Distal revascularization and microvascular
|
|
|
- Johnathan Patterson
- 5 years ago
- Views:
Transcription
1 Distal revascularization and microvascular free tissue transfer: An alternative to amputation in ischemic lesions of the lower extremity Susan E. Briggs, M.D., Joseph C. Banis, Jr., M.D., Hermann Kaebnick, M.D., Bruce Silverberg, M.D., and Robert D. Acland, M.D., Louisville, Ky. Most lower extremity amputations result from compfications of diabetes and arteriosclerotic occlusive diseases below the inguinal ligament. Improved limb salvage has been achieved by an aggressive approach to distal revascularization in the severely ischemic lower extremity. There remains, however, a high incidence of amputation resulting from progession of the ulceration or gangrene into deeper and less well-vascularized tissues, such as tendon and bone. Even in the nonischemic extremity, such wounds rarely heal without flap coverage. Microvascular free tissue transfers promote healing by providing coverage with healthy, nondiseased, well-vasoalarized tissue for these diffioalt defects. Successful free flap transfer requires a high-pressure recipient inflow vessel. In contrast to individuals with nonarteriosclerotie lesions, many individuals with nonhealing ischemie lesions have no acceptable artery demonstrated on high-resolution angiography to serve as a recipient vessel. Limb salvage has been achieved in four candidates for amputation utilizing distal revascularization followed by free tissue transfer coverage of the ischemic lower leg defects. (J VAsc SuRG 1985; 2: ) In the United States 30,000 to 50,000 lower extremity amputations are performed yearly. Ninetyfive percent of these amputations result from complications of diabetes and arteriosclerotic occlusive disease below the inguinal ligament. ~-3 Infrainguinal arteriosclerotic occlusive disease may result in ischemic rest pain, ulceration, or gangrene. Improved limb salvage has been achieved by an aggressive approach to distal revascularization in the severely ischemic lower extremity? -9 Femorotibial and femoroperoneal saphenous vein bypass grafts have been performed with much success to facilitate healing of skin ulcerations, skin grafts, local pedicle flaps, and digital amputations in ischemic lesions of the lower extremity. Despite such aggressive approaches to revascularization in the lower extremity, many ischemic le- From the Department of Surgery, Universi~ of Louisville School of Medicine. Presented at the Ninth Annual Meeting of the Southern Association for Vascular Surgery, West Palm Beach Gardens, Fla., )ran. 30-Feb. 2, Reprint requests: Susan E. Briggs, M.D., Department of Surgery, University of Louisville School of Medicine, Ambulatory Care Building, Louisville, KY sions result in amputation. Causes of lower extremity amputations include nonreconstructible occlusive lesions, failed arterial reconstructions, and gangrenous lesions extending into deeper and less well-vascularized tissues (i.e., tendon and bone).9,1 Conventional methods of lower extremity wound management, such as skin grafts and local pedicle flaps, are usua[! r-', not successful in the treatment of such ischemic lesions. Microvascular free tissue transfer has provided an alternative to amputation in the management of these difficult wounds. 1H3 Microvascular free tissue transfers ("free flaps") have been used with significant success in the reconstruction of congenital defects, traumatic wounds with exposed and disrupted tendon and bone, and soft tissue, muscle, and osseous defects following radical cancer surgery and burn deformities. H-~8 The major criterion for consideration of free tissue transfers in the treatment of such lesions is the presence of an acceptable recipient vessel. Unlike individuals with nonarteriosclerotic lesions of the lower extremity, many individuals with lesions from arteriosclerotic occlusive disease and diabetes often have no recipient vessel to serve as the conduit for the free tissue transfer. We present our experience with an organized
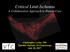
2 Volume 2 Number 6 November 1985 Distal revascularization and microvascular free tissue transfer 807 C' Fig. 1A-B. A, Arteriogram after revascularization demonstrating junction of saphenous vein bypass to posterior tibial artery, with single-vessel runoff to pedal arch. B, Transmetatarsal amputation defect of left foot, with unhealthy bacterially colonized granulation tissue over subjacent tendon and bone. protocol for limb salvage in patients with severe lower extremity ischemic lesions including tendon and bone. MATERIAL AND METHODS Four patients, ages 69 to 80 years, who presented with ischemic ulcerations of the lower extremity in- ~rolving tendon and bone, underwent distal revascularization and free tissue transfer for limb salvage (Table I). Three of the four patients were diabetic. All patients underwent preoperative arteriography often combined with digital subtraction angiography for evaluation of the distal vascular anatomy and pedal arch. Intraoperative angiography was performed following the distal revascularization. Free tissue transfers were performed as a separate operative procedure 2 to 3 weeks following the bypass. Postoperative assessment included clinical evaluation of wound stability and functional status and noninvasive Doppler pulse volume recordings (PVRs) every 6 months for assessment of vascular status. CASE REPORTS Case 1. A 63-year-old diabetic man presented with a 7 x 9 cm ulceration of the right heel with exposed Achilles tendon and calcaneus. Pulse examination revealed a 2/2 Table I. Patient profile Case Ischemic lesion Bypass Variety of flap 1 Heel (tendon/bone) AT Rectus abdominis 2 Toes (tendon/bone) PT Radial forearm 3 Ankle (tendon) AT Scapular 4 Ankle (tendon) PT Scapular AT = anterior tibial; PT = posterior tibial. right femoral pulse with no distal pulses palpable. An anterior tibial pulse was present at Doppler examination. The ankle-brachial index was Angiography demonstrated occlusion of the superficial femoral artery with reconstitution of the anterior tibial artery in the distal third of the leg. The posterior tibial and peroneal arteries were occluded. The patient underwent a right common femoral artery-to-distal anterior tibial artery reversed saphenous vein bypass graft. Two weeks later, he underwent free tissue transfer reconstruction of the remaining necrotic heel defect utilizing a rectus abdominis muscle flap covered with skin graft. The native anterior tibial artery distal to the saphenous vein graft was utilized as the recipient vessel for the free tissue transfer. The postoperative course was uneventful except for the slow wound healing typically demonstrated in the diabetic patient. The patient began walking 2 months postoperatively and has remained healed and symptom-free for 9 months.
