Clinical Experience With Montgomery Salivary Bypass Stents in the Esophagus
|
|
|
- Mark Chandler
- 6 years ago
- Views:
Transcription
1 Clinical Experience With Montgomery Salivary Bypass Stents in the Esophagus William H. Warren, MD, Claire Smith, MD, and L. Penfield Faber, MD Departments of Cardiovascular-Thoracic Surgery and Diagnostic Radiology, Rush Presbyterian-St. Luke's Medical Centre, Chicago, Illinois Thirty-seven patients with locally advanced malignancy (18, esophageal obstruction; 19, esophageal fistula formation) underwent attempted placement of a Montgomery salivary stent in the esophagus. This was unsuccessful in 3; in 2, because of inability to dilate, and, in 1, because of perforation. After dilation of the esophagus, there was no detectable underlying stricture in 11 patients; none of these patients experienced stent migration. Overall, there was 100% success in obliterating the fistulous tract, an 8.1% incidence of retrograde migration, no incidence of prograde migration, and no incidence of stent obstruction after discharge. Of the 34 patients with successfully placed stents, 27 were discharged from hospital, and were able to eat and drink without the need for intravenous supplementation or gastrostomy tube feedings. The survival in patients presenting with obstruction ranged from 1 to 13 months (mean, 8.0 months); the survival in patients presenting with a fistula ranged from 2 to 7 months (mean, 5.3 months). (Ann Thorac Surg 1994;57:1102-7) ne of the most challenging problems in esophageal 0 surgery is the management of patients with locally advanced, unresectable carcinoma of the esophagus. Therapeutic options in such patients include bypass operation, endoesophageal recanalization using BICAP electrocautery or neodymium:yttrium-aluminum-garnet photoablation, radiotherapy (external beam, brachytherapy, or both), and the placement of an esophageal stent. The purpose of this report is to summarize our clinical experience with the use of the Montgomery salivary stent placed entirely within the esophagus. Material and Methods Patients Since 1985, 37 patients with locally advanced and unresectable carcinoma have undergone attempted placement of a Montgomery salivary stent (E. Benson Hood Laboratories, Pembroke, MA) for treatment of a symptomatic esophageal obstruction, fistula formation, or both. In all cases, the tumors were considered unresectable based on clinical and radiologic findings. No patient was denied an attempted stent placement regardless of his or her general condition or anesthetic risk, the location and length of the tumor, and the tortuousity of the esophageal lumen. The sites of the primary malignancy were the esophagus (n = 20), lung (n = 14), larynx (n = 2), and breast (n = 1). Five of the carcinomas not primary to the esophagus caused obstruction by extrinsic compression without detectable involvement of the esophageal mucosa. In 31 patients, the tumor was in the upper third of the esophagus in 5, in the middle third in 21, and in the distal Presented at the Fortieth Annual Meeting of the Southern Thoracic Surgical Association, Panama City Beach, FL, Nov 4-6, Address reprint requests to Dr Warren, Suite 218, 1725 W Harrison St, Chicago, IL third but sparing the gastroesophageal junction in 5. Of the remaining 6 patients, 5 had undergone an esophiagogastrectomy and 1 had undergone a total gastrectomy; recurrent tumor developed at the anastomosis in all 6. Twenty-nine of the 37 patients had previously undergone chemotherapy or radiotherapy, or both, which initially had provided varying degrees of palliation. Patients presented with complaints referable to esophageall obstruction (n = 18), an esophagorespiratory fistula i(n = 16), a fistula between the esophagus and a right pneumonectomy space (n = 2), or a fistula to a subcarinal mediastinal abscess cavity (n = 1). A review of the perioperative complications, the length of hospital stay, the quality of life, and the length of survival was performed. Operative Technique Most procedures were performed with the patients under general anesthesia, although 2 patients had stent placement under sedation alone without intubation of' the airway. In patients with a known or suspected fistula to the respiratory tract, flexible bronchoscopy was performed initially. Retained secretions were aspirated, the site of the fistula was noted, and the endotracheal tube was placed beyond this point to minimize gastric bloating. Patients then underwent flexible esophagoscopy and the guidewire of an Eder-Puestow dilator was passed through the instrument channel into the stomach under fluoroscopic control. The esophagoscope was then withdrawn and the malignant stricture was dilated using Ilder- Puestow dilators. Whenever possible, the esophagus was further dilated using Maloney bougies until firm resistance was met. In 11 cases, no clinically detectable stricture remained at the completion of the dilation. The size of the stent (ranging from 8 to 20 mm outer diameter by The Society of Thoracic Surgeons /94/'$7.00
2 Ann Thorac Surg :!994; WARREN ET AL 1103 Fig 1. Montgomery salivary stents available in sizes ranging from 8 to 20 mm in outer diameter. [OD]) was selected based on the maximum dilatable diameter of the esophagus (Fig 1). The stent was passed using one of two techniques. In stents ranging from 10 to 14 mm OD, the stent was passed over a lubricated Maloney bougie and advanced into the esophagus such that the upper flange was below the level of the upper esophageal sphincter. At this level, the distal end of the stent almost always had passed beyond the stricture or fistula, and the Maloney bougie was withdrawn. The stent was then advanced farther using a rigid esophagoscope until it reached the desired position. In stents ranging from 16 to 20 mm OD, the stent was rnounted onto a flexible esophagoscope and advanced into the esophagus using a section of half-inch (1.25-cm) tubing that acted as a pusher (Fig 2). This silicone prosthesis is prone to tearing if grasped directly with foreign body forceps. If required, the stent can be repositioned more proximally using one or more Fogarty balloon catheters passed through the stent, which are then inflated and withdrawn, causing the stent to be pulled back. Results Of the 37 patients undergoing attempted stent placement, the stent could not be successfully placed in 3 patients, Fig 2. Method of insertion of stents of larger diameter. Under direct vbual control, the stent is advanced over the flexible esophagoscope using a length of Tygon tubing. Fig 3. A 16-mm Montgomery salivary stent placed through an esophagojejunostomy with recurrence of the carcinoma at the anastomosis (arrow). due to inability to dilate the stricture in 2 and due to intraoperative perforation of the esophagus in 1. Of the remaining 34 patients, all were extubated within 3 hours of the completion of the operation. On the first postoperative day, these patients underwent fluoroscopic examinations using barium sulfate contrast material. These studies demonstrated that the prosthesis had been successfully placed within the esophageal lumen through the strictured segment in all 15 patients presenting with obstruction. In all 19 patients presenting with a fistulous tract, the fistula had been successfully excluded. In 28 of the 34 cases in which the stent was successfully placed, the proximal flange was at least 1 cm below the upper esophageal sphincter and the distal tip was proximal to the gastroesophageal junction. In the remaining 6 cases, the stent was successfully placed across an anastomotic recurrence after a previous esophagogastrectomy (5 cases) or a total gastrectomy (1 case) (Fig 3). None of these 6 patients suffered symptomatic reflux. The degree of success in relieving dysphagia was related, in large part, to the diameter of the stent chosen. The diameters of the stents placed and the numbers of patients who received them were as follows: 8 mm, no patients; 10 mm, 3 patients; 12 mm, 4 patients; 14 mm, 5 patients; 16 mm, 10 patients; 18 mm, 9 patients; and 20 mm, 3 patients. Patients had no dietary restrictions, except to avoid apple and tomato skins and the pulp of fresh oranges. Patients were encouraged to eat as full a diet as they desired, including meat, provided it was chewed well. However, the patients with the smallest stents had the most advanced obstructions and sometimes had a limited appetite.
