Clinical Study Use of the Vascularized Iliac-Crest Flap in Musculoskeletal Lesions
|
|
|
- Dwight Washington
- 5 years ago
- Views:
Transcription
1 Hindawi Publishing Corporation BioMed Research International Volume 2013, Article ID , 6 pages Clinical Study Use of the Vascularized Iliac-Crest Flap in Musculoskeletal Lesions Cristiane Tonoli, Alexandre H. S. Bechara, Roberto Rossanez, William D. Belangero, and Bruno Livani Orthopaedic Department of HC-UNICAMP, P.O. Box 6142, Campinas, SP, Brazil Correspondence should be addressed to Cristiane Tonoli; cris tonoli@terra.com.br Received 26 April 2013; Accepted 5 September 2013 Academic Editor: Zbigniew Gugala Copyright 2013 Cristiane Tonoli et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Bone loss was in the past treated by several methods, such as bone distraction and the use of nonvascularized or tissue-bank bone grafts. With the advent of modern microsurgical techniques, the vascularized bone flap has been used with good results; it resolves local nutritional problems, repairs soft tissue that is often damaged by severe trauma, and treats bone loss due to tumors, pseudarthroses, and osteomyelitis. This paper reports the authors experience with the use of vascularized iliac-crest flaps to treat orthopedic pathologies in five patients with traumatic bone loss (<10 cm), three with osteomyelitis, and three with atrophic nonunion. In all cases, the same surgeon obtained a vascularized iliac-crest flap with a pedicle based on the deep iliac circumflex artery. All flaps consolidated within a mean period of 3 months. These findings demonstrate that the use of an iliac-crest flap is a treatment option in cases of bone loss and that it is associated with good functional results and minimal donor-site morbidity. 1. Introduction Reconstructive orthopedic surgery to treat bone loss due to severe trauma, pseudarthroses, chronic osteomyelitis, or tumors can be performed using a range of techniques, such as external or internal fixation and the use of endoprostheses or nonvascularized bone flaps [1 3]. However, these techniques do not resolve the vascularization problems that can occur in these morbid conditions. With the development ofthemicrosurgicaltechnique,thevascularizedboneflap hasproventobeagoodreconstructiveoptionbecauseit enables greater bone integration, higher consolidation rates, and better functional response [1, 4, 5]. The nonvascularized bone graft has been used with good results in cases with <6cm bone loss [2]. The vascularized fibula flap has achieved good functional results in defects >12cm [3], although some authors have reported high rates of donor-site morbidity, such as weakness (37%), flexion/extension difficulty (29 43%), flexion contractions, residual ankle pain, and fibular nerve lesions [6, 7]. In cases with intermediate amounts (5 10 cm) of bone loss, the use of the vascularized iliac-crest flap retains the benefits of a vascularized graft without incurring late donor-site morbidity [8]. Although iliac-crest flaps >12 cm have been used, they are not recommended because fractures may occur due to the stress applied to the lower limb [9]. Given the evidence of the benefits of vascularized iliac-crest flap application in cases of moderate bone loss, this flap was used to treat 11 patients with orthopedic lesions of different etiologies. 2. Patients and Methods After obtaining institutional ethics committee approval, we retrospectively identified all patients who had been treated with vascularized iliac-crest grafts between January 2009 and January The inclusion criteria were acute or chronic bone loss secondary to trauma or other bone lesions, need for graft-associated osteosynthesis, such as in cases of atrophic pseudarthrosis, or pseudarthrosis due to osteomyelitis. Exclusion criteria were prior trauma in the affected region, prior pathology, such as rheumatoid arthritis or peripheral vascular insufficiency (which could affect local vascularization and graft success), psychiatric or mental disorders, neurological damage, and institutionalization.
2 2 BioMed Research International Patient Age (years) Case 1 55 M Case 2 30 F Case 3 25 F Table 1: Clinical information. Sex Previous diagnosis Location Open fracture with bone loss in distal radius Fracture of distal radius with median nerve injury Open fracture of femur with bone loss Amount of bone loss Etiology of bone lesion (flap receptor) Left radius 6 cm Trauma Right radius 5 cm Trauma Left femur 8 cm Trauma Case 4 23 M Open fracture of foot with a lesion Right first metatarsal 6 cm Trauma and loss of soft tissue Case 5 34 M Open fracture Left femur 8 cm Trauma Case 6 09 M Case 7 66 M Case 8 24 F Case 9 56 M Case M Case F Closed fracture of forearm that developed osteomyelitis after osteosynthesis with Kirschner wires Closed fracture treated with immobilization plaster Closed forearm fracture that developed osteomyelitis after osteosynthesis with DCP Closed fracture that developed atrophic nonunion of the radius after osteosynthesis with DCP Open fracture that developed osteomyelitis and nonunion after osteosynthesis with DCP Closed fracture that developed atrophic nonunion of the radius after osteosynthesis with DCP M: male; F: female; DCP: dynamic compression plate. Left radius Right humeral diaphysis Right radius Nonunion, secondary to osteomyelitis Atrophic nonunion (conservative treatment) Nonunion, secondary to osteomyelitis Right radius Atrophic nonunion Left humerus Nonunion, secondary to osteomyelitis Right radius 5 cm Atrophic nonunion All qualifying medical charts were analyzed, and the subjects were asked to return as outpatients. Those who agreed to participate in the study were asked to provide written informed consent (legal representatives provided consent for patients <18 years of age). Medical records were examined, and radiographs were evaluated separately by two orthopedic surgeons. Both were part of the study but did not participate in the surgery and did not know the patients (blind study). Eleven patients were treated with vascularized iliac-crest flaps between January 2009 and January The etiology of bone loss (4 8 cm) was a motorcycle accident in cases 1 5(Table 1). Two patients had bone loss in the wrist (distal radius), two patients in the femur (distal femoral metaphysis), and one patient in the foot (first metatarsal). One patient (case 11) had bone loss in the left radius secondary to atrophic nonunion of a fracture treated with osteosynthesis and a dynamic compression plate (DCP). The other cases had no bone loss but atrophic nonunion of the right humerus (case 7) or right radius (case 9) or nonunion secondary to osteomyelitis with a history of previous osteosynthesis in the left forearm (case 6), the right forearm (case 8), or the left humerus (case 10)(Table 1). All surgeries were performed by a single experienced surgeon according to the technique described in the literature [9 11]. Each patient was placed in the supine position with the donor site raised. A skin incision was made from the location of the anterior superior iliac spine toward that of the inguinal ligament. The pedicle was based on the deep iliac circumflex artery, which emerges from the external oblique muscle adjacent to the superior border of the iliac crest. The oblique external and internal muscles were freed, and the pedicle was found between the transverse and oblique internal muscles. It was then dissected along the inguinal ligament to the external iliac artery, where the pedicle originates 2 cm above the ligament [12]. The deep iliac circumflex artery may originate from the femoral artery (42.2% of cases) or from the external iliac artery below (40.6%) or above (17.2%) the inguinal ligament [11]. The external diameter of the artery is 1 5 mm at its origin, and the distance to the anterior superior iliac spine is 6 27 (mean: 15.8 ± 5.6) mm. The receptor site was then prepared, the flap was removed byosteotomywithasaw,andthearterialpediclewasremoved after ensuring that it was sufficiently large (4 6 cm) to enable anastomosis [12]. After hemostasis, the donor site was sutured.
