Brief Resolved Unexplained Events (Apparent Life Threatening Events)
|
|
|
- Sharon Carson
- 6 years ago
- Views:
Transcription
1 Brief Resolved Unexplained Events (Apparent Life Threatening Events) Joel S. Tieder, MD, MPH Chair, AAP Subcommittee on Brief Resolved Unexplained Events Associate Professor Pediatrics Seattle Children s Hospital The University of Washington School of Medicine
2 Disclaimer Statements and opinions expressed are those of the authors and not necessarily those of the American Academy of Pediatrics. Mead Johnson sponsors programs such as this to give healthcare professionals access to scientific and educational information provided by experts. The presenter has complete and independent control over the planning and content of the presentation, and is not receiving any compensation from Mead Johnson for this presentation. The presenter s comments and opinions are not necessarily those of Mead Johnson. In the event that the presentation contains statements about uses of drugs that are not within the drugs' approved indications, Mead Johnson does not promote the use of any drug for indications outside the FDAapproved product label.
3 You will learn about 1. Historical framework and epidemiology 2. ALTE vs BRUE 3. Event characterization: explained vs unexplained 4. Risk stratification and new recommendations 5. Tools to implement change in your practice
4 Historical Framework and Epidemiology 1
5 What was an Apparent Life Threatening Event?
6 Definition of ALTE An episode in the first year of life that appears potentially life threatening to the observer and is characterized by some combination of: Color change Apnea Alteration in muscle tone Choking or gagging National Institutes of Health (1987) Consensus development conference on infantile apnea and home monitoring Pediatrics 79:
7 Defined decades ago to better understand SIDS
8 Epidemiology Conservatively 1 out of children hospitalized for an ALTE But scary events are very common 43% of healthy infants have had 20 sec apnea episode over 3 mo period 5% of parents recall seeing apnea event Normal in infants: choking, gagging, blue discoloration, tone changes, periodic and irregular breathing Monti MC, Borrelli P, Nosetti L, Tajè S, Perotti M, Bonarrigo D, Stramba Badiale M, Montomoli C. Incidence of apparent life-threatening events and post-neonatal risk factors. Acta Paediatr Mar 6. Kiechl-Kohlendorfer U, Hof D, Peglow UP, Traweger-Ravanelli B, Kiechl S. Epidemiology of apparent life threatening events. Arch Dis Child Mar;90(3): Ramanathan R, Corwin MJ, Hunt CE, et al. Cardiorespiratory events recorded on home monitors: comparison of healthy infants with those at increased risk for SIDS. JAMA 2001;285: Mitchell EA, Thompson JM. Parental reported apnoea, admissions to hospital and sudden infant death syndrome. Acta Paediatr 2001;90: ]
9 ALTE discharge diagnosis Most common Idiopathic (26-50%) GER (26-54%) Respiratory infection (8-11%) Seizure (9-11%) Less common Child maltreatment (<1%) Pertussis (0.05-9%) Cardiac arrhythmias (<1%) Bacterial infection (0-8%) Metabolic Disorder (1.5%) McGovern MC, Smith MB. Causes of apparent life threatening events in infants: a systematic review. Arch Dis Child Nov;89(11): Review.
10 AN ALTE IS NOT A WARNING SIGN FOR SIDS! No causal relationship of preexisting apnea or ALTE and SIDs Interventions to reduce SIDs have not reduced ALTEs (e.g. back to sleep) SIDS and ALTEs have different risk factors Bonkowsky, J. L., Guenther, E., Filloux, F. M., & Srivastava, R. (2008). Death, child abuse, and adverse neurological outcome of infants after an apparent life- threatening event. Pediatrics, 122(1), doi: /peds Esani N, Hodgman JE, Ehsani N, Hoppenbrouwers T. Apparent life-threatening events and sudden infant death syndrome: comparison of risk factors. J Pediatr Mar;152(3): Freed GE, Steinschneider A, Glassman M, Winn K. Sudden infant death syndrome prevention and an understanding of selected clinical issues. Pediatr Clin North Am Oct;41(5): Review.
11 ALTE a recipe for a testing/treatment cascade Broad differential diagnosis Anxiety provoking Common Low prevalence of disease Perceived reassurance from testing or hospitalization Poor understanding of true risk Use of nonspecific testing prone to false positive results
12 High Resource Use and Variation Multicenter study of patients hospitalized with ALTE Mean LOS = 4.4 (SD 5.6) days Mean adjusted charges = $15,567 (SD $28,510) Readmission = 2.5% but variable Tieder, JS et al. Variation in inpatient resource utilization and management of Apparent Life- Threatening Events. J Peds May;152(5):629-35, 635.
13 Resource Utilization Across Hospitals Percentage of ALTE Patients 0% 10% 20% 30% 40% 50% 60% 70% 80% 90% Lab Tests RSV Pertussis CBC Reflux Tests ph probe Upper GI Imaging Other Tests CT Chest xray Sleep testing EKG EEG Tieder, JS et al. Variation in inpatient resource utilization and management of Apparent Life-Threatening Events. J Peds May;152(5):629-35, 635. Medications Antiobiotics Anti-reflux Medians and Interquartile Ranges
14 For infants that are well appearing upon presentation Historical and PE features can identify risk Testing tailored to these risks of value True risk of a subsequent event or underlying disorder cannot be ascertained A more precise definition of an ALTE is needed Further research is warranted Systematic Review
15 The Event Formerly Known as ALTE 2
16 ALTE vs BRUE ALTE An episode in the first year of life that appears potentially life threatening to the observer and is characterized by some combination of BRUE Event occurring in an infant < 1 year where the observer reports a sudden, brief period of one or more of the following No explanation for event after appropriate history and PE
17 ALTE Color change Apnea Alteration in muscle tone Choking or gagging ALTE vs BRUE BRUE Cyanosis or pallor Absent, decreased, or irregular breathing Marked change in tone (hyper- or hypotonia) Altered level of responsiveness
18 ALTE vs BRUE ALTE Both chief complaint and diagnosis Not always lifethreatening Can have ongoing symptoms (e.g., fever, URI) Can have a diagnosis (e.g., meningitis, bronchiolitis) BRUE Diagnosis of exclusion Excludes patients with an explanation or diagnosis (e.g., GER) Excludes symptomatic infants (i.e., just an event)
19 Event characterization Explained vs Unexplained 3
20
21
22
23 Color ALTE Color change Apnea Alteration in muscle tone Choking or gagging BRUE Cyanosis or pallor Absent, decreased, or irregular breathing Marked change in tone (hyper- or hypotonia) Altered level of responsiveness
24 Color change-red, white, and blue
25 Normal explanations of turning blue briefly Peripheral cyanosis increased O2 extraction by peripheral tissue or vasoconstriction (e.g. shock) Acrocyanosis vasomotor instability
26 Blue episode can indicate something serious Central cyanosis bluish discoloration of oral mucous membranes
27 What about red and white episodes? Plethora: red is a normal in infants. Pallor: White or ashen can be normal or a sign of decreased perfusion Skin color difficult to determine in different skin tones and lighting
28 Apnea or changes to breathing ALTE Color change Apnea Alteration in muscle tone Choking or gagging BRUE Cyanosis or pallor Absent, decreased, or irregular breathing Marked change in tone (hyper- or hypotonia) Altered level of responsiveness
29 Normal explanations for episodic change in breathing Periodic breathing Typically developing infants have periods of cyclic breathing with pauses Occurs in nearly all pre-term infants and most term infants Decreases dramatically after 2 months of age Not a precursor for SIDS Irregular respirations Hallmark of active sleep (REM or dream sleep) Present at all ages Breath holding spell Acute decreases in oxygen saturation >10% from baseline are observed in most infants briefly during sleep
30 Concerning change in breathing Cessation of airflow x sec Central absence of respiratory effort from central respiratory center Obstructive paradoxical inverse movements of the chest wall and abdomen with decreased saturation Apnea of prematurity <37 weeks post-conceptional age may persist in infants < 28 wk
31 Muscle tone change ALTE Color change Apnea Alteration in muscle tone Choking or gagging BRUE Cyanosis or pallor Absent, decreased, or irregular breathing Marked change in tone (hyper- or hypotonia) Altered level of responsiveness
32 Normal explanations for episodic changes in tone Stimulation (i.e., laryngospasm) from coughing, gagging, choking, crying Startle and fencing reflex LOC from Breath holding spell
33 Concerning causes for episodic change Seizure: in tone Rhythmic and not extinguishable Eye deviation Limp Rigid Post-ictal Generalized/Altered mental status Infantile spasm
34 Apnea or changes to breathing ALTE Color change Apnea Alteration in muscle tone Choking or gagging BRUE Cyanosis or pallor Absent, decreased, or irregular breathing Marked change in tone (hyper- or hypotonia) Altered level of responsiveness
35 Normal explanation for episode of altered responsiveness Immature nervous system Somnolence LOC with Breath holding spell