3 1104 WARREN ET AL No patients complained of tracheal irritation or esophageal discomfort, even though, in 7, the proximal flange of the stent was placed within 2 cm of the upper esophageal sphincter (Fig 4). In 11 patients (7 with fistula formation and 4 with obstruction), there was no evidence of an underlying stricture after dilation. In these patients, either 18-mm or 20-mm stents were placed (Fig 5). None of these 11 patients had evidence of stent regurgitation or migration and palliation was excellent in all. Four patients had regurgitation of the stent. In 3 of these cases, the dislodgment occurred within 48 hours of placement, and all were successfully managed by immediate reinsertion of a larger stent. Two of these 3 cases occurred early in our experience and arose because the stent inserted was too small for the dilated lumen. None of these 3 patients suffered any further displacement during the remainder of their survivals beyond 2, 3, and 13 months. The fourth patient had undergone an esophagogastrectomy, and suffered extrinsic compression from recurrent tumor at the site of the anastomosis, 2 cm below the upper esophageal sphincter. After the stent migrated distally on two occasions, the stent was removed and the stricture was allowed to redevelop. A 14-mm stent was successfully placed 7 months later, and, as of the last examination 11 weeks later, remained in a good position. One stent was passed inadvertently into the stomach at the time of the procedure and a gastrotomy was necessary to retrieve it. Once the stent was properly placed within the esophagus, there was no clinical evidence of prograde Ann Thorac Surg 1994;57l102-7 A B Fig 5. ( A ) Thin barium swallow study obtained in a patient after a right pneumonectomy demonstrating a tracheoesophageal fistula through a subcarinal mass to the left of the main bronchus (arrow). (B)Contrast-enhanced esophagogram demonstrating the 18-mm stent in place with obliteration of the fistulous tract. Fig 4. A 14-mm Montgomery salivary stent placed high in the cervical esophagus. Note that the flange is immediately below the upper esophageal sphincter. migration of the stent during follow-up until the patient died more than 6 months later. None of the 37 patients died intraoperatively or postoperatively in the hospital as a result of stent insertion. However, of the 34 Patients who successfullyunderwent stent placement, 6 patients died in the hospital from pulmonary sepsis 2 to 18 days after the procedure. The
4 Ann Thorac Surg 1994: WARREN ET AL 1105 remaining 28 patients were discharged from the hospital after a hospital stay ranging from 1 to 15 days (mean, 4.6 days) in patients with obstruction and from 1 to 36 days (mean, 7.7 days) in patients with a fistula. All discharged patients were able to eat and drink, and did not need intravenous support. In 2 patients, a gastrostomy tube had been placed before the stent insertion and was used temporarily to supplement oral intake. During a clinical follow-up until death, no patient experienced any postoperative esophageal obstruction, including impaction of the stent with food or collapse of the stent resulting from extrinsic compression. Follow-up contrast studies were not routinely obtained. Overall, 11 of 37 (29.7%) patients died within 30 days of stent placement. Of these, 4 of 18 (22.2%) patients originally presented with obstruction and 7 of 19 (36.8%) patients presented with a fistula. Of the 34 patients undergoing successful stent placement, survival in the 17 patients presenting with esophageal obstruction ranged from 1 to 13 months (mean, 8.0 months); 6 of these patients survived for more than 6 months. The survival in the 19 patients with a fistula ranged from 2 to 7 months (mean, 5.3 months); 3 of these patients survived for 6 months. In most cases, the cause of death was inanition, complicated by pulmonary sepsis. Two patients died of a sudden upper gastrointestinal hemorrhage 1 and 2 weeks after an apparently uncomplicated stent placement. Both of these patients had bulky subcarinal carcinomas with fistula formation. No autopsy was obtained. Comment In 1955, Montgomery [l] devised a polyethylene prosthetic tube to bridge the gap between the pharyngostoma and the esophagostoma after laryngoesophagectomy and before reconstruction of the cervical esophagus. These stents were molded in varying diameters to accommodate pharyngeal and esophageal lumina. Currently, these prostheses are commercially available as silicone tubes measuring 18 cm in length with an external diameter ranging from 8 to 20 mm. We and others [2] have chosen to place appropriately sized stents entirely within the esophagus using a "push-through" technique in patients with an unresectable malignant esophageal obstruction, fistula formation, or both. The lack of postoperative obstructions in our patients is in sharp contrast to the experience of others who have used other types of stents and who have reported an incidence of obstruction as high as 30% [3]. Tumors have not overgrown the ends of the Montgomery salivary stent, nor compressed the stents to cause a functional obstruction. In addition, choosing a stent that provides a maximal inner diameter and a smooth lining minimizes food sticking and impaction. These tubes are held in place by the residual underlying stricture (when one exists), the proximal flange, and the intrinsic tone of the esophagus. Furthermore, the upper and lower esophageal sphincters tend to prevent migration proximally and distally. We believe that the ability to choose an appropriately sized stent to distend the maximally dilated esophagus is largely responsible for the low incidence of migration in our patients, which others, using other stents, have reported to range from 3.8% to 23% [3-91. In those patients with little or no detectable underlying stricture, some authors consider stents to be contraindicated due to the high incidence of migration [6, 13, 151. Others have used tissue adhesive, Ivalon sponges, and inflatable balloons to minimize this risk [ With our technique, the stent did not migrate in any of the 11 patients without a clinically detectable stricture. Silicone is a soft and pliable polymer and the wall thickness in the Montgomery stent is 1 mm, which is less irritating to the trachea when the upper flange is in the subcricoid area. The pliability of the silicone and the availability of the stent in varying diameters facilitate insertion, even when the esophageal lumen is markedly narrowed or tortuous. We had only a 5.4% (2 of 37) incidence of failure to intubate due to inability to pass the stent down a tortuous or narrowed esophagus; others have reported an incidence as high as 9.4% using other stent models [4]. In 4 patients in our series, Montgomery salivary stents were successfully placed after attempts to place other models had failed. In addition, we have noted a low incidence of failure to exclude a fistula, which others have reported to be as high as 26.5% [12, 191, and a low incidence of perforation, which others have reported to be as high as 18% using Keymed-Atkinson stents [3, 14, 201. The 30-day perioperative mortality reflects the poor health of patients who undergo these procedures. Our perioperative mortality and mean survival compare favorably with those reported for other series [2, 4, 51. In conclusion, we believe that the Montgomery-Hood salivary stent can be safely introduced into the esophagus with an attendant low operative mortality and an acceptably low complication rate. It produces reasonable palliation and also offers patients who otherwise live in misery an opportunity for survival beyond 6 months out of the hospital. This stent deserves further study, especially because it has been highly successful in excluding fistulous tracts, and in palliating patients with no underlying stricture in whom other esophageal prostheses traditionally have been contraindicated. Supported in part by the John and June Antalek Foundation, the Kole Foundation, and the contributors to the Thoracic Disease Research Fund. References 1. Montgomery WW. Plastic esophageal tube. Ann Otol Rhino1 Laryngol 1955;64: Richter JM, Hilgenberg AD, Christensen MR, et al. Endoscopic palliation of obstructive esophagogastric malignancy. Gastrointest Endosc 1988;34: Liakakos TK, Ohri SK, Townsend ER, Fountain SW. Palliative intubation for dysphagia in patients with carcinoma of the esophagus. Ann Thorac Surg 1992;53:46&3. 4. Buset M, des Marez B, Baize M, et al. Palliative endoscopic management of obstructive esophagogastric cancer: laser or prosthesis? Gastrointest Endosc 1987;33:
5 1106 WARREN ET AL Ann Thorac!Surg 1994; Alderson D, Wright PD. Laser recanalization versus endoscopic intubation in the palliation of malignant dysphagia. Br J Surg 1990;77: Angorn IB. Intubation in the treatment of carcinoma of the esophagus. World J Surg 1981;5: Segalin A, Little AG, Ruol A, et al. Surgical and endoscopic palliation of esophageal carcinoma. Ann Thorac Surg 1989; 48: den Hartog Jager FCA, Bartelsman JFWM, Tytgat GNJ. Palliative treatment of obstructing esophagogastric malignancy by positioning of a plastic prosthesis. Gastroenterology 1979; Girardet RE, Ransdell HT, Wheat MW. Palliative intubation in the management of esophageal carcinoma. Ann Thorac Surg 1974;18: Watson A. A study in the quality and duration of survival following resection, endoscopic intubation and surgical intubation in oesophageal carcinoma. Br J Surg 1982;69: Mason RC, Bright N, McColl I. Palliation of malignant dysphagia with laser therapy: predictability of results. Br J Surg 1991;78: Cusumano A, Ruol A, Segalin A, et al. Push-through intubation: effective palliation in 409 patients with cancer of the esophagus and cardia. Ann Thorac Surg 1992;53: Hegarty MM, Angorn IB, Bryer JV, Henderson BJ, LeRoux BT, Logan A. Pulsion intubation for palliation of carcinoma of the oesophagus. Br J Surg 1977;64:16G Chisholm RJ, Stoller JL, Carpenter CM, Burhenne HJ. Rasdiologic dilatation preceding palliative surgical tube placement for esophageal cancer. Am J Surg 1986;151: Burt M, Diehl W, Martini N, et al. Malignant esophagorespiratory fistula: management options and survival. Ann Thorac Surg 1991;52: Straumann A, Gyr K, Stalder GA. Occlusion of a malignant oesophago-bronchial fistula with an adhesive anchored endoprosthesis. Schweiz Rundsch Med Prax 1984;73: Robertson CS, Atkinson M. A modified prosthetic oesophageal tube to manage malignant oesophago-respiratory fistula. Lancet 1986;2: Irving JD, Simson JNL. A new cuffed oesophageal prosthesis for the management of malignant oesophago-respiratory fistula. Ann Coll Surg Engl 1988;70: Wang P-Y, Yeh T-J, Chen C-L, Chen C-Y. A spiral-grooved endoesophageal tube for management of malignant esophageal obstruction. Ann Thorac Surg 1985;39:50? Hine KL, Atkinson M. The diagnosis and management of perforations of esophagus and pharynx sustained during intubation of neoplastic esophageal strictures. Dig Dis Sci 1986:31: DISCUSSION DR KAMAL A. MANSOUR (Atlanta, GA): This is a good report in the field of palliation of unresectable carcinoma of the esophagus with or without tracheobronchial invasion. With the 4.5% mortality, 8% obstruction, 9% perforation, and 10% dislodgment reported for other plastic tubes, one is happy to welcome the Montgomery stent described by Dr Warren and his group today. He reported no intraoperative mortality in his experience with 37 patients, excellent relief of obstruction in all 15 such patients, and successful exclusion of esophagorespiratory fistula in all 19 affected patients. I agree with the use of the Montgomery endoesophageal stent in patients with primary unresectable lesions of the esophagus, as the proximal flange of the silicone tube sits on the ragged, irregular edge of the tumor. However, in patients with esophageal strictures caused by extrinsic compression from metastatic lung or breast carcinoma, presumably due to subcarinal node invasion, one wonders what prevents the tube from dislodgment. I also agree with its use in midesophageal lesions; however, for lesions at the distal end, particularly those fixed, unresectable lesions at the gastroesophageal junction, I believe a bypass procedure is preferable, as the tube would angulate because of the axis of the tumor at this location. Through a left thoracotomy, the esophagus is cut above the tumor, then the gastric fundus is brought through the enlarged hiatus and anastomosed to the esophagus. Finally, I have two questions for Dr Warren. First, you performed an esophagogastrectomy on the patient who sustained intraoperative perforation of the esophagus at the time of placement of the stent. Why did you not do that in the first place, as the lesion was evidently resectable to begin with? The second question is: how did you know that the stent was not responsible for the fatal upper gastrointestinal bleeding that occurred in the 2 patients 1 and 2 weeks postoperatively? DR DANIEL L. MILLER (Rochester, MN): I congratulate Dr Warren on his excellent results in an unfortunate group of patients. I have two questions. First, what treatments were used in the 2 patients whose stent placements were unsuccessful? And second, did any of the patients experience respiratory problems after stent placement, and, if so, what was done for them? DR WILLIAM A. COOK (North Andover, MA): There are two other types of esophageal stents available that have not been mentioned, both of which have very useful applications. One is the Wilson-Savary, which is a system that can be placed over a guidewire. In those patients who have very tight strictures, that can be most helpful. Then, of course, there is the grandfather of most of these, and that is the Fell tube, which is designed to be sutured to the wall of the stomach so that it cannot be displaced. One of the problems that exists with the intraesophageal tubes is that, if they go into the stomach, reflux can occur through them and be a troublesome complication. We have found over the years that the end of these tubes can be cut with a V on each!side so that it creates a "fish mouth" at the end of the tubing. This flap will close, more or less like a Heimlich valve closes, and prevent most of the reflux that occurs. Finally, with this Hood-type stent we have found that, even when they do displace, if there is a big enough lumen to reach the stent itself, because of the thinness of the stent wall, you can told up that upper flange and literally back it up to the position where you originally wanted to have it. DR WARREN: I thank the discussants for their thoughtful questions. One of the potential problems with placing these stents across the gastroesophageal junction is reflux. In this series, the stents only bridged this junction in 5 patients who had undergone an esophagogastrectomy previously. None of these patients was troubled by reflux, but this may be a problem in patients who have not undergone a previous resection. In that setting, a Penrose drain can be sutured to the end of the stent to act as a flap, much like a Heimlich valve on a chest tube. Doctor Doug Mathisen told me that he has used that technique with success. Doctor Mansour described a technique to bypass tumors at the gastroesophageal junction as an alternative to stent placement.
6 Ann Thorac Surg 1994;57: WARREN ET AL 1107 SALIVARY STEWS IN THE ESOPHAGUS Our experience with stents in these cases is limited to those 5 patients who had previously undergone an esophagogastrectomy and suffered an anastornotic recurrence. I do not believe that the technique of rolling the fundus up would be applicable in these patients. Doctor Miller, those 2 patients in whom we were unable to place a stent died shortly after the procedure and were not candidates for any other procedure, including laser esophagoscopy. They had very tight strictures resulting from previous irradiation and were very cachectic. I have tried performing laser esophagoscopy as an alternative to stent placement, but I believe that we can achieve faster and longer-lasting palliation by stenting rather photoablating these tumors. The patient who was perforated was 86 years old and led a bed-to-chair existence. He had an extensive tumor of the distal third of the esophagus, which was initially considered unresectable. It was the patient s and his family s wish to avoid major surgery, if possible. Upon performing exploration for the perforation, we were surprised to be able to carry out an esophagogastrectomy. After a stormy postoperative course, he was, in fact, discharged to a nursing home, where he died shortly thereafter. We were unable to get an autopsy to determine the cause of death. The Society of Thoracic Surgeons: Thirty-first Annual Meeting Mark your calendars for the Thirty-first Annual Meeting of The Society of Thoracic Surgeons, which will be held at the Palm Springs Convention Center in Palm Springs, California, January 30-February 1, Members may register for the Scientific Sessions at no charge. There will be a $250 registration fee for nonmember physicians except for Scientific and Poster Session presenters and residents. Registration for the Postgraduate Course is separate from the Annual Meeting. There will be a $65 registration fee for attendees of the Postgraduate Program, which will be held Sunday, January 29. The Postgraduate Course will provide in-depth coverage of thoracic surgical topics selected to enhance and broaden the knowledge of practicing thoracic and cardiac surgeons. Advance registration forms, hotel reservation forms, and details regarding transportation arrangements, as well as the complete meeting program, will be mailed to Society members this fall (1994). Nonmembers wishing to receive information on attending the meeting should write to the Society s Secretary, Richard P. Anderson. Richard P. Anderson, MD Secreta y The Society of Thoracic Surgeons 401 N Michigan Ave Chicago, IL (312)
Therapeutic Bronchoscopy Etiology - Benign Stenosis Post - intubation Trauma Post - operative Inflammatory Idiopathic
 Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Is a Metallic Stent Useful for Non Resectable Esophageal Cancer?
