PREFACE INTRODUCTION TO THE EMG TRAINING PROGRAM MANUAL
|
|
|
- Robert Small
- 5 years ago
- Views:
Transcription
1 PREFACE Welcome to the Electromyography Laboratory (EMG) and the Neuromuscular Program. In the following months you will be exposed to the anatomic, physiologic, clinical, and technical information necessary to perform electrodiagnostic studies. You will work closely with physician, nursing, and EMG technologist staff members who will guide you through the training process. The knowledge acquired during your training will be applicable to your clinical practice and enhance your understanding of neuromuscular pathophysiology. This knowledge will be acquired through direct teaching efforts of the staff and independent study. Opportunities are available to participate in research, although the major emphasis is clinical. We welcome and expect your active participation in the laboratory and sincerely hope you find the EMG training period productive and enjoyable. INTRODUCTION TO THE EMG TRAINING PROGRAM MANUAL The Electromyography Training Manual is a compilation of resident responsibilities, weekly lecture and clinic schedules, and didactic material. Residents and fellows should use this manual as a guide to learning the clinical and technical information necessary to perform electrodiagnostic studies. The manual defines the resident s responsibilities and lecture schedules. The manual serves as a supplement to texts, journals, and didactic teaching sessions and should not be used in lieu of other sources of information. The manual will be updated from time to time. Please take time to familiarize yourself with this manual prior to beginning the training period or within the first day or two in the EMG Laboratory. EMG LABORATORY STAFF Faculty James W. Teener, MD Director, Neuromuscular Program James K. Richardson, MD Director, Physical Medicine and Rehabilitation James W. Albers, MD, PhD Emeritus Professor of Neurology Brian Callaghan, MD Anthony E. Chiodo, MD Anita S. Craig, DO Lisa A. DiPonio, MD James T. Eckner, MD Eva L. Feldman, MD, PhD Gary W. Gallagher, MD Stephen Goutman, MD Anne G. Hartigan, MD Edward A. Hurvitz, MD Ann T. Laidlaw, MD James A. Leonard, Jr., MD Ann A. Little, MD Zachary London, MD Mary C. Spires, MD Mark J. Ziadeh, MD Page 1 of 2
2 LECTURES Every Wednesday at 7:15 a.m. there is an EMG Conference dedicated to fundamentals of electromyography. The topics repeat every 3 to 4 months so you will be able to hear the majority of these basic lectures during a 3 month neuromuscular elective. The residents also participate in the Wednesday 8:00 a.m. Neuromuscular Conference series. On the second Wednesday of every other month, the residents in the EMG Laboratory are responsible for organizing and presenting the conference. The Neuromuscular Fellows are responsible for the alternate Wednesday. You are free to choose any topic. We recommend avoiding esoteric topics. In addition, the residents or fellows write protocols and present the assigned case and EMG findings for the Neuromuscular Pathology Conference on the fourth Wednesday each month. The resident should have an understanding of the case including the EMG and biopsy findings and develop a differential diagnosis based on these findings. Ideally, the resident should arrange to meet with Dr. Mila Blaivas, the neuromuscular pathologist, to review the biopsy prior to the conference. The case and EMG findings should be discussed with the staff person assigning the cases prior to presentation. The residents attend all scheduled EMG/Neuromuscular Conferences and Neurology or PM&R Grand Rounds while in the EMG Laboratory. We welcome your attendance at all times throughout the rest of the year as well. Every Wednesday afternoon, after the last case has been completed, there is an informal discussion of interesting or problematic cases. Page 2 of 2
3 EMG ROTATION OBJECTIVES Zach London, MD University of Michigan Updated 6/23/2010 General Objectives for the Rotation I. KNOWLEDGE A. Peripheral nervous system anatomy B. Diseases and disorders of the peripheral nervous system C. Neuromuscular physiology D. Fundamentals of electromyography E. Normal values F. Ethics G. Infection control practices II. III. PHYSICAL SKILLS A. Electrode placement for nerve conduction studies B. Muscle localization and needle EMG technique C. Operating the EMG machine D. Entering data and generating a report INTERPRETATION SKILLS A. Interpretation of waveforms on nerve conduction studies and needle EMG B. Designing a logical approach to deciding which nerves and muscles to study C. Interpreting studies (localization, severity, pathophysiology, etc.) D. Using the interpretation to guide management of the patient You are encouraged to take advantage of every opportunity to do nerve conduction studies and operate the computers under supervision during the first month of your rotation. You will not be allowed to do your own needle examinations until you have passed the following tests: Nerve Conduction Studies Test Machine Test Written Test Please note: All objectives written in black are key concepts that will be tested on the EMG multiple choice test at day of the rotation. Objectives in red are concepts that you should learn by the end of the rotation, but will not be on the tests we give you. Page 1 of 16
4 NERVE CONDUCTION STUDIES TEST (Goal Day 5 of the rotation) Be able to set up nerve conduction studies for the following studies: 1. Sensory studies A. Median at the wrist B. Ulnar at the wrist C. Median midpalmar D. Ulnar midpalmar E. Radial at the forearm F. Sural at the calf G. Superficial peroneal at the ankle 2. Motor studies A. Median at the wrist B. Ulnar at the wrist C. Musculocutaneous motor at the axilla D. Spinal accessory at the trapezius E. Peroneal at the ankle F. Tibial at the ankle MACHINE TEST (Goal Day 10 of the rotation) 1. Know the following machine settings A. Sensory 1. Gain 2. Time Base 3. Filters B. Motor 1. Gain 2. Time Base 3. Filters C. F-response 1. Gain 2. Upper extremity time base 3. Lower extremity time base D. Needle 1. Filters 2. Be able to do the following nerve conduction studies A. Median sensory at the wrist (be able to recognize the amplitude, onset latency and peak latency) B. Ulnar motor at the wrist (be able to recognize amplitude and onset latency) C. Ulnar motor below the elbow (be able to recognize amplitude and onset latency, and calculate the conduction velocity in the forearm) D. Ulnar F-response E. Ulnar repetitive stimulation Page 2 of 16
5 EMG WRITTEN TEST (Goal Day of the rotation) OUTLINE I. Basic Concepts of Electricity and Electronics in Clinical EMG II. Nerve Conduction Studies III. Normal values IV. Repetitive Stimulation V. Needle EMG Resting Muscle VI. Needle EMG Motor Unit Activity VII. Electrodiagnostic Findings in Common Clinical Scenarios VIII. Pathophysiology of Peripheral Neuropathies IX. Normal Anatomy X. Compressive Neuropathies 1: Median Nerve XI. Compressive Neuropathies 2: Ulnar Nerve XII. Compressive Neuropathies 3: Peroneal Nerve XIII. Compressive Neuropathies 4: Radial Nerve XIV. Compressive Neuropathies 5: Uncommon Compressive Neuropathies XV. Anomalous Innervation XVI. Axonal vs. Demyelinating Neuropathy XVII. Radiculopathies and Plexopathies XVIII. Cranial Nerve Studies XIX. Motor Neuron Disease XX. Introduction to Muscle Pathology XXI. The Muscular Dystrophies XXII. Inflammatory/Metabolic Myopathies XXIII. Congenital/Storage Myopathies XXIV. Myotonia XXV. Neuromuscular Complications of Cancer XXVI. An Approach to the Diagnosis of Neuromuscular Disease in the Floppy Infant XXVII. SFEMG I. Basic Concepts of Electricity and Electronics in Clinical EMG A. What is charge? B. What is voltage? C. What is current? D. What is impedance? E. What are filters? F. What are amplifiers? II. Nerve Conduction Studies A. What is the difference between the anode and the cathode? B. What are the filter settings and gain settings for sensory and motor NCS? C. Where should G1 and G2 be placed? Page 3 of 16
6 D. What is the signal-to-noise ratio and when is this important? What can be done to improve the response? E. Motor Amplitude 1. What is the physiologic basis of the motor amplitude? 2. What are the units used to measure it? 3. Why do we record over the muscle motor point? 4. What types of disorders cause a reduction of the CMAP amplitude and how can these be distinguished electrodiagnostically? F. Sensory amplitude 1. What is the physiologic basis of the sensory amplitude? 2. What are the units used to measure it? 3. What is the localization value of a normal versus abnormal sensory amplitude in the setting of both normal and abnormal motor amplitudes in the corresponding motor nerve? G. Motor latency 1. What is the significance of the motor latency? 2. Do we look at the onset or peak? 3. What are the units? H. Sensory latency 1. What is the significance of the sensory latency? 2. Do we look at the onset or peak? 3. What are the units? I. Conduction velocity 1. What is the physiologic basis of a slow conduction velocity? 2. How do you calculate conduction velocity in a motor nerve? 3. What are the units? 4. Why do you need to stimulate at two different sites along the nerve for a motor conduction velocity but not for a sensory conduction velocity? J. What is the difference between and orthodromic and an antidromic study? K. Pitfalls 1. How can you tell if you re not over the motor point of the muscle? 2. What will happen to the NCS responses if the patient s skin is too cold (<32C)? 3. What is the significance of supramaximal stimulation? 4. What does 60 Hz interference look like and what can be done to eliminate it? L. F-response 1. What is the physiologic basis of the F-response? 2. How is the F-response performed? 3. Are the afferent and efferent arms of the F-response sensory or motor? 4. Is there a synapse in an F-response? 5. What disease states correlate with a prolonged F-response? 6. Do F-responses detect radiculopathies not found on needle exam? 7. Do you apply a supramaximal or submaximal stimulus in the F-response? M. H-Reflex 1. Are the afferent and efferent arms of the H-reflex sensory or motor? 2. Is there a synapse in the H-reflex? 3. What is the best nerve to study the H-reflex? 4. Do you apply a supramaximal or submaximal stimulus in the H-reflex? 5. What disease states correlate with a prolonged H-reflex? Page 4 of 16
