CHAPTER 7. End Stage Liver Disease in the ICU: Walking a Tightrope. Lynn A. Kelso, MSN, APRN, FCCM, FAANP University of Kentucky College of Nursing
|
|
|
- Georgia Potter
- 5 years ago
- Views:
Transcription
1 CHAPTER 7 End Stage Liver Disease in the ICU: Walking a Tightrope Lynn A. Kelso, MSN, APRN, FCCM, FAANP University of Kentucky College of Nursing Besey Oren, Assistant Professor Istanbul University Health Science Faculty 1
2 Learning objectives After reviewing the chapter the learner will be able to: 1. Discuss the pathophysiology of liver failure. 2. Describe clinical manifestations of liver failure. 3. Describe nursing implications, diagnositics and treatment required in the patient experiencing liver failure. Patients who suffer from end stage liver disease (ESLD) can present many challenges to the nurses caring for them. While they may appear to be stable, they are balancing on a very fine tightrope and life threatening complications can arise suddenly, requiring immediate attention to prevent catastrophic outcomes. The critical care nurse must be able to thoroughly assess for impending complications and always be prepared for a change in the patient s condition. The liver plays many roles in maintaining health. It clears the body of ingested toxins, manufactures numerous clotting factors, helps to maintain vascular oncotic pressure by producing albumin and plays a role in glycemic control. As the liver fails, it can no longer carry out these normal functions leading to the complications that are associated with ESLD. While the liver has a remarkable ability to recover and regenerate, when severe injury occurs, whether from disease, accumulation of toxins, such as alcohol, infection, such as chronic hepatitis, or other disorder, this regeneration can lead to fibrotic changes in the liver tissue. Once enough of the liver tissue becomes diseased and irreversible changes have occurred, a diagnosis of cirrhosis is made. These cirrhotic changes lead to an inability for normal blood flow through the liver as well as an inability for the liver to carry out its normal functions. The point is reached when there are not enough healthy hepatocytes remaining. The complications that are seen in ESLD are a direct result of these structural changes. HEPATIC ENCEPHALOPATHY Hepatic encephalopathy (HE) occurs in patients with ESLD as a result of a build-up of toxins able to cross the blood brain barrier and leads to changes in mental status. The exact cause of HE is unclear but there is strong association between elevation of circulating ammonia and severity of HE. Intestinal bacteria breakdown protein in the intestine leading to an increase in ammonia. When the cirrhotic liver is unable 2
3 to metabolize the absorbed ammonia, it enters the systemic circulation and is able to cross the blood brain barrier, leading to changes in neurotransmitters and alteration in neurological function (1). Hepatic encephalopathy is categorized by type and severity. There are 3 types of HE, type A which is associated with acute liver failure, type B associated with abnormal ammonia metabolism and no underlying liver disease, and type C associated with chronic liver failure (2). Hepatic encephalopathy is further defined by grades (Table 1). Once a patient deteriorates to Grade 2, transfer to the ICU is warranted, as a continuous decline can lead to inability to protect the airway and respiratory failure. These patients require intubation and mechanical ventilation until their mental status improves. 3
4 Table 1. Grades of Hepatic Encephalopathy Grades Clinical Signs and Symptoms 1 Mild changes in personality, decreased attention span, loss of calculating functions. No asterixis present 2 Worsening personality changes, disoriented, incontinence, asterixis can be seen, reversed sleep/wake patterns 3 Somnolent but arousable from sleep, obvious asterixis, very confused with slurred, incoherent speech 4 Comatose and may or may not respond to noxious stimulation, may see posturing Worsening HE can occur in patients who develop gastrointestinal (GI) bleeding or an infection. These patients must be closely monitored for decline in their mental status and the need for airway management (3). Lactulose can be used orally or via enema to trap ammonia and expel it from the GI tract. Doses should be titrated to 3 4 loose stools per day (2). Rifaximin, an antimicrobial, can be used to decrease GI bacteria which can decrease the amount of ammonia that is produced from digestion of protein. The usual dose is 550 mg two times per day (1). PORTAL HYPERTENSION As cirrhotic changes in the liver worsen, blood can no longer flow freely through the liver lobules. There is an increase in venous pressure leading to increased pressures within the portal system. The development of portal hypertension contributes to a number of the complications we see in patients with ESLD including, ascites, gastroesophageal varices and variceal bleeding. Ascites Ascites occurs when protein rich fluid accumulates in the peritoneal cavity. The increased pressure in the portal system increases the hydrostatic pressure in the vessels causing fluid rich in protein to be forced out of the vascular space into the abdomen. This increases the oncotic, or water-pulling, pressure within the abdomen causing further fluid to pulled in (4). Complications associated with ascites include infection, notably spontaneous bacterial peritonitis (SBP), and respiratory failure, occurring when enough fluid accumulates within the abdominal cavity to impede adequate respiratory function. SBP should be suspected in all ESLD patients who have any amount of 4
5 ascites and develop a fever and abdominal pain (3). A diagnostic paracentesis can performed to look for white blood cells and bacteria in the ascites. If an infection is present, antimicrobials need to be started and the ascites may need to be completely drained from the peritoneal cavity. Typically, ascites is controlled with diuretics. If enough fluid accumulates to compromise respiratory function, a therapeutic paracentesis may be performed to drain enough ascites to prevent the need for intubation and mechanical ventilation. Gastroesophageal Varices Although varices can occur anywhere within the splanchnic circulation, these collateral vessels are typically seen in the distal esophagus and the gastric fundus (5). An esophagogastroduodenoscopy (EGD) is used not only to diagnose varices, but to determine their severity and the likelihood of bleeding. Banding of problematic vessels can occur in order to prevent, or decrease the risk of a variceal hemorrhage (5). Beta blockers may also be used to decrease portal pressure and decrease the risk of bleeding, however patients must be closely monitored for systemic hypotension that may complicate this treatment option (5). Variceal Hemorrhage The rupture and bleeding from varices is the most life-threatening complication of ESLD. Immediate action is needed to protect the airway, maintain adequate perfusion and replacing both blood and clotting factors. Patients with bleeding varices require intubation and mechanical