The evaluation and management of acute musculoskeletal
|
|
|
- Asher Little
- 5 years ago
- Views:
Transcription
1 ONLINE EXCLUSIVE George E. Eldayrie, MD; Kristy Smith, MD; Michael Seth Smith, MD, CAQSM, PharmD Department of Community Health and Family Medicine (Drs. Eldayrie and K. Smith) and Department of Orthopedics and Rehabilitation (Dr. MS Smith), University of Florida, Gainesville Adult foot : A guide This review can help you refine your approach to the diagnosis and management of adult foot, while offering guidance on when to pursue advanced imaging. smithms@ortho.ufl.edu The authors reported no potential conflict of interest relevant to this article. PRACTICE RECOMMENDATIONS Manage most of the proximal fifth metatarsal metaphyseal-diaphyseal junction (Jones fracture) conservatively with appropriate treatment and close follow-up; refer for early surgical evaluation only those patients who are highly active and who are interested in a faster return to activity. B Use the Ottawa Ankle and Foot Rules to determine whether x-rays are needed in a patient with foot pain and a suspected fracture. A Start with weight-bearing x-rays and then consider computed tomography or magnetic resonance imaging for complete evaluation of suspected injury to the Lisfranc joint. C Strength of recommendation (SOR) A Good-quality patient-oriented evidence B Inconsistent or limited-quality patient-oriented evidence C Consensus, usual practice, opinion, disease-oriented evidence, case series The evaluation and management of acute musculoskeletal conditions are frequently handled by primary care providers. 1 It s estimated that up to 14% of orthopedic complaints encountered by family physicians involve, 2 and approximately 15% of these are foot. 2 Diagnosis requires radiographic evaluation, but ultrasound is proving useful, too. This article reviews the diagnosis and management of adult foot, with an emphasis on when advanced imaging and referral are indicated (TABLE 1,3-10 ). Phalanx : The most common foot Phalanx typically occur by crush injury, hyperextension, or direct axial force (eg, stubbing the toe). 3 Patients with phalanx typically present with pain at or near the site of injury, edema, ecchymosis, and erythema. Throbbing pain is characteristic, and dependent position may worsen the pain. 1 Emergently evaluate any fracture causing tenting of the skin, protrusion from the skin, or neurovascular compromise, and attempt realignment to regain neurovascular function. Most patients with phalanx have point tenderness over the site of the fracture; however, this may also occur with contusions. Placing a gentle loading force along the long axis of the bone distal to the injury may help you differentiate between a contusion and a fracture. 4 Pain observed with axial loading of the bone during examination points to a fracture rather than a contusion. Differential diagnosis Obtain imaging, including anterior-posterior (AP), lateral, and oblique views at a minimum, for all patients in whom you suspect. 5 Multiple of the phalanges are common; therefore, always thoroughly examine the phalanges adjacent to the injured one. Sesamoid bone are uncommon but do occur and are usually due to direct injury from jumping or landing. The E8 THE JOURNAL OF FAMILY PRACTICE NOVEMBER 2018 VOL 67, NO 11
2 TABLE Foot : How to manage, when to refer Fracture type Great toe Second to fifth phalanx Metatarsal shaft Fifth metatarsal tuberosity avulsion Fifth metatarsal Jones Lisfranc injury Mechanism of injury Crush, axial force, hyperextension 1,3,4 Crush, axial force, hyperextension 1,3 Direct crush, indirect rotation with forefoot flexed, and hindfoot or leg rotated 1,3 Ankle inversion (commonly with lateral ankle sprain) 1,3 Direct crush, ankle inversion 1 Axial load on plantar-flexed forefoot 1 Radiology Treatment Follow-up Indications for surgical referral / toe (AP, lateral, and oblique) 1,3,5 / toe (AP, lateral, and oblique) 1,3,5 oblique). MRI if stress fracture suspected 1,3,5 oblique) 1,3,5 oblique). MRI if stress fracture suspected 1,5 oblique) first. Weight bearing comparison views. CT/MRI if highly suspect and normal plain films 1,5 Short leg walking boot for 2-3 wks, then rigid shoe for 3-4 wks 1,3,4 Buddy taping and rigid-soled shoes for 4-6 wks 1,3 Posterior splint for 3-5 days to allow swelling to improve, NWB crutches. Then short leg walking cast/boot or hard sole shoe for 4-6 wks 1,3 Weight bearing as tolerated, short leg walking boot/ cast for 2 wks or hard sole shoe for 4-8 wks, progressive ROM 1,3 Posterior splint and NWB for 3-5 days to allow swelling to improve, then short leg NWB cast for 6-8 wks. If evidence of healing, then progress to walking boot and weight bearing. If no evidence of healing, then continued cast for 4 additional wks 1,3 Nonsurgical management is recommended only for patients who are not surgical candidates. This includes immobilization in a short leg cast for 8 wks and NWB 1 1 wk with repeat imaging. Every 2-4 weeks if fracture is intra-articular or requires reduction 1,3,4 1-2 wks with repeat imaging if intra-articular or required reduction. Then every 2-4 wks 1,3 1 wk with repeat imaging and again at 4-6 wks 1,3 Every 2-4 wks, repeat x-rays if continued pain 1,3 1 wk with repeat imaging at cast placement after splinting, then at 6-8 wks 1 Referral to surgical specialists is strongly indicated. Repeat imaging can be decided by surgical specialist 1 Fractures involving >25% of joint space, open, fracture dislocations, neurovascular compromise 1,3,4 Angulation >25 in dorsoplantar plane, >10 in mediolateral plane, rotation >20, involving >25% of joint space, open, fracture dislocations, neurovascular compromise 1,3 First metatarsal: Open, displaced, angulated, or intra-articular ; that cause neurovascular compromise. Lesser metatarsals: First metatarsal indications and multiple, dorsoplantar displacement >3 mm, dorsoplantar angulation >10 1,3 Displaced fracture >3 mm, step-off >1 mm over the cuboid surface, or fracture involving >60% of metatarsal cuboid joint surface 1,3 Failure to achieve healing with wks of nonsurgical management. Elite athletes or very active individuals may opt for surgical management, as this may shorten the treatment course 1,3 Majority of cases should be managed surgically, especially for those with any evidence of instability of the joint. Reserve nonsurgical treatment for patients who are not good surgical candidates due to pre-existing conditions or who are nonambulatory 1 CONTINUED MDEDGE.COM/JFPONLINE VOL 67, NO 11 NOVEMBER 2018 THE JOURNAL OF FAMILY PRACTICE E9
3 TABLE Foot : How to manage, when to refer (cont'd) Fracture type Cuboid Cuneiform Navicular Calcaneus Mechanism of injury High-velocity direct trauma, foot inversion with external rotation of the tibia, direct blow, or axial load on a plantar-flexed heel 1 Direct impact, axial loading on dorsiflexed or plantar-flexed foot with rotational force, or severe rotation of the midfoot in a fixed foot 1 Twisting force with foot in plantar flexion may cause avulsion. Tuberosity occur from eversion force. Body occur from hyperextension, direct trauma, flexion with rotation 1 Extra-articular occur from falls from height and landing on the heel. Forceful abduction of the forefoot can cause compression of the anterior calcaneal surface 1 Radiology Treatment Follow-up Indications for surgical referral (AP, lateral, and oblique). Consider weightbearing view if there is concern for Lisfranc ligament complex involvement 1,5 (AP, lateral, and oblique). Consider weightbearing view if there is concern for Lisfranc ligament complex involvement 1,5 oblique). MRI if stress fracture is highly suspected despite normal plain films 1,5 Lateral, axial and dorsoplantar view 1,5 Short leg walking cast/boot for 6 wks, then transition to rigid sole shoe for additional 6 