I. Permission to publish. II. Offprint order. III. Copyright Transfer Statement (sign only if not submitted previously) Dear Beate Gärtner,
|
|
|
- Bernice Glenn
- 6 years ago
- Views:
Transcription
1 Fax to: Beate Gärtner Springer Heidelberg, Heidelberg From: Re: Authors: International Urogynecology Journal DOI /s Translevator posterior intravaginal slingplasty: anatomical landmarks and safety margins Smajda Vanormelingen Vandewalle Ombelet Jonge Hinoul I. Permission to publish Dear Beate Gärtner, I have checked the proofs of my article and I have no corrections. The article is ready to be published without changes. I have a few corrections. I am enclosing the following pages: I have made many corrections. Enclosed is the complete article. II. Offprint order Offprint order enclosed Remarks: Date / signature I do not wish to order offprints III. Copyright Transfer Statement (sign only if not submitted previously) The copyright to this article is transferred to International Urogynecology Journal (for U.S. government employees: to the extent transferable) effective if and when the article is accepted for publication. The author warrants that his/her contribution is original and that he/she has full power to make this grant. The author signs for and accepts responsibility for releasing this material on behalf of any and all co-authors. The copyright transfer covers the exclusive right to reproduce and distribute the article, including reprints, translations, photographic reproductions, microform, electronic form (offline, online) or any other reproductions of similar nature. An author may self-archive an author-created version of his/her article on his/her own website and his/her institution s repository, including his/her final version; however he/she may not use the publisher s PDF version which is posted on Furthermore, the author may only post his/her version provided acknowledgement is given to the original source of publication and a link is inserted to the published article on Springer s website. The link must be accompanied by the following text: The original publication is available at The author is requested to use the appropriate DOI for the article (go to the Linking Options in the article, then to OpenURL and use the link with the DOI). Articles disseminated via are indexed, abstracted and referenced by many abstracting and information services, bibliographic networks, subscription agencies, library networks, and consortia. After submission of this agreement signed by the corresponding author, changes of authorship or in the order of the authors listed will not be accepted by Springer. Date / Author s signature
2 Journal: International Urogynecology Journal DOI: /s Offprint Order Form To determine if your journal provides free offprints, If you do not return this order form, we assume that please check the journal s instructions to authors. you do not wish to order offprints. You are entitled to a PDF file if you order offprints. If you order offprints after the issue has gone to press, Please checkmark where to send the PDF file: costs are much higher. Therefore, we can supply offprints only in quantities of 300 or more after this dr_smajda@hotmail.com time. For orders involving more than 500 copies, please ask the production editor for a quotation. Please note that orders will be processed only if a credit card number has been provided. Please enter my order for: Copies Price Prices include surface mail postage and handling. Customers in EU countries who are not registered for VAT should add VAT at the rate applicable in their country. VAT registration number (EU countries only): Please charge my credit card Eurocard/Access/Mastercard American Express Visa/Barclaycard/Americard Number (incl. check digits): _ Valid until: / Date / Signature: Send receipt to: Stefan Smajda Clinique Sainte Anne-Saint Rémi Dept. Obstetrics and Gynaecology 66 Bd. Graindor Brussels 1070, Belgium Ship offprints to: Stefan Smajda Clinique Sainte Anne-Saint Rémi Dept. Obstetrics and Gynaecology 66 Bd. Graindor Brussels 1070, Belgium
3 International Urogynecology Journal DOI /s Original Article Translevator posterior intravaginal slingplasty: anatomical landmarks and safety margins Stefan Smajda ( ) Linda Vanormelingen Giovanni Vandewalle Willem Ombelet Eric de Jonge Piet Hinoul S. Smajda Department of Obstetrics and Gynaecology, Clinique Sainte Anne Saint Rémi, Bd. Graindor 66, 1070 Brussels, Belgium W. Ombelet E. Jonge P. Hinoul Department of Obstetrics and Gynaecology, Ziekenhuis Oost-Limburg, 3600 Genk, Belgium L. Vanormelingen G. Vandewalle Department of Human Anatomy, Limburgs Universitair Centrum (L.U.C.), 3590 Diepenbeek, Belgium S. Smajda Phone: Fax: dr_smajda@hotmail.com Received: 20 July 2004 / Accepted: 14 November 2004 Abstract The posterior intravaginal sling is a new tension-free needle suspension technique. It is used for the treatment of middle compartment (vaginal vault or uterine) prolapse. The Prolene sling suspends the vagina at the upper border of level II support as described by DeLancey (Am J Obstet Gynecol 166:1717, 1992). Human cadaveric dissections were undertaken to explore the pertinent anatomy that is involved when using this blind needle technique. Pre-dissected cadaveric material was used to obtain didactic illustrations of the anatomy of the procedure. Description of the surgical technique using anatomical landmarks and relative distances of the needle to these landmarks will improve the surgeon s visual understanding of the procedure. The measurements obtained demonstrate that the needle stays at a minimal distance of 4 cm away from the major (pudendal) vessels that could potentially cause life-threatening haemorrhage. Keywords Anatomy Infracoccygeal sacropexy Vaginal vault prolapse 1
