix Absorbable Fixation System Absorbable Fixation Redefined Advancing the Fixation Experience. SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. Hernia Repair Fixation Challenges and
OptiFix Absorbable Fixation System Absorbable Fixation Redefined Advancing the Fixation Experience. SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. Hernia Repair Fixation Challenges and
Lyoplant Onlay. Adding another layer of confidence to every procedure. Aesculap Neurosurgery
 Adding another layer of confidence to every procedure Aesculap Neurosurgery Adding another layer of confidence to every procedure For more than 140 years, Aesculap Neurosurgery has developed products that
Adding another layer of confidence to every procedure Aesculap Neurosurgery Adding another layer of confidence to every procedure For more than 140 years, Aesculap Neurosurgery has developed products that
Pelvic Health Coding & Payment Quick Reference
 Payer policies will vary and should be verified prior to treatment for limitations on diagnosis, coding or site of service requirements. The coding options listed within this guide are commonly used codes
Payer policies will vary and should be verified prior to treatment for limitations on diagnosis, coding or site of service requirements. The coding options listed within this guide are commonly used codes
Pelvic Organ Prolapse: Diagnosis, Treatment, and Avoiding Complications
 Pelvic Organ Prolapse: Diagnosis, Treatment, and Avoiding Complications Christina Dancz and Morgan Fullerton Contents 1 Introduction... 2 2 Anatomy/Pathophysiology... 2 2.1 Level 1: The Cardinal and Uterosacral
Pelvic Organ Prolapse: Diagnosis, Treatment, and Avoiding Complications Christina Dancz and Morgan Fullerton Contents 1 Introduction... 2 2 Anatomy/Pathophysiology... 2 2.1 Level 1: The Cardinal and Uterosacral
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
