Transnasal endoscopic approach in the treatment of Graves ophthalmopathy: The value of a medial periorbital strip
|
|
|
- Alfred Ryan
- 6 years ago
- Views:
Transcription
1 European Annals of Otorhinolaryngology, Head and Neck diseases (2010) 127, ORIGINAL CLINICAL RESEARCH Transnasal endoscopic approach in the treatment of Graves ophthalmopathy: The value of a medial periorbital strip M.-A. Jimenez-Chobillon a,, R.-D. Lopez-Oliver b a Otolaryngology Department, National Institute of Respiratory Diseases Ismael Cosío Villegas, Calzada de Tlalpan 4502 Col. Sección XVI, Delegación Tlalpan, Mexico, Mexico b Ophtalmology Service, General Hospital Dr. Manuel Gea González, Mexico, Mexico Available online 20 May 2010 KEYWORDS Graves disease; Orbitopathy; Orbit decompression; Endoscopic Summary Objectives: Present our experience with orbital decompression using an endoscopic transnasal approach and test whether preservation of an anteroposterior periorbital strip overlying the medial rectus muscle can reduce the incidence of postoperative diplopia. Patient and methods: Retrospective, descriptive study conducted on 16 patients with Graves ophthalmopathy operated on with orbital decompression between 2004 and Results: Twelve women and four men (mean age, 34.6 years), a total of 30 orbits, were operated. A medial periorbital strip along the medial rectus muscle was preserved in 13 patients. A single case (7.7%) presented postoperative diplopia. The mean reduction of proptosis was 4.3 mm. Conclusions: The endoscopic transnasal approach provides comparable results to those obtained with other techniques. The incidence of postoperative diplopia seems to decrease when an anteroposterior periorbital periosteal strip is preserved along the medial rectus muscle Elsevier Masson SAS. All rights reserved. Introduction Graves ophthalmopathy is characterized by eyelid retraction, infiltrating ophthalmopathy and compressive ophthal- Work presented at the 116th Congress of the Société Française d Otorhinolaryngologie et de Chirurgie de la Face et du Cou, 6 October 2009 in Paris. Corresponding author. address: aljicho@gmail.com (M.-A. Jimenez-Chobillon). mopathy, which generally occur simultaneously with various degrees of severity [1]. Treatment is not systematically surgical, because certain patients present a favorable response to medical treatment combining corticosteroids and radiotherapy [2]. Decompressive surgery is usually reserved for Graves ophthalmopathy that is refractory to medical treatment. Its indications include exophthalmia, corneal ulcer, compressive neuropathy, ophthalmoplegia, and esthetic considerations [3]. All techniques seek to reposition the bony limits of the orbital wall [4] or reduce the volume /$ see front matter 2010 Elsevier Masson SAS. All rights reserved. doi: /j.anorl
2 98 M.-A. Jimenez-Chobillon, R.-D. Lopez-Oliver of the soft tissues contained in this cavity by fat removal [3,5,6]. Today, the endoscopic transnasal approach is one of the most frequently used for orbital decompression. Exposure of the medial wall of the orbit after endoscopic ethmoidectomy makes it possible to completely remove the lamina papyracea. The medial portion of the orbital floor and the optic nerve at the apex are also easily decompressed [7]. The functional and esthetic results obtained are generally at least as good as those obtained with external techniques. Therefore, the otorhinolaryngologist now takes part in the multidisciplinary management of this disease once reserved for the ophthalmologist and the endocrinologist. One of the most frequent complications of orbital decompression is postoperative diplopia, occurring in 20 [8] to 63% [9] of cases depending on the series. Certain authors do not consider it an actual complication, given its frequency. However, certain cases of diplopia will need to be treated surgically, and the surgeon should inform the patient of this possibility. To reduce the incidence of postoperative diplopia as much as possible, a variety of surgical techniques have been presented in the medical literature. Metson and Samaha propose preserving a medial periorbital strip along the medial rectus muscle and present excellent results [9]. This study aimed not only to present the results on a series of patients who had undergone orbital decompression via an isolated endoscopic approach, or combined with an external approach, but also to confirm the value of preserving a medial periorbital strip to reduce the incidence of postoperative diplopia. Patients and methods The files of all the patients presenting Graves ophthalmopathy who had been operated by endoscopic transnasal approach for excision of the medial orbital wall between December 2004 and February 2009 were analyzed retrospectively. The independent variables studied were sex, age, duration of postoperative follow-up, uni- or bilateral orbital involvement, whether or not a medial strip of orbital periosteum was preserved along the course of the medial rectus muscle, and whether or not the orbital floor was excised. The dependent variables sought were pre- and postoperative measurements obtained with Hertel exophthalmometry for each orbit operated on and the presence or absence of pre- and/or postoperative diplopia. The values obtained with exophthalmometry were considered normal between 14 and 21 mm [10]. Exophthalmia was considered mild with values between 21 and 24 mm and moderate to severe for any value above 24 mm [3]. In all cases, diplopia, ocular motricity and the degree of infiltration of the extraocular muscles were assessed by the ophthalmologist, but only the presence or absence of diplopia was described and retained as a variable in the study. The postoperative complications and the pre- and postoperative visual fields were also noted. Except for diplopia, which depends directly on the simultaneous action of both eyes, the rest of the data were analyzed in relation to the total number of orbits operated and not on the number of patients, because of the individual and independent behavior of each orbital unit. Finally, our results were compared with those reported by various series reported in the relevant literature. Surgical technique Except for preservation of the medial periorbital strip in certain patients, the same surgical technique was used under general anesthesia for all patients. An external infiltration of the supraorbital, supratrochlear, and infraorbital nerves was performed at the beginning of the intervention with a Xylocaine 2% solution with adrenaline 1:100,000, and tamponading of the nasal fossa was done with dressings soaked in a 0.05% oxymetazoline solution, which were removed after 10 min. Dissection of the ethmoid was begun using the 0-degree endoscopic lens, by resecting the anterior and posterior ethmoid cells. The base of the skull was identified and followed between the lamina papyracea and the conchal lamina as landmarks for the rest of the dissection. The agger nasi cell and the upper portion of the uncinate process were resected near the frontal recess, but the latter structure was preserved intact along with its mucosal lining. After ethmoid dissection (or before depending on the surgeon s decision), a middle meatotomy is performed. It should be large enough to prevent its obliteration with the orbital fat and thus avoid maxillary sinusitis. Then a large sphenoidotomy is made to join the lateral wall of the sphenoidal sinus and the lamina papyracea. Once this has been achieved, resection of the medial wall of the orbit is begun using a sickle knife, then continued with a