36 Concerning explanation for episode of altered responsiveness Seizure LOC Hypoxemia Hypoglycemia
37
38 History and PE are critical to diagnose BRUE!
39 Risk Stratification and Recommendations for Lower-Risk 4
40
41 Lower-Risk Criteria Age >60 days Prematurity: gestational age 32 weeks and postconceptional age 45 weeks First BRUE (no prior BRUE ever and not occurring in clusters) Duration of event <1 minute No CPR required by trained medical provider No concerning historical features No concerning physical examination findings
42 AAP and strength of recommendations
43
44 Pulmonology Need not admit the patient to the hospital solely for cardiorespiratory monitoring (B, Weak) May briefly monitor patients with continuous pulse oximetry and serial observations (D, Weak) Should not obtain a chest radiograph (B, Mod) Should not obtain measurement of blood gases (B, Mod) Should not initiate home cardio-respiratory monitoring (B, Mod) Should not obtain overnight polysomnography (B, Mod)
45 Cardiology May obtain a 12-lead electrocardiogram. (C, Weak) Should not obtain echocardiography (C, Moderate)
46 Child abuse Need not obtain neuroimaging (CT, MRI, US) to detect child abuse (C, Weak) Should obtain an assessment of social risk factors to detect child abuse (C, Weak)
47 Neurology Should not obtain neuroimaging (CT, MRI, US) to detect neurologic disorders (C, Mod) Should not obtain an EEG (electroencephalography) (C, Mod) Should not prescribe anti-epileptic medications (C, Mod)
48 Infectious Disease Should not obtain a WBC, blood culture, or CSF analysis or culture to identify an occult bacterial infection (B, Strong) Should not obtain a chest radiograph to assess for pulmonary infection (B, Mod) Need not obtain a UA (C, Weak) Need not obtain respiratory viral testing in infants (C, Weak) May obtain test for pertussis (B, Weak)
49 Gastroenterology
50 Gastroenterology Should not obtain investigations for GER (C, Mod) Should not prescribe acid suppression therapy (C, Mod)
51 Inborn Error of Metabolism Need not obtain blood glucose (C, Weak) Need not obtain serum lactic acid or bicarbonate (C, Weak) Should not obtain serum sodium, potassium, chloride, BUN, creatinine, calcium, or ammonia (C, Mod) Should not obtain venous or arterial blood gas (C, Mod) Should not obtain urine organic acids, plasma amino acids or plasma acylcarnitines (C, Mod)
52 Anemia Should not obtain laboratory evaluations for anemia (C. Mod)
53 Patient- and Family-Centered Care Should offer resources for CPR training to caregiver (C, Mod) Should educate caregivers about BRUEs (D, Weak) Should use shared decision making (C. Mod)
54 Implementation and Improvement 5
55 Implementation & Improvement: AAP.org Education AAP, AAFP, ACEP, ABP, SHM news and conference outlets Caregiver handout Webinar Work flow integration Crowdsourcing of orderset, H&P templates, algorithm QI, research, billing ICD-9/10 codes, MOC collaborative with QuIIN/VIP/PEMCRC Proposed quality measures Key Driver Diagram
56 Key Driver Diagram: AAP.org
57 Caregiver Handouts: AAP.org
58 Future Directions Guidance on Higher-Risk BRUEs Better identification of child abuse Understand epidemiology and risk Understand patient- and family-centered outcomes Empiric GER treatment
59 Take home points ALTEs are very different from SIDS Can you explain the event with careful history and physical exam? Remember child abuse can present as an ALTE/BRUE Is the patient asymptomatic and wellappearing? Is the patient in the lower-risk group? Perform diagnostic tests based on true, rather than perceived risk Use shared decision making and inform caregivers of potential harm to testing/hospitalization Goodbye ALTE Hello BRUE
60 A special thanks to AAP Sub-Committee Josh Bonkowsky Ruth Etzel Wayne Franklin David Gremse Bruce Herman Eliot Katz Leonard Krilov Lawrence Merrit Chuck Norlin Jack Percelay Robert Sapian Rick Shiffman Mike Smith AAP Support Ricardo Quinonez Diana Cunningham Caryn Davidson Lisa Krams Kymika Okechukwu and 40+ guideline reviewers SHM ALTE expert panel Rob in Altman Josh Bonkowsky Don Brand Ilene Claudius Diana Cunningham Jack Percelay Raymond Pitteti Mike Smith Taylor Marsh
61 Questions and Discussion
62 References (in order of appearance) 1. National Institutes of Health (1987) Consensus development conference on infantile apnea and home monitoring Pediatrics 79: Monti MC, Borrelli P, Nosetti L, Tajè S, Perotti M, Bonarrigo D, Stramba Badiale M, Montomoli C. Incidence of apparent life-threatening events and post-neonatal risk factors. Acta Paediatr Mar Kiechl-Kohlendorfer U, Hof D, Peglow UP, Traweger-Ravanelli B, Kiechl S. Epidemiology of apparent life threatening events. Arch Dis Child Mar;90(3): Ramanathan R, Corwin MJ, Hunt CE, et al. Cardiorespiratory events recorded on home monitors: comparison of healthy infants with those at increased risk for SIDS. JAMA 2001;285: Mitchell EA, Thompson JM. Parental reported apnoea, admissions to hospital and sudden infant death syndrome. Acta Paediatr 2001;90: ] 6. McGovern MC, Smith MB. Causes of apparent life threatening events in infants: a systematic review. Arch Dis Child Nov;89(11): Review. 7. Bonkowsky, J. L., Guenther, E., Filloux, F. M., & Srivastava, R. (2008). Death, child abuse, and adverse neurological outcome of infants after an apparent life- threatening event. Pediatrics, 122(1), doi: /peds Esani N, Hodgman JE, Ehsani N, Hoppenbrouwers T. Apparent life-threatening events and sudden infant death syndrome: comparison of risk factors. J Pediatr Mar;152(3): Freed GE, Steinschneider A, Glassman M, Winn K. Sudden infant death syndrome prevention and an understanding of selected clinical issues. Pediatr Clin North Am Oct;41(5): Review 10. Tieder JS et al. Variation in inpatient resource utilization and management of Apparent Life-Threatening Events. J Peds May;152(5):629-35, Tieder JS, Altman RL, Bonkowsky JL, Brand DA, Claudius I, Cunningham DJ, DeWolfe C, Percelay JM, Pitetti RD, Smith MB. Management of apparent life-threatening events in infants: a systematic review. J Pediatr Jul;163(1):94-9.e Tieder JS, et al. Brief Resolved Unexplained Events (Formerly Apparent Life-Threatening Events) and Evaluation of Lower-Risk Infants: Executive Summary
CLINICAL PRACTICE GUIDELINE Guidance for the Clinician in Rendering Pediatric Care EXECUTIVE SUMMARY FROM THE AMERICAN ACADEMY OF PEDIATRICS
 CLINICAL PRACTICE GUIDELINE Guidance for the Clinician in Rendering Pediatric Care Brief Resolved Unexplained Events (Formerly Apparent Life-Threatening Events) and Evaluation of Lower- Risk Infants: Executive
