The Roadmap to Close the Gap for Vision
|
|
|
- Emery Erik Leonard
- 5 years ago
- Views:
Transcription
1 The Roadmap to Close the Gap for Vision Contact Professor Hugh R Taylor AC Indigenous Eye Health Melbourne School of Population and Global Health The University of Melbourne Level 5, 207 Bouverie St Carlton, Victoria 3010 Phone: h.taylor@unimelb.edu.au Website: The Roadmap to Close the Gap for Vision and the Annual Updates on the Implementation of The Roadmap to Close the Gap for Vision have been endorsed by these organisations. Authorised by the Harold Mitchell Chair of Indigenous Eye Health, Melbourne School of Population and Global Health, The University of Melbourne. Copyright Copyright The University of Melbourne 2017 Copyright in this publication is owned by The University and no part of it may be reproduced without the permission of The University. Disclaimer Statement on Privacy Policy The University has used its best endeavours to ensure that material contained in this publication was correct at the time of printing. The University gives no warranty and accepts no responsibility for the accuracy or completeness of information and the University reserves the right to make changes without notice at any time in its absolute discretion. When dealing with personal or health information about individuals, The University of Melbourne is obliged to comply with the Information Privacy Act 2000 and the Health Records Act For further information refer to: privacy/ Intellectual Property Vision loss is 11% of the Indigenous health gap. Each additional dollar gives $2.50 of cost benefit. For further information refer to: School School School School of School ofof ofof Population Population Population Population Population and and and and and Global Global Global Global Global Health Health Health Health HealthMelbourne School of Population and Global Health 2015
2 This summary report was updated by Professor Hugh R Taylor AC and Mitchell D Anjou AM of Indigenous Eye Health, Melbourne School of Population and Global Health, The University of Melbourne. We acknowledge and thank the many community members, colleagues and stakeholders who have been consulted and participated in the development of these recommendations. This report summarises and develops the findings and recommendations presented in the following reports: Taylor HR, Anjou MD, Boudville AI, McNeil RJ. The Roadmap to Close the Gap for Vision: Full Report. Melbourne: Indigenous Eye Health Unit, Melbourne School of Population Health, The University of Melbourne, ISBN ; Taylor HR, Anjou MD, Boudville AI, McNeil RJ. The Roadmap to Close the Gap for Vision: Full Report: Supplements. 2012; available from: roadmap-to-close-the-gap-for-vision It also draws on the following reports: Taylor HR, Keeffe JE, Arnold AL, Dunn RA, Fox SS, Goujon N, Xie J, Still R, Burnett A, Marolia M, Shemesh T, Carrigan J and Stanford E (2009). National Indigenous Eye Health Survey, Minum Barreng (Tracking Eyes). Melbourne, Indigenous Eye Health Unit, Melbourne School of Population Health in collaboration with the Centre for Eye Research Australia and the Vision CRC (ISBN ) Turner A, Mulholland W and Taylor HR (2009). Outreach Eye Services in Australia. Melbourne, Indigenous Eye Health Unit, Melbourne School of Population Health, The University of Melbourne (ISBN ) Kelaher M, Ferdinand A, Ngo S, Tambuwla N and Taylor HR (2010). Access to Eye Health Services among Indigenous Australians: An area level analysis. Melbourne, Centre for Health Policy, Programs and Economics and Indigenous Eye Health Unit, Melbourne School of Population Health, The University of Melbourne (ISBN ) Taylor HR, Gruen R, Bragge P, Chau M, Wasiak J, Hewitt A, Forbes A, Parkhill A, Clavisi O, Burchill J, Carrigan J and Sekkoua H (2010). Accuracy of Screening Methods for Diabetic Retinopathy: A Systematic Review. Melbourne, The University of Melbourne and Monash University (ISBN ) Taylor HR, Gruen R, Wasiak J, Hewitt A, Bragge P, Chau M, Forbes A, Parkhill A, Clavisi O, Burchill J, Carrigan J, Ferguson R and Sekkouah H (2010). Trachoma, Antibiotic Treatments of Trachoma: A Systematic Review. Melbourne, The University of Melbourne and Monash University (ISBN ) Hooshmand J, Taylor HR and Stanford E (2010). Trachoma Resource Book. Melbourne, Indigenous Eye Health Unit, Melbourne School of Population Health, The University of Melbourne (ISBN ) Taylor HR, Dunt D, Hsueh YS and Brando A (2011). Projected Needs for Eye Care Services for Indigenous Australians. Melbourne, Indigenous Eye Health Unit, Melbourne School of Population Health, The University of Melbourne (ISBN ) Jones JN, Henderson G, Poroch N, Anderson I and Taylor HR (2011). A Critical History of Indigenous Eye Health Policy-Making: Towards Effective System Reform. Melbourne, Indigenous Eye Health Unit, Melbourne School of Population Health, The University of Melbourne (ISBN ) Hsueh YA, Brando A, Dunt D, Anjou MD and Taylor HR (2011). The Cost of Closing the Gap for Vision. Melbourne, Indigenous Eye Health Unit and Centre for Health Policy, Programs and Economics, Melbourne School of Population Health, The University of Melbourne (ISBN ) IEH (2015) Annual Update on the Implementation of The Roadmap to Close the Gap for Vision. Melbourne, Indigenous Eye Health, Melbourne School of Population Health, The University of Melbourne. All of these reports are available on the Indigenous Eye Health website at: Published by Indigenous Eye Health, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia First published September 2011 ISBN Reprinted July 2012 ISBN Revised and reprinted January 2013 ISBN Revised and reprinted April 2013 ISBN Revised and reprinted July 2014 ISBN Revised and reprinted September 2015 ISBN Reprinted (minor revision) September 2017 ISBN
3 Table of Contents Introduction 1 Highlights 1 Current Status of Indigenous Eye Health 2 Causes of Vision Loss 3 The Patient Journey 4 Planning the Pathway of Care 5 Diabetes and Eye Care 6 Recommendations and Conditions 7 Why Eye Care is Important 8 Nine False Reasons 9 Roadmap Recommendations 10 The Cost to Close the Gap for Vision 15 Activities for the Commonwealth 16 Regional Implementation 17 Indicators 17 Trachoma 18 Eye Health and Roadmap Resources 20 Glossary Inside back cover Introduction Good quality eye services are fundamental to improving the health of Indigenous Australians. This report builds on the National Indigenous Eye Health Survey. It recommends policy changes to improve the quality and sustainability of eye care services. We acknowledge and build on the successful eye care programs found in several areas that provide high quality eye care for Indigenous Australians. The Roadmap builds on community consultation and control, the regional delivery of services and national health reforms. It stresses the assessment of population-based needs, strong co-ordination, monitoring of performance and national accountability. It does not include implementation details, phase in costing or additional or replacement costs for infrastructure or equipment. Highlights > 2008 blindness rates in Indigenous adults are 6 times the rate in mainstream > Vision loss accounts for 11% of the health gap > 94% of the vision loss is preventable or treatable but 35% of Indigenous adults have never had an eye exam > The Roadmap consists of 42 specific interlocking recommendations > Eye services need to be increased in remote areas and their utilisation increased in all areas > Efficient eye care requires co-ordination along the pathway of care to improve efficiency and patient outcomes > Trachoma elimination needs to include all endemic areas and be continued until it is eliminated > Eye services require monitoring and evaluation of agreed performance indicators by a nationally accountable body > Closing this gap is evidence-based, sector-endorsed, cost effective and highly achievable 1
4 Current Status of Indigenous Eye Health The 2008 National Indigenous Eye Health Survey determined the magnitude, distribution and causes of vision loss in Aboriginal and Torres Strait Islander people NIEHS site locations It examined 1694 children (5 15 years) and 1189 adults (40 years and over) in 30 sites across the country. Indigenous children > > better vision than mainstream Indigenous adults > > 6 times as much blindness > > 94% of vision loss was unnecessary and is preventable or treatable The unmet need is similar in urban and regional areas as in remote areas Low Vision (<6/12) in Indigenous Adults AMD 2% Glaucoma 1% Cataract 27% Vision Loss in Adults 80% 70% 60% 50% Low vision in Indigenous Adults Blindness in Indigenous Adults Low vision in Non-Indigenous Adults Blindness in Non-Indigenous Adults Refractive Error 54% Trachoma 2% Optic Atrophy 1% Unknown 1% Corneal scarring 1% Retinitis Pigmentosa 1% Diabetic Retinopathy 12% Blindness (<6/60) in Indigenous Adults 40% 30% Refractive Error 14% Cataract 32% 20% Unknown 13% 10% 0% N/A Age Optic Atrophy 14% Trauma 4% Retinal detachment 4% Trachoma 9% Diabetic Retinopathy 9% Crude Prevalence Rates of Vision Loss in Indigenous Australians 2 State Children Adults Regions Children Adults Low Vision Blindness Low Vision Blindness Low Vision Blindness Low Vision Blindness NSW 3.3% 0.4% 5.7% 2.4% Major City 4.5% 0.6% 7.7% 2.6% NT 0.8% 0% 9.1% 3% Inner Regional 2.6% 0% 7.8% 2.4% QLD 0.9% 0.3% 11.6% 0.4% Outer Regional 1.5% 0% 6.6% 0.6% SA 0% 0% 9.3% 1.6% Remote 0.9% 0% 10.2% 0.8% TAS 0% 0% 4.7% 0% Very Remote Coastal 1.1% 0.3% 9.5% 1.1% VIC 0% 0% 6.9% 6.9% Very Remote Inland 0.3% 0.3% 12.7% 3.9% WA 1.9% 0.2% 12% 1.8% TOTAL 1.5% 0.2% 9.4% 1.9% Rates of vision loss do not show significant jurisdictional or regional variation the need for eye care is nationwide
5 Causes of Vision Loss Four conditions cause 94% of the vision loss. Each is readily amenable to treatment Key Finding 1. Refractive Error > > Only 20% of Indigenous adults wear glasses for distance compared to 56% in mainstream > > Lack of reading glasses meant that 39% could not see normal print > > An optometrist working in an Aboriginal Health Service led to much better outcomes 2. Cataract > > Blinding Cataract is 12 times more common in Indigenous adults > > But rates of Cataract surgery are 7 times lower > > Waiting time for Cataract surgery is 56% longer than mainstream > > Indigenous Australians are 4 times more likely to have to wait more than 1 year for Cataract surgery 3. Diabetes > > 37% of Indigenous adults have Diabetes and 13% have already lost vision > > 98% of blindness from Diabetes is preventable with early detection and timely treatment > > Only 20% have had an eye exam in the last year > > Only 37% needing laser surgery have received it 4. Trachoma > > Two thirds of remote communities have endemic Trachoma > > Adults with Trachoma scarring and in-turned lashes (trichiasis) are found across the country > > Trachoma can be eliminated with the SAFE Strategy (see pages 18 19) Implications > > Readily accessible eye services are needed for all Australians > > More and better co-ordinated visits by optometrists or ophthalmologists are required in more remote areas > > Better co-ordination and links between Aboriginal Health Services, clinics and hospitals are needed in urban areas > > Cataract surgery needs to be made readily available for all Australians > > Adequate and sustainable funding is required for visiting specialist services > > Proper funding for patient travel to regional hospitals for surgery is required > > Adequate surgical facilities, time and staff must be committed for Cataract surgery > > Excellent co-ordination is required between the patient, community, clinic, hospital and the surgical team > > All Indigenous people with Diabetes need an eye exam every year and better access to Diabetes education > > Good co-ordination and recall mechanisms are needed > > Sustainable funding (Medicare) is required for retinal photography > > Prompt referral is required for those found to have Diabetic eye disease > > Laser surgery should be available locally but good quality slit lamps and portable lasers are needed > > The extent of Trachoma needs to be mapped clearly > > All children at risk need to be checked regularly > > Elderly people across the country need to be checked for in-turned lashes (trichiasis) and operated on if necessary > > Trachoma elimination programs need to be fully implemented in endemic areas Vision loss causes 11% of the health gap; it is behind cardiovascular disease and diabetes, equal with trauma but ahead of alcoholism and stroke Most vision loss can be corrected overnight 3