Freer dissector and a Blakesley forceps, taking care to resect all of this structure up to the sphenoethmoidal union and the orbital apex. The bone resection stops below the frontal recess, preserving the lamina papyracea and the lacrimal bone at this level. Finally, the medial portion of the orbital floor is resected in the same way as the medial orbital wall. Once the periorbit has been exposed along the entire length of the ethmoid, a superior horizontal incision is made parallel to the base of the skull. A similar incision is carried 1 cm below and parallel to the first one, thus retaining an anteroposterior medial fringe of periosteum along the course of the medial rectus muscle (Fig. 1). After a light massage on the ocular globe so that the adipose tissue will partially occupy the dissected ethmoid, a partial lipectomy is performed with thin Blakesley forceps, while monitoring any substantial movement of the globe that could indicate direct traction on the medial rectus muscle. If necessary, the procedure is completed by enlarged excision of the orbital floor via an external approach. In this case, a transconjunctival or subciliary incision is made at the lower eyelid. After dissection of the orbicular muscle, the orbital septum is identified and followed on its anterior side up to the orbital ridge. Here, the periosteum is incised and lifted back, exposing the bone of the orbital floor. With a thin chisel, a fenestration is made on each side of the infraorbital nerve toward the maxillary sinus, so that the bony floor can be removed with bone-cutting Kerrison forceps. Medially, the dissection is carried toward the middle
3 Transnasal endoscopic approach in the treatment of Graves ophthalmopathy 99 maxillary sinus. When a transconjunctival incision is made, it is not closed. On the other hand, the subciliary incision is sutured with a continuous, nonresorbable suture. Nasal packing is not required unless substantial postoperative bleeding is present. Postoperative care Nasal lavages with saline solution and antalgics are initiated during the 1st postoperative day. Cold compresses are regularly placed on the eyelids for the first 24 h and eyedrops combining a corticosteroid and an antibiotic are instilled three times a day for 1 week. Per os antibiotics are only prescribed for patients requiring nasal tamponing. The patient is seen in consultation on the 3rd day and every week thereafter until satisfactory healing is achieved. Results Figure 1 Illustration showing orbital periosteal incisions with medial periosteal strip. C: cavum; IT: inferior turbinate; MS: maxillary sinus; SS: sphenoid sinus; ER: ethmoid roof; MPB: medial periosteal strip. meatus; laterally, it reaches the zygomatic angle. Finally, the bony canal of the infraorbital nerve is dissected and raised with a periosteal elevator, and the inferior orbital periosteum is opened via two or three anteroposterior incisions to allow prolapsus of the orbital fat into the Twelve women (75%) and four men (25%) between 21 and 61 years of age were operated. Two cases (12.5%) were operated on one side and 14 (87.5%) on both sides. A total of 30 orbits were operated. The duration of the postoperative follow-up was 6 36 months. The two cases of unilateral involvement were both men, in each case involving the left eye. In one of the unilateral cases, the orbital floor was not excised by the external approach because the endoscopic excision of the medial wall was sufficient. For the 29 remaining orbits, endoscopic transnasal resection of the medial wall was associated with resection of the orbital floor via the external subciliary or transconjunctival approach, depending on the surgeon s preference. Five orbits (16.7%) in our first three patients were operated without a periorbital medial strip on the medial Table 1 Pre- and postoperative exophthalmometric measurements (mm) obtained for each patient and each eye. Patient Right eye Left eye Preoperative Postoperative Follow-up Preoperative Postoperative Follow-up No No No No No Mean The Follow-up columns show the reduction in exophthalmia. No: not operated.
4 100 M.-A. Jimenez-Chobillon, R.-D. Lopez-Oliver Table 2 Relation between preservation of the medial periorbital strip and the presence of pre- and postoperative diplopia for each case. Patient Preserved periorbital strip Diplopia Right eye Left eye Preoperative Postoperative 1 No No No No 2 Not operated No No No 3 No No No Yes a 4 Yes Yes No No 5 Yes Yes No No 6 Yes Yes No No 7 Yes Yes No No 8 Yes Yes No No 9 Yes Yes No Yes a 10 Yes Yes No No 11 Yes Yes No No 12 Yes Yes No No 13 Yes Yes No No 14 Not operated Yes No No 15 Yes Yes No No 16 Yes Yes Yes a Yes a a Presence of diplopia. rectus muscle. The 25 following orbits (83.3%) underwent this preservation technique. Fifteen orbits presented slight proptosis and the 15 remaining orbits moderate or severe proptosis. The postoperative proptosis reduction was a mean 4.3 mm (Table 1), ranging from 2 to 8 mm. Three patients (18.7%) presented postoperative diplopia; one of them (6.2%) presented diplopia before surgery, which remained after the intervention. Of the 13 patients in whom the periorbital medial strip was preserved, a single patient (7.7%) presented diplopia caused by the operation. One case of postoperative diplopia occurred in one of the three patients (33.3%) who had not been treated with this technique (Table 2). Other postoperative complications were noted: presence of synechiae in four cases, including one bilateral (five ethmoids), malar hypesthesia after excision of the orbital floor in one case, unilateral postoperative epistaxis in one case, and one case of left frontoethmoid mucocele. No cases of meningeal rupture were noted. In all the patients, the visual fields were measured preand postoperatively. Eleven cases presented compressive neuropathy of the optic nerve, which improved in all cases after the surgery. The five patients who did not present alterations of the visual fields underwent surgery for purely esthetic reasons. Of the three patients who presented diplopia, two were operated on by a strabismus specialist and the third refused additional surgical treatment. All the patients were discharged from the hospital within 24 h of the intervention. Discussion Our series is comparable to most of those published in the literature, both in terms of its demographic data and its results. The various studies show that approximately 70% of affected patients are female [6,8,11], similar to the percentage reported in the present series (75%). However, the mean age of our patients was 34.6 years, whereas other authors reported means of 46.6 [8] and 49 years [11], which suggests that overall our patients were younger. The two cases of unilateral involvement presented in men, both on the left side. Other authors studying Graves exophthalmia did not find this male predominance or laterality [12,13]. The most important objective of the surgical treatment for Graves ophthalmopathy remains preserving vision. Blindness can result from elevation of intraorbital pressure with compression of the optic nerve. For this reason, we prefer endoscopic transnasal resection of the medial wall of the orbit, which allows easy decompression of the optic nerve at the orbital apex [7]. Moreover, it can be noted that our results on the compressive component of the ophthalmopathy are satisfactory, with all patients who presented altered visual fields showing clear functional recuperation after the intervention. Reduction of the exophthalmia is also as important as the optic nerve decompression, since proptosis of the globe can result in corneal ulcer and esthetic sequelae. In some cases, endoscopic excision of the medial wall and the medial portion of the orbital floor seems sufficient for treating exophthalmia [7]. However, in our series, only one case was resolved via a purely endoscopic approach; the others had to undergo a combined procedure with excision of the orbital floor via the external approach. This suggests that excision of several walls is often necessary to obtain good results, but also that the medial strip of orbital periosteum, kept intact in most of our cases, could be a limitation to the reduction of ocular globe protrusion during decompression. On the other hand, we observed that the mean regression of the exophthalmia obtained in our patients is comparable to what has been obtained by other authors who did not preserve this periosteal strip and who also resected
