Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery
|
|
|
- Clarence Lindsey
- 5 years ago
- Views:
Transcription
1 WOMEN'S HEALTH WOMEN'S HEALTH Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery Sandra A. Baydock, MD, 1 Catherine Flood, MD, 1 Jane A. Schulz, MD, 1 Dianna MacDonald, PT, 1 Deborah Esau, BScPT, 1 Sandra Jones, BPT, 1 Craig B. Hiltz, MSc² 1 Department of Obstetrics and Gynecology, University of Alberta, Edmonton AB 2 Consultant Statistician, Department of Obstetrics and Gynecology, University of Alberta, Edmonton AB Abstract Objective: To determine the prevalence of and risk factors for urinary and fecal incontinence four months after vaginal delivery. Methods: All patients who had vaginal deliveries at a tertiary care hospital over a three-month period were approached during their postpartum hospital stay regarding participation in the study. Participants underwent a telephone interview at four months after their delivery to determine the presence and type of any incontinence. Results: Of 632 patients, 145 (23%) had stress incontinence, 77 (12%) had urge incontinence, 181 (29%) had any urinary incontinence and 23 (4%) had fecal incontinence. In univariate analysis, stress incontinence was found to be increased in patients of age (26.2%) compared with patients < 30 years of age (19.3%) (RR 1.4; 95% CI , P = 0.05). Urge incontinence was increased in patients who had a forceps delivery (21%) compared with no forceps delivery (9%) (RR 2.2; 95% CI , P = 0.005), an episiotomy (32.4%) compared with no episiotomy (18.7%) (RR 1.9; 95% CI , P < 0.01) and a longer second stage of labour (108 min vs. 77 min, P = 0.01). The prevalence of any urinary incontinence was increased with forceps delivery (15.5%) compared with no forceps delivery (8.7%) (RR 1.5; 95% CI , P = 0.01) and maternal age of (34.1%) compared to < 30 years (23.5%) (RR 1.5; 95% CI , P = 0.003). In multivariate analysis, the two variables that remained significant for any urinary incontinence were maternal age (P < 0.01) and forceps delivery (P < 0.01). There were no identified risk factors for fecal incontinence. Conclusion: Urinary incontinence is common in women at four months post partum. Fecal incontinence is less common. Maternal age and forceps assisted delivery were risk factors for urinary incontinence. Key Words: Stress urinary incontinence, urge urinary incontinence, fecal incontinence, vaginal delivery Competing Interests: ne declared. Received on March 13, 2008 Accepted on April 16, 2008 Résumé Objectif : Déterminer la prévalence et les facteurs de risque de l incontinence urinaire et fécale, quatre mois à la suite d un accouchement vaginal. Méthodes : Sur une période de trois mois, au sein d un hôpital de soins tertiaires, nous avons sollicité la participation de toutes les patientes y ayant connu un accouchement vaginal et s y trouvant dans le cadre de leur hospitalisation postpartum. Les participantes se sont soumises à une entrevue téléphonique, quatre mois à la suite de l accouchement, en vue de déterminer la présence et le type de toute incontinence, le cas échéant. Résultats : Sur les 632 patientes, 145 (23 %) connaissaient une incontinence à l effort, 77 (12 %) connaissaient une incontinence par impériosité, 181 (29 %) connaissaient une incontinence urinaire (quel qu en soit le type) et 23 (4 %) connaissaient une incontinence fécale. Dans le cadre de l analyse univariée, il a été constaté que l incontinence à l effort connaissait une hausse chez les patientes de 30 ans (26,2 %), par comparaison avec les patientes de < 30 ans (19,3 %) (RR, 1,4; IC à 95 %, 1,0 1,8, P = 0,05). L incontinence par impériosité connaissait une hausse chez les patientes qui avaient subi un accouchement par forceps (21 %), par comparaison avec celles qui n avaient pas subi un tel accouchement (9 %) (RR, 2,2; IC à 95 %, 1,4 3,6, P = 0,005); une épisiotomie (32,4 %), par comparaison avec celles qui n en avaient pas subi une (18,7 %) (RR, 1,9; IC à 95 %, 1,2 2,9, P < 0,01); et un deuxième stade du travail prolongé (108 min, par comparaison avec 77 min, P = 0,01). La prévalence de l incontinence urinaire (quel qu en soit le type) connaissait une hausse en présence d un accouchement par forceps (15,5 %), par comparaison avec l absence d une telle intervention (8,7 %) (RR, 1,5; IC à 95 %, 1,1 2,1, P = 0,01), et en présence d un âge maternel de 30 ans (34,1 %), par comparaison avec un âge maternel de < 30 ans (23,5 %) (RR, 1,5; IC à 95 %, 1,1 1,9, P = 0,003). Dans le cadre de l analyse multivariée, l âge maternel de 30 ans (P < 0,01) et l accouchement par forceps (P < 0,01) constituaient les deux variables qui demeuraient significatives peu importe le type d incontinence urinaire. Aucun facteur de risque d incontinence fécale n a été identifié. Conclusion : L incontinence urinaire est courante chez les femmes dont l accouchement remonte à quatre mois. L incontinence fécale est moins courante. L âge maternel et l accouchement par forceps étaient des facteurs de risque en ce qui concerne l incontinence urinaire. J Obstet Gynaecol Can 2009;31(1): JANUARY JOGC JANVIER 2009
2 Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery INTRODUCTION Vaginal delivery is an established risk factor for urinary and fecal incontinence, 1 5 while delivery by Caesarean section appears to be protective. 1 3,6-8 Urinary and fecal incontinence reduce quality of life and may lead to increased health care costs and medical interventions. 9 The prevalence of urinary incontinence in the postpartum period ranges from 0.3% to 38%. 1 3,10 This range is derived from studies with differing definitions of urinary incontinence and variable follow-up periods. In addition, many studies have focused primarily on the development of stress or any urinary incontinence, while only a few studies examined the prevalence of postpartum urge incontinence. 1,2,11 Risk factors for incontinence after vaginal delivery, including parity, age, birth weight, forceps-assisted delivery, and maternal age, have been found in some studies but not in others. 1,2,12 15 Risk factors for postpartum urge incontinence have been poorly evaluated. 12 The prevalence of postpartum fecal incontinence has been more consistently reported to range between 4% and 5.5% after vaginal delivery. 4,16,17 While anal sphincter disruption appears to be an established risk factor for fecal incontinence, other factors such as episiotomy and instrumental delivery are more controversial. 