4 Stefan Smajda and Piet Hinoul contributed equally to this paper Introduction Midurethral needle suspensions used for the treatment of urodynamic stress incontinence have raised interest in the use of meshes and other needle suspensions in the treatment of female incontinence and urogenital prolapse. The infracoccygeal sacropexy was first described by Petros in 2001 [1]. The posterior intravaginal sling (IVS Tunneller, Tyco Healthcare, Norwalk, Conn., USA) tries to offer a minimally invasive procedure such as sacrospinous ligament fixation or sacrocolpopexy for the correction of apical vaginal prolapse. Cadaveric dissections were undertaken to improve comprehension of the anatomy involved in performing a posterior IVS procedure. Materials and methods Dissections and surgical procedures were performed on a total of nine embalmed whole female cadavers (3% formaldehyde) at the Department of Human Anatomy of the University of Limburg, Belgium. Initially the technique was performed on three embalmed cadavers. The IVS suspension needle that is used during a posterior IVS procedure was inserted prior to anatomical dissection for surgical landmarks. This method, however, did not achieve optimal quality illustrations of the anatomy of the procedure. Therefore, we decided to use pre-dissected specimens. The IVS suspension needle was inserted in six of these pre-dissected specimens in a similar way. No differences in the anatomy under consideration could be observed between the left and right hemipelves. The anatomical dissections were performed by anatomists on instructions of gynaecologists experienced with the posterior IVS with regard to anatomical landmarks that needed to be exposed to demonstrate the course of the IVS suspension needle. Distances between vital structures in the pelvis and the IVS suspension needle were measured and presented as averages of a total of 12 measurements. The needle insertion technique was performed as originally described by Petros [1]: Step 1: The dissection is initiated with a longitudinal or transverse incision at the posterior vaginal wall 1 2 cm inferior to the cervix or to the vault. On both sides of this incision a blunt pararectal dissection is performed until the pelvic side of the levator plate is reached. 2
5 Step 2: The IVS suspension needle is inserted through a small skin incision 2 cm lateral and below the external anal sphincter (left and right). The needle perforates the skin, the subcutaneous adipose tissue and enters the ischiorectal fossa. Step 3: The shaft of the IVS suspension needle is gripped at the level of the curvature (4 5 cm from the tip) to avoid excessive forward travel. The needle is pushed forward parallel to the rectum in the direction of the ischial spine and is guided by a finger placed in the vagina. Step 4: At the most cranial part of the ischiorectal fossa, the levator ani muscle is perforated at the level of a small depression that can be easily palpated medially to the ischial spine. Step 5: Once the levator plate is perforated, the IVS suspension needle is directed medially to perforate the rectovaginal fascia at the level of the apex: point C represents either the most distal (i.e. most dependent) edge of the cervix or the leading edge of the vaginal cuff (hysterectomy scar) [2]. The tape is anchored to the apex of the vaginal vault, to the uterosacral ligaments or to the posterior side of the supravaginal part of the cervix. Finally, the tape is gently stretched by pulling on each perineal end, and left tension free and unfixed. Results The IVS suspension needle is inserted 2 cm inferolateral to the external anal sphincter (5 and 7 o clock relative to the anus). This point of entry is situated halfway between the coccygeal bone (1) and the tuber ischiadicum (2) (10 cm). The needle perforates the skin, the subcutaneous adipose tissue and enters the ischiorectal fossa (3). The caudal border of m. gluteus maximus (4) is 1.5 cm dorsal to the point of insertion; hence, the muscle was not perforated in our cadaver specimens (Fig. 1). Fig. 1 Lithotomy position, caudal view: os coccygis (1), tuber ischiadicum (2), ischiorectal fossa (3), m. gluteus maximus (4), aa., vv. and nn. rectales (haemorrhoidales) inferiores (5). Arrows indicate the localisation of the skin incision sites. 3
6 The inferior rectal (haemorrhoidal) vessels and nerve (5) leave the main trunk of the pudendal vessels and run in the posterior part of the pudendal canal, more specifically near the ischial spine. They traverse the ischiorectal fossa in a horizontal plane (with patient in a supine position) 4 cm cranial to the external anal orifice. In the cadaveric specimens the needle passes 1.5 cm dorsal to these neurovascular branches and curves around them 1.5 cm cranially. These branches of the pudendal neurovascular bundle (6) can be injured if insertion of the needle occurs at the level of the anus or when the IVS suspension needle traverses the ischiorectal fossa less than 4 cm before curving. The IVS suspension needle traverses the ischiorectal fossa (3) for 9 cm cranially, lateral and inferior to the cone-shaped m. levator ani (7). At the most cranial part of the ischiorectal fossa (3) the m. levator ani (7) is perforated (Fig. 2). Fig. 2 Lithotomy position, lateral view of the left side: os coccygis (1), tuber ischiadicum (2), ischiorectal fossa (3), m. levator ani (7). The iliococcygeal part of m. levator ani (8a) is perforated at the height of a small depression between the border of the pelvic aspect of the sacrospinous ligament (m. coccygeus) (9) and m. levator ani (7), situated 1.5 cm medially to the ischial spine (10) (Fig. 3). 4