3 808 Briggs et al. Journal of VASCULAR SURGERY Fig. 1C-E. C, Pattern of radial forearm skin flap vascularized by radial artery and vein, with potential for cutaneous sensor}~ reconstruction by nerve anastomosis. D, Flap elevated, with artery and vein pedicle demonstrated superiorly, and lateral antebrachial cutaneous nerve demonstrated inferiorly. E, Reconstructed defect in early postoperative period, with photo-plethysmography monitoring device in place. Case 2. A 62-year-old diabetic woman presented with rest pain and dry gangrene of the toes of the left foot extending proximal to the level of the metatarsal heads. Pulse examination demonstrated a 2/2 left femoral pulse with no palpable distal pulses. A posterior tibial pulse was present at Doppler examination. The ankle-brachial index was Angiography demonstrated occlusion of the superficial femoral artery with reconstitution of the distal posterior tibial artery at the midcalf level. The patient underwent a left common femoral artery-to-distal posterior tibial artery reversed saphenous vein bypass graft. Ten days following revascularization, she underwent open transmetatarsal amputation of the gangrenous digits. Three weeks later, she underwent free tissue transfer reconstruction of her transmetatarsal amputation defect with the use of a radial forearm sensate skin flap. The revascularized native posterior tibial artery posterior to the medial malleolus was utilized as the recipient vessel for the free tissue transfer. Because of the significant underlying cardiopulmonary disease, all operative procedures were performed with the patient under regional and epidural blocks. Her postoperative course was marked by an absence of any cardiopulmonary complications, satisfactory wound healing, and return to progressively ambulatory status at "', month postoperatively (Fig. 1). ~ Case 3. An 80-year-old nondiabetic man came to the hospital complaining of rest pain and with a 3 x 6 cm ulceration of the posterior ankle overlying and involying the tendo Achillis. Pulse examination demonstrated 2/2 left femoral pulse, 1/2 left popliteal pulse, and no palpable distal pulses. A left anterior tibial pulse was demonstrated at Doppler examination. Angiography demonstrated a diseased but patent superficial femoral artery with occlusion of the posterior tibial and anterior tibial arteries in the midcalf. The peroncal artery was patent and the anterior tibial artery reconstituted at the level of the ankle. The ankle-brachial index was The patient underwent a common femoral artery-to-distal anterior tibial artery reversed saphenous vein bypass graft. Three weeks later, he underwent free tissue transfer reconstruction of the gangrenous lesion of the tendo Achillis with a scapular skin flap. The recipient vessel for the free tissue transfer was the
4 Volume 2 Number 6 November 1985 Distal revascularization and microvascular free tissue transfer 809 ) Fig. 2A-C. A, Necrotic defect (3 x 8 cm) of left posterior ankle involving tendo Achillis. B, Design of left scapular free flap showing relationship to scapular tip, and schematic demonstration of vascular supply. C, Healed reconstruction 3 months postoperatively. distal portion of the autogenous vein bypass graft. A postoperative arteriogram demonstrated patency of the distal bypass and free flap pedicle vessel. The patient is without symptoms and fully ambulatory with no wound breakdown 1 year postoperatively. Case 4. A 7J-year-old diabetic man presented with a 3 x 8 cm necrotic ulceration of the left posterior heel in. eluding the Achilles tendon. Pulse examination demongtrated a 2/2 left femoral pulse with no palpable distal pulses. A posterior tibial pulse was demonstrated at Doppler examination. The anlde-brachial index was An arteriogram demonstrated severe trifurcation disease with proximal posterior and anterior tibial artery occlusions. The peroneal artery was severely diseased with multiple stenotic areas. Reconstitution of the posterior tibial artery was noted at the ankle level. The patient underwent a reversed saphenous vein bypass graft from the common femoral artery to the distal posterior tibial artery at the medial malleolus. Two weeks later, the patient underwent free flap reconstruction of the necrotic posterior ankle defect with a scapular skin flap. The recipient vessel for the free flap transfer was the distal portion of the saphenous vein bypass graft. A postoperative arteriogram demonstrated patency of the distal bypass and the free flap pedicle vessel. The patient is without symptoms and fully ambulatory with no recurrence of ulceration at 1.5 years postoperatively (Fig. 2). Fig. 2 D. Arteriogram after reconstruction demonstrating saphenous vein bypass to distal posterior tibial artery, with flee flap pedicle arising from vein bypass graft noted just to left of vein bypass, proceeding distally to supply flap tissue.
5 810 Briggs et al. Journal of VASCULAR SURGERY DISCUSSION Successful revascularization is essential for wound healing and the avoidance of amputation in many lower extremity ischemic lesions. Distal arterial revascularization procedures with autogenous saphenous vein appear to offer the best long-term patency in limb salvage procedures involving the lower extremity. 6'8 Despite aggressive approaches to revascularization for limb salvage, including reconstructions to the level of the dorsalis pedis artery and posterior tibial artery below the ankle, 20% to 40% of patients will require major amputations. 3"6"8 In patients with potentially reconstructible lesions, failed arterial reconstructions and ischemic lesions extending to tendon and bone remain the leading causes of amputation. Despite bypass of the lower extremity occlusive disease, ischemic lesions involving the tendo Achillis, calcaneus, and midfoot are associated with particularly high rates of major amputations. Our experience indicates that the ultimate "limb procedure" need not be amputation in all cases of ischemic lesions involving tendon and bone. In the four patients described, the distal arterial bypass provided revascularization of the ischemic limb as well as the necessary conduit of blood supply for a free tissue transfer to reconstruct the severe ischemic lesions. This plan of management allowed us to avoid amputation in these patients with complex ischemicdiabetic wounds. Microsurgery is the technique of performing routine surgical procedures on otherwise inopcrably small structures with the aid of the surgical microscope. Microvascular free tissue transfer is the technique of transplanting healthy, well-vascularized, undamaged tissue ("flap") with its dominant vascular pedicle from one anatomic region to another using the surgical microscope to reconnect precisely the tiny vessels that provide blood supply to these flaps. Microvascular free tissue transfer is proving superior to other methods of wound management in providing coverage for difficult wounds of the lower extremity, particularly those lesions involving the distal third of the leg and foot where other local flaps are unavailable or unreliable, and those lesions extending into avascular or poorly vascularized tissues, such as tendon and bone. TM Free tissue transfer has the distinct advantage of freely allowing movement of skin, muscle, and bone as desired to achieve optimal functional and aesthetic results. More than 60 potential donor sites are available for free tissue transfers, thereby allowing wide flexibility in the choice of a donor site. 13 The ability to achieve coverage O f the ischemic defect with well-vascularized donor ti~sue from a site remote from the ischemic lesion prevents further local tissue disruption and complications with wound healing. Microvascular free flaps have an independent, well-defined blood supply of their own that does not rely on the recipient bed for vascular ingrowth, an advantage in patients with ischemic occlusive disease of the lower extremity. TM The prerequisites for successful free tissue transfer include an acceptable recipient inflow vessel. Few cases have been reported utilizing free tissue transfers in patients with arteriosclerotic occlusive disease of the lower extremityf 6q9 The limiting factor in selecting a recipient vessel for free tissue transfer in patients with peripheral vascular disease is the lowflow state in the arteriosclerotic vessel rather than the vessel wall disease itself. As opposed to individud'~ with nonarteriosclerotic lesions, radiologic assessment of the lower extremity vascular anatomy is essential when free tissue transfers are considered for reconstruction of ischemic lesions. Routine angiography often combined with intra-artcrial digital subtraction angiography has proved valuable in the selection of candidates for free tissue transfer. 