Pulsion Intubation Versus Traction Intubation for Obstructing Carcinomas of the Esophagus
|
|
|
- Martina Brooks
- 6 years ago
- Views:
Transcription
1 Pulsion Intubation Versus Traction Intubation for Obstructing Carcinomas of the Esophagus Helmut W. Unruh, M.D., F.R.C.S.(C), and K. Michael Pagliero, M.B.B.S., F.R.C.S. ABSTRACT Eighty-eight patients were intubated to relieve the dysphagia of malignant esophageal obstruction. Because of advanced metastatic disease or poor general condition, 49 patients could not be operated on and were intubated endoscopically. Under radiographic control, the Nottingham Introducer was used to position Atkinson or modified Celestin tubes. In 39 other patients, palliative resection could not be done or liver metastasis was found at preliminary exploration with a view to esophagectomy. In these patients, Celestin tubes were inserted by the traction technique. The pulsion intubation group was older than the traction intubation group but comparable in other respects. Hospital stay was significantly shorter for the pulsion intubation group (8.4 versus 18.6 days). Hospital mortality rates were comparable (14.3% in the pulsion intubation group versus 23.1% in the traction intubation group), and survival did not differ (93 days in the pulsion intubation group versus 137 days in the traction intubation group). Overall complication rates were similar, but there were two significant differences: (I) wound infection or dehiscence was a major problem in the traction intubation group, occurring in 23% of the patients; and (2) tube obstruction or displacement occurred more frequently in the pulsion intubation group (18.3% versus 5.1%) but did not constitute a serious problem. Perforation occurred in 4 patients (8.2%) in the pulsion intubation group but was fatal in only 1. Pulsion intubation offers distinct advantages over traction intubation in that hospital stay is decreased and morbidity reduced. Palliation of dysphagia due to malignant obstruction of the esophagus is often required. Methods of palliation include resection, bypass, radiotherapy, dilation, and intubation. Intubation can be achieved by the traction or the pulsion method. Traction intubation requires laparotomy with gastrotomy. Pulsion intubation is achieved endoscopically under radiographic control. We compared the two methods of intubation with regard to hospital stay, early and late mortality, survival times, and complications. From the Department of Surgery, The University of Manitoba Health Sciences Centre. Winnipeg, Man, Canada, and the Thoracic Surgery Unit, Royal Devon and Exeter Hospital (Wonford), Exeter, England. Accepted for publication Jan 17, Address reprint requests to Mr. Pagliero, Thoracic Surgery Unit, Royal Devon and Exeter Hospital (Wonford), Barrack Rd, Exeter EX2 5DW. England. Material and Methods Between the years of 1977 and 1983, 88 patients with malignant esophageal obstruction were treated with esophageal intubation. In each instance, a direct attack on the tumor itself by resection, bypass, or radiotherapy had been ruled out and intubation was employed merely to palliate severe dysphagia and combat associated malaise and weight loss. Diagnosis was established in all patients by prior fiberoptic endoscopy and biopsy. Staging of the disease was accomplished by physical examination and biochemical investigation including liver function tests which, when abnormal, were followed up with radionuclide liver scan, ultrasonic liver scan, or computed axial tomography. In general, localized tumors of the esophagus were treated with resection. In a few instances in which the patient was elderly or there was an associated medical condition that precluded operation, or to satisfy the patient's wishes, the tumor was treated with radical radiotherapy primarily. The group of patients under discussion in this article includes those who were thought to be unsuitable for either method of treatment by virtue of their general condition or the presence of distant metastases. These 88 patients fell into two distinct groups. The first group included 49 patients in whom the factors that determined need for palliative esophageal intubation were obvious without laparotomy. Palliation was achieved in these patients with pulsion intubation with the aid of fiberoptic endoscopy. The second group consisted of 39 patients in whom clinical assessment had suggested that the primary tumor would be resectable. Subsequent laparotomy, however, had shown that advanced local or metastatic disease had made palliative resection impossible or futile. Therefore, these patients were palliated with traction intubation during laparotomy using Celestin tubes (11 (Fig l).* Pulsion intubation is performed under general anesthesia and radiographic control. After the tumor is viewed with the endoscope, a stainless steel guidewire is passed through the narrowed lumen into the stomach, where its position is confirmed by fluoroscopic examination. A 45F bougie is then passed over the guidewire to dilate the obstruction. The endoscope is reintroduced to visualize the lower extent of the tumor so that an Atkinsont [2] or Celestin tube of appropriate length can be selected. The Atkinson tube (Fig 2) is made of latex rub- 'Celestin tubes:medoc (Glos) Ltd, PO Box 1, Tetbury, Gloucester CU) 8TL. England. 'Key Med Inc., 400 Airport Executive Park, Spring Valley, NY lw
2 338 The Annals of Thoracic Surgery Vol 40 No 4 October 1985 Fig 2. Atkinson tube. Fig 1. Traction Celestin tube. ber with a ridge at its lower end that discourages upward dislocation after insertion. The collecting funnel is fairly stiff at its narrow end to discourage passage through the tumor but is progressively softer toward its rim so that it molds gently with the contours of the esophagus without any tendency for pressure necrosis. Alternatively, a Celestin pulsion tube may be used (Fig 3). It is similar to that used for traction intubation but tries to overcome the disadvantage of not being sutured in place by the addition of a flange at its lower end. Eighteen Celestin flanged latex rubber tubes and 31 Atkinson silicon rubber tubes were used. Both tubes had similar cross-sectional diameters (Celestin tubes: external diameter, 16 mm, internal diameter, 12 mm; Atkinson tubes: external diameter, 16 mm, internal diameter, 11 mm). The tube is mounted on the Nottingham Introducer so that the nose cone of the Introducer just protrudes from its lower end. The plastic nose cone (Fig 4A) is made to expand by advancing a conical metal olive so that it grips the tube firmly from within. The Nottingham Introducer apparatus* consists of an inner rod to which the plastic nose cone is attached and an outer tube to which the Key Med Inc., 400 Airport Executive Park, Spring Valley, NY Fig 3. Pulsion Celestin tube.
3 339 Unruh and Pagliero: Pulsion Versus Traction Intubation A B Fig 4. Nottingham Introducer. (A) The apparatus consists of an inner rod to which a plastic nose cone is attached and an outer tube to which a metal olive is attached. (6) Mechanism at the proximal end of the device enables advancing or retarding the olive. metal olive is attached. The metal olive can be advanced and retarded by the mechanism shown in Figure 4B at the proximal end. After the Atkinson tube is mounted on the Nottingham Introducer, a plastic ramrod is passed over the proximal end of the apparatus so that its end comes to lie within the cup of the Atkinson tube. The whole apparatus is then passed over the guidewire (Fig 5) until the tube is positioned appropriately within the lumen of the malignant tumor as determined by roentgenographic control. When the cup of the tube is sited immediately above the tumor, the nose cone is relaxed and the Introducer is withdrawn, maintaining the position of the tube with the ramrod. Once this is achieved, the ramrod and guidewire are removed. Finally, the satisfactory position is confirmed by repeating the endoscopy to ensure that the funnel is above the tumor and that the lower end is distal to the site of obstruction. Postoperatively, the head of each patient s bed was slightly elevated. A liquid diet was begun after recovery from anesthesia; this was rapidly increased to a regular diet. The patients were all instructed to chew their food Fig 5. Insertion of tube by the pulsion method.
