Laparoscopic surgery for pelvic support defects
|
|
|
- Cordelia Dickerson
- 5 years ago
- Views:
Transcription
1 ~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons continue their quest for definitive surgical cure. Though there are three primary routes of access to reconstructive pelvic surgery (abdominal, vaginal and laparoscopic) it is the laparoscopic approach that appears to be the least utilized. This is in part due to the great degree of technical difficulty associated with laparoscopic suturing. This paper reviews the general principles and functional anatomy associated with normal vaginal support as well as the laparoscopic surgical approach to pelvic floor support defects. CUff Opin Obstet Gynecol 2002 Lippincott Williams & Wilkins. Urogynecology and Reconstructive Pelvic Surgery, "Atlanta Urogynecology Associates, Atlanta, Georgia and bharvard Medical School, Cambridge, Massachusetts, USA Correspondence to John R. Miklos MD, Atlanta Urogynecology Associates, 3400-C Old Mi~on Parkway, Suite 330, Alpharetta, GA 30005, USA Tel: ; fax: ; johnrmiklos@yahoo.com Introduction The anatomy, pathophysiology, and treatment of pelvic organ prolapse has significantly evolved over the last decade with increasing understanding of anatomy and development of minimally invasive surgical procedures. Although support for the pelvic viscera, the vagina, and neighboring structures involves a complex interplay between muscles, fascia, nerve supply, and appropriate anatomic orientation, the endopelvic faiscia and pelvic floor muscles provide most of the support function in the female pelvis. Laparoscopic reconstructive pelvic surgery requires a thorough knowledge of pelvic floor anatomy and its supportive components before repair of defective anatomy is attempted. This review examines contemporary concepts in pelvic support anatomy, describes the various laparoscopic surgical techniques currently available for reconstructive pelvic surgery, and summarizes currently published results of laparoscopic reconstructive pelvic surgery. Current Opinion in Obstetrics and Gynecology 2002, 14: Anatomy of pelvic support Female pelvic support is dependent upon a number of (Q 2002 Uppincott Williams & Wilkins different entities including: bone, muscle, nerves and 104Q-872X endopelvic fascia. Even though all of these entities play an important role in the support of the vagina, it is the integrity and the inherent support of the vagina itself that is usually the focus of surgical repair. This inherent support layer is called the endopelvic fascia. Endopelvic fascia To understand the pelvic support system of the female pelvic organs, it is useful to subdivide the support system into three axes: (1) the upper vertical axis, (2) the midhorizontal axis, and (3) the lower vertical axis. The endopelvic fascia, a network of connective tissue and smooth muscle, constitutes the physical matrix that envelopes the pelvic viscera and maintains the integrity of the axes supporting the bladder, urethra, uterus, vagina, and rectum in their respective anatomic relationships. DeLancey [1] further described the three levels of support axes as follows: level 1, superior suspension of the vagina to the cardinal-uterosacral complex; level 2, lateral attachment of the upper two thirds of the vagina; and level 3, distal fusion of the vagina into the urogenital diaphragm and perineal body. In this support system,the endopelvic fascia system is thought to be continuous, extending from the origin of the cardinal-uterosacral complex to the urogenital diaphragm, providing structural support to the vagina and adjacent organs (Fig. 1). 387
2 388 Endoscopic surgery Level 1: apical support The cardinal-uterosacral complex provides apical support by suspending the uterus and upper one third of the vagina to the bony sacrum. This complex can be described as two separate entities: the cardinal ligament and the uterosacraligament. The cardinal ligament is a fascial sheath of collagen that envelops the internal iliac vessels and then continues along the uterine artery, merging into the visceral capsule of the cervix, lower uterine segment and upper vagina. The uterosacral ligament is denser and more prominent than the cardinal ligament. Collagen fibers of the uterosacraligament fuse distally with the visceral fascia over the cervix, lower uterine segment, and upper vagina, forming the pericervical ring; proximally these fibers end at the presacral fascia overlying the second, third, and fourth sacral vertebrae. This complex appears to be the most supportive structure of the uterus and upper third of the vagina. Disruption of the cardinal-uterosacral complex may result in uterine descensus or vaginal vault (apex) prolapse (Fig. 2). Likewise, the most common cause of vaginal vault prolapse is previous hysterectomy with failure to adequately reattach the cardinal-uterosacral complex to the pubocervical fascia and rectovaginal fascia at the vaginal cuff intraoperatively (Fig. 3). the vaginal epithelium with no intervening fascia [2,3]. In normal pelvic supportive anatomy, the anterior pubocervical fascia, posterior rectovaginal fascia, cardinal-uterosacral ligaments and paracolpial fibers all converge, or fuse to form the pericervical ring. The integrity and continuity of these supportive tissues can be Figure 2. Uterine prolapse An enterocele is defined as a pelvic floor hernia where the parietal peritoneum comes into direct contact with Figure 1. Level 1 (apical suspension) and level 2 (lateral attachment) Uterine prolapse begins with breaking or cutting of uterosacral ligaments. The copyright for this figure is retained by Miklos and Kohli. Figure 3. Vaginal vault prolapse Level 1, paracolpium suspends the vagina apex from the lateral pelvic sidewall via the uterosacral-cardinal complex. Level 2, the anterior vaginal wall is attached laterally to arcus tendineus fascia pelvis and the posterior vaginal wall is attached laterally to the fascia overlying the levator ani muscle. Adapted with permission [1]. The copyright for this figure is retained by Miklos and Kohli. The apex of the vagina is prolapsed due to the lack of uterosacral ligaments attachment. The copyright for this figure is retained by Miklos and Kohli.
