Modern orthopedic and spine surgeons strive to minimize
|
|
|
- Jared Harris
- 5 years ago
- Views:
Transcription
1 SPINE Volume 39, Number 2, pp , Lippincott Williams & Wilkins DIAGNOSTICS Robot-Assisted Vertebral Body Augmentation A Radiation Reduction Tool Yair Barzilay, MD, * Josh E. Schroeder, MD, * Nurith Hiller, MD, Gordon Singer, MD,* Amir Hasharoni, MD, PhD, * Ori Safran, MD, * Meir Liebergall, MD, * Eyal Itshayek, MD, and Leon Kaplan, MD * Study Design. Retrospective. Objective. To assess radiation exposure time during robot-guided vertebral body augmentation compared with other published findings. Summary of Background Data. Rising incidence of vertebral compression fractures in the aging population result in widespread use of vertebral body cement augmentation with significant radiation exposure to the surgeon, operating room staff, and patient. Radiation exposure leads to higher cancer rates among orthopedic and spine surgeons and patients. Methods. Thirty-three patients with 60 vertebral compression fractures underwent robot-guided vertebral body augmentation performed by 2 surgeons simultaneously injecting cement at 2 levels under pulsed fluoroscopy. The age of patients was in the range from 29 to 92 (mean, 67 yr). One to 6 vertebrae were augmented per case (average 2). Twenty-five patients had osteoporotic fractures and 8 had pathological fractures. Robotic guidance data included execution rate, accuracy of guidance, total surgical time, and time required for robotic guidance. Radiation-related data included the average preoperative computed tomographic effective dose, radiation time for calibration, registration, placement of Kirschner wires, and total procedure radiation time. Radiation time per level and surgeon s exposure were calculated. Results. Kyphoplasty was performed in 15 patients (1 sacroplasty), vertebroplasty in 13, and intravertebral expanding implants in 5. The average preoperative computed tomographic effective dose was 50 msv (18 81). Average operative time was 118 minutes (49 350). Mean robotic guidance took 36 minutes. Average operative radiation time was 46.1 seconds per level (33 160). Average exposure time From the * Departments of Orthopedic Surgery ; Radiology; and Neurosurgery, Hadassah-Hebrew-University Medical Center, Jerusalem, Israel. Acknowledgment date: November 15, First revision date: February 18, Second revision date: April 28, Acceptance date: July 26, The device(s)/drug(s) is/are FDA-approved or approved by corresponding national agency for this indication. No funds were received in support of this work. Relevant financial activities outside the submitted work: consultancy, grants, patents, royalties, stocks, travel/accommodations/meeting expenses, payment for lecture, grants. Address correspondence and reprint requests to Yair Barzilay, MD, Spine unit, Department of Orthopedic Surgery, Hadassah-Hebrew-University Medical Center, Jerusalem, Israel; dbar@hadassah.org.il DOI: /BRS of the surgeons and the operating room staff per augmented level was 37.6 seconds. The execution rate was 99%, with an accuracy of 99%. Two complications (hemothorax and superficial wound infection) occurred. Conclusion. The radiation exposure of the surgeon and the operating room staff in a series of robot-assisted vertebral body augmentation was 74% lower than published results on fluoroscopy guidance and approximately 50% lower than the literature on navigated augmentation. Key words: radiation exposure, radiation reduction, robot-assisted spine surgery, vertebral body cement augmentation. Level of Evidence: 4 Spine 2014;39: Modern orthopedic and spine surgeons strive to minimize surgical exposure and increase precision in implant placement. This trend has led to greater use of fluoroscopic guidance, resulting in increased exposure to ionizing radiation for patients, surgeons, and operating room (OR) staff. Radiation exposure is a growing concern among orthopedic surgeons and OR staff. 1 3 Vertebral augmentation is a minimally invasive procedure aimed at reducing pain caused by osteoporotic and pathological vertebral compression fractures. Vertebroplasty was introduced in 1983 and kyphoplasty in , 5 Other systems for vertebral augmentation have been introduced more recently. 6 8 Vertebral augmentation is typically performed under fluoroscopy guidance, exposing the surgeon and the OR staff to significant radiation. 9 The estimated cancer incidence among surgeons who perform fluoroscopically assisted percutaneous vertebroplasty is 0.025%, 9 and the estimated incidence of fatal thyroid cancer is %, 25 times higher than the general population. 9 Average annual exposure to the eye lens is close to 8% of the 150-mSv threshold radiation dose needed to develop radiation-induced cataracts. Skin exposure during augmentation is up to 10% of the annual effective dose limit recommended by the International Commission on Radiological Protection. 9 Robot-assisted spine surgery is routinely performed in the authors institution for a variety of indications such as degenerative conditions, trauma, tumors, infections, and deformity correction. 10 The objective of this study was to compare Spine 153
2 radiation exposure time during robot-guided vertebral body augmentation to published results for similar surgical procedures conducted under fluoroscopic guidance. PATIENTS AND METHODS Thirty-three consecutive patients underwent robot-guided vertebral body augmentation for vertebral compression fractures in a total of 60 vertebrae. The demographic details, surgical indications, operated levels, and methods of augmentation are summarized in Table 1. All patients who underwent vertebral augmentation were included; all patients who had contraindications for augmentation were excluded. In 2 procedures, technical issues prevented robotic guidance (faulty cable in 1 case and failed fluoroscopy to computed tomographic [CT] registration in the second). These cases were excluded from analysis (2 vertebrae, 2 trajectories). This retrospective analysis was performed under a waiver of informed consent from our institutional review board (HMO ). All patients had signed informed consent forms for surgery. The use of robotic guidance was discussed with all patients before surgery. Because the robotic device has Food and Drug Administration and European Conformity approval and the technique is in routine clinical use, our institutional review board does not require modification to the informed consent form used for vertebral augmentation procedures. Preoperative CT examinations were performed in all patients with a 16-slice MDCT system (LightSpeed; GE Healthcare, Milwaukee, WI), craniocaudally, according to the robot manufacturer s instructions, using the following parameters: 140 kvp, 200 ma, mm slice thickness, a pitch of 0.5, and a matrix. Intraoperative fluoroscopy examination was performed with a GE OED inch fluoroscopy unit (GE Healthcare). The total filtration of the radiograph tube was 4.6-mm aluminum, the focus-to-image intensifier distance was 90 cm, and the input field was 23 cm in diameter. Exposure parameters were determined by means of an automatic brightness control. The radiograph unit was equipped with a permanent dose-area-product meter and a beam-on timer. Robotic Guidance SpineAssist (Mazor Surgical Technologies, Caesarea, Israel) is a miniature robot, which can be mounted on bone using 1 of 3 platforms (Bed Mount Device [Mazor Surgical Technologies], Hover-T Bridge [Mazor Surgical Technologies], Clamp [Mazor Surgical Technologies]). It is a semi-active system offering surgical tool guidance while leaving performance of the actual surgical operation, such as the drilling, in the surgeon s hands. The robotic procedure, consisting of 6 steps, has been described elsewhere 11 and is summarized briefly in the text hereafter: 1. Preoperative planning : CT scan-based planning to determine the optimal tracts for insertion of the augmentation needle. 2. Platform attachment : The optimal robotic platform is attached to the patient s bony anatomy. 3. Image acquisition and registration : Targets for image acquisition are connected to the robotic platform, and AP anteroposterior and 60 oblique fluoroscopic images are semi-automatically registered to the preoperative CT images. 4. Robot assembly and motion : The robot is attached to the mounting frame. It then moves and locks into position so that a guiding tube at the distal end of its arm is aligned with the planned screw/tool trajectory. Then the guiding tube is inserted through a small skin incision and gently tapped into the bony anatomy of the patient. 