4 340 The Annals of Thoracic Surgery Vol 40 No 4 October 1985 well and to drink adequate liquids to avoid bolus obstruction of the tube. They were also advised that severe symptomatic reflux of gastric contents was likely to occur, especially if the gastroesophageal junction had been traversed. They were therefore instructed to sleep with the head of the bed elevated and to avoid eating before going to bed. If required, antacids were prescribed for symptomatic relief. The second group of 39 patients all underwent laparotomy as a prelude to esophagectomy, and the extent of intraabdominal disease was carefully assessed. Lymph node involvement with metastatic carcinoma was not considered an absolute contraindication to palliative resection. Thus, all 39 patients had either liver metastasis or localized extensive tumor infiltration that precluded resection, and were therefore candidates for surgical palliation by traction intubation. A small high anterior gastrotomy was performed and a pilot bougie was passed from the mouth through the narrowed lumen of the tumor into the stomach. In a few patients, this proved impossible and it was necessary to pass a fine gumelastic bougie through the malignant stricture from below by means of the anterior gastrotomy; the elastic bougie was then used to guide the pilot bougie downward. A Celestin tube [l] (external diameter, 14 mm; internal diameter, 11 mm) was positioned by the traction technique and secured to the anterior gastric wall by a single suture tied over a small piece of felt. The gastrotomy was closed in standard fashion. The correct position of the tube was confirmed by fiberoptic endoscopy. After the return of bowel sounds, the postoperative management was similar to that described for the endoscopically inserted tubes. Table 1. Patient Data Variable No. of patients Age (yr) Sex Male Female Diagnosis Squamous cell carcinoma Adenocarcinoma Other Hospital stay (d) Hospital mortality Days until hospital mortality No. of deaths within 2 weeks of discharge Survival excluding early deaths 'Significance: p < hsignificance: p < Pulsion Intubation Group (14.3%) Traction lntubation Group " I 18.6b 9 (23.1%) Results The patient data are summarized in Table 1. The two groups were comparable with regard to size, sex ratio, and diagnosis. The patients in the pulsion intubation group were significantly older, however. This is explained by the selection process for the study, whereby the very elderly and individuals in poor general condition constituted a major part of the pulsion group. Hospital stay was significantly longer for the patients having traction intubation (18.6 days versus 8.4 days in the pulsion group) but hospital mortality, death within 2 weeks of discharge from the hospital, and survival in days were not significantly different. Among the 37 patients with pulsion intubation and the 30 with traction intubation who survived beyond the first 2 weeks after discharge, the average survival was 93 and 137 days, respectively. From Figure 6 it is apparent that in fact all but 1 patient had died within 12 months. The complications of both types of intubation are presented in Table 2. The total number of complications do not differ significantly between the two groups. Perforation recognized at the time of intubation or subsequently by the development of surgical emphysema occurred in 4 patients having pulsion intubation and was fatal in 1. One fatal perforation occurred in the traction intubation f 40- t- rn w m I- a io- W &--,.---*---, I Fig 6. The percentage of patients surviving is plotted against months of intubation. All patients having pulsion intubation died by 8 months, and only 1 patient having traction intubation survived longer than 12 months. group, but total perforation rates were not significantly different. The incidences of inability to intubate, development of aspiration pneumonia, and no symptomatic improvement were similar for both groups. Bolus obstruction of the tube required readmission to the hospital for bougienage, while tube displacement required repositioning or removal of the tube. The incidence of bolus obstruction was similar in both groups, but tube displacement occurred more frequently in the pulsion intubation group.
5 341 Unruh and Pagliero: Pulsion Versus Traction Intubation TaOle 2. Complications of lntubafiona Pulsion Traction lntubation lntubation Group Group Complication (N = 49) (N = 39) Perforation 4 (8.2) 1 (2.6) Nonfatal 3 0 Fatal 1 1 Failed insertion 3 (6.1) 1 (2.6) Wound-related problems Infection 0 7 (17.9)' Dehiscence 0 2 (5.1) Aspiration pneumonia 3 (6.1) 1 (2.6) Tube bolus obstruction 3 (6.1) 2 (5.1) Tube displacement 6 (12.2)b 0 No symptomatic improvement 2 (4.1) 1 (2.6) Overall complication rate 21 (42.9) 15 (38.5) "Values in parentheses are percentages hsignificance: p < 'Significance: 1' < There were 7 wound infections and 2 wound disruptions in the traction intubation group. Thus, the incidence of wound complications was 23%. More than 60% of patients with carcinoma of the esophagus will prove to have inoperable disease, and only 18% will survive one year 131. Nevertheless, palliation of the distressing symptom of dysphagia is often required. Resection gives the best palliation for dysphagia but may not be appropriate in a certain proportion of patients for reasons of poor general condition, advanced metastasis, or extensive local infiltration. Radiotherapy is effective in relieving dysphagia in only half the patients after a 4- to 6-week course of treatment and is often only temporary 141. Chemotherapy has no role in relieving dysphagia. Retrosternal gastric bypass for unresectable carcinomas [5] was compared with pulsion intubation by Angorn and Haffejee [6]. They found bypass to have a higher complication rate and significantly more postoperative catabolism. Therefore, bypass was not favored since the life expectancy of these patients is often very limited. Simple dilation may be the only procedure tolerated by a very sick patient, but symptomatic relief is unpredictable and often limited [7, 81. All of our patients had malignant esophageal obstruction with severe dysphagia requiring palliation. Eightyone patients had primary carcinoma of the esophagus or cardia, and the other 7 had obstruction due to other malignancies. In 4 of these patients, obstruction was caused by breast carcinoma metastatic to periesophageal lymph nodes. The other 3 cases of obstruction were due to bronchial carcinoma that had involved the esophagus by direct infiltration. One of the 3 patients had a malignant tracheoesophageal fistula that was successfully controlled by traction intubation, and the patient went on to survive 9 months. The patients having pulsion intubation were significantly older than those having traction intubation. This reflects the selection process in that the very elderly and more infirm were chosen for the pulsion group in addition to those with preoperatively proven hepatic metastases. Despite this, hospital mortality figures were similar. There were 5 deaths within 2 weeks of discharge from the hospital among the patients having pulsion intubation compared with none in those having traction intubation. This does not, however, constitute a statistically significant difference, and is also most likely a reflection of the selection process. The survival times of the patients who lived beyond 2 weeks after discharge did not differ significantly despite the older age and poorer general condition of those intubated endoscopically. However, the duration of stay in the hospital was significantly shorter for the patients having pulsion intubation. This not only has important implications with regard to