7 Fig. 3 Lithotomy position, superior view: m. levator ani (7), iliococcygeal part of m. levator (8a), ischiococcygeal part of m. levator (8b), sacrospinous ligament and m.coccygeus (9), ischial spine (10). The m. levator ani is perforated 4 cm caudal to the pudendal neurovascular structures (6). In this neurovascular bundle the pudendal nerve is the most medial structure. The pudendal artery is situated lateral to the nerve. Lateral to the artery run one or two pudendal veins. The utmost lateral structure in the bundle is a small nerve branch destined for the m. obturatorius internus (Fig. 4). Fig. 4 Lithotomy position, lateral side wall of right side of pelvis, inside view: aa., vv. and nn. pudenda (6), m. levator ani (7), sacrospinous ligament removed (9), ischial spine (10), arcus tendineus fasciae pelvis (white line) (11), arcus tendineus levator ani (12). The rectovaginal fascia (13) is perforated. The IVS suspension needle is angulated medially, remaining caudal and ventral to the pouch of Douglas. The distance to the anterior side of the rectum is 1.5 cm. Lateral to the rectum the mesh is positioned at a distance as close as 0.5 cm away from the serosa. This distance, however, underestimates the distance that the serosa is actually away during the positioning of the tunneler. Because the virtual space of the pararectal fossa is opened in a blunt fashion before positioning the tunneler, perforation of the levator plate can occur while pushing the rectum towards the contralateral side, several centimetres away from the needle s trajectory. Localisation of the outer margin of the rectum is facilitated by inserting a rectal pack (Fig. 5). 5
8 Fig. 5 Upright position, right side of pelvis, midsagittal view: rectovaginal fascia (13), pouch of Douglas (14). The trajectory of the IVS illustrates its proximity to the rectum, the point of perforation of the m. levator ani and the axis of the vagina directed towards the third sacral vertebra (Fig. 6). Fig. 6 Lithotomy position, lateral view of the left side of the m. levator ani, with its insertion on the pelvic side wall at the arcus tendineus levator ani. Discussion The dissections were undertaken to describe the trajectory of the IVS suspension needle relative to vital structures in the pelvis, in particular neurovascular structures. Visual depiction of the applied anatomy as shown in this article hopefully will result in an improved understanding of this blind /closed procedure. Although the real safety and efficacy of the posterior IVS procedure remains to be demonstrated in appropriately designed clinical trials, thorough knowledge of the 6
9 anatomical landmarks is a basic prerequisite. As embalmed bodies were used, inferences on the safety of the technique cannot be made as we are well aware that differences exist between the anatomical specimen and the pelvis of a live patient operated on. Petros [1] in his article describes the procedure as a level I reconstruction. According to our study, however, the IVS device passes 1.5 cm medial to the ischial spine through the iliococcygeus muscle. By definition, level I support is limited to the cardinal-uterosacral ligament; therefore, it seems more appropriate to state that the IVS procedure suspends the vagina at the upper border of level II, the support of the midvagina via lateral connections to the arcus tendineus fasciae pelvis [3]. From an anatomical perspective, the posterior IVS offers a more anatomical position of the vagina as it attaches the top (almost) to the level of its original position, namely the ischial spine. In comparison, the sacrospinous fixation will stretch the vagina in a more posterior and superior fashion [4]. The sacrocolpopexy does restore the normal anatomical position in the hollow of the sacrum (S3). However, surgery at this level can be complicated by the presence of presacral veins. Often the fixation of the mesh in these instances will be made at a higher level (S1-2), resulting in overcorrection with stretching of the vaginal vault. In both these procedures then the vagina is subjected to abnormal pressure predisposing the patient to develop iatrogenic prolapse of the posterior vaginal wall. Finally, we would like to suggest translevator intravaginal slingplasty as an anatomically more appropriate term for the infracoccygeal sacropexy originally described by Petros [1]. Conclusion Thorough knowledge of anatomy is essential for surgery. Applied anatomy is especially useful to improve the understanding of needle suspension techniques, as part of these are blind. All surgeons should be encouraged to use cadaveric studies prior to endeavouring to perform these new techniques. The cadaveric studies demonstrate that the IVS procedure is actually a suspension of the vagina at the upper border of DeLancey level II rather than a reconstruction of the level I support. The average distance between the needle used to perform the posterior IVS procedure and the pudendal neurovascular bundle is 4 cm, as measured on cadaveric specimens. References 1. Petros P (2001) Vault prolapse II: restoration of dynamic vaginal supports by infracoccygeal sacropexy, an axial day-case vaginal procedure. Int Urogynecol J 12:
10 2. Bump R, Mattiason A, Bo K, Brubaker L, DeLancey J, Klarskov P, Shull B, Smith A (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175: DeLancey J (1992) Anatomic aspects of vaginal eversion after hysterectomy. Am J Obstet Gynecol 166: Sze E, Meranus J, Kohli J, Miklos J, Karram M (2001) Vaginal configuration on MRI after abdominal sacrocolpopexy and sacrospinous ligament suspension. Int Urogynecol J 12:
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics.
 NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics. Anatomy above the arcuate line Skin Camper s fascia Scarpa s fascia External oblique
NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics. Anatomy above the arcuate line Skin Camper s fascia Scarpa s fascia External oblique
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
The Posterior Intravaginal Slingplasty treatment for apical prolapse: 3 years experience in a single centre setting
 F, V & V IN OBGYN, 2010, 2 (1): 1-8 Original paper The Posterior Intravaginal Slingplasty treatment for apical prolapse: 3 years experience in a single centre setting Piet HINOUL 1, Ruben VANSPAUWEN 2,
F, V & V IN OBGYN, 2010, 2 (1): 1-8 Original paper The Posterior Intravaginal Slingplasty treatment for apical prolapse: 3 years experience in a single centre setting Piet HINOUL 1, Ruben VANSPAUWEN 2,
REPRODUCTIVE SYSTEM By Dr.Ahmed Salman
 The University Of Jordan Faculty Of Medicine Anatomy Department REPRODUCTIVE SYSTEM By Dr.Ahmed Salman Assistant Professor of Anatomy &embryology Perineum It is the diamond-shaped lower end of the trunk
The University Of Jordan Faculty Of Medicine Anatomy Department REPRODUCTIVE SYSTEM By Dr.Ahmed Salman Assistant Professor of Anatomy &embryology Perineum It is the diamond-shaped lower end of the trunk
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Dana Alrafaiah. - Amani Nofal. - Ahmad Alsalman. 1 P a g e
 - 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
- 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
Imaging of Pelvic Floor Weakness. Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne
 Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Inferior Pelvic Border
 Pelvis + Perineum Pelvic Cavity Enclosed by bony, ligamentous and muscular wall Contains the urinary bladder, ureters, pelvic genital organs, rectum, blood vessels, lymphatics and nerves Pelvic inlet (superior
Pelvis + Perineum Pelvic Cavity Enclosed by bony, ligamentous and muscular wall Contains the urinary bladder, ureters, pelvic genital organs, rectum, blood vessels, lymphatics and nerves Pelvic inlet (superior
Table 2. First Generated List of Expert Responses. Likert-Type Scale. Category or Criterion. Rationale or Comments (1) (2) (3) (4)
 Table 2. First Generated List of Expert Responses. Likert-Type Scale Category or Criterion Anatomical Structures and Features Skeletal Structures and Features (1) (2) (3) (4) Rationale or Comments 1. Bones
Table 2. First Generated List of Expert Responses. Likert-Type Scale Category or Criterion Anatomical Structures and Features Skeletal Structures and Features (1) (2) (3) (4) Rationale or Comments 1. Bones
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
ig. 2. The organs and their outlet tubes.
 Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
ORIENTING TO BISECTED SPECIMENS ON THE PELVIS PRACTICAL
 ORIENTING TO BISECTED SPECIMENS ON THE PELVIS PRACTICAL The Pelvis is just about as complicated as head and neck and considerably more mysterious. You have to be able to visualize (imagine) the underlying
ORIENTING TO BISECTED SPECIMENS ON THE PELVIS PRACTICAL The Pelvis is just about as complicated as head and neck and considerably more mysterious. You have to be able to visualize (imagine) the underlying
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Development of the pelvic floor : implications for clinical anatomy Wallner, C.
 UvA-DARE (Digital Academic Repository) Development of the pelvic floor : implications for clinical anatomy Wallner, C. Link to publication Citation for published version (APA): Wallner, C. (2008). Development
UvA-DARE (Digital Academic Repository) Development of the pelvic floor : implications for clinical anatomy Wallner, C. Link to publication Citation for published version (APA): Wallner, C. (2008). Development
High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay
 High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay Poster No.: C-430 Congress: ECR 2009 Type: Educational Exhibit Topic: Abdominal and
High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay Poster No.: C-430 Congress: ECR 2009 Type: Educational Exhibit Topic: Abdominal and
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Perineum. Dept. of Human Anatomy Zhou Hong Ying
 Perineum Dept. of Human Anatomy Zhou Hong Ying OUTLINE Subdivision The Layers Urogenital Diaphragm Main Structures inside Superficial & Deep Perineal Spaces Ischioanal Fossa Perineum A narrow region Urogenital
Perineum Dept. of Human Anatomy Zhou Hong Ying OUTLINE Subdivision The Layers Urogenital Diaphragm Main Structures inside Superficial & Deep Perineal Spaces Ischioanal Fossa Perineum A narrow region Urogenital
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
ISSN (o): Sacrospinous fixation: an efficient technique for prevention and treatment of vault prolapse
 Original article www.ijrhs.com ISSN (o):2321 7251 Sacrospinous fixation: an efficient technique for prevention and treatment of vault Rajshree dayanand katke 1, Usha kiran. 2 1M.D.(Obstetrics & Gynecology),
Original article www.ijrhs.com ISSN (o):2321 7251 Sacrospinous fixation: an efficient technique for prevention and treatment of vault Rajshree dayanand katke 1, Usha kiran. 2 1M.D.(Obstetrics & Gynecology),
Perineum. done by : zaid al-ghnaneem
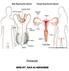 Perineum done by : zaid al-ghnaneem Hello everyone, this sheet will talk about 2 nd Lecture which is Perineum but there are some slides and info from 1 st Lecture. Everything included Slides + Pics Let
Perineum done by : zaid al-ghnaneem Hello everyone, this sheet will talk about 2 nd Lecture which is Perineum but there are some slides and info from 1 st Lecture. Everything included Slides + Pics Let
