Detection of inborn errors of metabolism in the newborn
|
|
|
- Barbara Blankenship
- 5 years ago
- Views:
Transcription
1 Arch Dis Child Fetal Neonatal Ed 2001;84:F205 F210 F205 REVIEW Willink Biochemical Genetics Unit, Manchester M27 4HA, UK A Chakrapani M A Cleary J E Wraith Correspondence to: Dr Cleary maureen@willink.demon.co.uk Accepted 17 November 2000 Detection of inborn errors of metabolism in the newborn A Chakrapani, M A Cleary, J E Wraith It is important for paediatricians and neonatologists to keep in mind inborn errors of metabolism (IEMs) as a cause of illness in the neonatal period, as many disorders are treatable and, in most cases, successful outcome is dependent on a rapid diagnosis and early instigation of therapy. Even with untreatable disorders, it is important to establish the diagnosis in the index case in order to allow prenatal diagnosis in subsequent pregnancies. In desperately sick neonates for whom no diagnosis is readily available, IEMs are near the top of the list of diverential diagnoses. IEMs can present in the newborn in a variety of ways. Typically, an IEM is suspected as a result of a suggestive combination of acute clinical symptoms without any prior warning. However, sometimes non-specific clues exist, such as a previous unexplained neonatal death and, in some families, the risk of an IEM is already highlighted by the presence of a previously avected child. IEMs may be detected through the newborn screening programme, though at present phenylketonuria is the only disorder for which mass screening is accepted in the UK. Some IEMs result in dysmorphism, and the investigation of these cases is not complete without considering metabolic causes. Finally, disorders that normally manifest in older children may sometimes cause abnormalities in the newborn period. Pathogenesis of IEMs placental protection Like all genetic disorders, IEMs are present from conception, and most defective enzymes are active in fetal life. Nevertheless, most conditions have no adverse consequences on the fetus, as the placenta provides an evective dialysis system for the removal of toxic metabolites. Thus most babies with an IEM are born in good condition and of normal birth weight. Some IEMs, such as galactosaemia, manifest only after the substrate for the deficient enzyme becomes available in the form of feeds. There are some exceptions to this concept of placental protection ; for example, disorders that avect energy metabolism, such as the primary lactic acidoses and glutaric aciduria type II or non-ketotic hyperglycinaemia where the primary defect is in cerebral intermediary metabolism and the substrate accumulation in body fluids represents an overflow from the brain. Clinical presentation of IEMs Maintaining a high index of suspicion of metabolic disease in an ill neonate is essential, and it must be borne in mind that some disorders, such as galactosaemia, can predispose to Gram negative septicaemia. The first step in the recognition of IEMs is a careful scrutiny of the family history and the obstetric notes. The majority of metabolic disorders presenting in the neonatal period are autosomal recessive, and thus a history of parental consanguinity can be a helpful clue. A few metabolic conditions are associated with maternal problems during pregnancies carrying avected fetuses. It has recently been recognised that some fetal disorders of fatty acid oxidation can predispose the mother to developing acute fatty liver of pregnancy (AFLP) and the HELLP syndrome of haemolysis, elevated liver enzymes, and low platelet count. 1 2 Steroid sulphatase deficiency can cause prolonged labour as a result of decreased placental oestrogen production, 3 and conditions associated with renal pathology can result in oligohydramnios. PATTERNS OF PRESENTATION Neurological abnormalities encephalopathy and seizures Two general patterns of presentation can be distinguished. The first is a baby, apparently healthy at birth, who after a symptom free interval develops non-specific symptoms such as lethargy, poor feeding, vomiting, or irritability. Metabolic acidosis, altered sensorium, convulsions, and hyperammonaemic coma become apparent soon afterwards. Normal ammonia concentrations in neonates are less than 65 µmol/l, 4 but we have frequently observed concentrations of up to 180 µmol/l in sick newborns. Higher ammonia concentrations warrant thorough investigation for metabolic causes. The organic acidaemias (propionic, methylmalonic, and isovaleric acidaemia) and the urea cycle defects classically present in this manner, and in either case respiratory alkalosis may be the initial acid base disturbance. 5 6 Maple syrup urine disease (MSUD) is a possibility when acid base disturbances and hyperammonaemia are not prominent features. The likelihood of a metabolic disorder is very high in the presence of ketonuria, as neonates otherwise do not readily produce ketones.
2 F206 Chakrapani, Cleary, Wraith The second pattern of involvement is a neonate who has overwhelming neurological illness with unconsciousness, convulsions, and apnoea in the absence of significant hyperammonaemia and acid base disturbances, and without an apparent symptom free interval. The diverential diagnosis includes non-ketotic hyperglycinaemia, molybdenum cofactor deficiency, pyridoxine dependent seizures, and the primary lactic acidoses. Mitochondrial and peroxisomal disorders can also present in this manner, and often result in severe hypotonia, with or without dysmorphism and congenital anomalies. Metabolic acidosis Unexplained, persistent metabolic acidosis is a common feature of IEMs that present neonatally. Calculation of the anion gap can be helpful, as conditions that cause acidosis with a normal anion gap are limited to those associated with renal and intestinal bicarbonate loss. The organic acidaemias and the primary lactic acidoses cause metabolic acidosis with a raised anion gap in the early stages. Most metabolic conditions result in acidosis in the late stages as encephalopathy and circulatory disturbances progress. Lactic acidosis Infants with lactic acidosis present a diycult diagnostic problem. A high plasma lactate can be secondary to hypoxia, cardiac disease, infection, or convulsions, whereas primary lactic acidosis may be caused by disorders of pyruvate metabolism and respiratory chain defects. Some IEMs (fatty acid oxidation disorders, organic acidaemias, and urea cycle defects) may also be associated with a secondary lactic acidosis. 7 As venous obstruction by tourniquet, crying, or breath holding may increase plasma lactate concentrations by two- to threefold, arterial samples are more reliable. Persistent increase of plasma lactate above 3 mmol/l in a neonate who was not asphyxiated and who has no evidence of other organ failure should lead to further investigations for an IEM. The lactic acidoses are a heterogeneous group of disorders, and many defects are tissue specific (for example, limited to muscle or the CNS). Often the infant dies without a diagnosis, and it is essential to collect the correct skin, muscle, and liver samples for enzyme and DNA analyses. Hypoglycaemia Inborn errors of metabolism should be considered in all patients with hypoglycaemia in the newborn period although most patients will turn out to have a diverent diagnosis. Samples should be collected during an episode of hypoglycaemia if possible. Fat oxidation defects, the hepatic forms of glycogen storage disease, and disorders of gluconeogenesis such as fructose-1,6 bisphosphatase deficiency can present in this way. An IEM that primarily avects liver function (see below) can also result in secondary hypoglycaemia. Cardiac disease Cardiac failure, particularly in the presence of hypertrophic cardiomyopathy and hypotonia, may suggest a mitochondrial respiratory chain defect, a long chain fatty acid oxidation disorder, or Pompe s disease (GSD II). Other lysosomal disorders may also be associated with cardiac disease, but dysmorphism is usually the revealing symptom (see below). The multisystem congenital disorders of glycosylation (CDG) can present soon after birth with cardiomyopathy and/or pericardial evusion. 