hospital costs but is also vitally important in view of the limited life expectancy for these patients. Failure to insert a tube at endoscopy is due to inability to pass the guidewire through the tumor, which occurred in 3 patients. In 1 patient undergoing traction intubation, it proved impossible to negotiate the stricture with a bougie. The results of esophageal intubation are very rewarding. Only 2 patients having pulsion intubation and 1 patient having traction intubation thought there was no symptomatic improvement despite patent tubes. Bolus obstruction by food is a relatively infrequent problem and can usually be resolved if the patient drinks aerated fluids. If hospital admission is necessary, the first procedure is to pass a nasogastric tube. Failing this, endoscopy is required (91. Should the tube become displaced, its removal and replacement is a simple matter [lo]. The guidewire is passed through the tube, and the Introducer is positioned in the tube with radiographic assistance. Once secure, the tube can be removed, resited, or replaced. The perforation rate with endoscopic intubation was 8.2%. This is comparable with that currently reported for Britain (111 and other parts of Europe [12]. Perforation is not synonymous with disaster. Often this problem manifests itself only as a slight amount of surgical emphysema, as it did in 3 of 4 of our patients with pulsion intubation, and is manageable with conservative measures because the tube usually bypasses the breach in the esophageal wall. Wound infection or dehiscence occurred in 23% of the patients having traction intubation. Such complications undoubtedly contributed to the longer hospital stay of these patients and are therefore a major disadvantage of this treatment. In addition, Angorn [ 131 demonstrated rapid improvement in nutritional status following endoscopic intubation. One would expect improvement to be much delayed after a major surgical procedure. Many patients experienced some degree of symptomatic reflux, but this was manageable by conservative measures, including antacids, and no patient required hospital readmission for this reason alone. However, the
6 342 The Annals of Thoracic Surgery Vol 40 No 4 October cases of aspiration pneumonia were caused by reflux. It is also likely that reflux was at least partially contributory in some, if not all, of the 3 patients who failed to achieve symptomatic improvement with intubation, since obstruction of the tubes was not noted at endos- COPY. Palliative intubation is highly effective in relieving the dysphagia of malignant esophageal obstruction. Because the endoscopically placed tube is not sutured distally to the stomach as is the surgically positioned tube, tube displacement occurs more frequently with pulsion intubation but does not pose major problems for the patient [9, 101. A high incidence of wound infection and dehiscence and a delay in nutritional status improvement (131 detract from the benefits of traction intubation. In addition, the hospital stay for patients having pulsion intubation is shorter, with hospital mortality and subsequent survival comparable to those for traction intubation. Therefore, we advocate pulsion intubation as an effective method for palliation in selected patients with inoperable disease. There will continue to be a group of patients in whom laparotomy is essential for staging and, thus, a continued need for traction intubation. Our results, however, indicate strongly that when a decision to intubate has been made before operation, the procedure should be accomplished by the pulsion method rather than by traction. References 1. Celestin LR: Permanent intubation in inoperable cancer of the esophagus and cardia. Ann R Coll Surg Engl 25:165, Atkinson M, Ferguson R, Parker GC: Tube introducer and modified Celestin tube for use in palliative intubation of oesophagogastric neoplasm at fibreoptic endoscopy. Gut 19:669, Earlam R, Cunha-Melo JR: Oesophageal squamous carcinoma: I. A critical review of surgery. Br J Surg 67381, Wilson SE, Plested WG, Carey JS: Esophagogastrectomy versus radiation therapy for midesophageal carcinoma. Ann Thorac Surg 10:195, Orringer MB, Sloan H: Substernal gastric bypass of the excluded thoracic esophagus for the palliation of esophageal carcinoma. J Thorac Cardiovasc Surg , Angorn IB, Haffejee AA: Pulsion intubation v. retrosternal gastric bypass for palliation of unresectable carcinoma of the upper thoracic esophagus. Br J Surg 70335, Belsey RHR: Palliative management of esophageal carcinoma. Ann Surg 139:789, Heit HA, Johnson LF, Siege1 SR, Boyce HW: Palliative dilatation for dysphagia in esophageal carcinoma. Ann Intern Med 89:629, Earlam R, Cunha-Melo JR Malignant esophageal strictures: a review of techniques for palliative intubation. Br J Surg 69:61, Ogilvie AL, Dronfield MW, Ferguson R, Atkinson M: Palliative intubation of the oesophagogastric neoplasms at fibreoptic endoscopy. Gut 23:1060, Bennett JR Intubation of gastro-oesophageal malignancies: a survey of current practice in Britain, Gut 22:336, Tytgat GN: Endoscopic methods of treatment of gastrointestinal and biliary stenosis. Endoscopy 1980 [Suppl], pp Angorn IB. Intubation in the treatment of carcinoma of the esophagus. World J Surg 5:535, 1981
Palliative intubation of oesophagogastric neoplasms at fibreoptic endoscopy
 Gut, 1982, 23, 1060-1067 Palliative intubation of oesophagogastric neoplasms at fibreoptic endoscopy A L OGILVIE,* M W DRONFIELD,t R FERGUSON,t and M ATKINSON From the University Hospital, Queen's Medical
Gut, 1982, 23, 1060-1067 Palliative intubation of oesophagogastric neoplasms at fibreoptic endoscopy A L OGILVIE,* M W DRONFIELD,t R FERGUSON,t and M ATKINSON From the University Hospital, Queen's Medical
Is a Metallic Stent Useful for Non Resectable Esophageal Cancer?
 Original Article Is a Metallic Stent Useful for Non Resectable Esophageal Cancer? Shinsuke Wada, MD, 1 Tsuyoshi Noguchi, MD, 1 Shinsuke Takeno, MD, 1 Hatsuo Moriyama, MD, 1 Tsuyoshi Hashimoto, MD, 1 Yuzo
Original Article Is a Metallic Stent Useful for Non Resectable Esophageal Cancer? Shinsuke Wada, MD, 1 Tsuyoshi Noguchi, MD, 1 Shinsuke Takeno, MD, 1 Hatsuo Moriyama, MD, 1 Tsuyoshi Hashimoto, MD, 1 Yuzo
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse
 The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction
 The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
Stenting for Esophageal Cancer Technical Issues and Outcomes
 Stenting for Esophageal Cancer Technical Issues and Outcomes Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Disclosures Research and Educational
Stenting for Esophageal Cancer Technical Issues and Outcomes Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Disclosures Research and Educational
The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control
 ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
Owen Dickinson. Consultant in Endoscopy & Interventional Radiology. Upper GI Stenting. Rotherham Foundation Trust
 Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Prospective randomised trial of laser therapy only and laser therapy followed by endoscopic intubation for the palliation of malignant dysphagia
 252 Gut, 1990, 31, 252-258 ALIMENTARY TRACT The Gastrointestinal Unit, Walton Hospital, Liverpool H Barr N Krasner A Raouf R J Walker Correspondence to: Dr N Krasner, The Gastrointestinal Unit, Walton
252 Gut, 1990, 31, 252-258 ALIMENTARY TRACT The Gastrointestinal Unit, Walton Hospital, Liverpool H Barr N Krasner A Raouf R J Walker Correspondence to: Dr N Krasner, The Gastrointestinal Unit, Walton
Combined Collis-Nissen Reconstruction. of the esophagogastric junction at. Mark B. Orringer, M.D., and Herbert Sloan, M.D.
 Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
WallFlex Stents Technique Spotlights
 WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
101 Oesophageal cancers: a surgeon uses radiotherapy
 Annals of the Royal College of Surgeons of England (199) vol. 72, 32-4 11 Oesophageal cancers: a surgeon uses radiotherapy R J Earlam MChir FRCS Consultant Surgeon The London Hospital, Whitechapel, London
Annals of the Royal College of Surgeons of England (199) vol. 72, 32-4 11 Oesophageal cancers: a surgeon uses radiotherapy R J Earlam MChir FRCS Consultant Surgeon The London Hospital, Whitechapel, London
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: What is the treatment
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: What is the treatment
Esophageal Stents May Interfere with the Swallowing Reflex: An Illustrative Case History
 254 Journal of Pain and Symptom Management Vol. 16 No. 4 October 1998 Original Article Esophageal Stents May Interfere with the Swallowing Reflex: An Illustrative Case History Angel Lee, MRCP (UK), and
254 Journal of Pain and Symptom Management Vol. 16 No. 4 October 1998 Original Article Esophageal Stents May Interfere with the Swallowing Reflex: An Illustrative Case History Angel Lee, MRCP (UK), and
Endoscopic Palliation of Malignant Dysphagia
 Endoscopic Palliation of Malignant Dysphagia 1. Scope of the guideline This guidance has been produced to support endoscopic palliation of malignant dysphagia from oesophageal cancer. 2. Guideline background
Endoscopic Palliation of Malignant Dysphagia 1. Scope of the guideline This guidance has been produced to support endoscopic palliation of malignant dysphagia from oesophageal cancer. 2. Guideline background
Expandable stents in digestive pathology present use in an emergency hospital
 ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
by intubation Carcinoma of the oesophagus in Transkei: treatment
 Thorax 1989;44:42-47 Carcinoma of the oesophagus in Transkei: treatment by intubation M H COTTON, A M SAMMON From the Department of Surgery, Umtata Hospital, Transkei, South Africa ABSTRACT The management
Thorax 1989;44:42-47 Carcinoma of the oesophagus in Transkei: treatment by intubation M H COTTON, A M SAMMON From the Department of Surgery, Umtata Hospital, Transkei, South Africa ABSTRACT The management
Case Scenario 1. The patient has now completed his neoadjuvant chemoradiation and has been cleared for surgery.
 Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Quiz Adenocarcinoma of the distal stomach has been increasing in the last 20 years. a. True b. False
 Quiz 1 1. Which of the following are risk factors for esophagus cancer. a. Obesity b. Gastroesophageal reflux c. Smoking and Alcohol d. All of the above 2. Adenocarcinoma of the distal stomach has been
Quiz 1 1. Which of the following are risk factors for esophagus cancer. a. Obesity b. Gastroesophageal reflux c. Smoking and Alcohol d. All of the above 2. Adenocarcinoma of the distal stomach has been
ESOPHAGEAL CANCER. Dr. Paul Gardiner December 17, 2002 Discipline of Surgery Rounds
 ESOPHAGEAL CANCER Dr. Paul Gardiner December 17, 2002 Discipline of Surgery Rounds ESOPHAGEAL CANCER I. EPIDEMIOLOGY INCIDENCE, DIAGNOSIS & STAGING II. TREATMENT OPTIONS Current role of induction therapies
ESOPHAGEAL CANCER Dr. Paul Gardiner December 17, 2002 Discipline of Surgery Rounds ESOPHAGEAL CANCER I. EPIDEMIOLOGY INCIDENCE, DIAGNOSIS & STAGING II. TREATMENT OPTIONS Current role of induction therapies
Treatment of Esophageal Obstruction With Covered, Self-Expanding Esophageal Wallstents
 Treatment of Esophageal Obstruction With Covered, Self-Expanding Esophageal Wallstents Darroch W. O. Moores, MD, and Riivo Ilves, MD Division of Cardiothoracic Surgery,,, Albany Medical Center; and Department
Treatment of Esophageal Obstruction With Covered, Self-Expanding Esophageal Wallstents Darroch W. O. Moores, MD, and Riivo Ilves, MD Division of Cardiothoracic Surgery,,, Albany Medical Center; and Department
Esophageal Cancer. What is esophageal cancer?
 Scan for mobile link. Esophageal Cancer Esophageal cancer occurs when cancer cells develop in the esophagus. The two main types are squamous cell carcinoma and adenocarcinoma. Esophageal cancer may not
Scan for mobile link. Esophageal Cancer Esophageal cancer occurs when cancer cells develop in the esophagus. The two main types are squamous cell carcinoma and adenocarcinoma. Esophageal cancer may not
is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the
 My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
Epidemiology, aetiology and the patient pathway in oesophageal and pancreatic cancers
 Epidemiology, aetiology and the patient pathway in oesophageal and pancreatic cancers Dr Ian Chau Consultant Medical Oncologist Women's cancers Breast cancer introduction 3 What profession are you in?
Epidemiology, aetiology and the patient pathway in oesophageal and pancreatic cancers Dr Ian Chau Consultant Medical Oncologist Women's cancers Breast cancer introduction 3 What profession are you in?
A 16 yr old boy with aggressive ca esophagus. DR Ayunga A.O Physician-Garisa PGH Associate Faculty Lecturer-UON Afya Bora Fellow in Global Health
 A 16 yr old boy with aggressive ca esophagus DR Ayunga A.O Physician-Garisa PGH Associate Faculty Lecturer-UON Afya Bora Fellow in Global Health Cancer of esophagus in a 16yr old Y.N 16 yr old boy unwell
A 16 yr old boy with aggressive ca esophagus DR Ayunga A.O Physician-Garisa PGH Associate Faculty Lecturer-UON Afya Bora Fellow in Global Health Cancer of esophagus in a 16yr old Y.N 16 yr old boy unwell
EFFECTIVENESS OF RADIATION THERAPY IN THE TREATMENT OF CARCINOMA OF THE ESOPHAGUS*
 APRIL, 1970 EFFECTIVENESS OF RADIATION THERAPY IN THE TREATMENT OF CARCINOMA OF THE ESOPHAGUS* A RETROSPECTIVE STUDY Bv A. B. l RAZIER, M.I)., S. H. LEVITT, M.D., and L. S. DEGIORGI, M.D. RICHMOND, CARCINOMA
APRIL, 1970 EFFECTIVENESS OF RADIATION THERAPY IN THE TREATMENT OF CARCINOMA OF THE ESOPHAGUS* A RETROSPECTIVE STUDY Bv A. B. l RAZIER, M.I)., S. H. LEVITT, M.D., and L. S. DEGIORGI, M.D. RICHMOND, CARCINOMA
Endoscopic Treatment of Luminal Perforations and Leaks
 Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Effective Health Care
 Effective Health Care Comparative Effectiveness of Management Strategies for Gastroesophageal Reflux Disease Executive Summary Background Gastroesophageal reflux disease (GERD), defined as weekly heartburn
Effective Health Care Comparative Effectiveness of Management Strategies for Gastroesophageal Reflux Disease Executive Summary Background Gastroesophageal reflux disease (GERD), defined as weekly heartburn
National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia
 National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia Patient Details Surname: NHS number: Forename: Postcode: Sex: Male Female
National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia Patient Details Surname: NHS number: Forename: Postcode: Sex: Male Female
Determining Resectability and Appropriate Surgery for Esophageal Cancer
 Determining Resectability and Appropriate Surgery for Esophageal Cancer Peter Baik, DO, FACOS Thoracic Surgery Cancer Treatment Centers of America 1 Esophageal and Esophagogastric Junction Cancers Siewert
Determining Resectability and Appropriate Surgery for Esophageal Cancer Peter Baik, DO, FACOS Thoracic Surgery Cancer Treatment Centers of America 1 Esophageal and Esophagogastric Junction Cancers Siewert
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction
 A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL. September 17, Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous
 Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012
 Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
Determining the Optimal Surgical Approach to Esophageal Cancer
 Determining the Optimal Surgical Approach to Esophageal Cancer Amit Bhargava, MD Attending Thoracic Surgeon Department of Cardiovascular and Thoracic Surgery Open Esophagectomy versus Minimally Invasive
Determining the Optimal Surgical Approach to Esophageal Cancer Amit Bhargava, MD Attending Thoracic Surgeon Department of Cardiovascular and Thoracic Surgery Open Esophagectomy versus Minimally Invasive
Esophageal cancer. What is esophageal cancer? Esophageal cancer is a disease in which malignant (cancer) cells form in the tissues of the esophagus.