CLINICAL PRACTICE GUIDELINE Guidance for the Clinician in Rendering Pediatric Care Brief Resolved Unexplained Events (Formerly Apparent Life-Threatening Events) and Evaluation of Lower- Risk Infants: Executive
CLINICAL PRACTICE GUIDELINE Guidance for the Clinician in Rendering Pediatric Care EXECUTIVE SUMMARY FROM THE AMERICAN ACADEMY OF PEDIATRICS
 CLINICAL PRACTICE GUIDELINE Guidance for the Clinician in Rendering Pediatric Care Brief Resolved Unexplained Events (Formerly Apparent Life-Threatening Events) and Evaluation of Lower- Risk Infants: Executive
CLINICAL PRACTICE GUIDELINE Guidance for the Clinician in Rendering Pediatric Care Brief Resolved Unexplained Events (Formerly Apparent Life-Threatening Events) and Evaluation of Lower- Risk Infants: Executive
Home Cardiorespiratory Monitoring. Description. Section: Durable Medical Equipment Effective Date: April 15, 2017
 Subject: Home Cardiorespiratory Monitoring Page: 1 of 9 Last Review Status/Date: March 2017 Home Cardiorespiratory Monitoring Description Home cardiorespiratory monitors track respiratory effort and heart
Subject: Home Cardiorespiratory Monitoring Page: 1 of 9 Last Review Status/Date: March 2017 Home Cardiorespiratory Monitoring Description Home cardiorespiratory monitors track respiratory effort and heart
What s a BRUE? /pr. broo / EDAP Conference September 8, 2016 Josh Siembieda, MD FAAP
 What s a BRUE? /pr. broo / EDAP Conference September 8, 2016 Josh Siembieda, MD FAAP Objectives Review history of the definition of ALTE Discss the AAP BRUE Clinical Practice Gideline Overview of the differential
What s a BRUE? /pr. broo / EDAP Conference September 8, 2016 Josh Siembieda, MD FAAP Objectives Review history of the definition of ALTE Discss the AAP BRUE Clinical Practice Gideline Overview of the differential
BRUE and Apnea at Term, how do they relate?
 BRUE and Apnea at Term, how do they relate? Mary Elaine Patrinos, M.D. Attending Neonatologist Rainbow Babies and Children s Hospital Director, Infant Apnea Program Apnea at Term Can it happen? How does
BRUE and Apnea at Term, how do they relate? Mary Elaine Patrinos, M.D. Attending Neonatologist Rainbow Babies and Children s Hospital Director, Infant Apnea Program Apnea at Term Can it happen? How does
CLINICAL PRACTICE GUIDELINE Guidance for the Clinician in Rendering Pediatric Care
 CLINICAL PRACTICE GUIDELINE Guidance for the Clinician in Rendering Pediatric Care Brief Resolved Unexplained Events (Formerly Apparent Life-Threatening Events) and Evaluation of Lower-Risk Infants Joel
CLINICAL PRACTICE GUIDELINE Guidance for the Clinician in Rendering Pediatric Care Brief Resolved Unexplained Events (Formerly Apparent Life-Threatening Events) and Evaluation of Lower-Risk Infants Joel
This has great potential Apparent Life Threatening Events: Another Lengthy Time-consuming i Evaluation? Erich C. Maul, DO, FAAP Associate Program Dire
 Apparent Life Threatening Events: Actual Life Threatening Events? Erich C. Maul, DO, FAAP Associate Program Director, Pediatric Residency Assistant Professor of Pediatrics University of Kentucky College
Apparent Life Threatening Events: Actual Life Threatening Events? Erich C. Maul, DO, FAAP Associate Program Director, Pediatric Residency Assistant Professor of Pediatrics University of Kentucky College
In stable term infants, heart rates as low as 70 beats per minute while sleeping are acceptable. (Benitz, 2015)
 Clinical Performance Guideline Neonatal Resource Services Apnea and Bradycardia Medical Necessity Guideline Purpose: To provide guidelines for the management and follow-up of neonatal and infantile apnea
Clinical Performance Guideline Neonatal Resource Services Apnea and Bradycardia Medical Necessity Guideline Purpose: To provide guidelines for the management and follow-up of neonatal and infantile apnea
Relationship between the Clinical Characteristics and Intervention Scores of Infants with Apparent Life-threatening Events
 ORIGINAL ARTICLE Pediatrics http://dx.doi.org/0.3346/jkms.05.30.6.763 J Korean Med Sci 05; 30: 763-769 Relationship between the Clinical Characteristics and Intervention Scores of Infants with Apparent
ORIGINAL ARTICLE Pediatrics http://dx.doi.org/0.3346/jkms.05.30.6.763 J Korean Med Sci 05; 30: 763-769 Relationship between the Clinical Characteristics and Intervention Scores of Infants with Apparent
Clinical Performance Guideline Neonatal Resource Services Apnea and Bradycardia
 Clinical Performance Guideline Neonatal Resource Services Apnea and Bradycardia Medical Necessity Guideline Reviewed and Accepted by Corporate Medical Affairs Committee (CMAC) Date: October 2018 Purpose:
Clinical Performance Guideline Neonatal Resource Services Apnea and Bradycardia Medical Necessity Guideline Reviewed and Accepted by Corporate Medical Affairs Committee (CMAC) Date: October 2018 Purpose:
From ALTE to BRUE: Brief Resolved Unexplained Events
 From ALTE to BRUE: Brief Resolved Unexplained Events James P. McCord MD Medical Director, Pediatric Inpatient Services Randall Children s Hospital April 30, 2017 Objectives and Disclosures Objective: Become
From ALTE to BRUE: Brief Resolved Unexplained Events James P. McCord MD Medical Director, Pediatric Inpatient Services Randall Children s Hospital April 30, 2017 Objectives and Disclosures Objective: Become
PEDIATRIC RESPIRATORY ILLNESS MADE SIMPLE
 Copyright 2012 Joel Berezow, MD and The Pediatrics for Emergency Physicians Network All rights reserved. Duplication in whole or in part, or electronic transmission in any form, is prohibited THE PEDIATRICS
Copyright 2012 Joel Berezow, MD and The Pediatrics for Emergency Physicians Network All rights reserved. Duplication in whole or in part, or electronic transmission in any form, is prohibited THE PEDIATRICS
Clinical Policy Title: Apnea monitors for infants in-home use
 Clinical Policy Title: Apnea monitors for infants in-home use Clinical Policy Number: 11.02.00 Effective Date: October 1 2014 Initial Review Date: March 19 2014 Most Recent Review Date: April 19 2017 Next
Clinical Policy Title: Apnea monitors for infants in-home use Clinical Policy Number: 11.02.00 Effective Date: October 1 2014 Initial Review Date: March 19 2014 Most Recent Review Date: April 19 2017 Next
Clinical Policy Title: Apnea monitors for infants in-home use
 Clinical Policy Title: Apnea monitors for infants in-home use Clinical Policy Number: 11.02.00 Effective Date: October 1 2014 Initial Review Date: March 19 2014 Most Recent Review Date: April 10, 2018
