Surgery for Exophthalmos April 2004
|
|
|
- Alban Dennis Patrick
- 5 years ago
- Views:
Transcription
1 TITLE: Surgery for Exophthalmos SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 7, 2004 RESIDENT PHYSICIAN: Frederick S. Rosen, MD FACULTY ADVISOR: Matthew W. Ryan, MD SERIES EDITORS: Francis B. Quinn, Jr., MD and Matthew W. Ryan, MD ARCHIVIST: Melinda Stoner Quinn, MSICS "This material was prepared by resident physicians in partial fulfillment of educational requirements established for the Postgraduate Training Program of the UTMB Department of Otolaryngology/Head and Neck Surgery and was not intended for clinical use in its present form. It was prepared for the purpose of stimulating group discussion in a conference setting. No warranties, either express or implied, are made with respect to its accuracy, completeness, or timeliness. The material does not necessarily reflect the current or past opinions of members of the UTMB faculty and should not be used for purposes of diagnosis or treatment without consulting appropriate literature sources and informed professional opinion." Introduction Exophthalmos, or proptosis, occurs when there is a discordant relationship between the soft tissue and bone of the anterior orbit and the globe. The adult orbit has a fixed volume of approximately 30 ml. When the soft tissue contents of the orbit exceed this amount, exophthalmos occurs. As an example, an increase in soft tissue volume of 5 ml (16%) will result in 4-5 mm of proptosis. Graves disease represents the most common cause of bilateral exophthalmos. This condition is generally referred to as Graves orbitopathy (ophthalmopathy). Graves orbitopathy typically affects middle-aged women. It is 5 times more common in women than men. Peak incidence occurs in the 3 rd and 4 th decades of life, and is 6 times more common in Caucasians. Severe exophthalmos is more common in elderly men. In addition, there is an increased prevalence in smokers, and a genetic predisposition has been established. Though associated with Graves Disease, exophthalmos is NOT necessarily associated with hyperthyroidism. 20% of patients with Graves orbitopathy are euthyroid. Graves orbitopathy likely arises from autoimmune, primarily T-cell, dysfunction resulting in lymphocytic infiltration and immune complex deposition with resultant edema and proliferation of extraocular muscles, intraconal and extraconal fat, and the lacrimal gland. There is some deficit in T-cell function that results in the production of antibodies that are normally suppressed. There are both infiltrative and noninfiltrative ocular changes in Graves. Infiltrative changes involve mononuclear cells causing activation and proliferation of fibroblasts resulting in the production of collagen and glycosaminoglycans. The end result is edema and fibrosis. Noninfiltrative changes involve spastic retraction of eyelids, an increase in palpebral fissure width, and sympathetic hypertonia. 1
2 Ultimately, thickening of the external ocular muscles, orbital fat herniation, proptosis, retraction of both the upper and lower eyelids, descent of the eyelid-cheek complex, and divergence of gaze occur. In addition, one may see eyelid edema, conjunctivitis, photophobia, chemosis, lagophthalmos, headache, gritty sensation in the eye, retrobulbar pain, and tearing. Thickening of the superior rectus muscle can result in decreased venous flow via compression of the superior ophthalmic vein. Hypertrophy of the extraocular muscles can result in ophthalmoplegia and thus diplopia, most frequently involving the inferior and medial rectus muscles resulting in limitation of both upward and lateral gaze. As inflammation of the orbital contents occurs, an increase in soft tissue volume results in increased intraorbital pressure, which causes anterior displacement of the globe and stretch (and/or compression) of the optic nerve with the potential for optic neuropathy. The natural progression of Graves orbitopathy is from no signs or symptoms to eyelid retraction, lid lag, and edema, followed by soft tissue signs and symptoms, followed by proptosis, followed by involvement of extraocular movement, followed by corneal involvement, followed by visual loss secondary to optic neuropathy. Optic neuropathy occurs in less than 5% of Graves orbitopathy, but it is the most common cause of vision loss in this setting; the progression is usually insidious. This neuropathy usually occurs in patients with proptosis, but can occur in patients without significant proptosis. Except for cases of rapidly progressive exophthalmos (malignant exophthalmos) the eyelids are capable of closing sufficiently to protect the cornea. Thus, while approximately 50% of Graves patients experience eye symptoms, only approximately 5% of cases are severe enough to warrant intervention. Patient Evaluation On physical exam, hyperemia over the lateral rectus muscle is pathognomonic of Graves orbitopathy. In addition, one typically sees divergence of the globes on extreme gaze (e.g., looking up or laterally). A complete ophthalmologic exam is necessary. The amount of globe protrusion is measured using Hertel exophthalmometry. Assessment of visual acuity, visual fields, and color saturation must be performed to exclude optic neuropathy. Nasal endoscopy should be performed to diagnosis any sinonasal problems such as septal deviation or polyposis. In addition, the thyroid gland should be palpated. Radiographic imaging is an important part of the evaluation. A CT or MRI of the orbit and sinuses represents the standard of care. This helps to rule out other pathologic conditions of the orbit, especially in a case of unilateral exophthalmos. In addition, imaging will help to establish the presence or absence of sinusitis, septal deviation, and hypoplastic maxillary sinuses all of which will affect the approach to treatment. MRI measurement of T2 relaxation time can be useful for detecting external ocular muscle edema. Proptotic patients with an increased mean T2 relaxation time are more likely to respond to anti-inflammatory therapy, while those without T2 relaxation time prolongation are more likely to require orbital decompression. In Graves Disease, T3, Free T4 Index, TSH, TRH, and TSI (a type of IgG) are all 2
3 elevated. These generally return to normal after I-131 ablation of the thyroid. Differential Diagnosis 3 Graves orbitopathy may be unilateral (10-20%) or bilateral (80-90%). Pseudotumor cerebri represents the second most common cause of bilateral exophthalmos. CT or MRI shows generalized edema of the orbital soft tissues and occasionally the brain. However, there is no specific enlargement of the external ocular muscles. The use of high dose corticosteroids will generally improve the proptosis within 24 to 48 hours. Meningioma en plaque results in severe exophthalmos with eyelid edema. Usually, the lower lid is affected without lid retraction. Axial myopia is a common cause of unilateral exophthalmos. This is diagnosed by retinoscopy and A-scan ultrasound. Inflammatory pseudotumor mimics a neoplasm with the sudden onset of proptosis, lid edema, pain, ophthalmoplegia, and visual loss. This typically responds to steroids. Lymphoma of the orbit typically causes eccentric proptosis. CT or MRI typically demonstrates a mass, or masses, located near the orbital apex. Other orbital masses, generally associated with unilateral proptosis, include metastasis, vascular anomalies, neurofibromas, and retinoblastoma. In addition, congenital shallowness of the orbits, such as in Apert or Crouzon Syndromes, may be the cause of proptosis. In such cases, surgery is generally cosmetic. Treatment With the exception of acute and progressive Graves orbitopathy (malignant exophthalmos), the disease is self-limited in the majority of patients. Serial testing of visual fields allows for early detection of malignant exophthalmos. If left untreated, progression to blindness from either corneal exposure or optic neuropathy will result. Medical treatment should be the first step in addressing Graves orbitopathy. This is typically managed by the Endocrinologist. I-131 and levothyroxine are used to achieve euthyroid status. While exophthalmos generally improves with correction of hyperthyroidism, this is not always the case. Surgical treatment of Graves orbitopathy is generally delayed until both the status of the orbit and the thyroid have stabilized for 6 months. An exception to this rule occurs in the 1-2% of patients who experience acute deterioration in visual fields or visual acuity secondary to optic neuropathy. These patients may be treated initially with prednisone mg/day for 2 weeks. If visual dysfunction does not improve, or prolonged use of steroids is required, then decompression of the orbit is indicated. Low dose radiation therapy to the orbits represents another non-surgical option. This is NOT appropriate in the acute or subacute setting with associated visual loss because of the early