3 '" Pelvic compromised in patients who have had a complete hysterectomy, as previously described [4-6]. An enterocele is likely to be directly related to a disruption of the fusion of the proximal margins of the pubocervical and rectovaginal fascia (Fig. 4). Although vaginal mucosa may cover this defect, it is not supportive, which greatly increases the likelihood that an enterocele will eventually develop within the vaginal cavity. Though it is possible to have an enterocele without concurrent vaginal vault prolapse, the two defects usually occur concomitantly. Although the depth and overall anatomic configuration of the cul-de-sachave been implicated in the development support defects Miklos et a/. 389 prolapse known as a cystocele, urethrocele or a cystourethrocele(fig. 6) Posteriorly, the rectovaginal septum, found between the vaginal epithelium and the rectum, attaches laterally to the fascia over the levator ani muscles. The rectovaginal septum lies between the vaginal epithelium and rectum, suspended superiorly by the cardinal-uterosacral comfigure 5. Space of Retzius: normal anatomy of the enterocele, they have never been proven to be the primary causes. Level 2: lateral support Level 2 provides horizontal support to the bladder, upper two thirds of the vagina, and rectum. Additionally, the vaginal wall itself has inherent support because of its fibromuscular composition, which is often referred to as fascia. Anterior support of the vaginal wall is provided by the pubocervical fascia, and posterior support is provided by the rectovaginal fascia. The pubocervical fascia, found between the bladder and the vaginal epithelium, attaches laterally to the arcus tendinous fascia pelvis, also referred to as the white line (Fig. 5). The white line is a linear thickening of the parietal fascia overlying the levator ani muscles and can be traced along its course, starting at its origin at the ischial spine, along the pelvic sidewall (obturator internus muscle) to its insertion into the pubic bone. A breech in the integrity of the pubocervical fascia or a defect in its lateral attachment at the white line can result in an anterior vaginal wall The copyright for this figure is retained by Miklos and Kohli. Figure 6. Paravaginal defects Figure 4. Enterocele Peritoneum Pubocervical fascia Enterocele is defined as peritoneum in direct contact with vaginal epithelium with no intervening fascia. Note the difference between vault prolapse in Fig. 3 and enterocele here. The copyright for this figure is retained by Miklos and Kohli. Lateral vaginal wall defects result in cystourethrocele as seen from the space of Retzius. The copyright for this figure is retained by Miklos and Kohli.
4 390 Endoscopic surgery plex and laterally attached.o the fascia of iliococcygeal muscle and distally fused to the perineal body. This intact rectovaginal septum is the support system of the posterior vaginal wall and helps maintain the rectum in its posterior position. A breech in the integrity of the rectovaginal septum or a defect in its lateral attachment to the iliococcygeal muscles often results in development of a rectocele (Fig. 7). Level 3: distal support The vagina and its support structures of pubocervical and rectovaginal septum traverse the urogenital hiatus to distally fuse into the parietal fascia of the pubococcygeal Figure 7. Rectovaginal fascia and puborectal muscles and the perineal membrane. The rectovaginal septum fuses to the perineal body and the pubocervical fascia fuses to the perineal membrane of the urogenital triangle, which subsequently fuses to the pubic bone. Level 1 support: laparoscopic approach to enterocele repair and vaginal vault suspension The foundation for the surgical correction of enterocele and vaginal vault prolapse is based upon sound anatomical principles already discussed. Irrespective of the surgical approach utilized the surgeon must determine and repair the specific apical defect or defects present. Site-specific enterocele repair and vaginal vault suspension As previously mentioned, level 1 support involves the long paracolpial fibers which suspend the proximal vagina and cervicovaginal junction. The cardinal and uterosacral ligaments previously described merge with these fibers and attach to the pericervical ring. This network of connective tissue fibers and smooth muscle serves to prevent vaginal eversion. A disruption of the integrity of these fibers, as opposed to stretching, results in apical vaginal vault eversion (Fig. 3). The most common cause of this condition is hysterectomy with failure to adequately reattach the cardinal-uterosacral complex to the pubocervical fascia and rectovaginal fascia at the vaginal cuff. (a) Normal anatomy. (b) Rectocele caused by a defect in the rectovaginal fascia. The copyright forthis figure is retained by Miklos and Kohli. Enterocele repair begins first by anatomically defining the fascia defect present that resulted in the herniation of peritoneum and bowel through the apex of the vagina. An enterocele is defined as a pelvic hernia where the parietal peritoneum comes into direct contact with vaginal epithelium with no intervening fascia (Fig. 4). The development of an enterocele is likely to be directly rel.ated to a disruption of the fusion of the proximal margins of the anterior pubocervical fascia and posterior rectovaginal fascia or failure to surgically reattach these two fascial margins at the time of vaginal cuff closure. It is possible that the surgeon may not incorporate the apex of the pubocervical or the rectovaginal fascia at the time of closure of the vaginal cuff. Instead the surgeon may be only incorporating vaginal mucosa and unintentionally neglecting the reattachment of the supportive fascial layers. Poor surgical closure or disruption at the apex of the pubocervical and rectovaginal fascia results in parietal peritoneum in direct contact with vaginal epithelium. Chronic rises of intraabdominal pressure will ultimately exploit this vaginal weakness with stretching of the peritoneum and vaginal mucosa and clinically evident sym pto ma tic enterocele.
5 '" Pelvic support defects Miklos et a/. 391 Laparoscopic uterosacral-ligament vault suspension and enterocele repair The technique of laparoscopic uterosacral-ligament vaginal vault suspension and enterocele repair begins with identification of the vaginal vault apex, the proximal uterosacraligaments and the course of the pelvic ureter. The identification of the vaginal vault and the delineation of the rectovaginal and pubocervical fascia are facilitated by the use of a vaginal probe (Fig. 8). Using the vaginal probe, traction is placed cephalad and ventrally, causing the uterosacral ligaments to stretch so they can be identified and traced backward to their most proximal point of origin, lateral to the sacrum. At this level, the uterosacral ligament is usually about 2-3 cm below the pelvic ureter. The peritoneum overlying the vaginal apex is incised to expose the pubocervical fascia anteriorly and the rectovaginal fascia posteriorly. If the enterocele sac is large, it may be excised and the apical edges of the pubocervical and rectovaginal fascia should be exposed (Fig. 9). A full-thickness purchase of the uterosacral ligament at its proximal portion is secured with nonabsorbable sutures. These sutures are then placed full thickness, excluding the vaginal mucosa, through the ipsilateral rectovaginal fascia and then corresponding pubocervical fascia in the region of the lateral vaginal fornix. Extracorporeal knot tying secures the uterosacral ligament to the apex of the newly formed vaginal cuff, which consists of pubocervical and rectovaginal fascia. Suture tying not only elevates and secures the apex of the vagina to the uterosacral ligament (vault suspension), but it also allows for coaptation of the rectovaginal and pubocervical fascia at the apex (enterocele repair) (Figs 10, 11). Laparoscopic sacral colpopexy Abdominal sacral colpopexy remains one of the most successful operations for the treatment of vaginal vault prolapse with excellent results on long-term follow-up. If the surgeon utilizes laparoscopy as a means of surgical access and performs the sacral colpopexy in the same Figure 9. Excision of enterocele sac Please note it is the apex of the vagina which has been excised. The copyright for this figure is retained by Miklos and Kohli. Figure 10. Enterocele repair Figure 8. Reducing the enterocele Identifying pubocervical and rectovaginal fascia utilizing a vaginal probe. The copyright for this figure is retained by Miklos and Kohli. Enterocele repair is accomplished by the reapproximation of the anterior pubocervical and posterior rectovaginal fascia. Failure to suspend the apex of the vagina will result in a persistent apical vault prolapse as seen here. The copyright for this figure is retained by Miklos and Kohli.