ventilation. Volume replacement can include crystalloid solutions as well as blood transfusions to attain a hemoglobin of 8g/dL. Fresh frozen plasma (FFP) is needed to replace clotting factors that are not adequately produced in the diseased liver with the goal of an INR < 1.5. Platelet transfusion may be necessary to increase the platelet count to > 50 x 10 9 /L (5). In order to control bleeding, an EGD may be performed to identify the vessel. If bleeding can t be controlled with banding during the EGD, balloon tamponade may be necessary. Pharmacological intervention is also necessary including splanchnic vasoconstriction with medications such as somatostatin or octreotide (5). Vasopressin, the most potent splanchnic vasoconstrictor, may be used, however there are numerous side effects associated with its use and patients need to be closely monitored for the development of both peripheral and cardiac ischemia (5). Patients who develop variceal hemorrhage are also at a higher risk of developing bacterial infections and should receive a course of prophylactic antimicrobials (5). 5
6 COAGULOPATHY The liver is responsible for the production of many of the clotting factors necessary for normal coagulation. In addition, Vitamin K, a fat soluble vitamin, is needed to for the production of many components of coagulation. In ESLD, the liver may not be able to synthesize adequate clotting factors which is reflected in an elevation of the prothrombin time and INR. If there is not adequate bile production, Vitamin K may not be absorbed in sufficient amounts. When there is active bleeding, or if there is a high risk of bleeding, FFP may be transfused to decrease the INR to < 1.5. Vitamin K may be given orally or intravenously in attempts to decrease the INR, however, if the liver is unable to produce clotting factors, no change in the INR may be seen (4). HEPATOPULMONARY SYNDROME in patients with ESLD, changes in the pulmonary vasculature may be seen which can lead to hypoxemia. Hepatopulmonary syndrome (HPS) is not clearly understood and there are currently no ideal therapies, beyond liver transplantation, that can lead to improved oxygenation (6). Patients who suffer from HPS may qualify for liver transplantation even if their liver disease is not severe enough to warrant transplantation. Additional respiratory complications can occur as a result of abdominal ascites. An hepatic hydrothorax occurs when ascitic fluid passes up from the peritoneal cavity and through the diaphragm (7). This is typically seen in the right pleural space and, depending upon the volume, can compromise ventilation. HEPATORENAL SYNDROME Hepatorenal syndrome may be seen in patients with ESLD. Decreased renal function can occur from actual damage to nephrons, can be a consequence of liver failure or can be a combination of the two. It can be difficult to differentiate between HPS and other causes of renal failure in patients with ESLD and the diagnosis of HRS is typically made when other causes of acute renal failure have been excluded (8). Patients who have HRS typically suffer from oliguria that is not responsive to either volume or diuretics (3). These patients frequently are hyponatremic and have a low urine sodium level, similar to that seen with pre-renal renal failure. Although there are temporizing therapies that can be started, including intermittent hemodialysis or continuous renal replacement therapy, liver transplantation is the best option for patients who are eligible to be transplanted (8). Renal function may not immediately return to normal and patients and 6
7 families have to be made aware that renal replacement therapy may be needed for a period of time after receiving a liver transplant. SUPPORT Without a liver transplant, patients with ESLD will not survive and this can be devastating to both the patient and the family. There is a tremendous amount of psychosocial support that is needed. Not all patients are good candidates, or are eligible to receive a transplant. Any complication can be the one that leads to their death. Even those who are on the waiting list for a new liver may develop complications that will remove them from the waiting list. This then requires patient and family discussions related to the level of aggressive, life sustaining therapies and end-of-life care. It is a difficult balancing act to maintain normal functioning for as long as possible. One small change, such as an infection, can lead a patient to lose their balance on that tightrope and end up critically ill in your ICU. References: 1. Scott LJ: Rifaximin: A review of its use in reducing recurrence of overt hepatic encephalopathy episodes. Drugs 2014; 74: Leise MD, Poterucha JJ, Kamath PS, Kim WR: Management of hepatic encephalopathy in the hospital. May Clin Proc 2014; 89(2): Kelso LA: Caring for patients with end-stage liver disease. Nursing2008 Crit Care 2008; 3(2): Kelso LA: Alterations in liver function. In: Wagner KD, Hardin-Pierce MG (Eds), High-Acuity Nursing, 6 th ed. Boston: Pearson; 2013: Garcia-Tsao G, Sanyal AJ, Grace ND, Carey WD: Prevention and management of gastroesophageal varices and variceal hemorrhage in cirrhosis. Am J of Gastroenterol 2007; 102: Koch DG, Fallon MB: Hepatopulmonary syndrome. Curr Opin Gastroenterol 2014; 30: Baikati K, Le DL, Jabbour II, et al: Hepatic hydrothorax. Am J Therapeutics 2014; 21: Wadei HM, Mai ML, Ahsan N, Gonwa TA: Hepatorenal syndrome: Pathophysiology and management. Clin J Am Soc Nephrol 2006; 1:
PORTAL HYPERTENSION An Introduction to the Culprit of Many Liver Failure Complications
 PORTAL HYPERTENSION An Introduction to the Culprit of Many Liver Failure Complications Edy G. Trujillo, RN, MSN, ACNP-BC Liver Transplant RRUCLA Medical Center July 31, 2018 What Do We All Look Forward
PORTAL HYPERTENSION An Introduction to the Culprit of Many Liver Failure Complications Edy G. Trujillo, RN, MSN, ACNP-BC Liver Transplant RRUCLA Medical Center July 31, 2018 What Do We All Look Forward
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Accelerated intravascular coagulation and fibrinolysis (AICF) in liver disease, 390 391 Acid suppression in liver disease, 403 404 ACLF.
Index Note: Page numbers of article titles are in boldface type. A Accelerated intravascular coagulation and fibrinolysis (AICF) in liver disease, 390 391 Acid suppression in liver disease, 403 404 ACLF.
ACG & AASLD Joint Clinical Guideline: Prevention and Management of Gastroesophageal Varices and Variceal Hemorrhage in Cirrhosis
 ACG & AASLD Joint Clinical Guideline: Prevention and Management of Gastroesophageal Varices and Variceal Hemorrhage in Cirrhosis Guadalupe Garcia-Tsao, M.D., 1 Arun J. Sanyal, M.D., 2 Norman D. Grace,
ACG & AASLD Joint Clinical Guideline: Prevention and Management of Gastroesophageal Varices and Variceal Hemorrhage in Cirrhosis Guadalupe Garcia-Tsao, M.D., 1 Arun J. Sanyal, M.D., 2 Norman D. Grace,
LIVER CIRRHOSIS. The liver extracts nutrients from the blood and processes them for later use.
 LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
following the last documented transfusion; thereafter, evaluate the residual impairment(s).