wks. Stress can be managed with NWB crutches for 2 weeks, then transition to walking boot, as tolerated 1,7 Short leg walking cast/boot for 6 wks, then rigid-sole shoe for additional 6 wks 1,6,8 Dorsal avulsion fracture: Short leg walking cast/boot for 6-8 wks. Tuberosity fracture: Short leg walking cast/boot for 4-6 wks. Body fracture: Below-the-knee walking cast for 6-8 wks, then longitudinal arch support 1,9 Anterior, medial, or lateral process : Short leg walking cast/ boot for 4-6 wks. Tuberosity : Short leg NWB cast with 5-10 equinus for 6-8 wks. Body: Active exercise 1,10 There is no consensus on follow-up, but every 2-4 wks is appropriate. Consider repeating imaging at 6 wks if pain continues There is no consensus on follow-up, but every 2-4 wks is appropriate. Consider repeating imaging at 6 wks if pain continues Repeat radiographs after 4-6 wks of immobilization. If nonunion at 6 wks, continue immobilization for 2-4 wks. For body, repeat imaging at 6 wks and every 2-4 wks until union is seen 1,9 After immobilization, repeat plain films to document healing at 4-6 wks for anterior, medial, or lateral process, and after 6-8 weeks for tuberosity. Then transition to formal physical therapy for foot and ankle ROM and strengthening 1,10 AP, anterior-posterior; CT, computed tomography; MRI, magnetic resonance imaging; NWB, non-weight bearing; ROM, range of motion. Severe comminution, displacement, or fracture with concomitant dislocation. >2 mm step-off 1,7 Severe comminution, displacement, or fracture with concomitant dislocation. >2 mm step-off 1,6,8 Large displaced dorsal avulsion involving >20% of talonavicular articular surface; tuberosity with >1 cm displacement proximally; any displaced body fracture; after 10 wks of nonoperative treatment and evidence of nonunion 1,9 Open, intra-articular, or subtalar ; with significant displacement or chronic pain or nonunion after conservative treatment; significantly displaced causing widening of the heel 1,10 most common sesamoid to be injured is the medial sesamoid of the great toe, although the lateral sesamoid can also be injured. Bipartite sesamoids can occur and may confuse the examiner due to their similar appearance on x-rays to a sesamoid fracture. 1 These normal variants often appear smooth and are commonly bilateral as opposed to the jagged or E10 THE JOURNAL OF FAMILY PRACTICE NOVEMBER 2018 VOL 67, NO 11
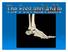
4 ADULT FOOT FRACTURES abrupt edges of a fracture. Stress occur as well and are typically due to overusetype injuries. Other causes of pain similar to that experienced with phalanx include soft tissue injuries to adjacent ligaments, tendons, and muscles. To help discern the cause of pain, evaluate nail beds for subungual hematomas, indicating injury to the nail bed causing bleeding and pressure under the nail. Obvious deformities of the toes or metatarsal-phalangeal joints signal the possibility of a fracture-dislocation. First metatarsophalangeal (MTP) sprain ( turf toe, a condition common in athletes who hyperextend the toe, such as when pushing off from hard surfaces like turf) and gout can also present with acute pain in the first phalanx. Treatment Due to the role of the great toe in weight bearing and balance, great toe are sometimes managed differently than in Toes 2 through 5. Proper alignment and healing from a fracture in the first toe are critical to prevent future pain and other sequelae. Refer for orthopedic evaluation great toe with displacement, angulation, rotational deformity, neurovascular compromise, >25% involvement of the joint space, or obvious dislocation. 1 If referral is not indicated, treat great toe with a short leg walking cast/boot for 2 to 3 weeks followed by buddy taping and use of a hard-soled shoe for 3 to 4 weeks. 1 With regard to the lesser toes, refer patients with fracture-dislocations, displaced intra-articular, and that do not reduce easily. Nondisplaced of the lesser toes do not require surgical referral. 1 These can be treated with splinting (buddy taping) and use of rigid-sole shoes for 4 to 6 weeks. Treatment duration depends largely on patient compliance; generally, continue treatment until point tenderness resolves. 1 Treatment of sesamoid consists of resting the affected foot with a walking boot, hard-soled shoe, or donut pad under the sesamoid bone to help distribute weight on the foot when standing. Length of treatment is approximately 6 to 8 weeks for most. 1 Consider surgical referral if nonoperative management is unsuccessful. Metatarsal : Look for malalignment Metatarsal account for 5% of all foot encountered in primary care. 2 These typically occur as a result of falls, direct trauma, or rotational injuries (eg, ankle and foot sprains). 1 In athletes, the most common cause of these is high rotational force. Patients typically present with pain over the injury site, swelling, bruising, and pain with weight bearing. As part of your exam, look for malalignment, rotational deformities, and evidence of open fracture. Palpation at the site of the fracture may increase the pain; however, as is true with phalanx, contusions may also cause significant tenderness upon palpation. Also assess range of motion with special attention to signs of malrotation and evaluate the adjacent metatarsals, as multiple bones, ligaments, or both are often involved. 1 Fifth metatarsal are the most common in adults, likely because of decreased cortical thickness as compared with the other metatarsals. 3,11 In addition, multiple soft tissue attachments connect at the proximal aspect of the fifth metatarsal. Classification of these types of metatarsal is based on anatomic location. 3 Jones are one type of fracture at the proximal aspect of the fifth metatarsal that occur at the metaphyseal-diaphyseal junction specifically (FIGURE 1). Because this area receives its blood supply from small terminal vessels, here have a high risk of non-union and, thus, should be top of mind in any patient with tenderness at the base of the fifth metatarsal. MRI/ultrasound in addition to plain films? Use the Ottawa Ankle and Foot Rules to determine the need for foot radiographs in the acute setting. 12 If indicated, imaging should include AP, lateral, and oblique views of the foot. 5 Consider magnetic resonance imaging (MRI) if you suspect a stress fracture, which typically presents as an overuse injury in athletes. Ultrasound may be effective for identifying metatarsal, as well. 13 Ultrasound can be used to visualize of the long Ultrasound can be used to visualize of the long bones and to identify displacement, angulation, and step-offs. MDEDGE.COM/JFPONLINE VOL 67, NO 11 NOVEMBER 2018 THE JOURNAL OF FAMILY PRACTICE E11