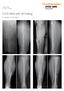
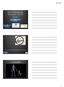
3 BioMed Research International 3 Figure 1: Case 4 soft-tissue loss. At the anastomosis site, 2000 units of heparin were administered intravenously. No heparin was used postoperatively, but oral acetyl salicylic acid (100 mg) was prescribed for 30 days. Osteosynthesis was performed at the receptor site using DCPsandscrewsorKirschnerwires(case4). Continuity of the medullar canal was reestablished in all cases. Consolidation was verified clinically and radiologically. Clinical criteria included absence of pain, lack of mobility at the fracture site, and return to daily activities (work and leisure). The radiological criteria included absence of implant failure (signs of loosening or breakage), signs of graft incorporation andbonefracturehealing,continuityofthetrabecularbone through the bone fragments and graft, presence of bone callus,andpresenceofatleastthreeoutoffourcorticesin the anteroposterior and lateral radiographs [13]. 3. Results All flaps consolidated within a mean period of 3 months. Soft tissue and musculature adjacent to the iliac crest, which shared an arterial supply with the flap, were transferred with the graft in case 4 (Figure1). The distal perfusion deficit (Figure 2) was recovered by the same procedure with good results (Figures 3 and 4). In case 6, consolidation occurred rapidly (within 4 weeks) because the patient was a child, but a purulent fistula persisted, necessitating a second procedure to remove the plate and provide local debridement. In many of the cases reported here, the iliac-crest flap was used to treat lesions that were due to high-energy trauma; this flap was also used to treat other serious fractures and nerve or vascular lesions, including traumatic amputations (case 10,four fingers)and late amputations(case 8, right leg amputation after vascular graft failure) (Table 2). Thefollow-upperiodrangedfrom7to36months.All patients reported postoperative pain at the donor site, which Figure 2: Case 4 reduced perfusion. Figure 3: Case 4 final radiograph of consolidated bone graft. was intense in the first postsurgical days but disappeared after 4 weeks. Common analgesics were used to relieve pain. Late morbidity (contour irregularity of the basin) occurred in case Discussion Several traditionally used bone reconstruction techniques yield limited results when bone loss is associated with disruption of the local blood supply. This complex situation is commonly encountered in cases of high-energy trauma, chronic osteomyelitis, pseudarthrosis, and tumor resection, and the only feasible solution is often amputation. The use of a vascularized bone graft resolves issues related to bone nutrition and permits simultaneous soft-tissue reconstruction [14, 15].
4 4 BioMed Research International Patient Consolidation time (months) Follow-up period (months) Complications Table 2: Casuistry. Type of synthesis Duration of postoperative pain at donor site (days) Associated lesions Case plates 5 Case plates 8 Median nerve lesion (trauma) Case plates 9 Closed femoral neck fracture and open femoral and tibial diaphysis fractures (all ipsilateral) Case Kirschner Medial malleolus fracture 10 wires (ipsilateral) Closed tibial plateau fracture Case plates 14 (ipsilateral) and closed right distal radius and forearm fractures Case Persistent infection requiring second 1plate 8 procedure Case plate 10 Case plate 15 Right sacroiliac joint lesion, left ischiopubic branch fracture, right femur and tibia open fractures, popliteal artery vascular injury and vascular graft failure after 2 days requiring leg amputation Case Third semitubular 21 plate Case LCP 21 Brachial plexus injury (ipsilateral) + traumatic amputation of fingers 2 5 Case DCP(radius) Contour + third irregularity of semitubular basin plate (ulna) 30 LCP: locking compression plate; DCP: dynamic compression plate. Figure 4: Case 4 final clinical result. The advantages of the vascularized bone flap over the conventional bone graft are better osseointegration, higher consolidation rates, and improved functional response [1, 4, 5].Hence,incasesofseverebonelossorinsituationsinwhich other procedures have yielded poor results, the vascularized bone flap is a better option than the nonvascularized graft because it provides more tissue viability, in terms of vascular nutrition, during the bone healing process. Due to this improved local blood supply, bone production, and intrinsic stability, the vascularized flap has demonstrated faster bone consolidation and a better functional outcome [1, 3, 5, 13, 14, 16]. The vascularized iliac-crest flap is superior to the fibula flap for the treatment of small defects because its size enables better adaptation and because donor-site morbidities, such as ankle rigidity or instability and fibular nerve lesions, can be prevented [17, 18]. The selection of the best donor site and the choice of a vascularized or conventional bone graft are multifactorial processes that must take into account not only the defect size, but also the compatibility between donor site and receptor regions, structural features of the graft (cortical, spongy, or osteomuscular), mechanical demands of the defect site, duration of the procedure, and donor-site morbidity. Therefore, even in cases with <6cmofboneloss,thevascularized bone graft is often the best option, especially for defects
5 BioMed Research International 5 in the extremities (hands and feet) that demand greater mechanical freedom and precision of movement. In a study ofanklearthritisduetomassivebonelosssecondaryto tumors,osteomyelitis,andtrauma,bishopetal.[6]reported that iliac-crest flaps were appropriate for defects <4cm.The vascularized iliac-crest flap has also been used successfully for reconstruction of the maxilla and mandible (97%) [9], distal radius [12], and carpals [19] and for the treatment of ankle instability [20]. The vascularized fibular flap has shown good results in the treatment of defects with 26 cm bone loss [15]. The complication rates are low (11.5%) [7]andincludecontracture of hallux flexion (4.3%), ankle pain (4.1%), weakness (0.6%), and fibular nerve lesions (1.7%). Only a small percentage (13%) of patients with weakness and ankle instability (37%) [6] demonstrated weakness during a physical examination. Other complications include ankle stiffness, cellulitis, suture dehiscence [17, 18], and ankle valgus deformity [15, 21]. Rogers et al. [22] found no significant difference in donorsite morbidity between vascularized iliac-crest and fibula flaps. Although the removal of the iliac vascular graft is a more complicated procedure than the removal of the nonvascularized tricortical graft, the potential complications atthedonorsitearealmostthesame:hematoma,infection, postoperative pain, lesion of the lateral femoral cutaneous nerve, and the Trendelenburg gait. However, when bone loss is more than 6.0 cm, other options of vascularized bone grafts such as the scapula and fibula also present potential morbidity at the donorsite [22 24]. It is possible to use the iliac-crest flap in gaps from 6 cm to 10 cm and up to 12 cm. For greater bone loss, the vascularized fibula should be considered. Moreover, fibular graft is a strut graft therefore more resistent, but iliac graft as a cancelous bone graft has a higher healing potential than fibular strut graft [9]. The vascularized iliac-crest flap requires practice in microsurgical techniques as it is a complex procedure and is onlyindicatedincaseswherebonelossismorethan5to6cm. However, the results obtained using nonvascularized grafts in these conditions are not as good [4, 8, 25]. Although postoperative pain was the main donor-site morbidity in the present study, others have