2 ax Distal revascularization may provide a suitable recipient vessel in two ways in patients with no acceptable recipient vessel for free tissue transfer. Following revascularization, either the native vessel distal to the arterial bypass or the arterial bypass graft itself may be used as the recipient vessel for the free tissue transfer. The use of supplemental vein grafts to provide additional length of the vascular pedicle of the free flap and a tension-free vascular anastomosis affords the surgeon considerable freedom in the selection of suitable recipient arteries and vei~ ~- outside the zone of injury. Vein grafts of up to 40 cm in length are used successfully in free flap transfers. 11 One-vessel runoff, as present in three of these patients, does not preclude the successful use of free tissue transfer. Steal phenomena have not been documented in free tissue transfer. The flow rate in free flaps (2 to 10 ml/min) is limited by the vascular bed of the flap and is well below the potential inflow of the recipient vessel. The length of operative time necessary for performance of both the revascularization and the free tissue transfer may be a disadvantage in patients with cardiopulmonary disease. The operative risks of reconstruction vs. amputation must be critically and realistically assessed in all patients. In the four reported cases, distal revascularization was performed at a separate time from the free tissue transfer to allow
6 Volume 2 Number 6 November 1985 Distal revascularization and microvascular free tissue transfer 811 for evaluation of early technical difficulties and to avoid prolonged anesthesia. Careful preoperative planning allows a choice of regional anesthetic administration as an alternative to general anesthesia, both for the revascularization and "free flap" reconstruction. The most serious technical complication of "free flap" surgery is the potential for postoperative anastomotic thrombosis with resultant necrosis of the flap. 21'22 The success rate in experienced hands approaches 95%. 21'22 CONCLUSIONS Distal revascularization and free tissue transfer reconstruction offer a viable alternative to amputation in selected patients with ischemic lesions of the... :gwer extremity involving tendon and bone. The technique of utilizing the distal autogenous vein bypass graft as the recipient vessel for the free tissue transfer in the management of ischemic lesions of the lower extremity has not been previously reported. This preliminary experience suggests a broad potential for microvascular adjuncts in the treatment of patients with complex ischemic lesions of the lower extremity following successful revascularization. REFERENCES 1. LoGerfo FW, Coffman JD. Vascular and microvascular disease of the foot in diabetes. N Engl J Med 1984; 311: Barrier HB, Kaiser GC, Willman VL. Blood flow in the diabetic leg. Circulation 1971; 43: Stoney RJ. Ultimate salvage for the patient with limb-threatening ischemia. Realistic goals and surgical considerations. Am [1 Surg 1978; 136: Reichle FA, Martinson MW, Rankin KP. Infrapopliteal ar- '. terial reconstruction in the severely ischemic lower extremity. Ann Surg 1980; 191: Dardik H, Ibrahim IM, Dardik II. The role of the peroneal artery for limb salvage. Ann Surg 1979; 189: Yeager RA, Hobson RW, Jamil Z, Lynch TG, Lee BC, Jain K. Differential patency and limb salvage for polytetrafluoroethylene and autogenous saphenous vein in severe lower extremity ischemia. Surgery 1982; 91: Veith FJ, Gupta SK, Samson RH, Scher LA, Fell SC, Weiss P, Janko G, Flores SW, Rifldn H, Bernstein G, Haimovici H, Gliedman ML, Sprayregen S. Progress in limb salvage with reconstructive arterial surgery combined with new or improved adjunctive procedures. Ann Surg 1981; 194: Bergan JJ, Veith FJ, Bernhard VM, Yao JST, Flinn WR, Gupta SK, Scher LA, Samson RH, Towne JB. Randomization of autogenous vein and polytetrafluoroethylene grafts in femoral-distal reconstruction. Surgery 1982; 92: O'Mara CS, Flinn WR, Neiman HL, Bergan JJ, Yao JST. Correlation of foot arterial anatomy with early tibia[ bypass patency. Surgery 1981; 89: Hobson RW, Lynch TG, Jamil Z, Karanfilian RG, Lee BC, Padberg Jr FT, Long JB. Results of revascularization and amputation in severe lower extremity ischemia: A five-year clinical experience, J VAsc SUR6 1985; 2: Shaw WW. Microvascular free flaps. The first decade. Clin Hast Surg 1983; 10: Serafin D, Voci VE. Reconstruction of the lower extremity. Microsurgical composite tissue transplantation. Clin Hast Surg 1983; 10: Harii K. Microvascular free flaps for skin coverage. Indications and selections of donor sites. Clin Hast Surg 1983; 10: May Jr JW, Gallico III GG, Lukash FN. Microvascular transfer of free tissue for closure of bone wounds of the distal lower extremity. N Engl J Med 1982; 306: Takami H, Takahashi S, Ando M. Microvascular free musculocutaneous flaps for the treatment of avulsion injuries of the lower leg. J Trauma 1983; 23: Dabb RW, David RW. Latissirnus dorsi free flaps in the elderly: An alternative to below&nee amputation. Hast Reconstr Surg 1984; 73: Ohtsuka H, Kamiishi H, Shioya N. Successful free flap transfers in two diabetics. Hast Reconstr Surg 1978; 61: Ohtsuka H, Kamiishi H, Saito H, Ito M, Shioya N. Successful free flap transfers with diseased recipient vessels. Br J Hast Surg 1976; 29: van Gdder PA, Klopper PJ. Microvascular surgery and diseased vessels. Surgery 1981; 90: Flanigan DP, Williams LR, Keifer T, Schuler JJ, Behrend AJ. Prebypass operative arteriography. Surgery 1982; 92: Tumipseed WD, Detmer DE, Berkoff HA, Acher CW, Crummy AB, Belzer FO. Intra-arterial digital angiography: A new diagnostic method for determining limb salvage bypass candidates. Surgery 1982; 92: Harrison DH, GiBing M, Mott G. Methods of assessing the viability of free flap transfer during the postoperative period. Clin Hast Surg 1983; 10:21-36.
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Long-term results of infragenicular bypasses with autogenous vein originating from the distal superficial femoral and popliteal arteries
 Long-term results of infragenicular bypasses with autogenous vein originating from the distal superficial femoral and popliteal arteries Mark S. Rosenbloom, M.D., James J. Walsh, M.D., James J. Schuler,
Long-term results of infragenicular bypasses with autogenous vein originating from the distal superficial femoral and popliteal arteries Mark S. Rosenbloom, M.D., James J. Walsh, M.D., James J. Schuler,
Influence of vein size (diameter) on infrapopliteal reversed vein graft patency
 Influence of vein size (diameter) on infrapopliteal reversed vein graft patency Kurt R. Wengerter, MD, Frank J. Veith, MD, Sushil K. Gupta, MD, Enrico Ascer, MD, and Steven P. Rivers, MD, New York, N.Y.
Influence of vein size (diameter) on infrapopliteal reversed vein graft patency Kurt R. Wengerter, MD, Frank J. Veith, MD, Sushil K. Gupta, MD, Enrico Ascer, MD, and Steven P. Rivers, MD, New York, N.Y.
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
Will it heal? How to assess the probability of wound healing
 Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
FOR THE 18 MILLION INDIVIDUALS with diabetes mellitus in
 11 Evaluation and Management of Peripheral Arterial Disease Joseph L. Mills, Sr., MD FOR THE 18 MILLION INDIVIDUALS with diabetes mellitus in the United States, foot problems ulceration, infection, and
11 Evaluation and Management of Peripheral Arterial Disease Joseph L. Mills, Sr., MD FOR THE 18 MILLION INDIVIDUALS with diabetes mellitus in the United States, foot problems ulceration, infection, and
Popliteal-to-distal bypass for limb-threatening ischemia
 Popliteal-to-distal bypass for limb-threatening ischemia Jeffrey Marks, MD, Terry A, King, MD, Henry Baele, MD, Jeffrey Rubin, MD, and Cynthia Marmen, RN, Cleveland, Ohio In a subset of patients requiring
Popliteal-to-distal bypass for limb-threatening ischemia Jeffrey Marks, MD, Terry A, King, MD, Henry Baele, MD, Jeffrey Rubin, MD, and Cynthia Marmen, RN, Cleveland, Ohio In a subset of patients requiring
Exposure of the anterior tibial artery by medial popliteal extension
 Exposure of the anterior tibial artery by medial popliteal extension J. G. Sladen, FRCS(C), G. Kougeer, FRCS(C), and J. D. S. Reid, FRCS(C), Vancouver) British Columbia) Canada This report describes exploration
Exposure of the anterior tibial artery by medial popliteal extension J. G. Sladen, FRCS(C), G. Kougeer, FRCS(C), and J. D. S. Reid, FRCS(C), Vancouver) British Columbia) Canada This report describes exploration
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Stratifying Management Options for Patients with Critical Limb Ischemia: When Should Open Surgery Be the Initial Option for CLI?
