Neonatal Guidelines. Chapter 10: Metabolic V Date Revised : January 2017 Ratified 6 th February Date for Review: 1 st of March 2021
|
|
|
- Abraham Thompson
- 6 years ago
- Views:
Transcription
1 Neonatal Guidelines Chapter 10: Metabolic V Specialty: Neonatal Medicine Revised by: Jean Matthes Date Revised : January 2017 Ratified 6 th February 2017 Approved by: ABMU Joint Perinatal Forum Date for Review: 1 st of March
2 Directorate of Child Health Checklist for Clinical Guidelines being submitted for Approval by ABMU Joint Perinatal Forum Title of Guideline: Name(s) of revising author: Chair of Group or Committee supporting submission: Jean Matthes, Edited by S. Banerjee Neonatal Guideline Group Sujoy Banerjee Issue / Version No: Next Review / Guideline Expiry: Review date: 1 st March 2021 Details of persons included in consultation process: Neonatal Consultants, Neonatal junior doctors, Nursing Managers, Neonatal Pharmacist Brief outline giving reasons for document being submitted for ratification Routine Revision Name of Pharmacist (mandatory if drugs involved): Please list any policies/guidelines this document will supercede: Katherine Willson Chapter 10:Metabolic v2013 Keywords linked to document: Metabolic, neonate Date approved by ABMU Joint Perinatal Forum: 6 th February 2017 File Name: Used to locate where file is stores on hard drive 2
3 CONTENTS Topics Page number Introduction to IEM 4 Clinical presentation 4 Clinical Examination 6 Initial screen for metabolic disease 9 Further investigations for specific conditions 11 Treatment general principles 13 Treatment of hyperammonaemia 13 Some specific disorders 15 Notes on specimens 22 3
4 Inborn errors of metabolism Introduction: Inborn errors of metabolism (IEM) are individually rare. Some conditions may only be seen once in a professional s working life. But there are very many different conditions so their combined incidence is significant. Usually a high index of suspicion is required to make the diagnosis. Early detection and treatment may prevent lifelong neurological damage. Early discussions with the newborn screening laboratory in UHW may ensure that the correct investigations are taken and processed urgently rather than routinely, saving valuable time. Likewise a discussion with our biochemistry laboratory in ABMU is required to ensure that samples are sent to Cardiff expeditiously. These discussions are best undertaken consultant to consultant. A very useful Website for investigation and treatment of metabolic conditions is BIMDG the British inherited metabolic diseases group. This also covers what interim treatment may be given to a newborn infant who may have a disorder, whilst awaiting the results of the diagnostic tests. It also gives treatment regimens for specific conditions. Please refer to this site when implementing emergency treatment. Newborn screening is undertaken in Wales for glutaric aciduria, homocysteinuria, isovaleric acidaemia, maple syrup urine disease, phenylketonuria and medium chain acyl CoA dehydrogenase deficiency. These tests are done on the 5 day heel prick Guthrie test but the result may not routinely be available until the child is several weeks old. Earlier diagnosis is definitely beneficial. So if you suspect one of these disorders, do not wait for the routine Guthrie to be reported. Contact the laboratory and expedite the test! Metabolic conditions may present in the following ways Antenatally suspected: babies born to mothers with acute fatty liver of pregnancy [AFLP], or to mothers with recurrent HELLP syndrome [haemolysis, elevated liver enzymes and low platelets] are at increased risk of LCHAD. Abnormalities evident at birth: dysmorphic features, severe hypotonia, seizures and apnoea, hydrops and ascites. 4
5 Presentation following an asymptomatic interval [of varying lengths hours to weeks]. Presentation may be non-specific, and may mimic sepsis. a. Encephalopathy: poor feeding, persistent vomiting with no anatomical cause, persistent hiccups, seizures, coma. b. Acid-base disturbance c. Liver impairment d. Cardiac impairment e. Unexplained hypoglycaemia f. Hyperammonaemia g. Others: Unusual odours, Cataract, Neutropenia, Thrombocytopenia Other clues from the history. a. Parental consanguinity b. Previous neonatal death c. Recurrent non-immune hydrops fetalis d. Siblings with known inborn errors of metabolism In the work up of a baby presenting with any of the above, IEMs should be considered in the differential diagnosis. Therefore, in addition to any other investigations requested, a set of preliminary tests should be sent aiming to identify the presence of an IEM. Pathogenesis: Majority are autosomal recessive. A few are X-linked recessive, e.g. ornithine carbamyl transferase (OCT) deficiency. a) Problems making and breaking complex molecules. Making: Breaking: Zellweger Inability to synthesise peroxisomes Smith Lemli Opitz block in cholesterol synthesis CDG (congenital disorders of glycosylation) block in glycosylation Hurler Syndrome failure to breakdown mucopolysaccharides Tay Sachs failure to breakdown gangliosides Fabry disease failure to breakdown glycolipids 5
6 b) Intoxication: Urea cycle disorders block in ammonia clearance Organic acidaemias block in amino acid breakdown Galactosaemia block in Galactose metabolism c) Energy Insufficiency: Congenital lactic acidosis Respiratory chain disorders (mitochondrial disorders) Pyruvate metabolism disorders Energy supply - Fat oxidation defects (FAO) Glycogen storage disorders (GSD) Gluconeogenesis defect d) Deficiencies of glucose transporter enzymes (e.g. GLUT1) Clinical Examination: A careful clinical examination of all the systems is required. These include:- Dysmorphic features Cardiovascular system, especially tachycardia, capillary refill time, signs of cardiac failure. Respiratory - especially respiratory rate in metabolic acidosis, apnoea in altered conscious state. GIT - jaundice, hepatomegaly, splenomegaly. Neurological - conscious level, seizures, abnormal movements, tone, posture, irritability, feel the fontanel, measure the head circumference. Urinalysis glucose and ketones. Smell. Eyes look carefully for cataracts, corneal clouding. Fundus for pigment or cherry red spot. 6