6 The Patient Journey Successful eye health outcomes involve co-ordination of both eye care services and the patient journey The referral pathway is a leaky pipe with a blockage at its end It is often very inefficient and wasteful of services Many people drop out Because of this, others do not enter Levels of Co-ordination Community > > Community liaison provides a vital link between individual community members, their families and the clinic and its services > > This may include identification, transport, interpretation, translation and moral support Clinic, Primary Eye Care > > Referral of more complex cases to visiting eye team > > Maintenance of patient records and referral lists for visiting eye team > > Scheduling of visits by visiting eye teams > > Co-ordination with other visiting specialists > > Co-ordination of exam rooms, accommodation, equipment and local staff > > Make arrangements for referrals to Regional Hospital > > Schedule follow up visits as required Eye Team, Secondary Eye Care > > Co-ordination of visits with clinic and community > > Update patient records as necessary > > Communication and co-ordination between visiting optometrists and ophthalmologists > > Mechanism for communication and co-ordination with other visiting specialists > > Specific equipment items brought with team (e.g. lasers, slit lamp) > > Organise a list/information about patients waiting to be seen > > Assistance with patient identification, transport, translation, explanation and support > > Clerical support for forms and paper work > > Referral systems for further management or surgery Regional Hospital, Tertiary Eye Care > > Organisation of the clinic space, theatre time, staff, accommodation, travel and surgical supplies for the visiting eye teams > > Co-ordination with other visiting specialists > > Organisation and supply of surgical equipment > > Co-ordination of patients who require surgery with community and clinic > > Organisation of travel and other arrangements for patients National/State/Territory > > Co-ordination of other specialist and allied health visits with the visiting eye team > > Oversight of co-ordination performed at different levels, recruitment, training and support > > Oversight of distribution of visiting eye teams (and other specialists) including ratio of optometric and ophthalmic visits and frequency of visits 4
7 Planning the Pathway of Care Eye Care Co-ordination and Clinical Service Requirements for a Region and a Community Community (days*) Region of 10,000 people Visiting Hospital Total Service (days*) (days*) (days*) EFT Community (days*) 'Community of 500 people Visiting Hospital Service (days*) (days*) Total (days*) Optometry Clinics Patient organisation 2 hr/pt (specs hr) Transport 1 hr/patient Clinic organisation 4 hr/clinic day Team organisation 4 hr/clinic day Clinic support 8 hr/clinic day Optometry Consultations Glasses exams 640 people Diabetic exams 962 people Other eye exams 98 people 32 people 48 people 5 people Ophthalmology Clinics Patient organisation 2 hr/pt Transport 1 hr/pt Clinic organisation 4 hr/clinic day Team organisation 4 hr/clinic day Clinic support 8 hr/clinic day Ophthalmology Consultations Diabetic laser 112 people 6 people Hospital Patient organisation 2 hr/pt (3 hr preop) Transport 1 hr/pt Clinic organisation 4 hr/clinic day Team organisation 4 hr/clinic day Ophthalmology Surgery Catarct surgery 95 people Trichiasis surgery 36 people 5 people 2 people TOTAL Optometrist Optometry patients 1700 people Ophthalmologist Ophthalmology patients 243 people 85 people 12 people * days unless indicated as people 5
8 Diabetes and Eye Care No Indigenous person with Diabetes should be allowed to go more than one year without an eye examination Three quarters of those people needing annual eye care have Diabetes A multi-sectoral whole of system approach is required to address the significant burden of Diabetes and Diabetic eye disease The Pathways for Eye Care Community Those needing eye exam each year Eye Examina4on Optometrist/ Ophthalmologist Review in annual health check Refrac+ve Error 23% Trichiasis 1% Cataract 12% Glasses prescribed Refer requires surgery Hospital Cataract surgery Trichiasis surgery Those with Diabetes 76% Refrac+ve Error 33% Glasses prescribed Consulta4on Ophthalmologist Laser treatment Eye Examina4on Optometrist/ Ophthalmologist Cataract 18% Refer requires surgery Review in 12 months Camera/ Visual Acuity Diabe+c Re+nopathy 29% Refer requires treatment If we can fix and make the eye care pathway for people with Diabetes work effectively, we will have created the system change to support eye care for the whole community. 6
9 Recommendations and Conditions to illustrate the contribution of recommendations to the main eye conditions and reinforce the interdependence between components of the Roadmap Cataract Refractive error Diabetic retinopathy Trachoma 1 PRIMARY EYE CARE AS PART OF COMPREHENSIVE PRIMARY HEALTH CARE 1.1 Enhancing eye health capacity in primary health services 1.2 Health assessment items include eye health 1.3 Retinal photography 1.4 Eye health inclusion in clinical software 2 INDIGENOUS ACCESS TO EYE HEALTH SERVICES 2.1 Aboriginal Health Services and eye health 2.2 Cultural safety in mainstream services 2.3 Low cost spectacles 2.4 Hospital surgery prioritisation 3 CO-ORDINATION 3.1 Local eye care co-ordination 3.2 Clear pathways of care 3.3 Workforce identification and roles 3.4 Eye care support workforce 3.5 Case co-ordination 3.6 Partnerships and agreements 4 EYE HEALTH WORKFORCE 4.1 Provide eye health workforce to meet population needs 4.2 Improve contracting and management of visiting services 4.3 Appropriate resources for eye care in rural and remote areas 4.4 Increase utilisation of services in urban areas 4.5 Billing for visiting MSOAP supported services 4.6 Rural education and training of eye health workforce 5 ELIMINATION OF TRACHOMA 5.1 Definition of areas of risk 5.2 Effective interventions Surveillance and evaluation 5.4 Certification of elimination 6 MONITORING AND EVALUATION 6.1 Managing local eye service performance 6.2 State and National performance 6.3 Collating existing eye data sources 6.4 National benchmarks 6.5 Quality assurance 6.6 Primary health service self-audit in eye health 6.7 Program evaluation 7 GOVERNANCE 7.1 Community engagement 7.2 Local Hospital Networks and Primary Health Networks 7.3 State/Territory management 7.4 National oversight 7.5 Program interdependence 8 HEALTH PROMOTION AND AWARENESS 8.1 Eye health promotion 8.2 Social marketing eye care services 9 HEALTH FINANCING 9.1 Current spending on Indigenous eye health (non Trachoma) 9.2 Current spending on Trachoma 9.3 Full additional annual capped funding required 9.4 Cost to Close the Gap for Vision funded for five years Total number of recommendations A single change cannot fix the provision of eye care, each issue needs to be addressed 7
10 Why Eye Care is Important Doing Something about Vision Loss and Eye Health is Important Vision loss is common > > Most common self-reported health complaint > > Blindness rates are 6 times higher > > Blindness from Cataract is 12 times higher, surgery rates 7 times less Vision loss has a big impact > > 11% of Years of Life Lost to disability for Indigenous people > > Equal 3rd leading cause of the Gap for health > > Increases mortality rates by at least 2 fold > > Significantly affects the individual, family and community Vision loss is discrete and fixable > > Cataract surgery restores vision overnight and costs ~$3,000 per QALY > > New glasses improve vision right away > > Diabetic blindness: 98% is preventable and screening costs $15,000 per QALY > > Trachoma can be eliminated with the SAFE Strategy Vision loss provides a template for other specialist health care > > Requires active community engagement > > Requires good integration into primary health care > > Needs proper co-ordination within a regional basis > > Requires whole of system approach > > The lessons learnt will help link other specialist services with comprehensive primary care Vision loss can reflect the underlying social determinants of health > > Maintaining and restoring vision is important to be able to address social determinants eg. education and employment > > Achieving equity in eye health status may help close the overall health and social gaps 8
11 Nine False Reasons for Not Addressing Blindness Vision loss is not important in Indigenous communities: > > Vision loss is the equal third leading cause of the Gap in health after heart disease and Diabetes but ahead of trauma, stroke and alcoholism. Indigenous adults have six times more blindness than mainstream and vision loss represents 11% of the overall health gap. Blindness does not kill people we need to address the life threatening things: > > Even mild vision loss (<6/12) increases the risk of dying 2.6 times in mainstream Australia. Vision loss from Trachoma in African communities increases the risk of dying by 6.8 times. Mild vision loss prevents independent healthy living. Eye care is body part medicine, it is not holistic: > > The patient s journey for eye care starts in properly developed, comprehensive primary health care and requires seamless linkage with specialist services. Lessons learnt from integrating specialist eye care visits will inform ways to improve the linkage of primary and specialist care in other health areas. There are many other more pressing priorities than eye care: > > It is true that there are many health priority areas but 94% of vision loss is unnecessary and much of it can be rapidly reversed. A pair of glasses or Cataract surgery can eliminate vision loss overnight, whereas other chronic diseases (Diabetes, heart disease, alcoholism) cannot be reversed overnight. It is not worth spending the money on eye care, it is too expensive: > > Eye care is extraordinarily cost effective, for example Cataract surgery costs $3,000 per QALY and Diabetic Retinopathy examinations $15,000 per QALY. In Australia, each $1 spent on eye care yields a $5 return. We are already spending too much on Aboriginal health and the money is wasted: > > It is true we now spend $1.39 on Indigenous health for each $1 spent on mainstream. (A decade ago it was $0.80 for Indigenous health). As there is three times the morbidity (and vision loss), one would expect to spend at least three times as much even if delivery costs to remote areas were not higher than urban areas. In terms of Cataract surgery, seven times less surgery is done for Indigenous people. There are not enough specialists to provide the care required: > > The actual increase in the number of optometric and ophthalmic services required is quite small and with the appropriate co-ordination and resources, many specialists are willing to take on this work. This plan or Roadmap is too complex, it is not all necessary: > > Over the last 30 or so years multiple proposals have been made to address Indigenous eye health. None have worked properly as they overlooked different criteria. This Roadmap has been based on a careful review, new evidence and wide consultations. Each element is interlocked forming an integral chain. It will also provide a template for the delivery of other specialist services to primary care services. There is no more money to spend on Indigenous health: > > With a relatively small increase in expenditure, there will be a huge increase in efficiency and reduction in waste for Indigenous eye health services. A doubling in funding will increase glasses use by 2.5 times, Diabetes eye exams by 5 times and Cataract surgery by 7 times. 9