 Stratifying Management Options for Patients with Critical Limb Ischemia: When Should Open Surgery Be the Initial Option for CLI? Peter F. Lawrence, M.D. Gonda Vascular Center Division of Vascular Surgery
Stratifying Management Options for Patients with Critical Limb Ischemia: When Should Open Surgery Be the Initial Option for CLI? Peter F. Lawrence, M.D. Gonda Vascular Center Division of Vascular Surgery
Lower-Extremity Revascularization
 Lower-Extremity Revascularization The open approach to treating limb-threatening lower-extremity ischemia has proven to be an effective means of achieving revascularization. BY RICHARD F. NEVILLE, MD,
Lower-Extremity Revascularization The open approach to treating limb-threatening lower-extremity ischemia has proven to be an effective means of achieving revascularization. BY RICHARD F. NEVILLE, MD,
Surgical Options for revascularisation P E T E R S U B R A M A N I A M
 Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Fluorescent Angiography: Practical uses in the Clinical Setting
 Fluorescent Angiography: Practical uses in the Clinical Setting Charles Andersen MD, FACS, MAPWCA Chief Vascular/Endovascular/ Limb Preservation Surgery Service (Emeritus) Chief of Wound Care Service Madigan
Fluorescent Angiography: Practical uses in the Clinical Setting Charles Andersen MD, FACS, MAPWCA Chief Vascular/Endovascular/ Limb Preservation Surgery Service (Emeritus) Chief of Wound Care Service Madigan
Fluorescence Angiography in Limb Salvage
 Fluorescence Angiography in Limb Salvage Ryan H. Fitzgerald, DPM, FACFAS Associate Professor of Surgery-University Of South Carolina School of Medicine, Greenville Etiology of Lower extremity wounds Neuropathy
Fluorescence Angiography in Limb Salvage Ryan H. Fitzgerald, DPM, FACFAS Associate Professor of Surgery-University Of South Carolina School of Medicine, Greenville Etiology of Lower extremity wounds Neuropathy
Pedal Bypass With Deep Venous Arterialization:
 Pedal Bypass With Deep Venous Arterialization: Long Term Result For Critical Limb Ischemia With Unreconstructable Distal Arteries Pramook Mutirangura Professor of Vascular Surgery Faculty of Medicine Siriraj
Pedal Bypass With Deep Venous Arterialization: Long Term Result For Critical Limb Ischemia With Unreconstructable Distal Arteries Pramook Mutirangura Professor of Vascular Surgery Faculty of Medicine Siriraj
GLOBAL VASCULAR GUIDELINES: A NEW PATHWAY FOR LIMB SALVAGE
 GLOBAL VASCULAR GUIDELINES: A NEW PATHWAY FOR LIMB SALVAGE Michael S. Conte MD Professor and Chief, Vascular and Endovascular Surgery Co-Director, Center for Limb Preservation Co-Director, Heart and Vascular
GLOBAL VASCULAR GUIDELINES: A NEW PATHWAY FOR LIMB SALVAGE Michael S. Conte MD Professor and Chief, Vascular and Endovascular Surgery Co-Director, Center for Limb Preservation Co-Director, Heart and Vascular
Pedal or peroneal bypass: Which is better when both are patent?
 Pedal or peroneal bypass: Which is better when both are patent? Thomas M. Bergamini, MD, Salem M. George, Jr., MD, H. Todd Massey, MD, Peter K. Henke, MD, Thomas W. Klamer, MD, Glenn E. Lambert, Jr., MD,
Pedal or peroneal bypass: Which is better when both are patent? Thomas M. Bergamini, MD, Salem M. George, Jr., MD, H. Todd Massey, MD, Peter K. Henke, MD, Thomas W. Klamer, MD, Glenn E. Lambert, Jr., MD,
Eleven-year experience with tibiotibial bypass: An unusual but effective solution distal tibial artery occlusive disease and limited autologous vein
 Eleven-year experience with tibiotibial bypass: An unusual but effective solution distal tibial artery occlusive disease and limited autologous vein to Ross T. Lyon, MD, Frank J. Veith, MD, Ben U. Marsan,
Eleven-year experience with tibiotibial bypass: An unusual but effective solution distal tibial artery occlusive disease and limited autologous vein to Ross T. Lyon, MD, Frank J. Veith, MD, Ben U. Marsan,
Global Vascular Guideline on the Management of Chronic Limb Threatening Ischemia -a new foundation for evidence-based care
 Global Vascular Guideline on the Management of Chronic Limb Threatening Ischemia -a new foundation for evidence-based care Michael S. Conte MD Professor and Chief, Division of Vascular and Endovascular
Global Vascular Guideline on the Management of Chronic Limb Threatening Ischemia -a new foundation for evidence-based care Michael S. Conte MD Professor and Chief, Division of Vascular and Endovascular
Practical Point in Holistic Diabetic Foot Care 3 March 2016
 Diabetic Foot Ulcer : Vascular Management Practical Point in Holistic Diabetic Foot Care 3 March 2016 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai
Diabetic Foot Ulcer : Vascular Management Practical Point in Holistic Diabetic Foot Care 3 March 2016 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
Endovascular Should Be Considered First Line Therapy
 Revascularization of Patients with Critical Limb Ischemia Endovascular Should Be Considered First Line Therapy Michael Conte David Dawson David L. Dawson, MD Revised Presentation Title A Selective Approach
Revascularization of Patients with Critical Limb Ischemia Endovascular Should Be Considered First Line Therapy Michael Conte David Dawson David L. Dawson, MD Revised Presentation Title A Selective Approach
Combat Extremity Vascular Trauma
 Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion
 CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
The long-term value of composite limb salvage
 The long-term value of composite limb salvage grafts for John B. Chang, MD, and Theodore A. Stein, PhD, Roslyn, N.Y. Purpose: We determined the long-term efficacy of composite grafts for limb salvage when
The long-term value of composite limb salvage grafts for John B. Chang, MD, and Theodore A. Stein, PhD, Roslyn, N.Y. Purpose: We determined the long-term efficacy of composite grafts for limb salvage when
John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division
 John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division John Campbell, MD For the 12 months preceding this CME activity,
John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division John Campbell, MD For the 12 months preceding this CME activity,
Surgery is and Remains the Gold Standard for Limb-Threatening Ischemia
 Surgery is and Remains the Gold Standard for Limb-Threatening Ischemia Albeir Mousa, MD., FACS.,MPH., MBA Professor of Vascular and Endovascular Surgery West Virginia University Disclosure None What you
Surgery is and Remains the Gold Standard for Limb-Threatening Ischemia Albeir Mousa, MD., FACS.,MPH., MBA Professor of Vascular and Endovascular Surgery West Virginia University Disclosure None What you