 Adult Listings 5.01 Category of Impairments, Digestive System 5.02 Gastrointestinal hemorrhaging from any cause, requiring blood transfusion (with or without hospitalization) of at least 2 units of blood
Adult Listings 5.01 Category of Impairments, Digestive System 5.02 Gastrointestinal hemorrhaging from any cause, requiring blood transfusion (with or without hospitalization) of at least 2 units of blood
Management of the Cirrhotic Patient in the ICU
 Management of the Cirrhotic Patient in the ICU Peter E. Morris, MD Professor & Chief, Pulmonary, Critical Care and Sleep Medicine University of Kentucky Conflict of Interest Funding US National Institutes
Management of the Cirrhotic Patient in the ICU Peter E. Morris, MD Professor & Chief, Pulmonary, Critical Care and Sleep Medicine University of Kentucky Conflict of Interest Funding US National Institutes
Chronic Hepatic Disease
 Chronic Hepatic Disease 10 th Leading Cause of Death Liver Functions Energy Metabolism Protein Synthesis Solubilization, Transport, and Storage Protects and Clears drugs, damaged cells Causes of Liver
Chronic Hepatic Disease 10 th Leading Cause of Death Liver Functions Energy Metabolism Protein Synthesis Solubilization, Transport, and Storage Protects and Clears drugs, damaged cells Causes of Liver
Liver failure &portal hypertension
 Liver failure &portal hypertension Objectives: by the end of this lecture each student should be able to : Diagnose liver failure (acute or chronic) List the causes of acute liver failure Diagnose and
Liver failure &portal hypertension Objectives: by the end of this lecture each student should be able to : Diagnose liver failure (acute or chronic) List the causes of acute liver failure Diagnose and
Etiology of liver cirrhosis
 Liver cirrhosis 1 Liver cirrhosis Liver cirrhosis is the progressive replacement of normal hepatic cells by fibrous scar tissue, This scarring is accompanied by the loss of viable hepatocytes, which are
Liver cirrhosis 1 Liver cirrhosis Liver cirrhosis is the progressive replacement of normal hepatic cells by fibrous scar tissue, This scarring is accompanied by the loss of viable hepatocytes, which are
The Continuum of Care for Advanced Liver Disease: Partnering with the Liver Specialist. K V Speeg, MD, PhD UT Health San Antonio
 The Continuum of Care for Advanced Liver Disease: Partnering with the Liver Specialist K V Speeg, MD, PhD UT Health San Antonio Objectives Review staging of liver disease Review consequences of end-stage
The Continuum of Care for Advanced Liver Disease: Partnering with the Liver Specialist K V Speeg, MD, PhD UT Health San Antonio Objectives Review staging of liver disease Review consequences of end-stage
Management of Chronic Liver Failure/Cirrhosis Complications in Hospitals. By: Dr. Kevin Dolehide
 Management of Chronic Liver Failure/Cirrhosis Complications in Hospitals By: Dr. Kevin Dolehide Overview DX Cirrhosis and Prognosis Compensated Decompensated Complications Of Cirrhosis Management Of Complications
Management of Chronic Liver Failure/Cirrhosis Complications in Hospitals By: Dr. Kevin Dolehide Overview DX Cirrhosis and Prognosis Compensated Decompensated Complications Of Cirrhosis Management Of Complications
Management of Cirrhosis Related Complications
 Management of Cirrhosis Related Complications Ke-Qin Hu, MD, FAASLD Professor of Clinical Medicine Director of Hepatology University of California, Irvine Disclosure I have no disclosure related to this
Management of Cirrhosis Related Complications Ke-Qin Hu, MD, FAASLD Professor of Clinical Medicine Director of Hepatology University of California, Irvine Disclosure I have no disclosure related to this
Nursing Care & Management of the Pre-Liver Transplant Population. Christine Kiamzon, RN, MSN, PCCN 8 North Educator
 Nursing Care & Management of the Pre-Liver Transplant Population Christine Kiamzon, RN, MSN, PCCN 8 North Educator Objectives 1. Identify key nursing interventions in caring for pre-transplant ESLD patients.
Nursing Care & Management of the Pre-Liver Transplant Population Christine Kiamzon, RN, MSN, PCCN 8 North Educator Objectives 1. Identify key nursing interventions in caring for pre-transplant ESLD patients.
Nursing Care & Management of the Pre-Liver Transplant Population
 Nursing Care & Management of the Pre-Liver Transplant Population Christine Kiamzon, RN, MSN, PCCN 8 North Educator Objectives 1. Identify key nursing interventions in caring for pre-transplant ESLD patients.
Nursing Care & Management of the Pre-Liver Transplant Population Christine Kiamzon, RN, MSN, PCCN 8 North Educator Objectives 1. Identify key nursing interventions in caring for pre-transplant ESLD patients.
MANAGEMENT OF LIVER CIRRHOSIS: PRACTICE ESSENTIALS AND PATIENT SELF-MANAGEMENT
 MANAGEMENT OF LIVER CIRRHOSIS: PRACTICE ESSENTIALS AND PATIENT SELF-MANAGEMENT Sherona Bau, ACNP The Pfleger Liver Institute 200 UCLA Medical Plaza, Suite 214 Los Angeles, CA 90095 September 30, 2017 I
MANAGEMENT OF LIVER CIRRHOSIS: PRACTICE ESSENTIALS AND PATIENT SELF-MANAGEMENT Sherona Bau, ACNP The Pfleger Liver Institute 200 UCLA Medical Plaza, Suite 214 Los Angeles, CA 90095 September 30, 2017 I
Initial approach to ascites
 Ascites: Filling and Draining the Water Balloon Common Pathogenesis in Refractory Ascites, Hyponatremia, and Cirrhosis intrahepatic resistance sinusoidal portal hypertension Splanchnic vasodilation (effective
Ascites: Filling and Draining the Water Balloon Common Pathogenesis in Refractory Ascites, Hyponatremia, and Cirrhosis intrahepatic resistance sinusoidal portal hypertension Splanchnic vasodilation (effective
Treating patients with end-stage liver disease: Are we ready? Dr. Mino R. Mitri, M.D., C.M., M.Ed., FRCPC
 Treating patients with end-stage liver disease: Are we ready? Dr. Mino R. Mitri, M.D., C.M., M.Ed., FRCPC mino.mitri@ubc.ca No Conflict of Interest 157 patients 157 patients 6 transplanted Criteria Liver
Treating patients with end-stage liver disease: Are we ready? Dr. Mino R. Mitri, M.D., C.M., M.Ed., FRCPC mino.mitri@ubc.ca No Conflict of Interest 157 patients 157 patients 6 transplanted Criteria Liver
Esophageal Varices Beta-Blockers or Band Ligation. Cesar Yaghi MD Hotel-Dieu de France University Hospital Universite Saint Joseph
 Esophageal Varices Beta-Blockers or Band Ligation Cesar Yaghi MD Hotel-Dieu de France University Hospital Universite Saint Joseph Esophageal Varices Beta-Blockers or Band Ligation? Risk of esophageal variceal
Esophageal Varices Beta-Blockers or Band Ligation Cesar Yaghi MD Hotel-Dieu de France University Hospital Universite Saint Joseph Esophageal Varices Beta-Blockers or Band Ligation? Risk of esophageal variceal
COMPLICATIONS OF CIRRHOSIS: ASCITES & HEPATIC ENCEPHALOPATHY
 COMPLICATIONS OF CIRRHOSIS: ASCITES & HEPATIC ENCEPHALOPATHY DR. ESTER YAGUDAYEVA CLINICAL PHARMACIST HOSPICE PHARMACY SOLUTIONS OBJECTIVES Understand the prognosis of End Stage Liver Disease (ESLD) Identify
COMPLICATIONS OF CIRRHOSIS: ASCITES & HEPATIC ENCEPHALOPATHY DR. ESTER YAGUDAYEVA CLINICAL PHARMACIST HOSPICE PHARMACY SOLUTIONS OBJECTIVES Understand the prognosis of End Stage Liver Disease (ESLD) Identify
Beta-blockers in cirrhosis: Cons
 Beta-blockers in cirrhosis: Cons Eric Trépo MD, PhD Dept. of Gastroenterology. Hepatopancreatology and Digestive Oncology. C.U.B. Hôpital Erasme. Université Libre de Bruxelles. Bruxelles. Belgium Laboratory
Beta-blockers in cirrhosis: Cons Eric Trépo MD, PhD Dept. of Gastroenterology. Hepatopancreatology and Digestive Oncology. C.U.B. Hôpital Erasme. Université Libre de Bruxelles. Bruxelles. Belgium Laboratory
Conflict of interest disclosures. Complications of end stage liver disease. None. The many complications of Cirrhosis. Portal Hypertension.