Clinical Policy Title: Apnea monitors for infants in-home use Clinical Policy Number: 11.02.00 Effective Date: October 1 2014 Initial Review Date: March 19 2014 Most Recent Review Date: April 10, 2018
(C) The following criteria must be met for coverage of an apnea monitor:
 ACTION: Final DATE: 07/02/2018 10:05 AM 5160-10-09 Apnea monitors. TO BE RESCINDED (A) Definitions. (1) "Apnea monitors" are defined as cardiorespiratory monitoring devices capable of providing continuous
ACTION: Final DATE: 07/02/2018 10:05 AM 5160-10-09 Apnea monitors. TO BE RESCINDED (A) Definitions. (1) "Apnea monitors" are defined as cardiorespiratory monitoring devices capable of providing continuous
Fever in neonates (age 0 to 28 days)
 Fever in neonates (age 0 to 28 days) INCLUSION CRITERIA Infant 28 days of life Temperature 38 C (100.4 F) by any route/parental report EXCLUSION CRITERIA Infants with RSV Febrile Infant 28 days old Ill
Fever in neonates (age 0 to 28 days) INCLUSION CRITERIA Infant 28 days of life Temperature 38 C (100.4 F) by any route/parental report EXCLUSION CRITERIA Infants with RSV Febrile Infant 28 days old Ill
An apparent life-threatening event (ALTE) was defined at a consensus development conference convened in
 Management of Apparent Life-Threatening Events in Infants: A Systematic Review Joel S. Tieder, MD, MPH 1, Robin L. Altman, MD 2, Joshua L. Bonkowsky, MD, PhD 3, Donald A. Brand, PhD 4,5, Ilene Claudius,
Management of Apparent Life-Threatening Events in Infants: A Systematic Review Joel S. Tieder, MD, MPH 1, Robin L. Altman, MD 2, Joshua L. Bonkowsky, MD, PhD 3, Donald A. Brand, PhD 4,5, Ilene Claudius,
Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis
 Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis Gal S, Riskin A, Chistyakov I, Shifman N, Srugo I, and Kugelman A Pediatric Department and Pediatric Pulmonary Unit Bnai Zion
Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis Gal S, Riskin A, Chistyakov I, Shifman N, Srugo I, and Kugelman A Pediatric Department and Pediatric Pulmonary Unit Bnai Zion
SmartMonitor Helpful for Filing
 Apnea Monitor HCPCS E0618 or E0619 Overview The following information describes coverage and payment information regarding the use of the Circadiance SmartMonitor: Coding, coverage, payment, and documentation
Apnea Monitor HCPCS E0618 or E0619 Overview The following information describes coverage and payment information regarding the use of the Circadiance SmartMonitor: Coding, coverage, payment, and documentation
PEDIATRIC BRAIN CARE
 PEDIATRIC BRAIN CARE The brain matters most! OVERVIEW OF NEURO ASSESSMENT 1. Overall responsiveness/activity 2. The eyes 3.? Increased ICP 4. Movements 5.? Seizures 6. Other OVERALL RESPONSIVENESS/ ACTIVITY
PEDIATRIC BRAIN CARE The brain matters most! OVERVIEW OF NEURO ASSESSMENT 1. Overall responsiveness/activity 2. The eyes 3.? Increased ICP 4. Movements 5.? Seizures 6. Other OVERALL RESPONSIVENESS/ ACTIVITY
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Case #1. Inter-ictal EEG. Difficult Diagnosis Pediatrics. 15 mos girl with medically refractory infantile spasms 2/13/2010
 Difficult Diagnosis Pediatrics Joseph E. Sullivan M.D. Assistant Professor of Clinical Neurology & Pediatrics Director, UCSF Pediatric Epilepsy Center University of California San Francisco Case #1 15
Difficult Diagnosis Pediatrics Joseph E. Sullivan M.D. Assistant Professor of Clinical Neurology & Pediatrics Director, UCSF Pediatric Epilepsy Center University of California San Francisco Case #1 15
IAEM Clinical Guideline 9 Laryngomalacia. Version 1 September, Author: Dr Farah Mustafa
 IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE Management, Monitoring & Documentation of a Clinically Significant Cardiopulmonary Event (CSCPE) (NUR47) DATE: REVIEWED: PAGES: 9/09 9/17 1 of 6 PS1094
SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE Management, Monitoring & Documentation of a Clinically Significant Cardiopulmonary Event (CSCPE) (NUR47) DATE: REVIEWED: PAGES: 9/09 9/17 1 of 6 PS1094
Research in Medical Physics: Physiological Signals and Dynamics
 Research in Medical Physics: Physiological Signals and Dynamics Incidents of apnea or of sepsis create critical situations in a neonatal intensive care unit (NICU). Of the 4.2 million babies born annually
Research in Medical Physics: Physiological Signals and Dynamics Incidents of apnea or of sepsis create critical situations in a neonatal intensive care unit (NICU). Of the 4.2 million babies born annually
Objectives. Apnea Definition and Pitfalls. Pathophysiology of Apnea. Apnea of Prematurity and hypoxemia episodes 5/18/2015
 Apnea of Prematurity and hypoxemia episodes Deepak Jain MD Care of Sick Newborn Conference May 2015 Objectives Differentiating between apnea and hypoxemia episodes. Pathophysiology Diagnosis of apnea and
Apnea of Prematurity and hypoxemia episodes Deepak Jain MD Care of Sick Newborn Conference May 2015 Objectives Differentiating between apnea and hypoxemia episodes. Pathophysiology Diagnosis of apnea and
Pediatric Advanced Life Support
 Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
SLEEP STUDIES IN THE VERY, VERY YOUNG
 SLEEP STUDIES IN THE VERY, VERY YOUNG Julie DeWitte, RCP, RPSGT, RST Assistant Department Administrator Kaiser Permanente Fontana Sleep Center AAST Director-at-Large Board Member NEONATES THROUGH INFANCY
SLEEP STUDIES IN THE VERY, VERY YOUNG Julie DeWitte, RCP, RPSGT, RST Assistant Department Administrator Kaiser Permanente Fontana Sleep Center AAST Director-at-Large Board Member NEONATES THROUGH INFANCY
CASE-BASED SMALL GROUP DISCUSSION MHD II
 MHD II, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II Session 11 April 11, 2016 STUDENT COPY MHD II, Session 11, Student Copy Page 2 CASE HISTORY 1 Chief complaint: Our baby
MHD II, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II Session 11 April 11, 2016 STUDENT COPY MHD II, Session 11, Student Copy Page 2 CASE HISTORY 1 Chief complaint: Our baby
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Emergency Department Triage
 Emergency Department Triage Julia Fuzak, MD, Patrick Mahar, MD The Children s Hosital Denver, CO, USA 1/30/09 Hospital Pediatrico Juan Manuel Marquez Habana, Cuba Objectives What is does triage mean? Why
Emergency Department Triage Julia Fuzak, MD, Patrick Mahar, MD The Children s Hosital Denver, CO, USA 1/30/09 Hospital Pediatrico Juan Manuel Marquez Habana, Cuba Objectives What is does triage mean? Why