6 392 Endoscopic surgery Figure 11. Vault suspension Vault suspension is achieved by incorporating the uterosacral-cardinal complex with the newly constructed apex of the vagina. The copyright for this figure is retained by Miklos and Kohli. ~anner as in the open abdominal approach, operative cure rate should theoretically be equivalent. Port placement is based on the surgeon's preference, skill and acquired technique. Once the operative ports have been placed the vagina is elevated with a probe and the peritoneum overlying the vaginal apex is dissected posteriorly exposing the apex of the rectovaginal fascia. Next, anterior dissection is performed to delineate the apex of the pubocervical fascia. A separation between the rectovaginal and pubocervical fascia confirms an enterocele. If a small enterocele is present it should be repaired in a site-specific fashion by imbricating the stretched vaginal epithelium between the apical edges of the pubocervical and rectovaginal fascia. Permanent suture can be utilized in a continuous purse-string fashion or in interrupted fashion. A large enterocele should be resected so the excessive vaginal epithelium is not utilized as a point of mesh attachment. Theoretically, suturing the mesh to the enterocele sac, instead of the more supportive pubocervical and rectovaginal fascia, may predispose the patient to an increased risk of mesh erosion, suture pullout or surgical failure. Attention is then directed to the sacral promontory and the presacral space. The peritoneum overlying the sacml promontory is incised longitudinally and this peritoneal incision is extended to the cul-de-sac. A laparoscopic dissector is used to expose the anterior ligament of the sacral promontory through blunt dissection. Hemostasis is achieved using either coagulation or surgical clips. A cm x 2.5 cm polypropylene mesh graft is introduced through a 10 or 12 cm port. The vaginal apex is now directed anterior and cephalad exposing the rectovaginal fascia for application of the surgical graft. The mesh is then sutured to the rectovaginal fascia with three pairs of number 0 nonabsorbable sutures beginning distally and working towards the rectovaginal fascia apex. A second piece of mesh approximately 4 cm x 2.5 cm is then sutured in a similar fashion tp the pubocervical fascia. The surgeon should attempt to take stitches through the entire thickness of the vaginal wall, excluding the vaginal epithelium. These two meshes are then sewn together and the excess anterior mesh is trimmed as needed. The surgeon sutures the free end of the Y -shaped mesh to the anterior longitudinal ligament of the sacrum using two pairs of number 0 nonabsorbable suture. The mesh should be attached with minimal tension on the vagina. In an attempt to decrease surgical time some surgeons have utilized titanium bone tacks and hernia staplers for the mesh attachment to the anterior longitudinal ligament of the sacrum. Mter reducing intraabdominal pressure and inspecting the presacral space for hemostasis, the peritoneum is reapproximated with 2-0 polyglactin suture. Level 1 support procedures: clinical results Richardson [3] first described this anatomic defect for enterocele in 1995 in his landmark paper 'The anatomic defects in rectocele and enterocele'. Since that time, others have described laparoscopic surgical techniques which employ Richardson's anatomic theories in the treatment of enterocele and vaginal apex prolapse [7-9]. Recently Carter et 01. [10..] reported on eight patients who underwent the Richardson-Saye laparoscopic vaginal vault suspension and enterocele repair technique with e~cellent results. There are no other reports in the literature that evaluate clinical results of the laparoscopic uterosacral ligaments suspensions or traditional types of enterocele repairs such as the Halban and Moskowitz procedures. However, some have described their surgical technique or complications. Lyons [1.1] reviewed the technique and complications in 276 patients who had either a Moskowitz or Halban procedure. The worst complications encountered in this series were port site infections. Koninckx et a/. [12] emphasized using the carbon dioxide laser for vaporization of the enterocele sac, followed by uterosacral ligament shortening and suspension of the posterior vaginal wall. A modified Moschowitz procedure with approximation of the posterior vaginal fascia to the anterior wall of the rectum has also been described laparoscopically. Despite the paucity of data regarding long-term cure rates, the uterosacral ligament suspension and site specific enterocele repair remains a mainstay in many surgeons' armamentaria.