7 6. Do H-reflexes detect radiculopathies not found on needle exam? N. Physical Skills. How do you set up each of these nerve conduction studies? 1. Sensory nerves a. Median at the wrist b. Ulnar at the wrist c. Median midpalmar d. Ulnar midpalmar e. Radial at the forearm f. Sural at the calf g. Medial and lateral antebrachial cutaneous h. Lateral femoral cutaneous i. Superficial peroneal j. Medial plantar k. Lateral plantar 2. Motor nerves a. Ulnar b. Median c. Peroneal d. Tibial e. Musculocutaneous f. Radial g. Facial h. Spinal accessory i. Femoral j. Phernic III. Normal Values A. Sensory nerves. What are the normal amplitudes and latencies for each of these nerves? 1. Median 2. Ulnar 3. Median midpalmar 4. Ulnar midpalmar 5. Radial 6. Sural B. Motor nerves. What are the normal amplitudes and latencies for each of these nerves? 1. Ulnar 2. Median 3. Peroneal 4. Tibial 5. Facial C. What is a normal upper extremity motor conduction velocity? D. What is a normal lower extremity conduction velocity? E. F-responses. 1. What is a normal median/ulnar F-wave value? 2. What is a normal tibial/peroneal F-wave value? F. What is a normal tibial/soleus H-reflex value? Page 5 of 16
8 G. How are normal values affected by 1. Height 2. Age 3. Lower extremities vs. upper extremities 4. Proximal vs. distal segments of the same nerve IV. Repetitive Stimulation A. Which nerves are typically studied with repetitive simulation? B. What is the rate of stimulation that is given? C. Regarding the physiology of the neuromuscular junction 1. How is Ach synthesized? 2. What are quanta? 3. What is a mini-endplate potential (MEPP)? 4. What is an end-plate potential (EPP)? 5. What is a muscle fiber action potential (MFAP)? D. Explain the significance of primary, secondary, and tertiary stores of acetylcholine in neuromuscular transmission, and the ramifications of these various stores on repetitive stimulation testing. E. Describe the exercise protocol with repetitive stimulation. F. What is post-exercise facilitation and in which disorders is this a prominent finding? G. What are the expected findings with repetitive stimulation in each of the following disorders: 1. Myasthenia gravis 2. Lambert Eaton Myasthenic Syndrome 3. Botulinum intoxication V. Needle EMG - Resting Muscle A. How many locations should be evaluated in each muscle? B. What sweep speed and sensitivity are best for observing spontaneous activity? C. What sweep speed and sensitivity are best for observing voluntary motor units? D. Insertional activity 1. What causes increased insertional activity? 2. What causes decreased insertional activity? E. Endplate noise 1. What is endplate noise? 2. Are endplate spikes regular or irregular? 3. Is the initial deflection positive or negative? F. Fibrillation potentials and positive sharp waves 1. What is the physiologic basis of fibrillations and positive sharp waves? 2. How fast do fibrillations fire? (0.5-10Hz) How does this compare to normal motor units? (5-50 Hz) 3. Are fibrillations generally regular or irregular? 4. Is the initial deflection positive or negative? 5. What is the significance of tiny fibrillation potentials? 6. How long after nerve injury do positive waves and fibrillations appear? 7. What disease states other than nerve injury can produce positive waves and fibrillations? Page 6 of 16
9 8. Fibrillations are graded on a scale of What is the difference between 1+, 2+, 3+, and 4+ fibrillations? 9. Which myopathies can cause fibrillations? 10. Which myopathies generally do not cause fibrillations? 11. After denervation, please note that fibrillations may continue until complete reinnervation has occurred. G. Complex repetitive discharges 1. What causes complex repetitive discharges? 2. What is the appearance of a complex repetitive discharge on needle EMG? H. Myotonia 1. What is myotonia? 2. What are the features of a myotonic discharge on EMG? 3. What disease states are associated with myotonic discharges? 4. How can complex repetitive discharges be distinguished from myotonic discharges? I. Fasciculations 1. What is the physiologic difference between a fasciculation and a fibrillation? 2. Are fasciculations regular or irregular? 3. At what rate do fasciculations fire? 4. What conditions or disease states are associated with fasciculations? J. Myokymia 1. How can myokymia be distinguished from complex repetitive discharges? 2. How can myokymia be distinguished from tremor? 3. What disease states cause myokymia? K. What is the difference between cramp and neuromyotonia? VI. Needle EMG Motor Unit Activity A. How do you know you are recording directly over a motor unit action potential? B. Duration 1. What does the duration of a motor unit action potential (MUAP) reflect? 2. What is the physiologic basis for prolonged duration in neurogenic disease? 3. What does a long duration MUAP sound like? 4. What is the importance of MUAP rise time? C. Polyphasia 1. How do you calculate the number of phases in a MUAP? 2. In normals, what percent of MUAPs have 3 or 4 phases? 3. What is the morphological difference between phases and serrations? 4. What is the physiologic basis for increased polyphasia in neurogenic disease? 5. What is the physiologic basis for increased polyphasia in myopathic disease? D. Satellite potential 1. What does a satellite potential look like? 2. What is the physiologic basis for a satellite potential? E. Amplitude 1. What is the upper limit of normal for the amplitude of a MUAP? 2. What does the amplitude of a MUAP reflect? 3. What is the physiologic basis for high amplitude MUAPs in neurogenic disease? 4. What is the physiologic basis for low amplitude MUAPs in myopathic disorders? 5. What does a high-amplitude MUAP sound like? Page 7 of 16
10 F. Recruitment 1. What is the slowest frequency at which a voluntary motor unit can fire? 2. In a normal recruitment pattern, what is the ratio of firing frequency (in Hertz) of the fastest motor unit to number of units firing? 3. What is the difference between reduced recruitment and reduced activation? VII. Electrodiagnostic Findings in Common Clinical Scenarios A. In each of the following conditions, describe what would be expected on nerve conduction studies (sensory, motor and F-responses) and needle EMG (including the pattern of abnormal spontaneous activity, MUAP duration, amplitude, polyphasia, and recruitment) 1. Axonal loss a. Hyperacute axonal loss (<3d) b. Acute axonal loss (>1 week, <3-6 weeks) c. Subacute axonal loss (>3-6 weeks, <2-3 months) d. Subacute to chronic axonal loss (>2-3 months, <many months/years) e. Chronic axonal loss (>many months/years) 2. Demyelinating disease a. Acquired demyelinating polyneuropathy b. Hereditary demyelinating polyneuropathy c. Focal demyelination (a single distal lesion) 3. Myopathy producing muscle fiber necrosis 4. Myopathy not producing muscle fiber necrosis (metabolic myopathy) 5. Neuromuscular Junction Lesions (excluding abnormalities seen on repetitive stimulation and single fiber EMG) 6. Central nervous system disease B. What is the electrodiagnostic approach to the diagnosis of: 1. Painless weakness 2. Unsteady gait 3. Rhabdomyolysis 4. Elevated serum CK levels 5. Muscle cramps 6. Foot drop 7. Wrist drop/hand weakness VIII. Pathophysiology of Peripheral Neuropathies A. What is neurapraxia? B. What is neurotmesis? C. What is axonotmesis? D. What is Wallerian degeneration and how does it occur? E. Describe the histology of normal nerves and connective tissue. F. What are the effects on conduction of an axonopathy? IX. Normal Anatomy A. What are the nerve, nerve root, and trunk innervations of the following upper extremity muscles? 1. Rhomboids 2. Supraspinatus Page 8 of 16
11 3. Infraspinatus 4. Deltoid 5. Biceps Brachii 6. Serratus Anterior 7. Pectoralis Major clavicular 8. Pectoralis Major sternocostal 9. Brachioradialis 10. Ext carpi radialis longus 11. Triceps 12. Extensor carpi Ulnaris 13. Extensor digitorum communis 14. Extensor indicis 15. Extensor pollicis longus 16. Supinator 17. Pronator teres 18. Flexor carpi radialis 19. Flexor pollicis longus 20. Flexor digitorum profundus 1&2 21. Flexor digitorum superficialis 22. Abductor pollicis brevis 23. Opponens pollicis 24. Flexor carpi ulnaris 25. Flexor digitorum profundus 4&5 26. First dorsal interosseus of the hand 27. Abductor digiti quinti of the hand B. What are the nerve and nerve root innervations of the following lower extremity muscles? 1. Iliopsoas 2. Sartorius 3. Rectus femoris 4. Vastus lateralis 5. Vastus medialis 6. Adductor longus 7. Gluteus medius 8. Gluteus maximus 9. Quadratus femoris 10. Peroneus longus 11. Peroneus brevis 12. Anterior tibialis 13. Extensor digitorum longus 14. Extensor hallucis 15. Extensor digitorum brevis 16. Internal hamstrings 17. External hamstrings 18. Short head of the biceps femoris 19. Posterior tibialis 20. Medial gastrocnemius 21. Lateral gastrocnemius Page 9 of 16