5 Manage stress and stress reactions of the proximal fifth metatarsal with strict activity modifications and a non-weight bearing short leg cast, given the high risk of nonunion. PHOTO COURTESY OF: MICHAEL SETH SMITH, MD, CAQSM, PharmD FIGURE 1 Proximal fifth metatarsal Jones fracture metatarsal bones and identify displacement, angulation, and step-offs. Although its use in the United States has been limited for this purpose, studies in other countries are showing that it yields results comparable to plain films in the emergency department setting for diagnosis and initial management of these. 13 Differential diagnosis Multiple other diagnoses present similarly to metatarsal including: ligamentous/tendon/soft tissue injuries, interdigital neuroma, sesamoid, and Lisfranc ligament injury (which we'll discuss in a bit). Stress of the metatarsal, most commonly seen in the second metatarsal, are insidious in nature and are common with repetitive movement such as that made by gymnasts, dancers, and track athletes. 14 Metatarsalgia, which causes pain at the ball of the foot, is a condition that can stem from a myriad of causes including a low or high arch, biomechanics, and previous injury. Treatment Nondisplaced, minimally displaced (<3 mm), and minimally angulated (<10 dorsal/ plantar angulation) of any metatarsal shaft may be managed conservatively with a hard-soled shoe or walking boot with weight bearing as tolerated for 4 to 6 weeks. 1 Most stress (excluding fifth metatarsal stress ) may be treated similarly. Surgical referral is indicated for patients with any open fracture, first metatarsal with displacement, central metatarsal with >10 deformity, >3 mm of translation, multiple, or fifth metatarsal stress fracture. 1 Base of fifth metatarsal tuberosity avulsion can be managed nonoperatively with protected weight bearing in a boot or cast for 2 weeks or hard sole shoe for 4 to 8 weeks if the fracture is at the proximal tubercle (see Zone I, FIGURE 2). Jones (Zone II, FIGURE 2) or of the proximal diaphysis (Zone III, FIGURE 2) of the fifth metatarsal may also be managed nonoperatively in patients who are not competitive athletes. This can be done with a non-weight bearing (NWB) short leg cast for 6 to 8 weeks at a minimum. 4 If the patient is an athlete who wishes to resume competition, surgical referral is indicated, as the risk of nonunion is high with these. 15 Stress and stress reactions (early evidence of bone edema seen on MRI, indicating progression to stress fracture) of the proximal fifth metatarsal should be managed with strict activity modifications and a NWB short leg cast for 6 to 8 weeks, given the high risk of nonunion. Midfoot : The cuboid, cuneiforms, and navicular bone Although are less common in the midfoot, the midfoot serves an important role in weight bearing and stabilization. In addition, along with the metatarsal bones, the E12 THE JOURNAL OF FAMILY PRACTICE NOVEMBER 2018 VOL 67, NO 11
6 ADULT FOOT FRACTURES midfoot is critical to proper alignment and articulation. Cuboid and cuneiform Cuboid may occur with high-velocity trauma, foot inversion with external rotation of the tibia, a direct blow, or axial load on a plantar-flexed heel. Pain with weight bearing or with walking on toes is usually present. Cuneiform are less common and rarely occur in isolation. 6 Mechanisms of injury for cuneiform include direct impact, axial loading on a dorsiflexed or plantar-flexed foot with rotational force, and severe rotation of the midfoot section in a fixed foot. Pain is usually localized to the dorsal or dorsomedial aspect of the foot. With these 2 midfoot injuries, the exam should include palpation of the cuboid, navicular, and cuneiform bones and careful inspection of the Lisfranc joint, as this can be injured in midfoot. 7 Obtain AP, lateral, and oblique views of the foot, 5 and strongly consider bilateral weight-bearing films to evaluate for tarsometatarsal (TMT) joint complex injuries (typically Lisfranc joint complex injuries), given their association with midfoot 1 (FIGURE 3). If the fracture is at or near the TMT joint complex, obtain a CT scan or MRI regardless of plain film findings to evaluate the Lisfranc joint complex. Because the Lisfranc joint is particularly important in midfoot stability, untreated injuries can lead to impaired gait or chronic foot pain and deformity. Early identification and surgical referral for these injuries is crucial. Navicular Navicular are typically caused by a twisting mechanism with forced plantar flexion or forced dorsiflexion of the midfoot. They present with severe pain over the dorsal or dorsomedial foot, particularly while bearing weight. Tenderness to palpation over the navicular bone generally warrants imaging studies to rule out fracture, as undiagnosed can lead to severe long-term disability. Use Ottawa Ankle and Foot Rules 12 in the acute setting to determine the need for radiographs. If imaging is indicated, obtain AP, lateral, and oblique views. FIGURE 2 Zones of the proximal fifth metatarsal I Tuberosity may be seen on the AP view, while dorsal avulsions, talonavicular joint disruptions, and naviculo-cuneiform joint injuries are better seen on lateral views. 16 Patients, particularly cross-country and track athletes, presenting with insidious onset of pain over the navicular bone should be evaluated for stress fracture using MRI, even in the presence of normal radiographs. Differential diagnosis. Suspect Lisfranc joint complex injuries in any patient with mid-foot pain or fracture. The transverse arch of the foot is reliant upon the articulation of the second metatarsal with all 5 neighboring bones. The Lisfranc ligament is the strongest of 3 supporting ligaments to anchor the TMT joint complex. Other causes of mid-foot pain include soft tissue injury, contusion, and tendinopathy. In addition, other conditions that may cause pain in this area include cuboid syndrome, peroneal tendinopathy, Jones fracture, stress fracture, anterior calcaneal fracture, and sinus tarsi syndrome. Treatment. Nondisplaced of the cuboid or cuneiform may be treated with a short leg walking cast/boot for 6 weeks followed by the use of a shoe with a thin, rigid, longitudinal arch support for an additional 6 weeks. 1 Fractures requiring referral for surgical evaluation include that are open and with vascular or neurological compromise. Also refer comminuted II III Zone I represents the area of avulsion, denoted by a fracture proximal to the joint line of the fourth metatarsal and its interaction with the cuboid. Zone II is the site of a true Jones fracture, which is at high risk for nonunion. Zone III represents the area of diaphysis. MDEDGE.COM/JFPONLINE VOL 67, NO 11 NOVEMBER 2018 THE JOURNAL OF FAMILY PRACTICE E13
7 FIGURE 3 Non-weight bearing and weight bearing views of the right foot A B IMAGES COURTESY OF: MICHAEL SETH SMITH, MD, CAQSM, PharmD A comparison of the non-weight bearing view of the right foot (A) and the weight bearing view of the same right foot (B; with left foot for comparison) shows the widening between the base of the first and second metatarsals at the Lisfranc joint (arrow), indicating a Lisfranc injury. and those that present with >2 mm step-off. Lastly, midfoot that involve the Lisfranc joint should be immobilized and referred for orthopedic evaluation with instructions to the patient to avoid weight bearing until orthopedic evaluation. 8 Avulsion of the navicular bone may be managed nonoperatively with a short leg walking cast/boot if there is <20% involvement of the talonavicular surface. Simple nondisplaced body may also be managed conservatively with immobilization and protected weight bearing for 6 to 8 weeks. 15 Refer for surgical evaluation avulsion that are intra-articular or dorsal involving 20% or more of the talonavicular surface and tuberosity, given their risk of nonunion. 9 All navicular body that are not longitudinal in nature should also be referred for surgical evaluation. Navicular stress that do not extend into the plantar cortex may be managed conservatively with a minimum of 6 weeks of a short leg cast and strict NWB with close follow-up. 17 Calcaneal Calcaneal typically occur from severe axial load or fall from a height. Weight bearing is usually limited and secondary to significant pain. Tenderness to palpation over the calcaneus or with squeezing of the heel will produce pain on exam. Initial x-rays should include a lateral and axial view of the calcaneus. Additional imaging, including a CT scan, may be indicated for further evaluation to determine the extent of the fracture or to determine if a fracture is present despite normal x-rays. 10 Acute compartment syndrome occurs in 10% of calcaneal and must be considered in patients with calcaneal from severe trauma. 18 Tendon injuries of the ankle, hindfoot, and midfoot may present similarly but can be ruled out with clinical exam and appropriate imaging. Treatment Avulsion that do not involve more than 25% of the calcaneocuboid joint and nondisplaced calcaneal may be E14 THE JOURNAL OF FAMILY PRACTICE NOVEMBER 2018 VOL 67, NO 11