 Esophageal Cancer Esophageal cancer What is esophageal cancer? What are risk factors? Signs and symptoms Tests for esophageal cancer Stages of esophageal cancer Treatment options What is esophageal cancer?
Esophageal Cancer Esophageal cancer What is esophageal cancer? What are risk factors? Signs and symptoms Tests for esophageal cancer Stages of esophageal cancer Treatment options What is esophageal cancer?
Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 Final Pathology:
 Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 A 74 year old male with a history of GERD presents complaining of dysphagia. An esophagogastroduodenoscopy
Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 A 74 year old male with a history of GERD presents complaining of dysphagia. An esophagogastroduodenoscopy
Results of Conservative Treatment of Benign Esophageal Strictures: A Follow Up Study in 100 Patients
 GASTROENTEROLOGY 1982;82:487--93 Results of Conservative Treatment of Benign Esophageal Strictures: A Follow Up Study in 100 Patients. C. E. WESDORP, J. F. W. M. BARTELSMAN, F. C. A. DEN HARTOG JAGER,
GASTROENTEROLOGY 1982;82:487--93 Results of Conservative Treatment of Benign Esophageal Strictures: A Follow Up Study in 100 Patients. C. E. WESDORP, J. F. W. M. BARTELSMAN, F. C. A. DEN HARTOG JAGER,
Barrett s Esophagus. lining of the lower esophagus that bears his name (i.e., Barrett's esophagus). We now
 Shamika Johnson Anatomy & Physiology 206 April 20, 2010 Barrett s Esophagus What is Barrett s Esophagus? Norman Barrett was a pathologist. In 1950, he described an abnormality in the lining of the lower
Shamika Johnson Anatomy & Physiology 206 April 20, 2010 Barrett s Esophagus What is Barrett s Esophagus? Norman Barrett was a pathologist. In 1950, he described an abnormality in the lining of the lower
Intra-arterial chemotherapy for patients with
 Annals of the Royal College of Surgeons of England (980) vol 62 ASPECTS OF TREATMENT* ntra-arterial chemotherapy for patients with inoperable carcinoma of the pancreas Lord Smith of Marlow KBE MS PPRCS
Annals of the Royal College of Surgeons of England (980) vol 62 ASPECTS OF TREATMENT* ntra-arterial chemotherapy for patients with inoperable carcinoma of the pancreas Lord Smith of Marlow KBE MS PPRCS
Gastrointestinal Tract Cancer
 Gastrointestinal Tract Cancer Tumors of the Stomach Gastric adenocarcinoma Incidence and Epidemiology Incidence mortality rates USA High incidence: Japan, China, Chile, Ireland risk lower socioeconomic
Gastrointestinal Tract Cancer Tumors of the Stomach Gastric adenocarcinoma Incidence and Epidemiology Incidence mortality rates USA High incidence: Japan, China, Chile, Ireland risk lower socioeconomic
Therapeutic Bronchoscopy Etiology - Benign Stenosis Post - intubation Trauma Post - operative Inflammatory Idiopathic
 Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Polyflex Expandable Stents in the Treatment of Esophageal Disease: Initial Experience
 GENERAL THORACIC Polyflex Expandable Stents in the Treatment of Esophageal Disease: Initial Experience Arjun Pennathur, MD, Andrew C. Chang, MD, Kevin M. McGrath, MD, Gregory Steiner, BS, Miguel Alvelo-Rivera,
GENERAL THORACIC Polyflex Expandable Stents in the Treatment of Esophageal Disease: Initial Experience Arjun Pennathur, MD, Andrew C. Chang, MD, Kevin M. McGrath, MD, Gregory Steiner, BS, Miguel Alvelo-Rivera,
Adenocarcinoma of gastro-esophageal junction - Case report
 Case Report denocarcinoma of gastro-esophageal junction - Case report nupsingh Dhakre 1*, Ibethoi Yengkhom 2, Harshin Nagori 1, nup Kurele 1, Shreedevi. Patel 3 1 2 nd year Resident, 2 3rd year Resident,
Case Report denocarcinoma of gastro-esophageal junction - Case report nupsingh Dhakre 1*, Ibethoi Yengkhom 2, Harshin Nagori 1, nup Kurele 1, Shreedevi. Patel 3 1 2 nd year Resident, 2 3rd year Resident,
The Learning Curve for Minimally Invasive Esophagectomy
 The Learning Curve for Minimally Invasive Esophagectomy AATS Focus on Thoracic Surgery Mastering Surgical Innovation Las Vegas Nevada Oct. 27-28 2017 Scott J Swanson, M.D. Professor of Surgery Harvard
The Learning Curve for Minimally Invasive Esophagectomy AATS Focus on Thoracic Surgery Mastering Surgical Innovation Las Vegas Nevada Oct. 27-28 2017 Scott J Swanson, M.D. Professor of Surgery Harvard
Acquired pediatric esophageal diseases Imaging approaches and findings. M. Mearadji International Foundation for Pediatric Imaging Aid
 Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Observations on oesophageal length
 Thorax (1976), 31, 284. Observations on oesophageal length G. J. KALLOOR, A. H. DESHPANDE, and J. LEIGH COLLIS The Queen Elizabeth Hospital, Birmingham Kalloor, G. J., Deshpande, A. H., and Leigh Colfis,
Thorax (1976), 31, 284. Observations on oesophageal length G. J. KALLOOR, A. H. DESHPANDE, and J. LEIGH COLLIS The Queen Elizabeth Hospital, Birmingham Kalloor, G. J., Deshpande, A. H., and Leigh Colfis,
ENDOSCOPIC SELF-EXPANDABLE METAL STENTING FOR ADVANCED CARCINOMA OESOPHAGUS: A BETTER PALLIATIVE PROSPECTIVE
 22 Main Article ENDOSCOPIC SELF-EXPANDABLE METAL STENTING FOR ADVANCED CARCINOMA OESOPHAGUS: A BETTER PALLIATIVE PROSPECTIVE Swagata Khanna 1, Subhash Khanna 2 ABSTRACT: Endoscopic placement of metal stent
22 Main Article ENDOSCOPIC SELF-EXPANDABLE METAL STENTING FOR ADVANCED CARCINOMA OESOPHAGUS: A BETTER PALLIATIVE PROSPECTIVE Swagata Khanna 1, Subhash Khanna 2 ABSTRACT: Endoscopic placement of metal stent
Case Scenario year-old white male presented to personal physician with dyspepsia with reflux.