12 22. Abductor hallucis 23. Abductor digitorum (Ped) 24. First dorsal interosseus pedis X. Compressive Neuropathies 1: Median Nerve A. What is the difference between compressive neuropathy and entrapment neuropathy? B. What are the signs and symptoms of carpal tunnel syndrome? C. What are the risk factors for carpal tunnel syndrome? D. What are the AANEM electrodiagnostic criteria for carpal tunnel syndrome (sensory, midpalmar sensory, and motor)? E. What are our criteria for carpal tunnel syndrome? Note that these relative differences are not considered absolute or diagnostic. F. Proximal Median mononeuropathy 1. The pronator syndrome a. What is it and what are the symptoms? b. What are the expected nerve conduction and EMG findings? 2. Compression at the ligament of Struthers a. What are the signs and symptoms? b. What are the expected nerve conduction study and EMG findings? G. The anterior interosseus syndrome: 1. Which muscles are innervated by the anterior interosseus nerve? 2. What are the signs and symptoms? 3. What are the expected nerve conduction study and EMG findings? XI. Compressive Neuropathies 2: Ulnar Nerve A. What muscles are supplied by the ulnar nerve? B. Ulnar mononeuropathy at the elbow 1. What are the clinical features of ulnar mononeuropathy at the elbow? 2. What are risk factors for ulnar mononeuropathy at the elbow? 3. What are the expected nerve conduction study and EMG findings in ulnar mononeuropathy at the elbow? 4. How are the flexor carpi ulnaris and flexor digitorum profundus 4&5 useful localizing an ulnar mononeuropathy? 5. How can an ulnar mononeuropathy at the elbow be distinguished from ulnar mononeuropathy proximal to the elbow? C. Ulnar mononeuropathy at the wrist 1. What are the various branches of the ulnar nerve that can be affected at the wrist? 2. How do the clinical presentations vary? 3. What are the nerve conduction study findings associated with these? 4. How does evaluation of the dorsal ulnar cutaneous branch help differentiate ulnar neuropathy at the wrist from ulnar neuropathy at the elbow? XII. Compressive Neuropathies 3: Peroneal Nerve (fibular nerve) A. What muscle is supplied directly by the common peroneal branch of the sciatic nerve above the fibular head? B. What muscles are supplied by the deep peroneal nerve? C. What muscles are supplied by the superficial peroneal nerve? Page 10 of 16
13 D. Which of branch or branches of the peroneal nerve are usually involved in an entrapment neuropathy at the fibular head? E. What are the expected nerve conduction studies and EMG findings in peroneal mononeuropathy at the fibular head? XIII. Compressive Neuropathies 4: Radial Nerve A. What muscles are supplied by the radial nerve before the spiral groove? Which is the last one? B. What muscles are supplied by the radial nerve after the spiral groove but before the branch to the posterior interosseus? Which is the first one? C. What muscles are supplied by the posterior interosseus nerve? D. What is the first muscle innervated by the posterior interosseus nerve as it emerges from the supinator? E. What are the expected nerve conduction study and EMG findings in a radial neuropathy at the spiral groove? F. What are the expected nerve conduction study findings and needle EMG findings in a posterior interosseus syndrome? G. What is the arcade of Frohse? XIV. Compressive Neuropathies 5: Uncommon Compressive Neuropathies A. What is the difference between vascular and neurogenic thoracic outlet syndrome? B. What are the expected nerve conduction study and EMG findings in neurogenic thoracic outlet syndrome? C. What are the features of digital nerve entrapment of the hand? D. Sciatic neuropathy: 1. What muscles are supplied by the sciatic nerve? 2. What etiologic factors may contribute to sciatic mononeuropathy? 3. What are the expected nerve conduction and EMG findings? E. Tarsal Tunnel Syndrome: 1. What are the clinical features of tarsal tunnel syndrome? 2. What etiologic factors may contribute to tarsal tunnel syndrome? 3. What are the expected nerve conduction study and EMG findings? F. Femoral Neuropathy: 1. What are the sensory branches of the femoral nerve? 2. What is the clinical presentation of lateral femoral cutaneous neuropathy? 3. What muscles are innervated by the femoral nerve? G. What are the findings in long thoracic neuropathy? H. What are the findings in dorsal scapular neuropathy? I. What are the findings in suprascapular neuropathy? J. What are the findings in musculocutaneous neuropathy? K. What are the findings in ilioinguinal, genitofemoral, and saphenous neuropathies? L. What are the findings in obturator neuropathy? XV. Anomalous Innervation A. What are the three types of median-ulnar anastomoses? B. Which is the most common type of median-ulnar anastomosis? 1. What nerve conduction study finding suggests the presence of this anastomosis? 2. How would this anomaly be confirmed? Page 11 of 16
14 C. What are the findings in a patient with a median-to-ulnar anastomosis and carpal tunnel syndrome? D. What muscle may be innervated by an accessory peroneal nerve? E. How is an accessory peroneal nerve identified on nerve conduction studies? XVI. Axonal vs. Demyelinating Neuropathy A. What types of nerve fibers are involved in conveying pain: 1. Pain 2. Temperature 3. Pressure 4. Vibration 5. Two-point discrimination 6. Proprioception B. What physical exam findings may be present in patients with peripheral neuropathy? C. What electrodiagnostic findings differentiate peripheral neuropathy from polyradiculopathy? D. What electrodiagnostic findings are suggestive of an axonal peripheral neuropathy? E. Demyelinating peripheral neuropathy a. What electrodiagnostic findings are suggestive of an acquired demyelinating peripheral neuropathy? b. What conditions cause an acquired demyelinating peripheral neuropathy? c. What electrodiagnostic findings are suggestive of a hereditary demyelinating peripheral neuropathy? d. What conditions cause a hereditary demyelinating peripheral neuropathy? e. How can cool skin temperature be misleading in determining whether a peripheral neuropathy is axonal or demyelinating? f. What percentage of patients over 70 years old will have a sural sensory response? F. How do you define peripheral neuropathy in the geriatric population? G. Hereditary neuropathies 1. What are the most common hereditary neuropathies and how are they classified? 2. What genetic tests are available for hereditary neuropathies? 3. In approximately what fraction of hereditary demyelinating neuropathies is there no known family history? H. What is multifocal motor neuropathy and what are the findings on nerve conduction studies? XVII. Radiculopathies and Plexopathies A. Radiculopathy 1. What are the expected findings on motor nerve conduction studies in a radiculopathy? 2. What are the expected findings on sensory nerve conduction studies in a radiculopathy? 3. After an acute radiculopathy, which muscles (proximal or distal) will show abnormal spontaneous activity first? Which muscles will show changes of reinnervation first? 4. What are the most common cervical and lumbar radiculopathies? Page 12 of 16
15 5. What are the electrodiagnostic findings in lumbar spinal stenosis? 6. What is the minimum number of muscles that should be tested to screen for radiculopathy in an upper extremity? 7. What is the minimum number of muscles that should be tested to screen for radiculopathy in a lower extremity? 8. What abnormalities do you expect on needle exam in each of the following radiculopathies? a. L4 radiculopathy b. L5 radiculopathy c. S1 radiculopathy d. C5 radiculopathy e. C6 radiculopathy f. C7 radiculopathy g. C8 radiculopathy B. Plexopathy 1. How can you differentiate plexopathy from radiculopathy on the basis of nerve conduction studies? 2. What are the clinical features of an upper trunk brachial plexopathy? 3. What are the clinical features of a lower trunk brachial plexopathy? 4. Which nerves are supplied by the posterior cord? 5. Which nerves are supplied by the lateral cord? 6. Which nerves are supplied by the medial cord? 7. Draw the brachial plexus. 8. In an upper trunk plexopathy, which of the following sensory nerve action potentials will be affected? a. Median at D1 b. Median at D3 c. Ulnar d. Radial e. Medial antebrachial cutaneous f. Lateral antebrachial cutaneous 9. In a lower trunk plexopathy, which of the following sensory nerve action potentials will be affected? a. Median at D1 b. Median at D3 c. Ulnar d. Radial e. Medial antebrachial cutaneous f. Lateral antebrachial cutaneous 10. In a middle trunk plexopathy, which of the following sensory nerve action potentials will be affected? a. Median at D1 b. Median at D3 c. Ulnar d. Radial e. Medial antebrachial cutaneous f. Lateral antebrachial cutaneous Page 13 of 16
16 11. In a lateral cord plexopathy, which of the following sensory nerve action potentials will be affected? a. Median at D1 b. Median at D3 c. Ulnar d. Radial e. Medial antebrachial cutaneous f. Lateral antebrachial cutaneous 12. In a medial cord plexopathy, which of the following sensory nerve action potentials will be affected? a. Median at D1 b. Median at D3 c. Ulnar d. Radial e. Medial antebrachial cutaneous f. Lateral antebrachial cutaneous 13. In a posterior cord plexopathy, which of the following sensory nerve action potentials will be affected? a. Median at D1 b. Median at D3 c. Ulnar d. Radial e. Medial antebrachial cutaneous f. Lateral antebrachial cutaneous 14. What is diabetic amyotrophy? 15. What is brachial plexitis (Parsonage-Turner Syndrome?) 16. Are paraspinal muscles affected in plexopathy? C. Paraspinal Mapping 1. How much paraspinal denervation can one expect in the low back muscles of asymptomatic persons? 2. What is the specificity of needle EMG in differentiating clinically and radiographically apparent spinal stenosis from low back pain or no symptoms? 3. How does one place an EMG needle in the L5-innervated paraspinal muscles? XVIII. Cranial Nerve Studies A. For what clinical situations is a facial motor response a useful study? B. In the blink reflex, what pathway does the R1 represent? C. In the blink reflex, what pathway does the ipsilateral R2 represent? D. In the blink reflex, what pathway does the contralateral R2 represent? XIX. Motor Neuron Disease A. What are the different motor neuron diseases that affect adults and children and how are they can be distinguished clinically? B. What is the differential diagnosis for weakness with normal sensation? C. What are the clinical features of amyotrophic lateral sclerosis? D. In motor neuron disease: 1. What are the expected sensory and motor nerve conductions study findings? 2. What findings may be noted on repetitive stimulation? Page 14 of 16