8 ADULT FOOT FRACTURES managed conservatively by instructing patients to wear a NWB short leg cast/boot for 4 to 6 weeks. 1 Refer for surgical evaluation patients with calcaneal fracture fragments >1 cm, displacement >3 mm, open, joint involvement >25%, and those whose symptoms fail to resolve with conservative management. Stress can be managed conservatively with cessation of aggravating activities and immobilization in a walking boot until symptoms resolve, which typically takes 4 to 6 weeks. 1 JFP CORRESPONDENCE Michael Seth Smith, MD, CAQSM, PharmD, 3450 Hull Road, Gainesville, FL 32611; smithms@ortho.ufl.edu References 1. Eiff MP, Hatch RL, et al. Fracture Management for Primary Care. 3rd ed. Philadelphia, PA: Elsevier Saunders; Hatch RL, Rosenbaum Cl. Fracture care by family physicians. A review of 295 cases. J Fam Pract. 1994;38: Bica D, Sprouse RA, Armen J. Diagnosis and management of common foot. Am Fam Physician. 2016;93: Hatch RL, Hacking S. Evaluation and management of toe. Am Fam Physician. 2003;68: Snider RK. Essentials of Musculoskeletal Care. 2nd ed. Rosemont, IL: American Orthopedic Surgeons; Guler F, Baz AB, Turan A, et al. Isolated medial cuneiform : report of two cases and review of the literature. Foot Ankle Spec. 2011;4: Borrelli J, De S, Van Pelt M. Fracture of the cuboid. J Am Acad Orthop Surg. 2012;20: Pinney SJ, Sangeorzan BJ. Fractures of the tarsal bones. Orthop Clin North Am. 2001:32: Rosenbaum AJ, Uhl R, DiPreta JA. Acute of the tarsal navicular. Orthopedics. 2014;37: Sanders RW, Clare MP. Calcaneous. In: Rockwood and Green s Fractures in Adults. 7th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2010: Singer G, Cichocki M, Schalamon J, et al. A study of metatarsal in children. J Bone Joint Surg Am. 2008;90: Stiell IG, Greenberg GH, McKnight RD, et al. A study to develop clinical decision rules for the use of radiography in acute ankle injuries. Ann Emerg Med. 1992;21: Ekinci S, Polat O, Günalp M, et al. The accuracy of ultrasound evaluation in foot and ankle trauma. Am J Emerg Med. 2013;31: Welck MJ, Hayes T, Pastides P, et al. Stress of the foot and ankle. Injury. 2017;48: Hatch RL, Alsobrook JA, Clugston JR. Diagnosis and management of metatarsal. Am Fam Physician. 2007;76: Schildhauer TA, Coulibaly MO, Hoffman MF. Fractures and dislocations of the midfoot and forefoot. In: Rockwood and Green s Fractures in Adults. 8th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2015: Mayer SW, Joyner PW, Almekinders LC, et al. Stress of the foot and ankle in athletes. Sports Health. 2014;6: Kalsi R, Dempsey A, Bunney EB. Compartment syndrome of the foot after calcaneal fracture. J Emerg Med. 2012;43:e MDEDGE.COM/JFPONLINE VOL 67, NO 11 NOVEMBER 2018 THE JOURNAL OF FAMILY PRACTICE E15
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium
 MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
Foot Injuries. Dr R B Kalia
 Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Hany El-Rashidy and Anand Vora
 Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
Sports Injuries of the Foot and Ankle. Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018
 Sports Injuries of the Foot and Ankle Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018 I. Objectives A. By the end of the lecture attendees will
Sports Injuries of the Foot and Ankle Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018 I. Objectives A. By the end of the lecture attendees will
5 COMMON INJURIES IN THE FOOT & ANKLE
 5 COMMON INJURIES IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA MECHANISM OF INJURY HOW DID IT HAPPEN? HIGH ENERGY VS LOW ENERGY DIRECTION OF FORCES INVOLVED LIVING
5 COMMON INJURIES IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA MECHANISM OF INJURY HOW DID IT HAPPEN? HIGH ENERGY VS LOW ENERGY DIRECTION OF FORCES INVOLVED LIVING
Foot and Ankle Complaints.
 Foot and Ankle Complaints www.fisiokinesiterapia.biz INTRODUCTION Anatomy and Function Foot Ankle Common complaints Common diagnoses FOOT AND ANKLE ANATOMY 26 bones and 2 sesamoids Forefoot Metatarsals
Foot and Ankle Complaints www.fisiokinesiterapia.biz INTRODUCTION Anatomy and Function Foot Ankle Common complaints Common diagnoses FOOT AND ANKLE ANATOMY 26 bones and 2 sesamoids Forefoot Metatarsals
11/5/14. I will try to make this painless. Great, a Fracture, Now What? Objectives. Basics for Fracture Workup. Basics for Fracture Workup
 Great, a Fracture, Now What? I will try to make this painless Mary Greve MS, PA-C Department of Orthopedic Surgery Trauma Team University of Iowa Hospitals and Clinics Mary-Greve@uiowa.edu Pager 2121 Objectives
Great, a Fracture, Now What? I will try to make this painless Mary Greve MS, PA-C Department of Orthopedic Surgery Trauma Team University of Iowa Hospitals and Clinics Mary-Greve@uiowa.edu Pager 2121 Objectives
Goals. Initial management skeletal trauma. Physical Exam ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT 12/4/2010
 ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT Brian Feeley, MD UCSF Sports Medicine and Shoulder Surgery Goals Discuss common fractures and initial management, treatment guidelines Let your patients
ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT Brian Feeley, MD UCSF Sports Medicine and Shoulder Surgery Goals Discuss common fractures and initial management, treatment guidelines Let your patients
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/29/2012 Radiology Quiz of the Week # 105 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/29/2012 Radiology Quiz of the Week # 105 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Peggers Super Summaries: Foot Injuries
 Lisfranc Injury ANATOMY Roman arch with recessed 2 nd MT base AP medial side of intermediate cuneiform to 2 nd MT base Oblique medial side of lateral cuneiform with 3 rd MT base and 4 th with medial boarder
Lisfranc Injury ANATOMY Roman arch with recessed 2 nd MT base AP medial side of intermediate cuneiform to 2 nd MT base Oblique medial side of lateral cuneiform with 3 rd MT base and 4 th with medial boarder
radiologymasterclass.co.uk
 http://radiologymasterclass.co.uk Hip X-ray anatomy - Normal AP (anterior-posterior) Shenton's line is formed by the medial edge of the femoral neck and the inferior edge of the superior pubic ramus Loss
http://radiologymasterclass.co.uk Hip X-ray anatomy - Normal AP (anterior-posterior) Shenton's line is formed by the medial edge of the femoral neck and the inferior edge of the superior pubic ramus Loss
Review relevant anatomy of the foot and ankle. Learn the approach to examining the foot and ankle
 Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
LISFRANC FRACTURE-DISLOCATION
 LISFRANC FRACTURE-DISLOCATION Napoleon at Mont St. Bernard, Jacques-Louis David, 1800, Oil on Canvas, Musee du Louvre, Paris. This is Jacques-Louis David s immortal depiction of a young Napoleon Bonaparte,
LISFRANC FRACTURE-DISLOCATION Napoleon at Mont St. Bernard, Jacques-Louis David, 1800, Oil on Canvas, Musee du Louvre, Paris. This is Jacques-Louis David s immortal depiction of a young Napoleon Bonaparte,
CASE ONE CASE ONE. RADIAL HEAD FRACTURE Mason Classification. RADIAL HEAD FRACTURE Mechanism of Injury. RADIAL HEAD FRACTURE Imaging
 CASE ONE An eighteen year old female falls during a basketball game, striking her elbow on the court. She presents to your office that day with a painful, swollen elbow that she is unable to flex or extend
CASE ONE An eighteen year old female falls during a basketball game, striking her elbow on the court. She presents to your office that day with a painful, swollen elbow that she is unable to flex or extend
Index. Clin Sports Med 23 (2004) Note: Page numbers of article titles are in boldface type.