5 Transnasal endoscopic approach in the treatment of Graves ophthalmopathy 101 Table 3 Comparison of the means of reduced exophthalmia obtained for each author with the orbital walls resected and preservation or not of the medial strip of orbital periosteum. Author Resected orbital walls MSP Reduced proptosis Medial ½ Floor Floor Lateral Kennedy X X 4.7 Kasperbauer et al. X X 2.5 a Schaefer X X 3.65 Silver et al. 1 X X 4.37 Silver et al. 2 X X X 4.59 Sellari-Franceschini et al. X X 5.3 Cansiz et al. 1 X X 4.38 Cansiz et al. 2 X X X 7.75 a Bailey et al. X X X 5 Metson and Samaha X If necessary X 5.1 MEAN 4.73 Jiménez and López X X X 4.3 Our results are reported in the Jiménez et López. row. ½ floor, medial portion of the floor; MSP, medial strip of orbital periosteum. a The lower mean was obtained with excision limited to the medial wall of the orbit with the medial portion of the orbital floor, whereas the higher mean was obtained with resection of the medial, inferior, and lateral walls. two, sometimes three, orbital walls [7,14,15] (Table 3). Metson and Samaha reported a mean 5-mm reduction of exophthalmia, ranging from 4 to 7.5 mm, despite preservation of this orbital periosteal strip [9], whereas Schaefer et al. obtained a lower mean (3.65 mm) after excising the medial and inferior medial walls while not preserving the periosteal strip [15]. This allowed us to confirm that the medial periosteal strip does not seem to seriously limit the reduction of exophthalmia. In most series, substantial variations in the results obtained on exophthalmia reduction were reported [8,9,16]. The same phenomenon was found in our series, with a reduction of proptosis ranging from 2 to 8 mm. Cansiz et al. reported comparable ranges, from 3 to 7 mm for the group of patients who underwent excision of two orbital walls (medial and inferior), and from 5 to 12 mm when three orbital walls were excised (medial, inferior, and lateral) [17]. This would seem to justify excision of three walls for the most severe cases of exophthalmia. The results of a study by Silver et al., however, did not follow the same direction in that they reported a reduction of exophthalmia ranging from 0.5 to 8 mm for decompression of two orbital walls and a nearly identical variation ranging from 1 to 8 mm for decompression combining three walls [16]. In our series, the excision of the lateral wall was not required in any of the cases. It is also important to remember that reduction of exophthalmia is not solely dependent on the surgical technique used or the number of walls resected, but also in large part on the degree of fibrosis and infiltration of the orbit s soft tissues, notably around the extraocular muscles, which may explain the variability of the surgical results obtained in all of the series reviewed [11]. In our series, we chose to combine excision of the orbital floor via the external approach with excision of the medial wall, particularly in view of our experience in each of these techniques. This combination is associated with low morbidity, shorter hospital stays, fewer complications, and excellent recuperation of visual function in most cases [15]. It should be noted that all our patients were discharged from hospital in the first 24 h after surgery and that the complications presented were minor. In most series, diplopia is the most frequent complication in orbital decompressions [9], explaining why several techniques have been proposed to reduce its incidence. For example, some authors propose balanced orbital decompression of the medial and lateral walls, while the orbital floor is preserved to prevent inferior displacement of the globe [8,16]. This technique seems to reduce the incidence of postoperative diplopia. However, in a series of 13 patients, Kacker et al. reported 15.35% diplopia after this intervention [18]. Other studies report good results with preservation of a horizontal bony bridge at the angle of the medial and inferior walls of the ocular globe, attempting to prevent its inferomedial displacement [14,19], even though the preservation of this bony bridge presents certain difficulties [9], and Wright et al. only managed to preserve it in 71% of their cases, with their series nevertheless reporting 18% diplopia [20]. In this context, Metson and Samaha propose to preserve the anteroposterior strip of orbital periosteum along the course of the medial rectus muscle to prevent convergent strabismus and the resulting diplopia [9]. The technique is much simpler and the results are very encouraging because, in a series of 13 patients and 20 orbits operated, they report no cases of diplopia. These results have motivated us to use this technique. Of 13 patients operated preserving the medial strip of orbital periosteum, only one (7.7%) presented diplopia. However, our group of patients and our experience remain modest; prospective and comparative studies with larger groups would be necessary for definitive conclusions to be drawn. The appearance of synechiae is the most frequent complication of ethmoid surgery and we have observed
6 102 M.-A. Jimenez-Chobillon, R.-D. Lopez-Oliver this in five ethmoids (16.7%) on the operated sides. Even if the limited number of cases makes it impossible to carry out a multivariate analysis, there is a clear trend toward forming synechiae in narrow ethmoids given that the operative reports describe this anatomical variant in three of the four patients who presented this complication. The appearance of mucoceles is also classical after orbital decompression [21]. The case observed in our series accounts for 3.3% of the ethmoids operated and is also associated with the presence of ipsilateral synechiae and a narrow ethmoid. This patient was reoperated and the mucocele was marsupialized in the nasal fossa with no complications. The case of malar hypesthesia reported is undoubtedly related to excision of the bony conduit of the infraorbital nerve during excision of the inferior wall of the orbit. This complication is more frequent when the orbital floor approach is reached using a transmaxillary approach [22,23]. Carrasco et al. report that the incidence of postoperative malar hypesthesia after excision of the orbital floor via the transmaxillary approach is 46%, while it decreases to 6.1% when using the transconjunctival approach [22]. In our series, this accounted for only 3.4% of the cases (one case out of 29 resected orbital floors). It is also important to note that we found no cases of meningeal rupture. This complication can be present particularly during decompression of the lateral orbital wall, near the inferior orbital fissure and the middle cranial fossa [8], or during excision