7 '\ Pelvic support defects Miklos et al. 393 In 1994 Nezhat et oj. [13] were the first to report a series of 15 patients who underwent laparoscopic sacral colpopexy. They reported an apical vault cure rate of 100% on follow-up ranging from 3 to 40 months. In 1995, Lyons and Winer [14] reported four laparoscopic sacrospinous fixation and 10 laparoscopic sacral colpopexies. Ross [8] subsequently reponed on 19 patients who underwent laparoscopic sacral colpopexy, Burch colposuspension and modified culdeplasty in The author reponed seven complications including three cystotomies, two urinary tract infections, one seroma, and one inferior epigastric laceration. Despite two patients being lost to follow-up, he reponed a cure rate of 100% (thirteen out of thineen) for vaginal apex prolapse at 1 year [8]. Use of synthetic mesh for the treatment of vaginal vault prolapse has been performed since 1991 at The University of Auvergne, Clermont-Ferrand. More than 250 cases have been treated with an apical vault cure rate of approximately 92% [15ee]. Complications are rare with the most common being mesh extrusion (2%) and only in patients who underwent concomitant hysterectomy. Patients who had uterine suspensions or who have not had a concomitant hysterectomy have not experienced this complication (A. Wattiez, personal communication at the International Society of Gynecologic Endoscopy, Berlin 2002). Level 2 support: laparoscopic approach to cystocele repair As previously described, the pubocervical fascia of the anterior vaginal wall provides primary support for the bladder and urethra. The pubocervical fascia is apically suspended by the uterosacral-cardinal ligament complex, laterally attached at the fascia overlying the obturator internus via the arcus tendineous fascia pelvis, and distally fused to the pubic bone and urogenital diaphragm. A breech or break in the integrity of the pubocervical fascia may result in a cystocele. Fascial breaks can be defined by the location of the break: transverse defects occur as a horizontal defect at the pericervical ring, lateral or paravaginal defects (Fig. 6) occur at the insertion of the white line on the lateral pelvic sidewall, and midline defects occur along the longitudinal axis of the anterior vaginal wall. Successful surgical correction of the cystocele depends on the type of defect found in the pubocervical fascia. Clinical preoperative assessment in the office is important in determining the correct surgical approach. On examination of the anterior vagina, anterolateral support should be confirmed. If one or both anterolateral sulci are absent and vaginal rogation is present, then a detachment of the pubocervical fascia from the fascial white line -a paravaginal defect -should be suspected. Cystocele due to lateral defects can be treated in a sitespecific fashion by performing a paravaginal repair (Fig. 12). The paravaginal repair has been described via open abdominal, transvaginal and laparoscopic approaches [16]. The authors believe that the abdominal and laparoscopic approaches are the preferred method for the following reasons: (1) transvaginal paravaginal repairs requires extensive dissection and theoretically could lead to an increase in local neuropathy; (2) abdominal/ laparoscopic approaches allow for an unobstructed view of the white line and pubocervical fascial break, while the transvaginal approach reduces visualization and may impede the optimal site specific repair; (3) extensive lateral dissection for the transvaginal approach requires the surgeon to completely take down any remaining good lateral attachment, allowing for paravaginal access to the white line, and (4) the laparoscopic/abdominal approach, compared with the transvaginal approach, does not require splitting of the vaginal mucosa from the underlying fibromuscular 'fascia' and thus provides more secure suture attachment on the vagina. Laparoscopic paravaginal repair: technique Port placement is a matter of surgeon's preference. We routinely perform open laparoscopy at the inferior margin of the umbilicus and place three ancillary ports under direct vision. The bladder is filled in a retrograde manner with ml of normal saline, allowing for identification of the superior border of the bladder edge. Entrance into the space of Retzius is accomplished by a transperitoneal approach using a harmonic scalpel. The incision is made approximately 3 cm above the bladder Figure 12. Paravaginal repair Urethra The reapproximation of the pubocervical fascia to the obturator internus at the arcus tendineus fascia pelvis. The copyright for this figure is retained by Miklos and Kohli.
8 394 Endoscopic surgery reflection, beginning along obliterated umbilical ligamel of loose areolar tissue at the proper place of dissection. the medial border of rightnt. Immediate identification point of incision confirms a After the space of Retzius has been entered and the pubic ramus visualized, the bladder is drained in order to prevent injury during dissection. Separation of the loose areolar and fatty layers using blunt dissection develops the retropubic space, and dissection is continued until the retropubic anatomy is clearly visualized. The pubic symphysis and bladder neck are noted in the midline ad the obturator neurovascular bundle, Cooper's ligament and the arcus tendinous fascia pelvis are identified bilaterally along the pelvic sidewall (Fig. 5). The anterior vaginal wall and its point of lateral attachment from its origin at the pubic symphysis to its insertion at the ischial spine are identified. If paravaginal wall defects are present, then the lateral margins of the pubocervical fascia will be detached from the pelvic sidewall at the arcus tendinous fascia pelvis. To facilitate identification, it is often necessary to elevate the vagina with a finger in the vagina while gently dissecting the bladder and the paraurethral and paravesical fat medially. Often, the broken edge of the pubocervical fascia has fallen inferior to the bladder and its elevation is the optimal method to discern the discrete fascial break. Once appropriately dissected, the lateral margins of the detached pubocervical fascia and the broken edge of the white line can usually be clearly visualized, confirming the paravaginal defect. The first suture is placed near the apex of the vagina though the paravesical portion of the pubocervical fascia. The needle is then passed through the ipsilateral obturator internus muscle and fascia around the arcus tendineus fascia at its origin 1-2 cm distal to the ischial spine. The suture is secured using an extracorporeal knot-tying technique. Good tissue approximation is accomplished without a suture bridge. SutUres are placed sequentially along the margins of the paravaginal defects from the ischial spine toward the urethrovesical junction. If the patient does not demonstrate stress urinary incontinence or urethral hypermobility, a series of four to five sutures are placed ipsilaterally between the ischial spine and the mid urethra. If the patient has bilateral paravaginal defects, the same technique is employed on the opposite side (Fig..12). In our experience, unilateral paravaginal defects are rare. After reviewing 300 of our operative reports for patients undergoing paravaginal repair, 93% (279/300) of patients were found to have bilateral paravaginal defects. If patients have stress urinary incontinence a retropubic urethropexy procedure can be performed concomitantly. Incontinence and its laparoscopic treatment are beyond the scope of this paper. However, this information was recently reviewed and described by the authors [17]. Level 2 support procedures: clinical results Clinical results are lacking with respect to the laparoscopic approach to paravaginal repair. However, many surgeons, including the