 Clin Sports Med 23 (2004) 169 173 Index Note: Page numbers of article titles are in boldface type. A Achilles enthesopathy, calcaneal spur with, 133 clinical presentation of, 135 136 definition of, 131
Clin Sports Med 23 (2004) 169 173 Index Note: Page numbers of article titles are in boldface type. A Achilles enthesopathy, calcaneal spur with, 133 clinical presentation of, 135 136 definition of, 131
Complexities surrounding Lisfranc injuries
 Complexities surrounding Lisfranc injuries Lisfranc injuries are commonly associated with sporting injuries and are easily diagnosed with severe midfoot pain, swelling, deformity and inability to bear
Complexities surrounding Lisfranc injuries Lisfranc injuries are commonly associated with sporting injuries and are easily diagnosed with severe midfoot pain, swelling, deformity and inability to bear
Outline. Ankle/Foot Anatomy Ankle Sprains Ottawa Ankle Rules DDx: The Sprain That Wasn t
 Ankle Injuries Outline Ankle/Foot Anatomy Ankle Sprains Ottawa Ankle Rules DDx: The Sprain That Wasn t Anatomy: Ankle Mortise Bony Anatomy Lateral Ligament Complex Medial Ligament Complex Ankle Sprains
Ankle Injuries Outline Ankle/Foot Anatomy Ankle Sprains Ottawa Ankle Rules DDx: The Sprain That Wasn t Anatomy: Ankle Mortise Bony Anatomy Lateral Ligament Complex Medial Ligament Complex Ankle Sprains
Midfoot - Reduction & Fixation - ORIF - screw fixation - AO Surgery Reference. ORIF - screw fixation
 Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Recurrent Fifth Metatarsal Fractures. Carol Frey MD Fellowship Co - Director West Coast Sports Medicine Foundation UCLA Manhattan Beach, California
 Recurrent Fifth Metatarsal Fractures Carol Frey MD Fellowship Co - Director West Coast Sports Medicine Foundation UCLA Manhattan Beach, California General 5th MT fracture fairly common Mechanism: Hindfoot
Recurrent Fifth Metatarsal Fractures Carol Frey MD Fellowship Co - Director West Coast Sports Medicine Foundation UCLA Manhattan Beach, California General 5th MT fracture fairly common Mechanism: Hindfoot
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Financial Disclosure. Turf Toe
 Seth O Brien, CP, LP Financial Disclosure Mr. Seth O'Brien has no relevant financial relationships with commercial interests to disclose. Turf Toe Common in athletes playing on firm, artificial turf Forceful
Seth O Brien, CP, LP Financial Disclosure Mr. Seth O'Brien has no relevant financial relationships with commercial interests to disclose. Turf Toe Common in athletes playing on firm, artificial turf Forceful
Prevention and Treatment of Injuries. Anatomy. Anatomy. Tibia: the second longest bone in the body
 Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
ABC of Emergency Radiology
 l ja ) $% _2) < j> ~~~~~~~~~~~~~~~~~foot ABC of Emergency Radiology THE FOOT D A Nicholson, D O'Keeffe, P A Driscoll Accurate clinical assessment of injuries to the foot will avoid unnecessary exposure
l ja ) $% _2) < j> ~~~~~~~~~~~~~~~~~foot ABC of Emergency Radiology THE FOOT D A Nicholson, D O'Keeffe, P A Driscoll Accurate clinical assessment of injuries to the foot will avoid unnecessary exposure
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
FOOSH It sounded like a fun thing at the time!
 FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
Ankle Sprains and Their Imitators
 Ankle Sprains and Their Imitators Mark Halstead, MD Dr. Mark Halstead is the Associate Professor of the Departments of Orthopedics and Pediatrics at Washington University School of Medicine; Director of
Ankle Sprains and Their Imitators Mark Halstead, MD Dr. Mark Halstead is the Associate Professor of the Departments of Orthopedics and Pediatrics at Washington University School of Medicine; Director of
METATARSAL FRACTURE (Including Jones and Dancer s Fractures)
 METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
Introduction. The primary function of the ankle and foot is to absorb shock and impart thrust to the body during walking.
 The ankle 1 Introduction The primary function of the ankle and foot is to absorb shock and impart thrust to the body during walking. OSTEOLOGRY The term ankle refers primarily to the talocrural joint,
The ankle 1 Introduction The primary function of the ankle and foot is to absorb shock and impart thrust to the body during walking. OSTEOLOGRY The term ankle refers primarily to the talocrural joint,
A Patient s Guide to Flatfoot Deformity (Pes Planus) in Children
 A Patient s Guide to Flatfoot Deformity (Pes Planus) in Children 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Flatfoot Deformity (Pes Planus) in Children 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture
 CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Copyright 2012 by The McGraw-Hill Companies, Inc. All rights reserved. McGraw-Hill/Irwin
 CHAPTER 8: THE LOWER EXTREMITY: KNEE, ANKLE, AND FOOT KINESIOLOGY Scientific Basis of Human Motion, 12 th edition Hamilton, Weimar & Luttgens Presentation Created by TK Koesterer, Ph.D., ATC Humboldt State
CHAPTER 8: THE LOWER EXTREMITY: KNEE, ANKLE, AND FOOT KINESIOLOGY Scientific Basis of Human Motion, 12 th edition Hamilton, Weimar & Luttgens Presentation Created by TK Koesterer, Ph.D., ATC Humboldt State
Paul Alley MD,DPM,MS,FACS,FAAOS,BFD Eby Orthopaedics,Jasper,Indiana
 Paul Alley MD,DPM,MS,FACS,FAAOS,BFD Eby Orthopaedics,Jasper,Indiana Very common Bone=fractures Description (cracked,broke,busted,or smashed) A=anatomic area of bone eg: head,neck,shaft B=bone involved
Paul Alley MD,DPM,MS,FACS,FAAOS,BFD Eby Orthopaedics,Jasper,Indiana Very common Bone=fractures Description (cracked,broke,busted,or smashed) A=anatomic area of bone eg: head,neck,shaft B=bone involved
Radiographic Assessment of Pediatric Foot Alignment: Self-Assessment Module
 1.5 CME AJR Integrative Imaging LIFELONG LEARNING FOR RADIOLOGY Radiographic Assessment of Pediatric Foot Alignment: Self-Assessment Module Mahesh M. Thapa 1,2, Sumit Pruthi 1,2, Felix S. Chew 2 ABSTRACT
1.5 CME AJR Integrative Imaging LIFELONG LEARNING FOR RADIOLOGY Radiographic Assessment of Pediatric Foot Alignment: Self-Assessment Module Mahesh M. Thapa 1,2, Sumit Pruthi 1,2, Felix S. Chew 2 ABSTRACT
CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS
 CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS ABC s of Comprehensive Musculoskeletal Care December 1 st, 2007 Stephen Pinney MD Chief, UCSF Foot and Ankle Service Chronic problems typically occur gradually
CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS ABC s of Comprehensive Musculoskeletal Care December 1 st, 2007 Stephen Pinney MD Chief, UCSF Foot and Ankle Service Chronic problems typically occur gradually
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Copyright 2004, Yoshiyuki Shiratori. All right reserved.
 Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Unusual fracture combination with Charcot arthropathy and juvenile-onset diabetes
 Injury Extra (2008) 39, 291 295 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/inext CASE REPORT Unusual fracture combination with Charcot arthropathy and juvenile-onset diabetes
Injury Extra (2008) 39, 291 295 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/inext CASE REPORT Unusual fracture combination with Charcot arthropathy and juvenile-onset diabetes
Journal reading. Introduction. Introduction. Ottawa Ankle Rules. Method
 Journal reading Presenter: PGY 林聖傑 Supervisor: Dr. 林俊龍 102.12.23 The accuracy of ultrasound evaluation in foot and ankle trauma Salih Ekinci, MD American Journal of Emergency Medicine 31 (2013) 1551 1555
Journal reading Presenter: PGY 林聖傑 Supervisor: Dr. 林俊龍 102.12.23 The accuracy of ultrasound evaluation in foot and ankle trauma Salih Ekinci, MD American Journal of Emergency Medicine 31 (2013) 1551 1555
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Case Report A Case Report of Isolated Cuboid Nutcracker Fracture
 Case Reports in Orthopedics Volume 2016, Article ID 3264172, 5 pages http://dx.doi.org/10.1155/2016/3264172 Case Report A Case Report of Isolated Cuboid Nutcracker Fracture Takaaki Ohmori, 1,2 Shinichi
Case Reports in Orthopedics Volume 2016, Article ID 3264172, 5 pages http://dx.doi.org/10.1155/2016/3264172 Case Report A Case Report of Isolated Cuboid Nutcracker Fracture Takaaki Ohmori, 1,2 Shinichi
pedcat Clinical Case Studies
 pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
Physical Examination of the Foot & Ankle
 Inspection Standing, feet straight forward facing toward examiner Swelling Deformity Flatfoot (pes planus and hindfoot valgus) High arch (pes cavus and hindfoot varus) Peek-a-boo heel Varus Too many toes
Inspection Standing, feet straight forward facing toward examiner Swelling Deformity Flatfoot (pes planus and hindfoot valgus) High arch (pes cavus and hindfoot varus) Peek-a-boo heel Varus Too many toes
Dr Nabil khouri MD. MSc. Ph.D
 Dr Nabil khouri MD. MSc. Ph.D Foot Anatomy The foot consists of 26 bones: 14 phalangeal, 5 metatarsal, and 7 tarsal. Toes are used to balance the body. Metatarsal Bones gives elasticity to the foot in
Dr Nabil khouri MD. MSc. Ph.D Foot Anatomy The foot consists of 26 bones: 14 phalangeal, 5 metatarsal, and 7 tarsal. Toes are used to balance the body. Metatarsal Bones gives elasticity to the foot in
June 2013 Case Study. Author: T. Walker Robinson, MD, MPH, Nationwide Children s Hospital
 June 2013 Case Study Author: T. Walker Robinson, MD, MPH, Nationwide Children s Hospital Chief Complaint: Right ankle pain HPI: A 10 year old female dancer presents to the clinic with a five day history
June 2013 Case Study Author: T. Walker Robinson, MD, MPH, Nationwide Children s Hospital Chief Complaint: Right ankle pain HPI: A 10 year old female dancer presents to the clinic with a five day history
Bones = phalanges 5 metatarsals 7 tarsals
 The Foot (Bones) Bones = 26 14 phalanges 5 metatarsals 7 tarsals Toes (Phalanges) Designed to give wider base for balance and propelling the body forward. 1st toe (Hallux) Two sesamoid bones located under
The Foot (Bones) Bones = 26 14 phalanges 5 metatarsals 7 tarsals Toes (Phalanges) Designed to give wider base for balance and propelling the body forward. 1st toe (Hallux) Two sesamoid bones located under
Main Menu. Ankle and Foot Joints click here. The Power is in Your Hands
 1 The Ankle and Foot Joints click here Main Menu Copyright HandsOn Therapy Schools 2009 K.8 http://www.handsonlineeducation.com/classes/k8/k8entry.htm[3/27/18, 1:40:03 PM] Ankle and Foot Joint 26 bones
1 The Ankle and Foot Joints click here Main Menu Copyright HandsOn Therapy Schools 2009 K.8 http://www.handsonlineeducation.com/classes/k8/k8entry.htm[3/27/18, 1:40:03 PM] Ankle and Foot Joint 26 bones
Acute Ankle Injuries, Part 1: Office Evaluation and Management
 t June 08, 2009 Obesity [1] Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the
t June 08, 2009 Obesity [1] Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the
FOOSH It sounded like a fun thing at the time!
 FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Posterior Tibialis Tendon Dysfunction & Repair
 1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
Top 10 Ortho Urgent Care Injuries. J.C. Clark, M.D. ORA Orthopedics
 Top 10 Ortho Urgent Care Injuries J.C. Clark, M.D. ORA Orthopedics 10. Proximal Humerus Fractures Treatment Simple sling ICE, pain meds Button-down shirts Recliner to sleep in It will be up to the surgeon
Top 10 Ortho Urgent Care Injuries J.C. Clark, M.D. ORA Orthopedics 10. Proximal Humerus Fractures Treatment Simple sling ICE, pain meds Button-down shirts Recliner to sleep in It will be up to the surgeon
Traumatic Injuries to the Foot and Ankle
 Traumatic Injuries to the Foot and Ankle Dr. Joseph N. Daniel Clinical Associate Professor of Orthopaedic Surgery Foot and Ankle Service, The Rothman Institute Thomas Jefferson University Hospital Philadelphia,
Traumatic Injuries to the Foot and Ankle Dr. Joseph N. Daniel Clinical Associate Professor of Orthopaedic Surgery Foot and Ankle Service, The Rothman Institute Thomas Jefferson University Hospital Philadelphia,
 17.2 A-P Lower Leg Measure: A-P at mid-lower leg Protection: Apron draped over pelvis SID: 40 Table top No Tube Angle Film: 7 x17 I.D. down or diagonal 14 x 17 www.fisiokinesiterapia.biz A-P Lower Leg
17.2 A-P Lower Leg Measure: A-P at mid-lower leg Protection: Apron draped over pelvis SID: 40 Table top No Tube Angle Film: 7 x17 I.D. down or diagonal 14 x 17 www.fisiokinesiterapia.biz A-P Lower Leg
Injuries to the lower extremity II Aree Tanavalee MD Associate Professor Department of Orthopaedics Faculty of Medicine Chulalongkorn University
 Injuries to the lower extremity II Aree Tanavalee MD Associate Professor Department of Orthopaedics Faculty of Medicine Chulalongkorn University Topics Fracture of the shaft of the femur Fractures around
Injuries to the lower extremity II Aree Tanavalee MD Associate Professor Department of Orthopaedics Faculty of Medicine Chulalongkorn University Topics Fracture of the shaft of the femur Fractures around
Managing Tibialis Posterior Tendon Injuries
 Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations
 Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations Anish R. Kadakia, Mark S. Myerson, and Milap Patel Contents Mechanism of Injury... 2 Radiographic Evaluation... 3 Classification...
Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations Anish R. Kadakia, Mark S. Myerson, and Milap Patel Contents Mechanism of Injury... 2 Radiographic Evaluation... 3 Classification...
American Family Physician
 Page 1 of 12 American Family Physician Return to Previous Page Jul 1, 1998 Table of Contents Lisfranc Injury of the Foot: A Commonly Missed Diagnosis KEVIN E. BURROUGHS, M.D, Moses Cone Family Practice
Page 1 of 12 American Family Physician Return to Previous Page Jul 1, 1998 Table of Contents Lisfranc Injury of the Foot: A Commonly Missed Diagnosis KEVIN E. BURROUGHS, M.D, Moses Cone Family Practice
3 section of the Foot
 TERMINOLOGY 101 How many Bones 3 section of the Foot Bilateral Relating to both Plantar Relating to the bottom or sole Lateral Relating to the outside or farther from the median Medial Relating to the
TERMINOLOGY 101 How many Bones 3 section of the Foot Bilateral Relating to both Plantar Relating to the bottom or sole Lateral Relating to the outside or farther from the median Medial Relating to the
Section 3: Foot Subluxations and Dislocations
 Section 3: Foot Subluxations and Dislocations Case Study F: Lisfranc s Midfoot Dislocation Clinical History: J.K. a 28 year old female presents complaining of a painful right foot. She sustained an acute
Section 3: Foot Subluxations and Dislocations Case Study F: Lisfranc s Midfoot Dislocation Clinical History: J.K. a 28 year old female presents complaining of a painful right foot. She sustained an acute
Basic Care of Common Fractures Utku Kandemir, MD
 Basic Care of Common Fractures Utku Kandemir, MD Assistant Clinical Professor Trauma & Sports Medicine Dept. of Orthopaedic Surgery UCSF / SFGH History Physical Exam Radiology Treatment History Acute trauma
Basic Care of Common Fractures Utku Kandemir, MD Assistant Clinical Professor Trauma & Sports Medicine Dept. of Orthopaedic Surgery UCSF / SFGH History Physical Exam Radiology Treatment History Acute trauma
Fractures in the Immature Foot
 Fractures in the Immature Foot Kaye E. Wilkins, M.D. Clinical Professor Orthopaedics & Pediatrics University of Texas Health Science Center at San Antonio San Antonio, Texas (210) 692-1613 e-mail: drkwilkins@aol.com
Fractures in the Immature Foot Kaye E. Wilkins, M.D. Clinical Professor Orthopaedics & Pediatrics University of Texas Health Science Center at San Antonio San Antonio, Texas (210) 692-1613 e-mail: drkwilkins@aol.com
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/08/2012 Radiology Quiz of the Week # 102 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/08/2012 Radiology Quiz of the Week # 102 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Medical Practice for Sports Injuries and Disorders of the Lower Limb
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Lower Limb JMAJ 48(1): 25 29, 2005 Motonobu NATSUYAMA Chief Surgeon, Department of Orthopedic Surgery, Kantoh
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Lower Limb JMAJ 48(1): 25 29, 2005 Motonobu NATSUYAMA Chief Surgeon, Department of Orthopedic Surgery, Kantoh
Scar Engorged veins. Size of the foot [In clubfoot, small foot]
![Scar Engorged veins. Size of the foot [In clubfoot, small foot] Scar Engorged veins. Size of the foot [In clubfoot, small foot]](/thumbs/78/77722241.jpg) 6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
Leg and Ankle Problems in Primary Care.