12 Roadmap Recommendations 1. PRIMARY EYE CARE AS PART OF COMPREHENSIVE PRIMARY HEALTH CARE to improve identification and referral for eye care needs from primary health care INTENTION RECOMMENDATION OUTCOME 1.1 Enhancing eye health capacity in primary health services To ensure primary care staff (first point of contact) understand and include the appropriate basic eye checks and referral in routine screening/evaluation. That further education programs be developed and implemented to improve understanding of basic eye health among primary health care professionals and Aboriginal Health Services. Basic eye health is routinely incorporated as part of comprehensive primary care and patients with eye conditions are appropriately referred. 1.2 Health assessment items include eye health To ensure that vision and eye health is regularly assessed as part of primary screening and general health assessments. 1.3 Diabetic Retinopathy detection To improve the examination, early detection and referral of Diabetic Retinopathy by providing sustainable funding for retinal photography. That primary health care staff know and perform the vision and eye care components that are included in the health assessment forms with appropriate referral as needed. That a Medicare item be added to MBS to cover the service costs of taking and reading retinal photographs including the use of telemedicine. Poor vision and eye problems are detected early and referred for further assessment. Retinal screening is carried out routinely at primary health care level and Aboriginal Health Services have the capacity and are resourced to offer this service. 1.4 Eye health inclusion in clinical software To ensure that primary health care staff are prompted to perform the appropriate eye health assessments as part of routine comprehensive health care. That all clinical software packages used in Aboriginal Health Services include eye health checking components and modules consistent with national guidelines. Eye health components are integrated into primary health routine patient management systems. 2. INDIGENOUS ACCESS TO EYE HEALTH SERVICES to enhance access to Aboriginal and mainstream eye services INTENTION RECOMMENDATION OUTCOME 2.1 Aboriginal Health Services and eye health To strengthen the provision of eye health services within Aboriginal Health Services and increase their capacity to identify and refer people needing eye care. That where possible visiting eye health services, including VOS and MSOAP, are provided within Aboriginal Health Services. Increased utilisation of eye health services because they are provided in the culturally safe setting of Aboriginal Health Services. 2.2 Cultural safety in mainstream services To ensure that all components of the clinical pathway are culturally-safe including in public hospitals and private eye care, and that all staff appreciate Indigenous health needs and are able to facilitate the Indigenous patient s journey. That service providers involved in the co-ordination of eye care including Local Hospital Networks and Primary Health Networks, consult with local Aboriginal and Torres Strait Islander communities and improve the cultural awareness of their staff and services. All components of clinical pathway including public hospitals and private services maintain environments that give confidence for Indigenous people to safely access services. 2.3 Low cost spectacles To ensure cost certainty and to provide acceptable and affordable spectacles in a timely way. That nationally consistent Indigenous subsidised spectacle schemes be establish to provide low-cost, quality-assured, costcertain spectacles to Aboriginal and Torres Strait Islander people. People acquire and use the glasses they need because of cost certainty and acceptability leading to increased utilisation of eye services because Indigenous people are confident in obtaining useful glasses. 2.4 Hospital surgery prioritisation 10 To address the inequitable Cataract backlog due to inadequate surgical output and to ensure that hospital surgery waiting times are no longer a barrier to Indigenous eye care, and thus facilitate the uptake and flow through the referral pathway. That all jurisdictions aim to reduce the waiting time for Cataract surgery recognising Indigeneity and the high level of co-morbidities and improve consistency in clinical assessment categories across jurisdictions. The gap for un-operated Indigenous Cataract surgery is eliminated and the surgical pathway is opened because of increased community confidence in services.
13 3. CO-ORDINATION AND CASE MANAGEMENT to improve co-ordination of eye care services and the successful navigation of referral pathways INTENTION RECOMMENDATION OUTCOME 3.1 Local eye care co-ordination To establish local eye care co-ordination that includes a regional hospital with eye surgical facilities. At a local level there is capacity to provide comprehensive eye care for primary identification and referral for optometry and ophthalmology. That mechanisms for local co-ordination of eye care will be established within Local Hospital Networks and Primary Health Networks. All components of the eye care pathway are co-ordinated in each local region to ensure adequate access and use of comprehensive eye care including surgery. 3.2 Clear pathways of care To ensure that patients receive appropriate clinical care with minimal delays and without unnecessary visits by having well documented, understandable and well linked referral pathways. That local co-ordination of eye care is developed along with local referral pathways for all eye care services and these pathways are made known to all service providers involved. Patients experience a smooth passage throughout and fulfill the referrals required for eye health. 3.3 Workforce identification and roles To ensure that within each local area, all the necessary co-ordinating functions in the pathway of care are performed. That each local area identifies the (existing or additional) personnel and positions required for the proper co-ordination, organisation and delivery of the patient's journey along the pathway of eye care. The patient journey proceeds uninterrupted because the appropriate and culturally sensitive personnel are in place. 3.4 Eye care support workforce To ensure that within each local area, the workforce is appropriately skilled and resourced to meet the eye care needs of their community. That sufficient people in each local area are appropriately designated, trained and funded to organise and co-ordinate patients along the pathway of care. People understand and perform the coordination required to facilitate the patient s journey. 3.5 Case management To ensure that those with high need for eye care (such as Diabetes) receive the necessary eye examinations and that those who are referred for surgery receive that surgery. 3.6 Partnership and agreements To ensure that the pathway of care is readily navigated and leakage is reduced because all components of the local eye health system work together, communicate, share information and have common understandings and expectations. That a case management strategy be established within Aboriginal Health Services for all patients at high need for eye care and/or those referred for eye surgery. For patients who have Diabetes, case co-ordination should be provided by chronic disease co-ordinators. That local co-ordination of eye care builds on partnerships and agreements with local service providers and visiting eye services. All patients with Diabetes receive an annual eye examination and follow up and all patients referred for surgery receive it. Based on clear expectations and understandings, local eye care networks work efficiently and effectively. 11
14 4. EYE HEALTH WORKFORCE to increase availability and improve distribution of eye health workforce INTENTION RECOMMENDATION OUTCOME 4.1 Provide eye health workforce to meet population needs To ensure that the eye health workforce is sufficient to meet the population based needs of Indigenous Australians. That population-based needs analysis is used to determine eye health workforce requirements in all areas of Australia. Appropriate numbers of eye health providers are available in all areas of Australia. 4.2 Improve contracting and management of visiting services To increase the ease of use of funding for visiting services (MSOAP and VOS), so as to attract more visiting eye team services where needed and to improve coordination amongst all service providers. That the contracting of VOS and MSOAP be restructured to provide simple, flexible, coordinated and transparent operation and management of these services. MSOAP and VOS work smoothly and efficiently and that visiting optometry and ophthalmology services are properly coordinated. 4.3 Appropriate resources for eye care in rural and remote areas To ensure that the appropriate eye health workforce is available in rural and remote areas. That the eye health workforce and funding are allocated according to population needs with consideration of existing local services. Services in rural and remote areas are adequate to meet the needs for eye care. 4.4 Increase utilisation of services in urban areas To increase the accessibility and use of existing optometry services in urban and regional areas by making them available within the culturally appropriate environment of Aboriginal Health Services. That Indigenous VOS funding is available for major cities and inner regional areas to support delivery of visiting optometry services in Aboriginal Health Services. Increased use of optometry services provided within Aboriginal Health Services. 4.5 Billing for visiting MSOAP supported services To ensure cost certainty and remove barriers to local service uptake created by inconsistent and uncertain billing arrangements and the charging of additional fees. That visiting ophthalmologists supported by MSOAP agree to bulk-bill Indigenous patients for clinic services and that MSOAP consider loading arrangements to meet the true cost of service. Increased use of eye health services because of reduced or removed uncertainty of patient out-of-pocket expenses. 4.6 Rural education and training of eye health workforce To encourage newly trained optometrists and ophthalmologists to participate in Indigenous eye care delivery and regard it as a standard part of their ongoing practice and social responsibility. That during training, eye health providers complete a core component of rural and Indigenous eye health work. Funding should be specifically provided to cover supervision and trainee costs. More optometrists and ophthalmologists have exposure to and actively seek work in rural and remote areas and Indigenous communities. 5. ELIMINATION OF TRACHOMA to eliminate blinding Trachoma from Australia INTENTION RECOMMENDATION OUTCOME 5.1 Definition of areas of risk To ensure that Trachoma activities are conducted in all endemic areas. That the mapping of the extent of Trachoma is completed expeditiously. Areas with Trachoma are clearly defined. 5.2 Effective interventions To ensure that appropriate Trachoma interventions are properly delivered in endemic areas. That the SAFE strategy is fully and comprehensively implemented. Active Trachoma is rapidly eliminated from the endemic areas. 5.3 Surveillance and evaluation To ensure programs are effective and have the anticipated impact. That the ongoing monitoring and evaluation activities of the National Trachoma Reporting and Surveillance Unit should be continued. Success and progress are measured and reported. 5.4 Certification of elimination 12 To ensure the World Health Organization certifies the elimination of Trachoma in Australia. That Australia works closely with World Health Organization and participates in the GET 2020 process until Trachoma is eliminated. Australia is free of blinding Trachoma.