Blue Babies, Twitchy Toddlers, and Kool Kids. By Beth Paton, MSN, RN, PNP, CEN, CPEN, FAEN
 Blue Babies, Twitchy Toddlers, and Kool Kids By Beth Paton, MSN, RN, PNP, CEN, CPEN, FAEN I have no disclosures OBJECTIVES By the end of this presentation, the learner will Discuss etiologies of cyanosis
Blue Babies, Twitchy Toddlers, and Kool Kids By Beth Paton, MSN, RN, PNP, CEN, CPEN, FAEN I have no disclosures OBJECTIVES By the end of this presentation, the learner will Discuss etiologies of cyanosis
4/14/2010. Theoretical purpose of fever? Andrea Marmor, MD, MSEd Assistant Clinical Professor, Pediatrics UCSF April 13, 2010
 Andrea Marmor, MD, MSEd Assistant Clinical Professor, Pediatrics UCSF April 13, 2010 Parental touch? Absence of fever more reliable than presence. Axillary and tympanic Vulnerable to environmental and
Andrea Marmor, MD, MSEd Assistant Clinical Professor, Pediatrics UCSF April 13, 2010 Parental touch? Absence of fever more reliable than presence. Axillary and tympanic Vulnerable to environmental and
NEONATAL SEIZURES-PGPYREXIA REVIEW
 NEONATAL SEIZURES-PGPYREXIA REVIEW This is a very important Postgraduate topics will few Q asked in undergraduation also. Lets see them in detail. References: 1.Volpe s Neurology of newborn 2.Nelson s
NEONATAL SEIZURES-PGPYREXIA REVIEW This is a very important Postgraduate topics will few Q asked in undergraduation also. Lets see them in detail. References: 1.Volpe s Neurology of newborn 2.Nelson s
and Science of Home Infant Apnea Monitoring in the 1990s
 C A I A I S S U 1 s and Science of Home Infant Apnea Monitoring in the 1990s Sarah Whitaker, MSN, RNC The use of home apnea monitoring (HAM) continues as an accepted or recommended intervention for infants
C A I A I S S U 1 s and Science of Home Infant Apnea Monitoring in the 1990s Sarah Whitaker, MSN, RNC The use of home apnea monitoring (HAM) continues as an accepted or recommended intervention for infants
Faculty Disclosures. Objectives. Best Pediatric Emergency Medicine Articles for 2012
 Faculty Disclosures Best Pediatric Emergency Medicine Articles for 2012 Evelyn Porter MS, MD I do not have any significant financial interest or other relationships with the manufacturers of any products
Faculty Disclosures Best Pediatric Emergency Medicine Articles for 2012 Evelyn Porter MS, MD I do not have any significant financial interest or other relationships with the manufacturers of any products
GUIDELINE FOR THE MANAGEMENT OF APPARENT LIFE THREATENING EVENTS IN CHILDREN. Paul Davis, Consultant Paediatrician
 GUIDELINE FOR THE MANAGEMENT OF APPARENT LIFE THREATENING EVENTS IN CHILDREN Reference: ALTE Version No: 1 Applicable to Children admitted to the Children s Hospital for Wales, attending the ED or CAU
GUIDELINE FOR THE MANAGEMENT OF APPARENT LIFE THREATENING EVENTS IN CHILDREN Reference: ALTE Version No: 1 Applicable to Children admitted to the Children s Hospital for Wales, attending the ED or CAU
Pediatric Sleep-Disordered Breathing
 Pediatric Sleep-Disordered Breathing OSA in infants and young children is generally characterized by partial, persistent obstruction of the upper airway Continuum Benign primary snoring Upper-airway resistance
Pediatric Sleep-Disordered Breathing OSA in infants and young children is generally characterized by partial, persistent obstruction of the upper airway Continuum Benign primary snoring Upper-airway resistance
OB Well Baby Nursery Admission (Term) [ ] For specialty focused order sets for your patient, refer to: General
![OB Well Baby Nursery Admission (Term) [ ] For specialty focused order sets for your patient, refer to: General OB Well Baby Nursery Admission (Term) [ ] For specialty focused order sets for your patient, refer to: General](/thumbs/85/91909911.jpg) OB Well Baby Nursery Admission (Term) [3040000234] For specialty focused order sets for your patient, refer to: 3040000424 Neonatal Circumcision Order Set 3040000522 Neonatal Herpes Viral Order Set 3040000524
OB Well Baby Nursery Admission (Term) [3040000234] For specialty focused order sets for your patient, refer to: 3040000424 Neonatal Circumcision Order Set 3040000522 Neonatal Herpes Viral Order Set 3040000524
Community-Acquired Pneumonia OBSOLETE 2
 Community-Acquired Pneumonia OBSOLETE 2 Clinical practice guidelines serve as an educational reference, and do not supersede the clinical judgment of the treating physician with respect to appropriate
Community-Acquired Pneumonia OBSOLETE 2 Clinical practice guidelines serve as an educational reference, and do not supersede the clinical judgment of the treating physician with respect to appropriate
Respiratory Failure & Pneumonia Definitions Workgroup
 Respiratory Failure & Pneumonia Definitions Workgroup Purpose To develop standard clinical definitions on select diagnoses & categories to be used consistently across all hospitals in Maryland Definitions
Respiratory Failure & Pneumonia Definitions Workgroup Purpose To develop standard clinical definitions on select diagnoses & categories to be used consistently across all hospitals in Maryland Definitions
A Case of Severe Neonatal Dysphagia: Experience and Reason
 A Case of Severe Neonatal Dysphagia: Experience and Reason The Contemporary Management of Aerodigestive Disease in Children 2 nd Aerodigestive Meeting Vanderbilt University, Nashville, TN Friday, November
A Case of Severe Neonatal Dysphagia: Experience and Reason The Contemporary Management of Aerodigestive Disease in Children 2 nd Aerodigestive Meeting Vanderbilt University, Nashville, TN Friday, November
David Dredge, MD MGH Child Neurology CME Course September 9, 2017
 David Dredge, MD MGH Child Neurology CME Course September 9, 2017 } 25-40,000 children experience their first nonfebrile seizure each year } AAN/CNS guidelines developed in early 2000s and subsequently
David Dredge, MD MGH Child Neurology CME Course September 9, 2017 } 25-40,000 children experience their first nonfebrile seizure each year } AAN/CNS guidelines developed in early 2000s and subsequently
Polysomnography (PSG) (Sleep Studies), Sleep Center
 Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Anna & John J. Sie Center for Down Syndrome Affiliates
 Anna & John J. Sie Center for Down Syndrome Affiliates Types of Medical Research Bench or basic research: done in a controlled laboratory setting using nonhuman subjects Clinical research: answer questions
Anna & John J. Sie Center for Down Syndrome Affiliates Types of Medical Research Bench or basic research: done in a controlled laboratory setting using nonhuman subjects Clinical research: answer questions