 Leg and Ankle Problems in Primary Care www.fisiokinesiterapia.biz Leg and Ankle Presentations 4Trauma 4Pain Ankle Trauma 41. Twist and Fall--Fracture or Sprain 42. Patient hears/feels a pop--tendon or
Leg and Ankle Problems in Primary Care www.fisiokinesiterapia.biz Leg and Ankle Presentations 4Trauma 4Pain Ankle Trauma 41. Twist and Fall--Fracture or Sprain 42. Patient hears/feels a pop--tendon or
Commonly Missed Foot and Ankle Conditions. David Miller, DPM AMG Podiatry
 Commonly Missed Foot and Ankle Conditions David Miller, DPM AMG Podiatry Lisfranc Injuries Wide spectrum of injuries High energy Subtle subluxation which could be easily missed injuries Men are 2-4x s
Commonly Missed Foot and Ankle Conditions David Miller, DPM AMG Podiatry Lisfranc Injuries Wide spectrum of injuries High energy Subtle subluxation which could be easily missed injuries Men are 2-4x s
Case Report Painful Os Peroneum Syndrome: Underdiagnosed Condition in the Lateral Midfoot Pain
 Case Reports in Radiology Volume 2016, Article ID 8739362, 4 pages http://dx.doi.org/10.1155/2016/8739362 Case Report Painful Os Peroneum Syndrome: Underdiagnosed Condition in the Lateral Midfoot Pain
Case Reports in Radiology Volume 2016, Article ID 8739362, 4 pages http://dx.doi.org/10.1155/2016/8739362 Case Report Painful Os Peroneum Syndrome: Underdiagnosed Condition in the Lateral Midfoot Pain
Temporary bridge plating of the medial column in Chopart and Lisfranc injuries
 Temporary bridge plating of the medial column in Chopart and Lisfranc injuries by Alaa Mansour DPM 1*, Lawrence Fallat DPM, FACFAS 2 The Foot and Ankle Online Journal 10 (1): 5 Severe traumatic injuries
Temporary bridge plating of the medial column in Chopart and Lisfranc injuries by Alaa Mansour DPM 1*, Lawrence Fallat DPM, FACFAS 2 The Foot and Ankle Online Journal 10 (1): 5 Severe traumatic injuries
Feet First. Michael K. Cooper, DO FACOFP Family Practice/OMM St John Clinic - Claremore OOA 2018 Annual Convention
 Feet First Michael K. Cooper, DO FACOFP Family Practice/OMM St John Clinic - Claremore OOA 2018 Annual Convention Disclaimer I have no conflict of interest. I am not on any pharmaceutical company payroll
Feet First Michael K. Cooper, DO FACOFP Family Practice/OMM St John Clinic - Claremore OOA 2018 Annual Convention Disclaimer I have no conflict of interest. I am not on any pharmaceutical company payroll
Medical Foundations of Workers Compensation Conditions of the Feet
 Medical Foundations of Workers Compensation Conditions of the Feet Objective: This section will introduce the student to basic medical terms, familiarize them with common diagnoses, and review treatment
Medical Foundations of Workers Compensation Conditions of the Feet Objective: This section will introduce the student to basic medical terms, familiarize them with common diagnoses, and review treatment
Case Iselin's disease in a Thai boxer.
 Case 13609 Iselin's disease in a Thai boxer. Joris De Win 1, 3, Filip Vanhoenacker 2, 4, Els Goossens3 1: Department of Physical Medicine and Rehabilitation; University Ghent (UGent), Belgium; Email:de_win_joris@hotmail.com
Case 13609 Iselin's disease in a Thai boxer. Joris De Win 1, 3, Filip Vanhoenacker 2, 4, Els Goossens3 1: Department of Physical Medicine and Rehabilitation; University Ghent (UGent), Belgium; Email:de_win_joris@hotmail.com
Accurate determination of screw position in treating fifth metatarsal base fractures to shorten radiation exposure time
 Singapore Med J 2016; 57(11): 619-623 doi: 10.11622/smedj.2015196 Accurate determination of screw position in treating fifth metatarsal base fractures to shorten radiation exposure time Xu Wang 1, MD,
Singapore Med J 2016; 57(11): 619-623 doi: 10.11622/smedj.2015196 Accurate determination of screw position in treating fifth metatarsal base fractures to shorten radiation exposure time Xu Wang 1, MD,
Clarification of Terms
 Clarification of Terms The plantar aspect of the foot refers to the role or its bottom The dorsal aspect refers to the top or its superior portion The ankle and foot perform three main functions: 1. shock
Clarification of Terms The plantar aspect of the foot refers to the role or its bottom The dorsal aspect refers to the top or its superior portion The ankle and foot perform three main functions: 1. shock
AAP Boot Camp KNEE AND ANKLE EXAM
 AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
Recognizing common injuries to the lower extremity
 Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Radiographic Evaluation of Calcaneal Fractures. Kali Luker, PGY-1
 Radiographic Evaluation of Calcaneal Fractures Kali Luker, PGY-1 Anatomy Extraarticular Fractures Involve body, anterior process or tuberosity Treated with immobilization and NWB x 6 wks UNLESS Displaced
Radiographic Evaluation of Calcaneal Fractures Kali Luker, PGY-1 Anatomy Extraarticular Fractures Involve body, anterior process or tuberosity Treated with immobilization and NWB x 6 wks UNLESS Displaced
Fractures of the Hand in Children Which are simple? And Which have pitfalls??