of the medial wall toward the orbital apex [11]. Conclusion The endoscopic transnasal approach allows complete excision of the medial wall of the orbit in excellent conditions and better access to the orbital apex. It, therefore, makes it possible to treat not only exophthalmia, but also compressive neuropathy. Combined with resection of the orbital floor via the external subciliary or transconjunctival approach, this technique provides results that are at least as good as those obtained with other techniques, with reduced morbidity. The incidence of postoperative diplopia seems to decrease when a horizontal anteroposterior strip of orbital periosteum is retained along the medial rectus muscle, a simple procedure that can be performed by a trained surgeon. Conflict of interest statement None. References [1] El-Kaissi S, Frauman AG, Wall JR. Thyroid-associated ophthalmopathy: a practical guide to classification, natural history and management. Intern Med J 2004;34: [2] Stiebel-Kalish H, Robenshtok E, Hasanreisoglu M, Ezrachi D, Shimon I, Leibovici L. Treatment modalities for Graves ophthalmopathy: systematic review and meta-analysis. J Clin Endocrinol Metab 2009;94: [3] Chiarelli A. The plastic surgeon and Graves disease. Ann Ital Chir 2004;75: [4] Liberatore LA, Anand VK. Orbital decompression for Graves orbitopathy using a combined endoscopic and Caldwell- Luc approach. Oper Tech Otolaryngol Head Neck Surg 1996;7: [5] Adenis JP, Camezind P, Robert PY. Is incidence of diplopia after fat removal orbital decompression a predictive factor of choice of surgical technique for Graves ophthalmopathy? Bull Acad Natl Med 2003;187: [6] Robert PY, Rivas M, Camezind P. Decrease of intraocular pressure after fat-removal orbital decompression in Graves disease. Ophtal Plast Reconstr Surg 2006;22:92 5. [7] Kennedy DW, Goodstein ML, Miller NR, Zinreich SJ. Endoscopic transnasal orbital decompression. Arch Otolaryngol Head Neck Surg 1990;116: [8] Sellari-Franceschini S, Berrettini S, Santoro A, et al. Orbital decompression in Graves ophthalmopathy by medial and lateral wall removal. Otolaryngol Head Neck Surg 2005;133: [9] Metson R, Samaha M. Reduction of diplopia following endoscopic orbital decompression: the orbital strip technique. Laryngoscope 2002;112: [10] Sacks EH, Anand VJ, Lisman RD. Orbital decompression: endoscopic perspective. In: Anand VJ, Panje W, editors. Practical endoscopic sinus surgery. New York, NY: McGraw Hill; p [11] Kasperbauer JL, Hinkley L. Endoscopic orbital decompression for Graves ophthalmopathy. Am J Rhinol 2005;19: [12] Kendler DL, Lippa J, Rootman J. The initial clinical characteristics of Graves orbitopathy vary with age and sex. Arch Ophtalmol 1993;111: [13] Daumerie CH, Duprez T, Boschi A. Long-term multidisciplinary follow-up of unilateral thyroid-associated orbitopathy. Eur J Intern Med 2008;19: [14] Goldberg RA, Shorr N, Cohen MS. The medial orbital strut in the prevention of postdecompression dystopia in dysthyroid ophthalmopathy. Ophthalmol Plast Reconstr Surg 1992;8: [15] Schaefer SD, Soliemanzadeh P, Della Rocca DA, et al. Endoscopic and transconjunctival orbital decompression for thyroid-related orbital apex compression. Laryngoscope 2003;113: [16] Silver RD, Harrison AR, Goding GS. Combined endoscopic medial and external lateral orbital decompression for progressive thyroid eye disease. Otolaryngol Head Neck Surg 2006;134: [17] Cansiz H, Yilmaz S, Karaman E, et al. Three-wall orbital decompression superiority to 2-wall orbital decompression in thyroid-associated ophthalmopathy. J Oral Maxillofac Surg 2006;64: [18] Kacker A, Kazim M, Murphy M. Balanced orbital decompression for severe Graves orbitopathy: technique with treatment algorithm. Otolaryngol Head Neck Surg 2003;128: [19] Bailey KL, Tower RN, Dailey RA. Customized, single-incision, three-wall orbital decompression. Ophtal Plast Reconstr Surg 2005;21:1 9 [discussion 9 10]. [20] Wright ED, Davidson J, Codere F, Desrosiers M. Endoscopic orbital decompression with preservation of an inferomedial bony strut: minimization of postoperative diplopia. J Otolaryngol 1999;28: [21] Leung MK, Platt MP, Metson R. Revision endoscopic orbital decompression in the management of Graves orbitopathy. Otolaryngol Head Neck Surg 2009;141:46 51.
7 Transnasal endoscopic approach in the treatment of Graves ophthalmopathy 103 [22] Carrasco JR, Castillo I, Bilyk JR, et al. Incidence of infraorbital hypesthesia and sinusitis after orbital decompression for thyroid-related orbitopathy: a comparison of surgical techniques. Ophtal Plast Reconstr Surg 2005;21: [23] Pribitkin EA, McJunkin J, Kung B, Carrasco JR, Bilyk JR, Savino PJ. Technique selection for orbital decompression: combined endoscopic and transconjunctival versus combined endoscopic and transantral approach. Ear Nose Throat J 2009;88:E12.
Endoscopic transnasal orbital decompression for thyrotoxic orbitopathy
 Key words: Endoscopes; Exophthalmos; Keratitis; Orbital diseases; Thyrotoxicosis "# " APW Yuen KYW Kwan E Chan AWC Kung KSL Lam Hong Kong Med J 2002;8:406-10 Queen Mary Hospital, 102 Pokfulam Road, Hong
Key words: Endoscopes; Exophthalmos; Keratitis; Orbital diseases; Thyrotoxicosis "# " APW Yuen KYW Kwan E Chan AWC Kung KSL Lam Hong Kong Med J 2002;8:406-10 Queen Mary Hospital, 102 Pokfulam Road, Hong
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy
 Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
Graves disease may lead to exophthalmos that is
 Rev Bras Otorrinolaringol 2006;72(2):283-7 REVIEW ARTICLE Orbital endoscopic decompression in Graves Ophthalmopathy Wilma Terezinha Anselmo Lima 1, Mateus Perches 2, Fabiana Cardoso Pereira Valera 3, Ricardo
Rev Bras Otorrinolaringol 2006;72(2):283-7 REVIEW ARTICLE Orbital endoscopic decompression in Graves Ophthalmopathy Wilma Terezinha Anselmo Lima 1, Mateus Perches 2, Fabiana Cardoso Pereira Valera 3, Ricardo
Surgery for Exophthalmos
 Surgery for Exophthalmos Frederick S. Rosen, MD, Faculty Advisor: Matthew W. Ryan, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation April 7, 2004 1 Introduction
Surgery for Exophthalmos Frederick S. Rosen, MD, Faculty Advisor: Matthew W. Ryan, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation April 7, 2004 1 Introduction
Case Presentation: Indications for orbital decompression in TED: Modern surgical techniques for orbital decompression in TED: Inferomedial
 Case Presentation: Jonathan W. Kim, MD Director, Oculoplastic Surgery Stanford Medical Center 61 year old man with active Graves orbitopathy Visual acuity 20/30 OD 20/50 OS Left RAPD Bilateral optic disc
Case Presentation: Jonathan W. Kim, MD Director, Oculoplastic Surgery Stanford Medical Center 61 year old man with active Graves orbitopathy Visual acuity 20/30 OD 20/50 OS Left RAPD Bilateral optic disc
ORBIT/OPTIC NERVE DECOMPRESSION HISTORICAL PERSPECTIVE
 ORBIT AND OPTIC NERVE DECOMPRESSION Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College HISTORICAL PERSPECTIVE NORMAL AND
ORBIT AND OPTIC NERVE DECOMPRESSION Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College HISTORICAL PERSPECTIVE NORMAL AND
PROBLEM RECOMMENDATION
 PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
Mucocele of paranasal sinuses
 From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
James A. Garrity MD Department of Ophthalmology. Marius N. Stan MD Division of Endocrinology. Mayo Clinic Rochester, MN
 James A. Garrity MD Department of Ophthalmology Marius N. Stan MD Division of Endocrinology Mayo Clinic Rochester, MN Epidemiologic and diagnostic considerations for Graves orbitopathy (GO) 1. How common?