Prosthetic graft placement and creation of a distal arteriovenous fistula for secondary vascular reconstruction in patients with severe limb ischemia
 Prosthetic graft placement and creation of a distal arteriovenous fistula for secondary vascular reconstruction in patients with severe limb ischemia Michael J. H. M. Jacobs, MD, Igor D. Gregoric, MD,
Prosthetic graft placement and creation of a distal arteriovenous fistula for secondary vascular reconstruction in patients with severe limb ischemia Michael J. H. M. Jacobs, MD, Igor D. Gregoric, MD,
Disclosures. Talking Points. An initial strategy of open bypass is better for some CLI patients, and we can define who they are
 An initial strategy of open bypass is better for some CLI patients, and we can define who they are Fadi Saab, MD, FASE, FACC, FSCAI Metro Heart & Vascular Metro Health Hospital, Wyoming, MI Assistant Clinical
An initial strategy of open bypass is better for some CLI patients, and we can define who they are Fadi Saab, MD, FASE, FACC, FSCAI Metro Heart & Vascular Metro Health Hospital, Wyoming, MI Assistant Clinical
Efficacy of the dorsal pedal salvage in diabetic patients: Short-term observations. bypass for limb
 Efficacy of the dorsal pedal salvage in diabetic patients: Short-term observations bypass for limb Frank B. Pomposelli, Jr., MD, Stephen J. Jepsen, MD, Gary W. Gibbons, MD, David R. Campbell, MD, Dorothy
Efficacy of the dorsal pedal salvage in diabetic patients: Short-term observations bypass for limb Frank B. Pomposelli, Jr., MD, Stephen J. Jepsen, MD, Gary W. Gibbons, MD, David R. Campbell, MD, Dorothy
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Diagnosis and Endovascular Treatment of Critical Limb Ischemia: What You Need to Know S. Jay Mathews, MD, MS, FACC
 Diagnosis and Endovascular Treatment of Critical Limb Ischemia: What You Need to Know S. Jay Mathews, MD, MS, FACC Interventional Cardiologist/Endovascular Specialist Bradenton Cardiology Center Bradenton,
Diagnosis and Endovascular Treatment of Critical Limb Ischemia: What You Need to Know S. Jay Mathews, MD, MS, FACC Interventional Cardiologist/Endovascular Specialist Bradenton Cardiology Center Bradenton,
LIMB SALVAGE IN THE DIABETIC PATIENT
 LIMB SALVAGE IN THE DIABETIC PATIENT WHO? HOW? BEST? DISCLOSURES Educational grant from Cook Inc OBJECTIVES Review risk stratification and staging schemes for the threatened limb Discuss current concepts
LIMB SALVAGE IN THE DIABETIC PATIENT WHO? HOW? BEST? DISCLOSURES Educational grant from Cook Inc OBJECTIVES Review risk stratification and staging schemes for the threatened limb Discuss current concepts
Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps
 e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction
 Original Article Plastic and Aesthetic Research Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction Pradeoth Mukundan
Original Article Plastic and Aesthetic Research Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction Pradeoth Mukundan
17 FibulA FlAP Tor Chiu fibula flap 153
 17 Fibula Flap Tor Chiu Fibula Flap 153 Fibula Flap FLAP TERRITORY This flap includes a segment of the fibular bone with or without the overlying skin island on the peroneal/ lateral aspect of the calf.
17 Fibula Flap Tor Chiu Fibula Flap 153 Fibula Flap FLAP TERRITORY This flap includes a segment of the fibular bone with or without the overlying skin island on the peroneal/ lateral aspect of the calf.
Steal Syndrome: The Role of the Vascular Lab
 Steal Syndrome: The Role of the Vascular Lab Eighth Overlook Noninvasive Vascular Lab Symposium Larry A. Scher, M.D. Professor of Surgery Division of Vascular Surgery Montefiore Medical Center Albert Einstein
Steal Syndrome: The Role of the Vascular Lab Eighth Overlook Noninvasive Vascular Lab Symposium Larry A. Scher, M.D. Professor of Surgery Division of Vascular Surgery Montefiore Medical Center Albert Einstein
Limb Salvage Achieved by Paramalleolar Bypass with Topical Treatment
 14 83 89 2005 Limb Salvage Achieved by Paramalleolar Bypass with Topical Treatment Nobuyoshi Azuma, Masashi Inaba, Nobuyuki Akasaka, Masae Haga, Kazutomo Goh, Yumi Sasajima, Can C Erdem and Tadahiro Sasajima
14 83 89 2005 Limb Salvage Achieved by Paramalleolar Bypass with Topical Treatment Nobuyoshi Azuma, Masashi Inaba, Nobuyuki Akasaka, Masae Haga, Kazutomo Goh, Yumi Sasajima, Can C Erdem and Tadahiro Sasajima
Realistic expectations for pedal bypass grafts in patients with end-stage renal disease
 Realistic expectations for pedal bypass grafts in patients with end-stage renal disease Steven A. Leers, MD, Thomas Reifsnyder, MD, Rick Delmonte, DPM, and Michele Caron, DPM, Pittsburgh, Pa Purpose: Limb-threatening
Realistic expectations for pedal bypass grafts in patients with end-stage renal disease Steven A. Leers, MD, Thomas Reifsnyder, MD, Rick Delmonte, DPM, and Michele Caron, DPM, Pittsburgh, Pa Purpose: Limb-threatening
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function
 Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Critical Limb Ischemia A Collaborative Approach to Patient Care. Christopher LeSar, MD Vascular Institute of Chattanooga July 28, 2017
 Critical Limb Ischemia A Collaborative Approach to Patient Care Christopher LeSar, MD Vascular Institute of Chattanooga July 28, 2017 Surgeons idea Surgeons idea represents the final stage of peripheral
Critical Limb Ischemia A Collaborative Approach to Patient Care Christopher LeSar, MD Vascular Institute of Chattanooga July 28, 2017 Surgeons idea Surgeons idea represents the final stage of peripheral
KNEE DISLOCATION. The most common injury will be an anterior dislocation, and this usually results from a hyperextension mechanism.
 KNEE DISLOCATION Introduction Dislocation of the knee is a severe injury associated with major soft tissue injury and a high incidence of damage to the popliteal artery. There is displacement of the tibia
KNEE DISLOCATION Introduction Dislocation of the knee is a severe injury associated with major soft tissue injury and a high incidence of damage to the popliteal artery. There is displacement of the tibia
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatry. Procedure List. As Of. 01 April Government of Alberta
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Non-invasive examination
 Non-invasive examination Segmental pressure and Ankle-Brachial Index (ABI) The segmental blood pressure (SBP) examination is a simple, noninvasive method for diagnosing and localizing arterial disease.
Non-invasive examination Segmental pressure and Ankle-Brachial Index (ABI) The segmental blood pressure (SBP) examination is a simple, noninvasive method for diagnosing and localizing arterial disease.