4 edema associated with radiation. It is a reasonable alternative for stable Graves orbitopathy, though results are less dramatic. Usually the treatment course requires 200 cgy of fractionated photon radiation over 2 weeks. With this treatment, the condition typically arrests or improves; resolution is rare. In addition one must be very confident that the patient will not require surgery, since orbital decompression and fat manipulation becomes very difficult after the radiation. Because immune dysregulation is thought to be at the heart of Graves orbitopathy, immunomodulation would seem a logical treatment option. Both cyclophosphamide and cyclosporine have been tried, but long term efficacy has NOT been established. Surgery The goal of surgery is to enlarge the confining space of the orbit via removal of 1 to 4 walls of the bony orbit with incision of the periosteum to allow for prolapse of the orbital soft tissues into adjacent spaces. Theoretically, up to 15 mm of decompression can be achieved by removing all 4 walls (usually, surgery results in 3-7 mm of decompression). However, intractable strabismus and hypoglobus can result from excessive decompression. Patients must be made aware of the risks associated with decompression of the orbit. The most common complication is diplopia. Other potential complications include injury to the optic nerve or retina from prolonged globe retraction. Retrobulbar hematoma a potential cause of blindness is also a possibility. Injury to the infraorbital nerve and epistaxis may also occur. Indications for orbital decompression vary depending on time course. In the acute or subacute phase of the disease, surgery is indicated if steroids fail to improve visual disturbance OR if steroids are required for long-term maintenance of vision. Functional indications for surgery, generally present in the acute or subacute phase, include corneal exposure with keratitis, usually in patients with significant lid retraction. More commonly, functional indications are related to optic neuropathy. This may be manifested by decreased visual acuity, visual field defects, abnormal visual evoked potentials, and disk edema. Patients with optic neuropathy are usually older, usually have LESS proptosis, and usually have a shorter duration of eye disease. Globe prolapse anterior to the eyelids is another early indication. In the late phase, decompression is generally performed for cosmesis, which is a relative indication. Again, this should occur only after orbital findings have stabilized for approximately 6 months. In general, the more advanced the exophthalmos, the more extensive the surgery required to produce even a modest improvement. As a result, very few patients are satisfied with the initial surgical procedure. Needless to say, these patients frequently require more than orbital decompression. Strabismus surgery for the correction of diplopia and lid lengthening for eye lid retraction are common adjunctive procedures. Ideally, orbital decompression is performed first, followed by strabismus surgery and then lid lengthening. 4
5 Orbital Decompression For each of the 4 sides of the orbital aperture a technique has been described for orbital decompression. The name of the surgeon associated with each technique will be placed in parentheses. SUPERIOR ORBITAL DECOMPRESSION (Naffziger) This involves complete unroofing of the orbit via a frontal craniotomy. The advantage of this approach is that a very large amount of orbital bone can be removed. Major disadvantages include the need for a craniotomy and the transmission of pulsations from the brain to the globe postoperatively. The problem with pulsations can be overcome by using a titanium shield to support the frontal lobe. This approach must be performed in conjunction with neurosurgery. The optic nerve must be visualized. The orbital roof is removed from just anterior to the optic foramen anteriorly to the anterosuperior orbital rim. Periosteum must be left intact as bone is removed to prevent injury to the levator muscle. Once the entire superior periosteum has been uncovered, an H- shaped incision may be made in the periosteum to allow herniation of orbital fat into the cranial vault. Titanium mesh can then be secured with self-tapping screws to cover the orbital roof. The cranial flap is then replaced. A temporary tarsorrhaphy should be considered if edema associated with the procedure has caused an immediate worsening of proptosis. Postoperative steroids can be given for 3 days, at which time the tarsorrhaphy can be removed. 5 This approach is uncommon, but is most frequently used in the setting of orbital trauma. MEDIAL DECOMPRESSION (Sewell) This may be approached via a coronal incision, which should be considered for cosmesis, or, more commonly, a standard external ethmoidectomy incision. After incision, the medial canthal tendon is tagged and divided. The anterior and posterior ethmoid arteries are identified and the anterior artery is ligated with a clip. Beginning at the lacrimal fossa, a complete ethmoidectomy is performed. One must take care not to injure the optic nerve. When using a coronal incision, the medial canthal tendon is left intact. Ethmoidectomy is performed from above. There is a greater risk to the lacrimal sac and insertion of the trochlea because of the need for wider periosteal undermining for exposure. Once ethmoidectomy has been completed, the medial periosteum is incised (various incisions have been described) and the orbital fat is allowed to herniate or gently teased into the ethmoidectomy cavity. Great care must be taken to avoid injury to the medial rectus muscle. INFERIOR DECOMPRESSION (Hisch and Urbanek) This involves creation of an orbital floor blowout fracture while sparing the infraorbital nerve. The approach involves either a transconjunctival or a subciliary incision plus a Caldwell-
6 Luc maxillary antrostomy. This allows for visualization of the floor while removing bone via the antrostomy. The bone becomes thicker and denser as the surgeon reaches the posterior extent of the orbit. A total of 3 cm of bone removal from anterior to posterior is usually adequate and safe. Medially, the floor can be removed up to the lacrimal fossa, and laterally to the zygoma. After incision of the periorbita and decompression of orbital fat, forced duction testing should be performed to ensure that the extraocular muscles are not hindered. LATERAL DECOMPRESSION (Kronlein) This was the first technique for orbital decompression described in the literature (Dollinger, 1911). The approach options for this technique include a coronal incision, a direct rim incision (or lateral extension of a subciliary incision), an extended lateral canthotomy, or an upper lid crease incision with extension along a laugh line over the rim. When performed in combination with medial decompression or endoscopic decompression, it is best performed AFTER these techniques. The orbital contents can be gently retracted medially and protected allowing excellent exposure. Following incision, the periosteum over the lateral orbital rim is exposed from the reflection of the zygomatic arch to the zygomaticofrontal suture. An incision in the periosteum is made along the length of the lateral rim. The periosteum is then elevated on both the infratemporal fossa side and the orbital side of the lateral rim form cm posteriorly. The roof and floor of the orbit are also exposed. The lateral canthus is left intact. Leaving the lateral rim intact, as much orbital bone as possible is removed using a cutting burr to excavate the lateral orbital wall while the malleable protects orbital contents. Bone is removed to the level of the lateral periosteum, fascia of the temporalis muscle, and to the dura superiorly until the thick bone of the skull base is encountered posteriorly (a cm diameter circle of bone should be removed). The periorbita is then incised and the orbital fat teased out. Alternatively, the lateral rim can be cut and mobilized on a hinge of periosteum before bone removal, then fixated with a microplate or wire at the conclusion of the procedure. Of note, CSF leak was the most common complication in one series examining this technique (Graham). This occurred while burring down bone of the greater sphenoid wing with inadvertent penetration of the inner bony cortex and dura. Reportedly, these leaks were easily repaired intraoperatively without recurrence. COMBINED MEDIAL AND INFERIOR DECOMPRESSION (Walsh-Ogura) Like the inferior approach mentioned above, this involves a Caldwell-Luc/transantral approach. This was the surgical technique of choice for orbital decompression until the 1990 s, at which time endoscopic techniques became more popular. ENDOSCOPIC DECOMPRESSION Non-minimally invasive techniques are falling out of favor as the endoscopic approach becomes more prevalent. An endoscopic approach avoids an external incision, benefits from 6