15 6. MONITORING AND EVALUATION to capture and report information about progress and improvement of services and outcomes in Indigenous eye health INTENTION RECOMMENDATION OUTCOME 6.1 Managing local eye service performance To provide the appropriate service delivery data to inform local management, and allow aggregation of these data at regional, State/Territory and national levels. 6.2 State and National performance To provide State/Territory and national assessment of performance to assist local programs and provide accountability. 6.3 Collating existing eye data sources To avoid unnecessary duplication, existing eye care data sources are identified and utilised. 6.4 National benchmarks To ensure that national benchmarks are developed for the program to guide and support service delivery and create nationally consistent goals and approaches for eye care. That local co-ordination of eye care includes Local Hospital Networks and Primary Health Networks and collects and reports nationally consistent data on eye health programs, service delivery targets and patient outcomes. That local service delivery data be aggregated to provide State/Territory performance information and that this information is aggregated to provide national information. That sources of currently available eye health information are identified and drawn into a national eye health reporting framework. That an appropriate expert committee be established to develop clear, evidence based, eye health sector agreed minimum standards and targets to support eye care service delivery for Aboriginal and Torres Strait Islander people. Local services are improved by monitoring performance and progress is reported nationally and locally. Service delivery performance data are appropriately used and provide timely analysis and reporting at higher levels and locally. Data and eye health information from national sources are well managed, accessible and applied for eye health service improvements. Implementation of eye health programs is nationally consistent and supported by a robust evidence base that supports identification of good practice and continuous improvement. 6.5 Quality assurance To ensure that services provide high quality eye care and that program management follows best practice. That measures of service quality and outcomes are developed and applied to Indigenous eye health. Service quality and satisfaction for eye health outcomes are consistent nationally and all services attain high quality ratings. 6.6 Primary health service self-audit in eye health To ensure Aboriginal Health Services can easily assess their ability to provide quality eye care and conform to national benchmarks in eye care. That an audit tool for Aboriginal Health Services be developed to support delivery of appropriate eye health services. All Aboriginal Health Services provide well integrated eye care. 6.7 Program evaluation To identify progress and outcome successes and share with the broader health system. That the Close the Gap for Vision initiative is evaluated against program objectives, timelines and measures. The Gap for Vision is closed by
16 7. GOVERNANCE to ensure that there is national delivery of Close the Gap for Vision INTENTION RECOMMENDATION OUTCOME 7.1 Community engagement To ensure eye care services are acceptable and have the full support of the local Aboriginal community. That eye services are developed and delivered with the engagement of the local community. Indigenous communities use and champion their eye care services. 7.2 Local Hospital Networks and Primary Health Networks To ensure regional Indigenous eye care co-ordination is provided for within Local Hospital Networks and Primary Health Networks. 7.3 State/Territory management To provide high level advisory and management committees to review the workings and achievements of local eye networks and to ensure that there is State/ Territory government liaison. In particular to be able to identify areas where services are insufficient or not operating appropriately to meet community needs. 7.4 National oversight To provide continuity, oversight and accountability through monitoring national progress and assessing national priorities. 7.5 Program interdependence To ensure effective improvement in eye care, all the elements of this Roadmap need to be implemented in a clear, branded and unified approach by government, the sector and the community. That local co-ordination of eye care is part of the responsibility of Local Hospital Networks and Primary Health Networks. That State/Territory Indigenous eye health managers are appointed and State/ Territory Indigenous eye health committees are established to provide oversight and support for the Indigenous eye health system. That a National Oversight Body for Aboriginal and Torres Strait Islander eye health is established by government to oversee the implementation of strategies, develop national policy and funding for Indigenous eye health. Reporting to Commonwealth and State/Territory governments. That the recommendations be regarded as a comprehensive package to be known collectively as the Close the Gap for Vision initiative. Clearly articulated objectives, timelines and measures will need to be developed. Eye health is well co-ordinated with other health services at a regional level. Eye services within a State/Territory are performing at a high standard and achieving their objectives. National coverage, oversight and accountability is maintained with timely reports to government and to all service providers and stakeholders. Close the Gap for Vision recommendations be adopted and implemented across Australia and unnecessary vision loss is eliminated. 8. HEALTH PROMOTION AND AWARENESS to improve awareness and knowledge of eye health in communities to support self-empowerment INTENTION RECOMMENDATION OUTCOME 8.1 Eye health promotion To ensure that all community members and health service staff are aware of the importance of eye health. That an eye health promotion strategy aligned with Close the Gap for Vision be developed within each State/Territory to improve community awareness of eye health. Community members recognise their own need for eye care. 8.2 Social marketing eye care services To ensure that all community members and health service staff are aware of the availability of eye health services (including dates of visiting services) and know how to access them. That strategies for marketing of local eye services including visiting services is established at the level of Local Hospital Networks, Primary Health Networks and Aboriginal Community Controlled Health Organisations. Community members know about and are able to use eye services when they need them. 14
17 9. HEALTH FINANCING to ensure adequate funding is allocated to Close the Gap for Vision INTENTION RECOMMENDATION OUTCOME 9.1 Current spending on Indigenous eye health (non Trachoma) To estimate the current annual amount spent on Indigenous eye health (non Trachoma). 9.2 Current spending on Trachoma To estimate the current annual amount spent on Trachoma. That the current annual total expenditure on Indigenous eye health (non Trachoma) is estimated to be $17.40 million and this is not adequate. That the current annual total expenditure on Trachoma elimination is estimated to be $4.5 million and this should be continued. Currently there is six times more blindness in Indigenous adults than in mainstream and the current resources are not sufficient to provide adequate eye care. Funding is continued until Trachoma is eliminated. Additional resources needed for health promotion. 9.3 Full additional annual capped funding required* Estimate the additional capped funding required each year in service delivery for indigenous eye health to Close the Gap for Vision That an estimated additional annual capped funding of $19.5 million is provided per year for Indigenous eye health. For every one dollar spent for eye care in Australia, there is a five dollar return to the community. Indigenous Cataract surgery will be increased 7 times, Diabetic eye care increased 5 times and care of refractive error increased 2.5 times to reduce Indigenous blindness by 6 times. 9.4 Cost to 'Close the Gap for Vision' funded for 5 years* To estimate the additional five year forward amounts required for Indigenous eye health to Close the Gap for Vision. That an estimated additional capped funding of $68.25 million is provided over five years for Indigenous eye health. This funding will Close the Gap for Vision. Additional capped funding required to 'Close the Gap for Vision' (2011 dollars in millions)* Annual Cost Commonwealth 2.92 includes VOS, RHOF States/Territories includes State/Territory subsidised spectacle schemes, transport 2.01 Co-ordination includes Commonwealth and State/ Territory Aboriginal Health Workers and other co-ordinator salaries Governance and evaluation includes State/Territory and National committees and managers 1.25 Total Information presented in this table is derived from 'The Cost of Closing the Gap for Vision', University of Melbourne 2011 *estimates do not include new or additional infrastructure costs 15
18 Activities for the Commonwealth The Roadmap to Close the Gap for Vision requires full funding and implementation, but giving priority to the following activities the Commonwealth can progress specific Roadmap recommendations within existing programs. 1. National oversight and accountability > National function to monitor and review national data on an annual basis and report to all relevant federal and jurisdictional Ministers > National oversight for Aboriginal and Torres Strait Islander eye health to provide expert, technical and policy advice and recommendations to federal and jurisdictional governments > State/territory stakeholder group for jurisdictional overview 2. National leadership > National leadership > Establish benchmarks and nationally consistent reporting > Establish clinical pathways and standards of care > Support jurisdictional activity 3. Primary Health Networks > Work closely with ACCHOs > Assessment of local eye care needs and gap analysis > Service directory and referral protocols > Assessment of additional VOS and RHOF needs > Coordination and case management needs determined and supported > CTG/ICD chronic disease coordinators 4. Improve RHOF and VOS planning and coordination > Support and direct jurisdictional fund holders > Coordination between programs > Linkages with ACCHOs > Population based planning > RHOF and VOS bulk billed > Urban VOS > Report number of Indigenous services provided 5. Trachoma > Continuation of support and enhance health promotion > Fully engage Education and Housing Departments 6. Cataract surgery > Ensure equitable Indigenous waiting times and outcomes 7. Diabetes retinal examinations > Medicare item number for non-mydriatic retinal photography 8. Low cost spectacles > Nationally consistent provision, best practice and adequate 16
19 Regional Implementation By giving priority to the following activities, regions and jurisdictions can progress the implementation of the Roadmap recommendations. Define region and population and identify regional surgical hub > Use locally appropriate boundaries to define region > Use 2011 Census data for initial needs estimates and provide a starting point for planning this can be revised as new data becomes available > The prevalence data from the National Indigenous Eye Health Survey can be used to provide first order estimates of expected disease burden and local population-based needs > In consultation with the state/territory forum identify hospitals in the regions where public Cataract surgery is to be performed. 1. Establish regional collaborative network Include the regional Closing the Gap committee and other bodies in each region. Representatives should include Aboriginal Medical Services, Primary Health Network, Local Hospital District/Network, regional health authority/department, local eye care practitioners and local health services. State/ territory forum to provide state-level support. 2 Gap and needs analysis for service requirements Map current eye care provision (including visiting services) and compare to population-based needs estimate to determine service and other gaps. Look to VOS and RHOF support if additional services required. 3 Develop regional service directory and referral protocols Determine the current services and capacity of locally available services within each region, then develop regional referral protocols through the regional collaborative network. 4 Identify systems coordination and patient case management staff roles The identification of staff and allocation of roles and responsibilities needs to occur at the clinic, hospital and regional level with regional coordination and oversight. 5 Local planning and action through regional collaborative network Collaborative network meets regularly, shares and reviews data, and establishes and reviews plan. 6 Establish regional data collection and monitoring system Develop regional reporting and performance review systems using national performance indicators. 7 Ensure regional accountability and oversight Regional data report and reviewed every six months within and reported to state/territory forum. Indicators To be included in National Health Performance and Regional Reports Service utilisation 1 MBS 715 check (which includes an assessment of vision) 2 Cataract surgery rate 3 Cataract surgery rate within 90 days of booking 4 Retinal examination for people with Diabetes 5 Laser treatment and intravitreal injection rate for people with Diabetic retinopathy Service provision 6 Visiting optometry days (VOS) 7 Visiting ophthalmology days (RHOF) Jurisdictional performance 8 Subsidised spectacles 9 Trachoma prevalence rate national and jurisdictional 10 Trachoma treatment coverage with Azithromycin national and jurisdictional 17