4,17 The primary aim of this study was to determine the prevalence of stress, urge, and mixed urinary incontinence, as well as fecal incontinence, at four months after vaginal delivery. We also identified demographic or obstetrical risk factors for these conditions. The effect of delivery by Caesarean section was not reviewed in this study. MATERIALS AND METHODS This was a prospective, cohort study undertaken at a tertiary care obstetrical hospital in Edmonton, Alberta. All patients who underwent a spontaneous or operative vaginal delivery at the Royal Alexandra Hospital between January 1, 1999, and March 31, 1999, were approached during their postpartum admission for recruitment into the study. Inclusion criteria included having a singleton vaginal delivery, proficiency in English, and a permanent residence with a telephone. Patients were excluded if they had prepregnancy urinary or fecal incontinence, drug or alcohol abuse (which might affect a subject s ability to complete the questionnaire and the follow-up survey), or incontinence due to a medical, cognitive, or mobility impairment. Relevant demographic and obstetrical data were collected from prenatal records and hospital charts. At four months post partum, a telephone interview was conducted to determine the presence and type of incontinence. Maternal demographic, clinical, and obstetrical factors identified as independent variables were maternal age, birth weight, parity, weight gain during pregnancy (BMI was not consistently available), length of second stage of labour, postpartum urinary tract infection, mode of delivery, degree of obstetrical tear, breech delivery, epidural use, and episiotomy. Neonatal risk factors were limited to birth weight. The telephone interview consisted of a 19-item questionnaire designed to determine the presence, frequency, and severity of stress and urge urinary incontinence, or fecal incontinence. These were standardized questionnaires used by the tertiary care urogynaecology unit at the time of the study; validated tools for assessment of pelvic floor symptoms were not widely used or available. The timing of follow-up at four months post partum was selected to allow the urinary tract to return to pre-pregnancy structure and function; most women have return of normal function within two to three months of delivery Incontinence of urine was defined as urinary leakage at least once in a two week interval. Questions related to stress incontinence described urinary leaking with activities such as coughing, laughing, sneezing, bending, lifting, bouncing, or exercising. Urge incontinence was defined as urinary leaking associated with a strong desire to urinate. Fecal incontinence was defined as leakage of liquid or solid stool at least once every two weeks. Patients were also questioned regarding urinary frequency, pad use, nocturia, prepregnancy and antepartum incontinence (part of the screening questions), weight gain during pregnancy, and postpartum urinary tract infections. A pilot test of the questionnaire was conducted with 30 postpartum subjects to ensure the questions were specific and easy to understand. Categorical variables including age (arbitrarily divided into < 30 years or ), mode of delivery, episiotomy, use of epidural analgesia, and postpartum urinary tract infection were assessed using chi square or Fisher exact tests. Ratio variables including parity, weight gain during pregnancy, and birth weight were assessed by a Student t test. The rank variable of obstetrical tear was assessed using a Mann- Whitney U test. Logistic regression was used to examine factors affecting the presence of urinary incontinence and included all factors with a P value 0.10 on univariate analysis. All statistical analyses were performed using SPSS for Windows version 11.5 (SPSS Inc., Chicago IL). Ethics approval for the study was obtained from the University of Alberta Health Research Ethics Board. RESULTS A total of 717 patients were recruited into the study. Eighty-four patients were excluded because of pre-existing JANUARY JOGC JANVIER
3 WOMEN'S HEALTH Table 1. Characteristics Characteristic n (range) Mean maternal age 29 (17 43) Median parity 1 (0 8) Mean birth weight, grams 3302 ( ) Mean weight gain in pregnancy, pounds 31.5 (19 80) Mean length 2nd stage, minutes 80.5 (0 651) Postpartum UTI n (%) 600 (94.9) 32 (5.1) Forceps delivery n (%) ne Low/outlet Mid Rotation Breech data 564 (89.2) 18 (2.8) 42 (6.6) 2 (0.4) 5 (0.8) 1 (0.2) Vacuum delivery n (%) ne Low Mid 536 (84.8) 66 (10.4) 30 (4.8) Degree obstetrical tear n (%) data 225 (35.6) 113 (17.8) 218 (34.4) 66 (10.5) 9 (1.5) 1 (0.2) Epidural use n (%) 335 (53.0) 297 (47.0) Episiotomy n (%) ne Midline Mediolateral 503 (79.6) 88 (13.9) 41 (6.5) incontinence and one because of active perianal Crohn s disease. The final analysis included data from 632 patients. Baseline and delivery characteristics of study participants are shown in Table 1. The demographic variables of the study group included a mean maternal age of 29 years (range 17 43), a median parity of 1 (range 0 8), a mean birth weight of 3316 g (range g), and a mean maternal weight gain of 14.0 kg (range 8.5 to 35.7 kg). Peripartum variables included a mean duration of second stage of labour of 81 minutes (range 0 651), and mode of delivery included spontaneous vaginal delivery (536, 84.8%), forceps-assisted delivery (68, 10.8%), vacuumassisted delivery (96, 15.2% ). Some patients underwent a delivery that was both vacuum-assisted and forcepsassisted, and were included in both groups because of the small numbers. A total of 143 patients complained of stress urinary incontinence (23%), 77 patients complained of urge urinary incontinence (12%), and 181 patients complained of any type of urinary incontinence (29%). Twenty-three (4%) complained of fecal incontinence. There was a significant association between the two types of urinary incontinence (P < 0.01). For example, a patient with stress urinary incontinence was more likely to have urge urinary incontinence than a patient without stress incontinence. Fecal incontinence showed a significant association with stress or urge incontinence (P < 0.01 and P = 0.02, respectively). The results of the univariate analysis for the development of stress urinary incontinence are summarized in Table 2. The only variable identified as statistically significant was maternal age (RR 1.5; 95% CI ; P = 0.05). The results of the univariate analysis for the development of urge urinary incontinence are summarized in Table 3. Significant variables included maternal age (RR 1.5; 95% CI ; P = 0.05), forceps-assisted delivery (RR 2.2; 95% CI ; P = 0.001), episiotomy (RR 3.5; 95% CI ; P < 0.001) and increased length of second stage (108 minutes, SD 111, vs. 77 minutes, SD 87; P = 0.01). The results of the univariate analysis for the development of any urinary incontinence are summarized in Table 4. Significant variables included maternal age (RR 1.5; 95% CI ; P = 0.003) and forceps-assisted delivery (RR 1.5; 95% CI , P = 0.01). risk factors for fecal incontinence were identified. Multivariate analysis was used to evaluate risk factors (Table 5). For stress urinary incontinence, we performed logistic regression analysis controlling for maternal age, epidural use, and forceps-assisted delivery. Only a maternal age was significant (P = 0.02). In the analysis for urge urinary incontinence, we controlled for maternal age, length of second stage of labour, forceps-assisted delivery, and episiotomy. The only risk factor that remained significant after multivariate analysis was maternal age. When we examined risk factors for any urinary incontinence, we controlled for maternal age, forceps-assisted delivery, and birth weight. In this analysis, both maternal age (P = 0.004) and forceps delivery (P = 0.008) remained significant. 38 JANUARY JOGC JANVIER 2009