7 Clinical Presentation and Differential Diagnosis Seizures: When the usual causes of HIE, infection and biochemical causes have been excluded or seem unlikely, metabolic causes need to be considered. a) Isolated Seizures - Pyridoxine dependent seizures - Folinic acid responsive seizures - Biotin responsive multicarboxylase deficiency - Congenital malabsorption of magnesium b) Seizures with other Severe Neurological Signs - Non-ketotic hyperglycinaemia - Sulfite oxidase deficiency - Peroxisomal disorders - GLUT1 deficiency c) Seizures with pre-existing stupor, coma or hypoglycaemia - MSUD - Organic acidaemia - Urea cycle disorder Hypotonia: The most severe metabolic causes of hypotonia are:- - Congenital lactic acidosis - Respiratory chain disorders - Urea cycle disorders - Non ketotic hyperglycinaemia (NKH) - Sulphite oxidase (SO) Deficiency - Peroxisomal disorders Hepatic Presentation: a) Hepatomegaly and seizures suggest:- - Glycogen storage Type I or III 7
8 - Gluconeogenesis defects - Severe hyperinsulinism b) Liver Failure - Galactosaemia - Tyrosinaemia type 1 - Neonatal haemochromatosis - Respiratory chain disorders c) Cholestatic jaundice and failure to thrive - Alpha-1-antitrypsin deficiency - Inborn errors of bile acid metabolism - Peroxisomal disorders - Niemann Pick Type C disease - CDG syndrome - Cholesterol Biosynthesis Defects d) Hepatosplenomegaly - Lysosomal storage disorder Cardiac Presentation: a) Cardiac failure, Cardiomyopathy, Hypotonia and muscle weakness suggests:- - Respiratory chain disorders - Pompe disease - Fatty acid oxidation disorders b) Cardiac failure, pericardial effusions, cardiac tamponade, Cardiomyopathy - CDG syndrome c) Cardiomyopathy and conduction defects - Long chain fatty acid disorders 8
9 Initial screen for metabolic diseases: Unless one is looking for a specific condition (for example when there is a known positive family history), the following test must ALL be undertaken in an initial screen for metabolic disease. Blood gas Metabolic acidosis: organic acidemias, primary lactic acidosis, following collapse in any IEM (even urea cycle disorders!) Respiratory alkalosis: seen early in urea cycle defects Electrolytes, urea & creatinine Low urea in relation to creatinine early in urea cycle defects Calculate anion gap [Na + + K + ] [Cl - + HCO - 3 ]: increased > 20 in organic acidemias, primary lactic acidosis, some fatty acid oxidation defects Laboratory blood glucose (Unexplained hypoglycaemia): Hypoglycaemia in babies may accompany the following disorders fatty acid oxidation defects organic acidemias primary lactic acidosis glycogen storage disorders Endocrine causes eg cortisol deficiency, growth hormone deficiency, hyperinsulinaemia Liver enzymes, including albumin, and split bilirubin Elevated liver enzymes and bilirubin are found in : Galactosemia, Tyrosinaemia, peroxisomal disorders eg refsum s disease Full blood count and film Pancytopaenia: in secondary infection or overwhelming disease, which may complicate IEM. Ammonia <180mmol/L may be seen in any severe illness, but must consider IEM 9
10 >200mmol/L: IEM until proven otherwise: urea cycle disorders, organic acidemias, fatty acid oxidation defects, transient hyperammonemia of the newborn. NB emergency treatment of hyperammonemia in section Lactate Persisting >3mmol/L: primary lactic acidosis Beware of sampling errors best if free flowing arterial sample Exclude tissue hypoxia, congestive heart failure, sepsis, post convulsion CPK Urine Ketones: elevated in maple syrup urine disease (MSUD), absent in fatty acid oxidation defects (especially important when absent in presence of hypoglycaemia), Galactosemia, fructose 1,6 biphosphate aldolase deficiency Reducing substances Organic & amino acid profile: Further investigations Recurrent hypoglycaemia See Endocrine Chapter (Special investigations in hypoglycaemia) Do not delay correcting the low blood glucose if the blood is difficult to obtain and do not wait for the urine to be collected. Give 10% glucose 3mls / kg and increase the infusion rate from the baseline. Recheck the glucose within minutes and again at 1 hour Further investigations of raised ammonia (Discuss with lab urgently) U and E, Clotting, Glucose, lactate, blood gas Plasma amino acids requested. Blood spot acyl carnitine profile Urine amino acids Urine organic acids including orotic acid Ammonia >250 micromol/litre - start immediate treatment and arrange transfer to a specialist centre Monitor neurological status (Glasgow coma score or similar for infant) 10
11 Further Investigations according to clinical presentation. (Many of these tests will be done only in specialist centres) Presentation Condition Specific Investigation Encephalopathy Urea cycle defects Organic acidemias & MSUD Urine amino acids Urine organic acids Plasma amino acids Blood carnitine & acylcarnitines Fatty acid oxidation defects Primary lactic acidosis (e.g. puruvate dehydrogenase deficiency, respiratory chain defects) Non-ketotic hyperglycinaemia As above, plus: Blood for DNA mutation analysis CSF Lactate Mitochondrial DNA (blood & muscle) Muscle biopsy (histology & electron microscopy) Skin biopsy (enzymes of pyruvate metabolism) Plasma & CSF amino acids CSF: plasma glycine levels USS brain +/-MRI (agenesis corpus callosum, cerebellar abnormalities Molybdenum cofactor deficiency Pyridoxine dependent seizures Urine sulphite Urine amino acids ( hypoxanthine and taurine) Plasma and urine uric acid Pipecolic acid in plasma and CSF Trial of pyridoxine under EEG Liver Disorders Peroxisomal disorders Glycogen storage disease (types I, III, VI, IXX) Galactosaemia Blood VLCFA Leucocyte / liver biopsy (enzyme assay) Plasma lactate, CPK, uric acid Most diagnosed now on a specific genetic panel Red cell galactose-1-phosphate uridyl transferase activity If recently transfused, above test unreliable, so measure RBC galactose 1 phosphate as alternative ( ) Ophthalmology: for cataracts 11