20 Trachoma > > Trachoma is a major blinding infectious eye disease > > It occurs in areas with poor hygiene and living conditions > > Australia is the only developed country to still have Trachoma > > Blinding endemic Trachoma occurs in 60% of outback communities > > Late scarring and in-turned eyelashes (trichiasis) affects 1.4% of older Indigenous people across the country > > Trachoma is still the fourth leading cause of blindness The National Trachoma Surveillance and Reporting Unit (NTSRU) has collected data since 2006 NTSRU has defined the problem and the progress Data collection is still far from complete Trachoma can be prevented with WHO's SAFE Strategy: Surgery for trichiasis Antibiotic (Azithromycin) treatment Facial cleanliness and Environmental improvements WHO and all Governments including Australia have committed to the Global Elimination of Trachoma by 2020 (GET 2020). Trachoma Prevalence in Indigenous Children The SAFE Strategy is not fully implemented Trachoma screening is often incomplete Trichiasis screening is often forgotten Treatment is often not given or with poor coverage Clean faces campaign and health promotion is incomplete 'Every child with a dirty face is a health hazard' Trachoma prevalence in children aged 5-9 years and number of communities screened/ number of at risk communities in 2014 From 2014 Report of NTSRU Regional education and health promotion material 18
21 In 2009 the Australian Government committed to eliminate Trachoma in Australia Current Activities: > > $16 m ( ) was committed to start the elimination of Trachoma > > A further $16.5 m ( ) was committed to continue > > Implementation could have been faster, but once started great progress has been made, especially in the Northern Territory and Western Australia > > More communities have been screened > > More children have been examined > > Treatment coverage has improved > > Health education materials have been more widely used > > Clean faces, strong eyes campaign is underway > > AND Trachoma rates are starting to fall Milpa The Trachoma Goanna Trachoma rates of 14% in 2009 are now 4% in 2014 When the SAFE Strategy is properly implemented Trachoma rates show marked declines Community prevalence of active Trachoma in one region in the Northern Territory (de-identified data; each coloured line represents a separate community) What is needed now: > Funds to finish the job and eliminate Trachoma > Additional funds are needed for health promotion focusing on clean faces and safe bathrooms > Full engagement with Education and Housing Departments 19
22 Eye Health and Roadmap Resources A number of resources have been developed by IEH to assist with regional implementation and initiatives to close the gap for vision. These are listed below and available online at Regional Implementation Toolkit Regional implementation how to guide Eye care services calculator Regional implementation checklist Regional equipment checklist Regional hospital checklist Service directory template Referral pathway template Regional indicator tracking tool Roadmap resources and position papers National oversight National leadership Role for jurisdictions Mandatory MBS 715 eye checks Cataract monitoring Clinical practice software Indicators Revised costing of the Roadmap Developing linkages Health promotion resources Trachoma health promotion Diabetes eye health promotion Educational resources Diabetic retinopathy grading RAHC trachoma module RAHC eye care module RAHC eye health and diabetes module Trachoma grading and self directed learning Engaging with eye care service providers Fund holders and outreach funding Education and trachoma Diabetic retinopathy screening card Software roundtable report 2013 Regional implementation roundtable report 2014 Health promotion roundtable report 2014 Diabetic retinopathy health promotion workshop report 2015 Medicare Local Collaborative Framework 2013 VACKH Aboriginal Eye Health Strategy VACKH Aboriginal Eye health Strategy Regional Implementation Information Sheet Roadmap glossary The 2015 Annual Update on the Implementation of the Roadmap to Close the Gap for Vision was launched in November Annual Updates provide the most recent report of progress against the 42 recommendations of the Roadmap. These are available on-line at 20
July The Roadmap to Close the Gap for Vision
 July 2012 The Roadmap to Close the Gap for Vision This summary report was prepared by Professor Hugh R Taylor AC, Andrea Boudville*, Mitchell Anjou* and Robyn McNeil* of the Indigenous Eye Health Unit,
July 2012 The Roadmap to Close the Gap for Vision This summary report was prepared by Professor Hugh R Taylor AC, Andrea Boudville*, Mitchell Anjou* and Robyn McNeil* of the Indigenous Eye Health Unit,
We are nearly there. Close the Gap for Vision
 We are nearly there Close the Gap for Vision Executive summary Australia is on the verge of closing the gap in Indigenous eye health Elimination of trachoma Sight restoration for ~4,000 Indigenous Australians
We are nearly there Close the Gap for Vision Executive summary Australia is on the verge of closing the gap in Indigenous eye health Elimination of trachoma Sight restoration for ~4,000 Indigenous Australians
The Cost to Close the Gap for Vision
 The to Close the Gap for Vision This report was prepared by Dr Ya-Seng (Arthur) Hsueh*, Mr Alex Brando*, Professor David Dunt, Mr Mitchell Anjou* and Professor Hugh Taylor of the Centre for Health Policy,
The to Close the Gap for Vision This report was prepared by Dr Ya-Seng (Arthur) Hsueh*, Mr Alex Brando*, Professor David Dunt, Mr Mitchell Anjou* and Professor Hugh Taylor of the Centre for Health Policy,
Indigenous Eye Health Indicators
 Indigenous Eye Health Indicators This position paper frames pertinent Indigenous eye health indicators at the regional, jurisdictional, and national levels as recommended in the Roadmap to Close the Gap
Indigenous Eye Health Indicators This position paper frames pertinent Indigenous eye health indicators at the regional, jurisdictional, and national levels as recommended in the Roadmap to Close the Gap
Closing the Gap: Advancing Indigenous Eye Health Across Diverse Regions and Systems
 Closing the Gap: Advancing Indigenous Eye Health Across Diverse Regions and Systems Jatkar U, Anjou M, Schubert N, Roberts P, Taylor HR Uma Jatkar, Indigenous Eye Health National Rural Health Alliance
Closing the Gap: Advancing Indigenous Eye Health Across Diverse Regions and Systems Jatkar U, Anjou M, Schubert N, Roberts P, Taylor HR Uma Jatkar, Indigenous Eye Health National Rural Health Alliance
Evaluation of the Victorian Aboriginal Spectacles Subsidy Scheme
 Evaluation of the Victorian Aboriginal Spectacles Subsidy Scheme A Summary Report 2016 We acknowledge Barry Atkinson, Yorta Yorta artist, for the artwork Up Stream Down Stream that is featured in this
Evaluation of the Victorian Aboriginal Spectacles Subsidy Scheme A Summary Report 2016 We acknowledge Barry Atkinson, Yorta Yorta artist, for the artwork Up Stream Down Stream that is featured in this
Progressing Aboriginal and Torres Strait Islander eye health and vision care. Policy and funding proposal
 Progressing Aboriginal and Torres Strait Islander eye health and vision care Policy and funding proposal March 2013 Contents 1 Executive Summary 1 1.1 Purpose 1 1.2 Key recommendations 2 1.3 Vision 2020
Progressing Aboriginal and Torres Strait Islander eye health and vision care Policy and funding proposal March 2013 Contents 1 Executive Summary 1 1.1 Purpose 1 1.2 Key recommendations 2 1.3 Vision 2020
Insight of adult health checks an approach to Aboriginal and Torres Strait Islander eye examinations. Prof Hugh Taylor and Mr Mitchell Anjou
 Insight of adult health checks an approach to Aboriginal and Torres Strait Islander eye examinations Prof Hugh Taylor and Mr Mitchell Anjou Insight of adult health checks An approach to Aboriginal and
Insight of adult health checks an approach to Aboriginal and Torres Strait Islander eye examinations Prof Hugh Taylor and Mr Mitchell Anjou Insight of adult health checks An approach to Aboriginal and
Enhancing eye health capacity in primary health care: closing the gap for vision
 Rural Health West Aboriginal Health Conference Perth 1 July 2017 Enhancing eye health capacity in primary health care: closing the gap for vision Anjou MD, Jatkar U, Gilden R, Schubert NS, Roberts PI,
Rural Health West Aboriginal Health Conference Perth 1 July 2017 Enhancing eye health capacity in primary health care: closing the gap for vision Anjou MD, Jatkar U, Gilden R, Schubert NS, Roberts PI,
Building an eye care program with Aboriginal communities in Victoria a partnership approach
 Building an eye care program with Aboriginal communities in Victoria a partnership approach Genevieve Napper 1 and Cheryl Vickery 1 Kulan Barney 2, Jimi Peters 2, Mitchell Anjou 3, Tim Fricke 1,4, Jonathan
Building an eye care program with Aboriginal communities in Victoria a partnership approach Genevieve Napper 1 and Cheryl Vickery 1 Kulan Barney 2, Jimi Peters 2, Mitchell Anjou 3, Tim Fricke 1,4, Jonathan
Stronger eye care systems in Aboriginal primary health care
 Stronger eye care systems in Aboriginal primary health care Anna Morse 1,2, Colina Waddell 1,2, Jenny Hunt 3, Fiona MacFarlane 4, Daniel Jackman 5, Christine Corby 6, Tricia Keys 1,2 1 Brien Holden Vision
Stronger eye care systems in Aboriginal primary health care Anna Morse 1,2, Colina Waddell 1,2, Jenny Hunt 3, Fiona MacFarlane 4, Daniel Jackman 5, Christine Corby 6, Tricia Keys 1,2 1 Brien Holden Vision
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Hunter New England & Central Coast Please note: This Activity Work Plan was developed in response to the HNECC PHN
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Hunter New England & Central Coast Please note: This Activity Work Plan was developed in response to the HNECC PHN
Eye Care in Action: Optometry in Aboriginal health services
 Eye Care in Action: Optometry in Aboriginal health services Anna Morse & Luke Arkapaw Public Health Division Brien Holden Vision Institute A multidisciplinary collaborative global research, development,
Eye Care in Action: Optometry in Aboriginal health services Anna Morse & Luke Arkapaw Public Health Division Brien Holden Vision Institute A multidisciplinary collaborative global research, development,
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Murray PHN When submitting this Activity Work Plan 2016-2018 to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Murray PHN When submitting this Activity Work Plan 2016-2018 to the Department
Indigenous Eye Health So3ware Supports
 Indigenous Eye Health So3ware Supports Andrea Boudville 19 February 2014 Indigenous Eye Health Unit Melbourne School of PopulaFon and Global Health MSIA Webinar Indigenous Eye Health Unit Established in
Indigenous Eye Health So3ware Supports Andrea Boudville 19 February 2014 Indigenous Eye Health Unit Melbourne School of PopulaFon and Global Health MSIA Webinar Indigenous Eye Health Unit Established in
The NGO has worked with the AMS and REHC to achieve the following:
 Providing eye care to remote Indigenous communities in the Northern Territory: a case study examining success factors and challenges from a collaborative approach between a NGO and AMS Tricia Keys 1, Maree
Providing eye care to remote Indigenous communities in the Northern Territory: a case study examining success factors and challenges from a collaborative approach between a NGO and AMS Tricia Keys 1, Maree
Specialist Eye Health Guidelines
 Specialist Eye Health Guidelines for use in Aboriginal and Torres Strait Islander Populations Cataract Diabetic Retinopathy Trachoma Commonwealth of Australia 2001 This work is copyright. It may be reproduced
Specialist Eye Health Guidelines for use in Aboriginal and Torres Strait Islander Populations Cataract Diabetic Retinopathy Trachoma Commonwealth of Australia 2001 This work is copyright. It may be reproduced