8 Additional features include failure to thrive, facial dysmorphism, inverted nipples, and abnormal fat distribution. 9 X linked dilated cardiomyopathy and neutropenia (Barth syndrome) is a recently described entity with characteristic abnormalities on urine organic acid analysis. 10 Cardiac arrhythmias, with or without cardiomyopathy, have been described in most of these conditions. Liver dysfunction Galactosaemia is the commonest metabolic cause of liver dysfunction in the newborn period. Besides signs of liver disease, early onset cataracts are very suggestive. Other rarer IEMs such as hepatorenal tyrosinaemia, α 1 antitrypsin deficiency, neonatal haemochromatosis, and mitochondrial respiratory chain disorders must also be considered in the diverential diagnosis. Niemann Pick disease type C (NPC) is a lipid storage disorder that results from a defect of intracellular cholesterol esterification, and classically presents with neurodegenerative manifestations in childhood. 11 A significant proportion of patients, however, have neonatal manifestations with variable degrees of cholestasis, liver dysfunction, and hepatosplenomegaly, well before the onset of neurological illness. 12 Dysmorphism Besides CDG, other metabolic conditions can manifest with dysmorphism; for example, disorders that avect energy metabolism directly (pyruvate dehydrogenase deficiency, glutaric aciduria type II) or indirectly (3- hydroxyisobutyric aciduria) can result in various physical malformations including facial dysmorphism, and cardiac, renal, and skeletal defects. The disorders of peroxisomal biogenesis (the Zellweger spectrum ) can present with hypotonia associated with facial features resembling Down s syndrome. Patients with lysosomal disorders usually appear normal in early infancy, but some conditions (GM1 gangliosidosis, I-cell disease, and infantile sialic acid storage disease) can manifest in the first weeks of life with coarse facies, upper airway obstruction, and cardiac dysfunction. Severe defects in cholesterol synthesis (Smith Lemli Opitz syndrome, X linked chondrodysplasia punctata, and mevalonic aciduria) can also present with characteristic dysmorphic features and multiple anomalies. Other suggestive abnormalities Abnormal body odour is noted in some organic acidaemias, for example, the smell of maple syrup in maple syrup urine disease, and of sweaty feet in isovaleric acidaemia and glutaric aciduria type II. Most babies who have an unusual or powerful odour, however, do not have
3 Detection of inborn errors of metabolism in the newborn F207 Table 1 Metabolic conditions associated with hydrops fetalis Lysosomal disorders Mucopolysaccharidosis types IV and VII Gaucher disease type II GM1 gangliosidosis Niemann Pick disease type C Farber disease Infantile free sialic acid storage disease Sialidosis Galactosialidosis Mucolipidosis II (I cell disease) RBC enzyme abnormalities Glucose-6-phosphate dehydrogenase deficiency Pyruvate kinase deficiency Glucosephosphate isomerase deficiency Neonatal haemochromatosis Respiratory chain disorders Congenital disorders of glycosylation Glycogen storage disease type IV an IEM. Temperature instability has many common causes, but is also an early feature of Menke s syndrome. Non-immune hydrops fetalis can be associated with a number of metabolic disorders (table 1) Jaundice and bleeding diathesis occur in disorders that avect liver function, but may also be a late sign in other IEMs such as the urea cycle defects. Investigation of a neonate who may have an IEM As a wide variety of IEMs can present in the neonate, the level of clinical and biochemical experience required for their diagnosis and treatment is substantial. It is essential to discuss investigations with all the laboratories involved and to give some indication of urgency. Appropriate transportation to the metabolic laboratory must be arranged, and as much clinical information as possible must be provided on the request cards. The interpretation of many metabolic investigations can be confounded by medications and special feeds, hence a full drug and feeding history must be stated. The approach to diagnosis varies with the nature of severity of symptoms. In some situations, it is possible to make a good guess at the diagnosis clinically and then select the tests most likely to give the answer (see table 2). In Table 2 Investigations for the diagnosis of an IEM First line investigations Full blood count Urea and electrolytes Anion gap Blood gases Glucose Lactate Ammonia Liver function tests Urine reducing substances Urine ketones CSF lactate Second line investigations Urine amino acids Plasma uric acid Plasma amino acids Plasma carnitine and acylcarnitine profile Biotinidase Galactosaemia screening tests (e.g. Beutler) CSF amino acids Third line or specialised investigations Enzyme assays on skin fibroblasts or blood cells DNA mutation analysis Special metabolite assays (e.g. VLCFA, transferrin isoelectric focusing, etc) most cases, however, it is necessary to perform a group of tests, as many IEMs can cause very similar symptoms. THE METABOLIC SCREEN The scope of metabolic disorders is enormous and constantly expanding. The term metabolic screen (which would denote a set of investigations to rule out most known metabolic causes of illness) is therefore inappropriate, and such a request to a laboratory is meaningless. Specialised metabolic investigations in a sick neonate must always be dictated by the clinical situation, and directed towards specific conditions (table 3). Although techniques will vary, most laboratories will require samples of blood (2 3 ml each in heparinised and EDTA bottles, and a dried blood spot on a screening card) and urine (5 10 ml in a sterile container with no preservatives). It is good practice to save and freeze all urine passed for future analysis, and to save a heparinised blood sample before the first blood transfusion. Occasionally more unusual investigations, such as CSF analysis for organic and amino acids may be necessary. 17 It is best to discuss such tests with the laboratory to ensure that the samples are collected and preserved correctly. In many cases these investigations will provide a definitive diagnosis or a high suspicion of a specific IEM. The complete characterisation of the particular condition usually involves more specific studies, such as enzyme assays, DNA analysis, and family studies. Most of such work is performed on cultured skin fibroblasts or transformed lymphoblast cell lines at supraregional laboratories. Management while awaiting results The management should be dictated by the severity of symptoms. Very mild symptoms may require no change to the management. As milk feeds are often the source of the toxic metabolites, these should be stopped, if the symptoms are more than very mild, while preliminary results are awaited. Generally, intravenous 10% dextrose with added electrolytes should be used. In more severe cases, intravenous bicarbonate may be necessary to correct metabolic acidosis. Other additives should be dictated by the blood biochemistry with the aim of maintaining glucose and electrolyte homoeostasis. The extremely ill or rapidly deteriorating infant will require more aggressive therapy. Care must be taken to avoid overhydration in the presence of impaired renal function. Adequate correction of acidosis often requires very large doses of sodium bicarbonate (up to mmol/kg in some organic acidaemias) which may cause hypernatraemia, sometimes necessitating dialysis. Blood electrolytes should be checked frequently (4 6 hourly) during correction of the acidosis. If hyperammonaemia is present, treatment with sodium benzoate should be commenced (250 mg/kg loading dose, followed by an infusion of 250 mg/kg/24 hours). The long term neurological outcome of the urea