5. Trajectory execution : Drilling through the guiding tube along the planned trajectory is performed percutaneously. A hollow tube is then placed through the working channel and advanced into the pedicle and through the posterior vertebral wall. A Kirschner wire (K-wire) is then placed into the vertebral body and the hollow tube is withdrawn. This procedure is repeated until trajectories are drilled and K-wires are placed at all levels to be treated. At this point, robotic guidance is complete. The mounting system remains attached to allow a repeat robot-guided approach in case 1 of the trajectories is lost. 6. Vertebral body augmentation : In vertebroplasty, venous channels are blocked with slurry made of saline-contrastgelfoam media, 12 a bone marrow biopsy needle is introduced over the K-wire into the vertebral body, and a designated augmentation polymethyl methacrylate cement is injected with 2.5-mL syringes. In balloon kyphoplasty, the kit s introducer is placed over the K-wire and the procedure is performed according to the manufacturer s protocol. 13 When intravertebral expandable devices are used, the kit s introducer is placed over the K-wire and the procedure is performed according to the manufacturer s protocol. Cement is injected simultaneously by 2 surgeons into 2 ports at the same level or into 2 vertebrae in multilevel augmentation, with unilateral approaches with pulsed fluoroscopy monitoring for each 0.25 ml of injected cement. After the augmentation procedure, patients are allowed to walk freely. They are observed overnight and discharged home the next day. Data Collection Clinical data included patient demographics, indications for surgery, the number of operated levels, and the method of augmentation used. Robotic data included the platform chosen for each patient from 3 available platforms, rate of execution (executed/ planned trajectories), success of guidance ( i.e., rate of K-wire placement on the planned trajectory, as confirmed on intraoperative fluoroscopy), and robotic guidance time. In addition, intraoperative and postoperative challenges and perioperative complications were noted January 2014
3 TABLE 1. Patient Demographics Value Range Patient age (mean) Number of levels augmented 2 (mean) 1 6 M:F 9:24 Thoracic levels 22 T5 T12 Lumbar levels 38 L1 L5 Sacral levels 1 Sacrum Indication for surgery Tumor, 8; vertebral compression fracture, 25 The effective radiation dose (msv) from preoperative CT data was recorded for each patient. This parameter was calculated from the dose length product that is routinely reported for every CT examination performed in our scanner. The K conversion value was Radiation exposure for OR personnel was calculated on the basis of duration of intraoperative fluoroscopy required for calibration, registration, confirmation of K-wire placement within the vertebra, needle placement, and vertebral augmentation. This data were routinely collected during all robotic procedures. Effective doses were not recorded during surgery. Because of the retrospective nature of this study, we could not capture this data. On the basis of the literature, 80 seconds of intraoperative fluoroscopy delivers a radiation dose that is comparable with standard MDCT scan of the lumbar spine. Statistical Analysis Descriptive statistics were prepared to present the data and compared with published results describing fluoroscopyguided and navigation-assisted vertebral augmentation. RESULTS Between January 2008 and March 2010, 33 patients, including 24 females (72%) and 9 males (27%), with an average age of 67 years (range, yr) underwent robot-guided vertebral augmentation. The series included 85 robot-assisted trajectories in 60 augmented vertebrae. A range of 1 to 6 vertebrae were augmented per patient, with a mean of 2. Augmentation was performed in 22 thoracic vertebrae from T5 T12 (27 trajectories), 38 lumbar vertebrae from L1 L5 (56 trajectories), and 1 sacral vertebra (2 trajectories). In 25 patients (76%), augmentation was performed because of osteoporotic fractures; 8 (24%) experienced pathological fractures due to multiple myeloma or metastatic disease. Kyphoplasty was performed in 15 patients (46%), including 1 sacroplasty; vertebroplasty in 13 (39%), and an intravertebral expanding implant was used in 5 (15%). The average procedure time was 118 minutes (range, ), with variation according to the number of levels augmented and the need for surgical decompression or tumor debulking. Robotic guidance took an average of 35.8 minutes per case (range, 10 93). Average radiation time per level (reflecting the patient s exposure to radiation) was 41.6 seconds (range, s). Radiation exposure time for surgeons and OR staff per augmented level was 34.1 seconds on average (range, s). The average preoperative CT effective dose in this study was 50 msv (range 18 81). It is worth noting that the CT protocol that formed the basis for this study has been substantially revised as a result of this study. The current protocol delivers a dose that is a 75% reduction from this dose. The number of planned trajectories was in the range from 1 to 8 (mean, 2.7). The robot was mounted on a bed-mount device in 29 patients (88%), on the Hover-T Platform (Mazor Surgical Technologies) in 3 patients (9%), and on a clamp in 1 patient (3%). The mean execution rate (executed vs. planned trajectories) was 99% (range 83% 100%). One trajectory was aborted because it was out of the field of the fluoroscopy images taken for registration in a patient undergoing augmentation at nonconsecutive 6 levels. The surgeon opted to perform augmentation on this level manually instead of repeating the registration procedure. Mean accuracy was 98.8%. One trajectory was missed laterally (the K-wire insertion felt wrong and the check fluoroscopic images confirmed). The trajectory was corrected manually under fluoroscopic guidance. The missed trajectory did not result in any clinical complication. A loosened connection between the K-wire and the Hover-T Bridge was observed in 2 cases. This resulted in motion of the bridge with respiration. The loose connections were noticed in both cases. The connection was secured, new fluoroscopy images were acquired, and the trajectories were properly executed. There were 2 complications in the series. One patient developed a hemothorax 9 days after augmentation of T12 with an expandable intravertebral implant. A chest drain was inserted and the hemothorax resolved. Another patient undergoing combined open L3 L4 decompression and L3 vertebral body augmentation developed a superficial wound infection, which healed with administration of intravenous antibiotics and local care. DISCUSSION Osteoporotic vertebral compression fractures occur in up to 20% of the elderly population. 14 As the world population ages and life expectancies for patients with many cancers continue to increase, the frequency of vertebral compression fracture and vertebral augmentation procedures is rising. As a result, patients, surgeons, and OR staff members are exposed to increasing levels of radiation related to vertebral augmentation procedures. In addition, up to 40% of patients with cancer develop spinal metastases, 15 which often lead to compression fractures. The relative risk for cancer among orthopedic surgeons is 5.37 compared with the general population. 2 Malignancies in exposed personnel range from cancers of solid organs ( i.e., thyroid and pancreas) to skin and hematopoietic cancers. 2 In female orthopedic surgeons, the standardized prevalence ratio for all cancers is 1.9 ( P = ), and the ratio is 2.88 for Spine 155
4 breast cancer ( P < ), when compared with the general population. 1 The estimated radiation exposure to patients during large C-arm procedures is 12 to 14 msv ( mrem) per minute, and for mini C-arm use it is 1.2 to 4 msv ( mrem) per minute. 3 The annual whole-body limit for occupational exposure is 50 msv (5 rem). 9 Annual occupational limits are 150 msv (15 rem) for eye exposure, 300 msv (30 rem) for thyroid exposure, and 500 msv (50 rem) for other organs. 3 In the literature discussing radiation exposure in vertebral body augmentation, the use of navigation systems has been shown to reduce exposure time from 175 ± 23 seconds per level in fluoroscopy-guided procedures to 74 seconds per level under 2-dimensional imaging guidance and 99 seconds per level under 3-dimensional imaging guidance. 16 In the radiological literature, radiation exposure time reached 10 minutes per level in some vertebroplasty and kyphoplasty procedures. 