James A. Garrity MD Department of Ophthalmology Marius N. Stan MD Division of Endocrinology Mayo Clinic Rochester, MN Epidemiologic and diagnostic considerations for Graves orbitopathy (GO) 1. How common?
Learn Connect Succeed. JCAHPO Regional Meetings 2017
 Learn Connect Succeed JCAHPO Regional Meetings 2017 Financial Disclosure Evaluation and Treatment of Orbital Cellulitis Thomas E. Johnson, M.D. Bascom Palmer Eye Institute University of Miami School of
Learn Connect Succeed JCAHPO Regional Meetings 2017 Financial Disclosure Evaluation and Treatment of Orbital Cellulitis Thomas E. Johnson, M.D. Bascom Palmer Eye Institute University of Miami School of
CT of Maxillofacial Fracture Patterns. CT of Maxillofacial Fracture Patterns
 CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
Transnasal Endoscopic Sinonasal Surgery
 Reda kamel, Cadaveric dissection 1 Transnasal Endoscopic Sinonasal Surgery Cadaver Dissection Guide For Endoscopic Sinus Surgery Cairo University Egypt Reda Kamel Professor of Rhinology Cairo University
Reda kamel, Cadaveric dissection 1 Transnasal Endoscopic Sinonasal Surgery Cadaver Dissection Guide For Endoscopic Sinus Surgery Cairo University Egypt Reda Kamel Professor of Rhinology Cairo University
Radiological anatomy of frontal sinus By drtbalu
 2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
Surgery for Exophthalmos April 2004
 TITLE: Surgery for Exophthalmos SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 7, 2004 RESIDENT PHYSICIAN: Frederick S. Rosen, MD FACULTY ADVISOR: Matthew W. Ryan, MD SERIES
TITLE: Surgery for Exophthalmos SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 7, 2004 RESIDENT PHYSICIAN: Frederick S. Rosen, MD FACULTY ADVISOR: Matthew W. Ryan, MD SERIES
Pathophysiology. Surgery for Exophthalmos April 2000
 TITLE: Surgery for Exophthalmos SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 2000 RESIDENT PHYSICIAN: Stephanie Cordes, MD FACULTY ADVISOR: Karen Calhoun, MD SERIES EDITOR:
TITLE: Surgery for Exophthalmos SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 2000 RESIDENT PHYSICIAN: Stephanie Cordes, MD FACULTY ADVISOR: Karen Calhoun, MD SERIES EDITOR:
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Reasons for Failure and Surgical Revisions. Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology
 Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Epidemiology 3002). Epidemiology and Pathophysiology
 Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q
 The British Association of Plastic Surgeons (2004) 57, 37 44 Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q M. Kakibuchi*,
The British Association of Plastic Surgeons (2004) 57, 37 44 Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q M. Kakibuchi*,
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY
 COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
Frontal sinus disease continues to be one of the great
 Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Ophthalmic complications after surgery for nasal and sinus polyposis
 European Journal of Ophthalmology / Vol. 11 no. 3, 2001 / pp. 218-222 Ophthalmic complications after surgery for nasal and sinus polyposis P. VASSALLO, F. TRANFA, R. FORTE, A. D APONTE, D. STRIANESE, G.
European Journal of Ophthalmology / Vol. 11 no. 3, 2001 / pp. 218-222 Ophthalmic complications after surgery for nasal and sinus polyposis P. VASSALLO, F. TRANFA, R. FORTE, A. D APONTE, D. STRIANESE, G.
Boundaries Septum Turbinates & Meati Lamellae Drainage Pathways Variants
 The Fastest 20 Minutes in Michelle A. Michel, MD Professor of Radiology and Otolaryngology Medical College of Wisconsin, Milwaukee Overview Nasal cavity Anterior skull base Ostiomeatal complex Frontal
The Fastest 20 Minutes in Michelle A. Michel, MD Professor of Radiology and Otolaryngology Medical College of Wisconsin, Milwaukee Overview Nasal cavity Anterior skull base Ostiomeatal complex Frontal
CT of Maxillofacial Injuries
 CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis
 Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
Exposure techniques in endoscopic skull base surgery: Posterior septectomy, medial maxillectomy, transmaxillary and transpterygoid approach
 European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 284 288 Available online at www.sciencedirect.com TECHNICAL NOTE Exposure techniques in endoscopic skull base surgery: Posterior
European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 284 288 Available online at www.sciencedirect.com TECHNICAL NOTE Exposure techniques in endoscopic skull base surgery: Posterior
Intranasal location of lacrimal sac in Thai cadavers
 Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Maxillofacial and Ocular Injuries
 Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Study of success rates in endoscopic dacryocystorhinostomy with and without stenting. dacryocystorhinostomy with and
 Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Chapter Six. 1 of 6 11/3/2008 2:21 PM.