4 F208 Chakrapani, Cleary, Wraith Table 3 Metabolic investigations according to patterns of presentation Presentation Condition Specific investigations Encephalopathy Urea cycle defects Urine amino acids Organic acidaemias and MSUD Plasma amino acids Blood carnitine and acylcarnitine profile Skin biopsy for enzyme analysis Fatty acid oxidation defects As above, plus: Blood DNA mutation analysis Primary lactic acidoses (e.g. pyruvate dehydrogenase CSF lactate deficiency, pyruvate carboxylase deficiency and Mitochondrial DNA blood and muscle respiratory chain defects) Muscle biopsy histology and electron microscopy Skin biopsy enzymes of pyruvate metabolism Non-ketotic hyperglycinaemia Plasma and CSF amino acids Enzyme analysis on transformed lymphoblasts Molybdenum cofactor deficiency Urine sulphite (dipstick) Urine amino acids Plasma uric acid Skin biopsy for enzyme analysis Pyridoxine dependent seizures Trial of pyridoxine under EEG observation Hypoglycaemia Fatty acid oxidation defects As under encephalopathy Hypopituitarism Hormone levels (growth hormone, cortisol, ACTH, insulin, and C peptide) Adrenal dysfunction Hyperinsulinism Gluconeogenic defects (e.g. fructose-1,6 bisphosphatase deficiency) Blood gases (metabolic acidosis) Plasma lactate (for glycerol) Enzyme assay leucocytes or liver biopsy Glycogen storage disease (types I, III, VI, IX) Plasma lactate Enzyme assay leucocytes or liver biopsy Histology on liver biopsy Secondary to organic acidaemias or disorders avecting the liver As stated under respective sections Liver disease Galactosaemia Beutler test Red cell galactose-1-phosphate DNA mutation analysis Ophthalmology assessment for cataracts Tyrosinaemia type I Plasma amino acids Investigations for renal Fanconi s syndrome α 1 Antitrypsin deficiency Serum α 1 antitrypsin Protease typing Neonatal haemochromatosis Serum ferritin Liver biopsy Niemann Pick C Foam cells on bone marrow aspitrate, blood film, liver biopsy Filipin staining on skin biopsy Mitochondrial (respiratory chain) defects CSF lactate Mitochondrial DNA blood and muscle Muscle and liver biopsy histology and electron microscopy Cardiomyopathy Pompe s disease (GSD type II) Enzyme assay on lymphocytes or skin fibroblasts Fatty acid oxidation defects As stated under encephalopathy Mitochondrial (respiratory chain) defects As stated under liver disease CDG 1a syndrome Serum transferrin isoelectric focusing Enzyme assay on skin biopsy Lysosomal storage disorders White cell enzymes Urine oligosaccharides and mucolpolysaccharides Skin biopsy Dysmorphism Lysosomal storage disorders As under cardiomyopathy Disorders of sterol synthesis Plasma 7-dehydrocholesterol Skin biopsy CDG syndrome Serum transferrin isoelectric focusing Enzyme assay on skin biopsy Glutaric aciduria type II Blood carnitine/acylcarnitine profile Skin biopsy cycle defects depends on the rapidity of resolution of the initial hyperammonaemic coma. The use of medications alone is rarely suycient in this situation, and dialysis is usually necessary. Haemodialysis and haemodiafiltration are more evective than peritoneal dialysis, and if available, should be the methods of choice in the initial treatment of urea cycle defects, MSUD, and the organic acidaemias Exchange transfusion is not useful, except in desperate situations when dialysis is not immediately available. Secondary carnitine deficiency is common in many metabolic conditions, especially the organic acidaemias and fatty acid oxidation defects. Carnitine supplementation (100 mg/ kg/day in four divided doses) is therefore useful in infants with suspected metabolic disease while awaiting results. Respiratory depression and cerebral oedema caused by direct toxic evects of accumulating metabolites are commonly present. Ventilatory support should therefore be used early and continued until the baby is breathing vigorously. Clinical recovery to a degree suycient to withdraw ventilatory support can be delayed two to three days after correction of the metabolic abnormality. Maintainance of good hydration and tissue perfusion may necessitate the use of inotropes and colloid infusions. As most metabolic conditions are aggravated by tissue catabolism, nutritional support in the acute phase requires careful attention. Initially, 10% dextrose is suycient, but more concentrated solutions (up to 20%) should be used via a central line to induce mild hyperglycaemia (blood glucose 7 12 mmol/l) if feeds cannot be commenced within 24 hours. Anabolism can
5 Detection of inborn errors of metabolism in the newborn F209 Table 4 Specimen Investigations if death is inevitable and a metabolic cause is suspected Sampling details Plasma 3 5 ml lithium heparin sample, plasma separated and frozen Whole blood for DNA analysis 3 5 ml EDTA sample kept refrigerated (should not be frozen) (other whole blood samples can also be used) Blood spot for acylcarnitine analysis 2 3 spots on filter paper or Guthrie card Urine Frozen in a plain sterile container Skin biopsy for fibroblast culture Collected using aseptic technique, stored in a skin biopsy medium (if this is not available, viral culture medium or normal saline in a sterile container may be used) (should not be frozen) Muscle biopsy 1 cm 3 piece immediately frozen in liquid nitrogen or dry ice for enzymology, histology, and DNA analysis; one piece preserved in gluteraldehyde for electron microscopy Liver biopsy 1 cm 3 piece immediately frozen in liquid nitrogen or dry ice for enzymology, histology, and DNA analysis; one piece preserved in gluteraldehyde for electron microscopy be further promoted by infusing small doses of insulin (0.05 U/kg/h). After stabilisation, subsequent dietary management will vary depending on the specific diagnosis, and should be supervised by a dietician with experience in managing metabolic disease. Some metabolic disorders have vitamin responsive forms and in the past, a combination of vitamins and cofactors were administered to sick newborns while results were awaited. Nowadays, this blind vitamin treatment is not justified, as most metabolic conditions can be diagnosed fairly rapidly. Once the diagnosis is made, appropriate cofactor therapy can be used in therapeutic doses (approximately 100 times the daily requirement). Management when no diagnosis can be made Occasionally no clear diagnosis can be made on the initial investigations. Every evort must be made to keep such neonates alive until all investigations are completed. A sick neonate with hyperammonaemia merits full biochemical correction by dialysis, even if the initial biochemical tests are negative, as transient hyperammonaemia of the newborn (THAN) may be the underlying diagnosis. The majority of patients with THAN have been preterm infants who have mild respiratory distress syndrome. 