reported cellulitis (3.6%), deep vein thrombosis (3.6%), and femoral nerve neuropraxia (4.8%) as early complications. The main late complications reported are changes in anterolateral thigh sensitivity (27%), contour irregularity of the basin (20%), and hernias (9.7%) [23, 24]. The vascularized iliac-crest flap is an option for the treatment of bone loss, especially in small bones. Its advantages include a long pedicle (4 6 cm) and large diameter, which facilitate anastomosis [9]. Moreover, in cases of concomitant soft-tissue loss and perfusion deficit, this flap enables the transfer of muscle and skin covering the iliac crest because these tissues are supplied by the same artery (case 4,Figures 1 and 2).Thisoptionisalsousefulincasesofseverenonunion in which a conventional graft has failed. Furthermore, in cases of anastomosis failure, the iliac crest functions better than a long bone as a conventional graft due to its corticocancellous component. The limitations of this study include its retrospective design and small sample size. The cases presented is heterogeneous because bone loss in orthopedic traumatology cases is relatively rare and so are the indications for the use of the vascularized flap. The recipient bed must have a rich vascular supply, which in some cases of severe trauma and/or osteomyelitis/pseudarthrosis is not possible due to thepresenceofvascularinjurysecondarytotheseillnesses. Therefore, it is difficult to find similar bone-loss cases with an indication for a vascularized flap. Moreover, most of the patients are cases of high-energy trauma, a variable population depending on the circumstances of the trauma [8, 9]. Cases of bone loss are relatively rare and most often are severe cases with multiple fractures resulting from trauma, nonunion, or difficult-to-treat osteomyelitis. Therefore, the number is small as they are cases of major morbidity. However, in the case of locomotor trauma, the series reported using the vascularized iliac-crest flap is not small when compared to the literature [8, 20]. This flap is mostly used in head [22], neck, and maxillofacial surgery [9, 17]. Becausesometraumaticlesionsweretreateddirectlywith the vascularized bone graft, comparison with other types of treatment was not possible. However, the findings indicate that the vascularized iliac-crest flap is a reliable and safe treatment option that yields good results and is associated with minimal donor-site morbidity in cases of bone and muscle loss secondary to trauma and osteomyelitis. Acknowledgment This work was supported by (São Paulo State Research Foundation)FAPESP, SP, São Paulo, Brazil. References [1] V. M. Goldberg, J. W. Shaffer, G. Field, and D. T. Davy, Biology of vascularized bone grafts, Orthopedic Clinics of North America,vol.18,no.2,pp ,1987. [2] C. G. Finkemeier, Bone-grafting and bone-graft substitutes, JournalofBoneandJointSurgeryA,vol.84,no.3,pp , [3] A. R. Gazdag, J. M. Lane, D. Glaser, and R. A. Forster, Alternatives to autogenous bone graft: efficacy and indications, Journal of the American Academy of Orthopaedic Surgeons,vol. 3, no. 1, pp. 1 8, [4]J.W.Shaffer,D.T.Davy,G.A.Field,J.S.Bensusan,and G. J. Kellis, The superiority of vascularized compared to nonvascularized rib grafts in spine surgery shown by biological andphysicalmethods, Spine, vol. 13, no. 10, pp , [5]C.B.CuttingandJ.G.McCarthy, Comparisonofresidual osseous mass between vascularized and nonvascularized onlay bone transfers, Plastic and Reconstructive Surgery, vol. 72, no. 5,pp ,1983. [6] A.T.Bishop,M.B.Wood,andK.K.Sheetz, Arthrodesisofthe ankle with a free vascularized autogenous bone graft. Reconstruction of segmental loss of bone secondary to osteomyelitis, tumor, or trauma, The Journal of Bone & Joint Surgery, vol.77, no.12,pp ,1995. [7] T. R. Gaskill, J. R. Urbaniak, and J. M. Aldridge III, Free vascularized fibular transfer for femoral head osteonecrosis:
6 6 BioMed Research International donor and graft site morbidity, Journal of Bone and Joint Surgery A,vol.91,no.8,pp ,2009. [8] R. Legré, P. Samson, F. Tomei, and J. L. Jouve, Treatment of substance loss of the bones of the leg in traumatology by transfer of the free vascularized iliac crest. Aprospos of 13 cases, Revue dechirurgieorthopediqueetreparatricedel AppareilMoteur s, vol.84,no.3,pp ,1998. [9] G. I. Taylor, The current status of free vascularized bone grafts, Clinics in Plastic Surgery,vol.10,no.1,pp ,1983. [10] D. Martin, V. Pistre, V. Pinsolle, P. Pelissier, and J. Baudet, The iliac crest. Perspective on a donor site of exceptional free flaps, 20 years after its initial description, Annales de Chirurgie Plastique et Esthetique,vol.45,no.3,pp ,2000. [11] G. K. Huang, Z. Z. Liu, Y. L. Shen, R. Q. Hu, H. Miao, and Z. Y. Yin, Microvascularfreetransferofiliacbonebasedonthedeep circumflex iliac vessels, Journal of Microsurgery,vol.2,no.2,pp , [12] L. Pic Gomis and R. Gomis, Vascularized iliac crest and distal radius reconstruction, Chirurgie de la Main, vol. 29, supplement 1, pp. S49 S58, [13] M. Henry, Genicular corticoperiosteal flap salvage of resistant atrophic non-union of the distal radius metaphysis, Hand Surgery,vol.12,no.3,pp ,2007. [14] K.N.Malizos,Z.H.Dailiana,M.Innocenti,C.L.Mathoulin, R. Mattar Jr., and M. Sauerbier, Vascularized bone grafts for upper limb reconstruction: defects at the distal radius, wrist, and hand, Journal of Hand Surgery,vol.35,no.10,pp , [15]A.V.Korompilias,N.K.Paschos,M.G.Lykissas,I.Kostas- Agnantis,M.D.Vekris,andA.E.Beris, Recentupdatesof surgical techniques and applications of free vascularized fibular graft in extremity and trunk reconstruction, Microsurgery,vol. 31,no.3,pp ,2011. [16] S. Kakar, A. Duymaz, S. Steinmann, A. Y. Shin, and S. L. Moran, Vascularized medial femoral condyle corticoperiosteal flaps for the treatment of recalcitrant humeral nonunions, Microsurgery, vol. 31, no. 2, pp , [17]J.P.Anthony,J.D.Rawnsley,P.Benhaim,E.F.Ritter,S.H. Sadowsky, and M. I. Singer, Donor leg morbidity and function after fibula free flap mandible reconstruction, Plastic and Reconstructive Surgery,vol.96,no.1,pp ,1995. [18] P. J. Meagher and W. A. Morrison, Free fibula flap donor-site morbidity: case report and review of the literature, Journal of Reconstructive Microsurgery,vol.18,no.6,pp ,2002. [19] C. Harpf, M. Gabl, C. Reinhart et al., Small free vascularized iliac crest bone grafts in reconstruction of the scaphoid bone: a retrospective study in 60 cases, Plastic and Reconstructive Surgery,vol.108,no.3,pp ,2001. [20] U. M. Rieger, M. Haug, F. Schwarzl, D. F. Kalbermatten, B. Hintermann, and G. Pierer, Free microvascular iliac crest flap for extensive talar necrosis case report with a 16-year longterm follow up, Microsurgery, vol. 29, no. 8, pp , [21]K.Kanaya,T.Wada,H.Kura,T.Yamashita,M.Usui,andS. Ishii, Valgus deformity of the ankle following harvesting of a vascularized fibular graft in children, Journal of Reconstructive Microsurgery,vol.18,no.2,pp.91 96,2002. [22] S.N.Rogers,S.R.Lakshmiah,B.Narayanetal., Acomparison of the long-term morbidity following deep circumflex iliac and fibula free flaps for reconstruction following head and neck cancer, Plastic and Reconstructive Surgery, vol. 112, no. 6, pp , [23] C. Forrest, B. Boyd, R. Manktelow, R. Zuker, and V. Bowen, The free vascularised iliac crest tissue transfer: donor site complications associated with eighty-two cases, British Journal of Plastic Surgery,vol.45,no.2,pp.89 93,1992. [24] L. T. Kurz, S. R. Garfin, and R. E. Booth Jr., Harvesting autogenous iliac bone grafts. A review of complications and techniques, Spine,vol.14,no.12,pp ,1989. [25] R. Sanders and B. J. Mayou, A new vascularized bone graft transferred by microvascular anastomosis as a free flap, British Journal of Surgery,vol.66,no.11,pp ,1979.
Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle
 Acta Orthop. Belg., 2009, 75, 611-615 ORIGINAL STUDY Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle Luc DE SMET From the University
Acta Orthop. Belg., 2009, 75, 611-615 ORIGINAL STUDY Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle Luc DE SMET From the University
Fibula bone grafting in infected gap non union: A prospective case series
 2019; 3(1): 06-10 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2019; 3(1): 06-10 Received: 03-11-2018 Accepted: 06-12-2018 Dr. Mohammed Nazim M.S (Ortho),
2019; 3(1): 06-10 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2019; 3(1): 06-10 Received: 03-11-2018 Accepted: 06-12-2018 Dr. Mohammed Nazim M.S (Ortho),
The ipsilateral and contralateral fibulae have been
 Ipsilateral vascularised fibular transport for massive defects of the tibia R. M. Atkins, P. Madhavan, J. Sudhakar, D. Whitwell From the Bristol Royal Infirmary, Bristol, England The ipsilateral and contralateral
Ipsilateral vascularised fibular transport for massive defects of the tibia R. M. Atkins, P. Madhavan, J. Sudhakar, D. Whitwell From the Bristol Royal Infirmary, Bristol, England The ipsilateral and contralateral
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
4/28/2010. Fractures. Normal Bone and Normal Ossification Bone Terms. Epiphysis Epiphyseal Plate (physis) Metaphysis
 Fractures Normal Bone and Normal Ossification Bone Terms Epiphysis Epiphyseal Plate (physis) Metaphysis Diaphysis 1 Fracture Classifications A. Longitudinal B. Transverse C. Oblique D. Spiral E. Incomplete
Fractures Normal Bone and Normal Ossification Bone Terms Epiphysis Epiphyseal Plate (physis) Metaphysis Diaphysis 1 Fracture Classifications A. Longitudinal B. Transverse C. Oblique D. Spiral E. Incomplete
Management of Brachial Plexus & Peripheral Nerves Blast Injuries. First Global Conflict Medicine Congress
 Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Femoral reconstruction by single, folded or double free vascularised fibular grafts
 The British Association of Plastic Surgeons (2004) 57, 550 555 Femoral reconstruction by single, folded or double free vascularised fibular grafts K. Muramatsu*, K. Ihara, M. Shigetomi, S. Kawai Department
The British Association of Plastic Surgeons (2004) 57, 550 555 Femoral reconstruction by single, folded or double free vascularised fibular grafts K. Muramatsu*, K. Ihara, M. Shigetomi, S. Kawai Department
CASE REPORT. Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur
 PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture Dislocation of the Elbow in an Adult
 Hindawi Case Reports in Orthopedics Volume 2018, Article ID 5401634, 6 pages https://doi.org/10.1155/2018/5401634 Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture
Hindawi Case Reports in Orthopedics Volume 2018, Article ID 5401634, 6 pages https://doi.org/10.1155/2018/5401634 Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture
Is Distraction Histiogenesis a Reliable Method to Reconstruct Segmental Bone and Acquired Leg Length Discrepancy in Tibia Fractures and Non Unions?
 Is Distraction Histiogenesis a Reliable Method to Reconstruct Segmental Bone and Acquired Leg Length Discrepancy in Tibia Fractures and Non Unions? James J Hutson Jr MD Professor Orthopedic Trauma Ryder
Is Distraction Histiogenesis a Reliable Method to Reconstruct Segmental Bone and Acquired Leg Length Discrepancy in Tibia Fractures and Non Unions? James J Hutson Jr MD Professor Orthopedic Trauma Ryder
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
The earlier clinic experience of the reverse-flow anterolateral thigh island flap
 British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
Case Report Bilateral Distal Femoral Nailing in a Rare Symmetrical Periprosthetic Knee Fracture
 Case Reports in Orthopedics, Article ID 745083, 4 pages http://dx.doi.org/10.1155/2014/745083 Case Report Bilateral Distal Femoral Nailing in a Rare Symmetrical Periprosthetic Knee Fracture Marcos Carvalho,
Case Reports in Orthopedics, Article ID 745083, 4 pages http://dx.doi.org/10.1155/2014/745083 Case Report Bilateral Distal Femoral Nailing in a Rare Symmetrical Periprosthetic Knee Fracture Marcos Carvalho,
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
The study of distal ¼ diaphyseal extra articular fractures of humerus treated with antegrade intramedullary interlocking nailing
 2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
Case Report Pediatric Transepiphyseal Seperation and Dislocation of the Femoral Head
 Case Reports in Orthopedics Volume 2013, Article ID 703850, 4 pages http://dx.doi.org/10.1155/2013/703850 Case Report Pediatric Transepiphyseal Seperation and Dislocation of the Femoral Head Mehmet Elmadag,
Case Reports in Orthopedics Volume 2013, Article ID 703850, 4 pages http://dx.doi.org/10.1155/2013/703850 Case Report Pediatric Transepiphyseal Seperation and Dislocation of the Femoral Head Mehmet Elmadag,
The Open Orthopaedics Journal
 Send Orders for Reprints to reprints@benthamscience.ae 704 The Open Orthopaedics Journal, 2017, 11, (Suppl-4, M11) 704-713 The Open Orthopaedics Journal Content list available at: www.benthamopen.com/toorthj/
Send Orders for Reprints to reprints@benthamscience.ae 704 The Open Orthopaedics Journal, 2017, 11, (Suppl-4, M11) 704-713 The Open Orthopaedics Journal Content list available at: www.benthamopen.com/toorthj/
USE OF THE IPSILATERAL VASCULARISED FIBULA FOR
 USE OF THE IPSILATERAL VASCULARISED FIBULA FOR TIBIAL RECONSTRUCTION R. HERTEL, M. PISAN, R. P. JAKOB From the University of Berne, Switzerland Between 1989 and 1994 we used a vascularised ipsilateral
USE OF THE IPSILATERAL VASCULARISED FIBULA FOR TIBIAL RECONSTRUCTION R. HERTEL, M. PISAN, R. P. JAKOB From the University of Berne, Switzerland Between 1989 and 1994 we used a vascularised ipsilateral
Functional outcome of open reduction and internal fixation of clavicle fracture
 International Journal of Research in Medical Sciences Pillai MG. Int J Res Med Sci. 2016 Aug;4(8):3205-3210 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162255
International Journal of Research in Medical Sciences Pillai MG. Int J Res Med Sci. 2016 Aug;4(8):3205-3210 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162255
Case Report Correction of Length Discrepancy of Radius and Ulna with Distraction Osteogenesis: Three Cases
 Hindawi Publishing Corporation Case Reports in Orthopedics Volume 2015, Article ID 656542, 6 pages http://dx.doi.org/10.1155/2015/656542 Case Report Correction of Length Discrepancy of Radius and Ulna
Hindawi Publishing Corporation Case Reports in Orthopedics Volume 2015, Article ID 656542, 6 pages http://dx.doi.org/10.1155/2015/656542 Case Report Correction of Length Discrepancy of Radius and Ulna
Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report by
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report by
Ipsilateral Fibular Transport Using Ilizarov Taylor Spatial Frame for a Limb Salvage Reconstruction: a Case Report
 DOI 10.1007/s11420-008-9102-7 CASE REPORT Ipsilateral Fibular Transport Using Ilizarov Taylor Spatial Frame for a Limb Salvage Reconstruction: a Case Report Raheel Shafi, MD& Austin T. Fragomen, MD & S.