 1 of 6 11/3/2008 2:21 PM Email : myousefmian@hotmail.com Chapter Six FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
1 of 6 11/3/2008 2:21 PM Email : myousefmian@hotmail.com Chapter Six FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
Spheno-Ethmoidectomy
 Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
cme Combined Eyelid and Strabismus Surgery: Examining Conventional Surgical Wisdom Educational Objectives
 Article Combined Eyelid and Strabismus Surgery: Examining Conventional Surgical Wisdom Michael S. McCracken, MD; Jonathan D. del Prado, MD; David B. Granet, MD; Leah Levi, MBBS; Don O. Kikkawa, MD Abstract
Article Combined Eyelid and Strabismus Surgery: Examining Conventional Surgical Wisdom Michael S. McCracken, MD; Jonathan D. del Prado, MD; David B. Granet, MD; Leah Levi, MBBS; Don O. Kikkawa, MD Abstract
THE ORBITAL floor blowout
 ORGNA ARTCE Endoscopic Endonasal Repair of Orbital Floor Fracture Katsuhisa keda, D; Hideaki uzuki, D; Takeshi Oshima, D; Tomonori Takasaka, D ackground: High-resolution endoscopes and the advent of endoscopic
ORGNA ARTCE Endoscopic Endonasal Repair of Orbital Floor Fracture Katsuhisa keda, D; Hideaki uzuki, D; Takeshi Oshima, D; Tomonori Takasaka, D ackground: High-resolution endoscopes and the advent of endoscopic
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550013 Volume 1, Issue 3 Case Report Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report Peter Catalano, MD * and Michael
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550013 Volume 1, Issue 3 Case Report Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report Peter Catalano, MD * and Michael
Bony orbit Roof The orbital plate of the frontal bone Lateral wall: the zygomatic bone and the greater wing of the sphenoid
 Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Orbital and Ocular Adnexal Disorders with Red Eyes
 Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
ORIGINAL ARTICLE. Computed Tomographic Staging and the Fate of the Dependent Sinuses in Revision Endoscopic Sinus Surgery
 Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA
 ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA Anthony Po-Wing Yuen, FRCS, 1 Yiu Wah Fan, FRCS, 2 Ching Fai Fung, FRCS, 2 Kwan Ngai Hung, FRCS 2 1 Division of Otorhinolaryngology,
ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA Anthony Po-Wing Yuen, FRCS, 1 Yiu Wah Fan, FRCS, 2 Ching Fai Fung, FRCS, 2 Kwan Ngai Hung, FRCS 2 1 Division of Otorhinolaryngology,
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013
 FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
The surgical approach to the sphenoid sinus continues to
 A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
A comprehensive study on complications of endoscopic sinus surgery
 International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
Dr. Sami Zaqout Faculty of Medicine IUG
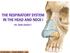 The Nose External Nose Nasal Cavity External Nose Blood and Nerve Supplies of the External Nose Blood Supply of the External Nose The skin of the external nose Branches of the ophthalmic and the maxillary
The Nose External Nose Nasal Cavity External Nose Blood and Nerve Supplies of the External Nose Blood Supply of the External Nose The skin of the external nose Branches of the ophthalmic and the maxillary
Functional Endoscopic Sinus Surgery
 WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
PTERYGOPALATINE FOSSA
 PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
A PLEA FOR LATERAL ORBITOTOMY WITH CERTAIN MODIFICATIONS*
 Brit. J. Ophthal. (1960) 44, 718. A PLEA FOR LATERAL ORBITOTOMY WITH CERTAIN MODIFICATIONS* BY H. B. STALLARD London THE frontiers of human interest and work are often disputed and, there is no exception
Brit. J. Ophthal. (1960) 44, 718. A PLEA FOR LATERAL ORBITOTOMY WITH CERTAIN MODIFICATIONS* BY H. B. STALLARD London THE frontiers of human interest and work are often disputed and, there is no exception
Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities
 10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
The sebaceous glands (glands of Zeis) open directly into the eyelash follicles, ciliary glands (glands of Moll) are modified sweat glands that open
 The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
Chapter 7. Skeletal System
 Chapter 7 Skeletal System 1 Skull A. The skull is made up of 22 bones: 8 cranial bones, 13 facial bones, and the mandible. B. The Cranium encloses and protects the brain, provides attachments for muscles,
Chapter 7 Skeletal System 1 Skull A. The skull is made up of 22 bones: 8 cranial bones, 13 facial bones, and the mandible. B. The Cranium encloses and protects the brain, provides attachments for muscles,
The modified endoscopic pre-lacrimal approach: how I do it
 Specialty Techniques Page 1 of 6 The modified endoscopic pre-lacrimal approach: how I do it Leslie T. Koh 1, Rataphol C. Dhepnorrarat 2 1 Department of Otolaryngology-Head & Neck Surgery, Changi General
Specialty Techniques Page 1 of 6 The modified endoscopic pre-lacrimal approach: how I do it Leslie T. Koh 1, Rataphol C. Dhepnorrarat 2 1 Department of Otolaryngology-Head & Neck Surgery, Changi General
Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy
 SV Manjunatha Rao, MM Rajshekar Original Article 10.5005/jp-journals-10013-1284 Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy 1 SV Manjunatha Rao, 2 MM Rajshekar ABSTRACT
SV Manjunatha Rao, MM Rajshekar Original Article 10.5005/jp-journals-10013-1284 Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy 1 SV Manjunatha Rao, 2 MM Rajshekar ABSTRACT
MAXILLOFACIAL TRAUMA. The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital
 MAXILLOFACIAL TRAUMA The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital Mandibular Injuries Mechanism of injury Assault, falls, RTA-Direct trauma
MAXILLOFACIAL TRAUMA The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital Mandibular Injuries Mechanism of injury Assault, falls, RTA-Direct trauma
Our Experience with Endoscopic Brow Lifts
 Aesth. Plast. Surg. 24:90 96, 2000 DOI: 10.1007/s002660010017 2000 Springer-Verlag New York Inc. Our Experience with Endoscopic Brow Lifts Ozan Sozer, M.D., and Thomas M. Biggs, M.D. İstanbul, Turkey and
Aesth. Plast. Surg. 24:90 96, 2000 DOI: 10.1007/s002660010017 2000 Springer-Verlag New York Inc. Our Experience with Endoscopic Brow Lifts Ozan Sozer, M.D., and Thomas M. Biggs, M.D. İstanbul, Turkey and
Imaging of the Paranasal Sinuses
 14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases.
 Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases. Akeem O Lasisi* and Aderemi A Adeosun Department of Otorhinolaryngology College of Medicine, University
Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases. Akeem O Lasisi* and Aderemi A Adeosun Department of Otorhinolaryngology College of Medicine, University
*in general the blood supply of the nose comes from branches of the internal and external carotid arteries.
 In the previous lecture we talked about the anatomy of the nasal cavity, today we will talk about its blood supply, venous drainage, innervations, and finally about the paranasal sinuses. When we describe
In the previous lecture we talked about the anatomy of the nasal cavity, today we will talk about its blood supply, venous drainage, innervations, and finally about the paranasal sinuses. When we describe
Omran Saeed. Luma Taweel. Mohammad Almohtaseb. 1 P a g e
 2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
Bones Ethmoid bone Inferior nasal concha Lacrimal bone Maxilla Nasal bone Palatine bone Vomer Zygomatic bone Mandible
 splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
FESS imaging - the role of MDCT
 FESS imaging - the role of MDCT Poster No.: C-0179 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Plascak, K. Makaruha, B. Klasic, L. Kavur, V. Vidjak; Zagreb/HR Keywords: Image verification,
FESS imaging - the role of MDCT Poster No.: C-0179 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Plascak, K. Makaruha, B. Klasic, L. Kavur, V. Vidjak; Zagreb/HR Keywords: Image verification,
Chapter Five. 1 of 8 11/3/2008 2:52 PM.