 Original Article Is a Metallic Stent Useful for Non Resectable Esophageal Cancer? Shinsuke Wada, MD, 1 Tsuyoshi Noguchi, MD, 1 Shinsuke Takeno, MD, 1 Hatsuo Moriyama, MD, 1 Tsuyoshi Hashimoto, MD, 1 Yuzo
Original Article Is a Metallic Stent Useful for Non Resectable Esophageal Cancer? Shinsuke Wada, MD, 1 Tsuyoshi Noguchi, MD, 1 Shinsuke Takeno, MD, 1 Hatsuo Moriyama, MD, 1 Tsuyoshi Hashimoto, MD, 1 Yuzo
DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA
 Solunum 3, Özel Sayı 2: 260-264, 2001 DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA Jean F DUMON* M C DUMON* SUMMARY This article reports a 4-year
Solunum 3, Özel Sayı 2: 260-264, 2001 DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA Jean F DUMON* M C DUMON* SUMMARY This article reports a 4-year
S tating disease, and for the vast majority of patients,
 Prospective, Randomized Trial of Palliative Treatment for Unresectablle Cancer of the Esophagus Carolyn E. Reed, MD, William H. Marsh, MD, Leta S. Carlson, MD, Cathy H. Seymore, MD, and John M. Kratz,
Prospective, Randomized Trial of Palliative Treatment for Unresectablle Cancer of the Esophagus Carolyn E. Reed, MD, William H. Marsh, MD, Leta S. Carlson, MD, Cathy H. Seymore, MD, and John M. Kratz,
Pulsion Intubation Versus Traction Intubation for Obstructing Carcinomas of the Esophagus
 Pulsion Intubation Versus Traction Intubation for Obstructing Carcinomas of the Esophagus Helmut W. Unruh, M.D., F.R.C.S.(C), and K. Michael Pagliero, M.B.B.S., F.R.C.S. ABSTRACT Eighty-eight patients
Pulsion Intubation Versus Traction Intubation for Obstructing Carcinomas of the Esophagus Helmut W. Unruh, M.D., F.R.C.S.(C), and K. Michael Pagliero, M.B.B.S., F.R.C.S. ABSTRACT Eighty-eight patients
Department of Thoracic Medicine, Chang Gung Memorial Hospital, Lin-Kuo Branch, Chang Gung Medical Foundation; Abstract
 DOI 10.6314/JIMT.2017.28(4).07 2017 28 243-251 Impacts of Airway Self-expandable Metallic Stent on Ventilator Weaning and Survival of Mechanically Ventilated Patients with Esophageal Cancer and Cental
DOI 10.6314/JIMT.2017.28(4).07 2017 28 243-251 Impacts of Airway Self-expandable Metallic Stent on Ventilator Weaning and Survival of Mechanically Ventilated Patients with Esophageal Cancer and Cental
Esophageal Stenosis Treatment by Interventional Radiology: Indications, Techniques and complications
 Esophageal Stenosis Treatment by Interventional Radiology: Indications, Techniques and complications Poster No.: C-0437 Congress: ECR 2013 Type: Authors: Keywords: DOI: Educational Exhibit M. Leyva Vásquez-Caicedo,
Esophageal Stenosis Treatment by Interventional Radiology: Indications, Techniques and complications Poster No.: C-0437 Congress: ECR 2013 Type: Authors: Keywords: DOI: Educational Exhibit M. Leyva Vásquez-Caicedo,
Owen Dickinson. Consultant in Endoscopy & Interventional Radiology. Upper GI Stenting. Rotherham Foundation Trust
 Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction
 The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
Stenting for Esophageal Cancer Technical Issues and Outcomes
 Stenting for Esophageal Cancer Technical Issues and Outcomes Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Disclosures Research and Educational
Stenting for Esophageal Cancer Technical Issues and Outcomes Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Disclosures Research and Educational
Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City
 Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Endoscopic Palliation of Malignant Dysphagia
 Endoscopic Palliation of Malignant Dysphagia 1. Scope of the guideline This guidance has been produced to support endoscopic palliation of malignant dysphagia from oesophageal cancer. 2. Guideline background
Endoscopic Palliation of Malignant Dysphagia 1. Scope of the guideline This guidance has been produced to support endoscopic palliation of malignant dysphagia from oesophageal cancer. 2. Guideline background
Information Technology Solutions
 2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
ISPUB.COM. Rare Cases: Tracheal/bronchial Obstruction. O Wenker, L Moehn, C Portera, G Walsh HISTORY ADMISSION
 ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control
 ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
Tracheoesophageal Fistula and Esophageal Atresia
 Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Treatment of Esophageal Obstruction With Covered, Self-Expanding Esophageal Wallstents
 Treatment of Esophageal Obstruction With Covered, Self-Expanding Esophageal Wallstents Darroch W. O. Moores, MD, and Riivo Ilves, MD Division of Cardiothoracic Surgery,,, Albany Medical Center; and Department
Treatment of Esophageal Obstruction With Covered, Self-Expanding Esophageal Wallstents Darroch W. O. Moores, MD, and Riivo Ilves, MD Division of Cardiothoracic Surgery,,, Albany Medical Center; and Department
ENDOSCOPIC SELF-EXPANDABLE METAL STENTING FOR ADVANCED CARCINOMA OESOPHAGUS: A BETTER PALLIATIVE PROSPECTIVE
 22 Main Article ENDOSCOPIC SELF-EXPANDABLE METAL STENTING FOR ADVANCED CARCINOMA OESOPHAGUS: A BETTER PALLIATIVE PROSPECTIVE Swagata Khanna 1, Subhash Khanna 2 ABSTRACT: Endoscopic placement of metal stent
22 Main Article ENDOSCOPIC SELF-EXPANDABLE METAL STENTING FOR ADVANCED CARCINOMA OESOPHAGUS: A BETTER PALLIATIVE PROSPECTIVE Swagata Khanna 1, Subhash Khanna 2 ABSTRACT: Endoscopic placement of metal stent
REMOVAL OF IMPACTED DENTURES WITH POLYPECTOMY SNARE
 JMBR: A Peer-review Journal of Biomedical Sciences June 2012, Vol. 11 No.1 pp 14-19 REMOVAL OF IMPACTED DENTURES WITH POLYPECTOMY SNARE *OKUGBO SU, **OKORO E, ***KESIEME E ABSTRACT Impacted dentures have
JMBR: A Peer-review Journal of Biomedical Sciences June 2012, Vol. 11 No.1 pp 14-19 REMOVAL OF IMPACTED DENTURES WITH POLYPECTOMY SNARE *OKUGBO SU, **OKORO E, ***KESIEME E ABSTRACT Impacted dentures have
Imaging of gastric bands and their complications: an educational pictorial review