21 Plasma ammonia concentrations may be greatly increased, but the plasma and urine amino acid analyses are not characteristic of any of the urea cycle defects. If treated aggressively, THAN is compatible with a good long term neurological outcome, and hyperammonaemia does not recur even on a normal protein diet. 22 The aetiology of this condition is unknown. Management when death is inevitable Some patients will not survive, despite intensive treatment. In such cases, establishing a diagnosis is very important for genetic counselling and for later prenatal diagnosis. A full autopsy is preferable for internal anomalies, but it is uncommon to arrive at a metabolic diagnosis based on routine autopsy findings alone. It is therefore essential to collect the relevant specimens and biopsy specimens before or shortly after death. It is useful to discuss the infant s poor prognosis frankly with the parents and to obtain their permission for autopsy and biopsies before the infant dies. In our experience, it is unusual not to obtain at least the minimum specimens required for a metabolic diagnosis, even if full autopsy is refused. These include a blood spot on a screening card, a lithium heparin, and an EDTA blood sample (3 5 ml each), all possible urine frozen in plain sterile containers, and a skin biopsy refrigerated in culture medium (table 4). If possible, muscle and liver biopsy specimens should also be obtained. Open liver biopsy is preferable, but needle biopsy is also of use if an open biopsy cannot be performed. One piece of each should be immediately frozen in liquid nitrogen or dry ice for enzyme analysis, and another stored in an appropriate medium (for example, gluteraldehyde) for electron microscopy. Management when an IEM is anticipated Sometimes the diagnosis of an IEM can be known or suspected in advance: there may be a previously avected sibling, specific antenatal testing may have established the diagnosis, or a mother may be a proven carrier of an X linked condition. The optimal management should be established prior to delivery. The choice is whether to treat the baby as avected while awaiting tests, or to investigate promptly and commence appropriate treatment when results are available. The decision will vary depending on the disorder in question, but should be made in collaboration with the paediatrician, obstetrician, and metabolic specialist. Many disorders (such as fatty acid oxidation defects and organic acidaemias) can be readily diagnosed by analysis of cord blood specimens using tandem mass spectrometry, and discussion with a metabolic laboratory before delivery should enable a rapid diagnosis. Withdrawal of treatment If clinical improvement does not occur within a few days, the infant is unlikely to recover near normal cerebral function. In such a situation, it is reasonable to discuss withdrawal of intensive life support measures with the parents. This is not diycult if the diagnosis is known and the prognosis can be explained with some certainty. Even if the exact diagnosis is not known, it is often possible to give the parents some idea of the likely group of conditions (for example, disorders of pyruvate metabolism or respiratory chain defects) that their child might have. Occasionally, a gravely ill neonate may survive withdrawal of intensive care against all expectations. Such infants are likely to have frequent acute episodes of deterioration, and depending on the degree of brain damage and the underlying condition, a decision to not undertake extraordinary measures to prolong life during the next episode may be made in discussion with the parents. 1 Ibdah J, Bennett MJ, Rinaldo P, et al. A fetal fatty acid oxidation disorder as a cause of liver disease in pregnant women. N Engl J Med 1999;340: Innes AM, Seargeant LE, Balachandra K, et al. Hepatic carnitine palmitoyl transferase I deficiency presenting as maternal illness in pregnancy. Pediatr Res 2000;47: Walter JH. Inborn errors of metabolism and pregnancy. J Inherit Metab Dis 2000;23:
6 F210 Chakrapani, Cleary, Wraith 4 Cooke RJ, Jensen RL. Plasma ammonia concentrations during the first 6 postnatal months, as measured with an ammonium selective electrode. Clin Chem 1983;29: Maestri NE, Clissod D, Brusilow SW. Neonatal onset ornithine transcarbamylase deficiency: a retrospective analysis. J Pediatr 1999;134: Walter JH, Wraith JE, Cleary MA. Absence of acidosis in the initial presentation of organic acidaemias. Arch Dis Child Fetal Neonatal Ed 1995;72:F Poggi-Travert F, Martin D, de Villemeur TB, et al. Metabolic intermediates in lactic acidosis: compounds, samples and interpretation. J Inherit Metab Dis 1996;19: Kristiansson B, Stibler H, Conradi N, et al. The heart and pericardial evusions in CDGS-I (carbohydrate deficient glycoprotein syndrome type I). J Inherit Metab Dis 1998;21: Imtiaz F, Worthington V, Champion M,et al. Genotypes and phenotypes of patients in the UK with carbohydrate deficient glycoprotein syndrome type I. J Inherit Metab Dis 2000;23: Barth P, Wanders RJ, Vreken P. X-linked cardioskeletal myopathy and neutropenia (Barth syndrome MIM ). J Pediatr 2000;135: Nyhan WL, Ozand P. Niemann Pick type C disease/ cholesterol processing abnormality. In: Atlas of metabolic diseases. London: Chapman and Hall Medical, 1998: Have your say eletters 12 Kelly DA, Portmann B, Mowat AP, et al. Niemann-Pick disease type C: diagnosis and outcome in children, with particular reference to liver disease. J Pediatr 1993;123: Clayton PT. Disorders of cholesterol biosynthesis. Arch Dis Child 1998;78: Ryan AK, Bartlett K, Clayton P, et al. Smith-Lemli-Opitz syndrome: a variable clinical and biochemical phenotype. J Med Genet 1998;35: Van Maldergem, Jauniaux E, Fourneau C, Gillerot Y. Genetic causes of hydrops fetalis. Pediatrics 1992;89: Stone DL, Sidransky E. Hydrops fetalis: lysosomal disorders in extremis. Adv Pediatr 1999;46: HoVman GF, Surtees RAH, Wevers RA. Cerebrospinal investigations for neurometabolic disorders. Neuropediatrics 1998;29: Falk MC, Knight JF, Roy LP, et al. Continuous venovenous haemofiltration in the acute treatment of inborn errors of metabolism. Pediatr Nephrol 1994;8: Schafer F, Straube E, Oh J, et al. Dialysis in neonates with inborn errors of metabolism. Nephrol Dial Tranplant 1999;14: Wong KY, Wong SN, Lam SY,et al. Ammonia clearance by peritoneal dialysis and continuous arteriovenous hemodiafiltration. Pediatr Nephrol 1998;12: Hudak M, Jones MD Jr, Brusilow S. DiVerentiation of transient hyperammonaemia of the newborn and urea cycle defects by clinical presentation. J Pediatr 1985;107: Yoshino M, Sakaguchi Y, Kuriya N, et al. A nationwide survey on transient hyperammonemia in newborn infants in Japan: prognosis of life and neurological outcome. Neuropediatrics 1991;22: If you wish to comment on any article published in Archives of Disease in Childhood you can send an eletter using the eletters link at the beginning of each article. Your response will be posted on Archives of Disease in Childhood online within a few days of receipt (subject to editorial screening).