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Murray PHN When submitting this Activity Work Plan 2016-2018 to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Murray PHN When submitting this Activity Work Plan 2016-2018 to the Department
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Gippsland When submitting this Activity Work Plan 2016-2018 to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Gippsland When submitting this Activity Work Plan 2016-2018 to the Department
DRUG AND ALCOHOL TREATMENT ACTIVITY WORK PLAN
 DRUG AND ALCOHOL TREATMENT ACTIVITY WORK PLAN 2016-2019 1 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-2019 Primary Health Tasmania t: 1300 653 169 e: info@primaryhealthtas.com.au
DRUG AND ALCOHOL TREATMENT ACTIVITY WORK PLAN 2016-2019 1 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-2019 Primary Health Tasmania t: 1300 653 169 e: info@primaryhealthtas.com.au
Primary Health Networks
 Primary Health Networks Activity Work Plan 2016-17 to 2018-19 Budget Central and Eastern Sydney PHN When submitting this Activity Work Plan 2016-2018 to the Department of Health, the PHN must ensure that
Primary Health Networks Activity Work Plan 2016-17 to 2018-19 Budget Central and Eastern Sydney PHN When submitting this Activity Work Plan 2016-2018 to the Department of Health, the PHN must ensure that
A Framework for Optimal Cancer Care Pathways in Practice
 A to Guide Care Cancer Care A for Care in Practice SUPPORTING CONTINUOUS IMPROVEMENT IN CANCER CARE Developed by the National Cancer Expert Reference Group to support the early adoption of the A to Guide
A to Guide Care Cancer Care A for Care in Practice SUPPORTING CONTINUOUS IMPROVEMENT IN CANCER CARE Developed by the National Cancer Expert Reference Group to support the early adoption of the A to Guide
Updated Activity Work Plan : Drug and Alcohol Treatment
 Web Version HPRM DOC/17/1043 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment This Drug and Alcohol Treatment Activity Work Plan template has the following parts: 1. The updated strategic
Web Version HPRM DOC/17/1043 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment This Drug and Alcohol Treatment Activity Work Plan template has the following parts: 1. The updated strategic
Primary Health Networks Drug and Alcohol Treatment Services Funding. Updated Activity Work Plan : Drug and Alcohol Treatment
 Primary Health Networks Drug and Alcohol Treatment Services Funding Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment Adelaide PHN This Activity Work Plan is an update to the 2016-18 Activity
Primary Health Networks Drug and Alcohol Treatment Services Funding Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment Adelaide PHN This Activity Work Plan is an update to the 2016-18 Activity
Executive Summary 10
 Executive Summary 10 In this section 12 Introduction 13 Radiation Oncology Services in Australia Key Issues 15 2012-2022 Strategic Directions and Objectives for the Radiation Oncology Sector 17 Policy
Executive Summary 10 In this section 12 Introduction 13 Radiation Oncology Services in Australia Key Issues 15 2012-2022 Strategic Directions and Objectives for the Radiation Oncology Sector 17 Policy
Vision and eye healthcare study in residential aged care facilities
 Vision and eye healthcare study in residential aged care facilities Study report Report prepared by: Rob Cummins, Director, Research & Policy Julie Heraghty, Former Chief Executive Officer Macular Disease
Vision and eye healthcare study in residential aged care facilities Study report Report prepared by: Rob Cummins, Director, Research & Policy Julie Heraghty, Former Chief Executive Officer Macular Disease
Changes to Australian Government Hearing Services Program and Voucher scheme
 Changes to Australian Government Hearing Services Program and Voucher scheme The Commonwealth Department of Health has published a report on its investigation into the future of the Hearing Services Program,
Changes to Australian Government Hearing Services Program and Voucher scheme The Commonwealth Department of Health has published a report on its investigation into the future of the Hearing Services Program,
Non mydriatic retinal photography
 Non mydriatic retinal photography A roundtable in preparation for new MBS items for people with diabetes Report Indigenous Eye Health Melbourne School of Population and Global Health 25 July 2016 TABLE
Non mydriatic retinal photography A roundtable in preparation for new MBS items for people with diabetes Report Indigenous Eye Health Melbourne School of Population and Global Health 25 July 2016 TABLE
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 South Eastern Melbourne PHN When submitting this Activity Work Plan 2016-2018 to the Department of Health, the PHN
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 South Eastern Melbourne PHN When submitting this Activity Work Plan 2016-2018 to the Department of Health, the PHN
Palliative Care. Working towards the future of quality palliative care for all
 Palliative Care Working towards the future of quality palliative care for all FEBRUARY 2019 Recommended citation Palliative Care Australia 2018, Palliative Care 2030 working towards the future of quality
Palliative Care Working towards the future of quality palliative care for all FEBRUARY 2019 Recommended citation Palliative Care Australia 2018, Palliative Care 2030 working towards the future of quality
The Future of Optometric Services in Primary Care in Wales
 IMPROVING HEALTH IN WALES The Future of Optometric Services in Primary Care in Wales a consultation document ISBN 0 7504 2968 2 Designed by CartoGraphic Services G/254/02-03 September 2002 INA - 15-02
IMPROVING HEALTH IN WALES The Future of Optometric Services in Primary Care in Wales a consultation document ISBN 0 7504 2968 2 Designed by CartoGraphic Services G/254/02-03 September 2002 INA - 15-02
Primary Health Networks Greater Choice for At Home Palliative Care
 Primary Health Networks Greater Choice for At Home Palliative Care Brisbane South PHN When submitting the Greater Choice for At Home Palliative Care Activity Work Plan 2017-2018 to 2019-2020 to the Department
Primary Health Networks Greater Choice for At Home Palliative Care Brisbane South PHN When submitting the Greater Choice for At Home Palliative Care Activity Work Plan 2017-2018 to 2019-2020 to the Department
April 2019 NATIONAL POLICY PLATFORM
 April 2019 NATIONAL POLICY PLATFORM There are crisis services available 24/7 if you or someone you know is in distress Lifeline: 13 11 14 www.lifeline.org.au people took their own lives in 2017 1 Over
April 2019 NATIONAL POLICY PLATFORM There are crisis services available 24/7 if you or someone you know is in distress Lifeline: 13 11 14 www.lifeline.org.au people took their own lives in 2017 1 Over
Eye health promotion by optometrists in rural Victoria
 Eye health promotion by optometrists in rural Victoria Lawrence Arnold, Ben Harris, Optometrists Association Victoria The Optometrists Association Victoria has been helping optometrists in rural Victoria
Eye health promotion by optometrists in rural Victoria Lawrence Arnold, Ben Harris, Optometrists Association Victoria The Optometrists Association Victoria has been helping optometrists in rural Victoria
Ministry of Health and Long-Term Care. Palliative Care. Follow-Up on VFM Section 3.08, 2014 Annual Report RECOMMENDATION STATUS OVERVIEW
 Chapter 1 Section 1.08 Ministry of Health and Long-Term Care Palliative Care Follow-Up on VFM Section 3.08, 2014 Annual Report RECOMMENDATION STATUS OVERVIEW # of Status of Actions Recommended Actions
Chapter 1 Section 1.08 Ministry of Health and Long-Term Care Palliative Care Follow-Up on VFM Section 3.08, 2014 Annual Report RECOMMENDATION STATUS OVERVIEW # of Status of Actions Recommended Actions
The first step to Getting Australia s Health on Track
 2017 The first step to Getting Australia s Health on Track Heart Health is the sequential report to the policy roadmap Getting Australia s Health on Track and outlines a national implementation strategy
2017 The first step to Getting Australia s Health on Track Heart Health is the sequential report to the policy roadmap Getting Australia s Health on Track and outlines a national implementation strategy
Growing an optometry workforce for Aboriginal and Torres Strait Islander communities
 Growing an optometry workforce for Aboriginal and Torres Strait Islander communities Genevieve Napper 1, Luke Arkapaw 2, Mitchell Anjou 3, Anna Morse 2, Michelle Pollard 2 1 Australian College of Optometry;
Growing an optometry workforce for Aboriginal and Torres Strait Islander communities Genevieve Napper 1, Luke Arkapaw 2, Mitchell Anjou 3, Anna Morse 2, Michelle Pollard 2 1 Australian College of Optometry;
Updated Activity Work Plan : Drug and Alcohol Treatment. Western NSW PHN
 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment Western NSW PHN 1 Overview This Drug and Alcohol Treatment Activity Work Plan covers the period from 1 July 2016 to 30 June 2019 and is
Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment Western NSW PHN 1 Overview This Drug and Alcohol Treatment Activity Work Plan covers the period from 1 July 2016 to 30 June 2019 and is
Improving Eye Health. Cardiff and Vale University Health Board
 Improving Eye Health Cardiff and Vale University Health Board Local Eye Care Plan 2013-2018 1. Introduction On the 18 th September 2013 the Welsh Government published Together for Health: Eye Health Care,
Improving Eye Health Cardiff and Vale University Health Board Local Eye Care Plan 2013-2018 1. Introduction On the 18 th September 2013 the Welsh Government published Together for Health: Eye Health Care,
Primary Health Networks
 Primary Health Networks REVISED Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 REVISED Drug and Alcohol Treatment Budget NEPEAN BLUE MOUNTAINS PHN When submitting this Activity Work Plan
Primary Health Networks REVISED Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 REVISED Drug and Alcohol Treatment Budget NEPEAN BLUE MOUNTAINS PHN When submitting this Activity Work Plan
The elements of cancer and palliative care reform in Victoria
 The elements of cancer and palliative care reform in Victoria Dr Chris Brook Executive Director Rural and Regional Health and Aged Care Services Department of Human Services 1 Overview Rural and regional
The elements of cancer and palliative care reform in Victoria Dr Chris Brook Executive Director Rural and Regional Health and Aged Care Services Department of Human Services 1 Overview Rural and regional
Support Facilitator Partners in Recovery - Ashfield
 Position Description September 2016 Position description Support Facilitator Partners in Recovery - Ashfield Section A: position details Employment Status Classification and Salary Location: Hours: Contract
Position Description September 2016 Position description Support Facilitator Partners in Recovery - Ashfield Section A: position details Employment Status Classification and Salary Location: Hours: Contract
Joint Standing Committee on the National Disability Insurance Scheme (NDIS) The Provision of Hearing Services under the NDIS
 Joint Standing Committee on the National Disability Insurance Scheme (NDIS) The Provision of Hearing Services under the NDIS Children and Young People with Disability Australia Submission January 2017
Joint Standing Committee on the National Disability Insurance Scheme (NDIS) The Provision of Hearing Services under the NDIS Children and Young People with Disability Australia Submission January 2017
Updated Activity Work Plan : Drug and Alcohol Treatment
 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment COORDINARE - South Eastern NSW PHN When submitting this Activity Work Plan 2016-17 to 2018-19 to the Department of Health, the PHN must
Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment COORDINARE - South Eastern NSW PHN When submitting this Activity Work Plan 2016-17 to 2018-19 to the Department of Health, the PHN must
Updated Activity Work Plan : Drug and Alcohol Treatment
 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment This Drug and Alcohol Treatment Activity Work Plan template has the following parts: 1. The updated strategic vision of each PHN, specific
Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment This Drug and Alcohol Treatment Activity Work Plan template has the following parts: 1. The updated strategic vision of each PHN, specific
POSITION DESCRIPTION:
 POSITION DESCRIPTION: SECTION A: POSITION CONTEXT Position Title Peer Lead Practitioner (consumer) Position Reference 10129 Position Type Classification Service/Department Area/Group/State Part-time 22.50
POSITION DESCRIPTION: SECTION A: POSITION CONTEXT Position Title Peer Lead Practitioner (consumer) Position Reference 10129 Position Type Classification Service/Department Area/Group/State Part-time 22.50