17 3. What findings are expected on needle examination and what is the distribution of involvement? E. A cervical lesion may cause polyradiculopathy (wasting and weakness of the upper limbs) and myelopathy (spasticity in the lower limbs). How can this be distinguished from ALS? F. What are the Escorial definitions of definite, probable, and possible motor neuron disease? What are the four body segments that can be tested to meet these criteria? G. What does muscle biopsy show in motor neuron disease? H. Why are thoracic paraspinal muscles useful in the EMG evaluation of ALS? XX. Introduction to Muscle Pathology A. Be able to identify each of the following in muscle tissue, and describe the clinical significance of the findings that are abnormal: 1. Normal H&E 2. Atrophic muscle fibers 3. Fiber type grouping 4. Increased glycogen storage 5. Split fibers 6. Central nuclei 7. Vacuoles 8. Z band, I band, and A band B. What are the features of Type I muscle fibers? C. What are the features of Type II muscle fibers? D. How do the following relate to each other: Muscle fibers, myofibrils, sarcomeres? XXI. The Muscular Dystrophies A. What are the clinical features, mode of inheritance, and EMG findings in: 1. Duchenne muscular dystrophy 2. Becker muscular dystrophy 3. Limb Girdle muscular dystrophy 4. Fascioscapulohumeral muscular dystrophy 5. Oculopharyngeal muscular dystrophy 6. Myotonic dystrophy B. How are muscular dystrophies classified? C. For which muscular dystrophies is a gene test available? XXII. Inflammatory/Metabolic Myopathies A. What are the clinical features and EMG characteristics of: 1. Dermatomyositis 2. Polymyositis 3. Steroid myopathy 4. Inclusion body myositis 5. Hypokalemic periodic paralysis 6. Hyperkalemic periodic paralysis 7. Statin myopathy B. What are the limitations of EMG in the diagnosis of steroid myopathy? C. What are the EMG findings in an incompletely treated inflammatory myopathy? Page 15 of 16
18 XXIII. Congenital/Storage Myopathies A. What are the clinical features and muscle biopsy findings in: 1. Central core myopathy 2. Nemaline myopathy 3. Myotubular (centronuclear) myopathy 4. Mitochondrial myopathy B. What are the clinical features and muscle biopsy findings in: 1. Acid maltase deficiency (Pompe s disease) 2. Myophosphorylase deficiency (McArdle s disease) 3. Carnitine palmitoyltransferase deficiency XXIV. Myotonia A. What are the clinical features of myotonic dystrophy? B. What are the clinical features of myotonia congenita? C. What are the clinical features of paramyotonia congenita? D. What ion channels are involved in each of the myotonic disorders? XXV. Neuromuscular Complications of Cancer 8.18 A. What conditions can cause facial myokymia? B. Describe the clinical picture in the various paraneoplastic syndromes of the peripheral nervous system. C. How can radiation plexopathy be differentiated from plexopathy caused by metastatic tumor? XXVI. An Approach to the Diagnosis of Neuromuscular Disease in the Floppy Infant 8.19 A. How do the nerve conduction study findings differ between normal infants and adults? B. What is the most likely diagnosis in a floppy infant with neuropathic motor unit changes on EMG? C. What is neonatal myasthenia gravis? XXVII. SFEMG 8.21 A. What is jitter and how is it measured? B. What is the significance of increased jitter? Page 16 of 16
19 Physical Medicine and Rehabilitation EMG Rotation Skills List 1. Machine Test 2. Anatomy Test 3. Neuromuscular Disease Test 4. EMG Wave Form Test 5. EMG Wave Form multiple choice Test Date Passed Examiner s Signature Observed Studies Diagnosis Observer Case Number Date 1. Complete NCS/EMG 2. Complete NCS/EMG 3. Complete NCS/EMG 4. Complete NCS/EMG SSEPs Studies Observed CPI# Date Signature Case #1 Case #2 Case #3
Index. Note: Page numbers of article titles are in boldface type.
 Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Abnormal EMG Patterns in Disease. Amanda C. Peltier, MD MS October 12, 2013
 Abnormal EMG Patterns in Disease Amanda C. Peltier, MD MS October 12, 2013 Disclosures I have no financial relationships to disclose that are relative to the content of my presentation. Basic Tenets of
Abnormal EMG Patterns in Disease Amanda C. Peltier, MD MS October 12, 2013 Disclosures I have no financial relationships to disclose that are relative to the content of my presentation. Basic Tenets of
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists
 Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Making sense of Nerve conduction & EMG
 Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
Electrophysiology of Brachial and Lumbosacral Plexopathies
 18 Electrophysiology of Brachial and Lumbosacral Plexopathies Juan A. Acosta and Elizabeth M. Raynor Summary Brachial and lumbosacral plexopathies represent a heterogeneous group of disorders including
18 Electrophysiology of Brachial and Lumbosacral Plexopathies Juan A. Acosta and Elizabeth M. Raynor Summary Brachial and lumbosacral plexopathies represent a heterogeneous group of disorders including
Nerve Conduction Studies and EMG
 Nerve Conduction Studies and EMG Limitations of other methods of investigations of the neuromuscular system - Dr Rob Henderson, Neurologist Assessment of Weakness Thanks Peter Silburn PERIPHERAL NEUROPATHY
Nerve Conduction Studies and EMG Limitations of other methods of investigations of the neuromuscular system - Dr Rob Henderson, Neurologist Assessment of Weakness Thanks Peter Silburn PERIPHERAL NEUROPATHY
A/Professor Arun Aggarwal Balmain Hospital
 A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
Peripheral Nervous Sytem: Upper Body
 Peripheral Nervous Sytem: Upper Body MSTN121 - Neurophysiology Session 10 Department of Myotherapy Cervical Plexus Accessory nerve (CN11 + C1-5) Motor: trapezius and sternocleidomastoid Greater auricular
Peripheral Nervous Sytem: Upper Body MSTN121 - Neurophysiology Session 10 Department of Myotherapy Cervical Plexus Accessory nerve (CN11 + C1-5) Motor: trapezius and sternocleidomastoid Greater auricular
Al-Balqa Applied University
 Al-Balqa Applied University Faculty Of Medicine *You can use this checklist as a guide to you for the lab. the items on this checklist represent the main features of the models that you have to know for
Al-Balqa Applied University Faculty Of Medicine *You can use this checklist as a guide to you for the lab. the items on this checklist represent the main features of the models that you have to know for
Table 1: Nerve Conduction Studies (summarised)
 Table 1: Nerve Conduction Studies (summarised) Sensory nerve conduction 1 week* 3 months Superficial radial sensory Normal, symmetric SNAP and CV No change Median to digit II Normal, symmetric SNAP and
Table 1: Nerve Conduction Studies (summarised) Sensory nerve conduction 1 week* 3 months Superficial radial sensory Normal, symmetric SNAP and CV No change Median to digit II Normal, symmetric SNAP and
Muscle Anatomy Review Chart
 Muscle Anatomy Review Chart BACK Superficial (5) Trapezius Transverse cervical a. Latissimus dorsi Thoracodorsal a. Rhomboideus major Dorsal scapular a. Rhomboideus minor Levator scapulae Intermediate
Muscle Anatomy Review Chart BACK Superficial (5) Trapezius Transverse cervical a. Latissimus dorsi Thoracodorsal a. Rhomboideus major Dorsal scapular a. Rhomboideus minor Levator scapulae Intermediate
Assessment of the Brachial Plexus EMG Course CNSF Halifax Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University
 Assessment of the Brachial Plexus EMG Course CNSF Halifax 2018 Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University Angela Scott, Association of Electromyography Technologists of
Assessment of the Brachial Plexus EMG Course CNSF Halifax 2018 Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University Angela Scott, Association of Electromyography Technologists of
The Human Muscular System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5th ed (2017) Chapters 10, 11, 12 INTRODUCTION
 Biology 322: Human Anatomy The Human Muscular System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapters 10, 11, 12 INTRODUCTION We will use a number of lab periods
Biology 322: Human Anatomy The Human Muscular System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapters 10, 11, 12 INTRODUCTION We will use a number of lab periods
ANATOMICAL GUIDE FOR THE ELECTROMYOGRAPHER
 ANATOMICAL GUIDE FOR THE ELECTROMYOGRAPHER ANATOMICAL GUIDE FOR THE ELECTROMYOGRAPHER The Limbs and Trunk By EDWARD F. DELAGI, M.D. JOHN IAZZETTI, M.D. ALDO O. PEROTTO, M.D. DANIEL MORRISON, M.D. Fourth
ANATOMICAL GUIDE FOR THE ELECTROMYOGRAPHER ANATOMICAL GUIDE FOR THE ELECTROMYOGRAPHER The Limbs and Trunk By EDWARD F. DELAGI, M.D. JOHN IAZZETTI, M.D. ALDO O. PEROTTO, M.D. DANIEL MORRISON, M.D. Fourth
Mononeuropathies of the Upper and Lower Extremity
 15 Mononeuropathies of the Upper and Lower Extremity Kevin R. Scott and Milind J. Kothari Summary Nerves of both the upper and lower extremities are frequently injured for a variety of reasons. In the
15 Mononeuropathies of the Upper and Lower Extremity Kevin R. Scott and Milind J. Kothari Summary Nerves of both the upper and lower extremities are frequently injured for a variety of reasons. In the
Human Anatomy Lab #7: Muscles of the Cadaver
 Human Anatomy Lab #7: Muscles of the Cadaver Table of Contents: Expected Learning Outcomes.... 1 Introduction...... 1 Identifying Muscles on Yourself.... 2 Muscles of the Anterior Trunk and Arm.. 2 Muscles
Human Anatomy Lab #7: Muscles of the Cadaver Table of Contents: Expected Learning Outcomes.... 1 Introduction...... 1 Identifying Muscles on Yourself.... 2 Muscles of the Anterior Trunk and Arm.. 2 Muscles
END-2300: NERVE CONDUCTION STUDIES
 END-2300: Nerve Conduction Studies 1 END-2300: NERVE CONDUCTION STUDIES Cuyahoga Community College Viewing:END-2300 : Nerve Conduction Studies Board of Trustees: 2002-04-04 Academic Term: 2003-08-21 Subject
END-2300: Nerve Conduction Studies 1 END-2300: NERVE CONDUCTION STUDIES Cuyahoga Community College Viewing:END-2300 : Nerve Conduction Studies Board of Trustees: 2002-04-04 Academic Term: 2003-08-21 Subject
Human Anatomy Biology 351
 1 Human Anatomy Biology 351 Upper Limb Exam Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
1 Human Anatomy Biology 351 Upper Limb Exam Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
Electrodiagnostics for Back & Neck Pain. Steven Andersen, MD Providence Physiatry Clinic
 Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Key Relationships in the Upper Limb
 Key Relationships in the Upper Limb This list contains some of the key relationships that will help you identify structures in the lab. They are organized by dissection assignment as defined in the syllabus.