INBORN ERRORS OF METABOLISM (IEM) IAP UG Teaching slides
 INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children
 National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
Training Syllabus CLINICAL SYLLABUS
 Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Best Practice Guidelines for the Biochemical Investigation of Patients with Foetal and Neonatal Hydrops
 National Metabolic Biochemistry Network Best Practice Guidelines for the Biochemical Investigation of Patients with Foetal and Neonatal Hydrops INTRODUCTION Hydrops is defined as the presence of skin oedema
National Metabolic Biochemistry Network Best Practice Guidelines for the Biochemical Investigation of Patients with Foetal and Neonatal Hydrops INTRODUCTION Hydrops is defined as the presence of skin oedema
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE
 SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
Inborn Errors of Metabolism in the Emergency Department. Will Davies June 2014
 Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Neonatal Guidelines. Chapter 10: Metabolic V Date Revised : January 2017 Ratified 6 th February Date for Review: 1 st of March 2021
 Neonatal Guidelines Chapter 10: Metabolic V2017.1 Specialty: Neonatal Medicine Revised by: Jean Matthes Date Revised : January 2017 Ratified 6 th February 2017 Approved by: ABMU Joint Perinatal Forum Date
Neonatal Guidelines Chapter 10: Metabolic V2017.1 Specialty: Neonatal Medicine Revised by: Jean Matthes Date Revised : January 2017 Ratified 6 th February 2017 Approved by: ABMU Joint Perinatal Forum Date
Module : Clinical correlates of disorders of metabolism Block 3, Week 2
 Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Paediatric Clinical Chemistry
 Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Inborn errors of metabolism around time of birth
 Review Inborn errors of metabolism around time of birth J V Leonard, A A M Morris Inborn errors of metabolism commonly present around the time of birth. Although most affected babies are born healthy and
Review Inborn errors of metabolism around time of birth J V Leonard, A A M Morris Inborn errors of metabolism commonly present around the time of birth. Although most affected babies are born healthy and
ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version)
 Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Presentation and investigation of mitochondrial disease in children
 Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Dysmorphology Guy Besley
 Dysmorphology Guy Besley Willink Biochemical Genetics Unit, Manchester Children s s Hospital Dysmorphic presentation Congenital malformation Disorder of embryogenesis Intrauterine insult infection; chromosomal/genetic
Dysmorphology Guy Besley Willink Biochemical Genetics Unit, Manchester Children s s Hospital Dysmorphic presentation Congenital malformation Disorder of embryogenesis Intrauterine insult infection; chromosomal/genetic
Inborn Errors of Metabolism (IEM)
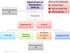 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition
 Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff
 Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism
 Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
The laboratory investigation of lactic acidaemia. J Bonham/T Laing
 The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Urea Cycle Defects. Dr Mick Henderson. Biochemical Genetics Leeds Teaching Hospitals Trust. MetBioNet IEM Introductory Training
 Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Inborn Error Of Metabolism :
 Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015
 Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE
 THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
Neonatal Biochemistry Investigation for Inherited Metabolic Disorders (IMDs)
 Neonatal Biochemistry Investigation for Inherited Metabolic Disorders (IMDs) Anne Green Birmingham Children s Hospital Leeds May 2005 Overview of how IMDs present cases Range of Disorders & Incidence disorders
Neonatal Biochemistry Investigation for Inherited Metabolic Disorders (IMDs) Anne Green Birmingham Children s Hospital Leeds May 2005 Overview of how IMDs present cases Range of Disorders & Incidence disorders
Inborn Errors of Metabolism Clinical Approach to Diagnosis and Treatment
 Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Childhood epilepsy: the biochemical epilepsies. Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary
 Childhood epilepsy: the biochemical epilepsies Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary Definitions Epileptic Seizure Manifestation(s) of epileptic (excessive and/or
Childhood epilepsy: the biochemical epilepsies Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary Definitions Epileptic Seizure Manifestation(s) of epileptic (excessive and/or
Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese. DOI: /neo.
 Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: 10.1542/neo.9-7-e291 The online version of this article, along
Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: 10.1542/neo.9-7-e291 The online version of this article, along
Hypoglycaemia of the neonate. Dr. L.G. Lloyd Dept. Paediatrics
 Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE. Bwee Tien Poll-The Amsterdam UMC The Netherlands
 CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA
 UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT
 Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up
 HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD
 Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
7 Medical Genetics. Hemoglobinopathies. Hemoglobinopathies. Protein and Gene Structure. and Biochemical Genetics
 SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting
 Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when
 CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center
 Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center Kefah Al-Qa qa MD*, Wajdi Amayreh MD*, Ali Al-Hawamdeh MD* ABSTRACT Objective: To describe the different
Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center Kefah Al-Qa qa MD*, Wajdi Amayreh MD*, Ali Al-Hawamdeh MD* ABSTRACT Objective: To describe the different
TITLE: NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA. Eilish O Connell, Clinical Education Facilitator, NCIMD
 NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA
 NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism
 Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
D evelopmental disabilities occur in approximately
 1128 REVIEW Developmental delay: when to suspect and how to investigate for an inborn error of metabolism M A Cleary, A Green... The purpose of this review is to provide a practical guideline on the suspicion
1128 REVIEW Developmental delay: when to suspect and how to investigate for an inborn error of metabolism M A Cleary, A Green... The purpose of this review is to provide a practical guideline on the suspicion
MetBioNet Best Practice Guidelines. Investigation of an inherited metabolic cause of cardiomyopathy
 Introduction MetBioNet Best Practice Guidelines Investigation of an inherited metabolic cause of Inborn errors of metabolism (IEM) account for at least 5% of cases of. In some disorders, is the major cause
Introduction MetBioNet Best Practice Guidelines Investigation of an inherited metabolic cause of Inborn errors of metabolism (IEM) account for at least 5% of cases of. In some disorders, is the major cause
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet
 Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Hyperglycaemia. Clinical presentation. Definition of hyperglycaemia. Approach to the problem
 Hyperglycaemia 1 Clinical presentation Hyperglycaemia is usually picked up incidentally on routine blood glucose assessment or in response to finding glycosuria. It may be noted as part of the workup of
Hyperglycaemia 1 Clinical presentation Hyperglycaemia is usually picked up incidentally on routine blood glucose assessment or in response to finding glycosuria. It may be noted as part of the workup of
Metabolic Changes in ASD. Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius
 Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Staff at the Nottingham Children s Hospital. Guidelines process; paediatric endocrinology team
 Hypoglycaemia Title of Guideline Contact Name and Job Title (author) Hypoglycaemia in infants and children: aetiology, investigation and treatment Dr. Hoong-Wei Gan ST6 Paediatric Endocrinology & Diabetes
Hypoglycaemia Title of Guideline Contact Name and Job Title (author) Hypoglycaemia in infants and children: aetiology, investigation and treatment Dr. Hoong-Wei Gan ST6 Paediatric Endocrinology & Diabetes
UREA CYCLE DISORDERS - The What, Why, How and When
 UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
Investigation of metabolic encephalopathy
 Investigation of metabolic encephalopathy Encephalopathy may be a presenting sign in a wide range of medical conditions. G F van der Watt, FCPath (SA) Chem, MMed, MB ChB, DA (SA) Principal Pathologist
Investigation of metabolic encephalopathy Encephalopathy may be a presenting sign in a wide range of medical conditions. G F van der Watt, FCPath (SA) Chem, MMed, MB ChB, DA (SA) Principal Pathologist
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Medical Foods for Inborn Errors of Metabolism
 Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Peroxisomal Disorders
 Peroxisomal Disorders George Gray Birmingham Childrens Hospital Peroxisomal Disorders Peroxisomes are large single membrane bound organelles that are present in the cytoplasm of all cells. They are formed
Peroxisomal Disorders George Gray Birmingham Childrens Hospital Peroxisomal Disorders Peroxisomes are large single membrane bound organelles that are present in the cytoplasm of all cells. They are formed
Information for health professionals
 Introduction of a new screening test for newborn babies in Wales Newborn bloodspot screening for Medium chain acyl-coa dehydrogenase deficiency (MCADD) Newborn bloodspot screening for MCADD is being introduced
Introduction of a new screening test for newborn babies in Wales Newborn bloodspot screening for Medium chain acyl-coa dehydrogenase deficiency (MCADD) Newborn bloodspot screening for MCADD is being introduced
Medium-chain acyl-coa dehydrogenase deficiency
 Medium-chain acyl-coa dehydrogenase deficiency Introductory information Written by: V. Prietsch & P. Burgard Reviewed & Revised for North America by: S. van Calcar Medium-chain acyl-coa dehydrogenase MCAD
Medium-chain acyl-coa dehydrogenase deficiency Introductory information Written by: V. Prietsch & P. Burgard Reviewed & Revised for North America by: S. van Calcar Medium-chain acyl-coa dehydrogenase MCAD
Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia
 Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Clinical Approach to Diagnosis of Lysosomal Storage Diseases
 Clinical Approach to Diagnosis of Lysosomal Storage Diseases M. Rohrbach, MD, PhD FMH Pädiatrie und FMH Medizinische Genetik Abteilung Stoffwechsel Universitätskinderklinik Zürich Lysosomal storage disorders
Clinical Approach to Diagnosis of Lysosomal Storage Diseases M. Rohrbach, MD, PhD FMH Pädiatrie und FMH Medizinische Genetik Abteilung Stoffwechsel Universitätskinderklinik Zürich Lysosomal storage disorders
Fatty Acid Oxidation Disorders
 Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social
Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social
Case Reports. Neonatal Seizure: A Rare Aetiology Easily Missed by Routine Metabolic Screening LY SIU, L KWONG, SN WONG, NS KWONG