7 limited morbidity, allows for excellent access to the optic nerve at the orbital apex when needed, and can be performed under local anesthestic. The eyes must be included in the surgical field, and are best protected with corneal shields. The procedure begins with a standard uncinectomy. A very large middle meatal antrostomy is created and the 30 degree endoscope should be used to identify the position of the infraorbital nerve in the roof of the maxillary sinus. A total ethmoidectomy is performed, and the sphenoid ostium is identified and enlarged. The lamina papyracea is then skeletonized, and the position of the anterior and posterior ethmoid arteries is noted. Classically, the middle turbinate is resected to improve exposure for post-operative cleaning (though some authors retain the middle turbinate because it prevents the prolapse of orbital fat from obstructing the sphenoid ostium). Similarly, a small piece of lamina should be retained in the frontal recess area to prevent prolapsing fat from obstructing the frontal sinus. A spoon curette or Freer elevator is then used to crack the lamina papyracea in its thin midportion and a Cottle is used to bluntly elevate bone away from the periorbita taking care to leave the periorbita intact so fat does not herniate into the field of view. Bone should be removed up to the roof of the ethmoid superiorly, the face of the sphenoid posteriorly, the maxillary line (nasolacrimal duct) anteriorly, and the maxillary antrostomy inferiorly. Finally, bone from the orbital floor is removed medial to V2 with downward pressure using a spoon curette on the remaining bony rim of the maxillary antrostomy. The bone typically fractures along the cleavage plane of the infraorbital canal. The periorbita is then incised with a sickle knife starting posteriorly, keeping the blade superficial to avoid injury to the extraocular muscles. In fact, a method of placing a guard on the sickle knife using a steri-strip to leave 2-3 mm of blade tip has been described. Multiple cuts in the periorbita or complete removal of periorbita should be performed to allow for herniation of orbital fat. Gentle orbital pressure during this technique encourages the extrusion of orbital fat. The advantages of this technique are a lack of external incisions and a decreased incidence of oral-antral fistula as compared to the Walsh Ogura technique. However, laterally, decompression of the orbital floor is limited by the infraorbital nerve. On average, 3.5 mm of exophthalmos can be corrected with the endoscope alone; an average of 5.4 mm can be corrected if this is combined with an open lateral decompression. Postoperatively, visual acuity and extraocular movement must be checked. Nasal packing must be avoided to prevent compression of the optic nerve. The patient can be discharged to home in less than 24 hours on oral antibiotics and nasal saline irrigation. Postoperative endoscopic cleaning is performed per routine for endoscopic sinus surgery. Nose blowing should be avoided for 2 weeks postoperatively. Bilateral orbital decompressions, when required, can be done at an interval of 1 week. 7
8 ORBITAL FAT REMOVAL This represents an alternative to traditional orbital decompressive procedures. With this procedure, the preoperative CT scan is helpful in demonstrating the location of orbital fat pockets. These fat pockets can then be approached via an upper lid crease and subciliary or transconjunctival incisions. The orbital septum in both upper and lower eyelids must be opened longitudinally and the fat compartments debulked. Excellent hemostasis must be obtained with the bipolar, and injury to the lacrimal gland in the superolateral quadrant is best avoided. Trauma to the inferior oblique muscle must also be avoided. As much as 6 mm of proptosis can be corrected with this technique, which correlates with the removal of 5 to 6 ml of fat. This may be a more useful technique when orbital fat involvement is the major underlying problem as opposed to extraocular muscle involvement or optic neuropathy. Choosing the Appropriate Technique For mild (2-3 mm) exophthalmos, any one of the decompression approaches may be used. For moderate exophthalmos (3-5 mm), inferior decompression alone may be sufficient. Alternatively, a combination of medial and lateral decompression may be used. For severe exophthalmos (5-7 mm), 3 wall decompression can be performed. Again, these external approaches have been largely supplanted by the endoscopic technique with or without lateral decompression. After healing and stabilization, one may need additional surgery for eyelid retraction. Resection of Muller s muscle may be adequate for slight upper eyelid retraction. For greater retraction, transection of the eyelid retractors with the insertion of cartilage or Gore-Tex grafts to lengthen the eyelids may help. Results and Complications The function and cosmesis of approximately 75% of patients stabilize or improve after surgical decompression. A corneal abrasion is a real possibility during orbital decompression. Most believe the cornea is best protected using a corneal shield. However, some advocate that it is better to leave the cornea exposed with frequent irrigation because a dilating pupil is an important early sign of excessive traction on the globe or optic nerve. (It is important to take frequent breaks while retracting on the globe.) Retrobulbar hematomas are best avoided by achieving excellent hemostasis with bipolar cautery and placement of a Penrose drain. If it occurs, it is considered an emergency. The skin incision should be opened, the hematoma evacuated, the orbit irrigated, bipolar cautery used for hemostasis, and a drain placed. Temporary neuropraxia of the infraorbital nerve is common, and may be difficult to avoid 8
9 in inferior decompression. Retinal hemorrhage is a rare complication, and almost always seems to occur in diabetic patients. This complication necessitates ophthalmologic consultation. Orbital cellulitis is also rare. It may be a good idea to treat those patients with purulent rhinorrhea or other evidence of sinusitis with prophylactic antibiotics preoperatively. Retinal vascular occlusion (heralded by pain in the eye and/or decreased vision), corneal ulcer, and retrobulbar hematoma represent the 3 major eye emergencies that may occur as a complication of decompressive surgery. At least the first 2 necessitate prompt ophthalmologic consultation. Furthermore, the patient should be instructed at discharge to seek immediate care for increased pain in the eye or decreased vision. Diplopia As many as 50% of patients experience some degree of diplopia postoperatively. In fact, some authors contend that virtually all patients undergoing orbital decompression will experience some degree of diplopia at some time during their postoperative course. Preoperative diplopia is often worsened by decompression. Many patients will experience spontaneous resolution of their diplopia once inflammation subsides. Other patients may have diplopia present only on peripheral gaze and do not require any further treatment. But, if significant diplopia is still present 6 to 8 months after decompression, then correction must be performed by ophthalmology. Several modifications have been proposed to avoid diplopia. One is complete removal of the inferior periorbita when performing inferior decompression. This is thought to prevent fibrosis of the periorbita to the inferior rectus. Another is orbital lipectomy rather than orbital decompression. Small series have shown that lipectomy alone is unlikely to worsen diplopia, and likely to make it better. Preservation of a bony orbital strut in the lamina papyracea, though technically difficult, has for several years been thought to play an important role in diplopia prevention. 