2. List the 8 pelvic spaces: list one procedure or dissection which involves entering that space.
 Name: Anatomy Quiz: Pre / Post 1. In making a pfannensteil incision you would traverse through the following layers: a) Skin, Camper s fascia, Scarpa s fascia, external oblique aponeurosis, internal oblique
Name: Anatomy Quiz: Pre / Post 1. In making a pfannensteil incision you would traverse through the following layers: a) Skin, Camper s fascia, Scarpa s fascia, external oblique aponeurosis, internal oblique
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
Pelvis MCQs. Block 1. B. Reproductive organs. C. The liver. D. Urinary bladder. 1. The pelvic diaphragm includes the following muscles: E.
 Pelvis MCQs Block 1 1. The pelvic diaphragm includes the following muscles: A. The obturator internus B. The levator ani C. The coccygeus D. The external urethral sphincter E. The internal urethral sphincter
Pelvis MCQs Block 1 1. The pelvic diaphragm includes the following muscles: A. The obturator internus B. The levator ani C. The coccygeus D. The external urethral sphincter E. The internal urethral sphincter
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Infracoccygeal sacropexy using mesh for uterine prolapse repair
 Infracoccygeal sacropexy using mesh for uterine Issued: January 2009 www.nice.org.uk/ipg280 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Infracoccygeal sacropexy using mesh for uterine Issued: January 2009 www.nice.org.uk/ipg280 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Prolapse & Stress Incontinence
 Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
-15. -Alaa Albandi. -Dr. Mohammad Almohtasib. 0 P a g e
 -15 -Alaa Albandi - -Dr. Mohammad Almohtasib 0 P a g e In this last lecture, we will talk about the sigmoid colon, rectum, and anal canal. Sigmoid colon It has a mesentery called pelvic mesocolon or sigmoidal
-15 -Alaa Albandi - -Dr. Mohammad Almohtasib 0 P a g e In this last lecture, we will talk about the sigmoid colon, rectum, and anal canal. Sigmoid colon It has a mesentery called pelvic mesocolon or sigmoidal
Guide to Pelvic Floor Multicompartment Scanning
 Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Tian-Ni Kuo 1, Ming-Ping Wu 1,2 *
 RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
Slide Read the tables it is about the difference between male & female pelvis.
 I didn t include the slides, this is only what the doctor read or said because he skipped a lot of things because we took it previously, very important to go back to the slides (*there is an edited version)
I didn t include the slides, this is only what the doctor read or said because he skipped a lot of things because we took it previously, very important to go back to the slides (*there is an edited version)
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
ischium Ischial tuberosities Sacrotuberous ligament The coccyx
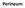 Perineum General lfeatures Region of below pelvic diaphragm A diamond shape space whose boundaries are those of the pelvic outlet Lower border of symphysis pubis Rami of pubis and ischium Ischial tuberosities
Perineum General lfeatures Region of below pelvic diaphragm A diamond shape space whose boundaries are those of the pelvic outlet Lower border of symphysis pubis Rami of pubis and ischium Ischial tuberosities
New Directions in Restoration of Pelvic Structure and Function
 2 New Directions in Restoration of Pelvic Structure and Function Peter E. Petros and Bernhard Liedl The fundamental theme of this chapter is that structure and function are intimately related. Abnormal
2 New Directions in Restoration of Pelvic Structure and Function Peter E. Petros and Bernhard Liedl The fundamental theme of this chapter is that structure and function are intimately related. Abnormal
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
TME and autonomic nerve preservation techniques: based on Video and Cadaveric anatomy
 TME and autonomic nerve preservation techniques: based on Video and Cadaveric anatomy Nam Kyu Kim M.D., Ph.D., FACS, FRCS, FASCRS Professor Department of Surgery Yonsei University College of Medicine Seoul,
TME and autonomic nerve preservation techniques: based on Video and Cadaveric anatomy Nam Kyu Kim M.D., Ph.D., FACS, FRCS, FASCRS Professor Department of Surgery Yonsei University College of Medicine Seoul,
Childbirth, chronic coughing, heavy lifting,
 OBG MANAGEMENT BY THOMAS JULIAN, MD Pelvic-support defects: a guide to anatomy and physiology Due to high postoperative failure rates, the traditional treatment for pelvic-organ prolapse hysterectomy with
OBG MANAGEMENT BY THOMAS JULIAN, MD Pelvic-support defects: a guide to anatomy and physiology Due to high postoperative failure rates, the traditional treatment for pelvic-organ prolapse hysterectomy with
Objectives. Pelvic Anatomy: Staying Out of Trouble. Disclosures. Anatomy 101. Anterior Abdominal Wall. Arcuate Line. Abheha Satkunaratnam MD, FRCS(C)
 Objectives Pelvic Anatomy: Staying Out of Trouble Abheha Satkunaratnam MD, FRCS(C) To focus on key anatomy for the gynaecologic surgeon advancing their minimally invasive gynaecologic skills To provide
Objectives Pelvic Anatomy: Staying Out of Trouble Abheha Satkunaratnam MD, FRCS(C) To focus on key anatomy for the gynaecologic surgeon advancing their minimally invasive gynaecologic skills To provide
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
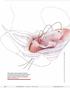 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Surgical treatments for vaginal apical prolapse
 Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option.
 Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Ex. 1 :Language of Anatomy
 Collin College BIOL 2401 : Human Anatomy & Physiology Ex. 1 :Language of Anatomy The Anatomical Position Used as a reference point when referring to specific areas of the human body Body erect Head and
Collin College BIOL 2401 : Human Anatomy & Physiology Ex. 1 :Language of Anatomy The Anatomical Position Used as a reference point when referring to specific areas of the human body Body erect Head and
Female Urology. Young-Suk Lee, Deok Hyun Han, Ji Youl Lee 1, Joon Chul Kim 2, Myung-Soo Choo 3, Kyu-Sung Lee
 www.kjurology.org DOI:1.4111/kju.21.51.3.187 Female Urology Anatomical and Functional Outcomes of Posterior Intravaginal Slingplasty for the Treatment of Vaginal Vault or Uterine Prolapse: A Prospective,
www.kjurology.org DOI:1.4111/kju.21.51.3.187 Female Urology Anatomical and Functional Outcomes of Posterior Intravaginal Slingplasty for the Treatment of Vaginal Vault or Uterine Prolapse: A Prospective,
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Laparoscopic surgery for pelvic support defects
 ~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
Lumbar Plexus. Ventral rami L1 L4 Supplies: Major nerves.. Abdominal wall External genitalia Anteromedial thigh
 Lower Limb Nerves Lectures Objectives Describe the structure and relationships of the plexuses of the lower limb. Describe the course, relationships and structures supplied for the major nerves of the
Lower Limb Nerves Lectures Objectives Describe the structure and relationships of the plexuses of the lower limb. Describe the course, relationships and structures supplied for the major nerves of the
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
Bony ypelvis. Composition: formed by coccyx, and their articulations Two portions
 Pelvis Bony ypelvis Composition: formed by paired hip bones, sacrum, coccyx, and their articulations Two portions Greater pelvis Lesser pelvis Terminal line ( pelvic inlet): formed by promontory of sacrum,
Pelvis Bony ypelvis Composition: formed by paired hip bones, sacrum, coccyx, and their articulations Two portions Greater pelvis Lesser pelvis Terminal line ( pelvic inlet): formed by promontory of sacrum,
Pelvis Perineum MCQs. Block 1.1. A. Urinary bladder. B. Rectum. C. Reproductive organs. D. The thigh
 Pelvis Perineum MCQs Block 1.1 1. The pelvic diaphragm includes the following muscles: A. The coccygeus B. The levator ani C. The external urethral sphincter D. The internal urethral sphincter E. The obturator
Pelvis Perineum MCQs Block 1.1 1. The pelvic diaphragm includes the following muscles: A. The coccygeus B. The levator ani C. The external urethral sphincter D. The internal urethral sphincter E. The obturator
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair vaginal vault prolapse The vaginal
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair vaginal vault prolapse The vaginal
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Pathogenesis of Chronic Pelvic Pain
 Pathogenesis of Chronic Pelvic Pain Yong-Chul Kim Department of anesthesia and pain medicine, Seoul National University College of Medicine 1 Overview Anatomy Nerve innervation CPP by pathology CPP by
Pathogenesis of Chronic Pelvic Pain Yong-Chul Kim Department of anesthesia and pain medicine, Seoul National University College of Medicine 1 Overview Anatomy Nerve innervation CPP by pathology CPP by
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Gökmen Sukgen, 1 Esra SaygJlJ YJlmaz, 2 and Eralp BaGer Introduction. 2. Case Presentation
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
mild Devices Kit - Instructions for Use
 INDICATION FOR USE The Vertos mild Devices are specialized surgical instruments intended to be used to perform lumbar decompressive procedures for the treatment of various spinal conditions. CONTENTS AND
INDICATION FOR USE The Vertos mild Devices are specialized surgical instruments intended to be used to perform lumbar decompressive procedures for the treatment of various spinal conditions. CONTENTS AND
Pelvic Floor Reconstruction
 3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
Bilateral iliococcygeal fixation for vaginal vault prolapse and enterocele repair using a new suturing device the digital needle driver
 BJOG: an International Journal of Obstetrics and Gynaecology August 2005, Vol. 112, pp. 1145 1149 DOI: 10.1111/j.1471-0528.2005.00616.x SURGICAL TECHNIQUE Bilateral iliococcygeal fixation for vaginal vault
BJOG: an International Journal of Obstetrics and Gynaecology August 2005, Vol. 112, pp. 1145 1149 DOI: 10.1111/j.1471-0528.2005.00616.x SURGICAL TECHNIQUE Bilateral iliococcygeal fixation for vaginal vault
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
The Language of Anatomy. (Anatomical Terminology)
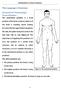 The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
Advances in Anatomy Embryology and Cell Biology
 Advances in Anatomy Embryology and Cell Biology Vol. 175 Editors F. Beck, Melbourne B. Christ, Freiburg W. Kriz, Heidelberg E. Marani, Leiden W. Kummer, Gießen R. Putz, München Y. Sano, Kyoto T. H. Schiebler,