 Complications of end stage liver disease Conflict of interest disclosures None Amir Qamar, MD Instructor of Medicine Brigham and Women s s Hospital Harvard Medical School Boston, MA 02115 The many complications
Complications of end stage liver disease Conflict of interest disclosures None Amir Qamar, MD Instructor of Medicine Brigham and Women s s Hospital Harvard Medical School Boston, MA 02115 The many complications
Definition: fibrosis and nodular regeneration resulting from hepatocellular injury
 Cirrhosis Understanding the liver: Patterns of LFT Abnormalities - Hepatocellular/Transaminitis: o Ratio of AST: ALT >2:1 ETOH (keep in mind AST is also produced by red cells, heart muscle) o If Aminotransferases
Cirrhosis Understanding the liver: Patterns of LFT Abnormalities - Hepatocellular/Transaminitis: o Ratio of AST: ALT >2:1 ETOH (keep in mind AST is also produced by red cells, heart muscle) o If Aminotransferases
Index. Crit Care Clin 19 (2003)
 Crit Care Clin 19 (2003) 331 335 Index A ACVECC. See American College of Veterinary Emergency and Critical Care (ACVECC). Aging. See also Elderly; Geriatric critical care. respiratory function effects
Crit Care Clin 19 (2003) 331 335 Index A ACVECC. See American College of Veterinary Emergency and Critical Care (ACVECC). Aging. See also Elderly; Geriatric critical care. respiratory function effects
Decompensated chronic liver disease
 Decompensated chronic liver disease Definition of decompensated chronic liver disease Patients with chronic liver disease can present with acute decompensation due to various causes. The decompensation
Decompensated chronic liver disease Definition of decompensated chronic liver disease Patients with chronic liver disease can present with acute decompensation due to various causes. The decompensation
Understanding this condition will help you provide optimal care for patients and their families.
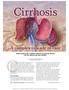 Cirrhosis A complex cascade of care ILLUSTRATION BY STEVE OH/PHOTOTAKE Understanding this condition will help you provide optimal care for patients and their families. By Ann Crawford, PhD, RN, CNS, CEN,
Cirrhosis A complex cascade of care ILLUSTRATION BY STEVE OH/PHOTOTAKE Understanding this condition will help you provide optimal care for patients and their families. By Ann Crawford, PhD, RN, CNS, CEN,
CHAPTER 1. Alcoholic Liver Disease
 CHAPTER 1 Alcoholic Liver Disease Major Lesions of Alcoholic Liver Disease Alcoholic fatty liver - >90% of binge and chronic drinkers Alcoholic hepatitis precursor of cirrhosis Alcoholic cirrhosis end
CHAPTER 1 Alcoholic Liver Disease Major Lesions of Alcoholic Liver Disease Alcoholic fatty liver - >90% of binge and chronic drinkers Alcoholic hepatitis precursor of cirrhosis Alcoholic cirrhosis end
Alpha-1 Antitrypsin Deficiency: Liver Disease
 Alpha-1 Antitrypsin Deficiency: Liver Disease Who is at risk to develop Alpha-1 liver disease? Alpha-1 liver disease may affect children and adults who have abnormal Alpha-1 antitrypsin genes. Keys to
Alpha-1 Antitrypsin Deficiency: Liver Disease Who is at risk to develop Alpha-1 liver disease? Alpha-1 liver disease may affect children and adults who have abnormal Alpha-1 antitrypsin genes. Keys to
Causes of Liver Disease in US
 Learning Objectives Updates in Outpatient Cirrhosis Management Jennifer Guy, MD MAS Director, Liver Cancer Program California Pacific Medical Center guyj@sutterhealth.org Review cirrhosis epidemiology,
Learning Objectives Updates in Outpatient Cirrhosis Management Jennifer Guy, MD MAS Director, Liver Cancer Program California Pacific Medical Center guyj@sutterhealth.org Review cirrhosis epidemiology,
Management of Hepatic Encephalopathy
 Management of Hepatic Encephalopathy Atif Zaman, MD MPH Oregon Health & Science University Professor of Medicine Division of Gastroenterology and Hepatology Disclosure 1. The speaker Atif Zaman, MD MPH
Management of Hepatic Encephalopathy Atif Zaman, MD MPH Oregon Health & Science University Professor of Medicine Division of Gastroenterology and Hepatology Disclosure 1. The speaker Atif Zaman, MD MPH
Norepinephrine versus Terlipressin for the Treatment of Hepatorenal Syndrome
 Norepinephrine versus Terlipressin for the Treatment of Hepatorenal Syndrome Disclosure I have no conflicts of interest to disclose Name: Margarita Taburyanskaya Title: PharmD, PGY1 Pharmacy Practice Resident
Norepinephrine versus Terlipressin for the Treatment of Hepatorenal Syndrome Disclosure I have no conflicts of interest to disclose Name: Margarita Taburyanskaya Title: PharmD, PGY1 Pharmacy Practice Resident
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACLF. See Acute-on-chronic liver failure (ACLF) Acute kidney injury (AKI) in ACLF patients, 967 Acute liver failure (ALF), 957 964 causes
Index Note: Page numbers of article titles are in boldface type. A ACLF. See Acute-on-chronic liver failure (ACLF) Acute kidney injury (AKI) in ACLF patients, 967 Acute liver failure (ALF), 957 964 causes
Medicines for Chronic Liver Disease
 UW MEDICINE PATIENT EDUCATION Medicines for Chronic Liver Disease Treating common conditions This handout gives basic information about how the liver works and what happens during liver failure. It describes
UW MEDICINE PATIENT EDUCATION Medicines for Chronic Liver Disease Treating common conditions This handout gives basic information about how the liver works and what happens during liver failure. It describes
CIRRHOSIS Definition
 Cirrhosis Update Robert S. Brown, Jr., MD, MPH Vice Chair, Transitions of Care Interim Chief, Division of Gastroenterology & Hepatology Weill Cornell Medical College CIRRHOSIS Definition Irreversible fibrous
Cirrhosis Update Robert S. Brown, Jr., MD, MPH Vice Chair, Transitions of Care Interim Chief, Division of Gastroenterology & Hepatology Weill Cornell Medical College CIRRHOSIS Definition Irreversible fibrous
CLINICAL How Should a Hospitalized Patient with Newly Diagnosed Cirrhosis Be Evaluated and Managed?
 CLINICAL How Should a Hospitalized Patient with Newly Diagnosed Cirrhosis Be Evaluated and Managed? The Hospitalist. 2016 August;2016(8) Author(s): Raj Sehgal, MD; Joshua Hanson, MD, MPH; Division OF The
CLINICAL How Should a Hospitalized Patient with Newly Diagnosed Cirrhosis Be Evaluated and Managed? The Hospitalist. 2016 August;2016(8) Author(s): Raj Sehgal, MD; Joshua Hanson, MD, MPH; Division OF The
End-Stage Liver Disease (ESLD): A Guide for HIV Physicians
 Slide 1 of 32 End-Stage Liver Disease (ESLD): A Guide for HIV Physicians Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California
Slide 1 of 32 End-Stage Liver Disease (ESLD): A Guide for HIV Physicians Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California
VARICEAL BLEEDING. Ram Subramanian MD Hepatology & Critical Care Medical Director of Liver Transplant Emory University, Atlanta.
 VARICEAL BLEEDING Ram Subramanian MD Hepatology & Critical Care Medical Director of Liver Transplant Emory University, Atlanta Disclosures: None OUTLINE Pathophysiology of portal hypertension Splanchnic
VARICEAL BLEEDING Ram Subramanian MD Hepatology & Critical Care Medical Director of Liver Transplant Emory University, Atlanta Disclosures: None OUTLINE Pathophysiology of portal hypertension Splanchnic
4/3/2014. Elizabeth Thompson, PharmD April Understand the importance of the liver and basic physiology.