DOI 10.1007/s11420-008-9102-7 CASE REPORT Ipsilateral Fibular Transport Using Ilizarov Taylor Spatial Frame for a Limb Salvage Reconstruction: a Case Report Raheel Shafi, MD& Austin T. Fragomen, MD & S.
KNEE DISLOCATION. The most common injury will be an anterior dislocation, and this usually results from a hyperextension mechanism.
 KNEE DISLOCATION Introduction Dislocation of the knee is a severe injury associated with major soft tissue injury and a high incidence of damage to the popliteal artery. There is displacement of the tibia
KNEE DISLOCATION Introduction Dislocation of the knee is a severe injury associated with major soft tissue injury and a high incidence of damage to the popliteal artery. There is displacement of the tibia
EVOS MINI with IM Nailing
 Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Surgical interventions in chronic osteomyelitis
 Kathmandu University Medical Journal (2005) Vol. 3, No. 1, Issue 9, 50-54 Surgical interventions in chronic osteomyelitis Shrestha BK 1, Rajbhandary T 2, Bijukachhe B 2, Banskota AK 3 1 Associate Professor,
Kathmandu University Medical Journal (2005) Vol. 3, No. 1, Issue 9, 50-54 Surgical interventions in chronic osteomyelitis Shrestha BK 1, Rajbhandary T 2, Bijukachhe B 2, Banskota AK 3 1 Associate Professor,
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints
 Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints ABSTRACT Chronically infected open knee joints present dif cult problem. Aggressive debridement of chronically infected soft tissue
Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints ABSTRACT Chronically infected open knee joints present dif cult problem. Aggressive debridement of chronically infected soft tissue
Clinical Study Masquelet Technique for Treatment of Posttraumatic Bone Defects
 Hindawi Publishing Corporation e Scientific World Journal Volume 2014, Article ID 710302, 5 pages http://dx.doi.org/10.1155/2014/710302 Clinical Study Masquelet Technique for Treatment of Posttraumatic
Hindawi Publishing Corporation e Scientific World Journal Volume 2014, Article ID 710302, 5 pages http://dx.doi.org/10.1155/2014/710302 Clinical Study Masquelet Technique for Treatment of Posttraumatic
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion
 CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
Osteosynthesis involving a joint Thomas P Rüedi
 Osteosynthesis involving a joint Thomas P Rüedi How to use this handout? The left column contains the information given during the lecture. The column at the right gives you space to make personal notes.
Osteosynthesis involving a joint Thomas P Rüedi How to use this handout? The left column contains the information given during the lecture. The column at the right gives you space to make personal notes.
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
HAND & MICROSURGERY PROCEDURE A ( RM RM 4800 ) PROCEDURE B ( RM RM 4400 ) PROCEDURE C ( RM RM 3600 )
 HAND & MICROSURGERY PROCEDURE A ( RM 4401 - RM 4800 ) 1 Brachial plexus Exploration with nerve graft 2 Brachial plexus Exploration with neurotisation 3 Brachial plexus Free functioning muscle transfer
HAND & MICROSURGERY PROCEDURE A ( RM 4401 - RM 4800 ) 1 Brachial plexus Exploration with nerve graft 2 Brachial plexus Exploration with neurotisation 3 Brachial plexus Free functioning muscle transfer
The gastrocnemius with soleus bi-muscle flap
 The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
Surgical treatment of aseptic nonunion in long bones: review of 193 cases
 J Orthopaed Traumatol (2007) 8:11 15 DOI 10.1007/s10195-007-0155-z ORIGINAL A. Megaro S. Marchesi U.E. Pazzaglia Surgical treatment of aseptic nonunion in long bones: review of 193 cases Received: 5 September
J Orthopaed Traumatol (2007) 8:11 15 DOI 10.1007/s10195-007-0155-z ORIGINAL A. Megaro S. Marchesi U.E. Pazzaglia Surgical treatment of aseptic nonunion in long bones: review of 193 cases Received: 5 September
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
Reintroducing the latissimus-rib free flap as a long bone substitute in the reconstruction of lower extremity injuries
 Case report Medical Journal of the Islamic Republic of Iran.Vol. 22, No. 2, August 2008. pp.104-110 Reintroducing the latissimus-rib free flap as a long bone substitute in the reconstruction of lower extremity
Case report Medical Journal of the Islamic Republic of Iran.Vol. 22, No. 2, August 2008. pp.104-110 Reintroducing the latissimus-rib free flap as a long bone substitute in the reconstruction of lower extremity
Free vascularized fibular graft for tibial pseudarthrosis in neurofibromatosis
 Acta Orthop Scand 1988;59(4):425-429 Free vascularized fibular graft for tibial pseudarthrosis in neurofibromatosis 03 17878 1 luli lrl Herman H. de Boer', Abraham J. Verbout', Hans K. L. Nielsen2 and
Acta Orthop Scand 1988;59(4):425-429 Free vascularized fibular graft for tibial pseudarthrosis in neurofibromatosis 03 17878 1 luli lrl Herman H. de Boer', Abraham J. Verbout', Hans K. L. Nielsen2 and
3.5 mm LCP Distal Tibia T-Plates
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Distal Tibia T-Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Distal Tibia T-Plates 2 AO Principles 4 Indications
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Distal Tibia T-Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Distal Tibia T-Plates 2 AO Principles 4 Indications
7/23/2018 DESCRIBING THE FRACTURE. Pattern Open vs closed Location BASIC PRINCIPLES OF FRACTURE MANAGEMENT. Anjan R. Shah MD July 21, 2018.
 BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
The Flower Medial Column Fusion Plate
 The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
PRONATION-ABDUCTION FRACTURES
 C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
Index. orthopedic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acetabular fractures thromboembolic disease after, 341 Achilles tendon rupture ACL. See Anterior cruciate ligament (ACL) Adolescent idiopathic
Index Note: Page numbers of article titles are in boldface type. A Acetabular fractures thromboembolic disease after, 341 Achilles tendon rupture ACL. See Anterior cruciate ligament (ACL) Adolescent idiopathic
TIPMED EXTERNAL FIXATION SYSTEMS
 TIPMED EXTERNAL FIXATION SYSTEMS ANATOMICAL LOCATIONS FOR EXTERNAL FIXATION SYSTEMS Humeral Dynamic Axial Fixator Elbow Fixator Pelvic Dynamic Axial Fixator Pennig Wrist Fixator Hand Fixator Finger Fixator
TIPMED EXTERNAL FIXATION SYSTEMS ANATOMICAL LOCATIONS FOR EXTERNAL FIXATION SYSTEMS Humeral Dynamic Axial Fixator Elbow Fixator Pelvic Dynamic Axial Fixator Pennig Wrist Fixator Hand Fixator Finger Fixator
EXPERT TIBIAL NAIL PROTECT
 EXPERT TIBIAL NAIL PROTECT Enhance your first line of defense This publication is not intended for distribution in the USA. CLINICAL EVIDENCE CONTENT AUTHOR TITLE OF CHAPTER PAGE ETN PROtect clinical evidence
EXPERT TIBIAL NAIL PROTECT Enhance your first line of defense This publication is not intended for distribution in the USA. CLINICAL EVIDENCE CONTENT AUTHOR TITLE OF CHAPTER PAGE ETN PROtect clinical evidence
Choice of spacer material for HTO! P. Landreau, MD Chief of Surgery Aspetar, Orthopaedic and Sports Medicine Hospital Doha, Qatar
 Choice of spacer material for HTO! P. Landreau, MD Chief of Surgery Aspetar, Orthopaedic and Sports Medicine Hospital Doha, Qatar High Tibial Osteotomy: HTO! Valgisation HTO Intended to transfer the mechanical
Choice of spacer material for HTO! P. Landreau, MD Chief of Surgery Aspetar, Orthopaedic and Sports Medicine Hospital Doha, Qatar High Tibial Osteotomy: HTO! Valgisation HTO Intended to transfer the mechanical
Infected forearm nonunion treated by bone transport after debridement
 Liu et al. BMC Musculoskeletal Disorders 2013, 14:273 RESEARCH ARTICLE Open Access Infected forearm nonunion treated by bone transport after debridement Tang Liu 1, Zhenyang Liu 2,3, Lin Ling 1* and Xiangsheng
Liu et al. BMC Musculoskeletal Disorders 2013, 14:273 RESEARCH ARTICLE Open Access Infected forearm nonunion treated by bone transport after debridement Tang Liu 1, Zhenyang Liu 2,3, Lin Ling 1* and Xiangsheng
Radiographic Positioning Summary (Basic Projections RAD 222)
 Lower Extremity Radiographic Positioning Summary (Basic Projections RAD 222) AP Pelvis AP Hip (Unilateral) (L or R) AP Femur Mid and distal AP Knee Lateral Knee Pt lies supine on table Align MSP to Center
Lower Extremity Radiographic Positioning Summary (Basic Projections RAD 222) AP Pelvis AP Hip (Unilateral) (L or R) AP Femur Mid and distal AP Knee Lateral Knee Pt lies supine on table Align MSP to Center
Fractures and dislocations around elbow in adult
 Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Title: An intramedullary free vascularized fibular graft combined with pasteurized
 Title: An intramedullary free vascularized fibular graft combined with pasteurized autologous bone graft in leg reconstruction for patients with osteosarcoma Names of authors Masataka Noguchi, Hiroo Mizobuchi,
Title: An intramedullary free vascularized fibular graft combined with pasteurized autologous bone graft in leg reconstruction for patients with osteosarcoma Names of authors Masataka Noguchi, Hiroo Mizobuchi,
ROTATIONAL PILON FRACTURES
 CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
Which treatment? How I do a Maquet Osteotomy? Maquet: Maquet: Biomechanics. Maquet: /21/10. Philippe Landreau, MD
 Which treatment? How I do a Maquet Osteotomy? Philippe Landreau, MD Paris, France And if the patient is young?! Anterior displacement of the tibial tuberosity design to reduce the joint reactive force
Which treatment? How I do a Maquet Osteotomy? Philippe Landreau, MD Paris, France And if the patient is young?! Anterior displacement of the tibial tuberosity design to reduce the joint reactive force
Carpal rows injuries!
 Carpal rows injuries! Michael Papaloïzos! Center for Hand Surgery and Therapy Geneva, Switzerland no conflict of interest to declare Fractures of carpal bones! The fractured scaphoid! Fracture-dislocations
Carpal rows injuries! Michael Papaloïzos! Center for Hand Surgery and Therapy Geneva, Switzerland no conflict of interest to declare Fractures of carpal bones! The fractured scaphoid! Fracture-dislocations
Baris Beytullah Koc, 1 Martijn Schotanus, 1 Bob Jong, 2 and Pieter Tilman Introduction. 2. Case Presentation
 Case Reports in Orthopedics Volume 2016, Article ID 7898090, 4 pages http://dx.doi.org/10.1155/2016/7898090 Case Report The Role of Dynamic Contrast-Enhanced MRI in a Child with Sport-Induced Avascular
Case Reports in Orthopedics Volume 2016, Article ID 7898090, 4 pages http://dx.doi.org/10.1155/2016/7898090 Case Report The Role of Dynamic Contrast-Enhanced MRI in a Child with Sport-Induced Avascular
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abscess, epidural, 822 824 Achilles tendon rupture, 894 895, 981 982 Acromioclavicular separations, shoulder pain in, 751 753 Adhesive capsulitis,
Note: Page numbers of article titles are in boldface type. A Abscess, epidural, 822 824 Achilles tendon rupture, 894 895, 981 982 Acromioclavicular separations, shoulder pain in, 751 753 Adhesive capsulitis,
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage
 Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Case Report Use of Nonvascularized Autologous Fibular Strut Graft in the Treatment of Major Bone Defect after Periprosthetic Knee Fracture
 Hindawi Case Reports in Orthopedics Volume 2017, Article ID 1650194, 5 pages https://doi.org/10.1155/2017/1650194 Case Report Use of Nonvascularized Autologous Fibular Strut Graft in the Treatment of Major
Hindawi Case Reports in Orthopedics Volume 2017, Article ID 1650194, 5 pages https://doi.org/10.1155/2017/1650194 Case Report Use of Nonvascularized Autologous Fibular Strut Graft in the Treatment of Major
Orthopedic Trauma. I have nothing to disclose. Objectives 3/7/2018. What is Orthopedic Trauma? What is Orthopedic Trauma? Trauma
 Orthopedic Trauma I have nothing to disclose. David Miller Memorial Trauma Symposium 2017 James Black, MD Mercy Orthopedic Trauma - Springfield 10/27/2017 Objectives What is Orthopedic Trauma? What is
Orthopedic Trauma I have nothing to disclose. David Miller Memorial Trauma Symposium 2017 James Black, MD Mercy Orthopedic Trauma - Springfield 10/27/2017 Objectives What is Orthopedic Trauma? What is
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Hand Microsurgery. A reliable option for lower extremity complex defect reconstructions: Two case reports with free osteocutaneous radial forearm flap
 Hand Microsurgery & Case Report Hand Microsurg 2017;6:51-55 doi:10.5455/handmicrosurg.219016 A reliable option for lower extremity complex defect reconstructions: Two case reports with free osteocutaneous
Hand Microsurgery & Case Report Hand Microsurg 2017;6:51-55 doi:10.5455/handmicrosurg.219016 A reliable option for lower extremity complex defect reconstructions: Two case reports with free osteocutaneous
Basic Radiographic Principles Part II