9 Decompression confined to the lateral wall rarely causes diplopia. A balanced decompression involving both the medial and lateral orbit is also far less likely to result in diplopia. Along those lines, avoidance of any involvement of the orbital floor is far less likely to result in diplopia. More recently, Metson has described the orbital sling technique during endoscopic orbital decompression. In this technique, 2 horizontal incisions are made in the medial periorbita that approximate the superior and inferior margins of the medial rectus muscle. These incisions sit approximately 10 mm apart beginning just anterior to the face of the sphenoid and extending all the way to the maxillary line. The remaining periorbita above and below the above mentioned incisions can then be removed to allow for prolapse of orbital fat. Thus, a medial sling of periorbita is left in place to protect the medial rectus muscle. Forced duction with lateral rotation of the globe can be used intraoperatively to confirm the location of the medial rectus before the
10 periorbital incisions are made. In Metson s series, no patients who underwent the orbital sling technique experienced worsened diplopia. Those patients who had a lateral decompression in addition to the orbital sling were even more likely to experience improvement in diplopia postoperatively. Another more recently described option is orbital rim advancement, which involves the use of onlay grafts to the bony orbit, rather than decompression of orbital contents, to change the globe-rim relationship. Goldberg reported a series in which onlay grafts (porous polyethylene) were used either in isolation or in combination with orbital decompression. The onlay is typically placed via an inferior transconjunctival approach with suspension of the suborbital orbicularis oculi fat (SOOF) from the implant (a SOOF lift). Using this onlay technique, proptosis decreased an average of 4.65 mm. This technique is most useful in fibrotic, woody orbits or when the bony orbits are shallow (e.g., congenitally hypoplastic maxilla). Conclusion The most common cause of bilateral exophthalmos is Graves orbitopathy. The presence or severity of Graves orbitopathy does not correlate well with the thyroid status of the patient. Though Graves orbitopathy is a product of autoimmune disease, definitive treatment remains primarily surgical. Treatment of Graves disease and Graves orbitopathy should be multidisciplinary and involve an endocrinologist, an ophthalmologist, and an otolaryngologist. 10 Preoperative imaging is vital and should include both the orbits and the sinuses. The current surgical treatment of choice is endoscopic orbital decompression or lateral decompression or both. Every effort should be made to protect the inferior and medial rectus muscles and to minimize the extent of postoperative diplopia, which remains common following orbital decompression. References Clauser L, Galie M, et al. Rationale of Treatment in Graves Ophthalmopathy. Plastic & Reconstructive Surgery. 108; , December Goldberg RA, Soroudi AE, McCann JD. Treatment of Prominent Eyes with Orbital Rim Onlay Implants: Four-Year Experience. Opthalmic Plastic and Reconstructive Surgery. 19; 38-45, January Gliklich RE. Endoscopic Orbital and Optic Nerve Decompression. Minimally Invasive Surgery of the Head, Neck, and Cranial Base. Phillip A. Wackym, Dale H. Rice, Steven D. Schaefer edd. Lippincott Williams & Wilkins. C pp Graham SM, Brown CL, et al. Medial and Lateral Orbital Wall Surgery for Balanced Decompression in Thyroid Eye Disease. Laryngoscope. 113; , July Holt JE, Holt GR. Surgery for Exophthalmos. Head and Neck Surgery Otolaryngology 3 rd Edition. Byron J. Bailey, ed. Lippincott Williams & Wilkins. C pp
11 Metson R, Samaha M. Reduction of Diplopia Following Endoscopic Orbital Decompression: The Orbital Sling Technique. Laryngoscope. 112; , October Shepard KG, Levin PS, Terris D. Balanced Orbital Decompression for Graves Opthalmopathy. Laryngoscope. 108; , November
Surgery for Exophthalmos
 Surgery for Exophthalmos Frederick S. Rosen, MD, Faculty Advisor: Matthew W. Ryan, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation April 7, 2004 1 Introduction
Surgery for Exophthalmos Frederick S. Rosen, MD, Faculty Advisor: Matthew W. Ryan, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation April 7, 2004 1 Introduction
Pathophysiology. Surgery for Exophthalmos April 2000
 TITLE: Surgery for Exophthalmos SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 2000 RESIDENT PHYSICIAN: Stephanie Cordes, MD FACULTY ADVISOR: Karen Calhoun, MD SERIES EDITOR:
TITLE: Surgery for Exophthalmos SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 2000 RESIDENT PHYSICIAN: Stephanie Cordes, MD FACULTY ADVISOR: Karen Calhoun, MD SERIES EDITOR:
ORBIT/OPTIC NERVE DECOMPRESSION HISTORICAL PERSPECTIVE
 ORBIT AND OPTIC NERVE DECOMPRESSION Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College HISTORICAL PERSPECTIVE NORMAL AND
ORBIT AND OPTIC NERVE DECOMPRESSION Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College HISTORICAL PERSPECTIVE NORMAL AND
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Case Presentation: Indications for orbital decompression in TED: Modern surgical techniques for orbital decompression in TED: Inferomedial
 Case Presentation: Jonathan W. Kim, MD Director, Oculoplastic Surgery Stanford Medical Center 61 year old man with active Graves orbitopathy Visual acuity 20/30 OD 20/50 OS Left RAPD Bilateral optic disc
Case Presentation: Jonathan W. Kim, MD Director, Oculoplastic Surgery Stanford Medical Center 61 year old man with active Graves orbitopathy Visual acuity 20/30 OD 20/50 OS Left RAPD Bilateral optic disc
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
James A. Garrity MD Department of Ophthalmology. Marius N. Stan MD Division of Endocrinology. Mayo Clinic Rochester, MN
 James A. Garrity MD Department of Ophthalmology Marius N. Stan MD Division of Endocrinology Mayo Clinic Rochester, MN Epidemiologic and diagnostic considerations for Graves orbitopathy (GO) 1. How common?
James A. Garrity MD Department of Ophthalmology Marius N. Stan MD Division of Endocrinology Mayo Clinic Rochester, MN Epidemiologic and diagnostic considerations for Graves orbitopathy (GO) 1. How common?
The sebaceous glands (glands of Zeis) open directly into the eyelash follicles, ciliary glands (glands of Moll) are modified sweat glands that open
 The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy
 Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
Endoscopic transnasal orbital decompression for thyrotoxic orbitopathy
 Key words: Endoscopes; Exophthalmos; Keratitis; Orbital diseases; Thyrotoxicosis "# " APW Yuen KYW Kwan E Chan AWC Kung KSL Lam Hong Kong Med J 2002;8:406-10 Queen Mary Hospital, 102 Pokfulam Road, Hong
Key words: Endoscopes; Exophthalmos; Keratitis; Orbital diseases; Thyrotoxicosis "# " APW Yuen KYW Kwan E Chan AWC Kung KSL Lam Hong Kong Med J 2002;8:406-10 Queen Mary Hospital, 102 Pokfulam Road, Hong
Orbital facia. Periororbital facia Orbital septum Bulbar facia Muscular facia
 Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
PROBLEM RECOMMENDATION
 PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
Bony orbit Roof The orbital plate of the frontal bone Lateral wall: the zygomatic bone and the greater wing of the sphenoid
 Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
! Women greater than men (4:1)» Typical of other autoimmune diseases
 1 2 3 4 : Overview and Diagnosis Suzanne K. Freitag, M.D. Director, Ophthalmic Plastic Surgery Massachusetts Eye and Ear Infirmary Harvard Medical School! I have no financial disclosures. Learning Objectives!