 Case Scenario 1 57-year-old white male presented to personal physician with dyspepsia with reflux. 7/12 EGD: In the gastroesophageal junction we found an exophytic tumor. The tumor occupies approximately
Case Scenario 1 57-year-old white male presented to personal physician with dyspepsia with reflux. 7/12 EGD: In the gastroesophageal junction we found an exophytic tumor. The tumor occupies approximately
DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA
 Solunum 3, Özel Sayı 2: 260-264, 2001 DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA Jean F DUMON* M C DUMON* SUMMARY This article reports a 4-year
Solunum 3, Özel Sayı 2: 260-264, 2001 DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA Jean F DUMON* M C DUMON* SUMMARY This article reports a 4-year
ESOPHAGEAL CANCER AND GERD. Prof Salman Guraya FRCS, Masters MedEd
 ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
Basic Principles of Esophageal Surgery. 1 Surgical Anatomy of the Esophagus... 3
 Contents Basic Principles of Esophageal Surgery 1 Surgical Anatomy of the Esophagus... 3 D. C. Broering, J. Walter, Z. Halata ] Topography of the esophagus... 3 ] Development of the esophagus... 4 ] Structure
Contents Basic Principles of Esophageal Surgery 1 Surgical Anatomy of the Esophagus... 3 D. C. Broering, J. Walter, Z. Halata ] Topography of the esophagus... 3 ] Development of the esophagus... 4 ] Structure
The first stents designed for use in the biliary tree and
 Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
ESPEN Congress Brussels Stenting of the esophagus and small bowel. Jean-Marc Dumonceau
 ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
Carcinoma of the Lung
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
Esophageal Dilatation (Bouginage)
 Esophageal Dilatation (Bouginage) Pages with reference to book, From 20 To 23 Ziauddin Shamsi, M. Aftab Anwar ( 5/16, Rimpa Plaza, M.A. Jinnah Road, Karachi. ) Esophageal dilatation is very important addition
Esophageal Dilatation (Bouginage) Pages with reference to book, From 20 To 23 Ziauddin Shamsi, M. Aftab Anwar ( 5/16, Rimpa Plaza, M.A. Jinnah Road, Karachi. ) Esophageal dilatation is very important addition
A review of the management of 100 cases of
 Thorax (1972), 27, 599. A review of the management of 100 cases of benign stricture of the oesophagus S. RAPTIS' and D. MEARNS MILNE Thoracic Unit, Frenchay Hospital One hundred cases of benign stricture
Thorax (1972), 27, 599. A review of the management of 100 cases of benign stricture of the oesophagus S. RAPTIS' and D. MEARNS MILNE Thoracic Unit, Frenchay Hospital One hundred cases of benign stricture
Icd 10 code for distal esophageal stricture Address Submit
 Icd 10 code for distal esophageal stricture Email Address Submit If an EGD is performed with a biopsy, and then the physician removes the scope and performs an Esophageal Dilation by unguided sound, it
Icd 10 code for distal esophageal stricture Email Address Submit If an EGD is performed with a biopsy, and then the physician removes the scope and performs an Esophageal Dilation by unguided sound, it
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
Covered stenting in patients with lifting of gastric and high esophago-tracheal fistula
 European Radiology Springer-Verlag 2003 DOI 10.1007/s00330-002-1818-z Tips and Tricks in Radiology Covered stenting in patients with lifting of gastric and high esophago-tracheal fistula T. Lehnert J.
European Radiology Springer-Verlag 2003 DOI 10.1007/s00330-002-1818-z Tips and Tricks in Radiology Covered stenting in patients with lifting of gastric and high esophago-tracheal fistula T. Lehnert J.
ORIGINAL ARTICLE. The Kirschner Operation in Unresectable Esophageal Cancer
 The Kirschner Operation in Unresectable Esophageal Cancer Current Application ORIGINAL ARTICLE Brian P. Whooley, MD; Simon Law, MBBChir, FRCS(Edin); Sudish C. Murthy, MD, PhD; Andreas Alexandrou, MD; Kent-Man
The Kirschner Operation in Unresectable Esophageal Cancer Current Application ORIGINAL ARTICLE Brian P. Whooley, MD; Simon Law, MBBChir, FRCS(Edin); Sudish C. Murthy, MD, PhD; Andreas Alexandrou, MD; Kent-Man
Esophageal Stenosis Treatment by Interventional Radiology: Indications, Techniques and complications
 Esophageal Stenosis Treatment by Interventional Radiology: Indications, Techniques and complications Poster No.: C-0437 Congress: ECR 2013 Type: Authors: Keywords: DOI: Educational Exhibit M. Leyva Vásquez-Caicedo,
Esophageal Stenosis Treatment by Interventional Radiology: Indications, Techniques and complications Poster No.: C-0437 Congress: ECR 2013 Type: Authors: Keywords: DOI: Educational Exhibit M. Leyva Vásquez-Caicedo,
Douglas G. Adler MD. ACG Regional Postgraduate Course - Nashville, TN Copyright 2013 American College of Gastroenterology
 Enteral Stents 2013: State of the Art Douglas G. Adler MD Associate Professor of Medicine Director of Therapeutic Endoscopy University of Utah School of Medicine Huntsman Cancer Center Esophageal Stents
Enteral Stents 2013: State of the Art Douglas G. Adler MD Associate Professor of Medicine Director of Therapeutic Endoscopy University of Utah School of Medicine Huntsman Cancer Center Esophageal Stents
S tating disease, and for the vast majority of patients,
 Prospective, Randomized Trial of Palliative Treatment for Unresectablle Cancer of the Esophagus Carolyn E. Reed, MD, William H. Marsh, MD, Leta S. Carlson, MD, Cathy H. Seymore, MD, and John M. Kratz,
Prospective, Randomized Trial of Palliative Treatment for Unresectablle Cancer of the Esophagus Carolyn E. Reed, MD, William H. Marsh, MD, Leta S. Carlson, MD, Cathy H. Seymore, MD, and John M. Kratz,
Jejunostomy after oesophagectomy, how and why I do it
 Jejunostomy after oesophagectomy, how and why I do it Graeme Couper. Consultant Oesophago-gastric Surgeon, The Royal Infirmary of Edinburgh BAPEN Conference 2010 2nd & 3rd November Harrogate International
Jejunostomy after oesophagectomy, how and why I do it Graeme Couper. Consultant Oesophago-gastric Surgeon, The Royal Infirmary of Edinburgh BAPEN Conference 2010 2nd & 3rd November Harrogate International
34th Annual Toronto Thoracic Surgery Refresher Course
 34th Annual Toronto Thoracic Surgery Refresher Course TREATMENT OPTIONS FOR ACHALASIA Dr. Carmine Simone Director, Intensive Care Unit Head, Division of Critical Care Departments of Medicine and Surgery
34th Annual Toronto Thoracic Surgery Refresher Course TREATMENT OPTIONS FOR ACHALASIA Dr. Carmine Simone Director, Intensive Care Unit Head, Division of Critical Care Departments of Medicine and Surgery
Pulmonary Valve Replacement
 Pulmonary Valve Replacement with Fascia Lata J. C. R. Lincoln, F.R.C.S., M. Geens, M.D., M. Schottenfeld, M.D., and D. N. Ross, F.R.C.S. ABSTRACT The purpose of this paper is to describe a technique of
Pulmonary Valve Replacement with Fascia Lata J. C. R. Lincoln, F.R.C.S., M. Geens, M.D., M. Schottenfeld, M.D., and D. N. Ross, F.R.C.S. ABSTRACT The purpose of this paper is to describe a technique of
Acquired oesophageal strictures in children: emphasis on the use of string - guided dilatations
 82 Original Article Acquired oesophageal strictures in children: emphasis on the use of string - guided dilatations Saleem M M ABSTRACT Introduction: Acquired oesophageal strictures are common in children.