 Basic Radiographic Principles Part II Kristopher Avant, D.O. October 19 th, 2016 I have no disclosures relevant to the material presented in this discussion. Good Stuff!!! 1 Really? Really! Musculoskeletal
Basic Radiographic Principles Part II Kristopher Avant, D.O. October 19 th, 2016 I have no disclosures relevant to the material presented in this discussion. Good Stuff!!! 1 Really? Really! Musculoskeletal
OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3
 OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3 HOW TO CITE THIS ARTICLE: Karan Mehta, Prashanth G. Shiblee Siddiqui,
OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3 HOW TO CITE THIS ARTICLE: Karan Mehta, Prashanth G. Shiblee Siddiqui,
Solitary Bone Cyst of the Lunate: A Case Report
 Cronicon OPEN ACCESS ORTHOPAEDICS Case Report Solitary Bone Cyst of the Lunate: A Case Report MihirDesai* and Shivanand Bandekar Department of Orthopedics, Goa Medical College, Goa, India *Corresponding
Cronicon OPEN ACCESS ORTHOPAEDICS Case Report Solitary Bone Cyst of the Lunate: A Case Report MihirDesai* and Shivanand Bandekar Department of Orthopedics, Goa Medical College, Goa, India *Corresponding
Debate: I Do Bone Transport. Disclosures. Bone Defects 5/10/2017
 Debate: I Do Bone Transport David W. Lowenberg, M.D. Clinical Pressor Department Orthopaedic Surgery Stanford University School Medicine Disclosures Board Directors: Foundation for Orthopaedic Trauma (FOT)
Debate: I Do Bone Transport David W. Lowenberg, M.D. Clinical Pressor Department Orthopaedic Surgery Stanford University School Medicine Disclosures Board Directors: Foundation for Orthopaedic Trauma (FOT)
PEM GUIDE CHILDHOOD FRACTURES
 PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
Wrist Joint Reconstruction With a Vascularized Fibula Free Flap Following Giant Cell Tumor Excision in the Distal Radius
 Wrist Joint Reconstruction With a Vascularized Fibula Free Flap Following Giant Cell Tumor Excision in the Distal Radius Chester J. Mays, BS, a Kyle Ver Steeg, MD, a Saeed Chowdhry, MD, b David Seligson,
Wrist Joint Reconstruction With a Vascularized Fibula Free Flap Following Giant Cell Tumor Excision in the Distal Radius Chester J. Mays, BS, a Kyle Ver Steeg, MD, a Saeed Chowdhry, MD, b David Seligson,
Distal tibial fractures are a poorly recognised complication with fibula free flaps
 CASE-BASED REVIEW Ann R Coll Surg Engl 2015; 97: 409 413 doi 10.1308/003588415X14181254790086 Distal tibial fractures are a poorly recognised complication with fibula free flaps A Durst, J Clibbon, B Davis
CASE-BASED REVIEW Ann R Coll Surg Engl 2015; 97: 409 413 doi 10.1308/003588415X14181254790086 Distal tibial fractures are a poorly recognised complication with fibula free flaps A Durst, J Clibbon, B Davis
Compartment Syndrome
 Compartment Syndrome Chapter 34 Compartment Syndrome Introduction Compartment syndrome may occur with an injury to any fascial compartment. The fascial defect caused by the injury may not be adequate to
Compartment Syndrome Chapter 34 Compartment Syndrome Introduction Compartment syndrome may occur with an injury to any fascial compartment. The fascial defect caused by the injury may not be adequate to
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Index. B Backslap technique depth assessment, 82, 83 diaphysis distal trocar, 82 83
 Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Kanji Mori, Kazuya Nishizawa, Akira Nakamura, and Shinji Imai. 1. Introduction. 2. Case Presentation
 Case Reports in Orthopedics Volume 2015, Article ID 301858, 4 pages http://dx.doi.org/10.1155/2015/301858 Case Report Atraumatic Occult Odontoid Fracture in Patients with Osteoporosis-Associated Thoracic
Case Reports in Orthopedics Volume 2015, Article ID 301858, 4 pages http://dx.doi.org/10.1155/2015/301858 Case Report Atraumatic Occult Odontoid Fracture in Patients with Osteoporosis-Associated Thoracic
Nonunion of the Femur Treated with Conventional Osteosynthesis Combined with Autogenous and Strut Allogeneic Bone Grafts
 Original Article 268 Nonunion of the Femur Treated with Conventional Osteosynthesis Combined with Autogenous and Strut Allogeneic Bone Grafts Lin-Hsiu Weng, MD; Jun-Wen Wang, MD Background: In this study,
Original Article 268 Nonunion of the Femur Treated with Conventional Osteosynthesis Combined with Autogenous and Strut Allogeneic Bone Grafts Lin-Hsiu Weng, MD; Jun-Wen Wang, MD Background: In this study,
Posteromedial approach to the distal humerus for fracture fixation
 Acta Orthop. Belg., 2006, 72, 395-399 ORIGINAL STUDY Posteromedial approach to the distal humerus for fracture fixation Cédric LAPORTE, Maurice THIONGO, Dominique JEGOU From the General Hospital of Meaux,
Acta Orthop. Belg., 2006, 72, 395-399 ORIGINAL STUDY Posteromedial approach to the distal humerus for fracture fixation Cédric LAPORTE, Maurice THIONGO, Dominique JEGOU From the General Hospital of Meaux,
Case Report Surgical Treatment of Posttraumatic Radioulnar Synostosis
 Case Reports in Orthopedics Volume 2016, Article ID 5956304, 4 pages http://dx.doi.org/10.1155/2016/5956304 Case Report Surgical Treatment of Posttraumatic Radioulnar Synostosis S. Pfanner, P. Bigazzi,
Case Reports in Orthopedics Volume 2016, Article ID 5956304, 4 pages http://dx.doi.org/10.1155/2016/5956304 Case Report Surgical Treatment of Posttraumatic Radioulnar Synostosis S. Pfanner, P. Bigazzi,
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System.
 LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
Management of a large post-traumatic skin and bone defect using an Ilizarov frame
 Acta Orthop. Belg., 2006, 72, 214-218 TECHNICAL NOTE Management of a large post-traumatic skin and bone defect using an Ilizarov frame Pieter D HOOGHE, Koen DEFOORT, Johan LAMMENS, Jos STUYCK From the
Acta Orthop. Belg., 2006, 72, 214-218 TECHNICAL NOTE Management of a large post-traumatic skin and bone defect using an Ilizarov frame Pieter D HOOGHE, Koen DEFOORT, Johan LAMMENS, Jos STUYCK From the
Gross Anatomy Coloring Book Series. Lower Extremity Arteries
 Gross Anatomy Coloring Book Series Lower Extremity Arteries 1 Femoral Artery and Associated Branches For the life of the flesh is in the blood. Leviticus 17:11 Femoral Artery and Associated Branches After
Gross Anatomy Coloring Book Series Lower Extremity Arteries 1 Femoral Artery and Associated Branches For the life of the flesh is in the blood. Leviticus 17:11 Femoral Artery and Associated Branches After
Tibial deformity correction by Ilizarov method
 International Journal of Research in Orthopaedics http://www.ijoro.org Case Report DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180422 Tibial deformity correction by Ilizarov method Robert
International Journal of Research in Orthopaedics http://www.ijoro.org Case Report DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180422 Tibial deformity correction by Ilizarov method Robert
Al Hess MD NERVE REPAIR
 Al Hess MD NERVE REPAIR Historical Aspects 300 BC Hippocrates, description of nervous system 200 AD Galen of Pergamon, nerve injury, questioned possibility of regeneration 600 AD Paul of Arginia, first
Al Hess MD NERVE REPAIR Historical Aspects 300 BC Hippocrates, description of nervous system 200 AD Galen of Pergamon, nerve injury, questioned possibility of regeneration 600 AD Paul of Arginia, first
Orthopedics in Motion Tristan Hartzell, MD January 27, 2016
 Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