1 2 3 4 : Overview and Diagnosis Suzanne K. Freitag, M.D. Director, Ophthalmic Plastic Surgery Massachusetts Eye and Ear Infirmary Harvard Medical School! I have no financial disclosures. Learning Objectives!
Graves Ophthalmopathy Overview. Graves Disease Hyperthyroidism TSIgs (anti-tsh-receptor-abs) Graves Disease 10/22/2010
 Graves Disease Robert Graves Graves Ophthalmopathy Overview Robert C. Kersten Dept. of Ophthalmology UCSF Triad Hyperthyroidism Eye findings Pretibial Myxedema (phalangeal acropachy-1%) Most common auto-immune
Graves Disease Robert Graves Graves Ophthalmopathy Overview Robert C. Kersten Dept. of Ophthalmology UCSF Triad Hyperthyroidism Eye findings Pretibial Myxedema (phalangeal acropachy-1%) Most common auto-immune
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY
 COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
13/02/1440 بسم ا هلل ا لرحمن ا لر حيم
 بسم ا هلل ا لرحمن ا لر حيم 1 Slowly progressive versus rapidly progressive proptosis by Ali M ISMAIL professor of ophthalmology @SOHAG U H Occuloplastic fellow @NNUH Occuloplastic fellow @Cambridge UH
بسم ا هلل ا لرحمن ا لر حيم 1 Slowly progressive versus rapidly progressive proptosis by Ali M ISMAIL professor of ophthalmology @SOHAG U H Occuloplastic fellow @NNUH Occuloplastic fellow @Cambridge UH
CT of Maxillofacial Injuries
 CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
MRI masterfile Part 5 WM Heme Strokes.ppt 1
 Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
CT of Maxillofacial Fracture Patterns. CT of Maxillofacial Fracture Patterns
 CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Learn Connect Succeed. JCAHPO Regional Meetings 2017
 Learn Connect Succeed JCAHPO Regional Meetings 2017 Financial Disclosure Evaluation and Treatment of Orbital Cellulitis Thomas E. Johnson, M.D. Bascom Palmer Eye Institute University of Miami School of
Learn Connect Succeed JCAHPO Regional Meetings 2017 Financial Disclosure Evaluation and Treatment of Orbital Cellulitis Thomas E. Johnson, M.D. Bascom Palmer Eye Institute University of Miami School of
Orbital and Ocular Adnexal Disorders with Red Eyes
 Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Lids and Orbits A Patient s Perspective. Dr. Paul Cauchi Consultant Ophthalmologist Southern General and Gartnavel General Hospitals, Glasgow
 Lids and Orbits A Patient s Perspective Dr. Paul Cauchi Consultant Ophthalmologist Southern General and Gartnavel General Hospitals, Glasgow Overview Pathophsiology. Symptoms. Signs. Management. Pathophysiology
Lids and Orbits A Patient s Perspective Dr. Paul Cauchi Consultant Ophthalmologist Southern General and Gartnavel General Hospitals, Glasgow Overview Pathophsiology. Symptoms. Signs. Management. Pathophysiology
Clues of a Ruptured Globe
 Definition any eye that has sustained a full thickness traumatic disruption of the cornea or sclera Overwhelmingly, rupture accidents occur in young men, small children and the elderly Corneal laceration
Definition any eye that has sustained a full thickness traumatic disruption of the cornea or sclera Overwhelmingly, rupture accidents occur in young men, small children and the elderly Corneal laceration
TRAUMA TO THE FACE AND MOUTH
 Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
EYE INJURIES OBJECTIVES COMMON EYE EMERGENCIES 7/19/2017 IMPROVE ASSESSMENT OF EYE INJURIES
 EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
Maxillofacial and Ocular Injuries
 Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Epidemiology 3002). Epidemiology and Pathophysiology
 Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
MRI masterfile Part 5 WM Heme Strokes.ppt 2
 Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
Graves disease may lead to exophthalmos that is
 Rev Bras Otorrinolaringol 2006;72(2):283-7 REVIEW ARTICLE Orbital endoscopic decompression in Graves Ophthalmopathy Wilma Terezinha Anselmo Lima 1, Mateus Perches 2, Fabiana Cardoso Pereira Valera 3, Ricardo
Rev Bras Otorrinolaringol 2006;72(2):283-7 REVIEW ARTICLE Orbital endoscopic decompression in Graves Ophthalmopathy Wilma Terezinha Anselmo Lima 1, Mateus Perches 2, Fabiana Cardoso Pereira Valera 3, Ricardo
Maxilla, ORBIT and infratemporal fossa. Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine
 Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Lower Eyelid Blepharoplasty. Mid-Year Seminar AOCOO-HNS Foundation September 21 st, 2013
 Lower Eyelid Blepharoplasty Mid-Year Seminar AOCOO-HNS Foundation September 21 st, 2013 The beauty of a woman must be seen from in her eyes, because that is the doorway to her heart, the place where love
Lower Eyelid Blepharoplasty Mid-Year Seminar AOCOO-HNS Foundation September 21 st, 2013 The beauty of a woman must be seen from in her eyes, because that is the doorway to her heart, the place where love
with laser resurfacing, 36, 37 Cryotherapy, lower eyelid cicatricial ectropion after, 151 Cutler-Beard flap. See Fullthickness
 INDEX A Abrasion, from silicone tubing, 230 Acquired immunodeficiency syndrome, eyelid tumor with, 193 AIDS. See Acquired immunodeficiency syndrome Anatomy, eyelid, 155 156 Aneurysm, cerebral, Muller s
INDEX A Abrasion, from silicone tubing, 230 Acquired immunodeficiency syndrome, eyelid tumor with, 193 AIDS. See Acquired immunodeficiency syndrome Anatomy, eyelid, 155 156 Aneurysm, cerebral, Muller s
1 Eyelids. Lacrimal Apparatus. Orbital Region. 3 The Orbit. The Eye
 1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY INFERIOR MAXILLECTOMY Tumours of the hard palate and superior alveolus may be resected by inferior maxillectomy (Figure 1). A Le Fort
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY INFERIOR MAXILLECTOMY Tumours of the hard palate and superior alveolus may be resected by inferior maxillectomy (Figure 1). A Le Fort
Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q
 The British Association of Plastic Surgeons (2004) 57, 37 44 Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q M. Kakibuchi*,
The British Association of Plastic Surgeons (2004) 57, 37 44 Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q M. Kakibuchi*,
MAXILLOFACIAL TRAUMA. The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital
 MAXILLOFACIAL TRAUMA The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital Mandibular Injuries Mechanism of injury Assault, falls, RTA-Direct trauma
MAXILLOFACIAL TRAUMA The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital Mandibular Injuries Mechanism of injury Assault, falls, RTA-Direct trauma
REVIEW OF HEAD AND NECK CRANIAL NERVES AND EVERYTHING ELSE
 REVIEW OF HEAD AND NECK CRANIAL NERVES AND EVERYTHING ELSE OLFACTORY NERVE CN I ANTERIOR CRANIAL FOSSA CRISTA GALLI OF ETHMOID OLFACTORY FORAMINA IN CRIBIFORM PLATE OF ETHMOID BONE CN I OLFACTORY NERVE
REVIEW OF HEAD AND NECK CRANIAL NERVES AND EVERYTHING ELSE OLFACTORY NERVE CN I ANTERIOR CRANIAL FOSSA CRISTA GALLI OF ETHMOID OLFACTORY FORAMINA IN CRIBIFORM PLATE OF ETHMOID BONE CN I OLFACTORY NERVE
Skull Base Volume 12 Month. Patients. Anterior/Midline. Pituitary CSF Leak. Lateral. Craniocervical Junction
 UC SF 2 11/7/2009 Skull Base Surgery in 2009 Ivan El-Sayed MD, FACS Director- Otolaryngology Minimally Invasive Skull Base Surgery Program Department Otolaryngology-Head and Neck Surgery University of
UC SF 2 11/7/2009 Skull Base Surgery in 2009 Ivan El-Sayed MD, FACS Director- Otolaryngology Minimally Invasive Skull Base Surgery Program Department Otolaryngology-Head and Neck Surgery University of
What was going on. Thyroid Related Orbitopathy. Pathophysiology. Definition GALLO EYE AND FACIAL PLASTIC SURGERY 3/16/2017
 GALLO EYE AND FACIAL PLASTIC SURGERY What was going on A. She found out the increase to her Premium and Deductible for employee health care next year B. She is getting an over agressive Physical Exam by
GALLO EYE AND FACIAL PLASTIC SURGERY What was going on A. She found out the increase to her Premium and Deductible for employee health care next year B. She is getting an over agressive Physical Exam by
Patterns of orbital disorders
 ISSN: 2250-0359 Volume 4 Issue 3.5 2014 Patterns of orbital disorders Balasubramanian Thiagarajan Stanley Medical College Abstract: This article discusses various patterns of presentations of orbital lesions.