 Liver Disease Elizabeth Thompson, PharmD thompse@sarmc.org April 2014 Objectives Understand the importance of the liver and basic physiology. Review hepatic disorders Recognize liver function scoring systems
Liver Disease Elizabeth Thompson, PharmD thompse@sarmc.org April 2014 Objectives Understand the importance of the liver and basic physiology. Review hepatic disorders Recognize liver function scoring systems
Evidence-Base Management of Esophageal and Gastric Varices
 Evidence-Base Management of Esophageal and Gastric Varices Rino Alvani Gani Hepatobiliary Division Department of Internal Medicine Faculty of Medicine Universitas Indonesia Cipto Mangunkusumo National
Evidence-Base Management of Esophageal and Gastric Varices Rino Alvani Gani Hepatobiliary Division Department of Internal Medicine Faculty of Medicine Universitas Indonesia Cipto Mangunkusumo National
WEEK. MPharm Programme. Liver Biochemistry. Slide 1 of 49 MPHM14 Liver Biochemistry
 MPharm Programme Liver Biochemistry Slide 1 of 49 MPHM Liver Biochemistry Learning Outcomes Assess and evaluate the signs and symptoms of illness Assess and critically appraise a patients medication regimen,
MPharm Programme Liver Biochemistry Slide 1 of 49 MPHM Liver Biochemistry Learning Outcomes Assess and evaluate the signs and symptoms of illness Assess and critically appraise a patients medication regimen,
Michele Bettinelli RN CCRN Lahey Health and Medical Center
 Michele Bettinelli RN CCRN Lahey Health and Medical Center Differentiate the types of varices Identify glue preparations utilized when treating gastric varices Review the process of glue administration
Michele Bettinelli RN CCRN Lahey Health and Medical Center Differentiate the types of varices Identify glue preparations utilized when treating gastric varices Review the process of glue administration
Gastrointestinal System: Accessory Organ Disorders
 Gastrointestinal System: Accessory Organ Disorders Mary DeLetter, PhD, RN Associate Professor Dept. of Baccalaureate and Graduate Nursing Eastern Kentucky University Disorders of Accessory Organs Portal
Gastrointestinal System: Accessory Organ Disorders Mary DeLetter, PhD, RN Associate Professor Dept. of Baccalaureate and Graduate Nursing Eastern Kentucky University Disorders of Accessory Organs Portal
Evaluating HIV Patient for Liver Transplantation. Marion G. Peters, MD Professor of Medicine University of California San Francisco USA
 Evaluating HIV Patient for Liver Transplantation Marion G. Peters, MD Professor of Medicine University of California San Francisco USA Slide 2 ESLD and HIV Liver disease has become a major cause of death
Evaluating HIV Patient for Liver Transplantation Marion G. Peters, MD Professor of Medicine University of California San Francisco USA Slide 2 ESLD and HIV Liver disease has become a major cause of death
Liver Failure. The most severe clinical consequence of liver disease is liver failure:
 Liver diseases I The major primary diseases of the liver are: - Viral hepatitis, - Nonalcoholic fatty liver disease (NAFLD), - Alcoholic liver disease, - Hepatocellular carcinoma (HCC) Hepatic damage also
Liver diseases I The major primary diseases of the liver are: - Viral hepatitis, - Nonalcoholic fatty liver disease (NAFLD), - Alcoholic liver disease, - Hepatocellular carcinoma (HCC) Hepatic damage also
ESLD a Guide for HIV Physicians. Marion Peters University of California San Francisco June 2015
 ESLD a Guide for HIV Physicians Marion Peters University of California San Francisco June 2015 Disclosures Honararia from Johnson and Johnson Roche Merck Gilead Spouse employee of Hoffman La Roche Natural
ESLD a Guide for HIV Physicians Marion Peters University of California San Francisco June 2015 Disclosures Honararia from Johnson and Johnson Roche Merck Gilead Spouse employee of Hoffman La Roche Natural
Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association
 CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
Renal Care and Liver Disease: Disease Trajectory and Hospice Eligibility
 Renal Care and Liver Disease: Disease Trajectory and Hospice Eligibility Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources/HEN Course Materials & Disclosure Course materials including
Renal Care and Liver Disease: Disease Trajectory and Hospice Eligibility Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources/HEN Course Materials & Disclosure Course materials including
The Yellow Patient. Dr Chiradeep Raychaudhuri, Consultant Hepatologist, Hull University Teaching Hospitals NHS Trust
 The Yellow Patient Dr Chiradeep Raychaudhuri, Consultant Hepatologist, Hull University Teaching Hospitals NHS Trust there s a yellow patient in bed 40. It s one of yours. Liver Cirrhosis Why.When.What.etc.
The Yellow Patient Dr Chiradeep Raychaudhuri, Consultant Hepatologist, Hull University Teaching Hospitals NHS Trust there s a yellow patient in bed 40. It s one of yours. Liver Cirrhosis Why.When.What.etc.
Entrustable Professional Activity
 Entrustable Professional Activity 1. EPA Title: Care of infants, children and adolescents with acute and chronic s 2. Description of Activity Practicing subspecialists must be trained to care for children
Entrustable Professional Activity 1. EPA Title: Care of infants, children and adolescents with acute and chronic s 2. Description of Activity Practicing subspecialists must be trained to care for children
Management of Cirrhotic Complications Uncontrolled Ascites. Siwaporn Chainuvati, MD Siriraj Hospital Mahidol University
 Management of Cirrhotic Complications Uncontrolled Ascites Siwaporn Chainuvati, MD Siriraj Hospital Mahidol University Topic Definition, pathogenesis Current therapeutic options Experimental treatments
Management of Cirrhotic Complications Uncontrolled Ascites Siwaporn Chainuvati, MD Siriraj Hospital Mahidol University Topic Definition, pathogenesis Current therapeutic options Experimental treatments
Liver Transplantation Evaluation: Objectives
 Liver Transplantation Evaluation: Essential Work-Up Curtis K. Argo, MD, MS VGS/ACG Regional Postgraduate Course Williamsburg, VA September 13, 2015 Objectives Discuss determining readiness for transplantation
Liver Transplantation Evaluation: Essential Work-Up Curtis K. Argo, MD, MS VGS/ACG Regional Postgraduate Course Williamsburg, VA September 13, 2015 Objectives Discuss determining readiness for transplantation
Upper gastrointestinal bleeding in children. Nguyễn Diệu Vinh, MD Department of Gastroenterology
 Upper gastrointestinal bleeding in children Nguyễn Diệu Vinh, MD Department of Gastroenterology INTRODUCTION Upper gastrointestinal (UGI) bleeding : arising proximal to the ligament of Treitz in the distal
Upper gastrointestinal bleeding in children Nguyễn Diệu Vinh, MD Department of Gastroenterology INTRODUCTION Upper gastrointestinal (UGI) bleeding : arising proximal to the ligament of Treitz in the distal
Program Disclosure. This program is supported by an educational grant from Salix Pharmaceuticals.
