Outcome of donor biliary complications following living donor liver transplantation
|
|
|
- Milo O’Neal’
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Korean J Intern Med 2018;33: Outcome of donor biliary complications following living donor liver transplantation Hyun Young Woo 1, In Seok Lee 2, Jae Hyuck Chang 2, Seung Bae Youn 2, Si Hyun Bae 2, Jong Young Choi 2, Ho Jong Chun 3, Young Kyoung You 4, Dong Goo Kim 4, and Seung Kew Yoon 2 1 Department of Internal Medicine and Medical Research Institute, Pusan National University Hospital, Busan; Departments of 2 Internal Medicine, 3 Radiology, and 4 Surgery, College of Medicine, The Catholic University of Korea, Seoul, Korea Received : July 27, 2017 Revised : October 25, 2017 Accepted : November 10, 2017 Correspondence to In Seok Lee, M.D. Division of Gastroenterology, Department of Internal Medicine, College of Medicine, Seoul St. Mary's Hospital, The Catholic University of Korea, 222 Banpo-daero, Seocho-gu, Seoul 06591, Korea Tel: Fax: isle@catholic.ac.kr Background/Aims: Biliary complications are the most common donor complication following living donor liver transplantation (LDLT). The aim of this study is to investigate the long-term outcomes of biliary complications in right lobe adultto-adult LDLT donors, and to evaluate the efficacy of endoscopic treatment of these donors. Methods: The medical charts of right lobe donors who developed biliary complications between June 2000 and January 2008 were retrospectively reviewed. Results: Of 337 right lobe donors, 49 developed biliary complications, including 36 diagnosed with biliary leakage and 13 with biliary stricture. Multivariate analysis showed that biliary leakage was associated with the number of right lobe bile duct orifices. Sixteen donors, five with leakage and 11 with strictures, underwent endoscopic retrograde cholangiography (ERC). ERC was clinically successful in treating eight of the 11 strictures, one by balloon dilatation and seven by endobiliary stenting. Of the remained three, two were treated by rescue percutaneous biliary drainage and one by conservative care. Of the five patients with leakage, four were successfully treated using endobiliary stents and one with conservative care. In overall, total 35 improved with conservative treatment. All inserted stents were successfully retrieved after a median 264 days (range, 142 to 502) and there were no recurrences of stricture or leakages during a median follow-up of 10.6 years (range, 8 to 15.2). Conclusions: All donors with biliary complications were successfully treated non-surgically, with most improving after endoscopic placement of endobiliary stents and none showing recurrence on long term follow-up. Keywords: Biliary complication; Tissue donors; Cholangiopancreatography, endoscopic retrograde; Liver transplantation INTRODUCTION The first successful adult-to-adult right lobe living donor liver transplantation (LDLT) was performed in Japan in 1994 [1]; since then, this procedure has been widely and increasingly performed. A worldwide shortage of deceased donors has resulted in LDLT becoming a major treatment strategy for end-stage liver diseases, including hepatocellular carcinoma [2-5]. Donor safety is as important as recipient safety and efficacy, resulting in donor ethical issues with regard to this procedure [2-4,6,7]. The morbidity and mortality rates for liver graft donors have been reported to be about 21% and 0.2% to 0.5%, respectively [6]. The most frequent donor com- Copyright 2018 The Korean Association of Internal Medicine This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( by-nc/4.0/) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited. pissn eissn
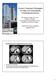
2 The Korean Journal of Internal Medicine Vol. 33, No. 4, July 2018 plications following LDLT are biliary complications. Recent studies have reported that 6% to 9% of donors experience biliary complications following LDLT [6-9] and that these complications are more common in right lobe than in left lobe donors [10,11]. Although most biliary complications are minor or transient and improve with conservative care, some require endoscopic, percutaneous, or surgical treatment and even long-term hospitalization. To date, however, few reports have assessed biliary complications experienced by right lobe donors after partial liver resection [10-13]. The present study describes the long-term outcomes of biliary complications in right lobe LDLT donors in our center, and the efficacy of endoscopic treatment for these complications. METHODS Between June 2000 and January 2008, 394 liver transplantation procedures were performed at Seoul St. Mary Hospital, South Korea. Of those, 341 were LDLT, with four involving left lobe donors and 337 involving right lobe donors. The baseline characteristics of the 337 right lobe donors are shown in Table 1. Their median age was 30 years (range, 16 to 62), and 221 (65.6%) were male. All donors underwent open hepatectomy. Intraoperative cholangiography of the intrahepatic duct (IHD) showed that 234 (69.4%) were classified as type I (i.e., the common hepatic duct was formed by fusion of the right and left hepatic ducts, and the right hepatic duct was formed by fusion of the right anterior segmental duct and right posterior segmental duct); 17 (5.0%) as type II (i.e., the common hepatic duct was formed by the fusion of the right anterior segmental duct, the right posterior segmental duct and left the hepatic duct); 40 (11.9%) as type III (i.e., the right posterior segmental duct drains into the left hepatic duct); and 46 (13.6%) as type IV (i.e., the right posterior segmental duct drains into the common hepatic duct) (Fig. 1). The number of bile duct orifices from the right lobe was defined as the number observed in the stump of the right hepatic duct after right lobe resection. Of the 337 donors, 211 (62.6%), 117 (34.7%), seven (2.1%), and two (0.6%) had one, two, three, and four orifices, respectively (Table 1). Table 1. Baseline characteristics of right lobe donors (n = 337) Characteristic Value Age, yr 30 (16 62) Sex Male 221 (65.6) Female 116 (34.4) Alkaline phosphatase, U/L a 99 (29 310) Total bilirubin, mg/dl a 0.6 ( ) γ-gtp, U/L a 14 ( ) No. of right lobe bile duct orifices (62.6) (34.7) 3 7 (2.1) 4 2 (0.6) Intrahepatic duct anatomy Type I 234 (69.4) Type II 17 (5) Type III 40 (11.9) Type IV 46 (13.6) No. of blood transfusions b 2 (0 9) (54.9) > (45.1) BMI, kg/m ( ) (46.3) > (53.7) Surgery time, min 360 ( ) (50.4) > (49.6) Weight of left lobe, g 511 (288 1,025) (44.8) > (55.2) Postoperative complication Total 92 (27.2) Grade 1 39 (11.5) Grade 2 25 (7.4) Grade 3 28 (8.3) Biliary complication Total 49 (14.5) Bile leakage 36 (10.6) Bile stricture 13 (3.8) Major (grade 3) 14 (4.1) Bile leakage 4 (1.1) Bile stricture 10 (2.9) Values are presented as median (range) or number (%). γ-gtp, gamma-glutamyltransferase; BMI, body mass index. a Before operation. b During operation
3 Woo HY, et al. Donor biliary complications in LDLT Clavien-Dindo grading system [14]. A C Figure 1. Representative cholangiograms showing variations in the anatomy of the intrahepatic ducts of right lobe donors. (A) Type I, the typical anatomy; (B) type II, triple confluence of the right anterior segmental duct, right posterior segmental duct, and left hepatic duct into the common hepatic duct; (C) type III, drainage of the right posterior segmental duct into the left hepatic duct; (D) type IV, drainage of the right posterior segmental duct into the common hepatic duct. Definition of biliary complications Biliary leakage was diagnosed either when an operatively installed drain contained 100 ml/day of bile-containing fluid or when a needle aspirate of intraabdominal fluid included bile juice. If leakage did not resolve following symptomatic care or percutaneous placement of a peritoneal drain, endoscopic retrograde cholangiography (ERC) was performed to confirm the diagnosis and as initial treatment. Biliary stricture was diagnosed when computed tomography or magnetic resonance imaging showed proximal bile duct dilatation and bile duct stenosis, in addition to abnormal liver function test results. The severity of postoperative complications (i.e., biliary complications) was assessed using the five-tier B D Endoscopic procedures All endoscopic procedures were performed after written informed consent was provided. After an overnight fast, ERC was performed using a video duodenoscope (Fujinon ED-450XT5, Fujinon, Saitama, Japan). The leakage site was confirmed using contrast media. Following insertion of a inch guidewire (Jagwire, Boston Scientific, Boston, MA, USA) into the intrahepatic bile duct proximal to the leakage site, an endobiliary plastic stent was introduced over the leakage site, with or without an endoscopic sphincterotomy (EST). Biliary strictures were dilated using a balloon catheter, or an endobiliary plastic stent was inserted into the bile duct proximal to the stricture site with or without EST. The diameter of the endobiliary stent was based on the lumen size of the donor bile duct. Amsterdam-type biliary stents (7 to 11.5 F in diameter, 10 to 16 cm in length; Medi-Globe, Achenmuhle, Germany) were used. ERC was again performed 6 months later in an outpatient clinic, or earlier if acute cholangitis or obstructive jaundice developed or the endoscopic retrograde biliary drainage (ERBD) stent was dislodged. During the follow-up ERC, the previous stent was removed and the degree of improvement in biliary leakage was evaluated. The plastic stent was reinserted if the biliary complication remained or recurred after stent retrieval. ERC was considered clinically successful if clinical, laboratory, and radiological abnormalities improved. To confirm the long-term outcome of donors with biliary complication, we checked each donor s status by telephone calls before this study. This study conformed to the ethical guidelines of the 1975 Declaration of Helsinki, and was approved by our Institutional Review Board (KC17RESI0510). All patients provided informed consent before the treatment. Statistical analysis Descriptive data are expressed as median (range) or proportion. Predictive variables associated with biliary complications were assessed using logistic regression analysis. The evaluated variables were donor sex, age, and body mass index; serum concentrations of aminotransferases, alkaline phosphatase, and total bilirubin; the anatomy of the donor intrahepatic bile duct; the number of bile duct orifices in the right lobe; intraop