ISSN: 2250-0359 Volume 4 Issue 3.5 2014 Patterns of orbital disorders Balasubramanian Thiagarajan Stanley Medical College Abstract: This article discusses various patterns of presentations of orbital lesions.
MAXILLA, ORBIT & PTERYGOPALATINE FOSSA. Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine
 MAXILLA, ORBIT & PTERYGOPALATINE FOSSA Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine Maxilla MAXILLA Superior, middle, and inferior meatus Frontal
MAXILLA, ORBIT & PTERYGOPALATINE FOSSA Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine Maxilla MAXILLA Superior, middle, and inferior meatus Frontal
Dr. Sami Zaqout, IUG Medical School
 The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma The face is vital to human appearance and function. Facial injuries can impair a patient
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma The face is vital to human appearance and function. Facial injuries can impair a patient
EYE TRAUMA: INCIDENCE
 Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Proptosis due to otolaryngology causes a study
 From the SelectedWorks of Balasubramanian Thiagarajan March 29, 2013 Proptosis due to otolaryngology causes a study Balasubramanian Thiagarajan Srikamakshi Kothandaraman Available at: https://works.bepress.com/drtbalu/11/
From the SelectedWorks of Balasubramanian Thiagarajan March 29, 2013 Proptosis due to otolaryngology causes a study Balasubramanian Thiagarajan Srikamakshi Kothandaraman Available at: https://works.bepress.com/drtbalu/11/
Pictorial review of extraconal and osseous orbital pathology - what can be found 'around' the orbits?
 Pictorial review of extraconal and osseous orbital pathology - what can be found 'around' the orbits? Poster No.: C-2011 Congress: ECR 2013 Type: Educational Exhibit Authors: M. Meissnitzer, T. Meissnitzer,
Pictorial review of extraconal and osseous orbital pathology - what can be found 'around' the orbits? Poster No.: C-2011 Congress: ECR 2013 Type: Educational Exhibit Authors: M. Meissnitzer, T. Meissnitzer,
Anatomy of the orbit. Lay-out. Imaging technique. 3 x 3. brief overview of the basic anatomy of the orbit and its structures
 Anatomy of the orbit Prof. Pia C Sundgren MD, PhD Department of Diagnostic Radiology, Clinical Sciences, Lund University, Sweden Lay-out brief overview of the basic anatomy of the orbit and its structures
Anatomy of the orbit Prof. Pia C Sundgren MD, PhD Department of Diagnostic Radiology, Clinical Sciences, Lund University, Sweden Lay-out brief overview of the basic anatomy of the orbit and its structures
Technique Guide. Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures.
 Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
PTERYGOPALATINE FOSSA
 PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures.
 Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Transnasal Endoscopic Sinonasal Surgery
 Reda kamel, Cadaveric dissection 1 Transnasal Endoscopic Sinonasal Surgery Cadaver Dissection Guide For Endoscopic Sinus Surgery Cairo University Egypt Reda Kamel Professor of Rhinology Cairo University
Reda kamel, Cadaveric dissection 1 Transnasal Endoscopic Sinonasal Surgery Cadaver Dissection Guide For Endoscopic Sinus Surgery Cairo University Egypt Reda Kamel Professor of Rhinology Cairo University
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
PERIORBITAL SWELLING - COMPLICATION FROM ADJACENT STRUCTURES CASE REPORTS AND REVIEW OF LITERATURE
 VOLUME 26, NO. 3 JUNE 1985 PERIORBITAL SWELLING - COMPLICATION FROM ADJACENT STRUCTURES CASE REPORTS AND REVIEW OF LITERATURE K Sukumaran S Chandran N Janakarajah P K Garg Department of Ophthalmology Faculty
VOLUME 26, NO. 3 JUNE 1985 PERIORBITAL SWELLING - COMPLICATION FROM ADJACENT STRUCTURES CASE REPORTS AND REVIEW OF LITERATURE K Sukumaran S Chandran N Janakarajah P K Garg Department of Ophthalmology Faculty
Oral Surgery Dr. Labeed Sami جامعة تكريت كلية طب االسنان املرحلة اخلامسة م.د. لبيد سامي حسن
 جامعة تكريت كلية طب االسنان جراحة الفم مادة املرحلة اخلامسة م.د. لبيد سامي حسن 6102-6102 1 5 th stage Fracture zygomatic complex As the zygomatic bone is closely associated with the maxilla, frontal and
جامعة تكريت كلية طب االسنان جراحة الفم مادة املرحلة اخلامسة م.د. لبيد سامي حسن 6102-6102 1 5 th stage Fracture zygomatic complex As the zygomatic bone is closely associated with the maxilla, frontal and
Ophthalmic complications after surgery for nasal and sinus polyposis
 European Journal of Ophthalmology / Vol. 11 no. 3, 2001 / pp. 218-222 Ophthalmic complications after surgery for nasal and sinus polyposis P. VASSALLO, F. TRANFA, R. FORTE, A. D APONTE, D. STRIANESE, G.
European Journal of Ophthalmology / Vol. 11 no. 3, 2001 / pp. 218-222 Ophthalmic complications after surgery for nasal and sinus polyposis P. VASSALLO, F. TRANFA, R. FORTE, A. D APONTE, D. STRIANESE, G.