Diabetic Eye Care; Workforce Challenges and opportunities
 Diabetic Eye Care; Workforce Challenges and opportunities Hugh R. Taylor, AC, MD April 2013 Bangkok How many ophthalmologists in practice and training worldwide? Study designed and conducted by ICO in
Diabetic Eye Care; Workforce Challenges and opportunities Hugh R. Taylor, AC, MD April 2013 Bangkok How many ophthalmologists in practice and training worldwide? Study designed and conducted by ICO in
National Palliative Care Strategy 2017 Draft 2.1. Draft AUGUST 2017 DRAFT 2.1 PREPARED FOR DEPARTMENT OF HEALTH
 National Palliative Care Strategy 2017 2.1 AUGUST 2017 DRAFT 2.1 PREPARED FOR DEPARTMENT OF HEALTH To receive this document in an accessible format phone 02 8233 9909, using the National Relay Service
National Palliative Care Strategy 2017 2.1 AUGUST 2017 DRAFT 2.1 PREPARED FOR DEPARTMENT OF HEALTH To receive this document in an accessible format phone 02 8233 9909, using the National Relay Service
Murrumbidgee PHN Activity Work Plan : Primary Health Networks Greater Choice for At Home Palliative Care
 Murrumbidgee PHN Activity Work Plan 2018-2019: Primary Health Networks Greater Choice for At Home Palliative Care 1 1. Planned activities funded under the Activity Primary Health Networks Greater Choice
Murrumbidgee PHN Activity Work Plan 2018-2019: Primary Health Networks Greater Choice for At Home Palliative Care 1 1. Planned activities funded under the Activity Primary Health Networks Greater Choice
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Country WA PHN When submitting this Activity Work Plan 2016-2019 to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Country WA PHN When submitting this Activity Work Plan 2016-2019 to the Department
Our footprints: a traveller s guide to the COAG implementation process in Western Australia
 Our footprints: a traveller s guide to the COAG implementation process in Western Australia Beverley Stone 1, Kevin Cox 1, Rosalie Miles 1, Susan Powe 1, Vicki O Donnell, Linda Waters 1 WA Country Health
Our footprints: a traveller s guide to the COAG implementation process in Western Australia Beverley Stone 1, Kevin Cox 1, Rosalie Miles 1, Susan Powe 1, Vicki O Donnell, Linda Waters 1 WA Country Health
Monitoring and Evaluation Framework for the Tackling Indigenous Smoking Programme
 Monitoring and Evaluation Framework for the Tackling Indigenous Smoking Programme 30 June 2016 Introduction... 3 Context the TIS programme... 4 2.1 TIS programme objectives... 5 2.2 The delivery of the
Monitoring and Evaluation Framework for the Tackling Indigenous Smoking Programme 30 June 2016 Introduction... 3 Context the TIS programme... 4 2.1 TIS programme objectives... 5 2.2 The delivery of the
Senate Submission. Out of pocket costs in Australian hearing health care June 2014
 Senate Submission Out of pocket costs in Australian hearing health care June 2014 PO Box 504, Brentford Square, Vic 3131 (Suite 7, 476 Canterbury Road, Forest Hill, Vic 3131) t: +61 3 9877 2727 f: +61
Senate Submission Out of pocket costs in Australian hearing health care June 2014 PO Box 504, Brentford Square, Vic 3131 (Suite 7, 476 Canterbury Road, Forest Hill, Vic 3131) t: +61 3 9877 2727 f: +61
CSD Level 2 from $57,170 $62,811 pa (Pro Rata) Dependent on skills and experience
 Position Description August 17 Position Description Peer Support Worker Section A: Position details Position title: Employment Status: Classification and Salary: Location: Hours: Peer Support Worker Part-Time
Position Description August 17 Position Description Peer Support Worker Section A: Position details Position title: Employment Status: Classification and Salary: Location: Hours: Peer Support Worker Part-Time
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Adelaide PHN This template was used to submit the Primary Health Network s (PHN s) Activity Work Plans to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Adelaide PHN This template was used to submit the Primary Health Network s (PHN s) Activity Work Plans to the Department
POSITION DESCRIPTION:
 POSITION DESCRIPTION: SECTION A: POSITION CONTEXT Position Title Peer Practitioner - Personalised Support Services Position Reference 10556 Position Type Part time, 22.8 hours per week, fixed term contract
POSITION DESCRIPTION: SECTION A: POSITION CONTEXT Position Title Peer Practitioner - Personalised Support Services Position Reference 10556 Position Type Part time, 22.8 hours per week, fixed term contract
Position Description Ovarian Cancer Australia Support Coordinator, Support Programs
 Position Description Ovarian Cancer Australia Support, Position Purpose The Support, is one of three roles responsible for the further development, coordination and implementation of Ovarian Cancer Australia
Position Description Ovarian Cancer Australia Support, Position Purpose The Support, is one of three roles responsible for the further development, coordination and implementation of Ovarian Cancer Australia
HEALTH CONSUMERS QUEENSLAND
 HEALTH CONSUMERS QUEENSLAND SUBMISSION TO The Inquiry into the establishment of a Queensland Health Promotion Commission Health and Ambulance Services Committee 27 th November 2015 Health Consumers Queensland
HEALTH CONSUMERS QUEENSLAND SUBMISSION TO The Inquiry into the establishment of a Queensland Health Promotion Commission Health and Ambulance Services Committee 27 th November 2015 Health Consumers Queensland
Ministry of Children and Youth Services. Follow-up to VFM Section 3.01, 2013 Annual Report RECOMMENDATION STATUS OVERVIEW
 Chapter 4 Section 4.01 Ministry of Children and Youth Services Autism Services and Supports for Children Follow-up to VFM Section 3.01, 2013 Annual Report RECOMMENDATION STATUS OVERVIEW # of Status of
Chapter 4 Section 4.01 Ministry of Children and Youth Services Autism Services and Supports for Children Follow-up to VFM Section 3.01, 2013 Annual Report RECOMMENDATION STATUS OVERVIEW # of Status of
Position is based Access Health & Community: Hawthorn and Doncaster East Manager, Alcohol and Other Drug Service
 Position Details Position Title Mode of Employment Award/EBA Classification Salary Packaging Department/Team Location Reports to Direct Reports Probationary Period Working with Children Check required
Position Details Position Title Mode of Employment Award/EBA Classification Salary Packaging Department/Team Location Reports to Direct Reports Probationary Period Working with Children Check required
Disability Care and Support Response to the Productivity Commission s Draft Report April 2011
 Disability Care and Support Response to the Productivity Commission s Draft Report April 2011 About the Australian Advisory Board on Autism Spectrum Disorders The Australian Advisory Board on Autism Spectrum
Disability Care and Support Response to the Productivity Commission s Draft Report April 2011 About the Australian Advisory Board on Autism Spectrum Disorders The Australian Advisory Board on Autism Spectrum
Peer Support Worker Street to Home
 Position Description September 17 Position description Peer Support Worker Street to Home Section A: position details Position title: Employment Status: Classification and Salary: Location: Hours: Peer
Position Description September 17 Position description Peer Support Worker Street to Home Section A: position details Position title: Employment Status: Classification and Salary: Location: Hours: Peer
Engaging stakeholders in prioritising and addressing evidence-practice gaps in maternal health care
 Engaging stakeholders in prioritising and addressing evidence-practice gaps in maternal health care Melanie Gibson-Helm 1, Jodie Bailie 2, Veronica Matthews 2, Alison Laycock 2, Jacqueline Boyle 1, Ross
Engaging stakeholders in prioritising and addressing evidence-practice gaps in maternal health care Melanie Gibson-Helm 1, Jodie Bailie 2, Veronica Matthews 2, Alison Laycock 2, Jacqueline Boyle 1, Ross
Submission to Department of Social Services on the Draft Service Model for delivery of integrated carer support services.
 Submission to Department of Social Services on the Draft Service Model for delivery of integrated carer support services. 16 December 2016 https://engage.dss.gov.au/a-new-integrated-carer-support-service-system
Submission to Department of Social Services on the Draft Service Model for delivery of integrated carer support services. 16 December 2016 https://engage.dss.gov.au/a-new-integrated-carer-support-service-system
Diabetic Retinopathy Position Paper SightFirst Long Range Planning (SFLRP) Working Group August 2008
 Diabetic Retinopathy Position Paper SightFirst Long Range Planning (SFLRP) Working Group August 2008 Introduction The mission of the Lions SightFirst program is to support the development of comprehensive
Diabetic Retinopathy Position Paper SightFirst Long Range Planning (SFLRP) Working Group August 2008 Introduction The mission of the Lions SightFirst program is to support the development of comprehensive
CONSUMER AND CARER PARTICIPATION POLICY. a framework for the mental health sector
 CONSUMER AND CARER PARTICIPATION POLICY a framework for the mental health sector developed by the National Consumer and Carer Forum Best Practice Principles for Inclusion in a Participation Policy
CONSUMER AND CARER PARTICIPATION POLICY a framework for the mental health sector developed by the National Consumer and Carer Forum Best Practice Principles for Inclusion in a Participation Policy
Community Support Worker - Macarthur Accommodation and Access Program (MAAP)
 Position Description Mar/Apr 2016 Position description Community Support Worker - Macarthur Accommodation and Access Program (MAAP) Section A: position details Position title: Employment Status Classification
Position Description Mar/Apr 2016 Position description Community Support Worker - Macarthur Accommodation and Access Program (MAAP) Section A: position details Position title: Employment Status Classification
The Hepatitis C Action Plan for Scotland: Draft Guidelines for Hepatitis C Care Networks
 The Hepatitis C Action Plan for Scotland: Draft Guidelines for Hepatitis C Care Networks Royal College of Physicians of Edinburgh Friday 12 October 2007 CONTENTS 1.0 ACCOUNTABILITY AND ORGANISATION 2.0
The Hepatitis C Action Plan for Scotland: Draft Guidelines for Hepatitis C Care Networks Royal College of Physicians of Edinburgh Friday 12 October 2007 CONTENTS 1.0 ACCOUNTABILITY AND ORGANISATION 2.0
Policy Statement Delivery of Oral Health: Special groups: Aboriginal and Torres Strait Islander Australians
 Policy Statement 2.3.5 Delivery of Oral Health: Special groups: Aboriginal and Torres Strait Islander Australians Position Summary Research must be funded to better understand the dental needs and issues
Policy Statement 2.3.5 Delivery of Oral Health: Special groups: Aboriginal and Torres Strait Islander Australians Position Summary Research must be funded to better understand the dental needs and issues
The Cancer Council NSW. Submission to the Legislative Assembly Public Accounts Committee. Inquiry into NSW State Plan Reporting
 The Cancer Council NSW Submission to the Legislative Assembly Public Accounts Committee Inquiry into NSW State Plan Reporting December 2007 2 Inquiry into NSW State Plan Reporting The Cancer Council NSW
The Cancer Council NSW Submission to the Legislative Assembly Public Accounts Committee Inquiry into NSW State Plan Reporting December 2007 2 Inquiry into NSW State Plan Reporting The Cancer Council NSW
POSITION DESCRIPTION:
 POSITION DESCRIPTION: SECTION A: POSITION CONTEXT Position Title Peer Practitioner (Consumer) Peer Recovery Communities Position Reference 10494 Position Type Full time 38 hours per week fixed term contract
POSITION DESCRIPTION: SECTION A: POSITION CONTEXT Position Title Peer Practitioner (Consumer) Peer Recovery Communities Position Reference 10494 Position Type Full time 38 hours per week fixed term contract
Prepared for Arthritis Australia October 2014
 Prepared for Arthritis Australia October 2014 Shona Bates, Charlotte Smedley, Melissa Wong, Rosemary Kayess, Karen R Fisher Research team Rosemary Kayess, Karen Fisher, Shona Bates, Charlotte Smedley,
Prepared for Arthritis Australia October 2014 Shona Bates, Charlotte Smedley, Melissa Wong, Rosemary Kayess, Karen R Fisher Research team Rosemary Kayess, Karen Fisher, Shona Bates, Charlotte Smedley,
Time for excellent palliative care in Queensland. 2018/2019 Palliative Care Queensland Pre-Budget Submission
 Time for excellent palliative care in Queensland 2018/2019 Palliative Care Queensland Pre-Budget Submission Executive Summary PCQ FOCUS AREA INITIATIVE ESTIMATED COST Individuals Matter Create a Statewide
Time for excellent palliative care in Queensland 2018/2019 Palliative Care Queensland Pre-Budget Submission Executive Summary PCQ FOCUS AREA INITIATIVE ESTIMATED COST Individuals Matter Create a Statewide
Updated Activity Work Plan : Drug and Alcohol Treatment