4 The Korean Journal of Internal Medicine Vol. 33, No. 4, July 2018 erative transfusions of packed red blood cells; remnant liver size (left lobe); and the duration of donor surgery. All statistical analyses were performed using SPSS version 13.0 software (SPSS Inc., Chicago, IL, USA). RESULTS Of the 337 right lobe donors, 49 (14.5%) developed biliary complications. Table 1 shows overall postoperative complication and biliary complication rates according Table 2. Donor factors associated with the development of biliary complications (leakage or stricture) following liver donation Characteristic No complication Biliary stricture (n = 13) p value a Biliary leakage (n = 36) p value a Age, yr 30 (16 62) 28 (18 51) (16 53) Sex Male 190 (66) 9 (69.2) 22 (61.1) Female 98 (34) 4 (30.8) 14 (38.9) Alkaline phosphatase, U/L c 98.5 (29 310) 83 (52 160) (31 247) Total bilirubin, mg/dl c 0.5 ( ) 0.6 ( ) ( ) γ-gtp, U/L c 14.1 ( ) 15 (7 28.9) ( ) No. of right lobe bile duct orifices (64.6) 6 (46.2) 19 (52.8) 2 98 (34) 6 (46.2) 13 (36.1) 3 4 (1.4) 1 (7.7) 2 (5.6) (5.6) p value b Intrahepatic duct anatomy Type I 206 (71.5) 8 (61.5) 20 (55.6) Type II 15 (5.2) 0 2 (5.6) Type III 30 (10.4) 4 (30.8) 6 (16.7) Type IV 37 (12.8) 1 (7.7) 8 (22.2) No. of blood transfusions d 2 (0 9) 2 (0-5) (0 4) (52.8) 8 (61.5) 25 (69.4) > (46.9) 5 (38.5) 11 (30.6) BMI, kg/m ( ) 25.2 ( ) ( ) (47.2) 3 (23.1) 17 (47.2) > (52.8) 10 (76.9) 19 (52.8) Surgery time, min 360 ( ) 390 ( ) ( ) (51.7) 5 (38.5) 16 (44.4) > (48.3) 8 (61.5) 20 (55.6) Weight of left lobe, g 508 (255 1,025) 541 ( ) ( ) (46.5) 4 (30.8) 13 (36.1) > (53.1) 9 (69.2) 22 (61.1) Values are presented as median (range) or number (%). γ-gtp, gamma-glutamyltransferase; BMI, body mass index. a p value by univariate analysis. b p value by multivariate analysis. c Before operation. d During operation
5 Woo HY, et al. Donor biliary complications in LDLT to the severity of complications. Biliary complications were the most common postoperative complication (49/92, 53.2%), with median time to biliary complications being 13 days (range, 1 to 109) after donation. The median age of the 49 donors was 30 years (range, 16 to 53) and 31 (63%) were male. The presenting symptoms and signs were fever (n = 6, 12%), jaundice (n = 11, 23%), collection of intra-abdominal fluid (n = 13, 28%), elevated liver enzymes (n = 16, 33%), and abdominal pain (n = 2, 4%). Of these 49 donors, 36 were diagnosed with biliary leakage and 13 with biliary strictures, including one patient with concomitant biliary leakage. Univariate analysis of factors potentially associated with biliary complications showed that anatomical IHD type (p = 0.043) and the number of bile duct orifices in the donated right lobe (p = 0.008) was significantly associated with biliary leakage (Table 2). In contrast, no donor factors were associated with biliary stricture. Of the donors with IHD types I, II, III and IV, 8.5% (20/234), 11.8% (2/17), 15% (6/40), and 17.4% (8/46), respectively, developed biliary leakage. Moreover, biliary leakage was observed in 9% (19/211), 11% (13/117), 28.6% Table 3. Clinical outcomes of donors with biliary complications after endoscopic retrograde cholangiography No. Age, yr Sex No. of bile duct orifices Days from LDLT to ERC Type of complication Type of treatment Duration of endobiliary stent placement, day No. of ERC Final state 1 28 Male 3 24 Stricture Stent + Rescue PTBD - 2 Stent and PTBD free Follow-up duration after stent removal, yr 2 51 Female 1 47 Stricture Balloon dilatation b 3 41 Male 2 29 Stricture EST + Stent (10 Fr) Stent free Female 1 40 Stricture EST + Stent (10 Fr) Stent free Male 2 43 Stricture Failed cannulation Conservative treatment 15.2 a b 6 38 Female 1 42 Stricture EST + Stent (10 Fr) Stent free Male 2 20 Stricture Failed cannulation Rescue PTBD - 1 Stent and PTBD free 8 24 Male 2 38 Stricture EST + Stent (10 Fr) Stent free Male 1 21 Stricture EST + Stent (10 Fr) Stent free Male 2 41 Stricture EST + Stent (7 Fr 2) c Stent free Male 2 43 Leakage and stricture 11.2 a EST + Stent (10 Fr) Stent free Male 2 51 Leakage Conservative care b Male 2 22 Leakage EST+ Stent (7 Fr) 502 d 5 Stent free Female 1 10 Leakage Stent (7 Fr) Stent free Male 3 20 Leakage Stent (7 Fr) Stent free Female 3 7 Leakage Stent (7 Fr) Stent free 8.1 LDLT, living donor liver transplantation; ERC, endoscopic retrograde cholangiography; PTBD, percutaneous transhepatic biliary drainage, EST, endoscopic sphincterotomy. a From removal of PTBD to last follow-up. b From the day of ERC to last follow-up. c Two endobiliary stents (7 Fr) were inserted. d Total duration of endobiliary stent placement
6 The Korean Journal of Internal Medicine Vol. 33, No. 4, July 2018 (2/7), and 100% (2/2), of the donors with one, two, three, and four biliary orifices, respectively. Anatomical IHD type was significantly associated with the number of bile duct orifices in the right lobe (p = 0.001), with multiple biliary orifices more frequently observed in donors with types II (14/17, 82.4%), III (38/40, 95%), and IV (45/46, 97.8%) than type I (29/234, 12.4%) IHD. Three or more biliary orifices were detected only in donors with types 1 Balloon dilatation 9 ERC 1 PTBD PTBD-free 8 Stent 11 Biliary stricture 7 Stent-free 1 Rescue PTBD PTBD-free 2 Failed ERC 1 Conservative care Figure 2. Flow diagram of outcomes in donors who underwent endoscopic retrograde cholangiography (ERC) due to biliary stricture following right lobe donation. PTBD, percutaneous transhepatic biliary drainage. II (1/17, 5.9%), III (5/40, 12.5%), and IV (3/46, 6.5%). Multivariate analysis found that the number of bile duct orifices was the only factor independently associated with biliary leakage (p = 0.010). Of the 49 donors with biliary complications, 16 donors, including five with leakage and 11 with strictures, underwent ERC; their clinical features and treatment outcomes are shown in Table 3. The median period between LDLT and ERC was 31.5 days (range, 7 to 51). The median number of ERC per donor was 2 (range, 1 to 5). None of these patients experienced any serious ERC-related complications, such as pancreatitis, bleeding, or infection. ERC was technically successful in nine of the 11 donors with biliary strictures, including one with concomitant leakage, but unsuccessful in two patients. Of the latter, one improved without further management and the other underwent percutaneous biliary drainage due to aggravating jaundice. Of the nine donors who underwent technically successful ERC, one underwent balloon dilation alone, whereas the other eight underwent insertion of an endobiliary stent without ballooning, with (n = 7) or without (n = 1) EST. Of the nine donors with strictures who underwent technically successful ERC procedures, eight experienced successful clinical outcomes, whereas one (Patient 1) required percutaneous biliary drainage because of continuing elevated biliru- A B Figure 3. Case of a 19-year-old male donor who presented with biliary stricture (Patient 9). (A) Endoscopic retrograde cholangiography (ERC) showing a common hepatic duct stricture (arrows). (B) Insertion of an endobiliary stent across the stricture. (C) ERC performed 264 days after stenting showing stricture improvement. C 710