17 In this series of patients, the average operative radiation exposure time was 41.6 seconds per level. During calibration and registration, the surgeon and OR staff are protected behind lead walls, and when this time is eliminated exposure time is further reduced to 34.1 seconds per level. The robotic method described here reduces exposure time by approximately 50% when compared with the shortest published results 16 ( Table 2 ). Cannulation of the vertebrae requires both AP and 60º oblique fluoroscopic images for registration, 2 fluoroscopic images to verify K-wire position prior to needle insertion, and 2 to 4 fluoroscopy images to verify positioning of the needles, for a total of 6 to 8 fluoroscopic images. The use of pulsed fluoroscopy, with 1 image taken for every 0.25 to 0.5 ml of cement injected through a port, with 2 surgeons working simultaneously on 2 ports, also reduces the amount of radiation. The use of pulsed fluoroscopy while cementing the vertebrae is safe, as long as cement is injected carefully and at the proper viscosity, thus preventing leakage and uncontrolled cementation. In this series of patients, no cementation-related complications occurred. The robot reduces the need for radiation exposure to the surgical staff by guiding the surgeon along a previously planned trajectory. In a prior report from our group 11 the accuracy of the surgical robot in guiding pedicle screws was 89.3%. In the current series, the accuracy of robotic guidance was 99%. This difference can be explained by the additional experience gained since the initial publication. Moreover, the planned entry points in vertebral augmentations were on a straight surface, on top of the ascending articular process. This entry point is less prone to skiving when compared with the entry point of a pedicle screw, near the mammillary process. In addition to the risk for hospital staff, 1 must take into consideration patients exposure. The robotic guidance technique requires a preoperative CT scan. The protocol was set according to the manufacturer demands and includes a high-kv study with very thin slices and slice overlap. As a TABLE 2. Comparison Between Published Results on Radiation Exposure During Freehand Augmentation and Navigation-Assisted Vertebral Body Augmentation and the Results in a Series of Robot-Guided Vertebral Body Augmentation Technique Freehand Freehand Computer navigation Robot-assisted Radiation Exposure per Level 175 ± 23 s 10.1 min ± 22 s Reference Izadpanah et al 16 (2009) Perisinakis et al 17 (2004) 74 ± 27 s in 2D mode/lumbar Izadpanah et al ± 38 s in 3D mode/thoracic (2009) Patients exposure, 41.6 s Current patient series Surgeon and OR staff exposure, 34.1 s According to this comparison, more than 50% reduction in radiation exposure to the surgeon can be achieved when using robotic guidance when compared with the best published results in navigation-assisted augmentation. OR indicates operating room. result, the radiation dose is relatively high compared with conventional CT examination of the spine. With the goal of reducing this dose, we initiated discussions with the robot manufacturer, which led to improvements in algorithms run by the robot software and the volumetric CT acquisition technique. These changes enable us to perform the preoperative CT using thicker slices and higher pitch values, with retrospective reconstruction of thinner slices from raw data. Currently, the dose is approximately 75% lower that exposure using the initial protocol, which was the basis for analysis in this study. Newer CT machines with sophisticated dose reduction software will probably permit further reductions of radiation exposure with acceptable or even improved image quality. This assumption warrants a prospective analysis. Patients with severe osteoporosis present a challenge, and may require the protocol suggested by the robot manufacturer. The field of view should be limited to the region of interest, enabling further reduction in radiation exposure to the patient. Reducing radiation exposure is especially important when treating young healthy patients, especially female patients, because their longer life expectancies increase the risk that radiation-induced malignancies could develop. 17 Most of the patients in this series were older than 60 years or patients with cancer. In these patients, the accuracy achieved by robotic guidance seems to justify the radiation exposure caused by the preoperative CT scan January 2014
5 CONCLUSION The use of robot guidance and pulsed fluoroscopy in vertebral body cement augmentation markedly reduces radiation exposure for surgeons and OR staff when compared with published results in similar procedures. Technical advances in CT equipment and modifications to CT protocols enable reduced radiation exposure from preoperative CT scans for patients, and may allow the use of these techniques in young, otherwise healthy patients. Key Points Vertebral body cement augmentation is associated with significant radiation exposure to the patient and the operating staff. Occupational radiation exposure is associated with increased cancer risk. A retrospective analysis of a series of robotguided vertebral cement augmentation was conducted. Robot-guided vertebral body cement augmentation performed by 2 surgeons, simultaneously injecting cement under pulsed fluoroscopy reduces radiation exposure to the surgeon and OR staff when compared with the published results on freehand and navigationassisted augmentation. References 1. Chou LB, Cox CA, Tung JJ, et al. Prevalence of cancer in female orthopaedic surgeons in the United States. J Bone Joint Surg Am 2010 ; 92 : Mastrangelo G, Fedeli U, Fadda E, et al. Increased cancer risk among surgeons in an orthopaedic hospital. Occup Med (Lond) 2005 ; 55 : Singer G. Occupational radiation exposure to the surgeon. J Am Acad Orthop 2005 ; 13 : Chiras J, Sola-Martinez MT, Weill A, et al. [Percutaneous vertebroplasty]. Rev Med Interne 1995 ; 16 : Hulme PA, Krebs J, Ferguson SJ, et al. Vertebroplasty and kyphoplasty: a systematic review of 69 clinical studies. Spine (Phila Pa 1976) 2006 ; 31 : Gao M, Lei W, Wu Z, et al. Biomechanical evaluation of fixation strength of conventional and expansive pedicle screws with or without calcium based cement augmentation. Clin Biomech (Bristol, Avon) 2011 ; 26 : Ghofrani H, Nunn T, Robertson C, et al. An evaluation of fracture stabilization comparing kyphoplasty and titanium mesh repair techniques for vertebral compression fractures: is bone cement necessary? Spine (Phila Pa 1976) 2010 ; 35 : E Jung MY, Shin DA, Hahn IB, et al. Serious complication of cement augmentation for damaged pilot hole. Yonsei Med J 2010 ; 51 : Harstall R, Heini PF, Mini RL, et al. Radiation exposure to the surgeon during fluoroscopically assisted percutaneous vertebroplasty: a prospective study. Spine (Phila Pa 1976) 2005 ; 30 : Larsson S. Cement augmentation in fracture treatment. Scand J Surg 2006 ; 95 : Devito DP, Kaplan L, Dietl R, et al. Clinical acceptance and accuracy assessment of spinal implants guided with SpineAssist surgical robot: retrospective study. Spine (Phila Pa 1976) 2010 ; 35 : Pedicelli A, Rollo M, Piano M, et al. Percutaneous vertebroplasty: optimizing the procedure after treatment of 250 vertebral levels under fluoroscopic guidance. Radiol Med 2009 ; 114 : Pateder DB, Khanna AJ, Lieberman IH. Vertebroplasty and kyphoplasty for the management of osteoporotic vertebral compression fractures. Orthop Clin North Am 2007 ; 38 : ; abstract vii. 14. Griffith JF, Guglielmi G. Vertebral fracture. Radiol Clin North Am 2010 ; 48 : Klimo P Jr, Schmidt MH : Surgical management of spinal metastases. Oncologist 2004 ; 9 : Izadpanah K, Konrad G, Sudkamp NP, et al. Computer navigation in balloon kyphoplasty reduces the intraoperative radiation exposure. Spine (Phila Pa 1976) 2009 ; 34 : Perisinakis K, Damilakis J, Theocharopoulos N, et al. Patient exposure and associated radiation risks from fluoroscopically guided vertebroplasty or kyphoplasty. Radiology 2004 ; 232 : Spine 157
Introduction of FIREFLY Technology
 Introduction of FIREFLY Technology FIREFLY Technology is a unique, patent-pending, pre-surgical planning and intra - operative navigation technology that is focused on spinal applications and is derived
Introduction of FIREFLY Technology FIREFLY Technology is a unique, patent-pending, pre-surgical planning and intra - operative navigation technology that is focused on spinal applications and is derived
IMAGE-GUIDED SPINE SURGERY
 SPINE NAVIGATION IMAGE-GUIDED SPINE SURGERY CONFIDENCE AND ACCURACY Brainlab Spinal Navigation combines state-of-the-art touch screen based image control with best-in-class registration methods for image-guided
SPINE NAVIGATION IMAGE-GUIDED SPINE SURGERY CONFIDENCE AND ACCURACY Brainlab Spinal Navigation combines state-of-the-art touch screen based image control with best-in-class registration methods for image-guided
Pedicle screw insertion : robotic assistance versus conventional C-arm fluoroscopy
 Acta Orthop. Belg., 2012, 78, 240-245 ORIGINAL STUDY Pedicle screw insertion : robotic assistance versus conventional C-arm fluoroscopy Constantin SCHizAS, Eric THEin, Barbara KwiATKOwSKi, Gerit KULiK
Acta Orthop. Belg., 2012, 78, 240-245 ORIGINAL STUDY Pedicle screw insertion : robotic assistance versus conventional C-arm fluoroscopy Constantin SCHizAS, Eric THEin, Barbara KwiATKOwSKi, Gerit KULiK
Reduction of Radiation Exposure in Percutaneous Pedicle Screw Placement by Using a New Extension Instrument
 Reduction of Radiation Exposure in Percutaneous Pedicle Screw Placement by Using a New Extension Instrument Franquiz M. Juan, Myers J.Behnam, Thomas A. Michael, Greenhalgh J. Travis, Shoup J. Andrew Study
Reduction of Radiation Exposure in Percutaneous Pedicle Screw Placement by Using a New Extension Instrument Franquiz M. Juan, Myers J.Behnam, Thomas A. Michael, Greenhalgh J. Travis, Shoup J. Andrew Study
Robotic Spine Surgery [TASE]: MZOR
![Robotic Spine Surgery [TASE]: MZOR Robotic Spine Surgery [TASE]: MZOR](/thumbs/94/121596111.jpg) Robotic Spine Surgery [TASE]: MZOR Nov. 2012 Forward Looking Statements Any forecast and/or forecasting statement, included in this presentation, is based on the Management's assessment at its discretion.