The lesser saphenous vein: Autogenous tissue for lower extremity revascularization
 The lesser saphenous vein: Autogenous tissue for lower extremity revascularization Fred A. Weaver, M.D., C. Robert Barlow, M.D., William H. Edwards, M.D., Joseph L. Mulherin, Jr., M.D., and Judith M. Jenkins,
The lesser saphenous vein: Autogenous tissue for lower extremity revascularization Fred A. Weaver, M.D., C. Robert Barlow, M.D., William H. Edwards, M.D., Joseph L. Mulherin, Jr., M.D., and Judith M. Jenkins,
Perfusion Assessment in Chronic Wounds
 Perfusion Assessment in Chronic Wounds American Society of Podiatric Surgeons Surgical Conference September 22, 2018 Michael Maier, DPM, FACCWS Cardiovascular Medicine Cleveland Clinic Disclosures Speaker,
Perfusion Assessment in Chronic Wounds American Society of Podiatric Surgeons Surgical Conference September 22, 2018 Michael Maier, DPM, FACCWS Cardiovascular Medicine Cleveland Clinic Disclosures Speaker,
Keisuke Miyake 1,2, Shinsuke Kikuchi 1, Hiroko Okuda 1, Atsuhiro Koya 1, Satomi Abe 3, Yoshiki Sawa 2, Tetsuo Ota 4 and Nobuyoshi Azuma 1*
 Miyake et al. Surgical Case Reports (2018) 4:40 https://doi.org/10.1186/s40792-018-0449-9 CASE REPORT Open Access Successful limb salvage through staged bypass combined with free gracilis muscle transfer
Miyake et al. Surgical Case Reports (2018) 4:40 https://doi.org/10.1186/s40792-018-0449-9 CASE REPORT Open Access Successful limb salvage through staged bypass combined with free gracilis muscle transfer
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Chronic Critical Limb Ischemia: Diagnosis, Treatment and Prognosis
 Chronic Critical Limb Ischemia: Diagnosis, Treatment and Prognosis JAMIE D. SANTILLI, M.D., and STEVEN M. SANTILLI, M.D., PH.D. University of Minnesota School of Medicine Minneapolis, Minnesota Chronic
Chronic Critical Limb Ischemia: Diagnosis, Treatment and Prognosis JAMIE D. SANTILLI, M.D., and STEVEN M. SANTILLI, M.D., PH.D. University of Minnesota School of Medicine Minneapolis, Minnesota Chronic
Distal By-Pass procedures can reduce limb loss
 Conventional treatment of the diabetic foot Distal By-Pass procedures can reduce limb loss Dr. Nikolaos Melas, PhD Vascular and Endovascular Surgeon Military Doctor Associate in 1st department of Surgery,
Conventional treatment of the diabetic foot Distal By-Pass procedures can reduce limb loss Dr. Nikolaos Melas, PhD Vascular and Endovascular Surgeon Military Doctor Associate in 1st department of Surgery,
Limb Salvage in Diabetic Ischemic Foot. Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017
 Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Imaging Strategy For Claudication
 Who are the Debators? Imaging Strategy For Claudication Duplex Ultrasound Alone is Adequate to Select Patients for Endovascular Intervention - Pro: Dennis Bandyk MD No Disclosures PRO - Vascular Surgeon
Who are the Debators? Imaging Strategy For Claudication Duplex Ultrasound Alone is Adequate to Select Patients for Endovascular Intervention - Pro: Dennis Bandyk MD No Disclosures PRO - Vascular Surgeon
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Transmetatarsal amputation in an at-risk diabetic population: a retrospective study
 The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
Current Vascular and Endovascular Management in Diabetic Vasculopathy
 Current Vascular and Endovascular Management in Diabetic Vasculopathy Yang-Jin Park Associate professor Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine Peripheral artery
Current Vascular and Endovascular Management in Diabetic Vasculopathy Yang-Jin Park Associate professor Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine Peripheral artery
Peripheral Artery Disease Interventions Utilizing the Angiosomal Approach to the Complex Wound
 Peripheral Artery Disease Interventions Utilizing the Angiosomal Approach to the Complex Wound Craig M. Walker, MD, FACC, FACP Chairman, New Cardiovascular Horizons Clinical Professor of Medicine Tulane
Peripheral Artery Disease Interventions Utilizing the Angiosomal Approach to the Complex Wound Craig M. Walker, MD, FACC, FACP Chairman, New Cardiovascular Horizons Clinical Professor of Medicine Tulane
Role of ABI in Detecting and Quantifying Peripheral Arterial Disease
 Role of ABI in Detecting and Quantifying Peripheral Arterial Disease Difference in AAA size between US and Surgeon 2 1 0-1 -2-3 0 1 2 3 4 5 6 7 Mean AAA size between US and Surgeon Kathleen G. Raman MD,
Role of ABI in Detecting and Quantifying Peripheral Arterial Disease Difference in AAA size between US and Surgeon 2 1 0-1 -2-3 0 1 2 3 4 5 6 7 Mean AAA size between US and Surgeon Kathleen G. Raman MD,
Access strategy for chronic total occlusions (CTOs) is crucial
 Learn How Access Strategy Impacts Complex CTO Crossing Arthur C. Lee, MD The Cardiac & Vascular Institute, Gainesville, Florida VASCULAR DISEASE MANAGEMENT 2018;15(3):E19-E23. Key words: chronic total
Learn How Access Strategy Impacts Complex CTO Crossing Arthur C. Lee, MD The Cardiac & Vascular Institute, Gainesville, Florida VASCULAR DISEASE MANAGEMENT 2018;15(3):E19-E23. Key words: chronic total
Practical Point in Diabetic Foot Care 3-4 July 2017
 Diabetic Foot Ulcer : Role of Vascular Surgeon Practical Point in Diabetic Foot Care 3-4 July 2017 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai University
Diabetic Foot Ulcer : Role of Vascular Surgeon Practical Point in Diabetic Foot Care 3-4 July 2017 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai University
The earlier clinic experience of the reverse-flow anterolateral thigh island flap
 British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report
 CASE REPORTS Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report Evan S. Cohen,/VII), Robert B. Holtzman, MD, and George W. Johnson, Jr., MD, Houston,
CASE REPORTS Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report Evan S. Cohen,/VII), Robert B. Holtzman, MD, and George W. Johnson, Jr., MD, Houston,
Femoral Artery. Its entrance to the thigh Position Midway between ASIS and pubic symphysis
 Lower Limb Vessels Lecture Objectives Describe the major arteries of the lower limb. Describe the deep and superficial veins of the lower limb. Describe the topographical relationships of the arteries
Lower Limb Vessels Lecture Objectives Describe the major arteries of the lower limb. Describe the deep and superficial veins of the lower limb. Describe the topographical relationships of the arteries
Resident Teaching Conference 3/12/2010
 Resident Teaching Conference 3/12/2010 Goals Definition and Classification of Acute Limb Ischemia Clinical Assessment of the Vascular Patient History and Physical Diagnostic Modalities Management of Acute
Resident Teaching Conference 3/12/2010 Goals Definition and Classification of Acute Limb Ischemia Clinical Assessment of the Vascular Patient History and Physical Diagnostic Modalities Management of Acute
ORIGINAL ARTICLE DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS
 DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abscess, with diabetic foot ulcers, 472 Achilles tendon, in calcanectomy, for osteomyelitis, 473, 483 in calcaneus anatomy, 477 478 in Syme