12 Tyrosinaemia type I Plasma amino acids Urine organic acids Coagulation Investigate for renal Fanconi s syndrome α 1 Antitrypsin deficiency Serum α 1 antitrypsin genotype Niemann-Pick A Acid sphingomyelinase in leukocytes ( ) ( ) HDL cholesterol and cholesterol and TG Foam cells on histiocytes in bone marrow Cardiomyopathy Mitochondrial defects (respiratory chain) Pompe s disease (GSD type II) Fatty oxidation defects Mitochondrial defects CDG 1a syndrome Lysosomal storage disorders CSF lactate Mitochondrial DNA (blood & muscle) Muscle biopsy (histology & electron microscopy) Lymphocyte / skin fibroblast (enzyme assay) As stated under encephalopathy As stated under liver disease Serum transferrin isoelectric focusing Dysmorphism Lysosomal storage disorders Disorders of sterol synthesis CDG (Congenital disorders of glycosylation) syndrome Glutaric aciduria type II Peroxisomal disorders (e.g. Zellweger) Skin biopsy (enzyme assay) White cell enzymes Urine oligosaccharides and mucopolysaccharides as in cardiomyopathy Urine organic acids Plasma 7-dehydrocholesterol Skin biopsy Serum transferrin isoelectric focusing Skin biopsy (enzyme assay) Urine organic acids Blood carnitine & acylcarnitine, VLFA 12
13 **There are also a variety of specialist investigations done, e.g., specific enzyme studies on blood or skin fibroblast, muscle biopsies, etc It is good practice to save and freeze all urine passed for future analysis, and to save a heparinised blood sample before the first blood transfusion. General treatment Acute: This must be commenced as soon as preliminary results suggest a possibility of IEM. Please see website of BIMDG emergency treatment guidelines for further details ABC: basic neonatal intensive care Discontinue all milk feeds Protein content increases amino acid load; toxic in urea cycle defects and organic acidemias. Carbohydrate load contains lactose. Galactose is toxic in Galactosemia Provide adequate calories high calorie, protein free nutrition parenterally, or enterally if specific diagnosis has been made and feeds are judged safe. Correct hypoglycaemia; consider insertion of central access (UVC) early on. Correct acidosis beware of hypernatremia if many NaHCO 3 corrections are given Correct electrolyte disturbances Be vigilant for sepsis; note that some IEMs predispose to sepsis, e.g. galactosemia Insulin for reinforcement of anabolism (dose u/kg/hr) may be considered Liaise with Specialist team early: Dr Graham Shortland Consultant in Metabolic Diseases at UHW if in doubt. Treatment of Hyperammonaemia: Metabolic UHW, led by Dr Graham Shortland, recommend early contact for advice. Remember NH3 is very neurotoxic and needs to be reduced quickly. NH3 > 250 needs the following to commence ASAP, as well as contacting Metabolic team. NH3 > 450 should have haemofiltration - i.e. urgent transfer to PICU. 13
14 (a) Increase glucose infusion rate (GIR) to 7-8mg/Kg/min, even when glucose measurements are normal, and if necessary add insulin if hyperglycemia ensues. This serves to inhibit catabolism of endogenous protein (b) Treat any acidosis / electrolyte imbalance (c) Sodium Benzoate 250mg/Kg IV bolus over 90 minutes, followed by 250mg/Kg over 24 hours as continuous IVI. Together with: (d) Sodium Phenylbutyrate 250mg/Kg IV bolus over 90 minutes, followed by 250mg/Kg over 24 hours as IVI. (e) L-Arginine 200mg/Kg IV bolus over 90 minutes, followed by 8mg/Kg/hour IVI (All the above three drugs are now stocked and available from Singleton NICU If not in stock or out of date contact on call pharmacist) (f) Re-check NH3 four hours after onset of steps (c) to (e), to check for response. Some Specific Disorders Only a few of the more common disorders are covered here in minimal detail. For all of these disorders please refer to the referenced texts and to the BIMDG emergency guidelines for management Glycine encephalopathy (non ketotic hyperglycinaemia) - Basic defect is the glycine cleavage system - Reduced fetal movements in utero - Neonatal disease usually presents early, within 48 hours after birth - Hiccups - Hypotonia - Depressed level of consciousness - Seizures with burst suppression pattern on EEG - Plasma glycine levels variable - CSF and urine glycine are elevated - Organic acids in urine are normal - May be agenesis of corpus callosum - Diagnosis confirmed on transformed lymphocytes or liver biopsy 14
15 Maple Syrup Urine Disease: - Presents at around 1 week of age - Seizures - Encephalopathy - Vomiting - Frequent hypoglycaemia - Severe keto-acidosis and increased anion gap - Typical sweet odour in urine - Elevated leucine, isoleucine and valine in blood and urine Tyrosinaemia Type 1: Type 1 is due to a deficiency of fumaryl acetoacetase (FAH). This causes a build up of fumaryl and maleyl acetoacetate, responsible for renal and hepatic damage. - Progressive liver disease and renal tubular dysfunction - Hypoglycaemia due to pancreatic islet cell hyperplasia - Plasma tyrosine and methionine are raised - Phosphate and potassium levels are low - Generalised aminoaciduria, glycosuria, phosphaturia, rickets - Urinary organic acid increase succinyl acetone Treatment: NTBC 2 (2 nitro 4 trifluoro methylbenzoyl 1, 3 cyclohexanedione). NTBC inhibits hydroxy phenylpyruvate dioxygenase, so reducing toxic metabolites. 15
16 Pathway for Degradation of Tyrosine: Hyperammonaemia differential diagnosis: Inherited disorders - Urea cycle disorders - Organic acidemias (e.g. propionic acidaemia, methylmalonic acidaemia, etc) - Fatty acid oxidation disorders - Other inborn errors (ornithine amino transferase deficiency, HHH syndrome, etc) Acquired disorders - Transient Hyperammonaemia - Perinatal asphyxia - Herpes simplex infection - Liver disease - Any severe illness 16
17 UREA CYCLE DISORDERS: The urea cycle is a metabolic pathway enabling detoxification of ammonia and producing urea. Incidence : OTC (ornithine transcarbamylase), ASS (arginosuccinic acid synthetase) deficiency, ASL (arginosuccinic acid Lyase) deficiency, ARG (arginase deficiency), and NAGs (N acetyl glutamate synthetase) CPS (carbamyl phosphate synthetase) each have incidence of 1:100,000 approx.. Symptoms: Vomiting, drowsiness becoming unconscious, seizures, shock, hepatomegaly Diagnosis: Raised ammonia (>200 µmol/l) Plasma glutamine > 800 µmol/l Normal urinary organic acid profile. Remember to check LFT s, glucose, ammonia and clotting, frequently. 17