Six Things That Changed How I Manage Graves Disease
 Six Things That Changed How I Manage Graves Disease Anthony DeWilde, OD FAAO Kansas City VAMC 6 Things 1. Thyroid status 2. Pathogenesis 3. Ocular signs/symptoms 4. Labs 5. Smoking 6. Mental Health Graves
Six Things That Changed How I Manage Graves Disease Anthony DeWilde, OD FAAO Kansas City VAMC 6 Things 1. Thyroid status 2. Pathogenesis 3. Ocular signs/symptoms 4. Labs 5. Smoking 6. Mental Health Graves
TOTAL MAXILLECTOMY, ORBITAL EXENTERATION
 TOTAL MAXILLECTOMY, ORBITAL EXENTERATION CC-BY-NC 3.0 Johan Fagan Total maxillectomy refers to surgical resection of the entire maxilla. Resection includes the floor and medial wall of the orbit and the
TOTAL MAXILLECTOMY, ORBITAL EXENTERATION CC-BY-NC 3.0 Johan Fagan Total maxillectomy refers to surgical resection of the entire maxilla. Resection includes the floor and medial wall of the orbit and the
Considerations in Oncologic Resection (mandible & maxilla)
 Considerations in Oncologic Resection (mandible & maxilla) Jeeve Kanagalingam MA, FRCS (ORL-HNS), FAMS Consultant ENT / Head & Neck Surgeon Tan Tock Seng Hospital Assistant Professor Lee Kong Chian School
Considerations in Oncologic Resection (mandible & maxilla) Jeeve Kanagalingam MA, FRCS (ORL-HNS), FAMS Consultant ENT / Head & Neck Surgeon Tan Tock Seng Hospital Assistant Professor Lee Kong Chian School
Ocular Urgencies and Emergencies
 Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
The orbit-2. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-2 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Eyelids The eyelids (act like the curtains) protect the eye from injury and excessive light by their closure The upper eyelid
The orbit-2 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Eyelids The eyelids (act like the curtains) protect the eye from injury and excessive light by their closure The upper eyelid
Anatomic Relations Summary. Done by: Sohayyla Yasin Dababseh
 Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
Unit VIII Problem 8 Anatomy: Orbit and Eyeball
 Unit VIII Problem 8 Anatomy: Orbit and Eyeball - The bony orbit: it is protecting our eyeball and resembling a pyramid: With a base directed: anterolaterally. And an apex directed: posteromedially. Notes:
Unit VIII Problem 8 Anatomy: Orbit and Eyeball - The bony orbit: it is protecting our eyeball and resembling a pyramid: With a base directed: anterolaterally. And an apex directed: posteromedially. Notes:
University of Florida ORBIT
 University of Florida ORBIT Dog Airedale Bulldog Great Dane Cat Horse bones EOM in fascial slings Periorbita: orbital septum to tarsal plate Periosteum of optic canal to optic nerve dura Tenon s capsule
University of Florida ORBIT Dog Airedale Bulldog Great Dane Cat Horse bones EOM in fascial slings Periorbita: orbital septum to tarsal plate Periosteum of optic canal to optic nerve dura Tenon s capsule
Assessment and Management of Ocular Trauma. Disclosure I have no direct financial interests in today s subject matter. 3/25/2019. Normal Eye Anatomy
 Assessment and Management of Ocular Trauma Samiksha Fouzdar Jain, MD,FRCS Department of Ophthalmology & Visual Sciences Truhlsen Eye Institute Disclosure I have no direct financial interests in today s
Assessment and Management of Ocular Trauma Samiksha Fouzdar Jain, MD,FRCS Department of Ophthalmology & Visual Sciences Truhlsen Eye Institute Disclosure I have no direct financial interests in today s
Bones Ethmoid bone Inferior nasal concha Lacrimal bone Maxilla Nasal bone Palatine bone Vomer Zygomatic bone Mandible
 splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
CLINICAL ASSESSMENT OF PATIENTS WITH GRAVES ORBITOPATHY
 44 MEDICINSKI GLASNIK / str. 44-48 Biljana Nedeljković-Beleslin 1 CLINICAL ASSESSMENT OF PATIENTS WITH GRAVES ORBITOPATHY Abstract: Clinical examination is the basis of a good assessment of a patient with
44 MEDICINSKI GLASNIK / str. 44-48 Biljana Nedeljković-Beleslin 1 CLINICAL ASSESSMENT OF PATIENTS WITH GRAVES ORBITOPATHY Abstract: Clinical examination is the basis of a good assessment of a patient with
C. Douglas Phillips MD FACR Director of Head and Neck Imaging Weill Cornell Medical College/NewYork-Presbyterian Hospital
 C. Douglas Phillips MD FACR Director of Head and Neck Imaging Weill Cornell Medical College/NewYork-Presbyterian Hospital Disclosures Neither I nor any family members have any pertinent financial relations
C. Douglas Phillips MD FACR Director of Head and Neck Imaging Weill Cornell Medical College/NewYork-Presbyterian Hospital Disclosures Neither I nor any family members have any pertinent financial relations
Maxillofacial Injuries Practical Tips
 Saturday, October 29, 2016 Maxillofacial Injuries Practical Tips Suyash Mohan MD, PDCC THE ROOTS OF PENN RADIOLOGY RADIOLOGICAL Assistant Professor of Radiology Assistant Professor of Neurosurgery Neuroradiology
Saturday, October 29, 2016 Maxillofacial Injuries Practical Tips Suyash Mohan MD, PDCC THE ROOTS OF PENN RADIOLOGY RADIOLOGICAL Assistant Professor of Radiology Assistant Professor of Neurosurgery Neuroradiology
Transnasal endoscopic approach in the treatment of Graves ophthalmopathy: The value of a medial periorbital strip
 European Annals of Otorhinolaryngology, Head and Neck diseases (2010) 127, 97 103 ORIGINAL CLINICAL RESEARCH Transnasal endoscopic approach in the treatment of Graves ophthalmopathy: The value of a medial
European Annals of Otorhinolaryngology, Head and Neck diseases (2010) 127, 97 103 ORIGINAL CLINICAL RESEARCH Transnasal endoscopic approach in the treatment of Graves ophthalmopathy: The value of a medial
Expanding Role of Orbital Decompression in Aesthetic Surgery
 Oculoplastic Surgery Preliminary Report Expanding Role of Orbital Decompression in Aesthetic Surgery Aesthetic Surgery Journal 2017, 1 7 2017 The American Society for Aesthetic Plastic Surgery, Inc. Reprints
Oculoplastic Surgery Preliminary Report Expanding Role of Orbital Decompression in Aesthetic Surgery Aesthetic Surgery Journal 2017, 1 7 2017 The American Society for Aesthetic Plastic Surgery, Inc. Reprints
CSF Leaks. Abnormal communication between the subarachnoid space and the tympanomastoid space or nasal cavity. Presenting symptoms:
 CSF Leaks Steven Wright, M.D. Faculty Advisor: Matthew Ryan, M.D. The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2005 CSF Leaks Abnormal communication
CSF Leaks Steven Wright, M.D. Faculty Advisor: Matthew Ryan, M.D. The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2005 CSF Leaks Abnormal communication
SINUS SURGERY. Dr Zenia Chow MBBS(hons), FRACS
 SINUS SURGERY Dr Zenia Chow MBBS(hons), FRACS Facial Plastic & Reconstructive Surgeon Otolaryngology, Head and Neck Surgeon ENDOSCOPIC SINUS SURGERY/FESS What are sinuses The sinuses are a connected system