Note: Page numbers of article titles are in boldface type. A Abscess, with diabetic foot ulcers, 472 Achilles tendon, in calcanectomy, for osteomyelitis, 473, 483 in calcaneus anatomy, 477 478 in Syme
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/30/2012 Radiology Quiz of the Week # 79 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/30/2012 Radiology Quiz of the Week # 79 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Disclosure. Speaker name: Prof. Hesham Aly Sharaf El-Din. I do not have any potential conflict of interest
 Disclosure Speaker name: Prof. Hesham Aly Sharaf El-Din I do not have any potential conflict of interest Introduction 5% of patients with upper limb AVF develop ipsilateral hand ischemia, recently termed
Disclosure Speaker name: Prof. Hesham Aly Sharaf El-Din I do not have any potential conflict of interest Introduction 5% of patients with upper limb AVF develop ipsilateral hand ischemia, recently termed
Case Discussion. Disclosures. Critical Limb Ischemia: A Selective Approach to Revascularization Works Best 4/28/2012. None. 58 yo M, DM, CAD, HTN
 Critical Limb Ischemia: A Selective Approach to Revascularization Works Best None Disclosures Michael S. Conte MD, FACS Division of Vascular and Endovascular Surgery Co-Director, Heart and Vascular Center
Critical Limb Ischemia: A Selective Approach to Revascularization Works Best None Disclosures Michael S. Conte MD, FACS Division of Vascular and Endovascular Surgery Co-Director, Heart and Vascular Center
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage
 Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
A new method for the prediction of peripheral vascular resistance from the preoperative angiogram
 A new method for the prediction of peripheral vascular resistance from the preoperative angiogram Wayne W. LaMorte, M.D., James O. Menzoian, M.D., Anton Sidawy, M.D., and Timothy Heeren, Ph.D., Boston,
A new method for the prediction of peripheral vascular resistance from the preoperative angiogram Wayne W. LaMorte, M.D., James O. Menzoian, M.D., Anton Sidawy, M.D., and Timothy Heeren, Ph.D., Boston,
THE popliteal artery is the second most common site of aneurysm. The
 POPLITEAL ANEURYSM Treatment by Vein Graft: Case Report A. W. HUMPHRIES, M.D. Department of Orthopedic Surgery F. A. LeFEVRE, M.D. and V. G. dewolfe, M.D. Department of Cardiovascular Disease THE popliteal
POPLITEAL ANEURYSM Treatment by Vein Graft: Case Report A. W. HUMPHRIES, M.D. Department of Orthopedic Surgery F. A. LeFEVRE, M.D. and V. G. dewolfe, M.D. Department of Cardiovascular Disease THE popliteal
Disclosures. Tips and Tricks for Tibial Intervention. Tibial intervention overview
 Tips and Tricks for Tibial Intervention Donald L. Jacobs, MD C Rollins Hanlon Endowed Professor and Chair Chair of Surgery Saint Louis University SSM-STL Saint Louis University Hospital Disclosures Abbott
Tips and Tricks for Tibial Intervention Donald L. Jacobs, MD C Rollins Hanlon Endowed Professor and Chair Chair of Surgery Saint Louis University SSM-STL Saint Louis University Hospital Disclosures Abbott
Clinical teaching/experi ence. Lectures/semina rs/conferences Self-directed. learning. Clinical teaching/experi ence
 Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Current Status of Endovascular Therapies for Critical Limb Ischemia
 Current Status of Endovascular Therapies for Critical Limb Ischemia Bulent Arslan, MD Associate Professor of Radiology Director, Vascular & Interventional Radiology Rush University Medical Center bulent_arslan@rush.edu
Current Status of Endovascular Therapies for Critical Limb Ischemia Bulent Arslan, MD Associate Professor of Radiology Director, Vascular & Interventional Radiology Rush University Medical Center bulent_arslan@rush.edu
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Acute arterial complications associated with total hip and knee arthroplasty
 From the Eastern Vascular Society Acute arterial complications associated with total hip and knee arthroplasty Keith D. Calligaro, MD, a Matthew J. Dougherty, MD, a Sean Ryan, MD, a and Robert E. Booth,
From the Eastern Vascular Society Acute arterial complications associated with total hip and knee arthroplasty Keith D. Calligaro, MD, a Matthew J. Dougherty, MD, a Sean Ryan, MD, a and Robert E. Booth,
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
The posterior approach to popliteal-crural bypass
 The posterior approach to popliteal-crural bypass Kenneth Ourie1, MD, Rochester) N. Y. Purpose: An evaluation of the posterior approach to popliteal-crural bypass was performed to assess the feasibility
The posterior approach to popliteal-crural bypass Kenneth Ourie1, MD, Rochester) N. Y. Purpose: An evaluation of the posterior approach to popliteal-crural bypass was performed to assess the feasibility
Popliteal Aneurysm: When is surgical therapy indicated? PROF. GRZEGORZ OSZKINIS
 Popliteal Aneurysm: When is surgical therapy indicated? PROF. GRZEGORZ OSZKINIS Asymptomatic mass - 38-40%will develop symptoms at a rate of 14%/yr Intermittent claudic ation (chronic ischemia) - 25%-40%
Popliteal Aneurysm: When is surgical therapy indicated? PROF. GRZEGORZ OSZKINIS Asymptomatic mass - 38-40%will develop symptoms at a rate of 14%/yr Intermittent claudic ation (chronic ischemia) - 25%-40%
Acknowledgements. No tengo conflictos de interés que revelar. I have no conflicts of interest to disclose. Michael S. Conte. David G.
 No tengo conflictos de interés que revelar I have no conflicts of interest to disclose. Critical Limb Ischemia : The Need for a New System to Define Disease Burden and Stratify Amputation Risk and Need
No tengo conflictos de interés que revelar I have no conflicts of interest to disclose. Critical Limb Ischemia : The Need for a New System to Define Disease Burden and Stratify Amputation Risk and Need
Free Flap Salvage in Lower Extremity Reconstruction via Use of Contralateral Lower Extremity Recipient Vessels
 THIEME Case Report 117 Free Flap Salvage in Lower Extremity Reconstruction via Use of Contralateral Lower Extremity Recipient Vessels KatelynG.Bennett,MD 1 Brian P. Kelley, MD 1 Theodore A. Kung, MD 1
THIEME Case Report 117 Free Flap Salvage in Lower Extremity Reconstruction via Use of Contralateral Lower Extremity Recipient Vessels KatelynG.Bennett,MD 1 Brian P. Kelley, MD 1 Theodore A. Kung, MD 1
ABSTRACT. Key words: Flaps, Adipofascial, Lower limb reconstruction. Khaldoun J. Haddadin, MD*, Samer Y. Haddad, MD. Introduction.
 DISTALLY BASED ADIPOFASCIAL FLAPS: A VERSATILE FLAP FOR THE RECONSTRUCTION OF LOWER LEG AND PROXIMAL FOOT DEFECTS AT THE ROYAL JORDANIAN REHABILITATION CENTER Khaldoun J. Haddadin, MD*, Samer Y. Haddad,
DISTALLY BASED ADIPOFASCIAL FLAPS: A VERSATILE FLAP FOR THE RECONSTRUCTION OF LOWER LEG AND PROXIMAL FOOT DEFECTS AT THE ROYAL JORDANIAN REHABILITATION CENTER Khaldoun J. Haddadin, MD*, Samer Y. Haddad,
Acute arterial thrombosis associated with total knee arthroplasty
 Acute arterial thrombosis associated with total knee arthroplasty Keith D. Calligaro, MD, Dominic A. DeLaurentis, MD, Robert E. Booth, MD, Richard H. Rothman, MD, Ronald P. Savarese, MD, and Matthew J.