4 Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery Table 2. Risk factors for stress urinary incontinence Variable SUI (143), n (%) SUI (489), n (%) RR 95% CI P 63 (44.1) 264 (54.0) (55.9) 225 (46.1) Forceps delivery 21 (14.6) 46 (9.0) (84.4) 443 (91.0) Epidural use 77 (54.0) 220 (45.0) (46.0) 269 (55.0) SUI: stress urinary incontinence Table 3. Risk factors for urge urinary incontinence Variable UUI (77), n (%) UUI (555), n (%) RR 95% CI P Forceps Episiotomy Length of 2nd stage, minutes (SD) 32 (41.6) 45 (58.4) 295 (53.2) 260 (46.8) (20.8) 51 (9.2) (79.2) 504 (90.8) 25 (32.4) 104(18.7) (67.6) 451(81.3) 108 (SD 111) 77 (SD 87) NA NA 0.01 UUI: urge urinary incontinence DISCUSSION This study was designed to determine the prevalence of urinary and fecal incontinence following vaginal delivery and to evaluate risk factors for these conditions. The reported prevalence of urinary incontinence after vaginal delivery varies from 0.3% to 38%. 1 3,10 Viktrup et al. reported a prevalence as low as 0.3% in primiparous women at three months post partum. 1 Other studies show a prevalence of urinary incontinence during the first six months post partum ranging from 21% to 38%, 1,3,10,16 which is consistent with our results (29% prevalence of any urinary incontinence). Patients were included in the study by Viktrup et al. 1 only if they met the strict International Continence Society s definition of incontinence, although 6% admitted to any urinary incontinence at three months post partum. The study population in the study by Viktrup et al. also consisted only of primiparous women, none of whom had a forceps-assisted delivery. 1 Our study population was heterogeneous for parity and mode of delivery, with 10.8% of our population undergoing a forceps-assisted delivery. Other studies confirm forceps delivery increases the prevalence of urinary incontinence in the first six months after delivery. 3,16 A significant association between the two types of urinary incontinence was found in our study. The presence of stress urinary incontinence increased the likelihood of a woman s also having urge urinary incontinence. Mixed urinary incontinence is a common entity in women, but the specific number of women developing urge incontinence is reported in only a few studies. 2,11 Although the etiology of stress urinary incontinence in the postpartum period may be related to pudendal nerve disruption, 4,5 the etiology of urge incontinence remains unclear. We also found a significant association between urinary and fecal incontinence, which has biological plausibility since the pudendal nerve JANUARY JOGC JANVIER
5 WOMEN'S HEALTH Table 4. Risk factors for any urinary incontinence Variable UI (181), n (%) UI (451), n (%) RR 95% CI P Forceps Birth weight, grams (SD) 77 (42.5) 104 (57.5) 250 (55.4) 201 (44.6) (15.5) 39 (8.7) (84.5) 412 (91.3) 3374 (498) 3273 (563) NA NA 0.07 UI: urinary incontinence Table 5. Multivariate analysis of risk factors for urinary incontinence Variable Stress incontinence 0.02* Urge incontinence 0.01* Length second stage of labour Any incontinence 0.01* Forceps 0.01* * denotes statistical significance innervates both striated sphincters involved in urinary and fecal continence. 4,5 A maternal age of was found to be significant on multivariate analysis for stress incontinence. Although urinary incontinence increases with advancing age in the general population, 21 postpartum urinary incontinence has not been consistently associated with advancing maternal age. Persson et al. 13 demonstrated that age 25 years at the time of first delivery was a risk factor for future incontinence surgery, but several short-term studies, all with less than one year of follow-up, failed to find a relationship between urinary incontinence and maternal age. 1,3,14,16 Nevertheless, Hatem et al. 15 found that, in primiparous women, maternal age > 35 years was associated with fecal incontinence and with concomitant fecal and urinary incontinence, but not with the development of urinary incontinence alone. Urge urinary incontinence in the postpartum period has been less well studied. The prevalence of urge incontinence in this study is consistent with other reports. 2,11 While maternal age, forceps-assisted delivery, episiotomy, and P length of second stage were identified as risk factors for urge incontinence in univariate analysis, only maternal age remained significant after multivariate analysis. Studies identifying risk factors for postpartum urge urinary in continence are limited. 6,11,12 However, head circumference > 38 cm and concomitant stress incontinence have been reported as risk factors, although these were not specifically examined in our study. 11,12 Many studies examining potential risk factors for postpartum incontinence include any form of incontinence in their analyses. We found that two variables, maternal age and forceps-assisted delivery, were significantly associated with any urinary incontinence. Several authors have noted an increased rate of incontinence in forcepsassisted delivery 3,14,16 ; this may be related to increased nerve and pelvic floor damage occurring during a forceps delivery. However, a few long-term studies failed to show this increased association with forceps delivery. 3,11,21 Our findings support the conclusion that forceps-assisted delivery has a detrimental effect on the urinary continence mechanism in the short term. Our observed rate of fecal incontinence (a prevalence of 4%) after vaginal delivery is consistent with several studies. 6,10,16,17 Several studies have established anal sphincter lacerations as risk factors for fecal incontinence, 5,22,23 although we did not find this relationship in our study. Only recognized third and fourth degree tears were reported in our study, and occult sphincter injuries may have been missed. Also, the number of patients with reported fecal incontinence was small (n = 23, 4%), and this limited our analysis. Sultan et al. reported a small percentage of patients with an intact perineum at delivery who were shown on ultrasound assessment to have internal anal sphincter defects. 4 Forceps delivery as a risk factor for fecal incontinence has been previously reported. 4,17 patients with 40 JANUARY JOGC JANVIER 2009