Robotic Spine Surgery [TASE]: MZOR Nov. 2012 Forward Looking Statements Any forecast and/or forecasting statement, included in this presentation, is based on the Management's assessment at its discretion.
During recent years, image guidance is increasingly
 SPINE Volume 37, Number 8, pp E496 E501 2012, Lippincott Williams & Wilkins TECHNIQUE Accuracy of Robot-Assisted Placement of Lumbar and Sacral Pedicle Screws A Prospective Randomized Comparison to Conventional
SPINE Volume 37, Number 8, pp E496 E501 2012, Lippincott Williams & Wilkins TECHNIQUE Accuracy of Robot-Assisted Placement of Lumbar and Sacral Pedicle Screws A Prospective Randomized Comparison to Conventional
PERFORATED CLICK X Augmentable pedicle screws for osteoporotic bone
 PERFORATED CLICK X Augmentable pedicle screws for osteoporotic bone Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE
PERFORATED CLICK X Augmentable pedicle screws for osteoporotic bone Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE
MISS in Thoracolumbar Fractures
 MISS in Thoracolumbar Fractures Guillem Saló Bru, MD, Phd Spine Unit. Orthopaedic Department. Hospital del Mar. Barcelona. Associated Professor. Universitat Autónoma de Barcelona. Introduction. The application
MISS in Thoracolumbar Fractures Guillem Saló Bru, MD, Phd Spine Unit. Orthopaedic Department. Hospital del Mar. Barcelona. Associated Professor. Universitat Autónoma de Barcelona. Introduction. The application
Dr. Christopher R. Good Virginia Spine Institute
 Dr. Christopher R. Good Virginia Spine Institute College University of Rochester Medical School University of Rochester School of Medicine Residency in Orthpaedic Surgery Cornell University Medical Center
Dr. Christopher R. Good Virginia Spine Institute College University of Rochester Medical School University of Rochester School of Medicine Residency in Orthpaedic Surgery Cornell University Medical Center
DePuy International Ltd St Anthony s Road Leeds LS11 8DT England Tel: +44 (0) Fax: +44 (0)
 Reference: 1. Data on file at DePuy Spine TM 2008 DePuy Spine International is a joint venture with Biedermann Motech, GmbH. This publication is not intended for distribution in the USA. X-ray on front
Reference: 1. Data on file at DePuy Spine TM 2008 DePuy Spine International is a joint venture with Biedermann Motech, GmbH. This publication is not intended for distribution in the USA. X-ray on front
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
VERTEBRAL AUGMENTATION EXCELLENCE. by VEXIM REDEFINING YOUR CONFIDENCE
 VERTEBRAL AUGMENTATION EXCELLENCE by VEXIM REDEFINING YOUR CONFIDENCE MASTERFLOW TM INJECTION SYSTEM HYDRAULIC PUMP EFFORTLESS INJECTION OF HIGH VISCOSITY CEMENT QUICK-STOP BUTTON CONTROLLED CEMENT FLOW
VERTEBRAL AUGMENTATION EXCELLENCE by VEXIM REDEFINING YOUR CONFIDENCE MASTERFLOW TM INJECTION SYSTEM HYDRAULIC PUMP EFFORTLESS INJECTION OF HIGH VISCOSITY CEMENT QUICK-STOP BUTTON CONTROLLED CEMENT FLOW
AcUMEDr. Locking Proximal Humeral Plate. PoLARUSr PHPt
 AcUMEDr Locking Proximal Humeral Plate PoLARUSr PHPt PoLARUSr PHPt LOCKING PROXIMAL HUMERAL PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons,
AcUMEDr Locking Proximal Humeral Plate PoLARUSr PHPt PoLARUSr PHPt LOCKING PROXIMAL HUMERAL PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons,
Kyphoplasty and Vertebroplasty
 Kyphoplasty and Vertebroplasty Policy Number: Original Effective Date: MM.06.007 01/11/2005 Line(s) of Business: Current Effective Date: HMO; PPO 02/01/2012 Section: Surgery Place(s) of Service: Inpatient;
Kyphoplasty and Vertebroplasty Policy Number: Original Effective Date: MM.06.007 01/11/2005 Line(s) of Business: Current Effective Date: HMO; PPO 02/01/2012 Section: Surgery Place(s) of Service: Inpatient;
UTERINE FIBROID EMBOLIZATION
 INTERVENTIONAL RADIOLOGY PROTOCOLS UTERINE FIBROID EMBOLIZATION Interventional Radiology Tower Health Medical Group offers the option to treat uterine fibroids with fibroid embolization (UFE), an alternative
INTERVENTIONAL RADIOLOGY PROTOCOLS UTERINE FIBROID EMBOLIZATION Interventional Radiology Tower Health Medical Group offers the option to treat uterine fibroids with fibroid embolization (UFE), an alternative
CPT 2015: Save Your Practice By Shaping Up Your Spinal Procedure Reporting
 2015 Physician Coding Survival Guide CHAPTER 10: NEUROSURGERY CPT 2015: Save Your Practice By Shaping Up Your Spinal Procedure Reporting Sacroplasty codes will now be inclusive of imaging guidance. You
2015 Physician Coding Survival Guide CHAPTER 10: NEUROSURGERY CPT 2015: Save Your Practice By Shaping Up Your Spinal Procedure Reporting Sacroplasty codes will now be inclusive of imaging guidance. You
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
VIPER Cortical Fix Fenestrated Screw System. Surgical Technique for OPEN & MIS Procedures
 VIPER Cortical Fix Fenestrated Screw System Surgical Technique for OPEN & MIS Procedures Image intensifier control This description alone does not provide sufficient background for direct use of DePuy
VIPER Cortical Fix Fenestrated Screw System Surgical Technique for OPEN & MIS Procedures Image intensifier control This description alone does not provide sufficient background for direct use of DePuy
Percutaneous Posterior Fixation: A Unique Entity to minimize Further Damage to Patient with Traumatic Spine
 Kaushal R Patel et al RESEARCH ARTICLE 10.5005/jp-journals-10039-1129 Percutaneous Posterior Fixation: A Unique Entity to minimize Further Damage to Patient with Traumatic Spine 1 Kaushal R Patel, 2 Jayprakash
Kaushal R Patel et al RESEARCH ARTICLE 10.5005/jp-journals-10039-1129 Percutaneous Posterior Fixation: A Unique Entity to minimize Further Damage to Patient with Traumatic Spine 1 Kaushal R Patel, 2 Jayprakash
PERCUTANEOUS BALLOON KYPHOPLASTY, RADIOFREQUENCY KYPHOPLASTY, AND MECHANICAL VERTEBRAL AUGMENTATION
 KYPHOPLASTY, AND MECHANICAL VERTEBRAL AUGMENTATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures,
KYPHOPLASTY, AND MECHANICAL VERTEBRAL AUGMENTATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures,
Surgical Technique & Product Catalogue. Guide for Open & MIS Procedures
 Surgical Technique & Product Catalogue Guide for Open & MIS Procedures INTRODUCTION The VIPER Cortical Fix Fenestrated Screw System is the first pedicle screw implant to offer enhanced fixation in both
Surgical Technique & Product Catalogue Guide for Open & MIS Procedures INTRODUCTION The VIPER Cortical Fix Fenestrated Screw System is the first pedicle screw implant to offer enhanced fixation in both
3. PATIENT POSITIONING & FRACTURE REDUCTION 3 8. DISTAL GUIDED LOCKING FOR PROXIMAL NAIL PROXIMAL LOCKING FOR LONG NAIL 13
 Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL NAIL INSERTION 6-7 7. PROXIMAL LOCKING
Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL NAIL INSERTION 6-7 7. PROXIMAL LOCKING
Intraoperative case studies. Portable full body 32-slice CT scanner
 Intraoperative case studies Portable full body 32-slice CT scanner Point-of-care CT imaging Your multi-departmental imaging solution Orthopedic surgery Arthroplasty Musculoskeletal disorders Hip replacement
Intraoperative case studies Portable full body 32-slice CT scanner Point-of-care CT imaging Your multi-departmental imaging solution Orthopedic surgery Arthroplasty Musculoskeletal disorders Hip replacement
Augmentable Pedicle Screws for Osteoporotic Bone. Perforated Click X. Surgical Technique
 Augmentable Pedicle Screws for Osteoporotic Bone Perforated Click X Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Augmentable Pedicle Screws for Osteoporotic Bone Perforated Click X Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Ref: Q400-09T1 EBI Spine. September 05/VS02. c/o BIOMET Spain Orthopaedics, S.L.