Key Relationships in the Upper Limb This list contains some of the key relationships that will help you identify structures in the lab. They are organized by dissection assignment as defined in the syllabus.
The Muscular System. Chapter 10 Part C. PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College
 Chapter 10 Part C The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.9: Muscles Crossing the Shoulder
Chapter 10 Part C The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.9: Muscles Crossing the Shoulder
Nerve Conduction Studies NCS
 Nerve Conduction Studies NCS Nerve conduction studies are an essential part of an EMG examination. The clinical usefulness of NCS in the diagnosis of diffuse and local neuropathies has been thoroughly
Nerve Conduction Studies NCS Nerve conduction studies are an essential part of an EMG examination. The clinical usefulness of NCS in the diagnosis of diffuse and local neuropathies has been thoroughly
Lumbosacral plexus lesion Lumbosacral plexus disorders G54.1 Neuralgic amyotrophy Neuralgic amyotrophy G
 ICD-9-CM and ICD-10-CM NEUROMUSCULAR DIAGNOSIS CODES Focal Neuropathy ICD-9-CM ICD-10-CM Mononeuropathy G56.00 Carpal tunnel syndrome 354.00 Other median nerve lesion 354.10 Lesion of ulnar nerve 354.20
ICD-9-CM and ICD-10-CM NEUROMUSCULAR DIAGNOSIS CODES Focal Neuropathy ICD-9-CM ICD-10-CM Mononeuropathy G56.00 Carpal tunnel syndrome 354.00 Other median nerve lesion 354.10 Lesion of ulnar nerve 354.20
Nerve Conduction Studies NCS
 Nerve Conduction Studies NCS Nerve conduction studies are an essential part of an EMG examination. The clinical usefulness of NCS in the diagnosis of diffuse and local neuropathies has been thoroughly
Nerve Conduction Studies NCS Nerve conduction studies are an essential part of an EMG examination. The clinical usefulness of NCS in the diagnosis of diffuse and local neuropathies has been thoroughly
EDX in Myopathies Limitations. EDX in Myopathies Utility Causes of Myopathy. Myopathy: Issues for Electromyographers
 Electrodiagnostic Assessment of Myopathy Myopathy: Issues for Electromyographers Often perceived as challenging Ian Grant Division of Neurology QEII Health Sciences Centre Halifax NS CNSF EMG Course June
Electrodiagnostic Assessment of Myopathy Myopathy: Issues for Electromyographers Often perceived as challenging Ian Grant Division of Neurology QEII Health Sciences Centre Halifax NS CNSF EMG Course June
Part 1: Communication between CNS & PNS
 Ch. 6: Peripheral Nervous System Objectives: 1. Communication between CNS & PNS: afferent (sensory) pathway versus efferent (motor) pathway of information. 2. Regulation of somatic (voluntary) motor system
Ch. 6: Peripheral Nervous System Objectives: 1. Communication between CNS & PNS: afferent (sensory) pathway versus efferent (motor) pathway of information. 2. Regulation of somatic (voluntary) motor system
Nerve Injury. 1) Upper Lesions of the Brachial Plexus called Erb- Duchene Palsy or syndrome.
 Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
The Clavicle Right clavicle Deltoid tubercle: Conoid tubercle, conoid ligamen Impression for the
 The Clavicle Muscle Attachment Sites in the Upper Limb Pectoralis major Right clavicle Smooth superior surface of the shaft, under the platysma muscle tubercle: attachment of the deltoid Acromial facet
The Clavicle Muscle Attachment Sites in the Upper Limb Pectoralis major Right clavicle Smooth superior surface of the shaft, under the platysma muscle tubercle: attachment of the deltoid Acromial facet
ORIGINS, ACQUISITION, AND IMPLICATIONS
 ORIGINS, ACQUISITION, AND IMPLICATIONS Ruple S. Laughlin MD Department of Neurology Rochester, MN Mayo Clinic Overview Nerve conduction studies (NCS) are utilized to evaluate large myelinated motor and
ORIGINS, ACQUISITION, AND IMPLICATIONS Ruple S. Laughlin MD Department of Neurology Rochester, MN Mayo Clinic Overview Nerve conduction studies (NCS) are utilized to evaluate large myelinated motor and
Head & Neck The muscle names are followed by the chapter number
 Head & Neck The muscle names are followed by the chapter number. Splenius capitis (9) 2. Occipitalis (2) Temporalis () 3. Temporalis () 4. Semispinalis capitis (9) Facial / Scalp (2) 5. Temporalis () Facial
Head & Neck The muscle names are followed by the chapter number. Splenius capitis (9) 2. Occipitalis (2) Temporalis () 3. Temporalis () 4. Semispinalis capitis (9) Facial / Scalp (2) 5. Temporalis () Facial
The Electrodiagnosis of Neuropathy: Basic Principles and Common Pitfalls
 Neurol Clin 25 (2007) 1 28 The Electrodiagnosis of Neuropathy: Basic Principles and Common Pitfalls Clifton L. Gooch, MD a, *, Louis H. Weimer, MD b a Columbia Neuropathy Research Center, Electromyography
Neurol Clin 25 (2007) 1 28 The Electrodiagnosis of Neuropathy: Basic Principles and Common Pitfalls Clifton L. Gooch, MD a, *, Louis H. Weimer, MD b a Columbia Neuropathy Research Center, Electromyography
Nerves of the upper limb Prof. Abdulameer Al-Nuaimi. E. mail:
 Nerves of the upper limb Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Brachial plexus Median nerve After originating from the brachial plexus in the axilla,
Nerves of the upper limb Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Brachial plexus Median nerve After originating from the brachial plexus in the axilla,
Epicranius (frontal belly) Zygomaticus minor. Zygomaticus major Buccinator
 Epicranius (frontal belly) Zygomaticus minor Zygomaticus major Buccinator Masseter Digastric (posterior belly) Stylohyoid Sternocleidomastoid Trapezius Scalenus Omohyoid (inferior belly) Orbicularis oris
Epicranius (frontal belly) Zygomaticus minor Zygomaticus major Buccinator Masseter Digastric (posterior belly) Stylohyoid Sternocleidomastoid Trapezius Scalenus Omohyoid (inferior belly) Orbicularis oris
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
The Muscular System Lab Power Point
 The Muscular System Lab Power Point Myoneural Junction Sarcoplasm Nucleus Myofibrils Sarcomere (black line to black line) Sarcolemma Myoneural space Nucleus Endomysium Motor Neuron Muscles of Facial Expression
The Muscular System Lab Power Point Myoneural Junction Sarcoplasm Nucleus Myofibrils Sarcomere (black line to black line) Sarcolemma Myoneural space Nucleus Endomysium Motor Neuron Muscles of Facial Expression
Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes
 Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes 1 This lab involves the second section of the exercise Spinal Cord, Spinal Nerves, and the Autonomic Nervous System,
Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes 1 This lab involves the second section of the exercise Spinal Cord, Spinal Nerves, and the Autonomic Nervous System,
UltraEMG Course Schedule 2015
 Ultra EMG February 20-25 Manchester Grand Hyatt San Diego, California Thursday February 19 Travel Date 5:00-6:00 Registration UltraEMG Course Schedule 2015 UltraEMG-MSK (Musculoskeletal Emphasis) Friday,
Ultra EMG February 20-25 Manchester Grand Hyatt San Diego, California Thursday February 19 Travel Date 5:00-6:00 Registration UltraEMG Course Schedule 2015 UltraEMG-MSK (Musculoskeletal Emphasis) Friday,
Neurophysiological Diagnosis of Birth Brachial Plexus Palsy. Dr Grace Ng Department of Paed PMH
 Neurophysiological Diagnosis of Birth Brachial Plexus Palsy Dr Grace Ng Department of Paed PMH Brachial Plexus Anatomy Brachial Plexus Cords Medial cord: motor and sensory conduction for median and ulnar
Neurophysiological Diagnosis of Birth Brachial Plexus Palsy Dr Grace Ng Department of Paed PMH Brachial Plexus Anatomy Brachial Plexus Cords Medial cord: motor and sensory conduction for median and ulnar
LATE RESPONSES IN THE ELECTRODIAGNOSIS OF CERVICAL RADICULOPATHIES