 Fractures of the Hand in Children Which are simple? And Which have pitfalls?? Kaye E Wilkins DVM, MD Professor of Orthopedics and Pediatrics Departments of Orthopedics and Pediatrics University of Texas
Fractures of the Hand in Children Which are simple? And Which have pitfalls?? Kaye E Wilkins DVM, MD Professor of Orthopedics and Pediatrics Departments of Orthopedics and Pediatrics University of Texas
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION. At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral)
 PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
SUBTLE CAVUS IN SPORTS INJURIES
 SUBTLE CAVUS IN SPORTS INJURIES MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA NON-NEUROMUSCULAR NORMAL VARIANT: 20-25% INCIDENCE LEDOUX, ET AL. FAI 24, 2003 FOREFOOT-DRIVEN / MORE SUBTLE
SUBTLE CAVUS IN SPORTS INJURIES MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA NON-NEUROMUSCULAR NORMAL VARIANT: 20-25% INCIDENCE LEDOUX, ET AL. FAI 24, 2003 FOREFOOT-DRIVEN / MORE SUBTLE
What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne
 What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne We don t know!! Population Studies 2300 children aged 4-13 years Shoe wearers Flat foot 8.6% Non-shoe wearers
What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne We don t know!! Population Studies 2300 children aged 4-13 years Shoe wearers Flat foot 8.6% Non-shoe wearers
Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve. Lumbar radiculopathy Instability MTPJ joint or inflammatory MPJ
 MORTON S NEUROMA 80% III web space (next common is II). Never occurs in III or IV Common in females in fifties Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve Rule out
MORTON S NEUROMA 80% III web space (next common is II). Never occurs in III or IV Common in females in fifties Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve Rule out
Pediatric Fractures. Objectives. Epiphyseal Complex. Anatomy and Physiology. Ligaments. Bony matrix
 1 Pediatric Fractures Nicholas White, MD Assistant Professor of Pediatrics Eastern Virginia Medical School Attending, Pediatric Emergency Department Children s Hospital of The King s Daughters Objectives
1 Pediatric Fractures Nicholas White, MD Assistant Professor of Pediatrics Eastern Virginia Medical School Attending, Pediatric Emergency Department Children s Hospital of The King s Daughters Objectives
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
EASILY MISSED FOOT AND ANKLE FRACTURES NORDIC TRAUMA COURSE 2016, AARHUS
 EASILY MISSED FOOT AND ANKLE FRACTURES NORDIC TRAUMA COURSE 2016, AARHUS Ken F. Linnau, MD, MS Emergency Radiology Harborview Medical Center University of Washington Seattle, WA Thanks to Claire K Sandstrom
EASILY MISSED FOOT AND ANKLE FRACTURES NORDIC TRAUMA COURSE 2016, AARHUS Ken F. Linnau, MD, MS Emergency Radiology Harborview Medical Center University of Washington Seattle, WA Thanks to Claire K Sandstrom
17/10/2017. Foot and Ankle
 17/10/2017 Alicia M. Yochum RN, DC, DACBR, RMSK Foot and Ankle Plantar Fasciitis Hallux Valgus Deformity Achilles Tendinosis Posterior Tibialis Tendon tendinopathy Stress Fracture Ligamentous tearing Turf
17/10/2017 Alicia M. Yochum RN, DC, DACBR, RMSK Foot and Ankle Plantar Fasciitis Hallux Valgus Deformity Achilles Tendinosis Posterior Tibialis Tendon tendinopathy Stress Fracture Ligamentous tearing Turf
ANKLE JOINT ANATOMY 3. TALRSALS = (FOOT BONES) Fibula. Frances Daly MSc 1 CALCANEUS 2. TALUS 3. NAVICULAR 4. CUBOID 5.
 ANKLE JOINT ANATOMY The ankle joint is a synovial joint of the hinge type. The joint is formed by the distal end of the tibia and medial malleolus, the fibula and lateral malleolus and talus bone. It is
ANKLE JOINT ANATOMY The ankle joint is a synovial joint of the hinge type. The joint is formed by the distal end of the tibia and medial malleolus, the fibula and lateral malleolus and talus bone. It is
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
Ankle sprain, one of the more common injuries that
 Scott Hall, MD; Greg Lundeen, MD; Ali Shahin, MD University of Nevada-Reno (Drs. Hall and Lundeen); Reno Orthopedic Clinic, Reno, Nev (Dr. Lundeen); Sierra Family Health, Carson City, Nev (Dr. Shahin)
Scott Hall, MD; Greg Lundeen, MD; Ali Shahin, MD University of Nevada-Reno (Drs. Hall and Lundeen); Reno Orthopedic Clinic, Reno, Nev (Dr. Lundeen); Sierra Family Health, Carson City, Nev (Dr. Shahin)
BUCKS MSK: FOOT AND ANKLE PATHWAY GP MANAGEMENT. Hallux Valgus. Assessment: Early Management. (must be attempted prior to any referral to imsk):
 Hallux Valgus Common condition: affecting around 28% of the adult population. Prevalence increases with age and in females. Observation: Lateral deviation of the great toe. May cause secondary irritation
Hallux Valgus Common condition: affecting around 28% of the adult population. Prevalence increases with age and in females. Observation: Lateral deviation of the great toe. May cause secondary irritation
Evidence-Based Examination of the Foot Presented by Alexis Wright, PT, PhD, DPT, FAAOMPT Practice Sessions/Skill Check-offs
 Evidence-Based Examination of the Foot Presented by Alexis Wright, PT, PhD, DPT, FAAOMPT Practice Sessions/Skill Check-offs Module Five: Movement Assessment of the Foot/Ankle (1 hour CEU Time) Skilled
Evidence-Based Examination of the Foot Presented by Alexis Wright, PT, PhD, DPT, FAAOMPT Practice Sessions/Skill Check-offs Module Five: Movement Assessment of the Foot/Ankle (1 hour CEU Time) Skilled
A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation
 Journal of Sport Rehabilitation, 1993, 2, 281-286 O 1993 Human Kinetics Publishers, Inc. A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation Keith M. Gorse, Graham Johnstone, and Jennifer
Journal of Sport Rehabilitation, 1993, 2, 281-286 O 1993 Human Kinetics Publishers, Inc. A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation Keith M. Gorse, Graham Johnstone, and Jennifer
X-Ray Rounds: (Plain) Radiographic Evaluation of the Ankle.
 X-Ray Rounds: (Plain) Radiographic Evaluation of the Ankle www.fisiokinesiterapia.biz Anatomy Complex hinge joint Articulations among: Fibula Tibia Talus Tibial plafond Distal tibial articular surface
X-Ray Rounds: (Plain) Radiographic Evaluation of the Ankle www.fisiokinesiterapia.biz Anatomy Complex hinge joint Articulations among: Fibula Tibia Talus Tibial plafond Distal tibial articular surface
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
Commonly missed fractures in the Emergency Department
 Commonly missed fractures in the Emergency Department Poster No.: C-2327 Congress: ECR 2015 Type: Educational Exhibit Authors: A. A. Tegzes; Cluj-Napoca/RO Keywords: Education, Digital radiography, Conventional
Commonly missed fractures in the Emergency Department Poster No.: C-2327 Congress: ECR 2015 Type: Educational Exhibit Authors: A. A. Tegzes; Cluj-Napoca/RO Keywords: Education, Digital radiography, Conventional
Anatomy of Foot and Ankle
 Anatomy of Foot and Ankle Surface anatomy of the ankle & foot Surface anatomy of the ankle & foot Medial orientation point medial malleous sustentaculum tali tuberosity of navicular TA muscle TP muscle
Anatomy of Foot and Ankle Surface anatomy of the ankle & foot Surface anatomy of the ankle & foot Medial orientation point medial malleous sustentaculum tali tuberosity of navicular TA muscle TP muscle
Anatomy 1% 29% 64% 6%
 Mortons Neuroma Perineural fibrosis of the plantar digital nerve Females 8-10 3 rd plantar webspace most commonly effected Burning pain Sensory changes 3&4 digits / interdigital space Etiology Excessive
Mortons Neuroma Perineural fibrosis of the plantar digital nerve Females 8-10 3 rd plantar webspace most commonly effected Burning pain Sensory changes 3&4 digits / interdigital space Etiology Excessive
POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY
 1 POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY The following instructions are general guidelines, but surgeon post-op instructions will dictate the individual patient's post-op management
1 POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY The following instructions are general guidelines, but surgeon post-op instructions will dictate the individual patient's post-op management
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program
 Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