18 Early metabolic alkalosis, but can have metabolic acidosis after collapse Treatment please see page 14 Organic Acid Disorders: a) Propionic acidaemia Poor feeding, vomiting, drowsiness, coma Diagnosis Raised ammonia Ketoacidosis Hyperglycinaemia Raised urine organic acid and ketones Increased anion gap Long Term Treatment High carbohydrate Protein restriction Sodium bicarbonate Sodium benzoate Carnitine mg/kg/day b) Methyl Malonic Acidaemia: Clinically similar to proprionic acidaemia. Presents with vomiting, acidosis and neurological depression. Treatment: Withdraw protein, high carbohydrate ± insulin Vitamin B 12 Biotin Galactosaemia This presents after a few days with vomiting, failure to thrive, jaundice, neurological sequelae and possibly a superadded septicaemia, e.g. E. coli, which often starts as a UTI. There is usually hepatomegaly and may be cataracts. If suspected, take urine for reducing 18
19 substances and blood (lithium heparin) for erythrocyte galactose 1 phosphate uridyl transferase. If the baby has previously received a blood transfusion, enzyme analysis is unreliable and diagnosis is achieved measuring Galactose 1 phosphate in blood. Treatment: Stop all lactose and Galactose in diet. Give Nutramigen milk. Lactic Acidosis: In neonates, lactic acidosis is usually secondary to tissue hypoxia, and is not usually associated with ketosis. Increased Lactate is raised in a number of inborn errors a) Respiratory Chain (mitochondrial) Disease Encephalopathy Hypotonia ± Hypoglycaemia Possible Cardiomyopathy Changes in basal ganglia and brain stem on MRI. Also have raised CSF lactate. b) Fructose 1-6 bisphosphatase Deficiency Severe anion gap metabolic acidosis presenting in first week of life A defect in gluconeogenesis pathway Muscle weakness, hepatomegaly Hyperventilation. Hypoglycaemia. Apnea and possible death. High alanine, lactate and pyruvate Diagnosis established by genetic testing Avoid fasting and give dextrose infusion. 19
20 c) Pyruvate Dehydrogenase Deficiency Encephalopathy Hypotonia Severe acidosis increased pyruvate and lactate and alanine Patients deteriorate when given a high glucose intake. May improve if given high doses of thiamine. Need a high lipid, high protein, low carbohydrate regime (ketogenic diet). d) Organic acidaemia ( eg methylmalonic, proprionic, isovaleric, and glutaric type 1 acidemia e) Glycogen Storage Disease (GSD) Type 1: Presents with: Profound hypoglycaemia Lactic acidosis Hyperuricaemia Hyperlipidaemia Hepatomegaly Patients with Type 1b also have chronic Neutropenia with functional deficiencies of neutrophils and monocytes, which required GMCSF therapy. f) Fatty Acid Oxidation Defects: - A number of enzyme defects have been identified enzymes have specificity based on length of carbon chain. - Medium chain acyl co A dehydrogenase (MCAD) deficiency is most common in Caucasians. - Usually presents with hypoketotic hypoglycaemia - Some can cause Cardiomyopathy - May have increased CPK, and transaminases - Characteristic pattern of urine organic acids - Blood spots on Guthrie for acyl carnitine analysis by tandem mass spectrometry 20
21 Peroxisomal Disorders: - Zellweger s Syndrome, Infantile Refsums Disease, neonatal adrenoleukodystrophy - Raised liver enzymes - Dysmorphic - Severe neurological abnormalities plus punctate epiphyseal calcification, liver fibrosis - Request analysis of very long chain fatty acids Further reading 1. Text book Pediatric endocrinology and inborn errors of metabolism K Sarafoglou 2. Text book Atlas of metabolic diseases WL Nyhan, BA Barshop, PT Ozand 21
22 NOTES ON SPECIMENS BIOCHEMISTRY SINGLETON: MORRISTON: MEDICAL MORRISTON: Any sample that needs to be processed outside Swansea, is transported by the biochemists to the Morriston lab first. Some assays require the sample to be frozen as soon it reaches the lab. If a frozen sample needs to be transferred to UHW, this requires special transport, which is routinely available only twice a month from Morriston, thus if results are needed urgently, the lab personnel must be contacted, by a senior member of our team, to arrange earlier transport. PAEDIATRIC SPECIMEN BOTTLES USED ON NICU Lithium heparin: green top Fluoride oxalate: yellow top EDTA: lilac top Substance Sample Special measures PLEASE adhere to these Ammonia 500 micro litres Immediately put bottle in ice EDTA Transport to lab immediately Lab where processed Morriston Lactate Plasma amino acids Carnitines Free fatty acids VLCFA Ketones (3-hydroxy butyric acid) Insulin & C-peptide 500 micro litres Fluoride oxalate 600 micro litres Lithium heparin 3 X blood spots on Guthrie card 500 micro litres Fluoride oxalate 600 micro litres Lithium heparin 500 micro litres Fluoride oxalate 600 micro litres Lithium heparin Send to lab immediately Send to lab immediately Immediately put bottle in ice Transport to lab immediately Singleton UHW, Cardiff UHW, Cardiff UHW, Cardiff Southmead Hospital, Bristol UHW, Cardiff UHW, Cardiff ACTH 500 micro litres EDTA Immediately put bottle in ice Transport to lab immediately Cortisol 600 micro litres Lithium heparin Growth hormone 600 micro litres Lithium heparin Remember diurnal variation not well developed in neonates UHW, Cardiff Morriston Morriston 22
INBORN ERRORS OF METABOLISM (IEM) IAP UG Teaching slides
 INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children
 National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition
 Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Inborn Errors of Metabolism (IEM)
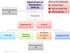 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Urea Cycle Defects. Dr Mick Henderson. Biochemical Genetics Leeds Teaching Hospitals Trust. MetBioNet IEM Introductory Training
 Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Module : Clinical correlates of disorders of metabolism Block 3, Week 2
 Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Inborn Errors of Metabolism in the Emergency Department. Will Davies June 2014
 Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT
 Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA
 UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
Training Syllabus CLINICAL SYLLABUS
 Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE
 THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD
 Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015
 Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism
 Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up
 HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
UREA CYCLE DISORDERS - The What, Why, How and When
 UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
Detection of inborn errors of metabolism in the newborn
 Arch Dis Child Fetal Neonatal Ed 2001;84:F205 F210 F205 REVIEW Willink Biochemical Genetics Unit, Manchester M27 4HA, UK A Chakrapani M A Cleary J E Wraith Correspondence to: Dr Cleary maureen@willink.demon.co.uk
Arch Dis Child Fetal Neonatal Ed 2001;84:F205 F210 F205 REVIEW Willink Biochemical Genetics Unit, Manchester M27 4HA, UK A Chakrapani M A Cleary J E Wraith Correspondence to: Dr Cleary maureen@willink.demon.co.uk
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting
 Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Metabolic Changes in ASD. Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius
 Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE
 SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Childhood epilepsy: the biochemical epilepsies. Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary
 Childhood epilepsy: the biochemical epilepsies Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary Definitions Epileptic Seizure Manifestation(s) of epileptic (excessive and/or
Childhood epilepsy: the biochemical epilepsies Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary Definitions Epileptic Seizure Manifestation(s) of epileptic (excessive and/or
Newborn Screening in Manitoba. Information for Health Care Providers
 Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Inborn Error Of Metabolism :
 Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Information for health professionals
 Introduction of a new screening test for newborn babies in Wales Newborn bloodspot screening for Medium chain acyl-coa dehydrogenase deficiency (MCADD) Newborn bloodspot screening for MCADD is being introduced
Introduction of a new screening test for newborn babies in Wales Newborn bloodspot screening for Medium chain acyl-coa dehydrogenase deficiency (MCADD) Newborn bloodspot screening for MCADD is being introduced
ESPEN Congress Madrid 2018
 ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
The laboratory investigation of lactic acidaemia. J Bonham/T Laing
 The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
Amino Acid Oxidation and the Urea Cycle
 Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese. DOI: /neo.
 Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: 10.1542/neo.9-7-e291 The online version of this article, along
Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: 10.1542/neo.9-7-e291 The online version of this article, along
Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism
 Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Paediatric Clinical Chemistry
 Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Inborn Errors of Metabolism Clinical Approach to Diagnosis and Treatment
 Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version)
 Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Introduction to Organic Acidemias. Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.
 Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Best Practice Guidelines for the Biochemical Investigation of Patients with Foetal and Neonatal Hydrops
 National Metabolic Biochemistry Network Best Practice Guidelines for the Biochemical Investigation of Patients with Foetal and Neonatal Hydrops INTRODUCTION Hydrops is defined as the presence of skin oedema
National Metabolic Biochemistry Network Best Practice Guidelines for the Biochemical Investigation of Patients with Foetal and Neonatal Hydrops INTRODUCTION Hydrops is defined as the presence of skin oedema
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM
 LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
7 Medical Genetics. Hemoglobinopathies. Hemoglobinopathies. Protein and Gene Structure. and Biochemical Genetics
 SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
Medical Foods for Inborn Errors of Metabolism
 Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
TITLE: NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA. Eilish O Connell, Clinical Education Facilitator, NCIMD
 NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
Lab Guide 2019 Metabolic Section Lab Guide
 Lab Guide 2019 Metabolic Section Lab Guide Quantitative Amino acids Plasma Plasma. Container/Tube: Preferred EDTA, Place immediately in ice. Acceptable: lithium heparin, sodium heparin. Patient preparation:
Lab Guide 2019 Metabolic Section Lab Guide Quantitative Amino acids Plasma Plasma. Container/Tube: Preferred EDTA, Place immediately in ice. Acceptable: lithium heparin, sodium heparin. Patient preparation:
Neonatal Biochemistry Investigation for Inherited Metabolic Disorders (IMDs)
 Neonatal Biochemistry Investigation for Inherited Metabolic Disorders (IMDs) Anne Green Birmingham Children s Hospital Leeds May 2005 Overview of how IMDs present cases Range of Disorders & Incidence disorders
Neonatal Biochemistry Investigation for Inherited Metabolic Disorders (IMDs) Anne Green Birmingham Children s Hospital Leeds May 2005 Overview of how IMDs present cases Range of Disorders & Incidence disorders
Presentation and investigation of mitochondrial disease in children
 Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Selective newborn screening of amino acid, fatty acid and organic acid disorders in the Kingdom of Bahrain.