Advances in Anatomy Embryology and Cell Biology Vol. 175 Editors F. Beck, Melbourne B. Christ, Freiburg W. Kriz, Heidelberg E. Marani, Leiden W. Kummer, Gießen R. Putz, München Y. Sano, Kyoto T. H. Schiebler,
Intraoperative Identification and Monitoring of the Somatic Nerves Critical to Potency Preservation during da Vinci Prostatectomy
 Intraoperative Identification and Monitoring of the Somatic Nerves Critical to Potency Preservation during da Vinci Prostatectomy J. Rasmussen, J. Schneider Background Since Walsh and Donker first introduced
Intraoperative Identification and Monitoring of the Somatic Nerves Critical to Potency Preservation during da Vinci Prostatectomy J. Rasmussen, J. Schneider Background Since Walsh and Donker first introduced
Prolapse and Urogynae. By Sarah Rangan & Daniel Warrell
 Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Comprehensive 3D Pelvic Floor Ultrasonography with emphasis on endovaginal (EVUS) and endoanal imaging (EAUS) W44, 30 August :00-18:00
 Comprehensive 3D Pelvic Floor Ultrasonography with emphasis on endovaginal (EVUS) and endoanal imaging (EAUS) W44, 30 August 2011 14:00-18:00 Start End Topic Speakers 14:00 14:10 Introduction: Pre-test,
Comprehensive 3D Pelvic Floor Ultrasonography with emphasis on endovaginal (EVUS) and endoanal imaging (EAUS) W44, 30 August 2011 14:00-18:00 Start End Topic Speakers 14:00 14:10 Introduction: Pre-test,
DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS
 8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
ARTICLE IN PRESS. FDA approval through the 510(k) process. 2 Therefore, any clinical information
 Evaluation of a transvaginal mesh delivery system for the correction of pelvic organ prolapse: subjective and objective findings at least 1 year after surgery Patrick J. Culligan, MD; Paul M. Littman,
Evaluation of a transvaginal mesh delivery system for the correction of pelvic organ prolapse: subjective and objective findings at least 1 year after surgery Patrick J. Culligan, MD; Paul M. Littman,
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
What is Kinesiology? Basic Biomechanics. Mechanics
 What is Kinesiology? The study of movement, but this definition is too broad Brings together anatomy, physiology, physics, geometry and relates them to human movement Lippert pg 3 Basic Biomechanics the
What is Kinesiology? The study of movement, but this definition is too broad Brings together anatomy, physiology, physics, geometry and relates them to human movement Lippert pg 3 Basic Biomechanics the
The Human Body: An Orientation
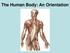 The Human Body: An Orientation Body standing upright Anatomical Position feet slightly apart palms facing forward thumbs point away from body Directional Terms Superior and inferior toward and away from
The Human Body: An Orientation Body standing upright Anatomical Position feet slightly apart palms facing forward thumbs point away from body Directional Terms Superior and inferior toward and away from
Introduction to Anatomical Terms. Packet #3
 Introduction to Anatomical Terms Packet #3 Directional Terms Directional terms describe the positions of structures relative to other structures or locations in the body. Introduction Superior vs. Inferior
Introduction to Anatomical Terms Packet #3 Directional Terms Directional terms describe the positions of structures relative to other structures or locations in the body. Introduction Superior vs. Inferior
Le fort s operation for prolapse uterus: A forgotten procedure
 2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
Introduction. Chapter 1. Structure and Function. Introduction. Anatomy and Physiology Integrated. Anatomy and Physiology Integrated Anatomy
 Introduction Chapter 1 An Introduction to A&P Study strategies crucial for success Attend all lectures, labs, and study sessions Read your lecture and laboratory assignments before going to class or lab
Introduction Chapter 1 An Introduction to A&P Study strategies crucial for success Attend all lectures, labs, and study sessions Read your lecture and laboratory assignments before going to class or lab
Elevate Anterior/Apical: 12-Month Data Showing Safety and Efficacy in Surgical Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Elevate Anterior/Apical: 12-Month Data Showing Safety and Efficacy in Surgical Treatment of Pelvic Organ Prolapse Edward J. Stanford, MD, MS,* Robert D. Moore, DO,Þ Jan-Paul W.R. Roovers,
ORIGINAL ARTICLE Elevate Anterior/Apical: 12-Month Data Showing Safety and Efficacy in Surgical Treatment of Pelvic Organ Prolapse Edward J. Stanford, MD, MS,* Robert D. Moore, DO,Þ Jan-Paul W.R. Roovers,
Prevention of Surgical Injuries in Gynecology
 in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
 Int Urogynecol J (2010) 21:515 522 DOI 10.1007/s00192-009-1064-x ORIGINAL ARTICLE High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
Int Urogynecol J (2010) 21:515 522 DOI 10.1007/s00192-009-1064-x ORIGINAL ARTICLE High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Applied Anatomy and Physiology of the Pelvic Floor. Dr David Tarver Consultant Radiologist, Poole
 Applied Anatomy and Physiology of the Pelvic Floor Dr David Tarver Consultant Radiologist, Poole Pelvic Floor 1. Sacrospinous Ligament 2. Levator Ani A Puborectalis B. Pubococcygeus C. Iliococcygeus 3.