6 Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery fecal incontinence who had forceps-assisted deliveries were identified in our study, and therefore risk factor analysis was not possible. Often fecal incontinence manifests at a time distant from the injury; therefore, longer follow-up of these patients, which we are pursuing, may be useful. CONCLUSION Urinary incontinence in previously continent patients is common after vaginal delivery. While we found that stress incontinence was the most common type of incontinence present at four months post partum, a significant number of women also developed urge incontinence. The two types of urinary incontinence are inter-related, as are urinary and fecal incontinence. Increased maternal age stands alone as the most significant risk factor for any urinary incontinence. REFERENCES 1. Viktrup L, Lose G, Rolff M, Barfoed K. The symptoms of stress incontinence caused by pregnancy or delivery in primiparas. Obstet Gynecol 1992;79: Wilson P, Herbison R, Herbison G. Obstetric practice and the prevalence of urinary incontinence three months after delivery. Br J Obstet Gynaecol 1996;103: Farrell S, Allen V, Baskett T. Parturition and urinary incontinence in primiparas. Obstet Gynecol 2001;97: Sultan A, Kamm M, Hudson C, Chir M, Thomas J, Bartram C. Anal-sphincter disruption during vaginal delivery. N Eng J Med 1993;329: Snooks S, Swash M, Setchell M, Henry M. Injury to innervation of pelvic floor sphincter musculature in childbirth. Lancet 1984;2(8402): MacLennan A, Taylor A, Wilson DH, Wilson D. The prevalence of pelvic floor disorders and their relationship to gender, age, parity and mode of delivery. BJOG 2000;107: Press JZ, Klein MC, Kaczorowski J, Liston RM, von Dadelszen P. Does Cesarean section reduce postpartum urinary incontinence? A systematic review. Birth 2007;34: Klein MC, Kaczorowski J, Firoz T, Hubinette M, Jorgensen S, Gauthier R. A comparison of urinary and sexual outcomes in women experiencing vaginal and Cesarean births. J Obstet Gynaecol Can 2005;27: Handa VL, Zyczynski HM, Burgio KL, Fitzgerald MP, Borello-France D, Janz NK, et al. The impact of fecal and urinary incontinence on quality of life 6 months after childbirth. Am J Obstet Gynecol 2007;197:636.e Morkved S, Bo K. Prevalence of urinary incontinence during pregnancy and postpartum. Int Urogynecol J Pelvic Floor Dysfunct 1999;10: Viktrup L, Lose G. Lower urinary tract symptoms 5 years after the first delivery. Int Urogynecol J Pelvic Floor Dysfunct 2000;11: Rortveit G, Daltveit A, Hannestad Y, Hunskaar S. Vaginal delivery parameters and urinary incontinence: the rwegian EPINCONT study. Am J Obstet Gynecol 2003;189: Persson J, Wolner-Hanssen P, Rydhstroem H. Obstetric risk factors for stress urinary incontinence: a population-based study. Obstet Gynecol 2000;96(3): Burgio K, Zyczynski H, Locher J, Richter H, Redden D, Wright K. Urinary incontinence in the 12-month postpartum period. Obstet Gynecol 2003;102: Hatem M, Pasquier JC, Fraser W, Lepire E. Factors associated with postpartum urinary/anal incontinence in primiparous women in Quebec. J Obstet Gynaecol Can 2007;29(3): Meyer S, Schreyer A, Grandi P, Hohlfeld A. The effects of birth on urinary continence mechanisms and other pelvic-floor characteristics. Obstet Gynecol 1998;92: MacArthur C, Bick D, Keighley M. Faecal incontinence after childbirth. Br J Obstet Gynaecol 1997;104: Morin K. Urologic consequences of childbirth: a review of the literature. Urol Nurs 1994;14: Creasy RK, Resnik R. Maternal-fetal medicine. 5th ed. Philadelphia PA: Saunders; Lee SJ, Park JW. Follow up evaluation of the effect of vaginal delivery on the pelvic floor. Dis Colon Rectum 2000;43(11): Rortveit G, Dalveit A, Hannestad Y, Hunskaar S. Urinary incontinence after vaginal delivery or cesarean section. N Eng J Med 2003;348: Fenner D, Genberg B, Brahma P, Marek L, DeLancey J. Fecal and urinary incontinence after vaginal delivery with anal sphincter disruption in an obstetrics unit in the United States. Am J Obstet Gynecol 2003;189: Tetzschner T, Sorenson M, Lose G, Christiansen J. Anal and urinary incontinence in women with obstetric anal sphincter rupture. Br J Obstet Gynaecol 1996;103: JANUARY JOGC JANVIER
NEW POSTNATAL URINARY INCONTINENCE : OBSTETRIC AND OTHER RISK FACTORS IN PRIMIPARAE. New postnatal urinary incontinence in primiparae
 Author Posting. The Authors 2006. This is the author s version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in BJOG, 113(2):208-17. doi:10.1111/j.1471-0528.2005.00840.x
Author Posting. The Authors 2006. This is the author s version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in BJOG, 113(2):208-17. doi:10.1111/j.1471-0528.2005.00840.x
Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship?
 DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
Anal incontinence after childbirth is more common than was previously believed. Anal incontinence after childbirth. Methods
 Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Urinary Incontinence after Vaginal Delivery or Cesarean Section
 The new england journal of medicine original article Urinary after Vaginal Delivery or Cesarean Section Guri Rortveit, M.D., Anne Kjersti Daltveit, Ph.D., Yngvild S. Hannestad, M.D., and Steinar Hunskaar,
The new england journal of medicine original article Urinary after Vaginal Delivery or Cesarean Section Guri Rortveit, M.D., Anne Kjersti Daltveit, Ph.D., Yngvild S. Hannestad, M.D., and Steinar Hunskaar,
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
K. Jundt 1, I. scheer 2, v. von Bodungen 1, F. Krumbachner 1, K. Friese 1, U. M. Peschers 3
 362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS
 P.L. Chou, et al ORIGINAL ARTICLE FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS Pei-Ling Chou, Fang-Ping Chen*, Li-Fen Teng Department of Obstetrics and Gynecology, Keelung Chang Gung
P.L. Chou, et al ORIGINAL ARTICLE FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS Pei-Ling Chou, Fang-Ping Chen*, Li-Fen Teng Department of Obstetrics and Gynecology, Keelung Chang Gung
(UI Urine incontinence)! " # $% &'! ( ) * " " +, -. &/ !!" # $%& /'0 = ='' &!( )'*(" &%: "## $ "% % &' ( )* .!
 39/0/5: 39//8:! "#/7 / 6 4 3!!" # $%& /'0 -. (SI Stress incontinence) '' &!( )'*("&%!%!" #$ :!*8>4 &'!% = / ;
39/0/5: 39//8:! "#/7 / 6 4 3!!" # $%& /'0 -. (SI Stress incontinence) '' &!( )'*("&%!%!" #$ :!*8>4 &'!% = / ;
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Screening of Immediate Post Partum Females for Urinary Incontinence Ami Vishal Mehta 1, Zarna
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Screening of Immediate Post Partum Females for Urinary Incontinence Ami Vishal Mehta 1, Zarna
Faecal incontinence persisting after childbirth: a 12 year longitudinal
 Author Posting. The Authors 2013. This is the authors version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obstetrics
Author Posting. The Authors 2013. This is the authors version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obstetrics
Faecal incontinence after childbirth
 Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Urogynaecology. Introduction. M Gyhagen, a M Bullarbo, a,b TF Nielsen, a,b I Milsom a
 DOI: 10.1111/1471-0528.12367 www.bjog.org Urogynaecology A comparison of the long-term consequences of vaginal delivery versus caesarean section on the prevalence, severity and bothersomeness of urinary
DOI: 10.1111/1471-0528.12367 www.bjog.org Urogynaecology A comparison of the long-term consequences of vaginal delivery versus caesarean section on the prevalence, severity and bothersomeness of urinary
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
INTERNATIONAL JOURNAL OF WOMEN'S HEALTH AND REPRODUCTION SCIENCES
 Original Article INTERNATIONAL JOURNAL OF WOMEN'S HEALTH AND REPRODUCTION SCIENCES http://www.ijwhr.net Urinary Incontinence During Pregnancy and Postpartum Incidence, Severity and Risk Factors in Alzahra
Original Article INTERNATIONAL JOURNAL OF WOMEN'S HEALTH AND REPRODUCTION SCIENCES http://www.ijwhr.net Urinary Incontinence During Pregnancy and Postpartum Incidence, Severity and Risk Factors in Alzahra
Stress urinary incontinence 4 years after the first delivery: a retrospective cohort survey.