7 Woo HY, et al. Donor biliary complications in LDLT bin concentration and fever (Fig. 2). Drainage was successful in treating fever and jaundice in this patient, allowing drain removal 1 month later. Two weeks later, however, this patient again developed fever and jaundice, and a follow-up ERC showed that the endobiliary stent had migrated towards the smaller intrahepatic bile duct. The stent was removed, with no further recurrence of biliary complications for 15.2 years. Endobiliary stents were removed from the other seven patients removed No leakage 1 Conservative care 5 Biliary leakage 5 ERC 4 Stent 4 Stent-free 1 CBD stone and removal Figure 4. Flow diagram of outcomes in donors who underwent endoscopic retrograde cholangiography (ERC) due to biliary leakage following right lobe donation. CBD, common bile duct. after a median 254 days (range, 142 to 385), with follow-up ERC showing stricture improvement and no evidence of leakage (Fig. 3). None of these patients experienced recurrence of stricture or leakage during a median follow-up of 11.2 years (range, 9.4 to 15.2). Of the five donors who underwent ERC due to leakage, four underwent endoscopic biliary drainage using a biliary stent. The remaining patient (Patient 12) had a subphrenic biloma and was treated conservatively because bile leakage was not evident on ERC (Fig. 4). The most frequent site of leakage was the anastomosis site of the resected right hepatic duct. The inserted endobiliary stents were retrieved at a median 205 days (range, 148 to 336) following ERC (Fig. 5). Follow-up ERC showed no evidence of leakage in any patient. One patient (Patient 13), however, developed obstructive jaundice, with a stone found in the common bile duct 15 days after stent removal. This patient underwent basket stone removal, balloon dilatation of a suspicious biliary stricture, and endobiliary stent reinsertion. The stent was removed 6 months later, with ERC showing no evidence of a stone or stricture in the bile duct. Following stent removal, these five patients with leakage have shown no recurrence of stricture or leakage for a median 8.6 years (range, 8 to 14.2). A B Figure 5. Case of a 26-year-old female donor who presented with bile leakage through the drain (Patient 14). (A) Endoscopic retrograde cholangiography (ERC) showing bile leakage from the resected right hepatic duct (arrow). (B) Insertion of an endobiliary stent over the leakage site. (C) Follow-up ERC showing improvement in biliary leakage and no other complications. C 711
8 The Korean Journal of Internal Medicine Vol. 33, No. 4, July 2018 Thirty-five donors, 32 with leakage and three with strictures, showed improvements following conservative treatment, with none of these patients experiencing recurrence during a median follow-up of 12.8 years (range, 8.9 to 16.3). DISCUSSION Although right liver LDLT is regarded as the primary treatment for selected adult patients with end-stage liver disease, concerns have been raised about donor safety. LDLT donors can experience various complications, with biliary complications being the most frequent. However, a multicenter survey of several recent large scale studies showed that donor hepatectomy can be performed successfully, with minimal and easily controlled complications, by using a meticulous and well-standardized technique [15,16]. In contrast to largescale studies, single center studies like ours have several advantages. First, specific complications such as biliary complications could be handled in a more detailed and standardized fashion. Second, unexpected intraoperative factors and/or pathologic factors may be identified as important predictors during the investigation. Therefore, this study is one of few focusing on the clinical course of biliary complications and the outcomes of endoscopic management of these complications in LDLT donors at a single center. The present study found that the overall postoperative complication rate was 27.2%. More than half of these were biliary complications (14.5%, 49/337), with 10.6% (36/337) of patients experiencing biliary leakage and 3.9% (13/337) having biliary strictures, including one donor who developed a stricture after resolution of the leakage. Donor morbidity rates associated with right hepatectomy for LDLT have been reported to range from 0% to 67%, with an average incidence of 31% [17]. The overall rate of biliary complications in LDLT donors has been reported to range from 6% to 9%, but the incidence has been found to vary among studies from 1.0% to 11.1% [6-9]. These variations in incidence rate may be due to differences in surgical skills or inconsistent definitions of complications and their grades. The incidence of biliary complications was somewhat higher in the present study than in previous studies. This higher incidence was likely due to our inclusion of only right lobe donors, who have been reported to have a higher rate of biliary complications, about 9% to 11% [10,11]. However, recent large-scale studies reported comparable outcomes in right lobe and left lobe donors [18-20]. These similar outcomes were likely due to strict donor selection and cumulative experience with surgical procedures and perioperative management [18-20]. We found that most biliary complications occurred during the early postoperative period. Biliary leakage has been found to occur more frequently in earlier than in late phase, with most of these patients showing improvements with conservative care. Biliary strictures develop later, with most requiring specific interventional treatment [10,21,22]. In this study, 88.8% of patients with biliary leakages and 23% of patients with biliary strictures showed improvement following conservative treatment, findings consistent with those of previous reports [9,10,12,13,21,22]. All patients with biliary complications requiring ERC improved without requiring surgical management. ERC was technically successful in 81% of patients with strictures and 100% of those with leakage, and endobiliary stent insertion was clinically successful in 72.7% and 100%, respectively, with the remaining donors responding to percutaneous treatment. Although the management of biliary leakage varies among studies, the approach to stricture is the same, endobiliary stent insertion. The technical and clinical success rates of ERC with stent insertion for stricture in this study were comparable to those of previous studies, although the numbers of events were very small [10,21,23]. In the present study, endobiliary stents were used to treat biliary leakage as well as strictures. Potential treatments for leakage include sphincterotomy, endoscopic nasobiliary drainage (ENBD), endobiliary stent drainage with or without sphincterotomy, percutaneous biliary drainage, and surgery [22,24,25]. Bile leakage after right hepatic duct resection during donor hepatectomy that does not improve with conservative care can be treated initially by endoscopic methods. Endoscopic treatment can reduce the bile duct-duodenal pressure gradient, bridge the defect at the leak site, divert bile away from the leak site, and prevent stricture formation during healing [25]. ENBD can provide visual confirmation of biliary healing using repeat cholangiography and can be easily removed. Therefore, temporary use of ENBD 712
9 Woo HY, et al. Donor biliary complications in LDLT is a safe and feasible method of following up leakage in patients with minor biliary leakage during a relatively short admission period. However, potential drawbacks of ENBD include patient discomfort, displacement, and electrolyte imbalance, drawbacks not observed following endobiliary stent insertion. Therefore, because of possible patient discomfort and the need for longer hospitalization, none of the donors in this study underwent ENBD for leakage. Rather, drainage with endobiliary stents was tried in patients who did not improve with conservative care. Biliary leakage is a risk factor for stricture, or is often associated with stricture [24,26,27]. Although prior leakage could not be confirmed in most of our patients with stricture, one patient with stricture had concomitant biliary leakage. Endobiliary stent insertion during the initial ERC may be more effective than ENBD for preventing stricture following leakage, as the stent could be maintained in the biliary system for a longer time. Several previous studies of endoscopic management of donor biliary complications reported that biliary leakage was treated with ENBD or ERBD alone, or ENBD followed by endobiliary stent insertion [10,12,21]. The optimal strategy for treating patients with biliary leakage has not yet been determined. Moreover, these strategies are difficult to compare because the number of events in each study was very small. Further studies are warranted. Some patients who failed ERC or did not show improvement with ERC were successfully managed with percutaneous drainage, suggesting that percutaneous transhepatic treatment is effective for treating bile leaks when endoscopic treatments have failed or are contraindicated [28-30]. Furthermore, percutaneous transhepatic biliary drainage (PTBD) was useful for treating long lasting combined complications. These include longterm maintenance of a large-profile catheter (12- to 14- Fr) through the percutaneous transhepatic tract during the indwelling period of the PTBD catheter. In contrast, endoscopic treatment requires cannulation of the ampulla of Vater during every procedural session, making the endoscopic approach more time-consuming and difficult. We also investigated donor factors predictive of biliary complications. Multivariate analysis showed that the number of right lobe biliary orifices was associated with the development of biliary leakage. In addition, the number of biliary orifices was closely associated with IHD anatomy. Right lobe donors have been reported to be more susceptible to leakage than left lobe donors because the biliary tract anatomy is more complex in the right lobe [7,10,22]. About half of right-lobe grafts have multiple biliary orifices [22], whereas left-lobe grafts usually have a single orifice. Furthermore, right lobe grafts require resection of the right hepatic duct closer to the bifurcation of the right and left hepatic ducts than do left hepatic ducts in left lobe grafts because the anterior and posterior segmental branches of the right hepatic duct often converge just proximal to the