 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment This Drug and Alcohol Treatment Activity Work Plan template has the following parts: 1. The updated strategic vision of each PHN, specific
Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment This Drug and Alcohol Treatment Activity Work Plan template has the following parts: 1. The updated strategic vision of each PHN, specific
strategic plan strong teeth strong body strong mind Developed in partnership with Rotary Clubs of Perth and Heirisson
 strategic plan 2012-2016 strong teeth strong body strong mind CONTENTS Introduction 2 Key Result Area 1 Dental Health Education 5 Key Result Area 2 Dental Treatment 7 Key Result Area 3 Advocacy 9 Key
strategic plan 2012-2016 strong teeth strong body strong mind CONTENTS Introduction 2 Key Result Area 1 Dental Health Education 5 Key Result Area 2 Dental Treatment 7 Key Result Area 3 Advocacy 9 Key
NPA LAS REVIEW ADVISORY GROUP WORKSHOP 19 OCTOBER 2018
 NPA LAS 2015-2020 REVIEW ADVISORY GROUP WORKSHOP 19 OCTOBER 2018 OBJECTIVES The review team wants to road test key findings, focusing on those which are contested Update the Advisory Group on progress
NPA LAS 2015-2020 REVIEW ADVISORY GROUP WORKSHOP 19 OCTOBER 2018 OBJECTIVES The review team wants to road test key findings, focusing on those which are contested Update the Advisory Group on progress
STRATEGIC PLAN
 2016-2021 STRATEGIC PLAN inspired Behind this plan are strategies that will transform oral health care in Victoria OUR ORGANISATION Dental Health Services Victoria (DHSV) is the lead oral health agency
2016-2021 STRATEGIC PLAN inspired Behind this plan are strategies that will transform oral health care in Victoria OUR ORGANISATION Dental Health Services Victoria (DHSV) is the lead oral health agency
Submission to the Commonwealth Government on the New National Women s Health Policy
 Submission to the Commonwealth Government on the New National Women s Health Policy 1 July, 2009. Authorised and written by: Patty Kinnersly, CEO, Women s Health Grampians Contact person for this submission:
Submission to the Commonwealth Government on the New National Women s Health Policy 1 July, 2009. Authorised and written by: Patty Kinnersly, CEO, Women s Health Grampians Contact person for this submission:
North Coast Primary Health Network Drug and Alcohol Treatment Updated Activity Work Plan
 North Coast Primary Health Network Drug and Alcohol Treatment Updated Activity Work Plan 2016-2019 Contents Overview... 3 Strategic Vision for Drug and Alcohol Treatment... 3 Planned activities: Drug and
North Coast Primary Health Network Drug and Alcohol Treatment Updated Activity Work Plan 2016-2019 Contents Overview... 3 Strategic Vision for Drug and Alcohol Treatment... 3 Planned activities: Drug and
Peer Support Association. Strategic Plan and Development Strategy
 Peer Support Association Strategic Plan and Development Strategy Outcomes of the Strategic Development Day for Peer Supporters 29 th November 2014 Hosted by CoMHWA and Carers WA Executive Summary This
Peer Support Association Strategic Plan and Development Strategy Outcomes of the Strategic Development Day for Peer Supporters 29 th November 2014 Hosted by CoMHWA and Carers WA Executive Summary This
Peer Work Leadership Statement of Intent
 Peer Work Leadership Statement of Intent A National Professional Association for Mental Health Peer Workers Peer work leaders from Queensland, Victoria and NSW and colleagues from the USA participated
Peer Work Leadership Statement of Intent A National Professional Association for Mental Health Peer Workers Peer work leaders from Queensland, Victoria and NSW and colleagues from the USA participated
Consumer Consultant. PTBA (ichris) Community Mental Health. Owner Angela Micheletto
 Position Description Position Title Position Number Consumer Consultant PTBA (ichris) Position Status Part time, 0.6 0.8 EFT, until 30 September 2017 Program Area Award/Agreement/ Classification Reports
Position Description Position Title Position Number Consumer Consultant PTBA (ichris) Position Status Part time, 0.6 0.8 EFT, until 30 September 2017 Program Area Award/Agreement/ Classification Reports
Guidelines for indigenous allied health, indigenous enrolled nurses, Aboriginal health workers and Aboriginal health practitioners applying for
 Guidelines for indigenous allied health, indigenous enrolled nurses, Aboriginal health workers and Aboriginal health practitioners applying for Credentialling as a Diabetes Educator Guidelines for indigenous
Guidelines for indigenous allied health, indigenous enrolled nurses, Aboriginal health workers and Aboriginal health practitioners applying for Credentialling as a Diabetes Educator Guidelines for indigenous
4 th A-TRAC Symposium
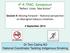 4 th A-TRAC Symposium Reflect. Unite. Take Action Session 4: Moving Forward National perspective on Aboriginal tobacco initiatives 4 September 2014 Dr Tom Calma AO National Coordinator Tackling Indigenous
4 th A-TRAC Symposium Reflect. Unite. Take Action Session 4: Moving Forward National perspective on Aboriginal tobacco initiatives 4 September 2014 Dr Tom Calma AO National Coordinator Tackling Indigenous
Clinical and Experimental Ophthalmology 2011; 39: doi: /j x. Key words: INTRODUCTION
 Clinical and Experimental Ophthalmology 2011; 9: 50 57 doi: 10.1111/j.1442-9071.2010.02475.x Original Article Funding models for outreach ophthalmology services Angus W Turner FRANZCO MSc(Oxon), 1 Will
Clinical and Experimental Ophthalmology 2011; 9: 50 57 doi: 10.1111/j.1442-9071.2010.02475.x Original Article Funding models for outreach ophthalmology services Angus W Turner FRANZCO MSc(Oxon), 1 Will
Published December 2015
 Published December 2015 Contents Executive summary 3 1. Introduction The changing story of cancer 6 2. Current state Poor performance 7 Fragmentation and duplication 7 Existing and developing programme
Published December 2015 Contents Executive summary 3 1. Introduction The changing story of cancer 6 2. Current state Poor performance 7 Fragmentation and duplication 7 Existing and developing programme
Support Facilitator Partners in Recovery Strathpine
 Position Description July 2014 Position description Support Facilitator Partners in Recovery Strathpine Section A: position details Employment Status Classification and Salary Location: Hours: Full time
Position Description July 2014 Position description Support Facilitator Partners in Recovery Strathpine Section A: position details Employment Status Classification and Salary Location: Hours: Full time
Women s Health Association of Victoria
 Women s Health Association of Victoria PO Box 1160, Melbourne Vic 3001 Submission to the Commonwealth Government on the New National Women s Health Policy 1 July, 2009. Contact person for this submission:
Women s Health Association of Victoria PO Box 1160, Melbourne Vic 3001 Submission to the Commonwealth Government on the New National Women s Health Policy 1 July, 2009. Contact person for this submission:
Community Advisory Council Terms of Reference
 Community Advisory Council Terms of Reference The role of the Community Advisory Councils (CACs) is to provide the Board of the Sunshine Coast Health Network Ltd (SCHN) trading as Central Queensland, Wide
Community Advisory Council Terms of Reference The role of the Community Advisory Councils (CACs) is to provide the Board of the Sunshine Coast Health Network Ltd (SCHN) trading as Central Queensland, Wide
Peer Support Worker. Position description. Section A: Position details. Organisational context
 Position Description February 18 Position description Peer Support Worker Section A: Position details Position title: Employment Status: Classification and Salary: Location: Hours: Peer Support Worker
Position Description February 18 Position description Peer Support Worker Section A: Position details Position title: Employment Status: Classification and Salary: Location: Hours: Peer Support Worker
The Silent Disease Inquiry into Hepatitis C in Australia
 Australian Government response to the House of Representatives Standing Committee on Health report: The Silent Disease Inquiry into Hepatitis C in Australia November 2016 LIST OF ABBREVIATIONS AHPPC Australian
Australian Government response to the House of Representatives Standing Committee on Health report: The Silent Disease Inquiry into Hepatitis C in Australia November 2016 LIST OF ABBREVIATIONS AHPPC Australian
Accessibility and quality of mental health services in rural and remote Australia. August Recommendations
 AMSANT submission to the Senate Community Affairs References Committee Inquiry: Accessibility and quality of mental health services in rural and remote Australia August 2018 Recommendations 1) Mental health
AMSANT submission to the Senate Community Affairs References Committee Inquiry: Accessibility and quality of mental health services in rural and remote Australia August 2018 Recommendations 1) Mental health
FINAL REPORT. as part of the National Visual Impairment Prevention Program. of the. Victorian Retinopathy Screening Development Project
 FINAL REPORT of the Victorian Retinopathy Screening Development Project as part of the National Visual Impairment Prevention Program Centre for Eye Research Australia July 2001 FINAL REPORT of the Victorian
FINAL REPORT of the Victorian Retinopathy Screening Development Project as part of the National Visual Impairment Prevention Program Centre for Eye Research Australia July 2001 FINAL REPORT of the Victorian
High Level Across Sector Support to Implement the Three Plans South Australian Aboriginal Chronic Disease Consortium Goal Vision
 Now I live my life like there s no tomorrow. I live for my children and I live for my family. It has been twenty years since my diagnosis with testicular cancer. I can truly say that I won the race and
Now I live my life like there s no tomorrow. I live for my children and I live for my family. It has been twenty years since my diagnosis with testicular cancer. I can truly say that I won the race and
Updated Activity Work Plan : Drug and Alcohol Treatment NEPEAN BLUE MOUNTAINS PHN
 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment NEPEAN BLUE MOUNTAINS PHN 1 Strategic Vision for Drug and Alcohol Treatment Funding The high priority service and treatment needs identified
Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment NEPEAN BLUE MOUNTAINS PHN 1 Strategic Vision for Drug and Alcohol Treatment Funding The high priority service and treatment needs identified
Who we are. We envision a world where high quality eye health and vision care is accessible to all people.
 Who we are The World Council of Optometry (WCO) is an international optometric association founded in 1927. The WCO represents over 200,000 optometrists in more than 60 countries, through almost 300 Country,
Who we are The World Council of Optometry (WCO) is an international optometric association founded in 1927. The WCO represents over 200,000 optometrists in more than 60 countries, through almost 300 Country,
Regional Strategic Plan
 Regional Strategic Plan 2012-15 Vision Working collaboratively with stakeholders and the community, so that people in the Loddon Mallee Region with a progressive life-limiting illness and their families/carers,
Regional Strategic Plan 2012-15 Vision Working collaboratively with stakeholders and the community, so that people in the Loddon Mallee Region with a progressive life-limiting illness and their families/carers,
Recommendation 2: Voluntary groups should be supported to build their capacity to promote mental health among their client groups.
 Submission to the independent review group examining the role of voluntary organisations in the operation of health and personal social services in Ireland May 2018 Introduction Mental Health Reform (MHR)
Submission to the independent review group examining the role of voluntary organisations in the operation of health and personal social services in Ireland May 2018 Introduction Mental Health Reform (MHR)
National Standards for Diabetes Education Programs
 National Standards for Diabetes Education Programs Australian Diabetes Educators Association Established 1981 National Standards For Diabetes Education Programs - ADEA 2001 Page 1 Published July 2001 by
National Standards for Diabetes Education Programs Australian Diabetes Educators Association Established 1981 National Standards For Diabetes Education Programs - ADEA 2001 Page 1 Published July 2001 by
Mental Health and AoD Community Briefing Outcomes
 The Community Briefing on 28 June was attended by almost 100 participants and data from 7 stations were gathered on the following topics: Suicide Prevention CALD and Indigenous Child and Youth Severe and
The Community Briefing on 28 June was attended by almost 100 participants and data from 7 stations were gathered on the following topics: Suicide Prevention CALD and Indigenous Child and Youth Severe and