authors, believe that laparoscopy is only a mode of surgical access. The technique of reconstructive surgery, if performed identically to the open approach, should have cure rates equal to that of abdominal procedures previously studied. There are limited data reviewing the complication rate of lower urinary tract injuries. Data on open Burch procedures alone, using two sutures bilaterally, report injury to the lower urinary tract to be approximately 10%. Speights et 01. [18] demonstrated a 2.3% bladder injury rate with no ureteral injury when performing a laparoscopic paravaginal repair with or without a Burch using four to five sutures bilaterally (total eight to ten sutures). The authors attribute the lower complication rate to the experience of the surgeons and the visualization afforded by laparoscopy. Level 2 and 3 support: laparoscopic approach to rectocele repair Laparoscopic repair of a rectocele is infrequently performed as most gynecologic surgeons find the vaginal approach to be preferred. However, in some cases including high rectocele or placement of mesh/graft from the perineal body to the uterosacral ligaments, the laparoscopic technique may have additional advantages. The technique employees open laparoscopy and placement of ports as previously described. The rectovaginal septum is opened using electrocautery, harmonic scalpel, or laser. Blunt dissection with dissectors, hydrodissection or sharp dissection may be used to open the rectovaginal space distally to the perineal body. This dissection should follow surgical planes and is often bloodless. The perineal body is sutured to the rectovaginal septum using delayed absorbable suture. The rectovaginal fascial defects are closed with number 0 nonabsorbable suture. If the rectovaginal fascia is detached from the iliococcygeus fascia, it is reattached with number 0 nonabsorbable suture. The medial aspect of the levator ani muscles may also be plicated, but care should be taken to avoid a posterior vaginal ridge [19]. Level 3 support procedures: clinical results There are few data regarding the use of laparoscopic reconstructive techniques for the treatment of rectocele. Laparoscopic rectocele repair using a polyglactin mesh was first described by Lyons and Winer [20] with an 80% cure rate in 20 women followed at 3-month intervals for 1 year. No long-term complications were noted [20]. Although associated with high success rates, the
9 Pelvic support defects Miklos et al. 395 procedure is technically challenging and deviates from the traditional vaginal approach to rectocele adopted by most gynecologic surgeons. Conclusion Laparoscopy should only be considered a mode of surgical access, which should not significantly change the technique of operative reconstructive surgery. Laparoscopy benefits the surgeon by improving visualization, decreasing blood loss and magnifying the pelvic floor defects which need to be repaired. Other advantages, including less postoperative pain, shorter hospital stays, shorter recovery time and earlier return to a better quality of life, have also been described in the literature. Disadvantages often cited in the literature include increased operative time and associated increased costs. The authors' personal experience is that operative time is similar and in many times reduced especially for patients with a high body mass index. However, complex operative laparoscopy is associated with a steep and lengthy learning curve after which operative time can be significantly reduced based on the surgeon's experience and laparoscopy skills as well as the quality of the operative team. A thorough knowledge of pelvic floor anatomy is essential before undertaking any type of reconstructive pelvic surgery, and advanced knowledge of laparoscopic surgery and suturing are essential to perform the surgical procedures discussed in this review. Despite the paucity of literature, laparoscopic pelvic reconstructive surgery will continue to be driven by patient demands as well as surgeon preference. With increasing experience, greater data should support its continued use and favorable longterm outcomes. References and recommended reading Papers of particular interest, published within the annual period of review, have been highlighted as:.of special interest..of outstanding interest Delancey JO. Anatomic aspects of vaginal eversion after hysterectomy. Am J Obstet Gyencol1992; 166: Richardson AC. The rectovaginal septum revisited: its relationship to rectocele and its importance in rectocele repair. Clin Obstet Gynecol 1 993; 36: Richardson AC. The anatomic defects in rectocele and enterocele. J Pelvic Surg 1995; 1: Kauppila 0, Punnonen R, Teisala K. Operative technique for the repair of posthysterectomy vaginal prolapse. Ann Chir Gynaecol 1986; 75: Symmonds RE, Williams TJ, Lee RA, Webb MJ. Post-hysterectomy enterocele and vaginal vault prolapse. Am J Obstet Gynecol 1981; 140: Cruikshank SH, Kovac SR. Anterior vaginal wall culdoplasty at vaginal hysterectomy to prevent posthysterectomy anterior vaginal wall prolapse. Am J Obstet Gyencol1996; 174: Ross JW. Apical vault repair, the cornerstone of pelvic floor reconstruction. Int Urogynecol J 1997; 8: Ross JW. Techniques of laparoscopic repair of total vault eversion after hysterectomy. J Am Assoc Gynecol Laparosc 1997; 4: Miklos JR, Kohli N, Lucente V, Saye WB. Site specific fascial defects in the diagnosis and surgical management of enterocele. Am J Obstet Gynecol 1998; 179: Carter JE, Winter M, Mendehlsohn S, et a/. Vaginal vault suspension and 00 enterocele repair by Richardson-Saye laparoscopic technique: description of training technique and results. J Soc Laproend Surg 2001; 5: Though this case series is limited by few patients and short term follow-up, a paucity in the literature addressing laparoscopic enterocele repair along with a well written description of the surgical techniques makes this paper a valuable resource for laparoscopic surgeons. 11 Lyons TL. Minimally invasive treatment of urinary stress incontinence and laparoscopoicalily direct repair of pelvic floor defects. Clin Obstet Gynecol 1995; 38: Koninckx PR, Poppe W, Deprest J. Carbon dioxide laser for laparoscopic enterocele repair. J Am Assoc Gyencol Laparoscop 1995; 2: Nezhat CH, Nezhat F, Nezhat C. Laparoscopic sacral colpopexy for vaginal vault prolapse. Obstet Gyneco11994; 4: Lyons TL, Winer WK. Vaginal vault suspension. Endosc Surg 1995; 3: Wattiez A, Canis M, Mage G, et a/. Promontofixation for the treatment of 00 prolapse. UrolClin NorthAm 2001; 28: This presents an excellent discussion of surgical technique by surgeons who have probably performed more laparoscopic prolapse surgery than almost any others in the world. 16 Miklos JR, Kohli N. "Paravaginal plus" Burch procedure: a laparoscopic approach. J Pelvic Surg 1998; 4: Miklos JR, Kohli N. Laparoscopic paravaginal repair plus Burch colposuspension: review and descriptive technique. Urology 2000; 56 (SuppI6A): Speights SE, Moore RD, Miklos JR. Frequency of lower urinary tract injury at laparoscopic burch and paravaginal repair. J Am Assoc Gynecol Laparosc 2000; 7: Paraiso MFR, Falcone T. Laparoscopic surgery for genuine stress urinary incontinence and pelvic organ prolapse. In: Walters MD, Karram MM, editors. Clinical urogynecology. 2nd ed. St Louis: CV Mosby; pp Lyons TL, Winer WK. Laparoscopic rectocele repair using polyglactin mesh. JAm Assoc Gynecol Laparosc. 1997; 4:
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Site-specific fascial defects in the diagnosis and surgical management of enterocele
 Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy
 Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Imaging of Pelvic Floor Weakness. Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne
 Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics.
 NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics. Anatomy above the arcuate line Skin Camper s fascia Scarpa s fascia External oblique
NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics. Anatomy above the arcuate line Skin Camper s fascia Scarpa s fascia External oblique
Prevention of Surgical Injuries in Gynecology
 in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
Inferior Pelvic Border
 Pelvis + Perineum Pelvic Cavity Enclosed by bony, ligamentous and muscular wall Contains the urinary bladder, ureters, pelvic genital organs, rectum, blood vessels, lymphatics and nerves Pelvic inlet (superior
Pelvis + Perineum Pelvic Cavity Enclosed by bony, ligamentous and muscular wall Contains the urinary bladder, ureters, pelvic genital organs, rectum, blood vessels, lymphatics and nerves Pelvic inlet (superior
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
ig. 2. The organs and their outlet tubes.
 Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
Table 2. First Generated List of Expert Responses. Likert-Type Scale. Category or Criterion. Rationale or Comments (1) (2) (3) (4)
 Table 2. First Generated List of Expert Responses. Likert-Type Scale Category or Criterion Anatomical Structures and Features Skeletal Structures and Features (1) (2) (3) (4) Rationale or Comments 1. Bones
Table 2. First Generated List of Expert Responses. Likert-Type Scale Category or Criterion Anatomical Structures and Features Skeletal Structures and Features (1) (2) (3) (4) Rationale or Comments 1. Bones
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
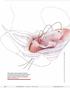 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Prolapse & Stress Incontinence
 Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks
 T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
ORIENTING TO BISECTED SPECIMENS ON THE PELVIS PRACTICAL
 ORIENTING TO BISECTED SPECIMENS ON THE PELVIS PRACTICAL The Pelvis is just about as complicated as head and neck and considerably more mysterious. You have to be able to visualize (imagine) the underlying
ORIENTING TO BISECTED SPECIMENS ON THE PELVIS PRACTICAL The Pelvis is just about as complicated as head and neck and considerably more mysterious. You have to be able to visualize (imagine) the underlying
Urinary Bladder. Prof. Imran Qureshi
 Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
Pelvis MCQs. Block 1. B. Reproductive organs. C. The liver. D. Urinary bladder. 1. The pelvic diaphragm includes the following muscles: E.
 Pelvis MCQs Block 1 1. The pelvic diaphragm includes the following muscles: A. The obturator internus B. The levator ani C. The coccygeus D. The external urethral sphincter E. The internal urethral sphincter
Pelvis MCQs Block 1 1. The pelvic diaphragm includes the following muscles: A. The obturator internus B. The levator ani C. The coccygeus D. The external urethral sphincter E. The internal urethral sphincter
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
LAPAROSCOPIC PARAVAGINAL REPAIR PLUS BURCH COLPOSUSPENSION: REVIEW AND DESCRIPTIVE TECHNIQUE
 ELSEVIER LAPAROSCOPIC PARAVAGINAL REPAIR PLUS BURCH COLPOSUSPENSION: REVIEW AND DESCRIPTIVE TECHNIQUE JOHN R. MIKLOS AND NEERAj KOHL! ABSTRACT The objective of this article was to review the available
ELSEVIER LAPAROSCOPIC PARAVAGINAL REPAIR PLUS BURCH COLPOSUSPENSION: REVIEW AND DESCRIPTIVE TECHNIQUE JOHN R. MIKLOS AND NEERAj KOHL! ABSTRACT The objective of this article was to review the available
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Desara and Desara Blue
 Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh)
 A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh) ABSTRACT In an effort to further decrease patient postoperative
A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh) ABSTRACT In an effort to further decrease patient postoperative
Desara Blue OV D I. Sling for Female Stress Urinary Incontinence. Instructions For Use
 Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
2. List the 8 pelvic spaces: list one procedure or dissection which involves entering that space.
 Name: Anatomy Quiz: Pre / Post 1. In making a pfannensteil incision you would traverse through the following layers: a) Skin, Camper s fascia, Scarpa s fascia, external oblique aponeurosis, internal oblique
Name: Anatomy Quiz: Pre / Post 1. In making a pfannensteil incision you would traverse through the following layers: a) Skin, Camper s fascia, Scarpa s fascia, external oblique aponeurosis, internal oblique
Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Desara TV and Desara Blue TV
 Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Female Urology. The Results of Grade IV Cystocele Repair Using Mesh. Introduction ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M
 Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
Gökmen Sukgen, 1 Esra SaygJlJ YJlmaz, 2 and Eralp BaGer Introduction. 2. Case Presentation
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Project Submitted Towards Completion Of Diploma In Minimal Access Surgery, Laparoscopy Hospital, New Delhi, India. AUGUST 2007.
 LAPAROSCOPIC MANAGEMENT OF VAULT PROLAPSE Member of world association of laparoscopic surgeons Project submitted toward completion of diploma in minimal access surgery,laparoscopy hospital, new Delhi.India,august2007
LAPAROSCOPIC MANAGEMENT OF VAULT PROLAPSE Member of world association of laparoscopic surgeons Project submitted toward completion of diploma in minimal access surgery,laparoscopy hospital, new Delhi.India,august2007
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
Vaginal McCall culdoplasty versus laparoscopic uterosacral plication to prophylactically address vaginal vault prolapse
 Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Slide Read the tables it is about the difference between male & female pelvis.
 I didn t include the slides, this is only what the doctor read or said because he skipped a lot of things because we took it previously, very important to go back to the slides (*there is an edited version)
I didn t include the slides, this is only what the doctor read or said because he skipped a lot of things because we took it previously, very important to go back to the slides (*there is an edited version)
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dana Alrafaiah. - Amani Nofal. - Ahmad Alsalman. 1 P a g e
 - 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
- 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after vaginal hysterectomy
 Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
This presentation will discuss the anatomy of the anterior abdominal wall as it pertains to gynaecological and obstetric surgery.