 Program Disclosure This activity has been planned and implemented in accordance with the Essential Areas and Policies of the Accreditation Council for Continuing Medical Education (ACCME) through the sponsorship
Program Disclosure This activity has been planned and implemented in accordance with the Essential Areas and Policies of the Accreditation Council for Continuing Medical Education (ACCME) through the sponsorship
JOURNAL PRESENTATION. Dr Tina Fan Tseung Kwan O Hospital 17 th Jan 2013
 JOURNAL PRESENTATION Dr Tina Fan Tseung Kwan O Hospital 17 th Jan 2013 THE COMBINATION OF OCTREOTIDE AND MIDODRINE IS NOT SUPERIOR TO ALBUMIN IN PREVENTING RECURRENCE OF ASCITES AFTER LARGE-VOLUME PARACENTESIS
JOURNAL PRESENTATION Dr Tina Fan Tseung Kwan O Hospital 17 th Jan 2013 THE COMBINATION OF OCTREOTIDE AND MIDODRINE IS NOT SUPERIOR TO ALBUMIN IN PREVENTING RECURRENCE OF ASCITES AFTER LARGE-VOLUME PARACENTESIS
Complications of Cirrhosis
 Complications of Cirrhosis Causes of Cirrhosis Alcohol Chronic Viral Hepatitis (B/C) Haemochromatosis Autoimmune Hepatitis NAFLD/NASH Primary Biliary Cirrhosis Primary Sclerosing Cholangitis 1-AT deficiency
Complications of Cirrhosis Causes of Cirrhosis Alcohol Chronic Viral Hepatitis (B/C) Haemochromatosis Autoimmune Hepatitis NAFLD/NASH Primary Biliary Cirrhosis Primary Sclerosing Cholangitis 1-AT deficiency
Yes No Unknown. Major Infection Information
 Rehospitalization Intervention Check any that occurred during this hospitalization. Pacemaker without ICD ICD Atrial arrhythmia ablation Ventricular arrhythmia ablation Cardioversion CABG (coronary artery
Rehospitalization Intervention Check any that occurred during this hospitalization. Pacemaker without ICD ICD Atrial arrhythmia ablation Ventricular arrhythmia ablation Cardioversion CABG (coronary artery
Management of Cirrhotic Patients Undergoing Non-Transplant Surgery
 Management of Cirrhotic Patients Undergoing Non-Transplant Surgery Jason S. Wakakuwa, M.D. Assistant Professor of Anesthesia Director, Transplant Anesthesia Beth Israel Deaconess Medical Center I have
Management of Cirrhotic Patients Undergoing Non-Transplant Surgery Jason S. Wakakuwa, M.D. Assistant Professor of Anesthesia Director, Transplant Anesthesia Beth Israel Deaconess Medical Center I have
הצגת מקרה- מפגש מכונים מאי 2017
 הצגת מקרה- מפגש מכונים מאי 2017 ד " ר ד נ י פ ל ד מ ן - מ כ ו ן ג ס ט ר ו ה ל ל י פ ה 2004 38 years Ethiopian F. D+4. Hepatitis and pancytopenia Type 2 DM. Etihilism. low compliance Imaging (US, CT): Cirrhosis,
הצגת מקרה- מפגש מכונים מאי 2017 ד " ר ד נ י פ ל ד מ ן - מ כ ו ן ג ס ט ר ו ה ל ל י פ ה 2004 38 years Ethiopian F. D+4. Hepatitis and pancytopenia Type 2 DM. Etihilism. low compliance Imaging (US, CT): Cirrhosis,
Dialyzing challenging patients: Patients with hepato-renal conditions
 Dialyzing challenging patients: Patients with hepato-renal conditions Nidyanandh Vadivel MD Medical Director for Living kidney Donor and Pancreas Transplant Programs Swedish Organ Transplant, Seattle Acute
Dialyzing challenging patients: Patients with hepato-renal conditions Nidyanandh Vadivel MD Medical Director for Living kidney Donor and Pancreas Transplant Programs Swedish Organ Transplant, Seattle Acute
Steps in Assessing Fibrosis 4/30/2015. Overview of Liver Disease Associated With HCV
 Overview of Liver Disease Associated With HCV Marion G. Peters, MD John V. Carbone, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco San Francisco,
Overview of Liver Disease Associated With HCV Marion G. Peters, MD John V. Carbone, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco San Francisco,
Complications of Cirrhosis
 What is Cirrhosis? Complications of Cirrhosis Paul J. Gaglio, MD Center for Liver Disease and Transplantation Columbia University College of Physicians and Surgeons NAFLD 1 PHYSICAL EXAM FINDINGS Decreased
What is Cirrhosis? Complications of Cirrhosis Paul J. Gaglio, MD Center for Liver Disease and Transplantation Columbia University College of Physicians and Surgeons NAFLD 1 PHYSICAL EXAM FINDINGS Decreased
PALLIATIVE CARE IN END-STAGE LIVER DISEASE
 PALLIATIVE CARE IN END-STAGE LIVER DISEASE Ken S. Ota, DO Family Medicine Banner Good Samaritan Medical Center Learning Objectives: Describe the common bio-psycho-social issues in end-stage liver disease
PALLIATIVE CARE IN END-STAGE LIVER DISEASE Ken S. Ota, DO Family Medicine Banner Good Samaritan Medical Center Learning Objectives: Describe the common bio-psycho-social issues in end-stage liver disease
GASTROINESTINAL BLEEDING. Dr.Ammar I. Abdul-Latif
 GASTROINESTINAL BLEEDING Dr.Ammar I. Abdul-Latif CLASSIFICATION OF G.I.BLEEDING GIB Appearance Acuity Site Apparent Acute Upper Obscure Chronic Lower UPPER&LOWER G.I.BLEEDING CAUSES OF UPPER G.I. BLEEDING
GASTROINESTINAL BLEEDING Dr.Ammar I. Abdul-Latif CLASSIFICATION OF G.I.BLEEDING GIB Appearance Acuity Site Apparent Acute Upper Obscure Chronic Lower UPPER&LOWER G.I.BLEEDING CAUSES OF UPPER G.I. BLEEDING
PACT module Acute hepatic failure. Intensive Care Training Program Radboud University Medical Centre Nijmegen
 PACT module Acute hepatic failure Intensive Care Training Program Radboud University Medical Centre Nijmegen Acute Liver Failure Acute on Chronic Liver Failure Acute loss of hepatocellular function in
PACT module Acute hepatic failure Intensive Care Training Program Radboud University Medical Centre Nijmegen Acute Liver Failure Acute on Chronic Liver Failure Acute loss of hepatocellular function in
CONTROLLED DOCUMENT. Cirrhosis Care Bundle CATEGORY: Clinical Guidelines. CLASSIFICATION: Clinical. Controlled Document CG201 Number:
 Cirrhosis Care Bundle CONTROLLED DOCUMENT CATEGORY: Clinical Guidelines CLASSIFICATION: Clinical Controlled Document CG201 Number: Version Number: 1 Controlled Document Clinical Guidelines Group Sponsor:
Cirrhosis Care Bundle CONTROLLED DOCUMENT CATEGORY: Clinical Guidelines CLASSIFICATION: Clinical Controlled Document CG201 Number: Version Number: 1 Controlled Document Clinical Guidelines Group Sponsor:
Hepatology on the AMU
 Hepatology on the AMU RCP day, 8 th February 2018 Jo Leithead Consultant in Hepatology and Liver Transplantation Addenbrookes Hospital Cambridge Is liver disease relevant to me? Williams R, Lancet 2014