Applied Anatomy and Physiology of the Pelvic Floor Dr David Tarver Consultant Radiologist, Poole Pelvic Floor 1. Sacrospinous Ligament 2. Levator Ani A Puborectalis B. Pubococcygeus C. Iliococcygeus 3.
Name: Block: Date: Begin by clicking on the link entitled: Anatomical References. 2. What organs do you think the cranial region holds?
 Virtual Pig Dissection ABSENT Assignment. Name: Block: Date: Go to this website: http://www.whitman.edu/biology/vpd/main.html You will be doing a pig dissection through the internet and answering questions
Virtual Pig Dissection ABSENT Assignment. Name: Block: Date: Go to this website: http://www.whitman.edu/biology/vpd/main.html You will be doing a pig dissection through the internet and answering questions
Medical Terminology: The Language of Medicine
 Medical Terminology: The Language of Medicine Word Parts: Roots Medical Terminology Language in the medical field is more extensive than the languages in many other fields. Rapid advances in science and
Medical Terminology: The Language of Medicine Word Parts: Roots Medical Terminology Language in the medical field is more extensive than the languages in many other fields. Rapid advances in science and
Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation in Treatment of Vaginal Vault Prolapse
 ISRN Obstetrics and Gynecology Volume 2013, Article ID 958670, 5 pages http://dx.doi.org/10.1155/2013/958670 Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation
ISRN Obstetrics and Gynecology Volume 2013, Article ID 958670, 5 pages http://dx.doi.org/10.1155/2013/958670 Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy
 Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery
 Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
10/15/2012. Pelvic Pain and Dysfunction
 Pain and Holly Bommersbach PT, MPT Angela De La Cruz PT, MPT Pain which occurs in the perineal and/or anal areas Pain in the lower abdomen, low back and/or pelvic girdle Pain may often affect other areas,
Pain and Holly Bommersbach PT, MPT Angela De La Cruz PT, MPT Pain which occurs in the perineal and/or anal areas Pain in the lower abdomen, low back and/or pelvic girdle Pain may often affect other areas,
Desara and Desara Blue
 Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Gluteal region DR. GITANJALI KHORWAL
 Gluteal region DR. GITANJALI KHORWAL Gluteal region The transitional area between the trunk and the lower extremity. The gluteal region includes the rounded, posterior buttocks and the laterally placed
Gluteal region DR. GITANJALI KHORWAL Gluteal region The transitional area between the trunk and the lower extremity. The gluteal region includes the rounded, posterior buttocks and the laterally placed
First stage Lec.1 : Introduction. Asst.Lec.Dr.ABDULRIDHA ALASADY
 First stage 2018-2019 Lec.1 : Introduction Asst.Lec.Dr.ABDULRIDHA ALASADY Anatomy the study of the structure and shape of the body and body parts & their relationships to one another aided by dissection
First stage 2018-2019 Lec.1 : Introduction Asst.Lec.Dr.ABDULRIDHA ALASADY Anatomy the study of the structure and shape of the body and body parts & their relationships to one another aided by dissection
ROBOTIC MESH SACROCOLPOPEXY
 ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3. October 17, 2014
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3 October 17, 2014 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) A. B. A B C. D. C D 2. Identify the structures. (2
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3 October 17, 2014 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) A. B. A B C. D. C D 2. Identify the structures. (2
Structural anatomy of the posterior pelvic compartment as it relates to rectocele
 Structural anatomy of the posterior pelvic compartment as it relates to rectocele John O.L. DeLancey, MD Ann Arbor, Michigan OBJECTIVE: This study was undertaken to define posterior compartment structural
Structural anatomy of the posterior pelvic compartment as it relates to rectocele John O.L. DeLancey, MD Ann Arbor, Michigan OBJECTIVE: This study was undertaken to define posterior compartment structural