 Neurology DOI: 10.15386/cjmed-382 LATE RESPONSES IN THE ELECTRODIAGNOSIS OF CERVICAL RADICULOPATHIES ANA MARIA GALAMB, IOAN DAN MINEA Department of Medical and Surgical Specialities, Faculty of Medicine,
Neurology DOI: 10.15386/cjmed-382 LATE RESPONSES IN THE ELECTRODIAGNOSIS OF CERVICAL RADICULOPATHIES ANA MARIA GALAMB, IOAN DAN MINEA Department of Medical and Surgical Specialities, Faculty of Medicine,
Synergist Muscles. Shoulder (glenohumeral joint) Flexion Deltoid (anterior fibers) Pectoralis major (upper fibers) Biceps Brachii Coracobrachialis
 Synergist Muscles Dr Gene Desepoli DrGeneLMT@gmail.com Shoulder (glenohumeral joint) Deltoid (anterior fibers) Pectoralis major (upper fibers) Biceps Brachii Coracobrachialis Deltoid (posterior fibers)
Synergist Muscles Dr Gene Desepoli DrGeneLMT@gmail.com Shoulder (glenohumeral joint) Deltoid (anterior fibers) Pectoralis major (upper fibers) Biceps Brachii Coracobrachialis Deltoid (posterior fibers)
Keywords. Abductor digiti minimi (ADM or ADQ) Abductor digiti quinti pedis (ADQp) Abductor hallucis (AH or AHB) Abductor pollicis brevis (APB)
 Keywords A-waves Abduct Abductor digiti minimi (ADM or ADQ) Abductor digiti quinti pedis (ADQp) Abductor hallucis (AH or AHB) Abductor pollicis brevis (APB) Accessory peroneal nerve Acetylcholine Action
Keywords A-waves Abduct Abductor digiti minimi (ADM or ADQ) Abductor digiti quinti pedis (ADQp) Abductor hallucis (AH or AHB) Abductor pollicis brevis (APB) Accessory peroneal nerve Acetylcholine Action
Contents. Preface xv. SECTION 1: Introduction to the Bodynamic System 1. SECTION 2: The Bodynamic Psycho-Motor Anatomy 29
 Contents Preface xv SECTION 1: Introduction to the Bodynamic System 1 Definitions in the Bodynamic System 3 Ego Formation through the Coding Elements 9 Examples of Formation of Coding 17 Using This Book
Contents Preface xv SECTION 1: Introduction to the Bodynamic System 1 Definitions in the Bodynamic System 3 Ego Formation through the Coding Elements 9 Examples of Formation of Coding 17 Using This Book
Evaluating the Patient With Focal Neuropathy With Needle Electromyography
 13 Evaluating the Patient With Focal Neuropathy With Needle Electromyography Lawrence R. Robinson, MD Professor Department of Rehabilitation Medicine University of Washington School of Medicine Seattle,
13 Evaluating the Patient With Focal Neuropathy With Needle Electromyography Lawrence R. Robinson, MD Professor Department of Rehabilitation Medicine University of Washington School of Medicine Seattle,
Peripheral Nervous System: Lower Body
 Peripheral Nervous System: Lower Body MSTN121 - Neurophysiology Session 11 Department of Myotherapy Lumbar Plexus Iliohypogastric nerve (T12-L1) Motor: Transverse abdominis and internal obliques Sensory:
Peripheral Nervous System: Lower Body MSTN121 - Neurophysiology Session 11 Department of Myotherapy Lumbar Plexus Iliohypogastric nerve (T12-L1) Motor: Transverse abdominis and internal obliques Sensory:
Netter's Anatomy Flash Cards Section 6 List 4 th Edition
 Netter's Anatomy Flash Cards Section 6 List 4 th Edition https://www.memrise.com/course/1577581/ Section 6 Upper Limb (66 cards) Plate 6-1 Humerus and Scapula: Anterior View 1.1 Acromion 1.2 Greater tubercle
Netter's Anatomy Flash Cards Section 6 List 4 th Edition https://www.memrise.com/course/1577581/ Section 6 Upper Limb (66 cards) Plate 6-1 Humerus and Scapula: Anterior View 1.1 Acromion 1.2 Greater tubercle
Muscles of the Upper Limb
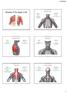 Muscles of the Upper Limb anterior surface of ribs 3 5 coracoid process Pectoralis minor pectoral nerves protracts / depresses scapula Serratus anterior Subclavius ribs 1-8 long thoracic nerve rib 1 ----------------
Muscles of the Upper Limb anterior surface of ribs 3 5 coracoid process Pectoralis minor pectoral nerves protracts / depresses scapula Serratus anterior Subclavius ribs 1-8 long thoracic nerve rib 1 ----------------
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
Human Anatomy and Physiology I Laboratory
 Human Anatomy and Physiology I Laboratory Gross Anatomy of the Muscular System (Two weeks) 1 This lab involves study of the laboratory exercise Gross Anatomy of the Muscular System. Complete the Review
Human Anatomy and Physiology I Laboratory Gross Anatomy of the Muscular System (Two weeks) 1 This lab involves study of the laboratory exercise Gross Anatomy of the Muscular System. Complete the Review
Muscular Nomenclature and Kinesiology - One
 Chapter 16 Muscular Nomenclature and Kinesiology - One Lessons 1-3 (with lesson 4) 1 Introduction 122 major muscles covered in this chapter Chapter divided into nine lessons Kinesiology study of human
Chapter 16 Muscular Nomenclature and Kinesiology - One Lessons 1-3 (with lesson 4) 1 Introduction 122 major muscles covered in this chapter Chapter divided into nine lessons Kinesiology study of human
BRACHIAL PLEXUS. DORSAL SCAPULAR NERVE (C5) supraclavicular branch innervates rhomboids (major and minor) and levator scapulae
 THE BRACHIAL PLEXUS DORSAL SCAPULAR NERVE (C5) supraclavicular branch innervates rhomboids (major and minor) and levator scapulae SCHEMA OF THE BRACHIAL PLEXUS THE BRACHIAL PLEXUS PHRENIC NERVE supraclavicular
THE BRACHIAL PLEXUS DORSAL SCAPULAR NERVE (C5) supraclavicular branch innervates rhomboids (major and minor) and levator scapulae SCHEMA OF THE BRACHIAL PLEXUS THE BRACHIAL PLEXUS PHRENIC NERVE supraclavicular
Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment
 Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment 7 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, HW Van Es, LH Van den Berg Annals of Neurology 2000;
Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment 7 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, HW Van Es, LH Van den Berg Annals of Neurology 2000;
BIOL 4260 Human Evolu3onary Anatomy Lecture 12: Limb Development. Lecture 2: Fossil Record
 BIOL 4260 Human Evolu3onary Anatomy Lecture 12: Limb Development Lecture 2: Fossil Record Outline Limb Evolution Limb Development Limb Function A Few Definitions Appendicular skeleton girdles & limbs Pectoral
BIOL 4260 Human Evolu3onary Anatomy Lecture 12: Limb Development Lecture 2: Fossil Record Outline Limb Evolution Limb Development Limb Function A Few Definitions Appendicular skeleton girdles & limbs Pectoral
Distal chronic spinal muscular atrophy involving the hands
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
June 1996 EMG Case-of-the-Month
 June 1996 EMG Case-of-the-Month This case is no longer available for CME credit. Cases prepared by: Ian MacLean, MD; Daniel Dumitru, MD; Lawrence R. Robinson, MD HISTORY Six weeks ago a 28-year-old woman
June 1996 EMG Case-of-the-Month This case is no longer available for CME credit. Cases prepared by: Ian MacLean, MD; Daniel Dumitru, MD; Lawrence R. Robinson, MD HISTORY Six weeks ago a 28-year-old woman
Lab # 2: Spinal Cord & Nerves, Reflexes and General Senses. A & P II Spring, 2014
 Lab # 2: Spinal Cord & Nerves, Reflexes and General Senses A & P II Spring, 2014 Objectives Be able to identify specified spinal cord structures and spinal nerves on models Be familiar with spinal nerve
Lab # 2: Spinal Cord & Nerves, Reflexes and General Senses A & P II Spring, 2014 Objectives Be able to identify specified spinal cord structures and spinal nerves on models Be familiar with spinal nerve
Conventional needle electromyography
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 5 Electromyography: Surface, needle conventional and single fiber - Level 1-2 Conventional
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 5 Electromyography: Surface, needle conventional and single fiber - Level 1-2 Conventional
Synapse Homework. Back page last question not counted. 4 pts total, each question worth 0.18pts. 26/34 students answered correctly!