 This presentation will discuss the anatomy of the anterior abdominal wall as it pertains to gynaecological and obstetric surgery. 1 The border of the anterior abdominal wall is defined superiorly by the
This presentation will discuss the anatomy of the anterior abdominal wall as it pertains to gynaecological and obstetric surgery. 1 The border of the anterior abdominal wall is defined superiorly by the
Surgical treatments for vaginal apical prolapse
 Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October :00-12:00
 W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation
 Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
TME and autonomic nerve preservation techniques: based on Video and Cadaveric anatomy
 TME and autonomic nerve preservation techniques: based on Video and Cadaveric anatomy Nam Kyu Kim M.D., Ph.D., FACS, FRCS, FASCRS Professor Department of Surgery Yonsei University College of Medicine Seoul,
TME and autonomic nerve preservation techniques: based on Video and Cadaveric anatomy Nam Kyu Kim M.D., Ph.D., FACS, FRCS, FASCRS Professor Department of Surgery Yonsei University College of Medicine Seoul,
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Technique Guide. Bard MK Hernia Repair. Featuring Modified Onflex Mesh SOFT TISSUE REPAIR. Anterior Approach to a Preperitoneal Inguinal Hernia Repair
 Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Childbirth, chronic coughing, heavy lifting,
 OBG MANAGEMENT BY THOMAS JULIAN, MD Pelvic-support defects: a guide to anatomy and physiology Due to high postoperative failure rates, the traditional treatment for pelvic-organ prolapse hysterectomy with
OBG MANAGEMENT BY THOMAS JULIAN, MD Pelvic-support defects: a guide to anatomy and physiology Due to high postoperative failure rates, the traditional treatment for pelvic-organ prolapse hysterectomy with
Pelvic Organ Prolapse: Diagnosis, Treatment, and Avoiding Complications
 Pelvic Organ Prolapse: Diagnosis, Treatment, and Avoiding Complications Christina Dancz and Morgan Fullerton Contents 1 Introduction... 2 2 Anatomy/Pathophysiology... 2 2.1 Level 1: The Cardinal and Uterosacral
Pelvic Organ Prolapse: Diagnosis, Treatment, and Avoiding Complications Christina Dancz and Morgan Fullerton Contents 1 Introduction... 2 2 Anatomy/Pathophysiology... 2 2.1 Level 1: The Cardinal and Uterosacral
Objectives. Pelvic Anatomy: Staying Out of Trouble. Disclosures. Anatomy 101. Anterior Abdominal Wall. Arcuate Line. Abheha Satkunaratnam MD, FRCS(C)
 Objectives Pelvic Anatomy: Staying Out of Trouble Abheha Satkunaratnam MD, FRCS(C) To focus on key anatomy for the gynaecologic surgeon advancing their minimally invasive gynaecologic skills To provide
Objectives Pelvic Anatomy: Staying Out of Trouble Abheha Satkunaratnam MD, FRCS(C) To focus on key anatomy for the gynaecologic surgeon advancing their minimally invasive gynaecologic skills To provide
Anterior vaginal wall prolapse occurs commonly
 Anterior vaginal wall prolapse: Innovative surgical approaches MARK D. WALTERS, MD, AND MARIE FIDELA R. PARAISO, MD Anterior vaginal wall prolapse occurs commonly and may coexist with disorders of micturition.
Anterior vaginal wall prolapse: Innovative surgical approaches MARK D. WALTERS, MD, AND MARIE FIDELA R. PARAISO, MD Anterior vaginal wall prolapse occurs commonly and may coexist with disorders of micturition.
The accomplished gynecologic surgeon
 For mass reproduction, content licensing and permissions contact Dowden Health Media. SURGICAL TECHNIQUES THE RETROPERITONEAL SPACE Keeping vital structures out of harm s way Knowledge of the retroperitoneal
For mass reproduction, content licensing and permissions contact Dowden Health Media. SURGICAL TECHNIQUES THE RETROPERITONEAL SPACE Keeping vital structures out of harm s way Knowledge of the retroperitoneal
High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay
 High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay Poster No.: C-430 Congress: ECR 2009 Type: Educational Exhibit Topic: Abdominal and
High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay Poster No.: C-430 Congress: ECR 2009 Type: Educational Exhibit Topic: Abdominal and
Le fort s operation for prolapse uterus: A forgotten procedure
 2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
Perineum. done by : zaid al-ghnaneem
 Perineum done by : zaid al-ghnaneem Hello everyone, this sheet will talk about 2 nd Lecture which is Perineum but there are some slides and info from 1 st Lecture. Everything included Slides + Pics Let
Perineum done by : zaid al-ghnaneem Hello everyone, this sheet will talk about 2 nd Lecture which is Perineum but there are some slides and info from 1 st Lecture. Everything included Slides + Pics Let
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Index. B Bladder, injury of, Bowel, injury of, , Brachytherapy, for cervical cancer, 357 Burns, electrosurgical,
 Perioperative Nursing Clinics 1 (2006) 375 379 Index Note: Page numbers of article titles are in boldface type. A Abdominal hysterectomy Acidosis, from insufflation, 323 Active electrode monitoring, in
Perioperative Nursing Clinics 1 (2006) 375 379 Index Note: Page numbers of article titles are in boldface type. A Abdominal hysterectomy Acidosis, from insufflation, 323 Active electrode monitoring, in
ISSN (o): Sacrospinous fixation: an efficient technique for prevention and treatment of vault prolapse
 Original article www.ijrhs.com ISSN (o):2321 7251 Sacrospinous fixation: an efficient technique for prevention and treatment of vault Rajshree dayanand katke 1, Usha kiran. 2 1M.D.(Obstetrics & Gynecology),
Original article www.ijrhs.com ISSN (o):2321 7251 Sacrospinous fixation: an efficient technique for prevention and treatment of vault Rajshree dayanand katke 1, Usha kiran. 2 1M.D.(Obstetrics & Gynecology),
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Functional Anatomy of the Pelvic Floor and Lower Urinary Tract
 CLINICAL OBSTETRICS AND GYNECOLOGY Volume 47, Number 1, 3 17 2004, Lippincott Williams & Wilkins, Inc. Functional Anatomy of the Pelvic Floor and Lower Urinary Tract JOHN T. WEI, MD* and JOHN O. L. DE
CLINICAL OBSTETRICS AND GYNECOLOGY Volume 47, Number 1, 3 17 2004, Lippincott Williams & Wilkins, Inc. Functional Anatomy of the Pelvic Floor and Lower Urinary Tract JOHN T. WEI, MD* and JOHN O. L. DE
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Pelvis Perineum MCQs. Block 1.1. A. Urinary bladder. B. Rectum. C. Reproductive organs. D. The thigh
 Pelvis Perineum MCQs Block 1.1 1. The pelvic diaphragm includes the following muscles: A. The coccygeus B. The levator ani C. The external urethral sphincter D. The internal urethral sphincter E. The obturator