 HK J Paediatr (new series) 2009;14:37-41 Case Reports Neonatal Seizure: A Rare Aetiology Easily Missed by Routine Metabolic Screening LY SIU, L KWONG, SN WONG, NS KWONG Abstract Key words We present the
HK J Paediatr (new series) 2009;14:37-41 Case Reports Neonatal Seizure: A Rare Aetiology Easily Missed by Routine Metabolic Screening LY SIU, L KWONG, SN WONG, NS KWONG Abstract Key words We present the
Very-long-chain acyl-coa dehydrogenase deficiency
 Very-long-chain acyl-coa dehydrogenase deficiency Introductory information Written by: V. Prietsch & P. Burgard Reviewed & Revised for North America by: S. van Calcar Very-long-chain acyl-coa dehydrogenase
Very-long-chain acyl-coa dehydrogenase deficiency Introductory information Written by: V. Prietsch & P. Burgard Reviewed & Revised for North America by: S. van Calcar Very-long-chain acyl-coa dehydrogenase
Summary. Syndromic versus Etiologic. Definitions. Why does it matter? ASD=autism
 Summary It is becoming clear that multiple genes with complex interactions underlie autism spectrum (ASD). A small subset of people with ASD, however, actually suffer from rare single-gene Important to
Summary It is becoming clear that multiple genes with complex interactions underlie autism spectrum (ASD). A small subset of people with ASD, however, actually suffer from rare single-gene Important to
Fatty Acid Oxidation Disorders
 Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social
Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social
Paediatric Hypoglycaemia and the Laboratory. AACB Webinar, 8 th April 2015 Tina Yen
 Paediatric Hypoglycaemia and the Laboratory AACB Webinar, 8 th April 2015 Tina Yen Synopsis Definition and classification Newborn and Neonatal Hypoglycaemia Transient Persistant Hypoglycaemia in infants
Paediatric Hypoglycaemia and the Laboratory AACB Webinar, 8 th April 2015 Tina Yen Synopsis Definition and classification Newborn and Neonatal Hypoglycaemia Transient Persistant Hypoglycaemia in infants
Methylmalonic aciduria
 Methylmalonic aciduria Introductory information Written by: F. Hörster, S. Kölker & P. Burgard Reviewed & Revised for North America by: S. van Calcar Methylmalonic aciduria MMA 2 Methylmalonic aciduria
Methylmalonic aciduria Introductory information Written by: F. Hörster, S. Kölker & P. Burgard Reviewed & Revised for North America by: S. van Calcar Methylmalonic aciduria MMA 2 Methylmalonic aciduria
The breakdown of fats to provide energy occurs in segregated membrane-bound compartments
 CPT1a deficiency The breakdown of fats to provide energy occurs in segregated membrane-bound compartments of the cell known as mitochondria. Carnitine palmitoyltransferase Ia (CPT1a) is a protein that
CPT1a deficiency The breakdown of fats to provide energy occurs in segregated membrane-bound compartments of the cell known as mitochondria. Carnitine palmitoyltransferase Ia (CPT1a) is a protein that
Fatty Acid Oxidation Disorders- an update. Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London
 Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Isovaleric Acidemia: Quick reference guide
 Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Neonatal Hypoglycemia. Presented By : Kamlah Olaimat 25\7\2010
 Neonatal Hypoglycemia Presented By : Kamlah Olaimat 25\7\2010 Definition The S.T.A.B.L.E. Program defines hypoglycemia as: Glucose delivery or availability is inadequate to meet glucose demand (Karlsen,
Neonatal Hypoglycemia Presented By : Kamlah Olaimat 25\7\2010 Definition The S.T.A.B.L.E. Program defines hypoglycemia as: Glucose delivery or availability is inadequate to meet glucose demand (Karlsen,
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion , version 1.1
 EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
Nutritional Interventions in Primary Mitochondrial Disorders
 Nutritional Interventions in Primary Mitochondrial Disorders Carolyn J Ellaway MBBS PhD FRACP CGHGSA Genetic Metabolic Disorders Service Sydney Children s Hospital Network Disciplines of Child and Adolescent
Nutritional Interventions in Primary Mitochondrial Disorders Carolyn J Ellaway MBBS PhD FRACP CGHGSA Genetic Metabolic Disorders Service Sydney Children s Hospital Network Disciplines of Child and Adolescent
So Much More Than The PKU Test
 Newborn Metabolic Screening So Much More Than The PKU Test Sarah Viall, MSN, PPCNP BC Newborn Screening Program Coordinator Division of Genetics & Metabolism Conflicts of Interest I have no conflicts of
Newborn Metabolic Screening So Much More Than The PKU Test Sarah Viall, MSN, PPCNP BC Newborn Screening Program Coordinator Division of Genetics & Metabolism Conflicts of Interest I have no conflicts of
Organic Acid Disorders
 Genetic Fact Sheets for Parents Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Genetic Fact Sheets for Parents Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Introduction to Organic Acidemias. Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.
 Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
THIAMINE TRANSPORTER TYPE 2 DEFICIENCY
 THIAMINE TRANSPORTER TYPE 2 DEFICIENCY WHAT IS THE THIAMINE TRANSPORTER TYPE 2 DEFICIENCY (hthtr2)? The thiamine transporter type 2 deficiency (hthtr2) is a inborn error of thiamine metabolism caused by
THIAMINE TRANSPORTER TYPE 2 DEFICIENCY WHAT IS THE THIAMINE TRANSPORTER TYPE 2 DEFICIENCY (hthtr2)? The thiamine transporter type 2 deficiency (hthtr2) is a inborn error of thiamine metabolism caused by
Inborn error of metabolism
 Inborn error of metabolism The lecture is given by Dr Kefah Al qa qa, Consultant metabolic pediatrician, in Queen Rania Al Abdulla children hospital, on Thursday 11/12/2014. Let s tart Metabolism: refers
Inborn error of metabolism The lecture is given by Dr Kefah Al qa qa, Consultant metabolic pediatrician, in Queen Rania Al Abdulla children hospital, on Thursday 11/12/2014. Let s tart Metabolism: refers
Newborn Bloodspot Screening Information for parents
 Newborn Bloodspot Screening Information for parents You will be offered a bloodspot screening test for your newborn baby for several rare but serious conditions. The sample for this test is usually taken
Newborn Bloodspot Screening Information for parents You will be offered a bloodspot screening test for your newborn baby for several rare but serious conditions. The sample for this test is usually taken
Newborn Screening in Manitoba. Information for Health Care Providers
 Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
What s New in Newborn Screening?
 What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is administered by the Illinois Department of Public Health.
What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is administered by the Illinois Department of Public Health.