 Imaging of gastric bands and their complications: an educational pictorial review Poster No.: C-1142 Congress: ECR 2014 Type: Educational Exhibit Authors: F. Moloney, M. Twomey, C. Bogue ; Cork/IE, IE,
Imaging of gastric bands and their complications: an educational pictorial review Poster No.: C-1142 Congress: ECR 2014 Type: Educational Exhibit Authors: F. Moloney, M. Twomey, C. Bogue ; Cork/IE, IE,
Icd 10 code for distal esophageal stricture Address Submit
 Icd 10 code for distal esophageal stricture Email Address Submit If an EGD is performed with a biopsy, and then the physician removes the scope and performs an Esophageal Dilation by unguided sound, it
Icd 10 code for distal esophageal stricture Email Address Submit If an EGD is performed with a biopsy, and then the physician removes the scope and performs an Esophageal Dilation by unguided sound, it
Palliative Treatment of Malignant Esophagopulmonary Fistulas With Covered Expandable Metallic Stents
 Vascular and Interventional Radiology Original Research Vascular and Interventional Radiology Original Research FOCUS ON: Kyung Rae Kim 1,2 Ji Hoon Shin 2 Ho-Young Song 2 Gi-Young Ko 2 Jin Hyoung Kim 2
Vascular and Interventional Radiology Original Research Vascular and Interventional Radiology Original Research FOCUS ON: Kyung Rae Kim 1,2 Ji Hoon Shin 2 Ho-Young Song 2 Gi-Young Ko 2 Jin Hyoung Kim 2
Novatech Products for Interventional Pulmonology
 Novatech Products for Novatech and Boston Medical Products Bringing you the finest products for Novatech is a manufacturer of top-quality medical products used successfully worldwide in the growing specialty
Novatech Products for Novatech and Boston Medical Products Bringing you the finest products for Novatech is a manufacturer of top-quality medical products used successfully worldwide in the growing specialty
The gastric tube is a commonly used reconstruction GENERAL THORACIC SURGERY
 GENERAL THORACIC SURGERY PHARYNGEAL REFLUX AFTER GASTRIC PULL-UP ESOPHAGECTOMY WITH NECK AND CHEST ANASTOMOSES Jan Johansson, MD a Folke Johnsson, MD, PhD a Susan Groshen, PhD b Bruno Walther, MD, PhD
GENERAL THORACIC SURGERY PHARYNGEAL REFLUX AFTER GASTRIC PULL-UP ESOPHAGECTOMY WITH NECK AND CHEST ANASTOMOSES Jan Johansson, MD a Folke Johnsson, MD, PhD a Susan Groshen, PhD b Bruno Walther, MD, PhD
Endoscopic Retrograde Cholangiopancreatography (ERCP)
 Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Achalasia and Laparoscopic Heller Myotomy
 1 Monterey County Surgical Associates 2 Upper Ragsdale Drive, Bldg B, Suite 230 Monterey, CA 93940 Phone: (831) 649-0808 Fax: (831) 649-8795 Mark Vierra, MD Achalasia and Laparoscopic Heller Myotomy Introduction
1 Monterey County Surgical Associates 2 Upper Ragsdale Drive, Bldg B, Suite 230 Monterey, CA 93940 Phone: (831) 649-0808 Fax: (831) 649-8795 Mark Vierra, MD Achalasia and Laparoscopic Heller Myotomy Introduction
Peroral Esophageal Intubation for Obstructive Carcinoma of the Esophagus
 Peroral Esophageal Intubation for Obstructive Carcinoma of the Esophagus Ralph J. Lewis, M.D., Philip J. Kunderman, M.D., Glenn E. Sisler, M.D., and James W. Mackenzie, M.D. ABSTRACT Seventeen patients
Peroral Esophageal Intubation for Obstructive Carcinoma of the Esophagus Ralph J. Lewis, M.D., Philip J. Kunderman, M.D., Glenn E. Sisler, M.D., and James W. Mackenzie, M.D. ABSTRACT Seventeen patients
Expandable stents in digestive pathology present use in an emergency hospital
 ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
Danis Procedure Pack - BASIC
 Danis Procedure Pack - BASIC Manufactured by: ELLA CS, s.r.o. Milady Horákové 504 500 06 Hradec Králové 6 Czech Republic Phone: +420 49 527 91 11 Fax: +420 49 526 56 55 E-mail: volenec@ellacs.eu Danis
Danis Procedure Pack - BASIC Manufactured by: ELLA CS, s.r.o. Milady Horákové 504 500 06 Hradec Králové 6 Czech Republic Phone: +420 49 527 91 11 Fax: +420 49 526 56 55 E-mail: volenec@ellacs.eu Danis
External trauma (MVA, surf board, assault, etc.) Internal trauma (Endotracheal intubation, tracheostomy) Other
 Etiology External trauma (MVA, surf board, assault, etc.) Internal trauma (Endotracheal intubation, tracheostomy) Other Systemic diseases (vasculitis, etc.) Chemo/XRT Idiopathic Trans nasal Esophagoscope
Etiology External trauma (MVA, surf board, assault, etc.) Internal trauma (Endotracheal intubation, tracheostomy) Other Systemic diseases (vasculitis, etc.) Chemo/XRT Idiopathic Trans nasal Esophagoscope
Esophageal injuries. Pre-test /11/10. 新光急診張志華醫師 Facebook.com/jack119. O What is the most common cause of esophageal injuries?
 Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 O What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic 1 Pre-test 2 O Which contrast
Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 O What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic 1 Pre-test 2 O Which contrast
Polyflex Expandable Stents in the Treatment of Esophageal Disease: Initial Experience
 GENERAL THORACIC Polyflex Expandable Stents in the Treatment of Esophageal Disease: Initial Experience Arjun Pennathur, MD, Andrew C. Chang, MD, Kevin M. McGrath, MD, Gregory Steiner, BS, Miguel Alvelo-Rivera,
GENERAL THORACIC Polyflex Expandable Stents in the Treatment of Esophageal Disease: Initial Experience Arjun Pennathur, MD, Andrew C. Chang, MD, Kevin M. McGrath, MD, Gregory Steiner, BS, Miguel Alvelo-Rivera,
Since central airway stenosis is often a lifethreatening. Double Y-stenting for tracheobronchial stenosis. Masahide Oki and Hideo Saka
 Eur Respir J 2012; 40: 1483 1488 DOI: 10.1183/09031936.00015012 CopyrightßERS 2012 Double Y-stenting for tracheobronchial stenosis Masahide Oki and Hideo Saka ABSTRACT: The purpose of the present study
Eur Respir J 2012; 40: 1483 1488 DOI: 10.1183/09031936.00015012 CopyrightßERS 2012 Double Y-stenting for tracheobronchial stenosis Masahide Oki and Hideo Saka ABSTRACT: The purpose of the present study
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Combined Collis-Nissen Reconstruction. of the esophagogastric junction at. Mark B. Orringer, M.D., and Herbert Sloan, M.D.
 Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Double Y-stenting for tracheobronchial stenosis
 ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
Bidirectional esophageal dilatation in pharyngoesophageal stenosis postradiotherapy
 OPERATIVE TECHNIQUES PICTORIAL ESSAY Bidirectional esophageal dilatation in pharyngoesophageal stenosis postradiotherapy Haim Gavriel, MD,* Cuong Duong, MB, BS, PhD, FRACS, John Spillane, MB, BS, FRACS,
OPERATIVE TECHNIQUES PICTORIAL ESSAY Bidirectional esophageal dilatation in pharyngoesophageal stenosis postradiotherapy Haim Gavriel, MD,* Cuong Duong, MB, BS, PhD, FRACS, John Spillane, MB, BS, FRACS,
Esophageal injuries. 新光急診張志華醫師 Facebook.com/jack119
 Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Esophageal Cancer. Source: National Cancer Institute
 Esophageal Cancer Esophageal cancer forms in the tissues that line the esophagus, or the long, hollow tube that connects the mouth and stomach. Food and drink pass through the esophagus to be digested.
Esophageal Cancer Esophageal cancer forms in the tissues that line the esophagus, or the long, hollow tube that connects the mouth and stomach. Food and drink pass through the esophagus to be digested.
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: What is the treatment
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: What is the treatment
GIT RADIOLOGY. Water-soluble contrast media (e.g. gastrograffin) are the other available agents.which doesn t cause inflammatory peritonitis..
 GIT RADIOLOGY Imaging techniques-general principles: Contrast examinations: Barium sulphate is the best contrast for GIT (with good mucosal coating & excellent opacification & being inert); but is contraindicated
GIT RADIOLOGY Imaging techniques-general principles: Contrast examinations: Barium sulphate is the best contrast for GIT (with good mucosal coating & excellent opacification & being inert); but is contraindicated
Foreign Body Management
 Foreign Body Management NYSGE Fellows Summer Course Susana Gonzalez, MD Assistant Professor of Medicine 1 Objectives Timing of endoscopy When? Anatomic location Where? High risk objects What? Choosing
Foreign Body Management NYSGE Fellows Summer Course Susana Gonzalez, MD Assistant Professor of Medicine 1 Objectives Timing of endoscopy When? Anatomic location Where? High risk objects What? Choosing
Rigid Bronchoscopic Intervention in Patients with Respiratory Failure Caused by Malignant Central Airway Obstruction
 ORIGINAL ARTICLE Rigid Bronchoscopic Intervention in Patients with Respiratory Failure Caused by Malignant Central Airway Obstruction Kyeongman Jeon, MD, Hojoong Kim, MD, Chang-Min Yu, MD, Won-Jung Koh,
ORIGINAL ARTICLE Rigid Bronchoscopic Intervention in Patients with Respiratory Failure Caused by Malignant Central Airway Obstruction Kyeongman Jeon, MD, Hojoong Kim, MD, Chang-Min Yu, MD, Won-Jung Koh,
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction
 A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
Case Report. Management of recurrent distal tracheal stenosis using an endoprosthesis: a case report* Abstract. Introduction.
 121 Case Report Management of recurrent distal tracheal stenosis using an endoprosthesis: a case report* André Germano Leite 1, Douglas Kussler 2 Abstract The authors report the case of a patient with
121 Case Report Management of recurrent distal tracheal stenosis using an endoprosthesis: a case report* André Germano Leite 1, Douglas Kussler 2 Abstract The authors report the case of a patient with
(a) (b) Plate 16.1 Esophageal tear after passage of the echoendoscope.
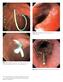 Plate 16.1 Esophageal tear after passage of the echoendoscope. Plate 11.1 Prophylactic pancreatic duct stents. 3-Fr, 4-cm long single-pigtail stent. 5-Fr, 3-cm long flanged stent. Plate 16.2 Esophageal
Plate 16.1 Esophageal tear after passage of the echoendoscope. Plate 11.1 Prophylactic pancreatic duct stents. 3-Fr, 4-cm long single-pigtail stent. 5-Fr, 3-cm long flanged stent. Plate 16.2 Esophageal
Long-gap Oesophageal Atresia
 Long-gap Atresia A guide for parents Nate (6 weeks old) Atresia Research Association Are there different types of OA? There are four main types of oesophageal atresia with or without TOF. These include
Long-gap Atresia A guide for parents Nate (6 weeks old) Atresia Research Association Are there different types of OA? There are four main types of oesophageal atresia with or without TOF. These include
Endoscopic Treatment of Luminal Perforations and Leaks
 Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endobronchial Management of Benign, Malignant, and Lung Transplantation Airway Stenoses
 Endobronchial Management of Benign, Malignant, and Lung Transplantation Airway Stenoses Joshua R. Sonett, MD, Robert J. Keenan, MD, Peter F. Ferson, MD, Bartley P. Griffith, MD, and Rodney J. Landreneau,
Endobronchial Management of Benign, Malignant, and Lung Transplantation Airway Stenoses Joshua R. Sonett, MD, Robert J. Keenan, MD, Peter F. Ferson, MD, Bartley P. Griffith, MD, and Rodney J. Landreneau,
Esophageal Dilatation (Bouginage)
 Esophageal Dilatation (Bouginage) Pages with reference to book, From 20 To 23 Ziauddin Shamsi, M. Aftab Anwar ( 5/16, Rimpa Plaza, M.A. Jinnah Road, Karachi. ) Esophageal dilatation is very important addition
Esophageal Dilatation (Bouginage) Pages with reference to book, From 20 To 23 Ziauddin Shamsi, M. Aftab Anwar ( 5/16, Rimpa Plaza, M.A. Jinnah Road, Karachi. ) Esophageal dilatation is very important addition
Clinical evaluation of treating an advanced esophageal carcinoma by using membrane-covered metallic stent
 Clinical evaluation of treating an advanced esophageal carcinoma by using membrane-covered metallic stent Xu meidong, Yao liqing, Zhong yunshi et al. Department of Endoscopy Center, Zhongshan Hospital,
Clinical evaluation of treating an advanced esophageal carcinoma by using membrane-covered metallic stent Xu meidong, Yao liqing, Zhong yunshi et al. Department of Endoscopy Center, Zhongshan Hospital,
Esophageal Stents May Interfere with the Swallowing Reflex: An Illustrative Case History
 254 Journal of Pain and Symptom Management Vol. 16 No. 4 October 1998 Original Article Esophageal Stents May Interfere with the Swallowing Reflex: An Illustrative Case History Angel Lee, MRCP (UK), and
254 Journal of Pain and Symptom Management Vol. 16 No. 4 October 1998 Original Article Esophageal Stents May Interfere with the Swallowing Reflex: An Illustrative Case History Angel Lee, MRCP (UK), and
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
WallFlex Stents Technique Spotlights
 WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
Combined airway and oesophageal stenting in malignant airway oesophageal fistulas: a prospective study
 Eur Respir J 2010; 36: 1370 1374 DOI: 10.1183/09031936.00049809 CopyrightßERS 2010 Combined airway and oesophageal stenting in malignant airway oesophageal fistulas: a prospective study F.J.F. Herth*,+,
Eur Respir J 2010; 36: 1370 1374 DOI: 10.1183/09031936.00049809 CopyrightßERS 2010 Combined airway and oesophageal stenting in malignant airway oesophageal fistulas: a prospective study F.J.F. Herth*,+,
Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W.
 UvA-DARE (Digital Academic Repository) Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W. Link to publication Citation for published version (APA): van den Berg, M. W.
UvA-DARE (Digital Academic Repository) Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W. Link to publication Citation for published version (APA): van den Berg, M. W.
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)?
 WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
The first stents designed for use in the biliary tree and
 Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Case Scenario 1. The patient has now completed his neoadjuvant chemoradiation and has been cleared for surgery.
 Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
TRACHEOBRONCHIAL FOREIGN BODY REMOVAL ADVICE IN DOGS AND CATS
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TRACHEOBRONCHIAL FOREIGN BODY REMOVAL ADVICE IN DOGS AND CATS Author : MIKE STAFFORD-JOHNSON, MIKE MARTIN Categories : Vets
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TRACHEOBRONCHIAL FOREIGN BODY REMOVAL ADVICE IN DOGS AND CATS Author : MIKE STAFFORD-JOHNSON, MIKE MARTIN Categories : Vets
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
CASE REPORTS. Giant Esophagus. An Unusual Case of Massive Idiopathic Hypertrophy
 CASE REPORTS An Unusual Case of Massive Idiopathic Hypertrophy and Dilatation of the Esophagus and Proximal Stomach Mark H. Wall, M.D., Epifanio E. Espinas, M.D., Arthur W. Silver, M.D., and Francis X.
CASE REPORTS An Unusual Case of Massive Idiopathic Hypertrophy and Dilatation of the Esophagus and Proximal Stomach Mark H. Wall, M.D., Epifanio E. Espinas, M.D., Arthur W. Silver, M.D., and Francis X.
Bactereda after Esophageal Dilation:
 Bactereda after Esophageal Dilation: A Clinical and Experimental Study E. S. Golladay, M.D., J. J. Tepas 111, M.D., L. R. Pickard, M.D., J. J. Seibert, M.D., R. W. Brown, M.D., and J. Alex Haller, Jr.,
Bactereda after Esophageal Dilation: A Clinical and Experimental Study E. S. Golladay, M.D., J. J. Tepas 111, M.D., L. R. Pickard, M.D., J. J. Seibert, M.D., R. W. Brown, M.D., and J. Alex Haller, Jr.,
A video demonstration of the Li s anastomosis the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma
 Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient
 CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient Purpose: To control bleeding from esophageal or gastric varices that have not responded to medical therapy (ie. Sclerotherapy,
CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient Purpose: To control bleeding from esophageal or gastric varices that have not responded to medical therapy (ie. Sclerotherapy,
Alyssa Brzenski MD May 2, 2012
 Alyssa Brzenski MD May 2, 2012 Overview Background Pre repair bronchoscopy Thorascopic repair To extubate or not? Esophageal atresia treatment of long gap esophageal atresia Complications following TEF/EA
Alyssa Brzenski MD May 2, 2012 Overview Background Pre repair bronchoscopy Thorascopic repair To extubate or not? Esophageal atresia treatment of long gap esophageal atresia Complications following TEF/EA
Postoperative esophageal leak management with the Polyflex esophageal stent
 Freeman, Ascioti, and Wozniak General Thoracic Surgery Postoperative esophageal leak management with the Polyflex esophageal stent Richard K. Freeman, MD, a Anthony J. Ascioti, MD, a and Thomas C. Wozniak,
Freeman, Ascioti, and Wozniak General Thoracic Surgery Postoperative esophageal leak management with the Polyflex esophageal stent Richard K. Freeman, MD, a Anthony J. Ascioti, MD, a and Thomas C. Wozniak,
Having a PEG tube inserted
 Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Acquired oesophageal strictures in children: emphasis on the use of string - guided dilatations
 82 Original Article Acquired oesophageal strictures in children: emphasis on the use of string - guided dilatations Saleem M M ABSTRACT Introduction: Acquired oesophageal strictures are common in children.
82 Original Article Acquired oesophageal strictures in children: emphasis on the use of string - guided dilatations Saleem M M ABSTRACT Introduction: Acquired oesophageal strictures are common in children.
CPT COD1NG UPDATES Gastroenterology CPT Advisors
 2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
Quiz Adenocarcinoma of the distal stomach has been increasing in the last 20 years. a. True b. False
 Quiz 1 1. Which of the following are risk factors for esophagus cancer. a. Obesity b. Gastroesophageal reflux c. Smoking and Alcohol d. All of the above 2. Adenocarcinoma of the distal stomach has been
Quiz 1 1. Which of the following are risk factors for esophagus cancer. a. Obesity b. Gastroesophageal reflux c. Smoking and Alcohol d. All of the above 2. Adenocarcinoma of the distal stomach has been
Introduction to Interventional Pulmonology
 Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL. September 17, Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous
 Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Case Report Reoperation for complicated tracheoesophageal fistula after surgery of a tracheal lymphoma
 Int J Clin Exp Med 2017;10(6):9659-9663 www.ijcem.com /ISSN:1940-5901/IJCEM0051182 Case Report Reoperation for complicated tracheoesophageal fistula after surgery of a tracheal lymphoma Wei Dai 1, Qiang
Int J Clin Exp Med 2017;10(6):9659-9663 www.ijcem.com /ISSN:1940-5901/IJCEM0051182 Case Report Reoperation for complicated tracheoesophageal fistula after surgery of a tracheal lymphoma Wei Dai 1, Qiang
Complication of Percutaneous Endoscopic Gastrostomy
 Complication of Percutaneous Endoscopic Gastrostomy Tube Ogori N. Kalu MD Morbidity & Mortality Conference General Surgery Service Kings County Hospital Center ACGME Core Competencies 1. Medical knowledge
Complication of Percutaneous Endoscopic Gastrostomy Tube Ogori N. Kalu MD Morbidity & Mortality Conference General Surgery Service Kings County Hospital Center ACGME Core Competencies 1. Medical knowledge
PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
 Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER AUGMENTATION FOR THE TREATMENT OF GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
4/24/2017. Tracheal Stenosis. Tracheal Stenosis. Tracheal Stenosis. Tracheal Stenosis. Tracheal Stenosis Endoscopic & Surgical Management
 Endoscopic & Surgical Management Pressure ulceration Healing: granulation cicatrization contraction Ann Surg 1969;169:334-348 Gary Schwartz, MD Department of Thoracic Surgery and Lung Transplantation Baylor
Endoscopic & Surgical Management Pressure ulceration Healing: granulation cicatrization contraction Ann Surg 1969;169:334-348 Gary Schwartz, MD Department of Thoracic Surgery and Lung Transplantation Baylor
Medical Illustration PLME 0400
 Introduction to Medical Illustration PLME 0400 October 17 From sketch to narrative From Sketch to Sketch: Point of view Degree of detail Visible and invisble parts Landmarks : Plan your moves The IKEA
Introduction to Medical Illustration PLME 0400 October 17 From sketch to narrative From Sketch to Sketch: Point of view Degree of detail Visible and invisble parts Landmarks : Plan your moves The IKEA
DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER
 November 2015 DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER 1 Background... 3 2 Dysphagia Grading... 3 3 Dysphagia General Guidelines... 4 4 Modes of Managing Dysphagia... 4 4.1 Modified consistency diet...
November 2015 DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER 1 Background... 3 2 Dysphagia Grading... 3 3 Dysphagia General Guidelines... 4 4 Modes of Managing Dysphagia... 4 4.1 Modified consistency diet...