An apparent life-threatening event (ALTE) is defined as an episode that is frightening to the observer, characterized by some
 Risk Factors for Extreme Events in Infants Hospitalized for Apparent Life-threatening Events HUSSEIN A. AL-KINDY, MD, JEAN-FRANÇOIS GÉLINAS, BSC, GEORGE HATZAKIS, PHD, AND AURORE CÔTÉ, MD Objective To
Risk Factors for Extreme Events in Infants Hospitalized for Apparent Life-threatening Events HUSSEIN A. AL-KINDY, MD, JEAN-FRANÇOIS GÉLINAS, BSC, GEORGE HATZAKIS, PHD, AND AURORE CÔTÉ, MD Objective To
1. Introduction Algorithm: Infant with Fever 0-28 Days Algorithm: Infant with Fever Days...3
 These guidelines are designed to assist clinicians and are not intended to supplant good clinical judgement or to establish a protocol for all patients with this condition. MANAGEMENT OF FEVER 38 C (100.4F)
These guidelines are designed to assist clinicians and are not intended to supplant good clinical judgement or to establish a protocol for all patients with this condition. MANAGEMENT OF FEVER 38 C (100.4F)
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
PEDIATRIC SLEEP GUIDELINES Version 1.0; Effective
 MedSolutions, Inc. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Requests for patients with atypical symptoms or clinical presentations
MedSolutions, Inc. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Requests for patients with atypical symptoms or clinical presentations
Kristin s Head Trauma Board Questions 11/07/14
 Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Panel Discussion: What s New with DRGs and ICD?
 Panel Discussion: What s New with DRGs and ICD? Moderator: Angie Comfort, RHIA, CDIP, CCS, CCS-P Thilo Koepfer, MD Wilbur Lo, MD, CDIP, CCA Objectives Get updated on the current status of ICD- 11 IR-DRG
Panel Discussion: What s New with DRGs and ICD? Moderator: Angie Comfort, RHIA, CDIP, CCS, CCS-P Thilo Koepfer, MD Wilbur Lo, MD, CDIP, CCA Objectives Get updated on the current status of ICD- 11 IR-DRG
Neonatal Seizure. Dr.Nawar Yahya. Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan. Supervised by:
 Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Apnea in the Newborn
 Apnea in the Newborn Developed by - Lisa Fikac, RNC-NIC, MSN Original Author - Stacey Cashwell, MSN, RN Expiration Date - 1/27/17 This continuing education activity is provided by Cape Fear Valley Health
Apnea in the Newborn Developed by - Lisa Fikac, RNC-NIC, MSN Original Author - Stacey Cashwell, MSN, RN Expiration Date - 1/27/17 This continuing education activity is provided by Cape Fear Valley Health
table of contents pediatric treatment guidelines
 table of contents pediatric treatment guidelines P1 PEDIATRIC PATIENT CARE...70 P2 APPARENT LIFE-THREATENING EVENT (ALTE)...71 P3 CARDIAC ARREST INITIAL CARE AND CPR...72 73 P4 NEONATAL CARE AND RESUSCITATION...74
table of contents pediatric treatment guidelines P1 PEDIATRIC PATIENT CARE...70 P2 APPARENT LIFE-THREATENING EVENT (ALTE)...71 P3 CARDIAC ARREST INITIAL CARE AND CPR...72 73 P4 NEONATAL CARE AND RESUSCITATION...74
Reviewing the recent literature to answer clinical questions: Should I change my practice?
 Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: PALS Revised: 11/2013
 NUMBERS Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: PALS Revised: 11/2013 Weight in kg = 8 + (age in yrs X 2) Neonate (less than 1 month)
NUMBERS Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: PALS Revised: 11/2013 Weight in kg = 8 + (age in yrs X 2) Neonate (less than 1 month)
Management of Acute Exacerbations of COPD
 MiCMRC Educational Webinar Management of Acute Exacerbations of COPD August 22, 2018 MiCMRC Educational Webinar Management of Acute Exacerbations of COPD Expert Presenter: Catherine A. Meldrum PhD RN MS
MiCMRC Educational Webinar Management of Acute Exacerbations of COPD August 22, 2018 MiCMRC Educational Webinar Management of Acute Exacerbations of COPD Expert Presenter: Catherine A. Meldrum PhD RN MS
11/27/2012. Objectives. What is Critical Congenital Heart Disease?
 Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn A presentation of Texas Pulse Oximetry Project: A Joint Educational Initiative of The University of Texas Health Science
Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn A presentation of Texas Pulse Oximetry Project: A Joint Educational Initiative of The University of Texas Health Science
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy
 An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
Diabetic Ketoacidosis: When Sugar Isn t Sweet!!!
 Diabetic Ketoacidosis: When Sugar Isn t Sweet!!! W Ricks Hanna Jr MD Assistant Professor of Pediatrics University of Tennessee Health Science Center LeBonheur Children s Hospital Introduction Diabetes
Diabetic Ketoacidosis: When Sugar Isn t Sweet!!! W Ricks Hanna Jr MD Assistant Professor of Pediatrics University of Tennessee Health Science Center LeBonheur Children s Hospital Introduction Diabetes
MedStar Health considers Continuous Home Pulse Oximetry medically necessary for the following indications:
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.006.MH Continuous Home Pulse Oximetry This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.006.MH Continuous Home Pulse Oximetry This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar
RESPIRATORY EMERGENCIES. Michael Waters MD April 2004
 RESPIRATORY EMERGENCIES Michael Waters MD April 2004 ASTHMA Asthma is a chronic inflammatory disease of the airways with variable or reversible airway obstruction Characterized by increased sensitivity
RESPIRATORY EMERGENCIES Michael Waters MD April 2004 ASTHMA Asthma is a chronic inflammatory disease of the airways with variable or reversible airway obstruction Characterized by increased sensitivity
The 14 th International Fragile X Conference, Garden Grove, CA, Friday, July 18 th, 2014
 Presenters: Sharon Kidd, MPH, PhD; Ave Lachiewicz, MD; Deborah Barbouth, MD; Robin Blitz, MD; Carol Delahunty, MD; Dianne McBrien, MD; Elizabeth Berry-Kravis, MD, PhD The 14 th International Fragile X
Presenters: Sharon Kidd, MPH, PhD; Ave Lachiewicz, MD; Deborah Barbouth, MD; Robin Blitz, MD; Carol Delahunty, MD; Dianne McBrien, MD; Elizabeth Berry-Kravis, MD, PhD The 14 th International Fragile X
Phases of Respiration
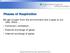 Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
POLICY All patients will be assessed for risk factors associated with OSA prior to any surgical procedures.