For healthcare professionals Methylmalonic Acidurias
 www.e-imd.org For healthcare professionals Methylmalonic Acidurias Methylmalonic acidurias (MMAurias) comprise a group of inborn errors of metabolism characterized by an isolated accumulation of methylmalonic
www.e-imd.org For healthcare professionals Methylmalonic Acidurias Methylmalonic acidurias (MMAurias) comprise a group of inborn errors of metabolism characterized by an isolated accumulation of methylmalonic
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Genetics
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
Newborn Bloodspot Screening Information for parents
 Newborn Bloodspot Screening Information for parents You will be offered a bloodspot screening test for your newborn baby for several rare but serious conditions. The sample for this test is usually taken
Newborn Bloodspot Screening Information for parents You will be offered a bloodspot screening test for your newborn baby for several rare but serious conditions. The sample for this test is usually taken
Metabolic Precautions & ER Recommendations
 Metabolic Precautions & ER Recommendations * To whom correspondence Sumit Parikh, should MD be addressed Center for Pediatric Neurology Cleveland Clinic Cleveland, OH UMDF 2010 The catabolic state Entering
Metabolic Precautions & ER Recommendations * To whom correspondence Sumit Parikh, should MD be addressed Center for Pediatric Neurology Cleveland Clinic Cleveland, OH UMDF 2010 The catabolic state Entering
Current Management and Future Developments in Metabolic Disease
 Current Management and Future Developments in Metabolic Disease APAGBI Annual Scientific Meeting Friday 15 th May 2015 Dr Saikat Santra Birmingham Children s Hospital, UK Outline Metabolic disorders in
Current Management and Future Developments in Metabolic Disease APAGBI Annual Scientific Meeting Friday 15 th May 2015 Dr Saikat Santra Birmingham Children s Hospital, UK Outline Metabolic disorders in
Newborn Screening: Blood Spot Disorders
 Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai
 Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai 11 day old male neonate admitted on 26/6 to our Hospital with c/olethargy -since day1 abnormal movements
Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai 11 day old male neonate admitted on 26/6 to our Hospital with c/olethargy -since day1 abnormal movements
Prevalence of selected disorders of inborn errors of metabolism in suspected cases at a Tertiary Care Hospital in Karachi
 Original Article Prevalence of selected disorders of inborn errors of metabolism in suspected cases at a Tertiary Care Hospital in Karachi Hema Satwani, 1 Jamal Raza, 2 Junji Hanai, 3 Shosuke Nomachi 4
Original Article Prevalence of selected disorders of inborn errors of metabolism in suspected cases at a Tertiary Care Hospital in Karachi Hema Satwani, 1 Jamal Raza, 2 Junji Hanai, 3 Shosuke Nomachi 4
Genetic Testing FOR DISEASES OF INCREASED FREQUENCY IN THE ASHKENAZI JEWISH POPULATION
 Carrier Screening and Diagnostic Testing for the Ashkenazi Jewish Population Genetic Testing FOR DISEASES OF INCREASED FREQUENCY IN THE ASHKENAZI JEWISH POPULATION Our Science. Your Care. An extensive
Carrier Screening and Diagnostic Testing for the Ashkenazi Jewish Population Genetic Testing FOR DISEASES OF INCREASED FREQUENCY IN THE ASHKENAZI JEWISH POPULATION Our Science. Your Care. An extensive
Guideline for the Prevention and Management of Neonatal Hypoglycaemia GL359
 Guideline for the Prevention and Management of Neonatal Hypoglycaemia GL359 Approval and Authorisation Approved by Job Title Date Paediatric Clinical Chair of Paediatric Clinical Governance Governance
Guideline for the Prevention and Management of Neonatal Hypoglycaemia GL359 Approval and Authorisation Approved by Job Title Date Paediatric Clinical Chair of Paediatric Clinical Governance Governance
NEWBORN METABOLIC SCREEN, MINNESOTA
 Lab Dept: Test Name: Chemistry NEWBORN METABOLIC SCREEN, MINNESOTA General Information Lab Order Codes: Synonyms: CPT Codes: Test Includes: PKUN Newborn Screen for Hyopothyroidism, Phenylketonuria (PKU),
Lab Dept: Test Name: Chemistry NEWBORN METABOLIC SCREEN, MINNESOTA General Information Lab Order Codes: Synonyms: CPT Codes: Test Includes: PKUN Newborn Screen for Hyopothyroidism, Phenylketonuria (PKU),
Metabolic diseases of the liver
 Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Salicylate (Aspirin) Ingestion California Poison Control Background 1. The prevalence of aspirin-containing analgesic products makes
 Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
Neonatal Hypoglycaemia
 Neonatal Hypoglycaemia Dr Shubha Srinivasan Paediatric Endocrinologist The Children s Hospital at Westmead Hypoglycaemia and the Brain CSF glucose is 2/3 that of plasma Intracerebral glucose 1/3 that of
Neonatal Hypoglycaemia Dr Shubha Srinivasan Paediatric Endocrinologist The Children s Hospital at Westmead Hypoglycaemia and the Brain CSF glucose is 2/3 that of plasma Intracerebral glucose 1/3 that of
Clinical Guideline. SPEG MCN Protocols Sub Group SPEG Steering Group
 Clinical Guideline SECONDARY CARE MANAGEMENT OF SUSPECTED ADRENAL CRISIS IN CHILDREN AND YOUNG PEOPLE Date of First Issue 24/01/2015 Approved 28/09/2017 Current Issue Date 16/06/2017 Review Date 01/09/2019
Clinical Guideline SECONDARY CARE MANAGEMENT OF SUSPECTED ADRENAL CRISIS IN CHILDREN AND YOUNG PEOPLE Date of First Issue 24/01/2015 Approved 28/09/2017 Current Issue Date 16/06/2017 Review Date 01/09/2019
ANATOMY OF A METABOLIC CRISIS: FAOD-style. Mark S. Korson, MD Tufts Medical Center Boston, MA
 ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
The role of the laboratory in diagnosing lysosomal disorders
 The role of the laboratory in diagnosing lysosomal disorders Dr Guy Besley, formerly Willink Biochemical Genetics Unit, Manchester Children s Hospital, Manchester M27 4HA, UK. Lysosomal disorders What
The role of the laboratory in diagnosing lysosomal disorders Dr Guy Besley, formerly Willink Biochemical Genetics Unit, Manchester Children s Hospital, Manchester M27 4HA, UK. Lysosomal disorders What
A Lawyer s Perspective on Genetic Screening Performed by Cryobanks
 A Lawyer s Perspective on Genetic Screening Performed by Cryobanks As a lawyer practicing in the area of sperm bank litigation, I have, unfortunately, represented too many couples that conceived a child
A Lawyer s Perspective on Genetic Screening Performed by Cryobanks As a lawyer practicing in the area of sperm bank litigation, I have, unfortunately, represented too many couples that conceived a child
ACUTE & CHRONIC ETHANOL EFFECTS An Overview
 ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
Neonatal Hypoglycemia
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Hypoglycemia. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Hypoglycemia. These podcasts are designed to give medical students an overview of key topics in pediatrics.
CARE OF THE NEWBORN HYPOGLYCAEMIA
 CARE OF THE NEWBORN HYPOGLYCAEMIA Background Definition A true blood glucose of less than 2.6 mmol/l venous sample. Neonatal hypoglycaemia is commonly defined as a true blood glucose of less than 2.6 mmol/l
CARE OF THE NEWBORN HYPOGLYCAEMIA Background Definition A true blood glucose of less than 2.6 mmol/l venous sample. Neonatal hypoglycaemia is commonly defined as a true blood glucose of less than 2.6 mmol/l