 1 of 8 11/3/2008 2:52 PM Email : myousefmian@hotmail.com Chapter Five FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
1 of 8 11/3/2008 2:52 PM Email : myousefmian@hotmail.com Chapter Five FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
Skull Base Danger Zones in FESS
 Skull Base Danger Zones in FESS Poster No.: C-2278 Congress: ECR 2014 Type: Educational Exhibit Authors: L. Renza Lozada, R. Carreño Gonzalez, G. Quintana Sanchez, 1 2 1 1 1 2 R. E. Figueroa ; Malaga/ES,
Skull Base Danger Zones in FESS Poster No.: C-2278 Congress: ECR 2014 Type: Educational Exhibit Authors: L. Renza Lozada, R. Carreño Gonzalez, G. Quintana Sanchez, 1 2 1 1 1 2 R. E. Figueroa ; Malaga/ES,
Trigeminal Nerve Worksheets, Distributions Page 1
 Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis
 Otolaryngology Head and Neck Surgery (2006) 134, 28-32 ORIGINAL RESEARCH A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis Roee Landsberg, MD, Yoram Segev, MD, Michael Friedman, MD,
Otolaryngology Head and Neck Surgery (2006) 134, 28-32 ORIGINAL RESEARCH A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis Roee Landsberg, MD, Yoram Segev, MD, Michael Friedman, MD,
1 Eyelids. Lacrimal Apparatus. Orbital Region. 3 The Orbit. The Eye
 1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
Ophthalmic Manifestations in ENT Diseases & Surgical Procedures
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 11, Issue 4 (Nov.- Dec. 2013), PP 87-92 Ophthalmic Manifestations in ENT Diseases & Surgical Procedures
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 11, Issue 4 (Nov.- Dec. 2013), PP 87-92 Ophthalmic Manifestations in ENT Diseases & Surgical Procedures
Expanding Role of Orbital Decompression in Aesthetic Surgery
 Oculoplastic Surgery Preliminary Report Expanding Role of Orbital Decompression in Aesthetic Surgery Aesthetic Surgery Journal 2017, 1 7 2017 The American Society for Aesthetic Plastic Surgery, Inc. Reprints
Oculoplastic Surgery Preliminary Report Expanding Role of Orbital Decompression in Aesthetic Surgery Aesthetic Surgery Journal 2017, 1 7 2017 The American Society for Aesthetic Plastic Surgery, Inc. Reprints
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Surgical anatomy of the deep lateral orbital wall
 European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 281-286 Surgical anatomy of the deep lateral orbital wall U. BEDEN 1, M. EDIZER 2, M. ELMALI 3, N. ICTEN 2, I. GUNGOR 1, Y. SULLU 1, D. ERKAN
European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 281-286 Surgical anatomy of the deep lateral orbital wall U. BEDEN 1, M. EDIZER 2, M. ELMALI 3, N. ICTEN 2, I. GUNGOR 1, Y. SULLU 1, D. ERKAN
Anatomical Variations in Osteomeatal Complex among Patients undergoing Functional Endoscopic Sinus Surgery
 V Narendrakumar, V Subramanian Original article 10.5005/jp-journals-10013-1259 Anatomical Variations in Osteomeatal Complex among Patients undergoing Functional Endoscopic Sinus Surgery 1 V Narendrakumar,
V Narendrakumar, V Subramanian Original article 10.5005/jp-journals-10013-1259 Anatomical Variations in Osteomeatal Complex among Patients undergoing Functional Endoscopic Sinus Surgery 1 V Narendrakumar,
SINUS ANATOMY AND FUNCTION
 EMBRYOLOGY AND DEVELOPMENT SINUS ANATOMY AND FUNCTION -4 th week gestation: -frontonasal process identified, arises over developing forebrain -ectodermal -contributes to nasal capsule -9 th and 10 th week
EMBRYOLOGY AND DEVELOPMENT SINUS ANATOMY AND FUNCTION -4 th week gestation: -frontonasal process identified, arises over developing forebrain -ectodermal -contributes to nasal capsule -9 th and 10 th week
Push Pull Technique for the Management of a Selected Superomedial Intraorbital Lesion
 THIEME Case Report e105 Push Pull Technique for the Management of a Selected Superomedial Intraorbital Lesion Paolo Castelnuovo, MD 1,4 Giacomo Fiacchini, MD 2 Francesca Romana Fiorini, MD 3 Iacopo Dallan,
THIEME Case Report e105 Push Pull Technique for the Management of a Selected Superomedial Intraorbital Lesion Paolo Castelnuovo, MD 1,4 Giacomo Fiacchini, MD 2 Francesca Romana Fiorini, MD 3 Iacopo Dallan,
ENDOSCOPIC SURGERY has. Endoscopic Transnasal Approach to the Pterygopalatine Fossa ORIGINAL ARTICLE. John M. DelGaudio, MD
 Endoscopic Transnasal Approach to the Pterygopalatine Fossa John. DelGaudio, D ORIGINAL ARTICLE Objective: To describe an endoscopic transnasal approach to the pterygopalatine fossa (PPF). Design: Case
Endoscopic Transnasal Approach to the Pterygopalatine Fossa John. DelGaudio, D ORIGINAL ARTICLE Objective: To describe an endoscopic transnasal approach to the pterygopalatine fossa (PPF). Design: Case
Research Article - Basic And Applied Anatomy Branching of the foramen rotundum. A rare variation of the sphenoid
 IJAE Vol. 119, n. 2: 148-152, 2014 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research Article - Basic And Applied Anatomy Branching of the foramen rotundum. A rare variation of the sphenoid Eugenio Bertelli,
IJAE Vol. 119, n. 2: 148-152, 2014 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research Article - Basic And Applied Anatomy Branching of the foramen rotundum. A rare variation of the sphenoid Eugenio Bertelli,
THYROID EYE DISEASE ORBITAL DECOMPRESSION SURGERY
 THYROID EYE DISEASE ORBITAL DECOMPRESSION SURGERY What is thyroid eye disease (TED)? TED is an autoimmune condition where the body s own immune system attacks the tissues of the thyroid gland and the eye
THYROID EYE DISEASE ORBITAL DECOMPRESSION SURGERY What is thyroid eye disease (TED)? TED is an autoimmune condition where the body s own immune system attacks the tissues of the thyroid gland and the eye
Computed tomography road map of the paranasal sinuses for treatment planning
 Computed tomography road map of the paranasal sinuses for treatment planning Poster No.: C-2607 Congress: ECR 2013 Type: Educational Exhibit Authors: N. Schembri, A. S. Gatt, D. Ellul, J. Brunton; Dundee/UK
Computed tomography road map of the paranasal sinuses for treatment planning Poster No.: C-2607 Congress: ECR 2013 Type: Educational Exhibit Authors: N. Schembri, A. S. Gatt, D. Ellul, J. Brunton; Dundee/UK
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study
 Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
CLINICAL SCIENCES. The Lacrimal Keyhole, Orbital Door Jamb, and Basin of the Inferior Orbital Fissure
 LINIL SIENES The Lacrimal Keyhole, Orbital oor Jamb, and asin of the Inferior Orbital Fissure Three reas of eep one in the Lateral Orbit Robert lan Goldberg, M; lexander J. Kim, M; Kristine M. Kerivan
LINIL SIENES The Lacrimal Keyhole, Orbital oor Jamb, and asin of the Inferior Orbital Fissure Three reas of eep one in the Lateral Orbit Robert lan Goldberg, M; lexander J. Kim, M; Kristine M. Kerivan
Communication issue - What should the radiologist report before functional endoscopic sinus surgery
 Communication issue - What should the radiologist report before functional endoscopic sinus surgery Poster No.: C-0509 Congress: ECR 2015 Type: Educational Exhibit Authors: A. M. Dobra 1, C. A. Badiu 1,
Communication issue - What should the radiologist report before functional endoscopic sinus surgery Poster No.: C-0509 Congress: ECR 2015 Type: Educational Exhibit Authors: A. M. Dobra 1, C. A. Badiu 1,
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit
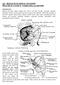 213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit OSTEOLOGY Identify the bones which comprise the walls of the orbit: maxilla, zygomatic, ethmoid, lachrymal, frontal, and
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit OSTEOLOGY Identify the bones which comprise the walls of the orbit: maxilla, zygomatic, ethmoid, lachrymal, frontal, and
Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K.