Hepatology on the AMU RCP day, 8 th February 2018 Jo Leithead Consultant in Hepatology and Liver Transplantation Addenbrookes Hospital Cambridge Is liver disease relevant to me? Williams R, Lancet 2014
Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased
 1 2 3 4 5 6 7 Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased Ingestion of Caustic Substances Poor Bowel Habits
1 2 3 4 5 6 7 Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased Ingestion of Caustic Substances Poor Bowel Habits
Alzheimer s Disease, Dementia, Related Disorders
 Alzheimer s Disease, Dementia, Related Disorders Stage 7 on the FAST Scale signifies the threshold of activity limitation that would support a six-month prognosis. The FAST Scale does not address the impact
Alzheimer s Disease, Dementia, Related Disorders Stage 7 on the FAST Scale signifies the threshold of activity limitation that would support a six-month prognosis. The FAST Scale does not address the impact
CrackCast Episode 28 Jaundice
 CrackCast Episode 28 Jaundice Episode overview: 1) Describe heme metabolism 2) List common pre-hepatic/hepatic/post-hepatic causes of jaundice Wisecracks: 1) What are clinical signs of liver disease? 2)
CrackCast Episode 28 Jaundice Episode overview: 1) Describe heme metabolism 2) List common pre-hepatic/hepatic/post-hepatic causes of jaundice Wisecracks: 1) What are clinical signs of liver disease? 2)
APPROPRIATE PATIENT SELECTION AS A KEY TO INCREASE THE BENEFIT/RISK RATIO FOR ELAD
 APPROPRIATE PATIENT SELECTION AS A KEY TO INCREASE THE BENEFIT/RISK RATIO FOR ELAD Ram Subramanian M.D. Hepatology and Critical Care Emory University School of Medicine Atlanta, USA OUTLINE Review the
APPROPRIATE PATIENT SELECTION AS A KEY TO INCREASE THE BENEFIT/RISK RATIO FOR ELAD Ram Subramanian M.D. Hepatology and Critical Care Emory University School of Medicine Atlanta, USA OUTLINE Review the
PORTAL HYPERTENSION. Tianjin Medical University LIU JIAN
 PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
British Society of Gastroenterology. St. Elsewhere's Hospital. National Comparative Audit of Blood Transfusion
 British Society of Gastroenterology UK Com parat ive Audit of Upper Gast roint est inal Bleeding and t he Use of Blood Transfusion Extract December 2007 St. Elsewhere's Hospital National Comparative Audit
British Society of Gastroenterology UK Com parat ive Audit of Upper Gast roint est inal Bleeding and t he Use of Blood Transfusion Extract December 2007 St. Elsewhere's Hospital National Comparative Audit
Primary Prophylaxis against Variceal Hemorrhage Pharmacotherapy vs Endoscopic Band Ligation
 Primary Prophylaxis against Variceal Hemorrhage Pharmacotherapy vs Endoscopic Band Ligation Siwaporn Chainuvati, MD Faculty of Medicine Siriraj Hospital Outline Natural history of esophageal varices Which
Primary Prophylaxis against Variceal Hemorrhage Pharmacotherapy vs Endoscopic Band Ligation Siwaporn Chainuvati, MD Faculty of Medicine Siriraj Hospital Outline Natural history of esophageal varices Which
Update in abdominal Surgery in cirrhotic patients
 Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
Cirrhosis Patient Teaching Information
 Cirrhosis Patient Teaching Information CIRRHOSIS What is Cirrhosis: Cirrhosis is the end stages of a liver disease. Over time, from years to decades, fibrosis (or scar tissue) progresses through stages
Cirrhosis Patient Teaching Information CIRRHOSIS What is Cirrhosis: Cirrhosis is the end stages of a liver disease. Over time, from years to decades, fibrosis (or scar tissue) progresses through stages
Ascites Management. Atif Zaman, MD MPH Oregon Health & Science University Professor of Medicine Division of Gastroenterology and Hepatology
 Ascites Management Atif Zaman, MD MPH Oregon Health & Science University Professor of Medicine Division of Gastroenterology and Hepatology Disclosure 1. The speaker Atif Zaman, MD MPH have no relevant
Ascites Management Atif Zaman, MD MPH Oregon Health & Science University Professor of Medicine Division of Gastroenterology and Hepatology Disclosure 1. The speaker Atif Zaman, MD MPH have no relevant
Portal hypertension is the main complication of cirrhosis
 GASTROENTEROLOGY 2001;120:726 748 Current Management of the Complications of Cirrhosis and Portal Hypertension: Variceal Hemorrhage, Ascites, and Spontaneous Bacterial Peritonitis GUADALUPE GARCIA TSAO
GASTROENTEROLOGY 2001;120:726 748 Current Management of the Complications of Cirrhosis and Portal Hypertension: Variceal Hemorrhage, Ascites, and Spontaneous Bacterial Peritonitis GUADALUPE GARCIA TSAO
Denver Shunts vs TIPS for Ascites
 Denver Shunts vs TIPS for Ascites Hooman Yarmohammadi MD Assistant Professor of Radiology Interventional Radiology & Image Guided Therapies Memorial Sloan-Kettering Cancer Center, New York, USA Hooman
Denver Shunts vs TIPS for Ascites Hooman Yarmohammadi MD Assistant Professor of Radiology Interventional Radiology & Image Guided Therapies Memorial Sloan-Kettering Cancer Center, New York, USA Hooman
New Strategies in the Management of Patients with Severe Sepsis
 New Strategies in the Management of Patients with Severe Sepsis Michael Zgoda, MD, MBA President, Medical Staff Medical Director, ICU CMC-University, Charlotte, NC Factors of increases in the dx. of severe
New Strategies in the Management of Patients with Severe Sepsis Michael Zgoda, MD, MBA President, Medical Staff Medical Director, ICU CMC-University, Charlotte, NC Factors of increases in the dx. of severe
REVIEW. Ariel W. Aday, M.D.,* Nicole E. Rich, M.D.,* Arjmand R. Mufti, M.D., and Shannan R. Tujios, M.D.
 REVIEW CON ( The Window Is Closed ): In Patients With Cirrhosis With Ascites, the Clinical Risks of Nonselective beta-blocker Outweigh the Benefits and Should NOT Be Prescribed Ariel W. Aday, M.D.,* Nicole
REVIEW CON ( The Window Is Closed ): In Patients With Cirrhosis With Ascites, the Clinical Risks of Nonselective beta-blocker Outweigh the Benefits and Should NOT Be Prescribed Ariel W. Aday, M.D.,* Nicole
Terlipressin: An Asset for Hepatologists!