 Stress urinary incontinence 4 years after the first delivery: a retrospective cohort survey. Xavier Fritel, Arnaud Fauconnier, Caroline Levet, Jean-Louis Bénifla To cite this version: Xavier Fritel, Arnaud
Stress urinary incontinence 4 years after the first delivery: a retrospective cohort survey. Xavier Fritel, Arnaud Fauconnier, Caroline Levet, Jean-Louis Bénifla To cite this version: Xavier Fritel, Arnaud
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study
 ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
Papers. Abstract. Introduction. Methods
 Conservative management of persistent postnatal urinary and faecal incontinence: randomised controlled trial Topic: 66;68;159;161 Cathryn M A Glazener, G Peter Herbison, P Don Wilson, Christine MacArthur,
Conservative management of persistent postnatal urinary and faecal incontinence: randomised controlled trial Topic: 66;68;159;161 Cathryn M A Glazener, G Peter Herbison, P Don Wilson, Christine MacArthur,
Midline episiotomy and anal incontinence: retrospective cohort study
 Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or???
 Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
2/25/2013. Speaker Disclosure. Learning Objectives. Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth
 Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
DOES POST PARTUM PELVIC FLOOR EXERCISES REDUCE ANAL AND URINARY INCONTINENCE?
 DOES POST PARTUM PELVIC FLOOR EXERCISES REDUCE ANAL AND URINARY INCONTINENCE?.* Mohamed El-Negeri', Mohamed Eltotongy \ Maged Elshamy AbdA. Yasser Abdel Dayem'", waleed Omar \ Waleed Thabet Elrefaei, Department
DOES POST PARTUM PELVIC FLOOR EXERCISES REDUCE ANAL AND URINARY INCONTINENCE?.* Mohamed El-Negeri', Mohamed Eltotongy \ Maged Elshamy AbdA. Yasser Abdel Dayem'", waleed Omar \ Waleed Thabet Elrefaei, Department
Operative Vaginal Delivery and Pelvic Floor Trauma. Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center
 + Operative Vaginal Delivery and Pelvic Floor Trauma Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center + Vaginal birth and the pelvic floor Mechanisms of injury Damage to
+ Operative Vaginal Delivery and Pelvic Floor Trauma Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center + Vaginal birth and the pelvic floor Mechanisms of injury Damage to
Among parous women, cesarean birth reduces the
 Pelvic Floor Disorders After Vaginal Birth Effect of Episiotomy, Perineal Laceration, and Operative Birth Victoria L. Handa, MD, MHS, Joan L. Blomquist, MD, Kelly C. McDermott, BS, Sarah Friedman, MD,
Pelvic Floor Disorders After Vaginal Birth Effect of Episiotomy, Perineal Laceration, and Operative Birth Victoria L. Handa, MD, MHS, Joan L. Blomquist, MD, Kelly C. McDermott, BS, Sarah Friedman, MD,
period, cesarean delivery is thought to protect against anal incontinence, 3 albeit incompletely. In this study, we investigated anal incontinence
 Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth
 Int Urogynecol J (8) 19:525 53 DOI.7/s192-7-472-z ORIGINAL ARTICLE The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth Jacobus
Int Urogynecol J (8) 19:525 53 DOI.7/s192-7-472-z ORIGINAL ARTICLE The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth Jacobus
Pregnancy and delivery: a urodynamic viewpoint
 British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1354-1359 Pregnancy and delivery: a urodynamic viewpoint *C. Chaliha Research Fellow (Urogynaecology),** J. M. Bland Professor (Medical
British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1354-1359 Pregnancy and delivery: a urodynamic viewpoint *C. Chaliha Research Fellow (Urogynaecology),** J. M. Bland Professor (Medical
Prevalence and risk factors for pelvic floor symptoms in women in rural El Salvador
 Int Urogynecol J (2007) 18:1065 1069 DOI 10.1007/s00192-006-0292-6 ORIGINAL ARTICLE Prevalence and risk factors for pelvic floor symptoms in women in rural El Salvador Begüm Özel & Anne Marie Borchelt
Int Urogynecol J (2007) 18:1065 1069 DOI 10.1007/s00192-006-0292-6 ORIGINAL ARTICLE Prevalence and risk factors for pelvic floor symptoms in women in rural El Salvador Begüm Özel & Anne Marie Borchelt
Natural progression of anal incontinence after childbirth
 Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
The urethral support system during pregnancy and after childbirth Wijma, Jacobus
 University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Impact of Delivery Types on Women s Postpartum Sexual Health
 Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse
 DOI: 10.1111/1471-0528.12075 www.bjog.org Epidemiology Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse C Glazener, a A Elders, a C MacArthur,
DOI: 10.1111/1471-0528.12075 www.bjog.org Epidemiology Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse C Glazener, a A Elders, a C MacArthur,
NIH Public Access Author Manuscript Int Urogynecol J. Author manuscript; available in PMC 2012 December 06.
 NIH Public Access Author Manuscript Published in final edited form as: Int Urogynecol J. 2011 December ; 22(12): 1491 1495. doi:10.1007/s00192-011-1458-4. URETHRAL CLOSURE PRESSURES AMONG PRIMIPAROUS WOMEN
NIH Public Access Author Manuscript Published in final edited form as: Int Urogynecol J. 2011 December ; 22(12): 1491 1495. doi:10.1007/s00192-011-1458-4. URETHRAL CLOSURE PRESSURES AMONG PRIMIPAROUS WOMEN
Occult anal sphincter injuries myth or reality?
 DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem
 Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Department of Obstetrics and Gynecology, School of Medicine, Pontificia Universidad Catolica de Chile, Santiago, Chile
 Efficacy and Safety of Tension-Free Vaginal Tape Compared With Transobturator Tape Among Obese Women With Stress Urinary Incontinence: A Retrospective Cohort Study Victor Miranda, MD, MSc, 1,2 Rodrigo
Efficacy and Safety of Tension-Free Vaginal Tape Compared With Transobturator Tape Among Obese Women With Stress Urinary Incontinence: A Retrospective Cohort Study Victor Miranda, MD, MSc, 1,2 Rodrigo
In healthy young women, anal sphincter tear at
 Risk Factors for Anal Sphincter Tear During Vaginal Delivery Mary P. FitzGerald, MD, Anne M. Weber, MD, MS, Nancy Howden, MD, MS, Geoffrey W. Cundiff, MD, and Mort B. Brown, PhD, for the Pelvic Floor Disorders
Risk Factors for Anal Sphincter Tear During Vaginal Delivery Mary P. FitzGerald, MD, Anne M. Weber, MD, MS, Nancy Howden, MD, MS, Geoffrey W. Cundiff, MD, and Mort B. Brown, PhD, for the Pelvic Floor Disorders
The effect of pregnancy and mode of delivery on the prevalence of urinary and fecal incontinence
 American Journal of Obstetrics and Gynecology (2005) 193, 512 8 www.ajog.org The effect of pregnancy and mode of delivery on the prevalence of urinary and fecal incontinence Vikki McKinnie, MD, a Steven
American Journal of Obstetrics and Gynecology (2005) 193, 512 8 www.ajog.org The effect of pregnancy and mode of delivery on the prevalence of urinary and fecal incontinence Vikki McKinnie, MD, a Steven
Association between mode of delivery and pelvic floor dysfunction
 Review article Association between mode of delivery and pelvic floor dysfunction 1848 52 BACKGROUND Normal vaginal delivery can cause significant strain on the pelvic floor. We present a review of the
Review article Association between mode of delivery and pelvic floor dysfunction 1848 52 BACKGROUND Normal vaginal delivery can cause significant strain on the pelvic floor. We present a review of the
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
TRENDS IN MAJOR RISK FACTORS FOR ANAL SPHINCTER LACERATIONS: A I 0-YEAR STUDY
 TRENDS IN MAJOR RISK FACTORS FOR ANAL SPHINCTER LACERATIONS: A I 0-YEAR STUDY N. L. McLeod, MD, FRCSC, I D. T. Gilmour, MD, FRCSC, 2 K. S. Joseph, MD, PhD, 3 S. A. Farrell, MD, FRCSC,4 E. R. Luther, MD,
TRENDS IN MAJOR RISK FACTORS FOR ANAL SPHINCTER LACERATIONS: A I 0-YEAR STUDY N. L. McLeod, MD, FRCSC, I D. T. Gilmour, MD, FRCSC, 2 K. S. Joseph, MD, PhD, 3 S. A. Farrell, MD, FRCSC,4 E. R. Luther, MD,
Effects of Combined Pelvic Floor Muscle Exercises in Patient with Urinary Incontinence
 MACROJOURNALS The Journal of MacroTrends in Health and Medicine Effects of Combined Pelvic Floor Muscle Exercises in Patient with Urinary Incontinence Vjollca Ndreu*, Fatjona Kamberi*, Enkeleda Sinaj*,
MACROJOURNALS The Journal of MacroTrends in Health and Medicine Effects of Combined Pelvic Floor Muscle Exercises in Patient with Urinary Incontinence Vjollca Ndreu*, Fatjona Kamberi*, Enkeleda Sinaj*,
The urethral support system during pregnancy and after childbirth Wijma, Jacobus
 University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
Does delayed child-bearing increase the risk of levator injury in labour?
 Australian and New Zealand Journal of Obstetrics and Gynaecology 2007; 47: 491 495 Blackwell Publishing Asia Original Article Delayed child-bearing and levator injury Does delayed child-bearing increase
Australian and New Zealand Journal of Obstetrics and Gynaecology 2007; 47: 491 495 Blackwell Publishing Asia Original Article Delayed child-bearing and levator injury Does delayed child-bearing increase
The Pelvic Floor: Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology
 The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
Vincent Letouzey, MD, PhD
 How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
It is well established that the development of
 Obstetrics Risk Estimation of Metabolic Syndrome at One and Three Years After a Pregnancy Complicated by Graeme N. Smith, MD, PhD, 1,2 Jessica Pudwell, MPH, 1,2 Mark Walker, MD, MSc, 3 Shi-Wu Wen, MB,
Obstetrics Risk Estimation of Metabolic Syndrome at One and Three Years After a Pregnancy Complicated by Graeme N. Smith, MD, PhD, 1,2 Jessica Pudwell, MPH, 1,2 Mark Walker, MD, MSc, 3 Shi-Wu Wen, MB,
Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England,
 DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION. Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital
 ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
Interventions METHODS
 Prevention of postpartum stress incontinence PREVENTION OF POSTPARTUM STRESS INCONTINENCE 69 There is good evidence that postnatal pelvic floor exercises are effective in the treatment of postpartum stress
Prevention of postpartum stress incontinence PREVENTION OF POSTPARTUM STRESS INCONTINENCE 69 There is good evidence that postnatal pelvic floor exercises are effective in the treatment of postpartum stress
Retrospective Review of Predisposing Factors and Surgical Outcomes in Obstetric Fistula Patients at a Single Teaching Hospital in Western Kenya
 GYNAEcOLOGY Retrospective Review of Predisposing Factors and Surgical Outcomes in Obstetric Fistula Patients at a Single Teaching Hospital in Western Kenya Erin McFadden, MD, 1 Sarah Jane Taleski, MHSc,
GYNAEcOLOGY Retrospective Review of Predisposing Factors and Surgical Outcomes in Obstetric Fistula Patients at a Single Teaching Hospital in Western Kenya Erin McFadden, MD, 1 Sarah Jane Taleski, MHSc,
Birth Trauma. H. P. Dietz. University of Sydney, Nepean Campus. Penrith, Australia
 Birth Trauma H. P. Dietz University of Sydney, Nepean Campus Penrith, Australia Procedures in US (2010): 1.6 Prolapse Urinary Incontinence Fecal Incontinence Prolapse 200.000 Urinary Incontinence 120.000
Birth Trauma H. P. Dietz University of Sydney, Nepean Campus Penrith, Australia Procedures in US (2010): 1.6 Prolapse Urinary Incontinence Fecal Incontinence Prolapse 200.000 Urinary Incontinence 120.000
Postpartum pelvic floor function performance after two different modes of delivery
 after two different modes of delivery H. Li 1,2, R.F. Wu 1,2, F. Qi 1,2, A.M. Xiao 1,2, Z. Ma 1,2, Y. Hu 1,2, W.Y. Zhang 1,2, W. Li 1,2 and Z.C. Wang 1,2 1 Department of Gynaecology, The Shenzhen Hospital,
after two different modes of delivery H. Li 1,2, R.F. Wu 1,2, F. Qi 1,2, A.M. Xiao 1,2, Z. Ma 1,2, Y. Hu 1,2, W.Y. Zhang 1,2, W. Li 1,2 and Z.C. Wang 1,2 1 Department of Gynaecology, The Shenzhen Hospital,
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Female pelvic floor anatomy is discussed in detail separately. (See "Surgical female urogenital anatomy".)