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Departement of Surgery Faculty of Medicine University Sumatera Utara
 SSS EESOPHAGEAL HPOSAGEAL DISORDERS IN SURGICAL PERSPECTIVE Departement of Surgery Faculty of Medicine University Sumatera Utara CONTENT 1. Esophageal Atresia 2. Achalasia 3. Esophageal Rupture 4. Tumor
SSS EESOPHAGEAL HPOSAGEAL DISORDERS IN SURGICAL PERSPECTIVE Departement of Surgery Faculty of Medicine University Sumatera Utara CONTENT 1. Esophageal Atresia 2. Achalasia 3. Esophageal Rupture 4. Tumor
Douglas G. Adler MD. ACG Regional Postgraduate Course - Nashville, TN Copyright 2013 American College of Gastroenterology
 Enteral Stents 2013: State of the Art Douglas G. Adler MD Associate Professor of Medicine Director of Therapeutic Endoscopy University of Utah School of Medicine Huntsman Cancer Center Esophageal Stents
Enteral Stents 2013: State of the Art Douglas G. Adler MD Associate Professor of Medicine Director of Therapeutic Endoscopy University of Utah School of Medicine Huntsman Cancer Center Esophageal Stents
Palliative intubation of oesophagogastric neoplasms at fibreoptic endoscopy
 Gut, 1982, 23, 1060-1067 Palliative intubation of oesophagogastric neoplasms at fibreoptic endoscopy A L OGILVIE,* M W DRONFIELD,t R FERGUSON,t and M ATKINSON From the University Hospital, Queen's Medical
Gut, 1982, 23, 1060-1067 Palliative intubation of oesophagogastric neoplasms at fibreoptic endoscopy A L OGILVIE,* M W DRONFIELD,t R FERGUSON,t and M ATKINSON From the University Hospital, Queen's Medical
Covered stenting in patients with lifting of gastric and high esophago-tracheal fistula
 European Radiology Springer-Verlag 2003 DOI 10.1007/s00330-002-1818-z Tips and Tricks in Radiology Covered stenting in patients with lifting of gastric and high esophago-tracheal fistula T. Lehnert J.
European Radiology Springer-Verlag 2003 DOI 10.1007/s00330-002-1818-z Tips and Tricks in Radiology Covered stenting in patients with lifting of gastric and high esophago-tracheal fistula T. Lehnert J.
Interventional Pulmonology
 Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia
 National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia Patient Details Surname: NHS number: Forename: Postcode: Sex: Male Female
National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia Patient Details Surname: NHS number: Forename: Postcode: Sex: Male Female
Carcinoma of the Lung
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
Airway Remodeling: Preliminary Experience with Bio-Absorbable Airway Stents in Adults Jaus MO, Gonfiotti A, Barale D, Macchiarini P
 Airway Remodeling: Preliminary Experience with Bio-Absorbable Airway Stents in Adults Jaus MO, Gonfiotti A, Barale D, Macchiarini P University Hospital Careggi Florence, Italy Disclosure Statement THE
Airway Remodeling: Preliminary Experience with Bio-Absorbable Airway Stents in Adults Jaus MO, Gonfiotti A, Barale D, Macchiarini P University Hospital Careggi Florence, Italy Disclosure Statement THE
ST-513-S ST-514-S 15ST-515-S
 Urmee Healthcare G-1, sho Plalav, (Jwala Estate), Opp. Flyover ridge, S. V. Road, orivali (W), Mumbai - 0 02. INDI +1 22 2 1, 4 5 Telefax : +1 22 2053 Email : deena@vsnl.com LRYNGOLOGY Hood Tracheal T-Tube
Urmee Healthcare G-1, sho Plalav, (Jwala Estate), Opp. Flyover ridge, S. V. Road, orivali (W), Mumbai - 0 02. INDI +1 22 2 1, 4 5 Telefax : +1 22 2053 Email : deena@vsnl.com LRYNGOLOGY Hood Tracheal T-Tube
ReShape Integrated Dual Balloon System Procedure Manual
 ReShape Integrated Dual Balloon System Procedure Manual 1 TABLE OF CONTENTS Introduction... 3 Product Description... 3 Overview... 3 Component description... 4 Intragastric Balloon... 4 Placement Catheter...
ReShape Integrated Dual Balloon System Procedure Manual 1 TABLE OF CONTENTS Introduction... 3 Product Description... 3 Overview... 3 Component description... 4 Intragastric Balloon... 4 Placement Catheter...
Results of Expandable Metal Stents for Malignant Esophageal Obstruction in 100 Patients: Short-Term and Long-Term Follow-up
 Results of Expandable Metal Stents for Malignant Esophageal Obstruction in 100 Patients: Short-Term and Long-Term Follow-up Neil A. Christie, MD, Percival O. Buenaventura, MD, Hiran C. Fernando, MD, Ninh
Results of Expandable Metal Stents for Malignant Esophageal Obstruction in 100 Patients: Short-Term and Long-Term Follow-up Neil A. Christie, MD, Percival O. Buenaventura, MD, Hiran C. Fernando, MD, Ninh
Basic Principles of Esophageal Surgery. 1 Surgical Anatomy of the Esophagus... 3
 Contents Basic Principles of Esophageal Surgery 1 Surgical Anatomy of the Esophagus... 3 D. C. Broering, J. Walter, Z. Halata ] Topography of the esophagus... 3 ] Development of the esophagus... 4 ] Structure
Contents Basic Principles of Esophageal Surgery 1 Surgical Anatomy of the Esophagus... 3 D. C. Broering, J. Walter, Z. Halata ] Topography of the esophagus... 3 ] Development of the esophagus... 4 ] Structure
EGD Data Collection Form
 Sociodemographic Information Type Zip Code Gender Height (in inches) Race Ethnicity Inpatient Outpatient Male Female Birth Date Weight (in pounds) American Indian (Native American) or Alaska Native Asian
Sociodemographic Information Type Zip Code Gender Height (in inches) Race Ethnicity Inpatient Outpatient Male Female Birth Date Weight (in pounds) American Indian (Native American) or Alaska Native Asian
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
Esophageal Bypass Using a Gastric Tube for a Malignant Tracheoesophageal/ Bronchoesophageal Fistula: A Report of 4 Cases
 Int Surg 2011;96:189 193 Case Report Esophageal Bypass Using a Gastric Tube for a Malignant Tracheoesophageal/ Bronchoesophageal Fistula: A Report of 4 Cases Takeshi Hanagiri, Masaru Morita, Yoshiki Shigematsu,
Int Surg 2011;96:189 193 Case Report Esophageal Bypass Using a Gastric Tube for a Malignant Tracheoesophageal/ Bronchoesophageal Fistula: A Report of 4 Cases Takeshi Hanagiri, Masaru Morita, Yoshiki Shigematsu,
Use of Magill Forceps to Remove Foreign Bodies in Children
 THIEME Original Article e91 Use of Magill Forceps to Remove Foreign Bodies in Children Murat Oncel, MD 1 Guven Sadi Sunam, MD 1 Cagdas Elsurer, MD 2 Huseyin Yildiran, MD 1 1 Department of Thoracic Surgery,
THIEME Original Article e91 Use of Magill Forceps to Remove Foreign Bodies in Children Murat Oncel, MD 1 Guven Sadi Sunam, MD 1 Cagdas Elsurer, MD 2 Huseyin Yildiran, MD 1 1 Department of Thoracic Surgery,
Clinical Case Presentation. Jared B. Smith, M.D. Surgical Grand Rounds, August 21, 2006
 Clinical Case Presentation Jared B. Smith, M.D. Surgical Grand Rounds, August 21, 2006 Clinical History CC: Can t swallow anything HPI: 50 y.o. male from western Colorado, greater than 2 years of emesis
Clinical Case Presentation Jared B. Smith, M.D. Surgical Grand Rounds, August 21, 2006 Clinical History CC: Can t swallow anything HPI: 50 y.o. male from western Colorado, greater than 2 years of emesis