 Ref: Q400-09T1 EBI Spine. September 05/VS02 c/o BIOMET Spain Orthopaedics, S.L. www.ebimedical.com EBI Omega 21 TM LP Since its introduction in 1996, and with thousands of patients treated so far, the
Ref: Q400-09T1 EBI Spine. September 05/VS02 c/o BIOMET Spain Orthopaedics, S.L. www.ebimedical.com EBI Omega 21 TM LP Since its introduction in 1996, and with thousands of patients treated so far, the
Conventus CAGE PH Surgical Techniques
 Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
SURGICAL TECHNIQUE GUIDE
 The following general surgical technique is for illustrative purposes only. As with all surgical procedures, the technique used in each case will depend on the surgeon s medical judgment as to the best
The following general surgical technique is for illustrative purposes only. As with all surgical procedures, the technique used in each case will depend on the surgeon s medical judgment as to the best
Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: A cadaveric study
 Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: A cadaveric study [ based on the homonymous paper from Prof.Lamartina et al. Anticipated publication
Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: A cadaveric study [ based on the homonymous paper from Prof.Lamartina et al. Anticipated publication
System. Humeral Nail. Surgical Technique
 System Humeral Nail Surgical Technique Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL
System Humeral Nail Surgical Technique Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL
I. II. SPINAL SYSTEM SURGICAL TECHNIQUE GUIDE
 I. GS1 II. SPINAL SYSTEM SURGICAL TECHNIQUE GUIDE Introduction The Gold Standard Orthopaedics, LLC GS1 Spinal System designed in conjunction with Richard Holt, M.D. incorporates both strength and function
I. GS1 II. SPINAL SYSTEM SURGICAL TECHNIQUE GUIDE Introduction The Gold Standard Orthopaedics, LLC GS1 Spinal System designed in conjunction with Richard Holt, M.D. incorporates both strength and function
Departement of Neurosurgery A.O.R.N A. Cardarelli- Naples.
 Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
REFERENCE DOCTOR Thoracolumbar Trauma MIS Options. Hyeun Sung Kim, MD, PhD,
 Thoracolumbar Trauma MIS Options Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean Neurosurgical Society / Korean
Thoracolumbar Trauma MIS Options Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean Neurosurgical Society / Korean
Retrospective Evaluation. Pain Physician 2012; 15: ISSN Bassem Georgy, MD
 Pain Physician 2012; 15:223-228 ISSN 1533-3159 Retrospective Evaluation Feasibility, Safety and Cement Leakage in Vertebroplasty of Osteoporotic and Malignant Compression Fractures Using Ultra-Viscous
Pain Physician 2012; 15:223-228 ISSN 1533-3159 Retrospective Evaluation Feasibility, Safety and Cement Leakage in Vertebroplasty of Osteoporotic and Malignant Compression Fractures Using Ultra-Viscous
UNIQUE ANATOMIES PATIENT-MATCHED SOLUTIONS. Surgical Technique
 UNIQUE ANATOMIES PATIENT-MATCHED SOLUTIONS Surgical Technique Joint Spine Sports Med MySpine Surgical Technique Joint Spine Sports Med 2 INTRODUCTION MySpine is a patient matched, pedicle targeted technology
UNIQUE ANATOMIES PATIENT-MATCHED SOLUTIONS Surgical Technique Joint Spine Sports Med MySpine Surgical Technique Joint Spine Sports Med 2 INTRODUCTION MySpine is a patient matched, pedicle targeted technology
Kyphoplasty and Vertebroplasty
 Kyphoplasty and Vertebroplasty Policy Number: Original Effective Date: MM.06.007 01/11/2005 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 06/27/2014 Section: Surgery Place(s)
Kyphoplasty and Vertebroplasty Policy Number: Original Effective Date: MM.06.007 01/11/2005 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 06/27/2014 Section: Surgery Place(s)
3.5 mm Locking Attachment Plate
 For Treatment of Periprosthetic Fractures 3.5 mm Locking Attachment Plate Surgical Technique Table of Contents Introduction 3.5 mm Locking Attachment Plate 2 Indications 4 Surgical Technique Preparation
For Treatment of Periprosthetic Fractures 3.5 mm Locking Attachment Plate Surgical Technique Table of Contents Introduction 3.5 mm Locking Attachment Plate 2 Indications 4 Surgical Technique Preparation
OPTICAL TOPOGRAPHIC IMAGING FOR SPINAL INTRAOPERATIVE 3D NAVIGATION IN MINIMALLY INVASIVE APPROACHES: INITIAL PRECLINICAL EXPERIENCE
 OPTICAL TOPOGRAPHIC IMAGING FOR SPINAL INTRAOPERATIVE 3D NAVIGATION IN MINIMALLY INVASIVE APPROACHES: INITIAL PRECLINICAL EXPERIENCE Authors: Daipayan Guha 1, Raphael J akubovic 2, Shaurya Gupta 1, Albert
OPTICAL TOPOGRAPHIC IMAGING FOR SPINAL INTRAOPERATIVE 3D NAVIGATION IN MINIMALLY INVASIVE APPROACHES: INITIAL PRECLINICAL EXPERIENCE Authors: Daipayan Guha 1, Raphael J akubovic 2, Shaurya Gupta 1, Albert
Asnis. Micro Cannulated screw system. Xpress operative technique
 Asnis Micro Cannulated screw system Xpress operative technique Asnis Micro Cannulated screw system Table of contents Indications, precautions & contraindications 3 Operative technique 4 This publication
Asnis Micro Cannulated screw system Xpress operative technique Asnis Micro Cannulated screw system Table of contents Indications, precautions & contraindications 3 Operative technique 4 This publication
M.I.S. MAKE IT SMART IN ONE SYSTEM. Surgical Technique. Hip Knee Spine Navigation
 M.I.S. MAKE IT SMART IN ONE SYSTEM Surgical Technique Hip Knee Spine Navigation M.U.S.T. Mini Open Surgical Technique Hip Knee Spine Navigation 2 C O N T E N T S 1 INTRODUCTION 4 2 SURGICAL TECHNIQUE 5
M.I.S. MAKE IT SMART IN ONE SYSTEM Surgical Technique Hip Knee Spine Navigation M.U.S.T. Mini Open Surgical Technique Hip Knee Spine Navigation 2 C O N T E N T S 1 INTRODUCTION 4 2 SURGICAL TECHNIQUE 5
Surgical technique. synex. The vertebral body replacement with ratchet mechanism.
 Surgical technique synex. The vertebral body replacement with ratchet mechanism. Table of contents Indications and contraindications 2 Implants 3 Surgical technique 4 Cleaning of instruments 10 Optional
Surgical technique synex. The vertebral body replacement with ratchet mechanism. Table of contents Indications and contraindications 2 Implants 3 Surgical technique 4 Cleaning of instruments 10 Optional
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
Service: Imaging. Vertebroplasty. Exceptional healthcare, personally delivered
 Service: Imaging Exceptional healthcare, personally delivered Your Doctor has requested that you have a vertebroplasty. We hope the following information will answer some of the questions you may have
Service: Imaging Exceptional healthcare, personally delivered Your Doctor has requested that you have a vertebroplasty. We hope the following information will answer some of the questions you may have
Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine.
 Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine. Technique Guide Instruments and implants approved by the AO Foundation
Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine. Technique Guide Instruments and implants approved by the AO Foundation
Index. Note: Page numbers of article titles are in boldface type.
 Orthop Clin N Am 38 (2007) 463 468 Index Note: Page numbers of article titles are in boldface type. A Andreas Vesalius, in history of spine pathology, 306 Anesthesia/anesthetics for PECD, 329 in minimally
Orthop Clin N Am 38 (2007) 463 468 Index Note: Page numbers of article titles are in boldface type. A Andreas Vesalius, in history of spine pathology, 306 Anesthesia/anesthetics for PECD, 329 in minimally
Pedicle screw instrumentation is used in the
 SPINE Volume 43, Number 17, pp E983 E989 ß 2018 Wolters Kluwer Health, Inc. All rights reserved. BIOMECHANICS Pullout Strength of Pedicle Screws Following Redirection After Lateral or Medial Wall Breach
SPINE Volume 43, Number 17, pp E983 E989 ß 2018 Wolters Kluwer Health, Inc. All rights reserved. BIOMECHANICS Pullout Strength of Pedicle Screws Following Redirection After Lateral or Medial Wall Breach
Surgical Technique Guide
 Surgical Technique Guide Minimally Invasive, Intramedullary Device For Distal Radius Fragility Fractures The Sonoma WRx Wrist Fracture Repair Device is flexible, inserting easily through a small incision
Surgical Technique Guide Minimally Invasive, Intramedullary Device For Distal Radius Fragility Fractures The Sonoma WRx Wrist Fracture Repair Device is flexible, inserting easily through a small incision
Appendix. International coding of diseases according to ICD 10-GM Reimbursement codes per country (in alphabetical order)
 The editors thank Mrs. B. Casteels (Vice President International, Health Policy & Government Relations, Kyphon International), for her help in summarising the current international reimbursement and coding
The editors thank Mrs. B. Casteels (Vice President International, Health Policy & Government Relations, Kyphon International), for her help in summarising the current international reimbursement and coding
Lapidus Arthrodesis System Instructions for Use
 Lapidus Arthrodesis System Instructions for Use Description The AlignMATE Lapidus Arthrodesis System consists of bone plates and bone screws (locking, non-locking and interfragmentary), which are intended
Lapidus Arthrodesis System Instructions for Use Description The AlignMATE Lapidus Arthrodesis System consists of bone plates and bone screws (locking, non-locking and interfragmentary), which are intended
Case Report. Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology
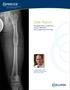 Case Report Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology S. Robert Rozbruch, MD Hospital for Special Surgery New York, NY, USA ABSTRACT This is a case illustrating a 4.5 cm
Case Report Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology S. Robert Rozbruch, MD Hospital for Special Surgery New York, NY, USA ABSTRACT This is a case illustrating a 4.5 cm
Medical Coverage Policy Percutaneous Vertebroplasty and Scaroplasty
 Medical Coverage Policy Percutaneous Vertebroplasty and Scaroplasty EFFECTIVE DATE: 02 01 2011 POLICY LAST UPDATED: 07 02 2013 OVERVIEW Percutaneous vertebroplasty is an interventional technique involving
Medical Coverage Policy Percutaneous Vertebroplasty and Scaroplasty EFFECTIVE DATE: 02 01 2011 POLICY LAST UPDATED: 07 02 2013 OVERVIEW Percutaneous vertebroplasty is an interventional technique involving
Headless Compession Screw 2.5 / 3.0
 SURGICAL TECHNIQUE Headless Compession Screw 2.5 / 3.0 Titanium or Stainless Steel Cannulated Headless Design Multiple Thread Options Torx Driver Sterile and Non-Sterile Options Simple Instrumentation
SURGICAL TECHNIQUE Headless Compession Screw 2.5 / 3.0 Titanium or Stainless Steel Cannulated Headless Design Multiple Thread Options Torx Driver Sterile and Non-Sterile Options Simple Instrumentation
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
 Visit our website on www.biotech-medical.com The DLP - Dorso-Lumbar Polyaxial Screw System has been designed to address the pathologies of the thoracolumbar spine. The DLP System contains a wide range
Visit our website on www.biotech-medical.com The DLP - Dorso-Lumbar Polyaxial Screw System has been designed to address the pathologies of the thoracolumbar spine. The DLP System contains a wide range
PFNA. With Augmentation Option.
 PFNA. With Augmentation Option. Superior anchor in osteoporotic bone Simple and reproducible procedure through standardized technique Intraoperative decision for augmentation PFNA. Proximal Femoral Nail
PFNA. With Augmentation Option. Superior anchor in osteoporotic bone Simple and reproducible procedure through standardized technique Intraoperative decision for augmentation PFNA. Proximal Femoral Nail
Technique Guide. Insight Retractor. Minimal invasive access system to the posterior thoracolumbar spine.
 Technique Guide Insight Retractor. Minimal invasive access system to the posterior thoracolumbar spine. Table of Contents Introduction Insight Retractor 2 AO Principles 4 Indications and Contraindications
Technique Guide Insight Retractor. Minimal invasive access system to the posterior thoracolumbar spine. Table of Contents Introduction Insight Retractor 2 AO Principles 4 Indications and Contraindications
The Most Reliable Spinal Solution
 MFG : 09.02.20 REV : 1 4CIS VANE introduces you the reliable pedicle screw The Most Reliable Spinal Solution Non-slip threaded joint Ergonomic design Wedged trapezoid thread Superior locking mechanism
MFG : 09.02.20 REV : 1 4CIS VANE introduces you the reliable pedicle screw The Most Reliable Spinal Solution Non-slip threaded joint Ergonomic design Wedged trapezoid thread Superior locking mechanism
Cement augmentation in spinal tumors: a systematic review comparing vertebroplasty and kyphoplasty
 35 35 43 Cement augmentation in spinal tumors: a systematic review comparing vertebroplasty and kyphoplasty Authors Josh E Schroeder¹, Erika Ecker², Andrea C Skelly², Leon Kaplan¹ Institutions ¹ Orthopedic
35 35 43 Cement augmentation in spinal tumors: a systematic review comparing vertebroplasty and kyphoplasty Authors Josh E Schroeder¹, Erika Ecker², Andrea C Skelly², Leon Kaplan¹ Institutions ¹ Orthopedic
Robotically Assisted Nerve and Facet Blocks: A Cadaveric Study 1
 Technical Report Robotically Assisted Nerve and Facet Blocks: A Cadaveric Study 1 Kevin Cleary, PhD, Dan Stoianovici, PhD, Alexandru Patriciu, MS, Dumitru Mazilu, PhD David Lindisch, RT, Vance Watson,
Technical Report Robotically Assisted Nerve and Facet Blocks: A Cadaveric Study 1 Kevin Cleary, PhD, Dan Stoianovici, PhD, Alexandru Patriciu, MS, Dumitru Mazilu, PhD David Lindisch, RT, Vance Watson,
Technique Guide. 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm LCP Distal Fibula Plates 2 AO Principles
Technique Guide 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm LCP Distal Fibula Plates 2 AO Principles
Technique Guide. 3.5 mm LCP Proximal Tibia Plate. Part of the Synthes Small Fragment LCP System.