Pelvis Perineum MCQs Block 1.1 1. The pelvic diaphragm includes the following muscles: A. The coccygeus B. The levator ani C. The external urethral sphincter D. The internal urethral sphincter E. The obturator
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3. October 17, 2014
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3 October 17, 2014 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) A. B. A B C. D. C D 2. Identify the structures. (2
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3 October 17, 2014 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) A. B. A B C. D. C D 2. Identify the structures. (2
Pelvic Floor Reconstruction
 3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
Bony ypelvis. Composition: formed by coccyx, and their articulations Two portions
 Pelvis Bony ypelvis Composition: formed by paired hip bones, sacrum, coccyx, and their articulations Two portions Greater pelvis Lesser pelvis Terminal line ( pelvic inlet): formed by promontory of sacrum,
Pelvis Bony ypelvis Composition: formed by paired hip bones, sacrum, coccyx, and their articulations Two portions Greater pelvis Lesser pelvis Terminal line ( pelvic inlet): formed by promontory of sacrum,
I. Permission to publish. II. Offprint order. III. Copyright Transfer Statement (sign only if not submitted previously) Dear Beate Gärtner,
 Fax to: +49622148768905 Beate Gärtner Springer Heidelberg, 69121 Heidelberg From: Re: Authors: International Urogynecology Journal DOI 10.1007/s00192-004-1264-3 Translevator posterior intravaginal slingplasty:
Fax to: +49622148768905 Beate Gärtner Springer Heidelberg, 69121 Heidelberg From: Re: Authors: International Urogynecology Journal DOI 10.1007/s00192-004-1264-3 Translevator posterior intravaginal slingplasty:
New Directions in Restoration of Pelvic Structure and Function
 2 New Directions in Restoration of Pelvic Structure and Function Peter E. Petros and Bernhard Liedl The fundamental theme of this chapter is that structure and function are intimately related. Abnormal
2 New Directions in Restoration of Pelvic Structure and Function Peter E. Petros and Bernhard Liedl The fundamental theme of this chapter is that structure and function are intimately related. Abnormal
DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS
 8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications
 Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
Gross Anatomy of the Urinary System
 Gross Anatomy of the Urinary System Lecture Objectives Overview of the urinary system. Describe the external and internal anatomical structure of the kidney. Describe the anatomical structure of the ureter
Gross Anatomy of the Urinary System Lecture Objectives Overview of the urinary system. Describe the external and internal anatomical structure of the kidney. Describe the anatomical structure of the ureter
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF)
 Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Lecture 56 Kidney and Urinary System
 Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
We welcome comments and corrections which will be used to improve the system annually.
 ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
Despite the growing body of medical
 SURGICAL TECHNIQUES BY VINCENT R. LUCENTE, MD, MBA, AND MILES MURPHY, MD Laparoscopic Burch colposuspension for stress urinary incontinence: When, how, and why? Female SUI is a common condition without
SURGICAL TECHNIQUES BY VINCENT R. LUCENTE, MD, MBA, AND MILES MURPHY, MD Laparoscopic Burch colposuspension for stress urinary incontinence: When, how, and why? Female SUI is a common condition without
Anatomy of Pelvic Floor Dysfunction
 Anatomy of Pelvic Floor Dysfunction Marlene M. Corton, MD KEYWORDS Pelvic floor Levator ani muscles Pelvic connective tissue Ureter Retropubic space Prevesical space NORMAL PELVIC ORGAN SUPPORT The main
Anatomy of Pelvic Floor Dysfunction Marlene M. Corton, MD KEYWORDS Pelvic floor Levator ani muscles Pelvic connective tissue Ureter Retropubic space Prevesical space NORMAL PELVIC ORGAN SUPPORT The main
Anatomy & Physiology Pelvic Girdles 10.1 General Information
 Anatomy & Physiology Pelvic Girdles 10.1 General Information ICan2Ed, Inc. In human anatomy, the pelvis (plural pelves or pelvises) is the lower part of. The area of the body that is between the abdomen
Anatomy & Physiology Pelvic Girdles 10.1 General Information ICan2Ed, Inc. In human anatomy, the pelvis (plural pelves or pelvises) is the lower part of. The area of the body that is between the abdomen
Clinical Study Initial Experience with Robotic Retropubic Urethropexy Compared to Open Retropubic Urethropexy
 Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3. October 16, 2015
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3 October 16, 2015 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) A. B. A B C. D. C D 2. Identify the structures. (2
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3 October 16, 2015 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) A. B. A B C. D. C D 2. Identify the structures. (2
yechniques,!nd Instrumentation
 yechniques,!nd Instrumentation l FERTILITY AND STERILITY Copyright 1996 American Society for Reproductive Medicine Vol. 6, No.1, January 1996 Printed on acid-free paper in U. S. A Laparoscopically assisted
yechniques,!nd Instrumentation l FERTILITY AND STERILITY Copyright 1996 American Society for Reproductive Medicine Vol. 6, No.1, January 1996 Printed on acid-free paper in U. S. A Laparoscopically assisted
Lecture 01 Internal surface of anterolateral abdominal wall. BY Dr Farooq Khan Aurakzai
 Lecture 01 Internal surface of anterolateral abdominal wall BY Dr Farooq Khan Aurakzai Dated: 21.12.2017 Internal surface of the anterolateral abdominal wall The internal ( posterior ) surface of the anterolateral
Lecture 01 Internal surface of anterolateral abdominal wall BY Dr Farooq Khan Aurakzai Dated: 21.12.2017 Internal surface of the anterolateral abdominal wall The internal ( posterior ) surface of the anterolateral
disfunzioni sessuali ed urinarie: come evitarle? D. Mascagni
 disfunzioni sessuali ed urinarie: come evitarle? D. Mascagni Cattedra di Chirurgia Generale Direttore: Prof. A. Filippini Verona, 2010 CHIRURGIA RADICALE PER CANCRO DEL RETTO SOTTOPERITONEALE 5cm 2 cm
disfunzioni sessuali ed urinarie: come evitarle? D. Mascagni Cattedra di Chirurgia Generale Direttore: Prof. A. Filippini Verona, 2010 CHIRURGIA RADICALE PER CANCRO DEL RETTO SOTTOPERITONEALE 5cm 2 cm
INJ. Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple Sutures: Surgical Technique and Results.
 Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