82 Original Article Acquired oesophageal strictures in children: emphasis on the use of string - guided dilatations Saleem M M ABSTRACT Introduction: Acquired oesophageal strictures are common in children.
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD
 Esophagus Anatomy/Physiology Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD Manometry Question 50 years old female with chest pain and dysphagia. Manometry
Esophagus Anatomy/Physiology Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD Manometry Question 50 years old female with chest pain and dysphagia. Manometry
CT PET SCANNING for GIT Malignancies A clinician s perspective
 CT PET SCANNING for GIT Malignancies A clinician s perspective Damon Bizos Head, Surgical Gastroenterology Charlotte Maxeke Johannesburg Academic Hospital Case presentation 54 year old with recent onset
CT PET SCANNING for GIT Malignancies A clinician s perspective Damon Bizos Head, Surgical Gastroenterology Charlotte Maxeke Johannesburg Academic Hospital Case presentation 54 year old with recent onset
Indian Journal of Basic and Applied Medical Research; December 2015: Vol.-5, Issue- 1, P
 Original article A study of clinical profile and therapeutic efficacy of esophageal dilatation with Savary- Gilliard dilators in benign strictures of middle and lower thirds of esophagus,without the use
Original article A study of clinical profile and therapeutic efficacy of esophageal dilatation with Savary- Gilliard dilators in benign strictures of middle and lower thirds of esophagus,without the use
DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER
 November 2015 DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER 1 Background... 3 2 Dysphagia Grading... 3 3 Dysphagia General Guidelines... 4 4 Modes of Managing Dysphagia... 4 4.1 Modified consistency diet...
November 2015 DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER 1 Background... 3 2 Dysphagia Grading... 3 3 Dysphagia General Guidelines... 4 4 Modes of Managing Dysphagia... 4 4.1 Modified consistency diet...
Peroral Esophageal Intubation for Obstructive Carcinoma of the Esophagus
 Peroral Esophageal Intubation for Obstructive Carcinoma of the Esophagus Ralph J. Lewis, M.D., Philip J. Kunderman, M.D., Glenn E. Sisler, M.D., and James W. Mackenzie, M.D. ABSTRACT Seventeen patients
Peroral Esophageal Intubation for Obstructive Carcinoma of the Esophagus Ralph J. Lewis, M.D., Philip J. Kunderman, M.D., Glenn E. Sisler, M.D., and James W. Mackenzie, M.D. ABSTRACT Seventeen patients
The Role of Radiation Therapy
 The Role of Radiation Therapy and Surgery in the Treatment of Bronchogenic Carcinoma R Adams Cowley, M.D., Morris J. Wizenberg, M.D., and Eugene J. Linberg, M.D. A study of the combined use of preoperative
The Role of Radiation Therapy and Surgery in the Treatment of Bronchogenic Carcinoma R Adams Cowley, M.D., Morris J. Wizenberg, M.D., and Eugene J. Linberg, M.D. A study of the combined use of preoperative
Esophageal cancer: Biology, natural history, staging and therapeutic options
 EGEUS 2nd Meeting Esophageal cancer: Biology, natural history, staging and therapeutic options Michael Bau Mortensen MD, Ph.D. Associate Professor of Surgery Centre for Surgical Ultrasound, Upper GI Section,
EGEUS 2nd Meeting Esophageal cancer: Biology, natural history, staging and therapeutic options Michael Bau Mortensen MD, Ph.D. Associate Professor of Surgery Centre for Surgical Ultrasound, Upper GI Section,
Medicinae Doctoris. One university. Many futures.
 Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Surgical Problems in Proximal GI Cancer Management Cardia Tumours Question #1: What are cardia tumours?
 Surgical Problems in Proximal GI Cancer Management Cardia Tumours Question #1: What are cardia tumours? Question #2: How are cardia tumours managed? Michael F. Humer December 3, 2005 Vancouver, BC Case
Surgical Problems in Proximal GI Cancer Management Cardia Tumours Question #1: What are cardia tumours? Question #2: How are cardia tumours managed? Michael F. Humer December 3, 2005 Vancouver, BC Case
Management of Neck Metastasis from Unknown Primary
 Management of Neck Metastasis from Unknown Primary.. Definition Histologic evidence of malignancy in the cervical lymph node (s) with no apparent primary site of original tumour Diagnosis after a thorough
Management of Neck Metastasis from Unknown Primary.. Definition Histologic evidence of malignancy in the cervical lymph node (s) with no apparent primary site of original tumour Diagnosis after a thorough
A cost analysis of endoscopic ultrasound in the evaluation of esophageal cancer Harewood G C, Wiersema M J
 A cost analysis of endoscopic ultrasound in the evaluation of esophageal cancer Harewood G C, Wiersema M J Record Status This is a critical abstract of an economic evaluation that meets the criteria for
A cost analysis of endoscopic ultrasound in the evaluation of esophageal cancer Harewood G C, Wiersema M J Record Status This is a critical abstract of an economic evaluation that meets the criteria for
Clinical evaluation of treating an advanced esophageal carcinoma by using membrane-covered metallic stent
 Clinical evaluation of treating an advanced esophageal carcinoma by using membrane-covered metallic stent Xu meidong, Yao liqing, Zhong yunshi et al. Department of Endoscopy Center, Zhongshan Hospital,
Clinical evaluation of treating an advanced esophageal carcinoma by using membrane-covered metallic stent Xu meidong, Yao liqing, Zhong yunshi et al. Department of Endoscopy Center, Zhongshan Hospital,
LIFE EXPECTANCY AND INCIDENCE OF MALIGNANT DISEASE
 LIFE EXPECTANCY AND INCIDENCE OF MALIGNANT DISEASE IRA T. NATHANSON,' M.S., M.D., AND CLAUDE E. WELCH,2 M.A., M.D. (From the Collis P. Huntington Memorial Hospital, Harvard University, Boston, Mass., and
LIFE EXPECTANCY AND INCIDENCE OF MALIGNANT DISEASE IRA T. NATHANSON,' M.S., M.D., AND CLAUDE E. WELCH,2 M.A., M.D. (From the Collis P. Huntington Memorial Hospital, Harvard University, Boston, Mass., and
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)?
 WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
Michael A. Choti, MD, FACS Department of Surgery Johns Hopkins Medicine, Baltimore, MD
 Michael A. Choti, MD, FACS Department of Surgery Johns Hopkins Medicine, Baltimore, MD Surgical Therapy of Gastric Cancer CLINICAL QUESTIONS 1. How much of the stomach should be removed? 2. How many lymph
Michael A. Choti, MD, FACS Department of Surgery Johns Hopkins Medicine, Baltimore, MD Surgical Therapy of Gastric Cancer CLINICAL QUESTIONS 1. How much of the stomach should be removed? 2. How many lymph
PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
 Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
THORACIC MALIGNANCIES
 THORACIC MALIGNANCIES Summary for Malignant Malignancies. Lung Ca 1 Lung Cancer Non-Small Cell Lung Cancer Diagnostic Evaluation for Non-Small Lung Cancer 1. History and Physical examination. 2. CBCDE,
THORACIC MALIGNANCIES Summary for Malignant Malignancies. Lung Ca 1 Lung Cancer Non-Small Cell Lung Cancer Diagnostic Evaluation for Non-Small Lung Cancer 1. History and Physical examination. 2. CBCDE,
Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012
 Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012 Esophageal Leiomyoma Introduction Case presentation Operative video Discussion Esophageal Leiomyoma Benign tumors of the
Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012 Esophageal Leiomyoma Introduction Case presentation Operative video Discussion Esophageal Leiomyoma Benign tumors of the
Reflux Control Following Gastroplasty
 ORIGINAL ARTICLES Reflux Control Following Gastroplasty Robert D. Henderson, M.B.,.F.R.C.S.(C) ABSTRACT A Belsey gastroplasty was performed on 135 patients, 132 of whom were available for follow-up. Despite
ORIGINAL ARTICLES Reflux Control Following Gastroplasty Robert D. Henderson, M.B.,.F.R.C.S.(C) ABSTRACT A Belsey gastroplasty was performed on 135 patients, 132 of whom were available for follow-up. Despite
Surgical aspects of dysphagia
 Dysphagia Why is dysphagia important? Surgery Surgical aspects of dysphagia Adrian P. Ireland aireland@eircom.net Academic RCSI Department of Surgery, Beaumont Hospital Why important Definitons Swallowing
Dysphagia Why is dysphagia important? Surgery Surgical aspects of dysphagia Adrian P. Ireland aireland@eircom.net Academic RCSI Department of Surgery, Beaumont Hospital Why important Definitons Swallowing
Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
The Percutaneous Endoscopic Gastrostomy. Geoffrey Axiak Clinical Nutrition Nurse St. Luke s Hospital
 The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak Clinical Nutrition Nurse St. Luke s Hospital What is a P.E.G.? Percutaneous Endoscopic Gastrostomy Indications for P.E.G. Insertion In cases of long-term
The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak Clinical Nutrition Nurse St. Luke s Hospital What is a P.E.G.? Percutaneous Endoscopic Gastrostomy Indications for P.E.G. Insertion In cases of long-term
Bidirectional esophageal dilatation in pharyngoesophageal stenosis postradiotherapy
 OPERATIVE TECHNIQUES PICTORIAL ESSAY Bidirectional esophageal dilatation in pharyngoesophageal stenosis postradiotherapy Haim Gavriel, MD,* Cuong Duong, MB, BS, PhD, FRACS, John Spillane, MB, BS, FRACS,
OPERATIVE TECHNIQUES PICTORIAL ESSAY Bidirectional esophageal dilatation in pharyngoesophageal stenosis postradiotherapy Haim Gavriel, MD,* Cuong Duong, MB, BS, PhD, FRACS, John Spillane, MB, BS, FRACS,
LINX Reflux Management System
 LINX Reflux Management System Patient Information Caution: Federal (USA) Law restricts this device to sale by or on the order of a physician. LINX Reflux Management System 2 Table of Contents What is the
LINX Reflux Management System Patient Information Caution: Federal (USA) Law restricts this device to sale by or on the order of a physician. LINX Reflux Management System 2 Table of Contents What is the
Esophageal Stent Placement for the Treatment of Acute Intrathoracic Anastomotic Leak After Esophagectomy
 ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
INFORMED CONSENT FOR LAPAROSCOPIC ADJUSTABLE GASTRIC BAND. Please read this form carefully and ask about anything you may not understand.
 Please read this form carefully and ask about anything you may not understand. I consent to undergo laparoscopic placement of a laparoscopic Adjustable Gastric Band for the purposes of weight loss. I met
Please read this form carefully and ask about anything you may not understand. I consent to undergo laparoscopic placement of a laparoscopic Adjustable Gastric Band for the purposes of weight loss. I met
Surgical Management of Graft Redundancy after Colon Interposition for Esophageal Reconstruction. Case 1
 Case Report imedpub Journals www.imedpub.com Medical & Clinical Reviews DOI: 10.21767/2471-299X.1000059 Surgical Management of Graft Redundancy after Colon Interposition for Esophageal Reconstruction Abdelkader
Case Report imedpub Journals www.imedpub.com Medical & Clinical Reviews DOI: 10.21767/2471-299X.1000059 Surgical Management of Graft Redundancy after Colon Interposition for Esophageal Reconstruction Abdelkader
Imaging of gastric bands and their complications: an educational pictorial review
 Imaging of gastric bands and their complications: an educational pictorial review Poster No.: C-1142 Congress: ECR 2014 Type: Educational Exhibit Authors: F. Moloney, M. Twomey, C. Bogue ; Cork/IE, IE,
Imaging of gastric bands and their complications: an educational pictorial review Poster No.: C-1142 Congress: ECR 2014 Type: Educational Exhibit Authors: F. Moloney, M. Twomey, C. Bogue ; Cork/IE, IE,
Clinical Experience With Montgomery Salivary Bypass Stents in the Esophagus
 Clinical Experience With Montgomery Salivary Bypass Stents in the Esophagus William H. Warren, MD, Claire Smith, MD, and L. Penfield Faber, MD Departments of Cardiovascular-Thoracic Surgery and Diagnostic
Clinical Experience With Montgomery Salivary Bypass Stents in the Esophagus William H. Warren, MD, Claire Smith, MD, and L. Penfield Faber, MD Departments of Cardiovascular-Thoracic Surgery and Diagnostic
(a) (b) Plate 16.1 Esophageal tear after passage of the echoendoscope.
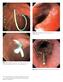 Plate 16.1 Esophageal tear after passage of the echoendoscope. Plate 11.1 Prophylactic pancreatic duct stents. 3-Fr, 4-cm long single-pigtail stent. 5-Fr, 3-cm long flanged stent. Plate 16.2 Esophageal
Plate 16.1 Esophageal tear after passage of the echoendoscope. Plate 11.1 Prophylactic pancreatic duct stents. 3-Fr, 4-cm long single-pigtail stent. 5-Fr, 3-cm long flanged stent. Plate 16.2 Esophageal
Type of intervention Palliative care. Economic study type Cost-effectiveness analysis.
 Natural course of inoperable esophageal cancer treated with metallic expandable stents: quality of life and cost-effectiveness analysis Xinopoulos D, Dimitroulopoulos D, Moschandrea I, Skordilis P, Bazinis
Natural course of inoperable esophageal cancer treated with metallic expandable stents: quality of life and cost-effectiveness analysis Xinopoulos D, Dimitroulopoulos D, Moschandrea I, Skordilis P, Bazinis