 Official reprint from UpToDate www.uptodate.com 2017 UpToDate Urinary incontinence and pelvic organ prolapse associated with pregnancy and childbirth Author: Victoria L Handa, MD Section Editor: Linda
Official reprint from UpToDate www.uptodate.com 2017 UpToDate Urinary incontinence and pelvic organ prolapse associated with pregnancy and childbirth Author: Victoria L Handa, MD Section Editor: Linda
How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial
 DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
A systematic review of etiological factors for postpartum fecal incontinence
 Acta Obstetricia et Gynecologica. 2010; 89: 302 314 ACTA REVIEW A systematic review of etiological factors for postpartum fecal incontinence ESTHER M.J. BOLS 1,2, ERIK J.M. HENDRIKS 1,2, BARY C.M. BERGHMANS
Acta Obstetricia et Gynecologica. 2010; 89: 302 314 ACTA REVIEW A systematic review of etiological factors for postpartum fecal incontinence ESTHER M.J. BOLS 1,2, ERIK J.M. HENDRIKS 1,2, BARY C.M. BERGHMANS
EXPECTING A BABY? SOME PREGNANT WOMEN CAN HAVE BLADDER AND BOWEL CONTROL PROBLEMS. YOU CAN GET HELP. HOW DO I KNOW IF I HAVE A PROBLEM?
 11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
Women s and Men s Health Intake Form Comprehensive Physical Therapy Center
 Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
The development of a questionnaire to measure the severity of symptoms and the quality of life before and after surgery for stress incontinence
 BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
Effect of postpartum pelvic floor muscle training in prevention and treatment of urinary incontinence: a one-year follow up
 British Journal of Obstetrics and Gynaecology August 2000, V01107, pp. 1022-1028 Effect of postpartum pelvic floor muscle training in prevention and treatment of urinary incontinence: a one-year follow
British Journal of Obstetrics and Gynaecology August 2000, V01107, pp. 1022-1028 Effect of postpartum pelvic floor muscle training in prevention and treatment of urinary incontinence: a one-year follow
Vaginal Parity and Pelvic Organ Prolapse
 The Journal of Reproductive Medicine Vaginal Parity and Pelvic Organ Prolapse Lieschen H. Quiroz, M.D., Alvaro Muñoz, Ph.D., Stuart H. Shippey, M.D., Robert E. Gutman, M.D., and Victoria L. Handa, M.D.
The Journal of Reproductive Medicine Vaginal Parity and Pelvic Organ Prolapse Lieschen H. Quiroz, M.D., Alvaro Muñoz, Ph.D., Stuart H. Shippey, M.D., Robert E. Gutman, M.D., and Victoria L. Handa, M.D.
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Pregnancy and childbirth: the effects on pelvic floor muscles
 Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Frequency of urinary incontinence with Pelvic organ prolapse and associated factors
 ORIGINAL ARTICLE Frequency of urinary incontinence with Pelvic organ prolapse and associated factors Dr. Raheela Mohsin 1, Dr.Ayesha Saba 2, Humera Ismail 3 1 Dr. Raheela Mohsin, Aga Khan University Hospital,
ORIGINAL ARTICLE Frequency of urinary incontinence with Pelvic organ prolapse and associated factors Dr. Raheela Mohsin 1, Dr.Ayesha Saba 2, Humera Ismail 3 1 Dr. Raheela Mohsin, Aga Khan University Hospital,
A Review of the Concordance of Diagnoses Made After Multi-Channel Urodynamics and Video Urodynamics in Women With Urinary Incontinence
 WOMEN'S HEALTH A Review of the Concordance of Diagnoses Made After Multi-Channel Urodynamics and Video Urodynamics in Women With Urinary Incontinence Jane A. Schulz, MD, 1 Kevin M. Smith, MB BCh, 2 Harold
WOMEN'S HEALTH A Review of the Concordance of Diagnoses Made After Multi-Channel Urodynamics and Video Urodynamics in Women With Urinary Incontinence Jane A. Schulz, MD, 1 Kevin M. Smith, MB BCh, 2 Harold
= 0.002) 117 #!. 12, : = 0.45; P
 Background: Psychosocial factors governing the use of postoperative, intravenous patient-controlled analgesia (PCA) have received little attention in spite of the fact that PCA is the most common modality
Background: Psychosocial factors governing the use of postoperative, intravenous patient-controlled analgesia (PCA) have received little attention in spite of the fact that PCA is the most common modality
Pelvic floor education for new mothers: timing the message for best effect
 Commonwealth Department of Health and Aged Care National Continence Management Strategy Innovative Grants Program Pelvic floor education for new mothers: timing the message for best effect Nicole Tweddle
Commonwealth Department of Health and Aged Care National Continence Management Strategy Innovative Grants Program Pelvic floor education for new mothers: timing the message for best effect Nicole Tweddle
Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes?
 Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes? Lawrence M. Leeman, MD, Rebecca G. Rogers, MD, Betsy Greulich, CNM, and Leah L. Albers, DrPH Background: To compare
Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes? Lawrence M. Leeman, MD, Rebecca G. Rogers, MD, Betsy Greulich, CNM, and Leah L. Albers, DrPH Background: To compare
URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS- SECTIONAL STUDY
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Aisha et al. SJIF Impact Factor 6.647 Volume 6, Issue 9, 1384-1391 Research Article ISSN 2278 4357 URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS-
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Aisha et al. SJIF Impact Factor 6.647 Volume 6, Issue 9, 1384-1391 Research Article ISSN 2278 4357 URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS-
Mode of delivery and fecal incontinence at midlife: a study of 2,640 women in the Gazel cohort Fritel Xavier
 Mode of delivery and fecal incontinence at midlife: a study of 2,640 women in the Gazel cohort Fritel Xavier 1 *, Ringa Virginie 1, Varnoux Noëlle 1, Zins Marie 2 3, Bréart 1 Gérard 1 Recherches épidémiologiques
Mode of delivery and fecal incontinence at midlife: a study of 2,640 women in the Gazel cohort Fritel Xavier 1 *, Ringa Virginie 1, Varnoux Noëlle 1, Zins Marie 2 3, Bréart 1 Gérard 1 Recherches épidémiologiques
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
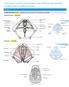 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
Pudendal Block and Urinary Dysfunction/Retention
 Date of Search: 22 Mar 17 Sources Searched: Medline, Embase, Cinahl, Google Scholar DISCLAIMER: Results of database and or Internet searches are subject to the limitations of both the database(s) searched,
Date of Search: 22 Mar 17 Sources Searched: Medline, Embase, Cinahl, Google Scholar DISCLAIMER: Results of database and or Internet searches are subject to the limitations of both the database(s) searched,
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
THE EFFECT OF AGE AND SAFETY MARGIN ON LOCAL RECURRENCE AND SURVIVAL AFTER BREAST CONSERVATIVE SURGERY FOR EARLY BREAST CANCER
 Copyright 2017 Balkan Medical Union vol. 52, no. 2, pp. 176-180 June 2017 ORIGINAL PAPER THE EFFECT OF AGE AND SAFETY MARGIN ON LOCAL RECURRENCE AND SURVIVAL AFTER BREAST CONRVATIVE SURGERY FOR EARLY BREAST
Copyright 2017 Balkan Medical Union vol. 52, no. 2, pp. 176-180 June 2017 ORIGINAL PAPER THE EFFECT OF AGE AND SAFETY MARGIN ON LOCAL RECURRENCE AND SURVIVAL AFTER BREAST CONRVATIVE SURGERY FOR EARLY BREAST
Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women who sustained a previous obstetric anal sphincter injury
 International Urogynecology Journal (2018) 29:1579 1588 https://doi.org/10.1007/s00192-018-3601-y ORIGINAL ARTICLE Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women
International Urogynecology Journal (2018) 29:1579 1588 https://doi.org/10.1007/s00192-018-3601-y ORIGINAL ARTICLE Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
This is the author's version of the work. It is posted here for personal use, not for
 1 This is the author's version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obsterics and Gynaecology 2013; DOI: 10.1111/1471-0528.12473
1 This is the author's version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obsterics and Gynaecology 2013; DOI: 10.1111/1471-0528.12473
Enuresis in childhood, and urinary and fecal incontinence in adult life: do they share a common cause?