bifurcation [10,12,22]. Therefore, right lobe donors with larger biliary stumps due to multiple biliary orifices would be more susceptible to biliary complications, especially leakage, than donors with fewer biliary orifices. This study had several limitations, including its retrospective design and the relatively small number of patients who underwent ERC due to biliary complications. However, only about 10% of LDLT donors experience biliary complications, with each case representing a different clinical situation. Moreover, most donors with biliary complications improve with conservative management. Therefore, comparative prospective studies that include all clinical situations would be very difficult to perform. From a practical perspective, the results of this study may provide valuable information about the actual clinical course of biliary complications in liver donors. In summary, the present study found that all donors with biliary complications were successfully treated using non-surgical management, and that most donors improved with endoscopic endobiliary stent insertion without long-term recurrence. These results suggest that endoscopic methods are useful and effective as a first option for treating right lobe LDLT donors who experience biliary complications that do not improve with conservative management. KEY MESSAGE 1. The most frequent donor complications following living donor liver transplantation (LDLT) are biliary complications. 2. All donors with biliary complications were 713
10 The Korean Journal of Internal Medicine Vol. 33, No. 4, July 2018 successfully treated non-surgically, with most improving after endoscopic placement of endobiliary stents and none showing recurrence on long term follow-up. 3. Endoscopic methods are useful and effective as first options for long-term treatment of right lobe LDLT donors who experience biliary complications that do not improve with conservative care. Conflict of interest No potential conflict of interest relevant to this article was reported. Acknowledgments This research was supported by the Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education (NRF-2017R1C1B ) and by clinical research grant from Pusan National University Hospital in REFERENCES 1. Yamaoka Y, Washida M, Honda K, et al. Liver transplantation using a right lobe graft from a living related donor. Transplantation 1994;57: Tanaka K, Yamada T. Living donor liver transplantation in Japan and Kyoto University: what can we learn? J Hepatol 2005;42: Lo CM. Complications and long-term outcome of living liver donors: a survey of 1,508 cases in five Asian centers. Transplantation 2003;75(3 Suppl):S12-S Trotter JF, Wachs M, Everson GT, Kam I. Adult-to-adult transplantation of the right hepatic lobe from a living donor. N Engl J Med 2002;346: Trotter JF. Living donor liver transplantation: is the hype over? J Hepatol 2005;42: Shiffman ML, Brown RS Jr, Olthoff KM, et al. Living donor liver transplantation: summary of a conference at The National Institutes of Health. Liver Transpl 2002;8: Brown RS Jr, Russo MW, Lai M, et al. A survey of liver transplantation from living adult donors in the United States. N Engl J Med 2003;348: Humar A. Donor and recipient outcomes after adult living donor liver transplantation. Liver Transpl 2003;9(10 Suppl 2):S42-S Ghobrial RM, Freise CE, Trotter JF, et al. Donor morbidity after living donation for liver transplantation. Gastroenterology 2008;135: Shio S, Yazumi S, Ogawa K, et al. Biliary complications in donors for living donor liver transplantation. Am J Gastroenterol 2008;103: Gruttadauria S, Marsh JW, Vizzini GB, et al. Analysis of surgical and perioperative complications in seventy-five right hepatectomies for living donor liver transplantation. World J Gastroenterol 2008;14: Hasegawa K, Yazumi S, Egawa H, et al. Endoscopic management of postoperative biliary complications in donors for living donor liver transplantation. Clin Gastroenterol Hepatol 2003;1: Fujita S, Kim ID, Uryuhara K, et al. Hepatic grafts from live donors: donor morbidity for 470 cases of live donation. Transpl Int 2000;13: Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 2004;240: Lauterio A, Di Sandro S, Gruttadauria S, et al. Donor safety in living donor liver donation: an Italian multicenter survey. Liver Transpl 2017;23: Lee JG, Lee KW, Kwon CHD, et al. Donor safety in living donor liver transplantation: the Korean organ transplantation registry study. Liver Transpl 2017;23: Beavers KL, Sandler RS, Shrestha R. Donor morbidity associated with right lobectomy for living donor liver transplantation to adult recipients: a systematic review. Liver Transpl 2002;8: Iida T, Ogura Y, Oike F, et al. Surgery-related morbidity in living donors for liver transplantation. Transplantation 2010;89: Abecassis MM, Fisher RA, Olthoff KM, et al. Complications of living donor hepatic lobectomy: a comprehensive report. Am J Transplant 2012;12: Uchiyama H, Shirabe K, Nakagawara H, et al. Revisiting the safety of living liver donors by reassessing 441 donor hepatectomies: is a larger hepatectomy complication-prone? Am J Transplant 2014;14: Yuan Y, Gotoh M. Biliary complications in living liver donors. Surg Today 2010;40:
11 Woo HY, et al. Donor biliary complications in LDLT 22. Yazumi S, Chiba T. Biliary complications after a rightlobe living donor liver transplantation. J Gastroenterol 2005;40: Taketomi A, Kayashima H, Soejima Y, et al. Donor risk in adult-to-adult living donor liver transplantation: impact of left lobe graft. Transplantation 2009;87: Kasahara M, Egawa H, Takada Y, et al. Biliary reconstruction in right lobe living-donor liver transplantation: comparison of different techniques in 321 recipients. Ann Surg 2006;243: Agarwal N, Sharma BC, Garg S, Kumar R, Sarin SK. Endoscopic management of postoperative bile leaks. Hepatobiliary Pancreat Dis Int 2006;5: Ostroff JW. Post-transplant biliary problems. Gastrointest Endosc Clin N Am 2001;11: Verdonk RC, Buis CI, Porte RJ, et al. Anastomotic biliary strictures after liver transplantation: causes and consequences. Liver Transpl 2006;12: Hwang S, Lee SG, Sung KB, et al. Long-term incidence, risk factors, and management of biliary complications after adult living donor liver transplantation. Liver Transpl 2006;12: Amesur NB, Zajko AB. Interventional radiology in liver transplantation. Liver Transpl 2006;12: Chang JM, Lee JM, Suh KS, et al. Biliary complications in living donor liver transplantation: imaging findings and the roles of interventional procedures. Cardiovasc Intervent Radiol 2005;28:
INTRODUCTION. Key Words: Biliary stenting; Biliary stricture; Duct-toduct biliary anastomosis; Endoscopic retrograde cholangiography; original article
 Gut and Liver, Vol. 4, No. 2, June 2010, pp. 226-233 original article Biliary Stricture after Adult Right-Lobe Living-Donor Liver Transplantation with Duct-to-Duct Anastomosis: Long-Term Outcome and Its
Gut and Liver, Vol. 4, No. 2, June 2010, pp. 226-233 original article Biliary Stricture after Adult Right-Lobe Living-Donor Liver Transplantation with Duct-to-Duct Anastomosis: Long-Term Outcome and Its
Biliary Anatomy in Living-related Liver Transplantation
 The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
Endoscopic Management of Postoperative Biliary Complications in Donors for Living Donor Liver Transplantation
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2003;1:183 188 Endoscopic Management of Postoperative Biliary Complications in Donors for Living Donor Liver Transplantation KAZUNORI HASEGAWA,* SHUJIRO YAZUMI,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2003;1:183 188 Endoscopic Management of Postoperative Biliary Complications in Donors for Living Donor Liver Transplantation KAZUNORI HASEGAWA,* SHUJIRO YAZUMI,*
Usefulness of the Rendezvous Technique for Biliary Stricture after Adult Right-Lobe Living-Donor Liver Transplantation with Duct-To-Duct Anastomosis
 Gut and Liver, Vol. 4, No. 1, March 2010, pp. 68-75 original article Usefulness of the Rendezvous Technique for Biliary Stricture after Adult Right-Lobe Living-Donor Liver Transplantation with Duct-To-Duct
Gut and Liver, Vol. 4, No. 1, March 2010, pp. 68-75 original article Usefulness of the Rendezvous Technique for Biliary Stricture after Adult Right-Lobe Living-Donor Liver Transplantation with Duct-To-Duct
Donor Safety in Living Donor Liver Transplantation: The Korean Organ Transplantation Registry Study
 ORIGINAL ARTICLE LEE ET AL. Donor Safety in Living Donor Liver Transplantation: The Korean Organ Transplantation Registry Study Jae Geun Lee, 1 Kwang-Woong Lee, 2 Choon Hyuck David Kwon, 3 Chong Woo Chu,
ORIGINAL ARTICLE LEE ET AL. Donor Safety in Living Donor Liver Transplantation: The Korean Organ Transplantation Registry Study Jae Geun Lee, 1 Kwang-Woong Lee, 2 Choon Hyuck David Kwon, 3 Chong Woo Chu,
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Since the first description of living-donor liver transplantation
 CLINICAL AND TRANSLATIONAL RESEARCH Endoscopic Management of Biliary Complications After Adult Living-Donor Versus Deceased-Donor Liver Transplantation Carlos Macías Gómez, 1,4 Jean-Marc Dumonceau, 2 Mariano
CLINICAL AND TRANSLATIONAL RESEARCH Endoscopic Management of Biliary Complications After Adult Living-Donor Versus Deceased-Donor Liver Transplantation Carlos Macías Gómez, 1,4 Jean-Marc Dumonceau, 2 Mariano
The authors have declared no conflicts of interest.
 Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Dual Catheter Placement Technique for Treatment of Biliary Anastomotic Strictures After Liver Transplantation
 LIVER TRANSPLANTATION 17:159-166, 2011 ORIGINAL ARTICLE Dual Catheter Placement Technique for Treatment of Biliary Anastomotic Strictures After Liver Transplantation Dong Il Gwon, 1 Kyu-Bo Sung, 1 Gi-Young
LIVER TRANSPLANTATION 17:159-166, 2011 ORIGINAL ARTICLE Dual Catheter Placement Technique for Treatment of Biliary Anastomotic Strictures After Liver Transplantation Dong Il Gwon, 1 Kyu-Bo Sung, 1 Gi-Young
Endoscopic Management of the Iatrogenic CBD Injury
 The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
of bile leakage after liver resecti
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Percutaneous embolization with n-bu of bile leakage after liver resecti Kuroki, Tamotsu; Kitasato, Amane; T Hiroaki; Taniguchi, Ken; Maeda, Shi
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Percutaneous embolization with n-bu of bile leakage after liver resecti Kuroki, Tamotsu; Kitasato, Amane; T Hiroaki; Taniguchi, Ken; Maeda, Shi
Bronchobiliary fistula treated with histoacryl embolization under bronchoscopic guidance: A case report
 Respiratory Medicine CME (2008) 1, 164 168 respiratory MEDICINE CME CASE REPORT Bronchobiliary fistula treated with histoacryl embolization under bronchoscopic guidance: A case report Jung Hyun Kim a,
Respiratory Medicine CME (2008) 1, 164 168 respiratory MEDICINE CME CASE REPORT Bronchobiliary fistula treated with histoacryl embolization under bronchoscopic guidance: A case report Jung Hyun Kim a,
Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy
 LETTERS FROM THE FRONTLINE Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy TO THE EDITOR: Despite advances
LETTERS FROM THE FRONTLINE Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy TO THE EDITOR: Despite advances
Obstructive jaundice due to a blood clot after ERCP: a case report and review of the literature
 Zhu et al. BMC Gastroenterology (2018) 18:163 https://doi.org/10.1186/s12876-018-0898-4 CASE REPORT Open Access Obstructive jaundice due to a blood clot after ERCP: a case report and review of the literature
Zhu et al. BMC Gastroenterology (2018) 18:163 https://doi.org/10.1186/s12876-018-0898-4 CASE REPORT Open Access Obstructive jaundice due to a blood clot after ERCP: a case report and review of the literature
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (9), Page
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (9), Page 5153-5160 Role of Interventional Radiology in the Management of Postoperative Biliary Complications 1 Hana Hamdy Nasif, 1 Mennatallah
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (9), Page 5153-5160 Role of Interventional Radiology in the Management of Postoperative Biliary Complications 1 Hana Hamdy Nasif, 1 Mennatallah
Naoyuki Toyota, Tadahiro Takada, Hodaka Amano, Masahiro Yoshida, Fumihiko Miura, and Keita Wada
 J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
담낭절제술후발생한미리찌증후군의내시경적치료 1 예
 Case Report The Korean Journal of Pancreas and Biliary Tract 2014;19:199-203 http://dx.doi.org/10.15279/kpba.2014.19.4.199 pissn 1976-3573 eissn 2288-0941 담낭절제술후발생한미리찌증후군의내시경적치료 1 예 인하대학교의학전문대학원내과학교실 이정민
Case Report The Korean Journal of Pancreas and Biliary Tract 2014;19:199-203 http://dx.doi.org/10.15279/kpba.2014.19.4.199 pissn 1976-3573 eissn 2288-0941 담낭절제술후발생한미리찌증후군의내시경적치료 1 예 인하대학교의학전문대학원내과학교실 이정민
The role of cholangiography with t-tube in the liver transplantation
 The role of cholangiography with t-tube in the liver transplantation Poster No.: C-0362 Congress: ECR 2012 Type: Educational Exhibit Authors: S. Magalhães, I. Ferreira, A. B. Ramos, F. Reis, M. Ribeiro
The role of cholangiography with t-tube in the liver transplantation Poster No.: C-0362 Congress: ECR 2012 Type: Educational Exhibit Authors: S. Magalhães, I. Ferreira, A. B. Ramos, F. Reis, M. Ribeiro
Abdominal Pain and Abnormal Liver Tests After Orthotopic Liver Transplantation
 Abdominal Pain and Abnormal Liver Tests After Orthotopic Liver Transplantation M. Muñoz-Navas 1, J. Baillie 2 1 University of Pamplona, Pamplona, Spain [Guest Discussant] 2 Dept. of Medicine, Duke University
Abdominal Pain and Abnormal Liver Tests After Orthotopic Liver Transplantation M. Muñoz-Navas 1, J. Baillie 2 1 University of Pamplona, Pamplona, Spain [Guest Discussant] 2 Dept. of Medicine, Duke University
Principles of ERCP: papilla cannulation, indications/contraindications and risks. Dr. med. Henrik Csaba Horváth PhD
 Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Current status of hepatic surgery in Korea
 Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria Ankit Chhoda
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria Ankit Chhoda
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options
 Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Role of Therapeutic Endoscopy in Hepatic Hydatid Disease after Surgical Intervention: Case Report
 ISPUB.COM The Internet Journal of Gastroenterology Volume 10 Number 2 Role of Therapeutic Endoscopy in Hepatic Hydatid Disease after Surgical Intervention: Case Report H Ono, M Okabe, T Kimura, M Kawakami,
ISPUB.COM The Internet Journal of Gastroenterology Volume 10 Number 2 Role of Therapeutic Endoscopy in Hepatic Hydatid Disease after Surgical Intervention: Case Report H Ono, M Okabe, T Kimura, M Kawakami,
Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter?
 Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter? Q. Lina Hu, MD; Jason B. Liu, MD, MS; Ryan J. Ellis, MD, MS; Jessica Y. Liu, MD, MS; Anthony
Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter? Q. Lina Hu, MD; Jason B. Liu, MD, MS; Ryan J. Ellis, MD, MS; Jessica Y. Liu, MD, MS; Anthony
Laparoscopic left hepatectomy in patients with intrahepatic duct stones and recurrent pyogenic cholangitis
 Korean J Hepatobiliary Pancreat Surg 212;16:15-19 Original Article Laparoscopic left hepatectomy in patients with intrahepatic duct stones and recurrent pyogenic cholangitis Sunjong Han, Insang Song, and
Korean J Hepatobiliary Pancreat Surg 212;16:15-19 Original Article Laparoscopic left hepatectomy in patients with intrahepatic duct stones and recurrent pyogenic cholangitis Sunjong Han, Insang Song, and
Percutaneous Transhepatic Release of an Impacted Lithotripter Basket and Its Fractured Traction Wire Using a Goose-Neck Snare: a Case Report
 Case Report DOI: 10.3348/kjr.2011.12.2.247 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(2):247-251 Percutaneous Transhepatic Release of an Impacted Lithotripter Basket and Its Fractured Traction
Case Report DOI: 10.3348/kjr.2011.12.2.247 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(2):247-251 Percutaneous Transhepatic Release of an Impacted Lithotripter Basket and Its Fractured Traction
STRICTURES OF THE BILE DUCTS Session No.: 5. Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy
 STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
Mirizzi syndrome with an unusual type of biliobiliary fistula a case report
 Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Bile Duct Injury during Lap Chole. Bile Duct Injury during cholecystectomy TOPICS. 1. Prevalence, mechanisms, prevention and diagnosis
 Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Original Policy Date 12:2013
 MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
Magnetic compression anastomosis is useful in biliary anastomotic strictures after living donor liver transplantation
 Magnetic compression anastomosis is useful in biliary anastomotic strictures after living donor liver transplantation Sung Ill Jang Department of Medicine, The Graduate School, Yonsei University Magnetic
Magnetic compression anastomosis is useful in biliary anastomotic strictures after living donor liver transplantation Sung Ill Jang Department of Medicine, The Graduate School, Yonsei University Magnetic
Endoscopic Papillary Balloon Dilation with Large Balloon after Limited Sphincterotomy for Retrieval of Choledocholithiasis
 Yonsei Medical Journal Vol. 47, No. 6, pp. 805-810, 2006 Endoscopic Papillary Balloon Dilation with Large Balloon after Limited Sphincterotomy for Retrieval of Choledocholithiasis Seungmin Bang, Myoung
Yonsei Medical Journal Vol. 47, No. 6, pp. 805-810, 2006 Endoscopic Papillary Balloon Dilation with Large Balloon after Limited Sphincterotomy for Retrieval of Choledocholithiasis Seungmin Bang, Myoung
Efficacy of endoscopic and percutaneous treatments for biliary complications after cadaveric and living donor liver transplantation
 Efficacy of endoscopic and percutaneous treatments for biliary complications after cadaveric and living donor liver transplantation Ju Sang Park, MD, Myung-Hwan Kim, MD, Sung Koo Lee, MD, Dong Wan Seo,
Efficacy of endoscopic and percutaneous treatments for biliary complications after cadaveric and living donor liver transplantation Ju Sang Park, MD, Myung-Hwan Kim, MD, Sung Koo Lee, MD, Dong Wan Seo,
KAHBPS-O-PL-01 KAHBPS-O-PL-02
 KAHBPS-O-PL-01 Proposal of future remnant liver-indocyanine green clearance rate for risk assessment of major hepatectomy - What is its cutoff? Department of Surgery, Asan Medical Center, University of
KAHBPS-O-PL-01 Proposal of future remnant liver-indocyanine green clearance rate for risk assessment of major hepatectomy - What is its cutoff? Department of Surgery, Asan Medical Center, University of
Post Laparoscopic Cholecystectomy Biloma in a Child Managed by Endoscopic Retrograde Cholangio-Pancreatography and Stenting: A Case Report
 pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2016.19.4.281 Pediatr Gastroenterol Hepatol Nutr 2016 December 19(4):281-285 Case Report PGHN Post Laparoscopic Cholecystectomy Biloma in
pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2016.19.4.281 Pediatr Gastroenterol Hepatol Nutr 2016 December 19(4):281-285 Case Report PGHN Post Laparoscopic Cholecystectomy Biloma in
Percutaneous Transhepatic Treatment of Hepaticojejunal Anastomotic Biliary Strictures After Living Donor Liver Transplantation
 LIVER TRANSPLANTATION 14:1323-1332, 2008 ORIGINAL ARTICLE Percutaneous Transhepatic Treatment of Hepaticojejunal Anastomotic Biliary Strictures After Living Donor Liver Transplantation Gi-Young Ko, 1 Kyu-Bo
LIVER TRANSPLANTATION 14:1323-1332, 2008 ORIGINAL ARTICLE Percutaneous Transhepatic Treatment of Hepaticojejunal Anastomotic Biliary Strictures After Living Donor Liver Transplantation Gi-Young Ko, 1 Kyu-Bo
Jennifer Hsieh 1, Amar Thosani 1, Matthew Grunwald 2, Satish Nagula 1, Juan Carlos Bucobo 1, Jonathan M. Buscaglia 1. Introduction
 How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
Gum O Jung and Dong Eun Park. Department of Surgery, Wonkwang University Hospital, Wonkwang University School of Medicine, Iksan, Korea
 Korean J Hepatobiliary Pancreat Surg 2012;16:110-114 Case Report Successful percutaneous management of bronchobiliary fistula after radiofrequency ablation of metastatic cholangiocarcinoma in a patient
Korean J Hepatobiliary Pancreat Surg 2012;16:110-114 Case Report Successful percutaneous management of bronchobiliary fistula after radiofrequency ablation of metastatic cholangiocarcinoma in a patient
Laparoscopic resection of hilar cholangiocarcinoma
 TECHNICAL ADVANCE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2015.89.4.228 Annals of Surgical Treatment and Research Laparoscopic resection of hilar cholangiocarcinoma Woohyung Lee,
TECHNICAL ADVANCE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2015.89.4.228 Annals of Surgical Treatment and Research Laparoscopic resection of hilar cholangiocarcinoma Woohyung Lee,
Clinical features of gallstone impaction at the ampulla of Vater and the effectiveness of endoscopic biliary drainage without papillotomy
 E806 THIEME Clinical features of gallstone impaction at the ampulla of Vater and the effectiveness of endoscopic biliary drainage without Authors Yuichi Takano 1, Masatsugu Nagahama 1, Naotaka Maruoka
E806 THIEME Clinical features of gallstone impaction at the ampulla of Vater and the effectiveness of endoscopic biliary drainage without Authors Yuichi Takano 1, Masatsugu Nagahama 1, Naotaka Maruoka
Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy
 Korean J Hepatobiliary Pancreat Surg 2011;15:152-156 Original Article Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy Suzy Kim 1,#, Kyubo
Korean J Hepatobiliary Pancreat Surg 2011;15:152-156 Original Article Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy Suzy Kim 1,#, Kyubo
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico
 Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
EGIS BILIARY STENT. 1. Features & Benefits 2. Ordering information 3. References
 EGIS BILIARY STENT 1. Features & Benefits 2. Ordering information 3. References 1. Features & Benefits (1) Features Superior flexibility & conformability 4 Types Single bare, Single cover, Double bare,
EGIS BILIARY STENT 1. Features & Benefits 2. Ordering information 3. References 1. Features & Benefits (1) Features Superior flexibility & conformability 4 Types Single bare, Single cover, Double bare,
Delayed Severe Hemobilia after Endoscopic Biliary Plastic Stent Insertion
 CASE REPORT Clin Endosc 2016;49:303-307 http://dx.doi.org/10.5946/ce.2015.081 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Delayed Severe Hemobilia after Endoscopic Biliary Plastic Stent Insertion
CASE REPORT Clin Endosc 2016;49:303-307 http://dx.doi.org/10.5946/ce.2015.081 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Delayed Severe Hemobilia after Endoscopic Biliary Plastic Stent Insertion
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Percutaneous Removal of Biliary Stone from Anomalous Right Hepatic Duct
 Percutaneous Removal of Biliary Stone from Anomalous Right Hepatic Duct Pages with reference to book, From 94 To 96 Tanveer ul Haq, Mohammed Younus Sheikh, Changes Khan Jadun, M.N. Ahmad, Yousuf H. Husen
Percutaneous Removal of Biliary Stone from Anomalous Right Hepatic Duct Pages with reference to book, From 94 To 96 Tanveer ul Haq, Mohammed Younus Sheikh, Changes Khan Jadun, M.N. Ahmad, Yousuf H. Husen
Afferent Loop Syndrome: Treatment by Means of the Placement of Dual Stents
 Vascular and Interventional Radiology Original Research Han et al. Use of Dual Stents for Treatment of Afferent Loop Syndrome Vascular and Interventional Radiology Original Research Kichang Han 1 Ho-Young