 Revised Date: Page: 1 of 7 SCOPE All Pre-Admission Testing (PAT) and Same Day Surgery (SDS) nurses at HRMC. PURPOSE The purpose of this policy is to provide guidelines for identifying surgical patients
Revised Date: Page: 1 of 7 SCOPE All Pre-Admission Testing (PAT) and Same Day Surgery (SDS) nurses at HRMC. PURPOSE The purpose of this policy is to provide guidelines for identifying surgical patients
Disclosures. Background. Definitions. Why Worry about these Infants? Goals. Bacterial infection in the neonate and young infant: a review
 Disclosures Bacterial infection in the neonate and young infant: a review Russell J. McCulloh, MD Med-Peds Infectious Diseases August 8, 2017 I have no financial interests to disclose Funding: Eva and
Disclosures Bacterial infection in the neonate and young infant: a review Russell J. McCulloh, MD Med-Peds Infectious Diseases August 8, 2017 I have no financial interests to disclose Funding: Eva and
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Patient Criteria for Ambulatory/Outpatient Ophthalmic Surgery: What's the real score? Richard Rivers, MD, PhD Dept. Anesthesiology Johns Hopkins
 Patient Criteria for Ambulatory/Outpatient Ophthalmic Surgery: What's the real score? Richard Rivers, MD, PhD Dept. Anesthesiology Johns Hopkins Outpatient surgery Steadily increasing since the 1970 s
Patient Criteria for Ambulatory/Outpatient Ophthalmic Surgery: What's the real score? Richard Rivers, MD, PhD Dept. Anesthesiology Johns Hopkins Outpatient surgery Steadily increasing since the 1970 s
Short Cases M I CHA E L DE RYNCK, M D U N I V ERSITY OF CA LG A RY F E BR UA RY
 Short Cases MICHAEL DERYNCK, MD UNIVERSITY OF CALGARY FEBRUARY 15 2018 Case 1: Beyond Bronchiolitis Presentation 2 month old, term girl Cough and rhinitis, increased work of breathing, wheeze and apnea
Short Cases MICHAEL DERYNCK, MD UNIVERSITY OF CALGARY FEBRUARY 15 2018 Case 1: Beyond Bronchiolitis Presentation 2 month old, term girl Cough and rhinitis, increased work of breathing, wheeze and apnea
Pediatrics. Blue Baby Syndrome (Cyanotic Newborn) and Hyperoxia Test. Definition. See online here
 Pediatrics Blue Baby Syndrome (Cyanotic Newborn) and Hyperoxia Test See online here Blue babies lack sufficient hemoglobin, resulting in the bluish discoloration of tissues, a term referred to as cyanosis.
Pediatrics Blue Baby Syndrome (Cyanotic Newborn) and Hyperoxia Test See online here Blue babies lack sufficient hemoglobin, resulting in the bluish discoloration of tissues, a term referred to as cyanosis.
Family Centered Pediatric Emergency Department Sickle Cell Assessment of Needs and Strengths (FC-Peds-ED-SCANS) Overall Algorithm
 Family Centered Pediatric Emergency Department Sickle Cell Assessment of Needs and Strengths (FC-Peds-ED-SCANS) Overall Algorithm Decision 1: Triage Decision 2: Analgesic Management Decision 3: Diagnostic
Family Centered Pediatric Emergency Department Sickle Cell Assessment of Needs and Strengths (FC-Peds-ED-SCANS) Overall Algorithm Decision 1: Triage Decision 2: Analgesic Management Decision 3: Diagnostic
Status Epilepticus in Children
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
SLEEP DISORDERED BREATHING The Clinical Conditions
 SLEEP DISORDERED BREATHING The Clinical Conditions Robert G. Hooper, M.D. In the previous portion of this paper, the definitions of the respiratory events that are the hallmarks of problems with breathing
SLEEP DISORDERED BREATHING The Clinical Conditions Robert G. Hooper, M.D. In the previous portion of this paper, the definitions of the respiratory events that are the hallmarks of problems with breathing
PEDIATRIC INFECTIOUS DISEASES UPDATE. Neonatal HSV. Recognition, Diagnosis, and Management Coleen Cunningham MD
 Neonatal HSV Recognition, Diagnosis, and Management Coleen Cunningham MD Important questions Who is at risk? When do you test? What tests do you perform? When do you treat? What is appropriate therapy?
Neonatal HSV Recognition, Diagnosis, and Management Coleen Cunningham MD Important questions Who is at risk? When do you test? What tests do you perform? When do you treat? What is appropriate therapy?
Evidence-based Management of Fever in Infants and Young Children
 Evidence-based Management of Fever in Infants and Young Children Shabnam Jain, MD, MPH Associate Professor of Pediatrics Emory University Medical Director for Clinical Effectiveness Objectives Understand
Evidence-based Management of Fever in Infants and Young Children Shabnam Jain, MD, MPH Associate Professor of Pediatrics Emory University Medical Director for Clinical Effectiveness Objectives Understand
Pediatric Thrombectomy
 Pediatric Thrombectomy Translating adult standard of care to pediatric patients DATE: September 16, 2016 PRESENTED BY: Ittai Bushlin MD, PhD and Adrienne McDougal, RN Objectives: Review acute management
Pediatric Thrombectomy Translating adult standard of care to pediatric patients DATE: September 16, 2016 PRESENTED BY: Ittai Bushlin MD, PhD and Adrienne McDougal, RN Objectives: Review acute management
Pediatic Neurology Consult and Referral Guidelines
 Pediatic Neurology Consult and Referral Guidelines Introduction We see children and teens from birth to 18 years. The most common reasons patients are referred to pediatric neurology services include:
Pediatic Neurology Consult and Referral Guidelines Introduction We see children and teens from birth to 18 years. The most common reasons patients are referred to pediatric neurology services include:
KENT STATE UNIVERSITY HEALTH CARE OF CHILDREN Nursing Pediatrics Case Studies: Child Dehydration
 Courtney Wiener 9/9/10 KENT STATE UNIVERSITY HEALTH CARE OF CHILDREN Nursing 30020 - Pediatrics Case Studies: Child Dehydration Introduction: Dehydration can be life threatening to a child since a majority
Courtney Wiener 9/9/10 KENT STATE UNIVERSITY HEALTH CARE OF CHILDREN Nursing 30020 - Pediatrics Case Studies: Child Dehydration Introduction: Dehydration can be life threatening to a child since a majority
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Child-Youth Epilepsy Overview, epidemiology, terminology. Glen Fenton, MD Professor, Child Neurology and Epilepsy University of New Mexico
 Child-Youth Epilepsy Overview, epidemiology, terminology Glen Fenton, MD Professor, Child Neurology and Epilepsy University of New Mexico New onset seizure case An 8-year-old girl has a witnessed seizure
Child-Youth Epilepsy Overview, epidemiology, terminology Glen Fenton, MD Professor, Child Neurology and Epilepsy University of New Mexico New onset seizure case An 8-year-old girl has a witnessed seizure
1/29/2014. Kimberly Johnson Hatchett, MD PGY-4 11/15/13
 Kimberly Johnson Hatchett, MD PGY-4 11/15/13 History of Present Illness 14 month old previously healthy infant boy presented via EMS after being found by his mother to be breathing loudly and non-responsive.