 05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
Pictorial review of extraconal and osseous orbital pathology - what can be found 'around' the orbits?
 Pictorial review of extraconal and osseous orbital pathology - what can be found 'around' the orbits? Poster No.: C-2011 Congress: ECR 2013 Type: Educational Exhibit Authors: M. Meissnitzer, T. Meissnitzer,
Pictorial review of extraconal and osseous orbital pathology - what can be found 'around' the orbits? Poster No.: C-2011 Congress: ECR 2013 Type: Educational Exhibit Authors: M. Meissnitzer, T. Meissnitzer,
Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision
 THIEME Original Research 73 Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision Jan Alessandro Socher 1 Jonas Mello 2 Barbara Batista Baltha 2 1 Department of Otorhinolaryngology,
THIEME Original Research 73 Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision Jan Alessandro Socher 1 Jonas Mello 2 Barbara Batista Baltha 2 1 Department of Otorhinolaryngology,
Lids and Orbits A Patient s Perspective. Dr. Paul Cauchi Consultant Ophthalmologist Southern General and Gartnavel General Hospitals, Glasgow
 Lids and Orbits A Patient s Perspective Dr. Paul Cauchi Consultant Ophthalmologist Southern General and Gartnavel General Hospitals, Glasgow Overview Pathophsiology. Symptoms. Signs. Management. Pathophysiology
Lids and Orbits A Patient s Perspective Dr. Paul Cauchi Consultant Ophthalmologist Southern General and Gartnavel General Hospitals, Glasgow Overview Pathophsiology. Symptoms. Signs. Management. Pathophysiology
ADVANCED ENDOSCOPIC ENDONASAL SINUS SURGERY
 Hands-On Dissection Guide on ADVANCED ENDOSCOPIC ENDONASAL SINUS SURGERY With Online Video Content Rainer WEBER, Werner HOSEMANN and Thomas KÜHNEL Hands-On Dissection Guide on ADVANCED ENDOSCOPIC ENDONASAL
Hands-On Dissection Guide on ADVANCED ENDOSCOPIC ENDONASAL SINUS SURGERY With Online Video Content Rainer WEBER, Werner HOSEMANN and Thomas KÜHNEL Hands-On Dissection Guide on ADVANCED ENDOSCOPIC ENDONASAL
A Computer-Assisted Anatomical Study of the Nasofrontal Region
 The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. A Computer-Assisted Anatomical Study of the Nasofrontal Region
The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. A Computer-Assisted Anatomical Study of the Nasofrontal Region
Major orbital complications of endoscopic sinus surgery
 598 Moorfields Eye Hospital, London EC1V 2PD, UK C Rene G E Rose R Lenthall I Moseley Correspondence to: Mr G E Rose, Orbital Clinic, Moorfields Eye Hospital, City Road, London EC1V 2PD, UK Accepted 20
598 Moorfields Eye Hospital, London EC1V 2PD, UK C Rene G E Rose R Lenthall I Moseley Correspondence to: Mr G E Rose, Orbital Clinic, Moorfields Eye Hospital, City Road, London EC1V 2PD, UK Accepted 20
Conventional Sinus Surgery Vs Fess
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
Dr.Ban I.S. head & neck anatomy 2 nd y جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102
 جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Pterygopalatine fossa: The pterygopalatine fossa is a cone-shaped depression, It is located between the maxilla,
جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Pterygopalatine fossa: The pterygopalatine fossa is a cone-shaped depression, It is located between the maxilla,
Protective Silastic sheet in combined transorbital and transnasal resection of sinonasal lesions*
 ORIGINAL CONTRIBUTION Protective Silastic sheet in combined transorbital and transnasal resection of sinonasal lesions* Nikul Amin 1, Thomas Jacques 2, Fiona Ting 1, Claire Hopkins 1, Pavol Šurda 1 Rhinology
ORIGINAL CONTRIBUTION Protective Silastic sheet in combined transorbital and transnasal resection of sinonasal lesions* Nikul Amin 1, Thomas Jacques 2, Fiona Ting 1, Claire Hopkins 1, Pavol Šurda 1 Rhinology
ORIGINAL ARTICLE. Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the Anterior Ethmoid
 Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Chapter 7 Part A The Skeleton
 Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Orbital facia. Periororbital facia Orbital septum Bulbar facia Muscular facia
 Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
CLINICAL SCIENCES. Minimally Invasive Orbital Decompression
 CLINICAL SCIENCES Minimally Invasive Orbital Decompression Local Anesthesia and Hand-Carved Bone Guy J. Ben Simon, MD; Robert M. Schwarcz, MD; Ahmad M. Mansury, BS; Lillian Wang, BS; John D. McCann, MD,
CLINICAL SCIENCES Minimally Invasive Orbital Decompression Local Anesthesia and Hand-Carved Bone Guy J. Ben Simon, MD; Robert M. Schwarcz, MD; Ahmad M. Mansury, BS; Lillian Wang, BS; John D. McCann, MD,