 Technique Guide 3.5 mm LCP Proximal Tibia Plate. Part of the Synthes Small Fragment LCP System. Table of Contents AO ASIF Principles of Internal Fixation 4 Indications/Contraindications 5 Surgical Technique
Technique Guide 3.5 mm LCP Proximal Tibia Plate. Part of the Synthes Small Fragment LCP System. Table of Contents AO ASIF Principles of Internal Fixation 4 Indications/Contraindications 5 Surgical Technique
CT Guided Procedures And Interesting Cases. Stephen Kim, MD Diagnostic and Interventional Radiology
 CT Guided Procedures And Interesting Cases Stephen Kim, MD Diagnostic and Interventional Radiology CT guided procedure benefits Precise lesion targeting Clear image guidance for needle placement Immediate
CT Guided Procedures And Interesting Cases Stephen Kim, MD Diagnostic and Interventional Radiology CT guided procedure benefits Precise lesion targeting Clear image guidance for needle placement Immediate
SpineJack. Ø 5.8 mm Ø 5.0 mm Ø 4.2 mm. Controlled Anatomical Restoration
 SpineJack Ø 5.8 mm Ø 5.0 mm Ø 4.2 mm Controlled Anatomical Restoration Introducing Controlled the Anatomical Surgical Restoration Technique SpineJack The SpineJack System is designed for the Anatomical
SpineJack Ø 5.8 mm Ø 5.0 mm Ø 4.2 mm Controlled Anatomical Restoration Introducing Controlled the Anatomical Surgical Restoration Technique SpineJack The SpineJack System is designed for the Anatomical
Surgical Technique Guide
 Sacroiliac Joint Fusion System Surgical Technique Guide Moving Life Forward Table of Contents SiCure Implant Overview...2 SiCure System Information...3 X-ray Basics...4 Patient Positioning....5 Surgical
Sacroiliac Joint Fusion System Surgical Technique Guide Moving Life Forward Table of Contents SiCure Implant Overview...2 SiCure System Information...3 X-ray Basics...4 Patient Positioning....5 Surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Single-Thread Screw Available in 25-45mm lengths (5mm Increments) Dual-Thread Screw Available in 30-45mm lengths (5mm Increments)
 Single-Thread Screw Available in 25-45mm lengths (5mm Increments) Dual-Thread Screw Available in 30-45mm lengths (5mm Increments) 4.5mm diameter screws All screws cannulated 12mm percutaneous incision
Single-Thread Screw Available in 25-45mm lengths (5mm Increments) Dual-Thread Screw Available in 30-45mm lengths (5mm Increments) 4.5mm diameter screws All screws cannulated 12mm percutaneous incision
Surgical Technique. Anterolateral and Medial Distal Tibia Locking Plates
 Surgical Technique Anterolateral and Medial Distal Tibia Locking Plates PERI-LOC Periarticular Locked Plating System Anterolateral and Medial Distal Tibia Locking Plates Surgical Technique Contents Product
Surgical Technique Anterolateral and Medial Distal Tibia Locking Plates PERI-LOC Periarticular Locked Plating System Anterolateral and Medial Distal Tibia Locking Plates Surgical Technique Contents Product
ACP. Anterior Cervical Plate System SURGICAL TECHNIQUE
 ACP Anterior Cervical Plate System SURGICAL TECHNIQUE ACP TABLE OF CONTENTS INTRODUCTION 4 INDICATIONS AND CONTRAINDICATIONS 5 WARNINGS AND PRECAUTIONS 6 IMPLANT DESCRIPTION 7 INSTRUMENTS 10 SURGICAL
ACP Anterior Cervical Plate System SURGICAL TECHNIQUE ACP TABLE OF CONTENTS INTRODUCTION 4 INDICATIONS AND CONTRAINDICATIONS 5 WARNINGS AND PRECAUTIONS 6 IMPLANT DESCRIPTION 7 INSTRUMENTS 10 SURGICAL
Surgical Technique Manual
 Surgical Technique Manual Surgeon Designers Richard G. Fessler, MD, PhD Northwestern University, Chicago, IL Robert A. Hart, MD Oregon Health and Science University, Portland, OR Robert Labrom, MD Queensland
Surgical Technique Manual Surgeon Designers Richard G. Fessler, MD, PhD Northwestern University, Chicago, IL Robert A. Hart, MD Oregon Health and Science University, Portland, OR Robert Labrom, MD Queensland
CT-guided percutaneous pedicle screw fixation followed by cementoplasty in the treatment of metastatic spinal disease
 CT-guided percutaneous pedicle screw fixation followed by cementoplasty in the treatment of metastatic spinal disease Claudio Pusceddu Dpt of Interventional Radiology Oncological Hospital AOBrotzu Cagliari
CT-guided percutaneous pedicle screw fixation followed by cementoplasty in the treatment of metastatic spinal disease Claudio Pusceddu Dpt of Interventional Radiology Oncological Hospital AOBrotzu Cagliari
Headless Compession Screw 4.5 / 6.5 SURGICAL TECHNIQUE. Titanium or Stainless Steel. Cannulated Headless Design. Multiple Thread Options.
 Headless Compession Screw SURGICAL TECHNIQUE 4.5 / 6.5 Titanium or Stainless Steel Cannulated Headless Design Multiple Thread Options Torx Driver Sterile and Non-Sterile Options Simple Instrumentation
Headless Compession Screw SURGICAL TECHNIQUE 4.5 / 6.5 Titanium or Stainless Steel Cannulated Headless Design Multiple Thread Options Torx Driver Sterile and Non-Sterile Options Simple Instrumentation
Advantages of MISS. Disclosures. Thoracolumbar Trauma: Minimally Invasive Techniques. Minimal Invasive Spine Surgery 11/8/2013.
 3 rd Annual UCSF Techniques in Complex Spine Surgery Program Thoracolumbar Trauma: Minimally Invasive Techniques Research Support: Stryker Disclosures Murat Pekmezci, MD Assistant Clinical Professor UCSF/SFGH
3 rd Annual UCSF Techniques in Complex Spine Surgery Program Thoracolumbar Trauma: Minimally Invasive Techniques Research Support: Stryker Disclosures Murat Pekmezci, MD Assistant Clinical Professor UCSF/SFGH
FREQUENTLY ASKED QUESTIONS
 FREQUENTLY ASKED QUESTIONS The following questions are representative of questions that patients and family members ask when they visit the Bone and Cancer Foundation website or contact the Foundation
FREQUENTLY ASKED QUESTIONS The following questions are representative of questions that patients and family members ask when they visit the Bone and Cancer Foundation website or contact the Foundation
TECHNICAL BROCHURE. Capture Facet Fixation System
 TECHNICAL BROCHURE Capture Facet Fixation System Table of Contents Product Overview...2 Instruments...4 Capture Facet Screw Surgical Technique Patient Preparation and Positioning...6 Guide Pin Placement...7
TECHNICAL BROCHURE Capture Facet Fixation System Table of Contents Product Overview...2 Instruments...4 Capture Facet Screw Surgical Technique Patient Preparation and Positioning...6 Guide Pin Placement...7
Biomet Vertebroplasty System. Surgical Technique
 Biomet Vertebroplasty System Surgical Technique Contents Introduction... Page 1 System Design Features... Page 2 Instruments... Page 3 Pre-Operative Planning... Page 4 And Patient Positioning Lumbar Entry
Biomet Vertebroplasty System Surgical Technique Contents Introduction... Page 1 System Design Features... Page 2 Instruments... Page 3 Pre-Operative Planning... Page 4 And Patient Positioning Lumbar Entry
Indications for Kyphoplasty and Vertebroplasty
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Threshold Pedicular Fixation System Surgical Technique
 Threshold Pedicular Fixation System Surgical Technique Table of Contents Patient Preparation and Positioning... 2 Determining Incision Location... 3 Assembling the Cannulated Awl... 4 Guide Wire Placement...
Threshold Pedicular Fixation System Surgical Technique Table of Contents Patient Preparation and Positioning... 2 Determining Incision Location... 3 Assembling the Cannulated Awl... 4 Guide Wire Placement...
ONE SYSTEM, MULTIPLE OPTIONS. Surgical Technique. Hip Knee Spine Navigation
 ONE SYSTEM, MULTIPLE OPTIONS Surgical Technique Hip Knee Spine Navigation MUST MINI Surgical Technique Hip Knee Spine Navigation INTRODUCTION The M.U.S.T. Mini posterior cervical screw system is a modular
ONE SYSTEM, MULTIPLE OPTIONS Surgical Technique Hip Knee Spine Navigation MUST MINI Surgical Technique Hip Knee Spine Navigation INTRODUCTION The M.U.S.T. Mini posterior cervical screw system is a modular
Surgical Technique. Targeter Systems Overview
 Surgical Technique Targeter Systems Overview PERI-LOC Locked Plating System Targeter Systems Overview Table of contents Product overview... 2 Introduction... 2 Indications... 2 Design features and benefits...
Surgical Technique Targeter Systems Overview PERI-LOC Locked Plating System Targeter Systems Overview Table of contents Product overview... 2 Introduction... 2 Indications... 2 Design features and benefits...