Acute arterial thrombosis associated with total knee arthroplasty Keith D. Calligaro, MD, Dominic A. DeLaurentis, MD, Robert E. Booth, MD, Richard H. Rothman, MD, Ronald P. Savarese, MD, and Matthew J.
Is the preferential use of polytetrafluoroethylene grafts for femoropopliteal bypass justified?
 Is the preferential use of polytetrafluoroethylene grafts for femoropopliteal bypass justified? William J. Quifiones-Baldrich, MD, Ronald W. Busuttil, MD, PhD, J. Dennis Baker, MD, Candace L. Vescera,
Is the preferential use of polytetrafluoroethylene grafts for femoropopliteal bypass justified? William J. Quifiones-Baldrich, MD, Ronald W. Busuttil, MD, PhD, J. Dennis Baker, MD, Candace L. Vescera,
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abscesses, 27 30 Acellular products, for bone healing, 55 56 Acetaminophen, 79 80 Achilles tendon lengthening, for pediatric flatfoot,
Index Note: Page numbers of article titles are in boldface type. A Abscesses, 27 30 Acellular products, for bone healing, 55 56 Acetaminophen, 79 80 Achilles tendon lengthening, for pediatric flatfoot,
Gross Anatomy Coloring Book Series. Lower Extremity Arteries
 Gross Anatomy Coloring Book Series Lower Extremity Arteries 1 Femoral Artery and Associated Branches For the life of the flesh is in the blood. Leviticus 17:11 Femoral Artery and Associated Branches After
Gross Anatomy Coloring Book Series Lower Extremity Arteries 1 Femoral Artery and Associated Branches For the life of the flesh is in the blood. Leviticus 17:11 Femoral Artery and Associated Branches After
Lower Extremity Reconstruction
 1 Chapter 21 Overview: Lower Extremity Reconstruction Louis Carter This subject is also partially covered in the chapters Flaps for Wound Coverage and Perforator Flaps. This chapter will deal with reconstruction
1 Chapter 21 Overview: Lower Extremity Reconstruction Louis Carter This subject is also partially covered in the chapters Flaps for Wound Coverage and Perforator Flaps. This chapter will deal with reconstruction
AN ABNORMAL UNILATERAL ORIGIN OF DORSALIS PEDIS ARTERY- A CASE REPORT
 AN ABNORMAL UNILATERAL ORIGIN OF DORSALIS PEDIS ARTERY- A CASE REPORT Authors:- Dr. Hetal Vaishnani, Dr.Subhsh Gujar, Dr.Savita Gadekar, Dr.K.V.Bondre, Dr.G.V.Shah Department of Anatomy S.B.K.S.Medical
AN ABNORMAL UNILATERAL ORIGIN OF DORSALIS PEDIS ARTERY- A CASE REPORT Authors:- Dr. Hetal Vaishnani, Dr.Subhsh Gujar, Dr.Savita Gadekar, Dr.K.V.Bondre, Dr.G.V.Shah Department of Anatomy S.B.K.S.Medical
PAD and CRITICAL LIMB ISCHEMIA: EVALUATION AND TREATMENT 2014
 PAD and CRITICAL LIMB ISCHEMIA: EVALUATION AND TREATMENT 2014 Van Crisco, MD, FACC, FSCAI First Coast Heart and Vascular Center, PLLC Jacksonville, FL 678-313-6695 Conflict of Interest Bayer Healthcare
PAD and CRITICAL LIMB ISCHEMIA: EVALUATION AND TREATMENT 2014 Van Crisco, MD, FACC, FSCAI First Coast Heart and Vascular Center, PLLC Jacksonville, FL 678-313-6695 Conflict of Interest Bayer Healthcare
Anthony J. Cavallo, DPM Sentara Podiatry Specialists 4/27/2018. Lose a toe, Save a Limb: The Value of Complex Foot Reconstructions
 Anthony J. Cavallo, DPM Sentara Podiatry Specialists 4/27/2018 Lose a toe, Save a Limb: The Value of Complex Foot Reconstructions Objectives Review the morbidity and mortality associated with amputation
Anthony J. Cavallo, DPM Sentara Podiatry Specialists 4/27/2018 Lose a toe, Save a Limb: The Value of Complex Foot Reconstructions Objectives Review the morbidity and mortality associated with amputation
Social History. Retired internist 2 scotches a day 50 pack-year history, stopped in 2005
 April 17, 2008 HPI 78 year old internist complains of 10 days of tingling and discomfort in left toes Unable to walk or sleep due to severe pain Pain worse with movement Redness in left toes Bilateral
April 17, 2008 HPI 78 year old internist complains of 10 days of tingling and discomfort in left toes Unable to walk or sleep due to severe pain Pain worse with movement Redness in left toes Bilateral
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications
 Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Distal hybrids - an option in long SFA CTO accompanied by severely compromized crural runoff
 Distal hybrids - an option in long SFA CTO accompanied by severely compromized crural runoff P. Kuryanov, A. Lipin, A. Antropov, K. Atmadzas, A. Atmadzas, Y. Eminov, A. Borisov, R. Sobolev, A.Orlov Limb
Distal hybrids - an option in long SFA CTO accompanied by severely compromized crural runoff P. Kuryanov, A. Lipin, A. Antropov, K. Atmadzas, A. Atmadzas, Y. Eminov, A. Borisov, R. Sobolev, A.Orlov Limb
Critical Limb Ischemia: Diagnosis and Current Management
 Research Article Joseph Karam, MD Elliot J. Stephenson, MD From: Minneapolis Heart Institutet at Abbott Northwestern Hospital, Minneapolis, MN Address for correspondence: Joseph Karam, MD Minneapolis Heart
Research Article Joseph Karam, MD Elliot J. Stephenson, MD From: Minneapolis Heart Institutet at Abbott Northwestern Hospital, Minneapolis, MN Address for correspondence: Joseph Karam, MD Minneapolis Heart
Angiosome revascularization strategies in real world practice: how much difference does it make?
 Angiosome revascularization strategies in real world practice: how much difference does it make? Peter A. Schneider, MD Kaiser Foundation Hospital Honolulu, Hawaii Disclosure Peter A. Schneider... I have
Angiosome revascularization strategies in real world practice: how much difference does it make? Peter A. Schneider, MD Kaiser Foundation Hospital Honolulu, Hawaii Disclosure Peter A. Schneider... I have
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Clinical and social consequences of Buerger disease
 Clinical and social consequences of Buerger disease Takashi Ohta, MD, Hiroyuki Ishioashi, MD, Minoru Hosaka, MD, and Ikuo Sugimoto, MD, Aichi, Japan Purpose: This study was undertaken to assess the clinical
Clinical and social consequences of Buerger disease Takashi Ohta, MD, Hiroyuki Ishioashi, MD, Minoru Hosaka, MD, and Ikuo Sugimoto, MD, Aichi, Japan Purpose: This study was undertaken to assess the clinical