Kimberly Johnson Hatchett, MD PGY-4 11/15/13 History of Present Illness 14 month old previously healthy infant boy presented via EMS after being found by his mother to be breathing loudly and non-responsive.
Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology (scores listed by Appropriate Use rating)
 Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology (scores listed by Appropriate Use rating) Table 1: Appropriate indications (median score 7-9) Indication
Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology (scores listed by Appropriate Use rating) Table 1: Appropriate indications (median score 7-9) Indication
A Clinical Guideline for the use of Intravenous Aminophylline in Acute Severe Asthma in Children
 For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager: Supported by: Assessed and approved by the:
For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager: Supported by: Assessed and approved by the:
Syncope in ED-Risk Stratification Ger McMahon
 Syncope in ED-Risk Stratification Ger McMahon 3-8% of ED presentations increasing with advancing age ED physicians ranked syncope as the 2 nd most common decision making dilemma >50% are admitted @ 75%
Syncope in ED-Risk Stratification Ger McMahon 3-8% of ED presentations increasing with advancing age ED physicians ranked syncope as the 2 nd most common decision making dilemma >50% are admitted @ 75%
Department of Paediatrics Clinical Guideline. Syncope Guideline
 Department of Paediatrics Clinical Guideline Syncope Guideline Definition Transient, self-limited loss of consciousness (TLOC), usually leading to falling. Onset is relatively rapid. Recovery is spontaneous,
Department of Paediatrics Clinical Guideline Syncope Guideline Definition Transient, self-limited loss of consciousness (TLOC), usually leading to falling. Onset is relatively rapid. Recovery is spontaneous,
greater than 10 will be considered ill appearing; a score of 10 or less will be considered well appearing.
 1 Use the Yale Observation Scale to assess whether the patient is ill or well appearing. A score greater than 10 will be considered ill appearing; a score of 10 or less will be considered well appearing.
1 Use the Yale Observation Scale to assess whether the patient is ill or well appearing. A score greater than 10 will be considered ill appearing; a score of 10 or less will be considered well appearing.
Disclaimer. This is a broad survey and cannot cover all differential diagnoses or each condition in thorough detail
 Objectives Pediatric Infections: Differentiating Benign from Serious Eileen Klein, MD, MPH Rashes Infectious vs non-infectious Viral vs bacterial Respiratory and GI illnesses When do you treat When do
Objectives Pediatric Infections: Differentiating Benign from Serious Eileen Klein, MD, MPH Rashes Infectious vs non-infectious Viral vs bacterial Respiratory and GI illnesses When do you treat When do
 NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
What s New in the Pulmonary Medicine Literature. 24 March 2017 Boca Raton Florida
 What s New in the Pulmonary Medicine Literature MARGARET M JOHNSON, MD ASSOCIATE PROFESSOR OF MEDICINE CHAIR, DIVISION OF PULMONARY MEDICINE JOHNSON.MARGARE T2@MAY O.E DU 24 March 2017 Boca Raton Florida
What s New in the Pulmonary Medicine Literature MARGARET M JOHNSON, MD ASSOCIATE PROFESSOR OF MEDICINE CHAIR, DIVISION OF PULMONARY MEDICINE JOHNSON.MARGARE T2@MAY O.E DU 24 March 2017 Boca Raton Florida
Steven Ringer MD PhD April 5, 2011
 Steven Ringer MD PhD April 5, 2011 Disclaimer Mead Johnson sponsors programs such as this to give healthcare professionals access to scientific and educational information provided by experts. The presenter
Steven Ringer MD PhD April 5, 2011 Disclaimer Mead Johnson sponsors programs such as this to give healthcare professionals access to scientific and educational information provided by experts. The presenter
Staging Sepsis for the Emergency Department: Physician
 Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
hour pneumogram and on the incidence of clinically important apnoea. Subjects and methods
 Archives of Disease in Childhood, 1986, 61, 891-895 Effect of caffeine of infancy on pneumogram and apnoea M ANWAR, H MONDESTIN, N MOJICA, R NOVO, M GRAFF, M HIATIT, AND T HEGYI Department of Pediatrics,
Archives of Disease in Childhood, 1986, 61, 891-895 Effect of caffeine of infancy on pneumogram and apnoea M ANWAR, H MONDESTIN, N MOJICA, R NOVO, M GRAFF, M HIATIT, AND T HEGYI Department of Pediatrics,
Neurodevelopmental Risk?
 Normal Newborn During transitional hypoglycemia normal newborns have an enhanced ketogenic response to fasting. Newborn brains have enhanced capability to use ketone bodies for fuel Allows newborns to
Normal Newborn During transitional hypoglycemia normal newborns have an enhanced ketogenic response to fasting. Newborn brains have enhanced capability to use ketone bodies for fuel Allows newborns to
Sample Selection- Vignettes
 Sample Selection- Vignettes Rangaraj Selvarangan, BVSc, PhD, D(ABMM) Professor, UMKC School of Medicine Director, Microbiology, Virology and Molecular Infectious Diseases Laboratory Director, Laboratory
Sample Selection- Vignettes Rangaraj Selvarangan, BVSc, PhD, D(ABMM) Professor, UMKC School of Medicine Director, Microbiology, Virology and Molecular Infectious Diseases Laboratory Director, Laboratory
Reassessment: Neuroimaging in the Emergency Patient Presenting with Seizure
 Reassessment: Neuroimaging in the Emergency Patient Presenting with Seizure This evidence-based report provides clinicians with information to identify which seizure patients in the emergency department
Reassessment: Neuroimaging in the Emergency Patient Presenting with Seizure This evidence-based report provides clinicians with information to identify which seizure patients in the emergency department
Utilizing Automated Adverse Event Detection
 Utilizing Automated Adverse Event Detection David C Stockwell, MD, MBA Executive Director of Improvement Science Medical Director of Patient Safety and Pediatric ICU Children s National Medical Center
Utilizing Automated Adverse Event Detection David C Stockwell, MD, MBA Executive Director of Improvement Science Medical Director of Patient Safety and Pediatric ICU Children s National Medical Center
2/13/13. Ann S. Botash, MD SUNY Upstate Medical University
 Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Bayfield-Ashland Counties EMS Council Pediatric Protocol PP-001 PREHOSPITAL CARE GUIDELINE
 INTRODUCTION: Pediatric emergencies may present a daunting challenge to prehospital care providers for a variety of reasons including: 1. The historical scarceness of primary training materials about the
INTRODUCTION: Pediatric emergencies may present a daunting challenge to prehospital care providers for a variety of reasons including: 1. The historical scarceness of primary training materials about the