 DIAGNOSTIC AND THERAPEUTIC ADVANCES IN HEPATOLOGY Terlipressin: An Asset for Hepatologists! S.K. Sarin and Praveen Sharma One Case Scenario A 48-year-old male with alcoholic cirrhosis who was abstinent
DIAGNOSTIC AND THERAPEUTIC ADVANCES IN HEPATOLOGY Terlipressin: An Asset for Hepatologists! S.K. Sarin and Praveen Sharma One Case Scenario A 48-year-old male with alcoholic cirrhosis who was abstinent
Management of Ascites and Hepatorenal Syndrome. Florence Wong University of Toronto. June 4, /16/ Gore & Associates: Consultancy
 Management of Ascites and Hepatorenal Syndrome Florence Wong University of Toronto June 4, 2016 6/16/2016 1 Disclosures Gore & Associates: Consultancy Sequana Medical: Research Funding Mallinckrodt Pharmaceutical:
Management of Ascites and Hepatorenal Syndrome Florence Wong University of Toronto June 4, 2016 6/16/2016 1 Disclosures Gore & Associates: Consultancy Sequana Medical: Research Funding Mallinckrodt Pharmaceutical:
-Cardiogenic: shock state resulting from impairment or failure of myocardium
 Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
EDUCATION PRACTICE. Management of Refractory Ascites. Clinical Scenario. The Problem
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1187 1191 EDUCATION PRACTICE Management of Refractory Ascites ANDRÉS CÁRDENAS and PERE GINÈS Liver Unit, Institute of Digestive Diseases, Hospital Clínic,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1187 1191 EDUCATION PRACTICE Management of Refractory Ascites ANDRÉS CÁRDENAS and PERE GINÈS Liver Unit, Institute of Digestive Diseases, Hospital Clínic,
Acute Liver Failure: Supporting Other Organs
 Acute Liver Failure: Supporting Other Organs Michael A. Gropper, MD, PhD Professor of Anesthesia and Physiology Director, Critical Care Medicine University of California San Francisco Acute Liver Failure
Acute Liver Failure: Supporting Other Organs Michael A. Gropper, MD, PhD Professor of Anesthesia and Physiology Director, Critical Care Medicine University of California San Francisco Acute Liver Failure
Liver Disease. By: Michael Martins
 Liver Disease By: Michael Martins Recently I have been getting a flurry of patients that have some serious liver complications. This week s literature review will be the dental management of the patients
Liver Disease By: Michael Martins Recently I have been getting a flurry of patients that have some serious liver complications. This week s literature review will be the dental management of the patients
Definition: HPS is a disease process with a triad of: 1- Liver disease. 2- Widespread intrapulmonary vasodilatation. 3- Gas exchange abnormality prese
 Hepatopulmonary syndrome (HPS) By Alaa Haseeb, MS.c Definition: HPS is a disease process with a triad of: 1- Liver disease. 2- Widespread intrapulmonary vasodilatation. 3- Gas exchange abnormality presenting
Hepatopulmonary syndrome (HPS) By Alaa Haseeb, MS.c Definition: HPS is a disease process with a triad of: 1- Liver disease. 2- Widespread intrapulmonary vasodilatation. 3- Gas exchange abnormality presenting
RENAL & HEMATOLOGY EMERGENCIES JEFF SIMONS B.S. F-PC
 RENAL & HEMATOLOGY EMERGENCIES JEFF SIMONS B.S. F-PC GOALS Overview of renal system anatomy / physiology Discuss common medical / trauma renal issues Identify associated assessment keys GOALS Introduction
RENAL & HEMATOLOGY EMERGENCIES JEFF SIMONS B.S. F-PC GOALS Overview of renal system anatomy / physiology Discuss common medical / trauma renal issues Identify associated assessment keys GOALS Introduction
BETA-BLOCKERS IN CIRRHOSIS.PRO.
 BETA-BLOCKERS IN CIRRHOSIS.PRO. Angela Puente Sánchez. MD PhD Hepatology Unit. Gastroenterology department Marques de Valdecilla University Hospital. Santander INTRODUCTION. Natural history of cirrhosis
BETA-BLOCKERS IN CIRRHOSIS.PRO. Angela Puente Sánchez. MD PhD Hepatology Unit. Gastroenterology department Marques de Valdecilla University Hospital. Santander INTRODUCTION. Natural history of cirrhosis
Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE
 Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE In critically ill patients: too little fluid Low preload,
Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE In critically ill patients: too little fluid Low preload,
Pharmacology in Liver Disease. Sandeep Whitehead Advanced Clinical Pharmacist Hepatology and Liver Transplant
 Pharmacology in Liver Disease Sandeep Whitehead Advanced Clinical Pharmacist Hepatology and Liver Transplant Objectives Outline the drug management for patients with: Ascites Spontaneous Bacterial Peritonitis
Pharmacology in Liver Disease Sandeep Whitehead Advanced Clinical Pharmacist Hepatology and Liver Transplant Objectives Outline the drug management for patients with: Ascites Spontaneous Bacterial Peritonitis
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 26.1 Define key terms introduced in this chapter. Slides 13 14, 21 22, 24 26, 31 26.2 Describe the structure and function of the hematologic system.
Introduction to Emergency Medical Care 1 OBJECTIVES 26.1 Define key terms introduced in this chapter. Slides 13 14, 21 22, 24 26, 31 26.2 Describe the structure and function of the hematologic system.
Chapter 26 - Hematologic_and_Renal_Emergencies
 Introduction to Emergency Medical Care 1 OBJECTIVES 26.1 Define key terms introduced in this chapter. Slides 13 14, 21 22, 24 26, 31 26.2 Describe the structure and function of the hematologic system.
Introduction to Emergency Medical Care 1 OBJECTIVES 26.1 Define key terms introduced in this chapter. Slides 13 14, 21 22, 24 26, 31 26.2 Describe the structure and function of the hematologic system.
Determining Eligibility for Hospice Care
 Determining Eligibility for Hospice Care Main Number: 203 739-8300 Toll Free Number: 888 357-3334 www.regionalhospicect.org Many people may not understand all that Regional Hospice can offer or they are
Determining Eligibility for Hospice Care Main Number: 203 739-8300 Toll Free Number: 888 357-3334 www.regionalhospicect.org Many people may not understand all that Regional Hospice can offer or they are
Hepatorenal Syndrome
 Necker Seminars in Nephrology Institut Pasteur Paris, April 22, 2013 Hepatorenal Syndrome Dr. Richard Moreau 1 INSERM U773, Centre de Recherche Biomédicale Bichat-Beaujon CRB3, 2 Université Paris Diderot
Necker Seminars in Nephrology Institut Pasteur Paris, April 22, 2013 Hepatorenal Syndrome Dr. Richard Moreau 1 INSERM U773, Centre de Recherche Biomédicale Bichat-Beaujon CRB3, 2 Université Paris Diderot
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute variceal bleeding management of, 251 262 balloon tamponade of esophagus in, 257 258 endoscopic therapies in, 255 257. See also Endoscopy,
Index Note: Page numbers of article titles are in boldface type. A Acute variceal bleeding management of, 251 262 balloon tamponade of esophagus in, 257 258 endoscopic therapies in, 255 257. See also Endoscopy,
Ontario s Adult Referral and Listing Criteria for Liver Transplantation
 Ontario s Adult Referral and Listing Criteria for Liver Transplantation Version 3.0 Trillium Gift of Life Network Ontario s Adult Referral & Listing Criteria for Liver Transplantation PATIENT REFERRAL
Ontario s Adult Referral and Listing Criteria for Liver Transplantation Version 3.0 Trillium Gift of Life Network Ontario s Adult Referral & Listing Criteria for Liver Transplantation PATIENT REFERRAL
Objectives 2/11/2016 HOSPICE 101
 HOSPICE 101 Overview Hospice History and Statistics What is Hospice? Who qualifies for services? Levels of Service The Admission Process Why Not to Wait Objectives Understand how to determine hospice eligibility
HOSPICE 101 Overview Hospice History and Statistics What is Hospice? Who qualifies for services? Levels of Service The Admission Process Why Not to Wait Objectives Understand how to determine hospice eligibility
On-Call Upper GI Bleeding. Upper Gastrointestinal Bleeding
 On-Call Upper GI Bleeding John R Saltzman MD, FACG Director of Endoscopy Brigham and Women s Hospital Associate Professor of Medicine Harvard Medical School Upper Gastrointestinal Bleeding 300,000000 hospitalizations/year
On-Call Upper GI Bleeding John R Saltzman MD, FACG Director of Endoscopy Brigham and Women s Hospital Associate Professor of Medicine Harvard Medical School Upper Gastrointestinal Bleeding 300,000000 hospitalizations/year