 Original Article ENURESIS AND URINARY AND FECAL INCONTINENCE GURBUZ et al. Enuresis in childhood, and urinary and fecal incontinence in adult life: do they share a common cause? AYSE GURBUZ, ATES KARATEKE
Original Article ENURESIS AND URINARY AND FECAL INCONTINENCE GURBUZ et al. Enuresis in childhood, and urinary and fecal incontinence in adult life: do they share a common cause? AYSE GURBUZ, ATES KARATEKE
Introduction. A joint report by IUGA and the ICS 1 defines anal incontinence (AI) as the unintentional loss of faeces or flatus.
 TD Naidoo J Moodley Introduction A joint report by IUGA and the ICS 1 defines anal incontinence (AI) as the unintentional loss of faeces or flatus. Faecal incontinence is a complaint of involuntary loss
TD Naidoo J Moodley Introduction A joint report by IUGA and the ICS 1 defines anal incontinence (AI) as the unintentional loss of faeces or flatus. Faecal incontinence is a complaint of involuntary loss
The Perineal Clinic: - the management of women following OASI
 The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
Birth trauma: short and long term effects of forceps delivery compared with spontaneous delivery on various pelvic floor parameters
 British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1360-1365 Birth trauma: short and long term effects of forceps delivery compared with spontaneous delivery on various pelvic floor
British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1360-1365 Birth trauma: short and long term effects of forceps delivery compared with spontaneous delivery on various pelvic floor
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
A non-invasive, safe and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1
 A non-invasive, safe and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1 INNOVO INNOVO has changed my life for the better. I no longer
A non-invasive, safe and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1 INNOVO INNOVO has changed my life for the better. I no longer
PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE?
 PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE? Kathy Curry, PT, DPT Physical Therapy Today Pelvic Health Physical Therapy () Objectives: Discuss components of pelvic
PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE? Kathy Curry, PT, DPT Physical Therapy Today Pelvic Health Physical Therapy () Objectives: Discuss components of pelvic
restore the pelvic floor
 restore the pelvic floor A non-invasive, safe, and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1 has changed my life for the better.
restore the pelvic floor A non-invasive, safe, and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1 has changed my life for the better.
ijer.skums.ac.ir Risk factors of pelvic organ prolapse in Iranian women: a cross-sectional study
 International Journal of Epidemiologic Research, 2014; 1 (1): 29-34. ijer.skums.ac.ir Risk factors of pelvic organ prolapse in Iranian women: a cross-sectional study Ashraf Direkvand-Moghadam 1 ; Zeinab
International Journal of Epidemiologic Research, 2014; 1 (1): 29-34. ijer.skums.ac.ir Risk factors of pelvic organ prolapse in Iranian women: a cross-sectional study Ashraf Direkvand-Moghadam 1 ; Zeinab
Fertility Treatment Decision-Making: The Effect of Insurance Coverage for Fertility Medications
 GYNAECOLOGY Fertility Treatment Decision-Making: The Effect of Insurance Coverage for Fertility Medications Claire Ann Jones, MD, 1 Laura Gra, hd, 2 Kimberl Liu, MD, FRCSC, MSL 1,3 1 Department of Obstetrics
GYNAECOLOGY Fertility Treatment Decision-Making: The Effect of Insurance Coverage for Fertility Medications Claire Ann Jones, MD, 1 Laura Gra, hd, 2 Kimberl Liu, MD, FRCSC, MSL 1,3 1 Department of Obstetrics
Impact of Patient Education on Knowledge of Influenza and Vaccine Recommendations Among Pregnant Women
 OBSTETRICS OBSTETRICS Impact of Patient Education on Knowledge of Influenza and Vaccine Recommendations Among Pregnant Women Mark H. Yudin, MD, MSc, 1 Maryam Salripour, BSc, CIC, MPH, 2 Michael D. Sgro,
OBSTETRICS OBSTETRICS Impact of Patient Education on Knowledge of Influenza and Vaccine Recommendations Among Pregnant Women Mark H. Yudin, MD, MSc, 1 Maryam Salripour, BSc, CIC, MPH, 2 Michael D. Sgro,
Perineometer as a strength assessment & training tool for pelvic floor muscles in stress urinary incontinent elderly women
 Original article: Perineometer as a strength assessment & training tool for pelvic floor muscles in stress urinary incontinent elderly women Dr. Shwetanjali Gandhe, Dr. Shyam Ganvir 1MPT student, Dept.
Original article: Perineometer as a strength assessment & training tool for pelvic floor muscles in stress urinary incontinent elderly women Dr. Shwetanjali Gandhe, Dr. Shyam Ganvir 1MPT student, Dept.
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider.
 Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Leaking Urine: Prevalence and Associated Factors in Australian Women
 Neurourology and Urodynamics 18:567 577 (1999) Leaking Urine: Prevalence and Associated Factors in Australian Women Pauline Chiarelli, 1 Wendy Brown, 2 * and Patrick McElduff 3 1 Faculty of Medicine and
Neurourology and Urodynamics 18:567 577 (1999) Leaking Urine: Prevalence and Associated Factors in Australian Women Pauline Chiarelli, 1 Wendy Brown, 2 * and Patrick McElduff 3 1 Faculty of Medicine and
Obstetric anal sphincter injury is the most common
 Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
PRE-OPERATIVE URODYNAMIC
 PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
Duloxetine in women awaiting surgery
 DOI: 1.1111/j.1471-528.6.879.x www.blackwellpublishing.com/bjog Review article H Drutz Ontario Power Generation Building, Toronto, Ontario, Canada Correspondence: Prof. Dr H Drutz, Mount Sinai Hospital,
DOI: 1.1111/j.1471-528.6.879.x www.blackwellpublishing.com/bjog Review article H Drutz Ontario Power Generation Building, Toronto, Ontario, Canada Correspondence: Prof. Dr H Drutz, Mount Sinai Hospital,
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