 Selective newborn screening of amino acid, fatty acid and organic acid disorders in the Kingdom of Bahrain. Jamal Golbahar PhD Associate Professor of Molecular Medicine, Department of Molecular Medicine,
Selective newborn screening of amino acid, fatty acid and organic acid disorders in the Kingdom of Bahrain. Jamal Golbahar PhD Associate Professor of Molecular Medicine, Department of Molecular Medicine,
Staff at the Nottingham Children s Hospital. Guidelines process; paediatric endocrinology team
 Hypoglycaemia Title of Guideline Contact Name and Job Title (author) Hypoglycaemia in infants and children: aetiology, investigation and treatment Dr. Hoong-Wei Gan ST6 Paediatric Endocrinology & Diabetes
Hypoglycaemia Title of Guideline Contact Name and Job Title (author) Hypoglycaemia in infants and children: aetiology, investigation and treatment Dr. Hoong-Wei Gan ST6 Paediatric Endocrinology & Diabetes
Most common is the congenital adrenogenital syndrome (AGS) or congenital adrenal hyperplasia (CAH) due to 21-hydroxylase deficiency.
 Newborn Screening Examination parameters: TSH-neonatal (hypothyreosis), 17-OH progesterone (AGS), galactose (galactosemia), galactose-uridyl transferase (galacto semia), biotinidase (biotinidase ), phenylalanine
Newborn Screening Examination parameters: TSH-neonatal (hypothyreosis), 17-OH progesterone (AGS), galactose (galactosemia), galactose-uridyl transferase (galacto semia), biotinidase (biotinidase ), phenylalanine
Inborn error of metabolism
 Inborn error of metabolism The lecture is given by Dr Kefah Al qa qa, Consultant metabolic pediatrician, in Queen Rania Al Abdulla children hospital, on Thursday 11/12/2014. Let s tart Metabolism: refers
Inborn error of metabolism The lecture is given by Dr Kefah Al qa qa, Consultant metabolic pediatrician, in Queen Rania Al Abdulla children hospital, on Thursday 11/12/2014. Let s tart Metabolism: refers
Hypoglycaemia of the neonate. Dr. L.G. Lloyd Dept. Paediatrics
 Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Newborn Screening: Blood Spot Disorders
 Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Nutritional Management of Inborn Errors of Metabolism. Kay Davis, RD, CSP Esther Berenhaut, RD, CSP, CSR Aug 28, 2017
 Nutritional Management of Inborn Errors of Metabolism Kay Davis, RD, CSP Esther Berenhaut, RD, CSP, CSR Aug 28, 2017 OBJECTIVES Brief overview of newborn screening of metabolic disorders, inheritance patterns.
Nutritional Management of Inborn Errors of Metabolism Kay Davis, RD, CSP Esther Berenhaut, RD, CSP, CSR Aug 28, 2017 OBJECTIVES Brief overview of newborn screening of metabolic disorders, inheritance patterns.
Hyperglycaemia. Clinical presentation. Definition of hyperglycaemia. Approach to the problem
 Hyperglycaemia 1 Clinical presentation Hyperglycaemia is usually picked up incidentally on routine blood glucose assessment or in response to finding glycosuria. It may be noted as part of the workup of
Hyperglycaemia 1 Clinical presentation Hyperglycaemia is usually picked up incidentally on routine blood glucose assessment or in response to finding glycosuria. It may be noted as part of the workup of
Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff
 Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Metabolic diseases of the liver
 Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick Neonatal Pharmacist
 CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital
 e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
ANATOMY OF A METABOLIC CRISIS: FAOD-style. Mark S. Korson, MD Tufts Medical Center Boston, MA
 ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
Investigation of metabolic encephalopathy
 Investigation of metabolic encephalopathy Encephalopathy may be a presenting sign in a wide range of medical conditions. G F van der Watt, FCPath (SA) Chem, MMed, MB ChB, DA (SA) Principal Pathologist
Investigation of metabolic encephalopathy Encephalopathy may be a presenting sign in a wide range of medical conditions. G F van der Watt, FCPath (SA) Chem, MMed, MB ChB, DA (SA) Principal Pathologist
Inborn errors of metabolism around time of birth
 Review Inborn errors of metabolism around time of birth J V Leonard, A A M Morris Inborn errors of metabolism commonly present around the time of birth. Although most affected babies are born healthy and
Review Inborn errors of metabolism around time of birth J V Leonard, A A M Morris Inborn errors of metabolism commonly present around the time of birth. Although most affected babies are born healthy and
Methylmalonic aciduria
 Methylmalonic aciduria Introductory information Written by: F. Hörster, S. Kölker & P. Burgard Reviewed & Revised for North America by: S. van Calcar Methylmalonic aciduria MMA 2 Methylmalonic aciduria
Methylmalonic aciduria Introductory information Written by: F. Hörster, S. Kölker & P. Burgard Reviewed & Revised for North America by: S. van Calcar Methylmalonic aciduria MMA 2 Methylmalonic aciduria
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA
 NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
Paediatric Hypoglycaemia and the Laboratory. AACB Webinar, 8 th April 2015 Tina Yen
 Paediatric Hypoglycaemia and the Laboratory AACB Webinar, 8 th April 2015 Tina Yen Synopsis Definition and classification Newborn and Neonatal Hypoglycaemia Transient Persistant Hypoglycaemia in infants
Paediatric Hypoglycaemia and the Laboratory AACB Webinar, 8 th April 2015 Tina Yen Synopsis Definition and classification Newborn and Neonatal Hypoglycaemia Transient Persistant Hypoglycaemia in infants
Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease
 Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease Patient s Name: Date of Birth: MRN in KFSH&RC: Please read carefully. Meticulous and prompt treatment
Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease Patient s Name: Date of Birth: MRN in KFSH&RC: Please read carefully. Meticulous and prompt treatment
MetBioNet Best Practice Guidelines. Investigation of an inherited metabolic cause of cardiomyopathy
 Introduction MetBioNet Best Practice Guidelines Investigation of an inherited metabolic cause of Inborn errors of metabolism (IEM) account for at least 5% of cases of. In some disorders, is the major cause
Introduction MetBioNet Best Practice Guidelines Investigation of an inherited metabolic cause of Inborn errors of metabolism (IEM) account for at least 5% of cases of. In some disorders, is the major cause
Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine
 Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine Harvey Levy, MD Mark Korson, MD Piero Rinaldo, MD, PhD Larry Sweetman, PhD K. Michael Gibson, PhD Charlie Roe, MD Jerry
Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine Harvey Levy, MD Mark Korson, MD Piero Rinaldo, MD, PhD Larry Sweetman, PhD K. Michael Gibson, PhD Charlie Roe, MD Jerry
Understanding metabolic disease
 Understanding metabolic disease Let s build a restaurant Chris Hendriksz Birmingham Children s Hospital 2006 The Task Let s build a restaurant! 2 Partners join to draw the plan. How can we change the
Understanding metabolic disease Let s build a restaurant Chris Hendriksz Birmingham Children s Hospital 2006 The Task Let s build a restaurant! 2 Partners join to draw the plan. How can we change the
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS
 PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE. Bwee Tien Poll-The Amsterdam UMC The Netherlands
 CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
Current Management and Future Developments in Metabolic Disease
 Current Management and Future Developments in Metabolic Disease APAGBI Annual Scientific Meeting Friday 15 th May 2015 Dr Saikat Santra Birmingham Children s Hospital, UK Outline Metabolic disorders in
Current Management and Future Developments in Metabolic Disease APAGBI Annual Scientific Meeting Friday 15 th May 2015 Dr Saikat Santra Birmingham Children s Hospital, UK Outline Metabolic disorders in
Newborn Bloodspot Screening (NBS) Training for Health Visitors. December 2017
 Newborn Bloodspot Screening (NBS) Training for Health Visitors www.newbornbloodspotscreening.wales.nhs.uk December 2017 Aims To enable you to gain a clear understanding of the following: Aim and rationale
Newborn Bloodspot Screening (NBS) Training for Health Visitors www.newbornbloodspotscreening.wales.nhs.uk December 2017 Aims To enable you to gain a clear understanding of the following: Aim and rationale
Inborn Errors of Metabolism. Metabolic Pathway. Digestion and Fasting. How is Expanded Newborn Screening Different? MS/MS. The body is a factory.
 Inborn Errors of Metabolism The body is a factory. Inborn errors of metabolism are rare genetic disorders in which the body cannot properly turn food into energy. The disorders are usually caused by defects
Inborn Errors of Metabolism The body is a factory. Inborn errors of metabolism are rare genetic disorders in which the body cannot properly turn food into energy. The disorders are usually caused by defects
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company Chapter 30 Outline Amino acids are obtained from the
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company Chapter 30 Outline Amino acids are obtained from the
CARE OF THE NEWBORN HYPOGLYCAEMIA
 CARE OF THE NEWBORN HYPOGLYCAEMIA Background Definition A true blood glucose of less than 2.6 mmol/l venous sample. Neonatal hypoglycaemia is commonly defined as a true blood glucose of less than 2.6 mmol/l
CARE OF THE NEWBORN HYPOGLYCAEMIA Background Definition A true blood glucose of less than 2.6 mmol/l venous sample. Neonatal hypoglycaemia is commonly defined as a true blood glucose of less than 2.6 mmol/l
Glycogen Storage Disease
 Glycogen Storage Disease 1 Introduction The food we eat is usually used for growth, tissue repair and energy. The body stores what it does not use. Excess sugar, or glucose, is stored as glycogen in the
Glycogen Storage Disease 1 Introduction The food we eat is usually used for growth, tissue repair and energy. The body stores what it does not use. Excess sugar, or glucose, is stored as glycogen in the
Inborn errors of metabolism
 ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
PARENTERAL NUTRITION
 PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
TITLE: NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS. Eilish O Connell, Clinical Education Facilitator, NCIMD
 NO. OF PAGES: Page 1 of 16 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NO. OF PAGES: Page 1 of 16 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
Dysmorphology Guy Besley
 Dysmorphology Guy Besley Willink Biochemical Genetics Unit, Manchester Children s s Hospital Dysmorphic presentation Congenital malformation Disorder of embryogenesis Intrauterine insult infection; chromosomal/genetic
Dysmorphology Guy Besley Willink Biochemical Genetics Unit, Manchester Children s s Hospital Dysmorphic presentation Congenital malformation Disorder of embryogenesis Intrauterine insult infection; chromosomal/genetic
ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt
ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt
Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center
 Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center Kefah Al-Qa qa MD*, Wajdi Amayreh MD*, Ali Al-Hawamdeh MD* ABSTRACT Objective: To describe the different
Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center Kefah Al-Qa qa MD*, Wajdi Amayreh MD*, Ali Al-Hawamdeh MD* ABSTRACT Objective: To describe the different
Lecture 10 - Protein Turnover and Amino Acid Catabolism