 Synapse Homework Back page last question not counted 26/34 students answered correctly! 4 pts total, each question worth 0.18pts Business TASS hours extended! MWF 1-2pm, Willamette 204 T and Th 9:30-10:30am,
Synapse Homework Back page last question not counted 26/34 students answered correctly! 4 pts total, each question worth 0.18pts Business TASS hours extended! MWF 1-2pm, Willamette 204 T and Th 9:30-10:30am,
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2014;38(1):109-115 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.1.109 Annals of Rehabilitation Medicine Sonographic Evaluation of the Peripheral Nerves
Case Report Ann Rehabil Med 2014;38(1):109-115 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.1.109 Annals of Rehabilitation Medicine Sonographic Evaluation of the Peripheral Nerves
DISSECTION SCHEDULE. Session I - Hip (Front) & Thigh (Superficial)
 DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
A Basic Approach to Common Upper Extremity Mononeuropathies and Brachial Plexopathies
 A Basic Approach to Common Upper Extremity Mononeuropathies and Brachial Plexopathies Paul E. Barkhaus, MD Aiesha Ahmed, MD Kerry H. Levin, MD Zachary Simmons, MD AANEM 60th Annual Meeting San Antonio,
A Basic Approach to Common Upper Extremity Mononeuropathies and Brachial Plexopathies Paul E. Barkhaus, MD Aiesha Ahmed, MD Kerry H. Levin, MD Zachary Simmons, MD AANEM 60th Annual Meeting San Antonio,
Nerves of Upper limb. Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh
 Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
Name this muscle. Name this muscle
 this muscle this muscle Pectoralis Major Pectoralis Minor Serratus anterior Pectoralis minor Serratus anterior this muscle Deltoid: The major abductor of the upper limb this muscle this muscle this muscle
this muscle this muscle Pectoralis Major Pectoralis Minor Serratus anterior Pectoralis minor Serratus anterior this muscle Deltoid: The major abductor of the upper limb this muscle this muscle this muscle
Muscles of the Cat. N Deltoid MUSCLES OF THE CHEST. Pectoralis major. (This muscle is superior to Pectoralis minor) MUSCLES OF THE CHEST
 MUSCLES OF THE CHEST Pectoralis major (This muscle is superior to Pectoralis minor) 1. MUSCLES OF THE CHEST Pectoralis minor (This muscle is inferior to Pectoralis major) 2. MUSCLES OF THE ARM Deltoid
MUSCLES OF THE CHEST Pectoralis major (This muscle is superior to Pectoralis minor) 1. MUSCLES OF THE CHEST Pectoralis minor (This muscle is inferior to Pectoralis major) 2. MUSCLES OF THE ARM Deltoid
Lower Limb Nerves. Clinical Anatomy
 Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Differential Diagnosis of Neuropathies and Compression. Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre
 Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Due in Lab weeks because of Thanksgiving Prelab #10. Homework #8. Both sides! Both sides!
 Lab 8 MUSCLES Due in Lab 10 2 weeks because of Thanksgiving Prelab #10 Both sides! Homework #8 Both sides! Refer to Muscles 22-23 Naming of muscles Origin Site of muscle attachment that doesn t move during
Lab 8 MUSCLES Due in Lab 10 2 weeks because of Thanksgiving Prelab #10 Both sides! Homework #8 Both sides! Refer to Muscles 22-23 Naming of muscles Origin Site of muscle attachment that doesn t move during
Biology 2401 Muscles List for CPC models
 Biology 2401 List for CPC models Italicized muscles are dissect and similar in the cat = Dissect and note the differences in human and cat Major of the Human Head Facial Expression Epicranius frontalis
Biology 2401 List for CPC models Italicized muscles are dissect and similar in the cat = Dissect and note the differences in human and cat Major of the Human Head Facial Expression Epicranius frontalis
2/4/2018. Identify the two reasons why muscle cells may go through muscle fatigue. Ch.7 Review. Sternocleidomastoid.
 Ch.7 Review Identify the two reasons why muscle cells may go through muscle fatigue Temporalis Depressor anguli oris Sternocleidomastoid Tibialis anterior 1 Gluteus medius Deltoid Adducts & rotates scapula
Ch.7 Review Identify the two reasons why muscle cells may go through muscle fatigue Temporalis Depressor anguli oris Sternocleidomastoid Tibialis anterior 1 Gluteus medius Deltoid Adducts & rotates scapula
Spinal nerves. Aygul Shafigullina. Department of Morphology and General Pathology
 Spinal nerves Aygul Shafigullina Department of Morphology and General Pathology Spinal nerve a mixed nerve, formed in the vicinity of an intervertebral foramen, where fuse a dorsal root and a ventral root,
Spinal nerves Aygul Shafigullina Department of Morphology and General Pathology Spinal nerve a mixed nerve, formed in the vicinity of an intervertebral foramen, where fuse a dorsal root and a ventral root,
inerve Guide to Nerves 2009
 inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
Wrist, Elbow Hand. Surface Recording Technique, Study from Median Thenar (MT) Muscle
 Surface ecording Technique, Study from Median Thenar (MT) Muscle Original Settings Sensitivity, duration of pulse, sweep speed, low-frequency filter, high- frequency filter, and the machine used were not
Surface ecording Technique, Study from Median Thenar (MT) Muscle Original Settings Sensitivity, duration of pulse, sweep speed, low-frequency filter, high- frequency filter, and the machine used were not
Disclosure. Entrapment Neuropathies - Overview. Common mononeuropathy sites. Definitions. Common mononeuropathy sites. Common mononeuropathy sites
 Disclosure Entrapment Neuropathies - Overview I receive compensation from Wiley- Blackwell publishers for my work as Editor-in-Chief of Muscle & Nerve Lawrence H. Phillips, II, MD Definitions Mononeuropathy:
Disclosure Entrapment Neuropathies - Overview I receive compensation from Wiley- Blackwell publishers for my work as Editor-in-Chief of Muscle & Nerve Lawrence H. Phillips, II, MD Definitions Mononeuropathy:
For convenience values outside the normal range are bolded. Normal values for the specified patient are stated below the tables.
 Case tudy 8 or convenience values outside the normal range are bolded. Normal values for the specified patient are stated below the tables. History: 60 year-ol man with a history of left hand weakness
Case tudy 8 or convenience values outside the normal range are bolded. Normal values for the specified patient are stated below the tables. History: 60 year-ol man with a history of left hand weakness
11/15/2018. Temporalis Elevates & retracts mandible. Masseter = Prime mover of jaw closure. Levator scapulae Supraspinatus Clavicle.
 Due in Lab 10 Lab 8 MUSCLES 2 weeks because of Thanksgiving Prelab #10 Both sides! Homework #8 Both sides! Refer to Muscles 22-23 Examples of Origin & Insertion Naming of muscles Origin Site of muscle
Due in Lab 10 Lab 8 MUSCLES 2 weeks because of Thanksgiving Prelab #10 Both sides! Homework #8 Both sides! Refer to Muscles 22-23 Examples of Origin & Insertion Naming of muscles Origin Site of muscle
MSK Imaging Conference. 07/22/2016 Eman Alqahtani, MD, MPH R3/PGY4 UCSD Radiology
 MSK Imaging Conference 07/22/2016 Eman Alqahtani, MD, MPH R3/PGY4 UCSD Radiology A 51 years old female with chronic thumb pain, and inability to actively flex the thumb interphalyngeal joint Possible trigger
MSK Imaging Conference 07/22/2016 Eman Alqahtani, MD, MPH R3/PGY4 UCSD Radiology A 51 years old female with chronic thumb pain, and inability to actively flex the thumb interphalyngeal joint Possible trigger
Sensory nerve conduction studies
 Genomläst 2007-01-31/meg Sensory nerve conduction studies Department of clinical neurophysiology University hospital Uppsala, Sweden 1997-12-16 Björn Falck, Erik Stålberg and Lena Eriksson Department of
Genomläst 2007-01-31/meg Sensory nerve conduction studies Department of clinical neurophysiology University hospital Uppsala, Sweden 1997-12-16 Björn Falck, Erik Stålberg and Lena Eriksson Department of
Chapter 14. The Nervous System. The Spinal Cord and Spinal Nerves. Lecture Presentation by Steven Bassett Southeast Community College
 Chapter 14 The Nervous System The Spinal Cord and Spinal Nerves Lecture Presentation by Steven Bassett Southeast Community College Introduction The Central Nervous System (CNS) consists of: The spinal
Chapter 14 The Nervous System The Spinal Cord and Spinal Nerves Lecture Presentation by Steven Bassett Southeast Community College Introduction The Central Nervous System (CNS) consists of: The spinal
Functional Anatomy of the Elbow
 Functional Anatomy of the Elbow Orthopedic Institute Daryl C. Osbahr, M.D. Chief of Sports Medicine, Orlando Health Chief Medical Officer, Orlando City Soccer Club Orthopedic Consultant, Washington Nationals
Functional Anatomy of the Elbow Orthopedic Institute Daryl C. Osbahr, M.D. Chief of Sports Medicine, Orlando Health Chief Medical Officer, Orlando City Soccer Club Orthopedic Consultant, Washington Nationals
Index. Phys Med Rehabil Clin N Am 14 (2003) Note: Page numbers of article titles are in boldface type.