Vascular and Interventional Radiology Original Research Han et al. Use of Dual Stents for Treatment of Afferent Loop Syndrome Vascular and Interventional Radiology Original Research Kichang Han 1 Ho-Young
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM
 A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
Cholangiocarcinoma: Radiologic evaluation and interventions
 November 2014 Cholangiocarcinoma: Radiologic evaluation and interventions Colin Nevins, Harvard Medical School Year III Agenda Initial course and work-up Endoscopic retrograde cholangiopancreatography
November 2014 Cholangiocarcinoma: Radiologic evaluation and interventions Colin Nevins, Harvard Medical School Year III Agenda Initial course and work-up Endoscopic retrograde cholangiopancreatography
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Donor Postoperative Biliary Complications After Living-Donor Liver Transplant
 ARTICle Donor Postoperative Biliary Complications After Living-Donor Liver Transplant Abuzer Dirican, Cengiz Ara, Koray Kutluturk, Mustafa Ozsoy, Mustafa Ates, Adil Baskiran, Burak Isik, Sezai Yilmaz Abstract
ARTICle Donor Postoperative Biliary Complications After Living-Donor Liver Transplant Abuzer Dirican, Cengiz Ara, Koray Kutluturk, Mustafa Ozsoy, Mustafa Ates, Adil Baskiran, Burak Isik, Sezai Yilmaz Abstract
Research Article Safety and Yield of Diagnostic ERCP in Liver Transplant Patients with Abnormal Liver Function Tests
 Diagnostic and erapeutic Endoscopy, Article ID 314927, 5 pages http://dx.doi.org/10.1155/2014/314927 Research Article Safety and Yield of Diagnostic ERCP in Liver Transplant Patients with Abnormal Liver
Diagnostic and erapeutic Endoscopy, Article ID 314927, 5 pages http://dx.doi.org/10.1155/2014/314927 Research Article Safety and Yield of Diagnostic ERCP in Liver Transplant Patients with Abnormal Liver
MAKING CONNECTIONS. Los Angeles Medical Center
 MAKING CONNECTIONS Los Angeles Medical Center Resident: Chris Molloy, MD Fellow: Christian Coroian, MD, MBA Attending: Tina Hardley, MD Program/Dept(s): Los Angeles Medical Center CHIEF COMPLAINT & HPI
MAKING CONNECTIONS Los Angeles Medical Center Resident: Chris Molloy, MD Fellow: Christian Coroian, MD, MBA Attending: Tina Hardley, MD Program/Dept(s): Los Angeles Medical Center CHIEF COMPLAINT & HPI
En-liang Li 1,2, Rong-fa Yuan 1, Wen-jun Liao 1, Qian Feng 1, Jun Lei 1, Xiang-bao Yin 1, Lin-quan Wu 1* and Jiang-hua Shao 1
 Li et al. BMC Surgery (2019) 19:16 https://doi.org/10.1186/s12893-019-0480-1 RESEARCH ARTICLE Open Access Intrahepatic bile exploration lithotomy is a useful adjunctive hepatectomy method for bilateral
Li et al. BMC Surgery (2019) 19:16 https://doi.org/10.1186/s12893-019-0480-1 RESEARCH ARTICLE Open Access Intrahepatic bile exploration lithotomy is a useful adjunctive hepatectomy method for bilateral
LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1157 1161 LIVER, PANCREAS, AND BILIARY TRACT Delayed and Unsuccessful Endoscopic Retrograde Cholangiopancreatography Are Associated With Worse Outcomes
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1157 1161 LIVER, PANCREAS, AND BILIARY TRACT Delayed and Unsuccessful Endoscopic Retrograde Cholangiopancreatography Are Associated With Worse Outcomes
Index words : Bile duct radiography, technology Bile ducts MR Bile ducts surgery Liver, transplantation
 Hilar Branching Anatomy of Living Adult Liver Donors: Comparison of T2-MR Cholangiography and Contrast Enhanced T1-MR Cholangiography in Terms of Diagnostic Utility 1 Joon Seok Lim, M.D. 1, Myeong-Jin
Hilar Branching Anatomy of Living Adult Liver Donors: Comparison of T2-MR Cholangiography and Contrast Enhanced T1-MR Cholangiography in Terms of Diagnostic Utility 1 Joon Seok Lim, M.D. 1, Myeong-Jin
Takuya SAKODA* ), Yoshiaki MURAKAMI, Naru KONDO, Kenichiro UEMURA, Yasushi HASHIMOTO, Naoya NAKAGAWA and Taijiro SUEDA ABSTRACT
 Hiroshima J. Med. Sci. Vol. 64, No. 3, 45~49, September, 2015 HIJM 64 8 45 Takuya SAKODA* ), Yoshiaki MURAKAMI, Naru KONDO, Kenichiro UEMURA, Yasushi HASHIMOTO, Naoya NAKAGAWA and Taijiro SUEDA Department
Hiroshima J. Med. Sci. Vol. 64, No. 3, 45~49, September, 2015 HIJM 64 8 45 Takuya SAKODA* ), Yoshiaki MURAKAMI, Naru KONDO, Kenichiro UEMURA, Yasushi HASHIMOTO, Naoya NAKAGAWA and Taijiro SUEDA Department
Research Article Risk Factors for Migration, Fracture, and Dislocation of Pancreatic Stents
 Gastroenterology Research and Practice Volume 2015, Article ID 365457, 6 pages http://dx.doi.org/10.1155/2015/365457 Research Article Risk Factors for Migration, Fracture, and Dislocation of Pancreatic
Gastroenterology Research and Practice Volume 2015, Article ID 365457, 6 pages http://dx.doi.org/10.1155/2015/365457 Research Article Risk Factors for Migration, Fracture, and Dislocation of Pancreatic
Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas
 CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Original article: SURGICAL TREATMENT FOR BENIGN BILIARY STRICTURES: SINGLE-CENTER EXPERIENCE ON 64 CASES
 Original article: SURGICAL TREATMENT FOR BENIGN BILIARY STRICTURES: SINGLE-CENTER EXPERIENCE ON 64 CASES Yunfeng Cui, Hongtao Zhang, Naiqiang Cui, Zhonglian Li* Department of Surgery, Tianjin Nankai Hospital,
Original article: SURGICAL TREATMENT FOR BENIGN BILIARY STRICTURES: SINGLE-CENTER EXPERIENCE ON 64 CASES Yunfeng Cui, Hongtao Zhang, Naiqiang Cui, Zhonglian Li* Department of Surgery, Tianjin Nankai Hospital,
Risk Factors for Development of Biliary Stricture in Patients Presenting with Bile Leak after Cholecystectomy
 Gut and Liver, Vol. 7, No. 3, May 2013, pp. 352-356 ORiginal Article Risk Factors for Development of Biliary Stricture in Patients Presenting with Bile Leak after Cholecystectomy Hosur Mayanna Lokesh,
Gut and Liver, Vol. 7, No. 3, May 2013, pp. 352-356 ORiginal Article Risk Factors for Development of Biliary Stricture in Patients Presenting with Bile Leak after Cholecystectomy Hosur Mayanna Lokesh,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
Current Treatment Strategies for Hilar and Intrahepatic Cholangiocarcinoma
 Current Treatment Strategies for Hilar and Intrahepatic Cholangiocarcinoma Jean-Nicolas Vauthey, MD, FACS Professor of Surgery Chief Hepato-Pancreato-Biliary Section Department of Surgical Oncology Crescent
Current Treatment Strategies for Hilar and Intrahepatic Cholangiocarcinoma Jean-Nicolas Vauthey, MD, FACS Professor of Surgery Chief Hepato-Pancreato-Biliary Section Department of Surgical Oncology Crescent
Biliary Cast Formation with Sclerosing Cholangitis in Critically Ill Patient: Case Report and Literature Review
 Case Report http://dx.doi.org/10.3348/kjr.2012.13.3.358 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(3):358-362 Biliary Cast Formation with Sclerosing Cholangitis in Critically Ill Patient:
Case Report http://dx.doi.org/10.3348/kjr.2012.13.3.358 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(3):358-362 Biliary Cast Formation with Sclerosing Cholangitis in Critically Ill Patient:
Single-stage management with combined tri-endoscopic approach. approach for concomitant cholecystolithiasis and choledocholithiasis
 Surg Endosc (2016) 30:5615 5620 DOI 10.1007/s00464-016-4918-6 and Other Interventional Techniques ENDOLUMINAL SURGERY Single-stage management with combined tri-endoscopic approach for concomitant cholecystolithiasis
Surg Endosc (2016) 30:5615 5620 DOI 10.1007/s00464-016-4918-6 and Other Interventional Techniques ENDOLUMINAL SURGERY Single-stage management with combined tri-endoscopic approach for concomitant cholecystolithiasis
A patient with an unusual congenital anomaly of the pancreaticobiliary tree
 A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
Current State of Living Donor Liver Transplantation
 REVIEW Current State of Living Donor Liver Transplantation Paige M. Porret, Kim M. Olthoff The discrepancy between the number of patients waiting for a liver and the available number of deceased donors
REVIEW Current State of Living Donor Liver Transplantation Paige M. Porret, Kim M. Olthoff The discrepancy between the number of patients waiting for a liver and the available number of deceased donors
Intraluminal Brachytherapy after Metallic Stent Placement in Primary Bile Duct Carcinoma 1
 Intraluminal Brachytherapy after Metallic Stent Placement in Primary Bile Duct Carcinoma 1 Kyu-Hong Park, M.D., Soon Gu Cho, M.D., Sung-Gwon Kang, M.D. 1,2, Don Haeng Lee, M.D. 3, Woo Cheol Kim, M.D. 4,
Intraluminal Brachytherapy after Metallic Stent Placement in Primary Bile Duct Carcinoma 1 Kyu-Hong Park, M.D., Soon Gu Cho, M.D., Sung-Gwon Kang, M.D. 1,2, Don Haeng Lee, M.D. 3, Woo Cheol Kim, M.D. 4,
Usefulness of Forward-Viewing Endoscope for Endoscopic Retrograde Cholangiopancreatography in Patients with Billroth II Gastrectomy
 ORIGINAL ARTICLE Clin Endosc 2012;45:397-403 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2012.45.4.397 Open Access Usefulness of Forward-Viewing Endoscope for Endoscopic
ORIGINAL ARTICLE Clin Endosc 2012;45:397-403 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2012.45.4.397 Open Access Usefulness of Forward-Viewing Endoscope for Endoscopic
Approach to the Biliary Stricture