 Lecture 10 - Protein Turnover and Amino Acid Catabolism Chem 454: Regulatory Mechanisms in Biochemistry University of Wisconsin-Eau Claire 1 Introduction 2 Proteins are degraded into amino acids. Protein
Lecture 10 - Protein Turnover and Amino Acid Catabolism Chem 454: Regulatory Mechanisms in Biochemistry University of Wisconsin-Eau Claire 1 Introduction 2 Proteins are degraded into amino acids. Protein
For Your Baby s Health Department of Health
 Newborn Screening For Your Baby s Health Department of Health Why is my baby tested? To help make sure your baby will be as healthy as possible. The blood test provides important information about your
Newborn Screening For Your Baby s Health Department of Health Why is my baby tested? To help make sure your baby will be as healthy as possible. The blood test provides important information about your
Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when
 CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
Isovaleric Acidemia: Quick reference guide
 Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Metabolic Emergencies and the Pediatrician
 Metabolic Emergencies and the Pediatrician Stephen G. Kahler, MD Professor of Pediatrics Section of Genetics and Metabolism, UAMS and ACH Hot Springs, AR March 8, 2012 INHERITED METABOLIC DISORDERS HOW
Metabolic Emergencies and the Pediatrician Stephen G. Kahler, MD Professor of Pediatrics Section of Genetics and Metabolism, UAMS and ACH Hot Springs, AR March 8, 2012 INHERITED METABOLIC DISORDERS HOW
NEWBORN METABOLIC SCREEN, MINNESOTA
 Lab Dept: Test Name: Chemistry NEWBORN METABOLIC SCREEN, MINNESOTA General Information Lab Order Codes: Synonyms: CPT Codes: Test Includes: PKUN Newborn Screen for Hyopothyroidism, Phenylketonuria (PKU),
Lab Dept: Test Name: Chemistry NEWBORN METABOLIC SCREEN, MINNESOTA General Information Lab Order Codes: Synonyms: CPT Codes: Test Includes: PKUN Newborn Screen for Hyopothyroidism, Phenylketonuria (PKU),
So Much More Than The PKU Test
 Newborn Metabolic Screening So Much More Than The PKU Test Sarah Viall, MSN, PPCNP BC Newborn Screening Program Coordinator Division of Genetics & Metabolism Conflicts of Interest I have no conflicts of
Newborn Metabolic Screening So Much More Than The PKU Test Sarah Viall, MSN, PPCNP BC Newborn Screening Program Coordinator Division of Genetics & Metabolism Conflicts of Interest I have no conflicts of
Metabolic Disorders Screened Overseas but not Screened in Australia Condition Features Inherited Diagnosis Treatment Newborn Screen
 Metabolic Disorders ed Overseas but not ed in Australia Biotinidase Deficiency Severe form causes seizures & delay Biotin can prevent complications NZ, USA Tyrosinaemia Type I Coma & death before age 10
Metabolic Disorders ed Overseas but not ed in Australia Biotinidase Deficiency Severe form causes seizures & delay Biotin can prevent complications NZ, USA Tyrosinaemia Type I Coma & death before age 10
Inborn Errors of Metabolism
 30 Inborn Errors of Metabolism Inborn errors of metabolism (IEM) are disorders in which there is a block in the normal metabolic pathway that is caused by a genetic defect of a specific enzyme. The number
30 Inborn Errors of Metabolism Inborn errors of metabolism (IEM) are disorders in which there is a block in the normal metabolic pathway that is caused by a genetic defect of a specific enzyme. The number
Nitrogen Metabolism. Overview
 Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Inherited Metabolic Disease
 IMD and Newborn Screening Specialist Portfolio Tutorial Jenna Waldron 17th March 2014 Inherited Metabolic Disease What is IMD? Gene mutations prevent synthesis of protein or cause synthesis of abnormal
IMD and Newborn Screening Specialist Portfolio Tutorial Jenna Waldron 17th March 2014 Inherited Metabolic Disease What is IMD? Gene mutations prevent synthesis of protein or cause synthesis of abnormal
UPDATE ON UREA CYCLE DISORDERS TREATMENT
 UPDATE ON UREA CYCLE DISORDERS TREATMENT George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Icahn School of Medicine at Mount Sinai Disclosure
UPDATE ON UREA CYCLE DISORDERS TREATMENT George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Icahn School of Medicine at Mount Sinai Disclosure
Jana Novotná, Bruno Sopko. Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ.
 Amino acid metabolism II. Urea cycle Jana Novotná, Bruno Sopko Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ. Nitrogen balance Tissue proteins
Amino acid metabolism II. Urea cycle Jana Novotná, Bruno Sopko Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ. Nitrogen balance Tissue proteins
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company In the cytosol of a cell amino groups from amino acids
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company In the cytosol of a cell amino groups from amino acids
Fatty Acid Oxidation Disorders- an update. Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London
 Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
inborn errors of metabolism biochemical basis
 inborn errors of metabolism biochemical basis What is an inborn error of metabolism (IEM)? Genetically determined biochemical disorders, that affect an individual s ability to convert nutrients or to use
inborn errors of metabolism biochemical basis What is an inborn error of metabolism (IEM)? Genetically determined biochemical disorders, that affect an individual s ability to convert nutrients or to use
ACUTE & CHRONIC ETHANOL EFFECTS An Overview
 ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN *
 For the use of a registered medical practitioner or a Hospital or a Laboratory only Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN * DESCRIPTION: NIRMIN * is a clear, colourless injection
For the use of a registered medical practitioner or a Hospital or a Laboratory only Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN * DESCRIPTION: NIRMIN * is a clear, colourless injection