Isolated congenital anterolateral bowing of the fibula : A case report with 24 years follow-up
 Acta Orthop. Belg., 2009, 75, 842-846 CASE REPORT Isolated congenital anterolateral bowing of the fibula : A case report with 24 years follow-up Karolien LELIEFELD, Hans VAN DER SLUIJS, Ibo VAN DER HAVEN
Acta Orthop. Belg., 2009, 75, 842-846 CASE REPORT Isolated congenital anterolateral bowing of the fibula : A case report with 24 years follow-up Karolien LELIEFELD, Hans VAN DER SLUIJS, Ibo VAN DER HAVEN
Knee Disarticulation Amputation
 Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
A comparative study of locking plate by MIPO versus closed interlocking intramedullary nail in extraarticular distal tibia fractures
 2018; 4(3): 145-149 ISSN: 2395-1958 IJOS 2018; 4(3): 145-149 2018 IJOS www.orthopaper.com Received: 26-05-2018 Accepted: 27-06-2018 Kanachur Institute of Medical Sciences Mangalore University Road, Natekal,
2018; 4(3): 145-149 ISSN: 2395-1958 IJOS 2018; 4(3): 145-149 2018 IJOS www.orthopaper.com Received: 26-05-2018 Accepted: 27-06-2018 Kanachur Institute of Medical Sciences Mangalore University Road, Natekal,
Original Research Article
 TREATMENT OF COMPLEX TIBIAL FRACTURES TYPES V AND VI OF SCHATZKER CLASSIFICATION BY DOUBLE PLATE FIXATION WITH SINGLE ANTERIOR INCISION Thoguluva Chandra Sekaran Prem Kumar 1, M. N. Karthi 2 1Senior Assistant
TREATMENT OF COMPLEX TIBIAL FRACTURES TYPES V AND VI OF SCHATZKER CLASSIFICATION BY DOUBLE PLATE FIXATION WITH SINGLE ANTERIOR INCISION Thoguluva Chandra Sekaran Prem Kumar 1, M. N. Karthi 2 1Senior Assistant
Musculoskeletal System
 Musculoskeletal System CPT CPT copyright 2011 American Medical Association. All rights reserved. Fee schedules, relative value units, conversion factors and/or related components are not assigned by the
Musculoskeletal System CPT CPT copyright 2011 American Medical Association. All rights reserved. Fee schedules, relative value units, conversion factors and/or related components are not assigned by the
Definition of anatomy 1 Questions 5
 Contents Chapter 1: Introduction 1 5 Definition of anatomy 1 Questions 5 Chapter 2: Skeletal System 6 74 Skeleton 6 Skeletal system 8 Bones of superior extremity 12 Articulated skeleton of hand 17 Clinical
Contents Chapter 1: Introduction 1 5 Definition of anatomy 1 Questions 5 Chapter 2: Skeletal System 6 74 Skeleton 6 Skeletal system 8 Bones of superior extremity 12 Articulated skeleton of hand 17 Clinical
Vasu Pai FRACS, MCh, MS, Nat Board Ortho Surgeon Gisborne
 Vasu Pai FRACS, MCh, MS, Nat Board Ortho Surgeon Gisborne FRACTURE MANAGEMENT I Simple closed fracture : Complete or Incomplete Stable or unstable II Open fracture III Multiple fracture IV Polytrauma Fractures
Vasu Pai FRACS, MCh, MS, Nat Board Ortho Surgeon Gisborne FRACTURE MANAGEMENT I Simple closed fracture : Complete or Incomplete Stable or unstable II Open fracture III Multiple fracture IV Polytrauma Fractures
Trauma surgeons insight: Speed, Cars, Crashes, The Recovery
 Trauma surgeons insight: Speed, Cars, Crashes, The Recovery Moderator Jerome Carslake NRSPP Manager ARRB Group P: +61 3 9881 1670 E: jerome.carslake@arrb.com.au Housekeeping Webinar is = 45 mins Question
Trauma surgeons insight: Speed, Cars, Crashes, The Recovery Moderator Jerome Carslake NRSPP Manager ARRB Group P: +61 3 9881 1670 E: jerome.carslake@arrb.com.au Housekeeping Webinar is = 45 mins Question
ARMS. Reconstruction of Large Femur and Tibia Defect with Free Vascularized Fibula Graft and Locking Plate INTRODUCTION.
 Original Article ARMS Archieves of Reconstructive Microsurgery pissn 2383-5257 eissn 2288-6184 Arch Reconstr Microsurg 2015;24(2):68-74 http://dx.doi.org/10.15596/arms.2015.24.2.68 Reconstruction of Large
Original Article ARMS Archieves of Reconstructive Microsurgery pissn 2383-5257 eissn 2288-6184 Arch Reconstr Microsurg 2015;24(2):68-74 http://dx.doi.org/10.15596/arms.2015.24.2.68 Reconstruction of Large
Trauma fixation choices chart your fracture
 Trauma fixation choices chart your fracture This brochure is intended for informational and educational purposes only. It is the responsibility of operating physicians to determine and utilize the appropriate
Trauma fixation choices chart your fracture This brochure is intended for informational and educational purposes only. It is the responsibility of operating physicians to determine and utilize the appropriate
Treatment of open diaphyseal fractures of long bones of the limbs. Biology and Medicine
 eissn: 09748369 Treatment of open diaphyseal fractures of long bones of the limbs Biology and Medicine Research Article Volume 7, Issue 1, Article ID: BM-065-15, 2015 Indexed by Scopus (Elsevier) www.biolmedonline.com
eissn: 09748369 Treatment of open diaphyseal fractures of long bones of the limbs Biology and Medicine Research Article Volume 7, Issue 1, Article ID: BM-065-15, 2015 Indexed by Scopus (Elsevier) www.biolmedonline.com
Functional anatomy and variability of the blood vessels of the upper and lower limbs. Anastasia Bendelic Human Anatomy Departament
 Functional anatomy and variability of the blood vessels of the upper and lower limbs Anastasia Bendelic Human Anatomy Departament Plan: 1. Variations of the branching pattern of the aortic arch 2. Arterial
Functional anatomy and variability of the blood vessels of the upper and lower limbs Anastasia Bendelic Human Anatomy Departament Plan: 1. Variations of the branching pattern of the aortic arch 2. Arterial
New 2010 CPT Codes (italic font represents a new or revised code/description)
 New 2010 CPT Codes (italic font represents a new or revised code/description) 14301 Adjacent tissue transfer or rearrangement, any area; defect 30.1 sq cm to 60.0 sq cm 14302 each additional 30.0 sq cm,
New 2010 CPT Codes (italic font represents a new or revised code/description) 14301 Adjacent tissue transfer or rearrangement, any area; defect 30.1 sq cm to 60.0 sq cm 14302 each additional 30.0 sq cm,
TIBIAXYS ANKLE FUSION
 TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
Radial Head Fractures Save or Replace?
 Radial Head Fractures Save or Replace? Current Solutions in Orthopedic Trauma Sepember 19, 2015 Jorge L. Orbay MD. Disclosure Skeletal Dynamics Elbow Joint Ulno-Humeral and Radio-Capitellar The key joint
Radial Head Fractures Save or Replace? Current Solutions in Orthopedic Trauma Sepember 19, 2015 Jorge L. Orbay MD. Disclosure Skeletal Dynamics Elbow Joint Ulno-Humeral and Radio-Capitellar The key joint
Arthroscopy Of the Ankle.
 Arthroscopy Of the Ankle www.fisiokinesiterapia.biz Ankle Arthroscopy Anatomy Patient setup Portal placement Procedures Complications Anatomy Portals Anterior Anteromedial Anterolateral Anterocentral Posterior
Arthroscopy Of the Ankle www.fisiokinesiterapia.biz Ankle Arthroscopy Anatomy Patient setup Portal placement Procedures Complications Anatomy Portals Anterior Anteromedial Anterolateral Anterocentral Posterior
MEDIAL EPICONDYLE FRACTURES
 MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
Case Report The Utility and Limitations of the Transfibular Approach in Ankle Trauma Surgery
 Case Reports in Orthopedics, Article ID 234369, 4 pages http://dx.doi.org/10.1155/2014/234369 Case Report The Utility and Limitations of the Transfibular Approach in Ankle Trauma Surgery Mustafa Yassin,
Case Reports in Orthopedics, Article ID 234369, 4 pages http://dx.doi.org/10.1155/2014/234369 Case Report The Utility and Limitations of the Transfibular Approach in Ankle Trauma Surgery Mustafa Yassin,