 Phys Med Rehabil Clin N Am 14 (2003) 445 453 Index Note: Page numbers of article titles are in boldface type. A Acid maltase deficiencies, electrodiagnosis of, 420, 422 Acquired peripheral neuropathy,
Phys Med Rehabil Clin N Am 14 (2003) 445 453 Index Note: Page numbers of article titles are in boldface type. A Acid maltase deficiencies, electrodiagnosis of, 420, 422 Acquired peripheral neuropathy,
Motor and sensory nerve conduction studies
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
[ resident s case problem ]
![[ resident s case problem ] [ resident s case problem ]](/thumbs/75/71507483.jpg) David G. Greathouse, PT, PhD, ECS, FAPTA1 Anand Joshi, MD2 Radiculopathy of the Eighth Cervical Nerve Radiculopathy involving the cervical nerve roots may be caused by spondylosis (degenerative joint disease
David G. Greathouse, PT, PhD, ECS, FAPTA1 Anand Joshi, MD2 Radiculopathy of the Eighth Cervical Nerve Radiculopathy involving the cervical nerve roots may be caused by spondylosis (degenerative joint disease
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5. September 30, 2011
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
In which arm muscle are intramuscular injections most often given? (not in text)
 AP1 Lab 9 - Muscles of the Arms and Legs Locate the following muscles on the models and on yourself. Recall anatomical position. Directional terms such as anterior, posterior, lateral, etc. all assume
AP1 Lab 9 - Muscles of the Arms and Legs Locate the following muscles on the models and on yourself. Recall anatomical position. Directional terms such as anterior, posterior, lateral, etc. all assume
5/21/2013. Muscle Anatomy. Thursday January, 24 th, Skeletal Muscle. Smooth Muscle. Cardiac Muscle
 Muscle Anatomy Thursday January, 24 th, 2013 Skeletal Muscle Cardiac Muscle Smooth Muscle 1 Smooth Muscle 1. Found in the walls of the digestive system, bladder, uterus and blood vessels 2. Involuntary
Muscle Anatomy Thursday January, 24 th, 2013 Skeletal Muscle Cardiac Muscle Smooth Muscle 1 Smooth Muscle 1. Found in the walls of the digestive system, bladder, uterus and blood vessels 2. Involuntary
Organization of the Lower Limb Audrone Biknevicius, Ph.D. Dept. Biomedical Sciences, OU HCOM at Dublin Clinical Anatomy Immersion 2014
 Organization of the Lower Limb Audrone Biknevicius, Ph.D. Dept. Biomedical Sciences, OU HCOM at Dublin Clinical Anatomy Immersion 2014 www.thestudio1.co.za LIMB FUNCTION choco-locate.com blog.coolibar.com
Organization of the Lower Limb Audrone Biknevicius, Ph.D. Dept. Biomedical Sciences, OU HCOM at Dublin Clinical Anatomy Immersion 2014 www.thestudio1.co.za LIMB FUNCTION choco-locate.com blog.coolibar.com
ARM Brachium Musculature
 ARM Brachium Musculature Coracobrachialis coracoid process of the scapula medial shaft of the humerus at about its middle 1. flexes the humerus 2. assists to adduct the humerus Blood: muscular branches
ARM Brachium Musculature Coracobrachialis coracoid process of the scapula medial shaft of the humerus at about its middle 1. flexes the humerus 2. assists to adduct the humerus Blood: muscular branches
Module 7 - The Muscular System Muscles of the Arm and Trunk
 Module 7 - The Muscular System Muscles of the Arm and Trunk This Module will cover the muscle anatomy of the arms and trunk. We have already seen the muscles that move the humerus, so this module will
Module 7 - The Muscular System Muscles of the Arm and Trunk This Module will cover the muscle anatomy of the arms and trunk. We have already seen the muscles that move the humerus, so this module will
Chapter 9. The Muscular System
 1 Chapter 9 The Muscular System 2 Introduction Skeletal muscles: movement in environment Smooth muscles: intestines, ureters, veins and arteries Cardiac muscle: pumps blood through heart and blood vessels
1 Chapter 9 The Muscular System 2 Introduction Skeletal muscles: movement in environment Smooth muscles: intestines, ureters, veins and arteries Cardiac muscle: pumps blood through heart and blood vessels
Case Studies in Peripheral Neurophysiology. Elliot L. Dimberg Mayo Clinic Florida 2015 American Clinical Neurophysiology Society Annual Meeting
 Case Studies in Peripheral Neurophysiology Elliot L. Dimberg Mayo Clinic Florida 2015 American Clinical Neurophysiology Society Annual Meeting Disclosures None Goals and Objectives To provide a concise,
Case Studies in Peripheral Neurophysiology Elliot L. Dimberg Mayo Clinic Florida 2015 American Clinical Neurophysiology Society Annual Meeting Disclosures None Goals and Objectives To provide a concise,
Lumbar Plexus. Ventral rami L1 L4 Supplies: Major nerves.. Abdominal wall External genitalia Anteromedial thigh
 Lower Limb Nerves Lectures Objectives Describe the structure and relationships of the plexuses of the lower limb. Describe the course, relationships and structures supplied for the major nerves of the
Lower Limb Nerves Lectures Objectives Describe the structure and relationships of the plexuses of the lower limb. Describe the course, relationships and structures supplied for the major nerves of the
A. All movements require muscle which are organs using chemical energy to contract.
 Ch 8 Muscles Introduction: A. All movements require muscle which are organs using chemical energy to contract. B. The three types of muscle in the body are skeletal, smooth, and cardiac muscle. C. This
Ch 8 Muscles Introduction: A. All movements require muscle which are organs using chemical energy to contract. B. The three types of muscle in the body are skeletal, smooth, and cardiac muscle. C. This
Case Example. Nerve Entrapments in the Lower limb
 Nerve Entrapments in the Lower limb February, 2013 William S. Pease, M.D. Ernest W. Johnson Professor of PM&R Case Example CC: Right ankle dorsiflexion weakness with minimal paresthesias HPI: 87 year-old
Nerve Entrapments in the Lower limb February, 2013 William S. Pease, M.D. Ernest W. Johnson Professor of PM&R Case Example CC: Right ankle dorsiflexion weakness with minimal paresthesias HPI: 87 year-old
Steps in EMG analysis
 Steps in EMG analysis at rest - spontaneous activity fibs, psw, myotonia, complex rep discharges fasciculations, myokymia at slight voluntary contraction - MUP shape parameters, stability (jiggle), behaviour
Steps in EMG analysis at rest - spontaneous activity fibs, psw, myotonia, complex rep discharges fasciculations, myokymia at slight voluntary contraction - MUP shape parameters, stability (jiggle), behaviour
ELECTROMYOGRAPHY SIGNAL ANALYSIS The ultimate goal of needle EMG is to obtain data that reflects the underlying morphology and pathophysiology of the
 ELECTROMYOGRAPHY SIGNAL ANALYSIS The ultimate goal of needle EMG is to obtain data that reflects the underlying morphology and pathophysiology of the muscle fibers and motor units, and identifies the changes
ELECTROMYOGRAPHY SIGNAL ANALYSIS The ultimate goal of needle EMG is to obtain data that reflects the underlying morphology and pathophysiology of the muscle fibers and motor units, and identifies the changes
EMG CASE No. 61, April 2003
 EMG CASE No. 61, April 2003 Presenting Symptom(s): Progressive left arm weakness, cramping, and muscle twitching. Case prepared by: Ann A. Little, M.D. James W. Teener, M.D. University of Michigan Department
EMG CASE No. 61, April 2003 Presenting Symptom(s): Progressive left arm weakness, cramping, and muscle twitching. Case prepared by: Ann A. Little, M.D. James W. Teener, M.D. University of Michigan Department
Upper limb Arm & Cubital region 黃敏銓
 Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
medial half of clavicle; Sternum; upper six costal cartilages External surfaces of ribs 3-5
 MUSCLE ORIGIN INSERTION ACTION NERVE Pectoralis Major medial half of clavicle; Sternum; upper six costal cartilages Lateral lip of intertubercular groove of horizontal adduction Medial and lateral pectoral
MUSCLE ORIGIN INSERTION ACTION NERVE Pectoralis Major medial half of clavicle; Sternum; upper six costal cartilages Lateral lip of intertubercular groove of horizontal adduction Medial and lateral pectoral
SECTION II: ILLUSTRATIONS OF SELECTED WAVEFORMS
 SECTION II: ILLUSTRATIONS OF SELECTED WAVEFORMS FIGURE 1 COMPOUND SENSORY NERVE ACTION POTENTIALS FIGURE 2 SHORT-LATENCY SOMATOSENSORY EVOKED POTENTIALS MEDIAN NERVE FIGURE 3 SHORT-LATENCY SOMATOSENSORY
SECTION II: ILLUSTRATIONS OF SELECTED WAVEFORMS FIGURE 1 COMPOUND SENSORY NERVE ACTION POTENTIALS FIGURE 2 SHORT-LATENCY SOMATOSENSORY EVOKED POTENTIALS MEDIAN NERVE FIGURE 3 SHORT-LATENCY SOMATOSENSORY
Neuroanatomy for Nerve Conduction Studies
 Neuroanatomy for Nerve Conduction Studies Kimberley Butler, R.NCS.T, CNIM, R. EP T. Jerry Morris, BS, MS, R.NCS.T. Kevin R. Scott, MD, MA Zach Simmons, MD AANEM 57 th Annual Meeting Québec City, Québec,
Neuroanatomy for Nerve Conduction Studies Kimberley Butler, R.NCS.T, CNIM, R. EP T. Jerry Morris, BS, MS, R.NCS.T. Kevin R. Scott, MD, MA Zach Simmons, MD AANEM 57 th Annual Meeting Québec City, Québec,