 Approach to the Biliary Stricture ACG Eastern Postgraduate Course Washington DC June 8, 2014 Steven A. Edmundowicz MD FASGE Chief of Endoscopy Division of Gastroenterology Professor of Medicine Disclosures
Approach to the Biliary Stricture ACG Eastern Postgraduate Course Washington DC June 8, 2014 Steven A. Edmundowicz MD FASGE Chief of Endoscopy Division of Gastroenterology Professor of Medicine Disclosures
CURRICULUM VITAE
 CURRICULUM VITAE Name Date of Birth Nationality Marital Status Permanent Address Sang Soo Lee, M. D. August 6, 1968 Korean Married, one child 217-704 Hanshin APT 137-949 Jamwon dong, Seocho-gu, Seoul,
CURRICULUM VITAE Name Date of Birth Nationality Marital Status Permanent Address Sang Soo Lee, M. D. August 6, 1968 Korean Married, one child 217-704 Hanshin APT 137-949 Jamwon dong, Seocho-gu, Seoul,
Percutaneous biliary drainage: complications and efficiency at short and mean terms: about 50 cases
 Percutaneous biliary drainage: complications and efficiency at short and mean terms: about 50 cases Poster No.: C-1497 Congress: ECR 2016 Type: Scientific Exhibit Authors: M. Matri, L. Ben Farhat, I. Marzouk
Percutaneous biliary drainage: complications and efficiency at short and mean terms: about 50 cases Poster No.: C-1497 Congress: ECR 2016 Type: Scientific Exhibit Authors: M. Matri, L. Ben Farhat, I. Marzouk
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica
 Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
ERCP in altered anatomy. Lars Aabakken Oslo University Hospital - Rikshospitalet Oslo, Norway
 ERCP in altered anatomy Lars Aabakken Oslo University Hospital - Rikshospitalet Oslo, Norway CO2 as insufflation gas Reduces post-procedure pain Reduces in-procedure bowel distension Improves the intubation
ERCP in altered anatomy Lars Aabakken Oslo University Hospital - Rikshospitalet Oslo, Norway CO2 as insufflation gas Reduces post-procedure pain Reduces in-procedure bowel distension Improves the intubation
Pre-operative prediction of difficult laparoscopic cholecystectomy
 International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
Study of post cholecystectomy biliary leakage and its management
 Original Research Article Study of post cholecystectomy biliary leakage and its management P. Krishna Kishore 1*, B. Manju Sruthi 2, G. Obulesu 3 1 Assistant Professor, Departmentment of General Surgery,
Original Research Article Study of post cholecystectomy biliary leakage and its management P. Krishna Kishore 1*, B. Manju Sruthi 2, G. Obulesu 3 1 Assistant Professor, Departmentment of General Surgery,
Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation
 Kasr El Aini Journal of Surgery VOL., 9, NO 3 January 2008 19 Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation A. Ayad ; W. Tobar; M.Hassan; A.Hosny; M.El Shazly;
Kasr El Aini Journal of Surgery VOL., 9, NO 3 January 2008 19 Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation A. Ayad ; W. Tobar; M.Hassan; A.Hosny; M.El Shazly;
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
WallFlex Biliary RX Fully Covered Stent System Prescriptive Information
 Caution/Rx Only: Federal Law (USA) restricts this device to sale by or on the order of a physician. Warning Contents supplied STERILE using an ethylene oxide (EO) process. Do not use if sterile barrier
Caution/Rx Only: Federal Law (USA) restricts this device to sale by or on the order of a physician. Warning Contents supplied STERILE using an ethylene oxide (EO) process. Do not use if sterile barrier
Vascular complications in percutaneous biliary interventions: A series of 111 procedures
 Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Two Consecutive Cases of Ampulla of Vater Cancer Combined with Annular Pancreas and Unusual Anatomic Variation
 Korean Journal of HBP Surgery Vol. 14, No. 3, September 2010 증례 Two Consecutive Cases of Ampulla of Vater Cancer Combined with Annular Pancreas and Unusual Anatomic Variation Annular pancreas is a rare
Korean Journal of HBP Surgery Vol. 14, No. 3, September 2010 증례 Two Consecutive Cases of Ampulla of Vater Cancer Combined with Annular Pancreas and Unusual Anatomic Variation Annular pancreas is a rare
Home Intravenous Antibiotic Treatment for Intractable Cholangitis in Biliary Atresia
 Home Intravenous Antibiotic Treatment for Intractable Cholangitis in Biliary Atresia Hye Kyung Chang, Jung-Tak Oh, Seung Hoon Choi, Seok Joo Han Division of Pediatric Surgery, Department of Surgery, Yonsei
Home Intravenous Antibiotic Treatment for Intractable Cholangitis in Biliary Atresia Hye Kyung Chang, Jung-Tak Oh, Seung Hoon Choi, Seok Joo Han Division of Pediatric Surgery, Department of Surgery, Yonsei
Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience
 Case Reports in Surgery Volume 2013, Article ID 821032, 4 pages http://dx.doi.org/10.1155/2013/821032 Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience Fransisca J. Siahaya,
Case Reports in Surgery Volume 2013, Article ID 821032, 4 pages http://dx.doi.org/10.1155/2013/821032 Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience Fransisca J. Siahaya,
CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S
 Medical Education Singapore Med.1 2007, 48 (4) : 361 CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S fit. B CD - -0 o -5 r t -10 Fig. I US images of the upper right abdomen
Medical Education Singapore Med.1 2007, 48 (4) : 361 CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S fit. B CD - -0 o -5 r t -10 Fig. I US images of the upper right abdomen
Influencing factors on postoperative hospital stay after laparoscopic cholecystectomy
 Korean J Hepatobiliary Pancreat Surg 2016;20:12-16 http://dx.doi.org/10.14701/kjhbps.2016.20.1.12 Original Article Influencing factors on postoperative hospital stay after laparoscopic cholecystectomy
Korean J Hepatobiliary Pancreat Surg 2016;20:12-16 http://dx.doi.org/10.14701/kjhbps.2016.20.1.12 Original Article Influencing factors on postoperative hospital stay after laparoscopic cholecystectomy
De novo hepatitis B virus infection developing after liver transplantation using a graft positive for hepatitis B core antibody
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2015.89.3.145 Annals of Surgical Treatment and Research De novo hepatitis B virus infection developing after liver transplantation
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2015.89.3.145 Annals of Surgical Treatment and Research De novo hepatitis B virus infection developing after liver transplantation
An Intraductal Papillary Neoplasm of the Bile Duct at the Duodenal Papilla
 Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation
 LETTERS FROM THE FRONTLINE Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation TO THE EDITOR: Hepatic artery (HA) reconstruction
LETTERS FROM THE FRONTLINE Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation TO THE EDITOR: Hepatic artery (HA) reconstruction
Cholecystectomy rate following endoscopic biliary interventions
 Original Article Brunei Int Med J. 2012; 8 (4): 166-172 Cholecystectomy rate following endoscopic biliary interventions Sky Lim 1, Lin Naing 1, Vui Heng Chong 2 1 Pengiran Anak Puteri Rashidah Sa adatul
Original Article Brunei Int Med J. 2012; 8 (4): 166-172 Cholecystectomy rate following endoscopic biliary interventions Sky Lim 1, Lin Naing 1, Vui Heng Chong 2 1 Pengiran Anak Puteri Rashidah Sa adatul
Adult-to-adult living donor liver transplantation Triumphs and challenges
 Falk Symposium No. 163 on Chronic Inflammation of Liver and Gut Adult-to-adult living donor liver transplantation Triumphs and challenges ST Fan, MS, MD, PhD, DSc Professor Sun CY Chair of Hepatobiliary
Falk Symposium No. 163 on Chronic Inflammation of Liver and Gut Adult-to-adult living donor liver transplantation Triumphs and challenges ST Fan, MS, MD, PhD, DSc Professor Sun CY Chair of Hepatobiliary
Role of Malabsorptive Endoscopic Procedures in Obesity Treatment
 FOCUSED REVIEW SERIES: Roles of Bariatric Endoscopy in Obesity Treatment Clin Endosc 2017;50:26-30 https://doi.org/10.5946/ce.2017.004 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Role of Malabsorptive
FOCUSED REVIEW SERIES: Roles of Bariatric Endoscopy in Obesity Treatment Clin Endosc 2017;50:26-30 https://doi.org/10.5946/ce.2017.004 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Role of Malabsorptive
Journal of Interventional Gastroenterology A Combination of Snare Polypectomy and APC Therapy for Prolapsing Common Bile Duct Adenoma
 Journal of Interventional Gastroenterology A Combination of Snare Polypectomy and APC Therapy for Prolapsing Common Bile Duct Adenoma --Manuscript Draft-- Manuscript Number: Full Title: Article Type: Section/Category:
Journal of Interventional Gastroenterology A Combination of Snare Polypectomy and APC Therapy for Prolapsing Common Bile Duct Adenoma --Manuscript Draft-- Manuscript Number: Full Title: Article Type: Section/Category:
Personal Profile. Name: 劉 XX Gender: Female Age: 53-y/o Past history. Hepatitis B carrier
 Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