Technique Guide. C1/C2 Access System. Percutaneous transarticular screw fixation.
 Technique Guide C1/C2 Access System. Percutaneous transarticular screw fixation. C1/C2 Access System Table of Contents General introduction 2 Indications/Contraindications 2 Image intensifier-assisted
Technique Guide C1/C2 Access System. Percutaneous transarticular screw fixation. C1/C2 Access System Table of Contents General introduction 2 Indications/Contraindications 2 Image intensifier-assisted
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM
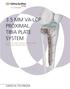 3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM Part of the DePuy Synthes Variable Angle Periarticular Plating System SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION 3.5 mm VA-LCP Proximal Tibial Plate 2 AO
3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM Part of the DePuy Synthes Variable Angle Periarticular Plating System SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION 3.5 mm VA-LCP Proximal Tibial Plate 2 AO
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
LUMBAR POSTERIOR MINIMALLY INVASIVE SYSTEM. Surgical Technique
 LUMBAR POSTERIOR MINIMALLY INVASIVE SYSTEM Surgical Technique Joint Spine Sports Med M.U.S.T. Mini Open Surgical Technique Joint Spine Sports Med CAUTION Federal law (USA) restricts this device to sale
LUMBAR POSTERIOR MINIMALLY INVASIVE SYSTEM Surgical Technique Joint Spine Sports Med M.U.S.T. Mini Open Surgical Technique Joint Spine Sports Med CAUTION Federal law (USA) restricts this device to sale
Control. Control Through VISCOSITY Control Through DELIVERY Control Through SIMPLICITY
 Control. Now that s CONFIDENCE. Control Through VISCOSITY Control Through DELIVERY Control Through SIMPLICITY Control throughviscosity Controlled Fill Cement Interdigitation Low viscosity cement Trabecular
Control. Now that s CONFIDENCE. Control Through VISCOSITY Control Through DELIVERY Control Through SIMPLICITY Control throughviscosity Controlled Fill Cement Interdigitation Low viscosity cement Trabecular
VIPER PRIME System Cadaver Time Study
 VIPER PRIME System Cadaver Time Study White Paper August 24, 2017 1. INTRODUCTION Minimally invasive surgical techniques to perform spinal stabilization have gained popularity in recent years due to the
VIPER PRIME System Cadaver Time Study White Paper August 24, 2017 1. INTRODUCTION Minimally invasive surgical techniques to perform spinal stabilization have gained popularity in recent years due to the
ACP1 CERVICAL PLATE SPINAL SYSTEM SURGICAL TECHNIQUE GUIDE II.
 I. ACP1 CERVICAL PLATE II. SPINAL SYSTEM SURGICAL TECHNIQUE GUIDE I. Introduction The Gold Standard Orthopaedics, LLC ACP1 Spinal System was designed with surgeons to incorporate strength, functionality,
I. ACP1 CERVICAL PLATE II. SPINAL SYSTEM SURGICAL TECHNIQUE GUIDE I. Introduction The Gold Standard Orthopaedics, LLC ACP1 Spinal System was designed with surgeons to incorporate strength, functionality,
Clinical Study Percutaneous Cement-Augmented Screws Fixation in the Fractures of the Aging Spine: Is It the Solution?
 BioMed Research International, Article ID 610675, 5 pages http://dx.doi.org/10.1155/2014/610675 Clinical Study Percutaneous Cement-Augmented Screws Fixation in the Fractures of the Aging Spine: Is It the
BioMed Research International, Article ID 610675, 5 pages http://dx.doi.org/10.1155/2014/610675 Clinical Study Percutaneous Cement-Augmented Screws Fixation in the Fractures of the Aging Spine: Is It the
TRANSLAMINAR FACET SCREW FIXATION
 1. Introduction: Although the new era in spine surgery is highly focused on preserving mobility, fusion is still an accepted way of treatment for a variety of spinal disorders. To stabilize the spine until
1. Introduction: Although the new era in spine surgery is highly focused on preserving mobility, fusion is still an accepted way of treatment for a variety of spinal disorders. To stabilize the spine until
TREAT SPINAL METASTASES WITH REPRODUCIBLE PRECISION
 TREAT SPINAL METASTASES WITH REPRODUCIBLE PRECISION OsteoCool RF Ablation System YOUR EXPERTISE OUR INNOVATION The OsteoCool RF Ablation System is cooled radiofrequency ablation technology. It offers simultaneous,
TREAT SPINAL METASTASES WITH REPRODUCIBLE PRECISION OsteoCool RF Ablation System YOUR EXPERTISE OUR INNOVATION The OsteoCool RF Ablation System is cooled radiofrequency ablation technology. It offers simultaneous,
CPT 2015: Prepare Your Coding Practice For New Codes As Technology Makes An Advance
 2015 Radiology Coding Survival Guide Section X : 2015 Coding Updates CPT 2015: Prepare Your Coding Practice For New Codes As Technology Makes An Advance Watch for changes in Vertebral fracture assessment,
2015 Radiology Coding Survival Guide Section X : 2015 Coding Updates CPT 2015: Prepare Your Coding Practice For New Codes As Technology Makes An Advance Watch for changes in Vertebral fracture assessment,
Three-dimensional imaging guided vertebral pedicle screw placement: accuracy analysis doi: /j.issn
 19 31 2015 07 23 Chinese Journal of Tissue Engineering Research July 23, 2015 Vol.19, No.31 ( 462000) 1 X 2 118 X X 1971 :R318 :A :2095-4344 (2015)31-04955-05 2015-06-02 http://www.crter.org 2010 12 2013
19 31 2015 07 23 Chinese Journal of Tissue Engineering Research July 23, 2015 Vol.19, No.31 ( 462000) 1 X 2 118 X X 1971 :R318 :A :2095-4344 (2015)31-04955-05 2015-06-02 http://www.crter.org 2010 12 2013
SYNEX The vertebral body replacement with ratchet mechanism
 SYNEX The vertebral body replacement with ratchet mechanism Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image
SYNEX The vertebral body replacement with ratchet mechanism Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image
Thunderbolt. surgical technique. MIS Pedicle Screw System. Where Nimble and Secure Intersect
 Thunderbolt TM MIS Pedicle Screw System Where Nimble and Secure Intersect surgical technique i www.choicespine.com System Features Dovetail set screw: Minimizes head splay and cross-threading Secure connection
Thunderbolt TM MIS Pedicle Screw System Where Nimble and Secure Intersect surgical technique i www.choicespine.com System Features Dovetail set screw: Minimizes head splay and cross-threading Secure connection
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Royal Oak Cervical Plate System
 Royal Oak Cervical Plate System Manufactured by Nexxt Spine, Inc. Royal Oak Cervical Plate System INTRODUCTION FEATURES AND BENEFITS Table of Contents SURGICAL TECHNIQUE Step 1. Patient Positioning Step
Royal Oak Cervical Plate System Manufactured by Nexxt Spine, Inc. Royal Oak Cervical Plate System INTRODUCTION FEATURES AND BENEFITS Table of Contents SURGICAL TECHNIQUE Step 1. Patient Positioning Step
5/19/2017. Interspinous Process Fixation with the Minuteman G3. What is the Minuteman G3. How Does it Work?
 Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
SYNFLATE SYSTEM SURGICAL TECHNIQUE
 SYNFLATE SYSTEM Vertebral augmentation system for the reduction of fractures and/or creation of a void in cancellous bone in the spine SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION SynFlate 2 AO Principles
SYNFLATE SYSTEM Vertebral augmentation system for the reduction of fractures and/or creation of a void in cancellous bone in the spine SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION SynFlate 2 AO Principles
Valencia Pedicle Screw Surgical Technique
 Valencia Pedicle Screw Surgical Technique VALENCIA CIRCUIT TABLE OF CONTENTS Design Rationale Indications for Use Surgical Technique 1. Pedicle Preparation 2. Screw Insertion 3. Rod Placement 4. Locking
Valencia Pedicle Screw Surgical Technique VALENCIA CIRCUIT TABLE OF CONTENTS Design Rationale Indications for Use Surgical Technique 1. Pedicle Preparation 2. Screw Insertion 3. Rod Placement 4. Locking