SINUS SURGERY Dr Zenia Chow MBBS(hons), FRACS Facial Plastic & Reconstructive Surgeon Otolaryngology, Head and Neck Surgeon ENDOSCOPIC SINUS SURGERY/FESS What are sinuses The sinuses are a connected system
Major orbital complications of endoscopic sinus surgery
 598 Moorfields Eye Hospital, London EC1V 2PD, UK C Rene G E Rose R Lenthall I Moseley Correspondence to: Mr G E Rose, Orbital Clinic, Moorfields Eye Hospital, City Road, London EC1V 2PD, UK Accepted 20
598 Moorfields Eye Hospital, London EC1V 2PD, UK C Rene G E Rose R Lenthall I Moseley Correspondence to: Mr G E Rose, Orbital Clinic, Moorfields Eye Hospital, City Road, London EC1V 2PD, UK Accepted 20
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit
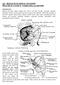 213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit OSTEOLOGY Identify the bones which comprise the walls of the orbit: maxilla, zygomatic, ethmoid, lachrymal, frontal, and
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit OSTEOLOGY Identify the bones which comprise the walls of the orbit: maxilla, zygomatic, ethmoid, lachrymal, frontal, and
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Evaluation of Extraocular Muscle Enlargement in Dysthyroid Ophthalmopathy
 Evaluation of Extraocular Muscle Enlargement in Dysthyroid Ophthalmopathy Yoko Murakami*,, Takashi Kanamoto*,, Toshikazu Tuboi*,, Toshine Maeda* and Yoichi Inoue* *Olympia Eye Hospital, Tokyo, Japan; Department
Evaluation of Extraocular Muscle Enlargement in Dysthyroid Ophthalmopathy Yoko Murakami*,, Takashi Kanamoto*,, Toshikazu Tuboi*,, Toshine Maeda* and Yoichi Inoue* *Olympia Eye Hospital, Tokyo, Japan; Department
GNK485 The eye and related structures. Prof MC Bosman 2012
 GNK485 The eye and related structures Prof MC Bosman 2012 Surface anatomy Bony orbit Eyeball and Lacrimal apparatus Extra-ocular muscles Movements of the eye Innervation Arterial supply and venous drainage
GNK485 The eye and related structures Prof MC Bosman 2012 Surface anatomy Bony orbit Eyeball and Lacrimal apparatus Extra-ocular muscles Movements of the eye Innervation Arterial supply and venous drainage
Omran Saeed. Luma Taweel. Mohammad Almohtaseb. 1 P a g e
 2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
Lateral Orbitotomy in the Management of Challenging Exotropia
 Lateral Orbitotomy in the Management of Challenging Exotropia Yahalom C (1, 2), Mc Nab A (3), Ben Simon G (3), Kowal L (1). 1- Centre for Eye Research Australia and Ocular Motility Clinic, Royal Victorian
Lateral Orbitotomy in the Management of Challenging Exotropia Yahalom C (1, 2), Mc Nab A (3), Ben Simon G (3), Kowal L (1). 1- Centre for Eye Research Australia and Ocular Motility Clinic, Royal Victorian
Reasons for Failure and Surgical Revisions. Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology
 Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Graves Ophthalmopathy Advances in Diagnosis and Treatment CONSTANCE L. FRY, MD ASSOCIATE PROFESSOR OF OPHTHALMOLOGY UT HEALTH SAN ANTONIO
 Graves Ophthalmopathy Advances in Diagnosis and Treatment CONSTANCE L. FRY, MD ASSOCIATE PROFESSOR OF OPHTHALMOLOGY UT HEALTH SAN ANTONIO Ophthalmic Manifestations GO is the #1 cause of unilateral and
Graves Ophthalmopathy Advances in Diagnosis and Treatment CONSTANCE L. FRY, MD ASSOCIATE PROFESSOR OF OPHTHALMOLOGY UT HEALTH SAN ANTONIO Ophthalmic Manifestations GO is the #1 cause of unilateral and
Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
 Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
Ophthalmic Trauma Update
 Ophthalmic Trauma Update Richard S. Davidson, M.D. Professor of Ophthalmology Vice Chair for Quality and Clinical Affairs UCHealth Eye Center University of Colorado School of Medicine August 5, 2017 Financial
Ophthalmic Trauma Update Richard S. Davidson, M.D. Professor of Ophthalmology Vice Chair for Quality and Clinical Affairs UCHealth Eye Center University of Colorado School of Medicine August 5, 2017 Financial
AFFECTIONS OF ORBIT IN ANIMALS
 AFFECTIONS OF ORBIT IN ANIMALS Anatomical considerations: The orbit is cone-shaped bony cavity and is incomplete laterally. Formed by six bones: frontal, lacrimal, sphenoid, palatine, zygomatic and maxillary.
AFFECTIONS OF ORBIT IN ANIMALS Anatomical considerations: The orbit is cone-shaped bony cavity and is incomplete laterally. Formed by six bones: frontal, lacrimal, sphenoid, palatine, zygomatic and maxillary.
Ocular and Periocular Trauma. Tina Rutar, MD. Assistant Professor of Ophthalmology and Pediatrics. Director, Visual Center for the Child
 Ocular and Periocular Trauma Tina Rutar, MD Assistant Professor of Ophthalmology and Pediatrics Director, Visual Center for the Child University of California, San Francisco Phone: 415-353-2560 Fax: 415-353-2468
Ocular and Periocular Trauma Tina Rutar, MD Assistant Professor of Ophthalmology and Pediatrics Director, Visual Center for the Child University of California, San Francisco Phone: 415-353-2560 Fax: 415-353-2468
Lower Eyelid Malposition
 Oculoplastic Surgeon s DDX for the Red Eye Geeta Belsare Been,MD The Center for Facial Plastic Surgery Barrington, IL Lower Eyelid Malposition Ectropion Involutional Cicatricial Paralytic Entropion Involutional
Oculoplastic Surgeon s DDX for the Red Eye Geeta Belsare Been,MD The Center for Facial Plastic Surgery Barrington, IL Lower Eyelid Malposition Ectropion Involutional Cicatricial Paralytic Entropion Involutional
Push Pull Technique for the Management of a Selected Superomedial Intraorbital Lesion
 THIEME Case Report e105 Push Pull Technique for the Management of a Selected Superomedial Intraorbital Lesion Paolo Castelnuovo, MD 1,4 Giacomo Fiacchini, MD 2 Francesca Romana Fiorini, MD 3 Iacopo Dallan,
THIEME Case Report e105 Push Pull Technique for the Management of a Selected Superomedial Intraorbital Lesion Paolo Castelnuovo, MD 1,4 Giacomo Fiacchini, MD 2 Francesca Romana Fiorini, MD 3 Iacopo Dallan,
Original Article Effect of lamina papyracea ingression on orbito-ocular complications after functional endoscopic sinus surgery
 Int J Clin Exp Med 2016;9(6):10317-10321 www.ijcem.com /ISSN:1940-5901/IJCEM0025371 Original Article Effect of lamina papyracea ingression on orbito-ocular complications after functional endoscopic sinus
Int J Clin Exp Med 2016;9(6):10317-10321 www.ijcem.com /ISSN:1940-5901/IJCEM0025371 Original Article Effect of lamina papyracea ingression on orbito-ocular complications after functional endoscopic sinus
Functional Endoscopic Sinus Surgery
 WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
The Nose and Sinuses. Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital
 The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
Carotid Cavernous Fistula
 Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
